Abstract
The accumulation of glutamate can excessively activate the N-methyl-d-aspartate (NMDA) receptors and cause excitotoxicity. Vitexin (5, 7, 4-trihydroxyflavone-8-glucoside, Vit) is a c-glycosylated flavone which was found in the several herbs, exhibiting potent hypotensive, anti-inflammatory, and neuroprotective properties. However, little is known about the neuroprotective effects of Vit on glutamate-induced excitotoxicity. In present study, primary cultured cortical neurons were treated with NMDA to induce the excitotoxicity. Pretreatment with Vit significantly prevented NMDA-induced neuronal cell loss and reduced the number of apoptotic neurons. Vit significantly inhibited the neuronal apoptosis induced by NMDA exposure by regulating balance of Bcl-2 and Bax expression and the cleavages of poly (ADP-ribose) polymerase and pro-caspase 3. Furthermore, pretreatment of Vit reversed the up-regulation of NR2B-containing NMDA receptors and the intracellular Ca2+ overload induced by NMDA exposure. The neuroprotective effects of Vit are related to inhibiting the activities of NR2B-containing NMDA receptors and reducing the calcium influx in cultured cortical neurons.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Vitexin (5, 7, 4-trihydroxyflavone-8-glucoside, Vit) is a c-glycosylated flavone (Fig. 1a), which was found in the Passion flower [1], Phyllostachys nigra bamboo leaves [2], Vitex agnus-castus (chaste tree or chasteberry) [3], Pearl millet (Pennisetum millet) [4], and Hawthorn [5]. Vit has received much attention because of its wide spectrum of pharmacological effects, such as anticancer effect [6, 7], antioxidant activity [8], antidepressant-like effect [9], antinociceptive activity [10], and anti-inflammatory activity [11]. In addition, Vit has neuroprotective effects on pentylenetetrazole-induced seizure in rats. Vit reduces minimal clonic seizures and generalized tonic–clonic seizures by increasing the seizure onset time, which possibly through interaction at the benzodiazepine site of the γ-aminobutyric acid type A receptor complex [12]. However, the effect of Vit on neural excitotoxicity induced by glutamate is not well known.
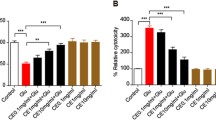
Effects of Vit on cell viability in cultured cortical neurons. a Chemical structure of vitexin. b Concentration-dependent cytotoxic effects of NMDA on the cell viability of cortical neurons. *P < 0.05, **P < 0.01 compared with control. c Time-dependent cytotoxic effects of NMDA on the cell viability of cortical neurons. *P < 0.05, **P < 0.01 compared with control. d Effects of Vit (1 and 10 μM), NVP-AAM077 (0.4 μM), and Ro 25-6981 (0.3 μM) on the cell viability of cortical neurons after exposure to NMDA. *P < 0.05, **P < 0.01 compared with NMDA alone
Glutamate is a primary excitatory neurotransmitter and plays a key role in synaptic plasticity, learning and memory, and excitotoxicity [13]. Glutamate receptors are divided into three categories: N-methyl-d-aspartate (NMDA), α-amino-3-hydroxy-5-methyl-4- isoxazolepropionic acid (AMPA), and kainate (KA) receptors. Glutamate accumulation can cause NMDA receptor-mediated excitotoxicity, which has been implicated in neurodegeneration [14]. NMDA receptors, a kind of glutamate-gated ion channels, are widely expressed in the central nervous system and highly permeable to calcium ions [15]. The overactivation of glutamate receptors can trigger high calcium ion (Ca2+) influx, which activates a number of enzymes that damage cell structures such as the cell membrane, cytoskeleton components, and DNA. This Ca2+ influx is thought to contribute to Ca2+-mediated excitotoxic neuronal cell death in the above-mentioned disease processes [15].
The aim of this study is to investigate the possible protective efficacy of Vit in neuronal apoptosis induced by NMDAR activation and to elucidate the underlying mechanisms. We found that pretreatment of Vit significantly attenuated exitotoxicity by depressing the apoptotic signaling pathways.
Materials and methods
Materials
Vitexin was purchased from the ShangHai PureOne Biotechnology (Shanghai, China). Purity: 98 % by High-performance liquid chromatography (HPLC). MTT [3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium-bromide], NVP-AAM077, Ro25-6981 and anti-β-actin antibody were purchased from Sigma (St. Louis, MO, USA). Anti-NR2A, and anti-procaspase-3 were purchased from Millipore (Billerica, MA, USA). Anti-NR2B, anti-Bax, and anti-Bcl-2 antibodies were purchased from Chemicon (Temecula, CA, USA). Dulbecco’s Modified Eagle’s Medium (DMEM) was purchased from Hyclone (Logan, UT, USA). Anti-PARP (poly ADP-ribose polymerase) antibody was purchased from Cell Signaling Technology (Danvers, MA, USA). Fetal bovine serum, Neurobasal medium, and B27 were purchased from Gibco (Invitrogen, Carlsbad, CA, USA). All of the other chemicals and reagents were standard commercially available biochemical quality.
