Abstract
Lecithin:cholesterol acyltransferase (LCAT) is the key circulating enzyme responsible for high-density lipoprotein (HDL) cholesterol esterification, HDL maturation, and potentially reverse cholesterol transport. To further explore LCAT’s mechanism of action on lipoprotein metabolism, we employed adeno-associated viral vector (AAV) serotype 8 to achieve long-term (32-week) high level expression of human LCAT in hCETP;Ldlr+/− mice, and characterized the lipid profiles in detail. The mice had a marked increase in HDL cholesterol, HDL particle size, and significant reduction in low-density lipoprotein (LDL) cholesterol, plasma triglycerides, and plasma apoB. Plasma LCAT activity significantly increased with humanized substrate specificity. HDL cholesteryl esters increased in a fashion that fits human LCAT specificity. HDL phosphatidylcholines trended toward decrease, with no change observed for HDL lysophosphatidylcholines. Triglycerides reduction appeared to reside in all lipoprotein particles (very low-density lipoprotein (VLDL), LDL, and HDL), with HDL triglycerides composition highly reflective of VLDL, suggesting that changes in HDL triglycerides were primarily driven by the altered triglycerides metabolism in VLDL. In summary, in this human-like model for lipoprotein metabolism, AAV8-mediated overexpression of human LCAT resulted in profound changes in plasma lipid profiles. Detailed lipid analyses in the lipoprotein particles suggest that LCAT's beneficial effect on lipid metabolism includes not only enhanced HDL cholesterol esterification but also improved metabolism of apoB-containing particles and triglycerides. Our findings thus shed new light on LCAT’s mechanism of action and lend support to its therapeutic potential in treating dyslipidemia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lecithin:cholesterol acyltransferase (LCAT) is a liver-produced circulating enzyme that transfers the fatty acyl chain from the sn-2 position of phosphatidylcholine (PC) to 3β-hydroxyl group in free cholesterol (FC) [1, 2]. The majority of circulating LCAT resides in HDL particles and is responsible for cholesterol esterification in HDL and HDL maturation from small nascent particles to large, cholesteryl ester (CE)-enriched particles [3, 4]. It has therefore been hypothesized that increased LCAT activity can increase HDL cholesterol level, promote the process of reverse cholesterol transport (RCT), normalize dyslipidemia, and potentially exert an anti-atherosclerotic effect [2, 5–7].
Since the discovery of LCAT in the 1960s [8], full and partial loss-of-function natural mutations have been identified and characterized, with their corresponding disease conditions designated as Familial LCAT deficiency (FLD) and Fish-eye disease (FED), respectively [9]. Clinical presentations of FLD and FED are highly variable but always associated with HDL deficiency [9, 10]. LCAT mutant allele carriers may also have elevated low-density lipoprotein (LDL) [11] and develop atherosclerosis to variable extent [12–15].
A number of LCAT loss-of-function or transgenic studies in preclinical species ranging from mouse to nonhuman primate have also been reported, with various effects on lipid metabolism and lesion development. LCAT knockout (KO) mice on the apolipoprotein E (apoE) KO or low-density lipoprotein receptor (LDLR) KO background had reduced HDL but paradoxically reduced atherosclerosis, possibly due to concomitant reduction in non-HDL [16]. Transgenic overexpression of LCAT in mice resulted in an increase in large, CE-enriched HDL but paradoxically accelerated atherosclerosis [17], which was ameliorated when cholesteryl ester transfer protein (CETP) transgene was further introduced [18]. In comparison, in higher, endogenous CETP-containing species such as rabbit, transgenic overexpression of LCAT resulted in not only significant increase in HDL, but also marked decrease in non-HDL, triglyceride, and lesion development [19]. Taken together, these results suggest that impacts of LCAT on lipid profile and lesion development are highly dependent on animal models and key parameters in lipid metabolism; gain of LCAT function in the right models may offer predictive benefit regarding therapeutic potential of targeting LCAT. Indeed, adenoviral vector (Ad)-mediated overexpression of human LCAT (hLCAT) in hamster, which has CETP and similar lipoprotein metabolism to human, resulted in not only increased HDL, but also increased biliary cholesterol excretion and increased hepatic transcription of Cyp7a1, suggesting increased RCT [20]. Ad-mediated overexpression of hLCAT in nonhuman primates also resulted in antiatherogenic lipid profile characterized by increased HDL, decreased apoB, increased LDL catabolism, and decreased triglycerides [21].
