Abstract
Nod-like receptor protein 3 (NLRP3)-associated neuroinflammation mediated by activated microglia is involved in the pathogenesis of depression. The role of the pore-forming protein gasdermin D (GSDMD), a newly identified pyroptosis executioner downstream of NLRP3 inflammasome mediating inflammatory programmed cell death, in depression has not been well defined. Here, we provide evidence that paeoniflorin (PF), a monoterpene glycoside compound derived from Paeonia lactiflora, ameliorated reserpine-induced mouse depression-like behaviors, characterized as increased mobility time in tail suspension test and forced swimming test, as well as the abnormal alteration of synaptic plasticity in the depressive hippocampus. The molecular docking simulation predicted that PF would interact with C-terminus of GSDMD. We further demonstrated that PF administration inhibited the enhanced expression of GSDMD which mainly distributed in microglia, along with the proteins involved in pyroptosis signaling transduction including caspase (CASP)-11, CASP-1, NLRP3, and interleukin (IL)-1β in the hippocampus of mice treated with reserpine. And also, PF prevented lipopolysaccharide (LPS) and adenosine triphosphate (ATP)-induced pyroptosis in murine N9 microglia in vitro, evidenced by inhibiting the expression of CASP-11, NLRP3, CASP-1 cleavage, as well as IL-1β. Furthermore, VX-765, an effective and selective inhibitor for CASP-1 activation, reduced the expression of inflammasome and pyroptosis-associated proteins in over-activated N9 and also facilitated PF-mediated inhibition of pyroptosis synergistically. Collectively, the data indicated that PF exerted antidepressant effects, alleviating neuroinflammation through inhibiting CASP-11-dependent pyroptosis signaling transduction induced by over-activated microglia in the hippocampus of mice treated with reserpine. Thus, GSDMD-mediated pyroptosis in activated microglia is a previously unrecognized inflammatory mechanism of depression and represents a unique therapeutic opportunity for mitigating depression given PF administration.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Depression is the leading cause of disability worldwide with global distribution of over 300 million people suffering from this psychiatric disorder, which is characterized by perpetual depressed mood, recurrent thoughts of death and suicide, social isolation, and anhedonia [1]. Unfortunately, 30–50% of depressed individuals are resistant to current antidepressant treatments. The mechanisms underlying depression include an imbalance in monoamine neurotransmission, impaired hippocampal neurogenesis, abnormal synaptic plasticity, as well as excessive neuroinflammation. More and more evidence underpins that neuroinflammation and inflammatory cytokines/chemokines orchestrate brain signal process involved in the psychopathology of depression [2, 3].
Notably, studies have revealed over-activated microglia in postmortem brain samples [4] and elevated levels of pro-inflammatory interleukin (IL)-1β, IL-6, tumor necrosis factor-α (TNF-α), and C-reactive protein (CRP) in serum/plasma and cerebrospinal fluid of depressed patients in the absence of comorbid somatic diseases [2, 3], suggesting that activation of inflammatory pathways may represent a significant component in the pathophysiology of depression [5]. Antidepressant treatments influencing inflammatory processes, downregulating microglial activation [6], specifically reducing peripheral IL-6, TNF-α, and the monocyte chemoattractant protein-1 (MCP-1) in depressed individuals [3, 7] further support the crucial roles of neuroinflammation in the etiology of depression. Excessive inflammation leads to the abnormal alterations in synaptic plasticity both morphologically and functionally, resulting in the dysfunction of emotion processing. Inflammasome-related inflammation is an ongoing process in psychiatric patients during diseased states [8]. Inflammasomes are cytosolic multiprotein complexes that are vital players of innate immunity and especially in the initiation of inflammatory responses in myeloid cells [9]. The NOD-like receptors (NLR) family, pyrin domain containing inflammasome (NLRP) is the most studied and best characterized protein complex during inflammation. Among these, NLRP3 inflammasome appears to be a central mediator by which psychological and physical stressors contribute to the development of depression-like symptoms.
Elevated expression levels of NLRP3 inflammasome and caspase (CASP)-1 in the blood cells and frontal cortex from depression patients are associated with higher concentrations of IL-1β and IL-18 in blood, correlating with depression severity [10, 11] and are further observed in rodent models of depression [12, 13]. The mitigation of depressive-like behaviors (DLB) by the blockade of NLRP3 further confirms that NLRP3 is a common mediator in the development of depression [14]. Intriguingly, CASP-1 KO resulted in the improved DLB, and administration of the CASP-1 inhibitor minocycline also ameliorated DLB [15]. Moreover, mice lacking CASP-1 are resistant to LPS-induced DLB, further supports the role of inflammasomes in depression [16]. It should also be noted that antidepressants can block or reverse stress-induced the activation of microglia and inflammasome [10]. Collectively, NLRP inflammasomes are central setscrews between stress, immune activation, and depression and may also link the severity and disease prognosis to pro-inflammatory cytokines and inflammasome platform [17].
Following NLRP3 inflammasome activation, as inflammasomes comprised-multiprotein complexes sense stress directly or indirectly, cleaved CASP-1 will cleave pro-IL-1β into its biological active form, mature IL-1β, and finally induces pyroptosis. Gasdermin D (GSDMD) is a recently identified pore-forming protein, which mediates pyroptosis [18, 19]. Pro-inflammatory caspases (CASP-1, CASP-4, CASP-5, and CASP-11) cleave the linker between the N-terminal and C-terminal domains in GSDMD, then N-terminal GSDMD domain fragments translocate to the plasma membrane forming membrane pores, leading to lytic cell death or the secretion of processed IL-1β and IL-18 through pores [20]. This type of inflammatory necrosis mediated by GSDMD accumulation occurs predominantly in macrophages, monocytes, and dendritic cells microglia and central nervous system (CNS) [21]. The disturbed neuroimmune functions and reciprocal neuron-microglia interactions act either as consequences or causes of this mental disease [2, 3, 22]. Microglia, as an innate immune cell in the CNS, has a high degree of morphological and functional plasticity and fulfills important immunological functions in the brain by responding to pathological stresses via phagocytosis and/or secreting inflammatory mediators. Microglia is activated to lead to pyroptosis and further aggravates neuroinflammation; therefore, they are regarded to play crucial roles in neuroinflammation and are suggested to contribute to various psychiatric disorders [23]. It is evidenced that abnormal alterations of synaptic plasticity contribute to the development of depression, and microglia eliminate or prune weak and inappropriate synapses in the synaptogenic period [24], highlighting the complexity and crucial role of microglia in synapse formation in the CNS. Chronic administration of the microglial activation inhibitor minocycline completely abolished the effect of peripheral inflammation on the field potentials and synaptic plasticity (LTP and LTD) [25]. However, to date, there have no reports on a pathophysiological role for GSDMD in neuroinflammation induced by over-activated microglia related to plasticity regulation in depression pathogenesis.
Paeoniflorin (PF) is one of the principal bioactive components derived from the root of Paeoniae Radix/P. lactiflora Pallas, a traditional Chinese herbal which has been widely used in the treatment of CNS diseases. It has been reported that PF possesses various pharmacological activities including antioxidant, antiinflammation, and neuroprotective effects on various types of cells [26, 27]. As a natural antioxidant, PF penetrates through the blood-brain barrier [28], and the neuroprotective effects of PF have been evidenced both in vivo and in vitro [29]. PF ameliorated declines in learning and memory capacity in AD mice and cerebral hypoperfusion model [30]. PF alleviated depression-like behaviors induced by chronic unpredictable mild stress by exerting antiinflammation [31]. We previously found that PF protected neural stem cells (NSCs) against oxidative stress injury and promoted NSCs proliferation through PI3K/Akt-1 signaling pathway [32]; thus, PF exerted a potential antidepressant effect by improving the impaired neurogenesis occurs in depression. All the collected evidence indicated that PF could offer antidepression effects through multi-targets.
In this study, we demonstrated that PF exerted antidepressant effects, repressing neuroinflammation through inhibiting CASP-11-dependent pyroptosis signaling transduction induced by over-activated microglia in the depressive hippocampus. Thus, GSDMD-mediated pyroptosis in activated microglia is a previously unrecognized inflammatory mechanism of depression and represents a unique therapeutic opportunity for mitigating depression given PF administration.
