Abstract
Background
Peak oxygen uptake (VO2) testing is commonly used to assess chronic heart failure (CHF) patients’ exercise tolerance. The test requires maximal effort; however, many participants have low confidence (self-efficacy) to perform optimally.
Purpose
This randomized controlled trial examined the effectiveness of a modeling intervention to increase Peak VO2 (PVO2) and self-efficacy in people diagnosed with CHF.
Methods
Twenty participants with a diagnosis of CHF were randomized to either an intervention (modeling DVD) or a control group. Both groups completed a measure of self-efficacy prior to performing two PVO2 tests, each separated by 7 days. After completing the first test (T1) the intervention group watched a 10-min coping model DVD. All participants returned 1 week later (T2) to complete identical study procedures.
Results
Analysis of covariance results showed that compared with the participants in the control group, those assigned to the modeling intervention had higher PVO2 at T2, F (1, 19) = 4.38, p = 0.05, ή 2 = 0.21 and self-efficacy, F (1, 19) = 5.80, p < 0.05, ή 2 = 0.25. Only partial support was found for change in self-efficacy mediating treatment outcome (PVO2).
Conclusions
Watching a modeling video is associated with increased PVO2 and self-efficacy. These results have implications for testing patients in a clinical setting to maximize exercise tolerance test results.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Chronic heart failure (CHF) is a progressive disorder of left ventricular remodeling resulting in impaired cardiac pump function and is associated with decreased exercise tolerance, increased hospital admissions, reduced quality of life, and high mortality [1–3]. The etiology of CHF is varied, including acute myocardial infarction, acute inflammation, valvular heart disease, and idiopathic [3].
Peak oxygen uptake (PVO2) is defined as the oxygen consumption at peak exercise and provides reliable information of exercise tolerance and prognosis in individuals with CHF [4, 5]. PVO2 has been shown to be related to measured functional performance (6-min walk test and questionnaires as well as health-related quality of life [6].
Exercise testing combined with assessment of gaseous exchange parameters is used to assess PVO2. Maximal effort is required as individuals must exceed their anaerobic threshold since PVO2 does not correlate with hemodynamic factors during rest [5]. Despite this, adequate data may not be recorded because individuals are apprehensive, unfamiliar with the procedures, and anxious about producing symptoms, which results in them not reaching their anaerobic threshold [5].
Self-efficacy is an important psychosocial determinant of exercise behavior in both clinical and nonclinical populations [7–10] and refers to an individual’s beliefs in his/her capabilities to execute the necessary courses of action to satisfy situational demands [11]. Self-efficacy is theorized to influence the activities that individuals choose to approach, the effort expended on such activities, and the degree of persistence demonstrated in the face of adverse stimuli [11, 12].
An important source of self-efficacy is modeling or observational learning [13], which typically involves watching others perform a task or behavior. Modeling has been shown to be a powerful instructional tool for acquiring motor skills, altering psychological responses, and changing behavior in both physical activity [14] and injury rehabilitation [15] contexts. Despite this evidence, modeling as an intervention has received limited attention in the realm of cardiac exercise testing. To the best of our knowledge, there are no randomized controlled trials (RCT) evaluating the effectiveness of a modeling intervention to increase PVO2 and self-efficacy and in people with CHF. The primary purpose of this study was to examine the effect of a modeling intervention (DVD) on Peak VO2 and self-efficacious expectations in people with CHF during a maximal treadmill test. A second purpose was to investigate whether self-efficacy served to mediate relations between the modeling intervention and PVO2. Most RCT intervention studies do not measure mediating variables, and priority should be placed on research that enhances our understanding of the underlying mechanisms for why our interventions work [16, 17].
Materials and Methods
Participants Recruitment and Demographics
Adults living in Auckland, New Zealand were eligible if they were aged between 18 and 65 years, able to give written informed consent, clinically documented and stable, New York Heart Association (NYHA) class II or III heart failure, and were able to communicate in English. Potential participants were excluded if they were admitted to hospital within the previous 6 weeks, had a cardiac transplant expected in the next 6 months, had a surgical remediable cause of heart failure, had a fixed rate pace maker, were not able to provide informed consent, had terminal cancer, were participating in any other clinical trials, or had exercise limitations other than heart failure (i.e., osteoarthritis).
Twenty-two participants (78% male) diagnosed with CHF (mean age = 64.77 years ± 13.04) were recruited from a Metropolitan Hospital in the Auckland region of New Zealand (NZ). One participant died from unrelated causes and one was unable to continue in the study due to their condition worsening, resulting in 20 participants providing complete data. Combination therapy (nitrates, diuretics, and, beta-blockers) was used in all patients.
