Abstract
Chandanasava is an Ayurvedic polyherbal fermented traditional medicine (FTM) used by traditional practitioners for millennia. Nevertheless, the mode of action and functional targets are still unknown. The current study includes a pharmacological network analysis to identify the Chandanasava compounds interacting with target proteins involved in chronic kidney disease (CKD) and cardiovascular disease (CVD). Sixty-one Chandanasava phytochemicals were obtained by GC–MS and screened using the Traditional Chinese Medicine Systems Pharmacology Database (TCMSP). The disease target genes were obtained from DisGeNET and GeneCards databases. Forty-five phytocompounds and 135 potential targets were screened for CKD and CVD target proteins and protein interaction networks were constructed. The pharmacological network was deciphered employing target proteins involved in the mechanical action of Chandanasava. The results indicated that 10 bioactive compounds exhibited higher binding affinity patterns with the screened 42 CKD and CVD target proteins. Gene Ontology and KEGG analysis revealed target pathways involved in CKD and CVD, which were further explored by detailed analysis and network-coupled drug profile screening. The molecular docking results showed piperine and melatonin as effective inhibitors/regulators of the hub genes of CKD and CVD. The current study establishing authentic bioactive compounds in FTM is based on deeper insights into recognized Ayurvedic medicines.
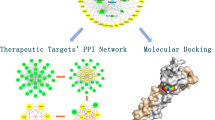
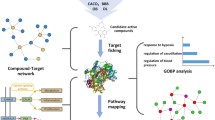
Graphical Abstract
Representing the workflow of the network pharmacological analysis

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Chronic kidney diseases (CKD) and cardiovascular diseases (CVD) correspond to multifaceted, complicated disorders affecting a global human population, causing escalated mortality and morbidity rates owing to hospice conditions and survival challenges [1]. The negative correlations are aggravated in non-dialysis-dependent renal failure, myocardial ischemia, heart failure, and hypertension [2, 3]. End-stage renal disease patients are corroborated for an increased risk for cardiovascular complications and necessitate proper management [4]. Glomerular filtration rate and myocardial infarction have been associated with many population-based randomized trials [5, 6]. Life expectancy and increased prevalence of CVD and CKD among diabetic patients require impact assessment for cost-effective protocols, economic burden, and premature mortality management [7]. Ayurveda possesses sufficient potential to be used to prevent and treat various ailments [8]. The Ayurvedic pharmacopeia contains a variety of medications, including fermented traditional medicines (FTM), which are classified as Arishta (decoctions) and Asava (infusions), comprising polyherbal formulations invigorated by naturally occurring intrinsic microorganisms. Arishta and Asava are traditionally regarded as distinct and effective therapeutic formulations due to their improved storage efficiency, strengthened pharmacological activities, improved separation of bioactive compounds from herbal ingredients, and increased efficacy of dosage forms for enhanced health benefits [9]. Arishta and Asava formulations represent the distinct herbal fermentation products have been identified previously based on their composition and therapeutic uses [10, 11].
Furthermore, they are used to treat a plethora of disease conditions in pediatrics, systemic diseases affecting the central nervous system, circulatory system, respiratory system, digestive system, urinary system, reproductive systems, immune disorders, skin diseases, poisonous insect and snake bites, and alcoholism together with commonly encountered illnesses [11, 12]. Among the Arishta and Asava, Chandanasava is the most used medicine composed of 24 different polyherbal components and prescribed to treat gastrointestinal diseases, urinary disorders, spermatorrhea, gonorrhea, and autoimmune disorders as well as a diuretic appetizer, and has a cooling effect throughout the body [10, 11]. It is based on classical Ayurvedic text, namely, Bhaishajya Ratnavali in Sanskrit, with the known composition [11, 13] (Supplementary table S1). Singular composition rather than the combinatorial formulation of Arishta/Asava shows a wide variety of pharmacological effects rendering significant medicinal attributes for advantageous applications [14, 15]. The bioactivity is likely to be much more than the therapeutic effects described in Ayurvedic traditional knowledge due to the presence of a wide range of phytochemicals. Ayurvedic medicaments balance the tridoshas in the body and hence cure multiple diseases simultaneously. The enormity of traditional Ayurvedic formulations dates back to the ages for confronting the ancient and rich knowledge of Charaka Samhita in authenticity and authoritative medical applications of Indian origin [16]. Further ample literature is affirmative that traditional Ayurvedic medicines are included in alternative medicinal realms based on Ashtangahrudyam and Bhaishajya Ratnavali [17, 18]. Moreover, therapeutic potentials of phytochemical Ayurvedic secondary metabolites have been included in the clinical trial literature and proved efficacious [19]. Nevertheless, natural product chemistry and drug discovery research are more inclined towards big data analytics for envisaging therapeutic roles in confirmed health augmentation and disease alleviation [20]. Hence, bioinformatics tools and computational biology platforms are largely resourced as effective tools for medicinal plant research in drug discovery, development, and deeper insights [21]. Databases for screening dietary supplements and plant metabolites were emphasized for rational applications in phytomedicine [22]. Further health implications based on phytochemicals of plant origin were directed for advantageous applications in the arena of computational informatics [23]. In recent times, the network pharmacology approach has been used to examine the underlying mechanisms of TIM and TCM in order to effectively investigate the therapeutic efficacy using curated biological databases [24, 25]. In view of these, the current study is aimed to investigate the phytochemicals from an Indian fermented traditional medicine, Chandanasava, to treat chronic kidney and cardiovascular diseases by network pharmacology-based approach.
Materials and Methods
Sample Collection
Ayurvedic polyherbal fermented traditional medicine (FTM), Chandanasava, was procured from Ashtanga Ayurvedics PVT, Limited, Tiruchirapalli, Tamil Nadu, India.
Solvent Extraction
Hexane and ethylacetate solvents were employed for Chandanasava in a liquid–liquid separation technique with minor modifications. A sample of 5 mL of Chandanasava and 100 mL of solvents were mixed in a 500-mL separating funnel and shaken well steadily for 15 min. After 5 min, the solvent phase was detached. The solvent phase was then harvested, and these steps were repeated two times using the same sample. Sodium thiosulphate (anhydrous) was added to the mixture extracts to eliminate moisture levels and condensed with a rotary concentrator (BUCHI R- 210, Buchi India Pvt Ltd), then purged with nitrogen gas till 1 mL was obtained.