In this report, we sought to further study LCAT’s mechanism of action on lipid metabolism in order to assess its therapeutic potential. We chose the mouse model that is hemizygous of the human CETP transgene driven by human apoAI promoter and hemizygous for the LDLR locus (hCETP;Ldlr+/−) because this model confers the mice with proatherogenic properties and bears high relevance to lipoprotein metabolism in humans. We employed the recombinant adeno-associated viral vector serotype 8 (AAV8) for liver-directed delivery of hLCAT. Recombinant AAV is an attractive system for target gene modulation because of its non-pathogenicity, low immunogenicity, and ability to mediate long-term expression in multiple differentiated tissues across various preclinical animal species [22–26]. AAV8 has been demonstrated to be highly liver tropic with excellent transduction efficiency in mouse liver [23, 27] and was therefore selected to overexpress hLCAT. Here, we describe our 4-week pilot study and 32-week long-term study of AAV8-mediated LCAT overexpression in hCETP;Ldlr+/− mice.
Methods
Generation of AAV Vectors
Human LCAT cDNA was obtained by polymerase chain reaction (PCR) from an Invitrogen ORF clone (Invitrogen IOH10295), and inserted into a pAAV Cis plasmid downstream of the liver-specific thyroxine binding globulin promoter. The pAAV cis plasmid and the production of AAV8-luciferase (“AAV-Luc”) and AAV8-hLCAT (“AAV-hLCAT”) were provided by the Viral Vector Core of the University of Massachusetts Medical School under a fee-for-service agreement. The AAV8 vectors were produced by the helper-free triple plasmid transfection method by cotransfecting the pAAV cis plasmid, an adenoviral helper plasmid, and a chimeric packaging plasmid in which the AAV2 rep gene was fused with the AAV8 cap gene. The AAV vectors were then purified using double cesium chloride gradient centrifugation, and titers were determined via a real-time PCR analysis.
Animal Studies
All animal procedures were approved by the Institutional Animal Care and Use Committee of Merck Research Laboratories. Male C57Bl/6 mice engineered to be hemizygous for a knockout of LDLR and hemizygous for the overexpression of the hCETP driven by the human ApoAI promoter within a C57Bl/6 background (hCETP;Ldlr+/−) were housed in temperature-, humidity-, and light-controlled rooms with ad libitum access to water and food (breeder chow diet 5021, Purina). The mice were 10-weeks (long-term study) or 18-weeks (pilot study) old at the beginning of the studies. AAV-hLCAT or AAV-Luc was administrated by tail vein injection at the dose of 1 × 1012 or 0.5 × 1012 Genome Copies (GC) per mouse in 100 μl physiological saline and were examined for 4 or 32 weeks, respectively. Blood was collected by tail vein bleeding at various intermediate time points postinjection to determine plasma hLCAT protein and HDL cholesterol. Body weight was monitored weekly throughout the studies. At the end of the studies, euthanization occurred in the mornings with the animals at ad libitum feeding state; blood was collected by cardiac puncture for measuring lipids and other metabolic parameters.
Analytical Methods for Plasma Lipids, Lipoproteins, and Apolipoproteins
LCAT protein was measured using a commercially available ELISA kit (ALPCO Diagnostics). LCAT activity was determined via a stable isotope-based liquid chromatography–mass spectrometry (LC/MS) method modified from the original proteoliposome-thin layer chromatography method [28]. Plasma apoAI and apoB levels were measured by an ELISA assay and an LC/MS assay, respectively. Total cholesterol (TC), HDL cholesterol (HDLc), triglycerides (TG), CE, FC, phospholipids (PL, including PC, lysophosphatidylcholines (LysoPC), and sphingomyelins) in unfractionated plasma were determined by commercially available kits (Wako Diagnostics); LDL cholesterol (LDLc) and very low-density lipoprotein cholesterol (VLDLc) were determined by fast performance liquid chromatography (FPLC). Lipid classes in the lipoprotein particles were analyzed via LC/MS. Details of the analytical methods are provided in the Supplemental Material.
Data Analysis
Data are presented as mean ± standard error of the mean. Two-tailed, two-parameter, unpaired Student’s t tests were performed between the AAV-hLCAT group and the AAV-Luc group, and P values that were <0.05 were considered statistically significant.
