Abstract
Mitochondria have a crucial role in the supply of energy to the brain. Mitochondrial alterations can lead to detrimental consequences on the function of brain cells and are thought to have a pivotal role in the pathogenesis of several neurologic disorders. This study was aimed to evaluate mitochondrial function, fusion–fission and biogenesis and autophagy in brain cortex of 6-month-old Goto–Kakizaki (GK) rats, an animal model of nonobese type 2 diabetes (T2D). No statistically significant alterations were observed in mitochondrial respiratory chain and oxidative phosphorylation system. A significant decrease in the protein levels of OPA1, a protein that facilitates mitochondrial fusion, was observed in brain cortex of GK rats. Furthermore, a significant decrease in the protein levels of LC3-II and a significant increase in protein levels of mTOR phosphorylated at serine residue 2448 were observed in GK rats suggesting a suppression of autophagy in diabetic brain cortex. No significant alterations were observed in the parameters related to mitochondrial biogenesis. Altogether, these results demonstrate that during the early stages of T2D, brain mitochondrial function is maintained in part due to a delicate balance between mitochondrial fusion–fission and biogenesis and autophagy. However, future studies are warranted to evaluate the role of mitochondrial quality control pathways in late stages of T2D.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Diabetes mellitus has become a worldwide epidemic with a substantial social and economic burden [1]. As a matter of fact, the prevalence of this disorder is rising dramatically, being estimated that 370 million people worldwide will be suffering from diabetes in 2030 [2]. Based on its etiology and clinical presentation, diabetes is mainly categorized in type 1 (T1D) or type 2 (T2D) diabetes [3]. T2D is the most prevalent form of diabetes and is marked by chronic hyperglycemia as a consequence of insulin resistance and partial insulin deficiency [3]. Among the wide range of chronic complications associated with diabetes, brain degenerative events, cognitive deterioration and dementia have assumed a pivotal importance in the last decades [4]. Particularly, diabetes is considered a major risk factor for the development of Alzheimer’s and Parkinson’s diseases [5, 6]. While the mechanistic link between diabetes and neurodegeneration remains enigmatic, scientific advances revealed that mitochondria could be in the basis of this interrelation [5–7]. In fact, mitochondria take center stage in the brain since neurons have a limited glycolytic capacity, making them highly dependent on aerobic oxidative phosphorylation to fulfill their energetic requirements [8]. Aside from their role in ATP generation, these organelles are also involved in the homeostasis of important cellular second messengers such as reactive oxygen species (ROS) and Ca2+ as well as in the control of apoptotic cell death [8].
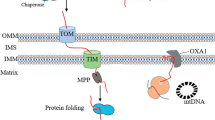
To ensure the maintenance of a healthy mitochondrial population, brain cells are equipped with mitochondrial quality control systems to regulate mitochondrial shape, function and mass. These mitochondrial quality control systems include, but are not restricted to mitochondrial fusion–fission, biogenesis and autophagy [9]. The frequent and balanced cycles of fusion and fission are crucial for neurons, given their unique architecture and special energy and Ca2+-buffering requirements at the synapse [10]. The core molecular machinery involved in mitochondrial fusion includes optic atrophy 1 (OPA1) and mitofusins 1 and 2 (Mfn1 and Mfn2, respectively). Whereas OPA1 can be found and is responsible for mitochondrial inner membrane fusion, Mfn1 and Mfn2 are found and are responsible for mitochondrial outer membrane fusion [11]. On the other hand, dynamin-related protein 1 (DRP1) and fission protein 1 (Fis1) are involved in mitochondrial fission [11]. Degradation of mitochondria through autophagy, usually termed as mitophagy, constitutes an important quality control process that degrades damaged/dysfunctional mitochondria [12].
So far, the role of mitochondrial quality control mechanisms has not been investigated in the early stages of diabetic brain. Taking into account that the maintenance of a healthy mitochondrial pool is crucial for normal brain functioning, the present study was aimed to uncover the impact of moderate T2D on brain cortical mitochondrial function, fission–fusion and biogenesis and autophagy. For that, several parameters were determined in the brains of 6-month-old Goto–Kakizaki (GK) rats: respiratory chain function, oxidative phosphorylation system, mitochondrial fusion–fission proteins levels, mitochondrial mtDNA copy number, protein levels of mitochondrial biogenesis-related transcription factors and markers of autophagy.
Materials and methods
Reagents
Bacterial protease from Bacillus licheniformis—type VIII, bovine serum albumin (BSA), phenylmethylsulfonyl fluoride (PMSF), dithiothreitol (DTT) and Tween 20 were obtained from Sigma-Aldrich (St. Louis, MO, USA). Digitonin was obtained from Calbiochem. Polyvinylidene difluoride (PVDF) Immobilon-P membranes were obtained from Millipore (Billerica, MA, USA). Enhanced chemifluorescence (ECF) reagent was obtained from Amersham Biosciences (Little Chalfont, UK). All the other chemicals used were of the highest grade of purity commercially available.
