Abstract
Opioid analgesics devoid of central side effects are unmet medical need in the treatment of acute pain (e.g. post-operative pain). Recently, we have reported on 14-O-methylmorphine-6-O-sulfate (14-O-MeM6SU), a novel opioid agonist of high efficacy producing peripheral antinociception in subchronic inflammatory pain in certain doses. The present study focused on the antinociceptive effect of 14-O-MeM6SU compared to morphine in formalin test of an early/acute (Phase I) and late/tonic (Phase II) pain phases. Subcutaneous 14-O-MeM6SU (253–1012 nmol/kg) and morphine (3884–31075 nmol/kg) dose dependently reduced the pain behaviors of both phases. Co-administered naloxone methiodide (NAL-M), a peripherally acting opioid antagonist, abolished the antinociceptive effect of 506 nmol/kg 14-O-MeM6SU. On the other hand, the effects of 14-O-MeM6SU (1012 nmol/kg) and morphine (15538 nmol/kg) were only partially affected by NAL-M, indicating the contribution of CNS to antinociception. Locally injected test compounds into formalin treated paws caused antinociception in both phases. Locally effective doses of test compounds were also injected into contralateral paws. Morphine showed effects in both phases, 14-O-MeM6SU in certain doses failed to produce antinociception in either phase. A NAL-M reversible systemic dose of 14-O-MeM6SU and the lowest systemic effective dose of morphine were evaluated for their sedative effects following isoflurane-induced sleeping (righting reflex). In contrast to morphine, 14-O-MeM6SU in certain antinociceptive doses showed no impact on sleeping time. These data highlight that high efficacy opioids of limited CNS penetration in certain doses mitigate somatic and inflammatory pain by targeting MOR at the periphery.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The management of acute moderate to severe pain by opioids is satisfactory, however their central side effects limit their use, particularly dependence [1]. Beside the well-documented central component of analgesic opioid action, growing data support the involvement of peripheral opioid receptors in analgesia. For instance, lack of opioid antinociception following peripheral administration was reported in animals subjected to genetic ablation of opioid receptors in nociceptive sensory neurons [2]. In addition, acute and sub-chronic inflammatory pain responds well both to systemically and locally applied opioids [3,4,5,6]. In rodents, opioid receptors have been reported to be overexpressed at the peripheral and spinal level following inflammation. This histological feature supports the appearance of peripheral antinociceptive effect of opioids following local or systemic administration [6]. Nevertheless, the clinical practice lacks of peripherally acting opioid agonist against pain with proper efficacy, favorable side effect profile and duration of effect.
Recently, we have investigated the peripheral antinociceptive component of different peptide and novel nonpeptide opioids after systemic or local administration in acute (mouse and rat writhing test) and subchronic inflammatory rat model (Complete Freund’s adjuvant model). In these studies, we have shown that the peripheral opioid antinociception observed appears to be dependent on the pain model applied and the physiochemical properties of peripherally administered opioids [3, 4]. Opioid agonists have been reported to produce antinociception in both formalin-evoked pain phases, whereas non-steroidal anti-inflammatory drugs (NSAIDs) proved to inhibit only Phase II [7]. Peripherally acting µ-opioid agonist, loperamide has been proven to produce an antinociceptive effect in the formalin test following subcutaneous administration [8]. Of note this pain model has nociceptive responses evoked by continuous acute stimulus, which makes it of clinical relevance. Further, this model has two pain phases defined as Phase I and II. Phase I is initiated by a direct stimulation of nociceptors. On the other hand, Phase II develops parallel with inflammatory processes [9]. Opioid analgesics of limited central adverse effects appear to be more favorable than NSAIDs when the cardiac and gastrointestinal adverse effects are considered. Although 14-O-methylmorphine-6-O-sulfate (14-O-MeM6SU) showed peripheral analgesia in certain doses in our previous studies, in formalin test 14-O-MeM6SU has not been tested yet. Therefore, we decided to go on to collect further evidence on the analgesic effect of 14-O-MeM6SU to increase our understanding of peripheral antinociception.
