Abstract
Osteopontin is a multifunctional matricellular protein that is expressed by many cell types. Through cell-matrix and cell-cell interactions the molecule elicits a number of responses from a broad range of target cells via its interaction with integrins and the hyaluronan receptor CD44. In many tissues osteopontin has been found to be involved in important physiological and pathological processes, including tissue repair, inflammation and fibrosis. Post-natal skeletal muscle is a highly differentiated and specialised tissue that retains a remarkable capacity for regeneration following injury. Regeneration of skeletal muscle requires the co-ordinated activity of inflammatory cells that infiltrate injured muscle and are responsible for initiating muscle fibre degeneration and phagocytosis of necrotic tissue, and muscle precursor cells that regenerate the injured muscle fibres. This review focuses on the current evidence that osteopontin plays multiple roles in skeletal muscle, with particular emphasis on its role in regeneration and fibrosis following injury, and in determining the severity of myopathic diseases such as Duchenne muscular dystrophy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Skeletal muscle structure, injury and repair
Skeletal muscle is largely composed of muscle fibres that are elongated cells, each containing multiple post-mitotic nuclei constituting a syncytium (Fig. 1). During embryonic development and post-natal regeneration, muscle fibres form by the fusion of mononucleate, mitotically active and determined myogenic cells known as myoblasts. Myoblasts in postnatal skeletal muscle are derived from quiescent myogenic cells, known as satellite cells, that remain sandwiched between the surrounding basal lamina and the cell membrane of postnatal muscle fibres (reviewed in Zammit et al. 2006).
A schematic representation showing the processes involved in regeneration of skeletal muscle following injury. a Mature skeletal muscle is composed of closely packed elongated muscle fibres which contain peripherally located, post-mitotic myonuclei sharing a common cytoplasm. Quiescent mononucleated satellite cells are located between the sarcolemma and the basement membrane of muscle fibres. b In response to damage, injured muscle fibres undergo necrosis, resulting in activation of endogenous satellite cells to form a pool of mitotic myoblasts, and infiltration of the site of injury from the vasculature by inflammatory cells including neutrophils and macrophages. Eventually, myoblasts align, fuse and terminally differentiate to form primitive muscle fibres called myotubes. c As skeletal muscle regeneration proceeds, whole muscle fibres or new segments of injured muscle fibres are formed by the terminal differentiation of myoblasts. In murine muscle, the nuclei of regenerated fibres remain centrally located
The ability of postnatal skeletal muscle to adapt to changing use or to regenerate in response to even very severe trauma is a remarkable characteristic of this tissue. In response to muscle injury, satellite cells become activated due to the action of mitogenic factors, including fibroblast growth factor 2 (FGF2) and hepatocyte growth factor, which are released from damaged muscle fibres (Allen et al. 1995; Chen et al. 1994; Tatsumi et al. 1998). As well as the activation of satellite cells, injury to skeletal muscles also induces their infiltration by inflammatory cells including neutrophils and macrophages (Nguyen and Tidball 2003). Inflammatory cells play crucial roles in promoting skeletal muscle regeneration (Lescaudron et al. 1999; Nguyen and Tidball 2003; Tidball 2005), and recent studies have highlighted the critical roles played by phenotypically distinct macrophages during the early (Th1 dominated) and later (Th2 dominated) inflammatory responses to muscle injury (Tidball 2011). As necrotic muscle fibres are removed from injured muscles, myoblasts formed by activation of satellite cells at the site of injury are induced to undergo myogenic differentiation, withdraw from the cell cycle, align and fuse to regenerate damaged segments of fibres (Fig. 1; Collins et al. 2005). The cues that induce myogenic differentiation in injured muscles are poorly understood, but undoubtedly involve components of the extracellular matrix and growth factors in the local microenvironment (Florini et al. 1991; von der Mark and Ocalan 1989).
Osteopontin structure & function
Osteopontin, also known as early T-lymphocyte activation 1 (ETA1) protein, secreted phosphoprotein 1 (SPP1) and bone sialoprotein 1 (BSP1), is an acidic glycoprotein that is a member of the small integrin-binding N-linked glycoprotein family of proteins. Expression of osteopontin has been reported in a wide range of cells including macrophages, smooth and skeletal muscle cells, endothelial cells, lymphocytes, osteoblasts and tumour cells (Chambers et al. 1996; O’Brien et al. 1994; Patarca et al. 1989; Weinreb et al. 1990; Uaesoontrachoon et al. 2008). Whilst osteopontin is predominantly a secreted molecule, an intracellular form of the molecule has been reported (Inoue and Shinohara 2011; Zohar et al. 1997). The secreted form of osteopontin can exist both as a soluble molecule with cytokine-like functions and as an immobilised matricellular protein (O’Regan et al. 1999) that can interact with certain variants of the hyaluronan receptor CD44 and with a variety of integrins (Denhardt et al. 2001) to activate intracellular signalling pathways and mediate cell-cell and cell-matrix interactions. The effects of binding of osteopontin to target cells include promoting attachment, proliferation, migration, chemotaxis and apoptosis of cells (Denhardt et al. 2001; Giachelli et al. 1998; Standal et al. 2004), thereby regulating many pathological and physiological processes, including tissue repair, inflammation and fibrosis (Berman et al. 2004; Denhardt et al. 2001; Duvall et al. 2007; Giachelli et al. 1998; Hashimoto et al. 2007; Liaw et al. 1994; Mori et al. 2008; O’Regan and Berman 2000; Sam et al. 2004, ).
