Abstract
Valproic acid (VPA), an established antiepileptic and antimanic drug, has recently emerged as a promising neuroprotective agent. Among its many cellular targets, VPA has been recently demonstrated to be an effective inhibitor of histone deacetylases. Accordingly, we have adopted a schedule of dietary administration (2% VPA added to the chow) that results in a significant inhibition of histone deacetylase activity and in an increase of histone H3 acetylation in brain tissues of 4 weeks-treated rats. We have tested this schedule of VPA treatment in an animal model of Parkinson’s disease (PD), in which degeneration of nigro-striatal dopaminergic neurons is obtained through sub-chronic administration of the mitochondrial toxin, rotenone, via osmotic mini pumps implanted to rats. The decrease of the dopaminergic marker tyrosine hydroxylase in substantia nigra and striatum caused by 7 days toxin administration was prevented in VPA-fed rats. VPA treatment also significantly counteracted the death of nigral neurons and the 50% drop of striatal dopamine levels caused by rotenone administration. The PD-marker protein α-synuclein decreased, in its native form, in substantia nigra and striatum of rotenone-treated rats, while monoubiquitinated α-synuclein increased in the same regions. VPA treatment counteracted both these α-synuclein alterations. Furthermore, monoubiquitinated α-synuclein increased its localization in nuclei isolated from substantia nigra of rotenone-treated rats, an effect also prevented by VPA treatment. Nuclear localization of α-synuclein has been recently described in some models of PD and its neurodegenerative effect has been ascribed to histone acetylation inhibition. Thus, the ability of VPA to increase histone acetylation is a novel candidate mechanism for its neuroprotective action.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Valproic acid (VPA, 2-propylpentanoic acid), a medium-branched chain fatty acid, has been used for decades as an antiepileptic and antimanic drug (Löscher 2002; Bowden 2003; Rogawski and Löscher 2004; Fountoulakis et al. 2005; Bialer and Yagen 2007). Recently, VPA has emerged to be a neuroprotective drug, promoting survival of neurons challenged by neurodegenerative insults and representing a potential therapeutic tool for both acute and chronic neurodegenerative diseases (Morland et al. 2004; Chuang 2005; Kim et al. 2007; Eleuteri et al. 2009; Monti et al. 2009). In addition to the reported wide-ranging VPA actions on neurotransmitter systems, ion channels, receptors, cellular signaling pathways, and transcription regulation (Manji et al. 1999; Chuang 2005; Monti et al. 2009), novel interest has been recently raised by the discovery of its inhibitory role on histone deacetylases (HDACs), a major class of enzymes operating in epigenetic regulation of cell function (Phiel et al. 2001; Gottlicher et al. 2001, 2004).
Regarding Parkinson’s disease (PD), relatively dated clinical data reported no amelioration of patients treated with VPA (Price et al. 1978; Nutt et al. 1979). However, recent in vitro studies have raised novel interest on the possible use of VPA in PD-like neurodegeneration. In neuroblastoma cells, apoptosis induced by rotenone, an inhibitor of mitochondrial complex 1, which induces PD-like neurodegeneration in vivo, was attenuated by VPA treatment (Pan et al. 2005). In another in vitro PD model, midbrain dopaminergic neurons cultured in a mixed condition with glial cells, VPA protected neurons from the dopaminergic toxin, 1-methyl-phenylpyridinium (MPP+), by stimulating the release of trophic substances from glia (Chen et al. 2006). In a study mimicking the inflammatory condition characterizing chronic neurodegenerative diseases, VPA protected cultured dopaminergic neurons from over-activated microglia-induced degeneration, by promoting microglia apoptosis (Chen et al. 2007). Using another PD-mimetic toxin, 6-hydrohydopamine (6-OHDA) on cerebellar granule neurons in culture, we recently found that VPA protected these neurons by increasing α-synuclein expression and preventing its monoubiquitination and nuclear translocation (Monti et al. 2007). Interestingly, a link between VPA neuroprotection and increased α-synuclein expression was also found in the same neurons subjected to a different neurotoxic insult, i.e., glutamate excitotoxicity (Leng and Chuang 2006).
These in vitro results prompted us to test, for the first time in vivo, possible neuroprotection of VPA on a recognized animal model of PD, the rotenone-induced degeneration of the rat dopaminergic nigral neurons projecting to the striatum (Bertarbet et al. 2000; Sherer et al. 2003a). Here we show that the depletion of nigro-striatal dopaminergic neurons caused by subchronic (7 days through osmotic mini pumps) rotenone administration was significantly counteracted by long-term (4 + 1 weeks) administration of VPA added to chow. Furthermore, the alterations of α-synuclein caused by rotenone, consisting in a selective decrease of the native protein and in an increase of its monoubiquitination in substantia nigra and striatum, were reversed by VPA.
Materials and Methods
Animals and Surgery
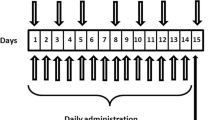
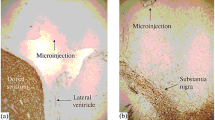
Male Wistar rats from Harlan Nossan, weighing 200–220 g at the beginning of the treatments, were used throughout the study. All animals were maintained on a 12:12 h light/dark cycle and given food and water ad libitum. The experiments were carried out in agreement with the Italian and European Community laws on the use of animals for experimental purposes. The experimental protocols were approved by a local bioethical committee and the experiments were performed under veterinary supervision. After acclimatation, rats of the VPA groups were fed for 4 weeks with standard chow added with 2% sodium valproate (Sigma, St Louis, MO). This regimen has been previously shown to result in the same rats in blood levels of 42 ± 6 mg/l valproic acid (Hao et al. 2004), which is close to the human therapeutic window (McElroy and Keck 1995). As previously reported (Eleuteri et al. 2009), daily intake of VPA was in the range of 1.4 g/Kg and this dietary regimen resulted in slight decrease of daily food intake and in significant decrease of body weight gain. After 4-week treatment, rats weighting 280–300 g (VPA-fed) or 330–350 g (standard diet) received 3 mg/kg/day of rotenone for further 7 days, through osmotic mini pumps implanted subcutaneously under light ether anesthesia. Alzet osmotic mini pumps (model 2ML1, Alzet Corporation, Palo Alto, CA) were filled with rotenone dissolved in equal volumes of dimethylsulfoxide (DMSO) and polyethylene glycol (PEG) and implanted under the skin on the back of each animal. Control rats received vehicle, DMSO/PEG (Sigma) (1:1) (Betarbet et al. 2000; Sherer et al. 2003a). During this period rats continued to receive the standard or the VPA-added diet. At the end of treatment, rats were killed by decapitation, the brains were sliced with a tissue chopper and the samples from the various brain regions were collected by micro-dissection on a cold plate under a stereomicroscope. To prepare total protein samples for western blot analysis the tissues were immediately frozen in dry ice and kept in the deep freezer until used. Then, they were homogenized in 50 mM Tris containing 5 mM EDTA, 0.1% SDS and a protease inhibitor cocktail (all chemicals from Sigma) and total protein content was determined (Lowry et al. 1951).
