Abstract
Alcohol use among older adults, often denied, is a real public health problem in view of the harmful consequences it induces. The objective of this systematic review was to identify articles on the biopsychosocial factors, assessment tools, and treatment options that have proved useful for the early detection and management of alcohol use among older adults. With a view to producing a narrative synthesis from several databases, 66 articles were identified and studied, of which 45.4% (n = 30) were published between 2015 and 2020. The review is reported according to PRISMA guidelines. Although differences appear to exist between the samples studied, the analyses show that biopsychosocial factors such as quality of life, well-being, emotions, perceived stress, coping strategies, and mood disorders are associated with unhealthy alcohol use. Psychosocial factors such as strong social support appear to be correlated with low levels of alcohol use and abstinence. In general, the tools used to screen for alcohol use are AUDIT, CAGE, DPI, CARET, and SMAST-G. Interventions to prevent and manage alcohol use in older adults include CBT and brief interventions. This review of the literature provides a better understanding of which assessment tools should be used for screening. Emphasis should be placed on process-oriented scientific studies, which to date do not exist. Psychological processes mediated by biopsychosocial factors would enable the development of effective prevention interventions to be conducted in order to improve the quality of life of older adults.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
The world’s population is rapidly aging (Beard & Bloom, 2015) and older adults (OA) are now living healthier and longer lives than previous generations (Bloom et al. 2015; Skirbekk et al. 2013). The rapid growth of the population combined with the improvement in health and life expectancy raises questions about alcohol use disorders (AUD) among OA and the various risks to their health. These unprecedented demographic and epidemiological changes have been associated in studies with increased prevalence of alcohol use (AU) and heavy drinking (HD) among OA in many countries (B. H. Han et al. 2017; Wilsnack et al. 2009). AU is very common and increasing among OA, especially the baby boom generation who are now reaching old age (Kelly et al. 2018a; Kuerbis & Sacco, 2013; Palle et al. 2017).
Knowledge about AU among OA is low. Prevalence studies are sporadic, underestimated, or restricted to estimates (Khadjesari et al. 2019; Menecier et al. 2015; Paille, 2014). In addition to cross-sectional studies defining HD among OA differently, global prevalence estimates suggest that approximately 52% of OA drink alcohol in the USA, China, Korea, Mexico, Chile, and 16 European countries, and 12% of them are heavy drinkers (Calvo et al. 2020). HD among OA varies across countries, with 4% in South Africa (Peltzer & Phaswana-Mafuya, 2013), 8.2% in Finland (Immonen et al. 2011b), and 13% in Japan (Midorikawa et al. 2019). In the USA, the rate of HD in OA is estimated to range from 9.7 to 14.5% (Blazer & Wu, 2009; B. H. Han et al. 2019; Parikh et al. 2015) or even as high as 22% (Breslow et al. 2017). For over 30 years, alcohol has been the most frequently used substance among OA worldwide and the number of at-risk users is expected to increase over the next two decades (Beck et al. 2015; Khan, 2017; Moore et al. 2009). AU tends to increase over time among OA, particularly among women (Beck et al. 2015; Breslow et al. 2017; Khan, 2017; Kuerbis & Sacco, 2012). AUD among OA have increased by 107% over the past 10 years (Grant et al. 2017). However, these prevalence rates may face several biases including underreporting of AU, social desirability bias, and memory bias (Richard et al. 2019). Findings from epidemiological studies are limited due to definitions and diagnostic criteria that are considered problematic (Rolland et al. 2017). Nonetheless, these trends are concerning and suggest that more research on later-life AU is needed (Menecier et al. 2018). The term of “unhealthy alcohol use” (UAU) used in this study is commonly defined as AU that exposes OA to multiple health risks through a range of behaviors including risky AU, problematic AU, HD, and AUD (Bazzi & Saitz, 2018; Holt & Tetrault, 2016; Williams et al. 2017).
Currently, there remains a social denial of UAU among OA. This topic is little known and generally taboo (Menecier et al. 2016). Increased vigilance for these behaviors in OA is encouraged by several authors in light of the impact on individual health but also on public health (B. H. Han et al. 2017; Nubukpo et al. 2012).This research is especially relevant because AU among OA is a public health problem in terms of the adverse consequences of increased morbidity and mortality, with a role in dementia and loss of autonomy, particularly in the case of falls (Ortolá et al. 2019; Shield et al. 2016; Wang & Andrade, 2013). OA are particularly vulnerable to alcohol-related harm because of the psycho-physiological changes associated with the aging process. OA are generally exposed to numerous cognitive, environmental, and biopsychosocial risk factors, so much so that the harmful effects of alcohol are likely to manifest themselves with low-dose consumption (lower than two drinks per day) (Arndt & Schultz, 2014; Rao & Roche, 2017). Among OA, UAU is often accompanied by multiple somatic, psychiatric, and psychological disorders, which are particularly detrimental to health. OA are more likely to have co-occurring mental health disorders and comorbidities including cognition (Kaufmann et al. 2018; Sachdeva et al. 2016), depression (Lai et al. 2015), anxiety (Grant et al. 2015), liver, cardiovascular, kidney, or neurological disorders that make any AU risky (Menecier et al. 2017; Wu & Blazer, 2014). In addition, heightened sensitivity to the effects of alcohol may be exacerbated by interactions between AU and concurrent use of medication, cannabis, or other narcotics (prescribed or not). These unhealthy behaviors in OA are important and growing parallel risk factors and concerns (Blazer & Wu, 2011; Daskalopoulou et al. 2018; Hoeck & Van Hal, 2013; Li et al. 2017, 2019).
The scientific literature highlights a real difficulty for health professionals in diagnosing the signs and symptoms of UAU (Menecier et al. 2015; Rolland et al. 2017). There are many barriers to the detection and diagnosis of UAU among OA. These include the lack of awareness, knowledge, and positive caring attitudes of health professionals regarding UAU among OA (Bhatia et al. 2015; Kuerbis et al. 2015). In particular, the lack of universal diagnostic criteria specific to OA, the use of non-specific diagnostic tools, the challenges of integrating systematic screening, and the difficulties of differential diagnosis of AUD associated with unidentified co-morbidities (Gell et al. 2015; Kuerbis et al. 2017). Indeed, other age-related conditions have similar physiological and psychological consequences, making screening complicated (Maynard et al. 2016). In Europe and the USA, projections indicate that the number of OA over 65 years of age requiring treatment for problematic AU is expected to triple by 2050 (Bobak et al. 2016; B. Han et al. 2009). Today, treatments implemented to treat AUD are not specific to OA (Bhatia et al. 2015; I. B. Crome & Crome, 2018). International research on treatments for UAU in OA (Moy et al. 2011) and evidence-based preventive practices and effective policies are scarce (Anderson et al. 2012; Veerbeek et al. 2019).
Given these challenges, and in the light of the lack of empirical evidence in the scientific literature, the aim of this systematic review is to identify articles on biopsychosocial factors, assessment tools, and treatment and prevention options to treat UAU among OA. A biopsychosocial model is a multidimensional approach to addictive behaviors that considers the biomedical, psychological, and social dimensions that interact closely and underlie the emergence of addiction (Barman, 2008; Lucchini, 1985). AU involves mechanisms through a “person-substance-environment triad” that responds to this biopsychosocial approach. Each component of the model takes into account all the factors that can lead to AU by considering multifactorial individual causes, from social contexts and those specific to the substance (Berquin, 2010; Brisson, 2014; Morel & Couteron, 2019). Recently, to refine the biopsychosocial model a study by Zegarra-Parodi et al. (2019) introduced the dimensions of religion and spirituality into the clinical scenarios. This study intends to answer the following questions: (a) what biopsychosocial factors have an impact on UAU in OA? (b) what screening tools for AU can be used in OA? (c) what therapeutic approaches are useful in the care of UAU in OA?
Search Methods Employed
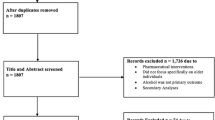
This literature review was written following the guidelines for writing and reading PRISMA systematic reviews (Moher et al. 2015; Shamseer et al. 2015; Zorzela et al. 2016). We conducted a search targeting only quantitative and qualitative scientific studies that specifically investigate AU among OA. Article titles and abstracts were independently reviewed by two reviewers and full-text articles were retrieved for possible inclusion. Figure 1 shows the PRISMA flow chart which illustrates the study selection process followed to identify relevant studies, with numbers and reasons for exclusion.
Keywords
The search strategies were designed using the thematic headings of the MeSH thesaurus. Table 1 shows the keywords used in online databases to identify relevant articles. The keywords were grouped under four search headings: Older adults; Alcohol; Psychological and psychiatric factors; Therapy and intervention. Also, given the number of studies conducted on alcohol specifically among young people, the term “binge-drinking” was deliberately omitted from the search. The Boolean operators 'OR', 'AND' and 'NOT' were used to separate, combine, or exclude terms or headings.
Database
The studies were identified via the following search engines and digital databases: Medline, PsycINFO, PubPsych, and Google Scholar. The bibliographic references of the included studies and similar literature reviews and meta-analyses were also consulted to identify articles that met the eligibility criteria.
Inclusion Criteria
Articles were selected according to the following inclusion criteria: (a) articles published in scientific journals; (b) original full-text qualitative or quantitative research articles written in English and published between 2010 and 2020, in order to have recent data; (c) all cross-sectional, longitudinal, randomized controlled trial, qualitative, cohort, and pilot studies; (d) studies involving people aged 65 and over (studies involving middle-aged adults (45–65 years) were accepted if they were associated or compared with OA); (e) studies in which AU in OA was the main variable studied. AU is defined as consumption in the past 12 months or over a lifetime, regardless of the amount and type of alcohol consumed; (f) studies evaluating the relationship between psychological factors and AU in OA and/or studies reporting findings on the effects of therapy or intervention on AU in OA.
Exclusion Criteria
Articles were excluded according to the following criteria: (a) full papers published before 2010; (b) papers not published in English; (c) studies including persons under 65 years of age; (d) studies comparing OA and young adults aged 18–45 years are discarded as they do not provide results specific to OA; (e) studies focusing mainly on organic pathologies or degenerations related to AU, e.g., metabolic syndromes, diabetes, periodontal diseases, the decline in kidney function, stroke, limitations in cognitive and physical function, cancers, coronary heart disease, etc. Because the results of these articles do not relate to alcohol consumption in older adults; (f) articles such as conference abstracts, conceptual papers, syntheses, literature reviews, or meta-analyses.
Data Extraction and Analysis
Data from the included articles were extracted in analytical grids to evaluate the international literature. The grids included, among other things, authors’ names, year of publication, period of data collection, country where the study was conducted, type of study, target outcome, method of screening for AU, psychiatric and psychological scale, demographic data, gender, average age, objectives, results of data analysis, and main outcomes.
Results of the Literature Search
Sixty-six studies were included in this review (Fig. 1). Of the 10,235 articles in the initial search results, 98% (n = 10,048) were initially excluded because they did not meet the inclusion criteria. The remaining 187 articles underwent full-text review and of these, 121 did not meet the inclusion criteria, leaving 66 separate articles deemed compliant for final inclusion. The descriptive characteristics of the articles and populations studied are summarized in Table 2. Among the 66 eligible studies, there were 459,00 participants (approximately 55% female), with a sample size ranging from 25 to 61,240 and an average age of 69.63 years. Studies were published from 2010 to 2020, of which 53% were conducted in the USA (n = 35). Studies were conducted in Europe (30.3%), Australia (7.5%), and Asia (7.5%), among others. Two studies examined only men.