Materials and Methods
Materials
Reserpine (RESP), fluoxetine (FLXT), Hoechst 33258, lipopolysaccharide (LPS, from Escherichia coli 0111: B4), adenosine 5’-triphosphate (ATP) disodium hydrate, and antibody for β-actin were obtained from Sigma-Aldrich (St. Louis, MO, USA). RPMI1640 cell culture media was purchased from Biochrom (Berlin, Germany). Fetal bovine serum (FBS) was provided by Invitrogen (Carlsbad, CA, USA). Antibodies for CASP-11 (ab180673), GSDMD (ab219800), CASP-1 (ab179515), IL-1β (ab972), Iba-1 (ab48004), CD68 (ab31630), and NeuN (ab104224) were obtained from Abcam (Cambridge, UK, USA), and antibody for NLRP3 (Cat#15101) was from Cell Signaling Technology (Danvers, MA, USA). All secondary antibodies conjugated with horseradish peroxidase (HRP) were purchased from Santa Cruz (CA, USA). Alexa Fluor 488 and 594 goat IgG were purchased from Molecular Probes (Eugene, OR, USA). BCA Kit, M-PER Protein Extraction Buffer, and enhanced chemiluminescent solution (ECL) were obtained from Pierce (Rockford, IL, USA). PVDF membrane was purchased from Roche (Mannheim, Germany). VX-765 (purity > 98%) was purchased from Selleckchem (Shanghai, China) and dissolved in sterile 0.1% DMSO to desire concentrations before use. PF (purity > 98%) was purchased from Shanghai Pure One Biotechnology (Shanghai, China) and reconstituted in sterile 0.9% saline to desire concentrations before use. Goat serum was obtained from BOSTER (Wuhan, China). All chemicals were obtained from Sigma unless otherwise stated.
Acute Depression Model and Drug Treatment
Six- to eight-week-old C57BL/6 male mice (body weight 20–25 g) were obtained from the Experimental Animal Center of Fourth Military Medical University (Certificate No. 201000082, Grade II). All experimental procedures were approved by the Ethics Committee of Fourth Military Medical University (Approval reference number No. KY20193145) in full accordance with the ethical guidelines of the National Institutes of Health for the care and use of laboratory animals. The room temperature (RT) was maintained at controlled 22 ± 24 °C with humidity (50–60%), and a reversed 12:12-h light/dark cycle with ad libitum access to food and water in the animal facilities. All the operations, including intragastric and intraperitoneal injection and behavioral test, were carried out gently and expertly. Before testing, the animals need to adapt to laboratory conditions for at least 1 week. Every effort was made to minimize the number of animals used and their suffering.
Thirty-six mice were pre-designated from 1 to 36 by an experimenter blind to the experiment design, and all the mice were randomly divided into six groups using a computer randomization table. There were 6 groups included in the study, Control, RESP model, RESP + FLXT, RESP + PF (10, 20, 40 mg/kg), and 6 mice of the same group were homed in one cage which was made of opaque polypropylene (380 × 325 × 180 mm, By-DSLH380). The model of acute depression was established by RESP (1 mg/kg) injected intraperitoneally (i.p.) once daily for 3 days (day 1–day 3) as described previously. The mice received PF (10, 20, 40 mg/kg) or vehicle (saline, 10 mL/kg) by intragastric administration (i.g.) once daily for 3 days consecutively before RESP insult and then followed by an additional 4-day administration (day 4–day 7). FLXT (20 mg/kg), a selective serotonin reuptake inhibitor (SSRI), served as a positive antidepressant as reported previously [14]. All experiments were performed at day 7 between 8:00 a.m. and 2:00 p.m. to minimize circadian influences after the last treatment. Animal DLB were evaluated after habituation for 15 min in the testing room. The brain tissues were collected for immunofluorescence staining and Western blot analysis after behavior tests.
Behavioral Tests
Animal DLB were evaluated after habituation for 15 min in the testing room. Open field test (OFT) was carried out first, followed by tail suspension test (TST), and finally forced swimming test (FST). Double blinding was used in behavioral tests, and all animals were subjected to all behavioral tests. The experiments were conducted and repeated three times.
Tail Suspension Test
Tail suspension test (TST) was performed in a quiet room as described previously [33]. Each mouse was suspended 50 cm above the floor and a small piece of adhesive taped to a wooden stick near the end of the mice tail about 2 cm, and the mice views were surrounded by a barrier. The mice tail test lasted 6 min, the total duration of immobility was recorded during the last 4 min of the test. Mice were considered as immobile when they showed hopelessness, in which the mice stopped struggling to overcome the abnormal position, and were nearly immobile or completely motionless after a period of struggling activity.
Forced Swimming Test
Forced swimming test (FST) is chosen to assess the desperate behavior as one of the most widely used tests of antidepressant actions. FST procedure was carried out according to the slightly modified method as previously described [33]. Mice were placed individually in a glass cylinder (height 25 cm, diameter 10 cm) filled with water to a depth of 11 cm at temperature 23–25 °C and forced to swim for 6 min; the lighting level (lux) around the glass cylinders is ≤ 0.005 lx. After the initial 2 min of vigorous activity, the total duration of immobility was recorded during the last 4 min of the test. The mice were accepted as immobile when they stopped swimming and kept motionless, making only necessary movements for keeping their heads above the water. Water in the beakers was regularly changed between subjects. The immobility time was recorded by a trained observer who was blind to the experiment design with the help of cumulative stopwatches. Data obtained in groups were expressed as means (in s) ± the standard error of the mean (SEM).
Open Field Test
To assess the effects of PF on spontaneous locomotor activities, each mouse was placed into the center of an open field apparatus (50 × 50 × 60 cm) and allowed to explore freely around the open field. The light level < 50 lx was chosen because of little influence on mice behavioral. The number of crossings (squares crossed) and time spent in central area were recorded during a test period of 15 min. The paths of the animal were recorded by a video camera above the arena and analyzed by a video tracking system (DigBehav system, Yishu Co., Ltd.). The arena was carefully cleaned with 70% alcohol and rinsed with water after each test. Mice received behavior tests 30 min after PF or FLXT treatment.
Golgi-Cox Staining and Spine Density Analysis
Golgi staining was performed as described previously [34]. Briefly, the mice brains were harvested after behavior tests and immersed in Golgi-Cox solution (1% potassium dichromate, 1% mercuric chloride, 0.75% potassium chromate), sealing tightly in the dark for 12 days at RT. Hippocampus sections (120 μm thick) were mounted onto slides using neutral balsam, and pictures were photographed under Olympus BX51 light microscope with a 100×/NA 1.4 oil immersion lens. Analyses were performed on basilar dendrites from CA1 neurons, total length of 100 μm. Spines of three dendrites from selected neuron were counted, and spine densities were measured by counting the number of spines of all types at 10-μm intervals on dendrites and analyzed using ImageJ. Statistical analyses for spine count were performed by pooling spine counts of all neurons after different treatments. All analyses were conducted by an experimenter blind to treatment.
In Silico Docking Study of PF with C-terminus of GSDMD Binding Protein
A study of in silico docking of PF with C-terminus of GSDMD binding protein was conducted. For this purpose, different ligands were prepared and optimized using the Prepare Ligands module, a protocol of Discovery Studio 3.5 (Accelrys Inc.), then converted to the SD file format. GSDMD binding protein (PDB code: 6AO3) structures were downloaded from the RCSB website (http://www.pdb.org) in PDB format. Before docking, the original crystal ligands and water molecules were removed from the protein-ligand complexes. Hydrogen atoms were added by application of CHARMM force field and the Momany-Rone partial charge default settings in Discovery Studio 3.5. The ligand-binding site was extracted from the PDB site. Docking analyses of PF with C-terminus of GSDMD in the presence of crystal ligands were performed by means of the CDOCKER module, which is accurate when active sites are known. This method meets the requirements of experimental verification. The number of generated poses was set to 100 for each ligand, and default settings were selected for other parameters.
