Abstract
Background
Degenerative disc disease(DDD)is one of the most important causes of low back pain (LBP). Programmed death of human nucleus pulposus mesenchymal stem cells (NPMSCs) plays an important role in the progression of DDD. Growth differentiation factor-5 (GDF-5) is a protein that promotes chondrogenic differentiation, and has been reported to slow the expression of inflammatory factors in nucleus pulposus cells. Compared with those in normal rats, MRI T2-weighted images show hypointense in the central nucleus pulposus region of the intervertebral disc in GDF-5 knockout rats.
Methods and results
We aimed to evaluate the role of GDF-5 and Ras homolog family member A (RhoA) in NPMSCs. We used lipopolysaccharide (LPS) to simulate the inflammatory environment in degenerative disc disease, and performed related experiments on the effects of GDF-5 on NPMSCs, including the effects of pyroptosis, RhoA protein, and the expression of extracellular matrix components, and the effects of GDF-5, on NPMSCs. In addition, the effect of GDF-5 on chondroid differentiation of NPMSCs was included. The results showed that the addition of GDF-5 inhibited the LPS-induced pyroptosis of NPMSCs, and further analysis of its mechanism showed that this was achieved by activating the RhoA signaling pathway.
Conclusion
These findings suggest that GDF-5 plays an important role in inhibiting the pyroptosis of NPMSCs and GDF-5 may have potential for degenerative disc disease gene-targeted therapy in the future.
Highlights
Lipopolysaccharides can induce pyroptosis of NPMSCs.
We demonstrate that GDF-5 can alleviate LPS-induced pyroptosis of NPMSCs.
This is dependent on the activation of the RhoA signaling pathway.
GDF-5 can promote the chondrogenic differentiation of NPMSCs.
GDF-5 plays a pivotal role in protecting NPMSCs from pyroptosis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Many people experience low back pain (LBP) in their lifetime, and LBP brings a huge economic burden to society [1]. There are many factors that affect LBP, such as vertebral instability [2], muscle and soft tissue strain [3], and degenerative disc disease (DDD) [4, 5]. DDD is one of the main causes of LBP.The intervertebral disc is mainly composed of water-rich nucleus pulposus tissue, the outer annulus fibrosus, and a cartilage endplate [6], and maintains the biomechanics and stability of the spine [7,8,9]. Research on the mechanism of DDD has always been a hotspot in the field of spinal surgery. Such as pyroptosis [10,11,12,13] and mitochondrial dysfunction [14, 15]et al.
Pyroptosis is a newly discovered form of programmed death that has appeared in recent years. Its main features are the condensation of the nucleus, the random fragmentation and degradation of chromatin DNA, the appearance of numerous pores in the cell membrane, the loss of the cell membrane’s ability to regulate the entry and exit of substances, and the loss of internal and external cells. Upon ion balance, osmotic swelling occurs and the membrane ruptures, releasing active substances such as cell contents, stimulating the body’s immune response, and recruiting more inflammatory cells [16,17,18,19]. Compared with apoptosis, pyroptosis is a more complete and violent form of programmed death, and is closely related to the occurrence of intervertebral disc degenerative diseases [10, 11].
Ras homolog family member A (RhoA) belongs to the Ras homolog family protein and is a small GTPase [16]. RhoA plays an important role in regulating the cytoskeleton, maintaining cell shape, and promoting cell migration. Rho-associated coiled-coil kinase (ROCK) is a downstream effector protein of RhoA. The signaling pathway composed of RhoA and ROCK is involved in processes such as cell migration, cytoskeleton reorganization, and apoptosis, and remodeling in vivo [20,21,22,23]. Growth differentiation factor-5 (GDF-5), also known as cartilage-derived morphogenetic protein-1 (CDMP-1) or bone morphogenetic protein-14 (BMP-14), is a member of the TGF-β/BMP superfamily [24]. In recent years, there have been an increased number of studies on GDF-5 in the field of bone and joints, but there is no research report on the link between GDF-5 and NPMSCs pyroptosis. We aimed to determine the effect of GDF-5 on NPMSCs pyroptosis and explore the possible mechanism thereof.
Materials and methods
Isolation and culture of NPMSCs
Degenerative NP tissues were collected from patients undergoing surgery due to IVDD (male, 2; female, 2; age, 45–58 years, mean = 52.75 years; Pfirrmann level ≥ II).All experiments in this study were approved by the Ethics Committee of the Sixth Medical Center of PLA General Hospital(Approval number: HZKY-PJ-2021-35). Written informed consent was obtained from the donors of tissue samples used in this study.The study was performed according to the tenets of the 2013 Declaration of Helsinki.Disc specimens were collected during surgery and rinsed with 1% penicillin-streptomycin-containing PBS solution(GIBCO,USA) 3–5 times to wash away the blood stains on the surface and remove the excess cartilage on the surface and the surrounding annulus fibrosus. We used sterile ophthalmic scissors to cut the specimens into small pieces of 1 × 1 × 1 mm, and then centrifuged the pieces at 1,000 g for 5 min; the supernatant was discarded. We then added 0.2% collagenase type II solution (Sigma,USA) and placed the samples in a 37 °C 5% CO2 incubator(Thermo Fisher, USA) to digest for 4 h. After digestion, we centrifuged at 1,000 g for another 5 min, and carefully discarded the supernatant. We then used a DMEM/F12(GIBCO,USA) solution containing 10% fetal bovine serum (FBS)(GIBCO,USA), and placed the samples back into the incubator for culture and passage. The medium was changed every 2–3 days, and the cells were cultured to the P2 generation for subsequent experiments; the remaining cells were cryopreserved for later use.
