Abstract
To improve the therapeutic efficacy of herpes simplex virus type 1 (HSV-1) thymidine kinase (tk)/ganciclovir (GCV) therapy, we have made recombinant tk chimeras fused with the arginine-rich (RXP) repeat of herpes simplex virus type 2 (HSV-2) US11 and examined their activity of intercellular trafficking and cytotoxicity. When examined the immunofluorescence staining patterns of RXP/tk fusion proteins in transfected COS7 cells, the RXP chimeras revealed a conservation of the trafficking activity of RXP. We also found that transfection of tkCΔ6-RXP (lacking the C-terminal six amino residues of tk), tk-RXP, and tkNΔ66-RXP (lacking the N-terminal 66 amino residues of tk) induced apoptosis even in the absence of GCV. The results suggest that these tk/RXP chimeras themselves have apoptosis-inducing activity, and that the HSV tk nucleoside-binding domain may be involved in the induction of apoptosis. Furthermore, treatment with 5 μM GCV induced efficient cell death in cells tranfected with tk-RXP in comparison to the cells transfected with tk (P < 0.0001).
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
HSV-1 thymidine kinase (tk) is extensively exploited in cancer suicide gene therapy [1]. First demonstrated a quarter century ago, anti-herpesviral drugs have a profound anti-cellular effect on HSV tk-expressing cells [2]. Since then, the use of HSV tk in suicide gene therapy has been intensively investigated. The prodrug, ganciclovir (GCV), is a guanosine analogue carrying a cyclic ribose; GCV is monophosphated by HSV-1 tk, then phosphorylated into a cytotoxic triphosphate derivative by the host tk enzymes. This acyclic dGTP analogue is incorporated into DNA, interfering with cellular DNA synthesis [3, 4]. Although the precise mechanisms whereby the HSV-tk/GCV system results in target cell death are not well understood, that the induction of apoptosis is involved. An advantage of tk gene therapy involves the bystander effect (BE), in which GCV sensitivity is propagated from tumor cells expressing HSV-tk to adjacent non-expressing cells [5–7]. As the toxic derivative purine or pyrimidine nucleosides cannot diffuse across cell membranes, HSV-tk/GCV-mediated killing requires cell-to-cell contact, likely through gap junction formation, to exhibit a BE [8, 9].
Several approaches have attempted to enhance the BE. Apigenin, a flavonoid, and lovastatin, an inhibitor of HMG-CoA reductase, both upregulate gap junction formation, resulting in an enhancement of antitumor response rate following GCV treatment in vivo [10]. Combined delivery of tk and either cytokines, such as IL-2 or IL-12 [11–14], or cell cycle inhibitors, including p27, have been attempted [15], but the therapeutic efficacies are unclear.
Peptides with the unusual characteristic of crossing cell membrane via noncanonical secretion or internalization have also been utilized to enhance the efficacy of tk/GCV suicide gene therapy [16]. We previously reported that the C-terminal Arg-X-Pro (RXP) repeat peptide of the HSV-2 segment protein US11 functions in intercellular trafficking [17]. Thus, the US11 RXP repeats may also significantly enhance or amplify gene therapy applications. In an attempt to improve the therapeutic efficacy of tk/GCV therapy, we fused HSV-1 tk to the RXP peptide and investigated the behavior and function of this fusion protein.
Materials and methods
Construction of chimera DNA expression vectors
DNA encoding the HSV-2 US11 protein, containing 19 tandem repeats of the Arg-X-Pro sequence, was amplified by PCR (TAKARA LA Taq) from purified HSV-2 186 strain DNA. Amplified DNA was fused to either the N- or C-termini of the HSV-1 thymidine kinase (tk) gene. DNA fragments encoding the N-terminal deletion mutants were amplified by PCR from the tk-RXP sequence. The Q125N site-specific mutation was introduced into the tkCΔ6-RXP gene using the PCR-based QuickChange Site-directed Mutagenesis Kit (Stratagene), according to the manufacturer’s instructions. Mutant DNA fragments were cloned into pcDNA3.1 (+) (Invitrogen) between the EcoRI and XbaI sites. Following digestion with HindIII and XbaI, the tk-RXP and tk-FLAG genes from pcDNA tk-RXP and pcDNA tk-FLAG, respectively, were inserted into the pHGCX expression vector that included a GFP expression cassette.
