Abstract
Iatrogenic immunodeficiency-associated lymphoproliferative disorders (IA-LPD) may arise in patients treated with immunosuppressive drugs for autoimmune disease or other conditions. Polymorphic EBV-positive B-lymphoproliferations often have features mimicking Hodgkin lymphoma and typically a self-limited, indolent course. We present an unusual case with isolated, intracerebral manifestation of polymorphic B-LPD with features of classic Hodgkin-lymphoma in an immunosuppressed patient treated with methotrexate and infliximab, including clinical-radiological features and a detailed description of morphological findings, together with a literature review on reported cases of primary CNS manifestation of cHL and IA-LPD with Hodgkin-like morphology. The patient achieved complete remission following neurosurgery with gross total tumor resection and drug withdrawal without any additional treatment. Post-operative staging revealed no evidence for focal relapse or systemic disease during the 18 months follow-up period. Among the previously reported 24 cases of primary, isolated Hodgkin lymphoma in the central nervous system, three similar cases of iatrogenic, IA-LPDs were identified and are discussed here. Polymorphic B-LPD are destructive lesions with a range of morphologic features and disease manifestations. It is clinically important to recognize the spectrum of proliferations with features of classic Hodgkin lymphoma in immunodeficiency, iatrogenic settings, because they are likely to impact the choice of treatment strategies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Iatrogenic, immunodeficiency-associated lymphoproliferative disorders (IA-LPDs) are defined as lymphoid proliferations or lymphomas, arising in patients after long-term treatment with immunosuppressive drugs for an underlying autoimmune disease or other (non-hematological) disease in the non-transplant setting [1]. Methotrexate was the first reported immunosuppressive agent associated with iatrogenic LPD [2, 3]. Later on, cases of large B-cell lymphoma and classic Hodgkin lymphoma (cHL) were described in patients treated with TNF inhibitors [4–7]. The iatrogenic, immunodeficiency-associated LPDs constitute a spectrum of disease manifestations, including both cHL and LPDs with Hodgkin-like features. The latter likely represent EBV-positive B-cell LPDs and have similar features as the newly recognized EBV-positive mucocutaneous ulcer (EBVMCU), typically with a self-limited, indolent course [8].
We present a case of iatrogenic, immunodeficiency-associated, EBV-positive polymorphic LPD with morphology mimicking Hodgkin lymphoma in the CNS after long-term treatment with both methotrexate and infliximab (TNF inhibitor). The patient had no evidence of systemic disease and achieved complete remission after neurosurgery and drug withdrawal without any additional treatment. Among the previously reported 24 cases of primary, isolated CNS manifestation of HL, three additional cases of iatrogenic, immunodeficiency-associated EBV-positive LPD were identified and are discussed here.
Clinical history
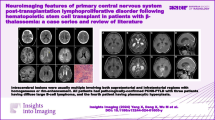
A 75-year-old woman presented to the emergency department with acute onset of hemiparesis, impaired consciousness, and facial droop. Her past medical history included a diagnosis of neurosarcoidosis and long-term immunosuppressive treatment with methotrexate and infliximab (TNF inhibitor) for at least 6 years. A magnetic resonance imaging scan (MRI) of the brain revealed a solitary, well-circumscribed, contrast-enhancing, left-sided supratentorial lesion measuring approximately 2 cm with significant perifocal edema and mass effect (Fig.1). The patient’s neurological symptoms slightly improved following pre-operative corticosteroid administration. She underwent craniotomy for gross total resection of the lesion. The excised specimen consisted of several tissue fragments measuring up to 1.8 × 1.4 × 0.8 cm. Histological examination revealed a sharply demarcated, EBV-positive polymorphic infiltrate with Hodgkin-like cells, consistent with a diagnosis of iatrogenic, immunodeficiency associated lymphoproliferative disorder (IA-LPD). Methotrexate and infliximab were immediately withdrawn. An extensive staging work-up, including ultrasound and CT scan of the chest and abdomen, revealed no lymphadenopathy or other sign of systemic disease. Bone marrow examination was normal. Further extensive laboratory tests were reported unrevealing, but specific information on EBV serology testing was not available. The patient’s postoperative course was uneventful. A CT of the brain 6 and 12 months after surgery demonstrated only minor post-operative changes, and the patient achieved complete remission without any additional treatment. She died 18 months after initial presentation secondary to bacterial pneumonia and SARS-CoV2 infection.
