Abstract
Cognitive-behavioral therapy (CBT) remains the only evidenced-based psychosocial treatment for pediatric anxiety. Adoption of CBT in community settings has been slow, and data on CBT use in schools specifically are limited. This study examined: (1) school-based clinicians’ perceptions of their treatment approach for pediatric anxiety disorders, use of therapeutic strategies reported after each session, and overall perceived confidence in treating anxiety disorders, and (2) independent evaluator (IE) ratings of clinicians’ use of CBT, the frequency and quality of specific CBT elements in sessions, and overall competence in treating anxiety. An exploratory aim examined whether clinician characteristics were associated with IE-rated CBT use. Participants included 25 school-based clinicians who delivered treatment as usual in a randomized controlled trial of treatments for anxious children and adolescents. At baseline, clinicians reported their approach to treating anxious youth. After each session (N = 475), they reported the therapeutic strategies they used. IEs rated audiotaped therapy sessions (N = 90). Results indicated a majority of school clinicians reported using a behavioral or cognitive-behavioral approach for anxiety (68% at baseline and in 76% of sessions). In contrast, 14% of the IE-rated sessions had the primary therapeutic strategy coded as cognitive-behavioral. Clinician confidence and IE competence ratings were also discrepant, with clinicians rating themselves as somewhat confident in treating anxious youth but IEs assigning a low competence rating. Use and quality of CBT elements based on IE-rating were low. Several clinician characteristics were associated with CBT use. Findings suggest a need to improve the training of school-based clinicians in EBTs for students with anxiety.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pediatric anxiety disorders are common and impair students’ daily functioning (Copeland, Shanahan, & Costello, 2011; Costello, Egger, & Angold, 2005; Merikangas et al., 2010; Swan & Kendall, 2016). With respect to academic functioning, excessive anxiety and anxiety disorders have been linked to poor academic performance (Hughes, Lourea-Waddell, & Kendall, 2008; Mazzone et al., 2007), excessive absenteeism and school refusal (Hansen, Sanders, Massaro, & Last, 1998), and school dropout (Breslau, Lane, Sampson, & Kessler, 2008; Duchesne, Vitaro, Larose, & Tremblay, 2008). Unfortunately, the vast majority of children and adolescents (hereafter referred to as children) suffering from an anxiety disorder do not receive any services (Chavira, Stein, Bailey, & Stein, 2004; Olfson et al., 2009; Wang et al., 2007). Reasons for this reality include both structural (e.g., cost, transportation, inconvenience) and attitudinal barriers (e.g., stigma, belief that the problem will get better on its own, perceived ineffectiveness of treatment; Andrade et al., 2014; Jagdeo, Cox, Stein, & Sareen, 2009; Sareen et al., 2007). Untreated anxiety tends to run a chronic and debilitating course, and leads to the onset of disorders later in life (Ginsburg et al., 2018; Scholten et al., 2013), highlighting the urgency of receiving early and effective treatment.
In an attempt to bridge this gap between need and service use, child mental health advocates have recommended offering school-based mental health treatment (Weist et al., 2017). School-based mental health services have numerous advantages including diminished cost, increased accessibility, and reduced stigma (American Academy of Pediatrics, 2004). Offering treatment in schools also provides a unique opportunity for clinicians to intervene “in real time” to help children practice facing their fears (exposures) in relevant anxiety-provoking situations—a key treatment ingredient of evidenced-based treatments for anxiety (Peris et al., 2015, 2017). Consequently, school-based treatment for anxiety represents a valuable option for anxious students.
Among extant psychosocial treatments (not including combination treatments that involve medication) for pediatric anxiety disorders, cognitive-behavioral therapy (CBT) is the only evidenced-based treatment (EBT) and has been shown to be effective for youth across age, gender, and racial/ethnic groups, as well as across different formats including individual, group, and family approaches (Higa-McMillan, Francis, Rith-Najarian, & Chorpita, 2016; In-Albon & Schneider, 2007; James, James, Cowdrey, Soler, & Choke, 2015). Long-term follow-up studies of CBT demonstrate that gains can be maintained over several years (see Gibby, Casline, & Ginsburg, 2017 for a review), highlighting the benefits of this treatment approach.
