Abstract
Cisplatin is the most effective and neurotoxic platinum chemotherapeutic agent. It induces a peripheral neuropathy characterized by distal axonal degeneration that might progress to degeneration of cell bodies and apoptosis. Most symptoms occur nearby distal axonal branches and axonal degeneration might induce peripheral neuropathy regardless neuronal apoptosis. The toxic mechanism of cisplatin has been mainly associated with DNA damage, but cisplatin might also affect neurite outgrowth. Nevertheless, the neurotoxic mechanism of cisplatin remains unclear. We investigated the early effects of cisplatin on axonal plasticity by using non-cytotoxic concentrations of cisplatin and PC12 cells as a model of neurite outgrowth and differentiation. PC12 cells express NGF-receptors (trkA) and respond to NGF by forming neurites, branches and synaptic vesicles. For comparison, we used a neuronal model (SH-SY5Y cells) that does not express trkA nor responds to NGF. Cisplatin did not change NGF expression in PC12 cells and decreased neurite outgrowth in both models, suggesting a NGF/trkA independent mechanism. It also reduced axonal growth (GAP-43) and synaptic (synapsin I and synaptophysin) proteins in PC12 cells, without inducing mitochondrial damage or apoptosis. Therefore, cisplatin might affect axonal plasticity before DNA damage, NGF/trkA down-regulation, mitochondrial damage or neuronal apoptosis. This is the first study to show that neuroplasticity-related proteins might be early targets of the neurotoxic action of cisplatin and their role on cisplatin-induced peripheral neuropathy should be investigated in vivo.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cisplatin (cis-diamminedichloroplatinum II) is a highly-effective chemotherapeutic agent that is widely used, alone or combined with other agents, in the treatment of several types of cancer; however it induces severe dose-limiting toxicities including peripheral neurotoxicity [13, 30, 39]. Other platinum compounds also induce peripheral neurotoxicity, but cisplatin is the most neurotoxic among them [2]. The neurotoxicity of cisplatin is both cumulative and dose-dependent [27].
The symptoms of cisplatin-induced neurotoxicity are sensory-related and occur symmetrically in hands and feet, in a so-called “gloves-and-stocking” distribution [5, 30]. Symptoms include numbness, tingling, pins and needles, burning, decreased or increased sensitivity and pain [21]. There are no effective measures to prevent or treat the neurosensory damage induced by cisplatin and symptoms may persist even after treatment discontinuation; most patients improve over time, but the recovery might be incomplete [6, 17].
Cisplatin-induced neurotoxicity has been associated with damage of mitochondrial and genomic DNA, but the precise mechanism is not clear [7, 23, 32]. First, cisplatin causes a distal dying-back axonal degeneration that might progress to degeneration of cell bodies and apoptosis [3, 25]. It is possible that axonal degeneration induce peripheral neuropathy regardless loss of cell bodies. In fact, despite neuronal apoptosis, symptoms occur nearby distal axonal branches [34]. In this scenario, early mechanisms of axonal damage might be involved. In fact, a study showed that NGF inhibits cisplatin-induced neuronal apoptosis in vitro, without reducing DNA adduct formation [29]. Another study showed decreased levels of circulating NGF in patients treated with cisplatin and with neuropathic symptoms [31]. Additionally, it has been demonstrated that cisplatin inhibits neurite outgrowth in vitro [24], but the mechanism is unclear. Altogether, these findings suggest that cisplatin might affect NGF and axonal plasticity. The present study focus on these mechanisms of axonal damage that might involve NGF and neuroplasticity, but not necessarily DNA damage. The effects of cisplatin on neuroplasticity are unknown. We used a PC12-cell-neuronal model to address this issue.
PC12 are neuron-like cells that, when exposed to NGF, differentiate acquiring biochemical and morphological characteristics of sympathetic neurons [20]. They express NGF-high-affinity receptors (trkA) and respond to NGF by forming neurite extensions, branches and synaptic-like vesicles. Therefore, PC12 cells are a useful system to study the action of neurotoxic agents on neuronal differentiation and the involvement of NGF/trkA pathway [16, 20, 38].
Based on these premises, the present study investigates the effects of non-cytotoxic concentrations of cisplatin on axonal growth (GAP-43) and synaptic (synapsin I and synaptophysin) proteins, as well as in NGF expression in PC12 cells. We also evaluated neurite outgrowth in SH-SY5Y neuronal model, which has a different profile for neurotrophin receptors (trkB) and do not respond to NGF stimulation [22]. This is the first study to address neuroplasticity-related proteins as axonal targets of cisplatin.
Materials and Methods
Chemicals
Reagents were obtained from Sigma-Aldrich® (St. Louis, MO, USA), unless differently stated. Cell culture media were purchased from GIBCO®. Reagents for Western blot analysis were obtained from Bio-Rad Laboratories, Inc. (Hercules, CA, USA). Working concentrations of cisplatin were prepared in 0.9 % saline solution prior to assays. All solutions were prepared with ultra-pure water purified by a Milli-Q Gradient system (Millipore, Bedford, USA). In this study, high purity reagents were used (analytical grade minimum).
Cellular Cultures
PC12 and SH-SY5Y cells were obtained from the American Type Culture Collection, ATCC (Rockville, MD).