Primary mouse cortical neuronal culture
The Animal Care and Use Committee of the Fourth Military Medical University approved all animal protocols. Cultured prefrontal cortex neurons were derived from E18 C57Bl/6 mice as Wang et al. [16] described. Briefly, the prefrontal cortex was dissected, minced, and trypsinized for 15 min using 0.125 % trypsin (Invitrogen, Carlsbad, USA). Cells were then seeded onto 96-well plates, 24-well plates, 6-well plates, or 100 mm dishes. All plates were precoated with 50 μg/ml poly-d-lysine (Sigma) and grown in Neurobasal medium (Invitrogen) supplemented with B27 and 2 mM glutamine (Invitrogen). In B27/Neurobasal medium, glial growth was reduced to less than 0.5 % as assessed by immunocytochemistry for glial fibrillary acidic protein (GFAP). The vast majority of cultured cells were immunoreactive for neuron-specific enolase [17]. The cultures were incubated at 37 °C in 95 % air/5 % carbon dioxide with 95 % humidity. The media was changed every 2 days during the maturation of cortical neurons. Cultures were used for experiments on the 10th day in vitro (DIV 10). The neurons were briefly rinsed with phosphate-buffered saline (PBS) and added new Neurobasal medium without B27, and then treated with Vit for 24 h. Then, NMDA and glycine (10 μM) were added to the medium with Vit for another 30 min. The cells were washed twice and returned to the original culture medium for another 24 h. Then, cell viability, staining, western-blot, and imaging were performed.
Cell viability analysis
The MTT assay was used to detect cell viability as Liu et al. [18] described. Neurons were cultured in 96-well plates at a density of 1 × 104 per well. The substrate MTT was dissolved in DMEM medium and added to each well at a final concentration of 0.5 mg/ml and then incubated at 37 °C for 4 h. Then the medium was then replaced by 150 μl dimethyl sulfoxide (DMSO) to dissolve the formazan product. The optical density (OD) was read on a Universal Microplate Reader (Elx 800, Bio-TEK instruments Inc., USA) at 570 nm (using 630 nm as a reference). Cell viability was presented as a percentage of the absorbance of untreated cultures. All data are expressed as mean ± SEM of three independent experiments and each mean included data from six wells.
Hoechst 33258 and PI double staining
Cell death was determined by propidium iodide (PI, Sigma) and Hoechst 33258 (Sigma) double fluorescent staining as Zhang et al. [19] described. Neurons were cultured in 24-well plates at a density of 600 cells/mm2. The cells were exposed to NMDA for 30 min. 24 h after NMDA treatment, the cells were stained with PI (10 μg/ml) and Hoechst 33258 (10 μg/ml) for 15 min, and then fixed in 4 % paraformaldehyde for 10 min. Hoechst 33258 is excited by UV light at around 350 nm and emits blue fluorescence light at 461 nm. Hoechst 33258 is often used to distinguish the compact chromatin of apoptotic nuclei from that of normal cells [20]. Propidium iodide, a red-fluorescence dye (excited at 620 nm), is only permeant to dead cells. Staining was imaged and analyzed using Olympus Fluoview FV100 (Olympus, Japan). To assess apoptotic nuclei and dead/dying neurons, three visual fields were randomly selected from each well.
Western blot analysis
In order to further explore the mechanisms involved in VIT-mediated neuroprotection, we examined the effects of VIT on signaling pathways related to survival by Western blot analysis as described previously [21]. Neurons were cultured in 6-well plates at a density of 2 × 106 cells/well. After each treatment, cells were rinsed twice with PBS and lysed by M-PER Protein Extraction Buffer containing 1× protease inhibitor cocktail. Cell protein was quantified by a BCA Kit and equal amounts of protein (50 μg) separated on 10 % polyacrylamide gel followed by transferred onto an Immun-Blot PVDF membrane. The membrane was blocked for 1 h with 5 % non-fat milk in Tris–phosphate buffer containing 0.05 % Tween 20 (TBS·T). It was further incubated overnight at 4 °C with primary antibodies including anti-NR2A (dilution ratio1:400), anti-NR2B (dilution ratio1:1,000), anti-Bax (dilution ratio 1:400), anti-Bcl-2(dilution ratio 1:400), Anti-PARP (dilution ratio 1:1,000), anti-pro-caspase-3 (dilution ratio 1:1,000), and β-actin (dilution ratio1:10,000) as a loading control. The membranes were incubated with horseradish peroxidase-conjugated secondary antibodies (anti-rabbit IgG for the primary antibodies), and bands were visualized using an ECL system (Perkin Elmer).