The adoption of CBT and other EBTs into community settings has been slow (McHugh & Barlow, 2010). In the school setting, several factors may account for this phenomenon. First, the school culture puts a high priority on educational needs such as educational assessments to determine special education eligibility. Furthermore, the amount of mandated meetings regarding individualized education plans (IEPs) and written psychological/educational reports take up almost 80% of school mental health personnel time (Curtis et al., 2008; Walcott, Charvat, McNamara, & Hyson, 2016). Interventions directly impacting student mental health, such as individual counseling, account for a relatively small amount of school clinician time (Bramlett, Murphy, Johnson, & Wallingsford, 2002; Hosp & Reschly, 2002; Walcott et al., 2016). Additionally, students suffering from anxiety are often overlooked, as they are less likely to show disruptive classroom behaviors than students with externalizing disorders, and are therefore less likely to be referred to school clinicians (Lane, Pierson, Robertson, & Little, 2004; Schoenfeld & Janney, 2008), making advanced training in CBT for these presenting problems a lower priority. Another important factor limiting the adoption of EBTs into the school setting is the diversity among school districts across the USA in terms of resources, which are often confounded with ethnicity, race, and socioeconomic status. For example, schools in rural areas often do not have full-time mental health professionals, leaving no one to provide these services (Koller & Bertel, 2006). Additionally, school mental health providers include a variety of professionals, such as school psychologists, school counselors, and social workers; hence, there is variation in their training in EBTs and ability to provide treatment for children with internalizing disorders (Foster et al., 2005).
Despite the benefits of using EBTs for anxiety disorders, their adoption and implementation in schools have not been sufficiently studied (Hicks, Shahidullah, Carlson, & Palejwala, 2014). One exception is that of Hicks et al. (2014) who surveyed 392 nationally certified school psychologists about their use of EBTs. Interestingly, nearly 71% of respondents indicated a perceived lack of adequate training in EBTs and a higher percent of those who attended an APA-accredited program, versus those who did not, took course work in EBTs. Data were collected by self-report rather than independent evaluators (IEs) listening to treatment sessions, an approach that would enhance the validity of these findings.
To the best of our knowledge, no study has assessed school clinicians’ current treatment practices for pediatric anxiety disorders. Considering the increasing awareness of the need to improve and expand school-based mental health services, these data could be helpful to assess the training needs of school clinicians, inform allocation of funds, and eventually improve the quality of care for anxious students.
Current Study
The primary aim of the current study was to describe “treatment as usual” (TAU) provided by school-based clinicians to students diagnosed with an anxiety disorder. Specifically, we examined: (1) clinicians’ perceptions of their: (a) primary approach when treating anxious students, (b) in-session therapeutic strategies (e.g., CBT, play therapy, psychodynamic) with anxious students, and (c) perceived confidence in treating pediatric anxiety disorders, and (2) IE ratings based on audiotaped sessions of: (a) CBT versus non-CBT therapeutic strategies with anxious students, (b) the frequency and quality of 11 CBT elements (e.g., set agenda, assign homework), and (c) overall competence in providing effective treatment for anxious students. An exploratory aim examined clinician characteristics as factors associated with IE-rated use of CBT.
Method
Participants
Clinicians
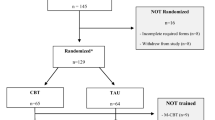
Twenty-five school clinicians who participated in a randomized controlled trial evaluating a modular CBT for youth with anxiety disorders served as participants. These clinicians came from a larger sample of 145 total clinicians consented, 64 randomized to TAU, and 53 trained in TAU study procedures; only 25 provided TAU to one or more students. The clinicians in the current study worked in 24 elementary, middle, and high schools in Maryland (n = 12) and Connecticut (n = 12). Clinicians were 96% females, 72% White (16% were Black, 8% were Multi-racial, and one clinician elected not to respond). The majority of clinicians had a master’s degree (64%), and 32% had postgraduate training (i.e., sixth-year degree, certificate of advanced study, or doctorate degree), primarily in the areas of school psychology (n = 13, 52%) or social work (n = 9, 36%). Their years of experience after graduation varied from 0 to 32 (M = 15.0, SD = 7.5), with 44% of them licensed in the state they worked. On average, clinicians reported carrying 23.1 active cases (range 8–60), and that 23.4% of children on their caseload were anxious.
Child Clients
Session data from 50 students were used in the current study. These participants came from a larger sample of 216 total students enrolled, 68 assigned to TAU, and 50 students received TAU from their school clinician and were among their first three enrolled cases. About half (n = 26, 52%) of the students were male, the mean age was 11.3 years old (SD = 3.5) and the mean grade was 6th grade (SD = 3.5). With respect to racial backgrounds, the majority of students were White (n = 28, 56%), 20 (40%) were Black and two students (4%) self-described as Multi-racial. Four students (8%) were of Hispanic ethnicity. Family income was under $31,000 for 26% of the sample (n = 13), between $31,000 and 80,000 for 32% of the sample (n = 16), and over $80,000 for 36% of the sample (n = 18), with income not reported for three students (6%). Forty-two percent of the sample (n = 21) reported receiving income-based free or reduced price lunch. All met criteria for a primary anxiety disorder.
Procedures
All clinicians volunteered to participate in a randomized controlled study evaluating treatments for anxious youth and signed written informed consent in compliance with institutional review board policies. Clinicians were recruited through e-mails to the school districts, flyers, and word of mouth. After completing baseline study measures, consented school clinicians were randomized to be trained in CBT or provide TAU.
