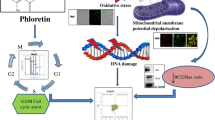
Abstract
Phosphatidylinositol 3-kinase (PI3-K)/PTEN/Akt signaling is over activated in various tumors including colon cancer. Activation of this pathway regulates multiple biological processes such as apoptosis, metabolism, cell proliferation, and cell growth that underlie the biology of a cancer cell. In the present study, the chemopreventive effects have been observed of Diclofenac, a preferential COX-2 inhibitory non-steroidal anti-inflammatory drugs, and Curcumin, a natural anti-inflammatory agent, in the early stage of colorectal carcinogenesis induced by 1,2-dimethylhydrazine dihydrochloride in rats. The tumor-promoting role of PI3-K/Akt/PTEN signal transduction pathway and its association with anti-apoptotic family of proteins are also observed. Both Diclofenac and Curcumin downregulated the PI3-K and Akt expression while promoting the apoptotic mechanism. Diclofenac and Curcumin administration significantly increased the expression of pro-apoptotic Bcl-2 family members (Bad and Bax) while decreasing the anti-apoptotic Bcl-2 protein. An up-regulation of cysteine protease family apoptosis executioner, such as caspase-3 and -9, is seen. Diclofenac and Curcumin inhibited the Bcl-2 protein by directly interacting at the active site by multiple hydrogen bonding, as also evident by negative glide score of Bcl-2. These drugs stimulated apoptosis by increasing reactive oxygen species (ROS) generation and simultaneously decreasing the mitochondrial membrane potential (ΔΨ M). Diclofenac and Curcumin showed anti-neoplastic effects by downregulating PI3-K/Akt/PTEN pathway, inducing apoptosis, increasing ROS generation, and decreasing ΔΨ M. The anti-neoplastic and apoptotic effects were found enhanced when both Diclofenac and Curcumin were administered together, rather than individually.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Apoptosis or programmed cell death plays a vital role in controlling cell number in many developmental and physiological stages, tissue homeostasis, and regulation of immune system, while dysregulation of apoptotic process is involved in the development of neoplastic transformation and tumor growth [1, 2]. Apoptosis plays an essential role as a protective mechanism against tumor cells which are aberrated or excess cells that have been improperly produced [3]. Therefore, various kinds of effective apoptosis-enhancing agents that target cancer cells may represent a useful mechanistic approach to both chemoprevention and chemotherapy of cancer.
Phosphatidylinositol 3-kinase (PI3-K)/Akt signal transduction plays an important role in cell growth via inhibition of apoptosis in various types of human cancers [4]. Akt, a serine/threonine kinase or called protein kinase B, is a key component of cell survival pathway and is a major downstream target of PI3-K [5]. Akt is activated by a dual regulatory mechanism that requires both translocation to the plasma membrane and targeted phosphorylation [6]. The generation of phosphatidylinositol 3,4,5-triphosphate (PIP3) takes place on the inner layer of the plasma membrane, and the following PI3-K activation recruits Akt and its activation by both phosphoinositide-dependent protein kinase-1 (PDK1), which phosphorylates Akt at Thr-308, and PDK1-independent mechanisms, which result in Akt phosphorylation at Ser-473 [7]. The activity of Akt is negatively regulated by tumor suppressor protein, phosphatase, and tensin homolog deleted on chromosome ten (PTEN), which is frequently mutated in human malignancy [8]. Upon activation, Akt phosphorylates and/or interacts with a number of molecules to exert its normal cellular functions, which include directed roles in cell proliferation, survival, and differentiation [9]. Akt also promotes cell survival by phosphorylating and inactivating key proteins of the apoptotic machinery, such as Bad and caspase-9, and up-regulation of Bcl-2 family anti-apoptotic proteins by transcriptional activation [10].
Numerous epidemiological studies have demonstrated the relation between diet and cancer and the potential of dietary components, in particular polyphenols as promising chemopreventive agents [11]. Curcumin, a major component extracted from rhizomes of the plant Curcuma longa Linn (also termed as turmeric), has been extensively studied for its wide range of biological activities, including anti-inflammatory, anti-oxidant, anti-infection, and anti-cancer properties [12]. Curcumin is also pharmacologically safe as it is a naturally occurring compound used as a food-coloring agent and in traditional medicines to treat various diseases in Asian countries and also as carrier in nanomedicines [13, 14]. There is increasing interest in the application that combination of cancer chemopreventive agents may produce considerably stronger protective effects against carcinogenesis than each chemopreventive agent could do so individually [15, 16]. We had shown earlier that the combinatorial regimen of non-steroidal anti-inflammatory drugs (NSAIDs) and natural compounds produced enhanced chemopreventive effects in early colon cancer than the administration of either agent alone [17, 18]. Taken together, the results of these studies provide strong validation for combining a chemopreventive approach that targets the oncogenic pathway PI3-K/Akt/PTEN in conjunction with apoptosis-inducing chemopreventives. The present study was designed to evaluate the potential chemopreventive efficacy of a natural anti-inflammatory agent, Curcumin, and a preferentially selective COX-2 inhibitory NSAID, Diclofenac, alone and also in combination, in colorectal cancer in rats, which was induced by 1,2-dimethylhydrazine dihydrochloride (DMH). The role of PI3-K/Akt/PTEN pathway and its association with anti-apoptotic family of proteins, and the molecular basis of such interaction were also studied through flexible molecular docking by GLIDE software from Schrodinger (USA) programme suite.
Materials and methods
Chemicals
DMH and a Bradford re-agent were purchased from Sigma-Aldrich (St. Louis, MO, USA). Diclofenac was a generous gift from Ranbaxy Pharmaceuticals (Gurgaon, India). A primary antibody against PI3-K, PTEN, PDK1, Akt, Bcl-2, Bax, Bad, apoptotic protease-activating factor-1 (Apaf-1), Cyt c, caspase-3, caspase-9, and β-actin was purchased from Santa Cruz Biotechnology, Inc., CA (USA). Alkaline phosphatase-conjugated secondary antibodies and BCIP-NBT were purchased from Genei, Bangalore (India). All other chemicals and reagents used in the present study were of analytical grade and purchased from the reputed Indian manufacturers.
Animal procurement
Male Sprague–Dawley rats of body weight (b.w.) between 150 and 200 g were obtained from the Central Animal House, Panjab University after the approval of the present protocol by the Ethics Committee of Animal Care. They were acclimatized and given rodent chow and water ad libitum for at least 1 week. They were maintained as per the principles and guidelines of the Committee for the Purpose of Control and Supervision on Experiments on Animals, Ministry of Environment Science and Forests, Govt. of India. They were housed three per cage in polypropylene cages with a wire mesh top and a hygienic bed of husk (regularly changed) in a well-ventilated animal room. The animals were also maintained at the ambient temperature and humidity and under a 12-h photoperiod of light and darkness, respectively.
