Abstract
Purpose of Review
This study aims to systematically review and summarise the efficacy and safety of yoga for osteoarthritis. Medline (through PubMed), Scopus, and the Cochrane Library were searched through April 2018 for randomised controlled trials of yoga for osteoarthritis. Primary outcomes were pain intensity, function, and quality of life; secondary outcomes were mental health and safety. Risk of bias was assessed using the Cochrane tool and quality of evidence through GRADE.
Recent Findings
Nine trials including 640 individuals with mainly lower extremity osteoarthritis aged 50–80 years were identified, with 80.3% female participants (median). Meta-analyses revealed very low–quality evidence for the effects of yoga on pain (vs. exercise: standardised mean difference (SMD) = − 1.07; 95%CI − 1.92, − 0.21; p = 0.01; vs. non-exercise: SMD = − 0.75; 95%CI − 1.18, − 0.31; p < 0.001), physical function (vs. exercise: SMD = 0.80; 95%CI 0.36; 1.24; p < 0.001; vs. non-exercise: SMD = 0.60; 95%CI 0.30, 0.98; p < 0.001), and stiffness (vs. exercise: SMD = − 0.92; 95%CI − 1.69, − 0.14; p = 0.008; vs. non-exercise: SMD = − 0.76; 95%CI − 1.26, − 0.26; p = 0.003) in individuals with knee osteoarthritis. Effects were not robust against potential methodological bias. No effects were found for quality of life, and depression, or for hand osteoarthritis. Safety was rarely reported.
Summary
The findings of this meta-analysis indicate that yoga may be effective for improving pain, function, and stiffness in individuals with osteoarthritis of the knee, compared to exercise and non-exercise control groups. Due to the low methodological quality and potential risk of bias, only a weak recommendation can be made at this time for the use of yoga in adults with osteoarthritis of the knee.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Osteoarthritis is characterised by damage to the synovial joint organ [1]. The most commonly affected joints include the knees, and about one in four adults over 55 years of age reported a significant knee pain episode in the last year. The pain and stiffness resulting from osteoarthritis impair function in patients’ basic activities of daily living, severely affecting their quality of life [2, 3]. Conservative therapeutic approaches to treating osteoarthritis rely mainly on non-pharmacological and/or pharmacological therapy [4]. However, costs and limited adherence to continued physical therapy and potential side effects of long-term pharmacological therapy limit their use.
The prescription of regular exercise is a first-line treatment to reduce pain and improve function [4]. Despite tremendous research activity in the field of osteoarthritis, there is little knowledge about the most effective type, frequency, and dosage of exercise interventions, including yoga [5, 6]. Yoga, is a form of mind-body therapy originating in ancient India and in the Western context constitutes a number of practices, including physical practices (postures, asanas), breath regulation techniques (pranayama), mental practices (meditation, mindfulness), and relaxation with some yoga styles also incorporating discussions of yoga philosophy and lifestyle advice [7]. Yoga has become a popular means of achieving and maintaining well-being and health [8]. The prevalence of yoga use is increasing worldwide, with the 12-month prevalence of yoga practice in the USA in 2012 being 13.2%, compared to only 5.1% in 2002 [6, 9]. The prevalence and burden of osteoarthritis disorders, the reported beneficial effects of yoga practice, and increased publication of clinical trials indicate that a systematic review is required. The aim of this review was to systematically assess and meta-analysis efficacy and safety of randomised controlled trials of yoga in individuals with osteoarthritis. This systematic review was planned and carried out in accordance with the following guidelines: PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) [10] and the recommendations of the Cochrane Collaboration [11].
Eligibility Criteria
Types of Studies
Randomised controlled trials (RCTs), cluster-randomised trials, and randomised cross-over studies. Articles published in any languages were considered eligible.
Types of Participants
To be eligible for the review, studies were required to include adults diagnosed with osteoarthritis, i.e. all studies on patients with osteoarthritis of the knee, hip, hand, feet, and spine were considered. No restrictions were applied regarding age, gender, and comorbidities, and diagnostic criteria utilised, but subgroup analyses were conducted for patients diagnosed using the American College of Rheumatology (ACR) diagnostic criteria.
Types of Interventions
Studies that assessed yoga as the main intervention were included. No restrictions regarding yoga style, length, or frequency of the intervention period were applied; multicomponent interventions employing postures, breathing, and/or meditation, as well as studies employing single components only, were acceptable. Differences between various types of experimental interventions were examined in subgroup analyses if applicable. When co-interventions (such as pharmacotherapy) were applied, studies were eligible only if all participants in all groups received the same co-interventions.
Types of Control Interventions
Studies comparing yoga to exercise or any non-exercise control (e.g. no treatment, usual care, attention-control, or non-exercise active control interventions) were eligible. Separate meta-analyses were conducted for different control conditions if applicable.
