Abstract
Doxorubicin (DOX) has been used in a variety of human malignancies for decades, in particular of lymphoma. But increased cardiomyocyte apoptosis has been implicated in its cardiotoxicity. Resveratrol (RES) generates cardiovascular protective effects by heme oxygenase-1(HO-1)-mediated mechanism. The present study was designed to determine whether RES protected cardiomyocyte against apoptosis through induction of HO-1 in lymphoma nude mouse in vivo. After being developed into lymphoma model, 40 male Balb/c nude mice were randomized to one of the following four treatments (10 mice per group): control, DOX, DOX + RES and DOX + RES + HO-1 inhibitor (zinc protoporphyrin IX, ZnPP). The results showed that DOX injection markedly decreased the body weight, the heart weight and the ratio of heart weight to body weight, but inversely increased cardiomyocyte apoptosis and the level of serum lactate dehydrogenase and creatine kinase. Moreover, DOX injection attenuated HO-1 expression and enzymatic activity as well as increased P53 expression, modulated Bcl-2/Bax expression and enhanced caspase 3 activity. These cardiotoxic effects of DOX were ameliorated by its combination with RES. However, the protective effects of RES were reversed by the addition of ZnPP. Taken together, it is concluded that HO-1 plays a core role for protective action of RES in DOX-induced cardiomyocyte apoptosis in lymphoma nude mice.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Doxorubicin (DOX)-based chemotherapy improves survival in patients with lymphoma; however, side effects of irreversible cardiomyopathy and heart failure (HF) limit its clinical use [1–4]. Cardiotoxicity is reported in 14–49 % of lymphoma patients treated with DOX [5–7]. Previous studies demonstrated that cardiomyocyte apoptosis plays an important role in DOX-induced cardiotoxicity [8]. Heme oxygenase-1(HO-1) is a cytoprotective enzyme that plays a key role in host defense against oxidative stress and apoptosis [8]. The down-modulation of HO-1 expression and its association with decreased anti-apoptotic effect in DOX-induced cardiotoxicity have recently been stressed [8]. Thus, it is of great interest to investigate the therapeutic potential of a chemical that induces HO-1 gene expression in DOX-induced cardiomyocyte apoptosis.
Resveratrol (RES), a polyphenol found in red wine, possesses comprehensive biochemical and physiological actions, including estrogenic, anti-platelet and anti-inflammatory properties [9]. Interestingly, RES generates cardiovascular protective effect by up-regulated HO-1-mediated mechanism [10]. Recent studies also revealed the protective abilities of RES in DOX-induced cardiomyocyte apoptosis [11, 12]. However, whether or not RES affects DOX-induced cardiomyocyte apoptosis in lymphoma in vivo, especially mediated by induction of HO-1, is unknown.
Accordingly, in the present study, we developed a lymphoma nude mouse model to elucidate (1) whether RES was effective in protecting cardiomyocyte against DOX-induced apoptosis and (2) whether the protective effect of RES was mediated by induction of HO-1 in vivo.
Methods
Animal Preparation
Male BALB/c nude mice (4–6 weeks of age) were obtained from Shanghai Laboratory Animal Center, Chinese Academy of Science, and were acclimated for 1 week before the start of studies. Mice received sterile rodent chow and water ad libitum and were housed in sterile filter-top cages with 12-h light/dark cycles. All in vivo studies were conducted in compliance with the Guide for the Care and Use of Laboratory Animals published in China.
Human Lymphoma Cell Lines Culture and Lymphoma Nude Mice Model
The human Burkitt's lymphoma cell lines (Raji) were obtained from Shanghai institute of Biochemistry and Cell Biology, Chinese Academy of Science. Raji cells were grown in RPMI supplemented with 10 % heat-inactivated fetal bovine serum (Gibco, USA). Cells were grown as suspension cultures and maintained in a humidified atmosphere at 37 °C and 5 % CO2. The cells were washed twice with phosphate-buffered saline (PBS). Cell number and viability of the cells were determined with the trypan blue dye exclusion method using a hemocytometer. A suspension of 5 × 107 Raji cells in 100 uL PBS was injected subcutaneously on the right flanks of a nude mouse. Tumor volumes were measured in two dimensions by using a vernier caliper. Tumor volumes were calculated using the formula: (length × width2) × 0.5 [13].
