Abstract
The effects of adipose-derived mesenchymal stem cells (ADMSC) transplantation on degeneration, regeneration and skeletal muscle function were investigated in dystrophin-deficient mice (24-week-old). ADMSC transplantation improved muscle strength and, resistance to fatigue. An increase in fiber cross-sectional area and in the number of fibers with centralized nuclei and augment of myogenin content were observed. In ADMSC-treated muscles a decrease in muscle content of TNF-α, IL-6 and oxidative stress measured by Amplex® reagent were observed. The level of TGF-β1 was lowered whereas that of VEGF, IL-10 and IL-4 were increased by ADMSC treatment. An increase in markers of macrophage M1 (CD11 and F4-80) and a decrease in T lymphocyte marker (CD3) and arginase-1 were also observed in ADMSCs-treated dystrophic muscle. No change was observed in iNOS expression. Increased phosphorylation of Akt, p70S6k and 4E-BP1 was found in dystrophic muscles treated with ADMSC. These results suggest that ADMSC transplantation modulates inflammation and improves muscle tissue regeneration, ameliorating the dystrophic phenotype in dystrophin-deficient mice.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Duchenne muscular dystrophy (DMD) is a X-linked lethal genetic disorder characterized by dystrophin deficiency due to genetic mutation in the dystrophin gene at Xp21 [1]. Dystrophin is a subsarcolemmal protein that connects cytoskeletal actin to sarcolemma and extracellular matrix through a large protein complex [2]. DMD is a progressive and lethal degenerating disease of both skeletal and cardiac muscles and affects 1 in 3500 boys. Mdx mouse is the most used DMD experimental model and displays a reduced life span.
In recent years, the stem cell transplantation became one of the most promising treatment to restore dystrophin in DMD patients. Some authors demonstrated that transplantated haematopoietic stem cells stimulate skeletal muscle repair in dystrophin-deficient mice [3–10]. On the other hand, the transplantation of other type of adult stem cell, mesenchymal stem cell (MSC) found in bone marrow, umbilical cord tissue and adipose tissue, emerged as an attractive alternative for DMD treatment. MSCs are easily expanded in vitro and under specific conditions can differentiate into osteoblasts, adipocytes, chondrocytes, and myoblasts. The first evidence of the potential use of MSCs for treatment of skeletal muscle disorders emerged from the study of Wakitani and co-workers [11]. These authors reported that MSCs isolated from bone marrow differentiate into multinucleated myotubes when treated with 5-azacytidine [11]. Experiments of co-culture demonstrated that bone marrow-derived MSC fused and restored the expression of full-length dystrophin in cultured myotubes obtained from biopsy of DMD patients [12]. Adipose tissue is an abundant and easily accessible source of MSCs and therefore this tissue is of great interest for stem cell therapy, since the cells can be obtained by liposuction. Zuk and co-workers [13] demonstrated that human adipose-derived (ADMSC) can differentiate in vitro into adipogenic, chondrogenic, osteogenic, and myogenic cell lineages. The ADMSC transplantation may be therapeutically used as strategy to treat muscular dystrophy. The transplantation of ADMSCs leads to muscle regeneration in mdx mice and SJL dystrophic mice [14, 15]. However, the mechanism of its beneficial effects needs to be established.
Transplanted allogenic MSCs may directly fuse with DMD muscle fiber and express normal dystrophin gene or differentiate into new skeletal muscle fibers. Myogenic differentiation of MSC requires DNA demethylation treatment, pre-transplantation coculture with myoblasts and in vivo muscle engraftment [14, 16–19]. The effects of MSC transplantation in muscle dystrophy may be also due to the modulation of microenvironment in dystrophic skeletal muscle. Treatments that promote angiogenesis and reduce fibrosis have positive effects in dystrophic skeletal muscle [20–22]. Few studies have focused on the effect of ADMSC transplantation on functional parameters inflammation and angiogenesis in dystrophic skeletal muscle. In the present study, the effect of local injections of ADMSCs on strength (muscle twitch and tetanic forces acute muscle fatigue, and content of pro-inflamatory and anti-inflammatory cytokines, oxidative stress, degeneration, regeneration and protein synthesis signalling was investigated in dystrophin-deficient mice.
Methods
Animals and Ethical Aspects
Male C57BL/10 mice (24-week-old) and male dystrophin-deficient mdx mice (24-week-old) were obtained from the Institute of Biomedical Sciences and Nuclear Research Institute (IPEN) of the University of São Paulo. The animals were maintained in groups of five with water and food ad libitum in a room with 12/12 h light–dark cycle at 22°C. All experimental procedures were carried out in agreement with the Guide for the Care and Use of Laboratory Animals (Institute of Laboratory Animal Resources, National Academy of Sciences, Washington, D).
