Abstract
Objective
Sleep duration is an important factor influencing health outcomes. The association between sleep duration and kidney function remains elusive. This study aimed to explore the association between sleep duration and chronic kidney disease (CKD) amongst Chinese adults.
Methods
We conducted a cross-sectional study based on the China Health and Nutrition Survey (CHNS) in the wave of 2009. Participants were divided into three groups: ≤ 6 h/day (short sleepers), 7–8 h/day (regular sleepers) and ≥ 9 h/day (long sleepers) according to self-reported sleep duration. CKD was defined as estimated glomerular filtration rate < 60 mL/min/1.73 m2.
Results
A total of 8096 Chinese adults (45.9% men) with a mean age of 50.6 years were included in the study. Compared with regular sleepers, both short and long regular sleepers had a higher prevalence of CKD. A U-shaped relationship between sleep duration and CKD was displayed by restricted cubic spline curve (P-overall < 0.001, P-nonlinear < 0.001). Multivariate logistic regression models revealed that both short and long sleep duration were clinically associated with higher odds of CKD, after adjustments for covariates [adjusted odds ratio (OR) 1.25 and 1.30; 95% confidence interval (CI) 1.00–1.56 and 1.08–1.54, for short and long sleep duration, respectively]. In subgroup analyses, we found the association was still observed in participants without hypertension or diabetes mellitus.
Conclusion
Short or long sleep duration was associated with CKD in the general population.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Chronic kidney disease (CKD) is a growing public health concern with an estimated prevalence of 8–16% worldwide [1], and approximately 11% in China [2]. Individuals with CKD endure compromised health-related quality of life, and have a greater risk for progression to end-stage renal disease, cardiovascular diseases and even death [3]. CKD is often asymptomatic at early stages, and the low awareness rate allows CKD to progress through to advanced stages [4]. Unfortunately, there is no treatment to cure CKD at present [5]. Pharmaceutical therapy to delay CKD progression, such as angiotensin-converting enzyme inhibitors, angiotensin receptor blockers and sodium–glucose co-transporter-2 inhibitors, is also limited in clinical practice [5]. Screening for risk factors is favourable for developing preventive and therapeutic interventions in the management of CKD. Nontraditional CKD risk factors have been increasingly recognised as major threats to kidney health [6]. Emerging evidence suggests a high prevalence of sleep disorders in CKD patients, including insufficient sleep, poor sleep quality and sleep apnoea [6].
Sleep is a complex physiological process that is vital for human health and well-being [7]. Approximately one-third of the human lifetime is spent in sleep; however, many adults report habitually insufficient sleep duration in modern society [8]. Sleep duration is increasingly recognised as an important lifestyle contributor to health outcomes in the general population, particularly short sleep duration [8,9,10]. Previous studies have reported longitudinal associations of short sleep duration with greater risk of obesity, diabetes mellitus, cardiovascular disease and all-cause mortality [9, 11]. Interestingly, long sleep duration, generally defined as sleep durations ≥ 9 h, is also associated with increased health risks [12].
With this regard, observational studies have been increasingly carried out to explore the association between sleep duration and CKD, but their results were inconsistent. Several studies demonstrated that both short and long sleep duration were independently associated with an increased risk of CKD, and suggested a U-shaped relationship between sleep duration and CKD [13,14,15]. In contrast, other studies reported that short sleep duration was not significantly related to CKD [16, 17]. A previous meta-analysis study supported a lack of significant association between short sleep duration and CKD [18]. Therefore, more investigations were needed to ascertain the inconsistent results in different populations. To assess the relationship between sleep duration and CKD, we analysed data derived from a large survey population of the China Health and Nutrition Survey (CHNS).
Methods
Study cohort and participants
The CHNS is a prospective cohort study conducted across nine provinces in China including Liaoning, Jiangsu, Shandong, Henan, Hubei, Hunan, Guangxi, Guizhou and Heilongjiang province. The survey used a multistage, random cluster design to sample with probability proportionate. The CHNS was approved by the Institutional Review Boards of the University of North Carolina at Chapel Hill and the National Institute for Nutrition and Health, Chinese Center for Disease Control and Prevention. More detailed information about CHNS can be obtained elsewhere [19].