Carrageenan-induced paw edema
Carrageenan-induced paw edema is a suitable experiment for evaluating anti-edematous effects in animal model [19]. To induce acute phase inflammation in paw, rats were injected subcutaneously (s.c.) 0.1 ml of 1 % (w/v) carrageenan suspension in saline into the subplantar region of the hind paw of the rats according to the method developed by Winter et al. [20]. The test group 1 of rats was treated orally with various doses of Diclofenac, i.e., 4, 8, and 12 mg/kg/b.w. Test group 2 of rats was administered orally with various doses of Curcumin, i.e., 25, 50, and 75 mg/kg b.w. Test group 3 of rats was treated with both Diclofenac and Curcumin orally in combination, i.e., 4 + 25, 4 + 50, 4 + 75, 8 + 25, 8 + 50, 8 + 75, 12 + 25, 12 + 50, and 12 + 75 mg/kg/b.w., respectively, of the two drugs. The reference group received a dose of 5 mg/kg Indomethacin, orally. The swelling in the paw and its remission were measured up to 5 h after the injection at intervals of 1 h with a volume displacement plethysmometer. Percent inhibition in the hind paw after carrageenan injection was calculated using the formula
where C t is the mean paw volume for each group at time t and C o is the mean paw volume for each group before carrageenan injection [19].
Treatment schedule
Animals were assorted into the following groups.
Control group, vehicle treated
Animals were administered the vehicle (1 mM EDTA–saline) s.c. in weekly injection and 0.5 % carboxymethyl cellulose sodium salt per oral (p.o.) daily.
DMH group
Animals were administered with DMH weekly at a dose of 30 mg/kg b.w. (s.c.). The dose of DMH in early carcinogenesis has been established in our laboratory earlier [18, 21]. DMH was freshly prepared in 1 mM EDTA–saline and pH adjusted to 7.0 using dilute NaOH solution.
DMH + Diclofenac group
Diclofenac was given daily (p.o.) within its therapeutic anti-inflammatory dose (ED50 for rats, 8 mg/kg b.w.) along with the weekly administration of 30 mg/kg b.w. of DMH.
DMH + Curcumin group
Curcumin was administered p.o. daily (ED50 for rats, 50 mg/kg b.w.) along with the weekly administration of 30 mg/kg b.w. of DMH.
DMH + Diclofenac + Curcumin group
Both Diclofenac (8 mg/kg b.w.) and Curcumin (50 mg/kg b.w.) were administered p.o. daily along with the weekly dose of 30 mg/kg b.w. of DMH s.c.
After 6 weeks, animals were kept on overnight fasting with drinking water ad libitum and sacrificed the following day under an over anesthesia with ether. The animal b.w.s in all the groups were recorded once in a week.
Gross morphology
The colons were removed and flushed clear with ice-cold physiological saline (NaCl solution, 9 g/l). These were opened longitudinally along the median, laid flat, and examined by hand-held lens for the incidence of tumors and macroscopic neoplastic lesions/plaques called the multiple plaque lesions (MPLs). The colons were divided into proximal, medial, and distal segments [21].
Histopathology
Colon tissue embedding and sectioning were performed as described earlier [18]. De-waxed sections were then stained in hematoxylin and eosin, mounted in DPX, viewed under ×400, and photographed.
Isolation of colonocytes
Colonocytes were obtained from the freshly isolated colons by the method of Mouille et al. 2004 as described earlier [16, 18]. Trypan blue dye exclusion was performed each time for every group of isolated colonocytes, and the viability of cells observed ~90 %.
Western blot
Cell lysate preparation and western blots were performed as described earlier [22]. Immunoblot was prepared using primary antibodies (PI3-K: 1:1,000, PDK1: 2 µg, Akt: 1:1,000, PTEN: 1:1,000, Bcl-2: 1:1,000, Bad: 1:1,000, Bax: 1:500, Apaf-1: 1:1,000, Cyt c: 1:1,000, caspase-9: 1:1,000, caspase-3: 1:1,000, and β-actin: 1:1,000) from Santa Cruz Biotechnology, Inc., CA (USA) and alkaline phosphatase-conjugated respective IgG secondary antibodies at a dilution of 1:10,000 (Genei, Bangalore, India). Protein concentration was determined by the method of Bradford [23].
Immunofluorescence
Immunofluorescence analysis was done as described earlier with primary antibodies of Bcl-2, Bax, Akt, and Bad at a dilution of 1:1,000, then incubated with respective FITC-conjugated secondary anti-body, and observed under a fluorescence microscope (Axioscope A1, Carl Zeiss, Germany) [24].
mRNA expression by reverse transcriptase polymerase chain reaction (RT-PCR) and further validation by quantitative real-time PCR (qRT-PCR)
Isolation of total RNA, selection of specific pairs of primers, RT-PCR, and qRT-PCR were performed as described earlier [22]. Details of accession numbers, primer sequences, and final product (amplicon) size of Akt, Bcl-2, Bax, Bad, and β-actin are provided in Suppl. Table 1. Results shown here are the mean normalized values of cDNA levels with the reference gene [21].
Molecular docking
Molecular docking studies were done using various tools of Schrodinger suite 2011 (USA) as described earlier by Rana et al. [18]. Glide extra-precision mode was subsequently used to provide a better correlation between good poses and good scores [25].
Analysis of mitochondrial membrane potential (ΔΨ M) with Rhodamine 123 (R123)
The photo selective laser dye R123 is shown to be a specific probe for the detection of alterations in mitochondrial membrane potential in the cells. For the fluorescent microscopy of the colonocytes with R123, the method of Johnson et al. was used [26]. To quantify the ΔΨ M, the flow cytometry of colonocytes was done by labeling them with R123. 2 × 106 cells/ml were washed twice, re-suspended in PBS, and incubated with a final concentration of 10 mg/ml of R123 (stock in PBS) for 15 min at 37 °C. R123 fluorescence (λ ex ~ 546 nm and λ em ~ 590 nm) was detected by BD FACS Calibur flow cytometer with FL-2 filter (propidium iodide-channel), where the data were acquired and analyzed by BD Cell Quest Pro software. For quantification of cells by fluorescence microscopy, a total of 300 cells from four different slides were observed for each animal group [21]. Spectrofluorometric measurement of ΔΨ M with R123 was carried out with a dual-wavelength Perkin Elmer Luminescence Spectrometer LS 55 using a 2-ml, 1 cm path length quartz cuvette installed with FL WinLab software 4.00.02.
