Opinion statement
Bladder dysfunction, which is commonly associated with neurologic disorders, can present in myriad ways, from complete retention of urine to total urinary incontinence. The multiple options for treating neurogenic bladder dysfunction range from minimally invasive lifestyle changes to major surgical interventions. Interventions may be driven by patient-reported nuisance or by medical necessity, as in the case of impaired compliance with associated upper urinary tract compromise. Pharmacologic treatment has long been the mainstay in the management of bladder dysfunction, particularly for overactive bladder symptoms [1]. While there are many different medications for overactive bladder dysfunction, most are in the category of antimuscarinics. Each medication has a slightly different side effect profile, which may be important in the drug selection process [2]. When these are not tolerated or are ineffective, beta agonists, phosphodiesterase inhibitors, tricyclic antidepressants, and the gamma aminobutyric acid (GABA)-B agonist baclofen can be added or substituted. For difficulty emptying, alpha adrenergic antagonists can be used [3]. Intravesical options are also available for overactive bladder (OAB) symptoms. The most common is botulinum toxin, which works by decreasing the activity of the detrusor smooth muscle, thereby decreasing OAB symptoms [4]. Percutaneous nerve stimulation may also be used [5•].
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
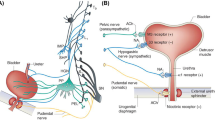
Normal bladder function involves two phases: storage and emptying. A normal functioning bladder must have adequate compliance to store urine without leakage or reflux as a result of elevated intravesical pressure. During the emptying stage, the bladder must contract and the urinary sphincter (made up of smooth and striated muscle) must synergistically relax to allow adequate urinary flow and complete bladder emptying. Bladder dysfunction results from a failure to properly store urine or to properly empty. The bladder is controlled by a complex neurologic network, including both autonomic (sympathetic and parasympathetic) and somatic innervation. All neuronal connections must work together to achieve proper urologic function. Neurologic diseases can affect both emptying and storage of urine. Bladder function can be impeded in demyelinating central nervous system diseases, such as multiple sclerosis, which can cause bladder overactivity and associated incontinence, as well as impaired emptying secondary to detrusor sphincter dyssynergia.
There are many considerations when treating patients with bladder dysfunction stemming from neurological disease, the first of which is to determine whether the patient primarily has overactive bladder dysfunction or emptying dysfunction. There are several lifestyle changes that can be made for both. For overactive bladder symptoms, reduction in caffeine and restriction of artificial sugars and alcohol have been found to be helpful [2]. It can also be helpful to have patients commit to timed voiding (voiding at specific intervals prior to the onset of urgency symptoms) and to keep a voiding diary [2]. For difficulty emptying, patients can be instructed to double-void (attempting to void again, with or without the use of Valsalva maneuver or direct bladder compression, following a normal volitional void). If retention of urine is not responsive to conservative options or if patients experience untoward effects from retained urine, they can also be taught to do intermittent self-catheterization.
Pharmacologic treatment is usually the second step in treatment of bladder dysfunction. For OAB, the major category of medications is the antimuscarinics, which differ from each other in central nervous system penetration that produces sedation and in other adverse effects (see below).
Surgical options include neurostimulation with sacral neuromodulation. In this procedure, a tined- lead electrode is implanted directly into the S3 foramen adjacent to the sacral nerve plexus and connected to a battery source, which then uses electrical stimulation to control frequency, urgency to void, and urge incontinence [1]. More permanent surgical options, including sphincterotomy for difficulty emptying, are rarely used due to their irreversible nature and risk for complications from surgery itself. As a last resort, bladder augmentation or urinary diversion surgery can be performed, but this is reserved for patients with poor bladder compliance and potential for damage to the upper urinary tract [3].
Treatment
Diet and lifestyle
For overactive bladder symptoms:
-
Caffeine restriction can decrease OAB symptoms
-
Restriction of artificial sugar/alcohol or other irritant can decrease symptoms.
