Abstract
Host resistance to Leishmania infection is mediated by cellular immune responses leading to macrophage activation and parasite killing. Interleukin-18 (IL-18) known as interferon-γ (IFN-γ) inducing factor, stimulates IFN-γ production by T cells. Taking into account the important role of IL-18 in the defense against visceral leishmaniasis (VL) and the known effect of IL-18 gene polymorphisms on its production, the aim of this study was to investigate the probable relationship between IL-18 gene polymorphisms and the susceptibility to VL. The study groups included 118 pediatric patients who suffered from VL and 156 non-relative healthy people as the controls from the same endemic area. IL-18 gene polymorphisms at the positions −656 G/T, −137 G/C and +105A/C (codon 35/3) were analyzed by polymerase chain reaction-restricted fragment length polymorphism (PCR–RFLP). The results showed that the frequency of T allele at the position -656 was significantly higher in the controls, compared with that in the patients (P = 0.047), but it couldn’t tolerate Bonferroni correction. Regarding the IL-18 genotypes, there was no significant difference between the patients and controls. Although the frequencies of ATG single haplotype and AGG/ATG double haplotype were significantly higher in the controls (P = 0.043) and the patients (P = 0.044), respectively, the two P values couldn’t tolerate Bonferroni correction. Furthermore, a strong linkage disequilibrium was observed among the −656, −137 and +105 single nucleotide polymorphisms of IL-18 gene (all Ps < 0.001). In conclusion, this study suggests that the inheritance of T allele at the position −656 may be considered as a genetic factor for resistance to VL.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Visceral leishmaniasis (VL) is a systemic infectious disease caused by an intracellular protozoan belonging to Leishmania species. The majority of VL cases are caused by L. chagasi (in Latin America), L. donovani (in Africa, India, and south Asia), and L. infantum (in the Mediterranean littoral and the Middle East region) [1]. L. tropica is also reported as a causative agent for VL [2]. The disease is characterized clinically by prolonged fever, weight loss, hepatomegaly, splenomegaly, hypergammaglobulinemia and pancytopenia leading to death in the absence of treatment. The worldwide incidence of VL is estimated to be annually around 500,000 with over 50,000 deaths [1].
Leishmania can survive and replicate inside macrophages by modulating the antimicrobial activity of the cells as well as increasing the host cell membrane fluidity and disrupting lipid rafts which in turn affects the antigen presentation capability of host antigen presenting cells (APCs) [3]. Host resistance to Leishmania infection is mediated by cellular immune response and requires effective activation of macrophages, dendritic cells (DCs) and antigen specific CD4+ and CD8+ T cells [4]. CD4+ T cells are responsible for the production of cytokines critical for the activation of macrophages such as IFN-γ [5]. After exposure to IFN-γ, intracellular killing in macrophages occurs by nonoxidative mechanisms through the generation of nitric oxide and its metabolites from l-arginine after the induction of inducible nitric oxide synthase [6]. Then, IFN-γ is the key cytokine in immune response against leishmaniasis.
Interleukin-18 (IL-18), a member of the IL-1 cytokine superfamily, is now considered as a key regulator of innate and acquired immune responses [6, 7]. It is originally identified as a factor capable of inducing IFN-γ production by T cells. This cytokine promotes neutrophil activation, reactive oxygen intermediate synthesis, cytokine release, and cell degranulation [7–9]. Furthermore, recent studies suggest that IL-18 up-regulates intracellular adhesion molecule-1 (ICAM-1) and vascular cell adhesion molecule-1 (VCAM-1) expression on the endothelial cells [10]. Several studies have demonstrated the importance of IL-18 in immunity against VL and the outcome of the disease. It is shown that during the infection of phagocytes with different species of Leishmania, the release of IL-18 is increased [11]. Furthermore, it is proved that Leishmania infected IL-18-deficient mice had significantly lower IFN-γ production as well as lower serum IL-12 levels, indicating a reduced Th1 response [12]. Hence, IL-18 could be considered as an inducer for Th1 response in Leishmania infection.
Studies have shown that the maximal capacity of cytokine production varies among individuals and correlates with single nucleotide polymorphisms (SNPs) in the cytokine genes [13–15]. Moreover, it is shown that gene polymorphisms could play important roles in susceptibility and/or resistance of different people to the same infectious diseases [16–18]. Considering the importance of IL-18 in the defense against VL and the effect of IL-18 gene polymorphisms on its production, this study aimed at investigating the probable association between IL-18 gene polymorphisms and susceptibility to VL.