Results
Sustained hLCAT Expression and HDL Raising was Achieved After a Single Dose of AAV-hLCAT
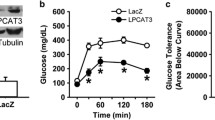
A pilot study was first carried out where AAV-Luc and AAV-hLCAT were injected into the mice at 1 × 1012 GC per mouse, along with saline control (n = 8 per group). Animals were sacrificed at 4 weeks postinjection. A Taqman analysis of the liver samples from the AAV-hLCAT-treated group demonstrated a high expression of hLCAT mRNA (not shown). Plasma hLCAT protein analysis via a commercially available, pre-validated, and hLCAT-specific [29] ELISA confirmed that AAV-hLCAT treatment produced a markedly high (∼800 μg/ml) level of circulating hLCAT (Fig. 1a). The ELISA did not detect any signal in the plasma from AAV-Luc- or saline-treated mice (not shown). A 2.1-fold increase in HDL was observed at 2 weeks postinjection, and the effect persisted until the end of the 4-week study (Fig. 1b). Taken together, the pilot study demonstrated that AAV-mediated hLCAT expression was robust and led to an increase in HDL, the hallmark of LCAT overexpression.
AAV-mediated hLCAT expression and HDL raising was achieved in a pilot 4-week study. Saline, AAV-hLCAT, or AAV-Luc was injected into hCETP;Ldlr+/− mice at 1 × 1012 GC per mouse at day 0. The mice were maintained on breeder chow diet until takedown at 28 days postinjection. a Plasma hLCAT protein levels at study termination as determined by ELISA. No hLCAT protein was detected in the AAV-Luc- or saline-treated groups (not shown). b Plasma HDLc (HDL) levels from intermediate and terminal bleeds as measured by the Wako kit. n = 8 per group; *p < 0.05 compared to AAV-Luc
Given the pilot study yielded a hLCAT level that is tremendously higher than circulating LCAT level in humans, which is between 1 and 10 μg/ml by multiple methods [30, 31], we lowered the vector dose to half of the pilot study and injected the mice with AAV-hLCAT or AAV-Luc at 0.5 × 1012 GC/mouse, along with saline control (n = 9 per group). Plasma levels of hLCAT and HDL were monitored until study termination at 32 weeks postinjection. Human LCAT was present at about 300 μg/ml at 2 weeks and declined slightly over the course of the experiment to a final concentration of 220 μg/ml at study termination (Fig. 2a). Although endogenous LCAT level in mice is unknown, it is likely in the similar magnitude to humans. We therefore have achieved likely more than a 20-fold overexpression of hLCAT above endogenous background in these mice. Prolonged increase in HDL (1.4- to 2-fold increase compared to the Luc group, and up to 150 mg/dL) was also observed from 2 weeks on until study termination (Fig. 2b).
Sustained hLCAT expression and HDL raising were observed in the 32-week study. Saline, AAV-hLCAT or AAV-Luc was injected into hCETP;Ldlr+/− mice at 0.5 × 1012 GC per mouse at day 0. The mice were maintained on breeder chow diet until takedown at 32 weeks postinjection. a Plasma hLCAT protein levels at various intermittent time points as determined by ELISA. hLCAT protein was not detectable in the AAV-Luc- or saline-treated groups (not shown). b Plasma HDL levels as measured by the Wako kit. c Ex vivo LCAT activity from terminal bleeds as determined by the modified LC/MS methods. Relative quantitations of newly formed CE species (d6-CE 18:2, d6-CE 18:1, d6-CE 20:4, and d6-CE 22:6) were generated from LC/MS, then expressed as fold over the Luc group, with the average of the Luc group defined as onefold. n = 9 per group; *p < 0.05 compared to AAV-Luc
Next, we evaluated functional properties of the overexpressed hLCAT protein from terminal bleeds with an LC/MS activity assay that also reveals fatty acyl chain preference of LCAT. A significant increase in the formation of four d6-CE product species was observed in the hLCAT group compared to the Luc group. Moreover, the fold increase of the hLCAT group over the Luc group was much higher in d6-CE 18:2 and d6-CE 18:1 than in d6-CE 20:4 and d6-CE 22:6 (Fig. 2c). This observation is consistent with the fact that human LCAT favors 18:2 and 18:1 more than 20:4 and 22:6 at the sn-2 position, whereas mouse LCAT is the opposite[32, 33]. No other deuterium-labeled CE species were detected, consistent with the fact that 18:2, 18:1, 20:4, and 22:6 constitute the majority of fatty acyl groups in the sn-2 position of egg yolk PC in the substrate [34, 35]. In conclusion, circulating hLCAT in these hCETP;Ldlr+/− mice was functionally active, and its substrate specificity was characteristic of the human enzyme.
