Abstract
Lipoic acid (α-LA) (1,2-dithiolane3-pentanoic acid (C8H14O2S2) is also called thioctic acid with an oxidized (disulfide, LA) and a reduced (di-thiol: dihydro-lipoic acid, DHLA) form of LA. α-LA is a potent anti-oxidative agent that has a significant potential to treat neurodegenerative disorders. α-LA is both hydrophilic and hydrophobic in nature. It is widely distributed in plants and animals in cellular membranes and in the cytosol, which is responsible for LA’s action in both the cytosol and plasma membrane. A systematic literature review of Bentham, Scopus, PubMed, Medline, and EMBASE (Elsevier) databases was carried out to understand the Nature and mechanistic interventions of the α-Lipoic acid for central nervous system diseases. Moreover, α-LA readily crosses the blood-brain barrier, which is a significant factor for CNS activities. The mechanisms of α-LA reduction are highly tissue-specific. α-LA produces its neuroprotective effect by inhibiting reactive oxygen species formation and neuronal damage, modulating protein levels, and promoting neurotransmitters and anti-oxidant levels. Hence, the execution of α-LA as a therapeutic ingredient in the therapy of neurodegenerative disorders is promising. Finally, based on evidence, it can be concluded that α-LA can prevent diseases related to the nervous system.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Alpha-lipoic acid (α-LA) is an essential antioxidant derived from octanoic acid’s energy metabolism. Due to its versatile nature and numerous therapeutic properties, it has gained the attention of researchers globally. α-LA is considered as a vital nutrient due to which its health effects are perceived after an increase in diet (600–1800 mg/day), and 600–2400 mg/day is considered a safe dose. α-LA is present in both plants and animals, and high concentration is found in tomatoes, spinach, broccoli (plant sources), liver, kidney, heart (animal sources) (Fig. 1). α-LA contains “8 carbons with 2 sulfur atoms in dithiol ring”. In the liver, α-LA can be synthesized naturally via several enzymatic reactions from octanoic acid and cysteine [1].
The Brief description showing alpha-lipoic acid (α-LA), via inhibiting oxidative damage and chronic inflammation, can be an essential therapeutic agent in treating neurodegenerative disorders. The figure also shows where the α-LA is present in the highest concentration with respect to plant and animal sources
α-LA is absorbed via various carriers, including monocarboxylic and sodium-dependent multivitamin carriers. Due to these multiple absorptive routes, α-LA absorption may be affected by substrate competition and subject to transcriptional and post-transcriptional regulation of specific carrier proteins. The oxidized and reduced forms of dihydrolipoic acid (DHLA), both of which are antioxidants and anti-inflammatory agents, are responsible for the effects of α-LA on the cellular mechanism (Fig. 2) [2, 3]. It works by inhibiting neuron damage, removing free radicals, regulating nerve growth factor (NGF), reducing lipid peroxidation, and preventing T lymphocytes and monocytes from migrating into the CNS [3, 4].
Recently, α-LA attracted enormous attention in neurodegenerative disease management as a potential therapeutic option. The present review is focused on the role of α-LA in various neurodegenerative diseases, including Parkinson’s disease (PD), Alzheimer’s disease (AD), stroke, multiple sclerosis, epilepsy, and spinal cord injury (SCI) [5]. In these neurodegenerative disorders, the disease’s progression starts from subsequent energy deficiency and mitochondrial dysfunction in the disease’s early stages [6]. In earlier studies, α-LA was found to have a protective effect on the mitochondria. Indirectly, α-LA boosts mitochondrial biogenesis and improves the antioxidant system [7].
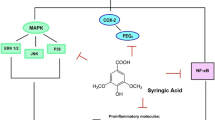
Furthermore, because of its ability to regulate specific genes encoding Nrf-2 and NF-κB, α-LA is referred to as a pleiotropic molecule. The mechanisms of action of α-LA indicate that it acts indirectly on the activation of signal transduction pathways [8] via interactions with second messengers, such as cyclic adenosine monophosphate (cAMP). α-LA causes an increase in cAMP via inhibiting the release of proinflammatory cytokines such as IL-2, TNF-α, and IFN-γ. Moreover, cAMP encourages the production of an anti-inflammatory cytokine (IL-10) which is responsible for chemokines, cytokine receptor inhibition, inflammatory mediators inhibition induced by lipopolysaccharide (LPS). cAMP activates protein kinase A (PKA) by attaching to its regulatory subunits, releasing the catalytic subunits from inhibition, and allowing phosphorylation of a variety of downstream substrates. Because of the enormous variety of ligands and GPCRs available, cAMP regulates many physiological and pathological processes through activating PKA [9]. α-LA action on NF-κB also affects inflammatory mediators expressions, which includes PGE2, iNOS, COX-2, IL-1β, TNF-α, and IL-6 [9,10,11]. Activation of NF-κB comprises ubiquitination and phosphorylation under inflammatory response. The epigenetic mechanisms, such as dysfunction of histone acetylation, DNA methylation, and miRNAs regulation, play a vital role in neurodegenerative disorders pathology [12]. The precise mechanisms by which α-LA acts on direct or indirect epigenetic regulatory pathways remain unknown. Thus, a better insight into the mechanism of action of α-LA may influence the development of more efficient therapies for neurodegenerative disorders.
Materials and methods
A systematic literature review of PubMed, Medline, Bentham, Scopus, and EMBASE (Elsevier) databases was carried out with the keywords “Alpha-lipoic acid, neurodegenerative disease diseases, Neuroprotection, Dihydrolipoic acid, Mitochondrial dysfunction, Oxidative stress.” The review was conducted using the above keywords to collect the latest articles and understand the Nature of the extensive work done on α-Lipoic acid in neurodegenerative diseases.
De Novo Synthesis of α-LA and Itsitsnctions
α-LA, also known as thioctic acid or 1,2-dithiolane-3-pentanoic acid, contains a single chiral center and is found in both forms, i.e., R-&S-enantiomers. On the other hand, only R-LA is amide linked to conserved lysine residues, making it an essential cofactor in biological systems [5]. In human cells, fatty acids are synthesized de novo in the cytoplasm by fatty acids synthesis type 1 (FAS-I) and in the mitochondria by fatty acids synthesis type 2 (FAS-II) [13]. The human body can only produce a finite amount of α-LA via de novo catabolism, which is why α-LA should be considered an essential nutrient. α-LA is involved in Proteins’ energy process, carbohydrates, and fats metabolism because of its fat- and water-soluble properties. On the other hand, α-LA is also considered a unique antioxidant scavenging almost all forms of free radicals (oxygen and nitrogen) due to its sulfur content structure. DHLA (reduced form of α-LA) tends to restore vitamin E, glutathione, and ascorbate from these radical forms. DHLA potentially increases choline acetyltransferase (ChAT) activity, essential for cognitive functions and neuronal homeostasis [5]. The biological effects of α-LA are also associated with its anti-mutagenic and anti-carcinogenic activities [2, 14] (Fig. 3).
Figure describing the role of α-LA as anti-oxidant, anti-inflammatory, and metal chelator; NF-κβ (nuclear factor kappa-light-chain-enhancer of activated B cells); NDD (Neurodegenerative Disease); TNF-α (Tumor Necrosis Factor); IL-6 and IL-1β (Interleukin); ROS (Reactive Oxygen Species); Cu (Copper); Fe (Iron)
Lipoid Acid and neurodegenerative Diseases
α-LA has gained much attention as a nutritional supplement with promising therapeutic benefits in treating or preventing various diseases, including neurodegenerative diseases. α-LA has been found to reduce mitochondrial dysfunction while protecting against cognitive dysfunction associated with neurodegenerative diseases. Thus, this section will summarize and discuss key findings supporting the use of α-LA as an adjuvant in treating neurodegenerative disorders via different signalling pathways.
