Abstract
Background
Three recent lawsuits that address declaration of brain death (BD) garnered significant media attention and threaten to limit physician power to declare BD.
Methods
We discuss these cases and their consequences including: the right to refuse an apnea test, accepted medical standards for declaration of BD, and the irreversibility of BD.
Results
These cases warrant discussion because they threaten to: limit physicians’ power to determine death; incite families to seek injunctions to continue organ support after BD; and force hospitals to dispense valuable resources to dead patients in lieu of patients with reparable illnesses or injuries.
Conclusions
Physicians, philosophers, religious officials, ethicists, and lawyers must work together to address these issues and educate both the public and medical community about BD.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
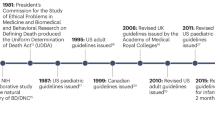
When a Harvard ad hoc committee introduced the concept of brain death (BD) in 1968, they believed that because society granted physicians the power to determine death, it was not necessary to legislate that BD was legally equivalent to cardiopulmonary death [1]. But declaration of death has non-medical consequences such as mourning, criminal prosecution, inheritance, and taxation. So, in 1981, President Carter created a task force of physicians, philosophers, religious officials, ethicists, and lawyers. This task force produced what later became the Uniform Determination of Death Act (UDDA) which defines BD as legally equivalent to cardiopulmonary death [2]. In 1995, the American Academy of Neurology (AAN) published guidelines for determination of BD [3]. These guidelines were updated in 2010, and after an extensive review of the literature, the authors noted that there were no cases of recovery after BD determination using the AAN guidelines [4]. Today, BD is acknowledged as legal death throughout the United States of America and around the world [5, 6].
Nonetheless, there are still people, including physicians, who conceptually, religiously, or morally perceive that death can only be declared when the heart stops beating. BD is defined as loss of function of the brain, but declaring BD does not require death of every neuron. As a result, some people conceptually view BD as a legal fiction [7]. Although major Catholic, Jewish, and Muslim societies support the concept of BD, some devout communities continue to believe that these religions only endorse cessation of respiration, heartbeat, and circulation as true death [8]. Orthodox Jewish, Japanese Shinto, Buddhist, Muslim, and Native American populations are commonly cited as groups that have religious objections to BD [9].
According to the AAN guidelines, organ support should be discontinued after declaration of BD unless organ donation is planned, but four states offer accommodation exceptions and allow organ support to be continued after BD [3, 10]. California, Illinois, and New York offer brief accommodation to families who object to BD. In New Jersey, if a patient has moral or religious objections to BD, they are considered alive until cardiopulmonary arrest. But in other states, there are no guidelines about how to manage situations in which families object to BD on religious or other grounds [10].
Surveys show that public comprehension of the distinctions between BD (legal death), a coma (a temporary gross impairment in brain function), and a persistent vegetative state (a permanent unconscious state with retention of the ability to breathe without assistance and preservation of some brainstem reflexes) is poor [11, 12]. Public exposure to the topic of BD is often limited to media, cinema, or television portrayals of BD, which are frequently inaccurate or sensationalistic [13, 14].
Recently, there have been a number of widely publicized lawsuits that have threatened to undermine the concept of BD and limit physician power to determine death [15–17].
Right to Refuse Apnea Testing
Mirranda Grace Lawson, a two-year-old, was brought to the Virginia Commonwealth Health System (VCUHS) in May 2016 after choking led to cardiopulmonary arrest. Because she was unresponsive and had no brainstem reflexes, physicians planned to perform an apnea test to determine whether she was BD. Her parents objected, citing that: (1) according to their Christian beliefs, Mirranda Grace was still alive because her heart was beating; (2) as her parents, only they could make healthcare decisions on her behalf; and (3) the apnea test could be harmful and was therefore not in her best interests. Although the Circuit Court ruled that VCUHS could perform the test, the Lawsons filed an appeal, but this was withdrawn in December 2016 after Mirranda’s cardiopulmonary arrest [15, 18, 19]. However, in a similar case in Montana in September 2016, the court prohibited clinicians from performing an apnea test, stating that parents of sound mind have the right to choose or refuse medical treatment for their children based upon their rights to autonomy and privacy [20].