Identification of intracellular reactive oxygen species (ROS)
Intracellular levels of ROS were estimated using the fluorescent probe, 2,7-dichlorofluorescein diacetate (DCFH-DA). DCFH-DA diffuses through the cell membrane readily and enzymatically hydrolyzed by intracellular esterases to non-fluorescent DCFH, which is then rapidly oxidized to highly fluorescent DCF in the presence of ROS [27]. Quantification of colonocytes with higher ROS was further done by detection of DCF fluorescence intensity (λ ex ~ 485 nm and λ em ~ 530 nm) in BD FACS Calibur flow cytometer (Becton–Dickinson, San Jose, California, USA) with FL-1 filter (FITC-channel), where the data were acquired and analyzed by BD Cell Quest Pro software (version 5.1). Spectrofluorometric measurement of ROS with DCFH-DA and DCF fluorescence intensity was first detected in LS 55 Luminescence Spectrometer, Perkin Elmer, at different time intervals with excitation wavelength 485 nm and emission wavelength at 530 nm which was found proportional to the amount of ROS formed inside the colonocytes.
Apoptotic studies
Fluorescence microscopy using the DNA-binding fluorescent dyes, acridine orange (AO), and ethidium bromide (EB) was employed to study the morphology of the isolated colonocytes undergoing apoptosis. Briefly, 10 µl of the cell suspension (106 cells/ml) was mixed in PBS (pH 7.4) containing AO (1 mg/ml) and EB (1 mg/ml). Of this mixture, 10 µl was placed on a clean glass slide and covered with coverslip, and a minimum of 300 cells were counted (×400) using a fluorescence microscope (Axioscope A1, Carl Zeiss, Germany). The index of apoptosis was calculated as the percentage of the total number of cells with apoptotic nuclei to the total number of cells counted as had been reported earlier [21].
Statistical analysis
Data were expressed as mean ± SD of four independent observations for each group. One-way analysis of variance (ANOVA) was done to compare the means between the different treatments using post hoc comparison by least significant difference method. The statistical software package SPSS v14 for windows was used for the purpose. A value of p ≤ 0.05 was considered significant in this study.
Results
Carrageenan-induced paw edema
Edema developed following injection of carrageenan serves as an index of acute inflammatory change and can be determined from the differences in paw volume measured immediately after carrageenan injection and then every hour till 5 h. Carrageenan-induced paw edema test was done to examine the anti-inflammatory effects of Diclofenac and Curcumin individually and in combination. Rats were administered various doses of Diclofenac (4, 8, and 12 mg/kg), Curcumin (25, 50, and 75 mg/kg), and both Diclofenac and Curcumin in combination (4 + 25, 4 + 50, 4 + 75, 8 + 25, 8 + 50, 8 + 75, 12 + 25, 12 + 50, and 12 + 75) orally 1 h before carrageenan administration. Results revealed that the individual administration of Diclofenac at a dose of 8 mg/kg (Fig. 1a) and Curcumin at a dose of 50 mg/kg (Fig. 1b) could produce maximum inhibition of inflammation to an extent of 51.4 and 65.2 %, respectively, and the results were comparable to that of Indomethacin as a standard anti-inflammatory drug (Fig. 1a–c). Indomethacin significantly decreased paw edema at 4 h after carrageenan injection. However, their combination (Diclofenac at dose of 8 mg/kg + Curcumin at dose of 50 mg/kg) was able to produce a significant inhibition of inflammation to an extent of 94.5 % (Fig. 1c). Therefore, the present results of the Diclofenac and Curcumin on the chemoprevention of cancer are in good agreement of the anti-inflammatory dose range of the drug, as shown in the rat model.
Effects of Diclofenac and Curcumin alone, and in combination on paw edema induced by carrageenan. a Percent inhibition showed by various doses of Diclofenac (4, 8, and 12 mg/kg/b.w.) on paw edema induced by carrageenan. Diclofenac at a dose of 8 mg/kg produced maximum inhibition of inflammation of 51.4 %, and the results were comparable to that of Indomethacin as a standard anti-inflammatory drug. b Percent inhibition showed by various doses of Curcumin (25, 50, and 75 mg/kg/b.w.) on paw edema induced by carrageenan. Curcumin at a dose of 50 mg/kg/b.w. produced maximum inhibition of 65.2 %. c Percent inhibition after administration of various doses of Diclofenac and Curcumin in combination (4 + 25, 4 + 50, 4 + 75, 8 + 25, 8 + 50, 8 + 75, 12 + 25, 12 + 50, and 12 + 75 mg/kg/b.w., respectively). Combination of Diclofenac at dose of 8 mg/kg with Curcumin at dose of 50 mg/kg was able to produce a significant inhibition of inflammation to an extent of 94.5 %
Morphological analysis of colon for MPLs
Among all the five groups, DMH alone showed higher MPL incidence (100 %), while the co-administration of Diclofenac and Curcumin reduced the MPL incidence as compared to DMH group (Table 1). MPLs were recognized as either raised or non-raised lesions with identifiable tissue growth in DMH-treated animals, often appearing singly or in multiple forms throughout the length of the colon (Fig. 2a). Although Diclofenac and Curcumin when given alone reduced the number of MPLs significantly, the combination of the two drugs showed far less number of MPLs. Colons from control group did not show any occurrence of MPL.
a Gross anatomy of the colon showing normal mucosal surface in the control animals and mucosal plaque lesions (MPLs) in DMH-treated animals. The animals from DMH + Diclofenac, DMH + Diclofenac, and DMH + Diclofenac + Curcumin groups showed fewer MPLs. MPLs are shown in circles. b Histopathological examination of the colonic tissues after 6 weeks of treatment. Control group showing normal intact crypt architecture. DMH-treated group exhibits severe dysplasia and hyperplasia of crypt cells (black arrows) and nuclei enlarged and deeply stained (blue arrows). Treatment with Diclofenac and Curcumin corrected these carcinogenic changes. (Color figure online)
Histopathological examination
After 6 weeks of treatment, colonic tissues were examined histopathologically by H&E staining where we can see the intact cylindrical shape and architecture of crypts in the control group. Also, there is an obvious relationship between crypt and stromal interspace. However, in DMH group, the inter-relationship between crypt architecture and stromal tissues has largely been distorted with the presence of dysplasia. Also, high grade hyperplasia can be seen as characterized by increased number of deeply stained nuclei due to the presence of highly proliferative cells. Simultaneous administration with Diclofenac and Curcumin largely corrected these carcinogenic changes. However, mild grade hyperplasia can still be evident. The effect is much more pronounced in DMH + Diclofenac + Curcumin group where typical crypt architecture and crypt shape are found as shown in Fig. 2b.
