Abstract
Objective
The present study aimed to examine nutritional risk factors such as poor appetite, malnutrition or obesity affecting health related quality of life in elderly.
Design and participants
This is a cross-sectional population-based study consisted of 407 elderly (142 men and 265 women) mean aged 71.7±6.54 years.
Measurements
Questionnaire including the demographic and general characteristics, health information, nutritional habits was performed by face-to-face interviews. Daily food consumption was assessed using 24-hour dietary recall. Mini Nutrition Assessment (MNA) and Mini Nutrition Assessment-Short Form (MNA-SF) were used for assessment of nutrition status. Appetite was evaluated using the Simplified Nutritional Appetite Questionnaire (SNAQ). Health related life quality scale (Short Form Health Survey-SF36) was used for evalution health related quality of life.
Results
According to MNA and MNA-SF 6.1%; 4.2% of elderly people were malnutrition and 40.3%; 21.9% of them were at risk of malnutrition respectively. Accordingly, SNAQ 28.7% of elderly were risk at loss of weight. Health related quality of life scores of women were significantly lower than men. Good nutritional (MNA-SF) and good appetite (SNAQ) status, increased 1.69, 1.48 fold in the mental component summary scale scores respectively. SNAQ was the best determinant of physical component summary scale score had the greatest positive effect, good appetite status increased approximately 2.2 fold in physical scores. Polypharmacy and high BMI decreased health related quality of life in elderly.
Conclusion
Determinants of quality of life are preventable and treatable with early and appropriate interventions in elderly.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Ageing is a global phenomenon that is both inevitable and predictable. According to demographic data the elderly population has been increasing dramatically all over the world. Especially since 2000, the elderly population has increased faster (1). Worldwide, there were 901 million people aged 60 years or over in 2015, an increase of 48 percent over the 607 million older persons globally in 2000 (2). The number of people aged 65 or older was approximately 6.5 million in Turkey, 8.5% of total population was elderly in 2017 (3). The aging process or changes related to secondary events or diseases cause rapid deterioration of body functions in the last phase of life (4). For this reason healthy aging is important for the maintaining physical, mental health and functionality. Because of that health related quality of life is emerged as the key goal for health promotion for the elderly people (5). Health related quality of life is a subjective multidimensional construct reflecting functional status, emotional and social well being, as well as general health. It is known that one of the crucial factors affecting quality of life is the nutritional status. At the same time an impaired nutritional status frequently leads to resulted in impaired functional status besides that general health. Good nutritional and psychological status can promote the quality of life in the elderly and can decrease the mortality and morbidity (6, 7).
There is a certain relationship between malnutrition risk and quality of life in older people. Along with the increase of malnutrition prevalence with aging, comorbidity and mortality increase in the elderly (6, 8). Especially digestive problems, sense perception such as loss of taste, smell and appetite or swallowing and chewing difficulties affect eating and/or food intake and so that health related quality of life such as mobility, activities of daily living and mental health is also affected (9).
In old age, appetite is the most important risk factor associated with food and nutritional deficiencies. There are many reasons that affect the appetite mechanisms in the aging process. These include physiological changes, psychological conditions, acute and chronic diseases and number of medication (10). Adequate and balanced nutrition is one of the most important factors affecting health related quality of life in elderly. But the reduction in appetite affect nutrition intake of elderly even it cause nutritional deficiencies and weight loss by decreasing in daily energy intake. And also poor appetite is associated with poor healthcare outcomes, including increased mortality. So appetite is important for health related quality of life in elderly because promoting better appetite increase food intake and enhance healthcare outcomes in elderly (10, 11).
There are limitations about assessment of energy, nutrient intake, appetite and health related life quality of elderly in studies. Studies have indicated that relationship between malnutrition and health related quality of life (12-16) but a few studies have shown a similar relationship a loss of appetite and health related quality of life (9, 17). The aim of the present study was to examine nutritional risk factors such as poor appetite and malnutrition affecting health related quality of life in elderly.