Animals housing and treatment
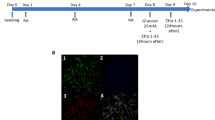
GK and respective Wistar control rats were obtained from our animal colony (Laboratory Research Center, Faculty of Medicine, University of Coimbra) and maintained under controlled light (12-h day/night cycle) and humidity with ad libitum access to water and powdered rodent chow. GK rats are nonobese and spontaneously diabetic animals produced by selective breeding of Wistar rats. Following procedures approved by the Federation of European Laboratory Animal Science Associations (FELASA), fasted 6-month-old animals were sacrificed by decapitation.
Measurements of biochemical parameters
Blood glucose was determined immediately after sacrifice by a glucose oxidase reaction, using a glucometer (Glucometer-Elite, Bayer). Glycated hemoglobin (HbA1c) levels were determined using Systems SYNCHRON CX 4 (Beckman). This system utilizes two cartridges, Hb and A1c to determine A1c concentration as a percentage of the total Hb. The hemoglobin is measured by a colorimetric method and the A1c concentration by a turbidimetric immunoinhibition method.
Preparation of mitochondrial fraction
Brain cortical mitochondria were isolated from rats by the method of Moreira et al. [13], using 0.02 % digitonin to allow the release of mitochondria from the synaptosomal fraction. Briefly, after animal decapitation, the cortex was immediately separated and homogenized at 4 °C in 10 ml of isolation medium (225 mM mannitol, 75 mM sucrose, 5 mM HEPES, 1 mM EGTA, 1 mg/ml BSA, pH 7.4) containing 5 mg of the bacterial protease (Sigma). Single brain homogenates were brought to 30 ml and then centrifuged at 2,000g for 5 min. The resulting supernatant was then centrifuged at 12,000g for 10 min. The pellet, including the fluffy synaptosomal layer, was resuspended in 10 ml of the isolation medium containing 0.02 % digitonin and centrifuged at 12,000g for 10 min. The brown mitochondrial pellet without the synaptosomal layer was resuspended again in 10 ml of medium and centrifuged at 12,000g for 5 min. The pellet was resuspended in 10 ml of washing medium (225 mMmannitol, 75 mM sucrose, 5 mM HEPES, pH 7.4) and centrifuged at 12,000 g for 5 min. The final mitochondrial pellet was resuspended in the washing medium and the protein amount determined by the biuret method calibrated with BSA [14].
Measurements of mitochondrial respiration
Oxygen consumption of mitochondria was registered polarographically with a Clark oxygen electrode [15] connected to a suitable recorder in a thermostated water-jacketed closed chamber with magnetic stirring. The reactions were carried out at 30 °C in 1 ml of standard respiratory medium (100 mM sucrose, 100 mM KCl, 2 mM KH2PO4, 5 mM Hepes and 10 μM EGTA; pH 7.4) with 0.5 mg of protein. State 3 of respiration (consumption of oxygen in the presence of substrate and ADP) was initiated with ADP (50 nmol/mg protein). States 3 and 4 (consumption of oxygen after ADP phosphorylation) of respiration, respiratory control ratio (RCR = State 3/State 4) and ADP/O index (a marker of the mitochondrial ability to couple oxygen consumption to ADP phosphorylation during State 3 of respiration) were determined according to Chance and Williams [16].
Measurements of ΔΨ m
The transmembrane potential (ΔΨ m) was monitored by evaluating the transmembrane distribution of the lipophilic cation TPP+ (tetraphenylphosphonium) with a TPP+-selective electrode prepared according to Kamo et al. [17] using an Ag/AgCl-saturated electrode (Tacussel, model MI 402) as reference. TPP+ uptake has been measured from the decreased TPP+ concentration in the medium sensed by the electrode. The potential difference between the selective electrode and the reference electrode was measured with an electrometer and recorded continuously in a Linear 1200 recorder. The voltage response of the TPP+ electrode to log[TPP+] was linear with a slope of 59 ± 1, which is in a good agreement with the Nernst equation. Reactions were carried out in a chamber with magnetic stirring in 1 ml of the standard medium (100 mM sucrose, 100 mM KCl, 2 mM KH2PO4, 5 mM Hepes and 10 μM EGTA; pH 7.4) containing 3 μM TPP+. This TPP+ concentration was chosen in order to achieve high sensitivity in measurements and to avoid possible toxic effects on mitochondria [18]. The ΔΨ m was estimated by the equation: ΔΨ m (mV) = 59 log(v/V) − 59 log(10ΔE/59 − 1), as indicated by Kamo et al. [17] and Muratsugu et al. [19]. v, V and ΔE stand for mitochondrial volume, volume of the incubation medium and deflection of the electrode potential from the baseline, respectively. This equation was derived assuming that TPP+ distribution between the mitochondria and the medium follows the Nernst equation and that the law of mass conservation is applicable. A matrix volume of 1.1 μl/mg protein was assumed. No correction was made for the “passive” binding contribution of TPP+ to the mitochondrial membranes, because the purpose of the experiments was to show relative changes in potentials rather than absolute values. As a consequence, we can anticipate a slight overestimation on ΔΨ m values. However, the overestimation is only significant at ΔΨ m values below 90 mV, therefore, far from our measurements. Mitochondria (0.5 mg/ml) were energized with 5 mM succinate (substrate of complex II) in the presence of 2 μM rotenone (inhibitor of complex I) in order to activate the mitochondrial electron transport chain. After a steady-state distribution of TPP+ had been reached (ca. 1 min of recording), ΔΨ m fluctuations were recorded.