Results of the Reviewed Studies
Biopsychosocial Factors
The biopsychosocial model conceptualized by Engel (Engel, 1977) systematically considers biomedical, psychological, and social factors and their complex interactions in understanding human health, illness, and health care delivery. The main outcomes reported by articles investigating biopsychosocial factors related to AU among OA are outlined in Table 3.
Quality of Life and Well-being
In a Spanish study (Ortolá et al. 2016), the authors found that compared to non-drinkers, the physical component score of the SF-12 QoL scale was significantly and slightly better for both moderate and heavy drinkers in the fully fitted model. On the other hand, there was no significant association between OAs’ AU and scores on the mental component of the SF-12 scale. Two studies (Li et al. 2017, 2019) found that lower life satisfaction was associated with a higher likelihood of AU in the Chinese sample and that higher life satisfaction was associated with a lower likelihood of high AU in the Norwegian sample. In a European study (Fuentes et al. 2017) the authors found that former drinkers, OA who had never drunk, and heavy drinkers had lower self-reported well-being than moderate drinkers. The significant negative association of HD with well-being was particularly strong in Southern Europe, especially among women. In South Africa, a study (Martinez et al. 2014) showed that quality of life (health, self-satisfaction, and money) was significantly lower among older men with UAU compared to abstainers, although this association was not significant in the adjusted analysis. Canadian research (Kaplan et al. 2012) has shown that the rate of decline in health-related quality of life over time was significantly greater among OA with declining AU than among moderate drinkers.
Coping Strategies
In studying the impact of coping strategies on UAU in OA, the authors of one study (Sacco et al. 2014) noted that stressful life events were associated with an increased likelihood of AUD among OA. Higher levels of perceived stress and victimization were also associated with AUD, but only among older men. However, there was no significant association between stressful events and perceived stress with UAU in OA. In a study of the older lesbian, gay, and bisexual (LGB) population the authors (Bryan et al. 2017) suggested that UAU is not motivated by a coping strategy to cope with a stressful situation, as day-to-day discrimination was a positive stressor positively associated with UAU only among men. Identity stigma was not significantly associated with AU among LGB OA. Withdrawal from alcohol dependence was associated with a lower likelihood of UAU among LGB OA, particularly among women. No significant association was found between perceived stress and UAU among men, but perceived stress was associated with a lower likelihood of low-risk AU among women. This suggests that women are more likely to use coping strategies other than AU under stressful conditions. A statistically significant (p < 0.01) mediating process was found in a US study (Brennan et al. 2010) among OA initiated by AU to reduce tension and the use of avoidance coping strategies to cope with stressors that were correlated with a statistically significant decrease over time in AU. According to several studies (Martinez et al. 2014; Moos et al. 2010a, b, c), AU to reduce tension, low religious involvement and/or low regular participation in religious activities predicted a higher likelihood of UAU among OA. In a longitudinal study (Platt et al. 2010), the authors reported that the importance of religion among OA was strongly correlated with a low risk of UAU, with a decrease in AU over time, not an increase. They argued that religious involvement offers more opportunities for contact with people who disapprove of excessive AU and is therefore an effective social coping strategy to deal with stressful situations. In an Irish study (Villiers-Tuthill et al. 2016), the authors reported that the perception of the positive consequences of aging in OA was negatively correlated with UAU, while a strong negative emotional representation of aging significantly increased the risk of UAU. According to the authors, these results suggest that UAU and positive behavior in the aging process could be identified as coping strategies for coping with life-changing events.
Psychosocial Factors
Six studies have shown in their analyses significant and positive associations between high levels of perceived social support and/or social activity and UAU among older women (Agahi et al. 2019; Bryan et al. 2017; Choi & DiNitto, 2011c; Dare et al. 2014; Moos et al. 2010a; Moos, Schutte, et al. 2010a, b, c). Another study (Platt et al. 2010) reports findings that that more frequent socialization with neighbors and having relatives living nearby were significantly associated with increased AU among OA. In two studies (Moos et al. 2010a; Moos et al. 2010a, b, c), the authors showed that OA who had positive relationships with their spouses or partners and peer approval of AU were significantly associated with the likelihood of having UAU over time. One study (Brennan et al. 2010) reports similar results and also pointed out that OA who have more frequent interactions with family members and friends are more likely to experience a slower rate of decline in AU as they age. In contrast, three studies (Agahi et al. 2019; Hoeck & Van Hal, 2013; Martinez et al. 2014) showed that older women with low levels of social contact and low levels of social activity were less likely to drink. However, studies report conflicting results. Two studies (Martinez et al. 2014; Platt et al. 2010) reported that having regular visits from friends or neighbors in close proximity was associated with a low risk of UAU, decreased AU, and abstention among OA. A Netherlands study (Van den Berg et al. 2014) showed that OA who abstained or had UAU had significantly less social support than OA who consumed moderately. Another study (Martinez et al. 2014) highlighted a significant association between OA low-risk AU and very low social engagement compared to abstainers. Russian(Gugushvili et al. 2018) and American(Moos et al. 2010a) research has found that OA who communicate less than once a year with their families or relatives were regular drinkers compared to those who stayed in daily contact. In 2020, one study (Villalonga-Olives et al. 2020) shows a negative interaction of positive social support on the number of drinking days that was stronger among women than men, while negative social support and social cohesion were significantly associated with AU only among women. However, four studies in this literature review found no significant association between psychosocial factors and AU among OA (Canham et al. 2016; Iparraguirre, 2015; Martinez et al. 2014; Sacco et al. 2014).
Psychiatric Comorbidities
Twelve studies showed correlations between psychiatric comorbidities and AU in OA. Among them, six studies (Blazer & Wu, 2011; Forlani et al. 2014; B. H. Han et al. 2017; Lin et al. 2014; Muñoz et al. 2018; Vaughan et al. 2014) showed that OA with mood disorders, anxiety disorders or personality disorders have a significantly higher probability of developing an AUD in their lifetime. Similarly, six studies (Bobo et al. 2013; Bryant & Kim, 2013; Choi et al. 2015; Choi & DiNitto, 2011c; Schonfeld et al. 2010; Van den Berg et al. 2014) showed that UAU among OA was significantly associated with a high likelihood of having a psychiatric comorbidity. An Irish study (Carvalho et al. 2018) found that older women, rather than men, reported that HD increased the risk of depression and anxiety. These results are comparable in three studies with different methodologies (Choi & DiNitto, 2011a; Fornazar et al. 2013; Tait et al. 2012). (Immonen et al. 2011a) reported that older at-risk drinkers differed from moderate drinkers in their reasoning when they reported drinking for a “meaningless life,” “to relieve anxiety,” or “to relieve depression.” However, nine studies (Bobo et al. 2013; Cheng et al. 2016; Gea et al. 2013; Ivan et al. 2014; Kim et al. 2015; Moos et al. 2010b; Paulson et al. 2018; Platt et al. 2010; Rodriguez et al. 2010) found significant negative correlations between alcohol consumption and low anxiety, low depression, or decreased or no depression in OA. Nevertheless, several studies (Choi & DiNitto, 2011b; Cousins et al. 2014; Hoeck & Van Hal, 2013; Ilomäki et al. 2013; Iparraguirre, 2015; Parikh et al. 2015; Sacco et al. 2016) have shown no significant association between AU and psychiatric comorbidities.
Alcohol Screening Tools
Several articles (Table 2) relied on different self-report, hetero-report, multidimensional, and self-reported quantity and frequency tools. Table 4 presents a summary of the results of studies specific to alcohol screening tools for OA.
Self-Declared Quantity and Frequency
In this systematic review of the literature, 78.8% of the studies analyzed (n = 52) used self-reported quantities and frequencies of AU by OA. In an American research (Kuerbis et al. 2017), participants reported their consumption through a series of questions from the Quantity-Frequency Variability—30 items (QFV-30; Miller & Del Boca, 1994; Tonigan et al. 1997).
Multidimensional Tools
The frequency, quantity, and trajectories of AU among OA were measured in four studies (Brennan et al. 2010; Moos et al. 2010a, b; Moos, Schutte, et al. 2010a, b, c) using adapted components of the Health and Daily Living form (HDL; Moos et al. 1990) assessing different health-related factors including AU. In a Danish research (Wieben et al. 2018), to assess the AU of OA, the authors used the Addiction Severity Index scale (ASI; McLellan et al. 1992). The ASI provides a multidimensional assessment of AU behavior. It uses generic composite scores that reflect the level of problems in seven domains including alcohol. An inverse association for the ASI composite score of alcohol with abstinence was found, showing that a worse baseline ASI is significantly associated with lower abstinence. In another Spanish research (Gea et al. 2013), the Food-Frequency Questionnaire (FFQ; Fernández-Ballart et al. 2010) was administered to assess AU. The FFQ is a validated food assessment tool that estimates the frequency and quantity of foods and beverages including alcohol.
WHO STEPwise approach to Surveillance (STEPS) standardized instrument guidelines were followed by the authors of one study(Martinez et al. 2014) to measure blood alcohol content (WHO, 2006). The diagnosis of AUD in OA was carried out in two studies (Lin et al. 2014; Sacco et al. 2014) using the Alcohol Use Disorder and Associated Disabilities Interview Schedule DSM-IV edition (AUDADIS-IV; Grant et al. 1995) an assessment method that included AU, smoking, family history of depression and selected psychiatric disorders from Axis I and II of the DSM-IV. The Brief Addiction Monitor (BAM; Cacciola et al. 2013) was used in a study to assess substance use behaviors, including alcohol.
Hetero-assessment Tools
Eleven studies diagnosed AUD in OA by referring to different versions of the Diagnostic and Statistical Manual of mental disorders (DSM). Two studies (Moos et al. 2010b; Moos, Schutte, et al. 2010a, b, c) used the DSM-III-R (American Psychiatric Association, 1990) to assess AU problems. Eight studies (Andersen et al. 2019; Blazer & Wu, 2011; Choi et al. 2015; B. H. Han et al. 2017; Lin et al. 2014; Muñoz et al. 2018; Sacco et al. 2014; Vaughan et al. 2014) used the abuse or dependence criteria defined by DSM-IV (American Psychiatric Association, 1998). One study (Andersen et al. 2019) used DSM-5 (American Psychiatric Association, 2013) substance use criteria to analyze AUD in OA. To make the diagnosis and include OA, one study (Wieben et al. 2018) used the criteria for alcohol abuse or dependence from the Classification of Mental and Behavioral Disorders (ICD-10-R; World Health Organization, 2009). Two studies (Andersen et al. 2019; Moore et al. 2011) used retrospective assessment methods to track AU over time have using the Time Line Follow Back (TLFB (Sobell & Sobell, 1992)) and the FORM 90 (Miller, 1996). One study (Sacco et al. 2016) evaluated the feasibility, acceptability, and validity of a modified daily diary to measure AU. In this study, OA were interviewed by telephone about their AU the previous day, the type of alcohol consumed, the number of units of alcohol consumed, the setting in which they drank, and whether they were alone when they drank. The results highlighted that a modified daily diary is acceptable and non-binding, especially for OA with physical limitations.