Parkinson’s disease
The pathogenesis of PD depends on the dopaminergic neurons relapse in the substantia nigra pars compacta causing reduction of dopaminergic terminals in the striatum. Excessive levels of free radicals in Parkinson’s or dopamine and melanin auto-oxidization to reactive free radicals may result in the occurrence of oxidative reaction [15]. The mechanism behind augmented oxidative stress is mitochondria dysfunction, making the cells prone to external toxins. Studies showed that mitochondria could be a promising target to lead the therapeutic approach in neurodegenerative disorders, including PD. α-LA is considered a mitochondrial nutrient, and based on this, a study showed effective results of prevention of mitochondrial dysfunction on combined pretreatment of α-LA and acetyl-L-carnitine in a cellular model of PD [16] via decreased complex I activity, ATP production, and mitochondrial membrane potential. In the early stages, motor symptoms like rigidity, tremor, and bradykinesia occur due to neuronal deficit in the nigrastratum region. Later, it may progress to slow voluntary activities declined voice volume. It has also been known that mitochondria have a crucial role in the apoptotic cell death pathway via ‘death agonists’ such as Bax. Therefore, oxidative stress and mitochondrial dysfunction might change the threshold of apoptotic pathways activation in responses to Bax and other various pro-apoptotic molecules [16, 17]. Mitochondrial dysfunction leads to impaired energy metabolisms which remove cells susceptible to weak excitotoxicity, causing alterations in the “energy-dependent cell membrane potential.”
Further, this excitotoxic injury might increase free radical generation enhancing cellular damage. Studies revealed that antioxidants improved mitochondrial function and exerted neuroprotective effects against neurodegenerative disorders. Another critical role of α-LA in PD has been its ability to alter monoamine concentrations across the brain, which could have therapeutic implications in neurodegenerative disorders such as PD [18]. It is well established that oxidative stress contributes to dopaminergic degeneration in Parkinson’s disease (PD). In general, areas of the brain that are high in catecholamines (CA) are more vulnerable to ROS action. α-LA stimulates the release of noradrenaline and dopamine by encouraging release or decreasing the rate of monoamine metabolism and altering the acetylcholine concentration by increasing acetylcholinesterase activity. Dopamine metabolism via “monoamine oxidase or auto-oxidation” resulted in the production of hydrogen peroxide, which caused inflammation and ROS-induced tissue injury [19]. Since α-LA has demonstrated antioxidant activity, it may be pharmacologically helpful in managing neurodegenerative disorders involving oxidative stress, such as Parkinson’s disease. In various studies, it has been seen that α-LA acts by attenuating oxidative stress, enhancing norepinephrine, serotonin, and dopamine levels, providing neuroprotection [20]. α-LA was proven effective in the MPTP mouse model of Parkinson’s disease via inhibiting the activation of the apoptotic signalling cascade and the translocation of Daxx (death-associated protein) in the ventral midbrain and striatum, thereby preventing dopaminergic cell loss [21].
α-LA provides partial neuroprotection against 6-OHDA neurotoxicity, partly due to reducing oxidative stress burden and inhibiting the AMPK/mTOR autophagy pathway [22]. This, in combination with other therapies, may be beneficial in neurodegenerative disorders such as PD [15]. α-LA increased the number of neurons in the SNpc of parkinsonian rats treated with rotenone, protected dopaminergic neurons from degeneration, and decreased α-synuclein deposits in the substantia nigra (SN). Additionally, the authors demonstrated that α-LA inhibited the stimulation of nuclear factor- κB (NF-κB) and the expression of pro-inflammatory cytokines in M1 microglia [23, 24]. Overall, it has been seen that α-LA can be used as an effective treatment in PD.
Alzheimer’s disease
AD is characterized by progressive loss of cognitive functions, including memory, reasoning, and language, during daily social activities. Alzheimer’s disease causes dementia and mainly affects middle to old-aged individuals [24, 25]. Although the exact mechanism underlying AD’s pathogenesis has yet to be discovered, several hypotheses have been proposed to justify its origin. According to the previous studies known as the amyloid cascade hypothesis, in the pathological cascade of AD, clustering of A-beta peptides in amyloid plaques is the very first step. Hyperphosphorylation of the tau protein and β-amyloid peptide deposits (Aβ) is amongst those recognized in the scientific milieu [26]. Aβ buildup activates immune system cells, promoting inflammatory cytokines production, oxidative stress, and an increase in Aβ production, resulting in a vicious cycle that lasts the rest of the person’s life [27]. Increased oxygen consumption, polyunsaturated fat content, low regenerative capacity, and low antioxidant concentration contribute to brain tissue’s oxidative damage [23, 28]. As per the oligomer hypothesis, it has been seen that AD begins with synaptic dysfunction caused by soluble A-beta oligomers, resulting in changes in neurotransmitters and the cholinergic system. These alterations include disrupting basal cholinergic neurons in the forebrain cortex and decreased acetylcholine production. Acetylcholine synthesis has been impaired by glucose depletion in AD brains since acetylcholine metabolism was correlated with the glycolytic pathway and pyruvate formation [29]. Thus, oxidative stress and energy depletion are vital biochemical hallmarks of the disease. According to these findings, α-LA may also be capable of directly increasing the concentration of the substrate acetyl-CoA required for Ach synthesis [30]. In AD progression, Oxidative stress to brain tissue leads to free radical superoxide, further resulting in neuronal damage. The evaluation of oxidative stress and tissue damage markers could indicate this pathology’s progression and severity [31].
Ibuprofen and lipoic acid (IBU-LA) treatment have the potential to keep a high neuroglobin (Ngb) level in an AD model, enabling Ngb to perform either its neuroprotective function, via p-Akt and p-CREB activation, or its anti-apoptotic effect, by affecting the mitochondrial apoptotic pathway. It thus supports a valuable tool in therapeutic strategy to slow AD progression. LA is thought to interfere with AD pathogenesis, including by increasing acetylcholine (Ach) production via activation of choline acetyltransferase (ChAT) and by increasing glucose uptake. LA’s are related to its antioxidant properties and involved in scavenging of reactive oxygen species (ROS), thereby increasing the levels of active reduced glutathione; scavenging lipid peroxidation products, such as 4-hydroxynonenal (HNE) and acrolein (prop-2-enal); and downregulation of redox-sensitive pro-inflammatory mediators such as tumor necrosis factor-alpha (TNF-) and inducible nitric oxide (iNO) via NF-κB and upregulation of phase II enzymes via NRF-2 [32, 33]. LA is an essential supplement for restoring brain glucose metabolism, which is involved in the upregulation of GLUT3, GLUT4, VEGF, OGG1/2, MTH1, and HK activity in the AD via BDNF/TrkB/HIF-1 pathway [34]. In terms of treatment, antioxidants and oxidative stress biomarkers could estimate clinical outcomes and benefits. However, there is not much data on using biomarkers in AD described as predictors of clinical outcomes or severity [35]. α-LA appears to enhance the PI3K/Akt pathway of insulin signaling and alter synaptic deficits in Alzheimer’s mouse models [36, 37]. In the brains of elderly rats, Pd-LA improved mitochondrial energy status. The research also supports Pd-LA as adjunctive therapy in people with mild or moderate dementia caused by Alzheimer’s disease and standard cholinesterase inhibitors [38]. As a result, α-LA may be considered for augmentation therapy in Alzheimer’s disease.
