Abstract
Purpose of Review
Androgen deprivation therapy (ADT) is an important adjunctive therapy to external beam radiation therapy (RT) for the definitive management of prostate cancer. The role of ADT is well-established for locally advanced or high-risk disease in conjunction with standard doses of RT, but less defined for intermediate-risk disease or with dose-escalated RT. The goal of this review is to summarize evidence evaluating the combination of ADT/RT, focusing on recent trials and current controversies as they pertain to the practicing clinician.
Recent Findings
The benefit of ADT on biochemical control is maintained with dose-escalated RT according to recently reported phase III studies. Furthermore, there is now prospective, randomized evidence to support the addition of ADT to RT in the post-prostatectomy setting.
Summary
ADT continues to play an important role for prostate cancer patients receiving dose-escalated RT. Future research is needed to identify subgroups most likely to benefit from this combination.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
There is level 1 evidence to support the addition of androgen deprivation therapy (ADT) to external beam radiation therapy (RT) for primary treatment of unfavorable-risk, non-metastatic prostate cancer. However, a number of questions remain regarding the role of ADT for prostate cancer patients receiving RT, such as the optimal duration of ADT and how to best select patients who will benefit from combined therapy. This review will summarize the rationale for combining ADT with RT, and focus on recent evidence and controversies surrounding this approach for intact and post-operative prostate cancer patients as they pertain to the practicing clinician.
Mechanism of Action
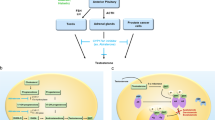
When combined with RT to treat prostate cancer, ADT has been shown to improve local control, and reduce the risk of distant metastasis. Relatively recent work has elucidated a possible mechanism which accounts for improved local control through radiation sensitization. Normally, androgens stimulate DNA repair genes via the androgen receptor and thereby counteract the DNA-damaging effects of ionizing radiation [1]. Hormonal therapy may sensitize prostate cancer cells to ionizing radiation by disrupting this pathway. Other mechanisms may also contribute, such as the ability for hormonal therapy to reduce intra-prostatic hypoxia [2]. Conceptually, the addition of ADT to RT shifts the sigmoidal dose response curve for tumor control to the left, increasing the probability of tumor cell kill at a given RT dose without a corresponding shift of the normal tissue complication curve (Fig. 1). The radiation-sensitizing properties of ADT are supported by the significantly reduced rates of positive post-treatment prostate biopsies after combined ADT/RT compared to RT alone [3]. This finding has important implications for disease outcomes, as persistent local disease can lead to development of distant metastases [4]. The effect of ADT on distant control in the setting of RT is more difficult to explain, as multiple randomized studies have failed to demonstrate a similar benefit for men treated with radical prostatectomy, suggesting that this effect could be uniquely associated with the administration of RT [5,6,7,8,9]. Other anti-tumor mechanisms may be involved such as effects on subclinical micrometastases, since the early reduction in distant metastases observed with addition of ADT is not well explained by DNA repair pathways or a simple translation of local failures which progress to distant disease. Some of this effect may be immune mediated, as ADT has been shown to elicit immune responses, while RT promotes immunogenic cell death and antigen presentation [10].
Dose response curve for tumor control and severe normal tissue complications with and without ADT. a A model to illustrate the local effects of radiation therapy on tumor control. A slight increase in dose (such as 8 Gy at 2 Gy/fraction, separating points A and B) can have a significant impact on local control in the external beam dose range where the sigmoidal response curves are the steepest. Hormonal therapy acts as a radiation sensitizer and shifts the tumor control probability curve to the left, improving local control at both points A and B. The shift results in less impact in the higher dose range of brachytherapy (point C). b To illustrate the impact of ADT on tumor control probability, estimated 5-year biochemical recurrence-free survival (bRFS) rates from select randomized trials are plotted against radiation dose. A sigmoidal curve is drawn according to data from randomized trials (focusing on the dose range of 64-80 Gy) showing how hormonal therapy (gold) shifts the dose response curve of radiation alone (blue) to the left
Evidence Supporting ADT + RT: Classic Randomized Trials
Multiple randomized trials support the addition of ADT to conventional dose (≤70 Gy) RT for primary treatment of intact prostate cancer (Table 1) [3, 11, 13, 15, 17, 19, 27, 28]. These landmark trials demonstrated improved disease-free survival (DFS) and overall survival (OS) with ADT/RT compared to RT alone. However, many of these studies were conducted prior to widespread PSA screening and predominantly included men with locally advanced disease. Furthermore, the timing and duration of ADT varied widely, given before, during, and/or after RT and ranging from 4 months to indefinitely. Since the inception of these trials, improvements in radiation techniques have enabled safe escalation of radiation dose, which has been associated with improvements in biochemical control compared to conventional dose RT in the absence of ADT [29,30,31,32,33,34]. Therefore, it is unclear whether the effect of ADT observed in older trials necessarily applies today with dose-escalated RT and PSA screening. Subsequent trials have attempted to determine the ideal duration of ADT and refine patient selection for combination therapy.
Defining the Optimal Duration of ADT
High-Risk Patients
Practice guideline: long-term ADT (2 years, 4 months) given neoadjuvantly, concurrently, and adjuvantly is recommended for men with high-risk disease.
In high-risk patients (T3, Gleason score ≥ 8, or PSA > 20) long-term (LT) ADT is the current standard of care according to national guidelines [35]. This recommendation is based on the results of two large randomized trials demonstrating disease-specific survival (DSS) and overall survival (OS) benefits to LT-ADT (28–36 months) over short-term (ST) ADT (4–6 months) in men with high-risk or locally advanced disease receiving conventional dose RT (Table 2) [36, 37]. In EORTC 22961, 5-year overall survival was superior with 3 years of ADT compared to 6 months. In RTOG 9202, 10-year disease-free survival (DFS) and DSS endpoints were improved with 28 months of ADT compared to 4 months. In a post hoc subgroup analysis, there was a survival advantage with LT-ADT in men with Gleason score ≥ 8 [36]. In contrast, in a recently published secondary analysis including the 133 patients classified as intermediate-risk with median follow-up of 11 years, there was no benefit to LT-ADT in terms of overall and disease-specific survival or biochemical outcomes for this subgroup [42]. Overall, these studies suggest improved outcomes with LT-ADT over ST-ADT in high-risk patients receiving conventional dose RT.