-
Reduction of excessive fluid intake can decrease OAB symptoms.
-
Timed voiding/bladder training can diminish bladder urgency and associated leakage by consistently voiding at defined intervals prior to the sensation of bladder urgency.
-
Urge suppression strategies can lessen the intensity of or diminish involuntary contractions, preventing leakage.
-
Kegel exercises can increase pelvic floor muscle strength and the urinary sphincter's ability to hold urine. They can also cause reflexive relaxation of detrusor smooth muscle, lessening urgency and diminishing involuntary bladder contractions.
-
Treatment of constipation can lessen OAB symptoms.
For difficulty emptying:
-
Pelvic floor relaxation during voiding can improve bladder emptying by allowing the urethral sphincter and surrounding pelvic floor muscles to relax with each void
-
Double voiding, which involves voiding or attempting to void a second time with or without the use of Valsalva or compression within a few minutes of the first void, gives the bladder another opportunity to empty
Non-pharmacologic intervention for difficulty emptying:
-
Clean intermittent catheterization can be used when the patient is unable to empty effectively on their own. A catheter is inserted in the bladder every 3–8 hours in lieu of or following voiding.
-
An indwelling urethral catheter or suprapubic tube can be used to drain the bladder in patients unable to catheterize themselves. This is a last-resort option due to the risk of complications from an indwelling foreign body (urinary tract infection, tract erosion, need for a bag, odor, accidental spillage of the bag, and loss of cycling of the bladder).
Pharmacologic treatment
Overactive bladder
Drug therapy is used for OAB symptoms primarily to decrease urinary frequency, lessen bladder urgency, and reduce episodes of urinary incontinence. Drug therapy can also effectively relax detrusor smooth muscle to lower intradetrusor pressure in patients with poor bladder compliance. Anti-cholinergics and anti-muscarinics are the mainstays of treatment, but when these are not tolerated or are ineffective, beta agonists, phosphodiesterase inhibitors, and tricyclic antidepressants can be added or substituted. Drug therapy with alpha-adrenergic agents can be initiated when poor bladder emptying is encountered.
- Specific drugs :
-
anticholinergics – oxybutynin
- Standard dosage :
-
oral: 5 mg IR/5–15 mg ER (Ditropan XL); patch 3.9 mg/day (Oxytrol); 3 % gel 64 mg/day (Gelnique) [6]
- Contraindications :
-
Narrow-angle glaucoma, urinary retention, gastroparesis, intestinal obstruction
- Main drug interactions :
-
interacts with potassium salts and slows passage through the GI tract
- Main side effects :
-
Most common side effects include dry mouth, dry eyes, blurred vision, dizziness, drowsiness, and mild constipation [2]. CNS side effects such as cognitive dysfunction, memory impairment, and headache are rare.