Alternative splicing of the human, but not mouse, SPP1 gene has been reported (Saitoh et al. 1995). The full length isoform (OPNa) is encoded by 7 exons, whereas OPNb lacks exon 5 and OPNc lacks exon 4 (Fig. 2a). Alternative splicing is thought to influence the degree of phosphorylation of the isoforms and thus their biological properties (Gimba and Tilli 2013). Osteopontin consists of a number of functional domains (Fig. 2b; Kazanecki et al. 2007), and is extensively posttranslationally modified by glycosylation, phosphorylation and sulphation and may be subject to further processing by cross-linking and proteolytic cleavage. Specific posttranslational modifications and processing of osteopontin alter the properties of the molecule and have functional significance. For example, the degree of phosphorylation regulates the adhesive properties of osteopontin (Christensen et al. 2007); moreover a cryptic binding site revealed by thrombin’s proteolytic cleavage of osteopontin increases its adhesive properties by allowing binding to integrins in a non-RGD dependent manner (Yokosaki et al. 1999). Thus, alternative splicing, posttranslational modification, cross-linking and proteolysis of osteopontin give rise to a potential array of different isoforms of osteopontin that differ in the extent and type of their modifications and, therefore, their biological properties.
a Genomic structure and alternative splicing of human SPP1 gene. Exons 1 to 7 of SPP1 are represented by open boxes. The exons contained in the three identified human osteopontin transcripts are shown. b A schematic diagram of osteopontin structure showing approximate sites of glycosylation (G), reactive glutamines (Q) phosphorylation (P) and proteolytic cleavage by thrombin and matrix-metalloproteinases. Sites responsible for RGD-dependent (RGD) and RGD-independent (SVVYGLR) integrin binding, as well as hydroxyapatite (pAsp), calcium and heparin binding are indicated
Osteopontin as a link between inflammation and myogenesis during regeneration of injured skeletal muscles
Induction of osteopontin expression following skeletal muscle injury, associated with infiltrating inflammatory cells, necrotic muscle fibres and endogenous myogenic cells (Fig. 3), has been reported by a number of studies (Barbosa-Souza et al. 2011; Hirata et al. 2003; Hoffman et al. 2013; Uaesoontrachoon et al. 2013). One study measured an approximately 100-fold increase in expression of osteopontin mRNA over baseline within 12 and 24 h after muscle injury, returning to baseline between 14 and 16 days post injury (Hoffman et al. 2013). In vitro, FGF2, has been shown to strongly induce osteopontin expression by myogenic cells, and recombinant osteopontin was found to significantly affect myoblast attachment, proliferation and migration (Uaesoontrachoon et al. 2008). Furthermore, the form in which the molecule was presented to myogenic cells determined the nature of the response; osteopontin immobilised onto tissue culture substrata promoted adhesion and differentiation but not proliferation of cells of the myogenic cell line C2C12, whereas osteopontin presented in solution stimulated adhesion to fibronectin coated substrata and proliferation of C2C12 cells as well as inhibiting differentiation and migration of these cells (Uaesoontrachoon et al. 2008).
Co-immunolocalisation of desmin and osteopontin in the tibialis anterior muscle of a 12 week old mdx mouse. Strong desmin staining is observed in regenerated (centrally nucleated) muscle fibres as well as in single, infiltrating cells (arrowed). Osteopontin expression is low in mature and regenerated muscle fibres and high in single, infiltrating cells (arrowed). Nuclei counter stained with 4′,6-diamidino-2-phenylindole, bar = 50 μm
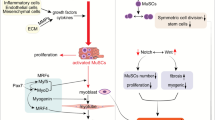
The rapidity and magnitude of the induction of osteopontin expression in response to muscle injury coupled with its known effects on inflammatory and myogenic cells suggests that osteopontin is an important factor during the degenerative and regenerative events that follow skeletal muscle injury. This hypothesis was tested using a whole muscle autografting model of muscle injury that causes a single severe injury, leading to acute osteopontin expression, a characteristic pattern of inflammatory infiltration, and muscle fibre degeneration and regeneration in wild type mice (Uaesoontrachoon et al. 2013). In autografted muscles of osteopontin null mice, inflammatory infiltration (macrophages and neutrophils) and degenerative changes were reduced 3 days after injury, and the early regenerative response (5 days post-injury) was delayed, compared to wild type autografted muscles (Uaesoontrachoon et al. 2013). These observations indicate that osteopontin is involved in the inflammatory, degenerative and regenerative events that occur in early skeletal muscle regeneration. Based on these studies we have proposed a model for osteopontin’s effect on muscle degeneration and regeneration (Fig. 4). The ability of factors such as FGF2, which is released by injured muscle fibres (Chen et al. 1994), to induce osteopontin expression by myogenic cells (Uaesoontrachoon et al. 2008), suggests that these cells present at the site of injury may be some of the first cells to express osteopontin directly in response to muscle injury. Local secretion of soluble osteopontin may contribute to both the retention of a pool of proliferative myoblasts at the site of injury and infiltration of the injured muscle by macrophages and neutrophils (Giachelli et al. 1998; Banerjee et al. 2006; Koh et al. 2007). As macrophages in particular are a rich source of osteopontin (Giachelli et al. 1998; Hirata et al. 2003), osteopontin expression by these inflammatory cells could play an equally crucial part in osteopontin’s role in muscle regeneration by helping to amplify the initial osteopontin expression in the muscles. At later stages in muscle regeneration, osteopontin may increasingly become incorporated into the remodelled extracellular matrix, for example by binding to fibronectin and others of its constituents (Mukherjee et al. 1995). As an immobilised molecule osteopontin may then promote attachment of myoblasts to the extracellular matrix, and support their terminal differentiation into new muscle fibres (Uaesoontrachoon et al. 2008).