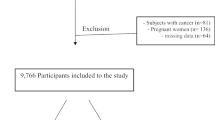
In the 2009 wave of the CHNS, blood samples were first collected and assessed in 9549 participants. Then, we excluded those without data of serum creatinine data (n = 86), adolescents (n = 822), pregnant women (n = 62), those who had protein intake more than 110 g/day (n = 379), and those without information of sleep duration (n = 104). A total sample of 8096 participants (3720 men and 4376 women) was included in the final analysis.
Definition of chronic kidney disease
Venous blood was collected from each participant after overnight fasting by medically trained staff based on standard protocols. The serum was separated and stored in the ultra-low temperature freezer. Samples were analysed at a national central laboratory under strict quality control (Medical Laboratory Accreditation Certificate ISO 15189:2007) in Beijing. Serum creatinine levels were measured using picric acid method (Hitachi 7600 automated analyzer). Detailed information was available at the website (https://www.cpc.unc.edu/projects/china/data/datasets/biomarker-data). Serum creatinine is formed as a result of the non-enzymatic dehydration of muscle creatine, which is the most widely used measure of renal function in clinical practice. In this study, serum creatinine was used to estimate glomerular filtration rate (GFR) based on the Chronic Kidney Disease Epidemiology Collaboration (CKD-EPI) equation [20]. The CKD-EPI equation, expressed as a single equation, is GFR = 141 × min(Scr/κ, 1)α × max(Scr/κ, 1)−1.209 × 0.993Age × 1.018 [if female] × 1.159 [if black], where Scr is serum creatinine in mg/dl, κ is 0.7 for females and 0.9 for males, α is − 0.329 for females and − 0.411 for males, min indicates the minimum of Scr/κ or 1, and max indicates the maximum of Scr/κ or 1. CKD was defined as estimated GFR < 60 mL/min/1.73 m2 according to Kidney Disease: Improving Global Outcomes (KDIGO) 2012 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease [21].
Define of sleep duration
Sleep duration was assessed using a self-reported questionnaire to obtain the time that the participant slept. The questionnaire on physical activity included the question that “How many hours each day do you usually sleep, including during both daytime and nighttime?” For the analysis, participants were categorised into 3 groups according to self-reported sleep duration per day: ≤ 6 h (short sleepers), 7–8 h (regular sleepers) and ≥ 9 h (long sleepers) [22].
Covariates
Demographic and behaviour data were obtained by the CHNS questionnaire and physical examination including age, sex, height, weight, hypertension, myocardial infarction, diabetes mellitus and lifestyle information (smoking and drinking). Body mass index (BMI) was calculated as body weight (kg)/height2 (m2). Smoking status was categorised as past or current smoked, and never. Urbanisation was categorised as urban and rural residence. Education level was categorised as primary school and below, and middle school and above. Hypertension, myocardial infarction, diabetes mellitus were derived from the questions “Has a doctor ever told you that you suffer from hypertension, myocardial infarction or diabetes mellitus?”.
Statistical analysis
The continuous variables with normal distribution were expressed by mean (standard deviation). The categorical variables were presented by frequency (percentage). The differences between groups were compared by ANOVA tests for continuous variates and Chi-square tests for categorical variates. Restricted cubic spline analysis was used to evaluate the nonlinear association between sleep duration and CKD. Multivariable logistic regression models were performed to explore whether sleep duration influenced CKD independently. Model 1 was only adjusted by age and sex. Model 2 was adjusted for factors from Model 1 plus BMI, race, residence site, education level, smoking status, alcohol consumption, hypertension, myocardial infarction and diabetes mellitus. Subgroup analyses based on age (≥ 60 or < 60 years), sex (male or female), BMI (≥ 24 or < 24 kg/m2), hypertension (yes or no) and diabetes (yes or no) were used to evaluate the relationship between sleep duration and CKD in these subgroups and the potential interaction between sleep duration and these stratified variables. All the data were cleaned, merged and analysed using R software (version 4.1.3). A two-tailed P value < 0.05 was determined to be statistically significant.