- Cost/cost effectiveness :
-
5 mg tab (100) $328.40, 10 mg tab (100) $328.75, 15 mg tab (100) $336.95; Oxytrol 3.9 mg/24-hr patches: 8/$250.80 or 24/$731.48 [7]
- Specific drugs :
-
antimuscarinics – tolterodine (Detrol) [8]
- Standard dosage :
-
1–2 mg daily IR, 2–4 mg LA
- Contraindications :
-
narrow-angle glaucoma, urinary retention, gastroparesis, intestinal obstruction
- Main drug interactions :
-
metabolized by the cytochrome P450 system
- Main side effects :
-
dry mouth, dry eyes, mild constipation, and blurred vision; tachycardia, QT prolongation (never more than 500 msec) and CNS side effects are rare [2]
- Cost/cost effectiveness :
-
Capsule, 24-hour Detrol LA oral 2 mg (90): $734.24, 4 mg (90): $734.24. Capsule, 24-hour Detrol oral 1 mg (140): $679.08, 2 mg (140): $696.65. Capsule, 24-hour tolterodine tartrate oral 1 mg (90): $297.83, 2 mg (90): $305.69 [7]
- Specific drugs :
-
antimuscarinics – trospium (Sanctura) [9]
- Standard dosage :
-
20 mg IR/60 mg ER
- Contraindications :
-
narrow angle glaucoma, renal failure, urinary retention, gastroparesis, intestinal obstruction
- Main drug interactions :
-
can interact with other drugs that are eliminated by the renal tubules, causing both drugs to build up in the system; common interactions through this mechanism occur with ranitidine and metformin
- Main side effects :
-
same as above; trospium is made up of quaternary amines which have fewer CNS side effects; common side effects are constipation and fatigue [2]
- Special points :
-
quaternary amines cross the blood–brain barrier less often, resulting in fewer CNS side effects; trospium is metabolized primarily by the kidneys (as opposed to the liver, which metabolizes the vast majority of the other antimuscarinics)
- Cost/cost effectiveness :
-
Capsule, 24-hour (Sanctura XR oral) 60 mg (90): $673.68, Capsule, 24-hour (trospium chloride ER Oral) 60 mg (90): $606.30. Tablet (Sanctura oral) 20 mg (90): $381.58. Tablet (trospium chloride oral) 20 mg (90): $255.39 [7]
- Specific drugs :
-
solifenacin (VESIcare) [10]
- Standard dosage :
-
5–10 mg daily
- Contraindications :
-
same as above; glaucoma, urinary retention
- Main drug interactions :
-
metabolized by cytochrome P450 enzymes, tertiary amine
- Main side effects :
-
same as above, possibly less dry mouth than tolterodine
- Cost/cost effectiveness :
-
5 mg (90): $730.46, 10 mg (90): $730.46 [7]
- Specific drugs :
-
darifenacin (Enablex) [6]
- Standard dosage :
-
7.5 or 15 mg/day
- Contraindications :
-
same as above; urinary retention, glaucoma
- Main drug interactions :
-
slows down gastric emptying, should not be combined with other medications that slow gastric emptying
- Main side effects :
-
dry mouth, constipation, headache, blurred vision, tachycardia, QT prolongation
- Cost/cost effectiveness :
-
(Enablex oral) 7.5 mg (90): $647.31, 15 mg (90): $647.31 [7]
- Specific drugs :
-
fesoterodine (Toviaz) [11]
- Standard dosage :
-
4–8 mg daily
- Contraindications :
-
same as above; glaucoma, urinary retention
- Main drug interactions :
-
same as tolterodine
- Main side effects :
-
same as tolterodine
- Special points :
-
breaks down to the same end product as tolterodine
- Cost/cost effectiveness :
-
(Toviaz oral) 4 mg (90): $597.66, 8 mg (90): $597.66 [7]
- Specific drugs :
-
beta agonists – mirabegron (Myrbetriq) [12•]
- Standard dosage :
-
25–50 mg daily
- Contraindications :
-
uncontrolled hypertension
- Main drug interactions :
-
metabolized by CYP450, can interact with other drugs hepatically metabolized
- Main side effects :
-
hypertension, urinary retention, headache, tachycardia
- Cost/cost effectiveness :
-
(Myrbetriq oral) 25 mg (90): $750.60, 50 mg (90): $750.60 [7]
- Specific drugs :
-
phosphodiesterase inhibitors – sildenafil (Viagra) [13]
- Standard dosage :
-
50–100 mg daily
- Contraindications :
-
none
- Main drug interactions :
-
when combined with alpha blockers, can cause hypotension
- Main side effects :
-
hypotension, vision changes, headache
- Special points :
-
reduced LUTS symptoms in patients taking it for erectile dysfunction, relaxes smooth muscle, including the detrusor, and also relaxes the smooth muscle of the outflow tract
- Cost/cost effectiveness :
-
Tablet (Revatio oral) 20 mg (90): $2315.05
Tablet (sildenafil citrate oral) 20 mg (90): $1818.46
Tablet (Viagra oral) 25 mg (90): $2880.48, 50 mg (90): $2880.48, 100 mg (90): $2880.48 [7]
- Specific drugs :
-