Material and methods
Sampling and data collection
This is a cross-sectional population-based study consisted of 407 elders (mean age 71.7±6.54 years). A simple randomized sampling method was used for identifying of districts in center of Ankara, the capital of Turkey. The elderly was visited in their homes and those who agreed to participate voluntarily were recruited in the study. Elders or their parents informed about the study and signed a voluntary participation form which adhered to Declaration of Helsinki protocols (World Medical Association). Participation rate of the study was 89% and 85% of the elderly were evaluated. The data were collected in face-to-face interviews and a questionnaire was applied including the demographic and general characteristics, health information, nutritional habits, health related life quality scale (The Health Survey Short Form-SF36), Mini Nutrition Assessment (MNA), Mini Nutrition Assessment-Short Form (MNA-SF) and Simplified Nutritional Appetite Questionnaire (SNAQ).
Anthropometric measurements
Anthropometric measurements, including weight, height, waist and mid upper arm circumferences were measured by well-trained investigators, using standard measurement protocols. Participants were weighed using an electronic scale to the nearest 0.1 kg. Height was measured with a stadiometer to the nearest 0.1 cm. Waist circumference was measured at the mid-point, above the iliac crest and below the lowest rib margin at minimum respiration, using a flexible tape to the nearest 0.1 cm (18). Weight and height obtained was used to calculate body mass index (BMI) that was calculated as weight (kg) divided by height squared (m2) (19).
Dietary Intake
Daily food consumption was assessed using 24 hour dietary recall. Researchers determined amounts of all nutrients in consumed foods by using photographic atlas of food portion size and amounts (20). Dietary data from the food records were entered into a food analysis software Nutrition Information Systems (BEBIS) to calculate the total daily intake of energy and nutrients (21).
Assessment of nutrition status
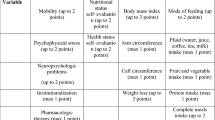
The Mini Nutrition Assessment (22) consists of 18 items structured in 4 parts: anthropometric assessment, global assessment, dietary assessment and self-assessment. The maximum possible score for the MNA full form is 30 points. This questionnaire composed of 18 different questions and anthropometric measures for ranking participants in three levels (malnutrition with scores less than 17, at risk of malnutrition with 17 and 23.5 scores and normal status with 24 and 30 scores). The revised MNA-SF (23), a shortened form of the MNA, is also used for nutritional screening, in this study. The MNA-SF comprises six questions, including BMI, declined food intake over the past 3 months as a result of a loss of appetite/digestive problems or swallowing difficulties, weight loss during last 3 months, mobility, neuropsychological problems and psychological stress or acute disease in the past 3 months. The scores from all questions are summed together, giving a minimum score of 0 and a maximum score of 14. Higher scores indicating better nutritional status at both two forms. The score is >12 points greater, the patient is said to have normal nutritional status, scores between 8 and 11 indicate the person is at risk of malnutrition, and, if the score is ≤7 points, the patient is said to be malnutrition.
Evaluation of appetite
Appetite was measured using the SNAQ. The SNAQ is the short, reliable and simple appetite assessment tools that predicts risk of weight loss. The SNAQ is composed of four questions. Each question presents five options for answer which are represented by the letters from A to E. These letters based on the following numerical scale: A = 1, B = 2, C = 3, D = 4 and E = 5. When summed up and total score which may range from 4 to 20. Higher scores demonstrate a better appetite. The lower scores are higher the risk for weight loss. Score≤14 indicates that risk for loss of weight (24).
Assessment of the health related quality of life (SF36)
The SF-36 is a short form questionnaire with 36 items that measure eight health related quality of life scales. They are physical functioning (PF), role limitation due to physical health (RP), bodily pain (BP), general health perceptions (GH), vitality (VT), social functioning (SF), role limitations as a result of emotional problems (RE) and general mental health (MH). For each quality of life scale tested and item scores were coded, summed, and transformed into a scale from 0 (worst) to 100 (best) using the standard SF-36 scoring algorithms. Two summary measures, physical and mental summary component scale scores were also calculated using algorithm described by the developers (25).
Statistical analysis
Statistical analysis was performed with version 16 SPSS. Health related quality of life scores (SF36) of individuals are presented as the means and they were compared according to gender using a t-test for two independent samples. Spearman’s rank correlation coefficient was used to test the association between quality of life scales and markers of nutritional status and appetite. Finally, multiple linear regression analysis was carried out to identify variables that made an important contribution to the variability of quality of life and to explore the contribution of age, number of medicine used, MNA, SNAQ scores to physical and mental component summary scale scores.
