Abstract
Atherosclerosis is a chronic inflammatory disease that is the underlying cause of cardiovascular disease which initiates from endothelial dysfunction from genetic and environmental risk factors, including biomechanical forces: blood flow. Endothelial cells (ECs) lining the inner arterial wall regions exposed to disturbed flow are prone to atherosclerosis development, whereas the straight regions exposed to stable flow are spared from the disease. These flow patterns induce genome- and epigenome-wide changes in gene expression in ECs. Through the sweeping changes in gene expression, disturbed flow reprograms ECs from athero-protected cell types under the stable flow condition to pro-atherogenic cell conditions. The pro-atherogenic changes induced by disturbed flow, in combination with additional risk factors such as hypercholesterolemia, lead to the progression of atherosclerosis. The flow-sensitive genes and proteins are critical in understanding the mechanisms and serve as novel targets for antiatherogenic therapeutics.
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Atherosclerosis is a chronic, progressive, and lipid-driven inflammatory disease implicated in myocardial infarction, ischemic stroke, and peripheral arterial disease [1]. Until recently, therapeutic atherosclerosis intervention focused primarily on pharmacologically limiting hypercholesterolemia or arterial hypertension. Nevertheless, the use of these highly effective lipophilic drugs or antioxidant vitamins has not ameliorated atherosclerosis. Atherogenesis is driven by a combination of genetic and environmental risk factors leading to persistent chronic inflammation in endothelial cells (ECs). Interestingly, atherosclerotic lesions preferentially develop at arterial bifurcations or curvatures, where migrating stagnation and flow separation create disturbed blood flow (D-flow). Conversely, the medial wall of bifurcation or relatively straight portion of arterial regions exposed to stable unidirectional flow (S-flow) is spared from plaque development [2,3,4]. Despite overarching experimental evidence, blood flow and its role in focal atherosclerotic plaque development remain elusive.
ECs in the intimal wall of arteries are exposed to hemodynamic forces including circumferential stress, induced by the cyclic strain of hydrodynamic pressure, and wall shear stress (WSS) through constant and rhythmic blood flow. ECs are equipped with a variety of mechano-sensory complexes on the apical surface, cell–cell junction, and cell–matrix adhesion sites to translate biomechanical cues [5,6,7,8]. Through these mechanisms of action, endothelial genes, regulated by blood flow, are known as mechano-sensitive or mechano-responsive genes [9,10,11,12,13,14,15,16]. Differential blood flows precisely control the level of mechano-sensitive genes and proteins to determine the focal nature of atherosclerosis. While S-flow regulates expression levels of atheroprotective genes such as Krüppel-like factor 2 and 4 (KLF2 and KLF4), tissue inhibitor of metalloproteinases-3 (TIMP3), endothelial nitric oxide synthase (eNOS), and Kallikrein-like 10 (KLK10) [17,18,19,20], D-flow has been widely recognized to upregulate proatherogenic genes such as vascular cell adhesion molecule-1 (VCAM-1), matrix metalloproteinases (MMPs), and bone morphogenic protein-4 (BMP4) [21,22,23]. In addition to mechano-sensitive genes, flow-responsive microRNAs (miRs) play pivotal roles in promoting atherosclerosis [10, 24]. In this review, we provide an overview of atherosclerosis progression, biomechanical forces in arteries exerted by blood flow, and mechano-sensitive genes and proteins involved in atherosclerosis to further our understanding of flow-sensitive mechanisms underlying atherosclerosis.
Progression of Atherosclerosis
Atherogenesis involves a complex multi-cellular inflammatory cascade [25,26,27,28]. In nascent atheroma, aberrant production and accumulation of low-density lipoprotein (LDL) in subendothelial layers and subsequent increase in the expression of leukocyte adhesion and chemoattractant molecules such as VCAM-1, soluble ICAM-1, monocyte chemoattractant protein-1 (MCP-1), P-selectin, and E-selectin. Adhered monocytes then transmigrate and differentiate into phagocytic macrophages in the intima [29,30,31]. Ingested LDL transforms intimal macrophages into “foam cells” that aggravate inflammatory responses by secreting a variety of proinflammatory cytokines, chemokines, and reactive oxygen species (ROS). This process, in parallel, recruits excessive monocytes and vascular smooth muscle cells, leading to fatty streaks and intimal thickening of subendothelial layers. The vascular wall remodels both outward and inwardly as the plaque expands, while endothelial inflammation and immune cell deposition persist along with increasing lipid accumulation, leading to the development of the lipid-rich necrotic core. Chronic inflammatory responses further produce matrix metalloproteinases (MMPs) and concurrently degrade the extracellular matrix (ECM) to promote the formation of fibrous cap. Subsequent rupture of the fibrous cap increases the accessibility of thrombogenic constituents and consequent thrombotic plaque formation [1, 32, 33]. Plaque progression and mechanisms underlying atherogenesis are summarized in Fig. 1.

Modified from Kumar et al., created with BioRender.com. Abbreviations: D-flow, disturbed flow; EC, endothelial cell; LDL, low-density lipoprotein; oxLDL, oxidized LDL; S-flow, stable flow; VSMC, vascular smooth muscle cell
Progression of atherosclerosis. Atherosclerosis initiates endothelial dysfunction, which activated ECs by various cardiovascular risk factors including hypertension, hyperlipidemia, diabetes, smoking, and disturbed flow which is found in the branching points of arteries. Activated ECs secrete adhesion molecules recruiting monocytes which are differentiated into macrophages. Fatty streak forms and oxidized LDL and macrophage form a foam cell which secretes proinflammatory markers. Persistent inflammation state leads to the development of fibrous cap and thinner fibrous cap ruptures which induces coagulation cascade and thrombosis.
Endothelial dysfunction reflects pro-inflammatory endothelial phenotype prone to atherogenesis [34, 35]. In inflamed, dysfunctional ECs, permeability rapidly increases and impairs barrier function. A plethora of studies elucidated that D-flow, prevalent in arterial branches and curvature, induces endothelial dysfunction. A recent study further documented that D-flow-mediated oxidative stress promotes endothelial dysfunction and impairs vascular homeostasis by leveraging reactive oxygen species (ROS) and atheroprotective nitric oxide (NO) bioavailability [2]. This pathophysiological state of ECs initiates monocyte recruitment [7, 9].
Atherogenesis roots from the accumulation of mesenchymal cells in the intimal layer of the artery [36]. The advent of lineage tracing analyses revealed an endothelial origin of neointimal mesenchymal cells that continue to express endothelial but acquire new mesenchymal, myofibroblast-like phenotypes [36, 37]. This transdifferentiation of ECs is indicative of endothelial-to-mesenchymal transition (EndMT). Analogous to epithelial-to-mesenchymal transition, EndMT is characterized by the acquisition of profibrotic phenotypes: loss of cell–cell contact, changes in cell morphology, disruption in cell polarity, loss of junctional proteins, increased cell proliferation, and motility into adjacent tissue with exaggerated extracellular matrix production [38,39,40]. During EndMT, EC markers such as CD31 and VE-cadherin reduce, whereas the mesenchymal markers such as alpha-smooth muscle actin (α-SMA), calponin, N-cadherin, and vimentin increase [41,42,43]. Robust clinical and experimental evidence supports that D-flow-mediated EndMT contributes to the initiation of atherosclerosis.
In addition to EndMT, a recent single-cell assay for transposase-accessible chromatin using sequencing (scATACseq) in a partial carotid ligation (PCL) model of mouse atherosclerosis has identified that chronic exposure to D-flow increases the number of ECs expressing markers of monocyte and macrophages [16]. This phenotypic change concomitantly increased proatherogenic genes such as Ctgf, Serpine1, Edn1, and Thsp1, whereas it reduced atheroprotective Klf2 & 4 gene expression [44]. This acquisition of ECs to immune cell-like phenotype was termed a novel endothelial cell-immune cell-like transition (EndICLT). These results overall suggested that D-flow concurrently reprograms ECs genomically and epigenetically during atherogenesis. Nevertheless, flow-sensitive mechanisms whereby D-flow-mediated EndICLT is implicated in pathobiological processes of atherosclerosis warrant further investigation.
Once resident in arterial walls, monocytes infiltrate into the intima and differentiate into intimal macrophages [32]. Chemoattractant molecules such as MCP-1 regulate this direct transmigration of monocytes at the site of lesions. Despite its protective role against oxidized LDL (oxLDL), intimal macrophages expressing scavenger receptor proteins perpetuate local inflammatory responses and ingest atherogenic lipoproteins. Consecutive monocyte accumulation, aberrant cholesterol metabolism, and consequent oxLDL ingestion transform intimal macrophages into “foam cells” [45]. Recent studies in genetically engineered mice revealed that scavenger receptor type A and CD36-dependent signaling pathways contribute to foam cell formation [46, 47]. Foam cells serve as a source of proinflammatory cytokines and ROS and consequent local inflammatory responses that aggravate atherosclerosis. Foam cells are further implicated in diverse pathways of programmed cell death including apoptosis, autophagy, necroptosis, and pyrotosis, contributing to the necrotic core of plaque. While foam cells are differentiated primarily from macrophages, ECs, activated vascular smooth muscle cells (VSMCs) with ectopic levels of scavenger receptor and cholesterol esterase, and hematopoietic stem and progenitor cells also emerged as additional sources of foam cells [48].