Types of Outcome Measures
For inclusion in this review, RCTs had to assess at least one primary outcome measured using validated generic or disease-specific self- or clinician-rated scales:
-
Pain intensity
-
Function or disability, as measured using validated scales, or physical function tests
-
Quality of life
Secondary outcomes included:
-
Mental health, e.g. depression or anxiety
-
Safety, assessed as the number of participants with adverse events, adverse effects, or side effects
Search Methods
The following electronic databases were searched from their inception through 24 April, 2018: Medline (through PubMed), Scopus, and the Cochrane Library. The literature search was constructed around search terms for “yoga” and “osteoarthritis”. For PubMed, the following search strategy was used: ((Osteoarthritis[MeSH Terms] OR Arthritis[MeSH Terms] OR Osteoarthritis[Title/Abstract] OR Osteoarthr*[Title/Abstract] OR Arthrosis[Title/Abstract] OR Arthritis[Title/Abstract]) AND (Yoga[MeSH Terms] OR yoga[Title/Abstract] OR yogic[Title/Abstract] OR asana[Title/Abstract] OR pranayama[Title/Abstract] OR dhyana[Title/Abstract] OR yogasana[Title/Abstract] OR meditation[Title/Abstract] OR “surya namaskar” [Title/Abstract])). The search strategy was adapted for each database as necessary, and a filter for randomised controlled trials was added (“randomized controlled trial”[Publication Type] OR “clinical trial”[Publication Type] OR randomly[Title/Abstract] OR randomised[Title/Abstract] OR randomized[Title/Abstract] OR groups[Title/Abstract] OR trial[Title/Abstract] OR control[Title/Abstract] OR controlled[Title/Abstract]). In addition, hand searches were conducted on our own extensive database [12], reference lists of identified original articles or reviews, and table of contents of the International Journal of Yoga Therapy, the Journal of Yoga & Physical Therapy, and the International Scientific Yoga Journal SENSE.
Abstracts identified during the database and hand searches were screened by two review authors (RL, HC) independently, with potentially eligible articles read in full by two review authors (RL, HC) to determine whether they met the eligibility criteria. Disagreements were discussed with a third review author until consensus was reached. If necessary, additional information was obtained from the study authors.
Data Extraction and Management
Data on participants (e.g. age, gender, diagnosis), methods (e.g. randomisation, allocation concealment), interventions (e.g. yoga style, frequency, and duration), control interventions (e.g. type, frequency, duration), outcomes (e.g. outcome measures, assessment time points), and results were independently extracted by two review authors (RL, HC) using an a priori designed data extraction form. Discrepancies were discussed with a third review author until a consensus was reached. If necessary, study authors were contacted for additional information.
Risk of Bias in Individual Studies
Two review authors (RL, HC) independently assessed risk of bias on the following domains: selection bias (random sequence generation, allocation concealment), performance bias (blinding of participants and personnel), detection bias (blinding of outcome assessment), attrition bias (incomplete outcome data), reporting bias (selective reporting), and other bias using the Cochrane risk of bias tool [11]. Risk of bias was assessed as (1) low risk of bias, (2) unclear, or (3) high risk of bias [11]. Discrepancies were discussed with a third review author until a consensus was reached.
Assessment of Overall Effect Size
Meta-analyses were conducted using Review Manager 5 software (Version 5.3, The Nordic Cochrane Centre, Copenhagen, Denmark) by a random-effects model if at least two studies assessing this specific outcome were available.
For continuous outcomes, mean differences (MD) or standardised mean differences (SMD) with 95% confidence intervals (CI) were calculated depending on the outcome measure. Where no standard deviations were available, they were calculated from standard errors, confidence intervals, or t values [11], or attempts were made to obtain the missing data from the trial authors by email. Cohen’s categories were used to evaluate the magnitude of the overall effect size with SMDs between 0.2 and 0.5 categorised as small; 0.5 and 0.8 as medium, and above 0.8 as large effect sizes [13].
For the dichotomous outcome safety, odds ratios (RR) with 95% CI were calculated by dividing the odds of an adverse event in the intervention group (i.e. the number of participants with the respective type of adverse event divided by the number of participants without the respective type of adverse event) by the odds of an adverse event in the control group [11].
Assessment of Heterogeneity
Statistical heterogeneity between studies was analysed using the I2 statistics, and the magnitude of heterogeneity was categorised as (1) I2 = 0–24%: low heterogeneity; I2 = 25–49%: moderate heterogeneity; I2 = 50–74%: substantial heterogeneity; and I2 = 75–100%: considerable heterogeneity [11]. The chi2 test was used to assess whether differences in results were compatible with chance alone. Given the low power of this test when only a few studies or studies with low sample size are included in a meta-analysis, a p value ≤ 0.10 was considered to indicate significant heterogeneity [11].
Subgroup and Sensitivity Analyses
Subgroup analyses were planned according to the type of osteoarthritis (osteoarthritis of the knee vs other) and the diagnostic criteria (ACR vs other). To test the robustness of significant results, sensitivity analyses were conducted for studies with low risk of bias on the following domains: selection bias (random sequence generation and allocation concealment), detection bias (blinding of outcome assessment), and attrition bias (incomplete outcome data). If statistical heterogeneity was present in the respective meta-analysis, subgroup, and sensitivity analyses were also used to explore possible reasons for heterogeneity.