Materials and methods
Sample collection and DNA extraction
This study was carried out on 118 pediatric patients suffering from VL [56 females (47.5 %) and 62 males (52.5 %) with age range 6 months to 14 years, mean ± SD = 3.2 ± 2.3 years] and 156 non-relative healthy controls [72 females (46.1 %) and 84 males (53.9 %) with age range 9–16 years, mean ± SD = 12.9 ± 2.1 years] from the same endemic area. Some of the patients and controls were the same as those participating in our previous studies investigating the probable relationship between IL-1β, LT-α and TLR4 gene polymorphisms and susceptibility to VL [16, 19]. All the patients were admitted with the diagnosis of VL to the pediatric infectious diseases ward of Namazi hospital, affiliated with Shiraz University of Medical Sciences, Shiraz, Fars, Iran, based on clinical manifestation such as anemia, hepatosplenomegally and fever, with positive bone marrow smear and/or IFA (indirect fluorescent antibody) ≥1/128 for Leishmania parasite. Blood samples were taken from all the patients and controls following obtaining informed written consents from children’s parents, and DNA was extracted from all of the blood specimens using the salting out method. This study was approved by the Research Ethics Committee of Shiraz University of Medical Sciences.
Polymerase chain reaction-restriction fragment length polymorphism (PCR–RFLP)
IL-18 gene polymorphisms were analyzed by PCR–RFLP. For each sample, three PCR reactions were set up using three specific sets of primers [17] for the positions −656 G/T, −137 G/C and +105A/C (codon 35/3) of IL-18 gene. Each PCR cocktail contained 250 ng of genomic DNA, 1× PCR buffer, 0.5 μM specific primers set (Primm, Italy), 0.5 units Taq DNA polymerase, 0.2 mM dNTPs mix (all from CinnaGen, Iran), and specific concentration of MgCl2 (Table 1). PCRs were performed by a thermocycler set (5530 Mastercylcler, Eppendorf, Germany) under the following thermal conditions: a denaturation step for 3 min at 94 °C followed by 35 cycles of a denaturation for 45 s at 94 °C, annealing for 45 s at specific temperatures (Table 1), extension for 45 s at 72 °C and finally an extension step for 3 min at 72 °C. The products were digested by specific restriction enzymes (Fermentas, Lithuania) (Table 1). Lastly, the digested products were run on a 3 % agarose NA gel (Amersham Bioscience AB, Sweden) and studied on UV transilluminator after being stained by ethidium bromide (CinnaGen-Iran). The sequences of the primers, annealing temperatures, MgCl2 concentrations, restriction enzymes and DNA product sizes after digestion are shown in Table 1.
Statistical analysis
Allele and genotype frequencies were estimated by direct gene counting. Data were analyzed using Chi Square test with the level of significance set at less than 0.05 by EPI info 2000 and SPSS software version 16. Odds ratio and 95 % confidence interval were calculated by EPI info 2,000. Arlequin software package version 3.1 was used to estimate the haplotype and haplogenotype frequencies and Hardy–Weinberg equilibrium. Furthermore, linkage disequilibrium (LD) measures, R2 and D’, were estimated by LD2SNPing program V 2.0 (http://www.bio.kuas.edu.tw/LD2SNPing).
Results
In this study three known SNPs of IL-18 gene were analyzed using PCR–RFLP. The electrophoretic patterns of IL-18 gene polymorphisms are shown in Fig. 1. The results of the allele and genotype frequencies of IL-18 gene polymorphisms in the patient and control groups are demonstrated in Table 2. As it is shown, the frequency of T allele at position −656 was significantly higher in the controls compared with that in the patients (63.4 vs. 55.0 %, P = 0.047, OR = 0.71, 95 % CI = 0.49–1.01 and study power = 51 %), but it couldn’t tolerate Bonferroni correction. Furthermore, A allele at the position +105 and C allele at the position −137 were more frequent in the controls than in the patients, but the differences were not significant (74.4 vs. 71.2 %, P = 0.36, OR = 1.19, 95 % CI = 0.80–1.78 and 24.4 vs. 22.9 %, P = 0.68, OR = 0.92, 95 % CI = 0.61–1.40; respectively).