Foam cell–driven ECM proteins develop fibrous cap [49]. Interactions between macrophages and activated T cells expressing Th1 and Th2 cytokines contribute to chronic inflammatory responses [50, 51]. Immune responses play pleiotropic roles in regulating the progression of the lesion. Th1 secreted cytokine Interferon-γ (IFN-γ) decreases the expression of scavenger receptors, collagen synthesis, and SMC proliferation for an antiatherogenic effect. Conversely, IFN-γ upregulates macrophage production inducing the secretion of proinflammatory cytokines and MHC class 2 molecule which promotes atherogenesis [52]. Th2-expressed cytokines, IL-4, IL-10, and IL-13, further exert both proatherogenic and antiatherogenic effects. IL-4 downregulates the activation of INF-γ which represents the antiatherogenic effect, while inducing the LDL oxidation to increase the proatherogenic effect [53]. Furthermore, T-cells suppress the migration and proliferation of SMCs in the fibrous cap and decrease ECM production; the fibrous cap becomes thinner and eventually ruptures near the shoulder of the fibrous cap with subsequent thrombosis.
Biomechanical Forces in Arteries
A growing body of evidence supports that D-flow is a primary determinant of chronic inflammation and focal development of atherosclerotic lesions [9, 16, 21]. The arterial wall consists of three layers: the intima, media, and adventitia which possess unique and distinct roles to maintain homeostatic responses. The intima, the luminal arteriolar wall, is comprised of vascular endothelial and a mixture of connective tissues to form a protective barrier between the blood and the rest of the vessel wall. The medial wall, comprised of involuntary muscle and collagenous elastic fiber, provides mechanical support upon blood pressure-induced hydrodynamic pressure or circumferential stretch. Compared to the rest of the vessel wall, the adventitia is a relatively unorganized layer of the vessel wall comprised of primary fibroblasts and connective membranes to control the medial layer from overexpansion, while harboring vasa vasorum or regulate inflammatory cell trafficking (Fig. 2A) [54]. Vascular endothelium in the intimal wall is subjected to constant and rhythmic blood flow that exerts biomechanical forces: hemodynamic transmural pressure, circumferential strain induced by the pressure pulse, and WSS [55, 56]. While circumferential strain or transmural pressure is essential to protect endothelial function, WSS exerts a substantial impact in directing developmental and pathophysiological responses during atherogenesis (Fig. 2B) [57,58,59].
Hemodynamic forces in human arteries. A Anatomy of human aorta. The arterial wall consists of three layers; the intima, media, and adventitia. The intimal layer is comprised of endothelial cells and a mixture of connective tissue. The medial layer is primarily composed of involuntary smooth muscle cells and elastic collagenous fiber, while adventitia is consisting of fibroblast. B Hemodynamic forces. Within the arterial system. blood flow induces biomechanical forces including circumferential strain, wall shear stress, and transmural blood pressure. Figures are created with BioRender.com. Abbreviation: WSS, wall shear stress
WSS is defined as a frictional force by virtue of the viscosity and flow rate that acts tangentially on the endoluminal surface (Eq. 1) [60]:
where r is the radius of the vessel lumen, μ is the blood viscosity, and Q is the flow rate. In Poiseuille flow, the cross-section within the artery varies little, the resistance of the vessel or the pressure drop is negligible, and steady laminar flow with parabolic axial velocity develops in the relatively straight segment of the arterial wall. However, arteries are not uniformly straight, geometries may not radially conform, magnitude and direction of the physiologic blood flow and consequent WSS alter, and even a subtle perturbation can facilitate a significant impact on the endothelial microenvironment. ECs in the human arterial system are exposed to diverse flow patterns. Rheological properties of blood flow are evaluated by the Reynolds number (Re). Re is the ratio of the inertial momentum to viscous force within the blood.
where μ and ρ are the viscosity and density of blood respectively, D is the diameter of the vessel lumen, and Q is the flow rate (Eq. 2) [61, 62]. In modern fluid mechanics, Re is a measure of the stability of the blood flow.
At a low flow rate or flow in a smaller lumen (D < < 10 µm, low Re), viscous force or surface tension dominates over fluid inertia developing stokes flow. In this condition, transient nonaxial flow develops when viscous and inertial forces are comparable, but the streamline of blood flow relies on the geometry of the artery. In arterial circulation, the inertial force predominates over the viscous force, leading to a steady unidirectional laminar flow (Re < 2000). Continuous exposure to the laminar flow shifts EC to an atheroprotective phenotype: anti-inflammatory, anti-thrombotic, anti-coagulative, and anti-hypertrophic (Fig. 3A) [63]. Conversely, flow is disturbed and becomes turbulent when Re exceeds this value, and the lateral motion of blood flow becomes fully randomized. This condition transiently occurs at peak systole but is rarely achieved in healthy arteries with uniform surface geometry. Thus, D-flow tends to arise on the aberrant, irregular surface of lumen stenosis, aneurysms, or even in the arterial curvature [64,65,66]. D-flow is recognized as proatherogenic and systematically determines the eccentric nature of inflammatory responses, endothelial dysfunction, stress-related genes, and hampered extracellular matrix contributing to the pathogenesis of atherosclerosis (Fig. 3B) [67,68,69,70].

Modified from Cheng et al., 2017, created with BioRender.com Abbreviations: D-flow, disturbed flow; EC, endothelial cell; ECM, extracellular matrix; MWSS, mean wall shear stress
Wall shear stress in the human arterial system. A Disturbed, turbulent flow characterized by chronic inflammation and thrombosis develops in the lateral wall of bifurcated area and luminal stenosis. D-flow is proatherogenic. Chronic exposure to D-flow activates proatherogenic phenotypes in EC by increasing inflammatory gene expressions, ECM production, release of inflammatory cytokine and consequential leukocyte and monocyte adhesion, endothelial permeability, and cell proliferation and migration. B Laminar flow develops in the straight segment of the thoracic aorta. Continuous exposure to laminar flow reportedly increases anti-inflammatory, anti-thrombotic, and anti-coagulative phenotype. Created with BioRender.com. C MWSS values in the human arterial system.
WSS in the human arterial system diverges by anatomic location [71]. Descending aorta and common carotid arteries are exposed to high WSS, whereas vessels distal to the aortic root such as the brachial artery, common and superficial femoral arteries, infra-, suprarenal-, and supraceliac aorta are subjected to relatively lower WSS [72, 73]. Table 1 and Fig. 3C summarize anatomical differences in magnitudes of mean WSS (MWSS). In healthy individuals, WSS ranges between 1 and 20 dynes·cm−2 and instantaneously increases to nearly 40 dynes·cm−2 due to peak systolic pressure [71, 73]. Despite differences in value, the MWSS (time-averaged over cardiac cycles in large conduit arteries) throughout the human arterial system is presumed to be constant 15 dynes·cm−2 [74,75,76]. This deduction has been valued by various experimental models and was also recapitulated mathematically by Murray’s law of minimum work with the condition of uniform fluid viscosity [77].
Furthermore, WSS levels vary across species [78, 79]. In anesthetized laboratory animals, MWSS tends to be higher in smaller species. MWSS in dog arterial system ranges from 5.1 to 46.0 dynes·cm−2, whereas fluctuates from 12.2 to 156.8 dynes·cm−2 in rabbits with an average value of 23.3 dynes·cm−2, from 18.8 to 84 dynes·cm−2 and 28.0 to 142 dynes·cm−2 in rats and mice with the average value of 46.6 and 64.8 dynes·cm−2 respectively [80,81,82,83,84]. Although the degree of MWSS diverges due to various uses of anesthetics and differences in measurement methods, this heterogeneity in WSS can be explained by differences in luminal size, as WSS is inversely correlated with luminal diameter (Fig. 4).
Wall shear stress in the human arterial system. Species-dependent MWSS. Compared to human, MWSS in the arterial system tend to be higher in smaller species of laboratory animals, where the size of the vessel lumen is small. Figures are created with BioRender.com Abbreviations: MWSS, mean wall shear stress
Flow-Sensitive Endothelial Genes in Atherosclerosis
The aforementioned biomechanical forces including S-flow and D-flow are detected by numerous mechanosensors on ECs such as integrin, NOTCH1, platelet endothelial cell adhesion molecule-1 (PECAM-1 or CD31), vascular endothelial-cadherin (VE-cadherin), vascular endothelial growth factor receptor 2 (VEGFR2), and Piezo1 [44, 85]. Mechanosensors translate biomechanical forces to alter cell signaling pathways and functional changes in ECs by various flow-sensitive gene expressions. Flow-sensitive genes either upregulated in S-flow or downregulated in D-flow are shown to be anti-atherosclerosis genes, whereas the genes either upregulated in D-flow or downregulated in S-flow are shown to be pro-atherogenic genes.