Youth were referred to the study by school personnel, parents who received a flyer, teachers, and/or clinicians. Study staff confirmed eligibility and diagnoses using the Anxiety Disorders Interview Schedule (Silverman & Albano, 1996) which was administered by trained master’s- and doctoral-level evaluators. Eligible students were ages 6–18 and met DSM-IV criteria for a primary anxiety disorder. Youth were excluded if they had a medical or psychiatric condition contraindicating study treatment (e.g., suicidality) and needed immediate or alternative treatment, were receiving psychosocial treatment for anxiety, and/or were in the custody of state social services. Youth on stable doses of medication for a psychiatric disorder were included if they met inclusion criteria. Once a student was found eligible, clinicians were notified and expected to complete 12 weekly treatment sessions. The average number of TAU sessions received per child was 9.6 (average number of minutes per session was 20.0). Clinicians were instructed to audiotape all treatment sessions and complete a Session Summary Form (described below) after each session. For this study, only the first three cases treated by the TAU clinicians were included in order to minimize potential bias associated with any one clinician who may have seen more than three students over the course of the study. A total of 475 Session Summary Forms completed by clinicians were included in the current study. Data for this study also included randomly selected audiotapes for 25% of treatment sessions for each case enrolled when available. A total of 90 treatment sessions were coded by IEs masked to intervention condition. The sessions chosen were balanced in relation to the sample of overall sessions available. Specifically, of the sample of 90 TAU sessions in the current study, 38 (42%) were from sessions 1–4, 36 (40%) were from sessions 5–8, and 16 (18%) were from sessions 9–12.
Measures
Clinician Knowledge of CBT
The Clinician Knowledge of CBT is a 35-item measure completed by clinicians before training to assess their knowledge of CBT for pediatric anxiety. This measure was adapted from a 50-item measure designed to assess knowledge of CBT and shown to be sensitive to training-related increases in knowledge (Ginsburg, Becker, Kingery, & Nichols, 2008). Clinicians were asked to complete multiple-choice questions, such as “Which of the following is NOT an example of a therapeutic technique typically used in CBT? (a) relaxation training, (b) hypnosis, (c) problem solving, (d) exposure.” Higher percentages of correct answers indicate greater knowledge of CBT.
Evidence-Based Practice Attitude Scale Openness and Divergence Subscales (EBPAS; Aarons, 2004)
The EBPAS is a clinician-rated measure that assesses attitudes toward the adoption of evidence-based practices. Clinicians responded prior to study training by indicating the extent to which they agreed or disagreed with various statements on a 5-point Likert-type scale (0 = not at all, 4 = very great extent). For the current study, only the Divergence (four items) and Openness (four items) subscales were completed. The Divergence subscale assesses the extent to which the clinician perceives evidence-based practices as clinically useful or as important as their own clinical experience and lower scores reflect a value for EBTs. The Openness subscale assesses the extent to which the clinician is generally open to trying new interventions and would be willing to use new types of therapy and higher scores reflect greater openness (Aarons, 2004). Internal consistencies in the current sample were .54 for the Divergence subscale and .80 for the Openness subscale, similar to those in the measure development sample (.59 and .78, respectively; Aarons, 2004).
Therapist Background Questionnaire
This self-report measure was developed for the current study to assess clinicians’ demographic (e.g., age, gender, race) and professional characteristics. Specifically, the current study examined clinicians’: (1) primary theoretical orientation for treating anxiety disorders (i.e., psychodynamic, behavioral, cognitive or cognitive-behavioral, client-centered/humanistic, object relations, interpersonal, family systems/other family therapy, play therapy, or other); (2) completion of postgraduate training (i.e., sixth-year degree, certificate of advanced study, doctorate degree); (3) national certification in the field; (4) years of experience as a school clinician; (5) percentage of time spent conducting therapy in their current position; and (6) feelings of professional burnout, rated on a Likert-type scale ranging from 0 (never) to 10 (constantly).
Session Summary Form (SSF)
The SSF was adapted from prior work (Becker, Becker, & Ginsburg, 2012) and was completed by clinicians after each session. It contained items pertinent to treatment (e.g., therapeutic strategies used in session, who attended session, level of child engagement in the session, session length). In the current study, the therapeutic strategies and clinicians’ confidence in providing treatment were examined. The therapeutic strategies were: psychodynamic; behavioral; cognitive or cognitive-behavioral; client-centered/humanistic; object relations; interpersonal; family systems/other family systems; and other; and clinicians were instructed to select all that applied. Confidence was assessed through the question, “How confident are you in your ability to provide effective treatment for this anxious child?” with responses ranging from 0 (not at all confident) to 10 (extremely confident).
Treatment Adherence and Therapist Competence (TATC; Ginsburg, Becker, Drazdowski, & Tein, 2012)
The TATC is an IE-rated measure completed after reviewing audiotapes of treatment sessions. In the current study, 90 TAU sessions were reviewed and coded by postdoctoral fellows or licensed clinical psychologists. The current study examined
-
1.