Results
A total of 407 home dwelling elderly individuals were interviewed (142 men and 265 women) with a mean age of men and women 72.8±6.67 years; 71.1±6.41 years respectively (p<0.05). When we evaluated general and health information of elderly we found that education level of men were (6.7±4.16 years) higher than women (3.9±3.47) (p<0.05). Number of medication used and body mass index of individuals were similar both gender (men:3.3±2.67 number/day; women: 3.4±2.39 number/day, men: 27.5±4.28 kg/m2; women: 29.8±5.78 kg/m2 respectively) (p>0.05).
According to MNA and MNA-SF 6.1%; 4.2% of elderly people had malnutrition and about 40.3%; 21.9% of them were at risk of malnutrition respectively. Men generally showed more risk of malnutrition than women did, although the differences were not significant (χ2 :5.667; p=0.059; (χ2 :3.152; p=0.257 respectively). Accordingly, SNAQ tests 28.7% of elderly people were risk at loss of weight. Women had high level of malnutrition than men and these results was significant (χ2 :7.378; p=0.007) (data not shown).
Health related quality of life scores of women had lower scores than men in all subscales. The significant differences were found between genders in the subscales of SF-36 which are physical functioning, bodily pain, general health, vitality, role-emotional. In addition, physical component summary scales (men: 51.8±19.74; women: 43.4±16.22) and mental component summary scales (men: 55.6±16.03; women: 51.7±15.08) were found significant different between gender (p<0.05) (Table 1).
Elderly with malnutrition/malnutrition risk (MNA –SF, MNA) and good appetite (SNAQ) had lower life quality scores than well-nourished elderly in all subscales. The significant differences were found between groups in the all subscales of SF-36 (p<0.05) (Table 1)
Significant positively correlation was found between SF36- physical and mental component summary scale scores and MNA (r:0.365, p:0.000; r:0.293, p:0.000), MNA-SF (r:0.45, p:0.000; r:453, p:0.000), SNAQ (r:0.459, p:0.000; r:0.400, p:0.000), educational level (r:0.282, p:0.000; r:0.191, p:0.001) respectively. Also weak reverse relation were found between SF36-physical and mental scale scores and number of medication (r:-0.264, p:0.000; r:-0.173, p:0.001) and age (r:- 0.221, p:0.000; r:-0.187, p:0.000) respectively. There was no relationship between anthropometric measurements, number of main meal/snack and consumption of macronutrients with health related life quality of elderly (p>0,05). Energy (r: 0.200, p:0.000; r:0.152, p:0.000 respectively) and fiber intake (r: 0.161, p:0.001; r:0.201, p:0.000 respectively) were positively correlated with both physical and mental subscale scores of life quality (p<0.05). BMI were negatively correlated with physical component summary scale scores (r:-0.103 p:0.038) (Table 2).
Table 3 identifies the results of the multiple linear regression model, where five determinants significantly associated with physical component summary scale scores of elderlies. While the combination of three determinants factors (educational level, MNA-SF and SNAQ scores) had positive effects but the others (number of medication and high BMI) had negative effects on their physical component summary scale scores. Physical component summary scale scores increased linearly as educational level, MNA-SF and SNAQ scores increased (p< 0.05) and physical component summary scale scores decreased linearly as BMI and number of medication used increased (p< 0.05). SNAQ which was the best determinant of physical component summary scale score had the greatest positive effect and good appetite status increased 2.208 fold in physical scores. In addition to number of medication had the greatest negative effect on physical component summary scale scores and it decreased 1.940 fold in physical scores.
Number of medication, MNA-SF and SNAQ scores were important determinants for mental component summary scale scores of elders. While the combination of MNA-SF and SNAQ scores had positive effects but number of medication had negative effects on their mental component summary scale scores (p< 0.05). Good nutritional (MNA-SF) and good appetite (SNAQ) status, increased 1.687, 1.477 fold in the mental component summary scale scores in elderly population respectively. Increased number of medication was negative determinant of the mental status (Table 4).
Discussion
Evaluation of factors associated with the aging process and early diagnosis and preventing of malnutrition are important to avoiding a deterioration of quality of life in elderly (26). Malnutrition is associated with functional and cognitive impairment in older people and also it causes greater morbidity and reduced quality of life (27). Quality of life includes health status and life expectancy and depends on physical and psychological well-being and these factors can be influenced by nutritional status. So the nutritional status of elderly plays an important role in protecting health, improving quality of life (6, 8, 16).
