Abstract
Introduction
Prolactin is a peptide hormone mainly synthetized and secreted by the anterior pituitary gland, but also by extrapituitary tissues, such as mammary gland, decidua, prostate, skin, and possibly the brain. Similarly, prolactin receptor is expressed in the pituitary gland, many peripheral tissues, and in contrast to prolactin, its receptor has been consistently detected in several brain regions, such as cerebral cortex, olfactory bulb, hypothalamus, hippocampus, amygdala, among others. Classically, prolactin function has been related to the stimulation of lactogenesis and galactopoiesis, however, it is well known that prolactin induces a wide range of functions in different brain areas.
Purpose
The aim of this review is to summarize recent reports on prolactin and prolactin receptor synthesis and localization, as well as recapitulate both the classic functions attributed to this hormone in the brain and the recently described functions such as neurogenesis, neurodevelopment, sleep, learning and memory, and neuroprotection.
Conclusion
The distribution and putative expression of prolactin and its receptors in several neuronal tissues suggests that this hormone has pleiotropic functions in the brain.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Prolactin (PRL) is a pleiotropic hormone with a complex expression regulation that modulates diverse physiological processes, including angiogenesis, immune response, osmoregulation, reproductive behavior, and lactogenesis.
There are some important reviews about the molecular aspects of the regulation and function of PRL in several organisms [1, 2], and others related to specific hypothalamic areas involved in the control of lactation [3]. The aim of this review is to describe evidence about PRL expression and its physiological effects in several brain areas, including classical functions such as lactation as well as more recently discovered effects on neurogenesis, neural plasticity, and neuroprotection.
PRL and its pathway of molecular actions
PRL a single-chain polypeptide hormone, discovered in mammals around the 1930s by Oscar Riddle [4], was found in humans in 1970, by Friesen et al. It is mainly synthetized by the lactotrophs of the anterior pituitary gland [2, 5–7], but it seems to be locally produced by the central nervous system. PRL can also enter the brain via specific transporters located in the membranes of the choroid plexus [8]. A recent study reported that PRL transport into the mouse brain is independent of the prolactin receptor (PRL-R), and requires a transporter that has not been yet identified [9].
It has been reported that PRL is also synthetized and secreted by extra-pituitary tissues, including many target tissues, such as mammary gland, ovary, decidua, and immune tissues, where PRL can act as a local autocrine/paracrine factor with physiological/pathological significance [2, 5–7]. Some pioneering data suggest that PRL de novo synthesis and release occur in several extrapituitary localizations including neuronal tissues in humans [5]. Importantly, human PRL gene is more complex than that of rodents: PRL gene possesses a supradistal promoter, which allows its extrapituitary expression (for more details see review [5]). Various reports have consistently evidenced by reverse transcription polymerase chain reaction (RT-PCR), even after hypophysectomy, the expression of PRL transcripts in different brain areas, such as the amygdala, thalamus, cortex, caudate, hippocampus, cerebellum and brainstem of the rat [10–15], and in hypothalamus and cerebellum of rats and humans [10, 11]. In medial preoptic area (mPOA) [14], periventricular preoptic nucleus, bed nucleus of the stria terminalis (BNST), and paraventricular nucleus of the hypothalamus, particularly, the ventral region, PRL mRNA has been detected by in situ hybridization in sheep [14]. Importantly, PRL protein has only been detected by Western blot in amygdala, preoptic area and olfactory bulb in 135 day-old male sheep fetus [14]. The brain areas in which PRL expression has been detected by different methodological approaches are summarized in Fig. 1 and Table 1.
Expression of prolactin (PRL) and prolactin receptor (PRL-R) in the brain. The figure shows a sagittal section of the rat brain with indications of the areas containing putative cells expressing PRL, PRL-R or both of them. The regions containing PRL are indicated by a black circle and regions containing PRL-R are labeled by a white circle. In the figure, hypothalamic nuclei expressing PRL-R are shown. C-P caudate-putamen, BNST bed nucleus of the stria terminalis, GP globus pallidus
At the molecular level, PRL expression and regulation are tissue-specific. There are distinct PRL variants, which result from either alternative splicing or posttranslational modifications. The occurrence of PRL variants is responsible for some of the pleiotropic actions of this hormone, since PRL can form dimers, polymers, and aggregates. Marano and Ben-Jonathan published an extensive and complete revision of the molecular aspects of PRL synthesis and regulation in 2014 [2].
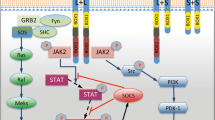
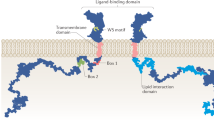
The biological actions of PRL are mediated by PRL-R, which is expressed in many PRL target tissues and in the brain [16–18]. The classical PRL-R consists of a single transmembrane domain, a ligand-binding extracellular domain, and a cytoplasmic domain required for signal transduction. Within the cytoplasmic part of PRL-R, there is a proline-rich BOX-1 domain—the JAK-2 kinase docking site [1, 19].
It has been demonstrated that some isoforms of PRL-R result from alternative splicing and proteolytic cleavage [1, 17]. The most common isoforms described for PRL-R are the long, intermediate, and short forms which result from the proteolytic cleavage of membrane-bound PRL-R [17, 20]. Short and long PRL-R forms have been also reported in different brain regions, such as: brainstem [10, 12, 13], choroid plexus [21–27], hippocampus [10, 28–30] and the hypothalamus [21–23, 26, 27, 30–35]. It has been reported that PRL-R long–long dimers activate second messenger pathways, via the activation of JAK-STAT-dependent signaling pathway that involves the phosphorylation of STAT5 in the brain [36]. Also, PRL-R modulates the mitogen-activated protein kinase pathway in the brain [2].
Although the classic role of PRL in female mammals is the stimulation of lactogenesis and galactopoiesis, this hormone induces a large number of functions, including over 300 separate actions that have been reported in both females and males [17, 37–41]. In the brain, PRL actions are related to sexual behavior [1, 17, 18, 41], maternal behavior [10, 21, 42], neuroprotection [42–45], and neurogenesis [44] among others. Moreover, an overexpression of PRL and PRL-R has been reported in the brain and the pituitary gland in lactation [46], stress [1, 47], and exposure to injury induced by hypoxia and ischemia [28].
PRL action in different brain areas
Olfactory bulb
Maternal care (licking/grooming)
It has been found a relationship between some maternal-specific behaviors of postpartum female rats and an increase in PRL-R gene expression in the olfactory bulb [48]. This area is important for the ability to discriminate different odors in postpartum (for example, pups or intruders) [49], thus, at the end of pregnancy and in parturition occur important changes in the regulation of olfaction that prepare the expecting mother to positively respond to the stimulus coming from the newborn [50]. Licking/grooming frequency has been used as a parameter to evaluate maternal care of pups, and some studies report that olfaction is critical for the onset of this behavior [48, 50]. A recent study shows that two sub-populations with high frequencies of licking/grooming (HL) and low frequencies of licking/grooming (LL) differ in PRL-R expression, HL mothers express more receptors in the olfactory bulb compared to LL [48], indicating that PRL is essential for the proper display of licking/grooming behavior. However, a limitation of this study is that only PRL-R mRNA expression was evaluated and not the translated protein.
Moreover, in female mice the immunoreactivity of phosphorylated (active) signal transducer and activator of transcription 5 (pSTAT5-ir) during late pregnancy and lactation in this area was observed [51]. Interestingly, PRL-R mRNA was not detected in the olfactory bulb of C57BL/6 J male mice [32], nevertheless, PRL-R mRNA has been detected by in situ hybridization in male and female fetus and newborn rats [52].
Neurogenesis
In the last two decades, several studies have revealed the potential role of PRL to regulate neurogenesis in the adult brain. PRL has been implicated in some maternal behavior in rodents. One of these adaptations is an increase in neurogenesis in the subventricular zone (SVZ) due to elevated PRL secretion in pregnant and lactating female mice [53, 54] to mediate several reproductive behaviors including paternal recognition of offspring, and male pheromone preference in females.
PRL-dependent increase in new neurons incorporated into the olfactory bulb that is correlated with the enhanced maternal behavior is observed after pregnancy [53]. Neurogenesis and PRL-R gene overexpression in females may contribute to adaptive behaviors during mating, pregnancy, and postpartum.
Interestingly, when PRL is administered during neonatal period, neurogenesis in hippocampal dentate gyrus and olfactory bulb is reduced, and produces psychopathological alterations during adult life [55].
Neurodevelopment
In fetal (60–135 gestation days) and adult sheep, the mRNA and protein of PRL was detected by RT-PCR, in situ hybridization and Western blot in different brain areas, suggesting PRL effects in sheep neurodevelopment [14]. Besides, in adult rat, PRL-R is expressed at low levels in the olfactory bulb but it is detected in abundance in the olfactory bulb of the fetal rat in late gestation. PRL-R mRNA and immunoreactive protein were detected in the olfactory bulb on embryonic day 18, and in postnatal day 5, PRL-R was expressed in abundance in mitral and tufted cells of the olfactory bulb. This evidence suggests that PRL participates in olfactory differentiation and development, and possible regulation of neonatal offspring behavior and maternal–infant interactions [52].
Cerebral cortex
mRNA and protein expression of PRL has been found in the cerebral cortex by RT-PCR [10], even after hypophysectomy in rodents, by radioimmunoanalysis, immunocytochemistryl, and immunoprecipitation assays [15]. It has been reported that PRL increases during hypoxic ischemic injury in this brain area in juvenile rats [28]. Nevertheless, the use of immunohistological methods cannot discriminate between pituitary and locally produced PRL, and cannot distinguish PRL variants or molecules with similar epitopes [5].