Results
A total of 8096 Chinese adults with a mean age of 50.6 ± 15.1 years and 3720 (45.9%) men were finally included in this study. The prevalence of CKD was 12.0% amongst the entire population. Demographic and clinical characteristics of all participants across sleep duration categories were displayed in Table 1. Amongst the 8096 participants, regular sleepers (7–8 h of sleep duration) were the most frequent, whilst 10.3% of participants had short sleep duration (≤ 6 h) and 22.8% of participants had long sleep duration (≥ 9 h). Regular sleepers were more likely to be younger and educated, and had the lowest prevalence of CKD, hypertension and diabetes mellitus. A statistical difference was also found in sex, BMI, race and residence site across sleep duration categories.
The restricted cubic spline analysis was used to identify the nonlinear association between sleep duration and CKD. As shown in Fig. 1, there was a U-shaped relationship (P-overall < 0.001, P-nonlinear < 0.001) between sleep duration and CKD taking 8 h sleep duration (median) as reference. Furthermore, results from multivariate logistic regression analyses with multiple covariates adjustments are present in Table 2. In the unadjusted model, both short and long sleep duration were significantly associated with CKD [odds ratio (OR) 2.20 and 1.73; 95% confidence interval (CI) 1.80–2.66 and 1.48–2.02, for short and long sleep duration, respectively]. After adjustments for covariates, short and long sleep duration retained their significant relationship with higher odds of CKD in adjusted model including age, sex, BMI, race, residence site, education level, smoking, alcohol consumption, hypertension, myocardial infarction and diabetes mellitus [OR (95% CI) for short and long sleep duration: 1.34 (1.08, 1.67) and 1.40 (1.18, 1.66) in model 1; 1.25 (1.00, 1.56) and 1.30 (1.08, 1.54) in model 2].
Subgroup analyses based on age, sex, BMI, hypertension and diabetes are shown in Fig. 2. The associations between short and long sleep duration and CKD risk disappeared in participants with age < 60 years old. In older adults, long sleep duration was continuously associated with the prevalence of CKD in the adjusted model, whereas short sleep duration not. By stratifying sex and BMI, there was only statically significance for long sleep duration in males and in participants with BMI < 24 kg/m2. In those without hypertension or diabetes, both short and long sleep duration correlated with the prevalence of CKD, which was not observed in those with hypertension or diabetes.
Discussion
Using data from CHNS, we found that both short and long sleepers had a higher prevalence of CKD compared with regular sleepers. There was a U-shaped relationship between sleep duration and CKD by restricted cubic spline analysis. Furthermore, multivariate logistic regression analyses also suggested that short or long duration was associated with an increased risk of CKD prevalence in all models. The association was still observed in participants without hypertension or diabetes mellitus in subgroup analyses.
The association between sleep duration and CKD has been reported inconsistent across different populations. In a cross-sectional study of Japanese middle-aged adults, short sleep duration (≤ 5 h) was not clearly associated with CKD [23]. In another Japanese prospective study, short sleep duration (≤ 5 h) was a risk factor for early CKD but only amongst shift workers, whilst long sleep duration was not associated with risk of CKD [24]. In contrast, Yamamoto et al. found that both short and prolonged sleep duration were significantly associated with deterioration of renal function in patients with CKD, even after adjusting for confounding factors [25]. In a cross-sectional study from 2004 to 2006 NHIS, Salifu et al. also found that both short and long sleep duration increased odds of self-reported CKD [26]. However, a linear relationship between objectively measured sleep duration and eGFR was observed in a Swiss general population [27]. In a cross-sectional study of elderly Chinese patients with hypertension, short sleep duration was associated with CKD [28]. More recently, Sun et al. revealed a U-shaped association between sleep duration and risk of CKD in middle-aged and older Chinese [14]. In a Mendelian randomisation analysis, causal effects of short sleep duration on CKD had been demonstrated in a large-scale general population cohort [29]. Either < 6 h or ≥ 9 h sleep duration was clinically associated with a higher prevalence of CKD [29]. Another Mendelian randomisation study demonstrated that there was no evidence of causal association between genetically predicted sleep duration and end-stage renal disease [30]. In the present study, we found that short (≤ 6 h) or long (≥ 9 h) sleep duration was associated with increased odds of CKD, which contributed to increasing the evidence regarding the association between sleep and CKD.