Cell culture, transfection and indirect immunofluorescence staining
Cos7 cells were cultured in Dulbecco’s modified minimal essential medium supplemented with 10% heat-inactivated FCS, 100 units/ml of penicillin and 2 mM of l-glutamine. Prior to transfection, COS7 cells were seeded in 35 mm dishes either containing coverslips or not. At 70–80% confluency, cells were transfected with the 4 μg of appropriate plasmids using Lipofectamine 2000 (Invitrogen), according to the manufacturer’s instructions. Thirty-six hours after transfection, the cells were fixed in 50% acetone/50% ethanol for 10 min on ice. Samples were then stained with anti-HSV-2 US11 or anti-FLAG (Sigma) antibodies at dilutions of 1:100. After a 30 min 37°C incubation period, coverslips were washed thoroughly in PBS, and stained with FITC-conjugated goat anti-rabbit or anti-mouse IgG (Sigma) for 30 min at 37°C. After rinsing again with PBS, the cell nuclei were stained with Promidium iodide (Sigma) for 5 min at 37°C, and then washed with PBS. The coverslips were quickly mounted onto glass slides with Perma Flour (Immunon) and subsequently analyzed with the Zeiss laser scanning microscope LSM510.
Intercellular trafficking of RXP fusion proteins
COS7 cells were transfected with pHGCX tk-FLAG or pHGCX tkCΔ6-RXP for 36 h as described above and stained with either anti-FLAG and anti-GFP (Sigma) antibodies or anti-HSV-2 US11 and anti-GFP (Sigma) antibodies for 30 min at 37°C. After the cells were washed in PBS, COS7 cells were then stained with FITC-conjugated goat anti-rabbit IgG (Sigma) and either TRITC-conjugated goat anti-mouse IgG (Sigma). The cells were quickly mounted onto glass slides with Perma Flour (Immunon) and subsequently analyzed with the Zeiss laser scanning microscope LSM510.
TUNEL assay
Apoptotic cells were confirmed with Apop Tag apoptosis detection kit (CHEMICON), in accordance with the manufacturer’s instructions. In brief, COS7 cells were grown on coverslips, and next day transfected with tk-FLAG, tkCΔ6-RXP, or HSV-2-US11 expression vectors. The cells were fixed in 1% paraformaldehyde in PBS for 10 min, and post-fixed in precooled ethanol:acetic acid 2:1 for 5 min. The cells were then stained with anti-FLAG or anti-HSV-2 US11 antibodies, and labeled with TRITC-conjugated goat anti-rabbit or anti-mouse IgG (Sigma). DNA fragments were labeled with the TdT-mediated dUTP nick end labeling (TUNEL) reaction mixture for 60 min at 37°C in a dark humidified atmosphere. The coverslips were then incubated with Converter alkaline phosphatase for 60 min at 37°C, and rinsed in PBS. Analysis was performed using the LSM510.
Western blot analysis
COS cells were transfected with tk-RXP, tkCΔ6-RXP, or tk-FLAG expression vectors. Thirty-six hours after transfection, the cells were resuspended in 0.2 ml lysis buffer (125 mM Tris pH 6.8, 2% SDS, 10% glycerol). Cell lysates were separated by 10% Tris–glycine SDS polyacrylamide gel electrophoresis and electrotransferred onto a nitrocellulose membrane (Millipore). The membrane was blocked with 5% skim milk dissolved in 0.05% Tween 20 in PBS. The membrane was probed with rabbit anti-Poly (ADP-ribose polymerase) antibody (1:1,000, Sigma), and then incubated with horseradish peroxidase-conjugated mouse anti-rabbit immunoglobulin (1:10,000, Biosource). Blots were developed using an enhanced chemiluminescence kit (Amersham Phamacia).
Annexin V-Cy3 staining
COS7 cells were transfected with tk-RXP, tk-FLAG, tkCΔ6-RXP, tkQ125NCΔ6-RXP, tkNΔ66-RXP or tkNΔ200-RXP expression vectors using lipofectamine 2000. Thirty-six hours after transfection, the cells were stained with annexin V-Cy3 (MBL). The cells were incubated in 200 μl 1 × binding buffer containing 2 μl annexin V-Cy3 at room temperature for 10 min in the dark. Next, the cells were fixed in 70% ethanol overnight at 4°C. Cells were also immunostained with HSV-2 anti-US11 or anti-FLAG antibodies. Analysis was performed by the LSM510.
