Abstract
As a 2-year project of the Japanese Society of Nuclear Medicine working group activity, normal myocardial imaging databases were accumulated and summarized. Stress-rest with gated and non-gated image sets were accumulated for myocardial perfusion imaging and could be used for perfusion defect scoring and normal left ventricular (LV) function analysis. For single-photon emission computed tomography (SPECT) with multi-focal collimator design, databases of supine and prone positions and computed tomography (CT)-based attenuation correction were created. The CT-based correction provided similar perfusion patterns between genders. In phase analysis of gated myocardial perfusion SPECT, a new approach for analyzing dyssynchrony, normal ranges of parameters for phase bandwidth, standard deviation and entropy were determined in four software programs. Although the results were not interchangeable, dependency on gender, ejection fraction and volumes were common characteristics of these parameters. Standardization of 123I-MIBG sympathetic imaging was performed regarding heart-to-mediastinum ratio (HMR) using a calibration phantom method. The HMRs from any collimator types could be converted to the value with medium-energy comparable collimators. Appropriate quantification based on common normal databases and standard technology could play a pivotal role for clinical practice and researches.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
In nuclear cardiology, providing reliable results is a basis for clinical practice and research. Since nuclear cardiology has been based on functional imaging, a number of parameters have been calculated based on myocardial perfusion imaging (MPI), metabolism and sympathetic imaging [1]. While normal values are important from a physiological viewpoint, the values are influenced by methodologies used for measurements of specific cardiac parameters. Taking left ventricular (LV) ejection fraction (EF) as an example, differences in the quantitative value exist among echocardiography, left ventriculography with contrast media, magnetic resonance imaging and X-ray computed tomography (CT), and some differences have been noticed even with nuclear imaging, including gated blood-pool study and gated MPI using single-photon emission computed tomography (SPECT) [2, 3]. The results also vary depending on the software used for analysis, in which Quantitative Gated SPECT/Quantitative Perfusion SPECT (QGS/QPS, Cedars Sinai Medical Center, Los Angeles, CA, USA), Emory Cardiac Toolbox (ECTb, Emory University/Syntermed Inc., Atlanta, GA, USA), and 4DM-SPECT/Corridor 4DM (Michigan University/INVIA, LLC, Ann Arbor, MI) are included [4–7]. In Japan, two software programs of Heart Function View/Heart Score View (HFV/HSV, Nihon Medi-Physics Co. Ltd., Tokyo, Japan) [8, 9] and cardioREPO (FUJIFILM RI Pharma, Co. Ltd., Tokyo, Japan/EXINI Diagnostics, Lund, Sweden) have also been developed [10]. When we overview a variety of software programs, the threshold of LVEF is critical not only for differentiation of normal versus abnormal LV function, but also for prognostic purposes [11–13], since a large number of patients could be included in the borderline range from 50 to 60%.
JSNM working group activities in 2007 and 2015
Both normal values and tracer distributions are important in myocardial SPECT imaging. Patient-related factors, such as sex and body habitus, may influence tracer distribution. In addition, various technical factors may also be of concern such as SPECT equipment, rotation range of camera heads, collimator types, scatter and attenuation corrections and crystal types, namely sodium iodide (NaI) or cadmium zinc telluride (CZT) [2].
The Japanese Society of Nuclear Medicine (JSNM) working group created SPECT databases for myocardial perfusion imaging, fatty acid and sympathetic imaging, and have provided normal files fitted for various software programs (JSNM working group database 2007) [14–16]. The normal MPI studies were defined as subjects with low likelihood of cardiac diseases with no evidences of the following conditions: underlying known cardiac diseases, electrocardiographic (ECG) evidence of ischemia or infarction, wall motion abnormality, arrhythmia inappropriate for gating and those with medications for hypertension and diabetes. Both patients who had normal coronary angiography and those who were not indicated for coronary angiography because of a low possibility of coronary artery disease were included. The MPI studies were performed with a standard dose of 99mTc-methoxyisobutylisonitrile (MIBI)/tetrofosmin (555-1110MBq) and 201Tl (74-111MBq).
In the working group database 2007, the databases were separately created for rotation range (180/360°), gender, stress and rest, and radiopharmaceutical types including 99mTc-MIBI/tetrofosmin, 201Tl, 123I-beta-methyliodophenylpentadecanoic acid (BMIPP) and 123I-meta-iodobenzylguanidine (MIBG) (Table 1). The collimator difference was only taken into considerations for planar 123I-MIBG imaging. As a result of the working group activity, normal databases applicable to conventional non-attenuation corrected SPECT could be used in any hospitals in Japan, and the initial multicenter validation showed comparable diagnostic accuracy to expert reading of MPI [17].
