Abstract
Purpose of the Review
Here, we review recent findings in the field of generating insulin-producing cells by pancreatic transcription factor (pTF)-induced liver transdifferentiation (TD). TD is the direct conversion of functional cell types from one lineage to another without passing through an intermediate stage of pluripotency. We address potential reasons for the restricted efficiency of TD and suggest modalities to overcome these challenges, to bring TD closer to its clinical implementation in autologous cell replacement therapy for insulin-dependent diabetes.
Recent Findings
Liver to pancreas TD is restricted to cells that are a priori predisposed to undergo the developmental process. In vivo, the predisposition of liver cells is affected by liver zonation and hepatic regeneration. The TD propensity of liver cells is related to permissive epigenome which could be extended to TD-resistant cells by specific soluble factors. An obligatory role for active Wnt signaling in continuously maintaining a “permissive” epigenome is suggested. Moreover, the restoration of the pancreatic niche and vasculature promotes the maturation of TD cells along the β cell function.
Summary
Future studies on liver to pancreas TD should include the maturation of TD cells by 3D culture, the restoration of vasculature and the pancreatic niche, and the extension of TD propensity to TD-resistant cells by epigenetic modifications. Liver to pancreas TD is expected to result in the generation of custom-made “self” surrogate β cells for curing diabetes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The first study of liver to pancreas transdifferentiation (TD) was published by our group 20 years ago: recombinant adenovirus-mediated ectopic expression of Pancreatic and Duodenal Homeobox-1(PDX1), a master regulator of pancreas organogenesis, activated insulin production, as well as its processing and secretion in mice liver in vivo [1]. Hepatic insulin production was sufficient to ameliorate the blood glucose levels in diabetic mice [1]. This plasticity of adult cells was rather surprising, as the leading dogma at that time was that adult cells in mammals, once committed to a specific lineage, become “terminally differentiated” and can no longer change their fate [2, 3]. Six years later, the reprogramming ability of adult somatic cells to pluripotency was demonstrated [4].
The in vivo model of PDX1-induced liver to pancreas TD revealed major characteristics of this process: (A) The ectopic pancreatic transcription factor is a short-term trigger to a relatively wide developmental process, that involves comprehensive alterations in gene expression [5]. (B) PDX1 plays a dual role in liver to pancreas TD; in addition to activating the pancreatic fate, it turns off the hepatic repertoire in each of the liver cells in a transient manner [6]. (C) PDX1 irreversibly activates the alternate pancreatic lineage only in a small population of cells [1, 5]. These three major characteristics were recapitulated in lineage reprogramming processes induced by other tissue-specific transcription factors between all other cell types, both in vivo or in tissue cultures, in vitro [7,8,9,10,11,12,13].
TD utilizes a transient ectopic expression of one or few genes (transcription factors) to induce stable alterations in the expression of hundreds of genes, allowing adult cells to gain alternate developmental fate and, consequently, functions [14, 15]. The newly gained function usually persists long after the ectopic gene expression vanishes [5]. The safety benefit of TD lies in the fact that this epigenetic process, does not involve foreign DNA insertions, pluripotency induction, or uncontrolled cell proliferation.
TD and pluripotency induction share common characteristics, as both are activated by master regulator transcription factors and mediated by massive alterations of the epigenome of adult somatic cells, allowing the potential generation of alternate autologous tissues. Unlike induced pluripotent stem cells (iPSCs) that display unlimited proliferation and clonal selection, the newly generated TD cells are mostly post-mitotic and display a defined function [16]. Both types of reprogrammed cells may display diverse levels of development and maturity [17•, 18••].
TD of adult extra-pancreatic tissues may result in the generation of custom-made “self” surrogate β cells for the treatment of diabetes, overcoming both the shortage in tissue availability from cadaveric donors and the need for anti-rejection treatment [19••].
Why Use Liver for Reprogramming Endocrine Pancreas?
The liver is the largest organ in the body with a high level of functional redundancy [20]. Unlike β cells, the liver regenerates efficiently, mainly by the proliferation of mature hepatocytes [21•, 22].
The liver and the pancreas are developmentally related to each other; both are derived from appendages of the upper primitive foregut endoderm [23, 24]. Liver and pancreas are also phylogenetically related; eels and worms have no separation between these two organs, called hepatopancreas [25, 26]. It has been suggested that the late separation of liver and pancreas during organogenesis in the primitive ventral endoderm, might have left both tissues with pluripotent cells that are capable of giving rise to both hepatic and pancreatic lineages [27]. Moreover, the two organs share many characteristics, including responsiveness to glucose, and a large group of specific transcription factors that are expressed in both tissues [28]. Thus, trans-conversion between the two endodermal tissues is conceivable.
A recent study reports that during embryonic organogenesis in mice, the homeoprotein TGIF2 acts as a developmental regulator of the pancreas versus liver fate decision. TGIF2 has been suggested to be sufficient to elicit liver to pancreas fate conversion both ex vivo and in vivo. Hepatocytes expressing TGIF2 undergo extensive transcriptional remodeling, which represses the original hepatic identity and, over time, induces a pancreatic progenitor-like phenotype [29•]. Whether this homeoprotein exerts similar effects in other species including humans is to be determined.