More recently, the Canadian PCS IV study compared 36 months of ADT to an intermediate duration of 18 months with conventional dose RT for high-risk, node-negative patients (majority clinical T2–3 with median PSA of 16 ng/ml and median Gleason score of 8) [38]. Preliminary results were presented at the American Society of Clinical Oncology (ASCO) conference in 2013 and suggest no significant differences in overall and disease-specific survival, biochemical failure, or distant metastases. The 10-year OS and DSS rates were 62 vs 59% (p = 0.275) and 84 vs 84% (p = 0.819) comparing 36 to 18 months of ADT [38]. While provocative, the trial was not designed as a non-inferiority trial and the hazard ratio for death comparing 18 to 36 months has a fairly wide confidence interval (HR = 1.15, 95% CI = 0.83–1.59), limiting the strength of conclusions about the safety of reducing the duration of ADT to 18 months.
Although LT-ADT is preferred for high-risk patients, the trials that established this standard of care used RT doses lower than what is commonly used today and included men with locally advanced disease who may stand to benefit more from prolonged ADT (the majority of patients in RTOG 9202 and EORTC 22961 had clinical T3–4 disease). In practice, completing multiple years of hormonal therapy can be challenging, and some men will choose to discontinue therapy due to side effects or physician concerns with age or comorbidity [43]. The heterogeneity of disease outcomes after therapy within the high-risk group has been increasingly recognized, and it is likely that certain subgroups derive greater benefit from LT-ADT. Prognostic factors such as PSA nadir may help identify a subset of high-risk patients who have acceptable outcomes with ST-ADT, although this has yet to be validated in a prospective fashion [44]. Furthermore, the effect of ADT over time appears to be non-linear, with the greatest benefits gained during the initial months and diminishing thereafter [45]. The reason for the differential effect of ADT over time is unclear, but may be related to the fact that complete response to therapy can be delayed by 18 or more months. Post-treatment biopsies within 18 months of RT can show indeterminate findings, whereas biopsies after 2.5 years are typically negative provided that sufficient radiation doses are given [46,47,48]. While LT-ADT remains the current standard for high-risk disease, further study is warranted to identify high-risk patients who could achieve acceptable disease control with ST-ADT or even no ADT.
Intermediate-Risk Patients
Practice guideline: short-term ADT (4–6 months) given neoadjuvantly and concurrently is recommended for men with intermediate-risk disease on an individualized basis.
The role of ADT is more controversial in the intermediate-risk group (T2b-c, Gleason score 7, or PSA 10–20 ng/ml). In general, ST-ADT (duration of 4–6 months) is considered standard when ADT is used. Several of the classic randomized trials supporting the addition of ADT to conventional dose RT included intermediate-risk patients, most notably DFCI 95–096 and RTOG 9408 [3, 19]. Both of these trials demonstrated improved overall survival with ST-ADT compared to no ADT. It should be noted that low-risk patients included in RTOG 9408 did not benefit from the addition of ADT, and ADT is not recommended for this subgroup [3].
Since then, other trials have attempted to define the optimal duration of ADT for intermediate-risk patients. In a multi-center phase III trial from Canada consisting of predominantly low- and intermediate-risk patients, there was no significant benefit to 8 months compared to 3 months of ADT given neoadjuvantly with conventional dose RT (5-yearfreedom from biochemical failure (FFbF) 75 vs 72%, p = 0.18) [39]. Similarly, in RTOG 9910, there was no improvement in any endpoint comparing 4 to 9 months of ADT with conventional dose RT (10-year DSS 95 vs 96%, p = 0.45; 10-year OS 66 vs 67%, p = 0.62) [40]. Furthermore, there was no benefit with the extended course of ADT in the subgroup of patients with more than one intermediate-risk factor. Given these results, a shorter duration of 4–6 months is preferred when ADT is recommended for intermediate-risk disease.
The decision of whether or not to recommend ADT for men with intermediate-risk disease is somewhat complex, given the heterogeneous nature of this group. Clinical factors, such as percentage of positive biopsy cores, can be used to help aid in patient selection for ADT [49]. A subsequent, larger retrospective analysis with long-term follow-up from MSKCC suggests that the presence of primary Gleason 4 disease, multiple intermediate-risk factors, or percent positive cores ≥50% may be useful to further risk stratify in this heterogeneous cohort [50]. Patients with “unfavorable” features behave similarly to men treated with high-risk disease (who may require ADT), while patients with “favorable” disease behave similarly to men treated with low-risk disease (who may not require ADT). The use of additional clinical risk factors can therefore aid decision making regarding the use of ADT for men who will receive RT.
Recognizing the shortcomings of the traditional Gleason grading, investigators have proposed a new grading system which differentiates Gleason 3 + 4 (grade group 2) from Gleason 4 + 3 (grade group 3) [51]. In this multi-institutional analysis of more than 20,000 men with prostate cancer, large differences in biochemical DFS were apparent between Gleason 3 + 4 vs 4 + 3 disease in patients treated with radical prostatectomy and also present to a lesser degree in patients receiving RT alone. However, the proposed grade groups were less discriminating when including patients treated with combined RT/ADT, likely due to the beneficial impact of ADT for higher-grade disease. Overall, the available evidence supports the use of primary Gleason 4 pattern among other clinical risk factors to further risk-stratify intermediate-risk patients and inform selection for ADT.
In addition to clinical risk factors, various biomarkers have been explored to improve risk stratification and guide individualized treatment decisions. Based on tissue samples collected from RTOG 86–10 and 92–02, several biomarkers have been identified as prognostic for disease outcomes (p16, Ki-67, VEGF/HiF-1 alpha) and/or predictive of response to therapy (p53 DNA, DNA ploidy, COX-2) [52]. For example, COX-2 expression was found to be an adverse prognostic factor for biochemical failure and distant metastasis in a cohort of over 500 patients from RTOG 92–02 [53]. Notably, the prognostic value of COX-2 expression was not seen in the LT-ADT arm, suggesting that LT-ADT might compensate for the detrimental impact of COX-2 expression [53]. In this way, biomarkers such as COX-2 could potentially be used to select patients for LT-ADT. However, prospective validation with independent datasets is necessary before incorporating tissue biomarkers into routine practice. Genomic classifiers are also being explored in this context and hold some promise [54].
Role of ADT with Dose-Escalated RT
Can ADT be Safely Omitted with Dose-Escalated RT?
With advances in treatment planning and delivery including intensity-modulated RT and image guidance, dose-escalated RT (which could be considered radiation dose ≥74 Gy) is now commonly prescribed, as multiple randomized trials have demonstrated that it improves biochemical outcomes compared to conventional doses of RT [29,30,31]. It is plausible to consider that the incremental benefit of dose escalation beyond conventional RT could diminish the impact of ADT, especially if the primary goal of ADT is to influence local control as a radiation sensitizer.