Gas Chromatography-Mass Spectrometry (GC–MS) Analysis of Ayurvedic FTM
Perkin Elmer Clarus 500 (CT, USA) instrument with a flame ionization detector with a capillary column (30 m length × 0.25 mm ID) coated with 5% phenyl 95% dimethylpolysiloxane with a film thickness of 0.25 μm was used for GC–MS analysis. The carrier gas was helium with a flow rate of 1 mL/min and the injection port was maintained at 280 °C and 1 μL of the sample was injected. The initial temperature of the column oven was 60 °C, ramped to 300 °C at a rate of 10°Cmin−1. In mass spectrometry, the full scan mode and 40–450 Daltons scan range were optimized for spectral data collection. The National Institute of Standards and Technology library was utilized to cross-match the obtained peaks with the standard.
Screening of Chemical Components from Biological Databases
Traditional Chinese Medicine Systems Pharmacology and Analysis Platform (TCMSP) were used to profile the phytoconstituents in Chandanasava. The respective constituents were identified using the GC–MS analysis and compounds were screened using the database [26]. Chandanasava’s phytoactive constituents were screened for oral bioavailability (OB) (> 30%) and drug-likeness (DL) (0:18) for assimilatory profiles. Absorption, distribution, metabolism, and excretion (ADME) properties of medicines and their oral administration in the bloodstream correspond to oral bioavailability [27]. The Pub Chem (https://pubchem.ncbi.nlm.nih.gov/) and Drug Bank (https://www.drugbank.ca/drugs) were used to obtain chemical information on the constituents, including their molecular formula and gene codes.
Screening of Phytochemicals and Diseases-Related Target Genes
DisGeNET and GeneCards database systems were used to acquire target genes information correlated to CKD with cardiovascular complications [28]. These databases were searched using the keywords “chronic kidney diseases” and “cardiovascular diseases” to identify the targeted disease and related genes.
Protein–Protein Interaction (PPI) Network Construction Based on Drug-Protein Interaction
A rough and basic interaction involving target genes for relevant bioactive metabolites in Chandanasava was built using the STRING version 11.0 to gather knowledge about the PPI network [29]. To validate the accuracy of our study, the species chosen is “Homo sapiens,” and the protein interaction is computed to a 70% similarity (0.700) high confidence level. The identified genes associated with the target diseases were cross-verified with the STITCH v5.0 server [30]. Cytoscape 3.8.0 software was used to build and validate the final PPI network based on the draft network data [31]. The network analyzer module in the Cytoscape is utilized for the network validation [32]. Cytohubba module in Cytoscape was used for profiling the disease hub genes associated with the disease targets [33].
Gene Ontology (GO) and KEGG Pathway Enrichment Analysis
Polyherbal Ayurvedic FTM Chandanasava components for target genes of CKD and CVD genes and appropriate for gene function and signaling cascades were obtained from the DAVID database system GO functional annotation, and KEGG pathway enrichment for deriving the biological process (BP), cellular components (CC), and molecular function (MF) of proteins used was analyzed [34].
Target Protein Pathway Network Construction
Enriched pathway associated with target diseased genes was further imported into the Cytoscape to derive an “Ingredient-Target-Pathway.” The network interconnections of Chandanasava constituents in the target protein pathway were built using nodes corresponding to diseases, targets, and associated pathways. The edges were elaborated on the connections between the nodes. A network model map for Chandanasava components and target genes for chronic renal and cardiovascular disease has subsequently arrived for a preliminary theoretical assessment of targeted medications.
Molecular Docking Analysis
Data Bank (https://www.rcsb.org/) and Drug Bank (a familiarity foot of pharmaceutical library) were used to obtain the tertiary structures of the top-hit hub proteins and generated secondary metabolites. The protein structures were prepared by removing hydrogen from the receptor and subtracting water molecules. Flexible docking with AUTODOCK VINA was used to study the molecular interaction between the top-hit hub proteins and ligands and binding sites were automatically detected [35]. The LigPlot+ software was used to identify the molecular interaction in a 2-dimensional view [36]. Finally, hydrogen bonds, hydrophobic interactions, and binding scores of the docked complex were noted.
Results
GC–MS Profiling of Chandanasava
The hexane and ethyl acetate fractions of the Chandanasava formulation were analyzed using gas chromatography-mass spectrometry. As illustrated in the overlay plot (Fig. 1A and B), the GC–MS spectra indicated the presence of a broad set of secondary metabolites that differ in retention times, molecular formulae, and peak areas. The total ion chromatogram of the Chandanasava formulation revealed that most of the compounds had a similar type of metabolic profile, while others exhibited variance (Fig. 1A and B). The peaks were integrated and correlated to the spectra databases available in the GC-MS libraries (NIST and Wiley library). In Chandanasava formulations, a total of 62 secondary metabolites were identified using GC–MS. Heterocyclic compounds, hydrocarbons, esters, acids, amines, halides, ethers, and aldehydes were present in the Chandanasava formulation.
Screening of Targets of Phytoconstituents from Chandanasava
The identified 61 compounds were searched by chemical name strategy using the TCMSP database to screen bioactive components in Chandanasava. The potential and pharmacologically effective phytochemicals were screened with the value of ≥ 30% OB and ≥ 0:18 DL (Table 1). The phytochemical compounds of the canonical SMILES are represented in Table 2. In a total of 61 compounds, 16 (MOL004067, MOL003353, MOL005028, MOL008670, MOL001573, MOL008712, MOL001230, MOL012364, MOL005117, MOL002139, MOL001212, MOL002092, MOL007525, MOL004791, MOL001212, and MOL001815) were eliminated due to the lack of related diseases and target proteins involved in CKD and CVD. After eliminating overlaps from 418 target genes, a total of 135 target genes for CKD and CVD were identified (Supplementary Table S2). Cytoscape 3.8.0 software view of the interaction of the 45 bioactive Chandanasava metabolites with their respective target genes was represented (Fig. 2). The analysis of component-target network consisted of 180 clusters and 418 edges. The red diamond clusters corresponded to the 45 phytocompounds, while the 7 yellow and 15 blue circle clusters corresponded to chronic kidney disease and cardiovascular disease, respectively. Moreover, 20 pink circle nodes represented both common genes of chronic kidney and CVD. The remaining 93 green circle nodes are attributed to the other target-related genes of the bioactive compounds. Eugenol, stigmasterol, isonipecotic acid, 1-methyl-4-phenyl-, ethyl ester, piperine, elemicin, 1,2-benzenedicarboxylic acid, dibutyl ester, and 5-hydroxymethylfurfural were found to have a strong interaction with multiple target genes among the 45 metabolites screened from Chandanasava. The results indicated that these active metabolites were the key components in the network which were attributed to the treatment of CKD and CVD.