Substantial studies have described an abnormal sleep duration with hypertension, diabetes mellitus and cardiovascular diseases [8, 31, 32], conditions that often accompany or cause CKD. It is, therefore, possible that hypertension or diabetes may exert a mediation or confounding effect on composite renal outcome amongst participants. The results from multivariate logistic regression analyses reported that both short and long sleep duration were independently associated with CKD, even after adjustments for covariates including hypertension, myocardial infarction and diabetes mellitus. In subgroup analyses, we still observed that short and long sleep duration correlated to higher odds of CKD in participants without hypertension or diabetes mellitus, but not in those with hypertension or diabetes mellitus. This indicated that the association between sleep duration and CKD might vary by baseline disease status. Further research is needed to investigate the association of sleep duration and CKD in different clinical settings, including hereditary diseases and glomerular or interstitial diseases.
There are several possible mechanisms in support of an adverse effect of inappropriate sleep duration on CKD. Previous studies have suggested that short sleep periods may cause disturbances in circadian rhythm, and further activation of the sympathetic nervous system could impair blood pressure control [6, 33]. Short sleep duration was also found to be associated with hormonal changes, reduced insulin sensitivity and impaired β-cell function, which contributed to the increased risk of diabetes mellitus [11, 34]. Thus, short sleep duration may play an indirect role in the development of CKD. Although underlying mechanisms of long sleep duration remained poorly understood, it could be speculated that higher proportions of daytime napping, snoring or obstructive sleep apnoea may be the main cause of long sleep duration, and these sleep disturbances correlated to the progression of CKD [29]. In addition, both short and long sleep duration have been associated with markers of inflammation [35,36,37], which may represent a possible mechanism by which inappropriate sleep duration affect kidney health. The underlying mechanisms of sleep duration on CKD are required in-depth research.
Our findings were based on a large-sample cohort, which ensured stability and reliability of results from multivariate logistic regression analyses. However, there were several limitations in the study. First, diagnosis of CKD was based on a single measurement of serum creatinine value, without monitoring repeatedly, which could not rule out participants with acute kidney injury or a transient increase on serum creatinine. Second, it was unable to eliminate the effects of potential confounding factors, such as shift work and treatment including sleeping-induced drugs, due to the limited information in this retrospective study. Considerable attention should be paid to these factors in further studies. Third, self-report sleep duration was subjective from a single questionnaire rather than objective method by supervised monitoring, which might be overestimated. Additional investigations are warranted using objective measures of sleep. Finally, the causal association between sleep duration and CKD could not be determined because of the cross-sectional design of our study, and warrants prospective cohort studies. Long-term healthy sleep interventions are needed to evaluate the potential effect of optimal sleep duration on CKD in the future.
Conclusion
In summary, short or long sleep duration was associated with CKD in the general population. Further investigations are needed to clarify the relationship between sleep duration and CKD, as well as possible mechanisms underlying this association.
Data availability
The datasets generated during and/or analysed during the current study are available at the website (http://www.cpc.unc.edu/projects/china/home.html).