Self-Assessment Tools
Eight international studies (Immonen et al. 2011a; Kim et al. 2015; Rodriguez et al. 2010; Sacco et al. 2016; Schonfeld et al. 2010; Tait et al. 2012; Tredal et al. 2013; Van den Berg et al. 2014) used the Alcohol Use Disorders Identification Test (AUDIT Aalto et al. 2011; Babor et al. 2001)) and four studies (Fornazar et al. 2013; Gilson et al. 2019; Villiers-Tuthill et al. 2016; Watson et al. 2013) used the short version, AUDIT-C (Bush et al. 1998). In one study (Sacco et al. 2016), AUDIT scores were significantly associated with daily statements about the total number of drinks consumed and drinking alone. Six studies (Bobo et al. 2013; Carvalho et al. 2018; Cousins et al. 2014; Hoeck & Van Hal, 2013; Ilomäki et al. 2013; Platt et al. 2010) used the CAGE scale to screen for AUD (Cut down, Annoyed, Guilty, Eye-opener (Mayfield et al. 1974). Another study (Platt et al. 2010) found in their study that a unit increase in the CAGE score was associated with an increased likelihood of being in the group of OA with increasing AU. On the other hand, an increase in the CAGE score made the OA less likely to be in the group with declining AU than in the abstentionist group. In addition, in one research study (Bobo et al. 2013), the authors noted that at-risk drinkers were significantly more likely to self-report recent HD and to have a high CAGE score compared to moderate drinkers. The Michigan Alcoholism Screening Test-Geriatric version was developed specifically for OA (MAST-G; (Blow et al. 1992)). In their study, the authors compared the MAST-G to the Fast Alcohol Screening Test (FAST (Hodgson et al. 2002)). The prevalence of alcohol abuse in OA was significantly underreported with the FAST (p < 0.0001). No subjects scored positive on this test, whereas the MAST-G recorded positive scores in OA. Two studies (Rodriguez et al. 2010; Schonfeld et al. 2010) used the shortened version of the MAST-G, the SMAST-G (Blow et al. 1998). An Australian version of the Alcohol Related Problems Survey(ARPS Fink et al. 2002; Moore et al. 2000, 2002; Oishi et al. 2001) renamed A-ARPS) was adapted and validated by authors of a study (Bright et al. 2015). The recalibrated scoring algorithms of the A-ARPS were used to reliably classify OA to reduce the incidence of AUD. Three studies (Ettner et al. 2014; Kuerbis et al. 2015; Moore et al. 2011) used the Comorbidity Alcohol Risk Evaluation Tool (CARET (Barnes et al. 2010)). CARET is an updated and revised version of the short version of ARPS (ShARPS). Four studies (Brennan et al. 2010; Moos et al. 2010b; Moos, Schutte, et al. 2010a, b, c; Watson et al. 2013) used the Drinking Problems Index (DPI (Finney et al. 1991)) to assess AU problems in OA. In 2019, One study (Gilson et al. 2019) validated the “Comprehensive Effects of Alcohol” (CEOA) questionnaire, which measures an OA’s expected outcome from AU in various domains (sociability, tension reduction, courage, sexuality, cognitive and behavioral problems, risk and aggression, and self-perception). The results highlighted the empirical validity with excellent fit and internal consistency of a two-factor expectation model comprising a negative 10-item expectation factor and a positive 10-item expectation factor. They concluded that the CEOA may provide a correct and more efficient measure of AU among OA.
Treatment Options
The outcomes of studies on therapies and interventions for the care of OA who consume alcohol are summarized in Table 5.
Brief Intervention
The development and examination of the effectiveness of the Florida Brief Intervention and Treatment for Elders (BRITE) project was conducted in one study (Schonfeld et al. 2010). Individuals who screened positive in SMAST-G were offered brief intervention and treatment with evidence-based practices and were reviewed at the exit of the intervention program and in follow-up interviews. The authors found that OA who received the brief intervention had a significant decrease in their SMAST-G score and also at the 30-day follow-up. A randomized controlled trial was conducted in a research study (Moore et al. 2011) to test the effectiveness of a multi-component primary care-based screening and education intervention to reduce at-risk AU among OA. After three months, compared to the control group, the authors found that there were fewer at-risk alcohol users in the group of participants who received the educational intervention. OA reported consuming fewer drinks in the past seven days, consuming less alcohol and having lower risk scores. After 12 months, only the difference in the number of drinks consumed remained statistically significant, but the educational intervention did not reduce UAU. Similar results were observed in another study of a brief mail intervention (Kuerbis et al. 2015). However, in two educational intervention studies, the authors (Duru et al. 2015; Ettner et al. 2014) showed that at 12 months discussing alcohol risk with a doctor, entering into an AU agreement and/or self-reporting the use of an AU diary was associated with a lower likelihood of UAU during therapeutic follow-up. In an attempt to compare the clinical and cost-effectiveness of a staged intensive care intervention versus a brief intervention in primary care, the authors of two studies (Vrdoljak et al. 2014; Watson et al. 2013) showed that there were no significant differences. Staggered intensive care did not confer an advantage over brief interventions in terms of reducing AU in the treatment of OA. In two studies (Lin et al. 2010a, b; Lin et al. 2010a, b), the authors found that brief telephone interventions were effective in reducing AU among OA in primary care settings. OA who answered the calls were more likely to switch to moderate AU at 3 months than those who did not answer any of the calls. Concerns about risk, reading the educational booklets and the perception of physicians advising OA to reduce AU were associated with early reductions in AU among OA with UAU at the first phone call from a health educator. Two other studies (B. H. Han et al. 2018; Kuerbis et al. 2017) demonstrated the effectiveness of an online screening and intervention tool that identified many OA with UAU. Most OA were receptive to the idea of receiving a plan to change their AU behavior. Moreover, in a study (Zanjani et al. 2018), the authors reported that preventive interventions consisting of posters, brochures for patients and pharmacists and public service announcements provided positive feedback and increased OA’s understanding of preventing alcohol and medication interactions (AMI), with statistically significant changes in the perceived importance of messages about UAU and the potential consequences of AMI.
Cognitive and Behavioral Therapies
Authors of one research study (Wieben et al. 2018) found that OA who consumed alcohol and received cognitive and behavioral therapies (CBT) had significantly higher compliance rates than middle-aged adults. Moreover, OA achieved a significant improvement in AU patterns in the first six months of CBT and reported abstinence or drinking no more than 3 drinks per day. Having undergone CBT was positively associated with abstinence and compliance with therapy increased the likelihood of abstinence. OA who received comprehensive and integrated outpatient treatment that combined psychosocial management for AUD with dependence had better outcomes at 6 months on a range of AU outcome measures compared with middle-aged patients (p < 0.001). One study (Andersen et al. 2019) sought to evaluate the addition of the Community Reinforcement Approach (CRA-S) to Motivational Enhancement Therapy (MET) in the treatment of OA with AUD. Both MET and MET + CRA-S resulted in reductions in AU in terms of the number of days of drinking, the number of days of binge drinking, and the amount of alcohol consumed per week. The results of the study showed that community reinforcement for OA did not alter the improvement in AU outcomes, as the chances of success in MET vs. MET + CRA-S conditions did not differ. Both treatment options also showed small improvements in patients’ quality of life.
Summary of Conclusions
The research reported in this review was part of a comprehensive synthesis of the evidence on AU among OA internationally to further knowledge of this phenomenon. A peak in the frequency of studies (45.4% (n = 30)) was observed between 2015 and 2020, indicative of the recent and growing interest in this issue. Indeed, unlike adolescents or young adults, there are very few studies and a lack of evidence and empirical data in the literature specific to AU in OA. Subsequently, a large number of scientists have shown an interest in the risk factors and consequences of AU in OA.
Analysis of the studies suggests that biopsychosocial factors have a strong influence on AU among OA despite the contrasting results. As the authors point out, these results show that certain variables determining AU can be the subject of appropriate psychological and psychiatric support in OA. Mood, anxiety, or personality disorders appear to have a significant influence and to increase the likelihood of UAU in OA (Blazer & Wu, 2011; Forlani et al. 2014; B. H. Han et al. 2017; Lin et al. 2014; Muñoz et al. 2018; Vaughan et al. 2014). The relationship between mental health diagnoses on AU has been confirmed, thus requiring special attention in clinical practice with OA. They constitute a heterogeneous group and report drinking for a variety of reasons. They may drink alcohol for medicinal purposes, for a self-perceived meaningless life and to relieve anxiety, loneliness or depression (Immonen et al. 2011a). The risks associated with AU are not minimal among OA. Clinicians need to be aware of these comorbidities during the care of a mental disorder. Studies have shown that end-of-life variables associated with social resources, social support, social learning, stress and coping strategy, and social control theories predicted UAU in OA. One of the most consistent predictors was the approval of AU by members of the social network(Moos, Brennan, et al. 2010a). These findings reflect long-term, two-way influencing processes in which OA’s social resources and UAU may amplify, attenuate or reverse each other (Moos, Schutte, et al. 2010a, b, c). Similarly, the use of avoidance coping strategies to manage stressors would seem to be the main variable predicting a decrease in AU over time (Brennan et al. 2010). Our results show that religious practice and being surrounded by people who disapprove of AU are protective factors in favor of abstinence (Martinez et al. 2014; Platt et al. 2010). Our interpretation of the results is that OA consume alcohol in social situations and that social integration also predicts continued AU habits. Social activity seems to be more strongly associated with more frequent AU than social contact (Agahi et al. 2019; Brennan et al. 2010; Hoeck & Van Hal, 2013; Martinez et al. 2014; Platt et al. 2010). Stressful life events, victimization, discrimination, and perceived stress also appear to be associated with AUD in OA (Sacco et al. 2014). Conversely, perceived stress among older women is associated with a lower likelihood of UAU (Bryan et al. 2017). Identity stigmatization was not significantly associated with AU in OA(Bryan et al. 2017; Sacco et al. 2014). We also found that aging representations of self-perception and emotions may foster UAU in OA(Villiers-Tuthill et al. 2016). Similarly, greater satisfaction with life appears to be a variable determining low AU among OA (Li et al. 2017, 2019). Negative perceptions of well-being appear to be associated with UAU in OA, particularly among women in southern Europe (Fuentes et al. 2017). However, we have previously pointed out that the results are very mixed, and several studies have not shown a significant relationship between AU in OA and biopsychosocial factors (Canham et al. 2016; Choi & DiNitto, 2011b; Cousins et al. 2014; Hoeck & Van Hal, 2013; Ilomäki et al. 2013; Iparraguirre, 2015; Martinez et al. 2014; Parikh et al. 2015; Sacco et al. 2014, 2016).
To detect UAU among OA, several scales and screening tools exist although some are adaptations of instruments initially created for young adults. Self-questionnaires, hetero-questionnaires, and self-report measures of AU are not binding for OA (Kuerbis et al. 2014). In this review, AUDIT (Aalto et al. 2011; Babor et al. 2001; Bush et al. 1998), CAGE (Mayfield et al. 1974), MAST-G(Blow et al. 1992, 1998), DPI (Finney et al. 1991), and CARET (Barnes et al. 2010) are the self-assessment scales commonly used in the majority of studies to identify AUD in OA. DSM-III-TR, DSM-IV, and DSM 5 (American Psychiatric Association, 1990, 1998, 2013) diagnostic criteria have been used in some studies to make a diagnosis of alcohol abuse and dependence. The validity of these diagnostic criteria has been shown in several studies (Denis et al. 2015; Fazzino et al. 2014; Hasin et al. 2012; Peer et al. 2013). Almost all the studies reviewed (78.8% n = 52) collected self-reported data to assess average AU, to estimate frequency, or to quantify AU through direct questions supported or not by visual aids.