Multilineage differentiation
For adipogenic differentiation, the cultured P2 generation NPMSCs were isolated, cultured, and inoculated into a six-well plate(Corning,USA) coated with gelatin solution in advance. The samples were cultured in adipogenic differentiation induction solution for three days, replaced with adipogenic differentiation induction solution B (Cyagen Biosciences,China) for 24 h, and then switched back to induction A solution(Cyagen Biosciences,China). When the cells appeared as obviously large lipid droplets, they were switched back to the induction B solution for 3–5 days. To end the culture, we fixed the cells with 4% neutral fixative (Solarbio,China) and then stained with Oil Red O(Solarbio,China) to observe the formation of lipid droplets.
For osteogenic differentiation, the cultured P2 generation NPMSCs were isolated, cultured, and inoculated in a six-well plate coated with gelatin solution in advance. A total of 2 ml of osteogenic differentiation induction medium(Cyagen Biosciences,China) was added to each well, and they were placed in a 37 °C 5% CO2 incubator for culture. The complete medium of mesenchymal stem cells was replaced every day and the culture was maintained for four weeks. After the induction culture, the cells were rinsed three times with PBS, fixed with 4% neutral fixative for 20 min, and washed another three times with PBS. We added alizarin red(Solarbio,China) staining solution for 15 min, discarded the alizarin red staining solution, washed the cells three times with PBS, and the cells were observed and photographed under a microscope.
For chondrogenic differentiation, we took the isolated and cultured P2 generation NPMSCs, centrifuged at 150 g for 5 min, inoculated in a 15 ml centrifuge tube(Corning,USA) at a density of 1 × 106, and again spun at 150 g for 5 min. A cell clump could clearly be seen at the bottom of the centrifuge tube. We carefully discarded the supernatant, slowly added chondrogenic differentiation complete induction medium(Cyagen Biosciences,China), unscrew the cap of the centrifuge tube, and gently placed the centrifuge tube in a 37 °C 5% CO2 incubator for static culture. After 24 h of induction and culture, we gently shook the bottom of the centrifuge tube to suspend the cell mass, and then put it back into the incubator for culture. Thereafter, fresh complete induction medium was replaced every two days. At the end of the induction culture, the medium supernatant was discarded, washed twice with PBS, fixed with 4% neutral fixative for 1 h, and the fixative was discarded. The cells were washed twice with PBS, dehydrated, embedded in paraffin, and sliced. The sections were then rehydrated and dewaxed, stained with Alcian blue(Solarbio,China) for 30 min, dehydrated and sealed with neutral gum, and observed under a microscope and photographed [25, 26].
Cell proliferation assay
A Cell Counting Kit-8 (CCK-8) (Dojindo, Japan) was used to examine the proliferation of NPMSCs cultured with different concentrations of GDF5(Proteintech,China). NPMSCs were seeded in 96-well plates(Corning,USA) at a density of 2 × 103/ml. These cells were cultured in eight groups (0, 1, 5, 10, 25, 50, 100 ug/ml) for 24, 48, and 72 h. The cells were incubated with 10 ul of CCK-8 reagent (Dojindo, Japan) in an incubator at 37 °C 5% CO2 for 2 h. The absorbance of the different groups was measured at 450 nm using a SpectraMax microplate reader(Thermo Fisher, USA) r\.
Quantitative real-time polymerase chain reaction (qPCR) analysis
After the cells were cultured in different concentrations of lipopolysaccharide(Sigma,USA) for 24 h, they were pretreated with 10 ug/ml lipopolysaccharide for 24 h, and 100 ng/ml GDF5 was added for 24 h. Then, total RNA was extracted with TRIzol reagent(Solarbio,China), and reverse transcribed into cDNA using reverse transcription reagent (TOYOBO, Japan). GAPDH served as an internal reference gene. The SYBR Premix Ex Taq PCR Kit (TOYOBO, Japan) and the LightCycler system (Roche, Switzerland) were used to analyze the obtained cDNA for real-time quantitative PCR (RT-qPCR). The primers used for RT-qPCR are listed in Table 1 and were synthesized by Sangon Biotech (Shanghai, China). The mRNA expression of target genes was calculated with the 2−ΔΔCt method.