Use of CBT versus other primary therapeutic strategy in the session: IEs could indicate psychodynamic, client-centered/humanistic, object relations, interpersonal, family systems/other family systems, play therapy, and other, but for the purpose of the current study these options were recoded as non-CBT. Raters indicated that a clinician used CBT if, after listening to the entire therapy session, the session contained any of the core CBT elements (i.e., psychoeducation about CBT model of anxiety, relaxation strategies, exposure, cognitive restructuring strategies, problem solving, and relapse prevention), or the clinician conducted a functional analysis of target behaviors (i.e., identified antecedents and consequences), or used learning strategies (e.g., reinforcement, extinction) to change target behaviors related to anxiety.
-
2.
Use and quality of 11 CBT elements: IEs determined whether clinicians used specific CBT strategies, which included providing an anxiety/mood rating check-in; setting and using an agenda; reviewing content from the previous session; reviewing assigned homework; working toward a specific treatment goal; teaching or reviewing a skill; modeling a skill; practicing a skill in session; using handouts/materials for a therapeutic purpose; reviewing the child’s progress; and assigning homework. For each item, IEs rated whether they used the element (yes/no) and then rated the quality of the implementation using a 4-point scale (1 = poor, 4 = very good) based on manualized scoring criteria. These items were aggregated in two summary measures, percentage of CBT elements observed and quality of CBT elements observed.
-
3.
Overall competence: IEs rated their overall perception of the clinicians’ competence in providing effective treatment during the session on an 11-point Likert-type scale (0 = not at all competent, 10 = extremely competent).
Interrater reliability was conducted on a subsample of the total number of IE-rated treatment sessions in the randomized controlled trial which included both CBT and TAU sessions (n = 61 total; 44 CBT, 17 TAU). Because the TAU sample was small, we present interrater reliability for both the full group and the TAU group. For the use of CBT, agreement between raters was 92% (75% in the TAU sample). One-way, random effects intraclass correlation coefficients (ICCs) for the percent of CBT elements observed and the quality of CBT elements were .76 and .70 (.67 and .58 for the TAU group, respectively). The ICC for overall competence was .58 (.11 for the TAU group).
Data Analytic Plan
To address the study aims, we calculated frequencies, percentages, and means (with standard deviations) to characterize clinicians’ self-reported therapeutic approach, use of specific therapeutic strategies, and clinicians’ self-reported confidence. Similarly, we calculated the frequency, percentages, and means (with standard deviations) to characterize IE-observed therapeutic strategies (CBT vs non-CBT), use and quality of CBT elements, and overall competence. To address the exploratory aim, we conducted separate linear regression analyses examining each individual clinician characteristic in relation to (a) the percentage of CBT elements and (b) quality of CBT elements observed by IEs. We also conducted separate logistic regression analyses examining each clinician characteristic in relation to IE-rated use of a behavioral or cognitive-behavioral approach in session.
Results
Table 1 presents clinicians’ self-reported treatment orientation and their reported in-session therapeutic strategies. Results indicated that a majority of school clinicians self-reported using a cognitive and/or behavioral approach to treat anxiety disorders in youth. Cognitive and/or behavioral strategies were also the most commonly reported in-session approaches. Overall, clinicians reported feeling somewhat confident (mean of 5.12 on 0–10 scale; SD = 2.13) in treating anxious students. Table 1 also presents the IE ratings (based on audiotaped sessions) of observed therapeutic strategies. The majority of IE-rated strategies were not cognitive and/or behavioral. To examine whether failure of random selection of IE-rated tapes may have affected the discrepancies between clinician and IE reports of strategies, we also examined clinician-reported strategies in the sample of tapes rated by IEs. Of the 89 IE-rated sessions with strategies identified, 84 (94%) had corresponding clinician reports, and clinicians reported using cognitive-behavioral strategies in 65 (77%) and IEs rated other strategies in 63 (75%) of these sessions. These percentages are consistent with the percentages in the larger sample of ratings by clinicians found in Table 1, suggesting random selection did not contribute to the discrepancies between clinician- and IE-reported strategies. With regard to the agreement on reported strategies within these 84 co-rated sessions, when IEs identified clinicians as using cognitive and/or behavioral strategies, clinicians also reported themselves as using these strategies in 92% of sessions (i.e., 11 of 12). However, when IEs identified clinicians as using non-cognitive-behavioral strategies, clinicians continued to report themselves as using cognitive-behavioral strategies in 75% of sessions (i.e., 54 of 72).
Table 2 presents the IE ratings of the frequency and quality of 11 CBT structure elements (e.g., sets agenda, assigns homework). The frequency and quality of CBT elements were generally low. The overall IE-rated competence score was 3.87 out of 10 (SD = 2.41). Among the factors examined in relation to CBT use shown in Table 3, postgraduate training, national certification, and more years of clinical experience were associated with greater use of CBT and CBT elements. Clinicians’ perceived value of EBTs was marginally associated with the use of CBT elements.
