Abstract
The human placenta produces high amounts of estradiol. 17β-hydroxysteroid dehydrogenase type 2 (17βHSD2) is expressed by placental endothelial cells and was proposed to regulate sex hormone levels. Previous results obtained in term placenta suggested that 17βHSD2 expression and activity differ among umbilical cord vessels. In this study, 17βHSD2 expression level and enzymatic activity, and estrogen receptor α and β expression levels, were measured in endothelial cell cultures from umbilical arteries (HUAEC) and vein (HUVEC) using real-time quantitative PCR, western blot, and radiolabeled steroids. 17βHSD2-specific activities were also measured in proximal and distal segments of freshly isolated umbilical cord arteries and vein. 17βHSD2 mRNA level and activity were higher in HUAEC than in HUVEC. Activity was higher in umbilical arteries than in the umbilical vein. In arteries, enzymatic activity was higher near the placenta, suggesting a gradient of expression. No difference was found in ERα expression, whereas ERβ was expressed at a higher level in HUAEC than in HUVEC. Expression profiles of estrogen receptors and 17βHSD2 suggest a vessel type-specific response to estrogens. Our data support a differential modulation of biologically active sex steroid levels according to the vessel type in the foeto-placental unit, with apparent higher inactivation in the arterial system.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The human placenta secretes large amounts of estrogens [estrone (E1) and estradiol (E2)] [1, 2]. E2 is important for the development and the maturation of several fetal organs and systems such as the lung and the hypothalamo-hypophyseal-adrenal axis. In the human placenta, E2 synthesis depends on dehydroepiandrosterone (DHEA) and its sulfate (DHEAS) from both fetal and maternal origin. The sulfatase converts DHEAS to DHEA, which is then converted into androstenedione by 3β-hydroxysteroid dehydrogenase type 1 (3βHSD). Androstenedione is aromatized into E1 by cytochrome P450 aromatase, and E1 is finally reduced into E2 by 17β-hydroxysteroid dehydrogenase (17βHSD) type 1. The human placenta expresses mainly two 17βHSD isoforms, namely, types 1 and 2. Type 1 exclusively reduces E1 into E2 [3, 4], whereas type 2 oxidizes E2 and testosterone into E1 and androstenedione, respectively, with similar affinity [5, 6], and catalyzes the conversion of 20α-dihydroprogesterone to progesterone. These two enzymes catalyze the last and only reversible step in the reaction sequences leading to E2.
In human placenta, 17βHSD1 is exclusively expressed by syncytium of floating villi [4, 7, 8], whereas 17βHSD2 is only expressed by endothelial cells of fetal vessels [8–10]. In term placenta and stem villi [11], some large vessels strongly express 17βHSD2 mRNA and protein, while others show a barely detectable signal [9, 10]. In contrast, 17βHSD2 protein is strongly and uniformly expressed in the paravascular capillary network of the stem villi and in the sinusoidal capillaries of terminal villi [10]. We previously showed using Northern blot that 17βHSD2 mRNA level was higher in umbilical arteries than in vein [9]. In addition, the signal in the total umbilical cord was weak in comparison to the villi, suggesting the presence of an expression gradient along the foeto-placental unit.
E2 has vasoprotective effects, including the regulation of vascular tone, and acts on endothelial cells via estrogen receptors alpha (ERα) and beta (ERβ) [12]. For example, estrogens induce the activation of endothelial nitric oxide synthase, resulting in rapid vasodilatation [13–15], and reduce the expression of endothelin-1 [16], a vasoconstrictor peptide. Hervé et al. [17] showed that human umbilical vein endothelial cells (HUVEC) express ERβ mRNA, but were unable to detect ERα mRNA. In HUVEC, ERβ, but not ERα, was detected by immunohistochemistry [18], whereas others demonstrated that HUVEC expresses both ERα and ERβ mRNA [19] and protein [20]. Tschugguel et al. [21] showed that ERα and ERβ mRNA and protein are expressed in human umbilical artery endothelial cells (HUAEC). To the best of our knowledge, no study has yet compared mRNA and protein expression levels of the two ER types in HUVEC and HUAEC. A differential distribution of ER and 17βHSD2 expression in endothelial cell types may be suggestive of a vessel type-specific response to E2, since 17βHSD2 inactivates the latter.
We tested the hypotheses that 17βHSD2 expression and activity would be different between HUVEC and HUAEC and that the activity would be higher in umbilical vessels isolated near the placental insertion point than in distal ones. We deemed that information to be relevant regarding the regulation of active estrogen and androgen levels in the placental unit in relation to the protection of the fetus and/or the mother to excessive hormone exposure. We quantified mRNA level and measured enzymatic activity of 17βHSD2 in HUAEC, HUVEC, human aortic endothelial cells (HAEC), and in total term villi. 17βHSD2 activity was also measured in umbilical artery and vein segments isolated from different regions of the cord. HAEC were included as a point of comparison for extra-placental endothelial cells. To better understand the role of 17βHSD2 and to further investigate ER expression profiles in endothelial cells of umbilical vessels, we quantified ERα and ERβ mRNA levels in HUAEC, HUVEC, HAEC, and in term villi. 17βHSD2, ERα, and ERβ were also studied by Western blot analysis in HUAEC, HUVEC, and total villi.