Regulation of PI3-K/PDK1/PTEN/Akt pathway during carcinogenesis
Abnormalities in the PI3-K/PDK1/PTEN/Akt pathway are common in cancers and have a role in variety of cellular functions, including cell growth, differentiation, development, and apoptosis. In the present study, we observed that the expression of PI3-K is higher in DMH group (Fig. 3a, b), suggesting that PI3-K up-regulation could have a role in neoplastic transformation. However, the expression of PI3-K decreased after Diclofenac and Curcumin treatment, and the decrease being more when both were given together. Both Diclofenac and Curcumin were able to raise the expression of PTEN, an antagonist of PI3-K, which attenuates the downstream signaling of activated PI3-K (Fig. 3a, b). PDK1 is a downstream mediator of PI3-K and is essential for the activation of Akt. Our results showed that PDK1 expression is up-regulated in DMH group, whereas Diclofenac and Curcumin co-administration lowered down its expression level (Fig. 3a, b). In silico studies showed that Diclofenac efficiently docked in the ATP-binding site of PI3-K with a valid glide score of −9.7 and forming hydrogen bond with the amino acid residue Val-882 (Suppl. Fig. 1a; Suppl. Table 2). However, Curcumin could not form a docked complex in the ATP-binding site of PI3-K.
Regulation of PI3-K/PTEN/PDK1 pathway during tumorigenesis. a Western immunoblot analysis showed that PI3-K and PDK1 were highly expressed in DMH group, whereas DMH + Diclofenac and DMH + Curcumin groups were having lesser expression levels. Expression of PI3-K and PDK1 was minimum in the DMH + Diclofenac + Curcumin group. PTEN expression was found to be increased in DMH + Diclofenac and DMH + Curcumin. b Quantitative analysis of the blots in densitometric units. Values are mean ± SD of three animals. b p ≤ 0.01 and c p ≤ 0.001 in comparison to control and z p ≤ 0.001 in comparison to DMH by one-way ANOVA
Akt mRNA expression via RT-PCR was found significantly up-regulated in DMH group which suggested the aberrant activation of Akt during tumorigenesis, whereas Diclofenac and Curcumin co-administration could down-regulate its expression (Suppl. Fig. 2a, b). These results were further validated by qRT-PCR (Suppl. Fig. 2c). Western immunoblot analysis and immunofluorescence analysis further confirm the higher amount of translated Akt in DMH group, whereas DMH + Diclofenac and DMH + Curcumin groups were having lesser Akt levels (Fig. 4a–c). The expression was additionally down-regulated in DMH + Diclofenac + Curcumin group (Fig. 4a–c; Suppl. Fig. 2a–c). Molecular docking studies showed that both Diclofenac and Curcumin formed a valid docked complex with ATP-binding site of Akt (Suppl. Fig. 2d, e) and having a glide score of −7.63 and −7.90, respectively. The amino acid residues involved in the formation of H-bonds are listed in Suppl. Table 2.
Akt expression via its activation and localization in the colonic tissues. a Western immunoblot analysis of Akt showed higher amount of translated protein in DMH group as compared to control, whereas DMH + Diclofenac and DMH + Curcumin groups were having lesser Akt levels as compared to DMH group. Expression was minimum in the DMH + Diclofenac + Curcumin group. β-Actin is serving as loading control. b Quantitative analysis of the blots in densitometric units. Values are mean ± SD of three animals. c p ≤ 0.001 in comparison to control and z p ≤ 0.001 in comparison to DMH by one-way ANOVA. c Expression of Akt in the colonic tissue sections (arrows) was analyzed by immunofluorescence. DMH group showed higher expression and localization of Akt (arrows) as compared to the other groups
Diclofenac and Curcumin triggers mitochondrial pathway of apoptosis
To further elucidate the role of PI3-K/Akt/PTEN pathway in promoting cell survival and blocking apoptosis in colon carcinogenesis, the expression of Bcl-2 family of proteins was checked. AO/EB staining of isolated colonocytes showed that both Diclofenac and Curcumin can induce apoptosis as shown in Fig. 5a, b. The number of apoptotic cells was increased in DMH + Diclofenac and Diclofenac + Curcumin groups as compared to DMH group (Fig. 5b). The results also showed that Bcl-2 is expressed higher in DMH group as shown by RT-PCR, qRT-PCR, western blot, and immunofluorescence analyses (Fig. 6a–f; Suppl. Fig. 3a, b). The expression of Bcl-2 was significantly lowered down in DMH + Curcumin and DMH + Diclofenac groups. However, the expression of pro-apoptotic Bad and Bax was downregulated both at transcriptional and translational level in DMH group (Fig. 6a–c; Suppl. Fig. 3a, b). Both Curcumin and Diclofenac administrations were able to upregulate the Bad and Bax expression. The elevated expression of Bad and Bax in paraffin sections in DMH + Curcumin and DMH + Diclofenac groups further showed that both Curcumin and Diclofenac triggered the mitochondrial pathway of apoptosis (Fig. 6a–e; Suppl. Fig. 3a–c). The extent of apoptosis is more in DMH + Curcumin + Diclofenac group. In silico studies further showed that both Diclofenac and Curcumin efficiently docked in the active site of Bcl-2. The structures of docked complex of Bcl-2 with Diclofenac and Curcumin are shown in Suppl. Fig. 3c, d. Diclofenac docked at the active site of Bcl-2, forming H-bond with Glu-133 residue and with glide score −6.82 (Suppl. Fig. 3c; Suppl. Table 2). Curcumin also docked efficiently forming H-bonds with Arg-143 and with glide score −7.25 (Suppl. Fig. 3d; Suppl. Table 2).