Quality of Evidence
The quality of evidence for each outcome was examined according to the Grading of Recommendations Assessment, Development and Evaluation (GRADE) recommendations based on the studies’ methodological quality and the confidence in the results. The evidence quality was rated as high, moderate, low, or very low based on the limitations of the respective studies, the inconsistency between the results of the respective studies, the indirectness of the evidence, the imprecision of the findings, the risk of publication bias, and the risk of other bias [14]. IF evidence obtained from RCTs is initially graded as high quality, this rating can be downgraded due to the risk of methodological bias, heterogeneity, differences in study characteristics between studies, wide confidence intervals, and risk of publication bias (see below).
Risk of Bias across Studies
Since less than 10 studies were included in each meta-analysis, publication bias was assessed.
Results
Literature Search
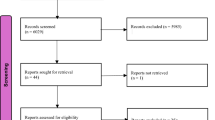
The results of the literature search and screening process are summarised in Fig. 1. The literature search returned 374 records. Of 258 non-duplicate records, 235 were excluded because they did not match the inclusion criteria. Twenty-four full-text articles were assessed and excluded because they had no control group (N = 4) [15,16,17,18], because they were not randomised (N = 4) [19,20,21,22], or because they did not include a non-yoga control group (N = 1) [23]. Finally, fifteen publications were included, reporting on a total of nine RCTs [24,25,26,27,28,29,30,31,32,33,34,35,36,37,38]. One trial included individuals with osteoarthritis and rheumatoid arthritis, and no separate data were provided by the trial authors when requested [26]; as such, this trial was not included in the meta-analyses.
Study Characteristics
Characteristics of the sample, interventions, outcome assessment, and results are shown in Table 1. Of the nine RCTs, seven originated in the USA [24,25,26,27, 32,33,34,35,36, 38], and one each in Canada [37] and India [28,29,30,31]. Five trials included participants with OA of the knee [24, 26, 28,29,30,31,32,33, 37], with four out of five using ACR criteria [24, 28,29,30,31,32,33, 37], two trials included participants with OA of lower extremities [25, 27, 34, 36], one trial included participants with OA of the hand using ACR criteria [38], and another trial did not specify the type of OA [35]. The systematic review provided a total of 640 patients (median study size of 54.5), with 80.3% female participants (median, range 56–100%), and age ranging from 50 to 80 years.
Four of the trials applied yoga in the Hatha yoga tradition [24, 26, 28,29,30,31,32,33], one trial used Iyengar yoga [38], three trials used chair yoga [25, 27, 34,35,36], and one applied a biomechanically based yoga intervention [37]. All but one studies on yoga interventions included postures [24,25,26,27,28,29,30,31,32,33,34, 36,37,38], and one study used a sitting meditation only [35]. Duration of the yoga interventions ranged from 8 to 12 weeks (median 8 weeks), with a total time of supervised yoga practice of 660 min (range 80–960 min), and four studies applied additional home practice [24, 26, 28,29,30,31,32,33]. One trial reported a co-intervention applied in both groups, namely transcutaneous nerve stimulation (TENS) and ultrasound [28,29,30,31].
Regarding control interventions, three studies applied an exercise control [28,29,30,31,32, 37], and 8 studies applied non-exercise controls, including waiting list control groups [24, 33], usual care [26, 38], educational control groups [27, 32, 34, 36], Reiki [35], and meditation [37].
All but one trial [26] measured pain intensity (e.g. by visual analogue scales (VAS), Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC), or McGill pain index), and function [38]. Five trials examined the quality of life [24, 26, 28,29,30,31,32,33, 37], and seven trials measured mental health outcomes such as anxiety and depression [25,26,27,28,29,30,31,32, 34,35,36,37]. Only four studies reported safety outcomes, including adverse events [26, 32], side effects [24, 33], and dropouts due to adverse events [28,29,30,31].
Risk of Bias in Individual Studies
The results of the risk of bias analyses can be found in Table 2. Results indicate that risk of bias was mixed, with six trials reporting adequate random sequence generation [24,25,26,27,28,29,30,31,32,33, 36, 37], but only one trial reporting adequate allocation concealment as well [26]. No trial had a low risk of bias for blinding of participants or personnel, or outcome assessment (for primary outcomes). All but three trials [34, 35, 38] had a low risk of attrition bias, but the risk of selective reporting was low in only two trials [26, 32]. All trials had a high risk of other bias, including but not limited to undeclared potential conflicts of interest, inadequate statistical testing, or inconsistencies between multiple publications of the same study.
Osteoarthritis of the Knee—Assessment of the Overall Effect
Significant effects were found for pain intensity for yoga compared to non-exercise controls based on four studies (SMD = − 0.75, 95%CI − 1.18, − 0.31, p < 0.001, I2 = 51%, chi2 = 6.07, p = 0.11), and three studies for the comparison yoga vs. exercise controls (SMD = − 1.07, 95%CI − 1.92, − 0.21, p = 0.01, I2 = 87%, chi2 = 15.58, p < 0.001) (Fig. 2; Table 3). When only studies with osteoarthritis of the knee according to ACR diagnosis were included, the effects remained significant. Effects on pain intensity were, however, not robust against selection bias (no studies left), or performance and detection bias, but robust against attrition bias for yoga vs. non-exercise controls based on one study [32].