Materials and methods
Cell culture and human tissue collection
Primary cultures of HUAEC, HUVEC, and HAEC were purchased from Clonetics (Basel, Switzerland, CC-2520, CC-2517, and CC-2535, respectively). HUAEC and HUVEC were derived from umbilical cords of term pregnancies. HUVEC were also isolated from three umbilical cords at term [22]. Informed consents were obtained according to the policies for the Human Studies and the Institutional Review Board of the Centre Hospitalier Universitaire de Québec (protocol 75-05-04). In brief, a canula was inserted into the umbilical cord vein. The vein was washed with phosphate-buffered saline (PBS) and then incubated with collagenase type 1 (Sigma-Aldrich, St. Louis, MO, USA), 0.1% in 0.02 M HEPES buffer, for 10 min at 37°C. The endothelial cell layer was detached using HEPES buffer and centrifuged at 100×g for 7 min. Cells were grown in gelatin-coated flasks according to Clonetics recommendations (endothelial cell EGM-2 medium, 2% FBS supplemented with VEGF, hFGF-B, R3-IGF-1, hEGF, ascorbic acid, and gentamicin). The purity of HUVEC cultures was confirmed visually. The latter method used leads to high-purity endothelial cell cultures with, rarely, a very limited contamination with smooth muscle cells. Such contamination is easily noticeable since endothelial and fibroblastic phenotypes are distinguishable visually. HUAEC and HUVEC were included in experiments at comparable cell passage number (5–10).
Steroid metabolism in whole cells
Cells (50000–100000) were incubated in 24-well plates with 1 ml of medium containing tritiated testosterone (2 × 106 dpm) (NEN Life Science Products, Boston, MA, USA) for 24 h. Media were frozen until steroid extraction, and 100 μl/well of methanol were added before DNA quantification using 3,5-diaminobenzoic acid as described [23, 24]. Steroids were extracted twice with 5 ml diethylether, evaporated, applied to silica gel-coated plates, and resolved in toluene–acetone (4:1, v/v). Radioactive signals were detected using a Storm apparatus (Molecular Dynamics Inc, Sunnyvale, CA, USA), spots were scraped, and dpm values were then determined by scintillation counting (model LS3801, Beckman, Mississauga, ON, Canada). The specific 17βHSD activity (in pmol/24 h) was calculated from the specific radioactivity of testosterone and the percentage of substrate converted to androstenedione from the dpm values measured, and was normalized per microgram of DNA.
17βHSD2 activity in sonicated cells
HUAEC, HUVEC, and HAEC (1 × 106) cells were homogenized in 0.04 M potassium phosphate, disrupted in a sonicator, and centrifuged at 1000×g for 10 min. Assays were run at pH 9.0 (0.08 M bicine) with 0.5 mM NAD and 1 μM of tritiated E2 or tritiated testosterone for 180 min. 17βHSD2 specific activity was measured as described [25]. Reaction mixtures were transferred to silica gel HL plates and air-dried. Unlabeled E2 and E1 (or testosterone and androstenedione) were added as carriers. The plates were developed in benzene–acetone (4:1) and air-dried. Steroids were located by a spraying of water, and the plates were allowed to air-dry. Spots were scraped for scintillation counting. The specific enzymatic activity (conversion of E2 to E1 or of testosterone to androstenedione) was calculated from the specific radioactivity of the substrate and the percentage of substrate converted to product from the dpm values measured, and expressed in pmol/mg of protein/30 min.
17βHSD2 activity in fresh tissues
Umbilical cords and placentas were collected at term (n = 3). Pieces of 2 cm3 of term villi were collected; decidua and membranes were removed. Cords were divided into three segments: proximal (placental side), central, and distal (fetal side). The central part was discarded. Vein and arteries from distal and proximal segments were dissected free of connective tissue (~5 cm). Tissues were washed in ice-cold PBS, homogenized in 0.25 M sucrose, 10 mM 2-mercaptoethanol, and 0.1 M bicine, pH 9.0, then centrifuged at 1500×g for 10 min. 17βHSD2 activity assays were performed as described (see previous section and [25]).