Endothelial Nitric Oxide Synthase (eNOS)
Since its discovery in the 1980s, a series of overarching studies elucidated that eNOS activation transduces a broad range of biophysical cues and regulates the production of endothelium-derived NO that maintains vascular tone and atheroprotective phenotype [15, 86]. eNOS is comprised of two monomers containing the amino-terminal oxidase and carboxy-terminal reductase domains [87, 88]. In response to S-flow, eNOS is regulated chronically by inducing expression levels and acutely by modulating enzymatic activity to produce NO [89]. While chronic exposure to S-flow has been shown to promote eNOS expression by transcriptional induction and stabilization of mRNA, cooperation between the domains creates an electron flux to oxidize L-arginine and produce NO in a Ca2+/CAM-dependent manner [90]. Phosphorylation of eNOS is reportedly accepted as a central mechanism of controlling eNOS activation: bovine S116, T497, S617, S635, and S1179 (human S1177) [91]. Ectopic level of NO is one of the earliest biomarkers of atherogenesis, and a plethora of studies have shown parallel roles of NO in attenuating inflammation, apoptotic cell death, and monocyte adhesion. For instance, NO reportedly serve as an antioxidant scavenging reactive oxygen species associated with a wide range of inflammatory cell signaling such as the NFkB pathway that consequently transcribes VCAM1 [92, 93]. NO has been shown to regulate key enzymes to trigger S-nitrosylation and caspase-dependent apoptosis (caspase-3, caspase-6, caspase-7, and caspase-8) [94,95,96,97]. Additionally, NO implicates recruiting TNF receptor–associated death domain protein (TRADD) by modulating the level of antiapoptotic heat shock protein-70 (HSP-70), Bcl-2 proteolysis, and ceramide production [97, 98]. Putative mechanisms against apoptosis include the NO-mediated PI3/Akt pathway by which S-flow mediates its activity. A growing body of evidence supports an atheroprotective effect of Akt/eNOS, which in turn reduces the amount of monocyte adhesion.
Krüppel-Like Factors 2 and 4 (KLF2/4)
KLF2 serves as a major regulator of bio-mechanical and bio-chemical cues [99, 100]. Early studies revealed that KLF2 plays parallel roles in antiatherogenic potential [101,102,103]. As a regulator of vascular inflammation, KLF2 is intimately associated with the NFkB pathway [104]. While KLF2 inhibits NFkB/p300 cooperation and subsequent activation of Vcam1 promoter, KLF2 prevents thrombin-mediated NFkB activation and compensates for the effect of proinflammatory cytokines and matrix-degrading enzymes [101, 104]. Ectopic overexpression of KLF2 downregulates inflammatory and prothrombotic factors through inhibition of its principal receptor protease-activated receptor 1 (Par1). As a corollary, the knockdown of KLF2 upregulates the NFkB pathway and exacerbates systemic atherosclerosis and coagulopathy [105, 106]. In addition, studies have unraveled that KLF2 transcriptionally prohibits endothelial inflammation and thrombosis by attenuating JUN N-terminal kinase (JNK) activation and activating transcription factor 2 (ATF2) nuclear localization, Vcam1 and Cd62 (also known as E-selectin) expressions, and activation of monocytes [103, 107]. KLF2/p300 cooperation further facilitates endothelial nitric oxide synthase (eNOS) binding and promotes vascular protection [101]. Independent DNA microarray and transcriptomic studies revealed biomechanical shear forces exert profound effects on regulating klf2. In human arteries, KLF2 is highly expressed in atheroprotective regions of the thoracic aorta, whereas the expression is low in the arterial bend or bifurcated carotid or iliac artery where the magnitude of shear is low [106, 108]. Flow regulation on KLF2 is under scrutiny. Studies suggested activations of MAPK kinase cascade (MEKK2,3/MEK5/ERK5/MEF2) and histone acetyltransferases CBP and p300, regulation of rho family GTPase, and inhibition of histone deacetylase HDAC4 and HDAC5 or flow-sensitive microRNAs (miR-92a, miR-32-5p) participate flow-dependent regulatory mechanisms of KLF2 [109,110,111]. EC are highly glycolytic and aberrant EC metabolism implicates atherosclerosis [112, 113]. Laminar WSS-mediated KLF2 reportedly reduce expression levels of glycolysis-related enzymes including 6-phosphofructo-2-kinase/fructose-2,6-biphosphatase-3 (PFKFB3) and phosphofructokinase-1. PFKFB3-increased glycolysis, as a corollary, partially reversed KLF2-mediated reduction of glycolysis [114]. Consistent with this manner, recent studies in mice revealed partial inhibition of PFKFB3 via pharmacokinetic molecules to suppress intraplaque angiogenesis and reduce plaque stabilization [115]. KLF4 is substantially expressed in ECs and maintains an anti-inflammatory, quiescent endothelial state in response to laminar flow or atherogenic stimuli [109, 110]. KLF4 shares a myriad of transcriptional targets and physiological similarities with klf2. Analogous to KLF2, KLF4 also modulates the level of eNOS and thrombomodulin for vascular protection and anti-thrombotic effects [106]. A host of studies in mice has further demonstrated the anti-inflammatory potentials of KLF4. Under D-flow, DNA methyltransferase 3A represses KLF4 expression by hypermethylation of the promoter region which in turn reduces MEF2 binding for upregulation [116, 117].
Bone Morphogenetic Protein 4 (BMP4)
Bone morphogenic proteins (BMP) are members of the TGF β family. Among 33 members of the TGF β family, BMP4 was identified as a potent inducer of bone formation when subcutaneously implanted in rats. While diverse roles of BMP4 in embryo- and developmental angiogenesis have been known for years, flow-sensitive BMP4 emerged as a critical regulator of endothelial inflammation during atherogenesis. While S-flow diminishes, exposure to D-flow has been shown to increase BMP4 expression in a time- and force-dependent manner, consequently inducing NFkB-dependent ICAM1 expression and subsequent monocyte adhesion [23]. Ectopic BMP4 overexpression in vitro further has been shown to increase ICAM1 expression but not VCAM1 or E-selectin [118]. In human coronary arteries, the endothelial lining over mild foam cells exhibited an evident increase in BMP4 expression compared to the minimally disease region of the artery. Beyond its crucial roles in promoting inflammation, D-flow-mediated BMP4, and its role in vascular oxidative stress and subsequent ROS production has been recently elucidated [64]. BMP4 has been shown to concurrently upregulate NADPH expression and activity via p47phox and Nox1 in an autocrine-like manner, while BMP4-dependent NADPH oxidase activation elevated the level of ROS production, NFkB activation, ICAM1 expression, and consequent monocyte adhesion.
Kallikrein-Related Peptidase 10 (KLK10)
Kallikrein-related peptidase (KLKs) is a subgroup of secreted serine protease implicated in the pathophysiology of cancers and a wide variety of cardiometabolic diseases [119]. Networks of their interaction control global immune responses and contribute to cell plasticity through the regulation of proliferation, migration, apoptosis, and invasion. Each KLK reveals a unique expression pattern and cellular function. KLK10, a putative member of 15 secreted KLKs, was originally identified as epithelial-specific (NES1) [120]. However, recent independent genome-wide microarray, scRNA seq, and scATAC seq studies carried out in the mouse PCL model uncovered endothelial KLK10 expression by which blood flow both genetically and epigenetically regulates during atherogenesis [14]. In the RCA, where 2 weeks of PCL surgery induce S-flow, endothelial KLK10 expression, and chromatin accessibility increase substantially, whereas decreases in athero-susceptible regions of the LCA. Atheroprotective roles of KLK10 have been recently examined by Williams et al. [59] This study revealed that 24 h of S-flow exposure increased endothelial KLK10 expression compared to D-flow-treated and static controls. While exposure to recombinant KLK10 (rKLK10) attenuated TNF-α-mediated inflammation and monocyte adhesion, p65 phosphorylation, subsequent nuclear translocation and activation of NFkB signaling, and thrombin-impaired endothelial permeability. As a corollary, silencing KLK10 expression via siRNA increased inflammation under the S-flow condition. These observations were corroborated in the mouse PCL model. In ApoE(−/−) mice, consecutive intravenous rKLK10 injection or ultrasound-driven KLK10 overexpression concurrently attenuated macrophage infiltration and the amount of plaque burden following 2 weeks of the PCL surgery. Intriguingly, rKLK10 had no effects on blood cholesterol as assessed by total, HDL, LDL, and triglyceride. This observation was in human coronary arteries, where luminal KLK10 expression was dramatically reduced in the athero-susceptible region of the artery. Taken together, these observations supported the notion that differential blood flows impart mechanical effects to regulate endothelial KLK10 expression during atherogenesis. Serine protease HTRA1 involves a KLK10-dependent mechanism. Whether S-flow regulates cooperation between KLK10 and HTRA1 for atheroprotection warrants further investigation.
Hypoxia Inducible Factor 1-alpha (HIF-1α)
Hypoxia-inducible factor 1-alpha (HIF-1α) is a central regulator of cellular responses to hypoxia and disturbed flow [121,122,123,124,125,126]. HIF-1α is generally regulated by physiological oxygen level, but the D-flow can regulate the HIF-1α in vascular ECs, leading to atherosclerosis or aortic valve calcification [69, 126, 127]. Activation of HIF-1α triggers transcription of many genes, which leads to the induction of various pathways including angiogenesis, metabolism, erythropoiesis, inflammation, and EndMT. In particular, endothelial HIF-1α knockout in the ApoE knockout mouse model study represented that endothelial HIF-1α promoted endothelial inflammation [128]. A partially carotid ligation mouse model study represented that the endothelial HIF-1α knockout group showed decreased Cxcl1, Ccl2, and Tnfa gene expression. Endothelial HIF-1α knockout animals showed reduced lesion area as well as macrophage recruitment inhibition. Also, endothelial HIF-1α regulates monocyte adhesion by regulating CXCL1-dependent pathways and HIF-1α increases endothelial inflammation by upregulation of miR-19a.