Western blotting
Twenty-four hours after treatment with different concentrations of LPS, the cells were treated with RIPA lysis buffer (Solarbio, China), and total protein was extracted. The extracted samples of each group were separated by SDS-PAGE(Solarbio, China) and transferred to a PVDF membrane(Solarbio, China). Membranes were then blocked with 5% nonfat dry milk or 5% bovine serum albumin (BSA) for 1 h, and then incubated with primary antibodies (Table 2) overnight at 4 °C. The membranes were subsequently incubated with secondary antibodies (Solarbio, China), which were diluted with antibody diluent (Beyotime, China) for 1 h at room temperature. Immunolabeling was detected using ECL ultra-sensitive luminescent solution(Solarbio, China). The BioSpectrum gel imaging system (Bio Rad Laboratories, Inc.) was used, and Image J software was used to measure the gray value of the target band. GAPDH was used as the internal reference to record the gray value of the target protein. The ratio to GAPDH was relative to protein expression.
Histology and immunohistochemistry
The intervertebral disc tissues of patients with Pfirrmann grade II and Pfirrmann grade IV degeneration were routinely embedded in paraffin, deparaffinized, dehydrated, stained with hematoxylin (Beyotime China), and stained at room temperature for 3 min. The tissues were washed and differentiated in 1% acidic alcohol (Beyotime, China) for 30 s, stained with eosin (Beyotime China) for 2 min at room temperature, and observed under a light microscope (Olympus Corporation, Japan).
We took the Pfirrmann grade II intervertebral disc tissue and Pfirrmann grade IV intervertebral disc tissue isolated during the operation and sliced them. After deparaffinization, each section was incubated in 3% H2O2(Beyotime, China) for 10 min and washed with PBS. The sections were then incubated with 0.1% trypsin(Beyotime, China) for 20 min at 37 °C and washed with PBS. The sections were blocked with 1% goat serum albumin(Beyotime, China) for 1 h at 37 °C without washing with PBS, and then incubated overnight at 4 °C with primary antibodies against Collagen-II (1:200). The next day, the sections were rinsed twice with PBS and incubated with enzyme-conjugated secondary antibodies(Beyotime, China) for 1 h at room temperature. At least three sections of each sample were observed under a microscope (Olympus Corporation, Japan).
Statistical analysis
Measurement data are expressed as mean ± standard deviation, and data that did not conform to normal distribution are expressed as median and interquartile range. Significant differences between groups were analyzed by one-way ANOVA or nonparametric tests using SPSS 22.0 software. A p < 0.05 was considered statistically significant.
Results
NPMSCs isolation and identification
After 7–8 days of primary cell isolation and culture, a small amount of cells in the cell culture flask appeared to adhere to the wall and were spindle-shaped. The cells reached 30–40% fusion rate in approximately 12 days. At approximately 15 days, the adherent fusion rate of the cells reached 70%, the cells were passaged, and the subsequent cell growth accelerated. The P3 cells grew more regular and spindle-shaped (Fig. 1). The cultured cells had stemness. Oil red O staining revealed intracellular lipid droplet formation after 28 days of adipogenic differentiation. After 30 days of osteogenic culture, the formation of mineralized nodules was observed by alizarin red staining. After 28 days of chondrogenic differentiation and culture, Alcian blue staining showed the existence of sulfated proteoglycans in the chondrocytes (Fig. 1).
P3 generation cells are observed as a long spindle shape under a light microscope and Multilineage differentiation capacities of NPMSCs in vitro. (b) Oil Red O staining for adipogenic differentiation, (c) Alcian Blue staining for chondrogenic differentiation. (d) Alizarin red staining for osteogenic differentiation
HE staining and immunohistochemical analysis
HE staining confirmed that the nucleus pulposus of the intervertebral disc tissue derived from Pfirrmann grade II showed normal staining of extracellular matrix and normal morphology of the nucleus pulposus (Fig. 6a). In Pfirrmann grade IV intervertebral disc tissue, the normal shape of the nucleus pulposus disappeared and was replaced by thick fibrous tissue, showing obvious eosinophilia (Fig. 6b). Immunohistochemical analysis showed that the intervertebral disc tissue of Pfirrmann grade II highly expressed type II collagen (Fig. 6c), and the intervertebral disc tissue of Pfirrmann grade IV, had low expression of type II collagen (Fig. 6d). This suggests that the loss of extracellular matrix is more pronounced as disc degeneration becomes progressive.
Cell proliferation of NPMSCs
When the cells were cultured with GDF5 for 24 h, the proliferation ability of NPMSCs did not change significantly. When the cells in the treatment group were cultured with different concentrations of GDF-5 for 48 h, the cells proliferated slightly with the increase of GDF-5 concentration. When the cells were incubated with GDF-5 for 72 h, the proliferation rate of the cells slowed down and showed a slight inhibitory effect (Fig. 2).