In the present study we set out to examine the antinociceptive effect of the recently synthetized 14-O-MeM6SU compared to morphine in an acute inflammatory pain animal model (formalin test) to analyze the contribution of the peripheral versus central MOR to antinociception, following systemic or local administration.
The pain behaviors were evoked by intraplantar (i.pl.) formalin injection (modelling hyperalgesia). Finally, righting reflex was assessed to measure the sleeping time of inhaled isoflurane in the absence and presence of certain systemic doses of test compounds.
Materials and Methods
Animals
Male Wistar rats of (200–300 g) were used. The animals were obtained from the local Animal House (Semmelweis University, Budapest, Hungary). The animals were kept in standard cages (5 or 6 animals/cage) in a room of 20 ± 2 °C temperature, 12-h/12-h light/dark cycle, in the local animal house of the Semmelweis University, Department of Pharmacology and Pharmacotherapy (Budapest, Hungary). Water and standard food were available ad libitum.
All housing and experiments were performed in accordance with the European Communities Council Directives (2010/63/EU), and local animal care committee (PEI/001/276-4/2013). All the researchers did the best effort to minimize the number of animals and their suffering.
Chemicals
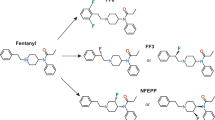
The morphine analog 14-O-MeM6SU (Fig. 1) was provided by the Department of Pharmaceutical Chemistry, Semmelweis University (Budapest, Hungary) and was synthesized and characterized as previously described [10]. Naloxone methiodide (NAL-M) and formalin solution was purchased from Sigma Aldrich Ltd. (Budapest, Hungary) and morphine hydrochloride from Alkaloida-ICN (Tiszavasvári, Hungary). Test compounds were dissolved in saline.
All compounds were stored and handled as described in the product information sheet.
Formalin Test: Model of Acute Inflammatory Pain
The test was performed as described previously [11]. Briefly, before the experiments the animals were daily wrapped in cloth except their right hindlimb left free, for three constitutive days (“handling)” in order to habituate them. Thereafter, animals were wrapped in cloth and 2.5% formalin solution was injected into the plantar surface of the right hind paw in a volume of 50 µl/rat. Immediately after the injection, animals were placed into Plexiglas observation chambers of 25, 25 and 25 cm in length, depth and height, respectively. The chambers were fixed above a mirror of 45° angle position allowing free viewing of the paws. Then, the antinociceptive action of the investigated agents were assessed by counting the number of nociceptive behaviors (shaking, flinching, licking and elevating the painful paw) for 60 min of 5 min time periods. Two observation phases were chosen (Phase I: 0–10 min and Phase II: 11–60 min) to determine the pain events.
The test compounds were injected subcutaneously (s.c.) (2.5 ml/kg) 15 min prior to formalin injection. NAL-M was s.c. co-administered with the test compounds. In the other set of experiments, the compounds were injected intraplantarly into the ipsilateral or contralateral paw (100 µl/animal) 5 min prior to the formalin solution injection. Researchers performing the experiments were blinded to the drugs applied.
Sleeping Time Measurement: “Righting Reflex” Method
The sleeping time was induced by inhaled 3% isoflurane in oxygen for 2 min with a 2 l/min flow rate via nose cone using a vaporizer (Eickemeyer Isoflo Vaporiser; Eickemeyer Veterinary Equipment Inc.). Thereafter, animals were immediately placed sideways on a pillow of 30 °C. The sleeping time (righting reflex, when the animals turned back on all four legs) was determined as previously described [4]. The animals were treated s.c. with 14-O-MeM6SU or morphine 60 or 30 min before inhaled anaesthetic, respectively. Control groups were treated with saline. The sleeping time was measured in seconds.
Statistical Analysis
Cumulated data of Phase I (0–10 min) and Phase II (11–60 min) was analyzed separately by one-way ANOVA followed by Fisher’s LSD post hoc test using the vehicle treated group as control.
Data obtained from the sleeping time measurement was analyzed with one-way ANOVA followed by Fisher’s LSD test. Results were considered statistically significant when P < 0.05. All the analysis was performed with a professional statistical software: GraphPad Prism 6.0 (GraphPad Software Inc., San Diego, CA).