Regarding the IL-18 genotypes, there was no significant difference between the patients and controls. In both control and patient groups, the most frequent genotypes were +105AA, −656TG and −137GG. The distribution of genotypic variants met the Hardy–Weinberg equilibrium except at the position +105 A/C.
The comparison of the haplotypes showed that the distribution of ATG haplotype (positions +105, −656 and −137, respectively) was higher in the controls compared with that in the patients with VL (58.6 vs. 50.0 %, P = 0.043, OR = 0.70, 95 % CI = 0.49–1.01, study power = 52 %), but the P value could not tolerate the Boferroni correction (Table 3). This haplotype was the most frequent one in both groups (58.6 and 50.0 % in the control and patient groups, respectively).
According to the genotyping data in the patients with VL and controls, 34 haplo-genotypes were reconstructed. The frequencies of the most common haplo-genotypes are demonstrated in Table 3 and the rare haplo-genotypes (less than 5 %) were omitted from the table. Distribution of AGG/ATG haplo-genotype was higher in the patients with VL than that in the controls (12.7 vs. 5.7 %; P = 0.044, OR = 2.38, 95 % CI = 0.94–6.15, study power = 50 %). Again, this P value was not likely to bear the Bonferroni correction. The most frequent haplo-genotype in both study groups was ATG/ATG (37.2 and 28.8 % in the control and patient groups, respectively).
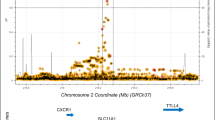
Moreover, strong LDs (P < 0.001 for all comparisons) were detected between −607, −137 and +105 SNPs in both control and patient groups. The LD measures, D′ and R2, are shown in Figs. 2 and 3.
Discussion
Similar to other intracellular parasites, resistance to Leishmania infection requires IL-12-driven Th1 immune response leading to the production of IFN-γ and activation of macrophages [20, 21]. IL-18 is a peliotropic cytokine which can regulate both natural and acquired immune systems [7–10]. The most well-known biological property of IL-18 is its capability to induce IFN-γ production in the presence of IL-12 [7, 8]. Actually, IL-18 and IL-12 show synergism in the induction of IFN-γ production by Th1, B cells and NK cells, promoting Th1 immune responses [7]. Moreover, IL-18 can directly enhance the proliferation and cytotoxicity of cytotoxic T cells and natural killer cells [22–25].
Bearing in mind the key role of IL-18 in the pathogenesis of leishmaniasis, this cytokine gene could be an important candidate in the determination of the disease outcome. Recent genetic studies suggest that some single nucleotide polymorphisms (SNPs) in the human IL-18 gene can affect the production of this cytokine [14, 15]. Considering the involvement of these polymorphisms in altering IL-18 level and the crucial role of this cytokine in the defense against VL, the present study aimed to investigate the probable relationship between IL-18 gene variants and the susceptibility and/or resistibility to Leishmania. In our previous study, we found a complete linkage disequilibrium (R2 = 1, P < 0.0001) for the two polymorphisms at the positions −656 and −607, as well as for three polymorphisms at the positions −137, +113 and +127 (R2 = 1, P < 0.0001) [26]. Therefore, in the present study, we just genotyped the polymorphisms of IL-18 gene at the positions −656, −137 and +105.
Previous studies showed that the presence of nucleotide G at the position −137 and A at the position +105 of IL-18 gene are associated with higher IL-18 production and potentially IFN-γ production [13–15]. So, we predicted that these high producing alleles must be more frequent in the controls, compared with those in VL patients; however, our results did not show any significant differences in the distribution of these alleles between the patients and controls. This lack of association may be due to the limited number of patients and controls participating in this study. Contrary to the two aforementioned polymorphic sites, the frequency of T allele at the position −656 was significantly higher in the controls than in the patients with VL. Then, T allele (−656) could be considered as a resistance factor for VL.
In addition to the genotypes and alleles, inherited combination of SNPs and polymorphic haplotypes can influence predisposition to different diseases. The frequency of ATG haplotype (positions +105, −656 and −137, respectively) was significantly higher in the controls and the inheritance of AGG/ATG haplo-genotype (positions +105, −656 and −137) was significantly more frequent in patients (P = 0.043 and P = 0.044, respectively). What is more, the inheritance of this haplo-genotype can suggest 2.38 times more chance for involvement in VL. Although the differences between the frequencies of ATG haplotype and AGG/ATG haplogenotype are significant among the study groups, again the P values could not bear Bonferroni correction.