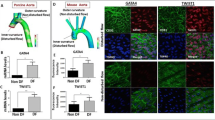
Fernandez and colleagues demonstrated that the HIF-1α activity is regulated by Ube2c, which is degraded by miR-483, and miR-483 mimic significantly reduces aortic valve calcification [126]. miR-483 is a flow-sensitive miRNA, which is downregulated to D-flow condition compared to S-flow and static condition. miR-483 mimic transfection study to human aortic valve endothelial cells (HAVECs) with D-flow condition represented that the EndMT markers (TWIST1, TRANSGELIN, SNAIL, and SLUG) and proinflammatory markers (IL6, ICAM1, and VCAM1) were significantly decreased. In addition, miR-483 regulated ASH2L and UBE2C expression under flow conditions, and UBE2C expression was increased under D-flow in HAVECs. UBE2C knockdown downregulated proinflammatory markers as well as EndMT markers but not miR-483 level, which means that UBE2C is not an upstream regulator of miR-483. In addition, UBE2C silencing upregulated pVHL expression which has a role in HIF-1α degradation. Interestingly, siUBE2C transfection to HAVECs result showed that knockdown of UBE2C decreased ubiquitinated pVHL levels. Porcine aortic valve (AV) leaflet ex vivo study revealed that both miR-483 mimic and PX-478, chemical HIF-1α inhibitor, decreased calcification as well as HIF-1α protein expression. In conclusion, flow-sensitive miR-483 regulates UBE2C gene expression which ubiquitinates pVHL. Ubiquitinated pVHL was degraded by proteasomal degradation, which leads to HIF-1α expression inducing overexpression of HIF-1α target genes including inflammation and EndMT. These results show the possibility that the HIF-1α inhibitor could be a therapeutic target for atherosclerosis.
The expression of HIF-1α is notably elevated in calcified human aortic valves (AVs) [129]. Moreover, the HIF-1α inhibitor PX-478 has been demonstrated to effectively impede AV calcification in both static and disturbed flow conditions. Given that increased mechanical strain is a prominent trigger for AV calcification, Salim and his colleagues conducted an investigation into the impact of PX-478 on AV calcification and collagen turnover under pathophysiological cyclic stretch conditions (15%). Porcine aortic valve (PAV) leaflets were subjected to cyclic stretching at 15% amplitude and 1 Hz frequency for a duration of 24 days within an osteogenic medium, both with and without PX-478. Additionally, PAV leaflets were subjected to cyclic stretching at both physiological (10%) and 15% strain for a duration of 3 days in a regular medium to assess its influence on HIF-1α mRNA expression. The PX-478 (100 µM) treatment could significantly inhibit PAV calcification under 15% stretch conditions. In contrast, a moderate concentration of PX-478 (50 µM) exhibited a more modest inhibitory effect on PAV calcification. Notably, 50 µM PX-478 also had a significant impact on reducing PAV collagen turnover under 15% cyclic stretch conditions. This research indicated that cyclic stretch (15% vs. 10%) did not yield any significant effect on HIF-1α mRNA expression within PAV leaflets. These outcomes suggest that the HIF-1α inhibitor PX-478 may exert its anti-calcific and anti-matrix remodeling effects in a manner that is independent of the degree of mechanical stretch applied.
SOX13
The aforementioned blood flow regulates endothelial inflammation and atherosclerosis by partially governing the expression of endothelial genes through flow-sensitive transcription factors (FSTFs). Through scRNAseq and scATACseq analyses in the PCL mouse model, 30 FSTFs have been identified, which included the anticipated KLF2/4 and novel FSTFs. These findings were further corroborated in mouse arteries in vivo and cultured human aortic ECs (HAECs). Among the FSTFs identified, eight proved to be conserved in both mice and humans, both in vivo and in vitro: SOX4, SOX13, SIX2, ZBTB46, CEBPβ, NFIL3, KLF2, and KLF4. SOX13 represented robust flow-sensitive regulation, endothelial preferential expression, and an as-yet-unknown flow-dependent function [130].
Subsequent experiments revealed that the knockdown of SOX13 using siRNA amplified endothelial inflammatory responses, even under unidirectional laminar shear stress (ULS) conditions, mimicking S-flow. RNAseq analysis unveiled 94 downregulated and 40 upregulated genes influenced by shear and SOX13. Notably, several cytokines, such as CXCL10 and CCL5, were among the most prominently upregulated genes in HAECs treated with SOX13 siRNA.
Moreover, when HAECs were treated with Met-CCL5, a specific CCL5 receptor antagonist, it prevented the endothelial inflammatory responses induced by siSOX13. Conversely, SOX13 overexpression was found to mitigate endothelial inflammation responses. In summary, SOX13 emerges as a novel, evolutionarily conserved FSTF that represses the expression of pro-inflammatory chemokines in ECs under s-flow conditions. Reduction of endothelial SOX13 triggers chemokine expression and inflammatory responses, representing a significant proatherogenic pathway.
Endothelial-to-Immune Cell-like-Transition (EndICLT)
Alongside systemic activation in pro-inflammatory pathways, D-flow reportedly increases EC plasticity and reprograms endothelial subpopulation to pro-atherogenic phenotype. Recent scRNA seq and scATAC seq carried out by Andueza et al. interrogated the effects of D-flow in endothelial phenotype and plasticity on a genomic and epigenomic basis [16]. This study uncovered that ECs are highly heterogeneous and plastic under D-flow conditions. Exposure to chronic D-flow increased SMC numbers by 2.3% and 18.2% in the LCA while elevating MΦ adhesion by 10.3 and 28.4% respectively along with changes in macrophage phenotypes. The level of proatherogenic genes such as ctgf, serpine1, and edn1 in the LCA endothelium further increased in a time-dependent manner, while immune cell marker genes in EC (C1qa, C1qb, C5ar1) concurrently increased under chronic D-flow condition. The combined approach of scRNA seq and scATAC seq further unraveled that D-flow alters chromatin accessibility of EndMT- (Tagln, Acta2, Cnn1, Snai1) and EndICLT-related genes (C1qa, C1qb, C5ar1, Tnf). This observation was recapitulated in HAEC by using a custom-built cone-and-plate viscometer. While 24 h of exposure to bidirectional oscillatory shear stress, mimicking D-flow, induced a concurrent increase in C1qa and C5ar1 transcriptional and EndMT-related genes. Conversely, in the RCA, where S-flow promotes atheroprotective phenotype, EC populations remained largely unchanged with dramatically low levels of SMC, MΦ, and T-cell populations, while EC clusters upregulated Krüppel-like Factor 2 and Krüppel-like factor 4 expression. Nevertheless, the pathobiological significance of End-ICLT promoting atherosclerosis remains incompletely understood. Whether End-ICLT is implicated in inflammation, clonal proliferation, apoptosis, EndMT, and endothelial progenitor cell (EPC) recruitment during atherogenesis warrants further investigation.
Flow-Sensitive miRNAs in Atherosclerosis
miRNAs are small single-stranded noncoding RNAs that regulate post-transcriptional gene expression. The base-pairing of miR with the 3'UTR of target mRNA leads to translational suppression and degradation of target mRNA. Flow-sensitive miRNAs play major roles in vascular dysfunction and atherosclerosis. miRNAs such as miR-23b and miR-101 are upregulated in S-flow or downregulated in D-flow, whereas miRNAs such as miR-19a, miR-92a, miR-487a, and miR-712/205 are upregulated in D-flow or downregulated S-flow.
miR-23b
Twenty-four-hour pulsatile shear (PS) to human umbilical vein endothelial cells (HUVECs) reduced cell proliferation and significantly increased cell number in the G1/G0 phase, while the cell number in the S phase was significantly decreased compared to static condition [131]. miRNA functional analysis revealed that miR-23b and miR-27b were correlated with the PS-applied EC growth arrest. In addition, antagomir-23b to inhibit miR-23b expression treatment to HUVECs reversed the PS-induced cell cycle arrest in the PS condition. Additionally, miR-23b was shown as a novel regulator of VSMC phenotype switching [132]. Animal studies revealed that miR-23b expression was inhibited after vascular injury, whereas gain-of-function studies showed that overexpression of miR-23b inhibited VSMC proliferation and migration. In addition, miR-23b significantly induced the VSMC marker genes including smooth muscle α-actin (ACTA2) and smooth muscle myosin heavy chain (MYH11). Luciferase reporter assay results showed that forkhead box O4 (FoxO4) is a direct target of miR-23b in VSMCs. These researches demonstrated that flow-sensitive miR-23b can contribute to maintaining cellular quiescence and cell cycle in a flow-dependent manner.
miR-101
miR-101 showed significantly increased expression in response to laminar shear stress (LSS) which is involved in the flow-regulated gene expression in HUVECs [133]. Bioinformatic analysis of the molecular targets of miR-101 showed that 3′UTR of the human mTOR gene is a potential target gene of miR-101. Luciferase activity assay using a reporter of mTOR-3′UTR containing miR-101 binding site represented that miR-101-transfected group showed decreased luciferase activity, indicating miR-101 repressed mTOR gene. mTOR protein level under the LSS condition was decreased in comparison with the static condition, whereas the miR-101 inhibitor–treated group under the LSS condition showed that the mTOR protein level was not changed compared with the static condition. Furthermore, miR-101 directly targets ATP-binding cassette transporter A1 (ABCA1) indicating that miR-101 promotes intracellular cholesterol retention by suppressing ABCA1 expression [134]. These studies suggested that miR-101 may regulate cellular functions via mTOR and ABCA1 pathways, which contribute to the anti-inflammation process and cholesterol efflux.
