Abstract
Pneumonectomy is a type of lung resection with high morbidity and mortality and is more commonly performed for the treatment of lung cancer. The aim of this study is to demonstrate the feasibility and safety of VATS pneumonectomy in the treatment of non-small cell lung cancer based on our own clinical experience. We retrospectively analyzed patients with NSCLC who underwent pneumonectomy between January 2016 and May 2021. Preoperative, operative, and postoperative results of VATS and thoracotomy groups were analyzed and compared. This study was approved by the local ethics committee and informed consent was obtained from all individual participants included in the study (Registration number: 49109414–604.02; Date: 24/01/2020). A total of 135 patients were included in the study. There were 20 patients who underwent VATS pneumonectomy and 115 patients who underwent open pneumonectomy. There was no difference between VATS and thoracotomy groups in terms of operative and postoperative complications. The mean visual analog scale score was significantly lower in the VATS group. In the light of the data of our study, we can conclude that VATS pneumonectomy is a safe and feasible procedure in selected patients.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Video-assisted thoracic surgery (VATS) has become the preferred method in most thoracic surgery procedures since it is associated with less postoperative pain, fewer complications, and shortened recovery time compared to conventional methods [1,2,3]. With the development of imaging technology and surgical instruments, VATS has become successfully applied even in extended lung resections [4,5,6]. Although there are many studies showing the superiority of VATS over a thoracotomy in lobar and sublobar resections, studies on pneumonectomy are limited.
Taking advantage of minimally invasive surgical techniques in pneumonectomy, which has higher postoperative mortality and morbidity compared to other types of lung resection, has the potential to improve postoperative outcomes in this patient group.
Thus, in this retrospective study, we aimed to demonstrate the effect of VATS on intraoperative and postoperative results by comparing it with thoracotomy in patients who underwent pneumonectomy for non-small lung cancer (NSCLC).
Material and Methods
Patients
This retrospective cohort study was approved by the local ethics committee.
We retrospectively analyzed patients with NSCLC who underwent pneumonectomy between January 2016 and May 2021. In our department, the first VATS lobectomy was performed in 2010 and the first VATS pneumonectomy in 2016. For this reason, we preferred to start the inclusion of patients from 2016.
Patients who underwent chest wall resection and carinal sleeve resection and diagnosed with carcinoid tumor were excluded from the study.
Preoperative pulmonary evaluation including spirometry, diffusing capacity for carbon monoxide (DLCO), and, if necessary, VO2max and cardiopulmonary exercise tests was performed for each patient. Flexible bronchoscopy was applied to each patient in the preoperative period. For preoperative mediastinal staging, a positron emission tomographic (PET) scan, endobronchial ultrasound (EBUS), and/or mediastinoscopy were performed according to the ESTS recommendations.
Surgical Technique
The two most important criteria in the selection of the surgical method were the size and location of the tumor. Although it is not a definite rule, thoracotomy was preferred more especially in tumors larger than 5 cm. Difficulty in retraction and manipulation of the lung, inadequate exposure, and difficulty in removing the specimen from the intercostal space after resection were the main factors that made the VATS method less preferred in large tumors. The second important criterion was tumor location. Central location and/or invasion of surrounding anatomical structures were the reason for choosing thoracotomy, especially in the early stages of the study period. However, with the increasing experience, VATS started to be preferred in locally advanced diseases like tumors with pericardium, diaphragm, or major vessel invasions. Therefore, VATS selection criteria are not firm and have changed over time with increasing experience. Another condition that necessitates the application of thoracotomy is the formation of air trapping due to central airway invasion-occlusion. In these cases, besides the difficulty of retraction and manipulation of the lung, it is also difficult to remove the specimen from the intercostal space.
Three ports were utilized in VATS group with non-rib-spreading technique. A 5–6-cm utility incision was placed at the 5th intercostal space (ICS) in the midaxillary line. A 1.5-cm camera port was placed in the anterior axillary line (at the 7th ICS) and a 1.5-cm posterior port was placed in the posterior axillary line at the same level of ICS. Thirty-degree thoracoscope was used in all cases. We routinely used ultrasonic or bipolar energy devices while performing hilar and mediastinal lymph node dissection.