Cell count assay
The COS7 cells were seeded in 35 mm dishes. At 70–80% confluence, cells were transfected with 4 μg/dish of pHGCX tk-RXP, pHGCX tk-FLAG, or pHGCX. After incubation at 37°C for 24 h, cells were incubated for 48 h by DMEM supplemented with 10% FBS and concentrations of GCV ranging from 0 to 5 μM. After harvesting by trypsinization, the number of surviving cells was quantified using a hemocytometer after trypan blue staining. The experiments were done in triplicate; data were analyzed by the student’s t-test. The levels are expressed as means ± ranges. Differences were considered significant when P ≤ 0.05.
Results and discussion
To investigate the ability of the HSV-2 US11 RXP repeat peptide to transport the HSV-1 tk protein from a primary expressing cell to neighboring recipient cells, we constructed expression vectors encoding RXP-tk, tk-RXP, tkCΔ6-RXP, tkNΔ66-RXP, tkNΔ200-RXP, tkQ125NCΔ6-RXP, and tk-FLAG fusion proteins. Expression of these proteins was driven by the cytomegalovirus immediate-early enhancer/promoter region (CMVP) in a mammalian expression plasmid, pcDNA3.1 (+) (Fig. 1). In addition, we created two CMVP-driven expression vectors encoding the tkCΔ6-RXP and tk-FLAG fusion proteins, using pHGCX into which GFP gene had been inserted as a marker. Forty-eight hours after transfection of these plasmids into COS7 cells using lipofectamine 2000 (Invitrogen), fusion protein expression could be detected by immunofluorescence staining with anti-US11 (generated in our laboratory) or anti-FLAG (Sigma) antibodies and anti-GFP antibodies (Sigma). The tk-RXP and tkCΔ6-RXP fusion proteins were localized to the cytoplasm with lower levels seen in the nuclei of transfected cells; these proteins, however, did not exhibit the distinct nucleolar accumulation that could be observed as expression of HSV-2 US11 alone (Fig. 2F, I; Fig. 5H, I). The RXP-tk fusion protein localized to both the cytoplasm and nucleus of transfected cells (Fig. 2J, L). Individual tk-positive cells were observed in monolayers transfected with tk-FLAG in low numbers; as expected, no spread of tk to the surrounding cells could be observed (Fig. 2A). The tk-RXP, tkCΔ6-RXP, and RXP-tk fusion proteins, however, spread to the majority of cells in the monolayers (Fig. 2D, G, J). With the exception of tk-FLAG, all of the fusion proteins examined spread from a primary expressing cell into neighboring cells (data not shown). To confirm the intercellular trafficking of RXP fusion proteins, we cloned DNA encoding tkCΔ6-RXP and tk-FLAG into the pHGCX vector, which contains a GFP expression cassette. After transfection of these plasmids, COS7 cells were double stained with either anti-FLAG or anti-HSV-2 US11 antibodies and anti-GFP antibodies. The tkCΔ6-RXP fusion protein spread to cells that did not express GFP (Fig. 3F), while tk-FLAG fusion protein remained localized within GFP-expressing cells (Fig. 3C). We previously reported that the HSV-2 US11 C-terminal RXP repeat peptide has the ability to carry GFP when fused to this peptide, across cell membrane [17]. We postulated that different conformations of RXP, varying in hydrophilicity and hydrophobicity, may be involved in membrane translocation. In this study, we also observed the ability of the RXP repeat to mediate the intercellular trafficking of tk and tk deletion mutants when incorporated into fusion proteins. HSV-1 tk/GCV therapy was sufficient to eradicate tumors in an animal model [18]. In clinical trials, however, tk/GCV suicide gene therapies were not as effective as expected, probably because of a low rate of gene delivery [19, 20]. A possible methodology to overcome this problem is to transfer tk to non-transfected cells by fusing it with a protein that is capable of intercellular trafficking. HIV-1 tat and HSV-1 VP22 have been fused to HSV-1 tk, which has enhanced tk suicide gene therapy [21–24]. In clinical use, the large size of VP22 may become a limitation for gene delivery [25]. The RXP repeat has the advantage of a much smaller size over VP22. Our results indicate that the tk-RXP fusion protein may be a feasible approach to enhance the effectiveness of tk/GCV suicide gene therapy.