Given that ADT can cause side effects, there is a desire to identify men who can avoid ADT and still achieve excellent oncologic outcomes with RT alone [55]. Retrospective studies of ADT plus dose-escalated RT have produced mixed results, with some suggesting a benefit to ADT and others showing none [56,57,58]. The omission of ADT may be most relevant for intermediate-risk patients due to the substantial heterogeneity within this group but could also apply to select high-risk patients. Randomized trials (primarily enrolling intermediate-risk patients) are beginning to mature that will help address this question.
EORTC trial 22991 investigated the addition of 6 months of ADT starting on day 1 of RT compared to RT alone for intermediate (64%) or high-risk patients (35%) [22•]. RT dose was 70, 74, or 78 Gy as determined by participating center. The 5-year biochemical DFS was significantly improved with 6 months of ADT compared to RT alone (83 vs 70%, p < 0.01). Furthermore, the benefit of ADT was observed in all RT dose levels. However, there was no difference in overall survival in this early report. As expected, hormone-related adverse effects were increased and sexual function impaired in the combination arm at 6- and 12-month time points; however, these differences diminished by 2 years. Preliminary results of two recently reported phase III trials also suggested a benefit to adding ST-ADT to dose-escalated RT for intermediate-risk patients. The Canadian PCS 3 trial randomized intermediate-risk patients to one of three arms: 70 Gy plus 6 months ADT, 76 Gy plus 6 months ADT, or 76 Gy RT alone [23]. Preliminary results reported at the 2016 ASTRO conference demonstrated improved 10 year DFS rates in the two arms receiving combined ADT/RT compared to the RT alone arm (10-year DFS rates 78, 78, and 67%, respectively, p = 0.016 and p = 0.001). In contrast, there were no significant differences in DFS between the two groups receiving ADT despite different RT dose levels. Furthermore, late GI toxicity was significantly lower in the 70 Gy RT + ADT arm compared to high-dose RT arms (5 vs 16%; p < 0.001). There was no significant difference in survival at 10 years. The GETUG 14 trial randomized intermediate-risk patients to 4 months of ADT or no ADT with dose-escalated RT (80 Gy). Although enrollment was closed prematurely due to poor accrual, preliminary results including 377 patients were recently reported at ASCO in 2016. There was a significant improvement in biochemical outcomes in the group receiving ADT (5-year biochemical DFS 84 vs 76%, p = 0.02) [24].
In sum, these trials demonstrate that ADT improves biochemical outcomes in the setting of dose-escalated RT. Longer follow-up is needed to assess the impact on overall survival. The continued benefit of ADT for external beam doses ≥74 Gy suggest that the dose range of 74–80 Gy is still on the steep portion of the sigmoid tumor response curve (Fig. 1), assuming that ADT acts primarily on local control.
Can the Duration of ADT be Reduced with Dose-Escalated RT?
Although dose-escalated RT may not obviate the need for ADT, it may allow for a shorter course. This would likely have significant quality of life implications, given that abbreviating ADT duration can allow for earlier to testosterone recovery. Thus far, only one phase III trial has reported on the impact of varying durations of ADT combined with dose-escalated RT. The DART 01/05 trial from Spain included intermediate (46%) or high-risk (54%) patients and compared 28 to 4 months of ADT with a minimum RT dose of 76 Gy (range 76–82 Gy) [41•]. With a median follow-up of 63 months, the primary endpoint of biochemical DFS was significantly improved with LT-ADT arm compared to ST-ADT (5-year biochemical DFS 90 vs 81%, p = 0.01). Five-year overall survival and distant metastasis-free survival was also significantly improved in the LT-ADT group. According to a subgroup analysis, the benefits seen with LT-ADT were most evident in high-risk patients for all endpoints. Importantly, patient characteristics were representative of what would be expected in modern practice, with the majority of patients clinical stage T1–2 and a median PSA of 11.0 ng/ml. At this time, the available evidence continues to support LT-ADT for high-risk patients.
In situations where a shorter course of ADT is considered, PSA response may be a tool to help guide this decision. In a multi-institutional retrospective analysis of over 450 men treated with dose-escalated RT, PSA nadir ≤0.2 ng/ml was an independent prognostic factor for freedom from distant metastases and cause-specific survival [44]. Men with PSA nadir ≤0.2 ng/ml had favorable outcomes whether ADT was given for <12 or ≥12 months. Other investigators have identified PSA nadir >0.5 ng/ml after completion of RT and 6 months of ADT as a surrogate marker for prostate cancer specific mortality [59]. These early markers of treatment response may help identify men more likely to benefit from prolonged ADT.
ADT Plus Brachytherapy
Brachytherapy, which involves exposure of the prostate to either temporary or implantable radioactive sources, enables dose escalation beyond that achievable with external beam RT. It is possible that ablative brachytherapy doses may reduce the need for ADT from a radiation sensitization standpoint, although ADT may still have a role in addressing occult micrometastases in high-risk patients. The majority of retrospective series on this topic suggest no benefit with the addition of ADT to brachytherapy; however, there is certainly the potential for selection bias in these reports [60]. Currently, there are limited data available to further clarify the role of ADT with brachytherapy.
Recently, the Canadian ASCENDE-RT randomized trial demonstrated a significantly higher rate of biochemical failure after dose-escalated external beam RT compared to low-dose-rate brachytherapy boost (hazard ratio = 2.04, p = 0.004) in men with intermediate- or high-risk disease who received 12 months of ADT [61•]. The duration of ADT was not randomized, but men in the brachytherapy boost arm had favorable biochemical outcomes, and the majority of patients with biochemical control had a PSA that was undetectable. This raises the possibility that the need for ADT may be modified for men treated with brachytherapy; however, prospective trials will be needed to test this hypothesis. Since brachytherapy can result in gland ablation (i.e., at the far right of a dose response curve), the role of ADT in this setting may shift more towards augmenting distant control rather than local control. Interestingly, a retrospective report of men treated with brachytherapy boost with Gleason score 9–10 disease, does demonstrate significantly higher rates of distant control at 10-years compared to men treated with external beam RT or radical prostatectomy (90, 67, and 62%, respectively, p < 0.01) [62]. Whether brachytherapy can further enhance the ability for ADT, or host immunity, to improve distant control rates beyond external beam RT is a hypothesis that requires further validation.