Degree of apoptosis in isolated colonocytes by AO/EB co-staining after 6 week treatment. a Fluorescence microscopic images (×400) of isolated colonocytes from various treatment groups. Viable cells appeared green, while apoptotic cells appeared yellow (arrows). Very few apoptotic cells were seen in DMH group as compared to control; however, significant amount of apoptotic cells was seen in DMH + Diclofenac and DMH + Curcumin groups as compared to DMH. Apoptotic cells were significantly higher in DMH + Diclofenac + Curcumin group. b Graph represents the percentage of apoptotic cells in different groups. Values are mean ± SD of three animals. a p ≤ 0.05 and c p ≤ 0.001 in comparison to control and z p ≤ 0.001 in comparison to DMH by one-way ANOVA. (Color figure online)
a Western blot analysis of anti-apoptotic protein Bcl-2 and pro-apoptotic Bad and Bax in various treatment groups. β-Actin is serving as loading control. b Quantitative analysis of the blots in densitometric units. Values are mean ± SD of three animals. c p ≤ 0.001 in comparison to control and z p ≤ 0.001 in comparison to DMH by one-way ANOVA. c Validation of RT-PCR results was done by quantitative real-time polymerase chain reaction, PCR (qRT-PCR). β-Actin served as a reference gene for the normalization of expression profiles in each group. Values are mean ± SD of three animals. b p ≤ 0.01 and c p ≤ 0.001 in comparison to control and y p ≤ 0.01 and z p ≤ 0.001 in comparison to DMH by one-way ANOVA. d Expression of Bcl-2 in the colonic tissue paraffin sections (arrows) was analyzed by immunofluorescence. DMH group showed higher expression and localization of Bcl-2 (arrows) as compared to the other groups. e Expression of Bad in the colonic tissue paraffin sections (arrows) was analyzed by immunofluorescence. DMH + Diclofenac and DMH + Curcumin groups showed higher expression and localization of Bad (arrows) as compared to the DMH group. f Expression of Bax in the colonic tissue paraffin sections (arrows) was analyzed by immunofluorescence. DMH + Diclofenac and DMH + Curcumin groups showed higher localization of Bax (arrows) as compared to the DMH group
The expression of Cyt c and Apaf-1 was observed higher in DMH + Curcumin and DMH + Diclofenac group as shown by western blot (Fig. 7a, b). It further showed the lower expression of caspase-3 and -9 in DMH group which was reverted back to normal in DMH + Diclofenac and DMH + Curcumin group (Fig. 7a, b). These findings validate the importance of the apoptosome formation and caspase cascade activation in the mitochondrial pathway of apoptosis.
a Western blot analysis of Apaf-1, Cyt c, caspase-3, and caspase-9 proteins in various treatment groups. DMH + Diclofenac and DMH + Curcumin groups showed higher expression of Apaf-1, Cyt c, caspase-3, and caspase-9 as compared to DMH. β-Actin is serving as loading control. b Quantitative analysis of the blots in densitometric units. Values are mean ± SD of three animals. a p ≤ 0.05, b p ≤ 0.01, and c p ≤ 0.001 in comparison to control and z p ≤ 0.001 in comparison to DMH by one-way ANOVA
Diclofenac and Curcumin downregulate ΔΨ M while increasing ROS production
Mitochondrial membrane potential (ΔΨ M) has been measured by photoselective laser dye R123. Quantification via flow cytometry showed an increased percentage of higher ΔΨ M colonocytes in DMH group (Fig. 8a, b). Curcumin and Diclofenac co-administration after DMH treatment reverted back the percentage of colonocytes having both higher ΔΨ M and lower ΔΨ M toward control group (Fig. 8a, b). Spectrofluorometric analysis also showed the increased R123 intensity in the DMH group (Fig. 8c), while fluorescent microscopy showed the presence of more number of higher ΔΨ M colonocytes in DMH group (Fig. 8d, e).
a Measurement of ΔΨ M in isolated colonocytes from various treatment groups by R123 as assessed by flow cytometry. Histogram showing relative values of R123 fluorescence on FL-2H channel (x-axis) with cell count (y-axis). b Graph showing the mean percentage of cells with higher and lower ΔΨ M in various treatment groups. A total of 104 events were recorded. DMH group showed higher mean percentage of cells with higher ΔΨ M as compared to control. a p ≤ 0.05 and c p ≤ 0.001 in comparison to control and y p ≤ 0.01 and z p ≤ 0.001 in comparison to DMH by one-way ANOVA. c Graph representing spectroscopic analysis of R123 stained colonocytes. DMH group showed high fluorescence intensity as compared to control. Values are mean ± SD of three animals. a p ≤ 0.05 and c p ≤ 0.001 in comparison to control and z p ≤ 0.001 in comparison to DMH by one-way ANOVA. d Fluorescence microscopic images (×400) of isolated colonocytes from various treatment groups stained with R123 fluorescent dye for the analysis of ΔΨ M. Brighter fluorescence with R123 suggests higher ΔΨ M (as shown by white arrows). DMH group is having more cells showing higher mitochondrial potential as compared to control. e Graph represents mean number of cell counted (a total of 300 cells from four different slides were observed for each animal group) under the fluorescent microscope. Values are mean ± SD of three animals. b p ≤ 0.01 and c p ≤ 0.001 in comparison to control and y p ≤ 0.01 and z p ≤ 0.001 in comparison to DMH by one-way ANOVA
Intracellular levels of ROS were estimated using the fluorescent probe, DCFH-DA. Flowcytometric analysis has shown more percentage of colonocytes with higher intracellular ROS in DMH + Diclofenac and DMH + Curcumin groups (Fig. 9a, b). Spectrofluorometric analysis also showed the lower ROS production in DMH group (Fig. 9c).
a Measurement of ROS production in isolated colonocytes from various treatment groups by changes in the fluorescence intensity of DCF. Histogram showing flow cytometric analysis of DCFH-DA on FL-1H channel (x-axis) with cell count (y-axis). b Graph represents mean percentage of cell (out of 104 events) with higher ROS (high DCF fluorescence). DMH + Diclofenac and DMH + Curcumin groups showed higher mean percentage of colonocytes having higher ROS as compared to DMH. Values are mean ± SD of three animals. b p ≤ 0.01 and c p ≤ 0.001 in comparison to control and y p ≤ 0.01 and z p ≤ 0.001 in comparison to DMH by one-way ANOVA. c Spectro-fluorimetric analysis of ROS production as assessed by DCFH-DA in isolated colonocytes of various treatment groups. The values are mean ± SD of four animals. c p ≤ 0.001 in comparison to control and z p ≤ 0.001 in comparison to DMH by one-way ANOVA
Discussion
Over the years, natural products have played a significant role in the development of anticancer drugs, as 60 % of the drugs are of natural origin [28]. Accumulating evidences had shown that a natural polyphenolic compound Curcumin has a potent anticancer effect both in vitro and in vivo on a variety of cancers including colorectal cancer [29, 30]. Curcumin is already used clinically and is approved by the Food and Drug Administration (USA) as a safe food additive, as Curcumin up to 12 g/day was safely administered to humans without major toxicity in Phase-I clinical studies [31, 32]. NSAIDs have also become promising anti-cancer agents because these can initiate apoptosis in the cancer cells [22, 33], and induction of apoptosis is becoming an important preventive approach [34]. In this regard, the present study has shown that both Curcumin, a preferential COX-2 inhibitor NSAID, and Diclofenac induce apoptosis in chemoprevention of DMH-induced colon carcinogenesis in rat model, and the chemopreventive effect is enhanced when both the drugs were administered together. The dose of the Curcumin (50 mg/kg b.w.) and Diclofenac (8 mg/kg b.w.) as taken in the present study is in good agreement of the anti-inflammatory dose range of the drugs, as shown by carrageenan-induced foot paw edema. Morphological examinations of the dissected colons from different animal groups showed that Curcumin and Diclofenac co-administration reduced the number of MPLs which are the macroscopic sites for tumor growth, suggesting that both the drugs inhibit tumor growth in the initiation stage of neoplasm.