Western Blot Analysis
Protein samples were harvested from mice hippocampus or cultured N9 microglial cells after various treatments. Total proteins were lysed by M-PER Protein Extraction Buffer according to the manufacturer’s instructions, and the protein concentrations were determined using a BCA Kit. Equal amounts of protein aliquots were used to check the expression levels of target proteins using anti-CASP-11 (1:1500), anti-GSDMD (1:1000), anti-CASP-1 (1:1000), anti-NLRP3 (1:1000), and anti-IL-1β (1:1000) through 10% SDS-PAGE gel electrophoresis, and β-actin served as a loading control. After incubation with the appropriate HRP-conjugated secondary antibody, the proteins were visualized using ECL. The density of immunoblots was conducted using ChemiDoc XRS (Bio-Rad, Hercules) and quantified using Quantity One version 4.1.0 (Bio-Rad).
Immunofluorescence
Mice were anesthetized with sodium pentobarbital (40 mg/kg, i.p.) after the last behavior test, and the depth of anesthesia mainly depended on the disappearance of corneal reflex, the response to clamp stimulation, and muscle relaxation. Then the mice were perfused intracardially with saline followed by 4% paraformaldehyde (PFA) in 0.1 M phosphate buffer solution (PBS, pH 7.4). After dehydration, sequential coronal sections of hippocampus (30 μm) were acquired on CM3050S freezing microtome (Leica, Germany), collected sequentially in PBS as free-floating sections. The cryo-sections containing hippocampus were washed with 0.1% Triton X-100 in PBS for 30 min and blocked in 10% goat serum for 1 h at RT. The slices were incubated with primary antibodies including anti-GSDMD (1:200), anti-Iba-1 (1:200), anti-CD68 (1:200), anti-NeuN (1:200) overnight at 4 °C, followed by Alexa Fluor secondary antibody incubation. Nuclei were counterstained with Hoechst 33258. Fluorescent signals were photographed and analyzed using confocal fluorescence microscopy (Olympus, Japan).
Cell Culture and Treatment
Cell line of murine microglia N9 were obtained and cultured in Memorial Institute RPMI1640 medium containing 10% FBS, 100 IU/mL penicillin, and 100 μg/mL streptomycin. The cells were incubated at 37 °C in the presence of 5% CO2, and the culture medium was changed daily. The maximum passage of the murine microglia N9 used did not exceed 20 generations. Cells were pretreated with PF (0, 1, 10, 100 μM) for 12 h and then stimulated with LPS (1 μg/mL) for 4 h and ATP (2.5 mM) for 0.5 h. For the experiment utilizing inhibitors, cells were pretreated with PF (10 μM) and/or VX-765 (10 μM) for 12 h and then treated with or without LPS/ATP as before. Samples are collected by centrifugation for subsequent experiments.
Statistical Analysis
Results were presented as the mean and SEM (mean ± SEM). The data were analyzed by one-way ANOVA followed by a post hoc Tukey’s test to compare the various groups. In all cases, p < 0.05 was considered statistically significant. All statistical analysis was performed using GraphPad Prism 7.03 and SPSS statistical software package version 20.0.
Results
Antidepressant Effects of PF Treatment on RESP-Induced Depression-Like Behavior in Mice
Reserpine treatment in rodents is a well-accepted model to induce depression-like behaviors that mimics monoamine dysfunction implicated in the development of depression15. The procedure of animal study was carried out as Fig. 1a. Three-day injection of RESP (1 mg/kg, i.p.) significantly resulted in behavioral despair in mice, which was manifested as an increase in total immobility duration of 189.00 ± 8.51 s compared with control (Ctrl) group of 106.60 ± 8.22 s (p < 0.01; Fig. 1b) in TST, and increased immobility time of 150.10 ± 11.19 s compared with Ctrl group of 73.29 ± 5.74 s (p < 0.01; Fig. 1c) in FST, indicating that RESP injection could lead to mice DLB. However, PF administration ameliorated DLB by reducing the immobility duration to 133.10 ± 10.22 s in 20 mg/kg group and 127.30 ± 7.02 s in 40 mg/kg group (p < 0.01, vs. RESP-insulted group; Fig. 1b) in TST, as well as decreasing the immobility time to 95.86 ± 5.88 s in 20 mg/kg group and 89.71 ± 8.01 s in 40 mg/kg (p < 0.05, vs. RESP-insulted group; Fig. 1c) in reserpinized mice evaluated by FST, showing the potential antidepressant effects of PF. FLXT (20 mg/kg), a classic SSRI, served as a positive antidepressant and reduced the immobility time of reserpinized mice to 127.00 ± 11.91 s (p < 0.05, vs. RESP-insulted group; Fig. 1b) in TST and 81.14 ± 8.15 s in FST (p < 0.01, vs. RESP-insulted group; Fig. 1c) as expected.
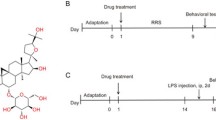
PF administration ameliorated depression-like behaviors in reserpinized mice. Mice were treated with reserpine (RESP, 1 mg/kg) by i.p injection for 3 days followed by PF administration (0, 10, 20, 40 mg/kg, i.g.) for 7 days, and fluoxetine (FLXT, 20 mg/kg) treatment served as a positive antidepressant. a Schematic illustration of the procedure for the experiment (detailed description showed in the Materials and Methods part). b The immobility time for each group were determined by tail suspension test (TST) and c forced swimming test (FST). d The total distance traveled and e time spent in the central area in each group were determined in open field test (OFT). Each value represents the mean ± SEM of three independent experiments (n = 6 mice/per group, *p < 0.05, **p < 0.01, ***p < 0.001, vs. Ctrl group; #p < 0.05, ##p < 0.01, ###p < 0.001, vs. RESP-insulted mice)
In addition, spontaneous locomotor activity of mice from each group was evaluated using OFT. The reserpinized mice showed DLB as evidenced by decreased locomotor activity, and the total distance in RESP-insulted group decreased to 11.87 ± 0.79 m compared with 31.36 ± 2.081 m in Ctrl group (p < 0.001; Fig. 1d). Accordingly, time spent in the central area reduced to 22.92 ± 1.50 s in reserpinized mice compared with 64.97 ± 1.70 s in Ctrl mice (p < 0.001; Fig. 1e). PF administration increased the total distance to 18.06 ± 0.70 m in 20 mg/kg group and 22.32 ± 0.78 in 40 mg/kg group (p < 0.01, PF 20 mg/kg group vs. RESP-insulted group; p < 0.001, PF 40 mg/kg group vs. RESP-insulted group; Fig. 1d); and the time spent in the central area increased to 36.41 ± 1.24 s in 10 mg/kg group, 45.43 ± 1.17 s in 20 mg/kg group, and 51.53 ± 1.42 s in 40 mg/kg group after PF treatment (p < 0.001, vs. RESP-insulted group; Fig. 1e). Similarly, FLXT administration (20 mg/kg) elevated the total distance of reserpinized mice to 25.70 ± 0.95 m in OFT, and the time spent in the central to 52.93 ± 2.36 s in reserpinized mice in OFT (p < 0.001, vs. RESP-insulted group; Fig. 1d, e). The effects of PF (10, 20, 40 mg/kg) and FLXT (20 mg/kg) on basal conditions were performed, and the data excluded the possibilities of PF on control mice (data not shown).
PF Administration Rescued the Reduction of Dendritic Spines within CA1 Neurons in Reserpine-Induced Depression Mice
Loss of spine in the hippocampus region has been ascribed to depression development. Given RESP-induced mice DLB, we predicted that PF administration would affect spine density upon RESP insult. In this study, Golgi-Cox-staining of CA1 pyramidal neurons was carried out to evaluate the changes of spine (Fig. 2a). Consistent with this hypothesis, the spine density in CA1 in reserpinized mice reduced to 7.43 ± 0.78 per 10 μm2 compared with 19.57 ± 0.84 per 10 μm2 in Ctrl mice (p < 0.001; Fig. 2b). PF administration restored the spine density to 12.71 ± 1.19 per 10 μm2 in 20 mg/kg group, and FLXT treatment increased the spine density to 15.57 ± 1.23 per 10 μm2 (p < 0.05, PF 20 mg/kg group vs. RESP-insulted group; p < 0.01, FLXT group vs. RESP-insulted group; Fig. 2b). Therefore, we demonstrated that PF rescued the reduction of dendritic spines within CA1 neurons in the hippocampus of mice treated with reserpine, and this may contribute to the alleviation of DLB upon RESP insult.