Discussion
Meta-analyses indicate that CBT is currently the only psychosocial EBT for anxious youth (James et al., 2015). The National Association of School Psychologists (NASP) advocates that school psychologists should be the leading mental health experts in the schools and should provide EBTs as needed (Thomas & Grimes, 2008). However, whether school-based clinicians are using CBT had not been examined using independent review of therapy sessions and thus was the primary aim of the current study. These data could inform training needs and allocation of funds, and improve the quality of care for anxious youth, an underserved population of students that experience academic, social, and behavioral impairment.
Findings indicated that the majority (68%) of school clinicians reported using a cognitive-behavioral approach with anxious youth. Similarly, when school clinicians reported what therapeutic strategies they used in each treatment session with an anxious child or adolescent (in over 450 sessions), the majority (67%) reported implementing some type of behavioral and/or cognitive-behavioral approach. Clinicians also reported that they felt somewhat confident in providing effective treatment for an anxious youth (mean score of 5 on 0–10 scale). Taken together, these findings may reflect the infiltration of EBTs into the training and/or clinical practice of school clinicians with this population—a sign that would be encouraging regarding the uptake of EBTs into schools. Findings also suggest room for improvement in the uptake of using CBT given that about 30% of clinicians reported that they do not use EBTs for this population. The second most common treatment strategy endorsed by these clinicians was a client-centered model—an approach that does not have any of the core ingredients of CBT (e.g., exposure), but may contain important non-specific support (e.g., active listening, warmth) and has been associated with positive treatment outcomes among anxious youth (Silk et al., 2018).
In contrast to clinician perspectives, IE ratings (based on a review of 90 audiotaped sessions) revealed that the most common therapeutic strategies were not cognitive-behavioral. According to IE notes on the TATCs, these non-cognitive-behavioral treatment sessions generally included casual conversation (e.g., about sports, birthdays, school, family) that did not have a specific therapeutic focus on anxiety or specific treatment goal articulated, playing board games and drawing (also with no link to anxiety or a specific treatment goal), and general non-specific emotional support. IEs (with expertise in CBT) rated clinicians’ overall competence in providing effective treatment for anxiety as below average (mean of 3.87 on the 0–10 scale) and significantly lower than clinician self-ratings of confidence. Discrepancies between self- and independent observer reports of treatment strategies have been previously documented in the literature (Hogue, Dauber, Lichvar, Bobek, & Henderson, 2015; Hurlburt, Garland, Nguyen, & Brookman-Frazee, 2010; Masia-Warner et al., 2013) and suggest potential biases in self-perceptions.
An examination of whether school clinicians used specific treatment strategies that are components of CBT as well as the quality of the implementation of these strategies indicated that almost 80% of treatment sessions included a mood/anxiety check-in and in over half of the sessions (approximately 65%), the clinician and student were working toward a therapeutic goal and the clinician taught or reviewed a therapeutic skill. In contrast, less than half of the sessions included other core CBT elements such as setting an agenda, assigning or reviewing homework requiring the child to practice therapeutic strategies, practicing a skill in session, using therapeutic handouts to foster skill acquisition, or monitoring students’ progress related to anxiety. Related, and of particular concern, is that the average quality of implementation of these elements ranged from poor (score of 1 on a 4-point scale) to fair (score of 2). Indeed, not one of the CBT element scores averaged a “good” or “very good” score (scores of 3 and 4, respectively). Interpretation of these findings suggests that while school clinicians use some elements of CBT with their anxious students, most are not used. The reasons for the low use of these therapeutic elements were not examined but may include lack of sufficient training and/or supervision, a perception that these strategies are not relevant or helpful, or a lack of time. Exploring these reasons and potential barriers is an important area of future research to increase adoption and quality implementation of EBTs.
An exploratory aim of the current study was to explore select clinician-related factors in relation to the use and quality of CBT for anxious youth. We examined seven variables in relation to CBT use including clinicians’ baseline CBT knowledge, professional training and certification, years of experience, burnout, attitudes toward adopting EBTs, and time engaged in providing therapy. Several of these factors were associated with the use of CBT or CBT elements (as rated by IEs). Specifically, clinicians with advanced degrees and those with national certifications were more likely to use CBT. This finding is partially consistent with Hicks et al. (2014), who found that clinicians in accredited programs were more likely to have taken courses in EBTs. It is likely that these advanced degrees and requirements for national certifications incorporate more EBT training, which translates to clinicians incorporating these strategies into their clinical practice. Clinician attitudes toward EBTs on the EBPAS were marginally associated with the use of CBT. Specifically, clinicians who scored high on the Divergence subscale (of the EBPAS) and thus endorsed opinions that research-based treatment manuals were not clinically useful and/or that their clinical experience was more important than clinical research trials were less likely to use CBT. Clinicians endorsing these attitudes may thus require additional evidence and/or experience showing the benefits of CBT for pediatric anxiety disorders. Of note, knowledge of CBT alone was unrelated to use/quality of CBT which suggests that additional training using experiential learning, coaching, and supervision may be essential to translate “knowing” into “using” evidenced-based practices for school clinicians as has been found in published reports (Beidas & Kendall, 2010; Eiraldi et al., 2018; Fixsen, Naoom, Blasé, Friedman, & Wallace, 2005; Sholomskas et al., 2005).