PI3-K–Akt signaling pathway is believed to play an important role in the genesis of some human cancers and is associated with cell proliferation, survival, and metastasis [35]. Also the activation of the PI3-K/Akt pathway confers chemotherapeutic resistance in numerous tumor types including colon cancer [36]. Therefore, the suppression of PI3-K/Akt signaling pathway is considered as a promising strategy for cancer treatment. The hyperactivation of Akt results in tumor cell survival and enhanced resistance to apoptosis through multiple signaling mechanisms [37]. Akt is activated upon its recruitment to membrane through the N-terminus pleckstrin homology domain which binds to PIP3 synthesized by PI3-K and then phosphorylation at Thr-308 by PDK1, which is also recruited to the plasma membrane by PIP3 [38, 39]. Our data showed an elevated expression of Akt in DMH-treated groups, both at transcriptional and translational levels, thus signifying its principal role in cancer. However, co-administration of Curcumin and Diclofenac significantly inhibited the elevated levels of PI3-K and PDK1 in DMH-treated animals and thereby downregulating the activation (phosphorylation) of Akt. Akt phosphorylation is a tightly regulated process, representing a balance between kinase-activating and phosphatase-inactivating events [40]. Several protein phosphatases, including the dual protein/lipid phosphatase PTEN which transforms PIP3 into PIP2, and canonical PP1 and PP2A were reported to bind and dephosphorylate Akt in an agonist-dependent manner [41]. In the present study, Curcumin and Diclofenac upregulated the PTEN expression, demonstrating that both the drugs can regulate the observed Akt level via enhancing PTEN expression.
In silico molecular docking is one of the most powerful techniques to discover novel ligands for receptors of known structure and may have tremendous impact in the prognosis of the disease [42]. Our results showed that Diclofenac efficiently docked into the ATP-binding site of PI3-K and therefore can inhibit PI3-K by obstructing the binding of ATP with PI3-K. Both Diclofenac and Curcumin docked into the ATP-binding site of Akt demonstrating that both may inhibit the kinase activity of Akt. However, Curcumin could not be docked into the ATP-binding site of PI3-K suggesting that the path followed by Curcumin to inhibit PI3-K may be some other uncharted pathway, perhaps by modulating other proteins like PDK1, PTEN, and Akt.
Apoptosis is an essential process leading to the programmed cell death and involves distinct morphological and biochemical changes that activate the evolutionarily conserved intracellular pathways to inhibit cancer growth and proliferation [43]. Apoptosis is controlled via two major pathways, including one that originates at the cell membrane (extrinsic) and another that involves mitochondria (intrinsic) [44]. Previous studies had suggested that Bcl-2 family of proteins plays a central role in the regulation of mitochondrial-dependent apoptosis [45]. The Bcl-2 family of proteins consisting of pro-apoptotic Bad, Bax, Bid, etc., and anti-apoptotic Bcl-2 and Bcl-xL are important regulators of apoptosis [46]. The balance between pro- and anti-apoptotic members of the Bcl-2 family determined the fate of the cells exposed to apoptotic signals [47]. Studies have suggested that Bcl-2 could be a crucial mediator downstream of PI3-K/Akt signaling, whereas activated Akt has been shown to promote cell survival and block apoptosis by downregulating the activity of pro-apoptotic members of the Bcl-2 family [48]. Akt prevents apoptosis by phosphorylation of the pro-apoptotic protein Bad and thus prevents its binding to the Bcl-xL and Bcl-2 anti-apoptotic family members [49]. Our results showed that Bcl-2 is highly expressed both at transcriptional and translational level in DMH group which revealed that Bcl-2 regulates the mitochondrial pathway of apoptosis and promote carcinogenesis. Both Curcumin and Diclofenac decreased Bcl-2 expression and increased the Bad and Bax expression both at transcriptional and translational level, signifying that both can initiate mitochondrial pathway of apoptosis. These findings further support the fact that Akt modulates cell survival pathway by regulating Bcl-2 expression. It has also been suggested that additional mechanisms might exist for the cell survival-promoting and apoptosis-inhibiting action of Akt [50].
As the apoptosis triggers, translocation of Bax to mitochondria and decreased expression of Bcl-2 resulted in permeabilization of mitochondria and the release of Cyt c, which further activated the caspase cascade [51]. A change in mitochondrial membrane permeability is essential for translocation of apoptogenic Cyt c and apoptosis-inducing factor into the cytoplasm [52]. In the cytosol, Cyt c oligomerizes with Apaf-1, procaspase-9, and ATP to form apoptosomes [53]. The results from the present study showed the elevated expression of Cyt c and Apaf-1 after Curcumin and Diclofenac administration as compared to DMH signifying the importance of apoptosome formation in apoptosis. Apoptosome formation leads to caspase-9 activation through induced proximity and subsequently culminates in proteolytic cleavage and thereby activation of the downstream executioner caspases-3 and -7 [54]. Activation of caspases is considered as a point of no return in the apoptotic process [55]. Activated caspase-3 is the key mediator of cell apoptosis cleaving intracellular proteins vital for cell survival and growth, such as PARP. The increased expression of caspased-9 and -3 after Curcumin and Diclofenac administration showed that both the drugs can activate caspases to induce apoptosis. However, the decreased expression of caspases-9 and -3 after DMH treatment showed that their inhibition may block apoptosis.