Finally, the liver is preferentially targeted by gene delivery tools such as recombinant adenoviruses, due to abundant adenoviruses receptors. Only about 5% of the systemically delivered recombinant adenoviruses are found in extra-hepatic tissues [30].
Liver to Pancreas Transdifferentiation, in Vitro
Functional activation of the endocrine pancreatic repertoire in liver cells in vitro has been studied in rodents, in pigs, in human-derived hepatic cells, and in primary human liver cultures [16, 31,32,33,34]. An in vitro experimental system allows analyzing the liver to pancreas TD under controlled, isolated conditions. Most of the studies described here were performed in primary cultures of adult human liver cells isolated from > 100 human liver donors [31, 32, 33, 34, 35•, 36••, 37••].
Primary Culture of Adult Human Liver Cells
Human liver cells can be efficiently expanded ex vivo, with the expense of undergoing epithelial to mesenchymal transition and massive hepatic dedifferentiation [6, 38]. Billions of cells can be generated from 1 g of tissue, reprogrammed or bio-banked for future use prior to TD induction [16, 38]. Upon ectopic pTF expression, adult human liver cells express a comprehensive repertoire of pancreatic genes and secrete mature, processed insulin in response to increasing glucose concentrations within the physiological range [31,32,33,34]. The TD liver cells (also called autologous insulin-producing cells; AIP cells) ameliorate diabetes following in vivo implantation [31].
TD Is a Rapid but Sequential and Hierarchical Developmental Process
PDX1 was the first pTF found to induce TD of extra-pancreatic tissues [1]. PDX1 is used in most TD protocols of pancreatic and extra-pancreatic tissues both in vivo and in vitro (see review [16]). However, additional pTFs augment its effect on the efficiency of the process [16, 33, 34, 39,40,41,42]. TD induction by concerted expression of several pTFs, as suggested in [34, 40, 43, 44] relies on the expectation that TD is a one-step process. However, this may not be the case, since despite its speed, TD is a sequential and temporally controlled process [33]. It was suggested that TD of human liver cells along the pancreatic lineage is a gradual and consecutive process [33]. Accordingly, only sequential ectopic expression of three pTFs initiated by PDX1 and concluded by MAFA 3 days later, in a hierarchical manner, resulted in increased maturation of the β-like cells, manifested by increased c-peptide secretion in vitro. In fact, it has been established that TD induced by either a concerted pTFs expression or by their introduction in a sequential but non-hierarchical mode resulted in generation of immature multihormonal pancreatic endocrine cells [33].
Pancreatic TD Propensity of Distinct Populations of Cells in the Liver
PDX1 activates the alternate pancreatic repertoire only in small populations of liver cells while its activity in repressing the hepatic repertoire of genes occurs in all liver cells [6, 1, 5, 45]. The differential effect of PDX1 on the activation of the pancreatic lineage and the repression of the hepatic repertoire of genes, suggests distinct regulation of the two processes. A higher developmental restriction or epigenetic barrier may control the activation of the alternate pancreatic lineage.
The differential propensity of liver cells in activating the pancreatic function in response to ectopic PDX1 expression is related to the phenotypic and functional heterogeneity of the cells in this organ. The adult liver cells exhibit phenotypic and functional zonation, named by the proximity to the central and portal veins of the hepatic lobules (pericentral and periportal cells, respectively) [21•, 46,47,48,49,50,51]. Wnt signaling and intracellular/nuclear β catenin levels are suggested to participate in controlling hepatic functional zonation [49, 46, 52]. The first 1–2 cell layers adjacent to the central veins, zone 3, display an active Wnt signaling pathway and express many β catenin-regulated genes. These cells are involved in ammonia detoxification and express high levels of glutamine synthetase and Axin2 [53•]. Periportal liver cells, in hepatic zone 1, express genes involved in gluconeogenesis and fatty acid and urea metabolism (CPS-1 for urea metabolism) [53•] and display a low Wnt signaling activity. It is conceivable that different cells in the liver may display distinct TD capacities.
TD propensity to pancreatic gene expression could be affected also by the distinct levels of the plasticity of liver cells. The liver displays a high regenerative capacity, in which the type of the regenerating cells depends on the type of the liver damage; in mouse liver homeostasis, axin2-positive hepatocytes located around the central vein have a higher proliferative capacity than hepatocytes located in the mediolobular or the in periportal area [22]. After a mild chronic damage, the undamaged hepatocytes located around the portal vein preferentially repopulate the liver. Conversely, a severe chronic liver damage induces a ductular reaction composed of ductal cells and liver progenitor cells. It is not yet determined whether these cells participate in liver regeneration in human pathologic conditions [54•, 55]. Thus, if cell proliferation is associated with increased cellular plasticity manifested at the level of chromatin compaction, then the ectopic pTFs may differentially affect cells localized in distinct areas in the liver [21•].