Lipids, Lipoproteins, and Apolipoproteins in Whole Plasma
Lipids, lipoproteins, and apolipoproteins in unfractionated whole plasma at study termination were analyzed, and results are shown in Table 1. Compared to the Luc group, the hLCAT group had a significant increase in plasma TC, HDLc, CE, FC, and PL, and a significant decrease in plasma LDLc and apoB. Plasma TG level in the hLCAT group also displayed a robust (45%) and significant reduction. VLDLc was overall at a much lower level than LDLc and trended toward decrease without reaching statistical significance. There was no significant difference in plasma apoAI level between the two groups. For additional parameters in unfractionated plasma, the hLCAT group had significantly lower FFA levels than the Luc group, whereas β-HBA (beta-hydroxybutyrate), glucose, AST (aspartate aminotransferase), and ALT (alanine aminotransferase) remained unchanged (not shown).
Lipid Analyses in the Lipoprotein Particles
Lipoproteins in plasma samples from the Luc group and hLCAT group were separated by two independent methods, FPLC and polyacrylamide gel electrophoresis. Both analyses revealed the increased HDL particle size in the hLCAT group (Fig. 3).
HDL particle size increased in the AAV-hLCAT group. Lipoproteins in the terminal bleeds were separated by two independent methods, FPLC and polyacrylamide gel electrophoresis. a FPLC profiles of the Luc group and the hLCAT group to illustrate appearance of larger HDL in the latter group. Y-axis is the absorbance at 600 nm from in-line colorimetric assay for TC. Each line represents one mouse in the group. b Polyacrylamide gel electrophoresis image of a representative sample from each group to illustrate slower migration of HDL in the hLCAT group. n = 9 per group
To isolate the lipoprotein particles for subsequent lipid analysis, the polyacrylamide gel electrophoresis system was chosen because it offers better separation of HDL from LDL compared to the FPLC system. Gel fragments containing VLDL, LDL, and HDL were excised, subjected to lipid extraction, followed by LC/MS analyses of all lipid species in major lipid classes (CE, PC, LysoPC, TG) as well as FC. HDL lipid compositional analysis (Fig. 4) demonstrated that HDL in the hLCAT group had significantly increased CE, significantly decreased TG, and marginally significantly decreased PC, compared to HDL in the Luc group. Moreover, percentage of CE in HDL lipids had increased from 28% in the Luc group to 43% in the hLCAT group, indicating that HDL particles in the hLCAT group became highly CE-enriched. The increase in HDL CE was predominantly in CE 18:1 and CE 18:2, while the increase in additional CE species was much more modest and statistically insignificant (Table 2). The hLCAT group thus displayed a humanized CE profile due to hLCAT expression.
Lipid composition in HDL. Lipoprotein particles from the AAV-Luc and AAV-hLCAT groups were isolated from gel electrophoresis, with their lipids subsequently extracted and quantitated by LC/MS. Top, a pie chart in which major lipid classes (CE, PC, LysoPC, TG, FC) are expressed as a percentage of total lipids in HDL. Bottom, mean ± standard error of mean for each lipid class in each HDL group. n = 8 per group; *p < 0.05 compared to AAV-Luc; †p = 0.05 compared to AAV-Luc
Given the robust plasma TG reduction in the preceding analysis (Table 1), we analyzed the TG content and composition in the lipoprotein particles in detail. HDL TG composition is delineated in Table 3. For all 18 detectable TG species, HDL TG in the hLCAT group either trended toward a decrease or displayed a significant decrease compared to HDL TG in the Luc group. The hLCAT group also exhibited a significant reduction in TG content in LDL, and a trend toward TG reduction in VLDL (Fig. 5a). In the hLCAT group, TG composition in HDL had a striking similarity to the TG composition in VLDL (Fig. 5b).
TG analysis in the lipoprotein particles. a Level of TG as determined by LC/MS, in VLDL, LDL, and HDL from the AAV-Luc group and AAV-hLCAT group. b Compositional analysis of TG in HDL and VLDL from the AAV-hLCAT group. Each TG species is expressed as percentage of total TG in the corresponding lipoprotein particle. All TG species that were detectable in HDL were included in the graph. n = 8 per group; *p < 0.05 compared to AAV-Luc
PC analysis in the lipoprotein particles indicated that while PC content in HDL of the hLCAT group had a marginally significant decrease, LDL PC content had no major change and VLDL PC trended toward increase (Fig. 6a). All major PC species appeared to change in the opposite directions in VLDL and HDL (Fig. 6b).