Concerning treatment options, the studies in this review showed that following and complying with CBT is associated with and increases the likelihood of abstinence (Wieben et al. 2018). Community reinforcement does not appear to change anything in the improvement in OA’s AU (Andersen et al. 2019). Our outcomes showed that interventions involving personalized feedback, educational materials, counseling and medical follow-up could be very effective (Kuerbis et al. 2015; Moore et al. 2011; Schonfeld et al. 2010). However, the results regarding the effects of the interventions were mixed (Duru et al. 2015; Ettner et al. 2014; Vrdoljak et al. 2014; Watson et al. 2013). Nonetheless, it should be noted that individual brief interventions that had positive effects included: an “intensive” brief intervention; a brief postal intervention with personalized feedback; group and family therapies; advice to reduce AU; motivational interviewing; therapeutic education; posters; brochures; telephone calls and web-based assessments (B. H. Han et al. 2018; Kuerbis et al. 2017; Lin et al. 2010a, b; Lin et al. 2010a, b; Zanjani et al. 2018). We find similar results in four studies demonstrating that interventions can reduce AU among OA and provide support to maintain and improve their health, while minimizing risk behaviors (Armstrong-Moore et al. 2018; Caputo et al. 2012; Dedert et al. 2015; Kelly et al. 2016, 2018b).
Within our study, it is plausible to distinguish several limitations. First, the conclusions of the literature review diverge because of the different assessment methods used, the interacting environmental factors, the heterogeneity of the study populations, and the potentially different AU patterns. Limitations of the outcomes in our review include the fact that self-reported AU is likely to be underestimated to some extent in all studies. The measurement instruments and scales used in the different study protocols were mostly self-report tools that may have led participants to report “fair” or “pleasant” responses. This phenomenon is social desirability bias in reporting AU that may impact screening for AUD and bias the level of accuracy of responses when collecting data in OA (Davis et al. 2010; Kypri et al. 2016). This may be exacerbated if OA feel stigmatized by AU in any way. Indeed, OA are likely to underreport or not accurately report their actual AU, particularly among heavy drinkers and women. However, scientific research suggests that self-reports should be considered as accurate, reliable and valid as other measures (Del Boca & Darkes, 2003; Kirchner et al. 2007; Sayers et al. 2004). In addition, 95.5% of the studies used screening tools for AU that were not specific to OA, which may represent a sensitivity bias in the UAU prevalence outcomes. Similarly, the different cross-sectional designs of some studies prevent us from making causal assertions about certain outcomes. Also, because of our non-inclusion criteria, some issues in our studies could not be addressed, such as the relationship between AU and medical comorbidities. Another limitation is that not investigating the impact of where OA live does not allow us to know whether or not living in a rural or urban setting is a risk or protective factor for AU and whether or not treatment options may or may not differ based on this distinction. Despite the multiracial nature of the countries included in our systematic review of the literature, a limitation of our results is the lack of information regarding race and possible associated differences in AU or UAU. Indeed, results focusing on race would raise possible social inequalities in health in terms of the impact of AU on biopsychosocial factors and treatment care. The aim was to provide an overview of treatment options reported in studies published over the past decade. The studies included in our review are primarily focused on early interventions, with an included population that appears to have a high literacy rate, thus being able to understand the posters and literature and participate in types of interventions such as CBT. Thus, one limitation of the outcomes on treatment options is that some of the brief interventions mentioned are only appropriate for OA with some level of education. In addition, no studies stipulate what is in place for the segment of the older adult population that cannot benefit from these types of interventions such as the homeless, those who do not have access to or knowledge of the use of certain technologies (e.g., telephone, computer,). In addition, little information on primary prevention or health promotion for OA was found in the literature to prevent the development of UAU. Interventions in primary care are limited by the fact that strategies, such as outreach to hard-to-serve isolated older adult populations, are not defined. In addition, OA may be more vulnerable to alcohol-related problems and may be seen more frequently in hospital emergency departments, shelters, or detoxification centers. Given the inequalities in terms of capacity, there is thus a need for a broader range of interventions and resource allocation to be developed for the different segments of the older adult population.
Conclusion
Beliefs that OA do not consume alcohol or do not consume it in a problematic manner have been dismissed. Excessive AU continues to increase significantly among OA, particularly women. These trends in AU present unique risks and challenges. Knowledge about AU in OA and the problems that contribute to the onset or maintenance of addiction in later years will need to be continually updated as we discover what motivates this generation of adults to drink. Unlike adolescents and younger adults, due to psychophysiological degeneration, OA are at risk and more vulnerable to UAU and complications often manifesting themselves in a specific forms that can be confused with geriatric syndromes. Thus, future research is needed to advance and develop specific screening tools for OA to distinguish the symptoms of AU from those of the aging process. Further longitudinal studies are also needed to examine the threshold, frequency and patterns of AU and the impact on the health of OA. Increased attention is required in public health initiatives. Effective treatment options do exist, but generally remain limited, as few health programs or services offer interventions tailored to OA. Denial of AUD in OA is not a solution. The health system will be called upon to invest in the well-being of OA by culturally acclimatizing services so that they are not prevented from being cared for because of their age. Future research should focus on the development of interventions that build on the knowledge, beliefs, social representations, and attitudes of caregivers in order to raise awareness and improve their role in primary health care for OA. Emphasis should be placed on process-oriented and multidimensional scientific studies. Psychological processes-mediating biopsychosocial factors would allow the development of effective preventive interventions to be conducted in order to improve the quality of life of OA and reduce health inequalities.
References
Aalto, M., Alho, H., Halme, J. T., & Seppä, K. (2011). The alcohol use disorders identification test (AUDIT) and its derivatives in screening for heavy drinking among the elderly. International Journal of Geriatric Psychiatry, 26(9), 881–885. https://doi.org/10.1002/gps.2498
Agahi, N., Dahlberg, L., & Lennartsson, C. (2019). Social integration and alcohol consumption among older people : A four-year follow-up of a Swedish national sample. Drug and Alcohol Dependence, 196, 40–45. https://doi.org/10.1016/j.drugalcdep.2018.12.011
American Psychiatric Association. (1990). Diagnostic and statistical manual of mental disorders : DSM-III-R (3. ed., rev.[Nachdr.]). American Psychiatric Association.
American Psychiatric Association (Éd.). (1998). Diagnostic and statistical manual of mental disorders : DSM-IV ; includes ICD-9-CM codes effective 1. Oct. 96 (4. ed., 7. print).
American Psychiatric Association (Éd.). (2013). Diagnostic and statistical manual of mental disorders : DSM-5 (5. ed). American Psychiatric Publishing.
Andersen, K., Behrendt, S., Bilberg, R., Bogenschutz, M. P., Braun, B., Buehringer, G., Ekstrøm, C. T., Mejldal, A., Petersen, A. H., & Nielsen, A. S. (2019). Evaluation of adding the Community reinforcement approach to motivational enhancement therapy for adults aged 60 years and older with DSM-5 alcohol use disorder : A randomised controlled trial. Addiction (Abingdon, England), 0(ja). https://doi.org/10.1111/add.14795
Anderson, P., Scafato, E., & Galluzzo, L. (2012). Alcohol and older people from a public health perspective. Annali Dell’istituto Superiore Di Sanità, 48(3), 232–247. https://doi.org/10.4415/ANN_12_03_04
Armstrong-Moore, R., Haighton, C., Davinson, N., & Ling, J. (2018). Interventions to reduce the negative effects of alcohol consumption in older adults : A systematic review. BMC Public Health, 18(1), 302. https://doi.org/10.1186/s12889-018-5199-x
Arndt, S., & Schultz, S. K. (2014). Epidemiology and demography of alcohol and the older person. In I. Crome, L.-T. Wu, R. T. Rao, & P. Crome (Éds.), Substance Use and Older People (p. 75‑90). John Wiley & Sons, Ltd. https://doi.org/10.1002/9781118430965.ch7
Babor, T. F., Higgins-Biddle, J. C., Saunders, J. B., & Monteiro, M. G. (2001). The alcohol use disorders identification test, guidelines for use in primary care. 41.
Barnes, A. J., Moore, A. A., Xu, H., Ang, A., Tallen, L., Mirkin, M., & Ettner, S. L. (2010). Prevalence and correlates of at-risk drinking among older adults : The Project SHARE Study. Journal of General Internal Medicine, 25(8), 840–846. https://doi.org/10.1007/s11606-010-1341-x
Bazzi, A., & Saitz, R. (2018). Screening for unhealthy alcohol use. JAMA, 320(18), 1869–1871. https://doi.org/10.1001/jama.2018.16069
Beard, J. R., & Bloom, D. E. (2015). Towards a comprehensive public health response to population ageing. Lancet (london, England), 385(9968), 658–661. https://doi.org/10.1016/S0140-6736(14)61461-6
Beck, F., Richard, J.-B., Guignard, R., Le Nézet, O., & Spilka, S. (2015). Les niveaux d’usage des drogues en France en 2014—Tendances 99—Mars 2015—OFDT. https://www.ofdt.fr/publications/collections/periodiques/lettre-tendances/les-niveaux-dusage-des-drogues-en-france-en-2014-tendances-99-mars-2015/
Berquin, A. (2010). Le modèle biopsychosocial : Beaucoup plus qu’un supplément d’empathie. Revue Médicale Suisse, 6(258), 1511‑1513. La Revue Medicale Suisse.
Bhatia, U., Nadkarni, A., Murthy, P., Rao, R., & Crome, I. (2015). Recent advances in treatment for older people with substance use problems : An updated systematic and narrative review. European Geriatric Medicine, 6(6), 580–586. https://doi.org/10.1016/j.eurger.2015.07.001
Blazer, D. G., & Wu, L.-T. (2009). The epidemiology of at-risk and binge drinking among middle-aged and elderly community adults : National Survey on Drug Use and Health. The American Journal of Psychiatry, 166(10), 1162–1169. https://doi.org/10.1176/appi.ajp.2009.09010016
Blazer, D. G., & Wu, L.-T. (2011). The epidemiology of alcohol use disorders and subthreshold dependence in a middle-aged and elderly community sample. The American Journal of Geriatric Psychiatry, 19(8), 685–694. https://doi.org/10.1097/JGP.0b013e3182006a96
Bloom, D. E., Chatterji, S., Kowal, P., Lloyd-Sherlock, P., McKee, M., Rechel, B., Rosenberg, L., & Smith, J. P. (2015). Macroeconomic implications of population ageing and selected policy responses. Lancet (london, England), 385(9968), 649–657. https://doi.org/10.1016/S0140-6736(14)61464-1
Blow, F., Brower, K., Schulenberg, J., Demo-Dananberg, L., Young, J., & Beresford, T. (1992). The Michigan alcoholism screening test-geriatric version (MAST-G): A new elderly-specific screening instrument. Alcoholism Clinical and Experimental Research, 16(2), 372.
Blow, F., Gillespie, B., Barry, K., Mudd, S., & Hill, E. (1998). Brief screening for alcohol problems in elderly populations using the Short Michigan Alcoholism Screening Test-Geriatric Version Smast-G. Alcoholism, Clinical and Experimental Research, 22(3), 131.