Calcium imaging
Calcium imaging was performed as previously described [22]. Neurons were cultured in 3.5-mm plates made especially for laser scanning microscope at a density 3 × 105 per plate. Cultured cells were washed twice using Mg2+-free extracellular solution (ECS) containing (in mM): NaCl, 140; KCl, 3; CaCl2, 2; HEPES, 10; and glucose, 10. The pH was adjusted to 7.2–7.3 with NaOH and osmotic pressure adjusted to 310 ± 5 with sucrose. Then, the neurons were incubated with 2 μM fluo-3/AM at 37 °C. After 30 min, the cultures were washed twice and returned to the original culture medium for an additional 30 min. The dye-loaded cells were measured for fluorescence using a confocal laser scanning microscope (Olympus, Japan). Prior to NMDA application, the dye-loaded cells were scanned for approximately 1 min to obtain a basal level of intracellular Ca2+. Vit (10 μM) was added 24 h before the detection of calcium imaging and present in the whole experimental process. Then, 200 μM NMDA was applied to the cultures, and an equal amount of ECS was added as a placebo. The change of Ca2+ concentration was estimated by the fluorescence ratio of the fluo-3/AM-loaded neurons for another 4 min. The results are expressed as changes relative to basal levels, and five cells were selected randomly for analysis.
Data analysis
Data were expressed as the mean ± SEM. Statistical comparisons were evaluated by a t test and one-way ANOVA was used for comparison among multiple groups. P<0.05 was considered to be statistically significant.
Results
Effects of Vit on cell viability in cultured cortical neurons
NMDA has been proven to be involved in the pathogenesis of neurodegenerative disorders associated with glutamate excitotoxicity. The neurons were exposed to increasing concentrations of NMDA (0, 50, 100, 200, and 400 μM) for 30 min. As expected, NMDA decreased cell viability in a concentration-dependent (Fig. 1b) and time-dependent (Fig. 1c) manner, as measured by the MTT assay. The neurons were exposed to 200 μM NMDA for 30 min in subsequent experiments because cell injury was significant in this paradigm (cell viability in NMDA treatment: 52.3 % ± 2.5 %). Cultured cortical neurons were pretreated with Vit for 24 h, and then treated with NMDA (200 μM) and glycine (10 μM) for another 30 min. The cells were returned to the original culture medium for 24 h. However, treatment with Vit significantly increased the cell viability of neurons in a concentration-dependent manner. Neuroprotection of 10 μM Vit was most effective. Vit (1 and 10 μM) alone showed no effect on cell viability. In addition, NR2B-selective antagonist Ro 25-6981 (0.3 μM) blocked cell death by NMDA exposure; however, NR2A-selective antagonist NVP-AAM077 (0.4 μM) did not affect the cell viability by NMDA exposure (Fig. 1d), suggesting the different the role of NMDA receptor subtypes in mediating the excitotoxicity.
Effects of VIT on NMDA-induced apoptosis in cultured cortical neurons
Hoechst 33258 and PI double-staining were performed to further determine the neuroprotective effects of Vit on NMDA-induced apoptosis in cultured cortical neurons. Hoechst 33258 and PI are popular fluorescent nucleic acid dye. Hoechst 33258 and PI emit blue and red fluorescence, respectively, when bound to double-stranded DNA. Hoechst 33258 can penetrate the cell membrane of necrotic and living cells, but PI cannot pass through the living cells. Therefore, PI is usually used to detect cell apoptosis and necrosis. Data demonstrated that 5.9 ± 4.5 % of the cells in the control group underwent cell death or apoptosis compared with 35.1 ± 2.6 % of the cells in the NMDA injury group (Fig. 2a, b). Treatment with Vit (1 μM) significantly decreased the number of apoptotic and necrotic cells (Fig. 2a, b). These data suggest that Vit protects neurons from excitotoxicity mediated by NMDA.
Hoechst 33258 and PI double-staining in cultured cortical neurons. a The representative fluorescence images obtained after Hoechst 33258, PI, and double-staining in cortical neurons. Scale bar 20 μm. b The percentage of apoptotic neurons in total neurons for control, NMDA, and NMDA + Vit (1 μM) treated groups. The apoptotic numbers were counted from three independent experiments. **P < 0.01 compared with control, ## P < 0.01 compared with NMDA alone
Effects of Vit on Bcl-2/Bax expression
Bcl-2 family members include both anti-apoptotic (e.g., Bcl-2 and Bcl-xl) and pro-apoptotic (e.g., Bax, Bad, Bak, and Bid) proteins. The ratio between the two subsets determines the susceptibility of the cells to a death signal [23]. Next, we detected the effects of Vit on the levels of Bcl-2 and Bax, and the ratio of Bax/Bcl-2. Western blot analysis showed that Bcl-2 and Bax were both expressed in non-injured cortical neurons, and Vit (10 μM) treatment alone did not alter the expression of these proteins. Compared with control, 200 μM NMDA exposure in cultured cortical neurons increased the levels of Bax (Fig. 3a, b), decreased the levels of Bcl-2 (Fig. 3a, b) and increased the ratio of Bax/Bcl-2 (Fig. 3a, b). However, pretreatment of Vit (10 μM) before NMDA exposure significantly reversed the levels of Bax (Fig. 3a, b) and Bcl-2 (Fig. 3a, c), and the ratio of Bax/Bcl-2 (Fig. 3a, d).