Measures
Peak VO2
A standardized exercise testing (ramp) protocol was implemented to assess Peak VO2 [5]. All testing was in accordance with American College of Sports Medicine [18] guidelines for exercise testing in patients with heart failure. Peak VO2 was expressed in absolute (l/min) and relative (ml/kg/min) units with the latter unit used for subsequent analysis.
Self-Efficacy
Self-efficacy
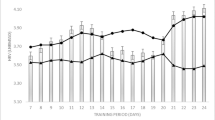
was assessed using a scale adapted from the Self-Efficacy Scale [19]. Participants rated their confidence to walk during a Peak VO2 test for increasing periods of time (i.e., 2, 4, 6, 8, 10, and 12 min) at three intensities (i.e., easy, moderate, and hard). A key was provided to define the various intensity levels. An example of one of the statements used was “I believe that I can walk for 2 minutes at an easy pace without stopping”. Mean scores were calculated with higher values indicating greater efficacy to walk for longer duration and greater intensity. Cronbach’s alpha was acceptable at both time points (T1 α = 0.95 and T2 α = 0.96).
Intervention
A behavioral modeling DVD (10 min duration) was developed by the first two authors detailing model’s responses before, during, and after the PVO2 test. The DVD consisted of edited interviews and various action shots of CHF patient models (two males and two females) performing a PVO2 test. Models demonstrated and verbalized increased confidence to perform the test and offered a variety of strategies to cope with the maximal effort and overcome the associated discomfort during the test (e.g., shortness of breath, sweating, increased heart rate). Emphasis was placed on strategies the models used (i.e., attention control, breathing regulation, goals, cue words) to focus their efforts during subsequent tests.
Interspersed with the role model presentation were vignettes with a cardiologist, which outlined the purpose of a PVO2 test, the importance of the diagnostic information, and the need for people to push themselves to their maximum. Information was also provided regarding procedural safety and the body’s responses to exercise. Conveying this type of information represents standard practice for cardiologists in preparing heart failure patients for this test and participants in the control condition received this content verbally.
Study Design and Procedure
A randomized controlled trial was conducted with participants assigned to either an intervention group (modeling DVD; n = 10) or a control group (no DVD; n = 10) via a central computer randomization service. The study protocol and related documents were approved by the Northern Regional Ethics Committee. Each participant attended two 1 h sessions at the hospital for PVO2 tests 1 week apart (T1 and T2). Prior to the first test (T1), a trained research assistant provided a verbal and written explanation of the study and obtained informed consent. Participants completed a demographic (see Tables 1 and 2) and the self-efficacy measure. Exercise testing was preformed on a treadmill (Sensormedics 2000 series) using a standardized ramp protocol. Although all participants had experience of treadmill cardiac stress testing, a familiarization period of 15 min was used, which also served to provide participant’s walking speed.
A qualified cardiopulmonary medical technician fitted each participant with a four lead EKG (GE, Cardiosoft, Germany), pulse-oximeter, and an oxygen flow sensing mouthpiece (Sensormedics, Vmax 22 Series). The flow sensor was calibrated twice with the following gas percentages: calibration 1—26% O2 in nitrogen and calibration 2—4% carbon dioxide and 16% O2 in nitrogen.
Participants sat for 5 min while baseline rest measurements were recorded (i.e., heart rate, O2 saturation, O2 consumption, and heart rate). Once completed, participants began walking at their ‘brisk walking pace’. Consistent with the ramp protocol, the incline of the treadmill was increased by 2% after each minute, and the test continued until patients either reached volitional fatigue or PVO2 was achieved. Care was taken to ensure that patients exceeded their anaerobic threshold so PVO2 could be established; therefore, the respiratory exchange ratio (RER) had to exceed 1.0 to indicate adequate effort. On completion of the test, participants indicated their reason for stopping and were asked to rate their perceived exertion on a scale from 0–10 [20]. Heart rate and EKG were recorded continuously and gas-exchange variables were recorded using breath by breath analysis. No participants completed the full ramp protocol (duration 13 minutes) at T1 due to either shortness of breath or muscle fatigue, while four completed the protocol at T2.
Following the test, those in the intervention group watched the modeling DVD (intervention) and were given a brochure that summarized the key points of the DVD. Participants were then asked to set and record a goal to achieve for the following test. Goals were specific to the test (i.e., time on the treadmill, PVO2). All participants returned 1 week later (T2) and underwent identical procedures. Prior to the second exercise test, the intervention group was asked to recall the information (i.e., use of strategies proposed by the model) from the DVD and their specific goals. The self-efficacy measure was administered at this time. The control group followed identical procedures but did not watch the DVD, receive the brochure, or set goals. All participants were asked not to change their normal physical activity patterns during the week.