After cell transplantation for 3 weeks (tumor length: 5–10 mm), mice were randomly divided into 4 groups (10 mice per group): (1) control group, (2) DOX (Sigma-Aldrich, USA) group, (3) DOX + RES (purity: 99.9 %, Nabio, China) group, and (4) DOX + RES + HO-1 inhibitor (ZnPP-IX, Sigma-Aldrich, USA) group. In each of the DOX-treated groups, DOX was injected intraperitoneally into the mice for six times for 2 weeks (cumulative dose of 12 mg/kg). In each of the RES-treated groups, RES was gavaged into mice (10 mg/kg/d, duration: 1 week before DOX injection until they were killed). In each of the ZnPP-treated groups, ZnPP was injected intraperitoneally (20 μmol/kg) into the mice three times per week (the duration was consistent with that of RES treatment). Control mice were injected with the same volume of sterile isotonic saline. Two weeks after the last DOX injection, all of the animals were killed after overnight fasting. Mice hearts were weighed and fixed in 10 % formalin for histological analysis or snap-frozen in liquid nitrogen followed by storage at −80 °C freezer until required.
Creatine Kinase (CK) and Lactate Dehydrogenase (LDH) Activities Assay
After the mice were sacrificed, blood was drawn from the vena cava inferior. The blood samples were allowed to clot, and the serum was used for the measurement of LDH and CK activities according to the manufacturer’s instructions (Nanjing Jiancheng Biotechnology Institute, China).
HO-1 Activity Assay
HO-1 activity was measured using a spectrophotometric assay of bilirubin production [14]. Briefly, aliquots of cytosolic extracts prepared as described for the immunoblotting assay were further centrifuged at 12,000×g for 15 min, and the supernatant was added to the following mixture: 2 mM MgCl2, 100 mM PBS, pH 7.4, biliverdin reductase, 20 mM hemin (Sigma-Aldrich, USA), 0.18 U/uL glucose-6-phosphate dehydrogenase (Sigma-Aldrich, USA), 2 mM glucose-6-phosphate and 0.8 mM NADPH. The reaction was conducted in the dark for 30 min at 37 °C and terminated by the addition of chloroform. The amount of extracted bilirubin was calculated on the basis of the difference in absorption between 464 and 530 nm, and an extinction coefficient of 40 mM−1 cm−1 was used to calculate bilirubin levels in terms of absorbance units per μg protein.
Caspase-3 Activity Assay
The caspase-3 activity was determined according to the previously published method [15]. Briefly, 1 ml of PBS was added to the heart tissues. Tissues were homogenized and centrifuged at 10,000×g at 4 °C for 10 min. The supernatant was discarded, and pellets were lysed in 100 μl of ice-cold lysis buffer [50 mM HEPES, pH 7.4, 0.1 % CHAPS, 1 mM dithiothreitol (DTT), 0.1 mM EDTA, 0.1 % NP40]. The assay for caspase-3 activity was carried out in a 96-well plate. Each well contained 30 μl of lysate, 70 μl of assay buffer (50 mM HEPES, pH 7.4, 0.1 % CHAPS, 100 mM NaCl, 10 mM DTT, and 1 mM EDTA) and 20 μl of caspase-3 colorimetric substrate Ac-DEVD-pNA (Sigma, USA). The 96-well plate was incubated at 37 °C for 2 h, during which time caspase in the sample was allowed to cleave the chromophore p-NA from the substrate molecule. Absorbance readings were obtained at 405 nm, with the caspase-3 activity being directly proportional to the colorimetric reaction. Protein content was determined using the Bradford method.
Immunohistochemistry
Mice were euthanized under anesthesia, and heart samples were harvested at the end of the study. The specimens were fixed in 10 % formalin for 24 h, and then left ventricular (LV) myocardial samples were embedded with paraffin and sectioned at three sections from base to apex. The paraffin sections, 5 μm thick, were deparaffinated and rehydrated with xylene and graded alcohol series. Sections were incubated overnight at 4 °C with primary antibody anti-bcl-2 and anti-bax (Santa Cruz, USA), rinsed (PBS) and incubated for 2 h with specie peroxidase-conjugated secondary antibody. The reaction was visualized with a solution of diaminobenzidine (DAB). Negative controls consisted of omission of primary antibody. For quantification, intensity optical density of Bcl-2 and Bax staining were calculated with Image Pro Plus version 6.0.