Construction of chimeric DNA. DNA encoding 19 tandem Arg-X-Pro (RXP) repeats of the HSV-2 US11 protein was amplified by PCR from HSV-2 186. Amplified DNA was fused to either the N- or C-termini of the HSV-1 thymidine kinase (tk) gene. DNA fragments encoding the N-terminal deletion mutants were amplified by PCR from the tk-RXP sequence. The Q125N site-specific mutation was introduced into the tk-RXP gene. Chimeric DNA fragments were cloned into pcDNA 3.1 (+) (Invitrogen)
Expression of chimeric DNA. COS7 cells were transfected with 4 μg tk-FLAG (A–C), tk-RXP (D–F), tkCΔ6-RXP (G–I), or RXP-tk (J–L) expression vectors using Lipofectamine 2000 (Invitrogen), and were then stained with either anti-HSV-2 US11 (D, G, J) or anti-FLAG (Sigma) antibodies, dilute 1:100 (A). FITC-conjugated goat anti-rabbit IgG (Sigma) or anti-mouse IgG (Sigma) antibodies were used as a secondary probe. Cells were also stained with Propidium Iodide (Sigma) (B, E, H, K). Analysis was performed using the LSM510. The tk-FLAG and RXP fusion protein signals are shown in green. Red stain indicates the nuclei
Trafficking of RXP fusion proteins. COS7 cells were transfected with pHGCX tk-FLAG (A–C) or pHGCX tkCΔ6-RXP (D–F) and stained with either anti-FLAG (A) and anti-GFP (Sigma) (B) antibodies or anti-HSV-2 US11 (D) and anti-GFP (E) antibodies. Cells were then stained with FITC-conjugated goat anti-rabbit IgG (Sigma) and either RITC-conjugated goat anti-mouse IgG (Sigma). Green signals indicate the tk-FLAG or tkCΔ6-RXP proteins. Red stain indicates GFP protein
In our observation of the intercellular trafficking activity of RXP fusion proteins, we noted that the nuclei of tkCΔ6-RXP expressing cells revealed a nuclear deformation suggestive of apoptotic change (Fig. 4K). Although the nuclear deformation is weaker than that seen in tkCΔ6-RXP-expressing cells, it was also present in cells tranfected with tk-RXP or tkNΔ66-RXP (Fig. 4H, N). We could not, however, find this nuclear deformational changes in cells transfected with any of the other chimeras (Fig. 4B, E, Q, T).
COS7 cells were transfected with the tk-FLAG (A–C), RXP-tk (D–F), tk-RXP (G–I), tkCΔ6-RXP (J–L), tkNΔ66-RXP (M–O), tkNΔ200-RXP (O–Q), or tkQ125NCΔ6-RXP (R–T) expression vectors. Cells were then fixed and stained with anti-FLAG (Sigma) (A) or anti-HSV-2-US11 (D, G, J, M, P, S) antibodies, labeled with FITC-conjugated goat anti-rabbit or anti-mouse IgG (Sigma) as appropriate, and stained with Promidium Iodide (Sigma) (B, E, H, K, N, Q, T). Analysis was performed using the LSM510. Green signals indicate the tk-FLAG or the RXP fusion proteins. The red stain indicates the nuclei
To determine if the nuclear deformation was due to apoptosis of cells, we analyzed transfected cells by TUNEL staining at 48 h after transfection with tkCΔ6-RXP, tk-FLAG, or HSV-2 US11. Each cell was co-stained with either anti-FLAG or anti-HSV-2 US11 antibodies. Apoptosis induction was limited to COS7 cells expressing tkCΔ6-RXP; the other cells were negative for TUNEL staining (Fig. 5). To confirm the apoptotic activity of RXP fusion proteins, we stained cells transfected with the chimeras with annexinV-Cy3 (Sigma), according to manufacturer’s instructions. Cells staining with annexinV-Cy3 were also stained with anti-US11 or anti-FLAG antibodies, then analyzed with a Zeiss laser scanning microscope LSM510. In cells expressing tk-RXP, tkCΔ6-RXP, or tkNΔ66-RXP, annexinV-Cy3 could be detected (Fig. 6A, B, E, F, I, J); annexinV-Cy3, however, was undetectable in cells expressing tk-FLAG, tkQ125NCΔ6-RXP, or tkNΔ200-RXP (Fig. 6C, D, G, H, K, L). These results indicate that tk-RXP, tkCΔ6-RXP, and tkNΔ66-RXP have the ability to induce apoptosis. The induction of apoptosis by tk-RXP and tkCΔ6-RXP was also confirmed by staining with anti-poly (ADP-ribose polymerase) antibody (PARP), which becomes detectable following cleavage of PARP into an 85 kD fragment (Fig. 7).