Subsequent working group activity of “Creation of common databases in nuclear cardiology and cross-calibration among software programs” began in October 2013, and a 2-year project was conducted (Table 2). In the current working group activity, data sets of gated and non-gated MPI were collected, and new SPECT databases of 201Tl and 99mTc-MIBI or tetrofosmin with multifocal collimation (IQ-SPECT, Siemens, Japan/USA) were added. In the additional databases, both exercise and pharmacological stresses were included, and well-controlled patients with single medication for hypertension, dyslipidemia and diabetes mellitus could be included. Normal values were determined for each software program and applied to clinical practice and works of research. Recently, although new software of phase analysis has been developed [18], normal values of the phase parameters have not been presented in Japan. We therefore decided on all normal phase dyssynchrony parameters including HFV and cardioREPO software, which are commonly used in Japan. A project of standardization of 123I- MIBG heart-to-mediastinum ratio (HMR) was also performed using the calibration phantom method [19, 20] as well as defect scoring based on a 17-segment polar map display [21, 22].
Normal myocardial perfusion databases in the JSNM working group 2015
The characteristics of normal MPI databases are summarized in Table 3 in the Japanese population including 201Tl and 99mTc-perfufion tracers. Inclusion of 201Tl databases reflected the recent situations in Japanese nuclear medicine practice. Recently in North America and Europe, 99mTc-MIBI and tetrofosmin have been widely used, and the use of 201Tl has been limited [23]. This has contributed to reduced radiation exposure due to nuclear imaging, and dual-isotope imaging has been discouraged. On the other hand, in Japan, half of the MPI study has been performed with 201Tl as of 2015. The background of this trend in Japan is due to composite factors in favor of 201Tl, which include better tracer extraction fraction, better defect contrast, sufficient image quality even with a dose of 74–111 MBq, and single administration for both stress and rest studies. However, 99mTc radiopharmaceuticals are more appropriate for 16-frame gating, rather than 8-frame gating, and have better physical characteristics for imaging. Moreover, from the viewpoint of radiation exposure and the possibility of stress-only study, when the study is very normal [24, 25], the use of 99mTc tracers will be increased in Japan.
As another characteristics of Japanese database, both 360° and 180° rotation acquisition databases were separately created. Although the 360° acquisition is still widely used in Japan with multi-detector systems, most of the cardiac studies are performed with a 180° acquisition in North America and Europe. When Japanese MPI studies with a 360° rotation acquisition were analyzed regarding perfusion defect scores with QGS, the 360° rotation acquisition database provided higher diagnostic accuracy compared with databases from a 180° rotation acquisition in the Japanese and American populations [26].
The normal perfusion databases are essential for appropriate quantification of perfusion defects. Since defect scores as summed stress/rest/difference scores (SSS/SRS/SDS) depend on normal databases and software algorithms, agreement among various software types is considered desirable, but non-negligible difference in scores does exit. Figure 1 shows a patient who showed a mild to moderate degree of ischemia, when QGS, HSV and cardioREPO are used for quantification. The scoring of SSS ranged from 6 to 9, showing only minor differences. Since the threshold of 10 % ischemia has been recognized as the indication for coronary intervention when coronary stenosis is >50 % [27–29], similar quantitative results at least regarding this threshold are desirable, and further comparative studies are required.
Myocardial perfusion database for short-time acquisition protocols
There are two possibilities for short-time acquisition protocols, namely multifocal collimation with IQ-SPECT (SMARTZOOM collimator; Siemens, Tokyo, Japan) and CZT camera of either D-SPECT (Biosensors Japan/Dynamic Spectrum, Israel; installed in 8 institutions as of December 2015) or NM530c (GE healthcare, Japan; installed in 8 institutions). This working group created databases for IQ-SPECT, and the database for CZT camera was investigated in another JSNM working group in 2014. Compared with the Anger camera, the CZT camera demonstrated dramatically higher performance, and the IQ-SPECT system with special cardiac-dedicated collimation also increased heart counts by focal magnification [30]. The CZT camera provided comparable diagnostic accuracy as assessed by fractional flow reserve [31]. Combined use of supine and prone imaging for detecting coronary artery disease using the scoring method was effective for accurate diagnosis [32], and additional automatic quantification based on standard databases is expected.
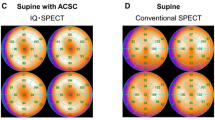
The IQ-SPECT system used multifocal collimators and achieved 4 times higher counts in the heart compared with the conventional parallel-hole collimator system [30, 33–35]. With the collaboration of IQ-SPECT users, 201Tl normal databases in supine and prone positions and CT-based attenuation correction were created with scatter correction and ordered subset conjugate gradient minimization reconstruction [36]. Additional 99mTc-MIBI/tetrofosmin databases will be completed in 2016. IQ-SPECT images show slightly different distribution of the radiotracer due to its specific collimation (Fig. 2). The prone position showed a higher count in the inferior walls than the supine position, and gender difference was observed. In contrast, CT-based attenuation correction demonstrated more homogeneous distribution of each wall, while the apical segment showed significantly decreased activity in both genders. These observations are common characteristics seen in attenuation-corrected SPECT images with parallel-hole collimation [37, 38]. The decreased apical wall activity is partly due to the physiologically thin apical wall and larger apical wall movement [39]. Although attenuation correction was considered potentially useful and recommended [40], its use is still limited in Japan, because nuclear medicine physicians and cardiologists have become accustomed to using conventional imaging without attenuation correction and inconsistency of the effects of attenuation correction regarding camera systems and processing tools [41]. However, since stress-only imaging in combination with attenuation correction is effective to appropriately identify low-risk patients [24, 25], and true quantification in a unit of Bq/ml is a goal of radioactivity measurement in SPECT, a CT-based attenuation correction approach should be further pursued.