Significant effects were found for physical function (via self-report) for yoga compared to non-exercise controls based on four studies (SMD = 0.60, 95%CI 0.30, 0.98, p < 0.001, I2 = 28%, chi2 = 4.14, p = 0.25), and two studies for the comparison yoga vs. exercise controls (SMD = 0.80, 95%CI 0.36, 1.24, p < 0.001, I2 = 0%, chi2 = 2.73, p = 0.43) (Table 3). When only studies with osteoarthritis of the knee according to ACR diagnosis were included, the effects remained significant. Effects on physical function, however, were not robust against selection bias (no studies left), or performance and detection bias, but robust against attrition bias (only 1 study in each comparison [32]).
Meta-analyses revealed no significant effect regarding quality of life, based on four studies for the comparison yoga vs. non-exercise controls (SMD 0.21, 95%CI − 0.20, 0.62, p = 0.31) and two studies for the comparison yoga vs. exercise controls (SMD 0.34, 95%CI − 0.10, 0.78, p = 0.13) Table 3.
Significant effects were found for stiffness for yoga compared to non-exercise controls based on two studies (SMD = − 0.76, 95%CI − 1.26, − 0.26, p = 0.003, I2 = 23%, chi2 = 1.31, p = 0.25), and two studies for the comparison yoga vs. exercise controls (SMD = − 0.92, 95%CI − 1.69, − 0.14, p = 0.008, I2 = 86%, chi2 = 7.02, p = 0.02) (Table 3). In all studies, osteoarthritis of the knee was diagnosed according to ACR criteria. Effects on stiffness were not robust against selection bias (no studies left), or performance and detection bias, but robust against attrition bias (only 1 study in each comparison [32]).
Meta-analyses further revealed no significant effect regarding depression, based on five studies for the comparison yoga vs. non-exercise controls (SMD − 0.18, 95%CI − 0.48, 0.12, p = 0.24), and two studies for the comparison yoga vs. exercise controls (SMD − 0.28, 95%CI − 0.72, 0.16, p = 0.22) Table 3.
The quality of evidence for pain, physical function, and stiffness were considered very low, i.e. a weak recommendation for yoga in individuals with osteoarthritis of the knee can be made.
Osteoarthritis of the Knee—Safety
Six studies reported some safety information; however, only two reported adverse events rather than side effects. Moonaz et al. [26] reported adverse events, and seven adverse events (of which several need to be considered serious adverse events, including two cases of cancer, and one rheumatoid arthritis diagnosis) in the yoga group were considered unrelated to the intervention, and no adverse events occurred in the control group. A report by Cheung et al. [32] only mentioned three non-serious adverse events in the exercise control group, yet health-related withdrawals in the flow diagram indicate that adverse events might have been under-reported. Another study by Cheung et al. [24, 33] reported that no side effects of yoga occurred but did not examine adverse events for the whole sample. Park et al. [25, 27, 36] reported no side effects, i.e. no adverse events during the intervention itself. Finally, studies by Ebnezar et al. [28,29,30,31], Kuntz et al. [37], and Park et al. [34] did not specifically examine safety but reported several dropouts in the study due to possible adverse events (respiratory tract infections, pneumonia, “unrelated health diagnosis”), yet they lacked detail and comprehensiveness.
Osteoarthritis of the Hand
Only one trial examined the effects of yoga on osteoarthritis of the hand [38]. Twenty-five patients were randomised to either Iyengar yoga for 10 weeks (once per week, 60 min each), or usual care (not further specified) in terms of pain via a visual analogue scale, and disability via the Health Assessment Questionnaire Disability Index. The authors found significant effects only on pain during activity but not on pain at rest or disability. Risk of bias was unclear or high for each domain. No safety information was reported.
Summary
Summary of Results
This systematic review and meta-analysis found that yoga may be beneficial for osteoarthritis of the knee with regard to pain intensity, physical function, and stiffness. Effect sizes for these outcomes were moderate to large, with lower confidence boundaries in the small to moderate range. None of the effects were not robust against potential bias, and no effects were found for yoga with regard to the quality of life or depression in individuals with knee osteoarthritis. For osteoarthritis of the hand, only one trial was available, with no consistent benefits beyond usual care. Only very limited safety information was reported.
Comparison to Prior Reviews
No systematic review has been conducted on the effects of yoga for osteoarthritis. Two current Cochrane reviews on the effects of exercise for osteoarthritis of the knee [39], and osteoarthritis of the hand [40] had included yoga in the search terms, but did not include any yoga trial due to the lack of trials at the time of the search [39], due to the lack of non-exercise control groups [39], or due to methodological issues [40].