PC12 cells were maintained at 37 °C in humidified atmosphere containing 5 % CO2 and 95 % air. The medium used was Dulbecco’s Modified Eagle Medium (DMEM; GIBCO®) supplemented with 10 % heat-inactivated horse serum (GIBCO®), 5 % heat-inactivated fetal bovine serum (FBS; GIBCO®), and 1 % antibiotic mixture (5 mg/mL penicillin, 5 mg/mL streptomycin and 10 mg/mL neomycin, PNS GIBCO®). Medium was changed every 3 days. To harvest PC12 cells, medium was removed and cells were detached with trypsin/EDTA solution (GIBCO®). Trypsin was inactivated by the addition of supplemented medium and after centrifugation, cells were suspended in the growth medium and plated at the density required by each assay.
SH-SY5Y cells were grown in F12 nutrient mixture (F12 HAM; Sigma Cell Culture, St. Louis, MO) supplemented with 15 % fetal bovine serum (GIBCO) and 1 % PNS. Cells were cultured in 75 cm2 tissue-culture flasks at 37 °C under a humidified atmospheric condition of 5 % CO2 and 95 % air. Medium was replaced every day. Confluent cultures were detached with trypsin/EDTA solution (Gibco®), inactivated with growth medium, centrifuged, and subcultured (1:2; every 2–3 days). Third-passage cells with 80 % confluence were used in the experiments.
Determination of the Working Concentration of Cisplatin
PC12 cells (2.0 × 105 cells/well) were plated in 24-well plates coated with poly-l-lysine (Sigma-Aldrich®, St. Louis, MO, USA) and incubated for 24 h for better adhesion. After this period, the medium was replaced by F-12K Nutrient Mixture Kaighn’s Modification (GIBCO®) supplemented with 1 % horse serum, 1 % antibiotic mixture and NGF (100 ng/mL). Cells were treated with serial dilutions of cisplatin (1, 5, 10, 20, 50 and 100 μM), incubated for 24 or 72 h and tested for cell viability and neurite outgrowth, respectively. The tested range of concentrations were based on a previous related study [24]. The lowest concentration of cisplatin able to decrease the number of differentiated cells, without causing significant cytotoxicity was chosen as the working concentration.
Neurite Outgrowth Assays
PC12 cells (2.0 × 105 cells/well) were plated in 24-well, poly-l-lysine-coated microplates (Sigma-Aldrich®, St. Louis, MO, USA) and incubated for 24 h for adhesion. Then, medium was replaced by F-12K Nutrient Mixture Kaighn’s Modification (GIBCO®) supplemented with 1 % horse serum, 1 % antibiotic mixture and NGF (100 ng/mL). Cells were treated with cisplatin 5 μM and incubated for 72 h.
SH-SY5Y neuroblastoma cells were incubated in 24-well plates (3 × 104 cells/well) in F12 HAM supplemented with 15 % FBS and 1 % antibiotic mixture (penicillin/Streptomycin/Neomycin, PSN GIBCO®) for 24 h for adhesion. After this period, the medium was replaced (F12 HAM supplemented with 1 % FBS, 1 % PSN) and cells were incubated for 5 days, during which the medium was renewed every 2 days. Two different experimental conditions were analyzed: (i) simultaneous treatment with cisplatin and retinoic acid (RA), and (ii) 24 h-pretreatment with cisplatin before addition of RA. In the first condition, cells were simultaneously treated with RA 10 µM and cisplatin 5 µM and incubated for 5 days. In the second condition, cells were treated with cisplatin 5 µM for 24 h, then the medium was replaced (to remove cisplatin) prior to the addition of RA 10 µM and further incubation for 5 days. The removal of cisplatin allows to investigate if the possible effect of cisplatin would derive or not of the simple inactivation of RA by a direct reaction with cisplatin.
For both cell lines, the morphometric analysis was performed on the images obtained under inverted-phase-contrast microscopy (Carl Zeiss Axio Observer A1 inverted microscope, ×400 magnification), after incubation for 24, 48 and 72 h. Quantitation was performed by using the Image J Software [35]. Cells with at least one neurite with a length equal to (or higher than) the cell body diameter were considered as differentiated [11].
MTT Assay—Dose-Response Curve
The MTT assay is based on the conversion of MTT to formazan (purple) by mitochondrial dehydrogenases of viable cells [19]. An aliquot of 200 μL of cell suspension (2.0 × 104 cells/well) was incubated with different concentrations of cisplatin (1, 5, 10, 20, 50, 100, 200 μM) in 96-well microplates at 37 °C, for 24 h, in a humid atmosphere with 5 % of CO2. Then, plates were incubated with 20 µL of MTT solution (5 mg/mL) for 3 h at 37 °C. After that, plates were centrifuged (1000 rpm, 5 min), the supernatant was discarded and 200 µL of DMSO was added to solubilize formazan. The absorbance was measured at 570 nm on a microplate reader (Multiskan FC, Thermo Scientific).