Normal values of LV function based on the updated gated SPECT databases
Normal values of LVEF and volumes were the basis for evaluating cardiac function in various cardiac diseases [2, 16]. According to the JSNM working group databases (2007), EF was calculated higher for females than males with QGS, and lower limits were approximately 50 % for males and 55 % for female patients, which were slightly higher compared with the study in the United States and Europe [14]. The normal values at rest created by the current JSNM database (2015) are shown using QGS software in Tables 4 and 5. In small hearts, however, underestimation of the true volume occurs and the effect is higher for ESV than for EDV, resulting in an increase in LVEF. This small-heart artifact is caused by the SPECT reconstruction method optimized for blurred myocardial walls. To minimize such artifacts, particularly in female subjects and children, cardioREPO has adopted a corrected algorithm for small hearts [16]. Average and standard deviation (SD) calculated in 69 subjects are shown in Fig. 3, focusing on the difference in software types.
Gated SPECT parameters of EF, EDV and ESV at rest calculated with four software programs, namely QGS, ECTb, cardioREPO (cREPO) and HFV, in the JSNM normal databases. Mean values and range (mean ± 2SD in brackets) are written in bars. The figure is adapted from Table 1 in Ref. [50]
Normal ranges of phase dyssynchrony parameters
Since four software programs are now available in Japan, normal values of the phase parameters were compared. Phase analysis has been used for more than 30 years using a planar gated blood-pool study. Fourier transform was applied to time-activity curves of each pixel, and phase and amplitude of the fundamental frequency were displayed as functional maps. The method was also used for gated blood-pool SPECT, and three-dimensional propagation patterns of phase were analyzed in patients with conduction anomalies and ventricular asynergy [42, 43]. Subsequently, the method was also applied to gated MPI, in which a proportionate relationship between count and wall thickness due to a partial volume effect was used for myocardial time-activity curves [44, 45]. Indications for cardiac resynchronization therapy (CRT) might be one of the promising applications [46, 47]. Although a number of parameters were proposed, most of the echocardiographic parameters lack validation in appropriate clinical settings, indicating striking variability, poor reproducibility, and limited predictive power [48, 49]. Whether a nuclear approach provides robust results over ECG and LVEF should be further investigated in patients who are indicated for CRT.
When the same original data are provided, nuclear medicine approach generally shows good reproducibility or precision for LVEF and volumes and good correlation to values derived from other modalities. In phase parameters, however, normal values were still not validated well. The working group activity therefore included determination of normal values of phase parameters for ECTb, QGS, HFV and cardioREPO (Fig. 4) [50]. Based on distribution of phase values in the LV, phase histogram is created, and parameters of phase bandwidth, in which 95 % of the phase distribution is included, phase standard deviation (PSD) and phase entropy are calculated. Phase entropy is an index of “disorder” defined by summation of [fi*log(fi)]/Log(n)], where f and n are frequency in the i-th bin and number of bins, respectively, which ranges from 0 to 1 (0–100%). When the normal values were determined at rest based on the working group database, the results could not be interchangeably used. However, some similarities in normal ranges existed between ECTb and cardioREPO and between QGS and HFV, which probably depended on the computation algorithm of each software program. The upper limit of PSD was 20° for ECTb and cardioREPO, and 10° for QGS and HFV. All software programs showed higher PSD and bandwidth in male subjects than in female subjects. In addition, the higher SD and bandwidth were related to the larger LV volume and the lower EF, which depended on software types. Finally, since the upper limit of the normal values was not the best threshold for the effective indication to CRT [47], the optimal threshold should be separately validated.
Comparison of phase parameters (phase bandwidth, phase SD, and phase entropy) at rest with four software programs using the JSNM normal databases. Mean values and range (mean ± 2SD in brackets) are written in bars. The figure is adapted from Table 2 in Ref. [50]
Standardization of 123I-MIBG HMR for multicenter studies
123I-MIBG has a long history of clinical use in Japan since 1992, and major indications have been chronic heart failure (CHF) and Lewy-body diseases [51]. Regarding application of MIBG in CHF, a number of studies in Japan, Europe and the United States have unanimously shown that low HMR and high washout rate (WR) were related to poor outcomes including cardiac death, progression of heart failure and occurrence of lethal arrhythmia [51–55]. In multicenter studies and meta-analysis, the threshold of HMR for poor prognosis was around 1.6–1.8. In contrast, patients who showed HMR >2.0 showed good prognosis. However, it has been understood that significant differences in HMR exist among hospitals depending on scinticameras and collimators [20, 56, 57]. In the JSNM working group normal databases, while average late HMR with a low-energy (LE) collimator was 2.5, that with a medium-energy (ME) collimator was 3.0 [1]. To obtain stable results, the recommendation of European Association of Nuclear Medicine Cardiovascular Committee and European Council of Nuclear Cardiology was to use the ME-type collimator [58]. However, in clinical practice a number of hospitals continue to use the LE high-resolution (HR) collimator in Europe and North America, and LE general purpose (GP) or low-medium energy (LME) has also been widely used in Japan.