tricyclic antidepressants – imipramine [14]
- Standard dosage :
-
150–300 mg daily
- Contraindications :
-
recent MI
- Main drug interactions :
-
class IA antiarrhythmics due to increase in QT
- Main side effects :
-
orthostatic hypotension, syncope, QT prolongation
- Special points :
-
helpful in groups of patients who have failed anti-muscarinic therapy alone, decreases bladder contractility and increases outlet resistance
- Cost/cost effectiveness :
-
Capsule (imipramine pamoate oral) 75 mg (90): $1517.19, 100 mg (90): $1517.19, 125 mg (90): $1517.19, 150 mg (90): $1517.19
Capsule (Tofranil-PM oral) 75 mg (90): $1995.60, 100 mg (90): $2035.11, 125 mg (90): $2074.65, 150 mg (90): $2114.13
Tablet (imipramine HCl oral) 10 mg (100): $42.96, 25 mg (100): $71.75, 50 mg (100): $121.85
Tablet (Tofranil oral) 10 mg (90): $704.01, 25 mg (90): $716.58, 50 mg (90): $729.15 [7]
- Specific drugs :
-
baclofen [2]
- Standard dosage :
-
20–80 mg/day [6]
- Contraindications :
-
caution in patients with psychiatric disorders
- Main drug interactions :
-
can combine with antihistamines to cause increased sedation
- Main side effects :
-
drowsiness, insomnia, rash, pruritus, sudden withdrawal can cause hallucinations
- Cost/cost effectiveness :
-
(baclofen oral) 10 mg (100): $59.65, 20 mg (100): $106.99 [7]
- Specific drugs :
-
Desmopressin [2]
- Standard dosage :
-
0.2–0.6 mg/day at bedtime PO
- Contraindications :
-
cannot be used in patients with severe renal impairment, can cause hypotension and therefore should be used in caution in patients with cardiac history
- Main drug interactions :
-
can combine with heparin to increase activity, reduced activity seen in patients taking lithium
- Main side effects :
-
hyponatremia, and therefore the need to restrict fluid intake one hour before taking the medication and 8 hours after
- Cost/cost effectiveness :
-
Tablet 0.1 mg tab: $287.97 (90), 0.2 mg tab: $521.97 (90)
Pharmacologic therapy
Difficulty emptying
- Specific drugs :
-
alpha-adrenergic antagonists –tamsulosin (Flomax); doxazosin (Cardura), terazosin (Hytrin), silodosin (Rapaflo), alfuzosin (Uroxatral) [3]
- Standard dosage :
-
tamsulosin 0.4 mg daily, generally given at bedtime
- Contraindications :
-
risk of increased drug levels if combined with hepatic metabolism inhibitors
- Main drug interactions :
-
risk of hypotension when combined with other alpha blockers
- Main side effects :
-
orthostatic hypotension
- Special points :
-
best used for patients with hesitancy, poor urinary stream, straining to urinate, incomplete bladder emptying, and outflow obstruction [15]
- Cost/cost effectiveness :
-
0.4 mg tab (100) $623.83 [7]
Interventional procedures
- Standard procedure :
-
intravesical botulinum neurotoxin type A (BoNT-A) [4]
- Contraindications :
-
difficulty emptying, acute UTI
- Complications :
-
can cause acute urinary retention, UTI
- Special points :
-
BoNT-A for overactive bladder/detrusor overactivity – inject 200 units reconstituted in 10–20 ml of injectable saline in approximately 10–20 sites throughout the bladder. Intrasphincteric injection can be used when detrusor sphincter dyssynergia prevents emptying
- Cost/cost effectiveness :
-
2-year period cost was $4,392 [16]
- Standard procedure :
-
percutaneous tibial nerve stimulation (PTNS) [5]
- Contraindications :
-
skin infection, inflammation at malleolus
- Complications :
-
none
- Special points :
-
minimally invasive treatment useful in medically refractory overactive bladder symptoms [17]
- Cost/cost effectiveness :
-
$1,773 for 12 weekly percutaneous tibial nerve stimulation treatments; cumulative discounted 2-year costs were $3,850 for PTNS [18••]; PTNS compared to the oral option tolterodine was found to be a greater cost initially but more cost-effective over time [19••]
- Standard procedure :
-
intrathecal baclofen [2]
- Contraindications :
-
active infection
- Complications :
-
seizures, meningitis, pump pocket infection
- Special points :
-
used in patients with detrusor overactivity due to spasticity from spinal cord lesions in the setting of concomitant muscle spasticity
- Cost/cost effectiveness :
-
used very infrequently, and therefore cost effectiveness data not available
Surgery
Surgery for neurogenic bladder dysfunction is a last resort due to the permanent nature of most of the procedures. In addition, patients with neurogenic bladder dysfunction can have changes in dysfunction status over time.