Many studies have limitations impact of energy and nutrient intake and appetite on quality of life [14, 28, 29]. Especially association between MNA with anthropometric measurements and quality of life in older people has been studied previously (8, 14, 28, 29) but relationship between quality of life with energy and nutrient intake and appetite are lacking. The present study investigated the relationship between quality of life with nutritional status and appetite in a group of home dwelling older people.
In general, poor quality of life was common in women and being female was best determinant for physical, and mental health with malnutrition/risk of malnutrition (30-32) Studies reported that women had lower scores on all subscales of the SF-36 than men in many studies (12, 31-33). These results were in accordance with the present study that women have a substantially worse health related quality of life scores on both the physical and mental scales of the SF36 (men: 51.8±19.74, women: 43.4±16.22; men:55.6±16.03, women: 51.7±15.08 respectively) (p<0.05). And especially role-physical and roleemotional subscales scores were very low in both gender (p<0.05). (Table 1).
Sociodemographic and lifestyle-related factors such as educational level, less physical activity, sleep duration, increased number of medication and aging affect life quality of life in elderly (31). Studies have determined that lower educational level and advanced age associated with an increasing deterioration of health status and quality of life (34-36). Therefore, the quality of life is very important determinant for improving quality of aging. Consistent with the previous studies it was found that quality of life was worse in older ages with a lower education level. In the present study, SF-36- physical and mental component summary scale scores were found negatively correlate with number of medicine. Similar to our result, Harrison and et. al. reported that increased number of medications were associated with lower quality of life scores in elderly (37).
Losing sense of smell and taste, decreasing ability to chew and swallow, impaired gastrointestinal function, comorbidities and polypharmacy leads to poor nutrition and increases the risk of malnutrition in elderly (38-40). It was known that malnutrition was common in elderly. Malnutrition prevalence was found according to MNA 6.1% and MNA-SF 4.2% and risk of malnutrition were 40.3%; 21.9% respectively in present study. Malnutrition is associated with physical, mental, and social disability so malnutrition usually causes greater morbidity and reduced quality of life (41). Common problems individuals with malnutrition were losing muscle mass and functional impairment which decreased health related quality of life (40, 42, 43). Impaired nutritional status can accelerate functional and mental problems in elderly. In this study, elderly with malnutrition/malnutrition risk (MNA–SF, MNA) had lower life quality scores in all subscales (p<0.05). (Table 1). MNA and MNA-SF scores of elderly significantly positive correlated with mental and physical component scores of SF-36 (Table 2). Elderly nutritional status is important determinant for mental and physical health.
Poor appetite was also an important risk factor affected the quality of life. Physiological changes, psychological problems, acute and chronic diseases and polypharmacy impair appetite with different mechanisms in elderly (10). According to appetite status (SNAQ) of elderly with ‘risk of loss of weight᾿had lower health related quality of life scores in all subscales (p<0.05) (Table 1). On the other hand, elderly with good appetite had increased SF-36-physical and mental component summary scale scores in this study. Better appetite also promotes adequate and balanced nutrition and increases dietary energy intake. It was found that dietary energy intake was positively correlated health related quality of life in present study (p<0.05), (Table 2).
MNA-SF scores had the greatest positive effect in the mental and physical component summary scale scores. (Table 3-4) So that it is considering that nutritional status may be an important influence on quality of life in elderly. In an another study reported that a strong relationship between malnutrition risk and poorer quality of life in elderly (12). Good nutrition improves quality of life in older people by promoting health and preventing dietary deficiency disease. (12, 40). Therefore, it is important to assess nutritional status when evaluating health related quality of life in older people.
Other nutritional indicators that may affect quality of life were also assessed in this study. It was not found any significant association between number of main meal/snack and dietary energy and nutrient intake (except dietary fiber intake) with life quality. A study (44) reported that a greater adherence to the Mediterranean diet was associated with better quality of life in elderly. Especially the health protective properties of Mediterranean diet become significant with the intake of fibre. Another finding of the current study suggests that dietary fibre intake was positive correlated health related quality of life of elderly in our study (p<0.05) (Table 2). Fruits and vegetables consumptions increase dietary fibre intake which is one of the most important components of the Mediterranean diet. So Mediterranean diet should promote due to their benefits on other health outcomes. However there is limited data about effects of specific food components of the Mediterranean diet on quality of life in older people (45).