Interaction network of Chandanasava ingredients with target diseases. Note: The red diamond nodes represent the 45 compounds, 7 yellow circle nodes represent the genes of chronic kidney diseases, 15 blue circle nodes represent the genes of cardiovascular diseases, 20 pink circle nodes represent the genes involved in both chronic kidney and cardiovascular diseases, and the remaining 93 green circle nodes represent the other related target corresponding genes of the compounds
Screening of Common Targets in Chandanasava for CKD and CVD
The common and corresponding targets for 27 CKD- and 35 CVD-related genes were obtained from the DisGeNET and GeneCards databases and were represented in the Venn diagram (Fig. 3A and B). The data output about these disease target genes obtained from DisGeNET and GeneCards was given (Supplementary Tables S3 and S4). The CKD- and CVD-associated genes interaction with 42 potential target genes obtained from Chandanasava components are represented in Table 3.
Venn diagram for the comparison of target receptors (42 genes) with Chandanasava ingredients retrieved from GeneCards and DisGeNET databases: Genes associated with chronic kidney diseases (A) and cardiovascular disease (B). The enriched protein–protein interaction network analysis of genes encoding target receptors of chronic kidney disease (C) and cardiovascular disease (D). The enrichment of p-value is p < 1.0e -16
Construction and Evaluation of Target Genes PPI Network
The STRING database was used to analyze selected CKD-associated target genes [28] and CVD-associated target genes [37], which were shown as an interaction network with a high confidence score of 0.700. For CKD, the network of PPI interactions between target genes was constructed using 26 clusters, 180 edges, and an average node degree of 13.8. PPI of CVD target genes, a total of 33 clusters and 191 edges, and an intermediate node degree of 11.6 were acquired, representing the target genes. Target genes involved in CKD: DRD1, DRD2, IL2, F10, CASP3, CREB1, and AHSA1 are shown (Fig. 3C), whereas CVD have a gene cluster as ADH1C, ADRA2A, SLC6A2, LTA4H, MAOA, ADRB1, SCN5A, ADRA1A, MMP8, PDE3A, DPEP1, AR, NFKBIA, MMP13, and KCNMA1 (Fig. 3D). The target gene functional network of 42 potential target genes in Chandanasava ingredients is depicted (Fig. 4). The evaluation of the protein–ligand interaction with 82 nodes and 149 edges resulted in the appropriate network. The red diamond nodes indicate 45 Chandanasava bioactive components, the yellow circle nodes denote 7 target proteins of CKD, and 15 blue circles show CVD. Moreover, the 20 pink circle nodes exhibit common genes of CKD and CVD.
Target protein interaction network of 40 potential target compounds in Chandanasava for the treatment of chronic kidney and cardiovascular diseases. Note: Red diamond represents interacted compounds, yellow and blue circle represent chronic kidney disease and cardiovascular disease respectively. The pink circle indicates genes involved in both diseases
GO Enrichment Analysis
DAVID server was utilized to perform the GO enrichment analysis against the disease-associated target genes. As illustrated in Fig. 5, a p-value (p < 0.05) was used to demarcate the best 20 significantly enriched terms in the BP and MF criteria. These findings revealed that these CKD and CVD target genes are involved in the molecular regulation of various biological processes. Totally, 189 BP primarily were attributed to significant functions for positive regulation of cellular transcription in the formation of RNA polymerase II promoter that negatively regulates the drug cell proliferation, inflammatory response, ERK1 and ERK2 cascade positive regulation, transcription factor positive regulatory activity, nitric oxide biosynthetic process positive regulation, lipopolysaccharide-mediated signaling pathway, and response to hypoxia along with the many other genes involved in biological processes. Among the 33 MF, the respective protein targets were binding with enzyme, norepinephrine, epinephrine interleukin-1 receptor, dopamine, protease, cytokine activity, protein homodimerization activity, binding, and serine-type endopeptidase activity that are compiled for molecular functioning genes.