Schematic diagram showing a proposed model of role for osteopontin during skeletal muscle repair. a Osteopontin expression is induced in response to injury to mature skeletal muscle. b Release of osteopontin from the site of injury promotes proliferation of myoblasts, formed from activated satellite cells, and infiltration of the muscle by blood-borne inflammatory cells including macrophages and neutrophils. Osteopontin expression at the site of injury is further augmented by its release from myoblasts and inflammatory cells. c High levels of soluble osteopontin in the site of injury helps retain a pool of proliferative myoblasts at the site of injury and promotes further infiltration of the muscles by inflammatory cells. d As osteopontin is immobilized by incorporation into the extracellular matrix terminal differentiation and fusion of myoblasts is favoured over proliferation, thereby promoting the formation of myotubes. e As skeletal muscle regeneration proceeds soluble osteopontin and inflammatory cells are lost from the site of injury, whilst immobilised osteopontin and myoblasts are retained. f During maturation of the regenerated muscle fibre, osteopontin is lost from the site of injury
The importance of macrophages in osteopontin’s effects on the response of skeletal muscle to injury has been highlighted in a study that has reported an age-related increase in osteopontin expression associated with a reduction in the regenerative capacity of skeletal muscle in response to injury (Paliwal et al. 2012). This study reported that osteopontin expression was elevated in serum and in myoblasts and macrophages isolated from injured muscles of old mice (22–24 months) compared to serum, myoblasts and macrophages isolated from injured muscles of young (2–3 months) mice. Furthermore, macrophages, exogenous recombinant osteopontin or osteopontin-neutralising antibodies significantly influenced myoblast proliferation, leading the authors to conclude that osteopontin expression is altered with aging and that increased osteopontin expression contributes to reduced skeletal muscle regeneration in older muscle by reducing the myogenic response of the endogenous myoblasts (Paliwal et al. 2012). Interestingly, this study also reported that injection of an osteopontin neutralising antibody into injured muscles of old mice significantly increased the number of regenerating fibres in muscles 5 days post injection. Conversely, injection of recombinant osteopontin into injured muscles of young mice significantly reduced the number of embryonic myosin positive regenerating fibres in muscles 5 days post injection. These findings appear to contradict the observation of greater numbers of centrally nucleated (regenerated) fibres 5 days post injury in the injured muscles of wild type mice compared to injured muscles of osteopontin- null mice at the same time point (Uaesoontrachoon et al. 2013). However, the difference in the timing of regeneration between the two models used and the transient nature of expression of the marker of regeneration used by (Paliwal et al. 2012) means that at the single time point studied, such comparisons are possibly misleading. Intriguingly, however, the use of recombinant osteopontin and osteopontin neutralising antibodies suggests that modulating osteopontin levels in injured muscles in vivo may be possible and may provide a novel approach to influencing the outcome of muscle repair following injury.
Osteopontin and disease severity in Duchenne muscular dystrophy
Duchenne muscular dystrophy (DMD) is a chronic muscle disease that invariably results in the death of affected individuals during the second decade of life, due to wasting and fibrosis of the muscles involved in respiration. The primary defect in DMD, and in the C57BL/10ScSn- Dmd mdx (mdx) strain of mouse, is the lack of the cytoskeletal protein dystrophin in the muscle fibres of affected individuals (Hoffman et al. 1987); dystrophin links the cytoskeleton of muscle fibres with the extracellular matrix and thus stabilises the sarcolemma (Ervasti 2007). The absence of dystrophin results in increased fragility and damage to muscle fibres in response to contraction (Petrof et al. 1993). The pathology of DMD and mdx muscles is characterised by persistent cycles of spontaneous focal necrosis of muscle fibres, inflammatory infiltration of sites of injury, phagocytosis of damaged sections of fibres by invading macrophages, and muscle fibre regeneration. In the muscles of patients with DMD, muscle fibre regeneration progressively fails, and as a result the muscles develop the typical severe secondary pathology of DMD that is characterised by fibrosis and fibro-fatty replacement of muscle fibres (Partridge 1997). With the exception of the diaphragm, the majority of the muscles of mdx mice retain the ability to regenerate efficiently and do not develop the severe secondary pathology associated with muscle fibrosis (Stedman et al. 1991).