Stroke
Stroke is the leading cause of long-term disability in developed countries, affecting millions of people [39]. Stroke is recognized as an abrupt loss of neurologic function due to a disruption in cerebral blood flow caused by hemorrhage or ischemia. The lack of oxygen and glucose in the brain can cause neurons to be unable to synthesize ATP, resulting in brain ischemia [40, 41]. Failure in ATP synthesis causes neuronal death through several congregating mechanisms, e.g., oxidative stress. According to previous research, oxidative stress is the major cause of brain injury in stroke and reperfusion following stroke [39, 41]. α-LA was given intravenously after reperfusion of a transient middle cerebral artery occlusion, showing a decrease in infarct size, oxidative damage, and brain edema while promoting neurologic recovery. α-LA helps treat and promote functional recovery after ischemic stroke by reducing oxidative damage, partly mediated by the Nrf2/HO-1 pathway [42, 57]. Both α-LA-Pretreatment and IPC therapy reduced neuroinflammation by inhibiting the TLR4/MyD88/NF-κB signalling pathway, resulting in substantial neuroprotection against IRI [43]. Under pathological conditions, the brain was highly susceptible to ROS, which causes damage due to reduced antioxidants, increased peroxidizable lipids, iron levels, and high oxygen uptake that function as pro-oxidants [44]. ROS overproduction continues even after ischemia when blood flow resumes, and brain oxygen tension rises. Therefore, ROS is considered one of the most critical components of tissue injury after reperfusion of an ischemic organ [39]. Oxidative stress resulting from ROS in brain hemorrhage ischemia and reperfusion contributes to stroke-induced neuronal death” thru both apoptosis and necrosis.
Many agents were identified as a neuroprotective therapeutic strategy for brain injury, such as Alpha-lipoic acid (α-LA) [45]. α-LA is an antioxidant frequently used to manage neurodegenerative disorders such as Alzheimer’s disease and Parkinson’s disease [21, 35, 36]. α-LA impacts various cellular processes, including free radical scavenging, endogenous antioxidant regeneration, recycling, metal chelation, and transcription factor activity variation [46]. α-LA was achieved by restoring the phosphorylation of Akt and GSK3-β levels in the hippocampus. α-LA reduced cerebral ischemia and reperfusion-induced damage in adult rats by triggering the PI3K/Akt signalling pathway when given for three days [47]. In a triple transgenic mouse model of AD (3xTg-AD), α-LA improves cognitive glucose uptake, stimulates the insulin receptor substrate and the PI3K/Akt signalling pathway, counteracting the impaired synaptic plasticity and growing input/output and long-term stimulation (LTP) [48]. α-LA has been shown to improve endothelial function, blood flow, and glutathione synthesis and play a key role in regulating antioxidant and anti-inflammatory gene expression in studies [7, 49]. α-LA rescued cortical neurons from damage caused by Aβ peptide- and hydrogen peroxide, implying that the neuroprotective effects were partially attributable to activation of the PKB/Akt signalling pathway [50, 51]. Recent research suggests that calcium may play a role in the neuroprotective effects of α-LA in ischemia/reperfusion. Due to ischemia, an increase in IC calcium level might have a significant role in neuronal damage. In cortical neuronal cells, α-LA has been shown to increase resting Ca2+ levels and decrease the Ca2+ rise elicited by glutamate [39]. It has been seen that after ischemic injury, instant α-LA treatment (20 mg/kg) had long-term (56 days) neuro-restorative effects against neural damage [52]. The neuroprotective effects of α-LA pretreatment for ischemic injury have been shown in several different experimental models of MCAO in rodents [51, 53,54,55,56].
Multiple sclerosis
Multiple sclerosis (MS) is a multifactorial neurodegenerative disease in which both inflammatory and neurodegenerative processes occur simultaneously, with inflammation decreasing while CNS deterioration progresses [58]. Apoptosis and excitotoxicity linked to calcium, glutamate overload, proteolytic enzyme production, ionic channel dysfunction, and mitochondriopathy are all factors in the progression of CNS complications in MS. Mitochondrial dysfunction results in ROS overproduction, further causing damage to neurons and glia [59, 60]. Oxidative stress also damages the mitochondria causing disruption of the ATP transport along the axon leading to neurological disorder [61,62,63,64,65,66]. The inflammatory component is essential due to axonal and neuronal loss and the fact that it initiates the degenerative cascade in the primary stage of MS [67]. Inflammatory processes are affected by the activation of mitochondrial dysfunction and microglia. Microglia activated by T-lymphocytes release proteolytic enzymes, cytokines, oxidative products, and free radicals. However, microglia also have many protective properties, such as neuroprotection, lowering of the inflammatory response, and stimulation of tissue repair [68,69,70]. It’s worth noting that the procedure is convoluted and poorly understood. The treatment aims to reduce inflammation, which is possible when free radicals are neutralized. There is a need for the course to reduce disease severity and cause faster diminution and less neuroinflammation [71]. α-LA as a dietary supplement helps suppress and treat the animal model of MS [72,73,74,75]. α-LA is an antioxidant, and the primary outcome is to focus on “disease-modifying therapy” in MS experimental and clinical trials (Table 1). α-LA has shown its neuroprotective effects and the capability to cross through BBB and suppress monocytes infiltration into CNS via “reducing the migration of monocytes and improving BBB stability” against oxidative stress attacks.
In conclusion, α-LA appears to benefit molecular mediators and inflammatory and antioxidant markers. α-LA may prove helpful in treating MS by inhibiting MMP-9 activity and interfering with T-cell migration into the CNS [76, 77]. Also, they determined the pharmacokinetics (PK), tolerability, and effects on matrix metalloproteinase-9 (MMP-9) and soluble intercellular adhesion molecule-1 (sICAMP-1) of oral α-LA in patients with MS [78, 79].
Spinal cord injury
SCI is characterized by the initial, primary injury resulting from secondary injury processes involving complex biochemical, molecular, and cellular changes and even more extensive damage [80, 81]. The secondary events, accompanied by SCI, include microvascular ischemia, oxidative stress, excitotoxicity, ion imbalance, and inflammation [81]. A growing body of evidence suggests that oxygen-free radicals play an essential role in progressive spinal cord degeneration after spinal injury [82,83,84,]. In this line, a study conducted in the animal model of SCI found that increased ROS production is an early and likely causal event that contributes to the spinal cord motor neuron death following SCI. Moreover, LA reduced SCI-induced oxidative stress and demonstrated its neuroprotection by inhibiting lipid peroxidation, glutathione depletion, and DNA fragmentation. Impaired mitochondrial function occurs rapidly and may occur due to the rapid accumulation of high levels of intracellular Ca2+ observed following traumatic injury. As a result, ROS are formed that can impair the function of several cellular components, such as lipids, through oxidative mechanisms. The cytotoxic consequences of lipid peroxidation have led to the development of therapeutic strategies utilizing lipid antioxidants [85,86,87,88,89,90,91,92,93,94].
Epilepsy
Epilepsy is a chronic brain disease evidenced by temporary central nervous system dysfunction caused by the paradoxical neuronal discharge. Epilepsy’s pathogenesis is hugely complex and has not been completely elaborated. Epilepsy is caused by abnormal neuronal discharge, which can be induced by various factors, including excitatory glutamate toxicity, oxidative stress injury, and intracellular calcium overload [95]. It is widely believed that neuronal damage is caused by a chain reaction of oxygen-free radicals triggered by oxidative stress [95]. Previous research has established a strong correlation between the level of Nrf2 expression and epileptic seizures. When cells are stimulated exogenously, such as by oxidative stress, Nrf2 is released from Keap1 and transferred to the nucleus. It combines with the ARE, thereby inducing the transcription of antioxidant genes [96]. α-LA possesses a high resistance to oxidative stress, thereby protecting various cell types from apoptosis [97]. α-LA has been shown to facilitate Nrf2-mediated ARE pathway activation and HO-1 induction in human retinal pigment epithelium [98]. Recent epilepsy treatments may rely on increasing Nrf2 protein expression as Nrf2 is present in the cell plasma under normal physiological conditions, covalently linked to the Kelch-like ECH-associated protein 1 (Keap1) [96, 99,100,101]. α-LA has been shown to reduce the number of epileptic seizures and improve behavioral and cognitive disorders in rats exposed to pentetrazol. α-LA reduced nerve cell apoptosis and ameliorated neurological deficits by increasing Nrf2 expression (Fig. 4). The study also indicated that α-LA might be a choice for neuroprotection in epilepsy therapy [102].