Protein extraction for Western blot analysis
Brain cortical tissue was homogenized in radio immunoprecipitation assay (RIPA) buffer containing 0.1 M PMSF, 0.2 M DTT, and protease and phosphatase inhibitors (commercial protease and phosphatase inhibitor cocktails from Roche Applied Science). The crude homogenate was incubated on ice for 15 min, frozen and defrozen 3 times to favor disruption, centrifuged at 20,000g for 10 min, at 4 °C, and the resulting supernatant collected and stored at −80 °C. The amount of protein content in the samples was analyzed by the bicinchoninic acid (BCA) protein assay using the BCA kit (Pierce Thermo Fisher Scientific, Rockford, IL).
Western blot analysis
The samples (50–75 μg per lane) were resolved by electrophoresis in 8–15 % sodium dodecyl sulfate (SDS)–polyacrylamide gels and transferred to PVDF membranes. Nonspecific binding was blocked by gently agitating the membranes in 5 % nonfat milk or 5 % BSA for phosphoproteins and 0.05 % Tween in Tris-buffered saline (TBS) for 1 h at room temperature. The blots were subsequently incubated with specific primary antibodies, overnight at 4 °C, with gentle agitation. Blots were washed three times (15 min), with Tris buffer containing 0.05 % Tween (TBS-T) and then were incubated with secondary antibodies for 1 h at room temperature with gentle agitation. After three washes with TBS-T, specific bands of immunoreactive proteins were visualized after membrane incubation with ECF for 5 min in a VersaDoc Imaging System (Bio-Rad), and the density of protein bands was calculated using the Quantity One Program (Bio-Rad). The primary antibodies used were: anti-Mfn1 (1:1,000; Santa Cruz Biotechnology); anti-Mfn2 (1:1,000; Santa Cruz Biotechnology); anti-OPA1 (1:1,000; BD Biosciences); anti-Fis1 (1:750; Imgenex); anti-DRP1 (1:1,000; BD Biosciences); anti-pser616 DRP1 (1:1,000; Cell Signaling); anti-mTOR (1:1,000; Cell Signaling); anti-pser2448 mTOR (1:1,000; Cell Signaling); anti-Beclin 1 (1:1,000; BD Biosciences); anti-LC3-II (1:1,000; Sigma); anti-Parkin (1:1,000; Abcam); anti-p62 (1:1,000; Sigma); anti-NRF1 (1:500; Santa Cruz Biotechnology); anti-TFAM (1:1,000; Santa Cruz Biotechnology); anti-ND1 (1:500; Santa Cruz Biotechnology); anti-MTCOI (1:1,000; Abcam); anti-beta actin (1:5,000; Sigma). The secondary antibodies used were: anti-mouse IgG alkaline phosphatase conjugate (1:10,000; Amersham Pharmacia Biotech); anti-rabbit IgG alkaline phosphatase conjugate (1:10,000; Amersham Pharmacia Biotech).
Total DNA extraction
Total DNA was extracted from tissues using the TRIzol Reagent (Sigma-Aldrich) according to the manufacturer’s instructions.
Determination of mtDNA Copy Number
Real-time qPCR analysis was performed to determine the mtDNA copy number, as described by Fuke et al. [20] with slight modifications. Relative quantification of mtDNA levels was determined by the ratio of the mitochondrial ND1 (mt-Nd1) gene to the single-copy, nuclear-encoded beta-2-microglobulin (β2MG) gene. Reactions were carried out in an iQ5 system (Bio-Rad), and efficiency of the reactions was determined for the selected primers using serial dilutions of DNA samples. Primer concentration and annealing temperature were optimized, and the specificity of the amplicons was determined by melting curve analysis. The reactions mixture consisted of Maxima SYBR Green qPCR Master Mix (Fermentas), sense and antisense primers (see Table 1 for details) and 20 ng of DNA. Each reaction was run in triplicate to calculate relative mtDNA copy number. Control (Ct) values of all samples were within the linear range. Ct value differences were used to quantify mtDNA copy number relative to the beta-2-microglobulin gene with the following equation: Relative copy number = 2ΔCt, where ΔCt is Ctβ2MG − CtND1.