Besides, many cerebral cortex areas also express PRL-R (the cingulate cortex, neocortex, prefrontal cortex and parietal cortex), in young and adult rats, in different physiological conditions, by different methods including in situ hybridization, RT-PCR, immunocytochemistry, and Western blot [21, 23, 28, 31, 33, 35, 48]. The cerebral cortex mainly contains mRNA for the expression of the long form of PRL-R [21, 22]. In lactating rats, there is an increase in the mRNA of the long form of PRL-R in hypothalamic nuclei and parietal cortex [23]. However, studies performed by RT-PCR in these areas may be inaccurate since dissection of each of the structures confers some difficulty and the wrong dissection of an area could cause masking or dilution of results. Contradictory data have been reported by Pi and Grattan [31] who did not observe significant staining in the cerebral cortex of either male or estrogen-treated ovariectomized rats [31]. In addition, other reports have not found PRL-R expression in male adult intact mice by in situ hybridization [32]. Also, recent studies report that in female mice there is an increase in pSTAT5-ir in different brain structures during late pregnancy and lactation [51].
Lactating rats have lower reactivity to stress than virgin rats, but display more aggressive behavior toward adult intruders. During the lactation period, c-fos increases in parietal and prefrontal cortices, indicating the activation of these areas [56] Hence, motherhood is associated with neuronal changes and plasticity in sensory systems, particularly in the brain cortex. Mother–pup interactions develop shortly after delivery and have a long-term impact on the brain and behavior of the former [57]. Certain maternal behaviors are regulated by auditory and olfactory cues given by the newborn, which activate some areas of the cortex [50, 58, 59]. Whether the activation of sensory systems during lactation are related with PRL action, merits further attention.
Additionally, PRL participates in glial responses following cortical injury caused by hypoxia. After damage, PRL-R protein and mRNA content increase in glia more than in neurons in cortex [28]. Astrocytes within the penumbra and within the glial scar (reactive cellular process that occurs after injury as a mechanism to protect and begin the healing process in the nervous system) express PRL and PRL-R, suggesting that hypoxia ischemia induces an activation of the PRL axis in regions of the cerebral cortex affected by injury [28].
Corpus callosum
It has been reported that the long form of PRL-R can be detected in the corpus callosum of adult virgin female rats using RT-PCR and Western blotting [60], suggesting that the cells of the corpus callosum respond to PRL. In contrast, other studies have shown no PRL-R mRNA expression in this area, but in adjacent areas [21]. In the gestational period, this tissue contributes to the proliferation or survival of oligodendrocytes. It has been suggested that one mechanism underlying the increased oligodendrocyte turnover seen in lactating females compared to virgin females is mediated by PRL. Interestingly, oligodendrocyte number in corpus callosum seems to increase in relation with PRL levels. Additionally, oligodendrocyte number positively correlated with the size of the litter, suggesting that PRL, whose concentration varies in accordance with the number of lactating pups, contributes to oligodendrocyte proliferation and/or survival [61]. Besides, in pregnant or virgin female mice treated with PRL an increase in the number of oligodendrocyte precursor cells and in the total number of myelinated axons in the corpus callosum has been observed [60].
Bed nucleus of the stria terminalis
Several authors have reported that PRL-R mRNA is expressed in this brain area by hybridization [21, 22, 27, 34], while PRL mRNA has been detected by in situ hybridization in adult and fetal sheep [14]. There is a slight increase in the number of cells expressing the long form of the receptor in the BNST on day 21 of gestation in the rat (near delivery) [51] and at 2 h postpartum [62]. In late pregnant and lactating female mice, there was a higher pSTAT5 immunoreactive cell density as compared with virgin females [51].
Lesions in BNST have shown that it is an important structure in the regulation of maternal care [63, 64] that it has also been implicated in male intruder-induced maternal aggression [65] and in the protection of pups from predators [66]. However, more research is required to determine the specific role of PRL in this brain area.
Choroid plexus
The highest levels and expression of short and long form PRL-R detected in the mammalian rat brain have been reported in the choroid plexus by Scatchard plot analysis, by RT-PCR, followed by Southern blot hybridization of PCR products, in situ hybridization and immunohistochemistry [18, 21–23, 26, 27]. It has been shown that PRL concentration increases in the choroid plexus after vascular injection of radiolabeled PRL [67]. Some studies have reported an increase in PRL-R mRNA levels in the choroid plexus during lactation that correlates with an increase in plasma PRL levels [51, 68]. It has been reported that PRL-R gene possesses five alternative first exons and its expression changes between tissues and physiological conditions. During lactation in mice, the expression levels of murine PRL-R gene exon variants (mE13, mE14, and mE15) increase as compared with diestrus mice in choroid plexus. Interestingly, in the choroid plexus PRL administration induces an increase in PRL-R under mE14 expression [69]. Besides, it has been reported that PRL-R mRNA expression in this tissue is mediated by mE14 in both male and female rats during postnatal development as detected by real time RT-PCR [25].
A recent report using knockout PRL-R mice demonstrated that PRL enter into the brain independently from its receptor. Importantly, the authors reported that PRL transport occurs mainly from the cerebral vasculature rather than the choroid plexus [9].
Additionally, it has been reported that restraint stress in male and female rats is followed by a prolonged increase in PRL plasma levels and in mRNA expression of long form PRL-R in choroid plexus likely to contribute to attenuate stress [24].
Hypothalamus
There are various reports that have detected mRNA expression of PRL in several nuclei of the hypothalamus in the female rat and fetus and adults sheep using RT-PCR, real time RT-PCR techniques and in situ hybridization [10, 11, 14, 26, 30, 70], and the protein has been detected by Western blot and immunocytochemistry [19, 71]. In this brain area, the increase in PRL during lactation and other physiological conditions induced PRL-R expression [21–23, 26, 27, 30–35, 70] in some hypothalamic nuclei, such as the ventromedial (VMN), supraoptic, paraventricular, arcuate [23], suprachiasmatic nucleus, and mPOA [19, 72]. It is important to mention that when microdissecting hypothalamic nuclei, there is a possible mixing of hypothalamic nuclei due to their small size and closeness. However, in histological studies the expression of PRL-R in situ has been recently reported in several hypothalamic nuclei (involved in sociosexual and maternal behavior), such as mPOA, arcuate, paraventricular, supraoptic, and VMN [51].
Ventromedial nucleus (VMN)
It has been reported that PRL-R mRNA expression in the VMN of female rat is not modified during pregnancy [22], but increases during lactation [23]. In contrast, PRL-R protein has been detected in the ovariectomized plus estrogen-treated rat or in diestrous rat [31]. PRL-R in the VMN has been implicated in the increased food intake of lactating rats [23].
The VMN is involved in feeding behavior control, evidenced by the fact that lesions in this area cause hyperphagia or weight gains in mammals, including rats [73], monkeys [74], and humans [73, 74]. Interestingly, intracerebroventricular PRL administration to virgin and ovariectomized female rats causes an increase in food intake [75, 76].
Supraoptic and paraventricular nuclei
During breastfeeding, magnocellular neurons in the supraoptic and paraventricular nuclei synthesize oxytocin and vasopressin, which in turn induce milk ejection [72, 77, 78], and maternal care behavior in mothers or even in virgin females [79–81]. An increase in PRL has been related to maternal care and milk ejection after delivery, both necessary for the survival of the offspring. In addition, PRL administration in virgin female rats promotes an increase in oxytocin and vasopressin plasma levels [82]. Recently, it was reported that pSTAT5, whose expression changes via activation PRL-R, is expressed in most oxytocin neurons of late-pregnant and lactating rats, but almost absent in oxytocin neurons of virgin rats, thus contributing to the adaptations required for offspring care [83]. Consistently, mice show an increase in pSTAT5-ir in paraventricular and supraoptic nuclei, during late pregnancy and lactation [51].
Vasopressin neurons are related to osmoregulation, increasing reabsorption of water in the kidney, which in conjunction with augmented drinking behavior restores the tonicity of blood. In pregnant rats (near to delivery), there is a decrease in serum osmotic pressure related to a high vasopressin status, in a similar manner during lactation, suckling stimulation induces release of vasopressin, which could dilute the blood, resulting in the increase in circulating blood volume [84]. However, recent data show that vasopressin increase during lactation could not be completely attributed to PRL, since only some vasopressin neurons express pSTAT5 in the supraoptic nucleus of late pregnant and lactating rats [83]. Additionally, intracerebroventricular PRL administration diminishes corticotropin-releasing factor in the parvocellular part of the paraventricular nucleus of ovariectomized estradiol-treated rats after acute restraint stress [85], suggesting that PRL helps to mitigate the stress response.
Apart from the classical functions in the hypothalamus, PRL has an important role in sleep regulation. It has been recognized that PRL is the major mediator to induce rapid eye movement sleep (REMS) after different stressors. Besides, it has been demonstrated that PRL exerts sleep effects that have been related with the activation of the corticotropin–corticosterone axis, which promotes PRL secretion in rats, increasing REMS [86–88]. The stimulation of PRL expression mediated by vasoactive intestinal peptide and peptide histidine methionine enhances REMS in rats, cats, and rabbits [89]. In agreement, the exposures to ether vapor [87], social defeat stress [90], and restraint stress [87, 90, 91] increase both PRL expression in lateral hypothalamus [91] and serum PRL levels [90, 91], promoting REMS [87, 90, 91] and NON-REMS [90, 92]. The molecular mechanism involved in the regulation of sleep by PRL remains unclear.