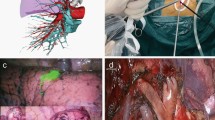
In VATS pneumonectomy, unless otherwise required, first the inferior and superior pulmonary vein, then the main pulmonary artery (Fig. 1a) and finally the bronchus were transected. In cases where there is main pulmonary artery invasion and excessive manipulation of the lung would create a risk of laceration of the artery, the pulmonary artery may also be dissected first. Dissection techniques of pulmonary veins are similar to VATS lobectomy. In right pneumonectomy, in order to safely dissect the main pulmonary artery and not leave a long stump, hilar lymph nodes should be dissected, and the artery should be isolated from the pulmonary vein inferiorly, the azygos vein superiorly, and the main bronchus posteriorly. In left pneumonectomy, especially the lymph nodes in the aorticopulmonary window should be removed and the tissues between the arcus aorta and the main pulmonary artery should be dissected. The staple size selected for the automatic stapler device should be appropriate for the width and wall thickness of the pulmonary artery. After transection of the vascular structures, all subcarinal lymph nodes were excised, and the main bronchus was isolated up to the carina level. After that, the main bronchus was suspended with a silicon sling (Fig. 1b). With this maneuver, it is possible to transect the main bronchus close to the carina. The endoscopic plastic bag was used while retrieving the specimen through the utility incision. In patients with large tumors, we used double endoscopic bags to prevent the bag from tearing.
a In this intraoperative image of the patient who underwent left pneumonectomy with VATS, all hilar structures were isolated, and the main pulmonary artery (white star) was gently retracted with vascular tape. The black arrow indicated the stump of the superior pulmonary vein located anterior to the main bronchus (black star). b The left main bronchus (black star) was isolated and retracted with tape to leave a short stump
We preferred open thoracotomy in cases with a requirement for chest wall or carina resection and presence of difficulty with securing a surgical margin at the main bronchus. The possible need for bronchial sleeve resection did not cause us to choose an open thoracotomy. We successfully performed complete-VATS bronchial sleeve lobectomy in 8 patients during the study period.
In the thoracotomy group, pneumonectomy was performed through the muscle-sparing lateral thoracotomy using a 15- to 20-cm lateral skin incision. The 5th or 6th ICS was used. The vascular structures were ligated and transfixed with non-absorbable sutures (mostly 2–0 or 1–0 silk). The main bronchus was transected and closed with a surgical stapling device. We chose to cut open the bronchus when the tumor was close to the surgical margin.
In cases at high risk for developing bronchopleural fistula, pericardial fat was used to reinforce the bronchial stump (Fig. 2). We routinely inserted a medium-bore clamp-release chest tube to stabilize the mediastinum for 2–3 days and removed it after bleeding and chylothorax are ruled out. Mediastinal balancing was performed by unclamping the chest tube twice a day, and it was terminated when the daily drainage amount fell below 200–300 cc.
Postoperative Follow-up
We have preferred to keep the patients in the intensive care unit (ICU) for the first 24 h after the operation.
Visual analog pain scale (VAPS) scores were recorded every 12 h after surgery and continued 3 days. The multimodal treatment includes local anesthetics, non-steroid anti-inflammatory drugs, opioids, and drugs to provide intercostal nerve blocks to manage postoperative pain. After the chest tube removal, patients who were in stable condition and enabled self-maintenance of normal daily activities were discharged.
Data on intraoperative and postoperative outcomes including length of operation, length of hospital stay, drainage duration, complications, and follow-up information were obtained.
Statistic
Statistical analysis was performed using SPSS 25.0 (SPSS Inc., Chicago, IL, USA).
Continuous variables, expressed as mean value ± standard deviation (SD), were compared by unpaired Student’s t-tests; categorical variables were analyzed using Chi-square tests. DFS and OS were estimated using the Kaplan–Meier method. Cox regression analyses were performed to define factors that would affect disease-free and overall survival. Statistical significance was set at p-value < 0.05 (all p values presented were 2-sided).
Results
A total of 115 males and 20 females were included in the study. Complete VATS pneumonectomy was performed in 20 patients, and conventional pneumonectomy was performed in 135 patients. Conversion to open thoracotomy was seen in 1 patient because of a calcified hilar lymph node. Patients’ characteristics are listed in Table 1.
We used thoracoscopy for exploration in some patients to see the degree of mediastinal invasion or to determine whether it would require chest wall resection. We did not consider such cases that started with VATS for exploration and continued with thoracotomy as “conversion to thoracotomy.”
The most common pneumonectomy indication was the presence of centrally located tumor, and no significant difference was found between VATS and thoracotomy in terms of indication rates (Table 2).
There were no statistically significant differences between VATS and thoracotomy groups in mean ages (64.2 vs. 61.7, p = 0.25), preoperative FEV1, comorbidities, operation side, tumor size, and pathological stages.
Postoperative drainage time (3.3 vs. 3.9, p = 0.38) and hospital stay (5.0 vs. 6.1, p = 0.25) were slightly longer in thoracotomy group; however, these differences were not statistically significant.