Figure Summarizes the role of α-LA in the pathophysiology of different neurodegenerative disorders via different signaling pathways; I.C. (Intracellular); Nrf-2 (Nuclear factor erythroid 2-related factor 2); Ach (Acetylcholine); BBB (Blood brain barrier); Co-A (Coenzyme A); MAO (Monoamine oxidase); Conc. (Concentration); AD (Alzheimer’s Disease); MS (Multiple Sclerosis); SCI (Spinal Cord Injury); PD (Parkinson’s Disease); NF-κβ (nuclear factor kappa-light-chain-enhancer of activated B cells)
Proteomic analysis on neurodegenerative disease
Proteomics is the study of protein levels, functions, and interactions on a large scale. It has been widely used in basic science and shows promise in clinical research, particularly in disease diagnostics [102, 103]. However, proteomics of the brain remains challenging due to the brains’ multiple regions with distinct functions. This section summarizes the proteins expressed differently and/or less oxidized in the mouse brain treated with α-LA. α-LA improves learning and memory by lowering protein oxidation and lipid peroxidation in the brains of SAMP8 mice (aged-normal mice) [102]. Proteins such as DRP-2, α-enolase, LDH, CK, and NF-L are protected by α-LA injection. The reduction of specific carbonyl levels and the increase in protein levels of specific proteins are linked to improved learning and memory in α-LA-treated SAMP8 mice. It has been suggested that oxidation of a-enolase may be responsible for the reduced levels of ATP production and acetylcholine concentration [104, 105]. By decreasing oxidative modification and increasing a-enolase protein levels in SAMP8 mice, α-LA injections imply that a-enolase activity can be preserved. A decrease in LDH carbonyl levels after injection of α-LA into SAMP8 mice suggests that α-LA treatment may help restore LDH’s ability to produce lactate in older SAMP8 mice.
As a result, in older SAMP8 mice, increased LDH activity may aid in neuronal recovery and, in turn, enhance learning and memory [106, 107]. In the brain’s grey matter, ATP concentration is thought to be controlled by an association between the proteins uMiCK and CK. Besides, only neurons expressing uMiCK have a mitochondrial synthesis of creatine phosphate, indicating that uMiCK protects neurons from energy shortages during increased energy demand. CKBB oxidation has been suggested to explain the decreased ATP production observed in the brains of aged SAMP8 mice [108]. Loss of CKBB activity in aged SAMP8 brains may necessitate an increase in uMiCK expression by injection of LA. Antioxidant defense systems in neurons and synapses would be restored due to this. The increased axonal dystrophy in the nucleus is due to decreased NF-L expression [102, 106]. When α-LA is administered to SAMP8 mice, the NF-L level in their aging brains rises, and the axonal dystrophy appears to be reduced, which improves learning and memory in the SAMP8 mice. An elevated specific carbonyl level of DRP-2 was also found [106], suggesting that oxidative deactivation of DRP-2 is to blame for the decline in learning and memory in older SAMP8. Using α-LA to treat aged SAMP8 mice reduces the oxidative modification of DRP2, possibly restoring DRP-2 activity and thus normal axonal neurogenesis. As a result, α-LA administration improved cognitive function using underlying proteomics mechanisms. More research outlining the proteomic studies should be explored to understand better how lipoic acid improves cognitive function.
Conclusion
As of now, it is not clear how valuable and effective α-LA is in the nervous system; still, antioxidants such as α-LA are known to be beneficial for our health. The antioxidant properties of α-LA and its role in the synthesis of Vit E, C, and GSH make it an attractive therapeutic agent for various diseases, including neurodegenerative disorders, in the future. α-LA has been studied in different studies which involved the treatment of various neural-related diseases. Considering the inflammatory pathways activated in most neural diseases’ pathological processes, α-LA can be regarded as a possibly helpful treatment in neurodegenerative disorders. α-LA and DHLA play a crucial role in biological processes, such as regulating several gene transcriptions and modulating enzymes and chemokines. α-LA is a viable choice for reestablishing mitochondrial function, as it acts as a cofactor for mitochondrial enzymatic complexes—a critical mechanism for energy production and metabolic regulation—as well as directly scavenging ROS in neurodegeneration. α-LA inhibits inflammasomes in neural tissues by decreasing pro-inflammatory mediators such as IL-2, IFN-γ, and TNF-α and raising anti-inflammatory cytokines such as IL-10. α-LA regulates the transcription of nuclear factors Nrf2 and NF-κB in physiological processes. Thus, α-LA is an agent with multiple actions on the neuronal machinery, acting in several mechanisms involved in the pathology of neurodegenerative disorders. Preclinical studies showed that α-LA attenuates neurodegeneration by modulating neuronal apoptotic pathways, supporting a neuroprotective role in Alzheimer’s, Ischemic injury, etc. Clinically, the use of α-LA in different trials highlighted that the administration of α-LA could significantly improve neurodegenerative-related disorders’ symptoms and slow down their deterioration. These characteristics make α-LA a viable supplement for treating neurodegenerative disorders as a therapeutic substitute. Therefore, α-LA can be shown as an effective therapeutic agent for neurodegenerative disorder therapy via different signaling pathways. α-LA appears to be a promising candidate for this type of multi-targeted therapy.
Availability of data and materials:
Not applicable.
Abbreviations
- α-LA:
-
Alpha lipoic acid
- PD:
-
Parkinson’s disease
- AD:
-
Alzheimer’s disease
- SCI:
-
spinal cord injury
- MDA:
-
Malondialdehyde
- TBARS:
-
Thiobarbituric acid reactive substances
- ROS:
-
Reactive oxygen species
- NOS:
-
Nitric oxide synthase
- MCAO:
-
Middle cerebral artery occlusion
- SOD:
-
Superoxide Dismutase
- ATP:
-
Adenosine triphosphate.