Arcuate nucleus
PRL has been involved in the suppression of fertility during lactation through the reduction of luteinizing hormone (LH) and gonadotropin-releasing hormone secretion into the portal blood [1, 3, 93, 94]. Kisspeptin neurons in the arcuate nucleus regulate LH pulsatility secretion [95] and most of neurons in this nucleus co-express PRL-R [96]. Thus, lactating rats present high PRL levels and reduced LH plasma levels. Also, virgin ovariectomized rats treated with PRL show a reduction of kisspeptin expression in the arcuate nucleus as well as low LH plasma levels [94, 97].
The arcuate nucleus is implicated in the negative feedback regulation of PRL secretion by an increase in tuberoinfundibular dopamine (TIDA) neuronal activity [98], which show an increase in dopamine turnover in response to PRL [46]. In this sense, the highest density of pSTAT5-ir cells was observed in the arcuate nucleus of female mice probably including TIDA neurons [51].
Recent findings show that another neuronal population, A15 dopaminergic neurons, of the rostral hypothalamus could participate in the regulation of GnRH secretion and negative feedback regulation of PRL. The pSTAT5 expression is induced during lactation or by the exogenous PRL administration to diestrus rats, accompanied by an increase in dopamine turnover, nevertheless, the role of these neurons is unclear, since A15 dopamine neurons co-express kisspeptin and innervate GnRH neurons that could participate in the suppression of fertility [46].
Medial preoptic area (mPOA)
Additionally, it has been observed that mRNA expression for the long form of PRL-R slightly increases in mPOA of female rats before delivery [22]. Treatment of experienced female rats with PRL increases PRL-R and PRL in this area, which has been involved in maternal behavior [99]. Similarly, the mPOA of female mice displayed high levels of pSTAT5 labeling at the end of pregnancy and in lactation [51]. It has been shown by RT-PCR, Western blot, and radioimmunoassays that suckling can induce synthesis and release of PRL in mPOA and PVN of lactating rats [100].
mPOA plays a crucial role in the full expression of maternal behavior and peripartum adaptations in lactating rats [64, 101]. Bilateral administration of PRL into mPOA promotes a rapid onset of maternal care in virgin female rats that have been pretreated with estradiol and progesterone [102]. It has been demonstrated that PRL-R is essential for appropriate performance of maternal behavior, PRL-R−/− females are sterile, but heterozygote PRL-R+/− mothers have offspring that show alterations in maternal behavior [17].
Suprachiasmatic nucleus
Neurons expressing the short form of PRL-R mRNA have been found in the suprachiasmatic nucleus [21, 31], which coordinates circadian events [103]. It is well known that suprachiasmatic nucleus regulates PRL secretion [104], and it has also been suggested that this nucleus is necessary for the circadian signal involved in the preovulatory surge of PRL during proestrus day in rodents. A lesion in this nucleus annuls the PRL surges [105–107]. Additionally, in many species of wild animals that breed seasonally such as sheep, PRL production shows an annual cycle and there is increased PRL secretion during the spring and summer season, regardless of the timing of the breeding season [108, 109].
PRL and endocrine development
Besides having effect in adults, some reports suggest that PRL is important for development of the hypothalamus of neonatal rats [17, 110]. In many mammals, PRL is present in maternal milk and can be absorbed by the intestinal epithelium of neonatal animals, and then transfer to the circulation [111]. Moreover, PRL-R expression is very high in the fetal brain but decreases in adulthood [112], suggesting that it should have significant effects during development. A decrease in milk PRL levels in lactating mothers (by daily injections of bromocriptine) during a critical postpartum period impaired the activity of the TIDA system in pups [110], and in their adulthood showed an increased latency to display maternal behavior in comparison to offspring of control mothers [113]. These data suggest that breast milk-PRL participates during the early postnatal period in the development of neural circuits that control negative feedback regulation of PRL and maternal behavior and negative feedback regulation of PRL [110, 113].
Hippocampus
Some studies have described the expression of PRL and PRL-R in in vivo and in vitro studies of rat hippocampus [10, 15, 22, 28, 30, 48, 114, 115]. This is an important brain region implicated in multiple physiological behaviors, including spatial information acquisition and retrieval, as well as consolidation and storage of memory, among others [116]. However, it has not traditionally been associated with motherhood.
Memory, cognition and learning
Scarce studies have analyzed the participation of PRL related to memory and learning, and the results of these limited reports are controversial. Compared to nulliparous rats, maternity is related to improved cognitive performance in primiparous and multiparous animals, which exhibited improved spatial memory in the dry land maze, greater exploration in the elevated plus-maze [117], and better performance in a radial arm maze [118–121]. In primiparous female rats, there was enhanced spatial working and reference memory compared with nulliparous females, although these memory-associated parameters did not improve with subsequent pregnancies [120]. Conversely, in pregnant women, high levels of PRL and steroid hormones (estradiol, progesterone, testosterone and cortisol) are associated with cognitive impairment in verbal recall and in tasks involving processing speed [121].
Studies in male rats with hyperprolactinemia show impaired object recognition without modifications in spatial learning [39]. In older men, higher PRL levels have been associated with lower cognitive performance in verbal and working memory [122]. On the other hand, studies on hippocampus-dependent memory show that PRL-R loss in null mice results in learning and memory deficits in both males and females [123]. Interestingly, kainic acid (KA) administration induces cognitive deficit in novel object recognition tests, that is prevented with PRL 1 h after KA administration [124]. Also, PRL null mice have learning and memory deficits in the Morris water maze test and Y-maze test that were reversed by PRL administration into the hippocampus, reinforcing the evidence that PRL is required for the acquisition of normal learning and memory in the adult mouse hippocampus [123].
Neurogenesis
PRL is also implicated in hippocampal neurogenesis [125, 126] and neuroprotection [114]. The hippocampal subgranular zone of the dentate gyrus is one of the two areas of the brain known to originate adult stem cells [127]. Different studies of hippocampal anatomy have also revealed that motherhood modifies cell proliferation and survival in the dentate gyrus of the hippocampus [125]. For example, PRL mediates the increase in SVZ neurogenesis associated with pregnancy [53], and male pheromone-stimulated neurogenesis in the adult female brain [128]. This increase could be mediated by PRL-R, since reduction of PRL-R diminishes neurogenesis [17].
Moreover, it has been demonstrated that infusion of PRL into the lateral ventricle of male mice significantly increases proliferation in the dentate gyrus [126]. Contrarily, psychosocial and physical stress impairs hippocampal cell proliferation and neurogenesis [129, 130]. The administration of PRL protects hippocampal neurogenesis in the dentate gyrus of chronically stressed adult male mice [29], in contrast, in newly born rats PRL reduces neurogenesis and cell survival in both dentate gyrus and olfactory bulb [55]. In this context, PRL-R-null female and male mice have a reduced number of hippocampal precursors, while the infusion of PRL into the adult dentate gyrus is able to promote the activation of a pool of latent precursor cells in this brain area [123]. Conversely, in an excitotoxicity model, KA administration causes pyramidal loss in CA1, CA3 and CA4 of the hippocampus of the female rat, and PRL treatment did not modify the neurogenesis rate [128].
Recent reports show that addition of exogenous PRL to primary culture adult hippocampal cells resulted in an increase in neurosphere number. Accordingly, PRL administered into the adult dentate gyrus significantly increased the neurosphere number. Additionally, PRL null mice showed a reduction in the number of hippocampal-derived neurospheres compared to wild type mice [123].
Neurodevelopment
PRL effects during neurodevelopment have been poorly studied and different effects have been observed depending on the age of the animal. Recently, it has been reported that the lack of PRL in breast milk produces different endocrine disruption in the hypothalamus [109, 112]. As we previously mentioned, neonatal administration of PRL on days 1–14 of postnatal life decreases hippocampal neurogenesis and olfactory bulb cell survival in pups. It is important to mention that PRL treatments were additional to PRL breastmilk source during lactation [55], which gives evidence to support that changes in PRL may affect the development of different circuits in the brain.
Interestingly, pregnant rats exposed to 20 h of REMS restriction (14th to 20th gestational day) exhibited an increase in plasma PRL levels, and their fetuses showed an increase of brain-derived neurotrophic factor in hippocampus [127] possibly due to PRL augment.
Neuroplasticity
PRL significantly participates in the neuroplasticity observed during pregnancy and lactation. For example, dendritic spines represent one cellular substrate of experience-related plasticity and synaptic stability [131]. Besides, it has been reported that there is an increase in dendritic spines in the CA1 region of the hippocampus during late pregnancy and early postpartum, an effect presumably brought about by the increase in PRL during these periods [132]. Similarly, some studies have shown that compared to nulliparous women, primiparous and multiparous females present dendritic remodeling in the CA1 and CA3 hippocampal regions. For instance, multiparity resulted in an enhanced spine density in the CA1 region, which was related to the number of male pups in the litter [133]. However, other studies reported no effects on the number of synaptic spines in the CA1 region during the postpartum period [134].