LDH Release
PC12 cells (1.0 × 106 cell/well) were seeded in 12-well plates and incubated (at 37 °C, 5 % CO2) for 24 h before treatment. Then, cells were exposed to different concentrations of cisplatin (1, 5, 10, 20, 41.66, 83.33, 166.33, 333.33 µM) for 24 h and the medium was collected in order to analyze the level of cytoplasmic lactate dehydrogenase (LDH) released into the medium, a marker of membrane integrity loss. Determination of released LDH activity was performed according to the instructions of the manufacturer (Colorimetric Lactate Dehydrogenase Activity Assay Kit TOX7, Sigma-Aldrich®, St. Louis, MO, USA).
Caspase-3 Activity
An aliquot of 1 mL of cell suspension (1.0 × 107 cell/well) was incubated with cisplatin 5 µM in 6-well plates (at 37 °C, for 24 h). After that, medium was removed and cells were assayed for caspase-3 activity by using the Colorimetric Caspase 3 Assay Kit (Sigma-Aldrich®, St. Louis, MO, USA) according to the manufacturer’s instructions. The activity of caspase-3 was assessed by monitoring the absorbance at 405 nm.
Western Blot Analysis
Preparation of Cell Lysate
PC12 cells (2.0 × 105 cells/well) were plated in 24-well plates coated with poly-l-lysine (Sigma-Aldrich®, St. Louis, MO, USA) and treated as describe above “Neurite Outgrowth Assays”. After 72 h of incubation, cells were detached with trypsin, transferred to the microcentrifuge tubes and centrifuged (1000 rpm, 5 min, 4 °C). The supernatant was discarded and the cell pellet was suspended in 40 μL Tris-Triton lysis buffer (10 mM Tris, pH 7.4, 100 mM NaCl, 1 mM EDTA, 1 mM EGTA, Triton X-100 1 %, 10 % glycerol, 0.1 % SDS, 0.5 % deoxycholate, 1:200 Protease Inhibitor Cocktail and 1 % Phosphatase Inhibitor Cocktail). After 10 min, the cell lysate was centrifuged at 12,000 rpm for 10 min at 4 °C and the supernatant was stored in freezer (−80 °C) until the assay. A 10 µL aliquot of cell lysate was assayed for protein determination by the Bradford method.
Determination of Protein in Cell Lysate (Bradford)
The Protein Assay Dye Reagent (Bio-Rad) was used according to the manufacturer’s instructions. Lysates and color reagent were diluted with water (1:5) and a calibration curve of BSA (40, 100, 200 and 400 mg/mL) was used. The absorbance (595 nm) was determined in a microplate reader (Multiskan FC, Thermo Scientific) and the concentrations of protein were calculated based on the calibration curve response and multiplied by the dilution factor (5).
SDS-Polyacrylamide Gel Electrophoresis (SDS-PAGE)
Samples were added to an equal volume of Laemmli sample buffer (65.8 mM Tris, pH 6.8, 26.3 % glycerol, 2.1 % SDS, 0.01 % bromophenol blue, 5 % β-mercaptoethanol) and heated to 98 °C for 5 min. Aliquots of 35 μL containing 10 μg total protein were applied to 10 % polyacrylamide gel (10 wells) and separated by SDS-PAGE (1 h, 160 V, Tris/glycine/SDS buffer).
Transfer
Proteins were transferred to nitrocellulose membranes (1 h, 0.37 A, Tris/glycine buffer).
Immune Reaction
Membranes were blocked (30 min, RT, 300 rpm) with 5 % milk or BSA solution in Tween 20/TBS buffer (TTBS). The membranes were incubated with the primary antibodies: anti-GAP-43 (1:1250), anti-Synaptophysin (1:400) or anti-Synapsin I (1:1000) overnight at 4 °C, 300 rpm. Then, the membranes were washed with TTBS and incubated (1h, RT, 300 rpm) with the secondary antibody conjugated with horseradish peroxidase (anti-mouse or anti-rabbit IgG—HRP. 1:20,000). The membranes were washed with TTBS and TBS and treated with 3 mL of chemiluminescence enhancer detection reagent (1:1) and images were captured by using ChemiDoc system (Bio-Rad Laboratories, Inc., Hercules, CA, USA). Quantitation was performed on the images based on the optical densitometry (OD) of the bands by using the open source software Image J software [35]. Finally, the membranes were stripped (2 % SDS, 62.5 mM Tris pH 6.8 and 100 mM mercaptoethanol) and reprobed for loading control with anti-β-actin (1:3000). OD values of GAP-43, synapsin I and synaptophysin bands were divided by the OD values of β-actin for normalization of the results [26].
Determination of NGF Expression
PC12 cells (2.0 × 105 cell/well) were plated in 24-well plates and incubated at 37 °C for 24 h prior to the following additions: cisplatin 5 µM, NGF 100 ng/mL (positive control). Untreated cells were used as negative control. Then cells were incubated at 37 °C for 72 h. After treatment, an aliquot of 100 µL of culture supernatant was analyzed by using Enzyme-Linked Immunosorbent Assay kit RAB0381 (Sigma-Aldrich®, St. Louis, MO, USA) as recommended by the manufacturer. The absorbance at 450 nm was determined in a microplate reader (Multiskan FC, Thermo Scientific).
Statistical Analysis
Data were expressed as means ± SEM. Statistical analysis was carried out by using One-way ANOVA (Analysis of Variance) for multiple comparison, followed by the Bonferroni post-test (GraphPad Prism Software, version 5.0 for Windows, San Diego, California, USA). Differences between pairs were analyzed by using the non-parametric Mann–Whitney test. Values of p < 0.05 were considered significant. Experiments were repeated three times using cell cultures from different days. The experiment of each day was performed in triplicate.