Isolation of Adipose-derived Mesenchymal Stem Cells
ADMSCs were isolated as previously described [17]. In brief, epididymal and retroperitoneal fat pads from male C57BL/10 mice were removed and washed several times in isolation buffer consisting of 1% BSA, 20 mM Hepes, 200 nM adenosine, and 1X Krebs–Ringer phosphate (KRP) buffer. Visible blood vessels were carefully dissected away. Fat tissue was minced into small fragments using surgical scissors. The fragments were digested at 37°C with Type I collagenase under constant agitation. Once digested, the samples were filtered through a 400 μm mesh filter to remove undigested tissue. The stromal–vascular fraction was separated from the adipocyte fraction by low-speed centrifugation. The supernatant contained the mature adipocytes that floated due to their high lipid content. The pellet contained the stromal components, which include the putative adipose-derived mesenchymal cells and the hematopoietic lineage cells. The adipocyte fraction was discarded. The stromal fraction was treated with 1X red blood cell lysis buffer (eBiosciences) for 5 min and then subsequently washed several times in isolation buffer. Cells were filtered again using a 70 μm nylon mesh filter and seeded at 3000 cells/cm2 in culture dish with DMEM containing 20% foetal bovine serum (FBS) and left overnight at 37°C and 5% CO2. In the following days, the culture medium was changed to remove non-adherent cells until obtaining a purified culture of adipose-derived mesenchymal stem cells. The cells were cultured for 4 weeks and shown a high expression of mesenchymal markers (CD90 and CD105) and not detectable expression of hematopoietic markers (CD34, CD45 and c-kit) by real time PCR. The capacity to differentiate in adipogenic, osteogenic, chondrogenic was analyzed as previously described [13].
Stem Cell Therapy
The culture medium was removed and cells were washed twice in phosphate buffer solution (PBS). Cells were re-suspended in PBS containing glucose (5.5 mM) and the transplantation of 106 ADMSCs was performed by local injections, once per week during 4 weeks, into middle point of the gastrocnemius muscle. The placebo group was injected with PBS only. The animals were sacrificed 1-week after the last injection.
Histological Analysis
Muscle sections (10 μm thick) were cut from the mid-belly region of gastrocnemius muscle using a cryostat. Sections were stained with Hematoxylin and Eosin (HE) for examination of fiber cross-sectional area (CSA) and centralized nuclei (a marker of the regenerating muscle fibers). Sections were imaged using an upright microscope with camera (Nikon DXM 1200, Japan). Digitized images were analyzed using Image Pro Plus Software (Media Cybernetics, Silver Spring, MD) in a double-blinded manner. The mean fiber CSA was determined by measuring the circumference of 100 adjacent fibers from the centre of each cross-section totalizing1 000 fibers per muscle tissue. Centralized nuclei were expressed as percentage of total number of fibers (%).
Determination of Muscle-Derived Reactive Oxygen Species
The production of reactive oxygen species (ROS) was evaluated in incubated muscle. Under anesthesia, gastrocnemius muscle were quickly removed and immediately incubated in oxygenated (95% O2–5% CO2) Krebs solution in the presence of 50 μM Amplex® UltraRed (A36006, Molecular Probes, Invitrogen Inc., Carlsbad, CA, USA) reagent and 0.1 U/mL horseradish peroxidase (HRP) for 60 min. In the presence of peroxidase, the Amplex® reagent reacts with hydrogen peroxide (H2O2) in a 1:1 stoichiometry to produce the red-fluorescent oxidized product, resorufin. The fluorescence of resorufin was determined in 530 nm wavelength (excitation) and 590 nm wavelength (emission). Measurements of ROS were calibrated using a known dose of exogenous H2O2 (10 μM – positive control) in the presence or absence of catalase (300 U/mL), glutathione peroxidase (5 U/mL) and reduced glutathione (0.5 mM). All measurements were conducted in Krebs solution (1 mL), pH 7.4, at 37°C.
Cytokine Determination in Skeletal Muscle
Measurement of cytokines was performed by ELISA in samples of skeletal muscle protein using Duo-set kits for IL-4, IL-6 and IL-10 (R&D Systems Inc., Minneapolis, MN, USA) and TNF-α (BD Pharmingen, San Jose, CA, USA). The results were normalized by skeletal muscle total protein detemined by Bradford’s method.
Analysis of Skeletal Muscle Strength
The mice were subjected to muscle strength analysis using in situ electrical stimulation as previously described [23, 24]. The animals were anesthetized by an intraperitoneal injection of pentobarbital (80 mg/kg) and both hindlimbs were fixed on an acrylic platform. The stimulated limb was placed on the platform with the hip joint at a 60° angle and the knee joint at a 60° angle. A hook was placed under the Achilles tendon and connected to an isometric force transducer (Grass Technologies, West Warwick, Rhode Island, USA). The skin was excised and the sciatic nerve was then accessed. Dorsiflexors, soleus and plantaris muscles were tenotomized. Maximum isotonic contractions (muscle twitches) were induced by electrical stimulation at a low-stimulation frequency (1 Hz) and a high-stimulation frequency (100 Hz) using a platinum electrode placed at the sciatic nerve. The resting length (L 0) of gastrocenmius was adjusted to obtain maximum tension (the ankle joint approximately at a 90° angle) upon stimulation using the MultiStim System D330 (Digitimer Ltd, Welwyn Garden City, Hertfordshire, UK). For determination of muscle twitch force, the stimulus consisted of a 500 μs pulse duration at 1 Hz with an adjusted voltage to produce maximum force. For determination of tetanic force, the frequency of electrical stimulus was elevated to 100 Hz. The muscle twitch force (peak of muscle twitch force) and tetanic force (peak of tetanus) were recorded using the AqDados® software (version 4.16, Lynx Tecnologia Eletrônica Ltda, São Paulo, Brazil). The muscle strength was analyzed using the AqAnalysis® software (version 4.16, Lynx Tecnologia Eletrônica Ltda, São Paulo, Brazil).