TUNEL staining. COS7 cells were transfected with the tk-FL0AG (A–C), tkCΔ6-RXP (D–F), or HSV-2-US11 expression vectors. The cells were stained with anti-FLAG (B) or anti-HSV-2 US11 (E, H) antibodies and labeled with TRITC-conjugated goat anti-rabbit or anti-mouse IgG (Sigma). Using an Apop Tag apoptosis detection kit (CHEMICON), biotin 16-dUTP was then added to the double or single stranded-DNA within these cells using terminal deoxynucleotidyltransferase to detect the free 3′ ends of newly cleaved DNA in situ (A, D, G). Analysis was performed using a Bio-Rad MRC-series confocal imaging system. Green staining indicates a TUNEL-positive cells
Annexin V-Cy3 staining. COS7 cells were transfected with tk-RXP (A, B), tk-FLAG (C, D), tkCΔ6-RXP (E, F), tkQ125NCΔ6-RXP (G, H), tkNΔ66-RXP (I, J), or tkNΔ200-RXP (K, L) expression vectors using lipofectamine 2000. Thirty-six hours after transfection, cells were stained with annexin V-Cy3 (B, D, F, H, J, L). Cells were also immunostained with HSV-2 anti-US11 (A, E, G, I, K) or anti-FLAG antibodies (C). Analysis was performed by a Bio-Rad MRC-series confocal imaging system. The red staining indicates annexin-positive cells
HSV-1 tk has ATP- (residues 56–63) [26, 27] and nucleoside (residues 96–176) [28]-binding domains in the N-terminal region. To investigate the association of these two domains with the apoptosis-inducing activity of tk-RXP, we deleted either 66 (tkNΔ66-RXP) or 200 (tkNΔ200-RXP) amino acids (aa) from the N-terminus of tk-RXP. We then transfected these tk-RXP deletion mutants and tkQ125NCΔ6-RXP, which has a point mutation in aa 125 of tk, into COS7 cells. Nuclear deformations similar to those seen in cells transfected with tk-RXP were observed in tkNΔ66-RXP expressing cells (Fig. 4N); apoptotic induction was detected in these cells by annexinV-Cy3 staining (Fig. 6I, J). In tkNΔ200-RXP (Fig. 6K, L), tkQ125NCΔ6-RXP (Fig. 6G, H), or tk-FLAG (Fig. 6C, D) expressing cells, neither nuclear deformation nor annexinV-Cy3 staining was observed. These results are summarized in Table 1. After the transfection of tk-RXP into HeLa and HEp-2 cells, we observed the apoptotic nuclear features (data not shown).
We then investigated the relationship of the HSV-1 tk domains, including the ATP-binding and nucleoside-binding domains, with the induction of apoptosis. Deletion of the tk ATP-binding domain did not affect apoptosis induction. Defects in both the ATP-binding and nucleoside-binding domains abrogated the ability of tk to induce apoptosis. In addition, a tk fusion protein bearing a single aa mutation from Q to N at aa 125 was deficient in apoptosis-inducing activity. This mutation results in a 50-fold decrease in the binding affinity for dT, and a threefold decrease in binding of acyclovir [29, 30], suggesting that this residue is critically related to DNA binding. These results suggest that HSV-2 US11 RXP repeat peptide and aa 67 to 175 of the nucleoside-binding domain in tk are required for the induction of apoptosis by the tk-RXP fusion protein. Thus far, the mechanism by which tk-RXP induces apoptosis remains unclear. The active site of HSV-1 tk resides at the N-terminal [31]. Fusion of two proteins is usually performed by joining the N-terminus of one to the C-terminus of the other. Such chimeras can result in improper folding of the protein [32, 33], causing a loss of activity. Here, the fusion of RXP to the N-terminus of tk might affect its translation, altering its activity and structure such that apoptosis was not induced. Thus, the active domain of tk described above is critical in apoptosis induction. The HSV-1 US11 RXP tandem repeat peptide binds both dsRNA and rRNA and accumulates in nucleoli [34], which supports the hypothesis that fusion proteins of HSV-1 US11 RXP could function to modulate the activity of RNA and ribosomes [17].