Recently, a task group from the American Brachytherapy Society performed a systematic review and proposed guidelines for the use of ADT with brachytherapy [63]. Although most studies reviewed were retrospective and heterogeneous, there does not appear to be a benefit to adding ADT to brachytherapy for low-risk and favorable intermediate-risk men. On the other hand, there may be an improvement in biochemical control with adding ADT to brachytherapy for unfavorable intermediate- and high-risk men or those with suboptimal implant dosimetry. However, the impact of ADT on cause-specific or overall survival is uncertain, and the authors recommend caution in prescribing ADT in older men or men with comorbidity. Several ongoing randomized trials examining the role of ADT with brachytherapy will provide further insight.
ADT + Post-prostatectomy RT
Practice guideline: offer concurrent ADT with salvage RT for select men based on clinical risk factors (e.g., higher Gleason score, higher PSA, pN1) and patient factors.
Given the benefit of ADT to primary RT for intact prostate cancer, it is reasonable to hypothesize that ADT could improve outcomes with adjuvant or salvage RT after prostatectomy; however, patient selection remains a challenge and is an ongoing area of research. The presence of high Gleason grade at the site of a positive surgical margin has been associated with increased risk of biochemical recurrence and proposed as a selection factor for adjuvant RT, but it is unknown whether the addition of ADT to adjuvant RT would improve outcomes [64]. In an updated analysis of SWOG 8794, patients with pathologic Gleason 8 disease or persistently detectable PSA were at high risk of disease progression (44–55% at 3 years) despite post-prostatectomy RT, suggesting that treatment intensification may be beneficial in this subset [65]. Subsequently, RTOG 0621 investigated the addition of 6 months ADT and 6 cycles of docetaxel to post-prostatectomy RT in high-risk patients defined as Gleason ≥8 and ≥pT3a with undetectable post-operative PSA or Gleason 7 with persistently elevated PSA [66]. The 3-year freedom from progression of 73% was improved compared to historical controls receiving post-prostatectomy RT alone. These preliminary results suggest that a subgroup of patients may benefit from concurrent ADT when immediate post-prostatectomy RT is delivered.
The results of two recently published phase III trials, GETUG-16 and RTOG 9601, now support the addition of ADT to salvage RT for rising PSA after prostatectomy (Table 1) [25••, 26•]. GETUG-16 demonstrated improved progression-free survival at 5 years with the addition of 6 months of ADT to salvage RT [26•]. With a median follow-up of 13 years, RTOG 9601 demonstrated improvements in late endpoints including distant metastasis-free, disease-specific, and overall survival at 12 years with the addition of 24 months of ADT to salvage RT [25••]. Many of the known prognostic factors for salvage RT were confirmed by these studies. In GETUG-16, higher PSA prior to RT, pT3b stage, negative surgical margins, and PSA doubling time less than 6 months were all associated with increased risk of relapse after salvage therapy [26•]. In RTOG 9601, the improvements in metastasis-free survival with ADT were greater for patients with PSA >1.5 ng/mL, Gleason score ≥8 or positive surgical margins [25••].
There were some notable differences between these two trials, however, which have implications for applying the results to current practice. For example, RTOG 9601 included some patients with persistently elevated PSA values after prostatectomy while GETUG-16 required an undetectable PSA for 6 months post-operatively. Also, RTOG 9601 allowed a higher upper limit PSA of 4 ng/ml compared to 2 ng/ml in GETUG-16. This distinction is relevant because a higher PSA level prior to RT was identified as a significant prognostic factor in both trials. In many practices, salvage RT is routinely offered at relatively low PSA levels, given the improved biochemical outcomes consistently observed with lower PSA levels prior to salvage RT [67]. Of note, the type and duration of androgen suppression differed: 6 months of goserelin in GETUG-16 vs 24 months of high-dose bicalutamide (150 mg daily) in RTOG 9601. This bicalutamide dosing regimen is no longer recommended, and most patients will receive standard GnRH agonists if the decision is made to offer ADT in conjunction with salvage RT. Overall, while these trials provide the first prospective, randomized evidence supporting the addition of ADT to salvage RT, a number of clinicopathologic factors (e.g., surgical margin status, Gleason score, lymph node involvement, pre-salvage RT PSA) as well as patient factors (age, comorbidity) can be used to decide whether to add ADT to salvage RT.
Adverse Effects and Toxicity Concerns
The oncologic benefits to ADT should be balanced against potential toxicity concerns and quality of life considerations [55]. The potential adverse effects of ADT are well-established, such as sexual dysfunction, hot flashes, weight gain, metabolic effects and decreased bone mineral density. Other potential concerns, such as cardiovascular toxicity, are more controversial but could have substantial consequences. Several large, observational studies have identified an association between ADT use and cardiovascular events, however this association has not been consistently observed in prospective studies [68, 69]. A potential link between ADT use and other diseases has also been reported, including neurocognitive issues (e.g., Alzheimer disease), diabetes, stroke, venous thromboembolism, frailty, etc. [70,71,72,73]. Men should be counseled about these risks, and interventions to reduce or manage side effects should be pursued such as exercise, lifestyle modifications, as well as involvement of the primary care physician, cardiologist, dietician, or other healthcare providers.
Ultimately, clinicians must weigh the relative benefits of combined ADT against the risks. In the treatment of prostate cancer, the use of hormonal therapy is another treatment variable, which complements a wide range of radiation dose (from conventional external beam doses of 70 Gy, up to ablative doses of brachytherapy) that a radiation oncologist can choose from to tailor treatment to fit the needs of the individual. It is desirable to allow life expectancy and medical comorbidity to influence the aggressiveness of prostate cancer treatment. Goals of therapy can vary for two patients with the same risk features of prostate cancer in a different clinical context, and should be adjusted according to whether disease recurrence would harm a patient’s quality of life or life expectancy.
Conclusions and Future Directions
In conclusion, ADT is an established adjunctive therapy for men with prostate cancer receiving RT. Level 1 evidence supports the role of ADT for locally advanced or high-risk patients, while the benefit of ADT in intermediate-risk patients is more controversial. A number of ongoing studies will help refine recommendations for ADT in various risk groups. RTOG 0815 is a phase III trial comparing 6 months of ADT to no ADT specifically in intermediate-risk patients. Furthermore, this trial will use the Adult Comorbidity Evaluation-27 (ACE-27) score to stratify patients and thereby will provide further insight into the risk-benefit ratio of ADT in regards to comorbidity. Also, additional randomized trials in the post-prostatectomy setting are underway including the RTOG 0534, which is examining the benefit of ST-ADT (4–6 months) compared to no ADT, and the RADICALS-HD, which is testing the duration of ADT (24 months vs 6 months vs none). Several trials incorporating novel hormonal therapy agents (e.g., abiraterone, enzalutamide) in the intact and post-prostatectomy settings are ongoing [74]. In addition, both RT and ADT may modulate the immune system, and multiple trials are underway testing the potential synergy of RT/ADT with various immunotherapies [10]. Finally, molecular biomarkers may improve the ability to risk-stratify men and optimally tailor therapies. Recently, a genomic classifier using tissue from biopsy samples has been shown to predict for distant metastases after ADT/RT for intermediate- and high-risk patients [54].
