Abstract
Introduction
To quantify early nonadherence to antipsychotic medications in patients with schizophrenia and its impact on short-term antipsychotic adherence, healthcare utilization, and costs.
Methods
Patients who initiated oral antipsychotic treatment between January 1, 2006 to September 30, 2009 were identified from the MarketScan®Commercial Claims and Encounters (CCE) database (Truven Health Analytics, Ann Arbor, Michigan, USA). Patients were required to have a diagnosis of schizophrenia determined by the International Classification of Disease, Ninth Revision, Clinical Modification (ICD-9-CM) code 295.x, be 13–65 years of age, and have ≥12 months of continuous coverage prior to and after (follow-up) the earliest antipsychotic usage (index event). Medication discontinuation was defined as a gap of 30 days in available therapy; early nonadherence was defined as having the gap 90 days from the index event. During the follow-up period, medication adherence was estimated with quarterly medication possession ratios (MPR), and all-cause and schizophrenia-related healthcare resource utilization and costs were determined.
Results
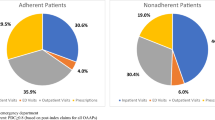
The mean time to discontinuation (TTD) was 39.5 ± 20.1 days for early nonadherence patients (n = 873) and 250.7 ± 103.3 days for patients who were adherent early (n = 589). Early nonadherence resulted in more hospitalizations (0.57 vs. 0.38; P = 0.0006) with longer length of stay (LOS, 5.0 vs. 3.0 days; P = 0.0013) and higher costs ($5,850 vs. $4,211; P = 0.0244); schizophrenia-related hospitalizations, LOS, and costs were also greater. Patients that were adherent used more schizophrenia-related medications (10.4 vs. 4.7; P < 0.0001), increasing pharmacy costs ($3,684 vs. $1,549; P < 0.0001). Early nonadherence was correlated with lower drug adherence at each quarter of the follow-up period.
Conclusion
Approximately 60% of patients with schizophrenia are nonadherent to antipsychotic medication early in treatment and are less likely to be adherent later. Early nonadherence resulted in more all-cause and schizophrenia-related hospitalizations with a greater LOS and cost of care.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
McGrath J, Saha S, Chant D, Welham J. Schizophrenia: a concise overview of incidence, prevalence, and mortality. Epidemiol Rev. 2008;30:67–76.
Vita A, Corsini P, Bonomi S, Sacchetti E, Cesana BM. Factors affecting antipsychotic drug discontinuation in the treatment of schizophrenia: evidence from a naturalistic, retrospective, 18-month follow-up study. Schizophr Res. 2008;104:302–304.
Haro JM, Novick D, Suarez D, Roca M. Antipsychotic treatment discontinuation in previously untreated patients with schizophrenia: 36-month results from the SOHO study. J Psychiatr Res. 2009;43:265–273.
Perkins DO, Gu H, Weiden PJ, McEvoy JP, Hamer RM, Lieberman JA. Predictors of treatment discontinuation and medication nonadherence in patients recovering from a first episode of schizophrenia, schizophreniform disorder, or schizoaffective disorder: a randomized, double-blind, flexible-dose, multicenter study. J Clin Psychiatry. 2008;69:106–113.
Ascher-Svanum H, Faries DE, Zhu B, Ernst FR, Swartz MS, Swanson JW. Medication adherence and long-term functional outcomes in the treatment of schizophrenia in usual care. J Clin Psychiatry. 2006;67:453–460.
Gilmer TP, Dolder CR, Lacro JP, et al. Adherence to treatment with antipsychotic medication and health care costs among Medicaid beneficiaries with schizophrenia. Am J Psychiatry. 2004;161:692–699.
Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40:373–383.
Quan H, Sundararajan V, Halfon P, et al. Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Med Care. 2005;43:1130–1139.
Lieberman JA, Stroup TS, McEvoy JP, et al; Clinical Antipsychotic Trials of Interventional Effectiveness (CATIE) Investigators. Effectiveness of antipsychotic drugs in patients with chronic schizophrenia. N Engl J Med. 2005;353:1209–1223.