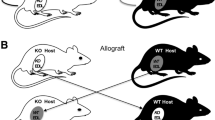
Osteopontin has been described as a component of the inflammatory milieu of dystrophin-deficient muscles (Haslett et al. 2002; Porter et al. 2002; Uaesoontrachoon et al. 2008; Zanotti et al. 2011), and muscles of individuals with dystrophies caused by deficiencies of other proteins (Turk et al. 2006). As osteopontin promotes inflammation and fibrosis in a wide range of tissues (Mori et al. 2008; Pardo et al. 2005), Spencer and colleagues tested the hypothesis that osteopontin may influence inflammation and fibrosis in dystrophin deficient muscles by crossing dystrophin-deficient mdx mice with osteopontin-null mice to produce double mutant mice (DMM), lacking both dystrophin and osteopontin (Vetrone et al. 2009). This study reported that osteopontin deficiency decreased neutrophils, but not macrophages, natural killer T-cells (NKT)-like cells and increased the number of CD3+/CD4+ cells in the inflammatory infiltrate of mdx muscles. The increase in CD3+/CD4+ cells was found to accompany an increase in FoxP3 mRNA expression, suggesting that these cells may represent a population of regulatory T-cells (Vetrone et al. 2009). Functionally, young (4 and 8 week old) DMM mice were found to have greater grip strength and a greater proportion of regenerating fibres in the quadriceps muscles than littermate mdx control mice. By 6 months of age, no significant difference in muscle strength was observed between DMM and mdx mice, however, at this time point collagen type 1 deposition in the diaphragm muscles and cardiac muscle as well as expression of TGFβ, a known fibrotic modulator (Andreetta et al. 2006), were significantly reduced in the DMM muscles. Thus, in mice ablation of osteopontin in dystrophin deficient muscles altered the composition of the inflammatory infiltrate, improved muscle strength and reduced muscle fibrosis, suggesting that chronic overexpression of osteopontin contributes to some of the most damaging aspects of the pathology of dystrophic muscles.
In contrast to the findings of Spencer and colleagues, a recent human genome wide association study found evidence that suggested higher levels of osteopontin expression may be beneficial to the muscles of patients with Duchenne muscular dystrophy. The study in question identified a single nucleotide polymorphism (rs28357094), which is found 66 bp upstream of the transcriptional start site of the human SPP1 gene, as a strong genetic modifier of DMD. The SNP rs28357094 had previously been characterised in human cell lines transfected with promoter constructs linked to a luciferase reporter (Giacopelli et al. 2004). In this system the T allele of rs28357094 was shown to bind SP1/SP3 transcription factors with higher affinity and to lead to higher transcriptional activity than the alternative G allele. Patients carrying the rarer G allele (G/T or G/G) were found to have lower grip strength and decreased age to loss of ambulation than patients homozygous for the T allele (T/T) and the association between genotype and grip strength was found to be strongest in steroid-treated non-ambulatory patients (Pegoraro et al. 2011). Whereas this study identified SPP1 as a significant modifier of disease it did not attempt to identify the mechanism by which SPP1 genotype influenced disease progression in patients with DMD. The most obvious explanation, given the observations by (Giacopelli et al. 2004), was that the T/T genotype results in higher levels of osteopontin than the G/G and G/T genotypes and higher levels of osteopontin had a protective or pro-regenerative effect on dystrophic muscle. Osteopontin expression at the level of mRNA and protein was measured in muscle biopsies from a cohort of patients with DMD who had previously been genotyped with respect to rs28357094 (Piva et al. 2012). Whilst this study found no significant association between the genotype of the SNP rs28357094 and osteopontin expression in muscle it did report significantly higher numbers of CD4+ and CD68+ cells in muscle biopsies from patients of the T/T genotype.
Together these studies have identified apparent roles for osteopontin in the progression of muscular dystrophy, but the precise mechanisms of such effects are still unclear. While the disease-modifying effect of the SNP rs28357094 cannot be attributed to the level of osteopontin expression in muscles from patients with DMD, it is possible that the SNP either influences osteopontin expression levels in other tissues or influences transcription in some other way. Whilst the mechanism of the effect of the SPP1 gene on muscle strength and disease progression in DMD remains elusive, one consequence of the finding that SPP1 genotype influences progression of Duchenne muscular dystrophy is the recommendation that in order to establish functionally homogenous study populations, patients involved in clinical trials should be stratified on the basis of SPP1 genotype (Bello et al. 2012).
Does osteopontin influence skeletal muscle development and postnatal growth?
Recent gene association studies have also identified the SNP rs28357094 as a significant modifier of muscle size in humans (Hoffman et al. 2013). This study attempted to measure the association between rs28357094 and a number of skeletal muscle phenotypes, including muscle size in untrained muscles and the response of muscles to either resistance training or eccentric exercise in a multicentre cohort of young males and females. The study reported that females within the study cohort with the less common combined G/T and G/G genotype of rs28357094 had significantly greater volume of untrained upper arm muscles than females with the more common T/T genotype. No significant associations were observed in males and no association between osteopontin genotype and muscle strength or responses of the upper arm muscle to resistance training were observed in either male or female subjects. Furthermore, this study also reported that in female osteopontin null mice, of the seven muscle groups studied five were found to be significantly smaller than in female wild type controls of the same age. In male osteopontin null mice two of the muscle groups analysed were significantly smaller than in male wild type controls, suggesting that osteopontin contributes to postnatal muscle size in a sexually dimorphic fashion in both mice and humans (Hoffman et al. 2013).