NPMSCs proliferation assay (a) Compared with the pure cell controls in the 0 ng/ml GDF-5 group, the increase of the drug concentration had no significant effect on the OD value at 24 h. (b) Compared with the 0 ng/ml GDF-5 group, the OD value of the 1 ng/ml GDF-5 group, 5 ng/ml GDF-5 group, 25 ng/ml GDF-5 group, 50 ng/ml GDF-5 group, and 100 ng/ml GDF-5 group increased after 48 h. (c) Compared with the 0 ng/ml GDF-5 group, the OD value of the 5 ng/ml GDF-5 group and the 10 ng/ml GDF-5 group decreased after 72 h; in general, the changes in the OD value of the groups at 72 hours were not significant. (d) RT-qPCR showing that, compared with the control group, the expression of aggrecan in the 50 ug/ml LPS group and the 100 ug/ml group decreased; (e) and that, in the 1 ug/ml group, 5 ug/ml group, 10 ug/ml group, 25 ug/ml group, and 50 ug/ml group, the expression of IL-1β mRNA was significantly increased. *p<0.05; **p<0.01; ***p<0.001; ****p<0.0001
LPS promotes pyroptosis and inhibits RhoA activation in NPMSCs
To confirm the effect of LPS on the RhoA pathway, we performed related qPCR and WB experiments, measured the mRNA levels of IL-1β and the extracellular matrix composition of aggrecan and RhoA in each treatment group, and compared these with the control group. The IL-1β The expression level of -1β was significantly increased. The expression of aggrecan and RhoA mRNA was decreased (Fig. 2). We determined the protein expression level of Gasdermin-D (GSDMD) in each treatment group, and there was no statistical difference compared with the control group. By measuring the protein expression level of GSDMD active fragment N-terminal fragment of GSDMD (GSDMD-N), compared with the control group, its expression level showed a gradual upward trend. By measuring the protein expression level of the active form of caspase-1, Caspase1/p20/p10, it was found that its expression level gradually increased with the increase of LPS concentration (Fig. 3). This suggests that the nucleus pulposus mesenchymal stem cells undergo pyroptosis under the action of LPS. To further clarify the role of RhoA in the pyroptosis of nucleus pulposus mesenchymal stem cells, we measured the expression level of RhoA. With the increase of drug concentration in the treatment group, the expression level of RhoA gradually decreased. Therefore, we determined that RhoA signaling is in the nucleus pulposus. Mesenchymal stem cells were inhibited during pyroptosis (Fig. 4b).
Expression of pyroptosis-related proteins (b) Compared with the control group, the expression of GSDMD did not change significantly under the action of different concentrations of LPS. (c) However, when the LPS concentration was 10 ug/ml, 50 ug/ml, and 100 ug/ml, the expression of GSDMD-N protein was significantly increased. (d) The expression of Caspase1/p20/p10 increased when the LPS concentration reached 5 ug/ml. *p<0.05; **p<0.01; ***p<0.001
Expression of RhoA protein and effect of GDF-5 on gene expression of IL-1β, RhoA and Sox9. (b) Compared with the control group, the expression of RhoA Protein was significantly decreased when the LPS concentration was 5 ug/ml, 10 ug/ml, 50 ug/ml, and 100 ug/ml. (c) Compared with the control group, the expression of IL-1β mRNA increased in the LPS group.Compared with the LPS+GDF-5 group, the expression of IL-1β mRNA decreased. (d) Compared with the control group, the expression of RhoA mRNA decreased in the LPS group. Compared with the LPS+GDF-5 group, the expression of RhoA mRNA increased. (e) Compared with the control group, the expression of Sox-9 mRNA in the LPS group decreased. Compared with the LPS+GDF-5 group, the expression of Sox-9 mRNA increased. **p<0.01; ***p<0.001; ****p<0.0001
GDF5 inhibits pyroptosis of NPMSCs by activating the RhoA signaling pathway
To further elucidate the roles of GDF-5 and RhoA signaling pathways in the pyroptosis of NPMSCs, we measured the mRNA expression level of IL-1β, the mRNA and protein expression levels of Sox-9, and RhoA in each treatment group. We found that, after the NPMSCs were treated with 10 µg/ml LPS for 24 h, the expression level of IL-1β was significantly increased, and the expression levels of Sox-9 and RhoA were decreased (Fig. 4). This indicated that GDF-5 could inhibit the expression levels of pyroptosis-related genes in nucleus pulposus mesenchymal stem cells, and could up-regulate the mRNA and protein expression levels of Sox-9 and RhoA (Fig. 5b,c). To confirm the link between GDF-5 and RhoA, we measured the RhoA expression level in the treatment group by adding the RhoA signaling pathway specific inhibitor CCG-1423, and we found that, with the addition of GDF-5, the expression of RhoA increased. After adding 10 µmol/L CCG-1423, the expression level of RhoA decreased (Fig. 5f). This showed that GDF-5 inhibits pyroptosis of nucleus pulposus mesenchymal stem cells by mediating the activation of RhoA signaling pathway.
