Abstract
Background
Hospital cancer registries are only required to report gastrointestinal stromal tumors (GISTs) if labeled malignant or metastatic, leading to potential loss of cases in national cancer registries. Our objective was to determine whether GISTs are underreported in the US.
Methods
Retrospective review of pathology reports between 2010 and 2013 with diagnosis of GIST was performed at two academic medical centers. Recurrent GISTs were excluded. Pathology reports were cross-referenced to cases reported by each cancer registry. Risk for metastasis/death was determined according to National Comprehensive Cancer Network (NCCN) guidelines.
Results
Forty-nine cases of non-recurrent GIST were identified. Only 19/49 (38.8 %) cases were reported. None of the 30 non-reported cases were labeled malignant/metastatic on final pathology. To illustrate malignant potential, these tumors were risk stratified. Most (60 %) of the non-reported cases were low risk, but there were 4 (13.3 %) cases each in the intermediate, high, and unknown risk groups. Additionally, 7/30 (23.0 %) cases were treated with tyrosine kinase inhibitors, highlighting clinical concern of malignant GIST.
Conclusions
Our results show that nearly two thirds of GIST cases have been underreported, suggesting that current reporting practices underestimate its true incidence. Revision of reporting guidelines may result in a more accurate estimation of the US disease burden of GIST.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Gastrointestinal stromal tumors (GISTs) are the most common mesenchymal tumors of the gastrointestinal tract with an estimated 3000–5000 new cases diagnosed annually in the US.1,2 Data regarding GIST diagnosis and treatment is initially collected at hospital cancer registries and subsequently reported to regional, state, and national cancer registries. In California, for example, hospital data is reported to a designated regional cancer registry, which reports to the California Cancer Registry (CCR). This data is then submitted for use on a national level to the Centers for Disease Control and Prevention’s National Program of Cancer Registries (NPCR) and the National Cancer Institutes’ Surveillance, Epidemiology and End Results (SEER) program.
For reporting on GIST, NPCR and SEER mandate that hospital cancer registries only report GIST cases that have been designated as either malignant or metastatic by a pathologist on a pathology report or by a clinician’s treatment notes. Advances in histopathologic diagnosis over the last two decades have helped differentiate GISTs from other soft tissue tumors and helped improve prognostication. These changes culminated in the 2002 publication of the National Institutes of Health (NIH) expert consensus guidelines on GIST re-classification, which outlined a risk stratification scheme utilizing tumor and clinical factors to assign each GIST a risk of disease progression or metastasis.3 As such, all GIST cases may harbor malignant potential and should not simply be considered benign. Furthermore, the College of American Pathologists (CAP) guidelines reflect these changes in GIST classification. Because the CAP protocol for GIST “regard(s) most GISTs as having at least some potential for distant metastasis,” tumors are described by risk assessment based on tumor size, mitotic index, and tumor location.4
The true incidence of GIST may be more accurately reflected on the level of hospital cancer registries where the data is collected and evaluated before reporting to state and national cancer registries. Due to potential loss of GIST cases collected at the local level, data accessible on the state and national cancer registry levels may underestimate the true incidence of GIST due to incongruent cancer registry reporting guidelines. Since the NIH re-classification, pathologists have been reporting GISTs and clinicians have been treating GISTs based on risk stratification.5 However, we hypothesize that a considerable proportion of GIST cases are not reported from hospital cancer registries, leading to an underestimation of the GIST incidence in state and national cancer registries. The objective of this study was to determine the rate of GIST underreporting.
Methods
Identification of Operative GIST Cases
Following approval by both hospitals’ institutional review boards, GIST cases between the years of 2010 to 2013 were identified at City of Hope National Medical Center and Loma Linda University Medical Center by query of each institution’s department of pathology database. Patients with recurrent GIST were excluded. Non-recurrent metastatic cases were included (i.e., nodal involvement at presentation). Patient characteristics and treatment-related data were tabulated, including surgical procedure and treatment with receptor tyrosine kinase inhibitors (TKI). Pathology reports were reviewed for tumor size, location, and mitotic index.
Cancer Registry-Reported GIST Cases
Pathology reports were cross-referenced with a list of each institution’s cancer registry cases that were reported to their respective regional registries. Cases from the Loma Linda University Medical Center Cancer Registry were reported to the San Bernardino/Riverside County registry, while cases from the City of Hope Cancer Registry were reported to the Los Angeles County registry. Each regional registry reports cases to CCR, which in turn provides data accessible on the national level via the Centers for Disease Control and Prevention’s NPCR and the National Cancer Institutes’ SEER program.