- CIRI:
-
Cerebral ischemia and reperfusion injury
- PGC1α:
-
Peroxisome proliferator-activated receptor-gamma coactivator
- MS:
-
Multiple sclerosis
- BBB:
-
Blood-brain barrier
- DHLA:
-
Dihydrolipoic acid
References
Park S, Karunakaran U, Ho Jeoung N, Jeon JH, Lee IK (2014) Physiological effect and therapeutic application of alpha lipoic acid. Curr Med Chem 21:3636–3645. doi: https://doi.org/10.2174/0929867321666140706141806
Gorąca A, Huk-Kolega H, Piechota A, Kleniewska P, Ciejka E, Skibska B (2011) Lipoic acid-biological activity and therapeutic potential. Pharmacol Rep 63:849–858. doi: https://doi.org/10.1016/s1734-1140(11)70600-4
Abdou RH, Abdel-Daim MM (2014) Alpha-lipoic acid improves acute deltamethrin-induced toxicity in rats. Can J Physiol Phar 92:773–779
Ferreira PM, Militão GC, Freitas RM (2009) Lipoic acid effects on lipid peroxidation level, superoxide dismutase activity and monoamines concentration in rat hippocampus. Neurosci Lett 464:131–134. doi: https://doi.org/10.1016/j.neulet.2009.08.051
Molz P, Schröder N (2017) Potential therapeutic effects of lipoic acid on memory deficits related to aging and neurodegeneration. Front pharmacol 8:849. doi: https://doi.org/10.3389/fphar.2017.00849
Kidd PM (2005) Neurodegeneration from mitochondrial insufficiency: nutrients, stem cells, growth factors, and prospects for brain rebuilding using integrative management. Altern Med Rev 10:268
Shay KP, Moreau RF, Smith EJ, Smith AR, Hagen TM (2009) Alpha-lipoic acid as a dietary supplement: molecular mechanisms and therapeutic potential. Biochim Biophys Acta Gen Subj 1790:1149–1160. doi: https://doi.org/10.1016/j.bbagen.2009.07.026
Salinthone S, Yadav V, Schillace RV, Bourdette DN, Carr DW (2010) Lipoic acid attenuates inflammation via cAMP and protein kinase A signaling. PLoS ONE 5:13058. https://doi.org/10.1371/journal.pone.0013058
Khan H, Gupta A, Singh TG, Kaur A (2021) Mechanistic insight on the role of leukotriene receptors in ischemic–reperfusion injury. Pharmacol Rep 1–15. doi: https://doi.org/10.1007/s43440-021-00258-8
Collins T, Read MA, Neish AS, Whitley MZ, Thanos D, Maniatis T (1995) Transcriptional regulation of endothelial cell adhesion molecules: NF-κB and cytokine‐inducible enhancers. FASEB J 9:899–909
Khan H, Sharma K, Kumar A, Kaur A, Singh TG (2022) Therapeutic implications of cyclooxygenase (COX) inhibitors in ischemic injury. Inflamm Res 17:1–6. https://doi.org/10.1007/s00011-022-01546-6
Zhang WJ, Frei B (2001) α-Lipoic acid inhibits TNF‐a‐induced NF‐κB activation and adhesion molecule expression in human aortic endothelial cells. FASEB J 15:2423–2432. doi: https://doi.org/10.1096/fj.01-0260com
White SW, Zheng J, Zhang YM, Rock CO (2005) The structural biology of type II fatty acid biosynthesis. Annu Rev Biochem 74:791–831. doi: https://doi.org/10.1146/annurev.biochem.74.082803.133524
Novotny L, Rauko P, Cojocel C (2008) alpha-Lipoic acid-the potential for use in cancer therapy Minireview. Neoplasma-Bratislava 55:81
Khan H, Garg N, Singh TG, Kaur A, Thapa K (2022) Calpain Inhibitors as Potential Therapeutic Modulators in Neurodegenerative Diseases. Neurochem Res 4:1–25. https://doi.org/10.1007/s11064-021-03521-9
Zhang H, Jia H, Liu J, Ao N, Yan B, Shen W, Wang X, Li X, Luo C, Liu J (2010) Combined R-α–lipoic acid and acetyl‐L‐carnitine exerts efficient preventative effects in a cellular model of Parkinson’s disease. J Cell Mol Med 14:215–225. doi: https://doi.org/10.1111/j.1582-4934.2008.00390.x
Grewal AK, Singh N, Singh TG (2019) Effects of resveratrol postconditioning on cerebral ischemia in mice: role of the sirtuin-1 pathway. Can J Physiol Pharmacol 97:1094–1101
Santos ÍM, Freitas RL, Saldanha GB, Tomé AD, Jordán J, Freitas RM (2010) Alterations on monoamines concentration in rat hippocampus produced by lipoic acid. Arq Neuropsiquiatr 68:362–366. https://doi.org/10.1590/S0004-282X2010000300006
Li DW, Li GR, Lu Y, Liu ZQ, Chang M, Yao M, Cheng W, Hu LS (2013) α-lipoic acid protects dopaminergic neurons against MPP+-induced apoptosis by attenuating reactive oxygen species formation. Int J Mol Med 32:108–114. doi: https://doi.org/10.3892/ijmm.2013.1361
Jalali-Nadoushan M, Roghani M (2013) Alpha-lipoic acid protects against 6-hydroxydopamine-induced neurotoxicity in a rat model of hemi-parkinsonism. Brain Res 1505:68–74. doi: https://doi.org/10.1016/j.brainres.2013.01.054
Karunakaran S, Diwakar L, Saeed U, Agarwal V, Ramakrishnan S, Iyengar S, Ravindranath V (2007) Activation of apoptosis signal regulating kinase 1 (ASK1) and translocation of death-associated protein, Daxx, in substantia nigra pars compacta in a mouse model of Parkinson’s disease: protection by α‐lipoic acid. FASEB J 21:2226–2236. doi: https://doi.org/10.1096/fj.06-7580com
Zhou L, Cheng Y (2019) Alpha-lipoic acid alleviated 6-OHDA-induced cell damage by inhibiting AMPK/mTOR mediated autophagy. Neuropharmacology 155:98–103
Zaitone SA, Abo-Elmatty DM, Shaalan AA (2012) Acetyl-L-carnitine and α-lipoic acid affect rotenone-induced damage in nigral dopaminergic neurons of rat brain, implication for Parkinson’s disease therapy. Pharmacol Biochem Behav 100:347–360. doi: https://doi.org/10.1016/j.pbb.2011.09.002
Li YH, He Q, Yu JZ, Liu CY, Feng L, Chai Z, Wang Q, Zhang HZ, Zhang GX, Xiao BG, Ma CG (2015) Lipoic acid protects dopaminergic neurons in LPS-induced Parkinson’s disease model. Metab Brain Dis 30:1217–1226. doi: https://doi.org/10.1007/s11011-015-9698-5
Irwin MH, Moos WH, Faller DV, Steliou K, Pinkert CA (2016) Epigenetic treatment of neurodegenerative disorders: Alzheimer and Parkinson diseases. Drug Dev Res 77:109–123. doi: https://doi.org/10.1002/ddr.21294
Sharma V, Kaur A, Singh TG (2020) Counteracting role of nuclear factor erythroid 2-related factor 2 pathway in Alzheimer’s disease. Biomed Pharmacother 129:110373. doi: https://doi.org/10.1016/j.biopha.2020.110373
Sharma VK, Singh TG, Mehta V (2021) Stressed mitochondria: a target to intrude alzheimer’s disease. Mitochondrion. https://doi.org/10.1016/j.mito.2021.04.004
Mancuso M, Coppede F, Migliore L, Siciliano G, Murri L (2006) Mitochondrial dysfunction, oxidative stress and neurodegeneration. J Alzheimer’s Dis 10:59–73. doi: https://doi.org/10.3233/jad-2006-10110
Nordberg A (1993) In Vivo Detection of Neurotransmitter Changes in Alzheimer’s Disease a. Ann. N. Y. Acad. Sci, 695:27–33. doi: https://doi.org/10.1111/j.1749-6632.1993.tb23022. x.