Results
The Antinociceptive Effect of 14-O-MeM6SU and Morphine on Formalin Induced Pain After Systemic Administration
Subcutaneous 14-O-MeM6SU (253, 506 and 1012 nmol/kg) or morphine (3884, 7769, 15,538 and 31,075 nmol/kg) attenuated the formalin-induced pain in a dose-dependent manner (Fig. 2a, b).
The antinociceptive effect of 14-O-MeM6SU and morphine after s.c. administration in rat formalin test after i.pl. administration of 50 µl 2.5% formalin into the right hind paw. Phase I lasted for 0–10 min and Phase II for 11–60 min. Each column represents the cumulative data of the given phase (number of nociceptive reactions). Drugs were administered in a 2.5 ml/kg volume. Both compounds showed a dose dependent antinociceptive action. Each value represents the mean ± SEM. (n = 4–11). *: Significant difference versus vehicle treated group in Phase I, p < 0.05 (one-way ANOVA followed by Fisher’s LSD post hoc test). +: Significant difference versus vehicle treated group in Phase II, p < 0.05 (one-way ANOVA followed by Fisher’s LSD post hoc test)
When both phases are considered, 14-O-MeM6SU in doses 506 and 1012 nmol/kg produced antinociception (Fig. 2a), whereas 253 nmol/kg was effective only in the second phase. On the other hand, s.c. morphine caused antinociception in all tested doses in Phase I and apart from the lowest dose in Phase II (Fig. 2b).
The Antagonist Effect of Co-administered NAL-M on the Antinociceptive Effect of 14-O-MeM6SU and Morphine After Systemic Administration in Rat Formalin Test
NAL-M (10.6 µmol/kg, s.c.), peripherally acting opioid antagonist abolished the antinociceptive effect of s.c. 506 nmol/kg 14-O-MeM6SU in both phases (Fig. 3a). On the other hand, NAL-M failed to antagonize the effect of 1012 nmol/kg 14-O-MeM6SU in Phase I, yet partially affected the antinociceptive effect in Phase II (Fig. 3a).
The antagonist effect of s.c. co-administered NAL-M (10.6 µmol/kg) on the antinociceptive effect of s.c. 14-O-MeM6SU (a) and morphine (b) in rat formalin test. NAL-M completely antagonized the effect of 506 nmol/kg 14-O-MeM6SU and partially antagonized the effect of 1012 nmol/kg 14-O-MeM6SU and 15,538 nmol/kg morphine. Each column represents the cumulative data of the given phase (number of nociceptive reactions). Drugs were administered in a 2.5 ml/kg volume. Each value represents the mean ± SEM. (n = 5–11). *: Significant Difference versus vehicle treated group in Phase I, p < 0.05 (one-way ANOVA followed by Fisher’s LSD post hoc test). +: Significant difference versus vehicle treated group in Phase II, p < 0.05 (one-way ANOVA followed by Fisher’s LSD post hoc test). #: Significant difference between the signed groups, p < 0.05 (one-way ANOVA followed by Fisher’s LSD post hoc test)
In case of morphine, NAL-M antagonized its antinociceptive effect in the dose of (15,538 nmol/kg, s.c.) in Phase I (Fig. 3b). In Phase II NAL-M only partially antagonized the antinociceptive action of the same dose of morphine. These data indicate the peripheral antinociceptive component of both compounds, but only 14-O-MeM6SU showed action that was of completely peripheral origin at the dose of 506 nmol/kg.
The Antinociceptive Effect of 14-O-MeM6SU and Morphine on Formalin Induced Pain After Local Administration
The locally (i.pl.) administered (into the ipsilateral paw) 14-O-MeM6SU at doses of (25.3, 50.6 and 101.2 nmol/rat) or morphine (971 and 1942 nmol/rat) were also tested. The smallest dose that significantly reduced the pain in Phase I was 25.3 and 1942 nmol/animal for 14-O-MeM6SU and for morphine, respectively (Fig. 4a, b). When both phases considered, 14-O-MeM6SU alleviated the pain reactions in a dose of 50.6 nmol/rat and morphine only at the dose of 1942 nmol/rat (Fig. 4a, b). Based on equianalgesic effect 14-O-MeM6SU was 77 and 38 more potent than morphine in Phase I and II, respectively.