Protein Preparation and Western Blotting
Total protein was extracted, and concentration was measured by the Bradford method (Thermo scientific, USA). As described earlier, 50 μg protein samples were separated on 12 % SDS-PAGE gels and transferred onto a polyvinylidene difluoride membrane (Bio-Rad). The membranes were blocked with 5 % nonfat dry milk in Tris-buffered saline containing 0.1 % Tween 20 and incubated with specific antibodies against HO-1, P53 (Santa Cruz, USA) and GAPDH (Cell Signal Technology, USA). After incubation with a secondary peroxidase-conjugated antibody, western blots were developed using SuperSignal West Femto Chemiluminescent Substrate (Thermo scientific, USA) and quantified by scanning densitometry. The ratio of the protein interested was subjected to GAPDH and was densitometrically analyzed by Quantity one (USA).
Apoptosis Assessment by TUNEL
To detect apoptosis, TUNEL (terminal deoxynucleotide transferase–mediated dUTP nick end labeling) staining was performed using In Situ Cell Apoptosis Detection Kits (Boster Biological Technology, China). According to the manufacturer’s instructions, paraffin-embedded LV sections of samples were deparaffinated and hydrated and then incubated in 20 g/mL protease K at room temperature for 5 min. After being washed twice, the samples were put into sodium citrate buffer (2 mmol/L citric acid, and 10 mmol/L trisodium citrate, pH 6.0) at 37 °C for 5 min. After being washed with PBS for 5 min twice, 20 mL TUNEL reaction mixture (1 mL terminal deoxynucleotidyl transferase, 1 mL digoxin-labeled d-UTP and 18 mL Labelling Buffer) was added to the sample and incubated at 37 °C for 60 min.
After rinsing, the sections were incubated with biotin–anti-digoxin antibody for 30 min at 37 °C and developed with DAB Substrate Kit. The slides were lightly counterstained with hematoxylin and then dehydrated and mounted. For each myocardial specimen, tissue sections were examined microscopically at 400× magnification, and 10 random fields per section were counted. The percentage of apoptotic cells was calculated by the apoptotic index, that is, dividing the number of positive-staining myocyte nuclei by the total number of myocyte nuclei.
Statistical Analysis
Data were expressed as mean ± standard deviation (SD) and were compared by analysis of variance and Student’s t test with SPSS 16.0 software. A P value less than 0.05 was considered statistically significant.
Results
RES Diminished DOX-Induced Losses of the Body Weight, The Heart Weight and the Ratio of Heart Weight to Body Weight
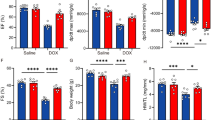
The body weight of lymphoma nude mice from various groups was comparable before treatment (data not shown). DOX injection significantly decreased the body weight, the heart weight and the ratio of heart weight to body weight, which were diminished by supplement with RES. Moreover, the aforementioned protective effect of RES was inhibited by the addition of ZnPP (Fig. 1).
RES diminished DOX-induced losses of the body weight, the heart weight and the ratio of heart weight to body weight, which were reversed by ZnPP. The body weight (a), the heart weight (b) and the ratio of heart weight to body weight (c) were significantly decreased by DOX, but RES treatment diminished DOX-related losses in the body weight, the heart weight and the ratio of heart weight to body weight. And supplementation with ZnPP reversed the protective effect of RES. *P < 0.05 versus control group; # P < 0.05 versus DOX group; & P < 0.05 versus DOX + RES group. n = 6
RES Alleviated DOX-Induced Cardiac Damage
As shown in Fig. 2, compared with the control group, DOX alone increased the serum CK and LDH levels significantly. The serum CK and LDH levels in combined treatments of RES and DOX were greatly decreased when compared with those in DOX group, which were reversed by supplemented with ZnPP.
RES Reduced Myocardial Cell Apoptosis Induced by DOX
That DOX-induced cardiotoxicity caused apoptosis in the lymphoma mouse heart was supported by increased number of TUNEL-positive cells (Fig. 3). The increased number of TUNEL-positive cells by DOX injection was significantly reduced by RES treatment, which was again reversed by supplementation with ZnPP (Fig. 3).