Another systematic review has examined the effects of yoga on rheumatic conditions, including osteoarthritis, rheumatoid arthritis, fibromyalgia, and carpal tunnel [41]. The review included only three trials on yoga for osteoarthritis—compared to nine in the current version, and the authors concluded that the overall quality of evidence was very low, and that only a weak recommendation could be made for the use of yoga in osteoarthritis. While the authors of the previous review were not able to conduct a meta-analysis, the increased number of publications in the last few years allowed for a meta-analysis at this time point, and effect estimates could be provided. Overall, our meta-analysis found benefits of yoga over exercise, and non-exercise controls including waiting list controls, usual care, and educational interventions. While the effect sizes were moderate to large on average, they had huge confidence intervals ranging from small to very large effects, and effects were not robust against bias.
How Yoga Might Work
Exercise interventions, in general, are considered beneficial for osteoarthritis of the knee [39], and similar mechanisms might come into effect with yoga. Yoga, for example, might improve leg muscle strength [42], especially muscles supporting the knee joint, which in turn will decrease joint load [43]. Improved muscle function might also increase microcirculation, and counter the progression of osteoarthritis [44]. Yoga sequences include a variety of postures to increase the range of motion, similar to static stretching, which might improve stiffness, and joint function [45]. Beyond physical activity, yoga also often incorporates breathing and relaxation exercises. These exercises stimulate the parasympathetic nervous system [46, 47], can help break the stress–pain cycle involved in chronic pain conditions, and can also facilitate the release of muscle tension and counter the muscle tightening that often occurs around vulnerable joints [48].
Finally, yoga exercises are considered effective for well-being and depression [49, 50]; however, no such effects were found in this meta-analysis, which might be due to the small sample size.
Implications for Practice
Only a weak recommendation can be given for the use of yoga as a treatment option for osteoarthritis. However, given the relatively low risk of yoga interventions [51] and their high popularity [6], they can be recommended for patients with preference towards yoga interventions, or patients not adhering to other types of physical activity. Several types of yoga seem to be effective, and both physically based interventions and more meditative approaches appeared effective in the included studies. However, some rather vigorous styles that are currently popular (e.g. hot yoga, yin yoga, and power yoga) have not been formally evaluated and may not be appropriate for this population. The dose of yoga varied considerably among studies. Regular engagement in physical activity at a minimum of three times per week is considered necessary to increase physical fitness and confer health benefits among most forms of exercise [52]. It is unclear what the minimum dose and duration of practice may be for yoga because no studies have directly evaluated such dose-response relationship and few studies have reported on class attendance. It is important to note that the most common styles of yoga represented in the literature focus on anatomical alignment and/or slow and gentle movements. For individuals with osteoarthritis, especially for sedentary or older patients with comorbidities, particular attention should be given to the proper modification of postures to address individual limitations and ensure safety. Thus, yoga therapists experienced in working with individuals with osteoarthritis and/or having a medical background should be preferred; and the yoga treatment should be planned in close consultation with the patient’s rheumatologist or general physician to avoid exacerbation of symptoms.
Implications for Research
The results of this review are limited by the low internal validity of the available data. Incomplete reporting, especially of allocation concealment, as well as the high risk of selective reporting and other bias, limits the internal robustness of the findings. Future reporting of clinical yoga trials should closely follow standard reporting guidelines, such as CONSORT (Consolidated Standards of Reporting Trials) [53] to improve their methodological transparency. The additional use of reporting guidelines for intervention content [54] and safety [55] in future research will aid the implementation of research into practice, by providing clinicians and yoga therapists with clear detail on the type and amount of yoga considered effective in osteoarthritis management. Prospective registration in clinical trial registries before patient recruitment will reduce selective reporting. Researchers are recommended to disclose the complete study protocol in every related publication, and journal editors are recommended not to accept any articles for publication that do not adhere to commonly accepted registration recommendations.
Interestingly, in one included trial, sitting meditation without any physical activity component improved function in osteoarthritis patients [35]. This hints to mechanisms of action of yoga in the condition beyond exercise. Future head-to-head comparisons of different yoga interventions focusing more on physical activity or meditation and breathing will help to find the most effective yoga intervention for osteoarthritis.
Finally, pragmatic trials are needed to examine the effectiveness of yoga in everyday patients to reflect real clinical practice.
Limitations
This systematic review has several limitations. Firstly, the paucity of trials in general, and the paucity of trials for specific osteoarthritis sub-forms in particular, rendered in-depth meta-analyses impossible. Secondly, several of the included trials did not apply standard diagnostic criteria (or did not report the use of those), such as the ACR criteria. Furthermore, only two out of nine trials were prospectively registered, and three trials were registered retrospectively, inducing potential reporting bias in favour of studies with significant results, and outcome measures. The included trials were also potentially biased, starting from unclear allocations concealment, to lack of blinding or lack of attempts to address it, reporting, and other bias during conduct, analyses, and publication of the studies. Future studies also need to improve reporting of trials and adherence to standard reporting guidelines (e.g. CONSORT) [56].
Conclusion
The findings of this meta-analysis indicate that yoga may be effective for improving pain, function, and stiffness in individuals with osteoarthritis of the knee, compared to exercise and non-exercise control groups. Due to the low methodological quality and potential risk of bias, only a weak recommendation can be made at this time for the use of yoga to improve pain and function in individuals with osteoarthritis of the knee.