Nuclei–cytosol Separation
To extract separately nucleic and cytosolic proteins (Caruccio and Banerjee 1999), tissues from different brain areas were homogenized in an extraction buffer with low salt (20 mM HEPES, pH 7.9, 10 mM NaCl, 3 mM MgCl2, 0.1% Nonidet P-40, 10% glycerol, 0.2 mM EDTA, 1 mM dithiothreitol (DTT), protease inhibitor cocktails, all from Sigma) and left on ice for 10–15 min with occasional tapping. The nuclei were pelleted by centrifuging at 700×g for 5 min at 4°C. The cytoplasmic supernatant fraction was collected in another Eppendorf tube. The nuclei were washed with 200 μl of a washing buffer (20 mM HEPES, pH 7.9, 0.2 mM EDTA, 20% glycerol, 1 mM DTT, protease inhibitor cocktails) to remove NP-40 and centrifuged at 700×g for 5 min at 4°C. The pelleted nuclei were then resuspended into 60 μl of an extraction buffer with salt (20 mM HEPES, pH 7.9, 400 mM NaCl, 0.2 mM EDTA, 20% glycerol, 1 mM DTT, protease and phosphatase inhibitor cocktails) on ice for 45 min with periodic mixing by tapping to extract the nuclear proteins. Following centrifugation at 14,500×g for 15 min at 4°C, the supernatants were removed. The cytoplasmic fraction was further clarified by adding 1/3 volume of a cytoplasmic extraction clarification buffer (20 mM HEPES, pH 7.9, 400 mM NaCl, 0.2 mM EDTA, 40% glycerol, 1 mM DTT, protease and phosphatase inhibitor cocktails) for 30 min at 4°C to equilibrate the cytoplasmic proteins with NaCl, followed by centrifugation at 14,500×g for 15 min. Total protein content was measured in both the cytoplasmic and the nuclear fractions (Lowry et al. 1951) before to aliquot and store them at −80°C. The samples were subsequently subjected to western blot analysis and some of the nuclear extracts were also used to measure histone deacetylase activity, as described below.
Western Blotting
Equal amounts of protein (30 μg for total extracts or 20 μg for nuclear and cytosolic fractions) from each sample were diluted in 4× loading buffer (200 mM Tris/HCl pH 7.0, 8% Sodium Dodecyl Sulfate, 40% glycerol, 0.4% bromophenol blue, and 200 mM DL-Dithiothreitol, all chemicals were from Sigma), sonicated and resolved in 12.5% sodium dodecyl sulfate–polyacrylamide gel electrophoresis before electroblotting. Membranes were incubated with antibodies against tyrosine hydroxylase (TH), α-synuclein (polyclonal C-20, which recognize the full-length forms of the protein), or ubiquitin (monoclonal P4D1, which is the most widely used clone of antibodies to recognize free ubiquitin as well as the mono- and polyubiquitinated protein) or histone H3 or acetylated (lys 9/14) histone H3 (all from Santa Cruz Biotechnology Inc., Santa Cruz, CA, USA) or β-actin (Sigma), diluted 1:1000 in phosphate-buffered saline (PBS) containing 0.1% Tween 20 and 5% defatted dry milk (Bio-Rad Laboratories, Hercules, CA, USA). Membranes were then incubated with horseradish peroxidase-linked secondary antibodies (Santa Cruz Biotechnology) and visualized by enhanced chemiluminescence (Amersham International, Buckinghamshire, UK). The specificity of α-synuclein antibody was tested by using a specific blocking peptide (Santa Cruz Biotechnology). The films were scanned and densitometry was performed using the software ‘NIH Image’ (Scion Image, Frederick, MD, USA). Quantitation of TH and α-synuclein was performed with reference to the invariant cytoskeletal protein, β-actin, as a loading control.
Immunoprecipitation
Tissues were homogenized in cold radioimmunoprecipitation (RIPA) buffer (50 mM Tris–HCl, pH 7.4, 150 mM NaCl, 1% NP-40, 0.25% Na-deoxycholate, 1 mM EDTA, 1 mM Na3VO4, 1 mM NaF, protease, and phosphatase inhibitor cocktails). The lysates were sonicated, pre-cleared for 30 min at 4°C with control IgG and protein A/G Plus agarose (Santa Cruz Biotechnology) and centrifuged at 1,000×g. Aliquots of the supernatants were incubated either with 2 μg (10 μl) of a monoclonal antibody against ubiquitin (clone P4D1; Santa Cruz Biotechnology) or of a polyclonal antibody against α-synuclein (C-20; Santa Cruz Biotechnology), together with 5 μg (20 μl) of protein A/G plus agarose and rocked at 4°C overnight. The protein G beads were pelleted and washed 3/4 times with RIPA buffer. The precipitates were resolved on 12.5% (wt/vol) sodium dodecyl sulfate–polyacrylamide gel electrophoresis and subjected to western blot analysis, as described above. Samples immunoprecipitated with the polyclonal anti-α-synuclein antibody (C-20; Santa Cruz Biotechnology) were detected with the monoclonal antibody against ubiquitin (clone P4D1; Santa Cruz Biotechnology) or, as controls, against either polyclonal (C-20; Santa Cruz Biotechnology) or monoclonal (clone 42; BD Biosciences Europe, Erembodegem, Belgium) α-synuclein or β-actin (Sigma). Homogenates immunoprecipitated with the monoclonal anti-ubiquitin antibody (clone P4D1; Santa Cruz Biotechnology) were reacted with the polyclonal anti-α-synuclein antibody (C-20; Santa Cruz Biotechnology) or with the polyclonal anti-ubiquitin antibody (FL-76; Santa Cruz Biotechnology), as controls.
Histone Deacetylase Activity
The activity of histone deacetylase was measured in the nuclear extracts from substantia nigra of control and 4-week VPA-fed rats by using a fluorometric assay kit (Biovision, Mountain View, CA 94043, USA). Briefly, equal amounts (50 μg) of each sample in duplicate were incubated in a 96-well plate with the fluorogenic substrate Boc-Lys(Ac)-AMC, at the final concentration of 400 μM, for 30 min at 37°C. The reaction was then stopped by adding a Lysine Developer and further incubated at 37°C for 30 min. Values were read in a Victor3V fluorimetric detector (PerkinElmer, Waltham, Massachusetts 02451, USA) with Ex. = 350–380 nm and Em. = 440–460 nm. A standard curve was prepared using known amounts (from 0 to 40 μM) of the Deacetylated Standard Boc-Lys-AMC. As negative controls, parallel samples were analyzed in the presence of the HDAC inhibitor Trichostatin A 20 μM and, as a positive control, measure of HDAC activity in HeLa nuclear extracts were run in parallel. The results were expressed as nmoles of deacetylated substrate/mg prot/h.