Analysis of Acute Skeletal Muscle Fatigue
The index of resistance to acute muscle fatigue was calculated using the curve decline of the initial tetanic force (considered as 100%) during 5 successive tetanic muscle contractions and was determined as the area under the muscle tension versus contraction curve.
Real-Time Polymerase Chain Reaction
Analysis of macrophage M1 markers (F4-80 and CD11), T lymphocyte marker (CD3) and Arginase-1 gene expression were performed using ROTOR GENE 3000 equipment (Corbett Research, Mortlake, Australia) and the reagent SYBR® Green as fluorescent dye. The reactions were performed in a final volume of 25 μl containing a mixture of 1 μl cDNA, 0.5 μl of each primer, forward and reverse, diluted in a 10 μM stock solution, 10.5 μl DEPC water and 12.5 μl Platinum® SYBR® green qPCR SuperMix UDG. After that, the amplification reaction was then performed, using the following conditions: a unique cycle at 95°C for 5 min, followed by 40 cycles containing the denaturation phase, 95°C for 1 min, the hybridization phase, 56°C for 1 min, and the extension phase, 70°C for 1 min. All analysis of the mRNA content was normalized to glyceraldehyde-3-phosphate dehydrogenase (GAPDH) mRNA levels. The primer sequences used are F4-80 sense 5´-CCTGAACATGCAACCTGCCAC-3´ and F4-80 antisense 5´-GGGCATGAGCAGCTGTAGGATC-3´, CD11 sense 5´-AGCAGGTGGCATTGTGGGAC-3´ and CD11 antisense 5´-ACCTCTGTTCTCCTCCTCTCCG-3´, CD3 sense 5´-GCGGTGGAACACTTTCTGGG-3´ and CD3 antisense 5´-CCGAGAAATCCTGGAGCACC-3´, Arginase-1 sense 5´-GGAAGAGTCAGTGTGGTGCTGG-3´and Arginase-1 antisense 5´-CAGGAGAAAGGACACAGGTTGC-3´, GAPDH sense 5´-AACTTTGGCATTGTGGAAGG-3´ and GAPDH antisense 5´-ACACATTGGGGGTAGGAACA-3´. The relative quantification was performed using the software qBase v1.3.4 (http://medgen.ugent.be/qbase/).
Western Blotting
Proteins were extracted in buffer containing Tris–HCl (100 mM), pH 7.5; EDTA (10 mM), pH 8.0; sodium pyrophosphate (10 mM); sodium fluoride (0.1 mM); sodium orthovanadate (10 mM); PMSF (2 mM); and aprotinin (10 μg/ml). The cell extracts were sonicated for 30 s at 4°C. The homogenates were centrifuged at 12,000 g for 20 min at 4°C and the supernatants were treated with Triton X-100 (1%) and transferred to a−80°C freezer until being used for Western blotting analysis. An aliquot from the supernatant was used to determine the total protein content by the Bradford method. The nonspecific sites were blocked with free-fat milk. The nitrocellulose membranes were then incubated with primary antibodies (against iNOS, VEGF, TGF-β1, Myogenin, phospho-Akt, (Ser473) total Akt, phospho-p70S6k, total p70S6k, phospho-4E-BP1, total 4E-BP1 and β-actin) overnight at 4°C and treated with a secondary HRP-conjugated antibody for 60 min at 4°C. Anti-myogenin (MAB3876) and anti-VEGF (ABS82) were purchased from Millipore (Billerica, MA, U.S.A.), anti-iNOS (ab15323) was from ABCAM (Cambridge, Mass., USA), anti-TGFβ1 (AV37894) was from Sigma-Aldrich Corporation (St. Louis, MO, USA), Beta-actin (4967) anti-Akt (9272), anti-phospho-Akt (Ser473) (4058), anti-p70S6k (2708), anti-phospho-p70S6k (Thr 389) (9234), anti-4E-BP1 (9644), anti-phospho 4E-BP1 (Thr 37/46) (2855) were from Cell Signaling Technology (Beverly, MA, USA).
Statistical Analysis
The results are presented as means ± SEM. Student’s t test was used for comparison between two groups and one-way ANOVA followed by Tukey’s posttest for analysis of three or more groups and Student’s t test for analysis of two groups. Differences between values were considered statistically significant for p < 0.05. All results were analyzed using the GraphPad Prism 4.0 statistical software (GraphPad Software, San Diego, CA, USA).
Results
No significant differences were observed in sciatic nerve properties such as rheobase and chronaxie (functional parameters of peripheral nerve) between controls and mdx mice (Data not shown). Compared to C57 mice, the mdx mice showed a decrease in both muscle twitch and tetanic force (Fig. 1). The twitch and tetanic forces of gastrocnemius muscle from mdx mice were 55% (1980 ± 286 mN/g versus 3594 ± 224 mN/g and 6678 ± 947 mN/g versus 12256 ± 1109 mN/g, respectively) of the value presented by C57 mice. The intramuscular injections of ADMSCs restored skeletal muscle strength (both muscle twitch and tetanic forces in dystrophic mice (Panels A and B of Fig. 1). The skeletal muscle from mdx mice presented a low resistance to fatigue (Panels C and D of Fig. 1). Mdx mice showed a decrease by 43% in the index of resistance to acute muscle fatigue. The contractile performance during successive tetanic contractions was increased by 36% in dystrophic muscle treated with ADMSCs suggesting an improvement in the resistance to muscle fatigue (Panels C and D of Fig. 1).