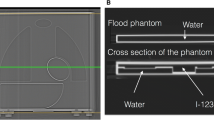
To adjust the differences in camera-collimators, while the multi-energy window acquisition method and direct empirical correction method have been proposed, they were not practical for applying the method to all possible camera-collimator conditions. The calibration phantom method was developed in Japan, which used specific phantoms to obtain two HMRs from anterior and posterior views [59]. Based on the phantom experiments in each institution, the conversion coefficient in each camera-collimator system was determined, and all the HMRs could be converted to the condition of the most common ME general purpose (GP) collimator with a conversion coefficient of 0.88 [19] (Table 6). The linear regression equation among the system used the formula passing on the coordinate of HMR (1,1). It is based on the assumption that HMR should be 1, when cardiac activity is equal to mediastinal activity. The experiments have already been performed in 500 hospitals in Japan, and in more than 30 camera-collimator conditions in Europe as of the end of 2015.
When the threshold HMR was converted to the condition of the MEGP collimator, the threshold of ADMIRE-HF (1.6, with LEHR), Sapporo Medical University (1.74, with LEGP) and the pooled database in Japan (1.68, with LE collimators in 6 hospitals) were converted to around 2.0 [51]. In a neurology field, the thresholds of differentiating Alzheimer disease and dementia with Lewy bodies were 2.0–2.2 in a multicenter study in Japan [60]. The effectiveness of standardization included not only diagnosis but also prognostic evaluation. The mortality rate in the Japanese pooled database was analyzed, and 2 and 5-year mortality risk models were created [61, 62]. In this multivariate model, parameters of age, sex, LVEF, New York Heart Association functional class, and late HMR were used. In addition, since 123I-MIBG WR differs significantly based on the use of background and decay correction and timing of late imaging, standardization of methodology is also required for calculating WR [63].
With the advent of the CZT camera, 123I-MIBG planar image may not be a part of clinical routine study. D-SPECT, however, provides a planogram comparable to the planar anterior view [64]. Based on these reconstructed planar images, HMR can be similarly calculated, although the camera field of view is narrow. When HMRs from the D-SPECT and the Anger camera were compared, a linear relationship was obtained. Moreover, when the Anger image HMR was standardized to HMR with the ME condition as proposed, both D-SPECT and planar standardized methods showed similar HMR values, indicating feasibility of standardization in including planar and SPECT studies [64, 65].
123I-MIBG defect scoring using normal SPECT databases
The degree of segmental defect in 123I-MIBG SPECT can be scored using a similar 17-segment model used for MPI. Although visual scoring can be used, the distribution of 123I-MIBG differs significantly in myocardial walls, showing lower count particularly in the inferior region. Although comparative scores between perfusion and 123I-MIBG have been used [22], appropriate databases are particularly important for 123I-MIBG imaging. The JSNM working group created 123I-MIBG databases for the first time to quantify defect scores and is clinically available now [1, 15] (Fig. 5). Moderate agreement could be observed between HMR and defect scores. However, the problem of defect scoring was in patients with a general decrease in the whole heart, since the scoring implicitly assumes that normal myocardial remains in some segments of the myocardium [66]. A new idea for scoring is necessary when HMR is very low in a whole heart, which is sometimes seen in Lewy-body diseases and severe heart failure. At present, defect scoring has a complimentary role for evaluating the severity of three-dimensional 123I-MIBG defects.
Importance of normal database and future trends
Standardized viewpoints based on normal databases are important for appropriate diagnosis in heart diseases. The JSNM working group provided information on normal control values and database sets as well on clinical works and research. Recently, conventional SPECT systems have been upgraded to SPECT-CT, which created different distribution patterns by CT-based attenuation corrections. In addition, solid-state cameras provide specific count distributions in the myocardium in addition to high resolution and sensitivity. Although we could not create all possible normal databases in this working group activity, common standard databases created by JSNM will contribute to standard interpretation of nuclear images. Moreover, since amount of ischemia is used for diagnostic threshold for the indications of coronary intervention, it is convenient if at least the diagnostic threshold determined by different software shows similar defect scores.
Phase parameters were determined in JSNM working group activity. However, it should be further investigated whether a nuclear approach shows advantages over conventional criteria using ECG and LVEF or echocardiography.
Regarding standardization of 123I-MIBG HMR, conversion to MEGP-collimator comparable values is occurring in Japanese hospitals. Various collimators including LEHR, LEGP, extended LE, MEGP and ME low penetration collimators are used at present in Japan. Although the HMR is a simple parameter of planar count ratio of the heart to background regions, it is important to consider that a minor difference potentially creates significant differences in prognosis. If correlation to SPECT methods and planar HMR becomes clear, wider application of MIBG can be anticipated using the standardized parameters. Since we found good correlation between D-SEPCT and standardized HMR using the Anger camera, creation of large standardized databases would be feasible after standardization. In future studies, clinical use of 123I-MIBG imaging should incorporate individual patient risk stratification and determine roles for therapeutic decision-making in patients with CHF [51, 67].