KEGG Pathway Enrichment Analysis
Potential targets of Chandanasava compounds correlated to disease, including CKD and CVD, were identified using the KEGG pathway module. KEGG pathway analyses of protein targets and pathway-target interaction networks were represented (Fig. 6). According to the study, the Chandanasava metabolites and target proteins network have 64 clusters and 243 edges. Appropriate p-values with < 0.05 correspond to 35 pathways for 29 potentially target genes screened with BH. These results exhibited that the target genes were primarily involved in TNF signaling, cGMP-PKG signaling, Toll-like receptor signaling, MAPK signaling, Adrenergic signaling in cardiomyocytes, cAMP signaling, NF-kappa B signaling, MAPK signaling, Renin secretion, T cell receptor signaling pathway, and so on. The target proteins involved in the TNF signaling pathway (TNF) were CCL2, FOS, JUN, NFKBIA, CREB1, CASP3, ICAM1, IL1B, IL6, MAPK14, PTGS2, and TNF; the cAMP signaling pathway interacted with FOS, JUN, NFKBIA, ADRB1, ADRB2, CREB1, DRD1, DRD2, and PDE3A; the protein targets involved in the cGMP-PKG signaling pathway such as ADRA1A, ADRA2A, ADRB1, ADRB2, CREB1, NOS3, PDE3A, and KCNMA1. The target proteins involved in Toll-like receptor signaling pathway were FOS, JUN, NFKBIA, IL1B, IL6, MAPK14, TLR4, and TNF; MAPK signaling pathway mainly interacted with the target proteins including FOS, JUN, CASP3, IL1A, IL1B, MAPK14, and TNF; NF-kappa B signaling pathway primarily consisted of NFKBIA, ICAM1, IL1B, PLAU, PTGS2, TLR4, and TNF; the protein targets in Adrenergic signaling in cardiomyocytes such as ADRA1A, ADRB1, ADRB2, CREB1, MAPK14, and SCN5A; T cell receptor signaling pathway of target proteins involved in FOS, JUN, NFKBIA, IL2, MAPK14, and TNF; Renin secretion target proteins consisted of ADRB1, ADRB2, CREB1, PDE3A, KCNMA1, and REN. NOD-like receptor signaling pathway mainly networked with CCL2, NFKBIA, IL1B, IL6, MAPK14, and TNF, the target proteins involved in Estrogen signaling pathways such as FOS, JUN, CREB1, ESR1, and NOS3. Multiple target genes could be found in a single pathway at any given time, and a single specific target gene can be found in various pathways. Analysis proves that a single pathway involving numerous protein targets is more significant than a single protein target interacting with multiple pathways. This is due to the fact that the impact of a single-target protein on the entire pathway may be minimal, whereas many target protein interactions can have a significant effect. The main target proteins are TNF, IL1B, IL6, JUN, FOS, NFKB1A, TLR4, MAPK14, CREB1, IL1A, CASP3, CCL2, IL2, and ICAM1. They were highly interacted/involved in these pathways and can be considered potential targets to treat various diseases. From the above-categorized results, the effective bioactive ingredients of polyherbal fermented medicine, Chandanasava, shows insight into potential target proteins in treating inflammation, chronic inflammation conditions, such as kidney-related diseases, cardiac diseases, rheumatoid arthritis, type 2 diabetes, bacterial and viral infections, boosting immunity, and other diseases.
Identification of Hub Genes Associated with Targeted Diseases
Hub genes are the essential genes that control and express all associated sub-proteins to perform their molecular and biological functions whenever required [25, 38]. Three hub genes from the top-hit ranking are associated with the target diseased gene network. Such genes are tumor necrosis factor (TNF, PDB: 2E7A:A) in rank 1 and interleukin-6 (IL6) and prostaglandin G/H synthase 2 (PTGS2) (PDB: 4CNI:C, 5F19:A) from ranks 2 and 3 (Fig. 7). Based on the DisGeNET and GeneCards databases search, 21 compounds have the best drug-likeness interacting properties against the three hub proteins. Such interactions are TNF (1 compound), IL6 (2 compounds), and PTGS2 (19 compounds). Therefore, these 21 compounds were further utilized for the molecular docking experiments with the three hub proteins.
Performance of Molecular Docking Studies
Piperine shows the best interaction with TNF and IL6 proteins (Fig. 8, Table 4). The binding score was confirmed as -7.08 for TNF. Ten hydrophobic and one hydrogen bonding interactions were found in Asn46 with a bonding distance of 2.55 Å. IL6 shows six hydrophobic, one hydrogen bonding interactions at Glu80 (2.54 Å), with a binding score of -5.47. The receptor protein PTGS2 against melatonin illustrates 11 hydrophobic and three hydrogen bonding interactions at Gly13 (2.62 Å) and Arg438 (3.12 Å, 2.50 Å) with the best binding score of -10.5. Among the two compounds, melatonin acts as a potential inhibitor for cardiovascular and chronic kidney disease. Overall, three compounds showed the best hydrogen bonding interaction and binding score out of 21 selected compounds.
Discussion
Ayurvedic pharmacopeia includes fermented traditional medicines (FTM) as described earlier for the effective polyherbal formulations that have been fermented by self-generated/native microbes [14]. Arishta and Asava are traditionally valuable therapeutic Ayurvedic formulations due to their superior storage efficacy, improved pharmacological value, improved drug molecule extraction from herbs, and efficacy of drug transport in the body [10, 11]. The phytocompounds of Chandanasava showed activity against arthritis using molecular docking and dynamic analysis [39]. Previous reports suggested that Chandanasava scavenges free radicals by the presence of novel biotransformed phytochemicals [40].
In this study, 61 bioactive metabolites in polyherbal fermented traditional medicine Chandanasava were identified using GC–MS metabolomics analysis. Among those, 40 potential phytochemicals were screened by TCMSP based on ADME properties. These potential compounds were subjected to a network pharmacology approach to treat CKD and CVD. The network chart was developed by 42 potential target proteins mined from different databases. Among the 40 active ingredients, eugenol < methoxy- > , stigmasterol, isonipecotic acid, 1-methyl-4-phenyl-, ethyl ester, piperine, elemicin, 5-hydroxymethylfurfural and 1,2-benzenedicarboxylic acid, and dibutyl ester were catalogued. Necessitated activities can corroborate the enhanced use in the treatment of CKD with cardiovascular complications. A single Chandanasava component may regulate numerous target proteins, while multiple components may regulate a single-target protein. Therefore, multi-target active compounds have more significant therapeutic potential and lesser adverse effects than single-target active compounds. This present assessment is the first report of a single component effect on target proteins in FTM network assessment. A total of 29 potentially target genes were primarily involved in TNF signaling, cGMP-PKG signaling, Toll-like receptor signaling, MAPK signaling, Adrenergic signaling in cardiomyocytes, cAMP signaling, NF-kappa B signaling, MAPK signaling, Renin secretion, and T cell receptor signaling pathway associated with the respective diseases based on GO and KEGG analysis. Based on a system pharmacology study, such bioactive components possess therapeutic potential on the inflammatory response, kidney, and cardiovascular disease–related health conditions. They can cure or prevent inflammatory diseases, kidney, and CVD complications.
