Abstract
Left paraduodenal hernia is an entrapment of the small bowel into the Landzert fossa, an unusual congenital peritoneal defect behind the descending mesocolon that results from failure of part of the descending mesocolon to fuse with the posterior parietal peritoneum (Doishita et al. in Radiographics, 36(1): 88–106, 2016). This fossa is reported to be present in approximately 2% of autopsy bodies. The authors present a case of a left paraduodenal hernia in a young woman.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Abnormalities in the formation and resorption of the dorsal mesentery may allow fossa to develop into which loops of bowel may herniate. The most common of these fossa are those near the duodenum.
A left paraduodenal hernia represents a hernia of the proximal jejunum into the mesentery of the descending colon. The opening of the left paraduodenal hernia is just lateral to the fourth portion of the duodenum at the Landzert fossa. This fossa is present when the inferior mesenteric vein and ascending left colon artery are incompletely fixed to the retroperitoneum and run along to its anteromedial border. Loops of jejunum can herniate beneath the mesentery of the descending colon, potentially causing small bowel obstruction or ischemia.1 The inferior mesenteric artery and vein are integral components of the hernia sac.2
Case Report
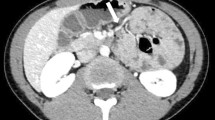
A 17 years old woman presents in our emergency department with the complaint of abdominal pain for 2 days. She had no complaints of nausea or vomiting. The abdomen was painful in her left quadrant and the bowel sounds were increased. Initially, she underwent an ultrasonography which was suspicious for an internal hernia. She then underwent an abdominal computerized axial tomography scan (Fig. 1) which revealed “an agglomerate of intestinal loops in the left upper quadrant, with a saccular configuration and densification of the enteric fat, positioned in retrogastric topography, in the anterior pararenal space (…) there was also an arch of the mesenteric vessels into the referred sac, compatible with a left paraduodenal hernia where the inferior mesentery vein were in the anteromedial part of the hernia.”3
The patient underwent an exploratory laparotomy that confirmed the diagnosis of a left paraduodenal hernia. During surgery, it was possible to see the herniation of a segment of small bowel into the Landzert fossa (Fig. 2) with the inferior mesenteric vein (IMV) anterior to the hernia sac (Fig. 3). The hernia was reduced and was possible to verify a segment of kinked small bowel, however, with any signs of ischemia. The bowel was put in an anatomical position and the fossa defect was sutured with a continued silk suture (Fig. 4).
The patient had a good recovery and was discharged after 3 days of surgery. She is currently doing well without any complaints.
References
Gore, Richard M., MD; Levine, Marc S., MD. Textbook of Gastrointestinal Radiology, Fourth Edition. Elsevier, 2017.
Townsend, Courtney M., JR., MD; Beauchamp, R. Daniel, MD; Evers, B. Mark, MD, et al. Sabiston Textbook of Surgery. 20th Edition. Elsevier, 2017.
Satoshi Doishita, Tohru Takeshita, Yasutake Uchima, et al. Internal Hernias in the Era of Multidetector CT: Correlation of Imaging and Surgical Findings. Radiographics, 2016; 36(1): 88–106.
Author information
Authors and Affiliations
Contributions
Aires Martins: performed the surgery and designed the manuscript; research and manuscript revision and approval.
Álvaro Gonçalves: analysis, revision, and approval.
Teresa Almeida: analysis, revision, and approval.
Rui Gomes: analysis, revision, and approval.
João Lomba: performed the surgery; revision and approval.
Alberto Midões: Director of General Surgery Department; revision and approval.
Corresponding author
Rights and permissions
About this article
Cite this article
Martins, A., Gonçalves, Á., Almeida, T. et al. Left Paraduodenal Hernia. J Gastrointest Surg 22, 925–927 (2018). https://doi.org/10.1007/s11605-017-3626-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-017-3626-4