In vivo studies in mice demonstrated the activation of insulin- and glucagon-producing cells in adult liver cells. However, different experiments resulted in different locations of these hormone-producing cells. In our previous studies, these cells were located at the vicinity of central veins, despite the random and uniform expression of ectopic PDX1 in 40–50% of the cells [1]. This preferred localization of transdifferentiated cells was exhibited in several studies [5, 1, 45]. Other groups reported that the hormone-producing cells were generated in parenchymal hepatocytes and later in periportal areas of the liver. While the expression of the hormones in the parenchymal hepatocytes was transient, the expression in the periportal areas was stable [39, 40, 56, 57]. Lineage tracing analyses revealed that the stable population of cells located in duct-like structures originated from SOX9 positive cells near the Canals of Hering in periportal areas of the liver [39, 40].
Taken together, the hepatic TD propensity to the pancreas could be related to several populations of hepatic progenitors displaying a relatively high level of plasticity [21•].
TD Is Activated in Predisposed Human Liver Cells, in Vitro
Despite the uniform morphology of the human hepatic derived cultures, in vitro, ectopic pTFs expression and the repression of the hepatic repertoire in > 90% of the cells, the activation of insulin expression occurred only in 5–15% of the cells [32, 33]. This may suggest that liver cells display a differential TD propensity and most of the human liver-derived cells in vitro resist pTF-induced activation of the pancreatic fate.
To analyze whether the in vivo TD predisposition is recapitulated in human liver cells propagated in vitro, primary cultures from different donors were separated into 2 groups based on GLUL (glutamine synthetase) enhancer activation, lineage tracing approach [36••]. The GLUL enhancer activity was chosen due to its restricted expression in hepatic pericentral cells [49]. GLUL-enhancer-controlled recombinase activity irreversibly and consistently “tagged” 5–15% of the cells in the liver cultures by GFP. GFP+ and GFP− cells were separately propagated and individually analyzed for pTF-induced TD. The GFP+ cells consistently exhibited efficient TD and insulin production in 64.1 ± 7.9% of the cells. The GFP− cells resisted the activation of the pancreatic lineage. Both TD-permissive (GFP+) and TD-resistant (GFP−) cells express the ectopic pTFs with similar efficiencies and display similar repression of hepatic genes [36••]. These data suggest that TD occurs in reprogramming-prone liver cells also in vitro. TD propensity has been proven stable and is inherited to daughter cells, as the cells proliferate in culture [36••].
Epigenetic Modulators Affect TD Propensity of Adult Liver Cells
Initial characterization of the TD-resistant and TD-prone liver cells suggested that the cells display epigenetic differences (Moshe Szyf and SF unpublished results). Modulation of genome-wide DNA and histone modifications may impact cellular gene expression pattern. Numerous small molecules that inhibit histone deacetylases (HDACs), histone methyltransferases, and DNA methyltransferases (DNMTs) were used to increase reprogramming efficiency of extra-pancreatic tissues toward pancreas. PTF-induced reprogramming of human skin fibroblast into insulin-producing cells was significantly improved by supplementing the TD process with romidepsin (Romi; an inhibitor of enzymatic activity of HDACs) and 5-azacytidine (5-Aza, an inhibitor of DNMT) [58]. Inhibition of histone lysine methyltransferase inhibitor substantially increased the number of insulin-positive cells in the liver [59]. Indeed, epigenetic alterations of TD-resistant human liver cells using HDAC inhibitors as sodium butyrate or suberoylanilide hydroxamic acid convert them into TD-prone cells [36••].
.
The Role of Wnt Signaling Pathways in Liver to Pancreas TD
Wnt signaling is an important regulator of liver development and liver zonation, orchestrating the division of the liver into functionally distinct metabolic zones [46]. Active Wnt signaling has been found obligatory for the pTFs induced liver to pancreas TD [36••]. Transient disruption of active Wnt signaling (by DKK), irreversibly prevent the pTF-induced TD activation also in the TD-predisposed group of liver cells [36••]. Thus, Wnt signaling inhibition converted TD-predisposed cells into TD-resistant liver cells. While active Wnt signaling per se was insufficient to activate a pTF-induced TD in resistant cells, it augmented the effect of the epigenetic alterations on promoting pTF-induced TD in resistant liver cells. Taken together, these data suggest a role for active Wnt signaling in stabilizing a TD-permissive epigenome [36••]. Interestingly, the combined effect of epigenetic modifications and canonical Wnt signaling activity has been suggested also to underlie the TD process of non-osteogenic cells into osteoblasts [60].