Furthermore, the TNF signaling cascade can activate various intracellular signaling pathways such as transcription factor NF-kappa B, apoptosis, cell survival, inflammation, and immunity [41]. Overexpression of TNFR1 (major receptor) can activate p38MAPK in response to external or internal stimuli, boosts IL-6 production and triggers the inflammatory response [42]. TNFR2 agonistic reactions are expressed in cells only upon health limitations and cause therapeutic implications based on signaling cascades involving endothelial cells, CD4 and CD8 T lymphocytes, oligodendrocytes, neuron subtypes, microglia, cardiac myocytes, thymocytes, etc. [43]. Many genes are activated by TNFR1 signaling, which is principally regulated by the NF-kappa B pathway that subsequently activates the MAPK cascade resulting in necroptosis or apoptosis and necroptosis [41]. On the other hand, TNFR2 signaling leads to survival via activating the NF-kappa B pathway, including the PI3K-dependent NF-kappa B pathway and the JNK pathway leading to cell death [44]. TNF signaling cascade regulates the expression of genes such as NFKBIA, CREB1, CASP3, ICAM1, IL1B, IL6, MAPK14, PTGS2, and TNF in many inflammatory diseases, including atherosclerosis, diabetics, and chronic kidney diseases affecting the inflammatory cascades [45]. Furthermore, danshen-shanzha decoction can interact and result in modulation of 41 potential targets and 16 signaling pathways correlated with metabolizing lipids that prevent endothelial dysfunction promoting cardiovascular protection against atherosclerosis [46]. MAPK14 (mitogen-activated protein kinase 14) represents the pivotal signal transducing component in proinflammatory cytokines, chemokines, and adhesion factors responsible for signaling from the cell membrane to the nucleus and responsible for intracellular responses and atherosclerosis [47].
The TCM Yangxinshi tablet was proven efficient for abating cardiovascular complications and enhancing immune power during heart failure [48]. Similarly, QiShenYiQi, Shenmai and Xuesaitong have been used to treat myocardial infarction and myocardial ischemia by promoting anti-apoptosis, anti-inflammation, antioxidant, and angiogenesis using animal models [49,50,51]. Furthermore, Buchang Naoxintong, Fufang Danshen formula have been traditionally used to treat CVD and stroke by regulating the corresponding inflammatory markers using literature and multi-compound target disease network [52]. In Indian traditional knowledge, Arjunarishta is cardiotonic; it rejuvenates and boosts the cardiovascular system by accelerating the blood flow in coronary arteries and controlling blood cholesterol levels and myocardial protection against ischemic damage [11]. There is substantial experimental evidence that it is beneficial in preventing cardiovascular disease alone or in combination with statins [53, 54]. Dashamoolarishta exhibited several therapeutics for anti-inflammation, analgesic, and anti-platelet properties effects by the animal model compared with standard drug aspirin [55]. Chronic kidney disease is thought to be caused by an immune response. It has a strong correlation with blood coagulation. MAPK14, NFKB1, cAMP, TLR4, TNF, IL6, TCR (CD28), and JUN are closely associated with inflammation, ECM, hypoxia, angiogenesis, and immune response. Previous studies reported that the TCM NE-THCQ exhibited anti-renal fibrosis activity by suppressing ECM deposition, decreasing inflammation, and regulating hypoxia through mechanistic signaling pathways [56]. Bu-shen-Huo-xue formula, a similar TCM, has been used to regulate coagulation and fibrinolytic balance to treat chronic kidney disease expression of the inflammatory marker using multi-target multi-components system pharmacology study [57]. A previous report demonstrated that Astragalus has medicinal properties in patients with diabetes, improving renal function [58]. Among the 29 target proteins, 13 (TNF, IL1B, IL6, JUN, FOS, NFKB1A, TLR4, MAPK14, CREB1, IL1A, CASP3, CCL2, IL2, and ICAM1) were highly involved in various pathways. The predicted PPINs were functionally validated based on gene ontology terms, experimentally determined interaction score (edges), and bonding interactions [59, 60]. Moreover, several recent experimental and molecular dynamic simulation studies were conducted for piperine and melatonin among selected hub proteins (TNF, IL6, and PTGS2), which show good interaction with each other [61,62,63]. Thus, the findings are functionally validated and associated with previous research.
The potential target proteins stimulate overexpression of cytokine levels, apoptosis, immune response, and inflammatory markers leading to chronic inflammation-associated diseases such as type 2 diabetes, CVD, chronic kidney failure, rheumatoid arthritis, insulin resistance, and cancer. Based on the analysis by network pharmacology, those bioactive ingredients regulate or alleviate signal pathways that have therapeutic effects on inflammation and kidney and cardiac diseases–related symptoms. Such compounds can treat or alleviate the symptoms of inflammation and kidney and cardiac diseases through the role of potentially interacted target proteins in metabolic pathways caused by the occurrence of diseases. The molecular docking analysis demonstrates that the compounds piperine and melatonin act as potent inhibitors for CKD and CVD. Furthermore, the compounds piperine and melatonin also exhibited antibiofilm activity, indicating evidence for arresting urinary tract infections that can complicate the CKD incidence and aggravation. Similarly, docking piperine with cyclin-dependent kinases is effective against oral cancer [37]. Moreover, the small molecule has been proven effective in controlling the COVID-19 pandemic [64]. Furthermore, melatonin has been confirmed for renal management during chronotherapy by targeting the renin-angiotensin system (RAS) through intra-renal targeting [65]. Hence, the small molecule interaction with the protein targets is affirmative of protective roles in chronic kidney disease, thereby could be indirectly attributed to managing cardiovascular implications through signaling cascades. However, further protein interaction crosstalk will effectively affirm the Chandanasava effects in infectious disease management. Hence, chronic kidney disease and cardiovascular complications in the perspectives of the FTM are addressed. Thus, the conceptualization of disease Vs disorder management for efficient clinical outcomes and mortality mitigation are attributed to FTM.
Conclusion
Bioactive potentials of phytomedicinal herbs such as Chandanasava in the arena of FTM are constituted of multiple active components. Still, the functional properties of disease management have yet to be revealed. Mechanisms of action for combating the versatile arresting modes require more molecular dissection modalities with interdisciplinary research. This analysis demonstrates that the identified compounds, piperine and melatonin from Chandanasava, have protective potentials to inhibit biofilm formation of infectious diseases involved in CKD associated with CVD as affirmative from comprehensive network analysis coupled with docking perspectives. The study indicates the scope of validating the claims of the traditional Ayurvedic medicines using the modern tools of biology, particularly FTM, which are least understood. Such approaches could yield new avenues and drug molecules. The study also highlighted that the multi-target active compounds have better therapeutic and low adverse effects than the single-target active compounds. It also demonstrates that a single phytochemical compound has the potential to interact with multiple cellular targets and is likely to be a therapeutic measure for simultaneously treating multiple disorders or syndromes. However, further experimental validation, such as in vitro and in vivo analysis, is warranted for better understanding leading to drug development.