Bobak, M., Malyutina, S., Horvat, P., Pajak, A., Tamosiunas, A., Kubinova, R., Simonova, G., Topor-Madry, R., Peasey, A., Pikhart, H., & Marmot, M. G. (2016). Alcohol, drinking pattern and all-cause, cardiovascular and alcohol-related mortality in Eastern Europe. European Journal of Epidemiology, 31, 21–30. https://doi.org/10.1007/s10654-015-0092-8
Bobo, J. K., Greek, A. A., Klepinger, D. H., & Herting, J. R. (2013). Predicting 10-year alcohol use trajectories among men age 50 years and older. The American Journal of Geriatric Psychiatry, 21(2), 204–213. https://doi.org/10.1016/j.jagp.2012.10.021
Brennan, P. L., Schutte, K. K., & Moos, R. H. (2010). Patterns and predictors of late-life drinking trajectories : A 10-year longitudinal study. Psychology of Addictive Behaviors : Journal of the Society of Psychologists in Addictive Behaviors, 24(2), 254–264. https://doi.org/10.1037/a0018592
Breslow, R. A., Castle, I.-J.P., Chen, C. M., & Graubard, B. I. (2017). Trends in alcohol consumption among older Americans : National health interview surveys, 1997–2014. Alcoholism, Clinical and Experimental Research, 41(5), 976–986. https://doi.org/10.1111/acer.13365
Bright, S. J., Fink, A., Beck, J. C., Gabriel, J., & Singh, D. (2015). Development of an Australian version of the alcohol-related problems survey : A comprehensive computerised screening tool for older adults. Australasian Journal on Ageing, 34(1), 33–37. https://doi.org/10.1111/ajag.12098
Brisson, P. (2014). Prévention des toxicomanies : Aspects théoriques et méthodologiques (Deuxième édition revue et augmentée). Les Presses de l’Université de Montréal.
Bryan, A. E. B., Kim, H.-J., & Fredriksen-Goldsen, K. I. (2017). Factors associated with high-risk alcohol consumption among LGB older adults : The Roles of gender, social support, perceived stress, discrimination, and stigma. The Gerontologist, 57(Suppl 1), S95–S104. https://doi.org/10.1093/geront/gnw100
Bryant, A. N., & Kim, G. (2013). The Relation between frequency of binge drinking and psychological distress among older adult drinkers. Journal of Aging and Health, 25(7), 1243–1257. https://doi.org/10.1177/0898264313499933
Bush, K., Kivlahan, D. R., McDonell, M. B., Fihn, S. D., & Bradley, K. A. (1998). The AUDIT alcohol consumption questions (AUDIT-C): An effective brief screening test for problem drinking Ambulatory Care Quality Improvement Project (ACQUIP) Alcohol Use Disorders Identification Test. Archives of Internal Medicine, 158(16), 1789–1795. https://doi.org/10.1001/archinte.158.16.1789
Cacciola, J. S., Alterman, A. I., DePhilippis, D., Drapkin, M. L., Valadez, C., Fala, N. C., Oslin, D., & McKay, J. R. (2013). Development and initial evaluation of the brief addiction monitor (BAM). Journal of Substance Abuse Treatment, 44(3), 256–263. https://doi.org/10.1016/j.jsat.2012.07.013
Calvo, E., Medina, J. T., Ornstein, K. A., Staudinger, U. M., Fried, L. P., & Keyes, K. M. (2020). Cross-country and historical variation in alcohol consumption among older men and women : Leveraging recently harmonized survey data in 21 countries. Drug and Alcohol Dependence, 215, 108219. https://doi.org/10.1016/j.drugalcdep.2020.108219
Canham, S. L., Mauro, P. M., Kaufmann, C. N., & Sixsmith, A. (2016). Association of alcohol use and loneliness frequency among middle-aged and older adult drinkers. Journal of Aging and Health, 28(2), 267–284. https://doi.org/10.1177/0898264315589579
Caputo, F., Vignoli, T., Leggio, L., Addolorato, G., Zoli, G., & Bernardi, M. (2012). Alcohol use disorders in the elderly : A brief overview from epidemiology to treatment options. Experimental Gerontology, 47(6), 411–416. https://doi.org/10.1016/j.exger.2012.03.019
Carvalho, A. F., Stubbs, B., Maes, M., Solmi, M., Vancampfort, D., Kurdyak, P. A., Brunoni, A. R., Husain, M. I., & Koyanagi, A. (2018). Different patterns of alcohol consumption and the incidence and persistence of depressive and anxiety symptoms among older adults in Ireland : A prospective community-based study. Journal of Affective Disorders, 238, 651–658. https://doi.org/10.1016/j.jad.2018.06.041
Cheng, H. G., Chen, S., McBride, O., & Phillips, M. R. (2016). Prospective relationship of depressive symptoms, drinking, and tobacco smoking among middle-aged and elderly community-dwelling adults : Results from the China Health and Retirement Longitudinal Study (CHARLS). Journal of Affective Disorders, 195, 136–143. https://doi.org/10.1016/j.jad.2016.02.023
Choi, N. G., & DiNitto, D. M. (2011a). Psychological Distress, binge/heavy drinking, and gender differences among older adults. The American Journal on Addictions, 20(5), 420–428. https://doi.org/10.1111/j.1521-0391.2011.00149.x
Choi, N. G., & DiNitto, D. M. (2011b). Drinking, smoking, and psychological distress in middle and late Life. Aging & Mental Health, 15(6), 720–731. https://doi.org/10.1080/13607863.2010.551343
Choi, N. G., & DiNitto, D. M. (2011c). Heavy/binge drinking and depressive symptoms in older adults : Gender differences. International Journal of Geriatric Psychiatry, 26(8), 860–868. https://doi.org/10.1002/gps.2616
Choi, N. G., DiNitto, D. M., & Marti, C. N. (2015). Alcohol and other substance use, mental health treatment use, and perceived unmet treatment need : Comparison between baby boomers and older adults. The American Journal on Addictions, 24(4), 299–307. https://doi.org/10.1111/ajad.12225
Cousins, G., Galvin, R., Flood, M., Kennedy, M.-C., Motterlini, N., Henman, M. C., Kenny, R.-A., & Fahey, T. (2014). Potential for alcohol and drug interactions in older adults : Evidence from the Irish longitudinal study on ageing. BMC Geriatrics, 14, 57. https://doi.org/10.1186/1471-2318-14-57
Crome, I. B., & Crome, P. (2018). Alcohol and age. Age and Ageing, 47(2), 164–167. https://doi.org/10.1093/ageing/afx191
Dare, J., Wilkinson, C., Allsop, S., Waters, S., & McHale, S. (2014). Social engagement, setting and alcohol use among a sample of older Australians. Health & Social Care in the Community, 22(5), 524–532. https://doi.org/10.1111/hsc.12110
Daskalopoulou, C., Stubbs, B., Kralj, C., Koukounari, A., Prince, M., & Prina, A. M. (2018). Associations of smoking and alcohol consumption with healthy ageing : A systematic review and meta-analysis of longitudinal studies. British Medical Journal Open, 8(4), e019540. https://doi.org/10.1136/bmjopen-2017-019540
Davis, C. G., Thake, J., & Vilhena, N. (2010). Social desirability biases in self-reported alcohol consumption and harms. Addictive Behaviors, 35(4), 302–311. https://doi.org/10.1016/j.addbeh.2009.11.001
Dedert, E. A., McDuffie, J. R., Stein, R., McNiel, J. M., Kosinski, A. S., Freiermuth, C. E., Hemminger, A., & Williams, J. W. (2015). Electronic Interventions for alcohol misuse and alcohol use disorders A systematic review. Annals of internal medicine, 163(3), 205–214. https://doi.org/10.7326/M15-0285
Del Boca, F. K., & Darkes, J. (2003). The validity of self-reports of alcohol consumption : State of the science and challenges for research. Addiction, 98(s2), 1–12. https://doi.org/10.1046/j.1359-6357.2003.00586.x
Denis, C. M., Gelernter, J., Hart, A. B., & Kranzler, H. R. (2015). Inter-observer reliability of DSM-5 substance use disorders. Drug and Alcohol Dependence, 153, 229–235. https://doi.org/10.1016/j.drugalcdep.2015.05.019
Duru, O. K., Xu, H., Moore, A. A., Mirkin, M., Ang, A., Tallen, L., Tseng, C.-H., & Ettner, S. L. (2015). Examining the Impact of separate components of a multi-component intervention designed to reduce at-risk drinking among older adults : The Project SHARE Study. Alcoholism, Clinical and Experimental Research, 39(7), 1227–1235. https://doi.org/10.1111/acer.12754
Engel, G. L. (1977). The Need for a new medical model : A challenge for biomedicine. Science, 196(4286), 129–136. https://doi.org/10.1126/science.847460
Ettner, S. L., Xu, H., Duru, O. K., Ang, A., Tseng, C.-H., Tallen, L., Barnes, A., Mirkin, M., Ransohoff, K., & Moore, A. A. (2014). The effect of an educational intervention on alcohol consumption, at-risk drinking, and health care utilization in older adults : The Project SHARE study. Journal of Studies on Alcohol and Drugs, 75(3), 447–457. https://doi.org/10.15288/jsad.2014.75.447
Fazzino, T. L., Rose, G. L., Burt, K. B., & Helzer, J. E. (2014). A test of the DSM-5 severity scale for alcohol use disorder. Drug and Alcohol Dependence, 141, 39–43. https://doi.org/10.1016/j.drugalcdep.2014.05.004
Fernández-Ballart, J. D., Piñol, J. L., Zazpe, I., Corella, D., Carrasco, P., Toledo, E., Perez-Bauer, M., Martínez-González, M. A., Salas-Salvadó, J., & Martín-Moreno, J. M. (2010). Relative validity of a semi-quantitative food-frequency questionnaire in an elderly Mediterranean population of Spain. The British Journal of Nutrition, 103(12), 1808–1816. https://doi.org/10.1017/S0007114509993837
Fink, A., Morton, S. C., Beck, J. C., Hays, R. D., Spritzer, K., Oishi, S., & Moore, A. A. (2002). The alcohol-related problems survey : Identifying hazardous and harmful drinking in older primary care patients. Journal of the American Geriatrics Society, 50(10), 1717–1722. https://doi.org/10.1046/j.1532-5415.2002.50467.x
Finney, J. W., Moos, R. H., & Brennan, P. L. (1991). The drinking problems index : A measure to assess alcohol-related problems among older adults. Journal of Substance Abuse, 3(4), 395–404. https://doi.org/10.1016/S0899-3289(10)80021-5
Forlani, M., Morri, M., Belvederi Murri, M., Bernabei, V., Moretti, F., Attili, T., Biondini, A., De Ronchi, D., & Atti, A. R. (2014). Anxiety symptoms in 74+ community-dwelling elderly : Associations with physical morbidity, depression and alcohol consumption. PLoS ONE, 9(2). https://doi.org/10.1371/journal.pone.0089859
Fornazar, R., Spak, F., Dahlin-Ivanoff, S., & Wilhelmson, K. (2013). Alcohol consumption among the oldest old and how it changes during two years [Research article]. International Scholarly Research Notices. https://doi.org/10.1155/2013/671218
Fuentes, S., Bilal, U., Galán, I., Villalbí, J. R., Espelt, A., Bosque-Prous, M., Franco, M., & Lazo, M. (2017). Binge drinking and well-being in European older adults : Do gender and region matter? European Journal of Public Health, 27(4), 692–699. https://doi.org/10.1093/eurpub/ckw246
Gea, A., Beunza, J. J., Estruch, R., Sánchez-Villegas, A., Salas-Salvadó, J., Buil-Cosiales, P., Gómez-Gracia, E., Covas, M.-I., Corella, D., Fiol, M., Arós, F., Lapetra, J., Lamuela-Raventós, R.-M., Wärnberg, J., Pintó, X., Serra-Majem, L., Martínez-González, M. A., & for the PREDIMED GROUP. (2013). Alcohol intake, wine consumption and the development of depression : The PREDIMED study. BMC Medicine, 11(1), 192. https://doi.org/10.1186/1741-7015-11-192
Gell, L., Meier, P. S., & Goyder, E. (2015). Alcohol consumption among the over 50s : International comparisons. Alcohol and Alcoholism, 50(1), 1–10. https://doi.org/10.1093/alcalc/agu082