PF treatment reversed the reduction of spine density in reserpinized CA1 area. Mice were insulted with reserpine (RESP, 1 mg/kg) by i.p injection for 3 days followed by PF treatment (0, 20 mg/kg, i.g.) for 7 days, and fluoxetine (FLXT, 20 mg/kg) treatment served as a positive antidepressant. a Representative sample for Golgi-Cox staining of CA1 pyramidal neurons for spine counting. b Left: representative images of basilar dendrites from Ctrl, RESP, RESP + FLXT, and RESP + PF (20 mg/kg) groups. Right: summary of spine counts from basilar dendrites. n = 40 neurons/4 mice per group; one-way ANOVA with LSD test, ***p < 0.001, vs. Ctrl mice; #p < 0.05, ##p < 0.01, vs. RESP-insulted mice
Structural Interactions of PF with C-Terminus of GSDMD
It is evidenced that NLRP inflammasomes links neuroinflammation to depression psychopathology. GSDMD, a recently identified pore-forming protein, mediates pyroptosis induced by NLRP3 inflammasomes, leading to lytic cell death or the secretion of IL-1β. To further explore the potential mechanism of PF-mediated antidepressant related to pyroptosis processed by GSDMD, molecular docking analysis was conducted. PF (cyan sticks in Fig. 3a) was docked to the C-terminus of GSDMD (cyan and blue ribbon in Fig. 3a) by means of the CDOCKER module of Discovery Studio (Accelrys Inc., San Diego, CA, USA). The hydroxide radical (OH) group at the chromen-one site of PF (Fig. 3a) interacts with C-terminus of GSDMD at the TYR376 site (green symbol in Fig. 3b) via hydrogen-bonding, which coincides well with the crystal ligand ifenprodil, a C-terminus of GSDMD agonist (yellow sticks in Fig. 3a). This suggests that PF could bind to C-terminus of GSDMD. Moreover, the phenyl moiety of PF can form π-π stacked interactions with TYR376, thus contributing to the stability of the protein-ligand complex (pink symbol in Fig. 3b).
Structural interactions of PF with C-terminus of GSDMD. a Structural representation of PF binding to C-terminus of GSDMD (PDB: 6AO3) as inferred from docking simulations (left). Ifenprodil was shown as yellow sticks, and PF was shown as cyan sticks (right). The –OH group of PF formed hydrogen bond with TYR376 C-terminus of GSDMD. The best-docked pose of PF in the active site coincided well with the crystal ligand ifenprodil. b 2D diagram of interaction between PF and C-terminus of GSDMD showed the major binding sites and bonding forces
PF Administration Inhibited the Elevated Pyroptosis Signaling Transduction CASP-11/GSDMD upon RESP Insult
The molecular docking analysis predicted the interaction of PF with GSDMD, a downstream of pyroptosis induced by NLRP3 inflammasomes, and then the changes of CASP-11/GSDMD pyroptosis signaling upon PF stimulation were further investigated in RESP-induced acute depression. Western blot results demonstrated that RESP insult robustly enhanced the expression levels of CASP-11, an initiator of pyroptosis, to 240.00% ± 13.9% (p < 0.01, vs. Ctrl; Fig. 4a, b), and NLRP3 to 200.20% ± 9.99% of Ctrl (p < 0.01, vs. Ctrl; Fig. 4a, c) in hippocampus, while 7-day treatment of PF resulted in a reduction of CASP-11 protein to 152.70% ± 10.11% of Ctrl in 20 mg/kg group and 134.70% ± 5.66% of Ctrl in 40 mg/kg group (p < 0.05, 20 mg/kg group and p < 0.01, 40 mg/kg group vs. RESP-insulted group; Fig. 4a, c), which was very closed to FLXT administration 132.70% ± 10.54% of Ctrl (p < 0.05, vs. RESP-insulted group; Fig. 4a, b). Also, PF administration led to a reduction of NLRP3 expression to 138.70% ± 6.93% of Ctrl at 20 mg/kg and 130.10% ± 9.76% of Ctrl at 40 mg/kg (p < 0.05, vs. RESP-insulted group; Fig. 4a, c), similar to FLXT administration 126.10% ± 12.05% of Ctrl group (p < 0.05, vs. RESP-insulted group; Fig. 4a, c).
PF administration suppressed the enhanced expression of CASP-11/GSDMD pyroptosis signaling transduction upon RESP insult. Mice were insulted with reserpine (RESP, 1 mg/kg) by i.p injection for 3 days followed by PF administration (0, 10, 20, 40 mg/kg, i.g.) for 7 days, and fluoxetine (FLXT, 20 mg/kg) treatment served as a positive antidepressant. The expression levels of (a) CASP-11 and NLRP3, (d) CASP-1, and (f) GSDMD and IL-1β in hippocampus from each group were determined by Western blot; β-actin served as a loading control. Summary of the expression levels of (b) CASP-11, (c) NLRP3, (e) CASP-1, (g) GSDMD, and (h) IL-1β. Each value represents the mean ± SEM of three independent experiments (n = 6 mice/per group, *p < 0.05, **p < 0.01, ***p < 0.001, vs. Ctrl group; #p < 0.05, ##p < 0.01, ###p < 0.001, vs. RESP-insulted mice)
Furthermore, the effect of PF administration on the activated CASP-1 was checked. The Western result indicated that PF treatment decreased the promoted expression of CASP-1 upon RESP insult (214.80% ± 10.13% of Ctrl, p < 0.001, vs. Ctrl; Fig. 4d, e) to 171.80% ± 9.22% of Ctrl at 20 mg/kg and 166.90% ± 7.97% of Ctrl at 40 mg/kg (p < 0.05, vs. RESP-insulted group; Fig. 4d, e), and FLXT administration reduced it to 141.90% ± 5.90% of Ctrl (p < 0.05, vs. RESP-insulted group; Fig. 4d, e). At the same time, we checked the expression changes of GSDMD and IL-1β, two important pyroptosis executioners downstream of inflammasome activation. A significant increase of GSDMD to 184.00% ± 7.07% (p < 0.001, vs. Ctrl; Fig. 4f, g) and IL-1β to 279.80% ± 12.7% of Ctrl (p < 0.001, vs. Ctrl; Fig. 4f, h) was observed in the reserpinized hippocampus by Western assay, while PF treatment suppressed the elevated GSDMD to 140.30% ± 7.75% at 20 mg/kg and 130.60% ± 10.24% at 40 mg/kg (p < 0.05, vs. RESP-insulted group; Fig. 4f, g), and IL-1β to 183.60% ± 9.57% at 20 mg/kg and 166.90% ± 7.97% in 40 mg/kg group after PF administration (p < 0.01, vs. RESP-insulted group; Fig. 4F, H). FLXT administration decreased the elevated expression of GSDMD to 131.70% ± 5.25% and IL-1β to 161.90% ± 15.79% of Ctrl (p < 0.01, vs. RESP-insulted group; Fig. 4F-H) as positive control. Taken together, inhibition of the enhanced expression of CASP-1/GSDMD pyroptosis signaling was responsible for the antidepressant-like effects of PF.