Physical changes include in body composition that occur with aging have potential adverse impacts in health related quality of life in older people (12) but there isn’t any significant association between anthropometric measurements (except BMI) with health related life quality of elderly in present study. High BMI values had a significant impact on the all cause of mortality and morbidity (46-48) and studies indicated that the most appropriate BMI range for the elderly was 25–27 kg/m2 for prevention morbidity Mean BMI of elderly were higher than 27 kg/m2 in both gender and also physical quality of life scores negatively correlated with BMI in present study (Table 2). It is important that normal ranges BMI for elderly in order to increase health related quality of life and functionality.
Conclusion
In this light, appetite and nutritional status may be described as two major determinants of mental and physical health for home dwelling elderly. The two determinants of quality of life are preventable and treatable with early and appropriate interventions in this group. Another determinant of quality of life was medication. Polypharmacy was negatively affected both physical and mental functioning. For this reason, rational approach to drug use should be adopted in old age. And also considerable result of this study, prevention of ≥27 kg/m2 BMI is important in order to improve health related quality of life in elderly.
In this study, reached a large elderly group and anthropometric measurements of individuals were taken. However, body compositions were not evaluated. High BMI affects negatively quality of life which may be due to the increase in fat mass as well as the loss of muscle mass and sarcopenic obesity. It will be useful to evaluate sarcopenic obesity in future studies.
Ethical Standards: The study protocol was approved by the Ethical Committee of the Gazi University of Ankara/Turkey (2017-473) and written informed consent was obtained from all participants.
Conflicts of interest: Authors declare no conflict of interest.
References
Acar Tek N. A Current Perspective on Health Sciences. In: Kaptanoğlu AY (ed) Nutritional Care and Management of Sarcopenia, Romania 2015, p:710–727.
World Population Ageing, 2015. Available:https://doi.org/www.un.org/en/development/desa/population/publications/,pdf/ageing/WPA2015_Report.pdf. Accessed 25 March 2018.
TUIK, 2017. Statistics for the elderly, 2017 https://doi.org/www.tuik.gov.tr/PreHaberBultenleri.do?id=27595 Accessed 25 March 2018.
Nair KS. Aging muscle Am J Clin Nutr 2005;81(5):953–63.
Jimenez-Redondo S, Beltran de Miguel B, Gavidia Banegas J, Guzman Mercedes L, Gomez-Pavon J, Cuadrado Vives C. Influence of nutritional status on healthrelated quality of life of non-institutionalized older people. J Nutr Health Aging 2014;18(4):359–64 doi:10.1007/s12603-013-0416-x.
Rasheed S, Woods RT. An investigation into the association between nutritional status and quality of life in older people admitted to hospital. J Hum Nutr Diet 2014;27(2):142–51 doi:10.1111/jhn.12072.
Payahoo L, Khaje-Bishak Y, Pourghassem Gargari B, Kabir-Alavi MB, Asgharijafarabadi M. Assessment of Nutritional and Depression Status in Free- Living El-derly in Tabriz, Northwest Iran. Health Promot Perspect 2013;3(2):288–93 doi:10.5681/hpp.2013.033.
Hernández-Galiot A, Goñi I. Quality of life and risk of malnutrition in a homedwelling population over 75 years old. Nutrition 2017;35:81–6.
Perry L, McLaren S. An exploration of nutrition and eating disabilities in relation to quality of life at 6 months post-stroke. Health Soc Care Community 2004;12(4):288–97.
Pilgrim AL, Robinson SM, Sayer AA, Roberts HC. An overview of appetite decline in older people. Nurs Older People 2015;27(5):29–35 doi:10.7748/nop.27.5.29.e697.
Giezenaar C, Chapman I, Luscombe-Marsh N, Feinle-Bisset C, Horowitz M, Soenen S. Ageing Is Associated with Decreases in Appetite and Energy Intake—A Meta-Analysis in Healthy Adults. Nutrients 2016;8(1):28 doi:10.3390/nu8010028.