Materials and methods
The tissue was fixed in 4% buffered paraformaldehyde solution and embedded in paraffin. Tissue sections were stained with hematoxylin-eosin and Giemsa. Immunohistochemical stainings included CD3 (2GV6), CD20 (clone L26), CD15 (MMA), CD30 (Ber-H2), CD45 (RP2-18), CD68 (PG-M1), BOB-1 (SP-92), OCT-2 (MRQ-2), CD79a (SP-18), CD23 (SP-23), MUM-1 (EP190), PAX5 (SP34), p53 (DO-7), Ki67 (30-9), CD138 (clone B-A38) (all Roche/Ventana), kappa/lambda (polyklonal, Dako), and LMP-1 (CS.1-4, Dako) using an automated immunostaining system (Ventana Medical Systems). In situ hybridization for Epstein-Barr virus RNA (EBER transcripts) was performed on formalin fixed paraffin sections (FFPE) using the EBER-1 probe (Novocastra Laboratories, New castle upon Tyne, UK). PCR-analysis for immunoglobulin (IG) gene rearrangements was performed using genomic DNA isolated from FFPE tissue blocks (QIAGEN Tissue kit) and BIOMED-2 primers according to the BIOMED-2 PCR based protocol [9].
Results
Routine H&E staining demonstrated a well-circumscribed, intracerebral lesion consisting of a polymorphous infiltrate with a mixture of small lymphocytes, numerous polyclonal plasma cells, eosinophils, histiocytes and scattered large, atypical mono- and multinucleated, Hodgkin- and Reed-Sternberg-like cells (Fig. 2). The large cells stained positive for CD30, CD79a, OCT-2, PAX5, MUM-1, and p53, but mostly negative for CD20. The cells lacked expression for CD15, BOB-1, and CD45. In situ hybridization for EBER showed a range of EBV+ cells, including both large cells and numerous small lymphocytes. PCR analysis showed no evidence for immunoglobulin heavy chain gene rearrangement (not shown). In the context of the combined clinical, morphological, and immunohistochemical findings and long-standing treatment with methotrexate and TNF inhibitor, a diagnosis of iatrogenic, immunodeficiency-associated EBV-positive polymorphic LPD with Hodgkin-like features was established.
Histological examination demonstrates a well-demarcated, intracerebral polymorphic infiltrate with small lymphocytes, numerous plasma cells, eosinophilic granulocytes, and scattered large cells with Hodgkin/Reed-Sternberg morphology (a,b). The atypical cells stain positive for CD30 (c), negative for CD15 (d) and CD20 (e), CD79a weakly positive (f), and positive for both LMP-1 (g) and EBER/EBV (h)
Review of the literature
Among the 24 published reports on primary, isolated CNS manifestation of cHL between 1980 and 2020 [10–33], three were diagnosed in patients with underlying autoimmune diseases and long-term immunosuppressive treatment. Therefore, these cases fall into the same WHO category of “other iatrogenic immunodeficiency-associated lymphoproliferative disorders” (Table 1) [18, 27, 28] . Two patients (66 and 47 years) with myasthenia gravis had been treated with azacytidine for 12 and > 20 years, and the other patient (74 years) had received long-term treatment with methotrexate and infliximab for rheumatoid arthritis. The lesions were intracerebral (frontoparietal lobe, cerebellum) and intraspinal, measuring between 1.4 cm and 3.5 cm in size. Complete surgical resection was achieved in two cases, while one patient with spinal engagement had diagnostic needle biopsies. Histology showed in all three cases a polymorphic infiltrate with scattered large, EBV+, and CD30+ HRS-like cells with variable expression of B-cell markers and negativity for CD15. PCR for heavy chain gene rearrangement indicated clonality in one case (no data available for the two other cases). Post-operative staging revealed no evidence for systemic disease in any of the patients. Two patients received additional radio-chemotherapy, while one patient was treated with radiotherapy only. All three patients were in complete remission at 3, 9, and 18 months follow-up, respectively. Therefore, the case presented here is the first reported case with complete remission without additional chemo- or radiation therapy.