There was no statistically significant difference between VATS and thoracotomy groups in terms of intraoperative and postoperative complications. As an intraoperative complication, vascular injury was observed during hilar dissection in two patients, and tracheal injury was thought to be secondary to intubation in one patient.
The most common postoperative complication was pneumonia in both groups. A total of 9 (%6.6) patients underwent re-operation due to postoperative bleeding.
In postoperative follow-up, mean VAPS score was found to be significantly higher in POD 1, 2, and 3 in the thoracotomy group (Table 3).
Intraoperative death was not observed in either group. However, there were 6 patients in total who developed mortality within 30 days postoperatively. There was no statistically significant difference in postoperative 30-day mortality between VATS and thoracotomy groups (1 (%5) vs. 5 (%4.3); p = 1.00).
Overall survival was 39.3 SD2.9 months, and disease-free survival was 35.7 SD2.9 months (Fig. 3). Overall and recurrence-free survival was found longer in the VATS group, but this result is not statistically significant (Table 4).
Discussion
With increasing experience and the development of minimally invasive surgical instruments, VATS has become available in many lung pathologies that were previously considered contraindicated. It has been shown that it can be successfully applied in locally advanced lung cancer cases such as chest wall, diaphragm, and pericardial invasion [7,8,9,10,11]. However, VATS pneumonectomy is still an uncommon procedure and there are several concerns about its feasibility.
One of these concerns is the suspicious in safety and feasibility of hilar dissection in VATS pneumonectomy, especially in centrally located large tumors [12, 13]. This concern is not unfounded because in some cases, safe manipulation of the lung can be difficult due to the size of the tumor and its proximity to hilar structures. However, modern surgical graspers, bipolar or ultrasonic energy devices, and advances in optics, including 3D cameras and ultra-high-definition monitors, make adequate exploration and safe hilar dissection possible.
Another point of discussion is the adequacy of VATS in evaluating resectability or suitability for parenchyma-sparing surgery in patients who are radiological candidates for pneumonectomy. The decision to perform pneumonectomy or sleeve lobectomy is not only based on the preoperative investigation but also intraoperative exploration. Incomplete exploration of the relationship between the hilar structures and the tumor may cause unnecessary pneumonectomies. Therefore, all cases with the possibility of pneumonectomy should be evaluated adequately in terms of suitability for sleeve lobectomy and, if necessary, open thoracotomy should be applied. We think that VATS has sufficient reliability to carry out this exploration. In our clinic, 8 patients with a radiological possibility of pneumonectomy were started with VATS and according to the exploration findings, videothoracoscopic bronchial sleeve lobectomy was performed after being evaluated as suitable for sleeve resection [14].
Previous articles on VATS pneumonectomy have provided encouraging results. Sahai and colleagues [15] reported retrospective analyses of 67 patients and demonstrated similar postoperative outcomes between thoracoscopic and open thoracotomy. Similarly, Nagai and colleagues [16] analyzed 47 patients who underwent VATS pneumonectomy and reported 17.4% major postoperative complication and 2.2% mortality, and they emphasized that these results were better when compared with the thoracotomy data in the literature.
As stated in the few similar studies in the literature, there is a risk of bias in patient selection for VATS pneumonectomy [13, 15, 16]. In this study, there was no significant difference between VATS and thoracotomy groups in terms of patient characteristics. However, the mean tumor size in the thoracotomy group was statistically significantly higher than in the VATS group (p = 0.019). This is the result of the tendency to choose thoracotomy rather than VATS in large tumors due to possible difficulty in removing the specimen from the thorax.
One of the most important findings in our study was the positive effect of VATS on postoperative patient comfort. The mean VAS scores for the first 3 days of the postoperative period were lower in the VATS group. The importance of postoperative pain control in preventing complications associated with thoracic surgery procedures is well known [17]. Although less postoperative pain was observed in the VATS group, there was no significant difference between VATS and thoracotomy groups in terms of postoperative complication rates.
We preferred to follow patients who were to stay in a remote area from the hospital up to the hospital for a few more days after chest tubes were removed. Therefore, although the mean drainage times were shorter in the VATS group, no significant difference was found between the thoracotomy group in terms of hospitalization times (p = 0.179).
Whichever technique is used, the main goal is to ensure R0 resection and not to compromise oncological principles in the treatment of lung cancer. When we evaluate the oncological results of the patients we included in the study, the overall and disease-free survival results were slightly longer in the VATS group, but there was no statistical significance. Achieving a clean surgical margin is one of the concerns about VATS pneumonectomy. However, we were able to provide a negative surgical margin by opening the pericardium when necessary, and we believe that VATS do not have any disadvantages in this regard.