Effects of Vit on the levels of Bax/Bcl-2, Parp, and pro-caspase-3 a Expression levels of Bax and Bcl-2 proteins were detected by Western blot. b The result showed that the levels of Bax markedly increased after exposure to NMDA in cultured cortical neurons. Pretreatment of 10 μM Vit significantly decreased the levels of Bax. c The levels of Bcl-2 significantly decreased after exposure to NMDA in cultured cortical neurons. Pretreatment of 10 μM Vit evidently increased the levels of Bcl-2. d The ratio of Bax/Bcl-2 was notably increased after NMDA exposure; however, the 10 μM Vit reversed the ratio. e Expression levels of Parp and pro-caspase-3 proteins were detected by Western blot. f The levels of Parp 116 significantly decreased after exposure to NMDA in cultured cortical neurons. Pretreatment of 10 μM Vit evidently prevented the decrease of Parp 116 by NMDA exposure. g The result showed that the levels of Parp 89 markedly increased after exposure to NMDA in cultured cortical neurons. Pretreatment of 10 μM Vit significantly decreased the levels of Parp 89. h The levels of pro-caspase-3 significantly decreased after exposure to NMDA in cultured cortical neurons. Pretreatment of 10 μM Vit evidently prevented the decrease of pro-caspase-3 by NMDA exposure. *P < 0.05, **P < 0.01 compared with control, # P < 0.05, ## P < 0.01 compared with NMDA alone
Effects of Vit on Parp and caspase-3 activation
Next, we detected the effects of Vit on the levels of cleavages of poly (ADP-ribose) polymerase (Parp) and caspase 3. Vit (10 μM) treatment alone did not alter the levels of Parp and pro-caspase 3 (Fig. 3e). Compared with control, 200 μM NMDA exposure increased the cleavages of Parp (116) shown as the decrease of Parp (116) levels (Fig. 3e, f) and the increase of Parp (89) levels (Fig. 3e, g), and decreased the levels of pro-caspase-3 (Fig. 3e, h). Pretreatment of Vit (10 μM) significantly reversed the levels of Parp (116) (Fig. 3e, f) and Parp (89) (Fig. 3e, g), and the pro-caspase-3 (Fig. 3e, h). These results indicate that Vit effectively prevents NMDA-induced Parp cleavage and caspase 3 activation.
Effects of VIT on expression of NR2A- and NR2B-containing NMDARs
NR2A- and NR2B-containing NMDARs are reported to link to different intracellular cascades and participate in different functions in neuronal cell survival or death after exposure to NMDA [24]. Blockades of NR2B-containing NMDA receptors promote neuronal survival, exerting a protective action against NMDA receptor-mediated neuronal damage [24–26]. This is consistent to our results that NR2B specific antagonist Ro25-6981 abolished the NMDA-induced cell loss (Fig. 1d). Next, Western blot was performed to further examine the effects of Vit on the expression of NMDAR subtypes. Levels of NR2B subtype expression was markedly increased after exposure to NMDA (Fig. 4a, b). Pretreatment of Vit (10 μM) significantly reduced the over-expression of NR2B subtype induced by NMDA exposure (Fig. 4a, b). However, neither NMDA exposure nor Vit (10 μM) treatment altered the levels of NR2A subtype receptors (Fig. 4a, c). Thus, downregulation of NR2B-containing NMDARs by Vit is suggested to be, at least partly, responsible for the neuroprotective effects against NMDA-induced excitotoxicity.