Rasheed S, Woods RT. Malnutrition and quality of life in older people: a systematic review and meta-analysis. Ageing Res Rev 2013;12(2):561–6 doi:10.1016/j.arr.2012.11.003.
Goodwin JS. Social, psychological and physical factors affecting the nutritional status of elderly subjects: separating cause and effect. Am J Clin Nutr 1989;50(5):1201–9; discussion 31-5.
Hickson M, Frost G. An investigation into the relationships between quality of life, nutritional status and physical function. Clin Nutr 2004;23(2):213–21 doi:10.1016/s0261-5614(03)00127-4.
Norman K, Schutz T, Kemps M, Josef Lubke H, Lochs H, Pirlich M. The Subjective Global Assessment reliably identifies malnutrition-related muscle dysfunction. Clin Nutr 2005;24(1):143–50 doi:10.1016/j.clnu.2004.08.007.
Heersink JT, Brown CJ, Dimaria-Ghalili RA, Locher JL. Undernutrition in hospitalized older adults: patterns and correlates, outcomes, and opportunities for intervention with a focus on processes of care. J Nutr Elder 2010;29(1):4–41 doi:10.1080/01639360903574585.
Donini LM, Savina C, Piredda M, et al. Senile anorexia in acute-ward and rehabilitations settings. J Nutr Health Aging 2008;12(8):511–17.
Lohman TG RA, Martoel R. Antropometric Standarsization Reference Manual, Michigan Üniversitesi, Human Kinetic Books, Champaign, İllinois, 1998.
WHO. Body mass index–BMI. https://doi.org/www.euro.who.int/en/health-topics/disease-prevention/nutrition/a-healthy-lifestyle/body-mass-index-bmi Accessed 27 March 2018
Rakıcıoğlu N, Acar Tek, Ayaz A., Pekcan G. Yemek ve Besin ve Fotoğraf Kataloğu: Ölçü ve Miktarlar. Ata Ofset Matbaacılık, Ankara, 2012.
Beslenme Bilgi Sistemleri. Ebispro for Windows S, Germany; Türkish version BEBİS; Data Bases: Bundeslebenmittelschlüssell,11.3 and other sorces, 2004.
Vellas B, Guigoz Y, Garry PJ, Nourhashemi F, Bennahum D, Lauque S, Albarede JL. The Mini Nutritional Assessment (MNA) and its use in grading the nutritional state of elderly patients. Nutrition 1999;15(2):116–22.
Kaiser MJ, Bauer J, Ramsch C, et al. Validation of the Mini Nutritional Assessment Short-Form (MNA®-SF): A practical tool for identification of nutritional status. J Nutr Health Aging 2009;13(9):782–8.
Wilson MMG TD, Rubenstein LZ, Chibnall JT, Anderson S, Baxi A, et al. Appetite assessment: simple appetite questionnaire predicts weight loss in community-dwelling adults and nursing home residents. Am J Clin Nutr 2005;82:1074–81.
Ware JE, Gandek B. Overview of the SF-36 health survey and the international quality of life assessment (IQOLA) project. J Clin Epidemiol 1998;51(11):903–12.
Kostka J, Borowiak E, Kostka T. Nutritional status and quality of life in different populations of older people in Poland Eur J Clin Nutr 2014;68(11):1210.
Méndez EE, Romero PJ, Fernández DM, et al. Do our elderly have an adequate nutritional status? Nutr Hosp 2012;28(3):903–13.
Kvamme JM, Olsen JA, Florholmen J, Jacobsen BK. Risk of malnutrition and healthrelated quality of life in community-living elderly men and women: the Tromso study. Qual Life Res 2011;20(4):575–82 doi:10.1007/s11136-010-9788-0.
Keller HH, Ostbye T, Goy R. Nutritional risk predicts quality of life in elderly community-living Canadians. J Gerontol A Biol Sci Med Sci 2004;59(1):68–74.
Lopez-Garcia E, Banegas Banegas JR, Gutierrez-Fisac JL, Perez-Regadera AG, Ganan LD, Rodriguez-Artalejo F. Relation between body weight and health-related quality of life among the elderly in Spain. Int J Obes Relat Metab Disord 2003;27(6):701–9. doi:10.1038/sj.ijo.0802275
Maseda A, Diego-Diez C, Lorenzo-López L, López-López R, Regueiro-Folgueira L, Millán-Calenti JC. Quality of life, functional impairment and social factors as determinants of nutritional status in older adults: The VERISAÚDE study. Clin Nutr 2017;S0261-5614(17)30148–6 doi: 10.1016/j.clnu.2017.04.009.