Transplantation of adipose-derived mesenchymal stem cells (ADMSCs) improves skeletal muscle strength in dystrophin-deficient skeletal muscle. Panel A, muscle twitch (isotonic contractions) determined at 1 Hz of electrical stimulus frequency. Panel B, tetanic force determined at 100 Hz of electrical stimulus frequency. Panel C, production of muscle tension during successive tetanic contractions determined at 100 Hz of electrical stimulus frequency. Panel D, index of resistance to acute muscle fatigue determined from the analysis of the area under the curve (muscle tension versus tetanic contractions). The results were compared by one-way ANOVA followed by Tukey’s test. # = p < 0.05 compared to C57BL/10 mice. * = p < 0.05 compared to mdx-untreated leg. ADMSC = Adipose-derived mesenchymal stem cells
The ADMSC transplantation increased the muscle fiber diameter (Fig. 2) but promoted only a small increase in the number of fibers containing centralized nuclei in dystrophic mice (Table 1) suggesting a possible paracrine and modulatory effects of transplanted stem cells in dystrophic muscle phenotype. The effect of ADMSC transplantation upon the content of pro-inflammatory cytokines in dystrophic skeletal muscle was also evaluated. Compared to C57 mice, the skeletal muscle from mdx mice showed increased content of TNF-α and IL-6 and decreased content of IL-10 and IL-4. The treatment with ADMSCs decreased the content of both TNF-α (by 2.2-fold) and IL-6 (2.4-fold) in gastrocnemius muscle from mdx mice (Panel B of Fig. 3). An increase in the content of IL-10 and IL-4 were observed in dytrophic muscle treated with ADMSCs (Panels E and F of Fig. 3). So, the ADMSC transplantation reduced the inflammatory process in dystrophic skeletal muscle.
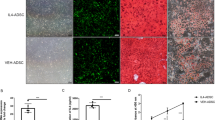
Transplantation of adipose-derived mesenchymal stem cells (ADMSCs) ameliorates histological phenotype and increased fiber cross-sectional area (CSA) in dystrophin-deficient skeletal muscle. In panel A, histological section of gastrocnemius muscle of C57BL/10 mice. Panel B, histological sections of gastrocnemius muscle of mdx-untreated leg. Panel C and D, histological sections of gastrocnemius muscle from mdx-treated leg. Muscle sections were stained with Hematoxylin and Eosin (HE).Panel E, the results were analyzed by the Anderson–Darling Normality Test. Muscle cross-sectional area (CSA) fiber was not normally distributed; therefore, the 95% confidence interval of the median was used and differences were considered significant when no overlap was found between the 95% confidence interval of the mean. Scale bar, 100 μm
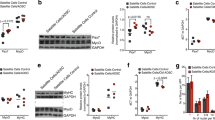
Transplantation of adipose-derived mesenchymal stem cells (ADMSC) decreases the content of inflammatory cytokines, reactive oxygen species (ROS) and did not change inducible nitric oxide synthase (iNOS) in dystrophin-deficient skeletal muscle. The results are presented as mean ± SEM of six observations. In the panels A and B, the content of TNF-α and IL-6 were not detectable by ELISA in gastrocnemius muscle from C57 mice. In the panels A and B, the results were analyzed by paired Student’s t test. In the panels C, D, E and F, the results were analyzed by one-way ANOVA followed by the Tukey’s test
Effect of adipose-derived mesenchymal stem cells (ADMSCs) on the content of VEGF and TGF-β1 in dystrophin-deficient skeletal muscle. The results are presented as mean ± SEM of six observations. The results are presented as mean ± SEM of six observations. The results were analyzed by one-way ANOVA followed by the Tukey’s test
Dystrophic skeletal muscle presented increased content of ROS (by 6.9-fold) and TGF-β1 (by 2.7-fold) (Panel C of Fig. 3 and Panel B of Fig. 5). The oxidative stress was also reduced in dystrophic skeletal muscle after treatment with ADMSCs (Panel C of Fig. 3) and VEGF content was increased by 1.6-fold (Panel A of Fig. 4) whereas the content of TGF-β1 was decreased by 2.5-fold (Panel B of Fig. 4) after ADMSCs treatment. No change was observed in the iNOS content.
Effect of adipose-derived mesenchymal stem cells (ADMSCs) on content of myogenin and protein synthesis pathway in dystrophin-deficient skeletal muscle. The results are presented as mean ± SEM of six observations. The results were analyzed by one-way ANOVA followed by the Tukey’s test and by the paired Student´s t test
Effect of adipose-derived mesenchymal stem cells (ADMSCs) on expression of macrophage M1 markers (F4/80 and CD11), T lymphocyte marker (CD3) and Arginase-1 in dystrophin-deficient skeletal muscle. The results are presented as mean ± SEM of six observations. The results were analyzed by one-way ANOVA followed by the Tukey’s test
The ADMSCs treatment stimulated protein synthesis in dystrophin-deficient skeletal muscle as demonstrated by the increased levels of Phospho-Akt (Ser473) (by 1.9-fold), Phospho-p70S6k (1.9-fold) and Phospho-4E-BP1 (by 2.2-fold) (Panels A, B and C of Fig. 5). An increase by 1.3-fold in the content of myogenin was also observed in dystrophin-deficient muscle after treatment with ADMSCs indicating an improvement in skeletal muscle regeneration (Panel D of Fig. 5). Skeletal muscle from mdx mice presents an increased expression of CD3 (by 9.5-fold) and arginase-1 (by 11-fold) compared to C57 control mice. Markers of macrophage M1 (F4-80 and CD11; by 1.9-fold and by 1.5-fold) were increased and T lymphocyte marker CD3 (by 2-fold) and arginase-1 (by 2-fold) were decreased in dystrophic muscle treated with ADMSCs compared to muscle from untreated leg (Fig. 6).