The Effect of the Vasculature and Extracellular Niche on TD Cells’ β-like Maturation
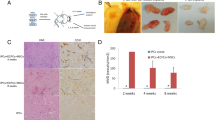
Pancreatic islets are highly vascularized structures. The blood vessels play an important role in providing nutrients as well as non-nutritional signals to pancreatic islets, creating a vascular niche in which cross talk between endocrine β cells and endothelial cells is essential to ensure proper β cell development and function [61,62,63,64,65]. The vasculature secretes several paracrine factors that modulate gene expression, proliferation, and β cell survival. Endocrine pancreatic cells express VEGF-A, a crucial factor in maintaining the microvasculature of the islet, maintenance of β cell mass and the revascularization of islets following transplantation [61, 65, 66]. A recent study suggests that co-implantation of Mesenchymal stem cells (MSCs) and Endothelial progenitor cells (EPCs) with AIP cells derived from TD liver cells led to doubling the survival rates and a threefold increase in insulin production, in vivo [37••]. Using EPC and MSC co-culture and its conditioned medium resulted in a significantly increased expression of pancreatic specific genes and an increase in glucose-regulated insulin secretion, compared with AIP cells that were cultured alone [37••]. Vasculature reconstruction is an important player in all regenerative medicine approaches including that for diabetes.
The reconstitution of the in vivo niche is expected to promote the liver to pancreas TD and the maturation of AIP cells. Indeed, Chaimov et al. have developed a novel artificial pancreas encapsulation platform for the treatment of diabetes, that is based on solubilized whole porcine pancreatic extracellular matrix (ECM) [35•]. These unique capsules were used to entrap AIP cells. The ECM-microcapsule provided both a pancreatic ECM and a natural fibrous 3D niche. The ECM-microcapsule increased the viability of the AIP cells and significantly improved insulin delivery upon in vivo implantation [35•].
In summary, pTFs induced liver to pancreas TD most probably results in AIP cells that are at a heterogeneous level of β cell-like maturation, in vitro. Exposing the cells to an in vivo-like niche may substantially induce their maturation, bringing them closer to their therapeutic implementation.
Summary and Directions for Future Research
The liver displays a high level of plasticity and an extensive rate of proliferation. Expanded liver cells can be bio-banked for future use. Together with its relative accessibility, the liver could serve as an advantageous cellular source for regenerating pancreas and possibly additional degenerated organs. The following findings characterize the process of fate conversion between liver and pancreas:
-
pTF-induced liver to pancreas TD takes place in animal models in vivo as well as in tissue cultures.
-
The pancreatic transcription factor PDX1 is indispensable in activating the pancreatic lineage; additional pTFs promote its effects on hepatic reprogramming.
-
PDX1 plays a dual role in liver to pancreas TD; it activates the pancreatic function only in predisposed liver cells, but represses the hepatic repertoire in all cells. Therefore, pTFs targeting to predisposed liver cells should increase TD safety in vivo.
-
Several populations of liver cells may display preferred propensity to TD. These cells are characterized by increased plasticity.
-
Active Wnt signaling is obligatory for pTF-induced liver to pancreas TD. Continuously active Wnt signaling most probably plays a role in maintaining a “permissive” epigenome needed for the developmental switch.
-
Pre-isolation and separate propagation of TD-predisposed liver cells increase the process efficiency upon ectopic expression of pTFs.
-
Both the vasculature and the pancreatic niche restorations promote the TD cells’ maturation both in vivo and in vitro.
Challenges and Future Studies
-
TD cells may display a heterogeneous level of β cell-like maturation which should be further analyzed by RNA sequencing in vitro and upon cells retrieval after in vivo implantation.
-
2D cultures used in the above TD experimental systems probably hinder the maturation of the generated cells. 3D clustering, which induces metabolic maturation by driving mitochondrial oxidative respiration (a process central to stimulus–secretion coupling in mature β cells [67]), should be used in the TD cultures.
-
The identification of membrane markers of mature TD cells, allowing their isolation prior to 3D clustering, should improve these cells’ therapeutic outcome.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Ferber S, Halkin A, Cohen H, Ber I, Einav Y, Goldberg I, et al. Pancreatic and duodenal homeobox gene 1 induces expression of insulin genes in liver and ameliorates streptozotocin-induced hyperglycemia. Nat Med. 2000;6(5):568–72.
Wagers AJ, Weissman IL. Plasticity of adult stem cells. Cell. 2004;116(5):639–48.
Filip S, English D, Mokry J. Issues in stem cell plasticity. J Cell Mol Med. 2004;8(4):572–7.
Takahashi K, Yamanaka S. Induction of pluripotent stem cells from mouse embryonic and adult fibroblast cultures by defined factors. Cell. 2006;126(4):663–76.
Ber I, Shternhall K, Perl S, Ohanuna Z, Goldberg I, Barshack I, et al. Functional, persistent, and extended liver to pancreas transdifferentiation. J Biol Chem. 2003;278(34):31950–7. https://doi.org/10.1074/jbc.M303127200.
Meivar-Levy I, Sapir T, Gefen-Halevi S, Aviv V, Barshack I, Onaca N, et al. Pancreatic and duodenal homeobox gene 1 induces hepatic dedifferentiation by suppressing the expression of CCAAT/enhancer-binding protein beta. Hepatology (Baltimore, Md). 2007;46(3):898–905.
Shen CN, Slack JM, Tosh D. Molecular basis of transdifferentiation of pancreas to liver. Nat Cell Biol. 2000;2:879–88.