This study has various limitations. First, this is a retrospective study; therefore, biases might exist in the design. Secondly, VATS group consists of a small number of patients, and this may directly affect the statistical significance. Third, VATS pneumonectomy has been performed in a selected group of patients, and selection criteria have changed over time with the increasing experience of the surgical team.
In the light of the data of our study, we can conclude that VATS pneumonectomy is safe and feasible procedure in selected patients. Eligible patients should be able to benefit from the advantages of VATS technique such as less postoperative pain and shorter drainage and hospitalization times. As mentioned in the “Material and Methods” section, there were no strict patient selection criteria, and with the increasing experience of the surgical team, the indications have expanded over time and will continue to expand.
References
McKenna RJ Jr, Houck W, Fuller CB (2006) Video-assisted thoracic surgery lobectomy: experience with 1,100 cases. Ann Thorac Surg 81:421–5 (discussion 425-6)
Onaitis MW, Petersen RP, Balderson SS et al (2006) Thoracoscopic lobectomy is a safe and versatile procedure: experience with 500 consecutive patients. Ann Surg 244:420–425
Flores RM, Park BJ, Dycoco J et al (2009) Lobectomy by video-assisted thoracic surgery (VATS) versus thoracotomy for lung cancer. J Thorac Cardiovasc Surg 138:11–18
Hennon MW, Demmy TL (2012) Video-assisted thoracoscopic surgery (VATS) for locally advanced lung cancer. Ann Cardiothorac Surg 1(1):37–42
Petersen RP, Pham D, Burfeind WR et al (2007) Thoracoscopic lobectomy facilitates the delivery of chemotherapy after resection for lung cancer. Ann Thorac Surg 83(4):1245–1249
Hennon M, Sahai RK, Yendamuri S et al (2011) Nwogu C. Safety of thoracoscopic lobectomy in locally advanced lung cancer. Ann Surg Oncol. 18(13):3732–6
Demmy TL, Nwogu CE, Yendamuri S (2010) Thoracoscopic chest wall resection: what is its role? Ann Thorac Surg 89:S2142–S2145
Mineo TC, Ambrogi V, Pompeo E et al (1996) En bloc minimal laser resection for T3-chest wall lung cancer in patients with poor pulmonary function. Chest 110(4):1092–1096
Santambrogio L, Cioffi U, De Simone M et al (2002) Video-assisted sleeve lobectomy for mucoepidermoid carcinoma of the left lower lobar bronchus: a case report. Chest 121:635–636
Nakanishi R, Fujino Y, Yamashita T et al (2014) Thoracoscopic anatomic pulmonary resection for locally advanced non-small cell lung cancer. Ann Thorac Surg 97(3):980–985
Gonfiotti A, Bongiolatti S, Bertolaccini L et al (2017) Italian VATS Group. Thoracoscopic lobectomy for locally advanced-stage non-small cell lung cancer is a feasible and safe approach: analysis from multi-institutional national database. J Vis Surg. 3:160
Conlan AA, Sandor A (2003) Total thoracoscopic pneumonectomy: indications and technical considerations. J Thorac Cardiovasc Surg 126:2083–2085
Nwogu CE, Glinianski M, Demmy TL (2006) Minimally invasive pneumonectomy. Ann Thorac Surg 82:e3-4
Ceylan KC, Acar A, Örs KŞ (2020) The initial experience on thoracoscopic sleeve lobectomy: continuous suturing technique of the bronchial anastomosis in 12 cases. Surg Laparosc Endosc Percutan Tech 30(5):476–479
Sahai RK, Nwogu CE, Yendamuri S et al (2009) Is thoracoscopic pneumonectomy safe? Ann Thorac Surg 88(4):1086–1092
Nagai S, Imanishi N, Matsuoka T et al (2014) Video-assisted thoracoscopic pneumonectomy: retrospective outcome analysis of 47 consecutive patients. Ann Thorac Surg 97(6):1908–1913
Yegin A, Erdogan A, Kayacan N et al (2003) Early postoperative pain management after thoracic surgery; pre- and postoperative versus postoperative epidural analgesia: a randomised study. Eur J Cardiothorac Surg 24(3):420–424
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
This retrospective cohort study was approved by the local ethics committee and informed consent was obtained from all individual participants included in the study (Registration number: 49109414–604.02; Date: 24/01/2020).
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ceylan, K.C., Batıhan, G. & Kaya, Ş.Ö. Three Ports One Lung: Videothoracoscopic Pneumonectomy for Lung Cancer. Indian J Surg 85 (Suppl 2), 452–458 (2023). https://doi.org/10.1007/s12262-022-03567-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12262-022-03567-1