Gilson, K.-M., Judd, F., & Bryant, C. (2019). Validation of the comprehensive effects of alcohol questionnaire in older adults. Substance Use & Misuse, 54(12), 2043–2052. https://doi.org/10.1080/10826084.2019.1627558
Grant, B. F., Chou, S. P., Saha, T. D., Pickering, R. P., Kerridge, B. T., Ruan, W. J., Huang, B., Jung, J., Zhang, H., Fan, A., & Hasin, D. S. (2017). Prevalence of 12-month alcohol use, high-risk drinking, and DSM-IV alcohol use disorder in the United States, 2001–2002 to 2012–2013: Results from the national epidemiologic survey on alcohol and related conditions. JAMA Psychiatry, 74(9), 911–923. https://doi.org/10.1001/jamapsychiatry.2017.2161
Grant, B. F., Goldstein, R. B., Saha, T. D., Chou, S. P., Jung, J., Zhang, H., Pickering, R. P., Ruan, W. J., Smith, S. M., Huang, B., & Hasin, D. S. (2015). Epidemiology of DSM-5 alcohol use disorder. JAMA Psychiatry, 72(8), 757–766. https://doi.org/10.1001/jamapsychiatry.2015.0584
Grant, B. F., Harford, T. C., Dawson, D. A., Chou, P. S., & Pickering, R. P. (1995). The alcohol use disorder and associated disabilities interview schedule (AUDADIS): Reliability of alcohol and drug modules in a general population sample. Drug and Alcohol Dependence, 39(1), 37–44. https://doi.org/10.1016/0376-8716(95)01134-K
Gugushvili, A., Azarova, A., Irdam, D., Crenna-Jennings, W., Murphy, M., McKee, M., & King, L. (2018). Correlates of frequent alcohol consumption among middle-aged and older men and women in Russia : A multilevel analysis of the PrivMort retrospective cohort study. Drug and Alcohol Dependence, 188, 39–44. https://doi.org/10.1016/j.drugalcdep.2018.03.038
Han, B., Gfroerer, J. C., Colliver, J. D., & Penne, M. A. (2009). Substance use disorder among older adults in the United States in 2020. Addiction, 104(1), 88–96. https://doi.org/10.1111/j.1360-0443.2008.02411.x
Han, B. H., Masukawa, K., Rosenbloom, D., Kuerbis, A., Helmuth, E., Liao, D. H., & Moore, A. A. (2018). Use of web-based screening and brief intervention for unhealthy alcohol use by older adults. Journal of Substance Abuse Treatment, 86, 70–77. https://doi.org/10.1016/j.jsat.2018.01.002
Han, B. H., Moore, A. A., Ferris, R., & Palamar, J. J. (2019). Binge drinking among older adults in the United States, 2015 to 2017. Journal of the American Geriatrics Society, 67(10), 2139–2144. https://doi.org/10.1111/jgs.16071
Han, B. H., Moore, A. A., Sherman, S., Keyes, K. M., & Palamar, J. J. (2017). Demographic trends of binge alcohol use and alcohol use disorders among older adults in the United States, 2005–2014. Drug and Alcohol Dependence, 170, 198–207. https://doi.org/10.1016/j.drugalcdep.2016.11.003
Hasin, D. S., Fenton, M. C., Beseler, C., Park, J. Y., & Wall, M. M. (2012). Analyses related to the development of DSM-5 criteria for substance use related disorders : 2 Proposed DSM-5 criteria for alcohol, cannabis, cocaine and heroin disorders in 663 substance abuse patients. Drug and alcohol dependence, 122(0), 28–37. https://doi.org/10.1016/j.drugalcdep.2011.09.005
Hodgson, R., Alwyn, T., John, B., Thom, B., & Smith, A. (2002). The FAST Alcohol screening test. Alcohol and Alcoholism (oxford, Oxfordshire), 37(1), 61–66. https://doi.org/10.1093/alcalc/37.1.61
Hoeck, S., & Van Hal, G. (2013). Unhealthy drinking in the Belgian elderly population : Prevalence and associated characteristics. European Journal of Public Health, 23(6), 1069–1075. https://doi.org/10.1093/eurpub/cks152
Holt, S., & Tetrault, J. (2016). Unhealthy alcohol use. Clinics in Liver Disease, 20(3), 429–444. https://doi.org/10.1016/j.cld.2016.02.003
Ilomäki, J., Gnjidic, D., Hilmer, S. N., Couteur, D. G. L., Naganathan, V., Cumming, R. G., Waite, L. M., Seibel, M. J., Blyth, F. M., Handelsman, D. J., & Bell, J. S. (2013). Psychotropic drug use and alcohol drinking in community-dwelling older Australian men : The CHAMP study. Drug and Alcohol Review, 32(2), 218–222. https://doi.org/10.1111/j.1465-3362.2012.00496.x
Immonen, S., Valvanne, J., & Pitkälä, K. H. (2011a). Older adults’ own reasoning for their alcohol consumption. International Journal of Geriatric Psychiatry, 26(11), 1169–1176. https://doi.org/10.1002/gps.2657
Immonen, S., Valvanne, J., & Pitkälä, K. H. (2011b). Prevalence of at-risk drinking among older adults and associated sociodemographic and health-related factors. The Journal of Nutrition, Health & Aging, 15(9), 789–794. https://doi.org/10.1007/s12603-011-0115-4
Iparraguirre, J. (2015). Socioeconomic determinants of risk of harmful alcohol drinking among people aged 50 or over in England. British Medical Journal Open, 5(7), e007684. https://doi.org/10.1136/bmjopen-2015-007684
Ivan, M. C., Amspoker, A. B., Nadorff, M. R., Kunik, M. E., Cully, J. A., Wilson, N., Calleo, J., Kraus-Schuman, C., & Stanley, M. A. (2014). Alcohol use, anxiety, and insomnia in older adults with generalized anxiety disorder. The American Journal of Geriatric Psychiatry : Official Journal of the American Association for Geriatric Psychiatry, 22(9), 875–883. https://doi.org/10.1016/j.jagp.2013.04.001
Kaplan, M. S., Huguet, N., Feeny, D., McFarland, B. H., Caetano, R., Bernier, J., Giesbrecht, N., Oliver, L., & Ross, N. (2012). Alcohol Use patterns and trajectories of health-related quality of life in middle-aged and older adults : A 14- year population-based study. Journal of Studies on Alcohol and Drugs, 73(4), 581–590.
Kaufmann, L., Huber, S., Mayer, D., Moeller, K., & Marksteiner, J. (2018). The CERAD neuropsychological assessment battery is sensitive to alcohol-related cognitive deficiencies in elderly patients : A retrospective matched case-control study. Journal of the International Neuropsychological Society: JINS, 24(4), 360–371. https://doi.org/10.1017/S1355617717001072
Kelly, S., Olanrewaju, O., Cowan, A., Brayne, C., & Lafortune, L. (2016). Alcohol in older people : Systematic reviews of interventions and context. The Lancet, 388, S64. https://doi.org/10.1016/S0140-6736(16)32300-5
Kelly, S., Olanrewaju, O., Cowan, A., Brayne, C., & Lafortune, L. (2018a). Alcohol and older people : A systematic review of barriers, facilitators and context of drinking in older people and implications for intervention design. PLoS One, 13(1), e0191189. https://doi.org/10.1371/journal.pone.0191189
Kelly, S., Olanrewaju, O., Cowan, A., Brayne, C., & Lafortune, L. (2018b). Interventions to prevent and reduce excessive alcohol consumption in older people : A systematic review and meta-analysis. Age and Ageing, 47(2), 175–184. https://doi.org/10.1093/ageing/afx132
Khadjesari, Z., Stevenson, F., Toner, P., Linke, S., Milward, J., & Murray, E. (2019). ‘I’m not a real boozer’ : A qualitative study of primary care patients’ views on drinking and its consequences. Journal of Public Health, 41(2), e185–e191. https://doi.org/10.1093/pubmed/fdy067
Khan, S. (2017). Troubles Concomitants De Santé Mentale Et De Consommation D’alcool Ou De Drogues Au Canada., 28(82), 9.
Kim, S.-A., Kim, E., Morris, R. G., & Park, W.-S. (2015). Exploring the non-linear relationship between alcohol consumption and depression in an elderly population in gangneung : The Gangneung health study. Yonsei Medical Journal, 56(2), 418–425. https://doi.org/10.3349/ymj.2015.56.2.418
Kirchner, J. E., Zubritsky, C., Cody, M., Coakley, E., Chen, H., Ware, J. H., Oslin, D. W., Sanchez, H. A., Durai, U. N. B., Miles, K. M., Llorente, M. D., Costantino, G., & Levkoff, S. (2007). Alcohol consumption among older adults in primary care. Journal of General Internal Medicine, 22(1), 92–97. https://doi.org/10.1007/s11606-006-0017-z
Knightly, R., Tadros, G., Sharma, J., Duffield, P., Carnall, E., Fisher, J., Salman1, S. (2016). Alcohol screening of older adults in a general acute care hospital: The FAST and MAST-G assessments. BJPsych Bulletin, 40, 72–76. https://doi.org/10.1192/pb.bp.114.049734
Kuerbis, A., Hail, L., Moore, A. A., & Muench, F. J. (2017). A pilot study of online feedback for adult drinkers 50 and older : Feasibility, efficacy, and preferences for intervention. Journal of Substance Abuse Treatment, 77, 126–132. https://doi.org/10.1016/j.jsat.2017.04.004
Kuerbis, A., & Sacco, P. (2012). The impact of retirement on the drinking patterns of older adults : A review. Addictive Behaviors, 37(5), 587–595. https://doi.org/10.1016/j.addbeh.2012.01.022
Kuerbis, A., & Sacco, P. (2013). A review of existing treatments for substance abuse among the elderly and recommendations for future directions. Substance Abuse: Research and Treatment, 7, 13–37. https://doi.org/10.4137/SART.S7865
Kuerbis, A., Sacco, P., Blazer, D. G., & Moore, A. A. (2014). Substance abuse among older adults. Clinics in Geriatric Medicine, 30(3), 629–654. https://doi.org/10.1016/j.cger.2014.04.008
Kuerbis, A., Yuan, S. E., Borok, J., LeFevre, P., Kim, G., Lum, D., Ramirez, K., Liao, D., & Moore, A. A. (2015). Testing the initial efficacy of a mailed screening and brief feedback intervention to reduce at-risk drinking in middle-aged and older adults : The Comorbidity Alcohol Risk Evaluation (CARE) Study. Journal of the American Geriatrics Society, 63(2), 321–326. https://doi.org/10.1111/jgs.13237
Kypri, K., Wilson, A., Attia, J., Sheeran, P., Miller, P., & McCambridge, J. (2016). Social desirability bias in the reporting of alcohol consumption : A randomized trial. Journal of Studies on Alcohol and Drugs, 77(3), 526–531. https://doi.org/10.15288/jsad.2016.77.526
Lai, H. M. X., Cleary, M., Sitharthan, T., & Hunt, G. E. (2015). Prevalence of comorbid substance use, anxiety and mood disorders in epidemiological surveys, 1990–2014: A systematic review and meta-analysis. Drug and Alcohol Dependence, 154, 1–13. https://doi.org/10.1016/j.drugalcdep.2015.05.031
Li, J., Wu, B., Selbæk, G., Krokstad, S., & Helvik, A.-S. (2017). Factors associated with consumption of alcohol in older adults - A comparison between two cultures, China and Norway : The CLHLS and the HUNT-study. BMC Geriatrics, 17https://doi.org/10.1186/s12877-017-0562-9
Li, J., Wu, B., Tevik, K., Krokstad, S., & Helvik, A. (2019). Factors associated with elevated consumption of alcohol in older adults—Comparison between China and Norway : The CLHLS and the HUNT Study. British Medical Journal Open, 9(8), e028646. https://doi.org/10.1136/bmjopen-2018-028646
Lin, J. C., Karno, M. P., Barry, K. L., Blow, F. C., Davis, J. W., Tang, L., & Moore, A. A. (2010a). Determinants of Early reductions in drinking in older at-risk drinkers participating in the intervention arm of a trial to reduce at-risk drinking in primary care. Journal of the American Geriatrics Society, 58(2), 227–233. https://doi.org/10.1111/j.1532-5415.2009.02676.x
Lin, J. C., Karno, M. P., Grella, C. E., Ray, L. A., Liao, D. H., & Moore, A. A. (2014). Psychiatric correlates of alcohol and tobacco use disorders in US adults aged 65 years and older : Results from the 2001–2002 National Epidemiologic Survey of Alcohol and Related Conditions. The American journal of geriatric psychiatry : official journal of the American Association for Geriatric Psychiatry, 22(11), 1356–1363.