References
Glassock RJ, Warnock DG, Delanaye P (2017) The global burden of chronic kidney disease: estimates, variability and pitfalls. Nat Rev Nephrol 13(2):104–114. https://doi.org/10.1038/nrneph.2016.163
Zhang L, Wang F, Wang L, Wang W, Liu B, Liu J, Chen M, He Q, Liao Y, Yu X, Chen N, Zhang JE, Hu Z, Liu F, Hong D, Ma L, Liu H, Zhou X, Chen J, Pan L, Chen W, Wang W, Li X, Wang H (2012) Prevalence of chronic kidney disease in China: a cross-sectional survey. Lancet 379(9818):815–822. https://doi.org/10.1016/S0140-6736(12)60033-6
Fletcher BR, Damery S, Aiyegbusi OL, Anderson N, Calvert M, Cockwell P, Ferguson J, Horton M, Paap M, Sidey-Gibbons C, Slade A, Turner N, Kyte D (2022) Symptom burden and health-related quality of life in chronic kidney disease: a global systematic review and meta-analysis. PLOS MED 19(4):e1003954. https://doi.org/10.1371/journal.pmed.1003954
Evans M, Lewis RD, Morgan AR, Whyte MB, Hanif W, Bain SC, Davies S, Dashora U, Yousef Z, Patel DC, Strain WD (2022) A Narrative review of chronic kidney disease in clinical practice: current challenges and future perspectives. Adv Ther 39(1):33–43. https://doi.org/10.1007/s12325-021-01927-z
Barrera-Chimal J, Girerd S, Jaisser F (2019) Mineralocorticoid receptor antagonists and kidney diseases: pathophysiological basis. Kidney Int 96(2):302–319. https://doi.org/10.1016/j.kint.2019.02.030
Turek NF, Ricardo AC, Lash JP (2012) Sleep disturbances as nontraditional risk factors for development and progression of CKD: review of the evidence. Am J Kidney Dis 60(5):823–833. https://doi.org/10.1053/j.ajkd.2012.04.027
Lane JM, Qian J, Mignot E, Redline S, Scheer F, Saxena R (2023) Genetics of circadian rhythms and sleep in human health and disease. Nat Rev Genet 24(1):4–20. https://doi.org/10.1038/s41576-022-00519-z
St-Onge MP, Grandner MA, Brown D, Conroy MB, Jean-Louis G, Coons M, Bhatt DL (2016) Sleep duration and quality: impact on lifestyle behaviors and cardiometabolic health: a scientific statement from the American heart association. Circulation 134(18):e367–e386. https://doi.org/10.1161/CIR.0000000000000444
Tobaldini E, Fiorelli EM, Solbiati M, Costantino G, Nobili L, Montano N (2019) Short sleep duration and cardiometabolic risk: from pathophysiology to clinical evidence. Nat Rev Cardiol 16(4):213–224. https://doi.org/10.1038/s41569-018-0109-6
Li J, Cao D, Huang Y, Chen Z, Wang R, Dong Q, Wei Q, Liu L (2022) Sleep duration and health outcomes: an umbrella review. Sleep Breath 26(3):1479–1501. https://doi.org/10.1007/s11325-021-02458-1
Antza C, Kostopoulos G, Mostafa S, Nirantharakumar K, Tahrani A (2021) The links between sleep duration, obesity and type 2 diabetes mellitus. J Endocrinol 252(2):125–141. https://doi.org/10.1530/JOE-21-0155
García-Perdomo HA, Zapata-Copete J, Rojas-Cerón CA (2019) Sleep duration and risk of all-cause mortality: a systematic review and meta-analysis. Epidemiol Psychiatr Sci 28(5):578–588. https://doi.org/10.1017/S2045796018000379
Hao Q, Xie M, Zhu L, Dou Y, Dai M, Wu Y, Tang X, Wang Q (2020) Association of sleep duration with chronic kidney disease and proteinuria in adults: a systematic review and dose-response meta-analysis. Int Urol Nephrol 52(7):1305–1320. https://doi.org/10.1007/s11255-020-02488-w
Sun H, Qin K, Zou C, Wang HH, Lu C, Chen W, Guo VY (2021) The association of nighttime sleep duration and quality with chronic kidney disease in middle-aged and older Chinese: a cohort study. Sleep Med 86:25–31. https://doi.org/10.1016/j.sleep.2021.08.007