PC analysis in the lipoprotein particles. a Level of PC as determined by LC/MS, in VLDL, LDL, and HDL from the AAV-Luc group and AAV-hLCAT group. b Change in PC species in VLDL and HDL. Results are expressed as percentage of change for each PC species, in either VLDL or HDL, in the hLCAT group compared to the Luc group. PC 28:4 and PC 30:4 were not included in this analysis as they were very minor species (<1% of total PC in the lipoprotein fractions). n = 8 per group; †p = 0.05 compared to AAV-Luc
Discussion
In this study, we achieved a robust and sustained overexpression of circulating hLCAT and concomitant HDL raising in hCETP;Ldlr+/− mice via a single dose of AAV-hLCAT. AAV-hLCAT-treated animals were healthy with normal body weight gain, normal liver enzyme levels, and normal liver pathology as compared to the AAV-Luc and saline control groups (not shown), suggesting hLCAT overexpression in these mice did not alter their general physiology. AAV-mediated LCAT expression also appeared titratable. Thus, dose-ranging studies could be further performed to identify a therapeutic window.
It has been suggested that increased HDL levels and large HDL particles may be associated with a reduced risk for cardiovascular diseases [36–39]. Increasing LCAT function is therefore an attractive therapeutic approach as it promotes HDL maturation from small pre-beta migrating particles to large CE-enriched particles. In our study, with a persisting, over 20-fold overexpression of LCAT and remarkable increase in LCAT activity, we observed a corresponding prominent (1.4- to 2-fold) increase in HDL cholesterol over the 32-week study period (Fig. 2). Circulating apoAI level remained the same (Table 1), suggesting that the major change was in HDL particle size as a result of CE-enrichment, rather than particle number. Indeed our FPLC and polyacrylamide gel fractionation systems both revealed the appearance of larger HDL particles (Fig. 3). Although additional studies are needed to delineate functional properties of these large HDL particles, our results demonstrate that chronic overexpression of hLCAT can elicit a prolonged effect of HDL raising, HDL particle enlargement, and a humanized HDL CE profile.
A significant reduction in LDL and apoB was also observed in our study. It had been demonstrated that hLCAT-transgenic rabbit had reduced apoB level due to increased apoB fractional catabolic rate (FCR) [40]; Ad-mediated short-term expression of hLCAT in nonhuman primates also exhibited apoB reduction due to increased FCR of LDL [21]. In comparison, LCAT overexpression in mice that lacked LDLR [41] or lacked CETP transgene [18] did not produce apoB reduction. We therefore hypothesize that our LDL and apoB lowering was due to enhanced LDL and apoB clearance through the retained copy of LDLR, after transfer of CE from CE-enriched HDL to non-HDL via CETP. It is to be noted here that since our mice were not on atherogenic diet, their apoB and LDL levels were modest. Future studies on atherogenic diet with analyses on LDL production rate and FCR are needed to further explore the mechanism of LDL reduction.
TG, PC, and LysoPC, as additional major lipid classes in circulation, were analyzed in the lipoprotein particles as well. We found that TG reduction was broad in the TG class and in lipoprotein fractions, and that TG composition in HDL was highly similar to VLDL (Fig. 5). The latter observation is consistent with the understanding that VLDL is the main origin for plasma TG, and that TG incorporation in HDL is primarily due to CETP action in these mice. Our observation of TG reduction is also consistent with the LCAT overexpression model in monkeys [21] and the observation that FLD patients typically have hypertriglyceridemia possibly due to defective chylomicron and VLDL clearance [15, 42]. It is plausible that hLCAT overexpression in these mice had resulted in increased lipase activity and VLDL lipolysis and that TG reduction in HDL was primarily driven by TG reduction in VLDL and mediated by CETP action. For PC analysis, the AAV-hLCAT-treated mice displayed a weak trend of reduced HDL PC (Fig. 6a), consistent with the finding that FLD patients tend to have increased HDL PC [42]; all major PC species appeared to change in opposite directions in VLDL and HDL (Fig. 6b), suggesting that phospholipid transfer protein activity may have been modulated. Total plasma PC had an insignificant 7% increase in the AAV-hLCAT-treated mice (not shown) and was consistent with the analysis of plasma PL (Table 1). For LysoPC analysis, somewhat counterintuitively, AAV-hLCAT-treated mice showed no difference from AAV-Luc-treated mice in LysoPC content or composition (Fig. 4 and not shown). A detailed understanding of the above results awaits future studies on circulating enzymes, particularly those involved in TG, PC, and LysoPC metabolism.