Power Calculation
With respect to PVO2, it was anticipated that a difference of at least 1.5 ml.kg.min−1 (standard deviation (SD) = 1.0 ml.kg.min−1) would be demonstrated between those in the intervention and control [4, 21]. It was calculated that approximately seven participants in each condition (modeling vs. control) would be needed to provide power of 80% (alpha = 0.05) and to detect a large effect size (0.40) [22].
Results
Treatment of the Data
To address the main hypothesis, a one-way (intervention vs. control) analysis of covariance (ANCOVA) was performed on PVO2 and self-efficacy. Preintervention (T1) PVO2 and self-efficacy served as covariates to remove the variance in respective postintervention scores thereby increasing the power and sensitivity of the F test [23]. Prior to conducting these analyses, the assumptions underlying the use of ANCOVA were tested and satisfied [24]. The alpha level for the ANCOVA analyses was 0.05, with effect sizes reported (eta-square ή 2).
Peak Oxygen Uptake
Descriptive data are presented in Table 3. Baseline imbalance existed for relative PVO2, F (1, 18) = 5.58; p = 0.03, but not for absolute PVO2, F (1, 18) = 3.09; p = 0.09. ANCOVA results showed significant differences in PVO2 (ml.kg.min−1) at T2, F (1, 19) = 4.38, p = 0.05, ή 2 = 0.21. Specifically, PVO2 values were higher for the intervention group (adjusted mean = 22.46) compared to the control group (adjusted mean = 19.95). The intervention group improved (from T1 to T2) PVO2 by 6.3% compared to the control who decreased by 1.3%.
Self-Efficacy
Descriptive data are presented in Table 3. Results revealed significant differences in self-efficacy scores at T2, F (1, 19) = 5.80, p < 0.05, ή 2 = 0.25. Adjusted mean values show the intervention group had higher self-efficacy scores (67.74) compared to the control group (48.96). The intervention group improved self-efficacy (from T1 to T2) by 28.6% compared to the control group which improved by 1.5%.
Test for Mediation
In accordance with the recommendations of Kraemer et al. [17] for testing mediators of treatment effects in randomized clinical trials, a hierarchical regression was conducted with posttreatment (T2) PVO2 serving as the criterion measure. According to Kraemer et al., a mediator would have to “measure an event or change occurring during treatment, and then, it must correlate with treatment choice, hence possibly be a result of treatment, and have either a main or interactive effect on the outcome” (p. 879). This approach differs from that proposed by Baron and Kenny [25] who suggested a mediator directly influences the outcome (main effect only). More important, directionality determines whether a variable is a mediator or moderator of treatment; mediation must occur during treatment. This approach to assessing mediation has particular relevance to the randomized controlled trial and was the rationale for adopting Kraemer et al.’s recommendations.
It was hypothesized that the intervention would increase PVO2 and result in an increase in self-efficacy (change). Change in self-efficacy would be the mechanism for the interventions effect (mediation). Variables were entered in the following order: step 1—intervention (condition), step 2—change in self-efficacy (T1 to T2), step 3—the interaction term, intervention × change in self-efficacy. Support for mediation is found when the mediator and/or interaction term can explain significant amounts of additional treatment outcome variance (step 2 and/or 3). Results showed that the intervention significantly predicted (R 2 = 0.34) posttreatment PVO2 at step 1, F(1,18) = 9.35, p = 0.007. Results at step 2 showed that self-efficacy change increased the R 2 by 10%, F(1,17) = 3.04, p = 0.10. When the interaction term was added (step 3), the change in R 2 increased by a further 10%, F(1,16) = 3.60, p = 0.07.
Discussion
This randomized controlled trial evaluated the effectiveness of a modeling intervention on PVO2 and self-efficacy in CHF patients. Compared with participants in the control group, those assigned to the modeling (DVD) intervention had higher PVO2 and self-efficacy scores. Results also showed that a modeling intervention was effective in increasing both PVO2 and self-efficacious beliefs. Physiologically, one would not expect to find difference in PVO2 over a period of 1 week. Our findings showed that the intervention group increased their PVO2 by 6.3% while the control group decreased their PVO2 by 1.3%. It is plausible that measurement error exists with VO2 testing; however, one would expect this to be similar for both groups; therefore, these results suggest that the CHF patients did not achieve their true PVO2 after the first test, and opportunity exists to maximize these outputs through intervention.