Kaur A, Anand C, Singh TG, Dhiman S, Babbar R (2019) Acetylcholinesterase inhibitors: a milestone to treat neurological disorders. Plant Arch 19:1347–1359
Zara S, De Colli M, Rapino M, Pacella S, Nasuti C, Sozio P, Di Stefano A, Cataldi A (2013) Ibuprofen and lipoic acid conjugate neuroprotective activity is mediated by Ngb/Akt intracellular signaling pathway in Alzheimer’s disease rat model. Gerontology 59:250–260. doi: https://doi.org/10.1159/000346445
Ooi L, Patel M, Muench G (2014) The thiol antioxidant lipoic acid and Alzheimer’s disease.Systems Biology of Free Radicals and Antioxidants2275–2288
Nietzel T, Mostertz J, Hochgräfe F, Schwarzländer M (2017) Redox regulation of mitochondrial proteins and proteomes by cysteine thiol switches. Mitochondrion 33:72–83. doi: https://doi.org/10.1016/j.mito.2016.07.010
Zhang YH, Yan XZ, Xu SF, Pang ZQ, Li LB, Yang Y, Fan YG, Wang Z, Yu X, Guo C, Ao Q (2020) α-Lipoic Acid Maintains Brain Glucose Metabolism via BDNF/TrkB/HIF-1α Signaling Pathway in P301S Mice. Front. Aging Neurosci 12:262. doi: https://doi.org/10.3389/fnagi.2020.00262
Ahmed HH (2012) Modulatory effects of vitamin E, acetyl-l-carnitine and α-lipoic acid on new potential biomarkers for Alzheimer’s disease in rat model. Exp Toxicol Pathol 64:549–556
Sancheti H, Akopian G, Yin F, Brinton RD, Walsh JP, Cadenas E (2013) Age-dependent modulation of synaptic plasticity and insulin mimetic effect of lipoic acid on a mouse model of Alzheimer’s disease. PLoS ONE 8:e69830. https://doi.org/10.1371/journal.pone.0069830
Khan H, Singh A, Thapa K, Garg N, Grewal AK, Singh TG (2021) Therapeutic modulation of the phosphatidylinositol 3-kinases (PI3K) pathway in cerebral ischemic injury. Brain Res 1761:147399. DOI: https://doi.org/10.1016/j.brainres.2021.147399
Ajith TA, Nima N, Veena RK, Janardhanan KK, Antonawich F (2014) Effect of palladium α-lipoic acid complex on energy in the brain mitochondria of aged rats. Altern Ther Health Med 20:27–35
Khan H, Grewal AK, Singh TG (2022) Pharmacological postconditioning by protocatechuic acid attenuates brain injury in ischemia-reperfusion (I/R) mice model: Implications of nuclear factor erythroid-2-related factor pathway. https://doi.org/10.1016/j.neuroscience.2022.03.016. Neuroscience
Abdel-Daim MM, El-Tawil OS, Bungau SG, Atanasov AG (2019) Applications of antioxidants in metabolic disorders and degenerative diseases: Mechanistic approach. Oxid. Med. Cell. Longev, 2019. https://doi.org/10.1155/2019/4179676
Khan H, Kashyap A, Kaur A, Singh TG (2020) Pharmacological postconditioning: a molecular aspect in ischemic injury. J Pharm Pharmacol 72:1513–1527. https://doi.org/10.1111/jphp.13336
Lv C, Maharjan S, Wang Q, Sun Y, Han X, Wang S, Mao Z, Xin Y, Zhang B (2017) α-Lipoic acid promotes neurological recovery after ischemic stroke by activating the Nrf2/HO-1 pathway to attenuate oxidative damage. Cell Physiol Biochem 43:1273–1287. doi: https://doi.org/10.1159/000481840
Zhang J, Xiao F, Zhang L, Wang X, Lai X, Shen Y, Zhang M, Zhou B, Lang H, Yu P, Hua F (2018) Alpha-lipoic acid preconditioning and ischaemic postconditioning synergistically protect rats from cerebral injury induced by ischemia and reperfusion partly via inhibition TLR4/MyD88/NF-κB signaling pathway. Cell Physiol Biochem 51:1448–1460. https://doi.org/10.1159/000495593
Grewal AK, Singh TG, Singh N (2020) Potential herbal drugs for ischemic stroke: a review. Plant Arch 20:3772–3783
Biewenga GP, Haenen GR, Bast A (1997) The pharmacology of the antioxidant lipoic acid. Gen Pharmacol-Vasc S 29:315–331. doi: https://doi.org/10.1016/s0306-3623(96)00474-0
Valko M, Leibfritz D, Moncol J, Cronin MT, Mazur M, Telser J (2005) Metals, toxicity and oxidative stress. Curr Med Chem 12:1161–1208. doi: https://doi.org/10.2174/0929867053764635
Dong Y, Wang H, Chen Z (2015) Alpha-lipoic acid attenuates cerebral ischemia and reperfusion injury via insulin receptor and PI3K/Akt-dependent inhibition of NADPH oxidase. Int J Endocrinol. doi: https://doi.org/10.1155/2015/903186
Sharma VK, Singh TG, Garg N, Dhiman S, Gupta S, Rahman M, Najda A, Walasek-Janusz M, Kamel M, Albadrani GM, Akhtar MF (2021) Dysbiosis and Alzheimer’s Disease: A Role for Chronic Stress?. Biomolecules 11:678. https://doi.org/10.3390/biom11050678
Guo S, Bragina O, Xu Y, Cao Z, Chen H, Zhou B, Morgan M, Lin Y, Jiang BH, Liu KJ, Shi H (2008) Glucose up-regulates HIF‐1α expression in primary cortical neurons in response to hypoxia through maintaining cellular redox status. J Neurochem 105:1849–1860. doi: https://doi.org/10.1111/j.1471-4159.2008.05287.x
Zhang L, qaing Xing G, Barker JL, Chang Y, Maric D, Ma W, Li BS, Rubinow DR (2001) α-Lipoic acid protects rat cortical neurons against cell death induced by amyloid and hydrogen peroxide through the Akt signalling pathway. Neurosci Lett 312:125–128. doi: https://doi.org/10.1016/s0304-3940(01)02205-4
Ma R, Wang X, Peng P, Xiong J, Dong H, Wang L, Ding Z (2016) α-Lipoic acid inhibits sevoflurane‐induced neuronal apoptosis through PI3K/Akt signalling pathway. Cell Biochem Funct 34:42–47. doi: https://doi.org/10.1002/cbf.3163
Choi KH, Park MS, Kim HS, Kim KT, Kim HS, Kim JT, Kim BC, Kim MK, Park JT, Cho KH (2015) Alpha-lipoic acid treatment is neurorestorative and promotes functional recovery after stroke in rats. Mol brain 8:1–16. doi: https://doi.org/10.1186/s13041-015-0101-6
Panigrahi M, Sadguna Y, Shivakumar BR, Kolluri SV, Roy S, Packer L, Ravindranath V (1996) α-Lipoic acid protects against reperfusion injury following cerebral ischemia in rats. Brain Res 717:184–188. doi: https://doi.org/10.1016/0006-8993(96)00009-1
Saklani P, Khan H, Gupta S, Kaur A, Singh TG (2022) Neuropeptides: Potential neuroprotective agents in ischemic injury. Life Sci 288:120186
Cao X, Phillis JW (1995) The free radical scavenger, α-lipoic acid, protects against cerebral ischemia-reperfusion injury in gerbils. Free Radic Res 23:365–370. doi: https://doi.org/10.3109/10715769509065257
Connell BJ, Saleh M, Khan BV, Saleh TM (2011) Lipoic acid protects against reperfusion injury in the early stages of cerebral ischemia. Brain Res 1375:128–136. doi: https://doi.org/10.1016/j.brainres.2010.12.045
Dos Santos SM, Romeiro CF, Rodrigues CA, Cerqueira AR, Monteiro MC (2019) Mitochondrial dysfunction and alpha-lipoic acid: Beneficial or harmful in Alzheimer’s disease? Oxid Med Cell Longev. doi: https://doi.org/10.1155/2019/8409329
Coles A, Alastair Compston A Coles (2008) Lancet 372:1502–1517. https://doi.org/10.1016/S0140-6736(08)61620-7