The antinociceptive effect of 14-O-MeM6SU and morphine after local administration in rat formalin test after i.pl. administration of 50 µl 2.5% formalin into the right hind paw. Phase I lasted for 0–10 min and Phase II for 11–60 min. Each column represents the cumulative data of the given phase (number of nociceptive reactions). Drugs were administered in a 100 µl/animal volume. Each value represents the mean ± SEM. (n = 4–11). *: Significant difference versus vehicle treated group in Phase I, p < 0.05 (one-way ANOVA followed by Fisher’s LSD post hoc test). +: Significant difference versus vehicle treated group in Phase II, p < 0.05 (one-way ANOVA followed by Fisher’s LSD post hoc test)
The Antinociceptive Effects of 14-O-MeM6SU or Morphine After Administration into the Contralateral Paw on Formalin-Induced Pain in Rats
Intraplantar (i.pl.) administration of 50.6 nmol/rat 14-O-MeM6SU into contralateral paw failed to affect formalin-induced pain in ipsilateral paw in either phases (Fig. 5a), though was effective when administered into ipsilateral (formalin treated) paw (Fig. 4). At a higher dose (101.2 nmol/rat) 14-O-MeM6SU showed antinociception only in Phase I. However, 1942 nmol/animal morphine injected into the contralateral paw (i.pl.) produced antinociceptive effect on both phases (Fig. 5b). This effect is in accordance with that obtained following s.c. 7769 nmol/kg (Fig. 2b).
The antinociceptive effect of 14-O-MeM6SU (a) and morphine (b) after administration into the contralateral paw. 14-O-MeM6SU did not show any effect in small dose (50.6 nmol/kg) while morphine showed significant antinociceptive effect in the smallest dose which was effective after local administration (1942 nmol/kg). Drugs were administered in a 100 µl/animal volume. Each column represents the cumulative data of the given phase (number of nociceptive reactions). Each value represents the mean ± SEM. (n = 4–5). *: Significant difference versus vehicle treated group in Phase I, p < 0.05 (one-way ANOVA followed by Fisher’s LSD hoc test in the case of 14-O-MeM6SU and unpaired t-test with two-tailed p value in the case of morphine). +: Significant difference versus vehicle treated group in Phase II, p < 0.05 (Unpaired t-test with two-tailed p value)
The Effect of Systemic 14-O-MeM6SU and Morphine on Isoflurane Induced Sleeping
We examined the impact of 14-O-MeM6SU and morphine on rat sleeping time initiated by inhaled isoflurane. Subcutaneous 506 nmol/kg but not 1012 nmol/kg failed to affect the sleeping time in rats evoked by inhaled isoflurane (Fig. 6a). Morphine significantly prolonged the rat sleeping time in a dose of 7769 and 15,538 nmol/kg (Fig. 6b). Longer sleeping time evoked by test compounds compared to saline, indicates the CNS effects (sedation).
Sleeping time of animals anaesthetized with inhaled isoflurane. 14-O-MeM6SU in 506 nmol/kg dose (effective dose in rat formalin test) did not influence the sleeping time. In a dose of 1012 nmol/kg and morphine in a 7769 nmol/kg dose significantly elevated the sleeping time (s). Data were obtained 60 min after the injection of 14-O-MeM6SU and 30 min in the case of morphine injection (times of peak effect). Drugs were administered in a 2.5 ml/kg volume. Each value represents the mean ± SEM. (n = 4–10). *: Significant difference versus saline treated control group p < 0.05 (one way ANOVA followed by Fisher’s LSD post hoc test)
Discussion
In the current study, we present for the first time the peripheral and central antinociceptive component of the novel non-peptide opioid agonist 14-O-MeM6SU compared to morphine following systemic or local administration in nociceptive assay modelling both the chemical (somatic) and inflammatory pain types (formalin test). There is no debate on the antinociceptive action of opioids following systemic administration in the treatment of moderate to severe pain, yet the adverse effects hamper their use [1]. However, to the best of our knowledge the clinical practice lacks of opioid agonists having peripheral antinociceptive effect without the unwanted central effects (e.g. respiratory depression, dependence).