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Polkinghorn WR, Parker JS, Lee MX, Kass EM, Spratt DE, Iaquinta PJ, et al. Androgen receptor signaling regulates DNA repair in prostate cancers. Cancer Discov. 2013;3(11):1245–53. doi:10.1158/2159-8290.CD-13-0172.
Milosevic M, Chung P, Parker C, Bristow R, Toi A, Panzarella T, et al. Androgen withdrawal in patients reduces prostate cancer hypoxia: implications for disease progression and radiation response. Cancer Res. 2007;67(13):6022–5. doi:10.1158/0008-5472.CAN-07-0561.
Jones CU, Hunt D, McGowan DG, Amin MB, Chetner MP, Bruner DW, et al. Radiotherapy and short-term androgen deprivation for localized prostate cancer. N Engl J Med. 2011;365(2):107–18. doi:10.1056/NEJMoa1012348.
Coen JJ, Zietman AL, Thakral H, Shipley WU. Radical radiation for localized prostate cancer: local persistence of disease results in a late wave of metastases. J Clin Oncol. 2002;20(15):3199–205. doi:10.1200/JCO.2002.01.086.
Witjes WP, Schulman CC, Debruyne FM. Preliminary results of a prospective randomized study comparing radical prostatectomy versus radical prostatectomy associated with neoadjuvant hormonal combination therapy in T2-3 N0 M0 prostatic carcinoma. The European study group on neoadjuvant treatment of prostate cancer. Urology. 1997;49(3A Suppl):65–9.
Soloway MS, Sharifi R, Wajsman Z, McLeod D, Wood DP Jr, Puras-Baez A. Randomized prospective study comparing radical prostatectomy alone versus radical prostatectomy preceded by androgen blockade in clinical stage B2 (T2bNxM0) prostate cancer. The Lupron depot neoadjuvant prostate cancer study group. J Urol. 1995;154(2 Pt 1):424–8.
Dalkin BL, Ahmann FR, Nagle R, Johnson CS. Randomized study of neoadjuvant testicular androgen ablation therapy before radical prostatectomy in men with clinically localized prostate cancer. J Urol. 1996;155(4):1357–60.
Goldenberg SL, Klotz LH, Srigley J, Jewett MA, Mador D, Fradet Y, et al. Randomized, prospective, controlled study comparing radical prostatectomy alone and neoadjuvant androgen withdrawal in the treatment of localized prostate cancer. Canadian Urologic Oncology Group. J Urol. 1996;156(3):873–7.
Van Poppel H, De Ridder D, Elgamal AA, Van de Voorde W, Werbrouck P, Ackaert K, et al. Neoadjuvant hormonal therapy before radical prostatectomy decreases the number of positive surgical margins in stage T2 prostate cancer: interim results of a prospective randomized trial. The Belgian Uro-Oncological Study Group. J Urol. 1995;154(2 Pt 1):429–34.
Kalina JL, Neilson DS, Comber AP, Rauw JM, Alexander AS, Vergidis J, et al. Immune modulation by androgen deprivation and radiation therapy: implications for prostate cancer immunotherapy. Cancers (Basel). 2017;9(2):13. doi:10.3390/cancers9020013.
Bolla M, Collette L, Blank L, Warde P, Dubois JB, Mirimanoff RO, et al. Long-term results with immediate androgen suppression and external irradiation in patients with locally advanced prostate cancer (an EORTC study): a phase III randomised trial. Lancet. 2002;360(9327):103–6.
Bolla M, Van Tienhoven G, Warde P, Dubois JB, Mirimanoff RO, Storme G, et al. External irradiation with or without long-term androgen suppression for prostate cancer with high metastatic risk: 10-year results of an EORTC randomised study. Lancet Oncol. 2010;11(11):1066–73. doi:10.1016/S1470-2045(10)70223-0.
Lawton CA, Winter K, Murray K, Machtay M, Mesic JB, Hanks GE, et al. Updated results of the phase III radiation therapy oncology group (RTOG) trial 85-31 evaluating the potential benefit of androgen suppression following standard radiation therapy for unfavorable prognosis carcinoma of the prostate. Int J Radiat Oncol Biol Phys. 2001;49(4):937–46.
Pilepich MV, Winter K, Lawton CA, Krisch RE, Wolkov HB, Movsas B, et al. Androgen suppression adjuvant to definitive radiotherapy in prostate carcinoma—long-term results of phase III RTOG 85-31. Int J Radiat Oncol Biol Phys. 2005;61(5):1285–90. doi:10.1016/j.ijrobp.2004.08.047.
Pilepich MV, Winter K, John MJ, Mesic JB, Sause W, Rubin P, et al. Phase III radiation therapy oncology group (RTOG) trial 86-10 of androgen deprivation adjuvant to definitive radiotherapy in locally advanced carcinoma of the prostate. Int J Radiat Oncol Biol Phys. 2001;50(5):1243–52.
Roach M 3rd, Bae K, Speight J, Wolkov HB, Rubin P, Lee RJ, et al. Short-term neoadjuvant androgen deprivation therapy and external-beam radiotherapy for locally advanced prostate cancer: long-term results of RTOG 8610. J Clin Oncol. 2008;26(4):585–91. doi:10.1200/JCO.2007.13.9881.
Denham JW, Steigler A, Lamb DS, Joseph D, Mameghan H, Turner S, et al. Short-term androgen deprivation and radiotherapy for locally advanced prostate cancer: results from the trans-Tasman radiation oncology group 96.01 randomised controlled trial. Lancet Oncol. 2005;6(11):841–50. doi:10.1016/S1470-2045(05)70348-X.
Denham JW, Steigler A, Lamb DS, Joseph D, Turner S, Matthews J, et al. Short-term neoadjuvant androgen deprivation and radiotherapy for locally advanced prostate cancer: 10-year data from the TROG 96.01 randomised trial. Lancet Oncol. 2011;12(5):451–9. doi:10.1016/S1470-2045(11)70063-8.