When a patient is comatose with absent brainstem reflexes, the last test of brainstem function is the apnea test. The patient is taken off of the ventilator for 8 min to determine whether the medullary chemoreceptors stimulate respiration in response to the rise of carbon dioxide in arterial blood. If spontaneous respirations occur, the patient is alive, so the test is aborted. If the patient cannot breathe without the assistance of the ventilator, death is declared and organ support is discontinued. It is not routine practice for neurologists to obtain consent from a family before evaluating for BD [5, 10, 15, 21]. Practitioners and families may be apprehensive about discontinuing the ventilator to perform this test, due to fear of hypotension, arrhythmias, hypoxemia, or development of a pneumothorax, but a retrospective study of 63 patients showed that the test was successfully completed 98% of the time. Although 6% of patients became hypoxic and 17% became hypotensive, no patients developed an arrhythmia or had a cardiac arrest during the test. Preoxygenation is imperative to minimize risk of harm [21].
Should families have the right to refuse apnea testing? Although a delay in determination of BD could potentially provide families with time to process the gravity of these situations, hospitals should have the fundamental right to know whether patients are alive or dead in order to facilitate appropriate triage of physician time and material resources [10].
It is dangerous to give families the power to decide whether or not clinicians can determine whether patients are dead. Families could delay declaration of BD if they: (1) see acceptance of death as giving up; (2) believe neurologic function can be regained; or (3) desire to continue to receive a patient’s government benefits. This would impact not just one patient and their family, but also clinicians, hospital personnel, and society. Perhaps most significantly, this would have repercussions for other patients needing intensive care unit (ICU) support [10].
Acceptable Medical Standards for Declaration of BD
Aden Hailu, a 20-year-old, suffered an anoxic event during an appendectomy in April 2015 at St. Mary’s Regional Medical Center in Nevada. She was unresponsive with no brainstem reflexes and no evidence of spontaneous respirations, so BD was declared. Her father objected and sought a court injunction mandating continued organ support [16]. It is unclear what motivated him to desire provision of ventilator support, nutrition, medications, and interventions in the setting of BD. Family members sometimes insist on treatment in the setting of futility due to religious or cultural beliefs, guilt, grief, faith in future medical advances to change prognosis, or concern that a physician’s prognosis is jaded by patient race or socioeconomic status [22]. Although a district court ruled that Hailu met the AAN criteria for BD and that organ support should be discontinued, Hailu’s father appealed [16].
In November 2015, the Supreme Court of Nevada reversed, reversed the ruling, questioning whether the AAN criteria represented “accepted medical standards,” and “established irreversible cessation of all functions of the entire brain, including the brainstem,” as required for BD under the UDDA. The Court specifically cited that an electroencephalogram was not performed to evaluate for electrocerebral silence. The Supreme Court directed the district court to answer these questions, but the case ended in January 2016 after Hailu’s cardiopulmonary arrest [16].
What are “accepted medical standards” for declaration of BD? The authors of the UDDA debated establishing clinical criteria for BD, but ultimately concluded that “it is not necessary—indeed, it would be a mistake—to enshrine any particular medical criteria, or any requirements for procedure or review, as part of a statute.” Instead, they embraced the need for BD to be based upon standards “accepted by a substantial and reputable body of medical men and women as safe and efficacious for the purpose for which [they are] being employed.” The UDDA authors further noted that “irreversibility” must be defined by the capabilities of physicians at any given moment, with the understanding that this could vary if technology changed over time [2].
Although there are philosophical, religious, and cultural variations in the definition of death, an international forum on death determination agreed that declaration of BD requires a clinical evaluation to demonstrate irreversible catastrophic brain injury leading to coma, absence of brainstem reflexes, and inability to breathe spontaneously. They noted that the use of an electroencephalogram is optional. They stated that cessation of brain function is irreversible if prerequisites for declaration of BD are fulfilled, confounding conditions are excluded, and the patient is refractory to all interventions, or no interventions are available or indicated [5]. The AAN guidelines for BD declaration are consistent with the international forum’s criteria [4, 5]. Surely, this consensus should be seen as the “accepted medical standard” the authors of the UDDA intended [2], but the Supreme Court of Nevada’s opinion perilously serves as precedent for any family who objects to BD on any ground [16].