Lipids in liver, bile, and feces were also analyzed and displayed no major changes between the Luc and the hLCAT groups (not shown). Absence of significant changes in these compartments despite prominent changes in circulating lipids suggests that the whole body lipid metabolism may have reached a new steady state. Acute phase studies instead, may allow a better view of responses in tissue lipid metabolism and mechanism of LCAT action; metabolic flux studies with a tracer approach in an atherosclerosis model may further elucidate LCAT’s role in reverse cholesterol transport and atherosclerosis.
Transcriptional regulation of LCAT expression in liver is poorly understood. Overexpression of LCAT protein under normal physiological conditions may not be easily achievable. Interpretation of our findings with regard to its therapeutic potential thus carries a limitation. Nonetheless, using the AAV8 delivery platform, we created an animal model that mimics chronic yet non-lifetime LCAT protein therapy. Unlike most LCAT transgenic mouse models, our model exhibited not only increased HDL, but also reduced LDL, triglycerides, and apoB. Our detailed characterization of major lipid classes in lipoprotein particles points to an intimate role of LCAT in metabolism of not only HDL and CE lipid class, but also apoB-containing particles and additional lipid classes. Our results thus pave the way for future studies on LCAT’s role in lipoprotein metabolism and dyslipidemia.
References
Osuga, T., & Portman, O. W. (1971). Origin and disappearance of plasma lecithin: cholesterol acyltransferase. American Journal of Physiology, 220, 735–741.
Glomset, J. A. (1968). The plasma lecithins:cholesterol acyltransferase reaction. Journal of Lipid Research, 9, 155–167.
Francone, O. L., Gurakar, A., & Fielding, C. (1989). Distribution and functions of lecithin:cholesterol acyltransferase and cholesteryl ester transfer protein in plasma lipoproteins. Evidence for a functional unit containing these activities together with apolipoproteins A-I and D that catalyzes the esterification and transfer of cell-derived cholesterol. Journal of Biological Chemistry, 264, 7066–7072.
Rader, D. J., Ikewaki, K., Duverger, N., Schmidt, H., Pritchard, H., Frohlich, J., et al. (1994). Markedly accelerated catabolism of apolipoprotein A-II (ApoA-II) and high density lipoproteins containing ApoA-II in classic lecithin: cholesterol acyltransferase deficiency and fish-eye disease. The Journal of Clinical Investigation, 93, 321–330.
Fielding, C. J., & Fielding, P. E. (1995). Molecular physiology of reverse cholesterol transport. Journal of Lipid Research, 36, 211–228.
Applebaum-Bowden, D. (1995). Lipases and lecithin: cholesterol acyltransferase in the control of lipoprotein metabolism. Current Opinion in Lipidology, 6, 130–135.
Dobiasova, M., & Frohlich, J. J. (1999). Advances in understanding of the role of lecithin cholesterol acyltransferase (LCAT) in cholesterol transport. Clinica Chimica Acta, 286, 257–271.
Glomset, J. A. (1962). The mechanism of the plasma cholesterol esterification reaction: plasma fatty acid transferase. Biochimica et Biophysica Acta, 65, 128–135.
Kuivenhoven, J. A., Pritchard, H., Hill, J., Frohlich, J., Assmann, G., & Kastelein, J. (1997). The molecular pathology of lecithin:cholesterol acyltransferase (LCAT) deficiency syndromes. Journal of Lipid Research, 38, 191–205.
Calabresi, L., Pisciotta, L., Costantin, A., Frigerio, I., Eberini, I., Alessandrini, P., et al. (2005). The molecular basis of lecithin:cholesterol acyltransferase deficiency syndromes: a comprehensive study of molecular and biochemical findings in 13 unrelated Italian families. Arteriosclerosis, Thrombosis, and Vascular Biology, 25, 1972–1978.
Hovingh, G. K., Hutten, B. A., Holleboom, A. G., Petersen, W., Rol, P., Stalenhoef, A., et al. (2005). Compromised LCAT function is associated with increased atherosclerosis. Circulation, 112, 879–884.
Gjone, E. (1974). Familial lecithin:cholesterol acyltransferase deficiency—a clinical survey. Scandinavian Journal of Clinical and Laboratory Investigation. Supplementum, 137, 73–82.