Quantitative real-time PCR
RNA extraction, cDNA synthesis, and real-time quantitative PCR were performed as described [26]. For details on the genes analyzed and on quantitative real-time PCR parameters, see [26], except for ERα and ERβ. Primers for ERα (NM_000125): 5′-AAGAGCTGCCAGGCCTGCC-3′ and 5′-TTGGCAGCTCTCATGTCTCC-3′; amplicon length, 167 bp. Primers for ERβ (NM_001437): 5′-ACAAGGGCATGGAACATCTGC-3′ and 5′-GGGTTCTGGGAGCCCTCTTT-3′; amplicon length, 171 bp. After enzyme activation (10 min, 95°C), 40 cycles were performed: 5 s, denaturation 95°C; 5 s, annealing temperature (ERα: 69°C; ERβ: 66°C); 20 s, elongation 72°C; and 5 s, temperature of fluorescence intensity reading (ERα: 83°C; ERβ: 86°C). Standard curves were prepared with PCR amplicons diluted in water containing 0.1× reverse transcriptase buffer [27]. We assessed the expression stability of five housekeeping genes (GAPDH, HPRT1, SDHA, TBP, and YWHAZ) using the geNorm software [28]. Mean normalization factors were calculated from the expression levels of SDHA, TBP, and YWHAZ.
Western blot analysis
Microsomal and cytosolic protein fractions were isolated from HUVEC and HUAEC cultures as described [9]. Cells were homogenized in ice-cold buffer containing 40 mM potassium phosphate (pH 7.0), 1.0 mM EDTA, and 20% (v/v) glycerol. Samples were centrifuged at 1000×g for 10 min and at 105000×g for 1 h. Supernatants were saved as cytosol, and pellets as microsomes. Protein concentrations were measured using the BCA Protein Assay Reagent (Pierce Chemical, Thermo Fisher Scientific, Rockford, IL, USA). The total term villi sample was prepared as described [10]. 35 μg of microsomal extracts from HUVEC and HUAEC and 15 μg of proteins from term villi were resolved by SDS-PAGE and transferred to nitrocellulose membranes (Bio-Rad, Mississauga, ON, Canada). Ponceau Red staining was used to assess the efficiency of the protein transfer. Membranes were blocked overnight at 4°C with 5% (w/v) fat-free milk powder in PBS containing 0.05% (v/v) Tween 20. Immunoreactions were performed with an anti-ERα (Santa Cruz Biotechnology, Santa Cruz, CA, USA), an anti-ERβ (ABR Bio Reagents, Thermo Fisher Scientific), or with an anti-17βHSD2 antibody [10] (1:500, 1:500, and 1:1000, respectively) for 2 h at room temperature. Bound antibodies were visualized with horseradish peroxidase-conjugated goat anti-rabbit antibodies using a Western Lightning kit (Perkin Elmer, Waltham, MA, USA).
Statistical analysis
Statistics were performed using GraphPad Prism 3.0 (GraphPad Software, La Jolla, CA, USA). One-way ANOVA followed by a Tukey’s test was used to compare groups. A P-value ≤0.05 was considered as significant.
Results
17βHSD2 mRNA level in HUVEC, HUAEC, HAEC, and term villi
17βHSD2 mRNA level was determined by real-time PCR in endothelial cell cultures and human total term villi (Fig. 1). 17βHSD2 mRNA level in HUAEC was about 22-fold higher than in HUVEC, and about 2.5-fold higher than in HAEC (P < 0.01 for both). As expected, 17βHSD2 mRNA level was significantly higher in term villi than in endothelial cell cultures (e.g., approximately 90-fold higher than in HUAEC, P < 0.0001).
17βHSD2 mRNA level in HUAEC, HUVEC, HAEC, and in term villi (TV). 17βHSD2 mRNA levels were determined by real-time PCR. 17βHSD2 expression levels were normalized by factors generated from expression levels of a set of stable housekeeping genes (SDHA, TBP, and YWHAZ), using the geNorm software (for details, see “Materials and methods”). Means ± SEM are presented. One-way ANOVA followed by Tukey’s test were used to compare 17βHSD2 mRNA level in HUAEC to level present in TV (+: P < 0.0001), HUVEC (*: P < 0.01), and HAEC (#: P < 0.01)
17βHSD2 activity in HUVEC, HUAEC, and HAEC
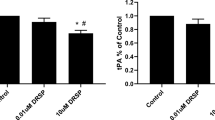
17βHSD2 activity was measured in whole cells using testosterone (Fig. 2a) and in sonicated cells using E2 or testosterone as substrate (Fig. 2b, c). 17βHSD2 activity measured in HUAEC was significantly higher than in HUVEC (30.5-fold, P < 0.001) or HAEC (2.5-fold, P < 0.001), while the activity in HAEC was also higher than in HUVEC (12-fold; P < 0.01). Similar results were obtained in sonicated cells: 17βHSD2 activity was higher in HUAEC than in HUVEC or HAEC (21.5-fold and 1.5-fold, respectively, using E2 as substrate, P < 0.01; 18.5-fold and 1.9-fold, respectively, using testosterone as substrate, P < 0.001).