Data Availability
All datasets generated for this study are included in the article/Supplementary Material.
References
Baigent, C., Burbury, K., & Wheeler, D. (2000). Premature cardiovascular disease in chronic renal failure. The Lancet, 356, 147–152.
Anavekar, N. S., McMurray, J. J., Velazquez, E. J., Solomon, S. D., Kober, L., Rouleau, J.-L., White, H. D., Nordlander, R., Maggioni, A., & Dickstein, K. (2004). Relation between renal dysfunction and cardiovascular outcomes after myocardial infarction. New England Journal of Medicine, 351, 1285–1295.
Smith, G. L., Lichtman, J. H., Bracken, M. B., Shlipak, M. G., Phillips, C. O., DiCapua, P., & Krumholz, H. M. (2006). Renal impairment and outcomes in heart failure: Systematic review and meta-analysis. Journal of the American College of Cardiology, 47, 1987–1996.
Brosius, F. C., III., Hostetter, T. H., Kelepouris, E., Mitsnefes, M. M., Moe, S. M., Moore, M. A., Pennathur, S., Smith, G. L., & Wilson, P. W. (2006). Detection of chronic kidney disease in patients with or at increased risk of cardiovascular disease: A science advisory from the American Heart Association Kidney And Cardiovascular Disease Council; the Councils on High Blood Pressure Research, Cardiovascular Disease in the Young, and Epidemiology and Prevention; and the Quality of Care and Outcomes Research Interdisciplinary Working Group: Developed in collaboration with the National Kidney Foundation. Circulation, 114, 1083–1087.
Hallan, S., Astor, B., Romundstad, S., Aasarød, K., Kvenild, K., & Coresh, J. (2007). Association of kidney function and albuminuria with cardiovascular mortality in older vs younger individuals: The HUNT II Study. Archives of Internal Medicine, 167, 2490–2496.
Van Biesen, W., De Bacquer, D., Verbeke, F., Delanghe, J., Lameire, N., & Vanholder, R. (2007). The glomerular filtration rate in an apparently healthy population and its relation with cardiovascular mortality during 10 years. European Heart Journal, 28, 478–483.
Wan, E. Y. F., Chin, W. Y., Yu, E. Y. T., Wong, I. C. K., Chan, E. W. Y., Li, S. X., Cheung, N. K. L., Wang, Y., & Lam, C. L. K. (2020). The impact of cardiovascular disease and chronic kidney disease on life expectancy and direct medical cost in a 10-year diabetes cohort study. Diabetes Care, 43, 1750–1758.
Golechha, M. (2020). Time to realise the true potential of Ayurveda against COVID-19. Brain, behavior, and immunity, 87, 130.
Maithani, M., Grover, H., Raturi, R., Gupta, V., & Bansal, P. (2019). Ethanol content in traditionally fermented ayurvedic formulations: Compromised good manufacturing practice regulations–compromised health. The American journal of drug and alcohol abuse, 45, 208–216.
Sekar, S., & Mariappan, S. (2008) Traditionally fermented biomedicines, arishtas and asavas from Ayurveda. Indian Journal of Traditional Knowledge, 7, 548–556.
Sekar, S., & Mariappan, S. (2010) Fermented medicines of Ayurveda: A treatise. ed. LAP LAMBERT Academic Publishing AG & Co. KG, Germany.
Mishra, A., Gupta, A., Gupta, V., Sannd, R., & Bansal, P. (2010). Asava and aristha: An ayurvedic medicine–An overview. International Journal of Pharmaceutical and Biological Archive, 1, 24–30.
Mita, N. (1930) Bhaishajya Ratnavali (Sanskrit). Lahore: Motilal Banarasi Dass. ed. The Punjab Sanskrit Depot
Sekar, S., & Vinothkanna, A. (2019). Polyherbal and submerge fermented medicines of Ayurveda: Convergence of tradition with scientific trends and needs. South African Journal of Botany, 121, 410–417.
Vinothkanna, A., Sathiyanarayanan, G., Balaji, P., Mathivanan, K., Pugazhendhi, A., Ma, Y., Sekar, S., & Thirumurugan, R. (2021). Structural characterization, functional and biological activities of an exopolysaccharide produced by probiotic Bacillus licheniformis AG-06 from Indian polyherbal fermented traditional medicine. International Journal of Biological Macromolecules, 174, 144–152.
Bhavana, K., & Shreevathsa, M. (2014) Medical geography in Charaka Samhita. Ayu, 35, 371–377.
Chaudhary, A., Singh, N., Dalvi, M., & Wele, A. (2011). A progressive review of Sandhana kalpana (Biomedical fermentation): An advanced innovative dosage form of Ayurveda. Ayu, 32, 408.
Prajapati, S. (2015). Therapeutic potential of Yashtimadhu (Glycyrrhiza glabra Linn.) in Bruhat-Trayi and Laghu-Trayi-A review. Research & Reviews: A Journal of Ayurvedic Science, Yoga and Naturopathy, 2, 26–33.
Wink, M. (2015). Modes of action of herbal medicines and plant secondary metabolites. Medicines, 2, 251–286.
Atanasov, A. G., Zotchev, S. B., Dirsch, V. M., & Supuran, C. T. (2021). Natural products in drug discovery: Advances and opportunities. Nature reviews Drug discovery, 20, 200–216.
Sharma, V., & Sarkar, I. N. (2013). Bioinformatics opportunities for identification and study of medicinal plants. Briefings in bioinformatics, 14, 238–250.
Durazzo, A., D’Addezio, L., Camilli, E., Piccinelli, R., Turrini, A., Marletta, L., Marconi, S., Lucarini, M., Lisciani, S., & Gabrielli, P. (2018). From plant compounds to botanicals and back: A current snapshot. Molecules, 23, 1844.