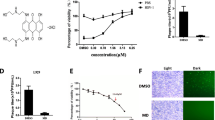
As the tk-RXP fusion protein induced apoptosis in COS7 cells in the absence of GCV, we compared the cytotoxicity of tk-RXP to that of tk-FLAG following the addition of GCV. COS7 cells were plated in 35 mm dishes transfected with 4 μg of pHGCX, pHGCX tk-RXP, or pHGCX tk-FLAG using lipofectamine 2000. Twenty-four hours after transfection, growth medium was replaced with a medium containing varying concentrations of GCV. After 48 h of culture in the presence of GCV, the number of surviving cells was counted by trypan blue staining. The survival percent of tk-RXP-transfected cells was 31.9% of the levels seen in mock-transfected cells given 5 μM GCV (Fig. 8). In contrast, the viability of tk-FLAG transfected cells was 72.6% of the mock cell numbers for the same dose of GCV, demonstrating that the tk protein carrying the RXP peptide exhibits increased cytotoxicity over that seen for tk-FLAG. As GCV inhibits hematosis, high intensity administration of GCV is limited [35], which influences the tk/GCV therapeutic efficacy. Our results indicated that the tk-RXP fusion protein induced apoptosis in transfected cells in the absence of GCV; therefore, the application of tk-RXP/GCV to cancer gene therapy would not only enhance the cytotoxicity of suicide gene therapy, but also reduce the adverse side effects of GCV.
Sensitivity of pHGCX tk-RXP, pHGCX tk-FLAG, or pHGCX vectors transfecting COS7 cells to GCV exposure. COS7 cells were transfected with 4 μg/dish of pHGCX tk-RXP, pHGCX tk-FLAG, or pHGCX. After incubation at 37°C for 24 h, cells were incubated for 48 h by DMEM supplemented with 10% FBS and concentrations of GCV ranging from 0 to 5 μM. The number of surviving cells was quantified using a hemocytometer after trypan blue staining. The experiments were done in triplicate; data were analyzed by the student’s t-test. The levels are expressed as means ± ranges. Differences were considered significant when P ≤ 0.05
In conclusion, this study demonstrated that the HSV-2 US11 RXP repeat peptide fusion protein provides the following advantages over previously explored suicide gene delivery techniques. The RXP repeat peptide can carry tk across cell membrane. In addition, the tk-RXP fusion protein can directly induce apoptosis. Apoptosis induction required both the nucleoside-binding domain (aa 67–175) of tk, including conservation of aa 125, and RXP at the C-terminus. The tk-RXP fusion protein could also enhance the cytotoxicity of the prodrug, GCV, suggesting that use of the tk-RXP fusion protein/GCV strategy may overcome critical limitations in current gene therapy methods.
References
I.J. van Dillen, N.H. Mulder, W. Vaalburg, E.F. de Vries, G.A. Hospers, Curr Gene Ther 2, 307–322 (2002)
Y. Nishiyama, F. Rapp, J Gen Virol 45, 227–230 (1979)
J. Balzarini, C. Bohman, E. De Clercq, J Biol Chem 268, 6332–6337 (1993)
D.D. Ilsley, S.H. Lee, W.H. Miller, R.D. Kuchta, Biochemistry 34, 2504–2510 (1995)
F.L. Moolten, Cancer Res 46, 5276–5281 (1986)
S.M. Freeman, C.N. Abboud, K.A. Whartenby, C.H. Packman, D.S. Koeplin, F.L. Moolten, G.N. Abraham, Cancer Res 53, 5274–5283 (1993)
J.M. DiMaio, B.M. Clary, D.F. Via, E. Coveney, T.N. Pappas, H.K. Lyerly, Surgery 116, 205–213 (1994)
J. Fick, F.G. Barker 2nd, P. Dazin, E.M. Westphale, E.C. Beyer, M.A. Israel, Proc Natl Acad Sci USA 92, 11071–11075 (1995)