Caspase 3 activity assay and apoptotic index detected by TUNEL staining. Up: Treatment with RES reduced myocardial caspase 3 activity in DOX-treated mice, which was reversed by ZnPP (n = 10). Middle: Representative photomicrographs are shown demonstrating TUNEL staining of heart sections from control group (a), DOX group (b), DOX + RES group (c) and DOX + RES + ZnPP group (d). TUNEL-positive cells are indicated by brown staining, and the TUNEL-positive cardiac myocytes are indicated by arrows (magnification: ×200). Bottom: Histogram showed the quantitative analysis of TUNEL-positive cells (n = 5). * P < 0.01 versus control group; # P < 0.01 versus DOX group; & P < 0.05 versus DOX + RES group
RES Weakened DOX-Induced Apoptosis Pathway Activation
The result of western blotting showed that DOX injection resulted in enhanced p53 expression in the myocardium of lymphoma nude mouse, but treatment with RES could weaken this impact. Additionally, the decreased P53 expression by RES administration was reversed by supplementation with ZnPP (Fig. 4).
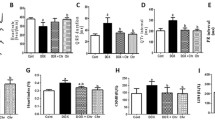
RES reversed DOX-induced inhibition of HO-1 expression and activation as well as P53 expression, which were inhibited by ZnPP. a HO-1 and P53 protein expression was studied by western blotting. Data were representative of four independent experiments. Histogram showed the analysis of HO-1 (b), P53 (c) protein expression and HO-1 activity (d, n = 10). *P < 0.01 versus control group; # P < 0.01 versus DOX group; & P < 0.05 versus DOX + RES group
Immunohistochemical analysis of the expression of pro-apoptotic or anti-apoptotic proteins showed that DOX injection significantly increased the expression of pro-apoptotic Bax protein, but decreased the expression of anti-apoptotic Bcl-2 protein in the myocardium. However, by the treatment of RES, the expression of Bax or Bcl-2 protein was down-regulated or up-regulated, respectively, which were attenuated by supplementation with ZnPP (Fig. 5, Table 1).
Representative immunohistochemical staining of Bcl-2 and Bax expression in myocardium. Up: Bcl-2 protein expression of control group (a), DOX group (b), DOX + RES group (c) and DOX + RES + ZnPP group (d). Bottom: Bax protein expression of control group (a), DOX group (b), DOX + RES group (c) and DOX + RES + ZnPP group (d). (magnification: ×200)
RES Blocked DOX-Induced Activation of Caspase-3
When compared with those in control group, more than 1.5-fold increases in myocardial caspase-3 activities were shown in DOX group, in which supplementation with RES suppressed the caspase-3 activities that were almost compatible with those of control animals. However, administration of ZnPP significantly inhibited the effect of RES on caspase-3 activity (Fig. 3).
RES Up-Regulated HO-1 Expression and Enzymatic Activity
As shown in Fig. 4, DOX inhibited the HO-1 expression and enzymatic activity in DOX-treated lymphoma nude mice; however, DOX supplemented with RES increased HO-1 expression and enzymatic activity compared with DOX alone, which were significantly suppressed by the addition of ZnPP.
RES had No Impact on DOX’s Anti-Tumor Capacity
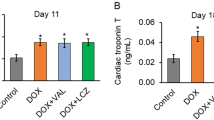
The tumor volume of various groups was comparable before treatment. However, at the end of our experiment, the tumor volume in control group was markedly larger than the remaining three groups, and no significant difference was found between the DOX, DOX + RES and DOX + RES + ZnPP groups (Fig. 6).
Discussion
The main findings of this work were as follows: (a) The decrease in HO-1 expression and enzymatic activity as well as increased cardiomyocyte apoptosis and damage were observed in lymphoma nude mice heart after injection of DOX. (b) Compared with DOX alone, DOX supplemented with RES precipitated HO-1 expression and enzymatic activity as well as protected cardiomyocyte against apoptosis and damage. (c) The protective effects of RES were reversed by HO-1 inhibitor (ZnPP), suggesting that the effects are, at least in part, mediated by HO-1. This study demonstrated the beneficial role of HO-1 in the attenuation of DOX-induced cardiomyocyte apoptosis by RES treatment in lymphoma nude mice.