Among the other reported cases in the literature diagnosed as isolated cHL in the CNS (summarized in Suppl. Table 1), one patient had an underlying autoimmune hyperthyroidism (Graves’ disease) treated with radioactive iodine [17], and another patient had been treated with immunosuppressive drugs after a renal transplant [32], while the past medical history was unremarkable in all other reported cases.
Discussion
We describe an unusual case of immunodeficiency-associated polymorphic B-cell LPD with cells mimicking Hodgkin cells which presented as a solitary lesion in the brain without evidence of systemic disease. The patient had a history of neurosarcoidosis and been treated with Methotrexate and Infliximab. Three similar cases with isolated CNS manifestation have been reported in immunocompromised patients, all with an indolent clinical course. In contrast to our case, these patients received combined radio-chemotherapy or radiotherapy only. Importantly, no evidence for systemic disease was detected during clinical follow-up. The described lesions had morphological features of classic Hodgkin lymphoma, e.g., presence of Hodgkin/Reed-Sternberg cells in an appropriate reactive/inflammatory background. Acknowledging the diverse overlapping histological patterns of cHL and EBV+ B-LPD with cells that mimic Hodgkin cells in the setting of iatrogenic immunodeficiency-associated LPD, a combination of clinical, morphological, and immunophenotypic findings is needed for reaching the correct diagnosis. For example, the lack of CD15-expression and variable expression of B-cell markers in CD30-positive HRS-like cells (all four cases) have been considered a feature against the diagnosis of cHL [34]. An additional useful parameter not typical for cHL is the wider range in cell size of the EBV-positive cells as highlighted by CD20, CD30, and EBER. EBV is almost always found in polymorphic LPD with Hodgkin-like features, including the newly recognized EBV-positive mucocutaneous ulcer [8]. Such cases have been described at different anatomic locations. In a more recent paper, Marcelis et al. describe a series of 72 biopsy-confirmed cases with immunomodulatory agent-related LPD of which the majority were non-Hodgkin lymphomas; cHL and polymorphic B-LPD represented 6 and 8 of the cases, respectively, and none of these presented as CNS manifestation. An association with EBV was seen in 75% of LPDs, with lower frequencies in other entities [35]. Given the clinical and histopathologic heterogeneity of IA-LPDs, the importance of adequate diagnostic material cannot be underemphasized [36].
Conclusion
Iatrogenic immunodeficiency-associated LPD constitute a spectrum of disease manifestations, including EBV+ B-LPD with Hodgkin-like cells and cases that fulfil the criteria of classic Hodgkin lymphoma. The primary, isolated CNS manifestation of cHL is exceedingly rare [37–39]. Correct diagnosis is facilitated by consideration of the clinical history and the observed spectrum of EBV-positive cells. The importance of recognizing underlying immunodeficiency is crucial for appropriate treatment choice and remains a challenge for hematologists and oncologists. However, the high regression rate upon withdrawal of immunosuppressive therapy in some cases points to a condition for which a graded approach with conservative management is advised in order to avoid unnecessary chemo-/radiotherapy.
Availability of data and material
Not applicable.
Code availability
Not applicable.