Further evidence for a possible link between osteopontin and muscle size comes from a study that reported differential expression of osteopontin during primary and secondary myogenesis between embryos of two breeds of pigs associated with differing muscularity (Murani et al. 2007). This study reported that during embryogenesis the levels of osteopontin expression in the more muscular Pietrain breed was significant lower than in the muscles of male and female pigs from the Duroc breed. The authors suggest that changes in the level of expression of a number of transcripts including osteopontin reflected a delay in primary myogenesis in the Pietrain breed possibly leading to an increased pool of myogenic cells that subsequently contribute to greater myogenesis and an increase in muscularity in postnatal animals of this breed. This study did not examine whether the differential osteopontin expression was influenced by gender and or whether it caused the different rates of myogenesis, but it does provide support for the hypothesis that osteopontin is involved in the determination of postnatal muscle size. Furthermore, in a separate study the same group reported a SNP in the 3′ end of the first intron of the Duroc Spp1 gene that encodes a C/EBPβ binding site. The less frequent G allele at this SNP was found to disrupt C/EBPβ binding, reducing transcriptional activity as well as influencing splice site selection leading to ubiquitous aberrant splicing of the gene (Murani et al. 2009).
The mechanism by which osteopontin may influence muscle development and or post-natal growth remains unclear. One possibility is that osteopontin functions either as a pro-myogenic growth factor such as IGF1, or as a negative regulator of myogenesis such as TGFβ1 or myostatin (Joulia et al. 2003; Ten Broek et al. 2010). However, the experiments to date suggest that osteopontin’s effects on the size of skeletal muscles are subtle with a decrease in osteopontin expression associated with increased muscle volume in human females and a total loss of expression in mice leading to a significant reduction in muscle weight. Whilst this may be as a result of differences in osteopontin’s function between species, it may also be a reflection of a more complex role that osteopontin plays in determining the size of postnatal skeletal muscles or the influence of alternative forms of the molecule, generated by alternative splicing or post translational modification or processing in the local environment.
Conclusions and future perspectives
To date, studies on the role of osteopontin in skeletal muscle pose almost as many questions as they answer. Current evidence suggests that acute osteopontin expression is required for normal muscle regeneration following a single severe injury (Uaesoontrachoon et al. 2013), but that overexpression of osteopontin reduces the regenerative response to injury in aged muscle (Paliwal et al. 2012). Similarly, in dystrophic mouse muscles chronic overexpression of osteopontin appears to be related to decreased muscle strength and fibrosis in mice (Vetrone et al. 2009), whereas in muscles from patients with Duchenne muscular dystrophy a SNP associated with osteopontin overexpression in vitro, has been found to be a significant positive modifier of the disease (Pegoraro et al. 2011). Currently, little work has been focused on identifying the form or forms of osteopontin found in injured or diseased skeletal muscle. Therefore, one possible explanation for the apparently contradictory observations is that osteopontin plays many roles, some of them antagonistic to others, in injured muscle, and that posttranslational modification, processing, timing, as well as absolute level of osteopontin expression influence the role that it plays. For example, in studies using the whole muscle grafting model or cardiotoxin injection models of muscle injury the muscles are subjected to a single severe injury resulting in a short lived acute overexpression of osteopontin. In contrast, due to the persistent cycles of injury that characterise them, dystrophic muscles are subjected to chronic osteopontin overexpression, furthermore, at least one enzyme responsible for processing osteopontin is known to be up-regulated in the muscles of mdx mice (Porter et al. 2002). Thus limited acute osteopontin overexpression may be beneficial for muscle regeneration by initiating inflammatory infiltration and muscle fibre degeneration in injured muscle, whereas chronic overexpression and processing of osteopontin by enzymes present in dystrophic muscles may lead to chronic inflammation of injured muscles and eventually to fibrosis and functional impairment. Further analysis of the structure and function of osteopontin in injured skeletal muscle may also provide much needed insights into the diverse and at times apparently contradictory roles that osteopontin plays in injured and dystrophic muscles.
Another area of potential future interest arises from osteopontin’s ability to induce expression of Th1-related cytokines by macrophages and T-cells (Ashkar et al. 2000; O’Regan et al. 1999). The importance of different macrophage phenotypes in the early, inflammatory, Th1 dominated phase and the later, regenerative Th2 dominated phase of the response of skeletal muscle to injury has only recently been described (Deng et al. 2012; Tidball 2011; Villalta et al. 2011). The possibility that osteopontin influences macrophage phenotype and therefore inflammation and regeneration in injured and diseased muscle warrants further investigation.