Neuroprotection
PRL has also shown an important role in hippocampal neuroprotection, evidenced by a decrease in the excitatory glutamatergic activity in the hippocampus [43], and in the cerebral cortex during lactation, with a diminished excitatory response to N-methyl-D-aspartate (NMDA) stimulation [135]. It is known that pregnancy reduces binding to excitatory amino acids in the hippocampus, including NMDA and non-NMDA receptors [136]. In addition, glutamate excitotoxicity has been involved in the development of neurological disorders such as epilepsy and cell death observed after hypoxia and ischemia [137, 138]. It has been shown that PRL is released into the systemic circulation in response to epileptic seizures, and long-term PRL treatment modulates seizure activity [139].
Pregnancy decreases the frequency of spontaneous recurrent seizures induced by KA [140]. Additionally, during lactation there is greater resistance in the female brain to NMDA-induced neuronal activity, expressed as a decrease in seizures and the absence of c-fos expression in specific regions of the brain [135]. Kainic acid administration mainly produced a loss of pyramidal cells of CA1 in diestrus rats; in contrast, there was a neuroprotective effect in lactating rats [43, 44, 141]. Since lactation protects pyramidal neurons of the dorsal hippocampus against KA-induced neuronal damage, it has been proposed as a natural model of neuroprotection [43, 44]. Interestingly, further studies have also demonstrated that pretreatment with systemic PRL prevents intracranial KA-induced excitotoxic damage in the dorsal hippocampus [42, 141], and diminishes the convulsive effects of KA on intact and OVX rats [42, 141]. Recently, a neuroprotective effect of PRL mediated by PRL-R was reported against glutamate excitotoxicity in an in vitro model using primary cell cultures of hippocampal neurons [114]. This effect implicated in part by NF-kB and restoration of the intracellular calcium homeostasis and mitochondrial activity [142].
Thalamus
In the rat thalamus there is evidence of PRL mRNA expression found by RT-PCR analysis [10] and the protein has been detected by Western blot and immunocytochemistry [15, 115]. Moreover, the finding in pregnant rats of scattered neurons expressing mRNA of the short form PRL-R suggests that they influence the mediation and coordination of PRL-regulated endocrine and behavioral events like reproduction, feeding, maternal care, and lactation, among others [21, 22, 40]. Nevertheless, the fact that there are so few cells expressing PRL-R in this structure suggests that the role of this hormone is not too relevant.
This brain area receives ascending afferents from sensory and motor pathways and projects them to the middle layers of the neocortex [143]. A higher level of N-acetylaspartate was observed in the thalamus of pregnant rats, which may be associated with increased dendritic sprouting, synaptogenesis or neurogenesis in this area [144]; however, further research is require to elucidate the role of PRL in this area.
Amygdala
The expression of PRL [10, 14, 15] and PRL-R [21, 22, 27] has been detected in the amygdala of rats and mice. Additionally, pSTAT5-ir was found in amygdala of pregnant and lactating female mice suggesting activation of PRL-R in this area [51]. However, its function in this area is not fully elucidated, but one possibility is that it participates in the circuit for maternal aggression, this network comprises lateral septum, the BNST, amygdala, the mPOA, the paraventricular nucleus, the VMN, and the locus coeruleus, among others [51]. Nevertheless, there was no significant correlation between serum PRL levels and maternal aggression to intruders in female mice [145].
Instead, pup-derived sensory stimulation of the mothers has been proposed as the pivotal factor promoting maternal aggression [51, 146]. Therefore, prolonged action of lactogenic agents (for example, PRL) during pregnancy and not its acute action after parturition can promote the onset of maternal aggression [51]. In accordance with this, vasopressin intracerebral microdialysis within the central amygdala of lactating Wistar rats has been positively correlated with the display of maternal aggressive behavior [147].
Also, several authors have speculated that a possible role of PRL in this brain region may be related to the modulation of the neuroendocrine stress axis by the limbic system [51]. Stimulation of the amygdala results in an “arrest” characteristic in the first phase of the stress response [148] and an increase in the release of the adrenocorticotropic hormone [149]. Chronic PRL treatment of virgin female rats significantly reduces c-fos mRNA expression within the central amygdala [150]. When acting on various relevant brain regions, PRL works as an anxiolytic agent. Besides, the intracerebroventricular and intravenous administration of PRL produced anxiolytic effects in both male and virgin female rats [150, 151]. Additionally, reports show low anxiety levels in pregnant and lactating rats [152, 153]. Hence, it has been suggested that PRL contributes to the attenuated stress response found in the peripartum period of pregnant women [150, 151].
PRL increases NREMS and REMS during recovery after stressors in hypothalamus and the dorsal raphe nucleus of rats [91, 92], but a microinjection of PRL in the central nucleus of the amygdala decreases NREMS, while REMS was not affected [154].
Basal ganglia
In the nuclei of basal ganglia, there is evidence of mRNA expression of PRL [10] and the long and short PRL-R forms (found by using RT-PCR combined with Southern hybridization) in the substantia nigra, nucleus caudate, putamen, globus pallidus, and ventral pallidum, in ovariectomized rats [155]. The expression of both forms of PRL-R in these brain areas provides evidence to support the hypothesis that PRL has direct actions on these regions [155]. However, more studies are required in this respect.
A high PRL concentration is involved in the pathogenesis of systemic lupus erythematosus in human beings, as well as in the autoimmune disease model of NZB/NZWF mice [156]. Some authors speculate that high PRL production is related to a reduction in striatal dopamine activity. In this sense, an inhibition of PRL release has been demonstrated in sheep following stimulation of the nucleus accumbens and caudate-putamen [157]. Furthermore, in NZB/NZWF mice model there was a significant increase in dopamine transporter binding in subdivisions of the caudate-putamen posterior nucleus [156], which suggests the possible participation of striatal dopamine system in PRL synthesis.
Raphe
Limited studies have been performed on PRL or PRL-R expression in raphe. PRL mRNA has been found in the brain stem, but it is not known whether this expression corresponds to the raphe nuclei or other nuclei located in pons [10, 12, 13]. Recently, Brown and coworkers reported expression of pSTAT5 in dorsal raphe and raphe obscurus on lactation day 7, suggesting the activation of PRL-R in these nuclei [158]. Additionally, serotonin (5-HT) stimulates PRL secretion in female rats, while the inhibition of the synthesis of 5-HT with p-chlorophenylalanine blocks diurnal PRL release in early pregnancy [159–161]. The serotonergic neurons of this tissue are involved in the regulation of suckling-induced PRL release in the hypothalamus [162]. Furthermore, neurotoxic lesions of the dorsal raphe impaired suckling-induced PRL secretion and lactational performance [162]. Similarly, female rats treated with a 5HT2 receptor agonist decreased the latency to initiate contact with pups and spent more time licking. Conversely, the administration of agonists for the serotonin 5HT1B receptor increased maternal aggression after delivery. Mothers with a genetic depletion of tryptophan hydroxylase 2, an enzyme responsible for the synthesis of 5-HT in the brain, display increases in pup killing, for review see [163], indicating that 5-HT produced by the raphe nuclei could indirectly regulate maternal behavior.
Recently, it has been reported that sleep deprivation induces an increase in PRL in the hypothalamus and dorsal raphe in the rat. In addition, PRL infusion into the dorsal raphe nucleus increased the time and length of REMS episodes 3 h after the administration [91].
Cerebellum
The expression of PRL mRNA and protein levels has been reported in cerebellum of male and female rats, mice and humans [10, 11, 15, 115, 164–166], with a decrease in its expression during aging [150]. The expression of the PRL-R has not been analyzed. Abs and collaborators [15] relate cerebellar hypoplasia of congenital origin and cerebellar ataxia with hypogonadotropic hypogonadism, a condition with low serum gonadotropin and PRL levels. This study mentions that there could be a relationship between cerebellar-dependent coordination disorders and low levels of hormones such as PRL [71], but no follow-up was done to this study, so there are no more available data.
Summary
PRL is recognized as a pleiotropic hormone in reproductive and peripheral tissues. More recently, evidence about its involvement in different brain functions, including cognition, memory, and maternal behavior has been accumulated. In the last few years, new functions have been attributed to PRL, such as neuroprotection against excitotoxicity and neurogenesis. In this context, continuous efforts in searching molecules with neuroprotective properties and/or stimulators of neurogenesis to treat different neurodegenerative diseases are in progress. In this sense, PRL becomes a promissory candidate for the development of neuro-regenerative therapies. The distribution and expression of PRL-R and possible PRL in neuronal tissues, including the forebrain and limbic system, suggest that this hormone has many functions in the brain. Nevertheless, more investigation needs to be conducted to better understand other functions of PRL and its mechanisms of action during physiological and pathological processes in the brain.