GIST Risk Stratification
GIST cases were classified for risk of metastasis or tumor-related death according to the National Comprehensive Cancer Network (NCCN) guidelines/Armed Forces Institute of Pathology (AFIP) criteria.6,7 Based on tumor size, mitotic rate, and tumor location, patients were grouped into no-risk, very-low-risk, low-risk, intermediate-risk, or high-risk groups (Table 1). For this study, no-risk, very-low-risk, and low-risk patients were combined into one group due to the small number of patients in the no-risk and very-low-risk tumor groups. Patients with colorectal and gastroesophageal junction GISTs were risk stratified according to the AFIP criteria for small intestinal GIST, since a prior large retrospective series has shown their recurrence-free survival to be similar.8 Patients with missing tumor size or missing number of mitoses had insufficient information to assign a risk classification and were grouped as unknown risk.
Results
Characteristics and Treatment Patterns of Non-reported GIST Cases
From 2010 to 2013, 49 cases of non-recurrent GIST were identified at the two institutions. Of these GIST cases, 30 (61.2 %) cases were not reported to a regional cancer registry, with 15 cases originating from each institution. These non-reported cases failed to include malignant or metastatic diagnoses on the pathology reports, even though nearly all patients were treated with surgical resection (n = 29 of 30, 96.7 %). The majority (n = 18 of 30, 60 %) of these cases were classified as low risk, but there were 4 (13.3 %) cases each in the intermediate-risk, high-risk, and unknown-risk groups (Table 2). Interestingly, nearly a quarter (n = 7 of 30, 23.0 %) of the patients with non-reported cases received treatment with TKI, further highlighting the treating physicians’ concern for malignant disease. In this group of TKI-treated non-reported GISTs, 2 cases were high risk, 1 was intermediate risk, 3 were low risk, and 1 was unknown risk (Table 2).
Characteristics and Treatment Patterns of Reported GIST Cases
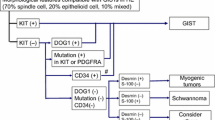
Only 19 of 49 (38.8 %) identified GIST cases were reported. Of 20 cases identified at Loma Linda University Medical Center, 5 (25 %) cases were reported, and of 29 cases identified at City of Hope Medical Center, 14 (48.3 %) were reported. Nine of the reported 19 cases were specifically identified as malignant or metastatic cases, including 8 (88.9 %) that were classified as high risk for disease progression or metastasis by NCCN criteria. All 8 of these patients underwent surgical resection, and 4 of the 8 (50.0 %) received treatment with a TKI (Table 3). The remaining 1 of 9 (11.1 %) cases could not be classified due to lack of information. This patient underwent biopsy confirming GIST at a referring institution, but was considered a poor surgical candidate and was treated with TKI alone.
The remaining 10 reported cases did not have the malignant or metastatic designation on pathology report, yet were still reported to regional cancer registries (Fig. 1). Further classification of these 10 cases without malignant or metastatic designation on pathology revealed 3 high-risk cases, 2 intermediate-risk cases, 4 low-risk cases, and 1 unknown-risk case (Table 3). Nine of 10 (90.0 %) patients underwent surgical resection, with one of the high-risk cases deemed non-operable secondary to multiple comorbid conditions. Eight of the 10 (80.0 %) cases received treatment with TKI. According to our institutions’ cancer registries, these cases were reported due to their treatment with TKI, which was used as a surrogate for the treatment of malignant GIST. The remaining 2 cases did not receive TKI but were still reported to a regional cancer registry without malignant or metastatic designation; one was reported for unclear reasons, while the other was flagged for registry removal due to reporting error.
Discussion
The incidence of GIST in the US has previously been reported in the range from 3000 to 5000 cases per year.1,2 Hospital cancer registries follow data collection guidelines outlined on the national level by the National Cancer Institutes’ SEER program and the Center for Disease Control and Prevention’s NPCR. In the state of California, local and regional cancer registries report data to CCR, which in turn provides data to both NPCR and SEER.9 In this study, we found that nearly two thirds of pathologically diagnosed GISTs at our institutions were not reported due to the lack of malignant or metastatic designation on pathology reports, despite 27 % of these non-reported cases falling into intermediate-risk to high-risk groups and 23 % receiving treatment with TKI. This suggests that the true incidence of GIST may be higher than published reports using national cancer registry data.