- Standard procedure :
-
InterStim neuromodulation [1]
- Contraindications :
-
anatomical abnormalities of the sacrum, skin infection/inflammation over the sacrum, mental inability of the patient to use the device. Should be removed before a patient gets an MRI (except head) and turned off if a patient becomes pregnant
- Complications :
-
infection of the pocket leading to need for removal, lead migration, lead fracture, failure of device
- Special points :
-
this is the most commonly used non pharmacological modality for overactive bladder symptoms, can also be used for non-obstructive urinary retention [20]
- Cost/cost effectiveness :
-
$1,857 for test sacral nerve stimulation. For ongoing therapy, the cost of the sacral nerve stimulation surgical implant was $22,970; cumulative discounted 2-year costs were $14,160 for sacral nerve stimulation [18••]
- Standard procedure :
-
sphincterotomy [2]
- Contraindications :
-
Patients who desire continence, anatomic obstruction such as BPH or bladder neck contracture
- Complications :
-
Urinary incontinence, urinary extravasation, and erectile dysfunction are possible but less likely if the cut is made at the 12 o'clock position
- Special points :
-
rarely done now due to its semi-permanent nature; intrasphincteric Botox is more commonly used. The procedure involves incision of the external urethral sphincter to allow better urinary flow, most commonly used in detrusor sphincter dyssynergia to release the poorly relaxing sphincter, can be done with a knife or laser
- Cost/cost effectiveness :
-
no data available
- Standard procedure :
-
urethral stenting (UroLume) [2]
- Contraindications :
-
bladder neck contracture, urethral stones, patient who desires continence
- Complications :
-
stent can migrate into the bladder and cause bladder calcifications, migrate proximal or distal to the sphincter, and fail
- Special points :
-
rarely done due to its semi-permanent nature; the procedure involves the placement of a urethral stent to allow the striated sphincter to remain open
- Cost/cost effectiveness :
-
no data available
- Standard procedure :
-
bladder augmentation – enterocystoplasty or autoaugmentation [2]
- Contraindications :
-
patients unwilling or unable to perform intermittent catheterization; enterocystoplasty cannot be done in patients whose intestinal tract is compromised, such as patients with inflammatory bowel disease
- Complications :
-
urine leak from surgical anastomosis, bladder calculi, UTI with enterocystoplasty and the use of intestinal segment are complications that come with any bowel surgery, including adhesions and small bowel obstructions.
- Special points :
-
primarily used in patients with poorly compliant bladders; patients have to be able to catheterize because ability to void is not guaranteed; bladder augmentation is a viable option in patients whose upper tracts and kidneys are being compromised by inability to properly empty.