Effects of Vit on the expression of NR2A and NR2B and calcium imaging a Expression levels of NR2A and NR2B proteins were detected by Western blot. b The result showed that the levels of NR2B markedly increased after exposure to NMDA in cultured cortical neurons. Pretreatment of 10 μM Vit significantly prevented the increase of NR2B by NMDA exposure. c Both NMDA and Vit treatment did not influence the levels of NR2A. **P < 0.01 compared with control, ## P < 0.01 compared with NMDA alone. d The green fluorescence under the laser scanning microscope at different time showed the concentration of calcium in neurons, which was stable during the experiment. e The fluorescence intensity showing the Ca2+ concentration was stable during detection by a laser scanning microscope for 300 s (n = 42 neurons). f 200 μM NMDA could evoke strong fluorescence intensity (n = 54 neurons) and pretreatment of Vit (10 μM) could significantly reduce fluorescence intensity in neurons (n = 46 neurons). Scale bar 20 μm
Inhibition of NMDA-induced Ca2+ overload by Vit
Sustained intracellular Ca2+ overload contributes to neuronal injury following excessive activation of NMDARs [27]. Next, we measured the calcium influx in cultured cortical neurons with treatment of NMDA or Vit. The fluorescence intensity can be regarded as an indicator of cytoplasmic Ca2+ concentration [28]. The Ca2+ concentration in cultured neuron was stable during our experiments (Fig. 4d, e). NMDA (200 μM) evoked a fast elevation of Ca2+ concentration for the next four minutes (Fig. 4d, f). Pretreatment with Vit (10 μM) could attenuate the amplitude of elevation in Ca2+ influx after NMDA exposure (Fig. 4d, f).
Discussion
In this study, the anti-excitotoxicity effect of Vit was investigated in cultured cortical neurons. Expressions of NMDA-induced apoptotic markers, such as Bcl-2 degradation, Bax expression, cleavages of Parp and pro-caspase 3, were all attenuated by Vit treatment. Our results suggest that Vit protects neurons from excitotoxicity through inhibiting cell apoptosis and calcium overload induced by NMDA exposure.
Glutamate plays a key role in neural transmission, development, and synaptic plasticity. Glutamate can binds to ionotropic receptors (iGluRs) and metabotropic receptors (mGluRs). The ionotropic GluRs include NMDA, KA, and AMPA receptors. Excessive accumulation of glutamate results in over activation of NMDA receptors, which induces excitotoxicity and causes neuronal damage [29]. Furthermore, activation of glutamate receptors triggers large increases in Ca2+ levels into neurons. Ca2+ acts as an important second messenger, activating several intracellular signaling cascades. Intracellular Ca2+ accumulation results in glutamate-induced neurotoxicity [30]. Excitotoxicity has been linked to several pathological states of the nervous system such as seizures, ischemia, anoxia, inflammation, and neurodegenerative disorders [30]. Vit has been found to exhibit antioxidant activity [8], antidepressant-like effect [9], and neuroprotective effects [12]. In this study, NMDA exposure greatly decreased the cell viability in cultured cortical neurons. However, Vit treatment concentration-dependently attenuated the cell loss. Specific NR2A- and NR2B-containing NMDA receptor antagonists NVP-AAM077 and Ro25-6981 were used to identify the NMDA receptor subunit roles in the excitotoxicity. The IC50 of NVP-AAM077 is 14 nM and 1.8 μM for NR2A and NR2B, respectively [31], and the IC50 of Ro25-6981 is 9 nM and 52 μM for NR2B and NR2A, respectively [32]. The concentration (0.4 μM) of NVP-AAM077 is high enough to antagonize NR2A and 0.3 μM of Ro25-6981 is specific for antagonize NR2B. In the previous and present study, we found NR2B specific antagonist Ro25-6981(0.3 μM) could abolished the excitotoxicity [33].
Hoechst 33258 and PI double-staining further testified the neuroprotective effects of Vit, which was related to regulation of Bcl-2 and Bax expression and the cleavages of Parp and pro-caspase 3. The ratio between Bax and Bcl-2 determines the susceptibility of cells to a death signal [34], and is widely used to show the effects of treatment on cell injury and survival. Vit decreased Bax expressin level while increased Bcl-2 level. Therefore, it significantly decreased the ratio of Bax/Bcl-2. Western blot revealed the different roles of NR2A- and NR2B-containing NMDARs in the neuroprotection of Vit. Treatments of NMDA and Vit did not change the expression of NR2A receptors, but NMDA increased the expression of NR2B, which is implied in mediating the excitotoxicity [24]. NMDAR overactivation is a critical step in the glutamate-induced excitotoxicity of CNS neurons. Both NR2A- and NR2B-containing NMDARs are linked to different intracellular cascades and have distinct roles in cell survival and excitotoxicity. The membrane distribution of NMDARs also influences excitotoxicity. Synaptic NMDARs have anti-apoptotic activities, whereas extrasynaptic NMDARs reportedly activate signs that promote neuronal death following ischemia [35, 36]. Furthermore, NR1/NR2B receptors are known to be expressed predominantly at extrasynaptic sites [37] and excitotoxicity is triggered by the selective activation of NMDARs containing the NR2B subunit [24, 25, 38, 39]. Pretreatment of Vit selectively reversed the protein levels of NR2B induced by NMDA exposure, implying that the neuroprotection of Vit is likely to antagonize a particular NMDAR subunit. This phenomenon is quite beneficial for neurodegenerative diseases relevant to glutamate excitotoxicity.