Immunohistochemistry
Animals were anaesthetized with ether and perfusion-fixed through heart with 4% paraformaldehyde in 0.1 mM phosphate buffer pH 7.4. Brains were removed, post-fixed overnight in the same fixative and washed in buffered 18% sucrose until sunk. Sections were cut with a freezing microtome at 40 μm thickness, permeabilized for 20 min with PBS containing 0.1% Triton X-100, followed by a 20-min incubation in methanol containing 0.3% H2O2 to quench endogenous peroxidase activity. Subsequently, sections were incubated for 30 min in PBS containing 2% normal goat serum to block non-specific binding sites. For immunohistochemical localization of tyrosine hydroxylase, we used a monoclonal antibody (TH-16) at a dilution of 1:10,000 (Sigma). Antibody exposure was performed overnight in the cold room, followed by a 90-min incubation with a secondary antibody HPR-linked (Amersham) and the immunoreaction was visualized using diaminobenzidine tetrahydrochloride as chromogen (Vectastain DAB Kit, Vector Laboratories, Burlingame, CA).
HPLC Analysis of Dopamine and Related Metabolites
Tissue levels of dopamine (DA) and its metabolites, 3,4-dihydroxyphenylacetic acid (DOPAC) and homovanillic acid (HVA) were quantified by high performance liquid chromatography (HPLC). Briefly, frozen striatum slices previously dissected from rat brain belonging to the three experimental groups were homogenized by sonication in 20 volumes of 0.1 M perchloric acid (HClO4). A small volume (20 μl) of the homogenate was collected for total protein content determination, while the remaining sample was centrifuged at 12,000g for 5 min at RT. In order to analyze the DA content, diluted aliquots of each sample were further extracted and purified on a precolumn cartridge system on line with the chromatographic apparatus, before column separation. For DOPAC and HVA levels determination, diluted aliquots of the same samples were directly injected into an automated reversed-phase HPLC system coupled with a colorimetric electrochemical detector. Analytical conditions for both DA and its metabolites were selected according to those previously described (Grossi et al. 1991).
DNA Fragmentation Assay
Cell Death Detection ELISA PLUS kit (Roche Diagnostics GmbH, DE-68305 Mannheim, Germany) was used to measure DNA fragmentation as an index of cell death in the substantia nigra from rats belonging to the different groups. The assay was performed following the manufacturer’s instructions, with few modifications (White and Barone 2001; Monti and Contestabile 2003). Collected samples kept in the deep freezer were gently homogenized in 4 volumes of lysis buffer and centrifuged twice at 200×g for 10 min. Supernatants used for the determination were read in a microplate reader at the end of reaction (Bio-Rad).
Statistical Analysis
All results were subjected to statistical analysis with one-way ANOVA followed by Bonferroni’s post hoc comparison test or with Student’s t-test, in order to evaluate the significance of the differences.
Results
Subcutaneous administration of rotenone at the dosage used in the present study resulted in death of some of the treated animals (8 out of 23) and in development of motor disturbances (reduced motor activity and rigidity) in several of the surviving ones. None of the vehicle-treated or VPA-fed, rotenone-treated animals died or showed similar motor disturbances at a comparable extent.
Western blot analysis of whole homogenates from the various brain regions dissected after 7 days of rotenone treatment showed a sizable decrease of the marker enzyme for dopaminergic neurons, TH, in the substatia nigra and striatum (Fig. 1a). Quantification of western blots confirmed the decrease in the expression of TH in these two regions of rotenone-treated rats, while no alterations were noticed in other brain regions taken as controls, such as the cortex, hippocampus, and cerebellum (Fig. 1b). Chronic dietary treatment with VPA abrogated the effect of rotenone administration on TH levels in the substantia nigra and striatum (Fig. 1c, d). Noticeably, VPA treatment per se, significantly increased the basal expression of TH in the substantia nigra but not in the striatum (Fig. 1c, d) or in other brain regions (not shown). The selective decrease of TH in the substantia nigra and striatum was in line with the known sensitivity of nigro-striatal dopaminergic neurons to rotenone toxicity (Sherer et al. 2003b; Meurers et al. 2008). To confirm that the observed decrease of TH levels was actually related to degeneration of nigro-striatal dopaminergic neurons and that VPA protected these neurons from rotenone toxicity we sought evidence from different experimental approaches. Immunohistochemistry for TH revealed a substantial decrease of stained cells in the substantia nigra of rotenone-treated rats and this deficit was largely rescued by VPA administration (Fig. 2a). The toxic effect of rotenone administration towards nigral neurons was quantitatively estimated through the use of a fragmented DNA detection kit previously used to assess cell death in brain tissue (White and Barone 2001; Monti and Contestabile 2003). Samples of the substantia nigra collected from rats subjected to rotenone administration from 6 days showed a remarkably high level of cell death compared to controls and VPA treatment reversed this effect (Fig. 2b). In the striatum of the same rats, rotenone treatment resulted in 50% decrease of dopamine level and this effect was significantly, even if not completely, counteracted by chronic VPA administration (Fig. 2c). Measurement in the same samples of the two main dopamine metabolites, DOPAC and HVA, allowed us to calculate a significant increase of the ratio DOPAC + HVA/Dopamine, indicative of an increased dopamine turn-over, caused by the rotenone and the rotenone + VPA treatments (Fig. 2d).