Friese MA, Schattling B, Fugger L (2014) Mechanisms of neurodegeneration and axonal dysfunction in multiple sclerosis. Nat Rev Neurol 10:225. doi: https://doi.org/10.1038/nrneurol.2014.37
Lassmann H (2013) Pathology and disease mechanisms in different stages of multiple sclerosis. J Neurol Sci 333:1–4. doi: https://doi.org/10.1016/j.jns.2013.05.010
Errea O, Moreno B, Gonzalez-Franquesa A, Garcia-Roves PM, Villoslada P (2015) The disruption of mitochondrial axonal transport is an early event in neuroinflammation. J Neuroinflammation 12:1–15
Bros H, Millward JM, Paul F, Niesner R, Infante-Duarte C (2014) Oxidative damage to mitochondria at the nodes of Ranvier precedes axon degeneration in ex vivo transected axons. Exp Neurol 261:127–135. DOI: https://doi.org/10.1016/j.expneurol.2014.06.018
El-Salem K, Al-Mistarehi AH, Khalil H, Al-Sharman A, Yassin A (2021) Serum Tumor Necrosis Factor-Alpha Levels Correlate with Cognitive Function Scales Scores in Multiple Sclerosis Patients. Mult Scler Relat Disord 47:102621. doi: https://doi.org/10.1016/j.msard.2020.102621
Haider L, Fischer MT, Frischer JM, Bauer J, Höftberger R, Botond G, Esterbauer H, Binder CJ, Witztum JL, Lassmann H (2011) Oxidative damage in multiple sclerosis lesions. Brain 134:1914–1924. doi: https://doi.org/10.1093/brain/awr128
González-González L, Pérez-Cortéz JG, Flores-Aldana M, Macías-Morales N, Hernández-Girón C (2015) Antioxidant use as dietary therapy in patients with multiple sclerosis. Medwave 15:e6065–e6065. doi: https://doi.org/10.5867/medwave.2015.01.6065
Thapa K, Khan H, Sharma U, Grewal AK, Singh TG (2020) Poly (ADP-ribose) polymerase-1 as a promising drug target for neurodegenerative diseases. Life Sci 118975. doi: https://doi.org/10.1016/j.lfs.2020.118975
Comabella M, Khoury SJ (2012) Immunopathogenesis of multiple sclerosis. Clin Immunol 142:2–8. doi: https://doi.org/10.1016/j.clim.2011.03.004
Kallaur AP, Reiche EM, Oliveira SR, Pereira WL, Alfieri DF, Flauzino T, de Meleck Proença C, Lozovoy MA, Kaimen-Maciel DR, Maes M (2017) Genetic, immune-inflammatory, and oxidative stress biomarkers as predictors for disability and disease progression in multiple sclerosis. Mol Neurobiol 54:31–44. doi: https://doi.org/10.1007/s12035-015-9648-6
Tully M, Shi R (2013) New insights in the pathogenesis of multiple sclerosis—role of acrolein in neuronal and myelin damage. Int J Mol Sci 14:20037–20047. doi: https://doi.org/10.3390/ijms141020037
Trapp BD, Ransohoff R, Rudick R (1999) Axonal pathology in multiple sclerosis: relationship to neurologic disability. Curr Opin Neurol 12:295–302. doi: https://doi.org/10.1097/00019052-199906000-00008
Smith KJ, Kapoor R, Felts PA (1999) Demyelination: the role of reactive oxygen and nitrogen species. Brain Pathol 9:69–92. doi: https://doi.org/10.1111/j.1750-3639.1999.tb00212.x
Waslo C, Bourdette D, Gray N, Wright K, Spain R (2019) Lipoic acid and other antioxidants as therapies for multiple sclerosis. Curr Treat Options Neurol 21:26. doi: https://doi.org/10.1007/s11940-019-0566-1
Yadav V, Marracci G, Lovera J, Woodward W, Bogardus K, Marquardt W, Shinto L, Morris C, Bourdette D (2005) Lipoic acid in multiple sclerosis: a pilot study. Mult Scler J 11:159–165. doi: https://doi.org/10.1191/1352458505ms1143oa
Chaudhary P, Marracci G, Yu X, Galipeau D, Morris B, Bourdette D (2011) Lipoic acid decreases inflammation and confers neuroprotection in experimental autoimmune optic neuritis. J Neuroimmunol 233:90–96. doi: https://doi.org/10.1016/j.jneuroim.2010.12.002
Minagar A, Alexander JS (2003) Blood-brain barrier disruption in multiple sclerosis. Mult Scler J 9:540–549. doi: https://doi.org/10.1191/1352458503ms965oa
Schreibelt G, Musters RJ, Reijerkerk A, de Groot LR, van der Pol SM, Hendrikx EM, Döpp ED, Dijkstra CD, Drukarch B, de Vries HE (2006) Lipoic acid affects cellular migration into the central nervous system and stabilizes blood-brain barrier integrity. J Immunol 177:2630–2637. doi: https://doi.org/10.4049/jimmunol.177.4.2630
Goel P, Jindal R, Singh T, Sharma S, Sharma P, Kaur H, Vohra K (2010) Focused Conference Group: Fc09-Inflammation And Immunopharmacology: New Tools For Old Diseases Role Of Ages Inhibitors In Inflammation And Rheumatoid Arthritis: Paper No.: 473. Basic Clin Pharmacol Toxicol 107:131–132
Goyal A, Kumar S, Nagpal M, Singh I, Arora S (2011) Potential of novel drug delivery systems for herbal drugs. Indian J Pharm Educ Res 45:225–235
Singh I, Rehni AK, Kalra R, Joshi G, Kumar M, Aboul-Enein HY (2007) Ion exchange resins: Drug delivery and therapeutic applications. Fabad J Pharm Sci 32:91
Dumont RJ, Verma S, Okonkwo DO, Hurlbert RJ, Boulos PT, Ellegala DB, Dumont AS (2001) Acute spinal cord injury, part I: pathophysiologic mechanisms. Clin Neuropharmacol 24:254–264. doi: https://doi.org/10.1097/00002826-200109000-00002
Bedreag OH, Rogobete AF, Sărăndan M, Cradigati A, Păpurică M, Roşu OM, Dumbuleu CM, Săndesc D (2014) Oxidative stress and antioxidant therapy in traumatic spinal cord injuries. Rom J Anaesth Intensive Care 21:123
Szabo TA, Warters RD, Kadry B, Stroud RE, Matthews RG, DeSantis SM, Spinale FG (2012) The effect of general vs spinal anesthesia on the inflammatory response in orthopedic surgery. cytokines, 6:11
Bains M, Hall ED (2012) Antioxidant therapies in traumatic brain and spinal cord injury. Biochim Biophys Acta Mol Basis Dis 1822:675–684. https://doi.org/10.1016/j.bbadis.2011.10.017
Hassler SN, Johnson KM, Hulsebosch CE (2014) Reactive oxygen species and lipid peroxidation inhibitors reduce mechanical sensitivity in a chronic neuropathic pain model of spinal cord injury in rats. J Neurochem 131:413–417. doi: https://doi.org/10.1111/jnc.12830
Slemmer JE, Shacka JJ, Sweeney MI, Weber JT (2008) Antioxidants and free radical scavengers for the treatment of stroke, traumatic brain injury and aging. Curr Med Chem 15:404–414. doi: https://doi.org/10.2174/092986708783497337
Liu W, Shi LJ, Li SG (2019) The immunomodulatory effect of alpha-lipoic acid in autoimmune diseases. Biomed Res Int. https://doi.org/10.1155/2019/8086257
Azbill RD, Mu X, Bruce-Keller AJ, Mattson MP, Springer JE (1997) Impaired mitochondrial function, oxidative stress and altered antioxidant enzyme activities following traumatic spinal cord injury. Brain Res 765:283–290. doi: https://doi.org/10.1016/s0006-8993(97)00573-8
Toklu HZ, Hakan T, Celik H, Biber N, Erzik C, Ogunc AV, Akakin D, Cikler E, Cetinel S, Ersahin M, Sener (2010) Neuroprotective effects of alpha-lipoic acid in experimental spinal cord injury in rats. J Spinal Cord Med 33:401–409. doi: https://doi.org/10.1080/10790268.2010.11689719