References
Swerdlow SH (2017) WHO classification of tumours of haematopoietic and lymphoid tissues. International Agency for Research on Cancer, Lyon
Kamel OW, van de Rijn M, Weiss LM, Del Zoppo GJ, Hench PK, Robbins BA, Montgomery PG, Warnke RA, Dorfman RF (1993) Brief report: reversible lymphomas associated with Epstein-Barr virus occurring during methotrexate therapy for rheumatoid arthritis and dermatomyositis. N Engl J Med 328(18):1317–1321. https://doi.org/10.1056/NEJM199305063281806
Salloum E, Cooper DL, Howe G, Lacy J, Tallini G, Crouch J, Schultz M, Murren J (1996) Spontaneous regression of lymphoproliferative disorders in patients treated with methotrexate for rheumatoid arthritis and other rheumatic diseases. J Clin Oncol 14(6):1943–1949. https://doi.org/10.1200/JCO.1996.14.6.1943
Brown SL, Greene MH, Gershon SK, Edwards ET, Braun MM (2002) Tumor necrosis factor antagonist therapy and lymphoma development: twenty-six cases reported to the Food and Drug Administration. Arthritis Rheum 46(12):3151–3158. https://doi.org/10.1002/art.10679
Loo EY, Medeiros LJ, Aladily TN, Hoehn D, Kanagal-Shamanna R, Young KH, Lin P, Bueso-Ramos CE, Manning JT Jr, Patel K, Thomazy V, Brynes RK, Goswami M, Fayad LE, Miranda RN (2013) Classical Hodgkin lymphoma arising in the setting of iatrogenic immunodeficiency: a clinicopathologic study of 10 cases. Am J Surg Pathol 37(8):1290–1297. https://doi.org/10.1097/PAS.0b013e31828e6564
Lopez-Olivo MA, Tayar JH, Martinez-Lopez JA, Pollono EN, Cueto JP, Gonzales-Crespo MR, Fulton S, Suarez-Almazor ME (2012) Risk of malignancies in patients with rheumatoid arthritis treated with biologic therapy: a meta-analysis. JAMA 308(9):898–908. https://doi.org/10.1001/2012.jama.10857
Miranda RN, Loo E, Medeiros LJ (2013) Iatrogenic immunodeficiency-associated classical hodgkin lymphoma: clinicopathologic features of 54 cases reported in the literature. Am J Surg Pathol 37(12):1895–1897. https://doi.org/10.1097/PAS.0000000000000095
Dojcinov SD, Venkataraman G, Raffeld M, Pittaluga S, Jaffe ES (2010) EBV positive mucocutaneous ulcer–a study of 26 cases associated with various sources of immunosuppression. Am J Surg Pathol 34(3):405–417. https://doi.org/10.1097/PAS.0b013e3181cf8622
Langerak AW, Groenen PJ, Bruggemann M, Beldjord K, Bellan C, Bonello L, Boone E, Carter GI, Catherwood M, Davi F, Delfau-Larue MH, Diss T, Evans PA, Gameiro P, Garcia Sanz R, Gonzalez D, Grand D, Hakansson A, Hummel M, Liu H, Lombardia L, Macintyre EA, Milner BJ, Montes-Moreno S, Schuuring E, Spaargaren M, Hodges E, van Dongen JJ (2012) EuroClonality/BIOMED-2 guidelines for interpretation and reporting of Ig/TCR clonality testing in suspected lymphoproliferations. Leukemia 26(10):2159–2171. https://doi.org/10.1038/leu.2012.246
Nagashima K, Mori S, Yoshimasu N, Takahashi K (1980) Primary Hodgkin’s disease of the falx cerebri. Acta Neuropathol 51(2):161–163. https://doi.org/10.1007/BF00690459
Bender BL, Mayernik DG (1986) Hodgkin’s disease presenting with isolated craniospinal involvement. Cancer 58(8):1745–1748. https://doi.org/10.1002/1097-0142(19861015)58:8%3c1745::aid-cncr2820580827%3e3.0.co;2-4
Doorly TP, Farrell MA, Phillips J (1987) Primary intracerebral Hodgkin’s lymphoma. J Neurol Neurosurg Psychiatry 50(8):1048–1050. https://doi.org/10.1136/jnnp.50.8.1048
Ashby MA, Barber PC, Holmes AE, Freer CE, Collins RD (1988) Primary intracranial Hodgkin’s disease. A case report and discussion. Am J Surg Pathol 12(4):294–299