Western Blot analysis of TH expression. a Representative Western Blot for TH and β-actin, as control, expression in substantia nigra (S.N.) and striatum (Str) from Rotenone- (R) and vehicle-treated rats (C). b Relative densitometry of TH expression in different brain areas, i.e., cerebellum (cer), cortex (ctx), hippocampus (hip), substantia nigra (S.N.), and striatum (Str), of Rotenone- and vehicle-treated rats. The level of TH was normalized for the β-actin content in each sample and the data were expressed as arbitrary units. Each bar represents the mean ± S.E. of 6–10 samples from different animals. ***P < 0.001, compared to control, Student’s t-test. c, d Western Blot analysis and its relative densitometry in vehicle-treated (C), Rotenone-treated (R), VPA + vehicle-treated (V), or VPA + Rotenone-treated (R + V) rats, shows that chronic VPA treatment completely abolishes the decrease of TH expression induced by Rotenone in both substantia nigra (S.N.) and striatum (Str) and, by itself, increases the basal TH expression in S.N. The level of TH was normalized for the β-actin content in each sample and the data were expressed as arbitrary units. Each bar represents the mean ± S.E. of 6–10 samples from different animals. *P < 0.05, ***P < 0.001, compared to control, ### P < 0.001, compared to Rotenone-treated animals, Bonferroni’s test after ANOVA
Effect of chronic VPA treatment on dopaminergic markers and cell death in Rotenone-treated rats. a Immunohistochemical analysis of TH expression in substantia nigra of vehicle-treated (C), Rotenone-treated (R), or VPA + Rotenone-treated (R + V) rats. Calibration bar, 200 μm. b Measure of DNA fragmentation in substantia nigra of vehicle-, Rotenone-, or VPA + Rotenone-treated rats. Data are expressed as Abs/mg prot and each bar represents the mean ± S.E. of 8–10 samples from different animals. c Quantification of dopamine content in the striatum of vehicle-, Rotenone-, or VPA + Rotenone-treated rats. Data are expressed as pmoles/μg prot and each bar represents the mean ± S.E. of 8–10 samples from different animals. d (DOPAC + HVA)/DA ratio in the striatum of vehicle-, Rotenone-, or VPA + Rotenone-treated rats. Each bar represents the mean ± S.E. of 8–10 samples from different animals. **P < 0.01, ***P < 0.001 compared to control and # P < 0.05, ## P < 0.01, ### P < 0.001 compared to Rotenone-treated animals, Bonferroni’s test after ANOVA
The chronic VPA treatment adopted here, has been previously shown to increase histone acetylation in brain tissue (Eleuteri et al. 2009). In the present study, we were able to show that the increased acetylation state of histone H3 in the nuclear fraction extracted from the substantia nigra of VPA-fed rats (Fig. 3a), correlated with a measurable inhibition of histone deacetylase activity in the same samples (Fig. 3b).
Chronic VPA treatment increases histone acetylation and inhibits HDACs activity in substantia nigra. a: Western blot analysis and its relative densitometry shows that the level of acetylated histone H3 on the lysines 9/14, normalized for total histone H3, increases in the substantia nigra nuclear fraction extracted from 4 week VPA-fed rats (V) compared to controls (C). Data are expressed as arbitrary units and each bar represents the mean ± S.E. of 6 samples from different animals. ***P < 0.001, compared to control, Student’s t-test. b HDACs activity in the same samples. Data are expressed in nmoles of acetylated substrate/mg prot/h. ***P < 0.001, compared to control, Student’s t-test
Decrease of TH in the substantia nigra and striatum was paralleled by a decreased expression in the same brain regions of the 19 kDa, native form of α-synuclein, while a substantial increase of a 27 kDa α-synuclein-immunoreactive band did occur (Fig. 4a–c). As we had previously observed that a protein of the same molecular size, found in neuronal cultures exposed to the dopaminergic toxin 6-OHDA, was a monoubiquitinated form of α-synuclein (Monti et al. 2007), we performed immunoprecipitation experiments to establish whether this was also the case for the present in vivo experiments. Immunoprecipitation of substantia nigra and striatum homogenates with α-synuclein antibody revealed an ubiquitin immunoreactive band of size corresponding to 27 kDa and the same was true for immunoprecipitates with ubiquitin antibody revealed with α-synuclein antibody (Fig. 4d). As described in the “Material and Methods” section, appropriate controls performed by crossing the antibodies used to challenge the immunoprecipitated samples gave negative results (data not shown), thus confirming that the 27 kDa α-synuclein-immunoreactive protein was a monoubiquitinated form of the protein. Furthermore, our results demonstrated that this form of α-synuclein was increased by rotenone treatment as the immunoreactive bands were much stronger than those of control animals (Fig. 4D).
Western Blot analysis (a) and the relative densitometries (b, c) of α-synuclein and β-actin, as control, expression in substantia nigra (S.N.) and striatum (Str) from Rotenone- (R) and vehicle-treated rats (C) and immunoprecipitation experiment that shows that the 27 kDa form of α-synuclein corresponds to monoubiquitinated α-synuclein (d). a, b, c Rotenone induces a significant decrease of the 19 kDa native form of α-synuclein and a significant increase of a 27 kDa form of the protein. The level of α-synuclein was normalized for the β-actin content in each sample and the data were expressed as arbitrary units. Each bar represents the mean ± S.E. of 6–10 samples from different animals. *P < 0.05, ***P < 0.001 compared to control, Student’s t-test. d Western Blot analysis (a) of immunoprecipitation for α-synuclein (polyclonal antibody) revealed with the monoclonal antibody against ubiquitin and of immunoprecipitation for ubiquitin (monoclonal antibody), stained with the polyclonal antibody against α-synuclein (see text for further details), performed in in substantia nigra (S.N.) and striatum (Str) from Rotenone- (R) and vehicle-treated rats (C)
Chronic treatment with VPA was also able to reverse the effect of rotenone treatment on α-synuclein, as both the decrease of the 19 kDa form and the increase of the 27 kDa form were abrogated (Fig. 5a–c). Interestingly, also in this case, VPA treatment was able, per se, to increase the level of the native form of α-synuclein in the substantia nigra and striatum (Fig. 5a–c). In a previous in vitro study (Monti et al. 2007), the monouniquitinated form of α-synuclein was found to be prevailingly localized in the nuclear compartment of injured neurons. We, therefore, performed a Western blot analysis on the cytosolic and the nuclear fractions of the substantia nigra of control and treated rats. The 19 kDa form of α-synuclein resulted decreased in the cytosolic fraction of rotenone-treated rats while the 27 kDa form was increased in the nuclear fraction of the substantia nigra of the same rats (Fig. 6a–c). In both cases, VPA treatment abrogated the altered expression caused by rotenone administration (Fig. 6a–c).