Jiang L, Xu H (2023) U-shaped relationship between sleep duration and CKD in US adults: data from national health and nutrition examination survey (NHANES) 2005–2014. Am J Nephrol. https://doi.org/10.1159/000531440
Petrov ME, Buman MP, Unruh ML, Baldwin CM, Jeong M, Reynaga-Ornelas L, Youngstedt SD (2016) Association of sleep duration with kidney function and albuminuria: NHANES 2009–2012. Sleep Health 2(1):75–81. https://doi.org/10.1016/j.sleh.2015.12.003
Kim CW, Chang Y, Sung E, Yun KE, Jung HS, Ko BJ, Kwon MJ, Hyun YY, Lee KB, Kim H, Shin H, Ryu S (2017) Sleep duration and quality in relation to chronic kidney disease and glomerular hyperfiltration in healthy men and women. PLoS ONE 12(4):e0175298. https://doi.org/10.1371/journal.pone.0175298
Cheungpasitporn W, Thongprayoon C, Gonzalez-Suarez ML, Srivali N, Ungprasert P, Kittanamongkolchai W, Caples SM, Erickson SB (2017) The effects of short sleep duration on proteinuria and chronic kidney disease: a systematic review and meta-analysis. Nephrol Dial Transplant 32(6):991–996. https://doi.org/10.1093/ndt/gfw072
Popkin BM, Du S, Zhai F, Zhang B (2010) Cohort profile: the China health and nutrition survey–monitoring and understanding socio-economic and health change in China, 1989–2011. INT J EPIDEMIOL 39(6):1435–1440. https://doi.org/10.1093/ije/dyp322
Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF 3rd, Feldman HI, Kusek JW, Eggers P, Van Lente F, Greene T, Coresh J, CKD-EPI (Chronic Kidney Disease Epidemiology Collaboration) (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150(9):604–12. https://doi.org/10.7326/0003-4819-150-9-200905050-00006
K/DOQI clinical practice guidelines for chronic kidney disease (2002) evaluation, classification, and stratification. Am J Kidney Dis 39(2 Suppl 1):S1-266
Watson NF, Badr MS, Belenky G, Bliwise DL, Buxton OM, Buysse D, Dinges DF, Gangwisch J, Grandner MA, Kushida C, Malhotra RK, Martin JL, Patel SR, Quan SF, Tasali E (2015) Recommended amount of sleep for a healthy adult: a joint consensus statement of the American academy of sleep medicine and sleep research society. Sleep 38(6):843–844. https://doi.org/10.5665/sleep.4716
Fujibayashi K, Fukuda H, Yokokawa H, Haniu T, Oka F, Ooike M, Gunji T, Sasabe N, Okumura M, Iijima K, Hisaoka T, Isonuma H (2012) Associations between healthy lifestyle behaviors and proteinuria and the estimated glomerular filtration rate (eGFR). J Atheroscler Thromb 19(10):932–940. https://doi.org/10.5551/jat.12781
Sasaki S, Yoshioka E, Saijo Y, Kita T, Tamakoshi A, Kishi R (2014) Short sleep duration increases the risk of chronic kidney disease in shift workers. J Occup Environ Med 56(12):1243–1248. https://doi.org/10.1097/JOM.0000000000000322
Yamamoto R, Shinzawa M, Isaka Y, Yamakoshi E, Imai E, Ohashi Y, Hishida A (2018) Sleep quality and sleep duration with CKD are associated with progression to ESKD. Clin J Am Soc Nephrol 13(12):1825–1832. https://doi.org/10.2215/CJN.01340118
Salifu I, Tedla F, Pandey A, Ayoub I, Brown C, McFarlane SI, Jean-Louis G (2014) Sleep duration and chronic kidney disease: analysis of the national health interview survey. Cardiorenal Med 4(3–4):210–216. https://doi.org/10.1159/000368205