Conclusion
The JSNM working group of nuclear cardiology created common normal databases fitted for conventional SPECT system and SPECT-CT imaging with multifocal collimators. While quantification by nuclear medicine software is supported by the normal values, the values are not interchangeable for any software types and the characteristics of the calculated parameters should be kept in mind for clinical application.
References
Nakajima K. Normal values for nuclear cardiology: Japanese databases for myocardial perfusion, fatty acid and sympathetic imaging and left ventricular function. Ann Nucl Med. 2010;24:125–35.
Go V, Bhatt MR, Hendel RC. The diagnostic and prognostic value of ECG-gated SPECT myocardial perfusion imaging. J Nucl Med. 2004;45:912–21.
DePuey EG, Nichols K, Dobrinsky C. Left ventricular ejection fraction assessed from gated technetium-99 m-sestamibi SPECT. J Nucl Med. 1993;34:1871–6.
Germano G, Kiat H, Kavanagh PB, Moriel M, Mazzanti M, Su HT, et al. Automatic quantification of ejection fraction from gated myocardial perfusion SPECT. J Nucl Med. 1995;36:2138–47.
Garcia EV, Faber TL, Cooke CD, Folks RD, Chen J, Santana C. The increasing role of quantification in clinical nuclear cardiology: the Emory approach. J Nucl Cardiol. 2007;14:420–32.
Germano G, Kavanagh PB, Slomka PJ, Van Kriekinge SD, Pollard G, Berman DS. Quantitation in gated perfusion SPECT imaging: the Cedars-Sinai approach. J Nucl Cardiol. 2007;14:433–54.
Ficaro EP, Lee BC, Kritzman JN, Corbett JR. Corridor4DM: the Michigan method for quantitative nuclear cardiology. J Nucl Cardiol. 2007;14:455–65.
Kobayashi K, Tsukamoto K. Myocardial image analysis software Heart Risk View, Heart Score View and Heart Function View (In Japanese). Kakuigaku Gijutsu (Nucl Med Techonology). 2014;34:136–44.
Nakae I, Hayashi H, Matsumoto T, Mitsunami K, Horie M. Clinical usefulness of a novel program “Heart Function View” for evaluating cardiac function from gated myocardial perfusion SPECT. Ann Nucl Med. 2014;28:812–23.
Nakajima K, Okuda K, Nystrom K, Richter J, Minarik D, Wakabayashi H, et al. Improved quantification of small hearts for gated myocardial perfusion imaging. Eur J Nucl Med Mol Imaging. 2013;40:1163–70.
Shaw L, Narula J. Risk Assessment and Predictive Value of Coronary Artery Disease Testing. J Nucl Med. 2009;50:1296–306.
Matsumoto N, Sato Y, Suzuki Y, Kasama S, Nakano Y, Kato M, et al. Incremental Prognostic Value of Cardiac Function Assessed by ECG-Gated Myocardial Perfusion SPECT for the Prediction of Future Acute Coronary Syndrome. Circ J. 2008;72:2035–9.
Nishimura T, Nakajima K, Kusuoka H, Yamashina A, Nishimura S. Prognostic study of risk stratification among Japanese patients with ischemic heart disease using gated myocardial perfusion SPECT: J-ACCESS study. Eur J Nucl Med Mol Imaging. 2008;35:319–28.
Nakajima K, Kumita S, Ishida Y, Momose M, Hashimoto J, Morita K, et al. Creation and characterization of Japanese standards for myocardial perfusion SPECT: database from the Japanese Society of Nuclear Medicine Working Group. Ann Nucl Med. 2007;21:505–11.
Matsuo S, Nakajima K, Yamashina S, Sakata K, Momose M, Hashimoto J, et al. Characterization of Japanese standards for myocardial sympathetic and metabolic imaging in comparison with perfusion imaging. Ann Nucl Med. 2009;23:517–22.
Nakajima K, Kusuoka H, Nishimura S, Yamashina A, Nishimura T. Normal limits of ejection fraction and volumes determined by gated SPECT in clinically normal patients without cardiac events: a study based on the J-ACCESS database. Eur J Nucl Med Mol Imaging. 2007;34:1088–96.
Nakajima K, Matsuo S, Kawano M, Matsumoto N, Hashimoto J, Yoshinaga K, et al. The validity of multi-center common normal database for identifying myocardial ischemia: Japanese Society of Nuclear Medicine working group database. Ann Nucl Med. 2010;24:99–105.
Chen J, Henneman MM, Trimble MA, Bax JJ, Borges-Neto S, Iskandrian AE, et al. Assessment of left ventricular mechanical dyssynchrony by phase analysis of ECG-gated SPECT myocardial perfusion imaging. J Nucl Cardiol. 2008;15:127–36.