References
Altman R, Asch E, Bloch D, Bole G, Borenstein D, Brandt K, et al. Development of criteria for the classification and reporting of osteoarthritis. Classification of osteoarthritis of the knee. Diagnostic and Therapeutic Criteria Committee of the American Rheumatism Association. Arthritis Rheum. 1986;29(8):1039–49.
Reginster JY. The prevalence and burden of arthritis. Rheumatology (Oxford). 2002;41(Supp 1):3–6.
Pereira D, Peleteiro B, Araujo J, Branco J, Santos RA, Ramos E. The effect of osteoarthritis definition on prevalence and incidence estimates: a systematic review. Osteoarthr Cartil. 2011;19(11):1270–85. https://doi.org/10.1016/j.joca.2011.08.009.
Zhang W, Doherty M, Arden N, Bannwarth B, Bijlsma J, Gunther KP, et al. EULAR evidence based recommendations for the management of hip osteoarthritis: report of a task force of the EULAR Standing Committee for International Clinical Studies Including Therapeutics (ESCISIT). Ann Rheum Dis. 2005;64(5):669–81. https://doi.org/10.1136/ard.2004.028886.
Lapane KL, Sands MR, Yang S, McAlindon TE, Eaton CB. Use of complementary and alternative medicine among patients with radiographic-confirmed knee osteoarthritis. Osteoarthr Cartil. 2012;20(1):22–8. https://doi.org/10.1016/j.joca.2011.10.005.
Cramer H, Ward L, Steel A, Lauche R, Dobos G, Zhang Y. Prevalence, patterns, and predictors of yoga use: results of a U.S. nationally representative survey. Am J Prev Med. 2016;50(2):230–5. https://doi.org/10.1016/j.amepre.2015.07.037.
Feuerstein G. The yoga tradition. Prescott: Hohm Press; 1998.
Barnes PM, Bloom B, Nahin RL. Complementary and alternative medicine use among adults and children: United States, 2007. Natl Health Stat Report 2008(12):1–23.
Clarke TC, Black LI, Stussman BJ, Barnes PM, Nahin RL. Trends in the use of complementary health approaches among adults: United States, 2002-2012. Natl Health Stat Report 2015(79):1–16.
Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ. 2009;339:b2535. https://doi.org/10.1136/bmj.b2535.
Higgins JPT, Green S. Cochrane handbook for systematic reviews of interventions. John Wiley & Sons Ltd: West Sussex; 2008.
Cramer H, Lauche R, Dobos G. Characteristics of randomized controlled trials of yoga: a bibliometric analysis. BMC Complement Altern Med. 2014;14:328. https://doi.org/10.1186/1472-6882-14-328.
Cohen J. Statistical power analysis for the behavioral sciences. Hillsdale, NJ: Lawrence Erlbaum Associates; 1998.
Guyatt GH, Oxman AD, Vist GE, Kunz R, Falck-Ytter Y, Alonso-Coello P, et al. GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ. 2008;336(7650):924–6. https://doi.org/10.1136/bmj.39489.470347.AD.
Brenneman EC, Kuntz AB, Wiebenga EG, Maly MR. A yoga strengthening program designed to minimize the knee adduction moment for women with knee osteoarthritis: a proof-of-principle cohort study. PLoS One. 2015;10(9):e0136854. https://doi.org/10.1371/journal.pone.0136854.
Bukowski EL, Conway A, Glentz LA, Kurland K, Galantino ML. The effect of iyengar yoga and strengthening exercises for people living with osteoarthritis of the knee: a case series. Int Q Community Health Educ. 2006;26(3):287–305. https://doi.org/10.2190/IQ.26.3.f.
Park J, McCaffrey R. Chair yoga: benefits for community-dwelling older adults with osteoarthritis. J Gerontol Nurs. 2012;38(5):12–22; quiz 4-5. https://doi.org/10.3928/00989134-20120410-01.
Taibi DM, Vitiello MV. A pilot study of gentle yoga for sleep disturbance in women with osteoarthritis. Sleep Med. 2011;12(5):512–7. https://doi.org/10.1016/j.sleep.2010.09.016.
Bedekar N, Prabhu A, Shyam A, Sancheti K, Sancheti P. Comparative study of conventional therapy and additional yogasanas for knee rehabilitation after total knee arthroplasty. Int J Yoga. 2012;5(2):118–22. https://doi.org/10.4103/0973-6131.98226.
Ghasemi GA, Golkar A, Marandi SM. Effects of hata yoga on knee osteoarthritis. Int J Prev Med. 2013;4(Suppl 1):S133–8.
Krejci M. Yoga training application in overweight control of seniors with arthritis/osteoarthritis. Fizjoterapia. 2011;19(2):3–8. https://doi.org/10.2478/v10109-011-0014-6.
Nambi GS, Shah AA. Additional effect of iyengar yoga and EMG biofeedback on pain and functional disability in chronic unilateral knee osteoarthritis. Int J Yoga. 2013;6(2):123–7. https://doi.org/10.4103/0973-6131.113413.
Buchanan DT, Vitiello MV, Bennett K. Feasibility and efficacy of a shared yoga intervention for sleep disturbance in older adults with osteoarthritis. J Gerontol Nurs. 2017;43:1–10. https://doi.org/10.3928/00989134-20170405-01.