Statistical analysis
Results are presented as mean ± SEM of the indicated number of animals. Statistical significance was determined using the unpaired two-tailed student’s t test.
Results
Characterization of the experimental animals
As shown in Table 2, GK rats presented a significant increase in HbA1c and postprandial glucose levels when compared to the respective control rats, which confirms the diabetic state of this animal model. Additionally, a marked reduction in body weight was also detected in GK rats (Table 2). No alterations in brain weight were observed (Table 2).
T2D does not affect mitochondrial bioenergetics in brain cortex
In a first approach to investigate the impact of T2D on mitochondrial bioenergetic function, mitochondrial respiration and oxidative phosphorylation were evaluated in freshly isolated brain cortical mitochondria energized with succinate, a complex II substrate. Our results revealed that mitochondrial coupling and oxidative phosphorylation efficiency given by the RCR and ADP/O indexes, respectively, remained unaltered in brain cortical mitochondria from GK rats when compared to the respective control mitochondria (Table 3). ΔΨ m is generated through the respiratory chain pumping of protons from the mitochondrial matrix to the intermembrane space. The proton gradient originates an electrochemical potential (Δp) resulting in a pH (ΔpH) and a voltage gradient (ΔΨ m) across the inner membrane. Lag phase represents the time necessary to mitochondria phosphorylate the exogenous ADP into ATP. As shown in Table 3, no statistical differences were found in ΔΨ m, ADP-induced depolarization and lag phase of brain cortical mitochondria from GK rats when compared to the respective control mitochondria.
Mitochondrial fission prevails in the early stages of T2D
Maintenance of mitochondrial functionality in response to metabolic stress requires fission and fusion of these dynamic organelles. Therefore, we next analyzed by Western blot the levels of mitochondrial fusion (Mfn1, Mfn2 and OPA1) and fission-related proteins (Fis1 and DRP1). Interestingly, a significant decrease in OPA1 protein levels was observed in the brain cortex of GK rats when compared to the respective control rats (Fig. 1C), whereas the levels of Mnf1 (Fig. 1A) and Mnf2 (Fig. 1B) proteins remained unchanged. Concerning the mitochondrial fission-related proteins, our results revealed that the protein levels of Fis1 (Fig. 2A) and DRP1 phosphorylated at serine residue 616 (Fig. 2B) remained statistically unchanged in brain cortices of GK rats when compared to the respective control rats.
Autophagy is decreased in the early stages of T2D
Autophagy is an essential pro-survival response to stress conditions (e.g., nutrient limitation) that allow the maintenance of cellular homeostasis by promoting the timely turnover of long-lived proteins and organelles, including mitochondria. However, under certain circumstances, autophagy can also trigger a cell death program [21]. Given this duality of autophagy and in an effort to dissect how autophagy behaves under diabetic conditions, the next step of this study was to determine the levels of some key proteins (mTOR, Beclin 1, p62 and LC3) associated to the autophagic process. Briefly, mTOR and Beclin 1 exert opposite effects on the regulation of autophagy. While mTOR acts a potent repressor, Beclin 1 functions as an inducer of the autophagic pathway. The autophagic substrate p62 binds directly to LC3, which is known to be a classic marker of autophagy and a participant in autophagosomal membrane elongation [21]. A significant decrease in LC3-II protein levels (Fig. 3C) was detected in the brain cortex of GK rats when compared to the respective control rats. Accordingly, GK rats exhibited a significant increase in the active form of mTOR (pser2448mTOR/mTOR) (Fig. 3A). Meanwhile, beclin 1 (Fig. 3B) and p62 (Fig. 3D) proteins levels remained unchanged in the brain cortex of GK rats. Overall, these findings suggest that in early stages of T2D, autophagy is decreased in the brain cortex.
Mitochondrial biogenesis is maintained in early stages of T2D
Preservation of normal mitochondrial function is known to depend, in part, on mitochondrial biogenesis. In this context, real-time PCR was used to quantify the copy number ratio of mtDNA to nuclear DNA (nDNA) in brain cortex samples. No significant alterations were observed in mtDNA copy number (Fig. 4A). Also the protein levels of a ND1, a mitochondrial subunit coded by mtDNA (Fig. 4B), and nuclear respiratory factor 1 (NRF1) and mitochondrial transcription factor A (TFAM), two transcription factors involved in mitochondrial biogenesis, remained statistically unchanged in the brains of GK rats when compared to the controls (Fig. 4C, D).