Baseline imbalances did exist between both groups for relative PVO2 (ml/kg/min) but not for absolute PVO2 (l/min). Because participants were randomized to the respective treatment groups, these differences can be considered random. In small studies especially, randomization may not yield entirely comparable groups and differences in one or more variables may exist [26]. Identified imbalances, however, do not invalidate these findings as any imbalance can be controlled for using appropriate adjusted analysis. In this case, an ANCOVA was used to adjust for baseline imbalance. Adjustment reduces the variance in the test statistic and because the covariates were highly correlated (r = 0.95) with the outcome, this produces a more sensitive analysis [26].
Changes in PVO2 are also clinically significant. In a situation in which one compares the clinical consequences experienced by two patients (as with an RCT), the effect size called area under the Receiver Operating Curve (AUC) can be used. AUC is the probability that the T patient has a treatment outcome preferable to the C patient [27]. Based on the adjusted mean values of PVO2, a Cohen’s d effect size of 0.5 was calculated and is equivalent to an AUC of 0.638. Because the AUC ranges from 0–1, a value of 0.638 indicates that those exposed to a modeling DVD were more likely to have an outcome better than those who did not. In short, adequate preparation of participants before treadmill testing using this and similar interventions has the potential to ensure individuals provide a true indication of their PVO2.
The modeling intervention was associated with a 28.6% increase in self-efficacy for the treatment group suggesting that in this population, modeled attainment is a powerful source of self-efficacious beliefs. Social cognitive theory posits that previous mastery experience is the most powerful source of self-efficacy [13]; however, in this study, self-efficacy scores increased modestly (1.5%) from T1 to T2 in the control group suggesting that previous mastery experiences may not be sufficient to provide the resources required to augment efforts during subsequent maximal testing. These findings suggest that standard pretest education and familiarization procedures may be inadequate to impart the confidence required to perform a maximal effort in CHF patients, resulting in an unsatisfactory test result. Indeed, additional information such as provided in the DVD may be required to provide individuals with specific coping strategies to deal with the discomfort and symptoms experienced during a maximal effort.
A second aim of this study was to examine whether self-efficacy served to mediate relations between the intervention and PVO2. Following Kraemer et al.’s recommendations [17] for testing mediators in randomized clinical trials, the conditions for mediation were partially met. Although change in self-efficacy and the interaction term both contributed 10% of additional variance in postintervention PVO2, respectively, these incremental amounts of variance were statistically nonsignificant. The interaction term (step 3) did approach statistical significance (p = 0.07) and was suggestive of mediation. This result is most likely a function of insufficient power (i.e., small sample) rather than self-efficacy being a poor mediator. Overall, these findings suggest that increasing participant’s self-efficacious beliefs to walk for longer periods of time at a greater intensity is likely to result in a maximal effort, thereby reflecting true PVO2. Mediator effects should be considered in evaluating future trials, and formal tests should be conducted on the premise that the treatment effect would be increased by appropriate manipulation of this mediator [17].
This study is not without limitations. The most notable is the small sample size which included patients with a NYHA functional class of II or III and stable heart failure, and, therefore, these results can not be generalized to other grades of heart failure or to other cardiac conditions. Participants in the control condition were not exposed to the goal setting intervention, which may suggest that this component of the intervention resulted in the change in PVO2, rather than role modeling. Although this effect cannot be ruled out, it is unlikely given the brief nature of this component. Future studies may choose to examine the separate components of the intervention. These findings nevertheless build on a growing body of evidence supporting the effectiveness of modeling as an intervention in rehabilitation [15, 28]. While our own modeling work continues in the area of smoking cessation, investigation of this type of intervention with other clinical populations (i.e., pulmonary disease, stroke, and diabetes) would be valuable.
In conclusion, watching a modeling video is associated with increased PVO2 and self-efficacy. Only partial support was found for change in self-efficacy mediating treatment outcome (PVO2). These results have implications for testing patients in a clinical setting to maximize exercise tolerance test results.
References
Pina IL, Apstein CS, Balady GJ, et al. Exercise and heart failure. Circulation. 2003; 107: 1210–1225.
Quittan M, Sturm B, Wiesinger GF, et al. Quality of life in patients with chronic heart failure: A randomized controlled trial of changes induced by a regular exercise program. Scand J Rehabil Med. 1999; 31: 223–228.
Francis GS. Pathophysiology of chronic heart failure. Am J Med. 2001; 110: 37S–46S.