PF Administration Suppressed Microglial Activation and Inhibited the Promoted Expression of GSDMD upon RESP Insult in Hippocampus
The activated microglia-mediated inflammatory response represents a significant component for pathophysiology of depression. Given GSDMD mainly distributes in microglia, the effect of PF on GSDMD in hippocampal microglia was further investigated. The immunofluorescence staining for Iba-1, a specific marker for activated microglia, was performed. As results revealed, RESP insult robustly activated microglia as well as enhanced the expression of GSDMD in the hippocampus compared with Ctrl group (Fig. 5A, B). However, PF treatment suppressed the promoted GSDMD expression and suppressed microglial activation compared with that of in RESP-insulted group (Fig. 5C), which was similar to that in FLXT-treated reserpinized mice (Fig. 5D). The effects of PF on microglia activation was further confirmed using CD68, another alternative marker, and similar data were obtained (Fig. S2). These data indicated that PF could reverse the elevated expression of GSDMD and suppress microglial activation induced by RESP insult, thus providing antidepressant effects.
PF treatment inhibited microglial activation and the suppressed expression of GSDMD in the reserpinized hippocampus. Mice were treated with reserpine (RESP, 1 mg/kg) by i.p injection for 3 days followed by PF administration (0, 20 mg/kg, i.g.) for 7 days, and fluoxetine (FLXT, 20 mg/kg) treatment served as a positive antidepressant. (A–D) Representative images of the colocalization of GSDMD with microglia in hippocampus from each group which were stained for Iba-1 (green) and GSDMD (red). Nuclei were counterstained with Hoechst in blue. Scale bar = 100 μm
PF Administration Inhibited the Enhanced Pyroptosis Signaling in Cultured Murine N9 Microglia upon LPS and ATP Stimulation
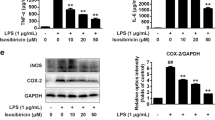
The inhibitory effects of PF on pyroptosis signaling transduction in activated microglia were further confirmed in cultured murine N9 microglia in vitro using double immunocytochemistry labeling for GSDMD and Iba-1. As showed in Fig. 6A, C, LPS/ATP stimulation robustly activated microglia as well as enhanced the expression of GSDMD in N9 microglia compared with Ctrl group. However, PF treatment suppressed microglial activation and the promoted GSDMD expression compared with that of LPS/ATP-induced group (Fig. 6C). Western blot data further demonstrated that LPS/ATP stimulation robustly promoted the expression levels of CASP-11 to 200.00% ± 22.94% of Ctrl (p < 0.001, vs. Ctrl; Fig. 7a, b) and NLRP3 to 301.90% ± 11.75% of Ctrl (p < 0.001, vs. Ctrl; Fig. 7a, c) in murine N9 microglia, while PF treatment reduced the elevated level of CASP-11 to 152.90% ± 10.52% at 10 μM and 129.10% ± 7.55% of Ctrl at 100 μM (p < 0.05, vs. LPS/ATP-induced group; Fig. 7a, b) and NLRP3 to 175.30% ± 11.01% at 10 μM and 141.80% ± 5.78% at 100 μM (p < 0.001, vs. LPS/ATP-induced group; Fig. 7a, c).
Immunocytochemistry staining of GSDMD in murine N9 microglia upon LPS/ATP insult after PF administration. N9 microglia were pretreated with PF (0, 10 μM) for 12 h followed by stimulation with LPS (1 μg/mL) for 4 h and ATP (2.5 mM) for 0.5 h. (A–C) The expression changes of GSDMD in microglia from each group were measured by immunostaining for Iba-1 in green and GSDMD in red. Nuclei were counterstained with Hoechst33258 in blue. PF administration suppressed the enhanced expression of GSDMD in murine N9 microglia upon LPS/ATP insult. Scale bar = 100 μm
PF administration inhibited the enhanced expression of CASP-11/GSDMD signaling transduction upon LPS and ATP-induced pyroptosis in murine N9 microglia in vitro. Murine N9 microglia were pretreated with PF (0, 1, 10, 100 μM) for 12 h and followed by stimulation with LPS (1 μg/mL) for 4 h and ATP (2.5 mM) for 0.5 h. The expression levels of (a) CASP-11 and NLRP3, (d) CASP-1, and (f) GSDMD and IL-1β from each group were determined by Western blot; β-actin served as a loading control. Summary of the expression levels of (b) CASP-11, (c) NLRP3, (e) CASP-1, (g) GSDMD, and (h) IL-1β. Each value represents the mean ± SEM of three independent experiments (n = 6/per group, *p < 0.05, **p < 0.01, ***p < 0.001, vs. Ctrl group, #p < 0.05, ##p < 0.01, ###p < 0.001, vs. LPS/ATP-induced group)
Meanwhile, we checked the changes of activated CASP-1 and found that LPS/ATP stimulation led to a significant increased level of cleaved CASP-1 to 218.20% ± 13.24% of Ctrl (p < 0.01, vs. Ctrl; Fig. 7d, e), and CASP-1 levels decreased to 160.30% ± 8.51% at 10 μM, 125.30% ± 8.44% of Ctrl at 100 μM upon PF treatment (p < 0.05, vs. LPS/ATP-induced group; Fig. 7d, e). At the same time, the activation of GSDMD and IL-1β, two important downstream targets of inflammasome-mediated pyroptosis, was further investigated. A significant increase of GSDMD (192.40% ± 11.16% of Ctrl, p < 0.01, vs. Ctrl; Fig. 7f, g) and IL-1β (296.50% ± 9.55% of Ctrl, p < 0.001, vs. Ctrl; Fig. 7f, h) was observed in LPS/ATP-stimulated microglia, while PF administration suppressed GSDMD to 157.9% ± 7.09% at 1 μM, 133.70% ± 4.76% at 10 μM, and 117.60% ± 9.27% of Ctrl at 100 μM (p < 0.05, vs. LPS/ATP-induced group; Fig. 7f, g) and IL-1β to 195.30% ± 9.00% at 1 μM, 156.90% ± 8.57% at 10 μM, and 131.90% ± 10.52% of Ctrl at 100 μM (p < 0.01, PF 1 μM group and p < 0.001, PF 10 and 100 μM group vs. LPS/ATP-induced group; Fig. 7f, h). Collectively, PF administration suppressed the promoted expression of pyroptosis signaling CASP-11/NLRP3/GSDMD/IL-1β upon LPS/ATP-induced pyroptosis in microglia.
CASP-1 Inhibitor VX-765 Facilitated PF-Mediated Inhibition of the Enhanced Expression of CASP-11/GSDMD Signaling Transduction upon LPS and ATP-Induced Pyroptosis in Murine N9 Microglia
To verify whether CASP-11/GSDMD pyroptosis signaling was involved in PF-mediated antidepressant effect, VX-765, an effective and selective inhibitor for CASP-1 activation, was utilized in cultured murine N9 microglia upon LPS/ATP stimulation. LPS/ATP stimulation robustly enhanced the expression levels of CASP-1 to 199.80% ± 8.66% of Ctrl as shown in Fig. 8a, b (p < 0.001, vs. Ctrl), and PF treatment reduced the level of CASP-1 to 143.60% ± 5.87% at 10 μM, VX-765 to 45.17% ± 7.31%, and PF + VX-765 to 43.50% ± 8.95% of Ctrl (p < 0.05, PF group and p < 0.001, VX-765, PF + VX-765 vs. LPS/ATP-induced group; p < 0.01, PF vs. PF + VX-765 group; Fig. 8a, b). The expression changes of GSDMD and IL-1β, two important downstream signaling targets of CASP-1-dependent pyroptosis, were further evaluated. We found significant increases of GSDMD to 212.40% ± 20.0% of Ctrl (p < 0.05, vs. Ctrl; Fig. 8c, d) and IL-1β to 298.20% ± 13.57% of Ctrl (p < 0.001, vs. Ctrl; Fig. 8c, E) upon LPS/ATP stimulation in microglia, while PF treatment decreased GSDMD to 152.20% ± 6.72%, VX-765 to 139.50% ± 7.86%, and PF + VX-765 to 117.60% ± 5.26% of Ctrl (p < 0.01, PF, VX-765 and PF + VX-765 vs. LPS/ATP-induced group; p < 0.05, PF, VX-765 vs. PF + VX-765 group; Fig. 8c, d); and IL-1β decreased to 187.00% ± 5.44% in PF-treated group, 151.90% ± 7.09% in VX-765-treated group, and 140.30% ± 7.35% of Ctrl in PF + VX-765-treated group (p < 0.001, PF, VX-765 and PF + VX-765 vs. LPS/ATP-induced group; p < 0.01, PF vs. PF + VX-765 group; Fig. 8c, e).