M. Mesnil, C. Piccoli, G. Tiraby, K. Willecke, H. Yamasaki, Proc Natl Acad Sci USA 93, 1831–1835 (1996)
R.L. Touraine, N. Vahanian, W.J. Ramsey, R.M. Blaese, Hum Gene Ther 9, 2385–2391 (1998)
Z. Ram, S. Walbridge, J.D. Heiss, K.W. Culver, R.M. Blaese, E.H. Oldfield, J Neurosurg 80, 535–540 (1994)
S.H. Chen, K. Kosai, B. Xu, K. Pham-Nguyen, C. Contant, M.J. Finegold, S.L. Woo, Cancer Res 56, 3758–3762 (1996)
B.W. O’Malley Jr., D.A. Sewell, D. Li, K. Kosai, S.H. Chen, S.L. Woo, L. Duan, Mol Endocrinol 11, 667–673 (1997)
S. Benedetti, M.G. Bruzzone, B. Pollo, F. DiMeco, L. Magrassi, B. Pirola, N. Cirenei, M.P. Colombo, G. Finocchiaro, Cancer Res 59, 645–652 (1999)
X. Danthinne, K. Aoki, A.L. Kurachi, G.J. Nabel, E.G. Nabel, J Virol 72, 9201–9207 (1998)
G. Elliott, P. O’Hare, Cell 88, 223–233 (1997)
T. Koshizuka, H. Takakuwa, F. Goshima, T. Murata, Y. Nishiyama, Biochem Biophys Res Commun 288, 597–602 (2001)
M. Lanuti G.P. Gao, S.D. Force, M.Y. Chang, C. El Kouri, K.M. Amin, J.V. Hughes, J.M. Wilson, L.R. Kaiser, S.M. Albelda, Hum Gene Ther 10, 463–475 (1999)
N.G. Rainov, Hum Gene Ther 11, 2389–2401 (2000)
N. Shand, F. Weber, L. Mariani, M. Bernstein, A. Gianella-Borradori, Z. Long, A.G. Sorensen, N. Barbier, Hum Gene Ther 10, 2325–2335 (1999)
A. Cascante, M. Huch, L.G. Rodriguez, J.R. Gonzalez, L. Costantini, C. Fillat, Hum Gene Ther 16, 1377–1388 (2005)
E. Tasciotti, M. Zoppe, M. Giacca, Cancer Gene Ther 10, 64–74 (2003)
C.S. Liu, B. Kong, H.H. Xia, K.A. Ellem, M.Q. Wei, J Gene Med 3, 145–152 (2001)
Z. Qiu, J.S. Harms, J. Zhu, G.A. Splitter, J Virol 78, 4224–4233 (2004)
M.S. Dilber, A. Phelan A. Aints, A.J. Mohamed, G. Elliott, C.I. Smith, P. O’Hare, Gene Ther 6, 12–21 (1999)
K. Wild, T. Bohner, A. Aubry, G. Folkers, G.E. Schulz, FEBS Lett 368, 289–292 (1995)
K. Wild, T. Bohner, G. Folkers, G.E. Schulz, Protein Sci 6, 2097–2106 (1997)
H. De Winter, P. Herdewijn, J Med Chem 39, 4727–4737 (1996)
B. Degreve R. Esnouf, E. De Clercq, J. Balzarini, Mol Pharmacol 59 285–293, (2001)
S. Kussmann-Gerber, O. Kuonen, G. Folkers, B.D. Pilger, L. Scapozza, Eur J Biochem 255, 472–481 (1998)
D.G. Brown, R. Visse, G. Sandhu, A. Davies, P.J. Rizkallah, C. Melitz, W.C. Summers, M.R. Sanderson, Nat Struct Biol 2, 876–881 (1995)
R.L. Moritz, L.D. Ward, G.F. Tu, L.J. Fabri, H. Ji, K. Yasukawa, R.J. Simpson, Growth Factors 16, 265–278 (1999)
S.J. Pernecky, M.J. Coon, Methods Enzymol 272, 25–34 (1996)
R.J. Roller, L.L. Monk, D. Stuart, B. Roizman, J Virol 70, 2842–2851 (1996)
M. Nokta, M.D. Tolpin, P.I. Nadler, R.B. Pollard, Antiviral Res 24, 17–26 (1994)
Acknowledgments
We are grateful to Dr. Y. Saeki (Massachusetts General Hospital, Boston, MA) for providing pHGCX vector. This study was supported in part by Grants for Scientific Research from the Ministry of Education, Science, Sports and Culture of Japan.
Author information
Authors and Affiliations
Corresponding author
Additional information
Chenhong Luo and Akihiro Nawa contributed equally to this work
Rights and permissions
About this article
Cite this article
Luo, C., Nawa, A., Yamauchi, Y. et al. Intercellular trafficking and cytotoxicity of recombinant HSV-1 thymidine kinase fused with HSV-2 US11 RXP repeat peptide . Virus Genes 34, 263–272 (2007). https://doi.org/10.1007/s11262-006-0013-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11262-006-0013-8