Xie H, Ye M, Feng R, Graf T. Stepwise reprogramming of B cells into macrophages. Cell. 2004;117(5):663–76.
Zhou Q, Brown J, Kanarek A, Rajagopal J, Melton DA. In vivo reprogramming of adult pancreatic exocrine cells to beta-cells. Nature. 2008;455(7213):627–32.
Vierbuchen T, Ostermeier A, Pang ZP, Kokubu Y, Sudhof TC, Wernig M. Direct conversion of fibroblasts to functional neurons by defined factors. Nature. 2010;463(7284):1035–41.
Ieda M, Fu JD, Delgado-Olguin P, Vedatham V, Hayashi Y, Bruneau BG, et al. Direct reprogramming of fibroblasts into functional cardiomyocytes by defined factors. Cell. 2010;142(3):375–86.
Huang P, Zhang L, Gao Y, He Z, Yao D, Wu Z, et al. Direct reprogramming of human fibroblasts to functional and expandable hepatocytes. Cell Stem Cell. 2014;14(3):370–84. https://doi.org/10.1016/j.stem.2014.01.003.
van Oevelen C, Kallin EM, Graf T. Transcription factor-induced enhancer modulations during cell fate conversions. Curr Opin Genet Dev. 2013;23(5):562–7. https://doi.org/10.1016/j.gde.2013.07.003.
Meivar-Levy I, Ferber S. New organs from our own tissues: liver-to-pancreas transdifferentiation. Trends Endocrinol Metab. 2003;14(10):460–6.
Meivar-Levy I, Ferber S. Regenerative medicine: using liver to generate pancreas for treating diabetes. Isr Med Assoc J. 2006;8(6):430–4.
Meivar-Levy I, Ferber S. Reprogramming of liver cells into insulin-producing cells. Best Pract Res Clin Endocrinol Metab. 2015;29(6):873–82. https://doi.org/10.1016/j.beem.2015.10.006.
• Firas J, Polo JM. Towards understanding transcriptional networks in cellular reprogramming. Curr Opin Genet Dev. 2017;46:1–8. https://doi.org/10.1016/j.gde.2017.06.001. Suggests the need to develop computational tools to reconstruct the transcriptional networks of starting and target cells, based on published data and single cells approaches to help tailoring accurate and specific developmental processes (Cell Mogrify).
•• Ellis C, Ramzy A, Kieffer TJ. Regenerative medicine and cell-based approaches to restore pancreatic function. Nature reviews Gastroenterology & hepatology. 2017;14(10):612–28. https://doi.org/10.1038/nrgastro.2017.93. Comprehensive review that describes progress and challenges in cell-based methods to restore pancreatic function, with a focus on optimizing the site for cell delivery and decreasing requirements for immunosuppression through encapsulation. Strategies to generate insulin-producing β cell surrogates in situ are discussed; obstacles to clinical application are highlighted.
•• Latres E, Finan DA, Greenstein JL, Kowalski A, Kieffer TJ. Navigating Two Roads to Glucose Normalization in Diabetes: Automated Insulin Delivery Devices and Cell Therapy. Cell metabolism. 2019;29(3):545–63. https://doi.org/10.1016/j.cmet.2019.02.007. This recent review summarizes the significant progress that has been made in automated insulin delivery devices and cell therapy for diabetes. It addresses the barriers to widespread implementation of cell replacement approaches, compared with those achieved for artificial pancreas systems. It describes the road ahead, including the challenges and opportunities, as a cure for diabetes via both approaches.
Desmet VJ. Organization principles. In: Arias IM, Boyer JL, Chisari FV, Fausto N, Schachter D, Shafritz DA, editors. The liver; biology and pathobiology. 4th ed. Philadelphia, PA: Lippincott Williams and Wilkins; 2001. p. 3–15.
• Gilgenkrantz H, Collin de L’Hortet A. Understanding Liver Regeneration: From Mechanisms to Regenerative Medicine. The American journal of pathology. 2018;188(6):1316–27. https://doi.org/10.1016/j.ajpath.2018.03.008. The review summarizes data published in the past 5 years in the liver regeneration field, discusses the mechanisms leading to regeneration disruption in chronic liver disorders, and addresses the potential use of novel approaches for regenerative medicine. A better understanding of the role of distinct liver cell populations in liver regeneration is potentially relevant for identifying cells that are predisposed to undergo TD to pancreas.
Wang B, Zhao L, Fish M, Logan CY, Nusse R. Self-renewing diploid Axin2(+) cells fuel homeostatic renewal of the liver. Nature. 2015;524(7564):180–5. https://doi.org/10.1038/nature14863.
Fukuda K, Kikuchi Y. Endoderm development in vertebrates: fate mapping, induction and regional specification. Develop Growth Differ. 2005;47(6):343–55. https://doi.org/10.1111/j.1440-169X.2005.00815.x.
Ober EA, Field HA, Stainier DY. From endoderm formation to liver and pancreas development in zebrafish. Mech Dev. 2003;120(1):5–18.