In this study, some P values could not tolerate Bonferroni correction. Also, statistical analysis didn’t show enough power. For example, −656 T allele was significantly higher in the controls than that in the patients (P = 0.047), but the study power didn’t support it (51 %). It might be due to the limited number of the participants in the study.
To the best of our knowledge, there is no published study report concerning IL-18 gene variants and VL in other countries. Therefore, it was impossible to compare the results of this study to others, so, further investigations into this issue seem warranted. Nevertheless, there are several studies on IL-18 gene variants and susceptibility to other infectious and non infectious diseases. In a previous study, it was shown that the inheritance of high producing alleles, genotypes, haplotypes and haplogenotypes of IL-18 gene can be considered as an influential genetic factor in the protection against Brucella infection [26]. Zhang et al. [27] suggested that Chinese people carrying C allele at the position −137 of IL-18 gene may be protected against HBV infection and individuals carrying AA genotype at the position −607 may be closely linked to the inhibition of HBV-DNA replication. Folwaczny and colleagues could not find any relationship between polymorphisms of IL-18 gene and predisposition to periodontitis [17]. Leung and colleagues could not provide any evidence supporting the probable role of IL-18 gene polymorphisms in the development of gastric intestinal metaplasia in Chinese population infected with H.pylori [28].
In conclusion, based on the present findings, it is suggested that the inheritance of T allele at the position −656 may be considered as a genetic factor for resistance to VL.
References
Desjeux P (2004) Leishmaniasis: current situation and new perspectives. Comp Immunol Microbiol Infect Dis 27(5):305–318
Alborzi A, Rasouli M, Shamsizadeh A (2006) Leishmania tropica-isolated patient with visceral leishmaniasis in southern Iran. Am J Trop Med Hyg 74:306–307
Chakraborty D, Banerjee S, Sen A, Banerjee KK, Das P, Roy S (2005) Leishmania donovani affects antigen presentation of macrophage by disrupting lipid rafts. J Immunol 175:3214–3224
Stanley AC, Engwerda CR (2007) Balancing immunity and pathology in visceral leishmaniasis. Immunol Cell Biol 85:138–147
Kharazmi A, Kemp K, Ismail A, Gasim S, Gaafar A, Kurtzhals JA, El Hassan AM, Theander TG, Kemp M (1999) T-cell response in human leishmaniasis. Immunol Lett 65:105–108
Green SJ, Meltzer MS, Hibbs JB Jr, Nacy CA (1990) Activated macrophages destroy intracellular Leishmania major amastigotes by an l-arginine dependent killing mechanism. J Immunol 1144:1278–1285
Dinarello CA (1999) IL-18: a TH1-inducing, proinflammatory cytokine and new member of the IL-1 family. J Allergy Clin Immunol 103(1 Pt 1):11–24
Nakanishi K, Yoshimoto T, Tsutsui H, Okamura H (2001) Interleukin-18 regulates both Th1 and Th2 responses. Annu Rev Immunol 19:423–474
Leung BP, Culshaw S, Gracie JA, Hunter D, Canetti CA, Campbell C, Cunha F, Liew FY, McInnes IB (2001) A role for IL-18 in neutrophil activation. J Immunol 167:2879–2886
Morel JC, Park CC, Woods JM, Koch AE (2001) A novel role for interleukin-18 in adhesion molecule induction through NF kappa B and phosphatidylinositol (PI) 3-kinase-dependent signal transduction pathways. J Biol Chem 276:37069–37075
Iannello D, Arena A, Buemi C, Calapai M, Stassi G, Gazzara D, Mastroeni P (2003) Differential induction of TNF alpha and IL-18 in human peripheral blood mononuclear cells infected with Leishmania major or Leishmania donovani. New Microbiol 26:399–404
Mullen AB, Lawrence CE, McFarlane E, Wei XQ, Carter KC (2006) Endogenous interleukin-18 is involved in immunity to Leishmania donovani but its absence does not adversely influence the therapeutic activity of sodium stibogluconate. Immunology 119:348–354