Stokke, K. T., Bjerve, K. S., Blomhoff, J. P., Oystese, B., Flatmark, A., Norum, K. R., et al. (1974). Familial lecithin:cholesterol acyltransferase deficiency. Studies on lipid composition and morphology of tissues. Scandinavian Journal of Clinical and Laboratory Investigation. Supplementum, 137, 93–100.
Homma, S., Murayama, N., Yoshida, I., Kusano, E., Kuriki, K., Saito, K., et al. (2001). Marked atherosclerosis in a patient with familiar lecithin: cholesterol acyltransferase deficiency associated with end-stage renal disease and diabetes mellitus. American Journal of Nephrology, 21, 415–419.
Funke, H., von Eckardstein, A., Pritchard, P. H., Hornby, A. E., Wiebusch, H., Motti, C., et al. (1993). Genetic and phenotypic heterogeneity in familial lecithin: cholesterol acyltransferase (LCAT) deficiency. Six newly identified defective alleles further contribute to the structural heterogeneity in this disease. The Journal of Clinical Investigation, 91, 677–683.
Lambert, G., Sakai, N., Vaisman, B. L., Neufeld, E. B., Marteyn, B., Chan, C. C., et al. (2001). Analysis of glomerulosclerosis and atherosclerosis in lecithin cholesterol acyltransferase-deficient mice. Journal of Biological Chemistry, 276, 15090–15098.
Berard, A. M., Foger, B., Remaley, A., Shamburek, R., Vaisman, B. L., Talley, G., et al. (1997). High plasma HDL concentrations associated with enhanced atherosclerosis in transgenic mice overexpressing lecithin-cholesteryl acyltransferase. Nature Medicine, 3, 744–749.
Foger, B., Chase, M., Amar, M. J., Vaisman, B. L., Shamburek, R. D., Paigen, B., et al. (1999). Cholesteryl ester transfer protein corrects dysfunctional high density lipoproteins and reduces aortic atherosclerosis in lecithin cholesterol acyltransferase transgenic mice. Journal of Biological Chemistry, 274, 36912–36920.
Hoeg, J. M., Santamarina-Fojo, S., Berard, A. M., Cornhill, J. F., Herderick, E. E., Feldman, S. H., et al. (1996). Overexpression of lecithin:cholesterol acyltransferase in transgenic rabbits prevents diet-induced atherosclerosis. Proceedings of the National Academy of Sciences of the United States of America, 93, 11448–11453.
Zhang, A. H., Gao, S., Fan, J. L., Huang, W., Zhao, T. Q., & Liu, G. (2004). Increased plasma HDL cholesterol levels and biliary cholesterol excretion in hamster by LCAT overexpression. FEBS Letters, 570, 25–29.
Amar, M. J., Shamburek, R. D., Vaisman, B., Knapper, C. L., Foger, B., Hoyt, R. F., Jr., et al. (2009). Adenoviral expression of human lecithin-cholesterol acyltransferase in nonhuman primates leads to an antiatherogenic lipoprotein phenotype by increasing high-density lipoprotein and lowering low-density lipoprotein. Metabolism, 58, 568–575.
Vandenberghe, L. H., Wilson, J. M., & Gao, G. (2009). Tailoring the AAV vector capsid for gene therapy. Gene Therapy, 16, 311–319.
Nakai, H., Fuess, S., Storm, T. A., Muramatsu, S., Nara, Y., & Kay, M. A. (2005). Unrestricted hepatocyte transduction with adeno-associated virus serotype 8 vectors in mice. Journal of Virology, 79, 214–224.
Inagaki, K., Fuess, S., Storm, T. A., Gibson, G. A., McTiernan, C. F., Kay, M. A., et al. (2006). Robust systemic transduction with AAV9 vectors in mice: efficient global cardiac gene transfer superior to that of AAV8. Molecular Therapy, 14, 45–53.
Wang, Z., Zhu, T., Rehman, K. K., Bertera, S., Zhang, J., Chen, C., et al. (2006). Widespread and stable pancreatic gene transfer by adeno-associated virus vectors via different routes. Diabetes, 55, 875–884.
Gao, G., Lu, Y., Calcedo, R., Grant, R. L., Bell, P., Wang, L., et al. (2006). Biology of AAV serotype vectors in liver-directed gene transfer to nonhuman primates. Molecular Therapy, 13, 77–87.
Gao, G. P., Alvira, M. R., Wang, L., Calcedo, R., Johnston, J., & Wilson, J. M. (2002). Novel adeno-associated viruses from rhesus monkeys as vectors for human gene therapy. Proceedings of the National Academy of Sciences of the United States of America, 99, 11854–11859.