Chronic VPA treatment reverts the Rotenone effect on α-synuclein expression. Western Blot analysis and its relative densitometry in vehicle-treated (C), Rotenone-treated (R), VPA + vehicle-treated (V) or VPA + Rotenone-treated (R + V) rats are shown in a–c. a Representative Western Blot. b VPA treatment completely reverts the decrease of the 19 kDa form of α-synuclein induced by Rotenone in both substantia nigra (S.N.) and striatum (Str) and, by itself, increases the basal level of the 19 kDa form of α-synuclein in S.N. c VPA treatment counteracts the Rotenone-induced increase of the 27 kDa monoubiquitinated form of α-synuclein in both S.N. and Str. The level of α-synuclein was normalized for the β-actin content in each sample and the data were expressed as arbitrary units. Each bar represents the mean ± S.E. of 6–10 samples from different animals. *P < 0.05, ***P < 0.001, compared to control, ### P < 0.001, compared to Rotenone-treated animals, Bonferroni’s test after ANOVA
Western Blot analysis of α-synuclein nuclear–cytosol distribution in substantia nigra (S.N.) from vehicle-treated, Rotenone-treated and Rotenone + VPA-treated rats. a Representative Western Blot of α-synuclein expression in nuclear (n) and cytosolic (c) extracts from subtantia nigra (S.N.) of vehicle-treated (C), Rotenone-treated (R), or Rotenone + VPA-treated (R + V) rats. b The 19 kDa form of native α-synuclein is mainly present in the cytosolic compartment, where its expression decreases in Rotenone-treated rats, while VPA reverts this effect. c The 27 kDa monoubiquitinated form has a primary nuclear localization and its nuclear level increases in Rotenone-treated rats, while VPA almost completely abolishes this effect. Each bar represents the mean ± S.E. of 3–4 samples from different animals. **P < 0.01, ***P < 0.001, compared to control, # P < 0.05, compared to Rotenone-treated animals, Bonferroni’s test after ANOVA
Discussion
The present study was undertaken to demonstrate whether VPA was neuroprotective in an animal model of PD and, additionally, to verify whether alterations in the expression and the molecular state of the disease-marker protein, α-synuclein, caused by the neurotoxic challenge could be reverted by treatment with the same drug. Our novel results are that chronic dietary administration of VPA significantly protects nigro-striatal dopaminergic neurons from rotenone-induced degeneration and that the alterations of α-synuclein observed in rotenone-treated animals are brought back to the normal condition in VPA-fed rats. The neuroprotective effect of VPA correlates with inhibition of histone deacetylase activity and with increased histone acetylation in the substantia nigra. In the present experiments, we have focused our attention on the effect of VPA on histone deacetylase and histone acetylation state as this mechanism is emerging as a very important one in promoting neuronal survival (Jeong et al. 2003; Leng and Chuang 2006; Sinn et al. 2007). While the correlation we have found indicates a role for histone deacetylase inhibition in the neuroprotective effect of VPA, the multiple functions described for this drug do not allow us to exclude the contribution of other known molecular targets of VPA with well-characterized neuroprotective role such as, for instance, heath shock proteins, neurotrophins, and anti-apoptotic genes (Chuang 2005; Monti et al. 2009).
The experimental model used here, essentially corresponds to the model of animal Parkinsonism originally devised to obtain degeneration of nigro-striatal dopaminergic neurons in rats (Bertarbet et al. 2000; Sherer et al. 2003a, b). The model and the reasons for the peculiar sensitivity of nigro-striatal dopaminergic neurons to brain concentrations of rotenone that only partially inhibit mitochondrial complex 1 have been discussed elsewhere (Sherer et al. 2003b). Furthermore, a recent study has confirmed, at the level of regulation of gene expression, the preferential response of these neurons also to sub-toxic doses of rotenone (Meurers et al. 2008). In the present study, by using a standard dosage of rotenone administration (3 mg/Kg/day), continuously delivered through osmotic mini pumps, and by limiting the time of exposure to 7 days, we were able to obtain a sizable decrease of dopaminergic markers in the substantia nigra and striatum of the treated rats and to significantly revert the effect of the neurotoxic insult through chronic dietary administration of VPA that results in blood concentration of the drug close to the human therapeutic window (Hao et al. 2004). This neuroprotective effect correlated well with cell death data in the substantia nigra and with the survival data that demonstrated substantial mortality (around 30%) in rotenone-treated rats and no mortality at all in rats subjected to the same treatment but chronically fed with VPA. While this correlation is well-supported by the combination of neuroprotection and survival data, protection of nigro-striatal dopaminergic neurons may not be the sole determinant for VPA pro-survival effect, due to the vast array of neuroprotective actions promoted by VPA (Chuang 2005; Monti et al. 2009). The neuroprotective effect also correlated with a significant VPA-stimulated increase in the expression of both TH and α-synuclein in the substantia nigra. The VPA effect on positive regulation of TH has been previously observed at the mRNA expression level in the rat locus coeruleus and may be part of a more generalized ability of histone deacetylase inhibitors to regulate expression of TH gene both in vivo and in vitro (Sands et al. 2000; DeCastro et al. 2005; D’Souza et al. 2009). We demonstrate here that also TH protein is upregulated in its expression in the substantia nigra of rats chronically treated with VPA. Why this effect appears to be specific for brain regions characterized by neurons provided with constitutive high expression of TH, such as the locus coeruleus and the substantia nigra, should be interesting to investigate in the future. Regarding α-synuclein, VPA-induced up-regulation of this protein has been previously described in primary neuronal cultures and has been related to a neuroprotective action (Leng and Chuang 2006; Monti et al. 2007), while present results are the first demonstration of a similar effect in vivo.