miR-19a
As mentioned previously, endothelial HIF-1α promoted atherosclerosis by upregulating miR-19a [128]. In addition, miR-19a expression was increased by LSS in HUVECs [135]. miR-19a-transfected ECs expressing eightfold higher miR-19a levels showed cyclin D1 downregulation which is the target mRNA of miR-19a. Overexpression miR-19a represented that the cell number of the G0/G1 phase is much higher than that of the S phase indicating that miR-19a overexpression inhibited the proliferation of ECs to suppress cyclin D1. In addition, atherosclerosis patients have lower levels of anti-inflammatory cytokine interleukin-10 (IL-10) and higher levels of miR-19a in peripheral B cells than those of healthy control groups [136]. Proinflammatory markers such as IL-4, IFN-γ, and TNF-α treatment increased miR-19a levels in B cells, whereas IL-10 mRNA was reduced after the proinflammatory markers treatment. Another target molecule of miR-19a is HMG box-transcription protein 1 (HBP1) [137]. HBP1 plays a role in inhibiting the expression of the macrophage migration inhibitory factor (MIF). TNF-α mediated miR-19a expression upregulates MIF by targeting HBP1, inducing the release of proinflammatory markers TNF-α and IL-6. Together, these results suggest that knockdown miR-19a can be a potent target for the antiatherogenic effect.
miR-92a
miR-92a is a regulator for both KLF4 and KLF2. miR-92 knockdown cell increased KLF4 expression, and miR-92a knock-in decreased KLF4 and KLF2 protein expression in human arterial ECs [138]. After TNF-α treatment to ECs, TNF-α induced inflammatory markers such as MCP-1, VCAM-1, and E-selectin (E-SEL) were increased; however, the miR-92a inhibitor–treated group showed decreased MCP-1, VCAM-1, and E-SEL, which regressed these proinflammatory marker expressions. In addition, endothelial nitric oxide synthase (eNOS) was downregulated in the TNF-α-treated group, while the miR-92a-treated group significantly increased eNOS expression compared to the TNF-α-treated group. Furthermore, miR-92a overexpression significantly decreased integrin subunits α5 (ITGA5) protein expression in HUVECs which has a pivotal role in vascular development and angiogenesis [139]. Luciferase activity results revealed that ITGA5 mRNA is a direct target of miR-92a. In addition, antagomir-92a treatment increased blood flow and therapeutic effect in a hind-limb ischemia mouse model. Together, these results suggested that inhibition of miR-92a can be a potent strategy for atherosclerosis.
miR-487a
miR-487a overexpression was observed in oscillatory shear (OS)-induced human aortic endothelial cells (HAECs). Also, miR-487a was overexpressed in the inner curvature of the aortic arch but not in the outer curvature of the aortic arch and the thoracic aorta in a rat model [140]. Oscillatory shear significantly increased the phosphorylation of Smad5 in the nucleus of ECs compared with the static condition and pulsatile shear (PS) condition, and Smad5 activation promoted miR-487a processing in ECs. Bioinformatics database indicated that human CBP and p53 can be a potential target of miR-487a. Additionally, luciferase activity results confirmed that CBP-3′UTR and p53-3′UTR have a binding site of miR-487a. In addition, overexpression of pre-miR-487a decreased CBP and p53 protein expression in ECs under static conditions. In contrast, anti-miR-487a transfection increased CBP and p53 protein expression in ECs. These results supported that both CBP and p53 are the direct target of miR-487a, and OS inhibited CBP and p53 protein expression via upregulation of miR-487a. By using the rat stenosis model, the abdominal aorta was constricted using a U-clip, and the oscillatory flow was generated in the downstream region. In vivo results suggested that miR-487a was overexpressed in the downstream region which was applied to the OS condition and modulated EC proliferation through the inhibition of Rb phosphorylation and cyclin A expression.
miR-712/205
miR-712 are overexpressed under D-flow after 48 h post-ligation surgery using a mouse PCL model [20]. miR-712 and miR-205 were investigated as proatherogenic miRNAs induced by D-flow [21]. Luciferase activity results revealed that TIMP3 is a direct target of miR-712, and TIMP3 expression under the OS condition was significantly decreased in comparison with the laminar shear (LS) condition. Pre-miR-712 transfection under LS condition expressed decreased TIMP3 protein expression, and anti-miR-712 transfection under OS condition expressed increased TIMP3 protein expression. In addition, the pre-miR-712-treated group under static and LS conditions increased TNF-α expression as well as increased permeability. Anti-miR-712 reduced atherosclerosis development in partial carotid ligation ApoE knockout mouse model, and recombinant adenoviral TIMP3 (AdTIMP3) significantly increased TIMP3 expression and consequently reduced atherosclerosis plaque. Since miR-712 is murine-specific and miR-205 is its homolog in humans from a seed-sequence matching study, pre-miR-205 was treated to HAECs indicating that decreased TIMP3 level was observed in both immortalized mouse aortic endothelial cells (iMAECs) and HAECs. This study suggested that targeting miR-712 and miR-205 may provide a potential treatment strategy for atherosclerosis.
Summary and Future Perspective
Here, we summarized the progression of atherosclerosis, biomechanical forces in arteries, and current knowledge of flow-sensitive genes in atherosclerosis. These studies showed that flow-sensitive genes play an important regulatory role in EC function and pro- or anti-atherogenesis. However, our knowledge of the flow-sensitive genes involved in atherosclerosis is still in its infancy, and further research on these flow-sensitive genes and anti-atherosclerosis is needed. Additionally, the development of new technologies and experimental methods, such as single-cell sequencing, organoids, organ-on-a-chip, and machine learning algorithm, will make significant contributions to the discovery of novel flow-sensitive genes and the elucidation of the relationship between flow-sensitive genes and atherosclerosis [141].
Treatment of atherosclerosis with precise gene regulation and delivery will be the next chapter. Advances in genomics and personalized medicine could lead to treatments tailored to an individual’s genetic makeup, improving treatment effectiveness and minimizing side effects. Precise gene editing technologies like CRISPR-Cas9 hold the potential for modifying gene expression or repairing genetic factors that contribute to validating novel flow-sensitive genes and treating atherosclerosis. Additionally, these techniques can be achieved by precision nanomedicine which can deliver genes or therapeutics to specific sites within the cardiovascular system by using nanotechnology, offering targeted treatment with fewer side effects.
To achieve precision nanomedicine, the following challenges have to be overcome. First, it is necessary to discover more flow-sensitive genes or master regulators for anti-atherosclerosis treatment. Even though a number of flow-sensitive genes related to endothelial dysfunction, inflammation, phenotype transition, and atherosclerosis have been investigated, numerous flow-sensitive genes still have to be validated to understand atherogenesis and anti-atherosclerosis. Second, it is necessary to develop precise gene delivery systems with minimal side effects. Since miRNAs can have a large number of target genes that can bind to a particular sequence, they may be likely to exhibit side effects other than the desired effect. Therefore, precise delivery of flow-sensitive genes to the desired target site should be developed.
In summary, flow-sensitive genes play a pivotal role in the development of atherosclerosis. Regulation of the function of flow-sensitive genes could lead to the diagnosis of atherosclerosis as well as the identification of novel therapeutic targets for atherosclerosis.
Data Availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Abbreviations
- S-flow:
-
Stable flow
- D-flow:
-
Disturbed flow
- EC:
-
Endothelial cells
- LAM:
-
Leukocyte adhesion molecule
- VCAM1:
-
Vascular adhesion molecule 1
- MMP:
-
Metalloproteinases
- BMP4:
-
Bone morphogenic protein
- miR:
-
Micro RNAs
- EndMT:
-
Endothelial to mesenchymal transition
- EndICLT:
-
Endothelial to immune cell-like transition
- ECM:
-
Extracellular matrix
- NO:
-
Nitic oxide
- ROS:
-
Reactive oxygen species
- SMA:
-
Smooth muscle actin
- scATACseq:
-
Single cell assay for transposase-accessible chromatin using sequencing
- EndICLT:
-
Endothelial cell-immune cell-like transition
- LDL:
-
Low-density lipoprotein
- oxLDL:
-
Oxidized LDL
- LRP1:
-
Lipoprotein receptor-related protein 1
- LOX1:
-
Lectin-like oxLDL 1 receptor
- VSMC:
-
Vascular smooth muscle cells
- IFNγ:
-
Interferonγ
- WSS:
-
Wall shear stress
- MWSS:
-
Mean WSS
- Re:
-
Reynold’s number
- TNF:
-
Tumor necrosis factor
- KLF2:
-
Krüppel-like factor 2
- KLF4:
-
Krüppel-like factor 4
- Par1:
-
Protease-activated receptor 1
- Jnk:
-
JUN N-terminal kinase
- ATF2:
-
Activating transcription factor 2
- eNOS:
-
Endothelial nitric oxide synthase
- TGF β:
-
Transforming growth factor β
- FSP1:
-
Fibroblast-specific protein 1
- vWF:
-
Von willlebrand factor
- AV:
-
Aortic valve
- VEC:
-
Valvular EC
- CYR61:
-
Cysteine-rich angiogenic inducer 61
- CTGF:
-
Connective tissue growth factor
- ANKRD1:
-
Ankyrin repeat domain 1
- LATS:
-
Large tumor suppressor
- HIF-1α:
-
Hypoxia inducible factor 1-alpha
- pVHL:
-
Von Hippel-Lindau protein
- PS:
-
Pulsatile shear
- MYH11:
-
Myosin heavy chain
- ABCA1:
-
ATP-binding cassette transporter A1
- IL-10:
-
Interleukin-10
- HBP1:
-
HMG box-transcription protein 1
- MIF:
-
Migration inhibitory factor
- MCP-1:
-
Monocyte chemoattractant protein-1
- ITGA5:
-
Integrin subunits α5
- HAEC:
-
Human aortic endothelial cells
- OS:
-
Oscillatory shear
- LS:
-
Laminar shear
- iMAEC:
-
Immortalized mouse aortic endothelial cells
References
Geovanini GR, Libby P. Atherosclerosis and inflammation: overview and updates. Clin Sci (Lond). 2018;132:1243–52.