Results
Effect of Cisplatin on the Differentiation of PC12 Cells
No significant difference was observed on the differentiation of cells treated with 1 μM cisplatin (6.07 %) in relation to control (6.43 %). Decreased percentage of differentiated cells was observed in cells treated with 5 μM cisplatin (4.33 ± 0.22 %), 10 μM cisplatin (4.24 ± 0.18 %) and 20 μM (1.72 ± 0.49 %) as compared to control; higher concentrations of cisplatin (50 and 100 μM) completely blocked cell differentiation (Fig. 1a). Figure 1b shows the morphological changes between the control and cells treated with 5 µM cisplatin, after 72 h of incubation. Cells in the control have large, square-shaped bodies and form more neurite extensions, while cells exposed to 5 μM cisplatin are mostly spherical and have fewer neurites as compared to the control.
Effect of different concentrations of cisplatin on the differentiation of PC12 cells after 72 h-incubation. Additions: NGF 100 ng/mL; cisplatin (100-5 serial dilution except 1 µM). a Bar graph. Each bar represents the mean ± SEM obtained from three independent experiments; each experiment was performed in triplicates. #Significantly different from the control group (p < 0.05). Cisplatin 1 µM had no effect, cisplatin (5–20 µM) significantly decreased differentiation and cisplatin (50 and 100 µM) completely blocked cell differentiation in relation to the control. b Photomicrographs showing the morphological changes of PC12 cells in control and in the group treated with 5 μM cisplatin, after 72 h of incubation. Cells in the control are square-shaped, larger and have more neurite extensions than cells exposed to 5 μM cisplatin (spherical-shaped)
Cytotoxicity of Cisplatin
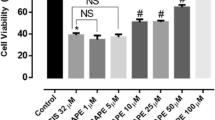
As shown in Fig. 2a (MTT assay), no significant reduction in the mitochondrial activity was observed in cells treated with 1 μM (94.86 ± 2.12 %), 5 μM (93.84 ± 2.10 %) or 10 μM (90.86 ± 1.42 %) of cisplatin. When cells were exposed to 20 μM of cisplatin (76.53 ± 1.50 %) or higher concentrations such as 50 μM (54.24 ± 1.83 %), 100 μM (52.78 ± 2.39 %) and 200 μM (43.13 ± 2.66 %), the viability of PC12 cells decreased significantly as compared to control (101.8 ± 2.55 %).
Cytotoxicity of different concentrations of cisplatin after 24 h-incubation. a MTT reduction assay: bar graph. b Dose-response curve: non-linear curve of the cellular viability (%) versus log of cisplatin concentrations. Equation: [Y = 100/(1 + 10^(LogIC50-X) × hillslope], in which hillslope is −1.682 and LogIC50 is 1.509. The calculated IC50 is 32.27 µM. c LDH assay: results are presented as means ± SEM obtained from three independent experiments; each experiment was performed in triplicate. Controls were normalized to 100 %. *Significantly different from the control group (p < 0.05). The mitochondrial toxicity of cisplatin started at 20 µM as shown by the MTT assay, whereas membrane integrity loss started at 167 µM as shown by the LDH release assay
The non-linear curve of the cellular viability (%) versus log of cisplatin concentrations is presented in Fig. 2b. The absorbance from MTT assay was normalized (0−100 % range) and the concentrations of cisplatin were transformed into the corresponding logarithm. IC50 (32.27 µM) was calculated by using the following equation: Y = 100/(1 + 10^(LogIC50-X) × hillslope).
The viability of PC12 cells exposed to serial dilutions of cisplatin was also assessed by monitoring of the release of the cytosolic enzyme LDH, which indicates loss of the integrity of the cytoplasmic membrane. Only the two highest concentrations of cisplatin (166 and 333 µM) significantly increased the release of LDH as compared to control.
Based on the neurite outgrowth (Fig. 1) and cytotoxicity (Fig. 2) assays, the working concentration of cisplatin (5 µM) was chosen. This was the lowest concentration of cisplatin that significantly decreased cell differentiation without causing significant cytotoxicity.
Effect of Cisplatin on Caspase-3 Activity
Cisplatin 5 μM (0.16 ± 0.014) did not alter the activity of caspase-3 as compared to control (0.14 ± 0.014) (Fig. 3).
Effect of Cisplatin 5 µM on the Differentiation of Retinoic-Acid-Stimulated SH-SY5Y Neuroblastoma Cells
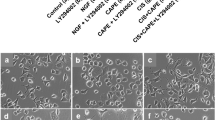
Retinoic acid increased the percentage of differentiated cells as compared to controls in all periods of incubation. When cells were incubated simultaneously with RA 10 µM and CIS 5 µM, the percentage of differentiated cells were reduced (Fig. 4). Figure 4f shows the increased neurite outgrowth and the morphological changes in cells treated with RA and the partial inhibition of these effects in cells treated simultaneously with cisplatin and RA.