Discussion
Although the molecular basis underlying cognitive deterioration and neurodegeneration in diabetes mellitus remains elusive, it has been attributed a central role to mitochondrial dysfunction [5]. Due to the characteristics of GK rats (nonobese, mild hyperglycemia and insulin resistance), the present study extends our knowledge on the role of quality control systems in the maintenance of mitochondrial bioenergetics in the early stages of T2D. Particularly, this study revealed that in the early stages of T2D: (1) mitochondrial fission prevails; (2) mitochondrial biogenesis is maintained; and (3) autophagy decreases. Collectively, these alterations seem to constitute an adaptive metabolic strategy to preserve mitochondrial bioenergetic function and restrict brain cells damage.
Within the brain, mitochondria regulate synaptic transmission, neurotransmitter recycling, dendritic and axonal transport, ion channels, and ion pump activity, which are processes with high energetic requirements [22]. In this sense, mitochondrial bioenergetic failure has been pinpointed as a mechanistic event underlying brain malfunction and neurodegeneration in diabetes mellitus [5]. Using isolated brain cortical mitochondria from 6-month-old GK rats, this study revealed that neither respiratory chain function nor oxidative phosphorylation efficiency was compromised in early stages of T2D-like pathology (Table 3). An age-related impairment of the respiratory chain and an uncoupling of oxidative phosphorylation were documented in brain mitochondria isolated from 12- to 24-month GK rats [23]. So, it is tempting to speculate that in young T2D animals, compensatory mechanisms exist involving mitochondrial quality control systems. Integration of mitochondrial fusion–fission, biogenesis and autophagy forms a surveillance mechanism to maintain a healthy mitochondrial population [12, 24]. Mitochondria form a dynamic, interconnected network within a cell, and frequent cycles of fusion and fission are crucial for mitochondrial respiration, mitochondrial trafficking and distribution, formation and function of synapses and dendritic spines, and mitochondrial quality control, particularly in postmitotic cells such as neurons [25, 26]. A significant decrease in OPA1 protein levels was observed in the brain cortex of GK rats (Fig. 1C). This observation points for a remodeling of brain mitochondrial network in T2D, where the balance of mitochondrial fusion–fission events seems to be shifted toward fission. The first evidence of an altered mitochondrial structure in “diabetic neurons” was provided by Schmeichel et al. [27]. Subsequent studies revealed that dorsal root ganglia (DRG) neurons from a T1D animal model or DGR neurons exposed to high glucose levels exhibit smaller mitochondria as a consequence of an excessive mitochondrial fragmentation/fission [28–30]. Remarkably, Leinninger and collaborators [28] sophisticatedly proposed that early mitochondrial fission promoted by the up-regulation of DRP1 represents a protective or metabolic fission in order to cope with hyperglycemia. However, in a later stage, excessive mitochondrial fission is associated with the activation of Bim and Bax, culminating in apoptosis [28]. More recently, it was also found an increase in the levels of mitochondrial fission protein DRP1 in cultured DRG neurons made insulin resistant by chronic exposure to hyperinsulinemic conditions [31]. Under hyperglycemic conditions, mitochondrial fission is also increased in pancreatic-β cells, hepatocytes, skeletal muscle cells and endothelial cells, promoting the disruption of mitochondrial network and accumulation of small mitochondria [32].
Mitochondrial fission is involved in mitochondrial motility and efficient dissemination of energy across cell structure–metabolic fission [33]. Distressing fission or fusion mechanisms either by inhibiting expression of the fission protein DRP1 or by overexpressing the fusion protein Mfn1 has been shown to prevent mitochondria from distributing to synapses due to defective mitochondrial trafficking, leading to the loss of mitochondria from dendritic spines and, consequently, to a reduction in synapse formation [34–37]. Cardoso and collaborators [38] have previously reported that synaptic integrity, given by the protein levels of synaptophysin, is preserved in the brain cortex of STZ-treated rats, a model of T1D. The maintenance of synaptic integrity was also documented in animal models of T2D [39]. Thereby, we hypothesize that mitochondrial fission could somehow facilitate the recruitment and transport of mitochondria to critical subcellular compartments with high energy demand, such as synaptic terminals, where these organelles remain stationary and preserve synaptic and neuronal function and integrity, in part by supplying ATP.