The majority of opioids available for clinical use produce their analgesic effects by activation of central MOR. These receptors in addition to their presence in CNS pain transmission relay points, can be also found on the peripheral primary sensory neurons (DRG and peripheral terminals) [12]. Thus the presence of peripheral MOR is a motive for opioid researchers to localize the analgesic action of opioids following systemic administration, particularly those having chemical structure limiting their access to CNS [6]. During inflammation the elevated level of the opioid receptors on the periphery as well as in the CNS might offer a desirable option in the treatment of acute inflammatory pain [4, 13]. In this study, we determined the peripheral and central analgesic components of the novel compound 14-O-MeM6SU compared to that of morphine in nociceptive assay modelling both the chemical (somatic) and inflammatory pain types (formalin test). Finally, we evaluated the sedative effects of test compounds applying the rat righting reflex test. The main finding of the present study is that 14-O-MeM6SU and morphine alleviated the pain following either systemic or local administration in formalin test. 14-O-MeM6SU but not morphine showed pure peripheral analgesic component only in certain doses. It can be concluded from the antagonist effect of systemic NAL-M (in a dose proved to have only peripheral impact) on certain antinociceptive doses of 14-O-MeM6SU [14, 15]. Indeed, the peripheral analgesic effect of 14-O-MeM6SU was dose dependent, which did not occur in the case of morphine. Morphine in systemic dose of 15,538 nmol/kg displayed central and peripheral analgesia, since systemic NAL-M did only partially affect it. This dual site of analgesic effect for morphine was shown in the mouse tail-flick test (thermal nociception) as well [16]. Although NAL-M significantly decreased the analgesic effect of morphine, but was not capable to abolish it indicating the contribution of CNS to the action of morphine (Fig. 3). This result is in accordance with our previous data showing similar morphine analgesic tendency utilizing the same method—though the dose of morphine was smaller (5278 nmol/kg) [5]. On the other side, NAL-M failed to reverse the analgesic effect of 14-O-MeM6SU when was tested in higher doses. Taken together, 14-O-MeM6SU but not morphine at certain doses showed peripheral analgesia (Fig. 3). These results further support the hypothesis that inflammatory pain can be alleviated satisfactorily through peripheral opioid receptor activation as previously reported in other inflammatory pain models [3, 4]. In addition, in certain doses 14-O-MeM6SU but not morphine showed no analgesia, when they were administered into the contralateral paw (Fig. 5). This result might indicate that this dose is too small to have action on the other paw (ipsilateral paw). If we accept that this dose shows analgesic action when administered to the ipsilateral paw, then we could conclude that the site of hitting the pain is in the periphery for 14-O-MeM6SU in the dose of 50.6 nmol/rat. Our current results are in agreement with our previous results and other studies obtained in other inflammatory pain models [4, 12, 16,17,18]. Finally, since opioid agonists are known to induce sedation [19, 20], we tested the impact of certain analgesic doses of morphine or 14-O-MeM6SU in the sleeping time evoked by isoflurane, an inhaled anesthetic agent [21]. 14-O-MeM6SU in contrast to morphine in some analgesic doses failed to prolong the sleeping time of isoflurane (Fig. 6). Once again, this evidence shows that morphine in the dose of 7769 nmol/kg (smallest effective dose in both phases) prolonged isoflurane induced sleeping time, whereas 14-O-MeM6SU did not alter the sleeping time in the dose of 506 nmol/kg (Fig. 6) under the present circumstances. Of note, in our previous study, 14-O-MeM6SU in dose of 253 nmol/kg or higher did prolong thiobutabarbital-induced sleeping time [4]. Indeed, presently our explanation for this issue is based on pharmacokinetic properties because the two anesthetic agents have different route of administration and different sleeping induction property. Based on these apparent discrepancies it can be hypothesized that the thiobutabarbital-induced sleeping time measurement is more sensitive under the present circumstances to reveal mild sedative effects induced by low-dose of opioids. However, this needs to be elaborated in the future, but the substantial result regarding the analgesia of 14-O-MeM6SU in the present work remains clear because the systemic dose of 506 nmol/kg was antagonized by the peripherally acting opioid antagonist, NAL-M. Thus, 506 nmol/kg and lower doses showed prominent peripheral analgesia, whereas the higher doses produced peripheral and central analgesia regardless their impact on sleeping time evoked by anesthetics.