17βHSD2 enzymatic activity in HUAEC, HUVEC, and HAEC. a The enzymatic activity in intact cells. Cells were incubated with tritiated testosterone (T) for 24 h. Results are expressed by μg of DNA. The values are the mean ± SEM from triplicate assays. b and c The enzymatic 17βHSD2 activity in sonicated cells. Enzymatic activities were assayed with estradiol (E2) (b) or T (c) with NAD as cofactor. One-way ANOVA followed by Tukey’s test were used to compare 17βHSD2 activity between HUAEC and HUVEC (*: P < 0.01), and between HUAEC and HAEC (#: P < 0.01). E 1 estrone; A androstenedione
17βHSD2 activity in proximal and distal segments of umbilical vessels, and in term villi
17βHSD2 activity was measured in freshly isolated arteries and veins from proximal and distal segments of umbilical cords, and in total term villi (Table 1). The terms “proximal” and “distal” refer to the placental side. For each sample, conversion of testosterone to androstenedione and/or of E2 to E1 was measured and normalized per microgram of protein. In the umbilical cord, enzyme activity was significantly higher in proximal or distal arteries than in the proximal or distal vein (E2 to E1, P < 0.01 for all; testosterone to androstenedione, P < 0.01 for all). Furthermore, 17βHSD2 activity measured in umbilical arteries was significantly higher in proximal segments than in distal segments (P < 0.01). As expected, 17βHSD2 activity was significantly higher in term villi than in other samples (testosterone to androstenedione, P < 0.01 for all). In enzymatic assays, the observed E2/T activity ratios were close to 1 with both arteries and vein (Table 1), which is consistent with 17βHSD2-specific enzymatic activity.
Estrogen receptors α and β mRNA levels in HUVEC, HUAEC, HAEC, and term villi
ERα (Fig. 3a) and ERβ (Fig. 3b) mRNA levels were determined by real-time PCR in HUVEC, HUAEC, HAEC, and in term villi. Distinct expression profiles of ER isoforms were observed in cell cultures. ERα expression level showed no difference between HUVEC and HUAEC, but was significantly higher in HAEC than in HUVEC (P < 0.05) and HUAEC (P < 0.01). ERβ mRNA level in HUAEC and HAEC was higher than in HUVEC (P < 0.001), but no difference was observed between HAEC and HUAEC. Both ERβ and ERα mRNA levels were significantly higher in term villi than in endothelial cell cultures (P < 0.001 for all).
ERα and ERβ mRNA levels in HUAEC, HUVEC, HAEC, and in term villi (TV). ERα (a) and ERβ (b) mRNA levels were determined by real-time PCR. Expression levels were normalized by factors generated from expression levels of a set of stable housekeeping genes (SDHA, TBP, and YWHAZ), using the geNorm software (for details, see “Materials and methods”). Means ± SEM are presented. One-way ANOVA followed by Tukey’s test were used to compare ERα or ERβ mRNA levels between HUVEC, HUAEC, HAEC, and TV. Significant differences were found for ERα between HUVEC or HUAEC, and HAEC (δ: P < 0.05) and TV (*: P < 0.01). Significant differences were found for ERβ between HUVEC and HUAEC (#: P < 0.01), HUVEC and HAEC (+: P < 0.01), and TV and cell cultures (*: P < 0.001)
17βHSD2, ERα, and ERβ proteins in HUAEC, HUVEC, and term villi
Western blot analysis was performed on microsomal protein fractions of HUAEC and HUVEC, and in a total protein extract from term villi using anti-17βHSD2, anti-ERα, and anti-ERβ antibodies. 17βHSD2 was easily detected in HUAEC (Fig. 4a), but was barely detectable in HUVEC (data not shown). A strong signal was detected in term villi (Fig. 4a), as expected [10]. Indeed, 15 μg of total term villi proteins showed an immunostained band of similar intensity to that obtained with 35 μg of microsomal HUAEC proteins, with 17βHSD2 being known to be enriched in the microsomal fraction [29]. A weak signal corresponding to ERα (66 kDa) was detected in microsomal fractions of HUVEC and HUAEC, and in total term villi (Fig. 4b). ERβ was also detected (56 kDa) in each sample (Fig. 4c). The intensity of the ERβ signal seems to be stronger in HUAEC microsomes than in HUVEC microsomes. The cytosolic fractions from HUAEC and HUVEC lacked immunostaining bands for ERα and ERβ (data not shown).