Discussion
The skeletal muscles from mdx mice display degeneration and regeneration with the associated pseudo or compensatory hypertrophy similar to that observed in the early stages of DMD boys [25–27]. Despite the compensatory hypertrophy, skeletal muscles from mdx mice present considerable loss in specific force (normalized by muscle weight or estimated muscle cross-sectional area) [27]. We demonstrated herein that one injection per week for four weeks of ADMSCs increases muscle fiber diameter and improves force generation in dystrophin-deficient skeletal muscle. The dystrophic muscles treated with ADMSCs also showed increased resistance to acute muscle fatigue compared with placebo-treated muscles. This is suggestive that transplanted ADMSCs lead to regeneration of skeletal muscle. But a modest increase in fibers containing centralized nuclei was observed and so this effect does not fully explain the great improvement in muscle strength.
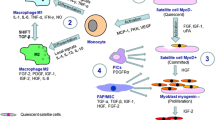
The transdifferentiation of ADMSCs into skeletal muscle fibers has been reported as the main mechanism underlying their therapeutic action [14, 15]. In the present study, the number of newly generated skeletal myocytes was too low to explain the great improvement in skeletal muscle function. Growing evidence supports the involvement of a paracrine mechanism in the reparative effect of adult stem cell transplantation. The contents of vascular endothelial growth factor (VEGF), basic fibroblast growth factor (bFGF), hepatocyte growth factor (HGF), insulin-like growth factor (IGF)-I are significantly increased in injured hearts treated with MSCs [28]. These paracrine factors may mediate endogenous regeneration of skeletal muscle via activation of resident muscle stem cells or preserving muscle mass. In the present study, we observed that ADMSC treatment leads to an increase in the content of myogenin in dystrophin-deficient skeletal muscle indicanting increased regeneration. Herein, we also demonstrated that ADMSC treatment increases the content of VEGF in dystrophin-deficient skeletal muscle supporting the proposition of the involvement of a paracrine mechanism. The VEGF overexpression ameliorates the skeletal muscle phenotype of mdx mice through angiogenic and pro-regenerative effects. Reductions of necrotic fibers area and increases of regenerating fibers area with an augmented number of myogenin positive cells and of fibers with centralized nuclei are reported after delivery of VEGF using recombinant adeno-associated virus (rAAV) vector [20].
Inflammatory and fibrogenic processes are involved in pathophysiology of mdx mice and may be also regulated by a paracrine action of the MSCs in dystrophin-deficient skeletal muscle. Oxidative stress is reported in several pathological conditions such as hypoxia, inflammation, disuse muscle atrophy, and muscular dystrophy [29]. In dystrophic skeletal muscle, reactive oxygen species (ROS) produced by immune cells and muscle fiber mediate cell death and similarities has been found between the DMD pathology of and skeletal muscle injury concerning to oxidative stress [30, 31]. Herein, we showed that ADMSC treatment causes an increase in the content of anti-inflammatory cytokines (IL-10 and IL-4) and a decrease in the content of TNF-α, IL-6 and ROS in dystrophin-deficient skeletal muscle suggesting a protective action of stem cell transplantation on inflammation-induced injury. iNOS expression could play a role in the pathophysiology of DMD [32]. iNOS mediates the nitric oxide (NO) synthesis which exerts a variety of biological functions including intracellular signal transduction, neurotransmission, vasodilatation and contractile responses of skeletal muscle fibers [33, 34]. In the presence of oxidative stress, as in dystrophic skeletal muscle, NO reacts with superoxide anion forming peroxynitrite that causes deleterious effect in muscle tissue including plasma membrane oxidative damage [35].
Dystrophin-deficient skeletal muscle releases a low amount of NO when compared to healthy muscle [36]. Thus, in spite of the unchanged iNOS content, possibly due to the increase in the VEGF content, the reduction of muscle-derived ROS in dystrophic muscle by ADMSC treatment presents a protective effect against plasma membrane oxidative damage due possibly to a low generation of peroxynitrite. The increased phosphorylation of Akt, (Ser473) p70S6k and 4E-BP1 in dystrophic muscle treated with ADMSCs points out that muscle mass preservation possibly occurred due to decreased inflammation (increased protein degradation) and increased protein synthesis. Activation of Akt/mTOR pathway by AKT phosphorylation at Ser473 residue induces muscle hypertrophy and inhibits apoptosis in mdx myotubes [37]. Akt inhibits the TSC complex by activating mTOR, and leading to p70S6K activation and protein synthesis [38].