Our present results highlight the role of peripheral and central analgesic actions of test compounds pharmacologically only when applying behavioral animal models. Cellular mechanism-based methods assessing the role of opioid receptors located at the periphery and central pain pathway would provide further evidence on the contribution of the peripheral and central opioid receptors to the observed analgesia; yet understanding the mechanism behind. We hypothesize that opioids of high efficacy could effectively activate opioid receptors on the pain pathway at both peripheral and central sites. This pharmacological profile is hosted by 14-O-MeM6SU as described in previous studies [4, 10].
Based on these results agents with high efficacy and limited penetration into the CNS might be a preferable choice in the treatment of different types of inflammatory pain, considering proper dose titration. Therefore 14-O-MeM6SU and similar compounds might be of high clinical value, even after systemic administration especially in the cases of severe acute inflammatory conditions. In contrast to locally injected opioids systemic administration might offer a possibility to avoid the risk of infections and physical damages [22].
Conclusion
The knowledge on the type of pain and its pathophysiological changes is a milestone prior to prescribing effective analgesics. 14-O-MeM6SU but not morphine can produce peripheral antinociception in certain doses following local and particularly systemic administration. The later administration could offer a future tool to avoid the risk of infections and physical damages following local injection of opioids.
References
Chou R, Fanciullo GJ, Fine PG et al (2009) Clinical guidelines for the use of chronic opioid therapy in chronic noncancer pain. J Pain 10:113–130.e22. https://doi.org/10.1016/j.jpain.2008.10.008
Gaveriaux-Ruff C, Nozaki C, Nadal X et al (2011) Genetic ablation of delta opioid receptors in nociceptive sensory neurons increases chronic pain and abolishes opioid analgesia. Pain 152:1238–1248. https://doi.org/10.1016/j.pain.2010.12.031
Khalefa BI, Mousa SA, Shaqura M et al (2013) Peripheral antinociceptive efficacy and potency of a novel opioid compound 14-O-MeM6SU in comparison to known peptide and non-peptide opioid agonists in a rat model of inflammatory pain. Eur J Pharmacol 713:54–57. https://doi.org/10.1016/j.ejphar.2013.04.043
Lackó E, Riba PP, Giricz ZZ et al (2016) New morphine analogs produce peripheral antinociception within a certain dose range of their systemic administration. J Pharmacol Exp Ther 359:171–181. https://doi.org/10.1124/jpet.116.233551
Fürst S, Riba P, Friedmann T et al (2005) Peripheral versus central antinociceptive actions of 6-amino acid-substituted derivatives of 14-O-methyloxymorphone in acute and inflammatory pain in the rat. J Pharmacol Exp Ther 312:609–618. https://doi.org/10.1124/jpet.104.075176
Obara I, Parkitna JR, Korostynski M et al (2009) Local peripheral opioid effects and expression of opioid genes in the spinal cord and dorsal root ganglia in neuropathic and inflammatory pain. Pain 141:283–291. https://doi.org/10.1016/j.pain.2008.12.006
Jourdan D, Ardid D, Bardin L et al (1997) A new automated method of pain scoring in the formalin test in rats. Pain 71:265–270. https://doi.org/10.1016/S0304-3959(97)03366-6
Shannon HE, Lutz EA (2002) Comparison of the peripheral and central effects of the opioid agonists loperamide and morphine in the formalin test in rats. Neuropharmacology 42:253–261. https://doi.org/10.1016/S0028-3908(01)00173-3