The key step in NMDA-induced neuronal cell apoptosis is the overload of intracellular Ca2+, followed by overstimulation of NMDARs [40]. Ca2+ overload triggers several downstream lethal reactions, including nitrosative stress, oxidative stress, and mitochondrial dysfunction [41]. In this study, the elevation of Ca2+ stimulated by NMDA was inhibited by Vit in cultured cortical neurons, suggesting that the neuroprotective effects of Vit is partially due to the inhibition of calcium influx through the NMDA receptors. In our previous researches, we also reported other components derived from traditional Chinese herbal medicine such as salidroside [42], hydroxysafflor yellow A [43], and hyperoside [44]. FMNT showed comparative neuroprotective effects as compared with other classic components mentioned above.
In conclusion, our results suggest that the neuroprotection of Vit is, at least partially, associated with the down-regulation of NR2B-containing NMDARs. The neuroprotective effects of Vit are closely related to the inhibition of apoptosis and Ca2+ overload induced by NR2B-containing NMDARs. We hope that findings of the present study may shed light upon the pharmacological basis for clinical application of Vit.
Abbreviations
- Caspase:
-
Cysteinyl aspartate-specific protease
- MTT:
-
(3-(4,5-Dimethylthiazol-2-yl-)-2,5-diphenyl-tetrazolium bromide
- NMDA:
-
N-methyl-d-asparate
- NMDAR:
-
NMDA receptor
- Vit:
-
Vitexin
References
Zucolotto SM, Fagundes C, Reginatto FH, Ramos FA, Castellanos L, Duque C, Schenkel EP (2012) Analysis of C-glycosyl flavonoids from South American Passiflora species by HPLC-DAD and HPLC-MS. Phytochem Anal 23(3):232–239
Lee HJ, Kim KA, Kang KD, Lee EH, Kim CY, Um BH, Jung SH (2010) The compound isolated from the leaves of Phyllostachys nigra protects oxidative stress-induced retinal ganglion cells death. Food Chem Toxicol 48(6):1721–1727
Hajdu Z, Hohmann J, Forgo P, Martinek T, Dervarics M, Zupko I, Falkay G, Cossuta D, Mathe I (2007) Diterpenoids and flavonoids from the fruits of Vitex agnus-castus and antioxidant activity of the fruit extracts and their constituents. Phytother Res 21(4):391–394
Gaitan E, Lindsay RH, Reichert RD, Ingbar SH, Cooksey RC, Legan J, Meydrech EF, Hill J, Kubota K (1989) Antithyroid and goitrogenic effects of millet: role of C-glycosylflavones. J Clin Endocrinol Metab 68(4):707–714
Ma LY, Liu RH, Xu XD, Yu MQ, Zhang Q, Liu HL (2010) The pharmacokinetics of C-glycosyl flavones of Hawthorn leaf flavonoids in rat after single dose oral administration. Phytomedicine 17(8–9):640–645
Papi A, Farabegoli F, Iori R, Orlandi M, De Nicola GR, Bagatta M, Angelino D, Gennari L, Ninfali P (2013) Vitexin-2-O-xyloside, raphasatin and (−)-epigallocatechin-3-gallate synergistically affect cell growth and apoptosis of colon cancer cells. Food Chem 138(2–3):1521–1530
Yang SH, Liao PH, Pan YF, Chen SL, Chou SS, Chou MY (2013) The novel p53-dependent metastatic and apoptotic pathway induced by vitexin in human oral cancer OC2 cells. Phytother Res 27(8):1154–1161
Praveena R, Sadasivam K, Kumaresan R, Deepha V, Sivakumar R (2013) Experimental and DFT studies on the antioxidant activity of a C-glycoside from Rhynchosia capitata. Spectrochim Acta A Mol Biomol Spectrosc 103:442–452
Can OD, Demir Ozkay U, Ucel UI (2013) Anti-depressant-like effect of vitexin in BALB/c mice and evidence for the involvement of monoaminergic mechanisms. Eur J Pharmacol 699(1–3):250–257
Gorzalczany S, Marrassini C, Mino J, Acevedo C, Ferraro G (2011) Antinociceptive activity of ethanolic extract and isolated compounds of Urtica circularis. J Ethnopharmacol 134(3):733–738