Scalbert, A., Andres-Lacueva, C., Arita, M., Kroon, P., Manach, C., Urpi-Sarda, M., & Wishart, D. (2011). Databases on food phytochemicals and their health-promoting effects. Journal of agricultural and food chemistry, 59, 4331–4348.
Lakshmanan, D. K., Murugesan, S., Rajendran, S., Ravichandran, G., Elangovan, A., Raju, K., Prathiviraj, R., Pandiyan, R., & Thilagar, S. (2021) Brassica juncea (L.) Czern. leaves alleviate adjuvant-induced rheumatoid arthritis in rats via modulating the finest disease targets-IL2RA, IL18 and VEGFA. Journal of Biomolecular Structure and Dynamics, 40, 8155–8168.
Sivakumar, T. R., Surendhiran, D., Chen, K., Lv, P., Vinothkanna, A., Prathiviraj, R., Sethupathy, S., & Sirajunnisa, A. R. (2021). Network pharmacology based analysis of Astragalus propinquus components for the treatment of rheumatoid arthritis and diabetes. South African Journal of Botany, 139, 92–105.
Ru, J., Li, P., Wang, J., Zhou, W., Li, B., Huang, C., Li, P., Guo, Z., Tao, W., & Yang, Y. (2014). TCMSP: A database of systems pharmacology for drug discovery from herbal medicines. Journal of cheminformatics, 6, 1–6.
Ge, Q., Chen, L., Yuan, Y., Liu, L., Feng, F., Lv, P., Ma, S., Chen, K., & Yao, Q. (2020). Network pharmacology-based dissection of the anti-diabetic mechanism of Lobelia chinensis. Frontiers in Pharmacology, 11, 347.
Mou, X., Zhou, D., Liu, K., Chen, L. J., & Liu, W. H. (2020). A bioinformatics and network pharmacology approach to the mechanisms of action of Shenxiao decoction for the treatment of diabetic nephropathy. Phytomedicine, 69, 153192.
Szklarczyk, D., Gable, A. L., Lyon, D., Junge, A., Wyder, S., Huerta-Cepas, J., Simonovic, M., Doncheva, N. T., Morris, J. H., & Bork, P. (2019). STRING v11: Protein–protein association networks with increased coverage, supporting functional discovery in genome-wide experimental datasets. Nucleic acids research, 47, D607–D613.
Kuhn, M., von Mering, C., Campillos, M., Jensen, L. J., & Bork, P. (2007). STITCH: Interaction networks of chemicals and proteins. Nucleic acids research, 36, D684–D688.
Doncheva, N. T., Morris, J. H., Gorodkin, J., & Jensen, L. J. (2018). Cytoscape StringApp: Network analysis and visualization of proteomics data. Journal of proteome research, 18, 623–632.
Su, G., Morris, J. H., Demchak, B., & Bader, G. D. (2014). Biological network exploration with Cytoscape 3. Current protocols in bioinformatics, 47(8.13), 11-18.13.24.
Chin, C.-H., Chen, S.-H., Wu, H.-H., Ho, C.-W., Ko, M.-T., & Lin, C.-Y. (2014). cytoHubba: Identifying hub objects and sub-networks from complex interactome. BMC systems biology, 8, 1–7.
Dennis, G., Sherman, B. T., Hosack, D. A., Yang, J., Gao, W., Lane, H. C., & Lempicki, R. A. (2003). DAVID: Database for annotation, visualization, and integrated discovery. Genome biology, 4, 1–11.
Trott, O., & Olson, A. J. (2010). AutoDock Vina: Improving the speed and accuracy of docking with a new scoring function, efficient optimization, and multithreading. Journal of computational chemistry, 31, 455–461.
Wallace, A. C., Laskowski, R. A., & Thornton, J. M. (1995). LIGPLOT: A program to generate schematic diagrams of protein-ligand interactions. Protein engineering, design and selection, 8, 127–134.
Rekha, U. V., Anita, M., Govindaraj Jayamathi, K., Deepa, S., Hussain, S., Bhuvaneswari, J., Ramya, V., Selvaraj, J., & Naveenraj, N. (2020). Molecular docking analysis of piperine with CDK2, CDK4, Cyclin D and Cyclin T proteins. Bioinformation, 16, 359.
Prathiviraj, R., & Chellapandi, P. (2020). Modeling a global regulatory network of Methanothermobacter thermautotrophicus strain ∆H. Network Modeling Analysis in Health Informatics and Bioinformatics, 9, 1–15.
Vinothkanna, A., Karthikeyan, B. S., Vijayan, R., & Sekar, S. (2018). Assessment of anti-arthritic potential of traditionally fermented ayurvedic polyherbal product chandanasava by molecular modelling, docking and dynamics approaches. International Journal of Computational Biology and Drug Design, 11, 346–368.
Vinothkanna, A., & Sekar, S. (2018). Influence of intrinsic microbes on phytochemical changes and antioxidant activity of the Ayurvedic fermented medicines: Balarishta and Chandanasava. Ayu, 39, 169.
Hayden, M. S. and Ghosh, S. (2014) Regulation of NF-κB by TNF family cytokines. Seminars in immunology, pp. 253–266. Elsevier
Wojdasiewicz, P., Poniatowski, Ł. A., & Szukiewicz, D. (2014) The role of inflammatory and anti-inflammatory cytokines in the pathogenesis of osteoarthritis. Mediators of Inflammation, 2014, 1–19.
Yang, S., Wang, J., Brand, D. D., & Zheng, S. G. (2018). Role of TNF–TNF receptor 2 signal in regulatory T cells and its therapeutic implications. Frontiers in immunology, 9, 784.
Wajant, H., & Siegmund, D. (2019). TNFR1 and TNFR2 in the control of the life and death balance of macrophages. Frontiers in cell and developmental biology, 7, 91.
Kurokouchi, K., Kambe, F., Yasukawa, K., Izumi, R., Ishiguro, N., Iwata, H., & Seo, H. (1998). TNF-α increases expression of IL-6 and ICAM-1 genes through activation of NF-κB in osteoblast-like ROS17/2.8 cells. Journal of Bone and Mineral Research, 13, 1290–1299.