D'Amico AV, Manola J, Loffredo M, Renshaw AA, DellaCroce A, Kantoff PW. 6-month androgen suppression plus radiation therapy vs radiation therapy alone for patients with clinically localized prostate cancer: a randomized controlled trial. JAMA. 2004;292(7):821–7. doi:10.1001/jama.292.7.821.
D'Amico AV, Chen MH, Renshaw AA, Loffredo M, Kantoff PW. Androgen suppression and radiation vs radiation alone for prostate cancer: a randomized trial. JAMA. 2008;299(3):289–95. doi:10.1001/jama.299.3.289.
D'Amico AV, Chen MH, Renshaw A, Loffredo M, Kantoff PW. Long-term follow-up of a randomized trial of radiation with or without androgen deprivation therapy for localized prostate cancer. JAMA. 2015;314(12):1291–3. doi:10.1001/jama.2015.8577.
• Bolla M, Maingon P, Carrie C, Villa S, Kitsios P, Poortmans PM, et al. Short androgen suppression and radiation dose escalation for intermediate- and high-risk localized prostate cancer: results of EORTC trial 22991. J Clin Oncol. 2016;34(15):1748–56. doi:10.1200/JCO.2015.64.8055. One of the first prospective, randomized trials to demonstrated improved biochemical outcomes with the addition of ADT to dose-escalated RT.
Nabid A, Carrier N, Vigneault E, Souhami L, Lemaire C, Brassard MA, Bahoric B, Archambault R, Vincent F, Nguyen TV. Radiation therapy with or without short-term androgen deprivation therapy in intermediate-risk prostate cancer: results of a phase 3 trial. Int J Radiat Oncol Biol Phys. 2016;94(1):4.
BM Dubray, J Salleron, SG Guerif, E Le Prise, A Reynaud-Bougnoux, J-M Hannoun-Levi, TD Nguyen, C Hennequin, J Cretin, M Fayolle-Campana, J-L Lagrange, J-M Bachaud, D Azria, A Grangirard, P Pommier, J-M Simon, M Habibian, P Bey, V Beckendorf. Does short-term androgen depletion add to high dose radiotherapy (80 Gy) in localized intermediate risk prostate cancer? Final analysis of GETUG 14 randomized trial (EU-20503/NCT00104741). J Clin Oncol. 2016;34(suppl; abstr 5021).
•• Shipley WU, Seiferheld W, Lukka HR, Major PP, Heney NM, Grignon DJ, et al. Radiation with or without antiandrogen therapy in recurrent prostate cancer. N Engl J Med. 2017;376(5):417–28. doi:10.1056/NEJMoa1607529. This phase III trial demonstrated improved long-term outcomes with addition of bicalutamide to post-prostatectomy RT.
• Carrie C, Hasbini A, de Laroche G, Richaud P, Guerif S, Latorzeff I, et al. Salvage radiotherapy with or without short-term hormone therapy for rising prostate-specific antigen concentration after radical prostatectomy (GETUG-AFU 16): a randomised, multicentre, open-label phase 3 trial. Lancet Oncol. 2016;17(6):747–56. doi:10.1016/S1470-2045(16)00111-X. One of the first prospective randomized trials to demonstrate improved biochemical outcomes with the addition of ADT to salvage RT.
Laverdiere J, Nabid A, De Bedoya LD, Ebacher A, Fortin A, Wang CS, et al. The efficacy and sequencing of a short course of androgen suppression on freedom from biochemical failure when administered with radiation therapy for T2-T3 prostate cancer. J Urol. 2004;171(3):1137–40. doi:10.1097/01.ju.0000112979.97941.7f.
See WA, Tyrrell CJ, Group CEPCT. The addition of bicalutamide 150 mg to radiotherapy significantly improves overall survival in men with locally advanced prostate cancer. J Cancer Res Clin Oncol. 2006;132(Suppl 1):S7–16. doi:10.1007/s00432-006-0132-6.
Peeters ST, Heemsbergen WD, Koper PC, van Putten WL, Slot A, Dielwart MF, et al. Dose-response in radiotherapy for localized prostate cancer: results of the Dutch multicenter randomized phase III trial comparing 68 Gy of radiotherapy with 78 Gy. J Clin Oncol. 2006;24(13):1990–6. doi:10.1200/JCO.2005.05.2530.
Kuban DA, Tucker SL. Dong L, Starkschall G, Huang EH, Cheung MR et al. long-term results of the M. D. Anderson randomized dose-escalation trial for prostate cancer. Int J Radiat Oncol Biol Phys. 2008;70(1):67–74. doi:10.1016/j.ijrobp.2007.06.054.
Zietman AL, Bae K, Slater JD, Shipley WU, Efstathiou JA, Coen JJ, et al. Randomized trial comparing conventional-dose with high-dose conformal radiation therapy in early-stage adenocarcinoma of the prostate: long-term results from Proton Radiation Oncology Group/American College of Radiology 95-09. J Clin Oncol. 2010;28(7):1106–11. doi:10.1200/JCO.2009.25.8475.
Dearnaley DP, Sydes MR, Graham JD, Aird EG, Bottomley D, Cowan RA, et al. Escalated-dose versus standard-dose conformal radiotherapy in prostate cancer: first results from the MRC RT01 randomised controlled trial. Lancet Oncol. 2007;8(6):475–87. doi:10.1016/S1470-2045(07)70143-2.
Beckendorf V, Guerif S, Le Prise E, Cosset JM, Bougnoux A, Chauvet B, et al. 70 Gy versus 80 Gy in localized prostate cancer: 5-year results of GETUG 06 randomized trial. Int J Radiat Oncol Biol Phys. 2011;80(4):1056–63. doi:10.1016/j.ijrobp.2010.03.049.
Michalski JM, Moughan J, Purdy JA, et al. Initial results of a phase 3 randomized study of high dose 3DCRT/IMRT versus standard dose 3D-CRT/IMRT in patients treated for localized prostate cancer (RTOG 0126). Int J Radiat Oncol Biol Phys. 2014;90(5):1263.
Network NCC. Prostate cancer (Version 2.2017). https://www.nccn.org/professionals/physician_gls/pdf/prostate.pdf. Accessed March 1, 2017.
Horwitz EM, Bae K, Hanks GE, Porter A, Grignon DJ, Brereton HD, et al. Ten-year follow-up of radiation therapy oncology group protocol 92-02: a phase III trial of the duration of elective androgen deprivation in locally advanced prostate cancer. J Clin Oncol. 2008;26(15):2497–504. doi:10.1200/JCO.2007.14.9021.
Bolla M, de Reijke TM, Van Tienhoven G, Van den Bergh AC, Oddens J, Poortmans PM, et al. Duration of androgen suppression in the treatment of prostate cancer. N Engl J Med. 2009;360(24):2516–27. doi:10.1056/NEJMoa0810095.