The mechanism of action of adult stem cell therapy is still unknown. Transplanted-ADMSCs are able to engraft into skeletal muscle of dystrophic mice when locally injected [14, 18] or delivered through the tail vein [15]. Studies [39, 40] have shown that only a low percentage of mobilized stem cells engrafted into injured organ. The hypotheses of paracrine actions including immunomodulation [41], syntheses of local mediators [42–44] that lead to inhibition of fibrosis and apoptosis, enhancement of angiogenesis, stimulation of proliferation and differentiation of tissue-resident adult stem cells has been postulated as the possible mechanism of action of transplanted MSCs. The ADMSC secrete angiogenic and antiapoptotic factors that elicit injured tissue protection and improve cardiac function in injured heart by supporting angiogenesis through VEGF production [45–48].
Exacerbated immune system response and inflammation promote secondary muscle injury in the muscular dystrophies. The treatment with Prednisolone [49] improved pathogenic features of the muscular dystrophy experimental models. The reduction in the content of pro-inflammatory cytokines (TNF-α and IL-6) and ROS, increase in the content of anti-inflammatory cytokines (IL-10 and IL-4) and expression of macrophages M1 markers (F4-80 and CD11) observed in the present study demonstrated a modulatory effect of transplanted-ADMSCs in chronic inflammation of skeletal muscle from mdx mice that confers a protection against inflammation-induced injury and can facilitate the spontaneous regeneration of skeletal muscle tissue. Increased production of TNF-α by immune cells and/or muscle cells contribute to myonecrosis and protein degradation (leading to muscle atrophy) in mdx mice through nuclear factor kappa-B (NF-kappaB) signalling. The inhibition of NF-kappaB signaling by pyrrolidine dithiocarbamate (PDTC) treatment in mdx mice increased forelimb strength, decreased muscle fatigue, reduced myonecrosis and enhanced muscle regeneration corroborating with the results presented in the present study [50]. The increase in macrophage M1 markers reported in the present study may be also associated to attenuation of dystrophic muscle phenotype. Macrophages play a significant role in muscle fibre membrane repair, regeneration and growth. Mice that received a series of intraperitoneal injections of anti-F4-80, which binds a mouse macrophage surface antigen presented macrophage depletion, reduced muscle regeneration capacity and muscle stem cell differentiation [51]. The TGF-β1 is an inhibitor of muscle stem cell differentiation and the reduction of TGF-β1, a fibrosis mediator, is associated to reduction in excessive collagen accumulation, and increased strength in skeletal muscle from mdx mice [52]. Arginine metabolism has an important role in fibrosis. Tissue fibrosis may be increased by dietary supplementation with arginine due to increased substrate availability for arginase. Dietary supplementation with arginine for 2 weeks in humans increased connective tissue deposition in wounds [53]. Arginine metabolism by arginase promotes fibrosis in muscular dystrophy and dietary supplementation with arginine exacerbates fibrosis of dystrophic heart and skeletal muscles [54]. In the present study, we also observed a decreased expression of arginase-1and CD3 (T-lymphocyte marker) in dystrophic muscle treated with ADMSCs. The reduction on CD3 expression demonstrated an immunosuppressory effect of ADMSC transplantation and also demonstrated the absence of stem cell-graft rejection by the host mdx mice
Taken as a whole, this pre-clinical study showed that local ADMSC transplantation increased skeletal muscle strength and preserved muscle mass dystrophic mdx mice by a mechanism associated to a decrease in inflammation and oxidative stress and an increase in VEGF content and angiogenesis with increased phosphorylation of p70S6k (inducing protein synthesis at the ribosome) and phosphorylation of 4E-BP1 (that inhibits the repression of mRNA translation) increasing muscle fiber diameter. These results support the proposition that ADMSC transplantation is a promising treatment for muscular dystrophies.
References
Leturcq, F., & Kaplan, J. C. (2005). Molecular bases of dystrophinopathies. J Soc Biol, 199, 5–11.
Burghes, A. H., Logan, C., Hu, X., et al. (1987). A cDNA clone from the Duchenne/Becker muscular dystrophy gene. Nature, 328, 434–437.
Ferrari, G., Cusella-De Angelis, G., & Coletta, M. (1998). Muscle regeneration by bone marrow-derived myogenic progenitors. Science, 279, 1528–1530.
Gussoni, E., Soneoka, Y., Strickland, C. D., et al. (1999). Dystrophin expression in the mdx mouse restored by stem cell transplantation. Nature, 401, 390–394.
McKinney-Freeman, S. L., Jackson, K. A., Camargo, F. D., et al. (2002). Muscle-derived hematopoietic stem cells are hematopoietic in origin. Proc Natl Acad Sci USA, 99, 1341–1346.
Fukada, S., Miyagoe–Suzuki, Y., Tsukihara, H., et al. (2002). Muscle regeneration by reconstitution with bone marrow or fetal liver cells from green fluorescent protein-gene transgenic mice. J Cell Sci, 115, 1285–1293.
LaBarge, M. A., & Blau, H. M. (2002). Biological progression from adult bone marrow to mononucleate muscle stem cell to multinucleate muscle fiber in response to injury. Cell, 111, 589–601.
Camargo, F. D., Green, R., Capetanaki, Y., et al. (2003). Single hematopoietic stem cells generate skeletal muscle through myeloid intermediates. Nat Med, 9, 1520–1527.
Corbel, S. Y., Lee, A., Yi, L., et al. (2003). Contribution of hematopoietic stem cells to skeletal muscle. Nat Med, 9, 1528–1532.