Our results point at a role of α-synuclein in PD-related neurodegeneration that challenges the dominant concept which attributes a primary neurotoxic role to α-synuclein in PD pathogenesis, based on its fibrillary accumulation in Lewy bodies and to its mutations in heritable forms of the disease (Polymeropoulos et al. 1997; Krüger et al. 1998; Norris et al. 2004; Zarranz et al. 2004). A growing body of evidence, indeed, suggests that α-synuclein is a survival factor in neuronal cultures (Alves da Costa et al. 2002; Seo et al. 2002; Jensen et al. 2003; Leng and Chuang 2006; Monti et al. 2007). Furthermore, while contrasting results have been obtained regarding overexpression of α-synuclein on neurotoxicity toward nigral dopaminergic neurons in intact animals (Masliah et al. 2000; Matsuoka et al. 2001; Rathke-Hartlieb et al. 2001; Kirik et al. 2002; Yamada et al. 2004), transgenic overexpression was neuroprotective against herbicide (paraquat)-induced degeneration of nigral neurons (Manning-Bog et al. 2003). Interestingly, in this latter study (Manning-Bog et al. 2003), a dissociation was reported between the deposition of intraneuronal α-synuclein and neurodegeneration. Thus, α-synuclein may be involved in neurodegeneration not only through a gain of toxic function but also through a loss of neuroprotective defense. Our present data provide novel evidence for a neuroprotective role of normal expression of α-synuclein in a model of PD-like neurodegeneration, as rotenone-induced degeneration of nigro-striatal dopaminergic neurons was accompanied by comparable decrease of the physiological 19 kDa form of the protein. The fact that VPA significantly protects these neurons from the challenge of rotenone toxicity and, in parallel, restores the levels of the physiological form of α-synuclein constitutes, for the first time in vivo, a strong indication for a link between VPA neuroprotection and α-synuclein expression so far only described in neuronal cultures (Leng and Chuang 2006; Monti et al. 2007). As discussed above, the multiplicity of potential neuroprotective targets of VPA renders a univocal interpretation of the results difficult. However, the recently emerged neuroprotective role of α-synuclein and the evidence that VPA mediates hyperacetylation of histone H3 at the α-synuclein promoter, thus enhancing gene expression (Leng and Chuang 2006; Monti et al. 2007), strongly suggest that VPA neuroprotection and VPA regulation of α-synuclein expression observed in the present study are functionally related events. Our results, additionally disclose a novel way of processing α-synuclein that seems to be relevant to understand PD-like neurodegeneration of nigro-striatal dopaminergic neurons, i.e., the strong increase of monoubiquitinated α-synuclein restricted to brain areas affected by neurodegeneration. Also this neurodegeneration-dependent modification of α-synuclein was prevented by VPA treatment and this result further strengthens the link between VPA neuroprotection and maintenance of α-synuclein physiological state. Recent reports, indeed, have demonstrated that Lewy bodies contain a fraction of monoubiquitinated α-synuclein and that increased levels of monoubiquitinated α-synuclein are toxic to dopaminergic neurons (Engelender 2008; Rott et al. 2008). In primary neuronal cultures, we have recently shown that exposure to the dopaminergic neurotoxin, 6-OHDA, results in a situation very similar to the one reported here in vivo, namely decrease of native α-synuclein, increase of its monoubiquitinated form and restoration to normal state by VPA treatment (Monti et al. 2007). We, furthermore, observed that part of the monoubiquitinated α-synuclein translocated to the nuclei of cultured neurons subjected to the neurotoxic insult (Monti et al. 2007). This prompted us to study whether a similar process also happened in our animal model and we were able to show that in the substantia nigra of rotenone-treated rats, the nuclear fraction was actually enriched in monoubiquitinated α-synuclein, an effect that was fully abrogated by VPA treatment. While polyubiquitination drives proteins towards proteasome degradation, monoubiquitination regulates several cellular processes (reviewed by Hicke 2001). In particular, a role is emerging for monoubiquitination in the nuclear–cytoplasmic shuttling of several proteins and for the involvement of this process in pathological states (Salmena and Pandolfi 2007). The neuronal nuclear localization of α-synuclein is known from its discovery and is implicit in its name (Maroteaux et al. 1988), but it has been rarely described in vivo in a systematic way (Yu et al. 2007). It has been previously observed that in paraquat- and in rotenone-treated rodents, α-synuclein localizes to the nuclei of nigral cells (Goers et al. 2003; Feng et al. 2006). These data suggested that the nuclear localization of α-synuclein in substantia nigra could be correlated to PD-like neurodegeneration. This suggestion was strongly supported by recent data demonstrating that neurodegeneration was promoted by nuclear localization of α-synuclein in a dopaminergic cell line, as well as in transgenic flies (Kontopoulos et al. 2006). Furthermore, α-synuclein mutations found in some forms of familial PD, A30P and A53T, caused increased nuclear targeting of the protein in cell cultures (Kontopoulos et al. 2006). The nuclear presence of monoubiquitinated α-synuclein in both glia and neurons has been previously described in a rare neurodegenerative disease, multiple system atrophy (Lin et al. 2004; Yoshida 2007). Thus, convincing experimental data are emerging that suggest a precise correlation between the nuclear localization of α-synuclein and neurodegeneration. Our present results provide correlative evidence that this may also be the case for PD-like neurodegeneration. Why and how α-synuclein promotes neurodegeneration when localized to the nucleus is still unclear, but recent data have provided a possible explanation based on α-synuclein interference with histone function in PD-like neurodegeneration. In paraquat-treated mice, it has been shown that α-synuclein forms complex with histones and increases its fibrillation rate under these conditions (Goers et al. 2003). Moreover, neurotoxicity obtained by targeting α-synuclein to the nucleus results from inhibition of histone acetylation (Kontopoulos et al. 2006). Accordingly, the neurotoxic effect of nuclear α-synuclein is reversed by administration of histone deacetylase inhibitors (Kontopoulos et al. 2006). VPA is a well-established inhibitor of histone deacetylases (Göttlicher et al. 2001; Göttlicher 2004; Phiel et al. 2001) and our present observations confirm that its chronic administration actually inhibits histone deacetylase and increases histone H3 acetylation in the substantia nigra. Thus, the neuroprotective effect of VPA and the concomitant decrease of nuclear synuclein reported in the present report could be the combined effects of VPA action on histone acetylation.