Irreversibility of BD
Jahi McMath, a 13-year-old, had a cardiopulmonary arrest at Children’s Hospital Oakland in December 2013 after she developed hemoptysis following a tonsillectomy, and BD was declared [17]. McMath’s mother objected to discontinuation of organ support and brought several lawsuits, citing that from her Christian faith perspective, death does not occur until the heart stops beating [17, 23]. She was ultimately given permission to relocate Jahi to New Jersey, where religious exemption to declaration of BD is offered, despite the fact that a California death certificate had already been issued and signed. McMath has remained on organ support in New Jersey, and her mother is currently suing Alameda County and the State of California in an effort to have her death certificate revoked [17].
A key tenet of BD is that although technology may allow an individual’s heart and lungs to function, there can be no possibility of restoration of brain function either spontaneously or through intervention [5]. Were McMath’s family to be successful at having her declared alive again, this would be a profound development. No evidence proving Jahi is alive has been formally presented thus far, but the mere suggestion that she could be alive (again) reinforces skepticism about the concept of BD among families who wish to continue organ support despite declaration of BD.
Discussion
Declaration of BD can often be complicated due to the emotionally charged nature of situations involving life and death [5, 10]. This is already exacerbated by poor understanding of BD, but the significant publicity about the Lawson, Hailu, and McMath cases (and many similar others) threatens to further escalate the complexities by: (1) limiting physicians’ power to determine death; (2) inciting families to seek injunctions to continue organ support after BD and request second opinions by physicians who are well-known opponents of BD; and (3) forcing hospitals to dispense valuable resources such as ventilators, beds, medications, and clinician time, to dead patients in lieu of patients with reparable illnesses or injuries [15–17, 24, 25].
A survey of neurologists who were asked to continue organ support after BD found that the most common reasons to continue treatment were the desire to avoid litigation, media coverage, and upsetting the family. As a result, support was continued until the time of cardiopulmonary arrest a third of the time [10]. Protracted organ support after declaration of death can be morally distressful for the healthcare team [24]. Additionally, it is economically challenging. During the six months that Lawson was hospitalized at VCUHS, the daily price for admission was nearly $10,000, which is broken down as follows: $5916 per day for a room in the pediatric ICU, $1533.26 per day for medications and nutrition, $900 per day for attending physician services, $724 per day for respiratory services, $490.40 per day for drug charges, $190.57 per day for laboratory tests, and $16.28 per day for hematology tests [15]. Lawson was never declared BD, but for patients who are declared BD, treatment is even more financially problematic because insurance companies often do not cover provision of futile treatment after death [15, 24, 26]. Although physicians sometimes inform families that support will be discontinued from a patient who is BD if another patient requires an ICU bed, this is rarely done in practice [10, 24, 27].
Conclusion
Just as a task force of physicians, philosophers, religious officials, ethicists, and lawyers formed to discuss the meaning of BD in the 1980s [2], these communities must once again work together to address the challenges created by the Lawson, Hailu, and McMath cases [15–17]. This should ideally be done on an international stage. To this end, the World Health Organization is attempting to create a single worldwide operational definition of death with practical guidelines on declaration of death [5]. Hopefully, these guidelines will address the issues we identified herein. Additionally, it is imperative that experts work to educate both the public and the medical community about BD, particularly when cases such as the Lawson, Hailu, and McMath cases are prominently featured in the news [15–17].
References
A definition of irreversible coma. Report of the Ad Hoc committee of the harvard medical school to examine the definition of brain death. JAMA. 1968;205:337–340.
Defining death: medical, legal and ethical issues in the determination of death. Washington D.C. 1981.
Wijdicks EFM. Determining brain death in adults. Neurology. 1995;45:1003–11.
Wijdicks EFM, Varelas PN, Gronseth GS, Greer DM. Evidence-based guideline update: determining brain death in adults: report of the Quality Standards Subcommittee of the American Academy of Neurology. Neurology. 2010;74:1911–8.
Shemie SD, Hornby L, Baker A, et al. International guideline development for the determination of death. Intensive Care Med. 2014;40:788–97.