References
Allen RE, Sheehan SM, Taylor RG, Kendall TL, Rice GM (1995) Hepatocyte growth factor activates quiescent skeletal muscle satellite cells in vitro. J Cell Physiol 165:307–312
Andreetta F, Bernasconi P, Baggi F, Ferro P, Oliva L, Arnoldi E, Cornelio F, Mantegazza R, Confalonieri P (2006) Immunomodulation of TGF-beta 1 in mdx mouse inhibits connective tissue proliferation in diaphragm but increases inflammatory response: implications for antifibrotic therapy. J Neuroimmunol 175:77–86
Ashkar S, Weber GF, Panoutsakopoulou V, Sanchirico ME, Jansson M, Zawaideh S, Rittling SR, Denhardt DT, Glimcher MJ, Cantor H (2000) Eta-1 (osteopontin): an early component of type-1 (cell-mediated) immunity. Science 287:860–864
Banerjee A, Apte UM, Smith R, Ramaiah SK (2006) Higher neutrophil infiltration mediated by osteopontin is a likely contributing factor to the increased susceptibility of females to alcoholic liver disease. J Pathol 208:473–485
Barbosa-Souza V, Contin DK, Filho WB, de Araujo AL, Irazusta SP, da Cruz-Hofling MA (2011) Osteopontin, a chemotactic protein with cytokine-like properties, is up-regulated in muscle injury caused by Bothrops lanceolatus (fer-de-lance) snake venom. Toxicon 58:398–409
Bello L, Piva L, Barp A, Taglia A, Picillo E, Vasco G, Pane M, Previtali SC, Torrente Y, Gazzerro E, Motta MC, Grieco GS, Napolitano S, Magri F, D’Amico A, Astrea G, Messina S, Sframeli M, Vita GL, Boffi P, Mongini T, Ferlini A, Gualandi F, Soraru G, Ermani M, Vita G, Battini R, Bertini E, Comi GP, Berardinelli A, Minetti C, Bruno C, Mercuri E, Politano L, Angelini C, Hoffman EP, Pegoraro E (2012) Importance of SPP1 genotype as a covariate in clinical trials in Duchenne muscular dystrophy. Neurology 79:159–162
Berman JS, Serlin D, Li X, Whitley G, Hayes J, Rishikof DC, Ricupero DA, Liaw L, Goetschkes M, O’Regan AW (2004) Altered bleomycin-induced lung fibrosis in osteopontin-deficient mice. Am J Physiol Lung Cell Mol Physiol 286:L1311–L1318
Chambers AF, Wilson SM, Kerkvliet N, O’Malley FP, Harris JF, Casson AG (1996) Osteopontin expression in lung cancer. Lung Cancer 15:311–323
Chen G, Birnbaum RS, Yablonka-Reuveni Z, Quinn LS (1994) Separation of mouse crushed muscle extract into distinct mitogenic activities by heparin affinity chromatography. J Cell Physiol 160:563–572
Christensen B, Kazanecki CC, Petersen TE, Rittling SR, Denhardt DT, Sorensen ES (2007) Cell type-specific post-translational modifications of mouse osteopontin are associated with different adhesive properties. J Biol Chem 282:19463–19472
Collins CA, Olsen I, Zammit PS, Heslop L, Petrie A, Partridge TA, Morgan JE (2005) Stem cell function, self-renewal, and behavioral heterogeneity of cells from the adult muscle satellite cell niche. Cell 122:289–301
Deng B, Wehling-Henricks M, Villalta SA, Wang Y, Tidball JG (2012) IL-10 triggers changes in macrophage phenotype that promote muscle growth and regeneration. J Immunol 189:3669–3680
Denhardt DT, Noda M, O’Regan AW, Pavlin D, Berman JS (2001) Osteopontin as a means to cope with environmental insults: regulation of inflammation, tissue remodeling, and cell survival. J Clin Invest 107:1055–1061
Duvall CL, Taylor WR, Weiss D, Wojtowicz AM, Guldberg RE (2007) Impaired angiogenesis, early callus formation, and late stage remodeling in fracture healing of osteopontin-deficient mice. J Bone Miner Res 22:286–297
Ervasti JM (2007) Dystrophin, its interactions with other proteins, and implications for muscular dystrophy. Biochim Biophys Acta 1772:108–117
Florini JR, Ewton DZ, Magri KA (1991) Hormones, growth factors, and myogenic differentiation. Annu Rev Physiol 53:201–216
Giachelli CM, Lombardi D, Johnson RJ, Murry CE, Almeida M (1998) Evidence for a role of osteopontin in macrophage infiltration in response to pathological stimuli in vivo. Am J Pathol 152:353–358
Giacopelli F, Marciano R, Pistorio A, Catarsi P, Canini S, Karsenty G, Ravazzolo R (2004) Polymorphisms in the osteopontin promoter affect its transcriptional activity. Physiol Genomics 20:87–96
Gimba ER, Tilli TM (2013) Human osteopontin splicing isoforms: known roles, potential clinical applications and activated signaling pathways. Cancer Lett 331:11–17
Hashimoto M, Sun D, Rittling SR, Denhardt DT, Young W (2007) Osteopontin-deficient mice exhibit less inflammation, greater tissue damage, and impaired locomotor recovery from spinal cord injury compared with wild-type controls. J Neurosci 27:3603–3611
Haslett JN, Sanoudou D, Kho AT, Bennett RR, Greenberg SA, Kohane IS, Beggs AH, Kunkel LM (2002) Gene expression comparison of biopsies from Duchenne muscular dystrophy (DMD) and normal skeletal muscle. Proc Natl Acad Sci U S A 99:15000–15005