Chen, C. H., & Albers, J. J. (1982). Characterization of proteoliposomes containing apoprotein A-I: a new substrate for the measurement of lecithin: cholesterol acyltransferase activity. Journal of Lipid Research, 23, 680–691.
Kobori, K., Saito, K., Ito, S., Kotani, K., Manabe, M., & Kanno, T. (2002). A new enzyme-linked immunosorbent assay with two monoclonal antibodies to specific epitopes measures human lecithin-cholesterol acyltransferase. Journal of Lipid Research, 43, 325–334.
Albers, J. J., Chen, C. H., & Adolphson, J. L. (1981). Lecithin:cholesterol acyltransferase (LCAT) mass; its relationship to LCAT activity and cholesterol esterification rate. Journal of Lipid Research, 22, 1206–1213.
Pahl, M. V., Ni, Z., Sepassi, L., Moradi, H., & Vaziri, N. D. (2009). Plasma phospholipid transfer protein, cholesteryl ester transfer protein and lecithin:cholesterol acyltransferase in end-stage renal disease (ESRD). Nephrology, Dialysis, Transplantation, 24, 2541–2546.
Grove, D., & Pownall, H. J. (1991). Comparative specificity of plasma lecithin:cholesterol acyltransferase from ten animal species. Lipids, 26, 416–420.
Liu, M., Bagdade, J. D., & Subbaiah, P. V. (1995). Specificity of lecithin:cholesterol acyltransferase and atherogenic risk: comparative studies on the plasma composition and in vitro synthesis of cholesteryl esters in 14 vertebrate species. Journal of Lipid Research, 36, 1813–1824.
Kuksis, A., & Marai, L. (1967). Determination of the complete structure of natural lecithins. Lipids, 2, 217–224.
Adlof, R. (1991). Fractionation of egg and soybean phosphatidylcholines by silver resin chromatography. Journal of Chromatography, 538, 469–473.
Castelli, W. P., Doyle, J. T., Gordon, T., Hames, C. G., Hjortland, M. C., Hulley, S. B., et al. (1977). HDL cholesterol and other lipids in coronary heart disease. The cooperative lipoprotein phenotyping study. Circulation, 55, 767–772.
Havel, R. J. (1979). High-density lipoproteins, cholesterol transport and coronary heart disease. Circulation, 60, 1–3.
Assmann, G., & Gotto, A. M., Jr. (2004). HDL cholesterol and protective factors in atherosclerosis. Circulation, 109, III8–III14.
Nicholls, S. J., Tuzcu, E. M., Sipahi, I., Grasso, A. W., Schoenhagen, P., Hu, T., et al. (2007). Statins, high-density lipoprotein cholesterol, and regression of coronary atherosclerosis. Jama., 297, 499–508.
Amar, M. E., Santamarina-Fojo, S., Brewer, H. B., Jr., & Hoeg, J. M. (1997). Overexpression of human lecithin:cholesterol acyltransferase in cholesterol-fed rabbits: LDL metabolism and HDL metabolism are affected in a gene dose-dependent manner. Metabolism, 38, 568–575.
Brousseau, M. E., Kauffman, R. D., Herderick, E. E., Demosky, S. J., Jr., Evans, W., Marcovina, S., et al. (2000). LCAT modulates atherogenic plasma lipoproteins and the extent of atherosclerosis in lecithin cholesterol acyltransferase transgenic mice. Journal of Biology, 20, 450–458.
Norum, K. R., Glomset, J. A., Nichols, A. V., & Forte, T. (1971). Plasma lipoproteins in familial lecithin: cholesterol acyltransferase deficiency: physical and chemical studies of low and high density lipoproteins. The Journal of Clinical Investigation, 50, 1131–1140.
Acknowledgments
We thank our colleagues Bo Wang and Christian Nunes for support of the tail vein injection, Beth Murphy for coordinating mice shipment, and Yong-hua Zhu for the pathology report.
Author information
Authors and Affiliations
Corresponding authors
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
ESM 1
(DOC 43 kb)
Rights and permissions
About this article
Cite this article
Chen, Z., Chu, D., Castro-Perez, J.M. et al. AAV8-Mediated Long-Term Expression of Human LCAT Significantly Improves Lipid Profiles in hCETP;Ldlr+/− Mice. J. of Cardiovasc. Trans. Res. 4, 801–810 (2011). https://doi.org/10.1007/s12265-011-9309-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-011-9309-8