DOX, a classical anti-neoplastic antibiotic that is still widely used in the treatment of a variety of various hematological malignancies and solid tumors, in particular of lymphoma [1–4]. Its clinical usage, however, carries substantial risk of cardiomyopathy and life-threatening HF [3, 4]. The exact mechanism of DOX-induced cardiotoxicity is not completely clear, but increased myocardial cell apoptosis may play an important role. Mitochondrial dysfunction is one of the most critical events associated with DOX-induced cardiomyocyte apoptosis, in which anti-apoptotic Bcl-2 and pro-apoptotic Bax genes are suggested to play a major role in determining cell’s survival or death after apoptotic stimuli [16, 17]. Previous study also showed that the P53 tumor suppressor gene may use transcriptional activation to regulate the gene products of the Bcl-2 family proteins, and then promoted caspase-3–mediated apoptosis [11]. To determine the cardiotoxic effect of DOX in lymphoma in vivo, we developed a lymphoma nude mouse model. In agreement with previous study, we found that DOX remarkably decreased the body weight, the heart weight and the ratio of heart weight to body weight in lymphoma nude mice, but inversely increased the number of apoptotic myocardial cells and the level of serum LDH and CK, and led to enhanced expression of P53 and Bax, decreased expression of Bcl-2 and increased activity of caspase 3.
In recent years, many studies have been conducted using adjunctive therapy to counteract the adverse cardiac effects of DOX. Nonetheless, to date, only few, if any, agents have been proven to be applicable in clinical practice [1]. RES, a polyphenol compound found in grapes and red wine in significant amounts, has been designated as the responsible agent of the French paradox [9]. It has been found that RES possesses many biologic activities, including estrogenic property, anti-platelet activity, anti-inflammatory function and anti-oxidative activity [9]. Previous studies have shown that RES protects cardiomyocyte against DOX-induced apoptosis [11, 12]. But its influence in animal model of malignancies in vivo is unknown. Moreover, the mechanism by which RES protects cardiomyocyte against apoptosis remains largely unclear. It has been said that the decreased HO-1 expression or enzymatic activity was associated with DOX-induced myocardial apoptosis [8]. Interestingly, RES possesses the ability to enhance the expression of HO-1 [10]. So we postulated that RES might protect cardiomyocyte against DOX-induced apoptosis by means of its ability to increase HO-1 expression in lymphoma nude mouse.
As expected, we found that DOX injection resulted in significant reduction in HO-1 expression or enzymatic activity. And supplementation with RES increased the HO-1 expression and enzymatic activity as well as inhibited the myocardial cell apoptosis and damage. Moreover, RES treatment diminished DOX-induced losses in the body weight, the heart weight and the ratio of heart weight to body weight. However, ZnPP, a HO-1 inhibitor, reversed the protective effect of RES toward DOX-induced HO-1 over-expression and enzymatic activation, myocardial apoptosis and damage.
HO-1, which catabolizes heme to biliverdin, carbon monoxide (CO) and iron, is induced by a variety of stressful stimuli, particularly oxidative damage, and serves as a protective gene in a wide range of pathophysiological situations [18]. It is demonstrated that HO-1 has an anti-apoptotic effect by inhibiting Fas/Fas ligand, caspases, pro-apoptotic Bax proteins and cytochrome c release, by virtue of heme degradation products such as CO and biliverdin/bilirubin [19, 20]. Myocyte-specific HO-1 overexpression in HF promoted tissue neovascularization and ameliorated myocardial P53 expression and apoptosis [21]. Concurrently, over-expression of HO-1 was associated with inhibition of caspase-3 and with increased expression of Bcl-xL [22]. Up-regulation of P53 inhibited Bcl-2 protein expression, increased the expression of Bax protein, contributed to the release of cytochrome c and promoted caspase-3-mediated apoptosis [11]. In the present study, the increase in P53 expression induced by DOX was alleviated in mice supplemented with RES, in which HO-1 expression or enzymatic activity was up-regulated. This finding was accompanied with the alteration of Bcl-2/Bax expression, the decrease in caspase-3 activity and the reduction in TUNEL-positive cells. And aforementioned protective effects of RES were diminished by adjunctive ZnPP therapy. So we postulated that HO-1 induction by RES might modulate Bcl-2/Bax expression and suppress caspase-3 activity through inhibition of P53 expression. Furthermore, a recent study showed that the protective effect of RES against DOX-induced cardiomyocyte apoptosis was associated with the up-regulation of SIRT1-mediated p53 deacetylation [11].