Zhang, J., Liang, R., Wang, L., & Yang, B. (2019). Effects and mechanisms of Danshen-Shanzha herb-pair for atherosclerosis treatment using network pharmacology and experimental pharmacology. Journal of ethnopharmacology, 229, 104–114.
Kyriakis, J. M., & Avruch, J. (2012). Mammalian MAPK signal transduction pathways activated by stress and inflammation: A 10-year update. Physiological reviews, 92, 689–737.
Chen, X., Sun, C., Laborda, P., Zhao, Y., Palmer, I., Fu, Z. Q., Qiu, J., & Liu, F. (2018). Melatonin treatment inhibits the growth of Xanthomonas oryzae pv. oryzae. Frontiers in Microbiology, 9, 2280.
Li, X., Wu, L., Liu, W., Jin, Y., Chen, Q., Wang, L., Fan, X., Li, Z., & Cheng, Y. (2014). A network pharmacology study of Chinese medicine QiShenYiQi to reveal its underlying multi-compound, multi-target, multi-pathway mode of action. PLoS ONE, 9, e95004.
Wang, L.-L., Zhao, X.-P., Zhao, Z.-Y., Fan, X.-H., & Li, Z. (2014) Network pharmacology study of mechanism on xuesaitong injection against retinal vein occlusion. China Journal of Chinese Materia Medica, 39, 2322–2325.
Wu, L., Wang, Y., Nie, J., Fan, X., & Cheng, Y. (2013) A network pharmacology approach to evaluating the efficacy of Chinese medicine using genome-wide transcriptional expression data. Evidence-Based Complementary and Alternative Medicine, 2013, 1–8.
Hao, D. C., & Xiao, P. G. (2014). Network pharmacology: A Rosetta stone for traditional C hinese medicine. Drug Development Research, 75, 299–312.
Dwivedi, S. (2007). Terminalia arjuna Wight & Arn.—A useful drug for cardiovascular disorders. Journal of Ethnopharmacology, 114, 114–129.
Rastogi, S., Pandey, M. M., & Rawat, A. (2016). Traditional herbs: A remedy for cardiovascular disorders. Phytomedicine, 23, 1082–1089.
Parekar, R. R., Bolegave, S. S., Marathe, P. A., & Rege, N. N. (2015). Experimental evaluation of analgesic, anti-inflammatory and anti-platelet potential of Dashamoola. Journal of Ayurveda and integrative medicine, 6, 11.
Zhou, Z., Chen, B., Chen, S., Lin, M., Chen, Y., Jin, S., Chen, W., & Zhang, Y. (2020) Applications of network pharmacology in traditional Chinese medicine research. Evidence-Based Complementary and Alternative Medicine, 2020, 1–7.
Shi, S.-H., Cai, Y.-P., Cai, X.-J., Zheng, X.-Y., Cao, D.-S., Ye, F.-Q., & Xiang, Z. (2014). A network pharmacology approach to understanding the mechanisms of action of traditional medicine: Bushenhuoxue formula for treatment of chronic kidney disease. PLoS ONE, 9, e89123.
Li, M., Wang, W., Xue, J., Gu, Y., & Lin, S. (2011). Meta-analysis of the clinical value of Astragalus membranaceus in diabetic nephropathy. Journal of ethnopharmacology, 133, 412–419.
Kumar, L. D., Prathiviraj, R., Selvakumar, M., Guna, R., Abbirami, E., & Sivasudha, T. (2020). HRLC-ESI-MS based identification of active small molecules from Cissus quadrangularis and likelihood of their action towards the primary targets of osteoarthritis. Journal of Molecular Structure, 1199, 127048.
Prathiviraj, R., Berchmans, S., & Chellapandi, P. (2019). Analysis of modularity in proteome-wide protein interaction networks of Methanothermobacter thermautotrophicus strain ΔH and metal-loving bacteria. Journal of Proteins and Proteomics, 10, 179–190.
Povinelli, A. P. R., Zazeri, G., Jones, A. M., & Cornélio, M. L. (2022). A computational–experimental investigation of the molecular mechanism of interleukin-6-piperine interaction. International Journal of Molecular Sciences, 23, 7994.
Suriagandhi, V., & Nachiappan, V. (2022) Therapeutic target analysis and molecular mechanism of melatonin-treated leptin resistance induced obesity: A Systematic Study of Network Pharmacology. Frontiers in Endocrinology, 13, 1–13.
Zhang, H., Wei, M., Sun, N., Wang, H., & Fan, H. (2022) Melatonin attenuates chronic stress-induced hippocampal inflammatory response and apoptosis by inhibiting ADAM17/TNF-α axis. Food Chemical Toxicology, 169, 1–14.
Rout, J., Swain, B. C., & Tripathy, U. (2020) In silico investigation of spice molecules as potent inhibitor of SARS-CoV-2. Journal of Biomolecular Structure and Dynamics, 40, 860–874.
Rahman, A., Hasan, A. U., & Kobori, H. (2019). Melatonin in chronic kidney disease: A promising chronotherapy targeting the intrarenal renin–angiotensin system. Hypertension Research, 42, 920–923.
Acknowledgements
The authors (AV and YM) acknowledge the “Foreign Scientist Talented Project” awarded by the Ministry of Science and Technology, China. The authors thank TN. Narayanan Varier and TR. Sasi Varier of Ashtanga Ayurvedics (P) Ltd., Tiruchirappalli, for the Ayurvedic medicine samples.
Author information
Authors and Affiliations
Contributions
A.V is the major contributor to this manuscript. A.V conducted the analysis, drafted the first version of the manuscript, and finalized the manuscript. A.V, R.P, and T.S collected the data and processed the graph and the table in the manuscript. Y.M and S.S conceptualized and supervised the investigation, as well as systematically evaluated the findings. The final manuscript was read and approved by all contributors.
Corresponding authors
Ethics declarations
Ethics Approval
Not applicable.
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Vinothkanna, A., Prathiviraj, R., Sivakumar, T.R. et al. GC–MS and Network Pharmacology Analysis of the Ayurvedic Fermented Medicine, Chandanasava, Against Chronic Kidney and Cardiovascular Diseases. Appl Biochem Biotechnol 195, 2803–2828 (2023). https://doi.org/10.1007/s12010-022-04242-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12010-022-04242-7