Sprung CL, Truog RD, Curtis JR, et al. Seeking worldwide professional consensus on the principles of end-of-life care for the critically ill. The consensus for Worldwide End-of-Life Practice for Patients in Intensive Care Units (WELPICUS) study. Am J Respir Crit Care Med. 2014;190:855–66.
Bernat JL. Controversies in defining and determining death in critical care. Nat Rev Neurol. 2013;9:164–73.
Lewis A, Varelas P, Greer D. Prolonging support after brain death: when families ask for more. Neurocrit Care. 2016;24:481–7.
Pope TM. Brain death: legal duties to accommodate religious objections. Chest. 2015;148:e69.
Lewis A, Adams N, Varelas P, Greer D, Caplan A. Organ support after death by neurologic criteria: results of a survey of US neurologists. Neurology. 2016;87:827–34.
Shah SK, Kasper K, Miller FG. A narrative review of the empirical evidence on public attitudes on brain death and vital organ transplantation: the need for better data to inform policy. J Med Ethics. 2015;41:291–6.
Siminoff LA, Burant C, Youngner SJ. Death and organ procurement: public beliefs and attitudes. Kennedy Inst Ethics J. 2004;14:217–34.
Lewis A, Weaver J, Caplan A. Portrayal of Brain Death in Film and Television. Am J Transplant. 2016 (Epub ahead of print).
Lewis A, Lord AS, Czeisler BM, Caplan A. Public education and misinformation on brain death in mainstream media. Clin Transplant. 2016;30:1082–9.
In Re: Mirranda Grace Lawson. 2016. CL16-2358, City of Richmond Circuit Court.
In Re: Guardianship of Hailu. 2015. 361 P.3d 5.
McMath vs. California. 2015. No. 3:15-06042, N.D. Cal.
Supreme Court of Virginia Apellate Case Management System. SCV Record Number 161321. [cited 2016 Dec 30].
Richer AD. Mirranda Grace Lawson dies; was focus of fight over brain death test [Internet]. Culpeper Star Expon. [cited 2016 Dec 30]. http://www.dailyprogress.com/starexponent/news/mirranda-grace-lawson-dies-was-focus-of-fight-over-brain/article_ce555172-c4b0-5bc1-82f3-be2d694b02aa.html.
In Re: Allen Callaway. 2016. DG-16-08.
Datar S, Fugate J, Rabinstein A, Couillard P, Wijdicks EFM. Completing the apnea test: decline in complications. Neurocrit Care. 2014;21:392–6.
Burkle CM, Benson JJ. End-of-life care decisions: importance of reviewing systems and limitations after 2 recent North American cases. Mayo Clin Proc. 2012;87:1098–105.
Choong KA, Rady MY. Re A (A Child) and the United Kingdom Code of Practice for the Diagnosis and Confirmation of Death: Should a Secular Construct of Death Override Religious Values in a Pluralistic Society? HEC Forum. 2016 (Epub ahead of print).
Flamm AL, Smith ML, Mayer PA. Family members’ requests to extend physiologic support after declaration of brain death: a case series analysis and proposed guidelines for clinical management. J Clin Ethics. 2014;25:222–37.
Liao S, Ito S. Brain death: ethical challenges to palliative care concepts of family care. J Pain Symptom Manage. 2010;40:309–13.
Khandelwal N, Benkeser D, Coe NB, Engelberg RA, Teno JM, Curtis JR. Patterns of cost for patients dying in the intensive care unit and implications for cost savings of palliative care interventions. J Palliat Med. 2016;19:1171–8.
Smith ML, Flamm AL. Accommodating religious beliefs in the ICU: a narrative account of a disputed death. Narrat Inq Bioeth. 2011;1:55–64.
Author's Contribution
Ariane Lewis was responsible for conception and design, drafting the manuscript, and final approval of the manuscript. Thaddeus Pope was responsible for conception and design, supervision, critical revision of the manuscript and final approval of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Ariane Lewis and Thaddeus Pope have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Lewis, A., Pope, T.M. Physician Power to Declare Death by Neurologic Criteria Threatened. Neurocrit Care 26, 446–449 (2017). https://doi.org/10.1007/s12028-017-0375-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-017-0375-x