In addition, whether RES affected the anti-tumor capacity of DOX was also evaluated in the present study. We found no marked difference in the tumor volume between the DOX, DOX + RES and DOX + RES + ZnPP groups at the end of our experiment. So we believed that RES had no impact on the anti-tumor capacity of DOX, which might be an effective adjunctive therapy to counteract the adverse cardiac effects of DOX during the lymphoma treatment.
In conclusion, our present study was the first to demonstrate the involvement of the HO-1 in the DOX-induced cardiomyocyte apoptosis in lymphoma nude mice model. We investigated the protective effect of RES on DOX-treated lymphoma nude mouse model and found that RES reduced DOX-induced cardiac damage and apoptosis. The induction of HO-1 by RES was related to the reduced cardiac damage and apoptosis, modulation of genes associated with apoptosis. Most importantly, these beneficial effects were reversed by the presence of HO-1 inhibitor (ZnPP), which strongly suggested that HO-1 played a core role in protective action of RES in DOX-treated lymphoma nude mice.
References
Wouters, K. A., Kremer, L. C., Miller, T. L., Herman, E. H., & Lipshultz, S. E. (2005). Protecting against anthracycline induced myocardial damage: A review of the most promising strategies. British Journal of Haematology, 131, 561–578.
Gianni, L., Herman, E. H., Lipshultz, S. E., Minotti, G., Sarvazyan, N., & Sawyer, D. B. (2008). Anthracycline cardiotoxicity: From bench to bedside. Journal of Clinical Oncology, 26, 3777–3784.
Limat, S., Demesmay, K., Voillat, L., Bernard, Y., Deconinck, E., Brion, A., et al. (2003). Early cardiotoxicity of the CHOP regimen in aggressive non-Hodgkin’s lymphoma. Annal of Oncology, 14, 277–281.
Aviles, A., Arevila, N., Diaz Maqueo, J. C., Gómez, T., García, R., & Nambo, M. J. (1993). Late cardiac toxicity of doxorubicin, epirubicin, and mitoxantrone therapy for Hodgkin’s disease in adults. Leukemia & Lymphoma, 11, 275–279.
Haddy, T. B., Adde, M. A., McCalla, J., Domanski, M. J., Datiles, M, 3rd, Meehan, S. C., et al. (1998). Late effects in long-term survivors of high-grade non-Hodgkin’s lymphomas. Journal of Clinical Oncology, 16, 2070–2079.
Hequet, O., Le, Q. H., Moullet, I., Pauli, E., Salles, G., Espinouse, D., et al. (2004). Subclinical late cardiomyopathy after doxorubicin therapy for lymphoma in adults. Journal of Clinical Oncology, 22, 1864–1871.
Limat, S., Demesmay, K., Voillat, L., Bernard, Y., Deconinck, E., Brion, A., et al. (2003). Early cardiotoxicity of the CHOP regimen in aggressive non-Hodgkin’s lymphoma. Annal of Oncology, 14, 277–281.
Bernuzzi, F., Recalcati, S., Alberghini, A., & Cairo, G. (2009). Reactive oxygen species-independent apoptosis in doxorubicin-treated H9c2 cardiomyocytes: Role for heme oxygenase-1 down-modulation. Chemico-Biological Interactions, 177, 12–20.
Delmas, D., Jannin, B., & Latruffe, N. (2005). Resveratrol: preventing properties against vascular alterations and ageing. Molecular Nutrition & Food Research, 49, 377–395.
Kim, J. W., Lim, S. C., Lee, M. Y., Lee, J. W., Oh, W. K., Kim, S. K., et al. (2010). Inhibition of neointimal formation by trans-resveratrol: Role of phosphatidyl inositol 3-kinase-dependent Nrf2 activation in heme oxygenase-1 induction. Molecular Nutrition & Food Research, 54, 1497–1505.