Historically, the classification and prognostication of GIST was hampered by the lack of a precise method of histopathologic diagnosis. GISTs were often grouped with other soft tissue neoplasms in the past, including leiomyoma and leiomyosarcoma.10 The discovery of the c-KIT mutation and the development of immunohistochemical staining for the c-KIT protein in the late 1990s5,11 provided major advancements in understanding the biology of GIST and improved the pathologic criteria for diagnosis. Prior to these findings, GISTs were rarely reported in the SEER database, totaling just 500–600 cases per year.3 With the number of diagnosed GIST cases increasing and the development of imatinib as targeted c-KIT therapy, the National Institutes of Health (NIH) convened a GIST workshop in 2001, publishing consensus guidelines for GIST diagnosis and prognostication. These guidelines outlined a risk classification schema for estimating metastatic risk based on tumor size and mitotic count, adding that the term “benign” probably should not be applied to GISTs any longer.3 The CAP guidelines have been revised to mirror the NIH’s GIST reclassification, with the explanatory notes in the GIST protocol echoing the fact that most GISTs have malignant potential.
While pathologists’ and clinicians’ view of GIST classification and prognosis has evolved rapidly over the last two decades, there appears to be a disconnect between national GIST data collection guidelines and the risk classification schema used to guide the pathologic assessment and clinical management of patients. National reporting guidelines only consider GIST cases coded as malignant or metastatic on pathology report or by clinician documentation to be reportable.12,13 If the GIST is not classified as either benign or malignant, the case would be coded as a tumor of uncertain malignant potential, which is not reportable.13 In contrast to the guidelines for cancer registry reporting, the updated GIST guidelines from the NCCN Task Force14 echo the notion that all GISTs have some degree of malignant potential, which is supported by large retrospective studies from the pre-imatinib era showing a 3–4 % disease progression rate even in GISTs categorized as low risk.6,7 This classification discordance can present a challenge for data abstractors on the hospital cancer registry level in determining whether cases should be reported to regional registries because they are asked to reconcile pathology reports and clinician notes that describe GIST in terms of risk stratification with the outdated dichotomous benign/malignant classification that is no longer used in clinical practice.12,13,15 As a result, a significant proportion of GIST cases are not captured in the state and national data, even cases that are high risk or intermediate risk of disease progression.
By only allowing cases specifically classified as overtly malignant or metastatic, the current guidelines exclude a sizeable proportion of cases from the state and national cancer registry data, including cases that have significant risk of disease progression or metastasis. Inclusion of these cases as tumors of uncertain malignant potential may retain valuable clinical information regarding GIST primary location, tumor size, mitotic count, KIT and PDGFR mutation status, surgical treatment, long-term recurrence, and survival outcomes. Not only would this provide researchers with more complete national registry data on GIST incidence but it would also allow researchers to risk stratify cases that are not necessarily reported as malignant or metastatic and correlate these cases with the site-specific factors already collected by the cancer registry programs. The relatively small sample size included in our study reflects the rarity of the disease, as well as a dearth of cases prior to 2010 at our institutions. Given its relative rarity, large registry data can be particularly helpful in determining tumor characteristics, treatment patterns, and outcomes.
In summary, current reporting guidelines for GIST may underestimate the true incidence of the disease, impacting the quality and reliability of the GIST data collected on the state and national levels. Taken together, our data suggests that the clinical perspective and management of GIST have outpaced the national guidelines for GIST reporting. Revision and standardization of cancer reporting guidelines may result in more accurate estimation of the US GIST disease burden, tumor characteristics, and patient treatment patterns.
References
Pisters, P.W., C.D. Blanke, M. von Mehren, J. Picus, A. Sirulnik, E. Stealey, J.C. Trent, and G.S.C. re, A USA registry of gastrointestinal stromal tumor patients: changes in practice over time and differences between community and academic practices. Ann Oncol, 2011. 22(11): p. 2523–9.
Rubin, J.L., M. Sanon, D.C. Taylor, J. Coombs, V. Bollu, and L. Sirulnik, Epidemiology, survival, and costs of localized gastrointestinal stromal tumors. Int J Gen Med, 2011. 4: p. 121–30.
Fletcher, C.D., J.J. Berman, C. Corless, F. Gorstein, J. Lasota, B.J. Longley, M. Miettinen, T.J. O’Leary, H. Remotti, B.P. Rubin, B. Shmookler, L.H. Sobin, and S.W. Weiss, Diagnosis of gastrointestinal stromal tumors: A consensus approach. Hum Pathol, 2002. 33(5): p. 459–65.