Hirata A, Masuda S, Tamura T, Kai K, Ojima K, Fukase A, Motoyoshi K, Kamakura K, Miyagoe-Suzuki Y, Takeda S (2003) Expression profiling of cytokines and related genes in regenerating skeletal muscle after cardiotoxin injection: a role for osteopontin. Am J Pathol 163:203–215
Hoffman EP, Brown RH Jr, Kunkel LM (1987) Dystrophin: the protein product of the Duchenne muscular dystrophy locus. Cell 51:919–928
Hoffman EP, Gordish-Dressman H, McLane VD, Devaney JM, Thompson PD, Visich P, Gordon PM, Pescatello LS, Zoeller RF, Moyna NM, Angelopoulos TJ, Pegoraro E, Cox GA, Clarkson PM (2013) Alterations in osteopontin modify muscle size in females in both humans and mice. Med Sci Sports Exerc 45:1060–1068
Inoue M, Shinohara ML (2011) Intracellular osteopontin (iOPN) and immunity. Immunol Res 49:160–172
Joulia D, Bernardi H, Garandel V, Rabenoelina F, Vernus B, Cabello G (2003) Mechanisms involved in the inhibition of myoblast proliferation and differentiation by myostatin. Exp Cell Res 286:263–275
Kazanecki CC, Uzwiak DJ, Denhardt DT (2007) Control of osteopontin signaling and function by post-translational phosphorylation and protein folding. J Cell Biochem 102:912–924
Koh A, da Silva AP, Bansal AK, Bansal M, Sun C, Lee H, Glogauer M, Sodek J, Zohar R (2007) Role of osteopontin in neutrophil function. Immunology 122:466–475
Lescaudron L, Peltekian E, Fontaine-Perus J, Paulin D, Zampieri M, Garcia L, Parrish E (1999) Blood borne macrophages are essential for the triggering of muscle regeneration following muscle transplant. Neuromuscul Disord 9:72–80
Liaw L, Almeida M, Hart CE, Schwartz SM, Giachelli CM (1994) Osteopontin promotes vascular cell adhesion and spreading and is chemotactic for smooth muscle cells in vitro. Circ Res 74:214–224
Mori R, Shaw TJ, Martin P (2008) Molecular mechanisms linking wound inflammation and fibrosis: knockdown of osteopontin leads to rapid repair and reduced scarring. J Exp Med 205:43–51
Mukherjee BB, Nemir M, Beninati S, Cordella-Miele E, Singh K, Chackalaparampil I, Shanmugam V, DeVouge MW, Mukherjee AB (1995) Interaction of osteopontin with fibronectin and other extracellular matrix molecules. Ann N Y Acad Sci 760:201–212
Murani E, Muraniova M, Ponsuksili S, Schellander K, Wimmers K (2007) Identification of genes differentially expressed during prenatal development of skeletal muscle in two pig breeds differing in muscularity. BMC Dev Biol 7:109
Murani E, Ponsuksili S, Seyfert HM, Shi X, Wimmers K (2009) Dual effect of a single nucleotide polymorphism in the first intron of the porcine secreted phosphoprotein 1 gene: allele-specific binding of C/EBP beta and activation of aberrant splicing. BMC Mol Biol 10:96
Nguyen HX, Tidball JG (2003) Interactions between neutrophils and macrophages promote macrophage killing of rat muscle cells in vitro. J Physiol 547:125–132
O’Brien ER, Garvin MR, Stewart DK, Hinohara T, Simpson JB, Schwartz SM, Giachelli CM (1994) Osteopontin is synthesized by macrophage, smooth muscle, and endothelial cells in primary and restenotic human coronary atherosclerotic plaques. Arterioscler Thromb 14:1648–1656
O’Regan A, Berman JS (2000) Osteopontin: a key cytokine in cell-mediated and granulomatous inflammation. Int J Exp Pathol 81:373–390
O’Regan AW, Chupp GL, Lowry JA, Goetschkes M, Mulligan N, Berman JS (1999) Osteopontin is associated with T cells in sarcoid granulomas and has T cell adhesive and cytokine-like properties in vitro. J Immunol 162:1024–1031
Paliwal P, Pishesha N, Wijaya D, Conboy IM (2012) Age dependent increase in the levels of osteopontin inhibits skeletal muscle regeneration. Aging (Albany NY) 4:553–566
Pardo A, Gibson K, Cisneros J, Richards TJ, Yang Y, Becerril C, Yousem S, Herrera I, Ruiz V, Selman M, Kaminski N (2005) Up-regulation and profibrotic role of osteopontin in human idiopathic pulmonary fibrosis. PLoS Med 2:e251
Partridge TA (1997) Models of dystrophinopathy, pathological mechanisms and assessment of therapies. In: Brown SC, Lucy JA (eds) Dystrophin: Gene Protein and Cell Biology. Cambridge University Press, Cambridge, pp 310–311
Patarca R, Freeman GJ, Singh RP, Wei FY, Durfee T, Blattner F, Regnier DC, Kozak CA, Mock BA, Morse HC 3rd et al (1989) Structural and functional studies of the early T lymphocyte activation 1 (Eta-1) gene. Definition of a novel T cell-dependent response associated with genetic resistance to bacterial infection. J Exp Med 170:145–161
Pegoraro E, Hoffman EP, Piva L, Gavassini BF, Cagnin S, Ermani M, Bello L, Soraru G, Pacchioni B, Bonifati MD, Lanfranchi G, Angelini C, Kesari A, Lee I, Gordish-Dressman H, Devaney JM, McDonald CM, Cooperative International Neuromuscular Research, G (2011) SPP1 genotype is a determinant of disease severity in Duchenne muscular dystrophy. Neurology 76:219–226