CASP-1 inhibitor VX-765 facilitated PF-mediated inhibition of pyroptosis synergistically in murine N9 microglia upon LPS/ATP stimulation. Murine N9 microglia were pretreated with PF (10 μM) and/or VX-765 (10 μM) for 12 h and followed by simulation with LPS (1 μg/mL) for 4 h and ATP (2.5 mM) for 0.5 h. The expression levels of (a) CASP-1, (c) GSDMD and IL-1β, and (f) CASP-11 and NLRP3 from each group were determined by Western blot; β-actin served as a loading control. Summary of the expression levels of (b) CASP-1, (d) GSDMD, (e) IL-1β, (g) CASP-11, and (h) NLRP3, respectively. Each value represents the mean ± SEM of three independent experiments (n = 6/per group, *p < 0.05, **p < 0.01, ***p < 0.001, vs. Ctrl group; #p < 0.05, ##p < 0.01, ###p < 0.001, vs. LPS and ATP-induced group; $ p < 0.05, $$ p < 0.01 vs. PF-treated group; and p < 0.05 vs. VX-765 group)
There is a feedback between CASP-1 and CASP-11 in the pathway to enhance the process of pyroptosis [18]; therefore, the expression changes of CASP-11 and NLRP3, two upstream signaling targets for CASP-1-dependent pyroptosis, were also investigated after VX-765 treatment. LPS/ATP insult promoted the expression levels of CASP-11 to 178.30% ± 9.45% (p < 0.01, vs. Ctrl; Fig. 8f, g) and NLRP3 to 263.50% ± 17.01% of Ctrl (p < 0.01, vs. Ctrl; Fig. 8f, h) in microglia, while PF treatment mitigated the level of CASP-11 to 131.20% ± 7.36%, VX-765 to 137.90% ± 8.40%, and PF + VX-765 to 133.10% ± 6.06% of Ctrl (p < 0.05, vs. LPS/ATP-induced group; Fig. 8F, G); PF treatment reduced the level of NLRP3 to 167.90% ± 6.64%, VX-765 to 157.00% ± 9.85%, and PF + VX-765 to 150.10% ± 9.00% of Ctrl (p < 0.05, PF and PF + VX-765 group vs. LPS/ATP-induced group; p < 0.01, VX-765 group vs. LPS/ATP-induced group; Fig. 8f, h). The combined treatment of PF + VX-765 did not further mitigate the enhancive expression of CASP-11 and NLRP3 compared with PF or VX-765 treatment alone. Collectively, the data revealed that VX-765 could suppress the cleaved CASP-1 production along affecting the upstream signaling proteins CASP-11 and NLRP3, thus resulted in the reduction of downstream targets GSDMD and IL-1β, which facilitated PF-mediated inhibition of pyroptosis synergistically in activated microglia.
Discussion
In this study, we demonstrated that PF administration significantly ameliorated mice depression-like behaviors induced by RESP insult, and the suppression of inflammasome-induced CASP-11/GSDMD pyroptosis pathway by activated microglia was responsible for PF-mediated antidepressant as predicted by molecular docking simulation. Moreover, PF administration corrected plasticity impairment in the reserpinized hippocampus. Furthermore, VX-765, an inhibitor for CASP-1 activation, enhanced the inhibition of pyroptosis mediated by PF administration in N9 microglia upon LPS/ATP stimulation. These results highlight that NLRP3 inflammasome-dependent pyroptosis acts as a potential causative factor in the pathogenesis of RESP-induced mice depression and PF exerts as a potential therapeutic compound for depression treatment.
It is estimated that a large proportion of depression patients could not benefit from the currently approved treatment. This lack of efficacy suggests that current therapies, mainly targeting neuron-centric mechanisms, fail to address important biological processes involved in depression pathology. There is an urgent need to explore the potential mechanism of glia instead of neuron in the etiology of depression. It is well accepted that glial cells are widely involved in a number of physiological functions in the CNS beyond the nutritional support to neurons. As the resident immune cells of the brain, microglia eliminate or prune weak and inappropriate synapses during synaptogenic period [24], ultimately leaving neurons with their adult connectivity, and disruptions in this process result in sustained deficits in synaptic connectivity [25]. Detrimental stimulation triggers the proliferation, migration, and abnormal activation of glia cells, results in the enhancive production of inflammatory cytokines such as IL-1β, IL-6, and TNF-α, and the cytokines induce inflammation attack, synaptic neuron damage, and mental processing dysfunction. Activated microglia was observed in limbic brain regions in animals subjected to psychosocial stress and postmortem brain tissue from depressed patients with higher presence of ramified Iba1-positive microglia [35]. Chronic administration of the microglial activation inhibitor minocycline completely abolished the effect of peripheral inflammation on the synaptic plasticity (LTP and LTD) [36], indicating the critical role of microglia in dynamic changes of plasticity upon stress. Therefore, microglia exerts a critical role as a sensor for pathological events in depression. Previous studies have indicated that hippocampus is highly resistant to inflammation under normal circumstances, and psychosocial stress can induce a stronger activation of microglia, causing further hippocampal damage due to the highest concentrations of microglia and IL-1β receptors in hippocampus [37]. Reduction of microglial activity by administration of the inhibitor minocycline abolishes the pro-ramifying effect of stress and reverses induction of DLB.
It is well-accepted that the model of acute depression is established by RESP injection [38], in which RESP depletes monoamine by irreversibly inhibiting the vesicular uptake of monoamines including serotonin, thus mimics the pathology of depression. Consistent with previous observations, our study revealed greater microglial activation in the reserpinized hippocampus (Fig. 5) associated with the induction of IL-1β that directly correlated with depression induced by RESP insult (Fig. 4), suggesting PF exerted antidepressant effect (Fig. 1) through suppressing microglia activation and IL-1β expression followed.
There are cross-links between serotonergic and immunological system in depression pathology. Various stresses activate TLR-4, NLRP3 inflammasome, NF-κB, as well as the secretion of IL-1β, IL-6, and other factors of the innate immune response. IL-4 modulates IL-1β-induced depressive behavior by inhibiting IL-1β-induced central glial activation and serotonin alteration [39, 40]. At the same time, serotonin, a classic neurotransmitter, exerts potential role in inflammatory signaling pathway. Pre-treatment with p-chlorophenylalanine, an inhibitor of serotonin synthesis, blocked the IL-1β-induced decrease in food intake and loss of body weight [41], confirming the ability of the brain serotonergic system to mediate the effects of IL-1β. As reported, the enzyme indole-2, 3-dioxygenase enzyme (IDO), which is responsible for synthesis of quinolinic acid, was activated with an associated reduction of serotonin synthesis upon persists stimulus. NMDA receptors were activated by quinolinic acid in the CNS and followed by the secretion of IL-6 and 1 L-1β, enhancing a bias of the tryptophan metabolism to produce quinolinic acid and interleukins, resulting in the reduction of serotonin synthesis, and strengthening the depressive development [42]. Fluoxetine injection into mice twice at 1 h and 12 h after transient middle cerebral artery occlusion (tMCAO) respectively alleviated neurological deficits and neuronal apoptosis, accompanied by inhibiting IL-1β, Bax, and p53 expression and upregulating anti-apoptotic protein Bcl-2 level [43]. These findings give us an insight into the potential of fluoxetine in terms of opening up novel therapeutic avenues for neurological diseases including stroke. Numerous evidence underpins that NLRP inflammasomes are central setscrews between stress, immune activation, and depression, linking the severity of depression to the inflammasome platform [44]. The NLRP3 inflammasome, a protein complex mainly constitutively expresses in microglia, is a critical component of inflammasomes that functions through recruitment of the precursor form of CASP-1, leading to the cleavage of CASP-1 that is responsible for the maturation and secretion of IL-1β and IL-18 [10, 13], and additionally induce pyroptosis [21]. The critical role of NLRP3 in depression psychopathology was further confirmed from NLRP3 knockout study. NLRP3 null mutant mice exhibited decreased anxiety and anhedonic behaviors under basal or unstressed conditions, whereas were resilient to the behavioral deficits under chronic stress conditions. Consistent with these findings, we found that RESP stress was sufficient to trigger the NLRP3 inflammasome pathway along with CASP-11 and CASP-1 in the hippocampus (Fig. 4) and thus may result in neuron dysfunction. However, PF administration exerted antidepressant through suppressing the promoted expression of proteins (Fig. 4), along with the improvement of impaired plasticity (Fig. 2).