Rabelo AS, Oliveira ID, Guimaraes AG, Quintans JS, Prata AP, Gelain DP, Venceslau EM, Santos JP, Quintans LJ Jr, Bonjardim LR, Barison A, Campos FR, Santos AD, Nogueira PC, Costa EV, Moraes VR, Araujo AA (2013) Antinociceptive, anti-inflammatory and antioxidant activities of aqueous extract from Remirea maritima (Cyperaceae). J Ethnopharmacol 145(1):11–17
Abbasi E, Nassiri-Asl M, Shafeei M, Sheikhi M (2012) Neuroprotective effects of vitexin, a flavonoid, on pentylenetetrazole-induced seizure in rats. Chem Biol Drug Des 80(2):274–278
Gonda X (2012) Basic pharmacology of NMDA receptors. Curr Pharm Des 18(12):1558–1567
Hu NW, Ondrejcak T, Rowan MJ (2012) Glutamate receptors in preclinical research on Alzheimer’s disease: update on recent advances. Pharmacol Biochem Behav 100(4):855–862
Paoletti P (2011) Molecular basis of NMDA receptor functional diversity. Eur J Neurosci 33(8):1351–1365
Wang H, Wu LJ, Kim SS, Lee FJ, Gong B, Toyoda H, Ren M, Shang YZ, Xu H, Liu F, Zhao MG, Zhuo M (2008) FMRP acts as a key messenger for dopamine modulation in the forebrain. Neuron 59(4):634–647
Brewer GJ, Torricelli JR, Evege EK, Price PJ (1993) Optimized survival of hippocampal neurons in B27-supplemented Neurobasal, a new serum-free medium combination. J Neurosci Res 35(5):567–576
Li ZL, Liu JC, Liu SB, Li XQ, Yi DH, Zhao MG (2012) Improvement of vascular function by acute and chronic treatment with the GPR30 agonist G1 in experimental diabetes mellitus. PLoS ONE 7(6):e38787
Zhang K, Li YJ, Yang Q, Gerile O, Yang L, Li XB, Guo YY, Zhang N, Feng B, Liu SB, Zhao MG (2013) Neuroprotective effects of oxymatrine against excitotoxicity partially through down-regulation of NR2B-containing NMDA receptors. Phytomedicine 20(3–4):343–350
Gonzalez-Juanatey JR, Pineiro R, Iglesias MJ, Gualillo O, Kelly PA, Dieguez C, Lago F (2004) GH prevents apoptosis in cardiomyocytes cultured in vitro through a calcineurin-dependent mechanism. J Endocrinol 180(2):325–335
Wu Y, Peng H, Cui M, Whitney NP, Huang Y, Zheng JC (2009) CXCL12 increases human neural progenitor cell proliferation through Akt-1/FOXO3a signaling pathway. J Neurochem 109(4):1157–1167
Zhang Y, Dong Z, Jin L, Zhang K, Zhao X, Fu J, Gong Y, Sun M, Yang B, Li B (2013) Arsenic trioxide-induced hERG K(+) channel deficiency can be rescued by matrine and oxymatrine through up-regulating transcription factor Sp1 expression. Biochem Pharmacol 85(1):59–68
Liu SB, Zhang N, Guo YY, Zhao R, Shi TY, Feng SF, Wang SQ, Yang Q, Li XQ, Wu YM, Ma L, Hou Y, Xiong LZ, Zhang W, Zhao MG (2012) G-protein-coupled receptor 30 mediates rapid neuroprotective effects of estrogen via depression of NR2B-containing NMDA receptors. J Neurosci 32(14):4887–4900
Liu Y, Wong TP, Aarts M, Rooyakkers A, Liu L, Lai TW, Wu DC, Lu J, Tymianski M, Craig AM, Wang YT (2007) NMDA receptor subunits have differential roles in mediating excitotoxic neuronal death both in vitro and in vivo. J Neurosci 27(11):2846–2857
Stanika RI, Pivovarova NB, Brantner CA, Watts CA, Winters CA, Andrews SB (2009) Coupling diverse routes of calcium entry to mitochondrial dysfunction and glutamate excitotoxicity. Proc Natl Acad Sci USA 106(24):9854–9859
Shen H, Yuan Y, Ding F, Liu J, Gu X (2008) The protective effects of Achyranthes bidentata polypeptides against NMDA-induced cell apoptosis in cultured hippocampal neurons through differential modulation of NR2A- and NR2B-containing NMDA receptors. Brain Res Bull 77(5):274–281
Vander Jagt TA, Connor JA, Weiss JH, Shuttleworth CW (2009) Intracellular Zn2+ increases contribute to the progression of excitotoxic Ca2+ increases in apical dendrites of CA1 pyramidal neurons. Neuroscience 159(1):104–114
Matsumoto Y, Yamamoto S, Suzuki Y, Tsuboi T, Terakawa S, Ohashi N, Umemura K (2004) Na+/H+ exchanger inhibitor, SM-20220, is protective against excitotoxicity in cultured cortical neurons. Stroke 35(1):185–190