Petrof BJ, Shrager JB, Stedman HH, Kelly AM, Sweeney HL (1993) Dystrophin protects the sarcolemma from stresses developed during muscle contraction. Proc Natl Acad Sci U S A 90:3710–3714
Piva L, Gavassini BF, Bello L, Fanin M, Soraru G, Barp A, Ermani M, Angelini C, Hoffman EP, Pegoraro E (2012) TGFBR2 but not SPP1 genotype modulates osteopontin expression in Duchenne muscular dystrophy muscle. J Pathol 228:251–259
Porter JD, Khanna S, Kaminski HJ, Rao JS, Merriam AP, Richmonds CR, Leahy P, Li J, Guo W, Andrade FH (2002) A chronic inflammatory response dominates the skeletal muscle molecular signature in dystrophin-deficient mdx mice. Hum Mol Genet 11:263–272
Saitoh Y, Kuratsu J, Takeshima H, Yamamoto S, Ushio Y (1995) Expression of osteopontin in human glioma. Its correlation with the malignancy. Lab Invest 72:55–63
Sam F, Xie Z, Ooi H, Kerstetter DL, Colucci WS, Singh M, Singh K (2004) Mice lacking osteopontin exhibit increased left ventricular dilation and reduced fibrosis after aldosterone infusion. Am J Hypertens 17:188–193
Standal T, Borset M, Sundan A (2004) Role of osteopontin in adhesion, migration, cell survival and bone remodeling. Exp Oncol 26:179–184
Stedman HH, Sweeney HL, Shrager JB, Maguire HC, Panettieri RA, Petrof B, Narusawa M, Leferovich JM, Sladky JT, Kelly AM (1991) The mdx mouse diaphragm reproduces the degenerative changes of Duchenne muscular dystrophy. Nature 352:536–539
Tatsumi R, Anderson JE, Nevoret CJ, Halevy O, Allen RE (1998) HGF/SF is present in normal adult skeletal muscle and is capable of activating satellite cells. Dev Biol 194:114–128
Ten Broek RW, Grefte S, Von den Hoff JW (2010) Regulatory factors and cell populations involved in skeletal muscle regeneration. J Cell Physiol 224:7–16
Tidball JG (2005) Inflammatory processes in muscle injury and repair. Am J Physiol Regul Integr Comp Physiol 288:R345–R353
Tidball JG (2011) Mechanisms of muscle injury, repair, and regeneration. Compr Physiol 1:2029–2062
Turk R, Sterrenburg E, van der Wees CG, de Meijer EJ, de Menezes RX, Groh S, Campbell KP, Noguchi S, van Ommen GJ, den Dunnen JT, ‘t Hoen PA (2006) Common pathological mechanisms in mouse models for muscular dystrophies. FASEB J 20:127–129
Uaesoontrachoon K, Yoo HJ, Tudor EM, Pike RN, Mackie EJ, Pagel CN (2008) Osteopontin and skeletal muscle myoblasts: association with muscle regeneration and regulation of myoblast function in vitro. Int J Biochem Cell Biol 40:2303–2314
Uaesoontrachoon K, Wasgewatte Wijesinghe DK, Mackie EJ, Pagel CN (2013) Osteopontin deficiency delays inflammatory infiltration and the onset of muscle regeneration in a mouse model of muscle injury. Dis Model Mech 6:197–205
Vetrone SA, Montecino-Rodriguez E, Kudryashova E, Kramerova I, Hoffman EP, Liu SD, Miceli MC, Spencer MJ (2009) Osteopontin promotes fibrosis in dystrophic mouse muscle by modulating immune cell subsets and intramuscular TGF-beta. J Clin Invest 119:1583–1594
Villalta SA, Deng B, Rinaldi C, Wehling-Henricks M, Tidball JG (2011) IFN-gamma promotes muscle damage in the mdx mouse model of Duchenne muscular dystrophy by suppressing M2 macrophage activation and inhibiting muscle cell proliferation. J Immunol 187:5419–5428
von der Mark K, Ocalan M (1989) Antagonistic effects of laminin and fibronectin on the expression of the myogenic phenotype. Differentiation 40:150–157
Weinreb M, Shinar D, Rodan GA (1990) Different pattern of alkaline phosphatase, osteopontin, and osteocalcin expression in developing rat bone visualized by in situ hybridization. J Bone Miner Res 5:831–842
Yokosaki Y, Matsuura N, Sasaki T, Murakami I, Schneider H, Higashiyama S, Saitoh Y, Yamakido M, Taooka Y, Sheppard D (1999) The integrin alpha(9)beta(1) binds to a novel recognition sequence (SVVYGLR) in the thrombin-cleaved amino-terminal fragment of osteopontin. J Biol Chem 274:36328–36334
Zammit PS, Partridge TA, Yablonka-Reuveni Z (2006) The skeletal muscle satellite cell: the stem cell that came in from the cold. J Histochem Cytochem 54:1177–1191
Zanotti S, Gibertini S, Di Blasi C, Cappelletti C, Bernasconi P, Mantegazza R, Morandi L, Mora M (2011) Osteopontin is highly expressed in severely dystrophic muscle and seems to play a role in muscle regeneration and fibrosis. Histopathology 59:1215–1228
Zohar R, Lee W, Arora P, Cheifetz S, McCulloch C, Sodek J (1997) Single cell analysis of intracellular osteopontin in osteogenic cultures of fetal rat calvarial cells. J Cell Physiol 170:88–100
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pagel, C.N., Wasgewatte Wijesinghe, D.K., Taghavi Esfandouni, N. et al. Osteopontin, inflammation and myogenesis: influencing regeneration, fibrosis and size of skeletal muscle. J. Cell Commun. Signal. 8, 95–103 (2014). https://doi.org/10.1007/s12079-013-0217-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12079-013-0217-3