Bachrach, E., Li, S., Perez, A. L., et al. (2004). Systemic delivery of human microdystrophin to regenerating mouse dystrophic muscle by muscle progenitor cells. Proc Natl Acad Sci USA, 101, 3581–3586.
Wakitani, S., Saito, T., & Caplan, A. I. (1995). Myogenic cells derived from rat bone marrow mesenchymal stem cells exposed to 5-azacytidine. Muscle Nerve, 18, 1417–1426.
Gonçalves, M. A., de Vries, A. A., Holkers, M., et al. (2006). Human mesenchymal stem cells ectopically expressing full-length dystrophin can complement Duchenne muscular dystrophy myotubes by cell fusion. Hum Mol Genet, 15, 213–221.
Zuk, P. A., Zhu, M., Mizuno, H., et al. (2001). Multilineage cells from human adipose tissue: implications for cell-based therapies. Tissue Eng, 7, 211–228.
Rodriguez, A. M., Elabd, C., Amri, E. Z., et al. (2005). Transplantation of a multipotent cell population from human adipose tissue induces dystrophin expression in the immunocompetent mdx mouse. J Exp Med, 201, 1397–1405.
Vieira, N. M., Bueno, C. R., Jr., Brandalise, V., et al. (2008). SJL dystrophic mice express a significant amount of human muscle proteins following systemic delivery of human adipose-derived stromal cells without immunosuppression. Stem Cells, 26, 2391–2398.
Bacou, F., el Andalousi, R. B., Daussin, P. A., et al. (2004). Transplantation of adipose tissue-derived stromal cells increases mass and functional capacity of damaged skeletal muscle. Cell Transplant, 13, 103–111.
Lee, J. H., & Kemp, D. M. (2006). Human adipose-derived stem cells display myogenic potential and perturbed function in hypoxic conditions. Biochem Biophys Res Commun, 341, 882–888.
Di Rocco, G., Iachininoto, M. G., Tritarelli, A., et al. (2006). Myogenic potential of adipose-tissue-derived cells. J Cell Sci, 119, 2945–2952.
Vieira, N. M., Brandalise, V., Zucconi, E., et al. (2008). Human multipotent adipose-derived stem cells restore dystrophin expression of Duchenne skeletal-muscle cells in vitro. Biol Cell, 100, 231–241.
Messina, S., Mazzeo, A., Bitto, A., et al. (2007). VEGF overexpression via adeno-associated virus gene transfer promotes skeletal muscle regeneration and enhances muscle function in mdx mice. FASEB J, 21, 3737–3746.
Gargioli, C., Coletta, M., De Grandis, F., et al. (2008). PlGF-MMP-9-expressing cells restore microcirculation and efficacy of cell therapy in aged dystrophic muscle. Nat Med, 14, 973–978.
Rando, T. A. (2008). Turning back time: reversing tissue pathology to enhance stem cell engraftment. Cell Stem Cell, 3, 232–234.
Pinheiro, C. H., Vitzel, K. F., & Curi, R. (2010). Effect of N-acetylcysteine on markers of skeletal muscle injury after fatiguing contractile activity. Scand J Med Sci Sports. doi:10.1111/j.1600-0838.2010.01143.x
Bassit, R. A., Pinheiro, C. H., Vitzel, K. F., et al. (2010). Effect of short-term creatine supplementation on markers of skeletal muscle damage after strenuous contractile activity. Eur J Appl Physiol, 108, 945–955.
Chamberlain, J. S., Metzger, J., Reyes, M., et al. (2007). Dystrophin-deficient mdx mice display a reduced life span and are susceptible to spontaneous rhabdomyosarcoma. FASEB J, 21, 2195–2204.
Moser, H. (1984). Review of studies on the proportion and origin of new mutants in Duchenne muscular dystrophy. In L. P. Ten Kate, P. L. Pearson, & A. M. Stadhouders (Eds.), Research into the Origin and Treatment of Muscular Dystrophy (pp. 41–52). Amsterdam: Excerpta Medica.
Lynch, G. S., Hinkle, R. T., Chamberlain, J. S., et al. (2001). Force and power output of fast and slow skeletal muscles from mdx mice 6–28 months old. J Physiol, 535, 591–600.
Gnecchi, M., Zhang, Z., Ni, A., et al. (2008). Paracrine mechanisms in adult stem cell signaling and therapy. Circ Res, 103, 1204–1219.
Lecarpentier, Y. (2007). Physiological role of free radicals in skeletal muscles. J Appl Physiol, 103, 1917–1918.
Irintchev, A. (1987). Muscle damage and repair in voluntarily running mice: strain and muscle differences. Cell Tissue Res, 249, 509–521.
Mendell, J. R. (1971). Duchenne muscular dystrophy: functional ischemia reproduces its characteristic lesions. Science, 172, 1143–1145.
Louboutin, J. P., Rouger, K., Tinsley, J. M., et al. (2001). iNOS expression in dystrophinopathies can be reduced by somatic gene transfer of dystrophin or utrophin. Mol Med, 7, 355–364.
Bredt, D., & Snyder, S. (1994). Nitric oxide: a physiologic messenger molecule. Ann Rev Biochem, 63, 175–195.
Kobzik, L., Reid, M., Bredt, D., et al. (1994). Nitric oxide in skeletal muscle. Nature, 372, 546–548.
Ischiropoulos, H. (1998). Biological tyrosine nitration: a pathophysiological function of nitric oxide and reactive oxygen species. Arch Biochem Biophys, 356, 1–11.