Mitochondrial fission together with autophagy form a surveillance mechanism to maintain a pool of healthy mitochondria by isolating and targeting damaged organelles for removal [40]. Autophagy assumes particular importance in postmitotic cells, such as neurons, since it constitutes a way of “cleaning” cells from metabolic debris [41]. During the last decade, autophagy has received increasing attention due to its involvement in various aspects of cell physiology, especially cell survival and maintenance of energy homeostasis under conditions of nutrient or energy deprivation–starvation [42]. However, autophagy can also trigger cell death, underscoring its nature as a double-edged sword that could be either protective or injurious depending on the cellular environment, the nature and intensity of the stimulus, and the levels of autophagy [43]. Our study revealed that autophagy is decreased in GK rats. Particularly, it was observed a decrease in LC3-II protein levels (Fig. 3C) and an increase in the protein levels of mTOR phosphorylated at serine residue 2448 (Fig. 3A). GK rats exhibit an insulin resistant state that in an initial phase is accompanied by hyperinsulinemia resulting from a compensatory increase in insulin secretion in response to increased insulin demand [44]. Since insulin activates the class I phosphatidylinositol 3-kinase and mTOR not only to stimulate glucose uptake and protein synthesis but also to inhibit autophagy, this could be a possible explanation for the diminished autophagy observed in the brain cortex of GK rats (Fig. 3) [45]. It has been documented that diminished autophagy is an adaptive response that limits cardiac dysfunction in T1D [46]. Inhibition of autophagy is a beneficial adaptive response that protects cardiomyocytes against high glucose toxicity [47]. In accordance with our data, these authors found that increased mTOR signaling underlies the inhibition of autophagy [47].
Our observations also revealed no significant alterations in mtDNA copy number and protein levels of ND1 and NRF1 and TFAM (Fig. 4). These results support the notion that mitochondrial biogenesis is spared in the early stages of T2D. According to our hypothesis, it was previously demonstrated that mitochondrial biogenesis and function are negatively affected by hyperglycemia in a time-dependent manner [48].
Taken together, our results suggest that mitochondrial fusion–fission and biogenesis and autophagy act as “mitocheckpoints” to sustain brain mitochondrial bioenergetics during the early stages of T2D in order to maintain brain cells health. However, it is of utmost importance to evaluate how these mechanisms interact during the progression of T2D. Within this scenario, future studies involving the genetic manipulation of key proteins involved in mitochondrial quality control will be crucial to gain further insights on the role of these mechanisms during the development of T2D.
References
Lam DW, LeRoith D (2012) The worldwide diabetes epidemic. Curr Opin Endocrinol Diabetes Obes 19(2):93–96. doi:10.1097/MED.0b013e328350583a
Wild S, Roglic G, Green A, Sicree R, King H (2004) Global prevalence of diabetes: estimates for the year 2000 and projections for 2030. Diabetes Care 27(5):1047–1053. doi:10.2337/diacare.27.5.1047
Umegaki H (2012) Neurodegeneration in diabetes mellitus. Adv Exp Med Biol 724:258–265. doi:10.1007/978-1-4614-0653-2_19
Sr-F J, Sa-Roriz TM, Rosset I, Camozzato AL, Santos AC, Chaves ML, Moriguti JC, Roriz-Cruz M (2009) (Pre)diabetes, brain aging, and cognition. Biochim Biophys Acta 1792(5):432–443. doi:10.1016/j.bbadis.2008.12.003
Correia SC, Santos RX, Carvalho C, Cardoso S, Candeias E, Santos MS, Oliveira CR, Moreira PI (2012) Insulin signaling, glucose metabolism and mitochondria: major players in Alzheimer’s disease and diabetes interrelation. Brain Res 1441:64–78. doi:10.1016/j.brainres.2011.12.063
Santiago JA, Potashkin JA (2013) Shared dysregulated pathways lead to Parkinson’s disease and diabetes. Trends Mol Med 19(3):176–186. doi:10.1016/j.molmed.2013.01.002