Cheung C, Wyman JF, Savik K. Adherence to a yoga program in older women with knee osteoarthritis. J Aging Phys Act. 2016;24(2):181–8. https://doi.org/10.1123/japa.2015-0048.
McCaffrey R, Park J, Newman D. Chair yoga: feasibility and sustainability study with older community-dwelling adults with osteoarthritis. Holist Nurs Pract. 2017;31(3):148–57. https://doi.org/10.1097/hnp.0000000000000184.
Moonaz SH, Bingham CO 3rd, Wissow L, Bartlett SJ. Yoga in sedentary adults with arthritis: effects of a randomized controlled pragmatic trial. J Rheumatol. 2015;42(7):1194–202. https://doi.org/10.3899/jrheum.141129.
Park J, McCaffrey R, Newman D, Liehr P, Ouslander JG. A pilot randomized controlled trial of the effects of chair yoga on pain and physical function among community-dwelling older adults with lower extremity osteoarthritis. J Am Geriatr Soc. 2017;65(3):592–7. https://doi.org/10.1111/jgs.14717.
Ebnezar J, Yogitha B. Effectiveness of yoga therapy with the therapeutic exercises on walking pain, tenderness, early morning stiffness and disability in osteoarthritis of the knee joint - a comparative study. J Yoga Phys Ther. 2012;2:114.
Ebnezar J, Nagarathna R, Yogitha B, Nagendra HR. Effect of integrated yoga therapy on pain, morning stiffness and anxiety in osteoarthritis of the knee joint: a randomized control study. Int J Yoga. 2012;5(1):28–36. https://doi.org/10.4103/0973-6131.91708.
Ebnezar J, Nagarathna R, Yogitha B, Nagendra HR. Effects of an integrated approach of hatha yoga therapy on functional disability, pain, and flexibility in osteoarthritis of the knee joint: a randomized controlled study. J Altern Complement Med. 2012;18(5):463–72. https://doi.org/10.1089/acm.2010.0320.
Ebnezar J, Nagarathna R, Bali Y, Nagendra HR. Effect of an integrated approach of yoga therapy on quality of life in osteoarthritis of the knee joint: a randomized control study. Int J Yoga. 2011;4(2):55–63. https://doi.org/10.4103/0973-6131.85486.
Cheung C, Wyman JF, Bronas U, McCarthy T, Rudser K, Mathiason MA. Managing knee osteoarthritis with yoga or aerobic/strengthening exercise programs in older adults: a pilot randomized controlled trial. Rheumatol Int. 2017;37(3):389–98. https://doi.org/10.1007/s00296-016-3620-2.
Cheung C, Wyman JF, Resnick B, Savik K. Yoga for managing knee osteoarthritis in older women: a pilot randomized controlled trial. BMC Complement Altern Med. 2014;14:160. https://doi.org/10.1186/1472-6882-14-160.
Park J, McCaffrey R, Newman D, Cheung C, Hagen D. The effect of Sit “N” Fit Chair Yoga among community-dwelling older adults with osteoarthritis. Holist Nurs Pract. 2014;28(4):247–57. https://doi.org/10.1097/hnp.0000000000000034.
Park J, McCaffrey R, Dunn D, Goodman R. Managing osteoarthritis: comparisons of chair yoga, Reiki, and education (pilot study). Holist Nurs Pract. 2011;25(6):316–26. https://doi.org/10.1097/HNP.0b013e318232c5f9.
Park J, Newman D, McCaffrey R, Garrido JJ, Riccio ML, Liehr P. The effect of chair yoga on biopsychosocial changes in English- and Spanish-speaking community-dwelling older adults with lower-extremity osteoarthritis. J Gerontol Soc Work. 2016;59(7–8):604–26. https://doi.org/10.1080/01634372.2016.1239234.
Kuntz AB, Chopp-Hurley JN, Brenneman EC, Karampatos S, Wiebenga EG, Adachi JD, et al. Efficacy of a biomechanically-based yoga exercise program in knee osteoarthritis: a randomized controlled trial. PLoS One. 2018;13(4):e0195653. https://doi.org/10.1371/journal.pone.0195653.
Garfinkel MS, Schumacher HR Jr, Husain A, Levy M, Reshetar RA. Evaluation of a yoga based regimen for treatment of osteoarthritis of the hands. J Rheumatol. 1994;21(12):2341–3.
Fransen M, McConnell S, Harmer AR, Van der Esch M, Simic M, Bennell KL. Exercise for osteoarthritis of the knee. Cochrane Database Syst Rev. 2015;1:Cd004376. https://doi.org/10.1002/14651858.CD004376.pub3.
Osteras N, Kjeken I, Smedslund G, Moe RH, Slatkowsky-Christensen B, Uhlig T, et al. Exercise for hand osteoarthritis. Cochrane Database Syst Rev. 2017;1:Cd010388. https://doi.org/10.1002/14651858.CD010388.pub2.
Cramer H, Lauche R, Langhorst J, Dobos G. Yoga for rheumatic diseases: a systematic review. Rheumatology (Oxford). 2013;52(11):2025–30. https://doi.org/10.1093/rheumatology/ket264.