Chiu J-J, Chien S. Effects of disturbed flow on vascular endothelium: pathophysiological basis and clinical perspectives. Physiol Rev. 2011;91:327–87.
Heo K-S, Fujiwara K, Abe J-i. Disturbed-flow-mediated vascular reactive oxygen species induce endothelial dysfunction. Circ J. 2011;75:2722–30.
Davies PF, Polacek DC, Handen JS, et al. A spatial approach to transcriptional profiling: mechanotransduction and the focal origin of atherosclerosis. Trends Biotechnol. 1999;17:347–51.
Tzima E, Irani-Tehrani M, Kiosses WB, et al. A mechanosensory complex that mediates the endothelial cell response to fluid shear stress. Nature. 2005;437:426–31.
Davies PF. Hemodynamic shear stress and the endothelium in cardiovascular pathophysiology. Nat Clin Pract Cardiovasc Med. 2009;6:16–26.
Simmons RD, Kumar S, Jo H. The role of endothelial mechanosensitive genes in atherosclerosis and omics approaches. Arch Biochem Biophys. 2016;591:111–31.
Villa-Roel N, Ryu K, Jo H. Role of Biomechanical stress and mechanosensitive miRNAs in calcific aortic valve disease. In Cardiovascular Calcification and Bone Mineralization, Aikawa, E., Hutcheson, J.D., Eds. Springer International Publishing: Cham, 2020;117–35. https://doi.org/10.1007/978-3-030-46725-8_6pp.
Kumar S, Kim CW, Simmons RD, et al. Role of flow-sensitive microRNAs in endothelial dysfunction and atherosclerosis: mechanosensitive athero-miRs. Arterioscler Thromb Vasc Biol. 2014;34:2206–16.
Kumar S, Kim CW, Son DJ, et al. Flow-dependent regulation of genome-wide mRNA and microRNA expression in endothelial cells in vivo. Sci Data. 2014;1:140039.
Simmons RD, Kumar S, Thabet SR, et al. Omics-based approaches to understand mechanosensitive endothelial biology and atherosclerosis. WIREs Syst Biol Med. 2016;8:378–401.
Dunn J, Thabet S, Jo H. Flow-dependent epigenetic DNA methylation in endothelial gene expression and atherosclerosis. Arterioscler Thromb Vasc Biol. 2015;35:1562–9.
Dunn J, Qiu H, Kim S, et al. Flow-dependent epigenetic DNA methylation regulates endothelial gene expression and atherosclerosis. J Clin Invest. 2014;124:3187–99.
Ni C-W, Qiu H, Rezvan A, et al. Discovery of novel mechanosensitive genes in vivo using mouse carotid artery endothelium exposed to disturbed flow. Blood. 2010;116:e66–73.
Boo YC, Jo H. Flow-dependent regulation of endothelial nitric oxide synthase: role of protein kinases. Am J Physiol Cell Physiol. 2003;285:C499–508.
Andueza A, Kumar S, Kim J, et al. Endothelial reprogramming by disturbed flow revealed by single-cell RNA and chromatin accessibility study. Cell Rep. 2020;33:108491.
van Thienen JV, Fledderus JO, Dekker RJ, et al. Shear stress sustains atheroprotective endothelial KLF2 expression more potently than statins through mRNA stabilization. Cardiovasc Res. 2006;72:231–40.
Kinderlerer AR, Ali F, Johns M, et al. KLF2-dependent, shear stress-induced expression of CD59. J Biol Chem. 2008;283:14636–44.
Hamik A, Lin Z, Kumar A, et al. Kruppel-like factor 4 regulates endothelial inflammation. J Biol Chem. 2007;282:13769–79.
Son DJ, Kumar S, Takabe W, et al. The atypical mechanosensitive microRNA-712 derived from pre-ribosomal RNA induces endothelial inflammation and atherosclerosis. Nat Commun. 2013;4:3000.
Nam D, Ni C-W, Rezvan A, et al. Partial carotid ligation is a model of acutely induced disturbed flow, leading to rapid endothelial dysfunction and atherosclerosis. Am J Physiol Heart Circ Physiol. 2009;297:H1535–43.
Magid R, Murphy TJ, Galis ZS. Expression of matrix metalloproteinase-9 in endothelial cells is differentially regulated by shear stress: role of c-Myc *. J Biol Chem. 2003;278:32994–9.
Jo H, Song H, Mowbray A. Role of NADPH Oxidases in disturbed flow- and BMP4- Induced inflammation and atherosclerosis. Antioxid Redox Signal. 2006;8:1609–19.
Kumar S, Williams D, Sur S, et al. Role of flow-sensitive microRNAs and long noncoding RNAs in vascular dysfunction and atherosclerosis. Vasc Pharmacol. 2019;114:76–92.
Ross R. Atherosclerosis-an inflammatory disease. N Engl J Med. 1999;340:115–26.
Libby P. Vascular biology of atherosclerosis: overview and state of the art. Am J Cardiol. 2003;91:3–6.
Lusis AJ. Atherosclerosis. Nature. 2000;407:233–41.
Libby P. Inflammation in atherosclerosis. Arterioscler Thromb Vasc Biol. 2012;32:2045–51.
Cybulsky MI, Gimbrone MA. Endothelial expression of a mononuclear leukocyte adhesion molecule during atherogenesis. Science. 1991;251:788–91.
Dong ZM, Chapman SM, Brown AA, et al. The combined role of P- and E-selectins in atherosclerosis. J Clin Invest. 1998;102:145–52.
Collins RG, Velji R, Guevara NV, et al. P-selectin or intercellular adhesion molecule (Icam)-1 deficiency substantially protects against atherosclerosis in apolipoprotein E–deficient mice. J Exp Med. 2000;191:189–94.
Glass CK, Witztum JL. Atherosclerosis. the road ahead. Cell. 2001;104:503–16.
Ridker PM. Residual inflammatory risk: addressing the obverse side of the atherosclerosis prevention coin. Eur Heart J. 2016;37:1720–2.
Mudau M, Genis A, Lochner A, et al. Endothelial dysfunction: the early predictor of atherosclerosis. Cardiovasc J Afr. 2012;23:222–31.
Bonetti PO, Lerman LO, Lerman A. Endothelial dysfunction: a marker of atherosclerotic risk. Arterioscler Thromb Vasc Biol. 2003;23:168–75.
Souilhol C, Harmsen MC, Evans PC, et al. Endothelial–mesenchymal transition in atherosclerosis. Cardiovasc Res. 2018;114:565–77.
Chen P-Y, Qin L, Baeyens N, et al. Endothelial-to-mesenchymal transition drives atherosclerosis progression. J Clin Invest. 2015;125:4514–28.
Souilhol C, Serbanovic-Canic J, Fragiadaki M, et al. Endothelial responses to shear stress in atherosclerosis: a novel role for developmental genes. Nat Rev Cardiol. 2020;17:52–63.
van Meeteren LA, Ten Dijke P. Regulation of endothelial cell plasticity by TGF-β. Cell Tissue Res. 2012;347:177–86.
Piera-Velazquez S, Li Z, Jimenez SA. Role of endothelial-mesenchymal transition (EndoMT) in the pathogenesis of fibrotic disorders. Am J Pathol. 2011;179:1074–80.
Dejana E, Hirschi KK, Simons M. The molecular basis of endothelial cell plasticity. Nat Commun. 2017;8:14361.
Cho JG, Lee A, Chang W, et al. Endothelial to mesenchymal transition represents a key link in the interaction between inflammation and endothelial dysfunction. Front Immunol. 2018;9:294.
Stenmark KR, Frid M, Perros F. Endothelial-to-mesenchymal transition. Circulation. 2016;133:1734–7.
Demos C, Williams D, Jo H. Disturbed Flow induces atherosclerosis by annexin A2-mediated integrin activation. Circ Res. 2020;127:1091–3.
Hahn BH, Grossman J, Chen W, McMahon M. The pathogenesis of atherosclerosis in autoimmune rheumatic diseases: roles of inflammation and dyslipidemia. J Autoimmun. 2007;28:69–75.
Silverstein RL. Febbraio M 2009 CD36, a scavenger receptor involved in immunity, metabolism, angiogenesis, and behavior. Sci Signal. 2009;2:re3.
Zani IA, Stephen SL, Mughal NA, et al. Scavenger receptor structure and function in health and disease. Cells. 2015;4:178–201.
Basatemur GL, Jørgensen HF, Clarke MCH, et al. Vascular smooth muscle cells in atherosclerosis. Nat Rev Cardiol. 2019;16:727–44.
Steinberg D, Witztum JL. Oxidized low-density lipoprotein and atherosclerosis. Arterioscler Thromb Vasc Biol. 2010;30:2311–6.
Hansson GK. Cell-mediated immunity in atherosclerosis. Curr Opin Lipidol. 1997;8:301–11.