Findings from this study should be interpreted in the context of several limitations. All clinicians were volunteers, predominantly Caucasian and female, restricting the generalizability to the broader population of school-based clinicians. Also, the study only examined clinicians’ practices with respect to the treatment of anxiety disorders. Thus, whether school-based clinicians use EBTs for other disorders is unknown. While clinician data were available on over 400 treatment sessions, IE-rated data were only available for 90 treatment sessions, which may have led to biased results; additionally, constructs (e.g., confidence vs. competence) were assessed somewhat differently across raters, and specific individual elements of cognitive-behavioral therapy such as exposure or cognitive restructuring were not coded. Future studies should strive to examine a larger number of treatment sessions and use more detailed coding of treatment strategies of these tapes. Finally, because anxious youth are often under-identified and undertreated, the youth in this study may not have otherwise received any treatment and the findings may have limited generalizability.
Despite these limitations, findings from this study suggest that while a majority of school-based clinicians report that they use cognitive and/or behavioral strategies for treating anxiety disorders (the most strongly supported EBT for these illnesses), the percent of clinicians actually using these strategies and the quality of implementation shows room for improvement. One approach for improving the quality of CBT may be to encourage and support school counselors in pursuing national certification and/or advanced training.
References
Aarons, G. A. (2004). Mental health provider attitudes towards adoption of evidence-based practice: The Evidence-Based Practice Attitude Scale (EBPAS). Mental Health Services Research,6, 61–74.
American Academy of Pediatrics. (2004). School-based mental health services. Pediatrics,113, 1839–1845.
Andrade, L. H., Alonso, J., Mneimneh, Z., Wells, J. E., Al-Hamzawi, A., Borges, G., et al. (2014). Barriers to mental health treatment: Results from the WHO World Mental Health surveys. Psychological Medicine,44, 1303–1317.
Becker, E. M., Becker, K. D., & Ginsburg, G. S. (2012). Modular cognitive behavioral therapy for youth with anxiety disorders: A closer look at the use of specific modules and their relation to treatment process and response. School Mental Health,4, 243–253.
Beidas, R. S., & Kendall, P. C. (2010). Training therapists in evidence-based practice: A critical review of studies from a systems-contextual perspective. Clinical Psychology: Science and Practice,17, 1–30.
Bramlett, R. K., Murphy, J. J., Johnson, J., & Wallingsford, L. (2002). Contemporary practices in school psychology: A national survey of roles and referral problems. Psychology in the Schools,39, 327–335.
Breslau, J., Lane, M., Sampson, N., & Kessler, R. C. (2008). Mental disorders and subsequent educational attainment in a US national sample. Journal of Psychiatric Research,42(9), 708–716.
Chavira, D. A., Stein, M. B., Bailey, K., & Stein, M. T. (2004). Child anxiety in primary care: Prevalent but untreated. Depression and Anxiety,20, 155–164.
Copeland, W., Shanahan, L., & Costello, E. J. (2011). Cumulative prevalence of psychiatric disorders by young adulthood: A prospective cohort analysis from the Great Smoky Mountains Study. Journal of the American Academy of Child and Adolescent Psychiatry,50, 252–261.
Costello, E. J., Egger, H. L., & Angold, A. (2005). The developmental epidemiology of anxiety disorders: Phenomenology, prevalence, and comorbidity. Child and Adolescent Psychiatric Clinics of North America,14, 631–648.
Curtis, M., Lopez, A., Castillo, J., Batsche, G., Minch, D., & Smith, J. (2008). The status of school psychology: Demographic characteristics, employment conditions, professional practices, and continuing professional development. Communique,36, 27–29.
Duchesne, S., Vitaro, F., Larose, S., & Tremblay, R. E. (2008). Trajectories of anxiety during elementary-school years and the prediction of high school noncompletion. Journal of Youth and Adolescence,37(9), 1134–1146.
Eiraldi, R., Mautone, J. A., Khanna, M. S., Power, T. J., Orapallo, A., Cacia, J., et al. (2018). Group CBT for externalizing disorders in urban schools: Effect of training strategy on treatment fidelity and child outcomes. Behavior Therapy,49, 538–550.