The exact physiological role and mechanism of GSDMD protein, a newly identified pyroptosis executioner downstream of inflammasome activation, in depression is not clear. In this study, we found that PF would interact with C-terminus of GSDMD as predicted by molecular docking simulation (Fig. 3). GSDMD mainly distributed in activated microglia upon RESP insult (Fig. 5), and the upregulation of GSDMD was further confirmed in the reserpinized hippocampus (Figs. 4 and 5) and LPS/ATP-activated N9 microglia in vitro (Figs. 6 and 7). These results highlight RESP-ignited robust pyroptosis neuroinflammation counted for depression etiology which was suppressed after PF administration (Fig. 4). The effects of PF on neurons besides microglia were further investigated. We also found that the expression of GSDMD increased in neuron in RESP model and decreased in PF-treated RESP model as shown in Fig. S1. These data indicated that PF could reverse the elevated expression of GSDMD in neurons induced by RESP insult, thus providing antidepressant effects. The protective effects of PF on neurons cannot be excluded at this stage, and further study needs to be explored. GSDMD is a downstream of pyroptosis induced by NLRP3 inflammasomes, and the mechanisms of how the interaction between PF and GSDMD results in the expression changes of NLRP3, CASP-1, and CASP-11 need further exploration.
It is well accepted that there are lots of dysfunctions beyond lack of serotonin underlying depression pathology, and PF owns various pharmacological activities including antioxidant, antiinflammation, and neuroprotective effects on various types of cells. Therefore, PF administration could provide improvement against depression through multiple targets [31], suggesting PF may work as a precursor of antidepressants for drug development. All listed above may provide some possible advantages of PF compared with FLXT.
Our findings that support previous studies on the role of the NLRP3 in depression psychopathology, to identify their importance in the antidepressant effect of PF, VX-765, a CASP-1 inhibitor, was further used. Interestingly, VX-765 facilitated PF-mediated inhibition of pyroptosis synergistically in over-activated microglia in vitro (Fig. 8). To the best of our knowledge, this study is the first to reveal NLRP3 inflammasome-mediated pyroptosis contributes to RESP-induced depression. Collectively, the data indicated that PF exerted antidepressant effects, alleviating neuroinflammation through inhibiting inflammasome-induced pyroptosis by over-activated microglia in the depressive hippocampus. This study might yield new candidate therapeutic targets for the treatment of depression.
References
Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: A systematic analysis for the global burden of disease study 2017. Lancet 392 (10159): 1789–1858
Jeon SW, Kim YK (2016) Neuroinflammation and cytokine abnormality in major depression: cause or consequence in that illness? World J Psychiatry 6(3):283–293
Liu JJ, Wei YB, Strawbridge R et al (2019) Peripheral cytokine levels and response to antidepressant treatment in depression: a systematic review and meta-analysis. Mol Psychiatry
Torres-Platas SG, Cruceanu C, Chen GG, Turecki G, Mechawar N (2014) Evidence for increased microglial priming and macrophage recruitment in the dorsal anterior cingulate white matter of depressed suicides. Brain Behav Immun 42:50–59
Rawdin BJ, Mellon SH, Dhabhar FS, Epel ES, Puterman E, Su Y, Burke HM, Reus VI et al (2013) Dysregulated relationship of inflammation and oxidative stress in major depression. Brain Behav Immun 31:143–152
Ramirez K, Shea DT, McKim DB, Reader BF, Sheridan JF (2015) Imipramine attenuates neuroinflammatory signaling and reverses stress-induced social avoidance. Brain Behav Immun 46:212–220
Hannestad J, DellaGioia N, Bloch M (2011) The effect of antidepressant medication treatment on serum levels of inflammatory cytokines: A meta-analysis. Neuropsychopharmacology 36(12):2452–2459
Singhal G, Jaehne EJ, Corrigan F et al (2014) Inflammasomes in neuroinflammation and changes in brain function: a focused review. Front Neurosci 8:315
Martinon F, Burns K, Tschopp J (2002) The inflammasome: a molecular platform triggering activation of inflammatory caspases and processing of proIL-beta. Mol Cell 10(2):417–426
Alcocer-Gomez E, de Miguel M, Casas-Barquero N et al (2014) NLRP3 inflammasome is activated in mononuclear blood cells from patients with major depressive disorder. Brain Behav Immun 36:111–117
Shelton RC, Claiborne J, Sidoryk-Wegrzynowicz M, Reddy R, Aschner M, Lewis DA, Mirnics K (2011) Altered expression of genes involved in inflammation and apoptosis in frontal cortex in major depression. Mol Psychiatry 16(7):751–762
Alcocer-Gomez E, Ulecia-Moron C, Marin-Aguilar F et al (2016) Stress-induced depressive behaviors require a functional NLRP3 inflammasome. Mol Neurobiol 53(7):4874–4882
Zhang Y, Liu L, Peng YL, Liu YZ, Wu TY, Shen XL, Zhou JR, Sun DY et al (2014) Involvement of inflammasome activation in lipopolysaccharide-induced mice depressive-like behaviors. CNS Neurosci Ther 20(2):119–124
Zhang Y, Liu L, Liu YZ, Shen XL, Wu TY, Zhang T, Wang W, Wang YX et al (2015) NLRP3 inflammasome mediates chronic mild stress-induced depression in mice via neuroinflammation. Int J Neuropsychopharmacol 18(8):pyv006
Wong ML, Inserra A, Lewis MD, Mastronardi CA, Leong L, Choo J, Kentish S, Xie P et al (2016) Inflammasome signaling affects anxiety- and depressive-like behavior and gut microbiome composition. Mol Psychiatry 21(6):797–805
Iwata M, Ota KT, Duman RS (2013) The inflammasome: pathways linking psychological stress, depression, and systemic illnesses. Brain Behav Immun 31:105–114
Lu S, Peng H, Wang L, Vasish S, Zhang Y, Gao W, Wu W, Liao M et al (2013) Elevated specific peripheral cytokines found in major depressive disorder patients with childhood trauma exposure: a cytokine antibody array analysis. Compr Psychiatry 54(7):953–961
Kayagaki N, Stowe IB, Lee BL, O’Rourke K, Anderson K, Warming S, Cuellar T, Haley B et al (2015) Caspase-11 cleaves gasdermin D for non-canonical inflammasome signalling. Nature 526(7575):666–671
Li S, Wu Y, Yang D et al (2019) Gasdermin D in peripheral myeloid cells drives neuroinflammation in experimental autoimmune encephalomyelitis. J Exp Med
Evavold CL, Ruan J, Tan Y, Xia S, Wu H, Kagan JC (2018) The pore-forming protein gasdermin D regulates interleukin-1 secretion from living macrophages. Immunity 48(1):35–44 e6
McKenzie BA, Mamik MK, Saito LB, Boghozian R, Monaco MC, Major EO, Lu JQ, Branton WG et al (2018) Caspase-1 inhibition prevents glial inflammasome activation and pyroptosis in models of multiple sclerosis. Proc Natl Acad Sci U S A 115(26):E6065–E6074
Wohleb ES, Franklin T, Iwata M, Duman RS (2016) Integrating neuroimmune systems in the neurobiology of depression. Nat Rev Neurosci 17(8):497–511
Kato TA, Watabe M, Kanba S (2013) Neuron-glia interaction as a possible glue to translate the mind-brain gap: a novel multi-dimensional approach toward psychology and psychiatry. Front Psychiatry 4:139
Filipello F, Morini R, Corradini I et al (2018) The microglial innate immune receptor TREM2Is required for synapse elimination and normal brain connectivity. Immunity 48(979–991):e8