Sickler GK, Hanson SK, Hsu SM, Papasozomenos SC (1990) Primary intracerebral Hodgkin’s disease: a case report. Clin Neuropathol 9(3):143–147
Clark CW, Callihan T, Schwarzberg L, Fontanesi J (1992) Primary intracranial Hodgkin’s lymphoma without dural attachment. Case report. J Neurosurgery 76:692–695
Klein R, Mullges W, Bendszus M, Woydt M, Kreipe H, Roggendorf W (1999) Primary intracerebral Hodgkin’s disease: report of a case with Epstein-Barr virus association and review of the literature. Am J Surg Pathol 23(4):477–481. https://doi.org/10.1097/00000478-199904000-00014
Biagi J, MacKenzie RG, Lim MS, Sapp M, Berinstein N (2000) Primary Hodgkin’s disease of the CNS in an immunocompetent patient: a case study and review of the literature. Neuro Oncol 2(4):239–243. https://doi.org/10.1093/neuonc/2.4.239
Herrlinger U, Klingel K, Meyermann R, Kandolf R, Kaiserling E, Kortmann RD, Melms A, Skalej M, Dichgans J, Weller M (2000) Central nervous system Hodgkin’s lymphoma without systemic manifestation: case report and review of the literature. Acta Neuropathol 99(6):709–714. https://doi.org/10.1007/s004010051185
Johnson MD, Kinney MC, Scheithauer BW, Briley RJ, Hamilton K, McPherson WF, Barton JH Jr (2000) Primary intracerebral Hodgkin’s disease mimicking meningioma: case report. Neurosurgery 47(2):454–456. https://doi.org/10.1097/00006123-200008000-00038 (discussion 456-457)
Heran NS, Yong RL, Heran MS, Yip S, Fairholm D (2006) Primary intradural extraarachnoid hodgkin lymphoma of the cervical spine. Case report. J Neurosurg Spine 5(1):61–64. https://doi.org/10.3171/spi.2006.5.1.61
Castro de AF, Junior AS, de Lins e Horta H, Neuenschwander LC, Fonseca RP, Lima SS, VS Lima (2007) Primary intracerebral Hodgkin lymphoma. Br J Haematol 138(5):562. https://doi.org/10.1111/j.1365-2141.2007.06710.x
Hwang CYS, Young-Jin K, Chul D (2007) Primary Cerebellar Hodgkin’s Lymphoma. J Korean Neurosurg Soc 42:149–152
Chotai N, Dutta R (2010) Primary intradural Hodgkin’s lymphoma in lumbosacral spine: a rare location. Clin Neuroradiol 20(4):247–249. https://doi.org/10.1007/s00062-010-0018-5
Foo WC, Desjardins A, Cummings TJ (2011) Primary intracerebral Hodgkin lymphoma with recurrence. Clin Neuropathol 30(2):75–79. https://doi.org/10.5414/npp30075
Kresak JL, Nguyen J, Wong K, Davis R (2013) Primary Hodgkin lymphoma of the central nervous system: two case reports and review of the literature. Neuropathology 33(6):658–662. https://doi.org/10.1111/neup.12035
Gessi M, Kuchelmeister K, Kellner U, Ritter M, Morgner A, Urbach H, Hanel M, Simon M, Pietsch T (2013) Unusual clinico-pathological features in primary Hodgkin’s lymphomas of the central nervous system. Acta Neurochir (Wien) 155(1):19–24. https://doi.org/10.1007/s00701-012-1535-6
Henkenberens C, Franzke A, Raab P, Oschlies I, Klapper W, Christiansen H (2014) Primary EBV-positive Hodgkin’s lymphoma of the CNS under azathioprine treatment: case report and review of the literature. Strahlenther Onkol 190(9):847–852. https://doi.org/10.1007/s00066-014-0670-9
Martinez DL, Gujrati M, Geoffroy F, Tsung AJ (2014) Isolated CNS Hodgkin’s lymphoma: implications for tissue diagnosis. CNS Oncol 3(6):383–387. https://doi.org/10.2217/cns.14.45
Sharaf N, Lobo B, Lee J, Prayson RA (2014) Primary Hodgkin lymphoma of the central nervous system. J Clin Neurosci 21(7):1271–1273. https://doi.org/10.1016/j.jocn.2013.10.034