Lin, J. C., Karno, M. P., Tang, L., Barry, K. L., Blow, F. C., Davis, J. W., Ramirez, K. D., Welgreen, S., Hoffing, M., & Moore, A. A. (2010b). Do health educator telephone calls reduce at-risk drinking among older adults in primary care? Journal of General Internal Medicine, 25(4), 334–339. https://doi.org/10.1007/s11606-009-1223-2
Martinez, P., Lien, L., Landheim, A., Kowal, P., & Clausen, T. (2014). Quality of life and social engagement of alcohol abstainers and users among older adults in South Africa. BMC Public Health, 14(1), 316. https://doi.org/10.1186/1471-2458-14-316
Mayfield, D., Mcleod, G., & Hall, P. (1974). The CAGE questionnaire : Validation of a new alcoholism screening instrument. American Journal of Psychiatry, 131(10), 1121–1123. https://doi.org/10.1176/ajp.131.10.1121
Maynard, S., Campbell, E., Boodhoo, K., Xenocostas, S., Gill, K., L’Équipe IRSC – Traitement de la toxicomanie (CIHR TEAM in substance abuse treatment). (2016). Inefficacité des formations didactiques comme outil d’intégration de services en dépendance dans les soins de première ligne. Drogues, Santé Et Société, 15(2), 19. https://doi.org/10.7202/1038628ar
McLellan, A. T., Kushner, H., Metzger, D., Peters, R., SmithGrissom, I. G., Pettinati, H., & Argeriou, M. (1992). The Fifth edition of the addiction severity index. Journal of Substance Abuse Treatment, 9(3), 199–213.
Menecier, P., Fernandez, L., Pichat, M., Lefranc, D., & Ploton, L. (2015). Connaissances soignantes à propos d’usage ou de mésusage d’alcool de sujets âgés. Alcoologie et Addictologie, 37(4), Art. 4
Menecier, P., Fernandez, L., Pichat, M., & Ploton, L. (2018). Attitudes et croyances soignantes envers des aînés mésusant d’alcool : Enquête hospitalière par questionnaire auprès de 315 agents. Psychotropes, 24(1), 55–76.
Menecier, P., Fernandez, L., Plattier, S., & Ploton, L. (2017). Troubles de l’usage d’alcool du sujet âgé : Un exemple pour aborder la complexité en santé. Annales Médico-Psychologiques, Revue Psychiatrique, 175(9), 763–769. https://doi.org/10.1016/j.amp.2016.10.015
Menecier, P., Rotheval, L., Plattier, S., Fernandez, L., & Ploton, L. (2016). Le déni en alcoologie, à travers ce qu’il n’est pas. Drogues, Santé Et Société, 15(2), 39. https://doi.org/10.7202/1038629ar
Midorikawa, H., Tachikawa, H., Aiba, M., Arai, T., Watanabe, T., & Tamiya, N. (2019). Factors associated with high-risk drinking in older adults : Evidence from a national survey in Japan. Geriatrics & Gerontology International, 19(12), 1260–1267. https://doi.org/10.1111/ggi.13808
Miller, W. R. (1996). Form 90 : A structured assessment interview for drinking and related behaviors : test manual. USDeptof Health and Human Services, Public Health Service, National Institutes of Health, National Institute on Alcohol Abuse and Alcoholism.
Miller, W. R., & Del Boca, F. K. (1994). Measurement of drinking behavior using the Form 90 family of instruments. Journal of Studies on Alcohol, Supplement, s12, 112‑118. https://doi.org/10.15288/jsas.1994.s12.112
Moher, D., Shamseer, L., Clarke, M., Ghersi, D., Liberati, A., Petticrew, M., Shekelle, P., Stewart, L. A., PRISMA-P Group. (2015). Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Systematic Reviews, 4(1), 1. https://doi.org/10.1186/2046-4053-4-1
Moore, A. A., Beck, J. C., Babor, T. F., Hays, R. D., & Reuben, D. B. (2002). Beyond alcoholism : Identifying older, at-risk drinkers in primary care. Journal of Studies on Alcohol, 63(3), 316–324. https://doi.org/10.15288/jsa.2002.63.316
Moore, A. A., Blow, F. C., Hoffing, M., Welgreen, S., Davis, J. W., Lin, J. C., Ramirez, K. D., Liao, D. H., Tang, L., Gould, R., Gill, M., Chen, O., & Barry, K. L. (2011). Primary Care based intervention to reduce at-risk drinking in older adults : A randomized controlled trial. Addiction (abingdon, England), 106(1), 111–120. https://doi.org/10.1111/j.1360-0443.2010.03229.x
Moore, A. A., Hays, R. D., Reuben, D. B., & Beck, J. C. (2000). Using a criterion standard to validate the Alcohol-Related Problems Survey (ARPS): A screening measure to identify harmful and hazardous drinking in older persons. Aging (milan, Italy), 12(3), 221–227. https://doi.org/10.1007/BF03339839
Moore, A. A., Karno, M. P., Grella, C. E., Lin, J. C., Warda, U., Liao, D. H., & Hu, P. (2009). Alcohol, tobacco and non-medical drug use in US adults aged 65 years and older : Data from the 2001–2002 National Epidemiologic Survey of Alcohol and Related Conditions. Journal of the American Geriatrics Society, 57(12), 2275–2281. https://doi.org/10.1111/j.1532-5415.2009.02554.x
Moos, R. H., Brennan, P. L., Schutte, K. K., & Moos, B. S. (2010). Social and financial resources and high-risk alcohol consumption among older adults. Alcoholism: Clinical and Experimental Research, 34(4), 646–654. https://doi.org/10.1111/j.1530-0277.2009.01133.x
Moos, R. H., Brennan, P. L., Schutte, K. K., & Moos, B. S. (2010b). Older adults’ health and late-life drinking patterns : A 20-year perspective. Aging & Mental Health, 14(1), 33–43. https://doi.org/10.1080/13607860902918264
Moos, R. H., Cronkite, R. C., Finney, J. W., Educational Testing Service, Social Ecology Laboratory (Palo Alto, Calif. ), & Far West Health Services Field Program. (1990). Health and daily living form manual. Social Ecology Laboratory ;
Moos, R. H., Schutte, K. K., Brennan, P. L., & Moos, B. S. (2010c). Late-Life and life history predictors of older adults of high-risk alcohol consumption and drinking problems. Drug and Alcohol Dependence, 108(1–2), 13–20. https://doi.org/10.1016/j.drugalcdep.2009.11.005
Morel, A., & Couteron, J.-P. (2019). Addictologie (3e éd). Dunod.
Moy, I., Crome, P., Crome, I., & Fisher, M. (2011). Systematic and narrative review of treatment for older people with substance problems. European Geriatric Medicine, 2(4), 212–236. https://doi.org/10.1016/j.eurger.2011.06.004
Muñoz, M., Ausín, B., Santos-Olmo, A. B., Härter, M., Volkert, J., Schulz, H., Sehner, S., Dehoust, M. C., Suling, A., Wegscheider, K., Canuto, A., Crawford, M. J., Grassi, L., Da Ronch, C., Hershkovitz, Y., Quirk, A., Rotenstein, O., Shalev, A. Y., Strehle, J., … Andreas, S. (2018). Alcohol use, abuse and dependence in an older European population : Results from the MentDis_ICF65+ study. PLoS ONE, 13(4). https://doi.org/10.1371/journal.pone.0196574
Nubukpo, P., Laot, L., & Clément, J.-P. (2012). Addictive behaviors in the aged. Gériatrie Et Psychologie Neuropsychiatrie Du Viellissement, 3, 315–324. https://doi.org/10.1684/pnv.2012.0355
Oishi, S. M., Morton, S. C., Moore, A. A., Beck, J. C., Hays, R. D., Spritzer, K. L., Partridge, J. M., & Fink, A. (2001). USING data to enhance the expert panel process : Rating indications of alcohol-related problems in older adults. International Journal of Technology Assessment in Health Care, 17(1), 125–136. https://doi.org/10.1017/S0266462301104113
Ortolá, R., García-Esquinas, E., Galán, I., & Rodríguez-Artalejo, F. (2016). Patterns of alcohol consumption and health-related quality of life in older adults. Drug and Alcohol Dependence, 159, 166–173. https://doi.org/10.1016/j.drugalcdep.2015.12.012
Ortolá, R., García-Esquinas, E., López-García, E., León-Muñoz, L. M., Banegas, J. R., & Rodríguez-Artalejo, F. (2019). Alcohol consumption and all-cause mortality in older adults in Spain : An analysis accounting for the main methodological issues. Addiction (abingdon, England), 114(1), 59–68. https://doi.org/10.1111/add.14402
Paille, F. (2014). Personnes âgées et consommation d’alcool : Texte court. Alcoologie et Addictologie, 1 vol 36, 61‑72.
Palle, C., Beck, F., & Richard, J.-B. (2017, juin). Usages d’alcool et dommages subis : Une perspective européenne—Tendances n° 118—Juin 2017—OFDT. https://www.ofdt.fr/publications/collections/periodiques/lettre-tendances/usages-dalcool-et-dommages-subis-une-perspective-europeenne-tendances-n-118-juin-2017/
Parikh, R. B., Junquera, P., Canaan, Y., & Oms, J. D. (2015). Predictors of binge drinking in elderly Americans. The American Journal on Addictions, 24(7), 621–627. https://doi.org/10.1111/ajad.12275
Paulson, D., Shah, M., Herring, D., Scott, R., Herrera, M., Brush, D., & Bassett, R. (2018). The relationship between moderate alcohol consumption, depressive symptomatology, and C-reactive protein : The Health and Retirement Study. International Journal of Geriatric Psychiatry, 33(2), 316–324. https://doi.org/10.1002/gps.4746
Peer, K., Rennert, L., Lynch, K. G., Farrer, L., Gelernter, J., & Kranzler, H. R. (2013). Prevalence of DSM-IV and DSM-5 Alcohol, cocaine, opioid, and cannabis use disorders in a largely substance dependent sample. Drug and Alcohol Dependence, 127, 215–219. https://doi.org/10.1016/j.drugalcdep.2012.07.009
Peltzer, K., & Phaswana-Mafuya, N. (2013). Problem drinking and associated factors in older adults in South Africa. African Journal of Psychiatry, 16(2), Art. 2. https://doi.org/10.4314/ajpsy.v16i2.13
Platt, A., Sloan, F. A., & Costanzo, P. (2010). Alcohol-Consumption trajectories and associated characteristics among adults older than age 50. Journal of Studies on Alcohol and Drugs, 71(2), 169–179.