The effect of GDF-5 on the expression of RhoA and Sox9 protein, and the effect of inhibitor CCG-1423 on RhoA signaling pathway. (b) Compared with the control group, the expression of Sox-9 protein in the LPS group decreased. Compared with the LPS+GDF-5 group, the expression of Sox-9 protein increased. (c) Compared with the control group, the expression of RhoA protein decreased in the LPS group. Compared with the LPS+GDF-5 group, the expression of RhoA protein increased. (f) Compared with the control group, the expression of RhoA increased in the GDF-5 group. Compared with the GDF-5+CCG-1423 group, the expression of RhoA decreased. **p<0.01; ***p<0.001
GDF-5 promotes chondroid differentiation of nucleus pulposus tissue
Compared with the standard normalized chondrogenic differentiation medium added with TGF-β, there was no significant difference in the expression of sulfated proteoglycan in the GDF-5 group, indicating that GDF-5 has the effect of promoting the chondroid differentiation of NPMSCs (Fig. 6).
HE staining of intervertebral discs, immunohistochemistry and chondrogenic differentiation of NPMSCs. (a, b) Compared with the Pfirrmann grade II group, HE staining showed that, in the Pfirrmann grade IV group, the nucleus pulposus was morphologically disordered, replaced by thick fibrous tissue. Immunohistochemical analysis showing the Pfirrmann grade II group highly expressed type II collagen (c), and the Pfirrmann grade IV had low expression of type II collagen (d). Cartilage differentiation ability. Compared with the normal group, there was no significant difference in the expression of sulfated proteoglycan after Alcian blue staining in the GDF-5 group
Discussion
The addition of GDF-5 inhibited the LPS-induced pyroptosis of NPMSCs, and further analysis of its mechanism showed that this was achieved by activating the RhoA signaling pathway. This suggests that GDF-5 plays an important role in inhibiting the pyroptosis of NPMSCs and that GDF-5 may have potential for DDD gene-targeted therapy in the future.
DDD is one of the main causes of clinical low back pain, and the main pathophysiological basis of degenerative disc disease is disc degeneration. The occurrence of intervertebral disc degeneration is closely related to the programmed cell death of the nucleus pulposus. Studies have focused on the apoptosis of nucleus pulposus cells and the reduction of extracellular matrix water content. In this study, the biological properties of intervertebral disc-derived cells were discussed in depth, not limited to the traditional study of apoptosis, but from a newer form of death, pyroptosis.
Pyroptosis was first discovered in infectious Shigella flexneri [27]. Propionibacterium acnes (P. acnes) is a low-virulence anaerobic bacterium that, as a low-grade bacterium, usually lurks in non-purulent intervertebral discs. Studies have shown that P. acnes is associated with intervertebral disc degeneration (IVDD) and LBP [28,29,30,31]. However, it can upregulate a variety of inflammatory cytokines and, in acne vulgaris, the release of a large amount of IL-1β is the main pathogenesis. IL-1β is an expression product of pyroptosis and, we believe, P. acnes is closely related to pyroptosis. Recent studies have also found that P. acnes can activate pyroptosis-related pathways and cause IVDD [32,33,34]. A study has suggested CGAS-STING-NLRP3 axis and pyroptosis in the progression of IVDD, providing a promising treatment for disc-derived LBP [35]. In our study, a cell pyroptosis model was successfully established using a LPS concentration gradient. Our experiments confirmed that the effect of pyroptosis on NPMSCs is related to the RhoA signaling pathway.
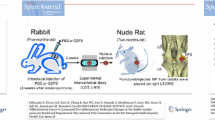
GDF-5 is a BMP homologous family protein that promotes chondrogenic differentiation. In a model of osteoarthritis, GDF-5 can promote the expression of extracellular matrix, type II collagen, and proteoglycan in chondrocytes. This inhibits the expression of cartilage catabolism factors MMP13 and ADAMTs5, thereby delaying the progression of osteoarthritis [36]. In a rat model of intervertebral disc degeneration, the researchers found that the intervertebral height and nucleus pulposus of the intervertebral disc could be delayed by injecting a drug delivery vehicle containing human adipose-derived stem cells and GDF-5 into the caudal space of the rat. This indicates that GDF-5 can promote the regeneration of nucleus pulposus tissue in the intervertebral disc [37]. A study by Shen et al. found that GDF-5 stimulation significantly reduced the expression of TNF-α and IL-1β in the LPS-stimulated group [35]. At the same time, the results of an ELISA showed that GDF-5 could reduce the LPS-induced increase in the expression of NO and PGE2. Further analysis of this mechanism showed that GDF-5 delayed the degeneration of nucleus pulposus cells in the intervertebral disc by inhibiting the activation of NF-κB signaling pathway [38]. Another study has shown that GDF-5 knockout mice have decreased water content in the intervertebral disc, and MRI T2-weighted imaging found that the nucleus pulposus in the intervertebral disc showed low signal [39]. Additionally, the lentiviral vector carrying the GDF-5 gene was transfected into NPMSCs, integrated into the chromosomal genome, and promoted the differentiation of NPMSCs into the nucleus pulposus cells [40]. Colombier et al. found that human adipose stromal cells (hASCs) could differentiate into nucleus pulposus-like cells under the co-culture of GDF-5 and TGF-β, and this mechanism may be related to the activation of Smad1/5/8 and Smad2/3 [41].