Yang H, Morrison CM, Conlon JM, Laybolt K, Wright JR Jr. Immunocytochemical characterization of the pancreatic islet cells of the Nile tilapia (Oreochromis niloticus). Gen Comp Endocrinol. 1999;114(1):47–56.
Kito H, Ose Y, Mizuhira V, Sato T, Ishikawa T, Tazawa T. Separation and purification of (cd, cu, Zn)-metallothionein in carp hepato-pancreas. Comp Biochem Physiol C. 1982;73(1):121–7.
Deutsch G, Jung J, Zheng M, Lora J, Zaret KS. A bipotential precursor population for pancreas and liver within the embryonic endoderm. Development (Cambridge, England). 2001;128:871–81.
Otsuka M, Hoshida Y, Kato N, Moriyama M, Taniguchi H, Arai M, et al. Liver chip and gene shaving. J Gastroenterol. 2003;38(Suppl 15):89–92.
• Cerda-Esteban N, Naumann H, Ruzittu S, Mah N, Pongrac IM, Cozzitorto C, et al. Stepwise reprogramming of liver cells to a pancreas progenitor state by the transcriptional regulator Tgif2. Nature communications. 2017;8:14127. https://doi.org/10.1038/ncomms14127. This study uncovers the reprogramming activity of TGIF2 and suggests a stepwise reprogramming paradigm, whereby a “lineage-restricted” dedifferentiation step precedes the identity switch.
Varda-Bloom N, Shaish A, Gonen A, Levanon K, Greenbereger S, Ferber S, et al. Tissue-specific gene therapy directed to tumor angiogenesis. Gene Ther. 2001;8(11):819–27.
Sapir T, Shternhall K, Meivar-Levy I, Blumenfeld T, Cohen H, Skutelsky E, et al. From the cover: cell-replacement therapy for diabetes: generating functional insulin-producing tissue from adult human liver cells. Proc Natl Acad Sci U S A. 2005;102(22):7964–9.
Aviv V, Meivar-Levy I, Rachmut IH, Rubinek T, Mor E, Ferber S. Exendin-4 promotes liver cell proliferation and enhances PDX1-induced liver to pancreas transdifferentiation. J Biol Chem. 2009;284(48):33509–20.
Berneman-Zeitouni D, Molakandov K, Elgart M, Mor E, Fornoni A, Dominguez MR, et al. The temporal and hierarchical control of transcription factors-induced liver to pancreas transdifferentiation. PLoS One. 2014;9(2):e87812. https://doi.org/10.1371/journal.pone.0087812.
Gefen-Halevi S, Rachmut IH, Molakandov K, Berneman D, Mor E, Meivar-Levy I, et al. NKX6.1 promotes PDX1-induced liver to pancreatic beta-cells reprogramming. Cell Reprogram. 2010;12(6):655–64. https://doi.org/10.1089/cell.2010.0030.
• Chaimov D, Baruch L, Krishtul S, Meivar-Levy I, Ferber S, Machluf M. Innovative encapsulation platform based on pancreatic extracellular matrix achieve substantial insulin delivery. Journal of controlled release : official journal of the Controlled Release Society. 2017;257:91–101. https://doi.org/10.1016/j.jconrel.2016.07.045. The paper unravels a novel encapsulation platform for the treatment of diabetes that is based on solubilized whole porcine pancreatic extracellular matrix (ECM). The ECM-microcapsule platform provides a natural fibrous 3D niche, supporting cell viability and differentiation, while significantly improving insulin delivery. In vivo, ECM-encapsulated cells were shown to be non-immunogenic and to significantly improve the glycemic control in diabetic mouse preclinical model.
•• Cohen H, Barash H, Meivar-Levy I, Molakandov K, Ben-Shimon M, Gurevich M, et al. The Wnt/beta-catenin pathway determines the predisposition and efficiency of liver-to-pancreas reprogramming. Hepatology (Baltimore, Md). 2018. https://doi.org/10.1002/hep.29827. The study suggests that liver to pancreas TD inefficiency is due to the fact that only 5–15% of the cells in culture are a priori predisposed to undergo the pTFs induced process. A TD-prone subpopulation of liver cells from > 15 human donors is identified and separated, using lineage tracing system based on the hepatic pericentral-specific enhancer of glutamine synthetase (GLUL). The individually propagated cells exhibit substantially increased TD efficiency and insulin production occurs in > 60% of the cells upon ectopic pTF expression. The paper suggests also that TD propensity could be extended to most of the liver cells by artificially inducing epigenetic modifications. A role for active Wnt signaling in promoting liver to pancreas TD is discussed.
•• Meivar-Levy I, Zoabi F, Nardini G, Manevitz-Mendelson E, Leichner GS, Zadok O, et al. The role of the vasculature niche on insulin-producing cells generated by transdifferentiation of adult human liver cells. Stem cell research & therapy. 2019;10(1):–53. https://doi.org/10.1186/s13287-019-1157-5. The study discloses the paracrine role of vasculature (ECFC and MSC co-culture as well as conditioned media) in promoting TD-liver cells maturation both in vitro and in increasing insulin-producing cells survival upon implantation in vivo. The reconstitution of the vascular niche is expected to be an important player in regenerative medicine approaches in general.