17βHSD2, ERα, and ERβ proteins in microsomal fractions of HUAEC and HUVEC, and in total term villi. Representative Western blot analyses of enriched microsomal protein fractions (35 μg) of HUAEC and HUVEC and of total protein extract (15 μg) from term villi are presented. 17βHSD2 is an endoplasmic reticulum-anchored enzyme and is therefore enriched in microsomal fractions. Expected bands of ~42 kDa were detected in HUAEC and in term villi using the anti-17βHSD2 antibody (a). Only a faint signal was observed in HUVEC even after overexposing the membrane (data not shown). Anti-ERα (b) and anti-ERβ (c) revealed the presence of specific bands at ~66 and ~56 kDa, respectively, in HUAEC, HUVEC, and in term villi. Please note that separate blots were used for each antibody, and all examined samples were loaded on each blot. Images were cropped to save space
Discussion
In human term placenta, 17βHSD2 mRNA and protein were localized exclusively in endothelial cells of fetal vessels [8–10] and were detected either at very high levels or at low or barely detectable levels in large blood vessels of the stem villi [9, 10]. Although placental arteries were identified as the major site of 17βHSD2 expression, 17βHSD2-negative and -positive vessels of either type have been observed [9, 10]. The human placental microvasculature is a complex network where differentiating arterial and venous vessels can be a demanding task, whereas the stem villi can be considered as trunks of the villous trees [11] and are mainly localized near the insertion point of the umbilical cord. This study compared the expression and enzymatic activity of 17βHSD2 in primary endothelial cell cultures isolated from umbilical arteries with the values found in cells isolated from the vein. Total term villi and HAEC were included as points of comparison. The enzymatic activity of 17βHSD2 was also measured in freshly isolated arteries and veins from proximal and distal segments of the cord. We show that 17βHSD2 mRNA level and enzymatic activity are significantly higher in HUAEC than in HUVEC. Accordingly, 17βHSD2 protein was detected in HUAEC microsomes by Western blot, but was barely detectable in microsomal fractions from HUVEC. In addition, higher 17βHSD2 activity was observed in umbilical arteries than in the vein, and likewise, in proximal relative to distal arterial segments. These results indicate that in umbilical endothelial cells, the expression and activity of 17βHSD2 should be regulated as a function of the vessel type. In addition, these data suggest that in larger vessels of the term placenta, 17βHSD2 expression is different between the arterial and the venous systems, as we previously observed [9, 10].
Maternal blood levels of estrogens rise continuously during all pregnancy. However, the level of E2 in the umbilical vein does not increase in parallel with that in the maternal vein, whereas the level of E1 in the umbilical vein continues to increase during pregnancy. These asymmetric releases of E2 and E1 in fetal and maternal circulation strongly suggest a control of the amounts of E2 entering into fetal circulation. In addition, E2 level is about 2-fold higher in the umbilical vein than in umbilical arteries at term (for details see [10] and references therein). In the third trimester of pregnancy, E2 plays an important role in the maturation of many fetal organs such as the lung, the skin, and the hypothalamo-hypophyseal-adrenal axis [1, 30–33]. In addition, excessive exposure to estrogenic compounds could have deleterious consequences on fetal development [34–38]. Indeed, reproductive disorders in both male and female have been associated with inappropriate exposure of the developing gonads to estrogens of pharmacological (e.g., diethylstilbestrol) or environmental (i.e., xenoestrogens) origin [39, 40]. Considering this reality, the strong 17βHSD2 expression in the placental endothelium where exchanges occur may protect fetal organ systems against excessive E2 exposure [39, 40]. An intriguing postulate is that 17βHSD2 expression might be modulated as a function of gestational time or fetal needs. Indeed, we previously showed that 17βHSD2 mRNA level is higher in total villi samples from term placentas than from mid-gestation placentas, and that 17βHSD2 in endothelial cells of the villi might control the amount of active and inactive estrogens in the fetal circulation [10]. In addition, a higher abundance of 17βHSD2 in the endothelium of umbilical arteries at term also suggests that this enzyme could minimize the fetal contribution to the maternal rise in E2 levels and also control the transfer of fetal androgens into the maternal circulation therefore, contributing to protect the maternal system against inappropriate androgenic effects [41, 42].
In homogenates of umbilical arteries and veins isolated from different segments of the cord, 17βHSD2 activity was significantly higher in arteries than in the vein, and significant differences in activity were found along the umbilical arteries. Indeed, 17βHSD2 activity was higher in proximal than in distal arterial segments. We previously demonstrated that 17βHSD2 mRNA and protein in human term placenta are more abundant in the sinusoidal capillaries of the terminal villi and in the paravascular capillary network than in large vessels of the stem villi [10]. The present evidence that 17βHSD2 activity in umbilical arteries is higher close to the placenta than to the fetus points to a gradient of 17βHSD2 expression along umbilical arteries, with higher level within the placenta, where exchanges occur. Although no such gradient was observed in umbilical vein segments, there is nevertheless a huge difference in 17βHSD2 expression levels between the cord and the placental villi.
In endothelial cells, E2 modulates the expression of genes involved in the control of vascular tone and causes a short-term vasodilatation by a non-genomic process, thus playing an important role in the modulation of blood flow. Reports on the expression of ERα and ERβ in umbilical endothelial cells are controversial [17–21]. In this study, both ERα and ERβ mRNAs were detected in HUAEC, HUVEC, HAEC, and in placental villi. No difference was noted for the expression of ERα between HUVEC and HUAEC. However, ERβ was expressed at lower level in HUVEC than in HUAEC or HAEC. Accordingly, ERα and ERβ protein were detected by Western blot in microsomal protein fractions of HUAEC and HUVEC, with a stronger ERβ signal in HUAEC than in HUVEC. Cytosolic fractions from HUAEC and HUVEC lacked immunostaining bands for ERα and ERβ (data not shown). This result is consistent with a report by Tschuggel et al. [21]. Positive expression of ERα and ERβ was also found in term villi, which contain several cell types, including endothelial cells, trophoblastic cells, and macrophages. Although only few studies have examined the expression of ERα and ERβ in human placenta [43, 44], both receptors have been localized in trophoblastic cells, while vascular pericytes and endothelial cells express ERα and ERβ, respectively [43].