In conclusion, our present results constitute, to our knowledge, the first evidence for a neuroprotective role of VPA in an animal model of PD and strongly corroborate previous results on VPA neuroprotection in models of PD-like neurodegeneration in culture (Pan et al. 2005; Chen et al. 2006, 2007; Monti et al. 2007). A recent study has shown that rotenone challenge regulates in nigral dopaminergic neurons the expression of a vast array of genes, some of which potentially dangerous while others neuroprotective (Meurers et al. 2008). By increasing histone acetylation in the same neurons, VPA may shift the balance towards expression of neuroprotective genes. Whether further studies will be able to confirm this hypothesis, novel perspectives will be opened for better comprehension of VPA action and for its possible use in therapy.
Abbreviations
- VPA:
-
Valproic acid
- PD:
-
Parkinson’s disease
- TH:
-
Tyrosine hydroxylase
- HDAC:
-
Histone deacetylase
- MPP+ :
-
1-Methyl-phenylpyridinium
- 6-OHDA:
-
6-Hydrohydopamine
- DMSO:
-
Dimethylsulfoxide
- PEG:
-
Polyethylene-glycol
- DOPAC:
-
Dihydroxyphenyl acetic acid
- HVA:
-
Homovanillic acid
References
Alves Da Costa C, Paitel E, Vincent B, Checler F (2002) Alpha-synuclein lowers p53-dependent apoptotic response of neuronal cells. Abolishment by 6-hydroxydopamine and implication for Parkinson’s disease. J Biol Chem 277:50980–50984
Betarbet R, Sherer TB, MacKenzie G, Garcia-Osuna M, Panov AV, Greenamyre JT (2000) Chronic systemic pesticide exposure reproduces features of Parkinson’s disease. Nat Neurosci 3:1301–1306
Bialer M, Yagen B (2007) Valproic acid: second generation. Neurotherapeutics 4:130–137
Bowden CL (2003) Valproate. Bipol Disord. 5:189–202
Caruccio L, Banerjee R (1999) An efficient method for simultaneous isolation of biologically active transcription factors and DNA. J Immunol Methods 230:1–10
Chen PS, Peng GS, Li G, Yang S, Wu X, Wang CC, Wilson B, Lu RB, Gean PW, Chuang DM, Hong JS (2006) Valproate protects dopaminergic neurons in midbrain neuron/glia cultures by stimulating the release of neurotrophic factors from astrocytes. Mol Psychiatry 11:1116–1125
Chen PS, Wang CC, Bortner CD, Peng GS, Wu X, Pang H, Lu RB, Gean PW, Chuang DM, Hong JS (2007) Valproic acid and other histone deacetylase inhibitors induce microglial apoptosis and attenuate lipopolysaccharide-induced dopaminergic neurotoxicity. Neuroscience 149:203–212
Chuang DM (2005) The antiapoptotic actions of mood stabilizers: molecular mechanisms and therapeutic potentials. Ann N Y Acad Sci 1053:195–204
D’Souza A, Onem E, Patel P, La Gamma EF, Nankova BB (2009) Valproic acid regulates catecholaminergic pathways by concentration-dependent threshold effects on TH mRNA synthesis and degradation. Brain Res 1247:1–10
DeCastro M, Nankova BB, Shah P, Patel P, Mally PV, Mishra R, La Gamma EF (2005) Short chain fatty acids regulate tyrosine hydroxylase gene expression through a cAMP-dependent signaling pathway. Mol Brain Res 142:28–38
Eleuteri S, Monti B, Brignani S, Contestabile A (2009) Chronic dietary administration of valproic acid protects neurons of the rat nucleus basalis magnocellularis from ibotenic acid neurotoxicity. Neurotox Res 15:127–132
Engelender S (2008) Ubiquitination of alpha-synuclein and autophagy in Parkinson’s disease. Autophagy 4:372–374
Feng Y, Liang ZH, Wang T, Qiao X, Liu HJ, Sun SG (2006) Alpha-synuclein redistributed and aggregated in rotenone-induced Parkinson’s disease rats. Neurosci Bull 22:288–293
Fountoulakis KN, Vieta E, Sanchez-Moreno J, Kaprinis SG, Goikolea JM, Kaprinis GS (2005) Treatment guidelines for bipolar disorder: a critical review. J Affect Disord 86:1–10
Goers J, Manning-Bog AB, McCormack AL, Millett IS, Doniach S, Di Monte DA, Uversky VN, Fink AL (2003) Nuclear localization of alpha-synuclein and its interaction with histones. Biochemistry 42:8465–8671
Göttlicher M (2004) Valproic acid: an old drug newly discovered as inhibitor of histone deacetylases. Ann Hematol 83:S91–S92
Göttlicher M, Minucci S, Zhu P, Krämer OH, Schimpf A, Giavara S, Sleeman JP, Lo Coco F, Nervi C, Pelicci PG, Heinzel T (2001) Valproic acid defines a novel class of HDAC inhibitors inducing differentiation of transformed cells. EMBO J 20:6969–6978
Grossi G, Bargossi AM, Lucarelli C, Paradisi R, Sprovieri C, Sprovieri G (1991) Improvements in automated analysis of catecholamines and related metabolites in biological samples by column-switching high-performance liquid chromatography. J Chromatogr 541:273–284
Hao Y, Creson T, Zhang L, Li P, Du F, Yuan P, Gould TD, Manji HK, Chen G (2004) Mood stabilizer valproate promotes ERK pathway-dependent cortical neuronal growth and neurogenesis. J Neurosci 24:6590–6599
Hicke L (2001) Protein regulation by monoubiquitin. Nat Rev Mol Cell Biol 2:195–201
Jensen PJ, Alter BJ, O’Malley KL (2003) Alpha-synuclein protects naive but not dbcAMP-treated dopaminergic cell types from 1-methyl-4-phenylpyridinium toxicity. J Neurochem 86:196–209
Jeong MR, Hashimoto R, Senatorov VV, Fujimaki K, Ren M, Lee MS, Chuang DM (2003) Valproic acid, a mood stabilizer and anticonvulsant, protects rat cerebral cortical neurons from spontaneous cell death: a role of histone deacetylase inhibition. FEBS Lett 542:74–78
Kim HJ, Rowe M, Ren M, Hong JS, Chen PS, Chuang DM (2007) Histone deacetylase inhibitors exhibit anti-inflammatory and neuroprotective effects in a rat permanent ischemic model of stroke: multiple mechanisms of action. J Pharmacol Exp Ther 321(3):892–901
Kirik D, Rosenblad C, Burger C, Lundberg C, Johansen TE, Muzyczka N, Mandel RJ, Björklund A (2002) Parkinson-like neurodegeneration induced by targeted overexpression of alpha-synuclein in the nigrostriatal system. J Neurosci 22:2780–2791
Kontopoulos E, Parvin JD, Feany MB (2006) Alpha-synuclein acts in the nucleus to inhibit histone acetylation and promote neurotoxicity. Hum Mol Genet 15:3012–3023
Krüger R, Kuhn W, Müller T, Woitalla D, Graeber M, Kösel S, Przuntek H, Epplen JT, Schöls L, Riess O (1998) Ala30Pro mutation in the gene encoding alpha-synuclein in Parkinson’s disease. Nat Genet 18:106–108
Leng Y, Chuang DM (2006) Endogenous alpha-synuclein is induced by valproic acid through histone deacetylase inhibition and participates in neuroprotection against glutamate-induced excitotoxicity. J Neurosci 26:7502–7512
Lin WL, DeLucia MW, Dickson DW (2004) Alpha-synuclein immunoreactivity in neuronal nuclear inclusions and neurites in multiple system atrophy. Neurosci Lett 354:99–102
Löscher W (2002) Basic pharmacology of valproate: a review after 35 years of clinical use for the treatment of epilepsy. CNS Drugs 16:669–694
Lowry OH, Rosenbrough RJ, Farr AL, Randall RJ (1951) Protein measurement with the Folin phenol reagent. J Biol Chem 193:265–275
Manji HK, Bebchuk JM, Moore GJ, Glitz D, Hasanat KA, Chen G (1999) Modulation of CNS signal transduction pathways and gene expression by mood-stabilizing agents: therapeutic implications. J Clin Psychiatry 60:27–39
Manning-Bog AB, McCormack AL, Purisai MG, Bolin LM, Di Monte DA (2003) Alpha-synuclein overexpression protects against paraquat-induced neurodegeneration. J Neurosci 23:3095–3099