Liu-Seifert H, Adams DH, Kinon BJ. Discontinuation of treatment of schizophrenic patients is driven by poor symptom response: a pooled post-hoc analysis of four atypical antipsychotic drugs. BMC Med. 2005;3:1–10.
McCombs J, Zolfaghari S, Ganapathy V. Impact of drug treatment history on comparative effectiveness research in schizophrenia. Value Health. 2011;14:679–686.
Moisan J, Gregoire JP. Patterns of discontinuation of atypical antipsychotics in the province of Quebec: A retrospective prescription claims database analysis. Clin Ther. 2010;32(Suppl. 1):S21–S31.
Yen CF, Chen CS, Ko CH, et al. Relationships between insight and medication adherence in outpatients with schizophrenia and bipolar disorder: prospective study. Psychiatry Clin Neurosci. 2005;59:403–409.
Altamura AC, Mauri M. Plasma concentrations, information and therapy adherence during longterm treatment with antidepressants. Br J Clin Pharmac. 1985;20:714–716.
Sun SX, Liu GG, Christensen DB, Fu AZ. Review and analysis of hospitalization costs associated with antipsychotic nonadherence in the treatment of schizophrenia in the United States. Curr Med Res Opin. 2007;23:2305–2312.
Marcus SC, Olfson M. Outpatient antipsychotic treatment and inpatient costs of schizophrenia. Schizophr Bull. 2008;34:173–180.
Verdoux H, Lengronne J, Liraud F, et al. Medication adherence in psychosis: predictors and impact on outcome. A 2-year follow-up of first-admitted subjects. Acta Psychiatr Scand. 2000;102:203–210.
Robinson D, Woerner MG, Alvir JM, et al. Predictors of relapse following response from a first episode of schizophrenia or schizoaffective disorder. Arch Gen Psychiatry. 1999;56:241–247.
Subotnik KL, Nuechterlein KH, Ventura J, et al. Risperidone nonadherence and return of positive symptoms in the early course of schizophrenia. Am J Psychiatry. 2011;168:286–292.
Law MR, Soumerai SB, Ross-Degnan D, Adams AS. A longitudinal study of medication nonadherence and hospitalization risk in schizophrenia. J Clin Psychiatry. 2008;69:47–53.
Weiden PJ, Kozma C, Grogg A, Locklear J. Partial compliance and risk of rehospitalization among California Medicaid patients with schizophrenia. Psychiatr Serv. 2004;55:886–891.
Kim B, Lee S, Yang YK, Park J, Chung Y. Longacting injectable antipsychotics for first-episode schizophrenia: the pros and cons. Schizophr Res Treatment. 2012;2012:1–8.
Peng X, Ascher-Svanum H, Faries D, Conley RR, Schuh KJ. Decline in hospitalization risk and health care cost after initiation of depot antipsychotics in the treatment of schizophrenia. Clinicoecon Outcomes Res. 2011;3:9–14.
Fuller M, Shermock K, Russo P, et al. Hospitalisation and resource utilisation in patients with schizophrenia following initiation of risperidone long-acting therapy in the Veterans Affairs Healthcare System. J Med Econ. 2009;12:317–324.
Niaz OS, Haddad PM. Thirty-five months experience of risperidone long-acting injection in a UK psychiatric service including a mirror-image analysis of in-patient care. Acta Psychiatr Scand. 2007;116:36–46.
Prikryl R, Prikrylova KH, Vrzalova M, Ceskova E. Role of long-acting injectable second-generation antipsychotics in the treatment of first-episode schizophrenia: a clinical perspective. Schizophr Res Treatment. 2012;2012:1–7.
Author information
Authors and Affiliations
Corresponding author
Additional information
To view enhanced content go to www.advancesintherapy.com
Rights and permissions
About this article
Cite this article
Offord, S., Lin, J., Mirski, D. et al. Impact of Early Nonadherence to Oral Antipsychotics on Clinical and Economic Outcomes Among Patients with Schizophrenia. Adv Therapy 30, 286–297 (2013). https://doi.org/10.1007/s12325-013-0016-5
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-013-0016-5