- Cost/cost effectiveness :
-
no data available
Assistive devices
Urinary collection devices
- Specific device :
-
bedpan/urinal
- Special points :
-
ease ability to urinate because the patient does not have to get up to urinate
- Usage :
-
can be used with patients who are less mobile or have fall risk
- Cost/cost effectiveness :
-
very low-cost
- Specific device :
-
commode
- Usage :
-
can be used for patients who have slow gait, can be set up nearby to prevent accidents
- Cost/cost effectiveness :
-
very low-cost, usually covered by insurance
- Specific device :
-
diapers/incontinence pads
- Usage :
-
can be worn to prevent accidents from leaking onto clothes
- Cost/cost effectiveness :
-
Relatively low-cost and can improve quality of life because patients are not as afraid of being farther away from a bathroom; sometimes covered by insurance
Physical/speech therapy and exercise
- Specific therapy :
-
pelvic floor muscle therapy (PFMT)
- Usage :
-
pelvic muscle exercises taught by a healthcare professional
- Special points :
-
usually used in combination with a pharmacological agent to improve overactive bladder symptoms by strengthening the pelvic floor muscles
- Specific therapy :
-
biofeedback
- Usage :
-
can be used to train a patient to control any bodily function
- Special points :
-
depends on the patient’s efforts and skill of the therapist; utilizes EMG sensors attached to a computer terminal so that patients get visual and/or auditory feedback when they are contracting their muscles properly
Emerging therapies
MRI-compatible neuromodulation would be an extremely useful modality in the neurologic population where bladder symptoms are mixed in nature, as neuromodulation can improve both emptying function and overactive bladder symptoms. MRI compatibility would allow patients whose neurologic disease is monitored with MRI to benefit from care.
PTNS is very effective for decreasing overactive bladder symptoms; however, its major cost and inconvenience comes from having to go to the doctor’s office weekly for 12 weeks, followed by a maintenance regimen. Home units for stimulation of the tibial (or other accessible peripheral) nerve would allow patients to institute therapy at home without the added cost and burden of weekly health care visits [21].
References and Recommended Reading
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Stansell LG, Smith AL, Jaffe WI. Treatment of neurogenic voiding dysfunction: an update. Curr Bladder Dysfunct Rep. 2011;6:37–44.
Campbell MF, Wein AJ, Kavoussi LR, editors. Campbell-Walsh Urology. Philadelphia: Saunders/Elsevier; 2007.
Kessler TM, Studer UE, Burkhard FC. The effect of terazosin on functional bladder outlet obstruction in women: a pilot study. J Urol. 2006;176(4 Pt. 1):1487.
Schurch B, de Sèze M, Denys P, Chartier-Kastler E, Haab F, Everaert K, et al. Botulinum toxin type a is a safe and effective treatment for neurogenic urinary incontinence: results of a single treatment, randomized, placebo controlled 6-month study. J Urol. 2005;174(1):196–200.
Peters KM, Carrico DJ, Wooldridge LS, Miller CJ, MacDiarmid SA. Percutaneous tibial nerve stimulation for the long-term treatment of overactive bladder: 3-year results of the STEP study. J Urol. 2013;189(6):2194–201. This study shows the effectiveness of PTNS over long term, it had already been shown to be effective in the short term but this study was the first well made study that showed the use of PTNS over a longer time period.
AthenaHealth. Epocrates essentials (13.9.1 ed.). United States: Epocrates, Inc.; 2013.
Walters Kluwer Health. (2013). Lexicomp.
Roberts R, Bavendam T, Glasser DB, Carlsson M, Eyland N, Elinoff V. Tolterodine extended release improves patient-reported outcomes in overactive bladder: results from the IMPACT trial. Int J Clin Pract. 2006;60(6):752–8.
Novara G, Galfano A, Secco S, et al. A systematic review and meta-analysis of randomized controlled trials with antimuscarinic drugs for overactive bladder. Eur Urol. 2008;54(4):740–63.