Nakajima K, Okuda K, Yoshimura M, Matsuo S, Wakabayashi H, Imanishi Y, et al. Multicenter cross-calibration of I-123 metaiodobenzylguanidine heart-to-mediastinum ratios to overcome camera-collimator variations. J Nucl Cardiol. 2014;21:970–8.
Nakajima K, Matsubara K, Ishikawa T, Motomura N, Maeda R, Akhter N, et al. Correction of iodine-123-labeled meta-iodobenzylguanidine uptake with multi-window methods for standardization of the heart-to-mediastinum ratio. J Nucl Cardiol. 2007;14:843–51.
Boogers MJ, Borleffs CJ, Henneman MM, van Bommel RJ, van Ramshorst J, Boersma E, et al. Cardiac sympathetic denervation assessed with 123-iodine metaiodobenzylguanidine imaging predicts ventricular arrhythmias in implantable cardioverter-defibrillator patients. J Am Coll Cardiol. 2010;55:2769–77.
Dimitriu-Leen AC, Scholte AJ, Jacobson AF. 123I-MIBG SPECT for evaluation of patients with heart failure. J Nucl Med. 2015;56(Suppl 4):25S–30S.
Einstein AJ, Moser KW, Thompson RC, Cerqueira MD, Henzlova MJ. Radiation dose to patients from cardiac diagnostic imaging. Circulation. 2007;116:1290–305.
Mathur S, Heller GV, Bateman TM, Ruffin R, Yekta A, Katten D, et al. Clinical value of stress-only Tc-99m SPECT imaging: importance of attenuation correction. J Nucl Cardiol. 2013;20:27–37.
Ueyama T, Takehana K, Maeba H, Iwasaka T. Prognostic value of normal stress-only technetium-99m myocardial perfusion imaging protocol. Comparison with standard stress-rest protocol. Circ J. 2012;76:2386–91.
Nakajima K, Okuda K, Kawano M, Matsuo S, Slomka P, Germano G, et al. The importance of population-specific normal database for quantification of myocardial ischemia: comparison between Japanese 360 and 180-degree databases and a US database. J Nucl Cardiol. 2009;16:422–30.
Hachamovitch R, Hayes SW, Friedman JD, Cohen I, Berman DS. Comparison of the short-term survival benefit associated with revascularization compared with medical therapy in patients with no prior coronary artery disease undergoing stress myocardial perfusion single photon emission computed tomography. Circulation. 2003;107:2900–7.
Hachamovitch R, Rozanski A, Shaw LJ, Stone GW, Thomson LE, Friedman JD, et al. Impact of ischaemia and scar on the therapeutic benefit derived from myocardial revascularization vs. medical therapy among patients undergoing stress-rest myocardial perfusion scintigraphy. Eur Heart J. 2011;32:1012–24.
Task Force on Myocardial Revascularization of the European Society of C, the European Association for Cardio-Thoracic S, European Association for Percutaneous Cardiovascular I, Wijns W, Kolh P, Danchin N, et al. Guidelines on myocardial revascularization. Eur Heart J. 2010;31:2501–55.
Imbert L, Poussier S, Franken PR, Songy B, Verger A, Morel O, et al. Compared performance of high-sensitivity cameras dedicated to myocardial perfusion SPECT: a comprehensive analysis of phantom and human images. J Nucl Med. 2012;53:1897–903.
Tanaka H, Chikamori T, Tanaka N, Hida S, Igarashi Y, Yamashita J, et al. Diagnostic performance of a novel cadmium-zinc-telluride gamma camera system assessed using fractional flow reserve. Circ J. 2014;78:2727–34.
Nishiyama Y, Miyagawa M, Kawaguchi N, Nakamura M, Kido T, Kurata A, et al. Combined supine and prone myocardial perfusion single-photon emission computed tomography with a cadmium zinc telluride camera for detection of coronary artery disease. Circ J. 2014;78:1169–75.
Caobelli F, Thackeray JT, Soffientini A, Bengel FM, Pizzocaro C, Guerra UP. Feasibility of one-eighth time gated myocardial perfusion SPECT functional imaging using IQ-SPECT. Eur J Nucl Med Mol Imaging. 2015;42:1920–8.
Horiguchi Y, Ueda T, Shiomori T, Kanna M, Matsushita H, Kawaminami T, et al. Validation of a short-scan-time imaging protocol for thallium-201 myocardial SPECT with a multifocal collimator. Ann Nucl Med. 2014;28:707–15.
Matsuo S, Nakajima K, Onoguchi M, Wakabayash H, Okuda K, Kinuya S. Nuclear myocardial perfusion imaging using thallium-201 with a novel multifocal collimator SPECT/CT: IQ-SPECT versus conventional protocols in normal subjects. Ann Nucl Med. 2015;29:452–9.
Nakajima K, Okuda K, Matsuo S, Kondo C, Sarai M, Horiguchi Y, et al. Multicenter normal Tl-201 databases with multifocal collimators for supine, prone and CT-based corrections (Abstract). J Nucl Med. 2015;56:1740.