Effect of cisplatin on the differentiation of SH-SY5Y cells after simultaneous addition of cisplatin 5 µM and retinoic acid (RA) 10 µM, and incubation for different periods: a 24, b 48, c 72, d 96 and e 120 h of incubation. Simultaneous treatment with 10 µM RA and 5 µM cisplatin reduced the percentage of differentiated cells in all periods of incubation. Bars represent means ± SEM of three independent experiments; each experiment was performed in triplicate. *Significantly different from control (p < 0.05); #significantly different from RA 10 µM (p < 0.05). f Phase-contrast photomicrographs after 120 h of incubation
Pretreatment with RA and cisplatin 5 µM reduced the percentage of differentiated cells in all periods of incubation (Fig. 5). Figure 5f shows the increased neurite outgrowth and the morphological changes induced by RA and the partial inhibition of this effect in cells treated with cisplatin prior to the addition of RA.
Effect of pretreatment with cisplatin 5 µM on the differentiation of SH-SY5Y cells stimulated with retinoic acid (RA) 10 µM. Periods of incubation: a CIS +RA 24, b 48, c 72, d 96 and e 120 h. Treatment with 5 µM cisplatin prior to treatment with RA reduced the percentage of differentiated cells in all periods of incubation. Bars represent means ± SEM of three independent experiments; each experiment was performed in triplicate. *Significantly different from control (p < 0.05); #significantly different from RA 10 µM (p < 0.05). f Phase-contrast photomicrographs after 120 h of incubation
Effect of Cisplatin on the Expression of GAP-43, Synapsin I and Synaptophysin
Cisplatin 5 μM reduced the expression of GAP-43 (1.06 ± 0.16), synapsin I (1.14 ± 0.06) and synaptophysin (1.11 ± 0.18) as compared to control (2.17 ± 0.33; 2.02 ± 0.21; 2.39 ± 0.33, respectively). Results are presented in Figs. 6, 7a, b and 8a, b, respectively.
Effect of cisplatin 5 µM on the expression of GAP-43. a Bar graph of the optical densitometry of the bands of GAP-43 normalized with β-actin (loading control). b Western blot bands. Cisplatin 5 μM reduced the expression of GAP-43 as compared to the control. Bars indicate means ± SEM of three independent experiments; each experiment was performed in triplicate. *Significantly different from control (p < 0.05)
Effect of cisplatin 5 µM on the expression of Synapsin I. a Bar graph of the optical densitometry of the bands of synapsin I normalized with β-actin (loading control). Cisplatin 5 μM reduced the expression of synapsin I as compared to the control. b Western blot bands. Bars indicate means ± SEM of three independent experiments; each experiment was performed in triplicate. *Significantly different from control (p < 0.05)
Effect of cisplatin 5 µM on the expression of Synaptophysin. a Bar graph of the optical densitometry of the bands of Synaptophysin normalized with β-actin (loading control). b Western blot bands. Cisplatin 5 μM reduced the expression of synaptophysin as compared to the control. Bars indicate means ± SEM of three independent experiments; each experiment was performed in triplicate. *Significantly different from control (p < 0.05)
Expression of NGF
Cisplatin 5 µM reduced the expression of NGF (0.018 ± 0.0019), but it was not significantly different from control (0.021 ± 0.0032) as depicted in Fig. 9.
Effects of cisplatin 5 µM on the expression of NGF in PC12 cells after 72 h of incubation. Cisplatin 5 µM decreased the expression of NGF but the difference was not significant. Bars indicate means ± SEM of three independent experiments; each experiment was performed in triplicate. No significant difference was observed between the groups
Discussion
Cisplatin-induced neurotoxicity has been associated with damage of mitochondrial and genomic DNA, but the precise mechanism is not clear [7, 23, 32]. Cisplatin causes a Wallerian-type axonal degeneration that precedes the neuronal apoptosis [21, 33]. Axons are very susceptible to the mitochondrial DNA damage induced by cisplatin [32], but cisplatin also seems to interfere with NGF and neurite outgrowth [24, 29, 31]. These findings suggest that cisplatin might impair axonal plasticity. The progression of cisplatin-induced neurotoxicity might have a similar time course observed in other neurotoxic processes, such as that induced by MPP+ (neurotoxin relevant to Parkinson’s disease), i.e., inhibition of differentiation occurs at early stages before death of neurons [14].
In order to address the early axonal damage induced by cisplatin, we evaluated the effects of a non-cytotoxic concentration (5 µM) of cisplatin on neurite outgrowth and on neurite-associated proteins (GAP-43; synapsin I and synaptophysin) in PC12 cells, widely used neuronal model to assess the outgrowth of neurites. Neurites are processes extended by cultured neurons or neuron-like cells upon trophic stimulation and they are precursors of axons and dendrites.