Abdenour Nabid NC, André-Guy M, Bahary J-P, Souhami L, Duclos M, Vincent F, Vass S, Bahoric B, Archambault R, Lemaire C. High-risk prostate cancer treated with pelvic radiotherapy and 36 versus 18 months of androgen blockade: results of a phase III randomized study. J Clin Oncol. 2013;31(suppl 6; abstr 3).
Crook J, Ludgate C, Malone S, Perry G, Eapen L, Bowen J, et al. Final report of multicenter Canadian phase III randomized trial of 3 versus 8 months of neoadjuvant androgen deprivation therapy before conventional-dose radiotherapy for clinically localized prostate cancer. Int J Radiat Oncol Biol Phys. 2009;73(2):327–33. doi:10.1016/j.ijrobp.2008.04.075.
Pisansky TM, Hunt D, Gomella LG, Amin MB, Balogh AG, Chinn DM, et al. Duration of androgen suppression before radiotherapy for localized prostate cancer: radiation therapy oncology group randomized clinical trial 9910. J Clin Oncol. 2015;33(4):332–9. doi:10.1200/JCO.2014.58.0662.
• Zapatero A, Guerrero A, Maldonado X, Alvarez A, Gonzalez San Segundo C, Cabeza Rodriguez MA, et al. High-dose radiotherapy with short-term or long-term androgen deprivation in localised prostate cancer (DART01/05 GICOR): a randomised, controlled, phase 3 trial. Lancet Oncol. 2015;16(3):320–7. doi:10.1016/S1470-2045(15)70045-8. This phase III trial demonstrated improved outcomes with longer duration ADT compared to shorter duration ADT with dose-escalated RT.
Mirhadi AJ, Zhang Q, Hanks GE, Lepor H, Grignon DJ, Peters CA, et al. Effect of long-term hormonal therapy (vs short-term hormonal therapy): a secondary analysis of intermediate-risk prostate cancer patients treated on NRG oncology RTOG 9202. Int J Radiat Oncol Biol Phys. 2017;97(3):511–5. doi:10.1016/j.ijrobp.2016.11.002.
Muralidhar V, Regan MM, Werner L, Nakabayashi M, Evan CP, Bellmunt J, et al. Duration of androgen deprivation therapy for high-risk prostate cancer: application of randomized trial data in a tertiary referral cancer center. Clin Genitourin Cancer. 2016;14(4):e299–305. doi:10.1016/j.clgc.2015.12.008.
Son CH, Hamstra DA, Feng FY, Liauw SL. High-risk prostate cancer treated with dose-escalated RT: an analysis of hormonal therapy use and duration, and prognostic implications of PSA nadir </=0.2 to select men for short-term hormonal therapy. Am J Clin Oncol. 2014; doi:10.1097/COC.0000000000000161.
Williams S, Buyyounouski M, Kestin L, Duchesne G, Pickles T. Predictors of androgen deprivation therapy efficacy combined with prostatic irradiation: the central role of tumor stage and radiation dose. Int J Radiat Oncol Biol Phys. 2011;79(3):724–31. doi:10.1016/j.ijrobp.2009.11.044.
Crook J, Malone S, Perry G, Bahadur Y, Robertson S, Abdolell M. Postradiotherapy prostate biopsies: what do they really mean? Results for 498 patients. Int J Radiat Oncol Biol Phys. 2000;48(2):355–67.
Stock RG, Stone NN, Kao J, Iannuzzi C, Unger P. The effect of disease and treatment-related factors on biopsy results after prostate brachytherapy: implications for treatment optimization. Cancer. 2000;89(8):1829–34.
Stock RG, Stone NN, Cesaretti JA, Rosenstein BS. Biologically effective dose values for prostate brachytherapy: effects on PSA failure and posttreatment biopsy results. Int J Radiat Oncol Biol Phys. 2006;64(2):527–33. doi:10.1016/j.ijrobp.2005.07.981.
Liauw SL, Fricano J, Correa D, Weichselbaum RR, Jani AB. Dose-escalated radiation therapy for intermediate-risk prostate cancer: patient selection for androgen deprivation therapy using percentage of positive cores. Cancer. 2009;115(8):1784–90. doi:10.1002/cncr.24176.
Zumsteg ZS, Spratt DE, Pei I, Zhang Z, Yamada Y, Kollmeier M, et al. A new risk classification system for therapeutic decision making with intermediate-risk prostate cancer patients undergoing dose-escalated external-beam radiation therapy. Eur Urol. 2013;64(6):895–902. doi:10.1016/j.eururo.2013.03.033.
Epstein JI, Zelefsky MJ, Sjoberg DD, Nelson JB, Egevad L, Magi-Galluzzi C, et al. A contemporary prostate cancer grading system: a validated alternative to the Gleason score. Eur Urol. 2016;69(3):428–35. doi:10.1016/j.eururo.2015.06.046.
Tran PT, Hales RK, Zeng J, Aziz K, Salih T, Gajula RP, et al. Tissue biomarkers for prostate cancer radiation therapy. Curr Mol Med. 2012;12(6):772–87.
Khor LY, Bae K, Pollack A, Hammond ME, Grignon DJ, Venkatesan VM, et al. COX-2 expression predicts prostate-cancer outcome: analysis of data from the RTOG 92-02 trial. Lancet Oncol. 2007;8(10):912–20. doi:10.1016/S1470-2045(07)70280-2.
Nguyen PL, Martin NE, Choeurng V, Palmer-Aronsten B, Kolisnik T, Beard CJ, et al. Utilization of biopsy-based genomic classifier to predict distant metastasis after definitive radiation and short-course ADT for intermediate and high-risk prostate cancer. Prostate Cancer Prostatic Dis. 2017; doi:10.1038/pcan.2016.58.
Nguyen PL, Alibhai SM, Basaria S, D'Amico AV, Kantoff PW, Keating NL, et al. Adverse effects of androgen deprivation therapy and strategies to mitigate them. Eur Urol. 2015;67(5):825–36. doi:10.1016/j.eururo.2014.07.010.
Valicenti RK, Bae K, Michalski J, Sandler H, Shipley W, Lin A, et al. Does hormone therapy reduce disease recurrence in prostate cancer patients receiving dose-escalated radiation therapy? An analysis of radiation therapy oncology group 94-06. Int J Radiat Oncol Biol Phys. 2011;79(5):1323–9. doi:10.1016/j.ijrobp.2010.01.009.