ROS are highly reactive metabolites generated during normal cell metabolism and have been established as key contributors to the regulation of apoptosis [56]. Indeed, the mitochondrial apoptotic signaling pathway has been described as an important downstream event mediated by ROS in apoptotic cell death [57]. ROS mediated the early as well as late steps of apoptosis that is associated with loss of mitochondrial membrane potential, release of Cyt c, and activation of caspase-3 [58]. Both Curcumin and Diclofenac increased the ROS generation which suggested that elevated intracellular ROS could be sufficient to trigger apoptosis. However, decreased ROS level in DMH as compared to control may suggest that cancer cells are more sensitive to excess ROS than the normal one. Higher number of high mitochondrial potential cells was found in DMH-treated animals, whereas their number decreased after co-administration with Diclofenac and Curcumin, further suggesting that the reduction or loss of ΔΨ M is an early indicator of apoptosis.
In conclusion, the present study showed that Diclofenac and Curcumin exert their anti-neoplastic effect by inhibition of PI3-K/Akt pathway. Akt inhibition was coupled with activation of mitochondrial apoptotic mechanism that is associated with significant increase in expression of pro-apoptotic Bcl-2 family members (Bad and Bax), decrease in anti-apoptotic Bcl-2 protein, and significant increase in caspases-3 and -9 levels. Both Diclofenac and Curcumin do stimulate apoptosis probably by activating apoptosome formation, increasing ROS generation, and decreasing ΔΨ M. Also, the anti-neoplastic effect is enhanced when both Diclofenac and Curcumin are administered together.
References
Jacobson MD, Weil M, Raff MC (1997) Programmed cell death in animal development. Cell 88:347–354
Danial NN, Korsmeyer SJ (2004) Cell death: critical control points. Cell 116:205–219
Ferreira CG, Epping M, Kruyt FA, Giaccone G (2002) Apoptosis: target of cancer therapy. Clin Cancer Res 8:2024–2034
Engelman JA (2009) Targeting PI3K signalling in cancer: opportunities, challenges and limitations. Nat Rev Cancer 9:550–562
Manning BD, Cantley LC (2007) AKT/PKB signaling: navigating downstream. Cell 129:1261–1274
Spencer JP, Rice-Evans C, Williams RJ (2003) Modulation of pro-survival Akt/protein kinase B and ERK1/2 signaling cascades by quercetin and its in vivo metabolites underlie their action on neuronal viability. J Biol Chem 2:34783–34793
Vivanco I, Sawyers CL (2002) The phosphatidylinositol 3-kinase AKT pathway in human cancer. Nat Rev Cancer 2:489–501
Parsons R (2004) Human cancer, PTEN and the PI-3 kinase pathway. Semin Cell Dev Biol 15:171–176
Franke TF, Hornik CP, Segev L et al (2003) PI3K/Akt and apoptosis: size matters. Oncogene 22:8983–8998
Pugazhenthi S, Nesterova A, Sable C et al (2000) Akt/protein kinase B up-regulates Bcl-2 expression through cAMP-response element-binding protein. J Biol Chem 275:10761–10766
Surh YJ (2003) Cancer chemoprevention with dietary phytochemicals. Nat Rev Cancer 3:768–780
Rarnsewak RS, DeWitt DL, Nair MG (2003) Cytotoxicity, antioxidant and anti-inflammatory activities of Curcumins I–III from Curcuma longa. Phytomedicine 7:303–308
Goel A, Kunnumakkara AB, Aggarwal BB (2008) Curcumin as “Curecumin”: from kitchen to clinic. Biochem Pharmacol 75:787–809
Gou M, Men K, Shi HS et al (2011) Curcumin-loaded biodegradable polymeric micelles for colon cancer therapy in vitro and in vivo. Nanoscale 3:1558–1567
Torrance CJ, Jackson PE, Montgomery E et al (2000) Combinatorial chemoprevention of intestinal neoplasia. Nat Med 6:1024–1028
Saini MK, Vaish V, Sanyal SN (2013) Role of cytokines and Jak3/Stat3 signaling in the 1,2-dimethylhydrazine dihydrochloride-induced rat model of colon carcinogenesis: early target in the anticancer strategy. Eur J Cancer Prev 23:215–228
Piplani H, Rana C, Vaish V, Sanyal SN (2013) Dolastatin, along with Celecoxib, stimulates apoptosis by a mechanism involving oxidative stress, membrane potential change and PI3-K/AKT pathway down regulation. Biochim Biophys Acta Gen Subj 1830:5142–5156
Rana C, Vaish V, Piplani H, Nehru B, Sanyal SN (2012) Nuclear Factor-κB is expressed in early colon cancer and its down-regulation by Curcumin and Diclofenac is associated with the suppression of proliferation and the induction of apoptosis. Biomed Prev Nutr 2:228–238
Abdelwahab SI, Koko WS, Taha MME et al (2012) In vitro and in vivo anti-inflammatory activities of columbin through the inhibition of cycloxygenase-2 and nitric oxide but not the suppression of NF-κB translocation. Eur J Pharmacol 678:61–70
Winter CA, Risley EA, Nuss GW (1962) Carrageenan-induced oedema in the hind paw of rat as an assay for anti-inflammatory activity. Proc Soc Exp Biol Ther 111:544–547
Piplani H, Rana C, Vaish V, Sanyal SN (2013) Up-regulation of p53 and mitochondrial signalling pathway in apoptosis by a combination of COX-2 inhibitor, Celecoxib and Dolastatin 15, a marine mollusk linear peptide in experimental colon carcinogenesis. Mol Carcinog 52:845–858
Vaish V, Piplani H, Rana C, Sanyal SN (2013) Angiostatic Properties of Sulindac and Celecoxib in the experimentally induced inflammatory colorectal cancer. Cell Biochem Biophys 66:205–227
Bradford MM (1976) A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein–dye binding. Anal Biochem 72:248–254
Mouille B, Robert V, Blacheir F (2012) Adaptative increase of ornithine production and decrease of ammonia metabolism in rat colonocytes after hyperproteic diet ingestion. J Physiol Gastrointest Liver Physiol 278:G344–G351
Piccagli L, Fabbri E, Borgatti M (2008) Docking of molecules identified in bioactive medicinal plants extracts into the p50 NF-kappaB transcription factor: correlation with inhibition of NF-kappaB/DNA interactions and inhibitory effects on IL-8 gene expression. BMC Struct Biol 8:38
Johnson LV, Walsh ML, Chen LB (1980) Localization of mitochondria in living cells with rhodamine 123. Proc Natl Acad Sci USA 177:990–994