RhoA acts as a bridge between GDF-5 and NPMSCs in this study. We established a pyroptosis model of NPMSCs by LPS, and determined the effect of pyroptosis on signaling pathways by detecting the expression of RhoA protein. We further determined the changes of RhoA by adding GDF-5. Our results confirmed that this can promote the expression of RhoA and can delay the decline of RhoA expression caused by LPS. Studies have confirmed that tissue-specific decellularized tissue matrix (DTM) has biological activities such as regulating cell metabolism. The nucleus pulposus tissue and the annulus fibrosus are assembled with DTM into two DTM hydrogels (referred to as DNP-G and DAF-G). Studies have also found that DNP-G and DAF-G can promote stem cell regeneration in the intervertebral disc through the integrin-mediated RhoA/large tumor suppressor homologues/yes-associated protein1 signaling pathway [36]. Low-intensity pulsed ultrasound can improve the function of radiation-induced rat mandible-derived bone marrow mesenchymal stem cells by activating the RhoA/ROCK signaling pathway, which may be a potential target for the treatment of osteoradionecrosis of the jaw [42].
Our study had some limitations. Although our study links RhoA, NPMSCs, and pyroptosis for the first time, we did not do a more in-depth study of pyroptosis. Design-related experiments have not been performed at the animal level and, in the future, animal experiments in SD rats may be constructed by increasing the spinal stress model [43] to verify the injection of GDF-5 and determine the expression of pyroptosis-related proteins in the model group and the experimental group.
Conclusion
We identified the important role of GDF-5 in protecting NPMSCs from lipopolysaccharide-induced pyroptosis for the first time, and explored the potential of GDF-5 to inhibit NPMSCs pyroptosis molecular mechanism. GDF-5 may have potential for gene-targeted therapy for DDD in the future.
Data Availability
All data and information can be obtained from the corresponding author on reasonable request.
Abbreviations
- CDMP-1:
-
Cartilage-derived morphogenetic protein-1
- DDD:
-
Degenerative disc disease
- FBS:
-
Fetal bovine serum
- GDF-5:
-
Growth differentiation factor-5
- GSDMD:
-
Gasdermin-D
- LBP:
-
Low back pain
- NPMSCs:
-
Nucleus pulposus mesenchymal stem cells
- ROCK:
-
Rho-associated coiled-coil kinase
References
Cashin AG, Wand BM, O’Connell NE, Lee H, Rizzo RR, Bagg MK, O’Hagan E, Maher CG, Furlan AD, van Tulder MW, McAuley JH (2023) Pharmacological treatments for low back pain in adults: an overview of Cochrane Reviews, Cochrane Database Syst Rev 4(4) Cd013815.
Hauser RA, Matias D, Woznica D, Rawlings B, Woldin BA (2022) Lumbar instability as an etiology of low back pain and its treatment by prolotherapy: a review. J Back Musculoskelet Rehabil 35(4):701–712
Li Y, Chen X, Li L, Zeng F, Li J, Lu L (2022) Effect of acupuncture along Meridians on Pain Degree and Treatment of Acute lumbar sprain. Dis Markers 2022:5497805
Shelby T, Mills ES, Ton A, Wang JC, Hah RJ, Qureshi SA, Alluri RK (2023) The role of sex hormones in degenerative disc disease, Global Spine J 21925682231152826
Velnar T, Gradisnik L (2023) Endplate role in the degenerative disc disease: a brief review. World J Clin cases 11(1):17–29
Pattappa G, Li Z, Peroglio M, Wismer N, Alini M, Grad S (2012) Diversity of intervertebral disc cells: phenotype and function. J Anat 221(6):480–496
Iatridis JC, Nicoll SB, Michalek AJ, Walter BA, Gupta MS (2013) Role of biomechanics in intervertebral disc degeneration and regenerative therapies: what needs repairing in the disc and what are promising biomaterials for its repair? The spine journal: official journal of the North American Spine Society 13(3):243–262
Desmoulin GT, Pradhan V, Milner TE (2020) Mechanical aspects of intervertebral disc Injury and Implications on Biomechanics. Spine 45(8):E457–e464
Cornaz F, Widmer J, Farshad-Amacker NA, Spirig JM, Snedeker JG, Farshad M (2021) Intervertebral disc degeneration relates to biomechanical changes of spinal ligaments. The spine journal: official journal of the North American Spine Society 21(8):1399–1407