Dubuisson D, Dennis SG (1977) The formalin test: a quantitative study of the analgesic effects of morphine, meperidine, and brain stem stimulation in rats and cats. Pain 4:161–174. https://doi.org/10.1016/0304-3959(77)90130-0
Lacko E, Varadi A, Rapavi R et al (2012) A novel µ-opioid receptor ligand with high in vitro and in vivo agonist efficacy. Curr Med Chem 19:4699–4707. https://doi.org/10.2174/092986712803306376
Coderre TJ, Yashpal K (1994) Intracellular messengers contributing to persistent nociception and hyperalgesia induced by L-glutamate and substance P in the rat formalin pain model. Eur J Neurosci 6:1328–1334. https://doi.org/10.1111/j.1460-9568.1994.tb00323.x
Rachinger-Adam B, Conzen P, Azad SC (2011) Pharmacology of peripheral opioid receptors. Curr Opin Anaesthesiol 24:408–413. https://doi.org/10.1097/ACO.0b013e32834873e5
Iwaszkiewicz KS, Schneider JJ, Hua S (2013) Targeting peripheral opioid receptors to promote analgesic and anti-inflammatory actions. Front Pharmacol 4:132. https://doi.org/10.3389/fphar.2013.00132
Lewanowitsch T, Irvine RJ (2002) Naloxone methiodide reverses opioid-induced respiratory depression and analgesia without withdrawal. Eur J Pharmacol 445:61–67. https://doi.org/10.1016/S0014-2999(02)01715-6
Bianchi G, Fiocchi R, Tavani A, Manara L (1982) Quaternary narcotic antagonists’ relative ability to prevent antinociception and gastrointestinal transit inhibition in morphine-treated rats as an index of peripheral selectivity. Life Sci 30:1875–1883. https://doi.org/10.1016/0024-3205(82)90467-2
Riba P, Ben Y, Nguyen T et al (2002) [Dmt1]DALDA is highly selective and potent at mu-opioid receptors, but is not cross-tolerant with systemic morphine. Curr Med Chem 9:31–39. https://doi.org/10.2174/0929867023371445
Khalefa BI, Shaqura M, Al-Khrasani M et al (2012) Relative contributions of peripheral versus supraspinal or spinal opioid receptors to the antinociception of systemic opioids. Eur J Pain 16:690–705. https://doi.org/10.1002/j.1532-2149.2011.00070.x
Janson W, Stein C (2003) Peripheral opioid analgesia. Curr Pharm Biotechnol 4:270–274. https://doi.org/10.2174/1389201033489766
McGuire JL, Awouters F, Niemegeers CJ (1978) Interaction of loperamide and diphenoxylate with ethanol and methohexital. Arch Int Pharmacodyn Ther 236:51–59
Craft RM, Leitl MD (2006) Potentiation of morphine antinociception by pentobarbital in female vs. male rats. Pain 121:115–125. https://doi.org/10.1016/j.pain.2005.12.009
Brohan J, Basavana G (2017) The role of GABA receptor agonists in anesthesia and sedation. CNS Drugs 31:845–856. https://doi.org/10.1007/s40263-017-0463-7
Stein C, Schäfer M, Machelska H (2003) Attacking pain at its source: new perspectives on opioids. Nat Med 9:1003–1008
Acknowledgements
The authors thank Semmelweis University Doctoral School (EFOP-3.6.3.-VEKOP-16-2017-00009) and Richter Gedeon Plc., Budapest, Hungary (Centenáriumi Alapítvány Research Grant) awarded to Dr. Mihály Balogh; ÚNKP-17-4 New National Excellence Program of the Ministry of Human Capacities (awarded to Dr. Zoltán S. Zádori).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Balogh, M., Zádori, Z.S., Lázár, B. et al. The Peripheral Versus Central Antinociception of a Novel Opioid Agonist: Acute Inflammatory Pain in Rats. Neurochem Res 43, 1250–1257 (2018). https://doi.org/10.1007/s11064-018-2542-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-018-2542-7