Shivane A, Smith ME, Lewis D, Berei T (2016) A rare case of primary intracerebral Hodgkin lymphoma. Clin Neuropathol 35(6):389–392. https://doi.org/10.5414/NP300964
Alfaseh A, Rajeh MN, Hamed G (2019) Primary central nervous system Hodgkin lymphoma: a case discussion and a hypothesis on the etiology. Avicenna J Med 9(1):28–31. https://doi.org/10.4103/ajm.AJM_104_18
Azriel A, Towner JE, Gaillard F, Box G, Rogers T, Morokoff A (2019) Solitary intraventricular Hodgkin lymphoma post-transplant lymphoproliferative disease (HL-PTLD): case report. J Clin Neurosci 69:269–272. https://doi.org/10.1016/j.jocn.2019.08.053
Williamson TJ, Wang M, Clark J, Williams J, Drnda A (2020) Primary intradural Hodgkin lymphoma of the conus medullaris and cauda equina: case report. CNS Oncol 9(3):CNS52. https://doi.org/10.2217/cns-2020-0002
Kamel OW, Weiss LM, van de Rijn M, Colby TV, Kingma DW, Jaffe ES (1996) Hodgkin’s disease and lymphoproliferations resembling Hodgkin’s disease in patients receiving long-term low-dose methotrexate therapy. Am J Surg Pathol 20(10):1279–1287. https://doi.org/10.1097/00000478-199610000-00015
Marcelis L, Berghen C, De Zutter A, Biesemans P, Vandenberghe P, Verhoef G, Gheysens O, Sagaert X, Dierickx D, Tousseyn T (2018) Other immunomodulatory agent-related lymphoproliferative diseases: a single-center series of 72 biopsy-confirmed cases. Mod Pathol 31(9):1457–1469. https://doi.org/10.1038/s41379-018-0054-2
Natkunam Y, Gratzinger D, Chadburn A, Goodlad JR, Chan JKC, Said J, Jaffe ES, de Jong D (2018) Immunodeficiency-associated lymphoproliferative disorders: time for reappraisal? Blood 132(18):1871–1878. https://doi.org/10.1182/blood-2018-04-842559
Cheah CY, Brockelmann PJ, Chihara D, Moskowitz AJ, Engert A, Jerkeman M, El-Galaly TC, Augustson B, Vose J, Bartlett NL, Villa D, Connors JM, Feldman T, Pinnix CC, Milgrom SA, Dabaja B, Oki Y, Fanale MA (2016) Clinical characteristics and outcomes of patients with Hodgkin lymphoma with central nervous system involvement: an international multicenter collaboration. Am J Hematol 91(9):894–899. https://doi.org/10.1002/ajh.24429
Gerstner ER, Abrey LE, Schiff D, Ferreri AJ, Lister A, Montoto S, Tsang R, Thiel E, Graus F, Behringer D, Illerhaus G, Weaver S, Wen P, Voloschin A, Harris NL, Batchelor TT (2008) CNS Hodgkin lymphoma. Blood 112(5):1658–1661. https://doi.org/10.1182/blood-2008-04-151563
Re D, Fuchs M, Schober T, Engert A, Diehl V (2007) CNS involvement in Hodgkin’s lymphoma. J Clin Oncol 25(21):3182. https://doi.org/10.1200/JCO.2007.12.5088
Funding
Open access funding provided by Karolinska Institute.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
Local institutional ethical guidelines are followed and informed; written consent regarding participation was obtained from the patient.
Informed consent
Consent was obtained from the patient at time of hospitalization which is documented in the hospital clinical journal.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This case report was orally presented at the 20th meeting (virtual) of the European Association of Hematopathology (EAHP 2021), lymphoma workshop.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Saft, L., Perdiki-Grigoriadi, M. & Rassidakis, G. Intracerebral manifestation of iatrogenic, immunodeficiency-associated polymorphic B-LPD with morphology mimicking Hodgkin lymphoma: a case report and literature review. J Hematopathol 15, 13–19 (2022). https://doi.org/10.1007/s12308-021-00478-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12308-021-00478-0