Guallar-Castillon P, Sendino AR, Banegas JR, Lopez-Garcia E, Rodriguez-Artalejo F. Differences in quality of life between women and men in the older population of Spain. Soc Sci Med 2005;60(6):1229–40 doi:10.1016/j.socscimed.2004.07.003
Konig HH, Heider D, Lehnert T, et al. Health status of the advanced elderly in six European countries: results from a representative survey using EQ-5D and SF-12. Health Qual Life Outcomes 2010;8:143 doi:10.1186/1477-7525-8-143.
Arber S, Cooper H. Gender differences in health in later life: the new paradox? Soc Sci Med 1999;48(1):61–76.
Eguez-Guevara P, Andrade FC. Gender differences in life expectancy with and without disability among older adults in Ecuador. Arch Gerontol Geriatr 2015;61(3):472–9 doi:10.1016/j.archger.2015.08.012.
Regidor E, Barrio G, de la Fuente L, Domingo A, Rodriguez C, Alonso J. Association between educational level and health related quality of life in Spanish adults. J Epidemiol Community Health 1999;53(2):75–82.
Harrison SL, Bradley C, Milte R, et al. Psychotropic medications in older people in residential care facilities and associations with quality of life: a cross-sectional study. BMC Geriatr 2018;18(1):60 doi:10.1186/s12877-018-0752-0.
Orfila F, Ferrer M, Lamarca R, Alonso J. Evolution of self-rated health status in the elderly: cross-sectional vs. longitudinal estimates. J Clin Epidemiol 2000;53(6):563–70.
Drewnowski A, Evans WJ. Nutrition, physical activity, and quality of life in older adults: summary. J Gerontol A Biol Sci Med Sci 2001;56(2):89–94.
Amarantos E, Martinez A, Dwyer J. Nutrition and quality of life in older adults. J Gerontol A Biol Sci Med Sci 2001;56(2):54–64.
Hernandez-Galiot A, Goni I. Quality of life and risk of malnutrition in a homedwelling population over 75 years old. Nutrition 2017;35:81–6. doi:10.1016/j. nut.2016.10.013
Lesourd B. Nutrition: a major factor influencing immunity in the elderly. J Nutr Health Aging 2004;8(1):28–37.
Stuck AE, Walthert JM, Nikolaus T, Bula CJ, Hohmann C, Beck JC. Risk factors for functional status decline in community-living elderly people: a systematic literature review. Soc Sci Med 1999;48(4):445–69.
Perez-Tasigchana RF, Leon-Munoz LM, Lopez-Garcia E, Banegas JR, Rodriguez-Artalejo F, Guallar-Castillon P. Correction: Mediterranean diet and health-related quality of life in two cohorts of community-dwelling older adults. plos One 2016;11(5):0155171. doi:10.1371/journal.pone.0155171
Pérez-Tasigchana RF, León-Muñoz LM, López-García E, Banegas JR, Rodríguez-Artalejo F, Guallar-Castillón P. Mediterranean Diet and health-related quality of life in two cohorts of community-dwelling older adults. PloS one 2016;11(3):0151596.
Grzegorzewska A, Wolejko K, Kowalkowska A, Kowalczyk G, Jaroch A. Proper BMI ranges for the elderly in the context of morbidity, mortality and functional status. Gerontologia Polska 2016;24:114–8.
Zhu J, Xiang YB, Cai H, et al. Associations of obesity and weight change with physical and mental impairments in elderly Chinese people. Maturitas 2018;108:77–83. doi:10.1016/j.maturitas.2017.11.015
Khan SS, Ning H, Wilkins JT, et al. Association of body mass index with lifetime risk of cardiovascular disease and compression of morbidity. JAMA cardiology, 2018. doi:10.1001/jamacardio.2018.0022.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Acar Tek, N., Karaçil-Ermumcu, M.Ş. Determinants of Health Related Quality of Life in Home Dwelling Elderly Population: Appetite and Nutritional Status. J Nutr Health Aging 22, 996–1002 (2018). https://doi.org/10.1007/s12603-018-1066-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-018-1066-9