Carvalho C, Cardoso S, Correia SC, Santos RX, Santos MS, Baldeiras I, Oliveira CR, Moreira PI (2012) Metabolic alterations induced by sucrose intake and Alzheimer’s disease promote similar brain mitochondrial abnormalities. Diabetes 61(5):1234–1242. doi:10.2337/db11-1186
Santos RX, Correia SC, Wang X, Perry G, Smith MA, Moreira PI, Zhu X (2010) Alzheimer’s disease: diverse aspects of mitochondrial malfunctioning. Int J Clin Exp Pathol 3(6):570–581
Zhu J, Wang KZ, Chu CT (2013) After the banquet: mitochondrial biogenesis, mitophagy and cell survival. Autophagy 9(11). doi:10.4161/auto.24135
DuBoff B, Feany M, Gotz J (2013) Why size matters - balancing mitochondrial dynamics in Alzheimer’s disease. Trends Neurosci 36(6):325–335. doi:10.1016/j.tins.2013.03.002
Chan DC (2006) Mitochondrial fusion and fission in mammals. Annu Rev Cell Dev Biol 22:79–99. doi:10.1146/annurev.cellbio.22.010305.104638
Twig G, Hyde B, Shirihai OS (2008) Mitochondrial fusion, fission and autophagy as a quality control axis: the bioenergetic view. Biochim Biophys Acta 1777(9):1092–1097. doi:10.1016/j.bbabio.2008.05.001
Moreira PI, Santos MS, Moreno A, Oliveira C (2001) Amyloid beta-peptide promotes permeability transition pore in brain mitochondria. Biosci Rep 21(6):789–800
Gornall AG, Bardawill CJ, David MM (1949) Determination of serum proteins by means of the biuret reaction. J Biol Chem 177(2):751–766
Estabrook RE (1967) Mitochondrial respiratory control and the polarographic measurement of ADP/O ratios. Methods Enzymol 10:41–47
Chance B, Williams GR (1956) The respiratory chain and oxidative phosphorylation. Adv Enzymol Relat Subj Biochem 17:65–134
Kamo N, Muratsugu M, Hongoh R, Kobatake Y (1979) Membrane potential of mitochondria measured with an electrode sensitive to tetraphenyl phosphonium and relationship between proton electrochemical potential and phosphorylation potential in steady state. J Membr Biol 49(2):105–121
Jensen BD, Gunter TR (1984) The use of tertaphenylphosphonium (TPP +) to measure membrane potentials in mitochondria: membrane binding and respiratory effects. Biophys J 45:92
Muratsugu M, Kamo N, Kurihara K, Kobatake Y (1977) Selective electrode for dibenzyl dimethyl ammonium cation as indicator of the membrane potential in biological systems. Biochim Biophys Acta 464(3):613–619
Fuke S, Kubota-Sakashita M, Kasahara T, Shigeyoshi Y, Kato T (2011) Regional variation in mitochondrial DNA copy number in mouse brain. Biochim Biophys Acta 1807(3):270–274. doi:10.1016/j.bbabio.2010.11.016
Santos RX, Cardoso S, Correia S, Carvalho C, Santos MS, Moreira PI (2010) Targeting autophagy in the brain: a promising approach? Cent Nerv Syst Agents Med Chem 10(2):158–168
Kann O, Kovacs R (2007) Mitochondria and neuronal activity. Am J Physiol Cell Physiol 292(2):C641–C657. doi:10.1152/ajpcell.00222.2006
Moreira PI, Santos MS, Moreno AM, Seica R, Oliveira CR (2003) Increased vulnerability of brain mitochondria in diabetic (Goto–Kakizaki) rats with aging and amyloid-beta exposure. Diabetes 52(6):1449–1456
Westermann B (2010) Mitochondrial fusion and fission in cell life and death. Nat Rev Mol Cell Biol 11(12):872–884. doi:10.1038/nrm3013
Chen H, Chan DC (2009) Mitochondrial dynamics—fusion, fission, movement, and mitophagy—in neurodegenerative diseases. Hum Mol Genet 18(R2):R169–R176. doi:10.1093/hmg/ddp326
Detmer SA, Chan DC (2007) Functions and dysfunctions of mitochondrial dynamics. Nat Rev Mol Cell Biol 8(11):870–879. doi:10.1038/nrm2275
Schmeichel AM, Schmelzer JD, Low PA (2003) Oxidative injury and apoptosis of dorsal root ganglion neurons in chronic experimental diabetic neuropathy. Diabetes 52(1):165–171
Leinninger GM, Backus C, Sastry AM, Yi YB, Wang CW, Feldman EL (2006) Mitochondria in DRG neurons undergo hyperglycemic mediated injury through Bim, Bax and the fission protein Drp1. Neurobiol Dis 23(1):11–22. doi:10.1016/j.nbd.2006.01.017
Edwards JL, Quattrini A, Lentz SI, Figueroa-Romero C, Cerri F, Backus C, Hong Y, Feldman EL (2010) Diabetes regulates mitochondrial biogenesis and fission in mouse neurons. Diabetologia 53(1):160–169. doi:10.1007/s00125-009-1553-y