Berman DS, Kang X, Nishina H, Slomka PJ, Shaw LJ, Hayes SW, et al. Diagnostic accuracy of gated Tc-99m sestamibi stress myocardial perfusion SPECT with combined supine and prone acquisitions to detect coronary artery disease in obese and nonobese patients. J Nucl Cardiol. 2006;13:191–201.
Slomka PJ, Nishina H, Abidov A, Hayes SW, Friedman JD, Berman DS, et al. Combined quantitative supine-prone myocardial perfusion SPECT improves detection of coronary artery disease and normalcy rates in women. J Nucl Cardiol. 2007;14:44–52.
Okuda K, Nakajima K, Matsuo S, Wakabayashi H, Taki J, Kinuya S. Cause of apical thinning on attenuation-corrected myocardial perfusion SPECT. Nucl Med Commun. 2011;32:1033–9.
Heller GV, Links J, Bateman TM, Ziffer JA, Ficaro E, Cohen MC, et al. American Society of Nuclear Cardiology and Society of Nuclear Medicine joint position statement: attenuation correction of myocardial perfusion SPECT scintigraphy. J Nucl Cardiol. 2004;11:229–30.
O’Connor M, Kemp B, Anstett F, Christian P, Ficaro EP, Frey E, et al. A multicenter evaluation of commercial attenuation compensation techniques in cardiac SPECT using phantom models. J Nucl Cardiol. 2002;9:361–76.
Machac J, Horowitz SF, Fagerstrom R, Levine R, Goldsmith SJ. Characterization and automatic identification of ECG conduction abnormalities using segmental multiharmonic Fourier analysis of gated blood-pool scintigrams. Eur J Nucl Med. 1985;11:210–6.
Nakajima K, Bunko H, Tada A, Tonami N, Hisada K, Misaki T, et al. Nuclear tomographic phase analysis: localization of accessory conduction pathway in patients with Wolff-Parkinson-White syndrome. Am Heart J. 1985;109:809–15.
Chen J, Garcia EV, Folks RD, Cooke CD, Faber TL, Tauxe EL, et al. Onset of left ventricular mechanical contraction as determined by phase analysis of ECG-gated myocardial perfusion SPECT imaging: development of a diagnostic tool for assessment of cardiac mechanical dyssynchrony. J Nucl Cardiol. 2005;12:687–95.
Cooke CD, Garcia EV, Cullom SJ, Faber TL, Pettigrew RI. Determining the accuracy of calculating systolic wall thickening using a fast Fourier transform approximation: a simulation study based on canine and patient data. J Nucl Med. 1994;35:1185–92.
O’Connell JW, Schreck C, Moles M, Badwar N, DeMarco T, Olgin J, et al. A unique method by which to quantitate synchrony with equilibrium radionuclide angiography. J Nucl Cardiol. 2005;12:441–50.
Henneman MM, Chen J, Dibbets-Schneider P, Stokkel MP, Bleeker GB, Ypenburg C, et al. Can LV dyssynchrony as assessed with phase analysis on gated myocardial perfusion SPECT predict response to CRT? J Nucl Med. 2007;48:1104–11.
Chung ES, Leon AR, Tavazzi L, Sun JP, Nihoyannopoulos P, Merlino J, et al. Results of the predictors of response to CRT (PROSPECT) trial. Circulation. 2008;117:2608–16.
Hawkins NM, Petrie MC, Burgess MI, McMurray JJ. Selecting patients for cardiac resynchronization therapy: the fallacy of echocardiographic dyssynchrony. J Am Coll Cardiol. 2009;53:1944–59.
Nakajima K, Okuda K, Matsuo S, Kiso K, Kinuya S, Garcia EV. Comparison of phase dyssynchrony analysis using gated myocardial perfusion imaging with four software programs: Based on the Japanese Society of Nuclear Medicine working group normal database. J Nucl Cardiol. 2016. doi:10.1007/s12350-015-0333-y.
Nakajima K, Nakata T. Cardiac 123I-MIBG Imaging for clinical decision making: 22-year experience in Japan. J Nucl Med. 2015;56(Suppl 4):11S–9S.
Jacobson AF, Senior R, Cerqueira MD, Wong ND, Thomas GS, Lopez VA, et al. Myocardial iodine-123 meta-iodobenzylguanidine imaging and cardiac events in heart failure. Results of the prospective ADMIRE-HF (AdreView Myocardial Imaging for Risk Evaluation in Heart Failure) study. J Am Coll Cardiol. 2010;55:2212–21.
Nakata T, Nakajima K, Yamashina S, Yamada T, Momose M, Kasama S, et al. A pooled analysis of multicenter cohort studies of 123I-mIBG imaging of sympathetic innervation for assessment of long-term prognosis in heart failure. JACC Cardiovasc Imaging. 2013;6:772–84.
Verschure DO, Veltman CE, Manrique A, Somsen GA, Koutelou M, Katsikis A, et al. For what endpoint does myocardial 123I-MIBG scintigraphy have the greatest prognostic value in patients with chronic heart failure? Results of a pooled individual patient data meta-analysis. Eur Heart J Cardiovasc Imaging. 2014;15:996–1003.