College of American Pathologists Protocol for the Examination of Specimens From Patients With Gastrointestinal Stromal Tumor (GIST). 2014 March 10, 2015; Available from: http://www.cap.org/ShowProperty?nodePath=/UCMCon/Contribution%20Folders/WebContent/pdf/cp-gist-14protocol.pdf.
Agaimy, A., Gastrointestinal stromal tumors (GIST) from risk stratification systems to the new TNM proposal: more questions than answers? A review emphasizing the need for a standardized GIST reporting. Int J Clin Exp Pathol, 2010. 3(5): p. 461–71.
Miettinen, M., H. Makhlouf, L.H. Sobin, and J. Lasota, Gastrointestinal stromal tumors of the jejunum and ileum: a clinicopathologic, immunohistochemical, and molecular genetic study of 906 cases before imatinib with long-term follow-up. Am J Surg Pathol, 2006. 30(4): p. 477–89.
Miettinen, M., L.H. Sobin, and J. Lasota, Gastrointestinal stromal tumors of the stomach: a clinicopathologic, immunohistochemical, and molecular genetic study of 1765 cases with long-term follow-up. Am J Surg Pathol, 2005. 29(1): p. 52–68.
Joensuu, H., A. Vehtari, J. Riihimaki, T. Nishida, S.E. Steigen, P. Brabec, L. Plank, B. Nilsson, C. Cirilli, C. Braconi, A. Bordoni, M.K. Magnusson, Z. Linke, J. Sufliarsky, M. Federico, J.G. Jonasson, A.P. Dei Tos, and P. Rutkowski, Risk of recurrence of gastrointestinal stromal tumour after surgery: an analysis of pooled population-based cohorts. Lancet Oncol, 2012. 13(3): p. 265–74.
California Department of Public Health: California Cancer Registry Overview. 2014 [cited 2014 November 4]; Available from: http://www.ccrcal.org/Inside_CCR/FAQ.shtml#ccr do1.
Nilsson, B., P. Bumming, J.M. Meis-Kindblom, A. Oden, A. Dortok, B. Gustavsson, K. Sablinska, and L.G. Kindblom, Gastrointestinal stromal tumors: the incidence, prevalence, clinical course, and prognostication in the preimatinib mesylate era--a population-based study in western Sweden. Cancer, 2005. 103(4): p. 821–9.
Hirota, S., K. Isozaki, Y. Moriyama, K. Hashimoto, T. Nishida, S. Ishiguro, K. Kawano, M. Hanada, A. Kurata, M. Takeda, G. Muhammad Tunio, Y. Matsuzawa, Y. Kanakura, Y. Shinomura, and Y. Kitamura, Gain-of-function mutations of c-kit in human gastrointestinal stromal tumors. Science, 1998. 279(5350): p. 577–80.
Surveillance, Epidemiology, and End Results Program: SEER Inquiry System (Question 20100014). 2014 [cited 2014 October 29]; Available from: seer.cancer.gov/seerinquiry/index.php?page = view&id = 20100014&type = q.
Surveillance, Epidemiology, and End Results Program: SEER Inquiry System (Question 20091021). 2014 [cited 2014 October 29]; Available from: seer.cancer.gov/seerinquiry/index.php?page = view&id = 20091021&type = q.
Demetri, G.D., M. von Mehren, C.R. Antonescu, R.P. DeMatteo, K.N. Ganjoo, R.G. Maki, P.W. Pisters, C.P. Raut, R.F. Riedel, S. Schuetze, H.M. Sundar, J.C. Trent, and J.D. Wayne, NCCN Task Force report: update on the management of patients with gastrointestinal stromal tumors. J Natl Compr Canc Netw, 2010. 8 Suppl 2: p. S1-41; quiz S42-4
Surveillance, Epidemiology, and End Results Program: SEER Inquiry System (Question 20021151). 2014 [cited 2014 October 29]; Available from: seer.cancer.gov/seerinquiry/index.php?page = viewid = 20021151&type = q.
Acknowledgments
The authors would like to thank Karen Koehn at the Loma Linda University Cancer Center Registry and Kelli Olsen at the City of Hope Cancer Registry for their assistance in the preparation and research of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Choi, A.H., Hamner, J.B., Merchant, S.J. et al. Underreporting of Gastrointestinal Stromal Tumors: Is the True Incidence Being Captured?. J Gastrointest Surg 19, 1699–1703 (2015). https://doi.org/10.1007/s11605-015-2860-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-015-2860-x