Fixsen, D. L., Naoom, S. F., Blasé, K. A., Friedman, R. M., & Wallace, F. (2005). Implementation research: A synthesis of the literature (FMHI Publication No. 231). Tampa: University of South Florida, Louis de la Parte Florida Mental Health Institute, The National Implementation Research Network.
Foster, S., Rollefson, M., Doksum, T., Noonan, D., Robinson, G., & Teich, J. (2005). School Mental Health Services in the United States, 2002–2003. DHHS Pub. No. (SMA) 05-4068. Rockville, MD: Center for Mental Health Services, Substance Abuse and Mental Health Services Administration.
Gibby, B. A., Casline, E. P., & Ginsburg, G. S. (2017). Long-term outcomes of youth treated for an anxiety disorder: A critical review. Clinical Child and Family Psychology Review,20, 201–225.
Ginsburg, G. S., Becker, K. D., Drazdowski, T. K., & Tein, J. (2012). Treating anxiety disorders in inner city schools: Results from a pilot randomized controlled trial comparing CBT and usual care. Child & Youth Care Forum,41, 1–19.
Ginsburg, G. S., Becker, K. D., Kingery, J. N., & Nichols, T. (2008). Transporting CBT for childhood anxiety disorders into inner-city school-based mental health clinics. Cognitive and Behavioral Practice,15, 148–158.
Ginsburg, G. S., Becker-Haimes, E. M., Keeton, C. P., Kendall, P. C., Iyengar, S., Sakolsky, D., et al. (2018). Results from the Child/Adolescent Anxiety Multimodal Extended Long-term Study (CAMELS): Primary anxiety outcomes. Journal of the American Academy of Child and Adolescent Psychiatry,57, 471–480.
Hansen, C., Sanders, S. L., Massaro, S., & Last, C. G. (1998). Predictors of severity of absenteeism in students with anxiety-based school refusal. Journal of Clinical Child & Adolescent Psychology,27(3), 246–254.
Hicks, T. B., Shahidullah, J. D., Carlson, J. S., & Palejwala, M. H. (2014). Nationally certified school psychologists’ use and reported barriers to using evidence-based interventions in schools: The influence of graduate program training and education. School Psychology Quarterly,29, 469–487.
Higa-McMillan, C. K., Francis, S. E., Rith-Najarian, L., & Chorpita, B. F. (2016). Evidence base update: 50 years of research on treatment for child and adolescent anxiety. Journal of Clinical Child & Adolescent Psychology,45, 91–113.
Hogue, A., Dauber, S., Lichvar, E., Bobek, M., & Hendersen, C. E. (2015). Validity of therapist self-report ratings of fidelity to evidence-based practices for adolescent behavior problems: Correspondence between therapists and observers. Administration and Policy in Mental Health and Mental Health Services Research,42, 229–243.
Hosp, J. L., & Reschly, D. J. (2002). Regional differences in school psychology practice. School Psychology Review,31, 11–29.
Hughes, A. A., Lourea-Waddell, B., & Kendall, P. C. (2008). Somatic complaints in children with anxiety disorders and their unique prediction of poorer academic performance. Child Psychiatry and Human Development,39(2), 211–220.
Hurlburt, M. S., Garland, A. F., Nguyen, K., & Brookman-Frazee, L. (2010). Child and family therapy process: Concordance of therapist and observational perspectives. Administration and Policy in Mental Health and Mental Health Services Research,37, 230–244.
In-Albon, T., & Schneider, S. (2007). Psychotherapy of childhood anxiety disorders: A meta-analysis. Psychotherapy and Psychosomatics,76, 15–24.
Jagdeo, A., Cox, B. J., Stein, M. B., & Sareen, J. (2009). Negative attitudes toward help seeking for mental illness in 2 population-based surveys from the United States and Canada. The Canadian Journal of Psychiatry,54, 757–766.
James, A. C., James, G., Cowdrey, F. A., Soler, A., & Choke, A. (2015). Cognitive behavioural therapy for anxiety disorders in children and adolescents. Cochrane Database of Systematic Reviews,2015(2), 1–106.
Koller, J. R., & Bertel, J. M. (2006). Responding to today’s mental health needs of children, families and schools: Revisiting the preserve training and preparation of school-based personnel. Education and Treatment of Children,29, 197–217.
Lane, K. L., Pierson, M. R., Roberston, E. J., & Little, A. (2004). Teachers’ views of prereferral interventions: Perceptions of and recommendations for implementation support. Education and Treatment of Children,27, 420–439.
Masia-Warner, C., Brice, C., Esseling, P. G., Stewart, C. E., Mufson, L., & Herzig, K. (2013). Consultants’ perceptions of school counselors’ ability to implement an empirically-based intervention for adolescent social anxiety disorder. Administration and Policy in Mental Health and Mental Health Services Research,40, 541–554.
Mazzone, L., Ducci, F., Scoto, M. C., Passaniti, E., D’Arrigo, V. G., & Vitiello, B. (2007). The role of anxiety symptoms in school performance in a community sample of children and adolescents. BMC Public Health,7, 347.