Zhang, C., Feng, Y., Qu, S., Wei, X., Zhu, H., Luo, Q., et al. (2011). Resveratrol attenuates doxorubicin-induced cardiomyocyte apoptosis in mice through SIRT1-mediated deacetylation of p53. Cardiovascular Research, 90, 538–545.
Oktem, G., Uysal, A., Oral, O., Sezer, E. D., Olukman, M., Erol, A., et al. (2012). Resveratrol attenuates doxorubicin-induced cellular damage by modulating nitric oxide and apoptosis. Experiment and Toxicologic Pathology, 64, 471–479.
Lopes de Menezes, D. E., Denis-Mize, K., Tang, Y., Ye, H., Kunich, J. C., Garrett, E. N., et al. (2007). Recombinant interleukin-2 significantly augments activity of rituximab in human tumor xenograft models of B-cell non-Hodgkin lymphoma. Journal of Immunotherapy, 30, 64–74.
Lee, Y. S., Kang, Y. J., Kim, H. J., Park, M. K., Seo, H. G., Lee, J. H., et al. (2006). Higenamine reduces apoptotic cell death by induction of heme oxygenase-1 in rat myocardial ischemia-reperfusion injury. Apoptosis, 11, 1091–1100.
Li, S. Y., Gomelsky, M., Duan, J., Zhang, Z., Gomelsky, L., Zhang, X., et al. (2004). Overexpression of aldehyde dehydrogenase-2 (ALDH2) transgene prevents acetaldehyde-induced cell injury in human umbilical vein endothelial cells: role of ERK and p38 mitogen-activated protein kinase. The Journal of Biological Chemistry, 279, 11244–112452.
Zhou, S., Starkov, A., Froberg, M. K., Leino, R. L., & Wallace, K. B. (2001). Cumulative and irreversible cardiac mitochondrial dysfunction induced by doxorubicin. Cancer Research, 61, 771–777.
Childs, A. C., Phaneuf, S. L., Dirks, A. J., Phillips, T., & Leeuwenburgh, C. (2002). Doxorubicin treatment in vivo causes cytochrome C release and cardiomyocyte apoptosis as well as increased mitochondrial efficiency, superoxid dismutase activity, and Bcl-2:Bax ratio. Cancer Research, 62, 4592–4598.
Ryter, S. W., Alam, J., & Choi, A. M. (2006). Heme oxygenase-1/carbon monoxide: from basic science to therapeutic applications. Physiological Reviews, 86, 583–650.
Kim, H. P., Ryter, S. W., & Choi, A. M. (2006). CO as a cellular signaling molecule. Annual Review of Pharmacology Toxicology, 46, 411–449.
Ollinger, R., Wang, H., Yamashita, K., Wegiel, B., Thomas, M., Margreiter, R., et al. (2007). Therapeutic applications of bilirubin and biliverdin in transplantation. Antioxidants & Redox Signaling, 9, 2175–2185.
Wang, G., Hamid, T., Keith, R. J., Zhou, G., Partridge, C. R., Xiang, X., et al. (2010). Cardioprotective and anti-apoptotic effects of heme oxygenase-1 in the failing heart. Circulation, 121, 1912–1925.
Sun, M. H., Pang, J. H., Chen, S. L., Han, W. H., Ho, T. C., Chen, K. J., et al. (2010). Retinal protection from acute glaucoma-induced ischemia-reperfusion injury through pharmacologic induction of heme oxygenase-1. Investigative Ophthalmology & Visual Science, 51, 4798–4808.
Acknowledgments
This study was supported by grant 2008Y052 from Youth foundation of Shanghai Municipal Health Bureau (Shanghai, China).
Conflict of interest
The authors have no financial and/or personal relationships with other people or organization that could influence this report.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gu, J., Song, Zp., Gui, Dm. et al. Resveratrol Attenuates Doxorubicin-Induced Cardiomyocyte Apoptosis in Lymphoma Nude Mice by Heme Oxygenase-1 Induction. Cardiovasc Toxicol 12, 341–349 (2012). https://doi.org/10.1007/s12012-012-9178-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12012-012-9178-7