Gotsman I, Gupta R, Lichtman AH. The influence of the regulatory t lymphocytes on atherosclerosis. Arterioscler Thromb Vasc Biol. 2007;27:2493–5.
Gupta S, Pablo AM, Jiang X-c, et al. IFN-gamma potentiates atherosclerosis in ApoE knock-out mice. J Clin Invest. 1997;99:2752–61.
Lee YW, Kim PH, Lee WH, et al. Interleukin-4, oxidative stress, vascular inflammation and atherosclerosis. Biomol Ther. 2010;18:135–44.
Majesky MW, Dong XR, Hoglund V, et al. The adventitia: a dynamic interface containing resident progenitor cells. Arterioscler Thromb Vasc Biol. 2011;31:1530–9.
Topper JN, Gimbrone MA Jr. Blood flow and vascular gene expression: fluid shear stress as a modulator of endothelial phenotype. Mol Med Today. 1999;5:40–6.
Tanaka H, Shimizu S, Ohmori F, et al. Increases in blood flow and shear stress to nonworking limbs during incremental exercise. Med Sci Sports Exerc. 2006;38:81–5.
Ando J, Yamamoto K. Effects of shear stress and stretch on endothelial function. Antioxid Redox Signal. 2011;15:1389–403.
Balachandran K, Sucosky P, Yoganathan AP. Hemodynamics and mechanobiology of aortic valve inflammation and calcification. Int J Inflam. 2011;2011:263870.
Williams D, Mahmoud M, Liu R, et al. Stable flow-induced expression of KLK10 inhibits endothelial inflammation and atherosclerosis. eLife. 2022;11:e72579.
Cunningham KS, Gotlieb AI. The role of shear stress in the pathogenesis of atherosclerosis. Lab Invest. 2005;85:9–23.
Ghalichi F, Deng X, De Champlain A, et al. Low Reynolds number turbulence modeling of blood flow in arterial stenoses. Biorheology. 1998;35:281–94.
Kinlay S, Grewal J, Manuelin D, et al. Coronary flow velocity and disturbed flow predict adverse clinical outcome after coronary angioplasty. Arterioscler Thromb Vasc Biol. 2002;22:1334–40.
Berk BC. Atheroprotective signaling mechanisms activated by steady laminar flow in endothelial cells. Circulation. 2008;117:1082–9.
Hwang J, Ing MH, Salazar A, et al. Pulsatile versus oscillatory shear stress regulates NADPH oxidase subunit expression: implication for native LDL oxidation. Circ Res. 2003;93:1225–32.
Harrison D, Griendling KK, Landmesser U, et al. Role of oxidative stress in atherosclerosis. Am J Cardiol. 2003;91:7a–11a.
Dewey CF Jr, Bussolari SR, Gimbrone MA Jr, et al. The dynamic response of vascular endothelial cells to fluid shear stress. J Biomech Eng. 1981;103:177–85.
Chien S. Effects of disturbed flow on endothelial cells. Ann Biomed Eng. 2008;36:554–62.
Baek KI, Li R, Jen N, et al. Flow-responsive vascular endothelial growth factor receptor-protein kinase C isoform epsilon signaling mediates glycolytic metabolites for vascular repair. antioxid. Redox Signal. 2018;28:31–43.
Wu D, Huang R-T, Hamanaka RB, et al. HIF-1α is required for disturbed flow-induced metabolic reprogramming in human and porcine vascular endothelium. eLife. 2017;6:e25217.
Li R, Jen N, Wu L, et al. Disturbed flow induces autophagy, but impairs autophagic flux to perturb mitochondrial homeostasis. Antioxid Redox Signal. 2015;23:1207–19.
Cheng C, Helderman F, Tempel D, et al. Large variations in absolute wall shear stress levels within one species and between species. Atherosclerosis. 2007;195:225–35.
Samijo SK, Willigers JM, Barkhuysen R, et al. Wall shear stress in the human common carotid artery as function of age and gender. Cardiovasc Res. 1998;39:515–22.
Callaghan FM, Grieve SM. Normal patterns of thoracic aortic wall shear stress measured using four-dimensional flow MRI in a large population. Am J Physiol Heart Circ Physiol. 2018;315:H1174–81.
Malek AM, Alper SL, Izumo S. Hemodynamic shear stress and its role in atherosclerosis. JAMA. 1999;282:2035–42.
LaBarbera M. Principles of design of fluid transport systems in zoology. Science. 1990;249:992–1000.
Girerd X, London G, Boutouyrie P, et al. Remodeling of the radial artery in response to a chronic increase in shear stress. Hypertension (Dallas, Tex : 1979). 1996;27:799–803.
Murray CD. The physiological principle of minimum work applied to the angle of branching of arteries. J Gen Physiol. 1926;9:835–41.
Li YH, Reddy AK, Taffet GE, et al. Doppler evaluation of peripheral vascular adaptations to transverse aortic banding in mice. Ultrasound Med Biol. 2003;29:1281–9.
Marano G, Palazzesi S, Vergari A, et al. Protection by shear stress from collar-induced intimal thickening: role of nitric oxide. Arterioscler Thromb Vasc Biol. 1999;19:2609–14.
Ibrahim J, Miyashiro JK, Berk BC. Shear stress is differentially regulated among inbred rat strains. Circ Res. 2003;92:1001–9.
Lee K, Choi M, Yoon J, et al. Spectral waveform analysis of major arteries in conscious dogs by Doppler ultrasonography. Vet Radiol Ultrasound. 2004;45:166–71.
Ross G, White FN, Brown AW, et al. Regional blood flow in the rat. J Appl Physiol. 1966;21:1273–5.
Snow HM, Markos F, O’Regan D, et al. Characteristics of arterial wall shear stress which cause endothelium-dependent vasodilatation in the anaesthetized dog. J Physiol. 2001;531:843–8.
LaDisa JF Jr, Olson LE, Molthen RC, et al. Alterations in wall shear stress predict sites of neointimal hyperplasia after stent implantation in rabbit iliac arteries. Am J Physiol Heart Circ Physiol. 2005;288:65–75.
Demos C, Tamargo I, Jo H. Chapter 1 - biomechanical regulation of endothelial function in atherosclerosis. In Biomechanics of Coronary Atherosclerotic Plaque, Ohayon, J., Finet, G., Pettigrew, R.I., Eds. Academic Press: 2021; vol. 4, pp 3–47.
Kwak BR, Bäck M, Bochaton-Piallat ML, et al. Biomechanical factors in atherosclerosis: mechanisms and clinical implications. Eur Heart J. 2014;35(3013–20):20a–20d.
Alderton WK, Cooper CE, Knowles RG. Nitric oxide synthases: structure, function and inhibition. Biochem J. 2001;357:593–615.
Fulton D, Gratton JP, Sessa WC. Post-translational control of endothelial nitric oxide synthase: why isn’t calcium/calmodulin enough? J Pharmacol Exp Ther. 2001;299:818–24.
Davis ME, Cai H, Drummond GR, et al. Shear stress regulates endothelial nitric oxide synthase expression through c-Src by divergent signaling pathways. Circ Res. 2001;89:1073–80.
Gachhui R, Abu-Soud HM, Ghosha DK, et al. Neuronal nitric-oxide synthase interaction with calmodulin-troponin C chimeras. J Biol Chem. 1998;273:5451–4.
Nishida K, Harrison DG, Navas JP, et al. Molecular cloning and characterization of the constitutive bovine aortic endothelial cell nitric oxide synthase. J Clin Invest. 1992;90:2092–6.
De Caterina R, Libby P, Peng HB, et al. Nitric oxide decreases cytokine-induced endothelial activation. Nitric oxide selectively reduces endothelial expression of adhesion molecules and proinflammatory cytokines. J Clin Invest. 1995;96:60–8.
Dimmeler S, Haendeler J, Nehls M, et al. Suppression of apoptosis by nitric oxide via inhibition of interleukin-1beta-converting enzyme (ICE)-like and cysteine protease protein (CPP)-32-like proteases. J Exp Med. 1997;185:601–7.
Dimmeler S, Hermann C, Galle J, et al. Upregulation of superoxide dismutase and nitric oxide synthase mediates the apoptosis-suppressive effects of shear stress on endothelial cells. Arterioscler Thromb Vasc Biol. 1999;19:656–64.
Li J, Billiar TR, Talanian RV, et al. Nitric oxide reversibly inhibits seven members of the caspase family via S-nitrosylation. Biochem Biophys Res Commun. 1997;240:419–24.
Tsao PS, Lewis NP, Alpert S, et al. Exposure to shear stress alters endothelial adhesiveness Role of nitric oxide. Circulation. 1995;92:3513–9.
Rössig L, Haendeler J, Hermann C, et al. Nitric oxide down-regulates MKP-3 mRNA levels: involvement in endothelial cell protection from apoptosis. J Biol Chem. 2000;275:25502–7.
Kim YM, de Vera ME, Watkins SC, et al. Nitric oxide protects cultured rat hepatocytes from tumor necrosis factor-alpha-induced apoptosis by inducing heat shock protein 70 expression. J Biol Chem. 1997;272:1402–11.
Sangwung P, Zhou G, Nayak L, et al. KLF2 and KLF4 control endothelial identity and vascular integrity. JCI insight. 2017;2:e91700.
Ghaleb AM, Yang VW. Krüppel-like factor 4 (KLF4): what we currently know. Gene. 2017;611:27–37.