References
A. Ignacak, M. Kasztelnik, T. Sliwa, R.A. Korbut, K. Rajda, T.J. Guzik, Prolactin—Not only lactotrophin a “new” view of the “old” hormone. J. Physiol. Pharmacol. 63(5), 435–443 (2012)
R.J. Marano, N. Ben-Jonathan, Minireview: extrapituitary prolactin: an update on the distribution, regulation, and functions. Mol. Endocrinol. 28(5), 622–633 (2014)
D.R. Grattan, I.C. Kokay, Prolactin: a pleiotropic neuroendocrine hormone. J. Neuroendocrinol. 20(6), 752–763 (2008)
R., Bates, E., Lahr, O., Riddle, The gross action of prolactin and follicle-stimulating hormone on the mature ovary and sex accessories of fowl. Am. J. Physiol. I(II), 361–368 (1935)
N. Ben-jonathan, J.L. Mershonf, D.L. Allen, R.W. Steinmetz, Extrapituitary prolactin: distribution, regulation, functions, and clinical aspects. Endocr. Rev. 17(6), 639–669 (1996)
S. Harvey, Extrapituitary growth hormone. Endocrine 38(3), 335–359 (2010)
S. Harvey, C. Arámburo, E.J. Sanders, Extrapituitary production of anterior pituitary hormones: an overview. Endocrine 41(1), 19–30 (2012)
R.J., Walsh, F.J., Slaby, B.I.Posner, A receptor-mediated mechanism for the transport of prolactin from blood to cerebrospinal fluid. Endocrinology 120(5), 1846–1850 (1987)
R.S.E. Brown, A.K. Wyatt, R.E. Herbison, P.J. Knowles, S.R. Ladyman, N. Binart, W.A. Banks, D.R. Grattan, Prolactin transport into mouse brain is independent of prolactin receptor. FASEB J. 30(2), 1002–1010 (2016)
N. Emanuele, J. Jurgens, M. Halloran, J. Tentler, A. Lawrence, M. Kelley, The rat prolactin gene is expressed in brain tissue: detection of normal and alternatively spliced prolactin messenger RNA. Mol. Endocrinol. 6(1), 35–42 (1992)
K. Fields, E. Kulig, R. Lloyd, Detection of prolactin messenger RNA in mammary and other normal and neoplastic tissues by polymerase chain reaction. Lab. Invest. 68(3), 354–360 (1993)
H. Ehmann, C. Salzig, P. Lang, E. Friauf, H. Nothwang, Minimal sex differences in gene expression in the rat superior olivary complex. Hear. Res. 245(1–2), 65–72 (2008)
W. DeVito, C. Avakian, S. Stone, C. Ace, Estradiol increases prolactin synthesis and prolactin messenger ribonucleic acid in selected brain regions in the hypophysectomized female rat. Endocrinology 131(5), 2154–2160 (1992)
C.E. Roselli, S. Bocklandt, H.L. Stadelman, T. Wadsworth, E. Vilain, F. Stormshak, Prolactin expression in the sheep brain. Neuroendocrinology 87(4), 206–215 (2008)
W. DeVito, Distribution of immunoreactive prolactin in the male and female rat brain: effects of hypophysectomy and intraventricular administration of colchicine. Neuroendocrinology 47(4), 284–289 (1988)
V. Goffin, P. Kelly, The prolactin/growth hormone receptor family: structure/function relationships. J. Mammary Gland Biol. Neoplasia 2(1), 7–17 (1997)
C. Bole-Feysot, V. Goffin, M. Edery, N. Binart, P. Kelly, Prolactin (PRL) and its receptor: action signal transduction pathways and phenotypes observed in PRL receptor knockout mice. Endocr. Rev. 19(3), 225–268 (1998)
M. Freeman, B. Kanyicska, A. Lenart, G. Nagy, Prolactin: structure, function and regulation of secretion. Physiol. Rev. 80, 1523–1631 (2000)
C. Clevenger, J. Kline, Prolactin receptor signal transduction. Lupus 10(10), 706–718 (2001)
X. Pi, J.L. Voogt, Sex difference and estrous cycle: Expression of prolactin receptor mRNA in rat brain. Mol. Brain Res. 103(1–2), 130–139 (2002)
J. Bakowska, J. Morrell, The distribution of mRNA for the short form of the prolactin receptor in the forebrain of the female rat. Brain Res. 116(1–2), 50–58 (2003)
J.C. Bakowska, J.I. Morrell, Atlas of the neurons that express mRNA for the long form of the prolactin receptor in the forebrain of the female rat. J. Comp. Neurol. 386(2), 161–177 (1997)
X.J. Pi, D.R. Grattan, Increased expression of both short and long forms of prolactin receptor mRNA in hypothalamic nuclei of lactating rats. J. Mol. Endocrinol. 23(1), 13–22 (1999)
T. Fujikawa, H. Soya, H. Yoshizato, K. Sakaguchi, K. Doh-Ura, M. Tanaka, K. Nakashima, Restraint stress enhances the gene expression of prolactin receptor long form at the choroid plexus. Endocrinology 136, 5608–5613 (1995)
J. Hirai, M. Nishita, N. Nakao, T.R. Saito, M. Tanaka, Regulation of prolactin receptor gene expression in the rat choroid plexus via transcriptional activation of multiple first exons during postnatal development and lactation. Exp. Anim. 62(1), 49–56 (2013)
S. Chiu, P.M. Wise, Prolactin receptor mRNA localization in the hypothalamus by in situ hybridization. J. Neuroendocrinol. 6(2), 191–199 (1994)
R.S. Brown, I.C. Kokay, A.E. Herbison, D.R. Grattan, Distribution of prolactin-responsive neurons in the mouse forebrain. J. Comp. Neurol. 518(1), 92–102 (2010)
T.A. Möderscheim, T. Gorba, P. Pathipati, I.C. Kokay, D.R. Grattan, C.E. Williams, A. Scheepens, Prolactin is involved in glial responses following a focal injury to the juvenile rat brain. Neuroscience 145(3), 963–973 (2007)
L. Torner, S. Karg, A. Blume, M. Kandasamy, H.G. Kuhn, J. Winkler, L. Aigner, I.D. Neumann, Prolactin prevents chronic stress-induced decrease of adult hippocampal neurogenesis and promotes neuronal fate. J. Neurosci. 29(6), 1826–1833 (2009)
E.A. Cabrera-Reyes, E. Vergara-Castañeda, N. Rivero-Segura, M. Cerbón, Sex differences in prolactin and its receptor expression in pituitary, hypothalamus, and hippocampus of the rat. Rev. Mex. Endocrinol. Metab. Nutr. 2(2), 60–67 (2015)
X.J. Pi, D.R. Grattan, Distribution of prolactin receptor immunoreactivity in the brain of estrogen-treated, ovariectomized rats. J. Comp. 394, 462–474 (1998)
Allen Institute for Brain Science, Allen Mouse Brain Atlas. http://mouse.brain-map.org/experiment/show/72340223 (2004).
M. Shamgochian, C. Avakian, N. Truong, S. Stone, K. Tang, W. DeVito, Regulation of prolactin receptor expression by estradiol in the female rat brain. Neuroreport. 6(18), 2537–2541 (1995)
P. Mann, R. Bridges, Prolactin receptor gene expression in the forebrain of pregnant and lactating rats. Brain Res. Mol. Brain Res. 105(1–2), 136–145 (2002)
S. Chiu, R.D. Koos, P.M. Wise, Detection of prolactin receptor (PRL-R) mRNA in the rat hypothalamus and pituitary gland. Endocrinology 130(3), 1747–1749 (1992)
S.H. Yip, R. Eguchi, D.R. Grattan, S.J. Bunn, Prolactin signalling in the mouse hypothalamus is primarily mediated by signal transducer and activator of transcription factor 5b but not 5a. J. Neuroendocrinol. 24(12), 1484–1491 (2012)
R. Das, B. Vonderhaar, Transduction of prolactin’s (PRL) growth signal through both long and short forms of the PRL receptor. Mol. Endocrinol. 9, 1750–1759 (1995)
J. Harris, P.M. Stanford, S.R. Oakes, C.J. Ormandy, Prolactin and the prolactin receptor: new targets of an old hormone. Ann. Med. 36(6), 414–425 (2004)
L. Torner, E. Tinajero, N. Lajud, A. Quintanar-Stéphano, E. Olvera-Cortés, Hyperprolactinemia impairs object recognition without altering spatial learning in male rats. Behav. Brain Res. 252, 32–39 (2013)
M.J. Patil, M.A. Henry, A.N. Akopian, Prolactin receptor in regulation of neuronal excitability and channels. Channels 8(3), 193–202 (2014)
F. Drago, Prolactin and sexual behavior: a review. Neurosci. Biobehav. Rev. 8, 433–439 (1984)
D. Tejadilla, M. Cerbón, T. Morales, Prolactin reduces the damaging effects of excitotoxicity in the dorsal hippocampus of the female rat independently of ovarian hormones. Neuroscience 169(3), 1178–1185 (2010)
A. Vanoye-Carlo, T. Morales, E. Ramos, A. Mendoza-Rodríguez, M. Cerbón, Neuroprotective effects of lactation against kainic acid treatment in the dorsal hippocampus of the rat. Horm. Behav. 53(1), 112–123 (2008)
V. Cabrera, D. Cantú, E. Ramos, A. Vanoye-Carlo, M. Cerbón, T. Morales, Lactation is a natural model of hippocampus neuroprotection against excitotoxicity. Neurosci. Lett. 461(2), 136–139 (2009)
V. Cabrera, E. Ramos, A. González-Arenas, M. Cerbón, I. Camacho-Arroyo, T. Morales, Lactation reduces glial activation induced by excitotoxicity in the rat hippocampus. J. Neuroendocrinol. 25(6), 519–527 (2013)