Xing H, Zhang Z, Mao Q, Wang C, Zhou Y, Zhou X, Ying L, Xu H, Hu S, Zhang N (2021) Injectable exosome-functionalized extracellular matrix hydrogel for metabolism balance and pyroptosis regulation in intervertebral disc degeneration. J Nanobiotechnol 19(1):264
Zhao K, An R, Xiang Q, Li G, Wang K, Song Y, Liao Z, Li S, Hua W, Feng X, Wu X, Zhang Y, Das A, Yang C (2021) Acid-sensing ion channels regulate nucleus pulposus cell inflammation and pyroptosis via the NLRP3 inflammasome in intervertebral disc degeneration. Cell Prolif 54(1):e12941
Che H, Li J, Li Y, Ma C, Liu H, Qin J, Dong J, Zhang Z, Xian CJ, Miao D, Wang L (2020) Y. Ren, p16 deficiency attenuates intervertebral disc degeneration by adjusting oxidative stress and nucleus pulposus cell cycle, eLife 9
Wang W, Jing X, Du T, Ren J, Liu X, Chen F, Shao Y, Sun S, Yang G, Cui X (2022) Iron overload promotes intervertebral disc degeneration via inducing oxidative stress and ferroptosis in endplate chondrocytes. Free Radic Biol Med 190:234–246
Song Y, Lu S, Geng W, Feng X, Luo R, Li G, Yang C (2021) Mitochondrial quality control in intervertebral disc degeneration. Exp Mol Med 53(7):1124–1133
Yin H, Wang K, Das A, Li G, Song Y, Luo R, Cheung JPY, Zhang T, Li S, Yang C (2021) The REDD1/TXNIP complex accelerates oxidative Stress-Induced apoptosis of Nucleus Pulposus cells through the mitochondrial pathway, oxidative medicine and cellular longevity 2021 7397516
Kovacs SB, Miao EA, Gasdermins (2017) Effectors of pyroptosis. Trends Cell Biol 27(9):673–684
Wang Y, Gao W, Shi X, Ding J, Liu W, He H, Wang K, Shao F (2017) Chemotherapy drugs induce pyroptosis through caspase-3 cleavage of a gasdermin. Nature 547(7661):99–103
Loveless R, Bloomquist R, Teng Y (2021) Pyroptosis at the forefront of anticancer immunity. J experimental Clin cancer research: CR 40(1):264
Yu P, Zhang X, Liu N, Tang L, Peng C, Chen X (2021) Pyroptosis: mechanisms and diseases. Signal Transduct Target therapy 6(1):128
Saci A, Carpenter CL (2005) RhoA GTPase regulates B cell receptor signaling. Mol Cell 17(2):205–214
Yang S, Kim HM (2012) The RhoA-ROCK-PTEN pathway as a molecular switch for anchorage dependent cell behavior. Biomaterials 33(10):2902–2915
Basant A, Glotzer M (2018) Spatiotemporal regulation of RhoA during Cytokinesis. Curr biology: CB 28(9):R570–r580
Liu J, Wada Y, Katsura M, Tozawa H, Erwin N, Kapron CM, Bao G, Liu J (2018) Rho-Associated Coiled-Coil kinase (ROCK) in Molecular Regulation of Angiogenesis. Theranostics 8(21):6053–6069
Malinauskas T, Peer TV, Bishop B, Mueller TD, Siebold C (2020) Repulsive guidance molecules lock growth differentiation factor 5 in an inhibitory complex. Proc Natl Acad Sci USA 117(27):15620–15631
Wehling N, Palmer GD, Pilapil C, Liu F, Wells JW, Müller PE, Evans CH, Porter RM (2009) Interleukin-1beta and tumor necrosis factor alpha inhibit chondrogenesis by human mesenchymal stem cells through NF-kappaB-dependent pathways. Arthritis Rheum 60(3):801–812
Kim GW, Han MS, Park HR, Lee EJ, Jung YK, Usmani SE, Ulici V, Han SW, Beier F (2015) CXC chemokine ligand 12a enhances chondrocyte proliferation and maturation during endochondral bone formation. Osteoarthr Cartil 23(6):966–974
Man SM, Karki R, Kanneganti TD (2017) Molecular mechanisms and functions of pyroptosis, inflammatory caspases and inflammasomes in infectious diseases. Immunol Rev 277(1):61–75
Yuan Y, Chen Y, Zhou Z, Jiao Y, Li C, Zheng Y, Lin Y, Xiao J, Chen Z, Cao P (2018) Association between chronic inflammation and latent infection of Propionibacterium acnes in non-pyogenic degenerated intervertebral discs: a pilot study, european spine journal: official publication of the european spine Society, the european spinal deformity Society, and the european section of the cervical. Spine Res Soc 27(10):2506–2517
Chen Z, Cao P, Zhou Z, Yuan Y, Jiao Y, Zheng Y (2016) Overview: the role of Propionibacterium acnes in nonpyogenic intervertebral discs. Int Orthop 40(6):1291–1298
Stirling A, Worthington T, Rafiq M, Lambert PA, Elliott TS (2001) Association between sciatica and Propionibacterium acnes, Lancet. (London England) 357(9273):2024–2025
Shan Z, Zhang X, Li S, Yu T, Mamuti M, Zhao F (2017) The influence of direct inoculation of Propionibacterium acnes on Modic Changes in the spine: evidence from a rabbit model, the Journal of bone and joint surgery. Am volume 99(6):472–481