Rao, R., & Roche, A. (2017). Substance misuse in older people. BMJ, 358, j3885. https://doi.org/10.1136/bmj.j3885
Richard, J.-B., Andler, R., Cogordan, C., Spilka, S., Nguyen-Thanh, V., & groupe Baromètre de Santé Publique France. (2019). La consommation d’alcool chez les adultes en France en 2017. Bulletin Epidémiologique Hebdomadaire, 5–6, 89–97.
Rodriguez, C. A., Schonfeld, L., King-Kallimanis, B., & Gum, A. M. (2010). Depressive symptoms and alcohol abuse/misuse in older adults : Results from the Florida BRITE Project. Best Practices in Mental Health, 6(1), 90–102.
Rolland, B., Naassila, M., Paille, F., & Aubin, H.-J. (2017). The role of general practitioners in the 2015 French Guidelines on Alcohol Misuse. Alcohol and Alcoholism, 52https://doi.org/10.1093/alcalc/agx054
Sacco, P., Bucholz, K. K., & Harrington, D. (2014). Gender differences in stressful life events, social support, perceived stress, and alcohol use among older adults : Results from a national survey. Substance Use & Misuse, 49(4), 456–465. https://doi.org/10.3109/10826084.2013.846379
Sacco, P., Smith, C. A., Harrington, D., Svoboda, D. V., & Resnick, B. (2016). Feasibility and utility of experience sampling to assess alcohol consumption among older adults. Journal of Applied Gerontology, 35(1), 106–120. https://doi.org/10.1177/0733464813519009
Sachdeva, A., Chandra, M., Choudhary, M., Dayal, P., & Anand, K. S. (2016). Alcohol-related dementia and neurocognitive impairment : A review study. International Journal of High Risk Behaviors & Addiction, 5(3). https://doi.org/10.5812/ijhrba.27976
Sayers, S. P., Brach, J. S., Newman, A. B., Heeren, T. C., Guralnik, J. M., & Fielding, R. A. (2004). Use of self-report to predict ability to walk 400 meters in mobility-limited older adults. Journal of the American Geriatrics Society, 52(12), 2099–2103. https://doi.org/10.1111/j.1532-5415.2004.52571.x
Schonfeld, L., King-Kallimanis, B. L., Duchene, D. M., Etheridge, R. L., Herrera, J. R., Barry, K. L., & Lynn, N. (2010). Screening and brief intervention for substance misuse among older adults : The Florida BRITE Project. American Journal of Public Health, 100(1), 108–114. https://doi.org/10.2105/AJPH.2008.149534
Shamseer, L., Moher, D., Clarke, M., Ghersi, D., Liberati, A., Petticrew, M., Shekelle, P., & Stewart, L. A. (2015). Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 : Elaboration and explanation. BMJ, 349https://doi.org/10.1136/bmj.g7647
Shield, K., D., Rylett, M., & Rehm, J. (2016). Public health successes and missed opportunities : Trends in alcohol consumption and attributable mortality in the WHO European Region, 1990–2014. 88.
Skirbekk, V., Stonawski, M., Bonsang, E., & Staudinger, U. M. (2013). The Flynn effect and population aging. Intelligence, 41(3), 169–177. https://doi.org/10.1016/j.intell.2013.02.001
Sobell, L. C., & Sobell, M. B. (1992). Timeline Follow-Back. In R. Z. Litten & J. P. Allen (Éds.), Measuring alcohol consumption : Psychosocial and Biochemical Methods (p. 41‑72). Humana Press. https://doi.org/10.1007/978-1-4612-0357-5_3
Tait, R. J., French, D. J., Burns, R., & Anstey, K. J. (2012). Alcohol use and depression from middle age to the oldest old : Gender is more important than age. International Psychogeriatrics, 24(8), 1275–1283. https://doi.org/10.1017/S1041610212000087
Tonigan, J. S., Miller, W. R., & Brown, J. M. (1997). The reliability of Form 90: An instrument for assessing alcohol treatment outcome. Journal of Studies on Alcohol, 58(4), 358–364. https://doi.org/10.15288/jsa.1997.58.358
Tredal, I., Soares, J. J. F., Sundin, Ö., Viitasara, E., Melchiorre, M. G., Torres-Gonzales, F., Stankunas, M., Lindert, J., Ioannidi-Kapolou, E., & Barros, H. (2013). Alcohol use among abused and non-abused older persons aged 60–84 years : An European study. Drugs Education, Prevention and Policy, 20(2), 96–109. https://doi.org/10.3109/09687637.2012.751087
Van den Berg, J. F., Kok, R. M., van Marwijk, H. W. J., van der Mast, R. C., Naarding, P., Oude Voshaar, R. C., Stek, M. L., Verhaak, P. F. M., de Waal, M. W. M., & Comijs, H. C. (2014). Correlates of alcohol abstinence and at-risk alcohol consumption in older adults with depression : The NESDO Study. The American Journal of Geriatric Psychiatry, 22(9), 866–874. https://doi.org/10.1016/j.jagp.2013.04.006
Vaughan, E. L., Robbins, M. J., & Escobar, O. S. (2014). Mental health, physical health problems, and drinking among Latino older adults. Journal of Latina/o Psychology, 2(4), 214–223. https://doi.org/10.1037/lat0000026
Veerbeek, M. A., ten Have, M., van Dorsselaer, S. A., Oude Voshaar, R. C., Rhebergen, D., & Willemse, B. M. (2019). Differences in alcohol use between younger and older people : Results from a general population study. Drug and Alcohol Dependence, 202, 18–23. https://doi.org/10.1016/j.drugalcdep.2019.04.023
Villalonga-Olives, E., Almansa, J., Shaya, F., & Kawachi, I. (2020). Perceived social capital and binge drinking in older adults : The Health and Retirement Study, US data from 2006-2014. Drug and Alcohol Dependence, 108099https://doi.org/10.1016/j.drugalcdep.2020.108099
Villiers-Tuthill, A., Copley, A., McGee, H., & Morgan, K. (2016). The relationship of tobacco and alcohol use with ageing self-perceptions in older people in Ireland. BMC Public Health, 16(1), 1–10. https://doi.org/10.1186/s12889-016-3158-y
Vrdoljak, D., Marković, B. B., Puljak, L., Lalić, D. I., Kranjčević, K., & Vučak, J. (2014). Lifestyle intervention in general practice for physical activity, smoking, alcohol consumption and diet in elderly : A randomized controlled trial. Archives of Gerontology and Geriatrics, 58(1), 160–169. https://doi.org/10.1016/j.archger.2013.08.007
Wang, Y.-P., & Andrade, L. H. (2013). Epidemiology of alcohol and drug use in the elderly. Current Opinion in Psychiatry, 26(4), 343–348. https://doi.org/10.1097/YCO.0b013e328360eafd
Watson, J. M., Crosby, H., Dale, V. M., Tober, G., Wu, Q., Lang, J., McGovern, R., Newbury-Birch, D., Parrott, S., Bland, J. M., Drummond, C., Godfrey, C., Kaner, E., & Coulton, S. (2013). AESOPS : A randomised controlled trial of the clinical effectiveness and cost-effectiveness of opportunistic screening and stepped care interventions for older hazardous alcohol users in primary care. Health Technology Assessment (winchester, England), 17(25), 1–158. https://doi.org/10.3310/hta17250
Wieben, E. S., Nielsen, B., Nielsen, A. S., & Andersen, K. (2018). Elderly alcoholics compared to middle-aged alcoholics in outpatient treatment – 6-month follow-up. Nordic Journal of Psychiatry, 72(7), 506–511. https://doi.org/10.1080/08039488.2018.1522373
Williams, E. C., Lapham, G. T., Shortreed, S. M., Rubinsky, A. D., Bobb, J. F., Bensley, K. M., Catz, S. L., Richards, J. E., & Bradley, K. A. (2017). Among patients with unhealthy alcohol use, those with HIV are less likely than those without to receive evidence-based alcohol-related care : A national VA study. Drug and Alcohol Dependence, 174, 113–120. https://doi.org/10.1016/j.drugalcdep.2017.01.018
Wilsnack, R. W., Wilsnack, S. C., Kristjanson, A. F., Vogeltanz-Holm, N. D., & Gmel, G. (2009). Gender and alcohol consumption : Patterns from the multinational GENACIS project. Addiction, 104(9), 1487–1500. https://doi.org/10.1111/j.1360-0443.2009.02696.x
World Health Organization (Éd.). (2009). The ICD-10 classification of mental and behavioural disorders : Clinical descriptions and diagnostic guidelines (Reprinted). World Health Organization.
Wu, L.-T., & Blazer, D. G. (2014). Substance use disorders and psychiatric comorbidity in mid and later life : A review. International Journal of Epidemiology, 43(2), 304–317. https://doi.org/10.1093/ije/dyt173
Zanjani, F., Allen, H., Schoenberg, N., Martin, C., & Clayton, R. (2018). Acceptability of intervention materials to decrease risk for alcohol and medication interactions among older adults. Evaluation and Program Planning, 67, 160–166. https://doi.org/10.1016/j.evalprogplan.2017.12.010
Zegarra-Parodi, R., Draper-Rodi, J., & Cerritelli, F. (2019). Refining the biopsychosocial model for musculoskeletal practice by introducing religion and spirituality dimensions into the clinical scenario. International Journal of Osteopathic Medicine, 32, 44–48. https://doi.org/10.1016/j.ijosm.2019.04.001
Zorzela, L., Loke, Y. K., Ioannidis, J. P., Golder, S., Santaguida, P., Altman, D. G., Moher, D., Vohra, S., PRISMAHarms Group. (2016). PRISMA harms checklist : Improving harms reporting in systematic reviews. BMJ (Clinical Research Ed), 352, i157.
Acknowledgements
The current review was conducted by the first author in partial fulfillment of the requirements for the doctoral degree in Health Psychology and Psychopathology at the University of Toulouse. The authors would like to thank Raquel Sanchez Rodriguez (PhD in Psychology, University of Toulouse) for their advice on review methods and search strategy.
Author information
Authors and Affiliations
Contributions
OM-M and VI contributed to the design of this study. FS supervised the conduct of the systematic review, data collection, analysis, interpretation, and preparation of the manuscript. OM-M was responsible for the literature search, data selection, and extraction process. VI and BJ also contributed to the data selection process, respectively. NF and BJ reviewed a subset of abstracts and provided advanced expertise on data collection, analysis, interpretation, and important intellectual content. OM-M, FS, BJ, and NF contributed to the data analysis, critical appraisal, writing the manuscript, and reviewed drafts and revisions of the manuscript. All authors contributed to and have approved the final manuscript. The corresponding author attests that all listed authors meet authorship criteria and that no others meeting the criteria have been omitted.
Corresponding author
Ethics declarations
Ethics Statement
Ethical approval for this study was not required.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Megherbi-Moulay, O., Igier, V., Julian, B. et al. Alcohol Use in Older Adults: A Systematic Review of Biopsychosocial Factors, Screening Tools, and Treatment Options. Int J Ment Health Addiction 22, 2073–2115 (2024). https://doi.org/10.1007/s11469-022-00974-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11469-022-00974-z