McHugh, R. K., & Barlow, D. H. (2010). The dissemination and implementation of evidence-based psychological treatments: A review of current efforts. American Psychologist,65, 73–84.
Merikangas, K. R., He, J., Brody, D., Fisher, P. W., Bourdon, K., & Koretz, D. S. (2010). Prevalence and treatment of mental disorders among U.S. children in the 2001–2004 NHANES. Pediatrics,125, 75–81.
Olfson, M., Mojtabai, R., Sampson, N. A., Hwang, I., Druss, B., Wang, P. S., et al. (2009). Dropout from outpatient mental health care in the United States. Psychiatric Services,60, 898–907.
Peris, T. S., Caporino, N. E., O’Rourke, S., Kendall, P. C., Walkup, J. T., Albano, A., et al. (2017). Therapist-reported features of exposure tasks that predict differential treatment outcomes for youth with anxiety. Journal of the American Academy of Child and Adolescent Psychiatry,56, 1043–1052.
Peris, T. S., Compton, S. N., Kendall, P. C., Birmaher, B., Sherrill, J., March, J., et al. (2015). Trajectories of change in youth anxiety during cognitive-behavior therapy. Journal of Consulting and Clinical Psychology,83, 239–252.
Sareen, J., Jagdeo, A., Cox, B. J., Clara, I., ten Have, M., Belik, S., et al. (2007). Perceived barriers to mental health service utilization in the United States, Ontario, and the Netherlands. Psychiatric Services,58, 357–364.
Schoenfeld, N. A., & Janney, D. M. (2008). Identification and treatment of anxiety in students with emotional or behavioral disorders: A review of the literature. Education and Treatment of Children,31, 583–610.
Scholten, W. D., Batelaan, N. M., van Balkom, A. J. L. M., Penninx, B. W. J. H., Smit, J. H., & van Oppen, P. (2013). Recurrence of anxiety disorders and its predictors. Journal of Affective Disorders,147, 180–185.
Sholomskas, D. E., Syracuse-Siewart, G., Rounsaville, B. J., Ball, S. A., Nuro, K. F., & Carroll, K. M. (2005). We don’t train in vain: A dissemination trial of three strategies of training clinicians in cognitive-behavioral therapy. Journal of Consulting and Clinical Psychology,73, 106–115.
Silk, J. S., Tan, P. Z., Ladouceur, C. D., Meller, S., Siegle, G. J., McMakin, D. L., et al. (2018). A randomized clinical trial comparing individual cognitive behavioral therapy and child-centered therapy for child anxiety disorders. Journal of Clinical Child & Adolescent Psychology,47, 542–554.
Silverman, W. K., & Albano, A. M. (1996). Anxiety Disorders Interview Schedule for DSM-IV: Child and parent versions. New York, NY: Oxford University Press.
Swan, A. J., & Kendall, P. C. (2016). Fear and missing out: Youth anxiety and functional outcomes. Clinical Psychology: Science and Practice,23, 417–435.
Thomas, A., & Grimes, J. (2008). Best practices in school psychology. Bethesda, MA: National Association of School Psychologists.
Walcott, C. M., Charvat, J., McNamara, K. M., & Hyson, D. M. (2016). School psychology at a glance: 2015 member survey results. Presented at the 2016 National Association of School Psychologists, special session 20.
Wang, P. S., Aguilar-Gaxiola, S., Alonso, J., Angermeyer, M., Borges, G., Bromet, E. J., et al. (2007). Use of mental health services for anxiety, mood, and substance disorders in 17 countries in the WHO world mental health surveys. The Lancet,9590, 841–850.
Weist, M. D., Bruns, E., Whitaker, K., Wei, Y., Kutcher, S., Larsen, T., et al. (2017). School mental health promotion and intervention: Experiences from four nations. School Psychology International,38, 343–362.
Acknowledgements
We are grateful for the hard work and support of many research assistants and school personnel throughout the course of the study. The authors would also like to thank all the clinicians, students, and parents who participated in the study. We are especially grateful to Kelly Drake, Jeff Pella, Sarah Williams, Amy Hale, Courtney Keeton, and Brian Padilla.
Funding
The research reported here was supported by the Institute of Education Sciences, US Department of Education, through Grant R324A120405 to Dr. Ginsburg. The opinions expressed are those of the authors and do not represent views of the institute or the US Department of Education.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Ginsburg serves as a consultant for Syneos Heath and receives funding from the National Institute of Mental Health and the Institute of Education Sciences. The other authors declare that they have no conflicts of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ginsburg, G.S., Muggeo, M., Caron, E.B. et al. Exploring Treatment as Usual for Pediatric Anxiety Disorders Among School-Based Clinicians. School Mental Health 11, 719–727 (2019). https://doi.org/10.1007/s12310-019-09331-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12310-019-09331-3