Meivar-Levy I, Sapir T, Berneman D, Weissbach T, Polak-Charcon S, Ravassard P, et al. Human liver cells expressing albumin and mesenchymal characteristics give rise to insulin-producing cells. J Transp Secur. 2011.
Banga A, Akinci E, Greder LV, Dutton JR, Slack JM. In vivo reprogramming of Sox9+ cells in the liver to insulin-secreting ducts. Proc Natl Acad Sci U S A. 2012;109(38):15336–41. https://doi.org/10.1073/pnas.1201701109.
Banga A, Greder LV, Dutton JR, Slack JM. Stable insulin-secreting ducts formed by reprogramming of cells in the liver using a three-gene cocktail and a PPAR agonist. Gene Ther. 2014;21(1):19–27. https://doi.org/10.1038/gt.2013.50.
Wang AY, Ehrhardt A, Xu H, Kay MA. Adenovirus transduction is required for the correction of diabetes using PDX1 or Neurogenin-3 in the liver. Mol Ther. 2007;15(2):255–63.
Yechoor V, Liu V, Paul A, Lee J, Buras E, Ozer K, et al. Gene therapy with neurogenin 3 and betacellulin reverses major metabolic problems in insulin-deficient diabetic mice. Endocrinology. 2009;150(11):4863–73. https://doi.org/10.1210/en.2009-0527.
Yang Y, Akinci E, Dutton JR, Banga A, Slack JM. Stage specific reprogramming of mouse embryo liver cells to a beta cell-like phenotype. Mech Dev. 2013;130(11-12):602–12. https://doi.org/10.1016/j.mod.2013.08.002.
Luo H, Chen R, Yang R, Liu Y, Chen Y, Shu Y, et al. Reprogramming of mice primary hepatocytes into insulin-producing cells by transfection with multicistronic vectors. J Diabetes Res. 2014;2014:716163. https://doi.org/10.1155/2014/716163.
Koizumi M, Doi R, Toyoda E, Tulachan SS, Kami K, Mori T, et al. Hepatic regeneration and enforced PDX1 expression accelerate transdifferentiation in liver. Surgery. 2004;136(2):449–57.
Burke ZD, Reed KR, Phesse TJ, Sansom OJ, Clarke AR, Tosh D. Liver zonation occurs through a beta-catenin-dependent, c-Myc-independent mechanism. Gastroenterology. 2009;136(7):2316–24.e1-3.
Torre C, Perret C, Colnot S. Molecular determinants of liver zonation. Prog Mol Biol Transl Sci. 2010;97:127–50.
Gebhardt R, Matz-Soja M. Liver zonation: novel aspects of its regulation and its impact on homeostasis. World J Gastroenterol. 2014;20(26):8491–504. https://doi.org/10.3748/wjg.v20.i26.8491.
Gebhardt R, Baldysiak-Figiel A, Krugel V, Ueberham E, Gaunitz F. Hepatocellular expression of glutamine synthetase: an indicator of morphogen actions as master regulators of zonation in adult liver. Prog Histochem Cytochem. 2007;41(4):201–66.
Jungermann K, Kietzmann T. Oxygen: modulator of metabolic zonation and disease of the liver. Hepatology (Baltimore, Md). 2000;31(2):255–60.
Kietzmann T, Jungermann K. Modulation by oxygen of zonal gene expression in liver studied in primary rat hepatocyte cultures. Cell Biol Toxicol. 1997;13(4-5):243–55.
Benhamouche S, Decaens T, Godard C, Chambrey R, Rickman DS, Moinard C, et al. Apc tumor suppressor gene is the “zonation-keeper” of mouse liver. Dev Cell. 2006;10(6):759–70.
• Halpern KB, Shenhav R, Matcovitch-Natan O, Toth B, Lemze D, Golan M, et al. Single-cell spatial reconstruction reveals global division of labour in the mammalian liver. Nature. 2017;542(7641):–352, 6. https://doi.org/10.1038/nature21065. A detailed genome-wide reconstruction of the spatial hepatic zonation. The entire transcriptome of thousands of mouse liver cells and their lobule coordinates on the basis of a panel of zonated landmark genes is being characterized with single-molecule fluorescence in situ hybridization. Using this approach, the zonation profiles of all liver genes with high spatial resolution has been achieved. Information herein can be used for identifying membrane markers of hepatic predisposed cells.
• Tsuchiya A, Lu WY. Liver stem cells: plasticity of the liver epithelium. World journal of gastroenterology. 2019;25(9):1037–49. https://doi.org/10.3748/wjg.v25.i9.1037. The article highlights recent findings about plasticity in the liver epithelium and the cellular source of regeneration during liver injury. Cellular sources of liver regeneration could be relevant for identifying liver cell populations that are predisposed to undergo pTF-induced liver to pancreas TD.