Schafer DP, Stevens B (2013) Phagocytic glial cells: sculpting synaptic circuits in the developing nervous system. Curr Opin Neurobiol 23:1034–1040
Liu HQ, Zhang WY, Luo XT, Ye Y, Zhu XZ (2006) Paeoniflorin attenuates neuroinflammation and dopaminergic neurodegeneration in the MPTP model of Parkinson's disease by activation of adenosine A1 receptor. Br J Pharmacol 148(3):314–325
Zhang LL, Wei W, Wang NP, Wang QT, Chen JY, Chen Y, Wu H, Hu XY (2008) Paeoniflorin suppresses inflammatory mediator production and regulates G protein-coupled signaling in fibroblast-like synoviocytes of collagen induced arthritic rats. Inflamm Res 57(8):388–395
Cao C, He X, Wang W, Zhang L, Lin H, du L (2006) Kinetic distribution of paeoniflorin in cortex of normal and cerebral ischemia-reperfusion rats after intravenous administration of Paeoniae Radix extract. Biomed Chromatogr 20(12):1283–1288
Tabata K, Matsumoto K, Murakami Y et al (2001) Ameliorative effects of paeoniflorin, a major constituent of peony root, on adenosine A1 receptor-mediated impairment of passive avoidance performance and long-term potentiation in the hippocampus. Biol Pharm Bull 24(5):496–500
Gu X, Cai Z, Cai M et al (2016) Protective effect of paeoniflorin on inflammation and apoptosis in the cerebral cortex of a transgenic mouse model of Alzheimer’s disease. Mol Med Rep 13:2247–2252
Liu SC, Hu WY, Zhang WY, Yang L, Li Y, Xiao ZC, Zhang M, He ZY (2019) Paeoniflorin attenuates impairment of spatial learning and hippocampal long-term potentiation in mice subjected to chronic unpredictable mild stress. Psychopharmacology 236(9):2823–2834
Wu YM, Jin R, Yang L, Zhang J, Yang Q, Guo YY, Li XB, Liu SB et al (2013) Phosphatidylinositol 3 kinase/protein kinase B is responsible for the protection of paeoniflorin upon H(2)O(2)-induced neural progenitor cell injury. Neuroscience 240:54–62
Xiao J, Song M, Li F et al (2017) Effects of GABA microinjection into dorsal raphe nucleus on behavior and activity of lateral habenular neurons in mice. Exp Neurol 298(Pt A):23–30
Zhang K, Li YJ, Guo Y, Zheng KY, Yang Q, Yang L, Wang XS, Song Q et al (2017) Elevated progranulin contributes to synaptic and learning deficit due to loss of fragile X mental retardation protein. Brain 140(12):3215–3232
Iwata M, Ota KT, Li XY, Sakaue F, Li N, Dutheil S, Banasr M, Duric V et al (2016) Psychological stress activates the inflammasome via release of adenosine triphosphate and stimulation of the Purinergic type 2X7 receptor. Biol Psychiatry 80(1):12–22
Riazi K, Galic MA, Kentner AC, Reid AY, Sharkey KA, Pittman QJ (2015) Microglia-dependent alteration of glutamatergic synaptic transmission and plasticity in the hippocampus during peripheral inflammation. J Neurosci 35:4942–4952
Farrar WL, Kilian PL, Ruff MR et al (1987) Visualization and characterization of interleukin 1 receptors in brain. J Immunol 139(2):459–463
Hanjie Y, Dan L, Mengxin S et al (2019) BDNF mediates the protective effects of scopolamine in reserpine-induced depression-like behaviors via up-regulation of 5-HTT and TPH1. Psychiatry Res 271:328–334
Iritani S, Tohgi M, Arai T, Ikeda K (2006) Immunohistochemical study of the serotonergic neuronal system in an animal model of the mood disorder. Exp Neurol 201(1):60–65
Park HJ, Shim HS, An K et al (2015, 2015) IL-4 inhibits IL-1beta-induced depressive-like behavior and central neurotransmitter alterations. Mediat Inflamm:941413
Zubareva OE, Krasnova IN, Abdurasulova IN, Bluthe RM, Dantzer R, Klimenko VM (2001) Effects of serotonin synthesis blockade on interleukin-1 beta action in the brain of rats. Brain Res 915(2):244–247
Ramirez LA, Perez-Padilla EA, Garcia-Oscos F et al (2018) A new theory of depression based on the serotonin/kynurenine relationship and the hypothalamic pituitary- adrenal axis. Biomedica 38(3):437–450
Shan H, Bian Y, Shu Z, Zhang L, Zhu J, Ding J, Lu M, Xiao M et al (2016) Fluoxetine protects against IL-1beta-induced neuronal apoptosis via downregulation of p53. Neuropharmacology 107:68–78
Kim HK, Andreazza AC, Elmi N, Chen W, Young LT (2016) Nod-like receptor pyrin containing 3 (NLRP3) in the post-mortem frontal cortex from patients with bipolar disorder: a potential mediator between mitochondria and immune-activation. J Psychiatr Res 72:43–50
Acknowledgments
This work was supported by the Key International Cooperation Projects of Shaanxi Province for Prof Wu (2020KWZ-021), National Natural Science Foundation of China (No. 81571328 for Prof Wu, No. 31800887 for Dr. Yang), Military Medicine Promotion Projects (No. 2018jsts09) for Prof Wu, and Research Foundation from Social Development Science and Technology Project of Shaanxi Province for Mr. Wang (2020JQ-464) and Dr. Yang (No. 2018SF-305).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
All experimental procedures were approved by the Ethics Committee of Fourth Military Medical University (Approval reference number No. KY20193145) in full accordance with the ethical guidelines of the National Institutes of Health for the care and use of laboratory animals.
Conflict of Interest
The authors declare that they have no conflicts of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
Fig. S1
PF administration inhibited the promoted expression of GSDMD in neurons upon RESP insult in hippocampus. Mice were treated with reserpine (RESP, 1 mg/kg) by i.p injection for 3 d followed by PF administration (0, 20 mg/kg, i.g.) for 7 d, and fluoxetine (FLXT, 20 mg/kg) treatment served as a positive antidepressant. (A-D) Representative images of the colocalization of GSDMD with neuron in hippocampus from each group which were stained for NEUN (green) and GSDMD (red). Nuclei were counterstained with Hoechst in blue. Scale bar = 100 μm. (PNG 3527 kb)
Fig. S2
PF treatment inhibited microglial activation and suppressed the expression of GSDMD in the reserpinized hippocampus. Mice were treated with reserpine (RESP, 1 mg/kg) by i.p injection for 3 d followed by PF administration (0, 20 mg/kg, i.g.) for 7 d, and fluoxetine (FLXT, 20 mg/kg) treatment served as a positive antidepressant. (A-D) Representative images of the colocalization of GSDMD with microglia in hippocampus from each group which were stained for CD68 (green) and GSDMD (red). Nuclei were counterstained with Hoechst in blue. Scale bar = 100 μm. (PNG 3428 kb)
Fig. S3
PF administration inhibited the enhanced secretion of IL-1β upon LPS and ATP-induced pyroptosis in murine N9 microglia in vitro. Murine N9 microglia were pretreated with PF (0, 1, 10, 100 μM) for 12 h and followed by stimulation with LPS (1 μg/mL) for 4 h and ATP (2.5 mM) for 0.5 h. The secreted IL-1β in the culture medium from each group was determined by ELISA method. Each value represents the mean ± SEM of three independent experiments (n = 6/per group, ***p < 0.001, vs. Ctrl group, ##p < 0.01, ###p < 0.001, vs. LPS/ATP-induced group). (PNG 549 kb)
Rights and permissions
About this article
Cite this article
Tian, DD., Wang, M., Liu, A. et al. Antidepressant Effect of Paeoniflorin Is Through Inhibiting Pyroptosis CASP-11/GSDMD Pathway. Mol Neurobiol 58, 761–776 (2021). https://doi.org/10.1007/s12035-020-02144-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-020-02144-5