Zumsteg ZS, Spratt DE, Pei X, Yamada Y, Kalikstein A, Kuk D, et al. Short-term androgen-deprivation therapy improves prostate cancer-specific mortality in intermediate-risk prostate cancer patients undergoing dose-escalated external beam radiation therapy. Int J Radiat Oncol Biol Phys. 2013;85(4):1012–7. doi:10.1016/j.ijrobp.2012.07.2374.
Feng FY, Blas K, Olson K, Stenmark M, Sandler H, Hamstra DA. Retrospective evaluation reveals that long-term androgen deprivation therapy improves cause-specific and overall survival in the setting of dose-escalated radiation for high-risk prostate cancer. Int J Radiat Oncol Biol Phys. 2013;86(1):64–71. doi:10.1016/j.ijrobp.2012.11.024.
D'Amico AV, Chen MH, de Castro M, Loffredo M, Lamb DS, Steigler A, et al. Surrogate endpoints for prostate cancer-specific mortality after radiotherapy and androgen suppression therapy in men with localised or locally advanced prostate cancer: an analysis of two randomised trials. Lancet Oncol. 2012;13(2):189–95. doi:10.1016/S1470-2045(11)70295-9.
Zelefsky MJ, Chou JF, Pei X, Yamada Y, Kollmeier M, Cox B, et al. Predicting biochemical tumor control after brachytherapy for clinically localized prostate cancer: the Memorial Sloan-Kettering Cancer Center experience. Brachytherapy. 2012;11(4):245–9. doi:10.1016/j.brachy.2011.08.003.
• Morris WJ, Tyldesley S, Rodda S, Halperin R, Pai H, McKenzie M, et al. Androgen suppression combined with elective nodal and dose escalated radiation therapy (the ASCENDE-RT trial): an analysis of survival endpoints for a randomized trial comparing a low-dose-rate brachytherapy boost to a dose-escalated external beam boost for high- and intermediate-risk prostate cancer. Int J Radiat Oncol Biol Phys. 2016; doi:10.1016/j.ijrobp.2016.11.026. This randomized trial demonstrated improved biochemical outcomes with brachtherapy boost compared to external beam RT in intermediate and high-risk patients receiving combined ADT/RT.
Kishan AU, Shaikh T, Wang PC, Reiter RE, Said J, Raghavan G, et al. Clinical outcomes for patients with Gleason score 9-10 prostate adenocarcinoma treated with radiotherapy or radical prostatectomy: a multi-institutional comparative analysis. Eur Urol. 2016; doi:10.1016/j.eururo.2016.06.046.
Keyes M, Merrick G, Frank SJ, Grimm P, Zelefsky MJ. American Brachytherapy Society task group report: use of androgen deprivation therapy with prostate brachytherapy-a systematic literature review. Brachytherapy. 2017; doi:10.1016/j.brachy.2016.11.017.
Savdie R, Horvath LG, Benito RP, Rasiah KK, Haynes AM, Chatfield M, et al. High Gleason grade carcinoma at a positive surgical margin predicts biochemical failure after radical prostatectomy and may guide adjuvant radiotherapy. BJU Int. 2012;109(12):1794–800. doi:10.1111/j.1464-410X.2011.10572.x.
Swanson GP, Hussey MA, Tangen CM, Chin J, Messing E, Canby-Hagino E, et al. Predominant treatment failure in postprostatectomy patients is local: analysis of patterns of treatment failure in SWOG 8794. J Clin Oncol. 2007;25(16):2225–9. doi:10.1200/JCO.2006.09.6495.
Hurwitz MD, Harris J, Sartor O, Xiao Y, Shayegan B, Sperduto PW, et al. Adjuvant radiation therapy, androgen deprivation, and docetaxel for high-risk prostate cancer postprostatectomy: results of NRG oncology/RTOG study 0621. Cancer. 2017; doi:10.1002/cncr.30620.
Tendulkar RD, Agrawal S, Gao T, Efstathiou JA, Pisansky TM, Michalski JM, et al. Contemporary update of a multi-institutional predictive nomogram for salvage radiotherapy after radical prostatectomy. J Clin Oncol. 2016; doi:10.1200/JCO.2016.67.9647.
Keating NL, O'Malley AJ, Smith MR. Diabetes and cardiovascular disease during androgen deprivation therapy for prostate cancer. J Clin Oncol. 2006;24(27):4448–56. doi:10.1200/JCO.2006.06.2497.
Nguyen PL, Je Y, Schutz FA, Hoffman KE, Hu JC, Parekh A, et al. Association of androgen deprivation therapy with cardiovascular death in patients with prostate cancer: a meta-analysis of randomized trials. JAMA. 2011;306(21):2359–66. doi:10.1001/jama.2011.1745.
Nead KT, Gaskin G, Chester C, Swisher-McClure S, Dudley JT, Leeper NJ, et al. Androgen deprivation therapy and future Alzheimer’s disease risk. J Clin Oncol. 2016;34(6):566–71. doi:10.1200/JCO.2015.63.6266.
Tsai HT, Keating NL, Van Den Eeden SK, Haque R, Cassidy-Bushrow AE, Ulcickas Yood M, et al. Risk of diabetes among patients receiving primary androgen deprivation therapy for clinically localized prostate cancer. J Urol. 2015;193(6):1956–62. doi:10.1016/j.juro.2014.12.027.
Ehdaie B, Atoria CL, Gupta A, Feifer A, Lowrance WT, Morris MJ, et al. Androgen deprivation and thromboembolic events in men with prostate cancer. Cancer. 2012;118(13):3397–406. doi:10.1002/cncr.26623.
Klil-Drori AJ, Yin H, Tagalakis V, Aprikian A, Azoulay L. Androgen deprivation therapy for prostate cancer and the risk of venous thromboembolism. Eur Urol. 2016;70(1):56–61. doi:10.1016/j.eururo.2015.06.022.
Locke JA, Dal Pra A, Supiot S, Warde P, Bristow RG. Synergistic action of image-guided radiotherapy and androgen deprivation therapy. Nat Rev Urol. 2015;12(4):193–204. doi:10.1038/nrurol.2015.50.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Greg Kauffmann and Stanley L. Liauw each declare no potential conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Prostate Cancer
Rights and permissions
About this article
Cite this article
Kauffmann, G., Liauw, S.L. The use of Hormonal Therapy to Augment Radiation Therapy in Prostate Cancer: An Update. Curr Urol Rep 18, 50 (2017). https://doi.org/10.1007/s11934-017-0698-3
Published:
DOI: https://doi.org/10.1007/s11934-017-0698-3