Wehling, M., Spencer, M. J., & Tidball, J. G. (2001). A nitric oxide synthase transgene ameliorates muscular dystrophy in mdx mice. J Cell Biol, 155, 123–131.
Gurpur, P. B., Liu, J., Burkin, D. J., et al. (2009). Valproic acid activates the PI3K/Akt/mTOR pathway in muscle and ameliorates pathology in a mouse model of Duchenne muscular dystrophy. Am J Pathol, 174, 999–1008.
Chung, J., Grammer, T. C., Lemon, K. P., et al. (1994). PDGF- and insulin-dependent pp 70S6k activation mediated by phosphatidylinositol-3-OH kinase. Nature, 370, 71–75.
Orlic, D., Kajstura, J., Chimenti, S., et al. (2001). Bone marrow cells regenerate infarcted myocardium. Nature, 410, 701–705.
Orlic, D., Kajstura, J., Chimenti, S., et al. (2001). Mobilized bone marrow cells repair the infarcted heart, improving function and survival. Proc Natl Acad Sci USA, 98, 10344–10349.
Aggarwal, S., & Pittenger, M. F. (2005). Human mesenchymal stem cells modulate allogeneic immune cell responses. Blood, 105, 1815–1822.
Caplan, A. I., & Dennis, J. E. (2006). Mesenchymal stem cells as trophic mediators. J Cell Biochem, 98, 1076–1084.
Tang, Y. L., Zhao, Q., Qin, X., et al. (2005). Paracrine action enhances the effects of autologous mesenchymal stem cell transplantation on vascular regeneration in rat model of myocardial infarction. Ann Thorac Surg, 80, 229–236.
Togel, F., Hu, Z., Weiss, K., et al. (2005). Administered mesenchymal stem cells protect against ischemic acute renal failure through differentiation-independent mechanisms. Am J Physiol Renal Physiol, 289, F31–F42.
Rehman, J., Traktuev, D., Li, J., Merfeld-Clauss, S., et al. (2004). Secretion of angiogenic and antiapoptotic factors by human adipose stromal cells. Circulation, 109, 1292–1298.
Al-Khaldi, A., Al-Sabti, H., Galipeau, J., et al. (2003). Therapeutic angiogenesis using autologous bone marrow stromal cells: improved blood flow in a chronic limb ischemia model. Ann Thorac Surg, 75, 204–209.
Nagaya, N., Fujii, T., Iwase, T., et al. (2004). Intravenous administration of mesenchymal stem cells improves cardiac function in rats with acute myocardial infarction through angiogenesis and myogenesis. Am J Physiol Heart Circ Physiol, 287, H2670–H2676.
Nagaya, N., Kangawa, K., Itoh, T., et al. (2005). Transplantation of mesenchymal stem cells improves cardiac function in a rat model of dilated cardiomyopathy. Circulation, 112, 1128–1135.
Wehling-Henricks, M., Lee, J. J., & Tidball, J. G. (2004). Prednisolone decreases cellular adhesion molecules required for inflammatory cell infiltration in dystrophin-deficient skeletal muscle. Neuromuscul. Disord., 14, 483–490.
Messina, S., Bitto, A., Aguennouz, M., et al. (2006). Nuclear factor kappa-B blockade reduces skeletal muscle degeneration and enhances muscle function in Mdx mice. Exp Neurol, 198(1), 234–241.
Tidball, J. G., & Wehling-Henricks, M. (2007). Macrophages promote muscle membrane repair and muscle fibre growth and regeneration during modified muscle loading in mice in vivo. J Physiol., 578(Pt 1), 327–336.
Vetrone, S. A., Montecino-Rodriguez, E., Kudryashova, E., et al. (2009). Osteopontin promotes fibrosis in dystrophic mouse muscle by modulating immune cell subsets and intramuscular TGF-beta. J Clin Invest., 119(6), 1583–1594.
Barbul, A., Lazarou, S. A., Efron, D. T., et al. (1990). Arginine enhances wound healing and lymphocyte immune responses in humans. Surgery, 108, 331–337.
Wehling-Henricks, M., Jordan, M. C., Gotoh, T., et al. (2010). Arginine metabolism by macrophages promotes cardiac and muscle fibrosis in mdx muscular dystrophy. PLoS One., 5(5), e10763.
Acknowledgements
C.H.J Pinheiro was scholar fellowship of São Paulo Research Foundation—FAPESP [2008/54693-9]. The authors thank Emilia Ribeiro, J.R. de Mendonça, Dr. Tatiana C. Alba Loureiro and Adhemar Pettri Filho for constant assistance. This work was also supported by the National Council for Scientific and Technological Development (CNPq) [573557/2008-0].
Author information
Authors and Affiliations
Corresponding author
Additional information
The authors declare no potential conflicts of interest.
Rights and permissions
About this article
Cite this article
da Justa Pinheiro, C.H., de Queiroz, J.C.F., Guimarães-Ferreira, L. et al. Local Injections of Adipose-Derived Mesenchymal Stem Cells Modulate Inflammation and Increase Angiogenesis Ameliorating the Dystrophic Phenotype in Dystrophin-Deficient Skeletal Muscle. Stem Cell Rev and Rep 8, 363–374 (2012). https://doi.org/10.1007/s12015-011-9304-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-011-9304-0