Abu Rmilah A, Zhou W, Nelson E, Lin L, Amiot B, Nyberg SL. Understanding the marvels behind liver regeneration. Wiley interdisciplinary reviews Developmental biology. 2019;8(3):e340. https://doi.org/10.1002/wdev.340.
Kojima H, Fujimiya M, Matsumura K, Younan P, Imaeda H, Maeda M, et al. NeuroD-betacellulin gene therapy induces islet neogenesis in the liver and reverses diabetes in mice. Nat Med. 2003;9(5):596–603.
Yechoor V, Liu V, Espiritu C, Paul A, Oka K, Kojima H, et al. Neurogenin3 is sufficient for transdetermination of hepatic progenitor cells into neo-islets in vivo but not transdifferentiation of hepatocytes. Dev Cell. 2009;16(3):358–73.
Katz LS, Geras-Raaka E, Gershengorn MC. Reprogramming adult human dermal fibroblasts to islet-like cells by epigenetic modification coupled to transcription factor modulation. Stem Cells Dev. 2013;22(18):2551–60. https://doi.org/10.1089/scd.2013.0134.
Akinci E, Banga A, Tungatt K, Segal J, Eberhard D, Dutton JR, et al. Reprogramming of various cell types to a beta-like state by Pdx1, Ngn3 and MafA. PLoS One. 2013;8(11):e82424. https://doi.org/10.1371/journal.pone.0082424.
Cho YD, Yoon WJ, Kim WJ, Woo KM, Baek JH, Lee G, et al. Epigenetic modifications and canonical wingless/int-1 class (WNT) signaling enable trans-differentiation of nonosteogenic cells into osteoblasts. J Biol Chem. 2014;289(29):20120–8. https://doi.org/10.1074/jbc.M114.558064.
Narayanan S, Loganathan G, Dhanasekaran M, Tucker W, Patel A, Subhashree V, et al. Intra-islet endothelial cell and beta-cell crosstalk: implication for islet cell transplantation. World J Transplant. 2017;7(2):117–28. https://doi.org/10.5500/wjt.v7.i2.117.
Cleaver O, Dor Y. Vascular instruction of pancreas development. Development (Cambridge, England). 2012;139(16):2833–43. https://doi.org/10.1242/dev.065953.
Aamodt KI, Powers AC. Signals in the pancreatic islet microenvironment influence beta-cell proliferation. Diabetes Obes Metab. 2017;19(Suppl 1):124–36. https://doi.org/10.1111/dom.13031.
Peiris H, Bonder CS, Coates PT, Keating DJ, Jessup CF. The beta-cell/EC axis: how do islet cells talk to each other? Diabetes. 2014;63(1):3–11. https://doi.org/10.2337/db13-0617.
Cao Z, Wang X. The endocrine role between beta cells and intra-islet endothelial cells. Endocr J. 2014;61(7):647–54.
Brissova M, Aamodt K, Brahmachary P, Prasad N, Hong JY, Dai C, et al. Islet microenvironment, modulated by vascular endothelial growth factor-a signaling, promotes beta cell regeneration. Cell Metab. 2014;19(3):498–511. https://doi.org/10.1016/j.cmet.2014.02.001.
Nair GG, Liu JS, Russ HA, Tran S, Saxton MS, Chen R, et al. Recapitulating endocrine cell clustering in culture promotes maturation of human stem-cell-derived beta cells. Nat Cell Biol. 2019;21(2):263–74. https://doi.org/10.1038/s41556-018-0271-4.
Acknowledgments
We thank the present and former students and post-doctorate fellows for their enormous contribution during the years.
Funding
Funding supporting part of the presented studies include JDRF, ISF, D-Cure, BioDisc and EFSD, “Autologous cell replacement therapy for diabetic patients by liver cells transdifferentiation” (Dia-cure), P_37_794, POC-A. 1- A.1.1.4-E-2015 (2016 - 2020)/ SMIS 106897, Orgenesis Ltd.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Irit Meivar-Levy is a Senior Scientist at Orgenesis LTD. In addition, Dr. Meivar-Levy has a patent which is licensed to Orgenesis.
Sarah Ferber is the CSO of Orgenesis Inc. In addition, Dr. Ferber has several patents on Transdifferentiation, which are licensed to Orgenesis.
Human and Animal Rights and Informed Consent
Ethical approval: All procedures performed in studies involving human participants were in accordance with the ethical standards of Sheba Medical Center Committee on Clinical Investigations (the institutional review board; 0395-13-SMC) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. All procedures performed in studies involving animals were in accordance with the ethical standards of the institution at which the studies were conducted and ethical approval was obtained from the Institutional Animal Care and Use Committee of Sheba Medical Center (1023/16, 732/12).
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Immunology, Transplantation, and Regenerative Medicine
Rights and permissions
About this article
Cite this article
Meivar-Levy, I., Ferber, S. Liver to Pancreas Transdifferentiation. Curr Diab Rep 19, 76 (2019). https://doi.org/10.1007/s11892-019-1198-2
Published:
DOI: https://doi.org/10.1007/s11892-019-1198-2