Arimitsu J, Hirano T, Higa S, Kawai M, Naka T, Ogata A, Shima Y, Fujimoto M, Yamadori T, Hagiwara K, Ohgawara T, Kuwabara Y, Kawase I, Tanaka T (2006) IL-18 gene polymorphisms affect IL-18 production capability by monocytes. Biochem Biophys Res Commun 342:1413–1416
Giedraitis V, He B, Huang WX, Hillert J (2001) Cloning and mutation analysis of the human IL-18 promoter: a possible role of polymorphisms in expression regulation. J Neuroimmunol 112:146–152
Liang XH, Cheung W, Heng CK, Wang DY (2005) Reduced transcriptional activity in individuals with IL-18 gene variants detected from functional but not association study. Biochem Biophys Res Commun 338:736–741
Moravej A, Rasouli M, Kalani M, Asaei S, Kiany S, Najafipour S, Koohpayeh A, Abdollahi A (2012) IL-1β (-511T/C) gene polymorphism not IL-1β (+3953T/C) and LT-α (+252A/G) gene variants confers susceptibility to visceral leishmaniasis. Mol Biol Rep 39(6):6907–6914
Folwaczny M, Glas J, Török HP, Tonenchi L, Paschos E, Bauer B, Limbersky O, Folwaczny C (2005) Polymorphisms of the interleukin-18 gene in periodontitis patients. J Clin Periodontol 32(5):530–534
Kalani M, Rasouli M, Moravej A, Kiany S, Rahimi HR (2011) Association of interleukin-15 single nucleotide polymorphisms with resistance to brucellosis among Iranian patients. Tissue Antigens 78(5):352–358
Rasouli M, Keshavarz M, Kalani M, Moravej A, Kiani S, Badiee P (2012) Toll-like receptor 4 (TLR4) polymorphisms in Iranian patients with visceral leishmaniasis. Mol Biol Rep 39(12):10795–10802. doi:10.1007/s11033-012-1973-5
Kaye PM, Svensson M, Ato M, Maroof A, Polley R, Stager S, Zubairi S, Engwerda CR (2004) The immunopathology of experimental visceral leishmaniasis. Immunol Rev 201:239–253
Lehmann J, Enssle KH, Lehmann I, Emmendörfer A, Lohmann-Matthes ML (2000) The capacity to produce IFN-gamma rather than the presence of interleukin-4 determines the resistance and the degree of susceptibility to Leishmania donovani infection in mice. J Interferon Cytokine Res 20:63–77
Dinarello C, Fantuzzi G (2003) Interleukin 18 and host defense. J Infectious Dis 187:370–384
Helmby H, Grencis RK (2002) IL-18 regulates intestinal mastocytosis and Th2 cytokine production independently of IFN-c during Trichinella spiralis infection. J Immunol 169:2553–2560
Wei XQ, Leung BP, Arthur HM, McInnes IB, Liew FY (2001) Reduced incidence and severity of collagen-induced arthritis in mice lacking IL-18. J Immunol 166:517–521
Netea MG, Kullberg BJ, Verschueren I, Van Der Meer JW (2000) Interleukin-18 induces production of proinflammatory cytokines in mice: no intermediate role for the cytokines of the tumor necrosis factor family and interleukin-1beta. Eur J Immunol 30:3057–3060
Rasouli M, Kalani M, Moravej A, Kiany S (2011) Interleukin-18 single nucleotide polymorphisms contribute to the susceptibility to brucellosis in Iranian patients. Cytokine 54(3):272–276
Zhang PA, Wu JM, Li Y, Yang XS (2005) Association of polymorphisms of interleukin-18 gene promoter region with chronic hepatitis B in Chinese Han population. World J Gastroenterol 11(11):1594–1598
Leung WK, Chan MC, To KF, Man EP, Ng EK, Chu ES, Lau JY, Lin SR, Sung JJ (2006) H. pylori genotypes and cytokine gene polymorphisms influence the development of gastric intestinal metaplasia in a Chinese population. Am J Gastroenterol 101(4):714–720
Acknowledgments
Our thanks are due to Miss. Esmat Kazemi and Dr. Hassan Khajehei for linguistic copy editing. We also thank Fars Province Health Center for their help with finding the patients. This study was financially supported by the Grants No. 91-15 and No. 91-8-2 respectively awarded by Prof. Alborzi Clinical Microbiology Research Center, Shiraz University of Medical Sciences, and Fasa University of Medical Sciences.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Moravej, A., Rasouli, M., Asaei, S. et al. Association of interleukin-18 gene variants with susceptibility to visceral leishmaniasis in Iranian population. Mol Biol Rep 40, 4009–4014 (2013). https://doi.org/10.1007/s11033-012-2479-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-012-2479-x