One role for 17βHSD2 might be to modulate ER-mediated processes in endothelial cells (e.g., the vascular tone). The complex distribution of estrogen receptors and 17βHSD2 among the sub-populations of endothelial cells suggests that the endothelial cell response to E2 may differ according to vessel type or size. Of note, the E2 levels the cells are exposed to also differ between vessel types. Interestingly, 17βHSD2 mRNA and activity were detected in the aortic endothelium (HAEC), suggesting that 17βHSD2 could modulate estrogenic action in this tissue as it may be the case in endothelial cells of the cord, which is in line with the hypothesis that 17βHSD2 might participate in the modulation of vascular tone in the umbilical cord.
In conclusion, this study shows that 17βHSD2 expression differs between endothelial cells isolated from umbilical arteries and those isolated from the umbilical vein, and supports our previous observations on larger vessels of the human term placenta. This study combines measurements of the enzyme converting E2 to E1 and of estrogen receptors expression in endothelial cells of the umbilical vessels. We can speculate that, in addition to a role in inactivating circulating sex steroids, 17βHSD2 could differentially modulate responses to estrogens and androgens in endothelial cells according to the vessel type. Further studies are needed to clarify the possible implication of 17βHSD2 in the regulation of ER occupancy in endothelial cells.
References
E.D. Albrecht, G.J. Pepe, Placental steroid hormone biosynthesis in primate pregnancy. Endocr. Rev. 11(1), 124–150 (1990)
G.J. Pepe, E.D. Albrecht, Regulation of the primate fetal adrenal cortex. Endocr. Rev. 11(1), 151–176 (1990)
Y. Tremblay, G.E. Ringler, Y. Morel, T.K. Mohandas, F. Labrie, J.F. Strauss III, W.L. Miller, Regulation of the gene for estrogenic 17-ketosteroid reductase lying on chromosome 17cen—q25. J. Biol. Chem. 264(34), 20458–20462 (1989)
C. Beaudoin, C.H. Blomquist, Y. Tremblay, Gene expression of 17 beta-hydroxysteroid dehydrogenase type 2 isozyme in primary cultures of human trophoblasts predicts different mechanisms regulating type 1 and type 2 enzymes. Endocrinology 136(9), 3807–3814 (1995)
L. Wu, M. Einstein, W.M. Geissler, H.K. Chan, K.O. Elliston, S. Andersson, Expression cloning and characterization of human 17 beta-hydroxysteroid dehydrogenase type 2, a microsomal enzyme possessing 20 alpha-hydroxysteroid dehydrogenase activity. J. Biol. Chem. 268(17), 12964–12969 (1993)
M.L. Casey, P.C. MacDonald, S. Andersson, 17 beta-Hydroxysteroid dehydrogenase type 2: chromosomal assignment and progestin regulation of gene expression in human endometrium. J. Clin. Invest. 94(5), 2135–2141 (1994)
M. Bonenfant, P.R. Provost, R. Drolet, Y. Tremblay, Localization of type 1 17beta-hydroxysteroid dehydrogenase mRNA and protein in syncytiotrophoblasts and invasive cytotrophoblasts in the human term villi. J. Endocrinol. 165(2), 217–222 (2000)
J. Takeyama, T. Suzuki, G. Hirasawa, Y. Muramatsu, H. Nagura, K. Iinuma, J. Nakamura, K.I. Kimura, M. Yoshihama, N. Harada, S. Andersson, H. Sasano, 17beta-hydroxysteroid dehydrogenase type 1 and 2 expression in the human fetus. J. Clin. Endocrinol. Metab. 85(1), 410–416 (2000)
M. Bonenfant, C.H. Blomquist, P.R. Provost, R. Drolet, P. D’Ascoli, Y. Tremblay, Tissue- and site-specific gene expression of type 2 17beta-hydroxysteroid dehydrogenase: in situ hybridization and specificenzymatic activity studies in human placental endothelial cells of the arterial system. J. Clin. Endocrinol. Metab. 85(12), 4841–4850 (2000)
R. Drolet, M. Simard, J. Plante, P. Laberge, Y. Tremblay, Human type 2 17 beta-hydroxysteroid dehydrogenase mRNA and protein distribution in placental villi at mid and term pregnancy. Reprod. Biol. Endocrinol. 5, 30 (2007)
J.D. Boyd, W.J. Hamilton, Development and structure of the human placenta from the end of the 3rd month of gestation. J. Obstet. Gynaecol. Br. Commonw. 74(2), 161–226 (1967)
M.E. Mendelsohn, R.H. Karas, The protective effects of estrogen on the cardiovascular system. N. Engl. J. Med. 340(23), 1801–1811 (1999)