Maroteaux L, Campanelli JT, Scheller RH (1988) Synuclein: a neuron-specific protein localized to the nucleus and presynaptic nerve terminal. J Neurosci 8:2804–2815
Masliah E, Rockenstein E, Veinbergs I, Mallory M, Hashimoto M, Takeda A, Sagara Y, Sisk A, Mucke L (2000) Dopaminergic loss and inclusion body formation in alpha-synuclein mice: implications for neurodegenerative disorders. Science 287:1265–1269
Matsuoka Y, Vila M, Lincoln S, McCormack A, Picciano M, LaFrancois J, Yu X, Dickson D, Langston WJ, McGowan E, Farrer M, Hardy J, Duff K, Przedborski S, Di Monte DA (2001) Lack of nigral pathology in transgenic mice expressing human alpha-synuclein driven by the tyrosine hydroxylase promoter. Neurobiol Dis 8:535–539
McElroy SL, Keck PE (1995) Misattribution of eating and obsessive-compulsive disorder symptoms to repressed memories of childhood sexual or physical abuse. Biol Psychiatry 37:48–51
Meurers BH, Zhu C, Fernagut PO, Richter F, Hsia YC, Fleming SM, Oh M, Elashoff D, Dicarlo CD, Seaman RL, Chesselet MF (2008) Low dose rotenone treatment causes selective transcriptional activation of cell death related pathways in dopaminergic neurons in vivo. Neurobiol Dis 33:182–192
Monti B, Contestabile A (2003) Selective alteration of DNA fragmentation and caspase activity in the spinal cord of aged rats and effect of dietary restriction. Brain Res 992:137–141
Monti B, Polazzi E, Batti L, Crochemore C, Virgili M, Contestabile A (2007) Alpha-synuclein protects cerebellar granule neurons against 6-hydroxydopamine-induced death. J Neurochem 103:518–530
Monti B, Polazzi E, Contestabile A (2009) Biochemical, molecular and epigenetic mechanisms of valproic acid neuroprotection. Curr Mol Pharmacol 2:95–109
Morland C, Boldingh KA, Iversen EG, Hassel B (2004) Valproate is neuroprotective against malonate toxicity in rat striatum: an association with augmentation of high-affinity glutamate uptake. J Cereb Blood Flow Metab 24(11):1226–1234
Norris EH, Giasson BI, Lee VM (2004) Alpha-synuclein: normal function and role in neurodegenerative diseases. Curr Top Dev Biol 60:17–54
Nutt J, Williams A, Plotkin C, Eng N, Ziegler M, Calne DB (1979) Treatment of Parkinson’s disease with sodium valproate: clinical, pharmacological, and biochemical observations. Can J Neurol Sci 6:337–343
Pan T, Li X, Xie W, Jankovic J, Le W (2005) Valproic acid-mediated Hsp70 induction and anti-apoptotic neuroprotection in SH-SY5Y cells. FEBS Lett 579:6716–6720
Phiel CJ, Zhang F, Huang EY, Guenther MG, Lazar MA, Klein PS (2001) Histone deacetylase is a direct target of valproic acid, a potent anticonvulsant, mood stabilizer, and teratogen. J Biol Chem 276:36734–36741
Polymeropoulos MH, Lavedan C, Leroy E, Ide SE, Dehejia A, Dutra A, Pike B, Root H, Rubenstein J, Boyer R, Stenroos ES, Chandrasekharappa S, Athanassiadou A, Papapetropoulos T, Johnson WG, Lazzarini AM, Duvoisin RC, Di Iorio G, Golbe LI, Nussbaum RL (1997) Mutation in the alpha-synuclein gene identified in families with Parkinson’s disease. Science 276:2045–2047
Price PA, Parkes JD, Marsden CD (1978) Sodium valproate in the treatment of levodopa-induced dyskinesia. J Neurol Neurosurg Psychiatr 41:702–706
Rathke-Hartlieb S, Kahle PJ, Neumann M, Ozmen L, Haid S, Okochi M, Haass C, Schulz JB (2001) Sensitivity to MPTP is not increased in Parkinson’s disease-associated mutant alpha-synuclein transgenic mice. J Neurochem 77:1181–1184
Rogawski MA, Löscher W (2004) The neurobiology of antiepileptic drugs. Nat Rev Neurosci 5:553–564
Rott R, Szargel R, Haskin J, Shani V, Shainskaya A, Manov I, Liani E, Avraham E, Engelender S (2008) Monoubiquitylation of alpha-synuclein by seven in absentia homolog (SIAH) promotes its aggregation in dopaminergic cells. J Biol Chem 283:3316–3328
Salmena L, Pandolfi PP (2007) Changing venues for tumour suppression: balancing destruction and localization by monoubiquitylation. Nat Rev Cancer 7:409–413
Sands SA, Guerra V, Morilak DA (2000) Changes in tyrosine hydroxylase mRNA expression in the rat locus coeruleus following acute or chronic treatment with valproic acid. Neuropsychopharmacology 22:27–35
Seo JH, Rah JC, Choi SH, Shin JK, Min K, Kim HS, Park CH, Kim S, Kim EM, Lee SH, Lee S, Suh SW, Suh YH (2002) Alpha-synuclein regulates neuronal survival via Bcl-2 family expression and PI3/Akt kinase pathway. FASEB J 16:1826–1828
Sherer TB, Kim JH, Betarbet R, Greenamyre JT (2003a) Subcutaneous rotenone exposure causes highly selective dopaminergic degeneration and alpha-synuclein aggregation. Exp Neurol 179:9–16
Sherer TB, Betarbet R, Kim JH, Greenamyre JT (2003b) Selective microglial activation in the rat rotenone model of Parkinson’s disease. Neurosci Lett 341:87–90
Sinn DI, Kim SJ, Chu K, Jung KH, Lee ST, Song EC, Kim JM, Park DK, Kun Lee S, Kim M, Roh JK (2007) Valproic acid- mediated neuroprotection in intracerebral hemorrhage via histone deacetylase inhibition and transcriptional activation. Neurobiol Dis 26:464–472
White LD, Barone S Jr (2001) Qualitative and quantitative estimates of apoptosis from birth to senescence in the rat brain. Cell Death Differ 8:345–356
Yamada M, Iwatsubo T, Mizuno Y, Mochizuki H (2004) Overexpression of alpha-synuclein in rat substantia nigra results in loss of dopaminergic neurons, phosphorylation of alpha-synuclein and activation of caspase-9: resemblance to pathogenetic changes in Parkinson’s disease. J Neurochem 91:451–461
Yoshida M (2007) Multiple system atrophy: alpha-synuclein and neuronal degeneration. Neuropathology 27:484–493
Yu S, Li X, Liu G, Han J, Zhang C, Li Y, Xu S, Liu C, Gao Y, Yang H, Uéda K, Chan P (2007) Extensive nuclear localization of alpha-synuclein in normal rat brain neurons revealed by a novel monoclonal antibody. Neuroscience 145:539–555
Zarranz JJ, Alegre J, Gómez-Esteban JC, Lezcano E, Ros R, Ampuero I, Vidal L, Hoenicka J, Rodriguez O, Atarés B, Llorens V, Gomez Tortosa E, del Ser T, Muñoz DG, de Yebenes JG (2004) The new mutation, E46K, of alpha-synuclein causes Parkinson and Lewy body dementia. Ann Neurol 55:164–173
Acknowledgments
The present work was supported by grants of the Italian Ministry for Universities and Research to A.C. (FIRB funding scheme) and M.V. (PRIN funding scheme). The authors wish to thank Dr. Gabriele Grossi of the Laboratorio Centralizzato, Policlinico S.Orsola-Malpighi, Bologna, for his assistance with dopamine measurements. The skilful technical assistance of Miss Monia Bentivogli is gratefully acknowledged.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Monti, B., Gatta, V., Piretti, F. et al. Valproic Acid is Neuroprotective in the Rotenone Rat Model of Parkinson’s Disease: Involvement of α-Synuclein. Neurotox Res 17, 130–141 (2010). https://doi.org/10.1007/s12640-009-9090-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12640-009-9090-5