Belardinelli R, Georgiou D, Cianci G, Purcaro A. Randomized, controlled trial of long-term moderate exercise training in chronic heart failure: Effects on functional capacity, quality of life, and clinical outcome. Circulation. 1999; 99: 1173–1182.
Lainchbury JG, Richards AM. Exercise testing in the assessment of chronic congestive heart failure. Heart. 2002; 88: 538–543.
Myers J, Zaheer N, Quaglietti S, et al. Association of functional and health status measures in heart failure. J Card Fail. 2006; 12: 439–445.
McAuley E, Blissmer B. Self-efficacy determinants and consequences of physical activity. Exerc Sport Sci Rev. 2000; 28: 85–88.
McAuley E, Courneya KS. Adherence to exercise and physical activity as health promoting behaviors: Attitudinal and self-efficacy influences. Appl Prev Psychol. 1993; 2: 65–77.
Parent N, Fontin F. A randomized, controlled trial of vicarious experience through peer support for male first-time cardiac surgery patients: Impacts on anxiety, self-efficacy expectation and self-reported activity. Heart Lung. 2000; 29: 389–400.
Maddison R, Prapavessis H. Using self-efficacy and intention to predict exercise compliance among patients with ischemic heart disease. J Sport Exerc Psychol. 2004; 26: 511–524.
Bandura A. Social foundations of thought and action. New York, NY: Prentice-Hall; 1986.
McAuley E, Courneya KS, Rudolph DL, Lox CL. Enhancing exercise adherence in middle-aged males and females. Prev Med. 1994; 23: 498–506.
Bandura A. Self-efficacy: The exercise of control. New York, NY: Freeman; 1997.
McCullagh P, Weiss MR. Observational learning: The forgotten psychological method in sport psychology. In: Van Raalte JL, Brewer BW, eds. Exploring sport and exercise psychology. 2nd ed. Washington DC: American Psychological Association; 2002: 131–149.
Maddison R, Prapavessis H, Clatworthy M. Modeling and rehabilitation following anterior cruciate ligament reconstruction. Ann Behav Med. 2006; 31: 89–98.
Baranowski T, Anderson C, Carmack C. Mediating variable framework in physical activity interventions. How are we doing? How might we do better? Am J Prev Med. 1998; 15: 266–297.
Kraemer HC, Wilson T, Fairburn CG, Agras WS. Mediators and moderators of treatment effects in randomized clinical trials. Arch Gen Psychiatry. 2002; 59: 877–883.
American College of Sports Medicine. ACSM’s guidelines for exercise testing and prescription. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2000.
McAuley E, Mihalko SL. Measuring exercise related self-efficacy. In: Duda JL, ed. Advances in sport and exercise psychology. Morgantown, WV: Fitness Information Technology; 1998: 371–389.
Borg G. Psychophysical bases of perceived exertion. Med Sci Sports Exerc. 1982; 5: 377–381.
Gottlieb SS, Fisher ML, Freudenberger R, et al. Effects of exercise training on peak performance and quality of life in congestive heart failure patients. J Card Fail. 1999; 5: 188–194.
Cohen J. Statistical power analysis for the behavioral sciences. Hillsdale, New Jersey: Erlbaum; 1988.
Stevens J. Applied multivariate statistics for the social sciences. 3rd ed. Mathway, NJ: Erlbaum; 1996.
Tabachnick BG, Fidell LS. Using multivariate statistics. 4th ed. New York, NY: Harper & Collins; 2001.
Baron RM, Kenny DA. The moderator–mediator variable distinction in social psychological research: Conceptual, strategic and statistical considerations. J Pers Soc Psychol. 1986; 51: 1173–1182.
Friedman LM, Furberg CD, DeMets DL. Fundamentals of clinical trials. 3rd ed. New York, NY: Springer; 1998.
Kraemer HC, Kupfer DJ. Size of treatment effects and their importance to clinical research and practice. Biol Psychiatry. 2005; 59: 990–996.
Flint FA. The psychological effects of modeling in athletic injury rehabilitation [doctoral dissertation]. University of Oregon, 1991.
Author information
Authors and Affiliations
Corresponding author
Additional information
Dr. Maddison is a senior research fellow at the Clinical Trials Research Unit and is supported by a National Heart Foundation of New Zealand Research Fellowship.
About this article
Cite this article
Maddison, R., Prapavessis, H., Armstrong, G.P. et al. A Modeling Intervention in Heart Failure. ann. behav. med. 36, 64–69 (2008). https://doi.org/10.1007/s12160-008-9050-y
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12160-008-9050-y