Agostini D, Verberne HJ, Burchert W, Knuuti J, Povinec P, Sambuceti G, et al. I-123-mIBG myocardial imaging for assessment of risk for a major cardiac event in heart failure patients: insights from a retrospective European multicenter study. Eur J Nucl Med Mol Imaging. 2008;35:535–46.
Inoue Y, Suzuki A, Shirouzu I, Machida T, Yoshizawa Y, Akita F, et al. Effect of collimator choice on quantitative assessment of cardiac iodine 123 MIBG uptake. J Nucl Cardiol. 2003;10:623–32.
Verberne HJ, Habraken JB, van Eck-Smit BL, Agostini D, Jacobson AF. Variations in 123I-metaiodobenzylguanidine (MIBG) late heart mediastinal ratios in chronic heart failure: a need for standardisation and validation. Eur J Nucl Med Mol Imaging. 2008;35:547–53.
Flotats A, Carrio I, Agostini D, Le Guludec D, Marcassa C, Schafers M, et al. Proposal for standardization of 123I-metaiodobenzylguanidine (MIBG) cardiac sympathetic imaging by the EANM Cardiovascular Committee and the European Council of Nuclear Cardiology. Eur J Nucl Med Mol Imaging. 2010;37:1802–12.
Nakajima K, Okuda K, Matsuo S, Yoshita M, Taki J, Yamada M, et al. Standardization of metaiodobenzylguanidine heart to mediastinum ratio using a calibration phantom: effects of correction on normal databases and a multicentre study. Eur J Nucl Med Mol Imaging. 2012;39:113–9.
Yoshita M, Arai H, Arai H, Arai T, Asada T, Fujishiro H, et al. Diagnostic accuracy of 123I-meta-iodobenzylguanidine myocardial scintigraphy in dementia with Lewy bodies: a multicenter study. PLoS One. 2015;10:e0120540.
Nakajima K, Nakata T, Yamada T, Yamashina S, Momose M, Kasama S, et al. A prediction model for 5-year cardiac mortality in patients with chronic heart failure using 123I-metaiodobenzylguanidine imaging. Eur J Nucl Med Mol Imaging. 2014;41:1673–82.
Nakajima K, Nakata T, Matsuo S, Jacobson AF. Creation of mortality risk charts using 123I meta-iodobenzylguanidine heart-to-mediastinum ratio in patients with heart failure: 2- and 5-year risk models. Eur Heart J Cardiovasc Imaging. 2016. doi:10.1093/ehjci/jev322.
Okuda K, Nakajima K, Sugino S, Kirihara Y, Matsuo S, Taki J, et al. Development and validation of a direct-comparison method for cardiac 123I-metaiodobenzylguanidine washout rates derived from late 3-hour and 4-hour imaging. Eur J Nucl Med Mol Imaging. 2016;43:319–25.
Bellevre D, Manrique A, Legallois D, Bross S, Baavour R, Roth N, et al. First determination of the heart-to-mediastinum ratio using cardiac dual isotope (123I-MIBG/99mTc-tetrofosmin) CZT imaging in patients with heart failure: the ADRECARD study. Eur J Nucl Med Mol Imaging. 2015;42:1912–9.
Nakajima K, Okuda K, Matsuo S, Agostini D. The time has come to standardize 123I-MIBG heart-to-mediastinum ratios including planar and SPECT methods. Eur J Nucl Med Mol Imaging. 2016;43:386–8.
Lebasnier A, Lamotte G, Manrique A, Peyronnet D, Bouvard G, Defer G, et al. Potential diagnostic value of regional myocardial adrenergic imaging using 123I-MIBG SPECT to identify patients with Lewy body diseases. Eur J Nucl Med Mol Imaging. 2015;42:1043–51.
Flotats A, Carrio I. Cardiac innervation imaging: implications for risk stratification and therapeutic decision-making. Curr Cardiovasc Imaging Rep. 2016;9:6.
Acknowledgments
This work was partly supported by the working group activity of the Japanese Society of Nuclear Medicine and by Grants-in-Aid for Scientific Research in Japan (PI: Kenichi Nakajima). Emory Cardiac Toolbox was kindly supplied by Syntermed, Inc. (Atlanta, GA, USA) and Corridor 4DM by INIVA Medical Solutions, LLC (Ann Arbor, MI, USA). The Authors also thank Karin Toth, MSc, for the batch processing of the data with cardioREPO, and Mr. Yu Yamanaka (Kanazawa Medical University) for his help in preparation of databases, and Mr. Ronald Belisle for editorial assistance in the preparation of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
KN has collaborative research with Fujifilm RI Pharma Co., Ltd., which supplies 123I-MIBG in Japan and developed software. KN also was involved in developing cardiac software with Nihon Medi-Physics (Tokyo, Japan).
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made.
The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder.
To view a copy of this licence, visit https://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Nakajima, K., Matsumoto, N., Kasai, T. et al. Normal values and standardization of parameters in nuclear cardiology: Japanese Society of Nuclear Medicine working group database. Ann Nucl Med 30, 188–199 (2016). https://doi.org/10.1007/s12149-016-1065-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12149-016-1065-z