SenBanerjee S, Lin Z, Atkins GB, et al. KLF2 Is a novel transcriptional regulator of endothelial proinflammatory activation. J Exp Med. 2004;199:1305–15.
Gimbrone MA Jr, García-Cardeña G. Endothelial cell dysfunction and the pathobiology of atherosclerosis. Circ Res. 2016;118:620–36.
Das H, Kumar A, Lin Z, et al. Kruppel-like factor 2 (KLF2) regulates proinflammatory activation of monocytes. Proc Natl Acad Sci USA. 2006;103:6653–8.
Lin Z, Hamik A, Jain R, et al. Kruppel-like factor 2 inhibits protease activated receptor-1 expression and thrombin-mediated endothelial activation. Arterioscler Thromb Vasc Biol. 2006;26:1185–9.
Lingrel JB, Pilcher-Roberts R, Basford JE, et al. Myeloid-specific Krüppel-like factor 2 inactivation increases macrophage and neutrophil adhesion and promotes atherosclerosis. Circ Res. 2012;110:1294–302.
Sweet DR, Fan L, Hsieh PN, et al. Krüppel-like factors in vascular inflammation: mechanistic insights and therapeutic potential. Frontiers in cardiovascular medicine. 2018;5:6.
Fledderus JO, Boon RA, Volger OL, et al. KLF2 primes the antioxidant transcription factor Nrf2 for activation in endothelial cells. Arterioscler Thromb Vasc Biol. 2008;28:1339–46.
Dekker RJ, van Soest S, Fontijn RD, et al. Prolonged fluid shear stress induces a distinct set of endothelial cell genes, most specifically lung Krüppel-like factor (KLF2). Blood. 2002;100:1689–98.
Turpaev KT. Transcription factor KLF2 and its role in the regulation of inflammatory processes. Biochemistry Biokhimiia. 2020;85:54–67.
Wu W, Xiao H, Laguna-Fernandez A, et al. Flow-dependent regulation of Kruppel-like factor 2 is mediated by microRNA-92a. Circulation. 2011;124:633–41.
Schober A, Weber C. Mechanisms of microRNAs in atherosclerosis. Annu Rev Pathol. 2016;11:583–616.
Mathieu P, Pibarot P, Després JP. Metabolic syndrome: the danger signal in atherosclerosis. Vasc Health Risk Manage. 2006;2:285–302.
Yang Q, Xu J, Ma Q, et al. PRKAA1/AMPKα1-driven glycolysis in endothelial cells exposed to disturbed flow protects against atherosclerosis. Nat Commun. 2018;9:4667.
Doddaballapur A, Michalik KM, Manavski Y, et al. Laminar shear stress inhibits endothelial cell metabolism via KLF2-mediated repression of PFKFB3. Arterioscler Thromb Vasc Biol. 2015;35:137–45.
Perrotta P, Van der Veken B, Van Der Veken P, et al. Partial inhibition of glycolysis reduces atherogenesis independent of intraplaque neovascularization in mice. Arterioscler Thromb Vasc Biol. 2020;40:1168–81.
Heo KS, Berk BC, Abe J. Disturbed flow-induced endothelial proatherogenic signaling via regulating post-translational modifications and epigenetic events. Antioxid Redox Signal. 2016;25:435–50.
Villarreal G Jr, Zhang Y, Larman HB, et al. Defining the regulation of KLF4 expression and its downstream transcriptional targets in vascular endothelial cells. Biochem Biophys Res Commun. 2010;391:984–9.
Endres M, Laufs U, Merz H, et al. Focal expression of intercellular adhesion molecule-1 in the human carotid bifurcation. Stroke. 1997;28:77–82.
Yousef GM, Luo LY, Diamandis EP. Identification of novel human kallikrein-like genes on chromosome 19q13.3–q13.4. Anticancer Res. 1999;19:2843–52.
Diamandis EP, Yousef GM, Clements J, et al. New nomenclature for the human tissue kallikrein gene family. Clin Chem. 2000;46:1855–8.
Wang GL, Jiang B-H, Rue EA, et al. Hypoxia-inducible factor 1 is a basic-helix-loop-helix-PAS heterodimer regulated by cellular O2 tension. Proc Natl Acad Sci U S A. 1995;92:5510–4.
Semenza GL. Hypoxia-inducible factor 1: master regulator of O2 homeostasis. Curr Opin Genet Dev. 1998;8:588–94.
Greijer A, Van der Wall E. The role of hypoxia inducible factor 1 (HIF-1) in hypoxia induced apoptosis. J Clin Pathol. 2004;57:1009–14.
Déry M-AC, Michaud MD, Richard DE. Hypoxia-inducible factor 1: regulation by hypoxic and non-hypoxic activators. Int J Biochem. 2005;37:535–40.
Maxwell PH, Dachs GU, Gleadle JM, et al. Hypoxia-inducible factor-1 modulates gene expression in solid tumors and influences both angiogenesis and tumor growth. Proc Natl Acad Sci U S A. 1997;94:8104–9.
Fernandez Esmerats J, Villa-Roel N, Kumar S, et al. Disturbed flow increases UBE2C (Ubiquitin E2 Ligase C) via loss of miR-483-3p, inducing aortic valve calcification by the pVHL (von Hippel-Lindau protein) and HIF-1α (hypoxia-inducible factor-1α) pathway in endothelial cells. Arterioscler Thromb Vasc Biol. 2019;39:467–81.
Feng S, Bowden N, Fragiadaki M, et al. Mechanical activation of hypoxia-inducible factor 1α drives endothelial dysfunction at atheroprone sites. Arterioscler Thromb Vasc Biol. 2017;37:2087–101.
Akhtar S, Hartmann P, Karshovska E, et al. Endothelial hypoxia-inducible factor-1α promotes atherosclerosis and monocyte recruitment by upregulating microRNA-19a. Hypertension (Dallas, Tex : 1979). 2015;66:1220–6.
Salim MT, Villa-Roel N, Vogel B, et al. HIF1A inhibitor PX-478 reduces pathological stretch-induced calcification and collagen turnover in aortic valve. Front Cardiovasc Med. 2022;9:1002067.
Demos C, Johnson J, Andueza A, et al. Sox13 is a novel flow-sensitive transcription factor that prevents inflammation by repressing chemokine expression in endothelial cells. Front Cardiovasc Med. 2022;9:979745.
Wang K-C, Garmire LX, Young A, et al. Role of microRNA-23b in flow-regulation of Rb phosphorylation and endothelial cell growth. Proc Natl Acad Sci U S A. 2010;107:3234–9.
Iaconetti C, De Rosa S, Polimeni A, et al. Down-regulation of miR-23b induces phenotypic switching of vascular smooth muscle cells in vitro and in vivo. Cardiovasc Res. 2015;107:522–33.
Chen K, Fan W, Wang X, et al. MicroRNA-101 mediates the suppressive effect of laminar shear stress on mTOR expression in vascular endothelial cells. Biochem Biophys Res Commun. 2012;427:138–42.
Zhang N, Lei J, Lei H, et al. MicroRNA-101 overexpression by IL-6 and TNF-α inhibits cholesterol efflux by suppressing ATP-binding cassette transporter A1 expression. Exp Cell Res. 2015;336:33–42.
Qin X, Wang X, Wang Y, et al. MicroRNA-19a mediates the suppressive effect of laminar flow on cyclin D1 expression in human umbilical vein endothelial cells. Proc Natl Acad Sci U S A. 2010;107:3240–4.
Ren Z-Q, Liu N, Zhao K. Micro RNA-19a suppresses IL-10 in peripheral B cells from patients with atherosclerosis. Cytokine. 2016;86:86–91.
Chen H, Li X, Liu S, et al. MircroRNA-19a promotes vascular inflammation and foam cell formation by targeting HBP-1 in atherogenesis. Sci Rep. 2017;7:12089.
Fang Y, Davies PF. Site-specific microRNA-92a regulation of Kruppel-like factors 4 and 2 in atherosusceptible endothelium. Arterioscler Thromb Vasc Biol. 2012;32:979–87.
Bonauer A, Carmona G, Iwasaki M, et al. MicroRNA-92a controls angiogenesis and functional recovery of ischemic tissues in mice. Science. 2009;324:1710–3.
Wang W-L, Chen L-J, Wei S-Y, et al. Mechanoresponsive Smad5 enhances MiR-487a processing to promote vascular endothelial proliferation in response to disturbed flow. Front Cell Dev Biol. 2021;9:647714.
Lee S, Jue M, Cho M, et al. Label-free atherosclerosis diagnosis through a blood drop of apolipoprotein E knockout mouse model using surface-enhanced Raman spectroscopy validated by machine learning algorithm. Bioeng Transl Med. 2023;8:e10529.
Acknowledgements
This study is supported by the National Institutes of Health 5T32HL007745-28 (KB).
Funding
National Institutes of Health, 5T32HL007745-28, Kyung In Baek
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Human Subjects/Informed Consent Statement
No human studies were carried out by the authors for this article.
Animal Studies
No animal studies were carried out by the authors for this article.
Additional information
Associate Editor Judith Sluimer oversaw the review of this article
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Baek, K.I., Ryu, K. Role of Flow-Sensitive Endothelial Genes in Atherosclerosis and Antiatherogenic Therapeutics Development. J. of Cardiovasc. Trans. Res. 17, 609–623 (2024). https://doi.org/10.1007/s12265-023-10463-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-023-10463-w