Vincent AM, Edwards JL, McLean LL, Hong Y, Cerri F, Lopez I, Quattrini A, Feldman EL (2010) Mitochondrial biogenesis and fission in axons in cell culture and animal models of diabetic neuropathy. Acta Neuropathol 120(4):477–489. doi:10.1007/s00401-010-0697-7
Kim B, McLean LL, Philip SS, Feldman EL (2011) Hyperinsulinemia induces insulin resistance in dorsal root ganglion neurons. Endocrinology 152(10):3638–3647. doi:10.1210/en.2011-0029
Yoon Y, Galloway CA, Jhun BS, Yu T (2011) Mitochondrial dynamics in diabetes. Antioxid Redox Signal 14(3):439–457. doi:10.1089/ars.2010.3286
Cagalinec M, Safiulina D, Liiv M, Liiv J, Choubey V, Wareski P, Veksler V, Kaasik A (2013) Principles of the mitochondrial fusion and fission cycle in neurons. J Cell Sci 126(Pt 10):2187–2197. doi:10.1242/jcs.118844
Tondera D, Czauderna F, Paulick K, Schwarzer R, Kaufmann J, Santel A (2005) The mitochondrial protein MTP18 contributes to mitochondrial fission in mammalian cells. J Cell Sci 118(Pt 14):3049–3059. doi:10.1242/jcs.02415
Hoppins S, Lackner L, Nunnari J (2007) The machines that divide and fuse mitochondria. Annu Rev Biochem 76:751–780. doi:10.1146/annurev.biochem.76.071905.090048
Verstreken P, Ly CV, Venken KJ, Koh TW, Zhou Y, Bellen HJ (2005) Synaptic mitochondria are critical for mobilization of reserve pool vesicles at Drosophila neuromuscular junctions. Neuron 47(3):365–378. doi:10.1016/j.neuron.2005.06.018
Santel A, Frank S, Gaume B, Herrler M, Youle RJ, Fuller MT (2003) Mitofusin-1 protein is a generally expressed mediator of mitochondrial fusion in mammalian cells. J Cell Sci 116(Pt 13):2763–2774. doi:10.1242/jcs.00479
Cardoso S, Santos RX, Correia SC, Carvalho C, Santos MS, Baldeiras I, Oliveira CR, Moreira PI (2012) Insulin-induced recurrent hypoglycemia exacerbates diabetic brain mitochondrial dysfunction and oxidative imbalance. Neurobiol Dis 49C:1–12. doi:10.1016/j.nbd.2012.08.008
Belanger A, Lavoie N, Trudeau F, Massicotte G, Gagnon S (2004) Preserved LTP and water maze learning in hyperglycaemic–hyperinsulinemic ZDF rats. Physiol Behav 83(3):483–494. doi:10.1016/j.physbeh.2004.08.031
Liesa M, Shirihai OS (2013) Mitochondrial dynamics in the regulation of nutrient utilization and energy expenditure. Cell Metab 17(4):491–506. doi:10.1016/j.cmet.2013.03.002
Terman A, Kurz T, Navratil M, Arriaga EA, Brunk UT (2010) Mitochondrial turnover and aging of long-lived postmitotic cells: the mitochondrial–lysosomal axis theory of aging. Antioxid Redox Signal 12(4):503–535. doi:10.1089/ars.2009.2598
Mizushima N (2005) The pleiotropic role of autophagy: from protein metabolism to bactericide. Cell Death Differ 12(Suppl 2):1535–1541. doi:10.1038/sj.cdd.4401728
Kang C, Avery L (2008) To be or not to be, the level of autophagy is the question: dual roles of autophagy in the survival response to starvation. Autophagy 4(1):82–84
King AJ (2012) The use of animal models in diabetes research. Br J Pharmacol 166(3):877–894. doi:10.1111/j.1476-5381.2012.01911.x
Meijer AJ, Codogno P (2006) Signalling and autophagy regulation in health, aging and disease. Mol Asp Med 27(5–6):411–425. doi:10.1016/j.mam.2006.08.002
Xu X, Kobayashi S, Chen K, Timm D, Volden P, Huang Y, Gulick J, Yue Z, Robbins J, Epstein PN, Liang Q (2013) Diminished autophagy limits cardiac injury in mouse models of type 1 diabetes. J Biol Chem 288(25):18077–18092. doi:10.1074/jbc.M113.474650
Kobayashi S, Xu X, Chen K, Liang Q (2012) Suppression of autophagy is protective in high glucose-induced cardiomyocyte injury. Autophagy 8(4):577–592. doi:10.4161/auto.18980
Palmeira CM, Rolo AP, Berthiaume J, Bjork JA, Wallace KB (2007) Hyperglycemia decreases mitochondrial function: the regulatory role of mitochondrial biogenesis. Toxicol Appl Pharmacol 225(2):214–220. doi:10.1016/j.taap.2007.07.015
Acknowledgments
Renato X. Santos has a PhD fellowship from the Fundação para a Ciência e a Tecnologia (SFRH/BD/43972/2008).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Santos, R.X., Correia, S.C., Alves, M.G. et al. Mitochondrial quality control systems sustain brain mitochondrial bioenergetics in early stages of type 2 diabetes. Mol Cell Biochem 394, 13–22 (2014). https://doi.org/10.1007/s11010-014-2076-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-014-2076-5