R. Brown, A. Herbison, D. Grattan, Effects of prolactin and lactation on A15 dopamine neurones in the rostral preoptic area of female mice. J. Neuroendocrinol. 27(9), 708–717 (2015)
J.A. Seggie, G.M. Brown, Stress response patterns of plasma corticosterone, prolactin, and growth hormone in the rat, following handling or exposure to novel environment. Can. J. Physiol. Pharmacol. 53(4), 629–637 (1975)
A.C. de Moura, V.M. Lazzari, R.O. Becker, M.S. Gil, C.A. Ruthschilling, G. Agnes, S. Almeida, A.B. da Veiga, A.B. Luicion, M. Giovenardo, Gene expression in the CNS of lactating rats with different patterns of maternal behavior. Neurosci. Res. 99, 8–15 (2015)
C.M. Larsen, I.C. Kokay, D.R. Grattan, Male pheromones initiate prolactin-induced neurogenesis and advance maternal behavior in female mice. Horm. Behav. 53(4), 509–517 (2008)
F. Lévy, M. Keller, P. Poindron, Olfactory regulation of maternal behavior in mammals. Horm. Behav. 46(3), 284–302 (2004)
H. Salais-López, E. Lanuza, C. Agustín-Pavón, F. Martínez-García, Tuning the brain for motherhood: prolactin-like central signalling in virgin, pregnant, and lactating female mice. Brain Struct. Funct. 222(2), 895–921 (2017)
M. Freemark, P. Driscoll, J. Andrews, P.A. Kelly, M. Royster, Ontogenesis of prolactin receptor gene expression in the rat olfactory system: potential roles for lactogenic hormones in olfactory development. Endocrinology 137(3), 934–942 (1996)
T. Shingo, C. Gregg, E. Enwere, H. Fujikawa, R. Hassam, C. Geary, J.C. Cross, S. Weiss, Pregnancy-stimulated neurogenesis in the adult female forebrain mediated by prolactin. Science 299(5603), 117–120 (2003)
R. Bridges, D. Grattan, Prolactin-induced neurogenesis in the maternal brain. Trends Endocrinol. Metab. 14(5), 199–201 (2003)
N., Lajud, R., Gonzalez-Zapien, A., Roque, E., Tinajero, J.J., Valdez, C., Clapp, L., Torner, Prolactin administration during early postnatal life decreases hippocampal and olfactory bulb neurogenesis and results in depressive-like behavior in adulthood. Horm. Behav. 64(5), 781–789 (2013)
A. Fleming, M. Korsmit, Plasticity in the maternal circuit: effects of maternal experience on Fos-Lir in hypothalamic, limbic, and cortical structures in the postpartum rat. Behav. Neurosci. 110(3), 567–582 (1996)
Y. Elyada, A. Mizrahi, Becoming a mother-circuit plasticity underlying maternal behavior. Curr. Opin. Neurobiol. 35, 49–56 (2015)
J.N. Lundström, A. Mathe, B. Schaal, J. Frasnelli, K. Nitzsche, J. Gerber, T. Hummel, Maternal status regulates cortical responses to the body odor of newborns. Front. Psychol. 4, 1–6 (2013)
L. Cohen, A. Mizrahi, Plasticity during motherhood: changes in excitatory and inhibitory layer 2/3 neurons in auditory cortex. J. Neurosci. 35(4), 1806–1815 (2015)
C. Gregg, V. Shikar, P. Larsen, G. Mak, A. Chojnacki, V.W. Yong, S. Weiss, White matter plasticity and enhanced remyelination in the maternal CNS. J. Neurosci. 27(8), 1812–1823 (2007)
M. Maheu, E. Akbari, A. Fleming, Callosal oligodendrocyte number in postpartum Sprague-Dawley rats. Brain Res. 24(1267), 18–24 (2009)
P. Mann, R. Bridges, Lactogenic hormone regulation of maternal behavior. Prog. Brain Res. 133, 251–262 (2001)
M. Numan, M. Numan, A lesion and neuroanatomical tract-tracing analysis of the role of the bed nucleus of the stria terminalis in retrieval behavior and other aspects of maternal responsiveness in rats. Dev. Psycobiol. 29(1), 23–51 (1996)
M. Numan, A neural circuitry analysis of maternal behavior in the rat. Acta Paediatr. Suppl. 397, 19–28 (1994)
A. Consiglio, A. Borsoi, G. Pereira, A. Lucion, Effects of oxytocin microinjected into the central amygdaloid nucleus and bed nucleus of stria terminalis on maternal aggressive behavior in rats. Physiol. Behav. 85(3), 354–362 (2005)
S. Kenny, L. Wright, A. Green, R. Mashoodh, T. Perrot, Expression of maternal behavior and activation of the bed nucleus of the stria terminalis during predatory threat exposure: modulatory effects of transport stress. Physiol. Behav. 17(123), 148–155 (2014)
L.P. Mangurian, R.J. Walsh, B.I. Posner, Prolactin enhancement of its own uptake at the choroid plexus. Endocrinology 131, 698–702 (1992)
R.A. Augustine, I.C. Kokay, Z.B. Andrews, S.R. Ladyman, D.R. Grattan, Quantitation of prolactin receptor mRNA in the maternal rat brain during pregnancy and lactation. J. Mol. Endocrinol. 31(1), 221–232 (2003)
H. Tabata, M. Kobayashi, J.H. Ikeda, N. Nakao, T.R. Saito, M. Tanaka, Characterization of multiple first exons in murine prolactin receptor gene and the effect of prolactin on their expression in the choroid plexus. J. Mol. Endocrinol. 48(2), 169–176 (2012)
X.J. Pi, D.R. Grattan, Differential expression of the two forms of prolactin receptor mRNA within microdissected hypothalamic nuclei of the rat. Brain Res. Mol. Brain Res. 59(1), 1–12 (1998)
R. Abs, E. Van Vleymen, P. Parizel, K. Van Acker, M. Martin, J. Martin, Congenital cerebellar hypoplasia and hypogonadotropic hypogonadism. J. Neurol. Sci. 98(2–3), 259–265 (1990)
G. Leng, R. Dyball, S. Luckman, Mechanisms of vasopressin secretion. Horm. Res. 37(1–2), 33–38 (1992)
G. Kennedy, The hypothalamic control of food intake in rats. Proc. R. Soc. Lond. B. Biol. Sci. 137(889), 535–549 (1950)
C.M., Brooks, E., Lambert, P., Bard, Experimental production of obesity in the monkey (Macaca mulatta). Fed. Proc. 1, 11 (1942)
D. Sauvé, B. Woodside, The effect of central administration of prolactin on food intake in virgin female rats is dose-dependent, occurs in the absence of ovarian hormones and the latency to onset varies with feeding regimen. Brain Res. 729(1), 75–81 (1996)
D. Sauve, B. Woodside, Neuroanatomical specificity of prolactin-induced hyperphagia in virgin female rats. Brain Res. 868(2), 306–314 (2000)
S. Mejía, L.M. Torner, M.C. Jeziorski, C. Gonzalez, M.A. Morales, G.M. Martínez de la Escalera, C.: Clapp, Prolactin and 16K prolactin stimulate release of vasopressin by a direct effect on hypothalamo-neurohypophyseal system. Endocrine 20(1–2), 155–162 (2003)
S. Mejía, M. Morales, M. Zetina, G. Martínez de la Escalera, C.: Clapp, Immunoreactive prolactin forms colocalize with vasopressin in neurons of the hypothalamic paraventricular and supraoptic nuclei. Neuroendocrinology 66(3), 151–159 (1997)
C. Pedersen, J. Ascher, Y. Monroe, A.J. Prange, Oxytocin induces maternal behavior in virgin female rats. Science 216(4546), 648–650 (1982)
J.M. Zimmermann-Peruzatto, V.M. Lazzari, A.C. de Moura, S. Almeida, M. Giovenardi, Examining the role of vasopressin in the modulation of parental and sexual behaviors. Front. Psychiatry 6, 1–8 (2015)
H.H. Van Tol, E.L. Bolwerk, B. Liu, J.P. Burbach, Oxytocin and vasopressin gene expression in the hypothalamo-neurohypophyseal system of the rat during the estrous cycle, pregnancy, and lactation. Endocrinology 122(3), 945–951 (1988)
N. Donner, I. Neumann, Effects of chronic intracerebral prolactin on the oxytocinergic and vasopressinergic system of virgin ovariectomized rats. Neuroendocrinology 90(3), 315–322 (2009)
R., Augustine, G., Bouwer, A., Seymour, D., Grattan, C., Brown, Reproductive regulation of gene expression in the hypothalamic supraoptic and paraventricular nuclei. J. Neuroendocrinol. (4), (2016). doi:10.1111/jne.12350
K. Suzuki, N. Koizumi, H. Hirose, R. Hokao, N. Takemura, S. Motoyoshi, Changes in plasma arginine vasopressin concentration during lactation in rats. Comp. Med. 50(3), 277–280 (2000)
N. Donner, R. Bredewold, R. Maloumby, I.D. Neumann, Chronic intracerebral prolactin attenuates neuronal stress circuitries in virgin rats. Eur. J. Neurosci. 25(6), 1804–1814 (2007)
L. Krulich, E. Hefco, P. Illner, C.B. Read, The effects of acute stress on the secretion of LH, FSH, prolactin and GH in the normal male rat, with comments on their statistical evaluation. Neuroendocrinology 16, 293–311 (1974)
B. Bodosi, F. Obál Jr., J. Gardi, J. Komlódi, J. Fang, J.M. Krueger, An ether stressor increases REM sleep in rats: possible role of prolactin. Am. J. Physiol. 279(5), 1590–1589 (2000)