First, we selected the appropriate concentration of cisplatin by evaluating the effect of several concentrations on differentiation and viability of PC12 cells. Cisplatin (1 µM) was not cytotoxic nor affected neurite outgrowth. The lower non-cytotoxic concentration of cisplatin that significantly decreased neurite formation was 5 µM. Another study in PC12 reported the same effects at similar concentrations [24]. To evaluate cytotoxicity, we performed two well-known assays, MTT reduction and LDH release. MTT assay monitors mitochondrial function, while LDH assay monitors the integrity of cell membrane [28]. According to our results, cisplatin induced mitochondrial damage from 20 µM concentration (IC50 = 33 µM) and induced LDH release from 167 µM concentration. No mitochondrial damage was observed in cells treated with 5 µM cisplatin. Additionally, we addressed apoptosis by evaluating the effect of cisplatin 5 µM on the activity of caspase-3, the final executioner in the apoptotic cascade. No significant difference was observed in relation to control. Altogether, LDH, MTT, caspase-3 and neurite outgrowth assays clearly showed that the selected concentration (5 µM) of cisplatin does not cause mitochondrial damage, cell body loss or apoptosis. On the other hand, it significantly impaired the differentiation induced by NGF in PC12 cells. Therefore, this concentration was selected to assess the early neurotoxic events induced by cisplatin.
PC12 cells express NGF-high-affinity receptors (trkA) and differentiate in the presence of NGF [37]. In fact, PC12 cells constitutes a useful system for studying trkA function [38]. In order to evaluate the involvement of NGF/trkA pathway, we investigated changes in the expression of NGF in PC12 cells and additionally, we evaluated neurite outgrowth in a second neuronal model (SH-SY5Y cells) with a distinct phenotype for neurotrophin receptors. SH-SY5Y cells do not express trkA; therefore, they do not respond to NGF stimulation. On the other hand, they express functional trkB in the presence of RA, and differentiate in the presence of RA alone or combined with another neurotrophin, BDNF [22]. In SH-SY5Y cells, cisplatin decreased neuritogenesis in relation to control in both treatment protocols, i.e., (i) simultaneous treatment with cisplatin and RA, and (ii) 24 h-pretreatment and removal of cisplatin, which excludes the possibility of the inactivation of RA by cisplatin. These results also suggest that trkA receptors are not early targets of cisplatin, since cisplatin decreased neuritogenesis in both cell lines, PC12 and SH-SY5Y, regardless the expression of trkA receptors. It might occur later, but data on this issue are controversial. A study suggested that cisplatin decreases the expression of trkA receptors in sensory neurons [1]; whereas another study reported that no significant change was observed in the expression of mRNA for trkA in a rat model of peripheral neurotoxicity [8].
Additionally, cisplatin did not significantly change the expression of NGF in PC12 cells, which corroborates the results in SH-SY5Y cells, i.e., that the early neurotoxic effects of cisplatin are not mediated by the NGF/trkA pathway. On the other hand, studies have shown reduced levels of circulating NGF in rat models of peripheral neuropathy and in chemotherapy patients with neurological deficits [8, 12]. A study in mice showed that cisplatin reduced the levels of NGF in several peripheral NGF-producing tissues, and that administration of exogenous NGF restored the neurological deficits induced by cisplatin in these animals [1]. Altogether, the previous and present findings suggest that cisplatin might affect the synthesis and availability of NGF at later stages of the neurotoxic process, when the neurological deficits are already in course, but not at early stages. It is possible that down-regulation of NGF results from the action of cisplatin on DNA [1], an event that might occur after axonal damage. Another explanation is that peripheral NGF-producing tissues might be more susceptible to cisplatin-DNA binding than neurons [8] or neuronal models such as PC12 cells.
Although cisplatin seems not to decrease NGF at early stages, it is possible that neuroplasticity-related proteins are affected by cisplatin in a process not mediated by NGF. To investigate this hypothesis, we evaluated the effect of 5 µM cisplatin on the expression of three neuronal proteins related to axonal growth (GAP-43) and synaptic communication (Synapsin I and Synaptophysin) [11]. Cisplatin reduced the expression of these three proteins. The growth-associated protein GAP-43 is a protein that is preferentially distributed in the growth cone and elongating axon during development and regeneration of neurite network, and formation of new synapses [9]. Synapsin I and synaptophysin, are localized in the presynaptic membrane and are respectively used as molecular markers for nerve terminal maturation and synaptogenesis [11, 40]. Down-regulation of these proteins suggest that cisplatin is able to impair peripheral neuroplasticity before inducing neuronal apoptosis. There is no data about the effects of cisplatin on these proteins, except for one study [18] that showed up-regulation of mRNA for GAP-43 in peripheral neurons of rats treated with cisplatin; however, the effect occurred only after a cumulative dose of 14 mg/kg. One hypothesis for these opposing findings is that, at first, cisplatin would decrease neuroplasticity and later, after severe damage, neurons would respond by stimulating regenerative processes to increase the expression of the same proteins.
Little is known about the neuroplasticity of the peripheral system [15, 36] and about the effects of cisplatin on axonal proteins. The results of the present study suggest that the impairment of axonal plasticity by cisplatin might have implications on the development/progression of neuropathies. In vitro systems are rapid and reliable tools to investigate the potential neurotoxicity of chemicals as well as the molecular mechanisms responsible for it [4, 10]. However, it is important that the mechanisms and potential targets shown under the homogeneous and controlled environment of cell culture be complemented in vivo, under the variety of nerve cells, integrated functions and compensatory mechanisms. Further studies should investigate the effect of cisplatin on peripheral neuroplasticity in animal models.
Conclusion
Cisplatin has the potential to impair axonal growth and synaptic communication and it might occur before DNA damage, NGF/trkA down-regulation, mitochondrial damage, cell bodies loss and apoptosis. This is the first study to show that neuroplasticity-related proteins might be early targets of the neurotoxic action of cisplatin and their role on cisplatin-induced peripheral neuropathy should be investigated in vivo.