H.P. Kim, J.Y. Lee, J.K. Jeong, S.W. Bae, H.K. Lee, I. Jo, Nongenomic stimulation of nitric oxide release by estrogen is mediated by estrogen receptor alpha localized in caveolae. Biochem. Biophys. Res. Commun. 263(1), 257–262 (1999)
K.H. Kim, K. Moriarty, J.R. Bender, Vascular cell signaling by membrane estrogen receptors. Steroids 73(9–10), 864–869 (2008)
T. Hayashi, K. Yamada, T. Esaki, M. Kuzuya, S. Satake, T. Ishikawa, H. Hidaka, A. Iguchi, Estrogen increases endothelial nitric oxide by a receptor-mediated system. Biochem. Biophys. Res. Commun. 214(3), 847–855 (1995)
M. Akishita, K. Kozaki, M. Eto, M. Yoshizumi, M. Ishikawa, K. Toba, H. Orimo, Y. Ouchi, Estrogen attenuates endothelin-1 production by bovine endothelial cells via estrogen receptor. Biochem. Biophys. Res. Commun. 251(1), 17–21 (1998)
M.A. Herve, G. Meduri, F.G. Petit, T.S. Domet, G. Lazennec, S. Mourah, M. Perrot-Applanat, Regulation of the vascular endothelial growth factor (VEGF) receptor Flk-1/KDR by estradiol through VEGF in uterus. J. Endocrinol. 188(1), 91–99 (2006)
B. Toth, G. Saadat, A. Geller, C. Scholz, S. Schulze, K. Friese, U. Jeschke, Human umbilical vascular endothelial cells express estrogen receptor beta (ERbeta) and progesterone receptor A (PR-A), but not ERalpha and PR-B. Histochem. Cell Biol. 130(2), 399–405 (2008)
A.H. Wagner, M.R. Schroeter, M. Hecker, 17beta-estradiol inhibition of NADPH oxidase expression in human endothelial cells. FASEB J. 15(12), 2121–2130 (2001)
A. Sobrino, M. Mata, A. Laguna-Fernandez, S. Novella, P.J. Oviedo, M.A. Garcia-Perez, J.J. Tarin, A. Cano, C. Hermenegildo, Estradiol stimulates vasodilatory and metabolic pathways in cultured human endothelial cells. PLoS One 4(12), e8242 (2009)
W. Tschugguel, W. Dietrich, Z. Zhegu, F. Stonek, A. Kolbus, J.C. Huber, Differential regulation of proteasome-dependent estrogen receptor alpha and beta turnover in cultured human uterine artery endothelial cells. J. Clin. Endocrinol. Metab. 88(5), 2281–2287 (2003)
E.A. Jaffe, R.L. Nachman, C.G. Becker, C.R. Minick, Culture of human endothelial cells derived from umbilical veins Identification by morphologic and immunologic criteria. J. Clin. Invest. 52(11), 2745–2756 (1973)
R.T. Hinegardner, An improved fluorometric assay for DNA. Anal. Biochem. 39(1), 197–201 (1971)
B. Fiszer-Szafarz, D. Szafarz, A. Guevara de Murillo, A general, fast, and sensitive micromethod for DNA determination application to rat and mouse liver, rat hepatoma, human leukocytes, chicken fibroblasts, and yeast cells. Anal. Biochem. 110(1), 165–170 (1981)
C.H. Blomquist, H.C. Hensleigh, D.L. Block, L.A. Feeney, Placental 17 beta-hydroxysteroid oxidoreductase, lactate dehydrogenase and malate dehydrogenase during the latter half of pregnancy in the mouse. J. Steroid Biochem. Mol. Biol. 46(1), 61–67 (1993)
M. Simard, J. Plante, M. Boucher, P.R. Provost, Y. Tremblay, Type 2 and 5 17beta-hydroxysteroid dehydrogenases and androgen receptor in human fetal lungs. Mol. Cell. Endocrinol. 319(1–2), 79–87 (2010)
M. Simard, E. Boucher, P.R. Provost, Y. Tremblay, Minimization of PCR efficiency differences between standards and samples through dilution of PCR amplicons in reverse transcription buffer. Anal. Biochem. 362(1), 142–144 (2007)
J. Vandesompele, K. De Preter, F. Pattyn, B. Poppe, N. Van Roy, A. De Paepe, F. Speleman, Accurate normalization of real-time quantitative RT-PCR data by geometric averaging of multiple internal control genes. Genome Biol. 3(7), RESEARCH0034 (2002)
C.H. Blomquist, D.G. Bealka, H.C. Hensleigh, G.E. Tagatz, A comparison of 17 beta-hydroxysteroid oxidoreductase type 1 and type 2 activity of cytosol and microsomes from human term placenta, ovarian stroma and granulosa-luteal cells. J. Steroid Biochem. Mol. Biol. 49(2–3), 183–189 (1994)
S.S. Khosla, S.A. Rooney, Stimulation of fetal lung surfactant production by administration of 17beta-estradiol to the maternal rabbit. Am. J. Obstet. Gynecol. 133(2), 213–216 (1979)