R.R. Gala, The physiology and mechanisms of the stress-induced changes in prolactin secretion in the rat. Life Sci. 46, 1407–1420 (1990)
F. Obal Jr., M. Opp, A.B. Cady, L. Johannsen, J.M. Krueger, Prolactin, vasoactive intestinal peptide, and peptide histidine methionine elicit selective increases in REM sleep in rabbits. Brain Res. 490, 292–300 (1989)
P. Meerlo, A. Easton, B.M. Bergmann, F.W. Turek, Restraint increases prolactin and REM sleep in C57BL/6J mice but not in BALB/cJ mice. Am. J. Physiol. 281(3), 846–854 (2001)
R.B. Machado, M.R. Rocha, D. Suchecki, Brain prolactin is involved in stress-induced REM sleep rebound. Horm. Behav. 89, 38–47 (2016)
R.M. Frieboes, H. Murck, G.K. Stalla, I.A. Antonijevic, A. Steiger, Enhanced slow wave sleep in patients with prolactinoma. J. Clin. Endocrinol. Metab. 83, 2706–2710 (1998)
K. Koike, A. Miyake, T. Aono, T. Sakumoto, M. Ohmichi, M. Yamaguchi, O. Tanizawa, Effect of prolactin on the secretion of hypothalamic GnRH and pituitary gonadotropins. Horm. Res. 35(1), 5–12 (1991)
R. Araujo-Lopes, J. Crampton, N. Aquino, R. Miranda, I. Kokay, A. Reis, C.R. Franci, D.R. Grattan, R.E. Szawka, Prolactin regulates kisspeptin neurons in the arcuate nucleus to suppress LH secretion in female rats. Endocrinology 155(3), 1010–1020 (2014)
J. Clarkson, X. d’Anglemont de Tassigny, W. Colledge, A. Caraty, A. Herbison, Distribution of kisspeptin neurones in the adult female mouse brain. J. Neuroendocrinol. 21(8), 673–682 (2009)
I.C. Kokay, S.L. Petersen, D.R. Grattan, Identification of prolactin-sensitive GABA and kisspeptin neurons in regions of the rat hypothalamus involved in the control of fertility. Endocrinology 152(2), 526–535 (2011)
I. Cohen-Becker, M. Selmanoff, P. Wise, Hyperprolactinemia alters the frequency and amplitude of pulsatile luteinizing hormone secretion in the ovariectomized rat. Neuroendocrinology 42(4), 328–333 (1986)
A. Lerant, M.E. Freeman, Ovarian steroids differentially regulate the expression of PRL-R in neuroendocrine dopaminergic neuron populations: A double label confocal microscopic study. Brain Res. 802(1–2), 141–154 (1998)
G. Anderson, D. Grattan, W. van den Ancker, R. Bridges, Reproductive experience increases prolactin responsiveness in the medial preoptic area and arcuate nucleus of female rats. Endocrinology 147, 4688–4694 (2006)
L. Torner, R. Maloumby, G. Nava, J. Aranda, C. Clapp, I.D. Neumann, In vivo release and gene upregulation of brain prolactin in response to physiological stimuli. Eur. J. Neurosci. 19(6), 1601–1608 (2004)
J.A. McHenry, D.R. Rubinow, G.D. Stuber, Maternally responsive neurons in the bed nucleus of the stria terminalis and medial preoptic area: Putative circuits for regulating anxiety and reward. Front. Neuroendocrinol. 38, 65–72 (2015)
R.S. Bridges, M. Numan, P.M. Ronsheim, P.E. Mann, C.E. Lupini, Central prolactin infusions stimulate maternal behavior in steroid-treated, nulliparous female rats. Proc. Natl. Acad. Sci. USA 87(20), 8003–8007 (1990)
F.K. Stephan, I. Zucker, Circadian rhythms in drinking behavior and locomotor activity of rats are eliminated by hypothalamic lesions. Proc. Natl. Acad. Sci. USA 69(6), 1583–1586 (1972)
C. Bethea, J. Neill, Lesions of the suprachiasmatic nuclei abolish the cervically stimulated prolactin surges in the rat. Endocrinology 107(1), 1–5 (1980)
K. Brown-Grant, G. Raisman, Abnormalities in reproductive function associated with the destruction of the suprachiasmatic nuclei in female rats. Proc. R. Soc. Lond. B Biol. Sci. 198(1132), 279–296 (1977)
J.T. Pan, R.R. Gala, Central nervous system regions involved in the estrogen-induced afternoon prolactin surge. II. Implantation studies. Endocrinology 117(1), 388–395 (1985)
J. Pan, R. Gala, Central nervous system regions involved in the estrogen-induced afternoon prolactin surge. I. Lesion studies. Endocrinology 117(1), 382–387 (1985)
I. Clarke, J. Cummins, D. de Kretser, Pituitary gland function after disconnection from direct hypothalamic influences in the sheep. Neuroendocrinology 36(5), 376–384 (1983)
J.D. Johnston, D.J. Skene, Regulation of mammalian neuroendocrine physiology and rhythms by melatonin. J. Endocrinol. 226(2), T187–T198 (2015)
S. Shyr, W. Crowley, C. Grosvenor, Effect of neonatal prolactin deficiency on prepubertal tuberoinfundibuler and tuberohypophyseal dopaminergic neuronal activity. Endocrinology 119(3), 1217–1221 (1986)
C. Grosvenor, N. Whitworth, Accumulation of prolactin in maternal milk and its transfer to circulation of neonate rat: a review. Endocrinol. Exp. 17, 271–282 (1983)
M. Royster, P. Driscoll, P. Kelly, M. Freemark, The prolactin receptor in the fetal rat: cellular localization of messenger ribonucleic acid, immunoreactive protein, and ligand-binding activity and induction of expression in late gestation. Endocrinology 136(9), 3892–3900 (1995)
A.I. Melo, M. Perez-Ledezma, C. Clapp, E. Arnold, J.C. Rivera, A.S. Fleming, Effects of prolactin deficiency during the early postnatal period on the development of maternal behavior in female rats: Mother’s milk makes the difference. Horm. Behav. 56(3), 281–291 (2009)
E. Vergara-Castañeda, D.R. Grattan, H. Pasantes-Morales, M. Pérez-Domínguez, E.A. Cabrera-Reyes, T. Morales, M. Cerbón, Prolactin mediates neuroprotection against excitotoxicity in primary cell cultures of hippocampal neurons via its receptor. Brain Res. 1636, 192–199 (2016)
N.V. Emanuele, L. Metcalfe, L. Wallock, J. Tentler, T.C. Hagen, C.T. Beer, D. Martinson, P.W. Gout, L. Kirsteins, A.M. Lawrence, Extrahyponthalamic brain prolactin: characterization and evidence for independence from pituitary prolactin. Brain Res. 421(1–2), 255–262 (1987)
H. Eichenbaum, Hippocampus: cognitive processes and neural representations that underlie declarative memory. Neuron 44(1), 109–120 (2004)
G. Love, N. Torrey, I. McNamara, M. Morgan, M. Banks, N. Hester, E.R. Glasper, A.C. Devries, C.H. Kinsley, K.G. Lambert, Maternal experience produces long-lasting behavioral modifications in the rat. Behav. Neurosci. 119(4), 1084–1096 (2005)
C.H. Kinsley, L. Madonia, G.W. Gifford, K. Tureski, G.R. Griffin, C. Lowry, J. Williams, J. Collins, H. McLearie, K.G. Lambert, Motherhood improves learning and memory. Nature 402(6758), 137–138 (1999)
J.L. Pawluski, B.L. Vanderbyl, K. Ragan, L.A. Galea, First reproductive experience persistently affects spatial reference and working memory in the mother and these effects are not due to pregnancy or “mothering” alone. Behav. Brain Res. 175(1), 157–165 (2006)
J.L. Pawluski, S.K. Walker, L.A. Galea, Reproductive experience differentially affects spatial reference and working memory performance in the mother. Horm. Behav. 49(2), 143–149 (2006)
J. Henry, B. Sherwin, Hormones and cognitive functioning during late pregnancy and postpartum: a longitudinal study. Behav. Neurosci. 126(1), 73–85 (2012)
T. Castanho, P. Moreira, C. Portugal-Nunes, A. Novais, P. Costa, J. Palha, N. Sousa, N.C. Santos, The role of sex and sex-related hormones in cognition, mood and well-being in older men and women. Biol. Psychol. 103, 158–166 (2014)
T.L. Walker, J. Vukovic, M.M. Koudijs, D.G. Blackmore, E.W. Mackay, A.M. Sykes, R.W. Overall, A.S. Hamlin, P.F. Bartlett, Prolactin stimulates precursor cells in the adult mouse hippocampus. PLoS One 7(9), 1–11 (2012)
J. Reyes-Mendoza, T. Morales, Post-treatment with prolactin protects hippocampal CA1 neurons of the ovariectomized female rat against kainic acid-induced neurodegeneration. Neuroscience 328, 58–68 (2016)
J.L. Pawluski, L.A. Galea, Reproductive experience alters hippocampal neurogenesis during the postpartum period in the dam. Neuroscience 149(1), 53–67 (2007)
G. Mak, S. Weiss, Paternal recognition of adult offspring mediated by newly generated CNS neurons. Nat. Neurosci. 13(6), 753–758 (2010)
G.V. Pardo, J.F. Goularte, A.L. Hoefel, A.L. de Castro, L.C. Kucharski, A. da Rosa Araujo, A.B.: Lucion, Effects of sleep restriction during pregnancy on the mother and fetuses in rats. Physiol. Behav. 1(155), 66–76 (2016)