Ogna A, Forni OV, Haba RJ, Tobback N, Andries D, Preisig M, Tafti M, Vollenweider P, Waeber G, Marques-Vidal P, Heinzer R (2016) Sleep characteristics in early stages of chronic kidney disease in the hypnolaus cohort. Sleep 39(4):945–953. https://doi.org/10.5665/sleep.5660
Guo X, Yu S, Li Z, Guo L, Zheng L, Yang H, Zou L, Hu W, Zhou Y, Zhu L, Zhang Y, Sun Y (2015) Self-reported sleep duration is associated with reduced glomerular filtration rate among adults with hypertension: a population-based study from rural northeast China. J Sleep Res 24(3):351–358. https://doi.org/10.1111/jsr.12274
Park S, Lee S, Kim Y, Lee Y, Kang MW, Kim K, Kim YC, Han SS, Lee H, Lee JP, Joo KW, Lim CS, Kim YS, Kim DK (2020) Short or Long sleep duration and CKD: a mendelian randomization study. J Am Soc Nephrol 31(12):2937–2947. https://doi.org/10.1681/ASN.2020050666
Li K, Zhao J, Yang W, Ye Z (2023) Sleep traits and risk of end-stage renal disease: a mendelian randomization study. BMC Med Genomics 16(1):76. https://doi.org/10.1186/s12920-023-01497-9
Jike M, Itani O, Watanabe N, Buysse DJ, Kaneita Y (2018) Long sleep duration and health outcomes: a systematic review, meta-analysis and meta-regression. Sleep Med Rev 39:25–36. https://doi.org/10.1016/j.smrv.2017.06.011
Itani O, Jike M, Watanabe N, Kaneita Y (2017) Short sleep duration and health outcomes: a systematic review, meta-analysis, and meta-regression. Sleep Med 32:246–256. https://doi.org/10.1016/j.sleep.2016.08.006
Seravalle G, Mancia G, Grassi G (2018) Sympathetic nervous system, sleep, and hypertension. Curr Hypertens Rep 20(9):74. https://doi.org/10.1007/s11906-018-0874-y
Davies SK, Ang JE, Revell VL, Holmes B, Mann A, Robertson FP, Cui N, Middleton B, Ackermann K, Kayser M, Thumser AE, Raynaud FI, Skene DJ (2014) Effect of sleep deprivation on the human metabolome. Proc Natl Acad Sci USA 111(29):10761–10766. https://doi.org/10.1073/pnas.1402663111
Meier-Ewert HK, Ridker PM, Rifai N, Regan MM, Price NJ, Dinges DF, Mullington JM (2004) Effect of sleep loss on C-reactive protein, an inflammatory marker of cardiovascular risk. J Am Coll Cardiol 43(4):678–683. https://doi.org/10.1016/j.jacc.2003.07.050
Patel SR, Zhu X, Storfer-Isser A, Mehra R, Jenny NS, Tracy R, Redline S (2009) Sleep duration and biomarkers of inflammation. Sleep 32(2):200–204. https://doi.org/10.1093/sleep/32.2.200
Dowd JB, Goldman N, Weinstein M (2011) Sleep duration, sleep quality, and biomarkers of inflammation in a Taiwanese population. Ann Epidemiol 21(11):799–806. https://doi.org/10.1016/j.annepidem.2011.07.004
Acknowledgements
The authors would like to express sincere appreciation to the Institutional Review Board of the University of North Carolina at Chapel Hill and the National Institute for Nutrition and Food safety at China Center for Disease Control and Prevention for providing original data publicly available.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial or non-for-profit sectors.
Author information
Authors and Affiliations
Contributions
Both NP and SL contributed to the design, analysis, interpretation, and writing and review of the paper. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Peng, N., Li, S. Short or long sleep duration was associated with chronic kidney disease in a Chinese nationwide cohort study. Int Urol Nephrol 56, 1695–1701 (2024). https://doi.org/10.1007/s11255-023-03861-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-023-03861-1