Taoka Y, Okajima K, Uchiba M, Johno M (2001) Methylprednisolone reduces spinal cord injury in rats without affecting tumor necrosis factor-α production. J Neurotrauma 18:533–543. https://doi.org/10.1089/089771501300227332
Tas N, Bakar B, Kasimcan MO, Gazyagci S, Ayva SK, Kılınc K, Evliyaoglu C (2010) Evaluation of protective effects of the alpha lipoic acid after spinal cord injury: An animal study. Injury 41:1068–1074. doi: https://doi.org/10.1016/j.injury.2010.05.027
Bernards CM, Akers T (2006) Effect of postinjury intravenous or intrathecal methylprednisolone on spinal cord excitatory amino-acid release, nitric oxide generation, PGE 2 synthesis, and myeloperoxidase content in a pig model of acute spinal cord injury. Spinal Cord 44:594–604. doi: https://doi.org/10.1038/sj.sc.3101891
Emmez H, Yildirim Z, Kale A, Tönge M, Durdağ E, Börcek A, Uçankuş LN, Doğulu F, Kiliç N, Baykaner MK (2010) Anti-apoptotic and neuroprotective effects of alpha-lipoic acid on spinal cord ischemia–reperfusion injury in rabbits. Acta Neurochir 152:1591–1601. doi: https://doi.org/10.1007/s00701-010-0703-9
Kumbasar U, Demirci H, Emmez G, Yıldırım Z, Gönül İI, Emmez H, Kaymaz M (2018) Protection from spinal cord ischemia-reperfusion damage with alpha-lipoic acid preconditioning in an animal model. Turk Gogus Kalp Damar Cerrahisi Derg 26:138. doi: https://doi.org/10.5606/tgkdc.dergisi.2018.14432
Marracci GH, Jones RE, McKeon GP, Bourdette DN (2002) Alpha lipoic acid inhibits T cell migration into the spinal cord and suppresses and treats experimental autoimmune encephalomyelitis. J Neuroimmunol 131:104–114. doi: https://doi.org/10.1016/s0165-5728(02)00269-2
Singh S, Singh TG, Rehni AK, Sharma V, Singh M, Kaur R (2021) Reviving Mitochondrial Bioenergetics: a relevant approach in epilepsy. Mitochondrion
Singh S, Singh TG, Rehni AK (2020) An Insight on Molecular Mechanisms & Novel Therapeutic Approaches in Epileptogenesis. CNS Neurol Disord - Drug Targets. doi: https://doi.org/10.2174/1871527319666200910153827
Trivedi P, Jena GB (2013) Role of α-lipoic acid in dextran sulfate sodium-induced ulcerative colitis in mice: studies on inflammation, oxidative stress, DNA damage and fibrosis. Food Chem Toxicol 59:339–355
Kim YS, Podder B, Song HY (2013) Cytoprotective effect of alpha-lipoic acid on paraquat-exposed human bronchial epithelial cells via activation of nuclear factor erythroid related factor-2 pathway. Biol Pharm Bull 36:802–811
Carmona-Aparicio L, Pérez-Cruz C, Zavala-Tecuapetla C, Granados-Rojas L, Rivera-Espinosa L, Montesinos-Correa H, Hernández-Damián J, Pedraza-Chaverri J, Sampieri A III, Coballase-Urrutia E, Cárdenas-Rodríguez N (2015) Overview of Nrf2 as therapeutic target in epilepsy. Int J Mol Sci 16:18348–18367. doi: https://doi.org/10.3390/ijms160818348
Liu Z, Yin X, Liu L, Tao H, Zhou H, Ma G, Cui L, Li Y, Zhang S, Yao L, Cai Z (2015) Association of KEAP1 and NFE2L2 polymorphisms with temporal lobe epilepsy and drug resistant epilepsy. Gene 571:231–236. doi: https://doi.org/10.1016/j.gene.2015.06.055
Nezu M, Suzuki N, Yamamoto M (2017) Targeting the KEAP1-NRF2 system to prevent kidney disease progression. Am J Nephrol 45:473–483. doi: https://doi.org/10.1159/000475890
Cheng Y, Luo F, Zhang Q, Sang Y, Chen X, Zhang L, Liu Y, Li X, Li J, Ding H, Mei Y (2018) α-Lipoic acid alleviates pentetrazol-induced neurological deficits and behavioral dysfunction in rats with seizures via an Nrf2 pathway. RSC Adv 8:4084–4092. doi: https://doi.org/10.1039/C7RA11491E
Poon HF, Farr SA, Thongboonkerd V, Lynn BC, Banks WA, Morley JE, Klein JB, Butterfield DA (2005) Proteomic analysis of specific brain proteins in aged SAMP8 mice treated with alpha-lipoic acid: implications for aging and age-related neurodegenerative disorders. Neurochem Int 46:159–168. doi:https://doi.org/10.1016/j.neuint.2004.07.008
Aluise CD, Robinson RA, Cai J, Pierce WM, Markesbery WR, Butterfield DA (2011) Redox proteomics analysis of brains from subjects with amnestic mild cognitive impairment compared to brains from subjects with preclinical Alzheimer’s disease: insights into memory loss in MCI. J Alzheimer’s Dis 23:257–269. doi: https://doi.org/10.3233/JAD-2010-101083
Bousette N, Gramolini AO, Kislinger T (2008) Proteomics-based investigations of animal models of disease. Proteom Clin Appl 2:638–653. doi: https://doi.org/10.1002/prca.200780043
Poon HF, Castegna A, Farr SA, Thongboonkerd V, Lynn BC, Banks WA, Morley JE, Klein JB, Butterfield DA (2004) Quantitative proteomics analysis of specific protein expression and oxidative modification in aged senescence-accelerated-prone 8 mice brain. Neuroscience 126:915–926. doi: https://doi.org/10.1016/j.neuroscience.2004.04.046
Ikegami S, Shumiya S, Kawamura H (1992) Age-related changes in radial-arm maze learning and basal forebrain cholinergic systems in senescence accelerated mice (SAM). Behav Brain Res 51:15–22. doi:https://doi.org/10.1016/S0166-4328(05)80307-9
Ebanks B, Ingram TL, Chakrabarti L (2020) ATP synthase and Alzheimer’s disease: Putting a spin on the mitochondrial hypothesis. Aging 12:16647. doi: https://doi.org/10.18632/aging.103867
Acknowledgements
The authors are grateful to the Chitkara College of Pharmacy, Chitkara University, Rajpura, Patiala, Punjab, India for providing the necessary facilities to carry out the research work.
Funding
Nil.
Author information
Authors and Affiliations
Contributions
Credit Author Statement:Conceptualization: Conceived and designed the experiments: Thakur Gurjeet Singh, Heena Khan, Randhir Singh. Analyzed the data: Heena Khan, Thakur Gurjeet Singh Wrote the manuscript: Heena Khan Editing of the Manuscript: Thakur Gurjeet Singh Critically reviewed the article: Randhir Singh, Thakur Gurjeet Singh Supervision: Thakur Gurjeet Singh, Mohamed M. Abdel-Daim.
Corresponding author
Ethics declarations
Ethics approval and consent to participate:
Not applicable.
Compliance with ethical standards
Not applicable.
Consent to participate:
Not applicable.
Conflict of interest
There are no conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Khan, H., Singh, T.G., Dahiya, R.S. et al. α-Lipoic Acid, an Organosulfur Biomolecule a Novel Therapeutic Agent for Neurodegenerative Disorders: An Mechanistic Perspective. Neurochem Res 47, 1853–1864 (2022). https://doi.org/10.1007/s11064-022-03598-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-022-03598-w