S.S. Khosla, G.J. Smith, P.A. Parks, S.A. Rooney, Effects of estrogen on fetal rabbit lung maturation: morphological and biochemical studies. Pediatr. Res. 15(9), 1274–1281 (1981)
K. Hanley, U. Rassner, Y. Jiang, D. Vansomphone, D. Crumrine, L. Komuves, P.M. Elias, K.R. Feingold, M.L. Williams, Hormonal basis for the gender difference in epidermal barrier formation in the fetal rat. Acceleration by estrogen and delay by testosterone. J. Clin. Invest. 97(11), 2576–2584 (1996)
M.L. Williams, K. Hanley, P.M. Elias, K.R. Feingold, Ontogeny of the epidermal permeability barrier. J. Investig. Dermatol. Symp. Proc. 3(2), 75–79 (1998)
J.A. Visser, A. McLuskey, M. Verhoef-Post, P. Kramer, J.A. Grootegoed, A.P. Themmen, Effect of prenatal exposure to diethylstilbestrol on Mullerian duct development in fetal male mice. Endocrinology 139(10), 4244–4251 (1998)
J.R. Palmer, E.E. Hatch, R.S. Rao, R.H. Kaufman, A.L. Herbst, K.L. Noller, L. Titus-Ernstoff, R.N. Hoover, Infertility among women exposed prenatally to diethylstilbestrol. Am. J. Epidemiol. 154(4), 316–321 (2001)
H.W. Horne Jr., Evidence of improved pregnancy outcome with diethylstilbestrol (DES) treatment of women with previous pregnancy failures: a retrospective analysis. J. Chronic Dis. 38(10), 873–880 (1985)
H.W. Horne Jr., R.B. Kundsin, Results of infertility studies on DES-exposed and non DES-exposed consecutive patients. Int. J. Fertil. 30(1), 46–49 (1001). (1985)
R.M. Giusti, K. Iwamoto, E.E. Hatch, Diethylstilbestrol revisited: a review of the long-term health effects. Ann. Intern. Med. 122(10), 778–788 (1995)
G. Delbes, C. Levacher, R. Habert, Estrogen effects on fetal and neonatal testicular development. Reproduction 132(4), 527–538 (2006)
L.J. Guillette Jr., B.C. Moore, Environmental contaminants, fertility, and multioocytic follicles: a lesson from wildlife? Semin. Reprod. Med. 24(3), 134–141 (2006)
M. Mustonen, M. Poutanen, A. Chotteau-Lelievre, Y. de Launoit, V. Isomaa, S. Vainio, R. Vihko, P. Vihko, Ontogeny of 17beta-hydroxysteroid dehydrogenase type 2 mRNA expression in the developing mouse placenta and fetus. Mol. Cell. Endocrinol. 134(1), 33–40 (1997)
M. Mustonen, V.V.T. Isomaa, J. Tapanainen, M. Poutanen, F. Stenbäck, R. Vihko, P. Vihko, Human 17beta-hydroxysteroid dehydrogenase type 2 messenger ribonucleic acid expression and localization in term placenta and in endometrium during the menstrual cycle. J. Clin. Endocrinol. Metab. 83(4), 1319–1324 (1998)
A. Bukovsky, M.R. Caudle, M. Cekanova, R.I. Fernando, J. Wimalasena, J.S. Foster, D.C. Henley, R.F. Elder, Placental expression of estrogen receptor beta and its hormone binding variant—comparison with estrogen receptor alpha and a role for estrogen receptors in asymmetric division and differentiation of estrogen-dependent cells. Reprod. Biol. Endocrinol. 1, 36 (2003)
B. Schiessl, I. Mylonas, C. Kuhn, S. Kunze, S. Schulze, K. Friese, U. Jeschke, Expression of estrogen receptor-alpha, estrogen receptor-beta and placental endothelial and inducible NO synthase in intrauterine growth-restricted and normal placentals. Arch. Med. Res. 37(8), 967–975 (2006)
Acknowledgments
We thank the nurses from the Centre Mère-Enfant at the Centre Hospitalier Universitaire de Québec for their precious collaboration. We also thank Dr. Martin Bonenfant, PhD, for technical support, Julie Plante, MSc, for technical support and for critical reading of the manuscript, and Dr. Richard Poulin, PhD, for editing of the manuscript. This study was supported by grants from the Natural Sciences and Engineering Research Council of Canada (NSERC 171140-05) and the Canadian Institutes of Health Research (MOP 84221) to YT. This manuscript is dedicated to the memory of Dr Charles H Blomquist, deceased in September 2009.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Simard, M., Drolet, R., Blomquist, C.H. et al. Human type 2 17beta-hydroxysteroid dehydrogenase in umbilical vein and artery endothelial cells: differential inactivation of sex steroids according to the vessel type. Endocrine 40, 203–211 (2011). https://doi.org/10.1007/s12020-011-9519-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-011-9519-5