Chapple CR, Fianu-Jonsson A, Indig M, Khullar V, Rosa J, Scarpa RM, et al. Treatment outcomes in the STAR study: a subanalysis of solifenacin 5 mg and tolterodine ER 4 mg. Eur Urol. 2007;52(4):1195–203.
Kelleher CJ, Tubaro A, Wang JT, Kopp Z. Impact of fesoterodine on quality of life: pooled data from two randomized trials. BJU Int. 2008;102(1):56–61.
Imran M, Najmi AK, Tabrez S. Mirabegron for overactive bladder: a novel, first-in-class β3 -agonist therapy. Urol J. 2013;10(3):935–40. This study is the first to use β3 agonists in the treatment of overactive bladder. It is truly a novel approach.
Madhuvrata P, Singh M, Hasafa Z, Abdel-Fattah M. Anticholinergic drugs for adult neurogenic detrusor overactivity: A systematic review and meta-analysis. Eur Urol. 2012;62(5):816–30.
Cameron AP, Clemens JQ, Latini JM, McGuire EJ. Combination drug therapy improves compliance of the neurogenic bladder. J Urol. 2009;182(3):1062–7.
Low Y, Liong ML, Yuen KH, et al. Terazosin therapy for patients with female lower urinary tract symptoms: a randomized, double blind, placebo controlled trial. J Urol. 2008;179(4):1461.
Siddiqui NY, Amundsen CL, Visco AG, Myers ER, Wu JM. Cost-effectiveness of sacral neuromodulation versus intravesical botulinum A toxin for treatment of refractory urge incontinence. J Urol. 2009;182(6):2799–804.
Ridout AE, Yoong W. Tibial nerve stimulation for overactive bladder syndrome unresponsive to medical therapy. J Obstet Gynaecol. 2010;30(2):111–4.
Martinson M, MacDiarmid S, Black E. Cost of neuromodulation therapies for overactive bladder: percutaneous tibial nerve stimulation versus sacral nerve stimulation. J Urol. 2013;189(1):210–6. This study compared two very commonly used methods of treating bladder dysfunction. Its importance is in showing the cost-effectiveness of both methods, and it showed that although initially PTNS is more cost-effective, over time SNS also becomes cost-effective.
Chen HW, Bercik RS, Werner EF, Thung SF. Cost-effectiveness of percutaneous tibial nerve stimulation versus extended release tolterodine for overactive bladder. J Urol. 2012;187(1):178–84. This study compared pharmacologic procedures with interventional procedures. While pharmacologic treatments are initially more cost-effective, it turns out that in the long-term, an interventional procedure, while costly at first, can become the more cost-effective option.
Jenks J, Hamid R, Shah J, Greenwell T, Betts C, Walleser S, et al. 1368 sacral nerve stimulation (SNS) for the treatment of idiopathic refractory overactive bladder: cost-effectiveness compared to optimal medical therapy, botulinum toxin a (boNT-A) and percutaneous tibial nerve stimulation (PTNS). J Urol. 2013;189(4, Supplement):e560.
Maurelli V, Petta F, Carsillo G, Miano R, Lamorte F, Perugia C, et al. [What to do if percutaneous tibial nerve stimulation (PTNS) works? A pilot study on home-based transcutaneous tibial nerve stimulation– Urologia. 2012;79(19):86–90.
Compliance with Ethics Guidelines
Conflict of Interest
Eliza Lamin declares that she has no conflict of interest.
Ariana L. Smith has received grant support from the NIH/NIDDK P20 Award.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Neurologic Manifestations of Systemic Disease
Rights and permissions
About this article
Cite this article
Lamin, E., Smith, A.L. Urologic Agents for Treatment of Bladder Dysfunction in Neurologic Disease. Curr Treat Options Neurol 16, 280 (2014). https://doi.org/10.1007/s11940-013-0280-3
Published:
DOI: https://doi.org/10.1007/s11940-013-0280-3