References
Aloe L, Manni L, Properzi F, De Santis S, Fiore M (2000) Evidence that nerve growth factor promotes the recovery of peripheral neuropathy induced in mice by cisplatin: behavioral, structural and biochemical analysis. Auton Neurosci 86(1–2):84–93. doi:10.1016/S1566-0702(00)00247-2
Amptoulach S, Tsavaris N (2011) Neurotoxicity caused by the treatment with platinum analogues. Chemother Res Pract 2011:843019. doi:10.1155/2011/843019
Asbury AK (1987) Sensory neuronopathy. Semin Neurol 7(1):58–66. doi:10.1055/s-2008-1041406
Bal-Price AK, Hogberg HT, Buzanska L, Coecke S (2010) Relevance of in vitro neurotoxicity testing for regulatory requirements: challenges to be considered. Neurotoxicol Teratol 32(1):36–41. doi:10.1016/j.ntt.2008.12.003
Brouwers EE, Huitema AD, Boogerd W, Beijnen JH, Schellens JH (2009) Persistent neuropathy after treatment with cisplatin and oxaliplatin. Acta Oncologica 48(6):832–841. doi:10.1080/02841860902806609
Carozzi VA, Canta A, Chiorazzi A (2015) Chemotherapy-induced peripheral neuropathy: what do we know about mechanisms? Neurosci Lett 596:90–107. doi:10.1016/j.neulet.2014.10.014
Carozzi VA, Marmiroli P, Cavaletti G (2010) The role of oxidative stress and anti-oxidant treatment in platinum-induced peripheral neurotoxicity. Curr Cancer Drug Targets 10(7):670–682
Cavaletti G, Pezzoni G, Pisano C et al (2002) Cisplatin-induced peripheral neurotoxicity in rats reduces the circulating levels of nerve growth factor. Neurosci Lett 322(2):103–106
Cho T, Tiffany-Castiglioni E (2004) Neurofilament 200 as an indicator of differences between mipafox and paraoxon sensitivity in Sy5Y neuroblastoma cells. J Toxicol Environ Health A 67(13):987–1000. doi:10.1080/15287390490447287
Costa LG, Giordano G, Guizzetti M (2011) In vitro neurotoxicology: an introduction. Methods Mol Biol 758:1–9. doi:10.1007/978-1-61779-170-3_1
Das KP, Freudenrich TM, Mundy WR (2004) Assessment of PC12 cell differentiation and neuritc growth: a comparison of morphological and neurochemical measures. Neurotoxicol Teratol 26(3):397–406. doi:10.1016/j.ntt.2004.02.006
De Santis S, Pace A, Bove L et al (2000) Patients treated with antitumor drugs displaying neurological deficits are characterized by a low circulating level of nerve growth factor. Clin Cancer Res 6(1):90–95
Decatris MP, Sundar S, O’Byrne KJ (2004) Platinum-based chemotherapy in metastatic breast cancer: current status. Cancer Treat Rev 30(1):53–81. doi:10.1016/S0305-7372(03)00139-7
dos Santos NA, Martins NM, Silva Rde B, Ferreira RS, Sisti FM, dos Santos AC (2014) Caffeic acid phenethyl ester (CAPE) protects PC12 cells from MPP+ toxicity by inducing the expression of neuron-typical proteins. Neurotoxicology 45:131–138. doi:10.1016/j.neuro.2014.09.007
Geuna S, Fornaro M, Raimondo S, Giacobini-Robecchi MG (2010) Plasticity and regeneration in the peripheral nervous system. Italian J Anat Embryol 115(1–2):91–94
Greene LA, Tischler AS (1976) Establishment of a noradrenergic clonal line of rat adrenal pheochromocytoma cells which respond to nerve growth factor. Proc Natl Acad Sci USA 73(7):2424–2428
Grothey A (2003) Oxaliplatin-safety profile: neurotoxicity. Semin Oncol 30(4 Suppl 15):5–13
Hamers FP, Plantinga LC, Verhaagen J, Neijt JP, Gispen WH (1996) Upregulation of B50/GAP-43 protein mRNA in rat dorsal root ganglia during cisplatin intoxication. J Neurosci Res 44(2):142–148. doi:10.1002/(SICI)1097-4547(19960415)44:2<142::AID-JNR6>3.0.CO;2-D
Hansen MB, Nielsen SE, Berg K (1989) Re-examination and further development of a precise and rapid dye method for measuring cell growth/cell kill. J Immunol Methods 119(2):203–210
Harrill JA, Mundy WR (2011) Quantitative assessment of neurite outgrowth in PC12 cells. In: Costa LG, Giordano G, Guizzetti M (eds) In vitro neurotoxicology: methods and protocols. Methods in molecular biology, vol 758. Humana Press, New York, pp 331–348
Hausheer FH, Schilsky RL, Bain S, Berghorn EJ, Lieberman F (2006) Diagnosis, management, and evaluation of chemotherapy-induced peripheral neuropathy. Semin Oncol 33(1):15–49. doi:10.1053/j.seminoncol.2005.12.010