Kim S, Bemben MG, Bemben DA. Effects of an 8-month yoga intervention on arterial compliance and muscle strength in premenopausal women. J Sports Sci Med. 2012;11(2):322–30.
Peeler J, Ripat J. The effect of low-load exercise on joint pain, function, and activities of daily living in patients with knee osteoarthritis. Knee. 2018;25(1):135–45. https://doi.org/10.1016/j.knee.2017.12.003.
Findlay DM. Vascular pathology and osteoarthritis. Rheumatology (Oxford). 2007;46(12):1763–8. https://doi.org/10.1093/rheumatology/kem191.
Middleton KR, Magaña López M, Haaz Moonaz S, Tataw-Ayuketah G, Ward MM, Wallen GR. A qualitative approach exploring the acceptability of yoga for minorities living with arthritis: ‘where are the people who look like me?’. Complement Ther Med. 2017;31:82–9. https://doi.org/10.1016/j.ctim.2017.02.006.
Bhimani NT, Kulkarni NB, Kowale A, Salvi S. Effect of Pranayama on stress and cardiovascular autonomic function. Indian J Physiol Pharmacol. 2011;55(4):370–7.
Sinha B, Sinha TD, Pathak A, Tomer OS. Comparison of cardiorespiratory responses between Surya Namaskar and bicycle exercise at similar energy expenditure level. Indian J Physiol Pharmacol. 2013;57(2):169–76.
Vallath N. Perspectives on yoga inputs in the management of chronic pain. Indian J Palliat Care. 2010;16(1):1–7. https://doi.org/10.4103/0973-1075.63127.
Cramer H, Anheyer D, Lauche R, Dobos G. A systematic review of yoga for major depressive disorder. J Affect Disord. 2017;213:70–7. https://doi.org/10.1016/j.jad.2017.02.006.
Desveaux L, Lee A, Goldstein R, Brooks D. Yoga in the management of chronic disease: a systematic review and meta-analysis. Med Care. 2015;53(7):653–61. https://doi.org/10.1097/mlr.0000000000000372.
Cramer H, Ostermann T, Dobos G. Injuries and other adverse events associated with yoga practice: a systematic review of epidemiological studies. J Sci Med Sport. 2018;21(2):147–54. https://doi.org/10.1016/j.jsams.2017.08.026.
Garber CE, Blissmer B, Deschenes MR, Franklin BA, Lamonte MJ, Lee IM, et al. American College of Sports Medicine position stand. Quantity and quality of exercise for developing and maintaining cardiorespiratory, musculoskeletal, and neuromotor fitness in apparently healthy adults: guidance for prescribing exercise. Med Sci Sports Exerc. 2011;43(7):1334–59. https://doi.org/10.1249/MSS.0b013e318213fefb.
Boutron I, Moher D, Altman DG, Schulz KF, Ravaud P. Extending the CONSORT statement to randomized trials of nonpharmacologic treatment: explanation and elaboration. Ann Intern Med. 2008;148(4):295–309.
Slade SC, Dionne CE, Underwood M, Buchbinder R, Beck B, Bennell K, et al. Consensus on exercise reporting template (CERT): modified Delphi study. Phys Ther. 2016;96(10):1514–24. https://doi.org/10.2522/ptj.20150668.
Ioannidis JP, Evans SJ, Gotzsche PC, O'Neill RT, Altman DG, Schulz K, et al. Better reporting of harms in randomized trials: an extension of the CONSORT statement. Ann Intern Med. 2004;141(10):781–8.
Moher D, Hopewell S, Schulz KF, Montori V, Gotzsche PC, Devereaux PJ, et al. CONSORT 2010 explanation and elaboration: updated guidelines for reporting parallel group randomised trials. Int J Surg. 2012;10(1):28–55. https://doi.org/10.1016/j.ijsu.2011.10.001.
Acknowledgements
DJH is supported by an NHMRC Practitioner Fellowship. JA is supported by an ARC Professorial Future Fellowship (FT140100195).
Author information
Authors and Affiliations
Contributions
(1) RL, HC, and DH contributed to the conception and design of the study and acquisition of data; RL conducted the analysis; RL, HC, DH, and JA contributed to the interpretation of data. (2) RL, HC, and DH contributed to the drafting the article; RL, HC, DH, and JA revised it critically for important intellectual content. (3) All authors gave final approval of the version to be submitted.
Corresponding author
Ethics declarations
Conflict of Interest
Romy Lauche, Jon Adams, and Holger Cramer each declare no potential conflicts of interest.
David J. Hunter has received person fees from Merck Serono, Pfizer, Lilly, and TLCBio,
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Complementary and Alternative Medicine
Rights and permissions
About this article
Cite this article
Lauche, R., Hunter, D.J., Adams, J. et al. Yoga for Osteoarthritis: a Systematic Review and Meta-analysis. Curr Rheumatol Rep 21, 47 (2019). https://doi.org/10.1007/s11926-019-0846-5
Published:
DOI: https://doi.org/10.1007/s11926-019-0846-5