Kistowska M, Gehrke S, Jankovic D, Kerl K, Fettelschoss A, Feldmeyer L, Fenini G, Kolios A, Navarini A, Ganceviciene R, Schauber J, Contassot E, French LE (2014) IL-1β drives inflammatory responses to propionibacterium acnes in vitro and in vivo. J Invest Dermatol 134(3):677–685
He D, Zhou M, Bai Z, Wen Y, Shen J, Hu Z (2020) Propionibacterium acnes induces intervertebral disc degeneration by promoting nucleus pulposus cell pyroptosis via NLRP3-dependent pathway. Biochem Biophys Res Commun 526(3):772–779
Tang G, Han X, Lin Z, Qian H, Chen B, Zhou C, Chen Y, Jiang W (2021) Propionibacterium acnes accelerates intervertebral disc degeneration by inducing pyroptosis of Nucleus Pulposus cells via the ROS-NLRP3 pathway, oxidative medicine and cellular longevity 2021 4657014
Zhang W, Li G, Luo R, Lei J, Song Y, Wang B, Ma L, Liao Z, Ke W, Liu H, Hua W, Zhao K, Feng X, Wu X, Zhang Y, Wang K, Yang C (2022) Cytosolic escape of mitochondrial DNA triggers cGAS-STING-NLRP3 axis-dependent nucleus pulposus cell pyroptosis. Exp Mol Med 54(2):129–142
Takahata Y, Hagino H, Kimura A, Urushizaki M, Yamamoto S, Wakamori K, Murakami T, Hata K, Nishimura R (2022) Regulatory Mechanisms of Prg4 and Gdf5 expression in articular cartilage and functions in Osteoarthritis, Int J Mol Sci 23(9)
Zhu J, Xia K, Yu W, Wang Y, Hua J, Liu B, Gong Z, Wang J, Xu A, You Z, Chen Q, Li F, Tao H, Liang C (2019) Sustained release of GDF5 from a designed coacervate attenuates disc degeneration in a rat model. Acta Biomater 86:300–311
Shen L, Wu Y, Han L, Zhang H (2018) Overexpression of growth and differentiation factor-5 inhibits inflammatory factors released by intervertebral disc cells. Experimental and therapeutic medicine 15(4):3603–3608
Feng C, Liu H, Yang Y, Huang B, Zhou Y (2015) Growth and differentiation factor-5 contributes to the structural and functional maintenance of the intervertebral disc. Cell Physiol biochemistry: Int J experimental Cell Physiol Biochem Pharmacol 35(1):1–16
Zhu K, Zhao R, Ye Y, Xu G, Zhang C (2022) Effect of lentivirus-mediated growth and differentiation factor-5 transfection on differentiation of rabbit nucleus pulposus mesenchymal stem cells. Eur J Med Res 27(1):5
Colombier P, Clouet J, Boyer C, Ruel M, Bonin G, Lesoeur J, Moreau A, Fellah BH, Weiss P, Lescaudron L, Camus A, Guicheux J (2016) TGF-β1 and GDF5 act synergistically to drive the differentiation of human adipose stromal cells toward Nucleus Pulposus-like cells, stem cells (Dayton. Ohio) 34(3):653–667
Zhang R, Wang Z, Zhu G, Wu G, Guo Q, Liu H, Chen L (2020) Low-intensity pulsed Ultrasound modulates RhoA/ROCK signaling of rat mandibular bone marrow mesenchymal stem cells to rescue their damaged Cytoskeletal Organization and Cell Biological function Induced by Radiation, stem cells international 2020 8863577
Sakai D, Nishimura K, Tanaka M, Nakajima D, Grad S, Alini M, Kawada H, Ando K, Mochida J (2015) Migration of bone marrow-derived cells for endogenous repair in a new tail-looping disc degeneration model in the mouse: a pilot study. The spine journal: official journal of the North American Spine Society 15(6):1356–1365
Funding
This study was supported by the Natural Science Foundation of China (No. 81772399 and 82102594).
Author information
Authors and Affiliations
Contributions
Chao Zhu and Dike Ruan designed the research. Chao Zhu wrote the manuscript. Qing Zhou and Zuqiang Wang contributed to the literature search. Chao Zhu and Qing Zhou performed the experiments. Zuqiang Wang, Junyou Zhang, Cheng Xu, and Dike Ruan reviewed and edited the article. All authors read and approved the article.
Corresponding author
Ethics declarations
Ethical approval
All experiments in this study were approved by the Ethics Committee of the Sixth Medical Center of PLA General Hospital(Approval number: HZKY-PJ-2021-35). Written informed consent was obtained from the donors of tissue samples used in this study.
Conflict of interest
The authors report no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhu, C., Zhou, Q., Wang, Z. et al. Growth differentiation factor 5 inhibits lipopolysaccharide-mediated pyroptosis of nucleus pulposus mesenchymal stem cells via RhoA signaling pathway. Mol Biol Rep 50, 6337–6347 (2023). https://doi.org/10.1007/s11033-023-08547-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-023-08547-6