Jamsa A, Hasslund K, Cowburn RF, Backstrom A, Vasange M (2004) The retinoic acid and brain-derived neurotrophic factor differentiated SH-SY5Y cell line as a model for Alzheimer’s disease-like tau phosphorylation. Biochem Biophys Res Commun 319(3):993–1000. doi:10.1016/j.bbrc.2004.05.075
Kelley MR, Jiang Y, Guo C, Reed A, Meng H, Vasko MR (2014) Role of the DNA base excision repair protein, APE1 in cisplatin, oxaliplatin, or carboplatin induced sensory neuropathy. PloS One 9(9):e106485. doi:10.1371/journal.pone.0106485
Klein R, Brown D, Turnley AM (2007) Phenoxodiol protects against Cisplatin induced neurite toxicity in a PC-12 cell model. BMC Neurosci 8:61. doi:10.1186/1471-2202-8-61
Krarup-Hansen A, Helweg-Larsen S, Schmalbruch H, Rorth M, Krarup C (2007) Neuronal involvement in cisplatin neuropathy: prospective clinical and neurophysiological studies. Brain 130(Pt 4):1076–1088. doi:10.1093/brain/awl356
L’Episcopo F, Serapide MF, Tirolo C et al (2011) A Wnt1 regulated Frizzled-1/beta-Catenin signaling pathway as a candidate regulatory circuit controlling mesencephalic dopaminergic neuron-astrocyte crosstalk: therapeutical relevance for neuron survival and neuroprotection. Mol Neurodegener 6:49. doi:10.1186/1750-1326-6-49
Lehky TJ, Leonard GD, Wilson RH, Grem JL, Floeter MK (2004) Oxaliplatin-induced neurotoxicity: acute hyperexcitability and chronic neuropathy. Muscle Nerve 29(3):387–392. doi:10.1002/mus.10559
Lobner D (2000) Comparison of the LDH and MTT assays for quantifying cell death: validity for neuronal apoptosis? J Neurosci Methods 96(2):147–152
McDonald ES, Randon KR, Knight A, Windebank AJ (2005) Cisplatin preferentially binds to DNA in dorsal root ganglion neurons in vitro and in vivo: a potential mechanism for neurotoxicity. Neurobiol Dis 18(2):305–313. doi:10.1016/j.nbd.2004.09.013
Park SB, Goldstein D, Krishnan AV et al (2013) Chemotherapy-induced peripheral neurotoxicity: a critical analysis. CA Cancer J Clin 63(6):419–437. doi:10.3322/caac.21204
Pisano C, Pratesi G, Laccabue D et al (2003) Paclitaxel and Cisplatin-induced neurotoxicity: a protective role of acetyl-l-carnitine. Clin Cancer Res 9(15):5756–5767
Podratz JL, Knight AM, Ta LE et al (2011) Cisplatin induced mitochondrial DNA damage in dorsal root ganglion neurons. Neurobiol Dis 41(3):661–668. doi:10.1016/j.nbd.2010.11.017
Quasthoff S, Hartung HP (2002) Chemotherapy-induced peripheral neuropathy. J Neurol 249(1):9–17
Raffa RB, Pergolizzi JV Jr (2013) Cancer chemotherapy-induced neuropathic pain. The underlying peripheral neuropathy. In: Raffa RB, Langford R, Joseph V, Pergolizzi J, Porreca F, Tallarida RJ (eds) Chemotherapy-induced neuropathic pain. CRC Press, Boca Raton, pp 113–135
Rasband WS (1997–2014) ImageJ, U.S. National Institutes of Health. Bethesda, Maryland, USA. http://imagej.nih.gov/ij/
Ray AL (2015) Neuroplasticity, sensitization, and pain In: Deer TR, Leong MS, Ray AL (eds) Treatment of chronic pain by integrative approaches. Springer, New York, pp 15–24
Slotkin TA, Seidler FJ (2010) Oxidative stress from diverse developmental neurotoxicants: antioxidants protect against lipid peroxidation without preventing cell loss. Neurotoxicol Teratol 32(2):124–131. doi:10.1016/j.ntt.2009.12.001
Tsoulfas P, Stephens RM, Kaplan DR, Parada LF (1996) TrkC isoforms with inserts in the kinase domain show impaired signaling responses. J Biol Chem 271(10):5691–5697
Wang D, Lippard SJ (2005) Cellular processing of platinum anticancer drugs. Nat Rev Drug Discov 4(4):307–320. doi:10.1038/nrd1691
Zhang W, Wang GM, Wang PJ, Zhang Q, Sha SH (2014) Effects of neural stem cells on synaptic proteins and memory in a mouse model of Alzheimer’s disease. J Neurosci Res 92(2):185–194. doi:10.1002/jnr.23299
Acknowledgments
The authors would like to thank CNPq (Conselho Nacional de Desenvolvimento Científico e Tecnológico) for the financial support (Grant Number 140106/2015-4).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ferreira, R.S., dos Santos, N.A.G., Martins, N.M. et al. Non-cytotoxic Concentration of Cisplatin Decreases Neuroplasticity-Related Proteins and Neurite Outgrowth Without Affecting the Expression of NGF in PC12 Cells. Neurochem Res 41, 2993–3003 (2016). https://doi.org/10.1007/s11064-016-2019-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-016-2019-5