Jayanarayanan S, Soman S, Peeyush KT, Anju TR, Paulose CS (2013) NMDA & AMPA Receptor mediated excitotoxicity in cerebral cortex of streptozotocin induced diabetic rat: ameliorating effects of curcumin. Chem Biol Interact 201(1–3):39–48
Spalloni A, Nutini M (1832) Longone P (2012) Role of the N-methyl-d-aspartate receptors complex in amyotrophic lateral sclerosis. Biochim Biophys Acta 2:312–322
Auberson YP, Allgeier H, Bischoff S, Lingenhoehl K, Moretti R, Schmutz M (2002) 5-Phosphonomethylquinoxalinediones as competitive NMDA receptor antagonists with a preference for the human 1A/2A, rather than 1A/2B receptor composition. Bioorg Med Chem Lett 12(7):1099–1102
Fischer G, Mutel V, Trube G, Malherbe P, Kew JN, Mohacsi E, Heitz MP, Kemp JA (1997) Ro 25-6981, a highly potent and selective blocker of N-methyl-D-aspartate receptors containing the NR2B subunit. Characterization in vitro. J Pharmacol Exp Ther 283(3):1285–1292
Li XB, Yang ZX, Yang L, Chen XL, Zhang K, Yang Q, Wu YM, Liu SB, Tao KS, Zhao MG (2012) Neuroprotective effects of flax lignan against NMDA-induced neurotoxicity in vitro. CNS Neurosci Ther 18(11):927–933
Zeng KW, Wang XM, Ko H, Kwon HC, Cha JW, Yang HO Hyperoside protects primary rat cortical neurons from neurotoxicity induced by amyloid beta-protein via the PI3 K/Akt/Bad/Bcl(XL)-regulated mitochondrial apoptotic pathway. Eur J Pharmacol 672 (1-3):45-55
Hardingham GE, Fukunaga Y, Bading H (2002) Extrasynaptic NMDARs oppose synaptic NMDARs by triggering CREB shut-off and cell death pathways. Nat Neurosci 5(5):405–414
Tu W, Xu X, Peng L, Zhong X, Zhang W, Soundarapandian MM, Balel C, Wang M, Jia N, Zhang W, Lew F, Chan SL, Chen Y, Lu Y (2010) DAPK1 interaction with NMDA receptor NR2B subunits mediates brain damage in stroke. Cell 140(2):222–234
Tovar KR, Westbrook GL (1999) The incorporation of NMDA receptors with a distinct subunit composition at nascent hippocampal synapses in vitro. J Neurosci 19(10):4180–4188
Zhou M, Baudry M (2006) Developmental changes in NMDA neurotoxicity reflect developmental changes in subunit composition of NMDA receptors. J Neurosci 26(11):2956–2963
Krapivinsky G, Krapivinsky L, Manasian Y, Ivanov A, Tyzio R, Pellegrino C, Ben-Ari Y, Clapham DE, Medina I (2003) The NMDA receptor is coupled to the ERK pathway by a direct interaction between NR2B and RasGRF1. Neuron 40(4):775–784
Sattler R, Tymianski M (2000) Molecular mechanisms of calcium-dependent excitotoxicity. J Mol Med (Berl) 78(1):3–13
Meldrum BS (2000) Glutamate as a neurotransmitter in the brain: review of physiology and pathology. J Nutr 130(4S Suppl):1007S–1015S
Shi TY, Feng SF, Xing JH, Wu YM, Li XQ, Zhang N, Tian Z, Liu SB, Zhao MG (2012) Neuroprotective effects of Salidroside and its analogue tyrosol galactoside against focal cerebral ischemia in vivo and H2O2-induced neurotoxicity in vitro. Neurotox Res 21(4):358–367
Yang Q, Yang ZF, Liu SB, Zhang XN, Hou Y, Li XQ, Wu YM, Wen AD, Zhao MG (2010) Neuroprotective effects of hydroxysafflor yellow A against excitotoxic neuronal death partially through down-regulation of NR2B-containing NMDA receptors. Neurochem Res 35(9):1353–1360
Zhang XN, Li JM, Yang Q, Feng B, Liu SB, Xu ZH, Guo YY, Zhao MG (2010) Anti-apoptotic effects of hyperoside via inhibition of NR2B-containing NMDA receptors. Pharmacol Rep 62(5):949–955
Acknowledgments
This research was supported by NSF of China, Nos. 31271126, 2011ZXJ091 06-01C, and 2011KTCL03-12.
Conflict of interest
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Le Yang and Zhi-ming Yang have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Yang, L., Yang, Zm., Zhang, N. et al. Neuroprotective effects of vitexin by inhibition of NMDA receptors in primary cultures of mouse cerebral cortical neurons. Mol Cell Biochem 386, 251–258 (2014). https://doi.org/10.1007/s11010-013-1862-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-013-1862-9