G. Mak, E. Enwere, C. Gregg, T. Pakarainen, M. Poutanen, I. Huhtaniemi, S. Weiss, Male pheromone-stimulated neurogenesis in the adult female brain: possible role in mating behavior. Nat. Neurosci. 10(8), 1003–1011 (2007)
E. Gould, B.S. McEwen, P. Tanapat, L.A. Galea, E. Fuchs, Neurogenesis in the dentate gyrus of the adult tree shrew is regulated by psychosocial stress and NMDA receptor activation. J. Neurosci. 17(7), 2492–2498 (1997)
R.S. Duman, J. Malberg, S. Nakagawa, Regulation of adult neurogenesis by psychotropic drugs and stress. J. Pharmacol. Exp. Ther. 299(2), 401–407 (2001)
E.A. Nimchinsky, B.L. Sabatini, K. Svoboda, Structure and function of dendritic spines. Annu. Rev. Physiol. 64, 313–353 (2001)
C.H. Kinsley, R. Trainer, G. Stafisso-Sandoz, P. Quadros, L.K. Marcus, C. Hearon, E.A. Meyer, N. Hester, M. Morgan, F.J. Kozub, K.G. Lambert, Motherhood and the hormones of pregnancy modify concentrations of hippocampal neuronal dendritic spines. Horm. Behav. 49(2), 131–142 (2006)
J.L. Pawluski, L.A. Galea, Hippocampal morphology is differentially affected by reproductive experience in the mother. J. Neurobiol. 66(1), 71–81 (2006)
J. Brusco, R. Wittmann, M. de Azevedo, A. Lucion, C. Franci, M. Giovenardi, A.A. Rasia-Filho, Plasma hormonal profiles and dendritic spine density and morphology in the hippocampal CA1 stratum radiatum, evidenced by light microscopy, of virgin and postpartum female rats. Neurosci. Lett. 438(3), 346–350 (2008)
R. Abbud, G. Hoffman, M. Smith, Cortical refractoriness to N-methyl-D,L-aspartic acid (NMDA) stimulation in the lactating rat: recovery after pup removal and blockade of progesterone receptors. Brain Res. 604(1–2), 16–23 (1993)
C.A. Standley, N-methyl-D-aspartate receptor binding is altered and seizure potential reduced in pregnant rats. Brain Res. 844(1–2), 10–19 (1999)
P. Anborgh, C. Godin, M. Pampillo, G. Dhami, L. Dale, S. Cregan, R. Truant, S.S. Ferguson, Inhibition of metabotropic glutamate receptor signaling by the huntingtin-binding protein optineurin. J. Biol. Chem. 280(41), 34840–34848 (2005)
M.R. Hynd, H.L. Scott, P.R. Dodd, Glutamate-mediated excitotoxicity and neurodegeneration in Alzheimer’s disease. Neurochem. Int. 45(5), 583–595 (2004)
M. Doretto, M. Oliveira-e-Silva, D. Ferreira-Alves, S. Pires, N. Garcia-Cairasco, A. Reis, Effect of lactation on the expression of audiogenic seizures: association with plasma prolactin profiles. Epilepsy Res. 54, 109–121 (2003)
P. Berzaghi Mda, D. Amado, E. Cavalheiro, Pregnancy decreases the frequency of spontaneous recurrent seizures in rats with kainic acid lesions of the hippocampus. Epilepsy Res. 1(2), 142–144 (1987)
T. Morales, M. Lorenson, A.M. Walker, E. Ramos, Both prolactin (PRL) and a molecular mimic of phosphorylated PRL, S179D-PRL, protect the hippocampus of female rats against excitotoxicity. Neuroscience 258, 211–217 (2014)
N.A. Rivero-Segura, E. Flores-Soto, S. García de la Cadena, I. Coronado-Mares, J.C. Gomez-Verjan, D.G. Ferreira, E.A. Cabrera-Reyes, L.V. Lopes, L. Massieu, M.: Cerbón, Prolactin-induced neuroprotection against glutamate excitotoxicity is mediated by the reduction of [Ca2+]i overload and NF-κB activation. PLoS One 12(5), e0176910 (2017)
A.M. Thomson, Neocortical layer 6, a review. Front. Neuroanat. 4, 13 (2010)
I.Y. Zhou, R.W. Chan, L.C. Ho, E.X. Wu, Longitudinal metabolic changes in the hippocampus and thalamus of the maternal brain revealed by proton magnetic resonance spectroscopy. Neurosci. Lett. 553, 170–175 (2013)
J. Broida, S.D. Michael, B. Svare, Plasmin prolactin levels are not related to the initiation, maintenance, and decline of postpartum aggression in mice. Behav. Neural. Biol. 32(1), 121–125 (1981)
M. Garland, B. Svare, Suckling stimulation modulates the maintenance of postpartum aggression in mice. Physiol. Behav. 44(3), 301–305 (1988)
O.J. Bosch, I.D. Neumann, Vasopressin released within the central amygdala promotes maternal aggression. Eur. J. Neurosci. 31(5), 883–891 (2010)
M. Davis, The role of the amygdala in fear and anxiety. Annu. Rev. Neurosci. 15, 353–375 (1992)
J. Allen, C. Allen, Role of the amygdaloid complexes in the stress-induced release of ACTH in the rat. Neuroendocrinology 15(3–4), 220–230 (1974)
N. Donner, R. Bredewold, R. Maloumby, I. Neumann, Chronic intracerebral prolactin attenuates neuronal stress circuitries in virgin rats. Eur. J. Neurosci. 25(6), 1804–1814 (2007)
L. Torner, N. Toschi, A. Pohlinger, R. Landgraf, I.D. Neumann, Anxiolytic and anti-stress effects of brain prolactin: improved efficacy of antisense targeting of the prolactin receptor by molecular modeling. J. Neurosci. 21(9), 3207–3214 (2001)
O. Picazo, A. Fernández-Guasti, Changes in experimental anxiety during pregnancy and lactation. Physiol. Behav. 54(2), 295–299 (1993)
D. Toufexis, S. Tesolin, N. Huang, C. Walker, Altered pituitary sensitivity to corticotropin-releasing factor and arginine vasopressin participates in the stress hyporesponsiveness of lactation in the rat. J. Neuroendocrinol. 11(10), 757–764 (1999)
L.D. Sanford, P. Nassar, R.J. Ross, J. Schulkin, A.R. Morrison, Prolactin microinjections into the amygdalar central nucleus lead to decreased NREM sleep. Sleep Res. Online 1, 109–113 (1998)
X. Pi, J.L. Voogt, D.R. Grattan, Detection of prolactin receptor mRNA in the corpus striatum and substantia nigra of the rat. J. Neurosci. Res. 67(4), 551–558 (2002)
B.D. Palma, D.C. Hipolide, S. Tufik, Effects on prolactin secretion and binding to dopaminergic receptors in sleep-deprived lupus-prone mice. Braz. J. Med. Biol. Res. 42(3), 299–304 (2009)
P. Malven, Inhibition of prolactin release in conscious sheep following stimulation of nucleus accumbens and caudate nucleus. Neuroendocrinology 28(3), 160–168 (1979)
R.S.E. Brown, A.E. Herbison, D.R. Grattan, Differential changes in responses of hypothalamic and brainstem neuronal populations to prolactin during lactation in the mouse. Biol. Reprod. 84, 826–836 (2011)
L. Caligaris, S. Taleisnik, Involvement of neurones containing 5-hydroxytryptamine in the mechanism of prolactin release induced by oestrogen. J. Neuroendocrinol. 62(1), 25–33 (1974)
G.A. Jahn, R.P. Deis, Effect of serotonin antagonists on prolactin and progesterone secretion in rats: Evidence that the stimulatory and inhibitory actions of serotonin on prolactin release may be mediated through different receptors. J. Endocrinol. 117(3), 415–422 (1988)
A. Mistry, J.L. Voogt, Role of serotonin in nocturnal and diurnal surges of prolactin in the pregnant rat. Endocrinology 125(6), 2875–2880 (1989)
L. Paut-Pagano, R. Roky, J. Valatx, K. Kitahama, M. Jouvet, Anatomical distribution of prolactin-like immunoreactivity in the rat brain. Neuroendocrinology 58(6), 682–695 (1993)
M. Angoa-Pérez, D. Kuhn, Neuronal serotonin in the regulation of maternal behavior in rodents. Neurotransmitter 2, 615–625 (2015)
M.C. Popesco, A. Frostholm, K. Rejniak, A. Rotter, Digital transcriptome analysis in the aging cerebellum. Ann. N.Y. Acad. Sci. 1019, 58–63 (2004)
A.L. Barofsky, J. Taylor, V.J. Massari, Dorsal raphe-hypothalamic projections provide the stimulatory serotonergic input to suckling-induced prolactin release. Endocrinology 113(5), 1894–1903 (1983)
P. Eriksson, E. Perfilieva, T. Bjork-Eriksson, A. Alborn, C. Nordborg, D. Peterson, F.H. Gage, Neurogenesis in the adult human hippocampus. Nat. Med. 4(11), 1313–1317 (1998)
Acknowledgements
This work was supported by PAPIIT, UNAM grant (IN220315 and IN216817). PhD. Limon-Morales O. is recipient of a DGAPA, UNAM Post-doctoral Fellowship grant.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Erika Alejandra Cabrera-Reyes and Ofelia Limón-Morales contributed equally to this work
Rights and permissions
About this article
Cite this article
Cabrera-Reyes, E.A., Limón-Morales, O., Rivero-Segura, N.A. et al. Prolactin function and putative expression in the brain. Endocrine 57, 199–213 (2017). https://doi.org/10.1007/s12020-017-1346-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-017-1346-x