LeBel CP, Ischiropoulos H, Bondy SC (1992) Evaluation of the probe 2′,7′-dichlorofluorescein as an indicator of reactive oxygen species formation and oxidative stress. Chem Res Toxicol 5:227–231
Gupta SC, Kim JH, Prasad S (2010) Regulation of survival, proliferation, invasion, angiogenesis, and metastasis of tumor cells through modulation of inflammatory pathways by nutraceuticals. Cancer Metastasis Rev 29:405–434
Aggarwal BB, Harikumar KB (2009) Potential therapeutic effects of curcumin, the anti-inflammatory agent, against neurodegenerative, cardiovascular, pulmonary, metabolic, autoimmune and neoplastic diseases. Int J Biochem Cell Biol 41:40–59
Park J, Conteas CN (2010) Anti-carcinogenic properties of curcumin on colorectal cancer. World J Gastrointest Oncol 22:169–176
Cheng AL, Hsu CH, Lin JK et al (2001) Phase I clinical trial of curcumin, a chemopreventive agent, in patients with high-risk or pre-malignant lesions. Anticancer Res 21:2895–2900
Sharma RA, McLelland HR, Hill KA (2001) Pharmacodynamic and pharmacokinetic study of oral Curcuma extract in patients with colorectal cancer. Clin Cancer Res 7:1894–1900
Wakabayashi K (2000) NSAIDs as cancer preventive agents. Asian Pac J Cancer Prev 1:97–113
Sun SY, Hail NJ, Lotan R (2004) Apoptosis as a novel target for cancer chemoprevention. J Natl Cancer Inst 5:662–672
Ahmad A, Biersack B, Li Y et al (2013) Deregulation of PI3K/Akt/mTOR signaling pathways by isoflavones and its implication in cancer treatment. Anticancer Agents Med Chem 13:1014–1024
Benistant C, Chapuis H, Roche S (2000) A specific function for phosphatidylinositol 3-kinase alpha (p85alpha–p110alpha) in cell survival and for phosphatidylinositol 3-kinase beta (p85alphap110beta) in de novo DNA synthesis of human colon carcinoma cells. Oncogene 19:5083–5090
Madhunapantula SV, Mosca PJ, Robertson GP (2011) The Akt signaling pathway: an emerging therapeutic target in malignant melanoma. Cancer Biol Ther 12:1032–1049
Bayascas JR (2010) PDK1: the major transducer of PI 3-kinase actions. Curr Top Microbiol 346:9–29
Raimondi MF (2011) Targeting PDK1 in cancer. Curr Med Chem 18:2763–2769
Yamada KM, Araki M (2001) Tumor suppressor PTEN, Modulator of cell signalling, growth, migration, and apoptosis. J Cell Sci 114:2375–2382
Van Kanegan MJ, Adams DJ, Wadzinski BE et al (2005) Distinct protein phosphatase 2A heterotrimers modulate growth factor signaling to extracellular signal-regulated kinases and AKT. J Biol Chem 280:36029–36036
Brooijmans N, Kuntz ID (2003) Molecular recognition and docking algorithms. Annu Rev Biophys Biomol Struct 32:335–373
Hengartner MO (2000) The biochemistry of apoptosis. Nature 407:770–776
Liu Y, Borchert GL, Surazynski A et al (2006) Proline oxidase activates both intrinsic and extrinsic pathways for apoptosis: the role of ROS/superoxides, NFAT and MEK/ERK signalling. Oncogene 25:5640–5647
Herman-Antosiewicz A, Powolny AA, Singh SV (2007) Molecular targets of cancer chemoprevention by garlic-derived organosulfides. Acta Pharmacol Sin 28:1355–1364
Adams JM, Cory S (2007) The Bcl-2 apoptotic switch in cancer development and therapy. Oncogene 26:1324–1337
Fletcher JI, Meusburger S, Hawkins CJ et al (2008) Apoptosis is triggered when prosurvival Bcl-2 proteins cannot restrain Bax. Proc Natl Acad Sci USA 2008(105):18081–18087
Maddika S, Ande SR, Panigrahi S et al (2007) Cell survival, cell death and cell cycle pathways are interconnected: implications for cancer therapy. Drug Resist Update 10:13–29
Asnaghi L, Calastretti A, Bevilacqua A (2004) Bcl-2 phosphorylation and apoptosis activated by damaged microtubules require mTOR and are regulated by Akt. Oncogene 23:5781–5791
Rathmell JC, Fox CJ, Plas DR et al (2003) Akt-directed glucose metabolism can prevent Bax conformation change and promote growth factor-independent survival. Mol Cell Biol 23:7315–7328
Kandasamy K, Srinivasula SM, Alnemri ES et al (2003) Involvement of proapoptotic molecules Bax and Bak in tumor necrosis factor-related apoptosis-inducing ligand (TRAIL)-induced mitochondrial disruption and apoptosis: differential regulation of cytochrome c and Smac/DIABLO release. Cancer Res 63:1712–1721
Kroemer G, Galluzz L, Brenner C (2007) Mitochondrial membrane permeabilization in cell death. Physiol Rev 87:99–163
Zou H, Li Y, Liu X et al (1997) An APAF-1.cytochrome c multimeric complex is a functional apoptosome that activates procaspase-9. J Biol Chem 23:11549–11597
Varghese J, Khandre NS, Sarin A (2008) Caspase-3 activation is an early event and initiates apoptotic damage in a human leukemia cell line. Apoptosis 8:363–370
Torkin R, Lavoi JF, Kaplan DR et al (2005) Induction of caspase-dependent, p53-mediated apoptosis by apigenin in human neuroblastoma. Mol Cancer Ther 4:1–11
Circu ML, Aw TW (2010) Reactive oxygen species, cellular redox systems, and apoptosis. Free Radic Biol Med 8:749–762
Miki H, Funato Y (2012) Regulation of intracellular signalling through cysteine oxidation by reactive oxygen species. J Biochem 151:255–261
Ying C, Geert A, Martens SA et al (2007) Increased oxygen radical formation and mitochondrial dysfunction mediate beta cell apoptosis under conditions of AMP-activated protein kinase stimulation. Free Radic Biol Med 42:64–78
Acknowledgments
Financial assistance from the Department of Atomic Energy (DAE) and Board of Research in Nuclear Physics (BRNS), Govt. of India (2009/37/45/BRNS) is gratefully acknowledged. We also acknowledge the contributions of Dr. Ravi Kumar Muttineni, Application Specialist, Schrodinger, India for helping us in performing the docking studies.
Conflict of interest
Authors have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Rana, C., Piplani, H., Vaish, V. et al. Downregulation of PI3-K/Akt/PTEN pathway and activation of mitochondrial intrinsic apoptosis by Diclofenac and Curcumin in colon cancer. Mol Cell Biochem 402, 225–241 (2015). https://doi.org/10.1007/s11010-015-2330-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-015-2330-5