Abstract
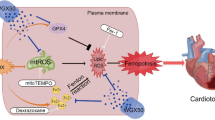
Understanding the molecular basis of doxorubicin (Dox)-induced cardiomyopathy is crucial to finding cardioprotective strategies. Oxidative stress-mediated pathways are known to contribute to cardiomyocyte apoptosis due to Dox. Improving the antioxidant defenses of cardiomyocytes could be one strategy for cardiac protection. We tested the effects of vitamin C (Vit C), a potent antioxidant, on Dox-induced cardiomyocyte apoptosis. Adult rat cardiomyocytes were incubated for 24 h with Dox (0.01–10 μM), with and without different concentrations of Vit C (5–100 μM). Exposure to Dox (10 μM) resulted in a 98% increase in the production of reactive oxygen species (ROS) and creatine kinase (CK) release, 70% increase in p53 as well as ASK-1 activation, 40% increase in p38 activation, 30% increase in pro-apoptotic Bax over anti-apoptotic Bcl-xl ratio and caspase activation, and about 20% reduction in cell viability. Vit C (25 μM) was able to mitigate Dox-induced changes by decreasing ROS and CK release by 50%, reducing p53 activation by 40%. The increase in ASK-1 and p38 was also significantly mitigated, and apoptosis was reduced while cardiomyocytes viability was improved. This study shows that Dox-induced cardiomyocyte death is mediated by a direct membrane effect as well as intracytoplasmic changes promoting the cardiomyocyte apoptosis. These findings suggest a nutritional approach of using Vit C for preventing Dox-induced cardiotoxicity and better management of cancer patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Anthracyclines (e.g., doxorubicin—Dox) are the most effective drugs available in the treatment of neoplastic diseases [1, 2]. However, a major factor limiting their use is a cumulative, dose-dependent cardiotoxicity resulting in a permanent loss of cardiomyocytes due to cell injury and apoptosis, leading to cardiomyopathy and heart failure [1, 3]. Dox-induced cardiomyopathy still remains an important clinical problem as there is increasing number of long-term cancer survivors [4]. Thus, understanding the mechanism of this cardiomyopathy as well as its prevention remains an important issue. There is increasing evidence that oxidative stress plays a role in Dox-induced cardiomyocyte apoptosis as well as cardiomyopathy [5–7].
Apoptosis signal-regulating kinase 1 (ASK1) is a member of the mitogen-activated protein kinase (MAPK) kinase kinase family, which activates both p38 kinase (p38) and c-Jun NH2-terminal protein kinase (JNK) pathways [8]. These kinases are activated in various types of stress-induced apoptosis [9] including Dox-induced cardiomyopathy [6, 10]. Another protein, the tumor suppressor p53, has also been shown to be upregulated in Dox-induced cardiotoxicity [11]. Upon activation, p53 is phosphorylated at Ser15 and translocated into the nucleus to induce the expression of genes associated with cell cycle arrest, DNA repair, and apoptosis [12]. Inhibition of any one or all of these signaling proteins has the potential of interfering with Dox-induced apoptosis.
Since oxidative stress has been suggested to be the major cause for Dox-induced cardiotoxicity, we investigated the beneficial effect of Vit C which is a diet-derived antioxidant and is a quencher of reactive oxygen species (ROS) [13]. In a recent review, it has been highlighted that most of western population are unlikely to benefit from Vit C supplements because of their adequate nutritional status [14]. However, in the same study it has been prospected that “there could be a large subpopulation with a potential health problem that remains uninvestigated”. One such group is comprised of cancer patients which are generally depleted of Vit C [15] making them more vulnerable to oxidative stress-mediated injury. Although experimental studies have shown that Vit C does not interfere with antitumor activity of Dox and it prolongs the life of mice, rats and guinea pigs treated with Dox [16–19], there is no adequate information available about the downstream pathways involving ASK1, p38, and p53 leading to increase in such a survival. Thus, the present study focuses on the effect of Vit C on oxidative stress and different downstream steps involved in cell death induced by Dox in isolated cardiomyocytes.
Materials and methods
The investigation conforms to the guide for the care and use of laboratory animals approved by the University of Manitoba Animal Care Committee following the guidelines established by the Canadian Council on Animal Care.
Cardiomyocyte isolation
Cardiomyocytes were isolated from normal adult male Sprague–Dawley rats (250–300 g) using a previously described procedure [7]. Hearts were excised and mounted on a modified Langendorff perfusion apparatus. The perfusate (modified Krebs buffer) contained 110 mM NaCl, 2.6 mM KCl, 1.2 mM KH2PO4, 1.2 mM MgSO4, 25 mM NaHCO3, and 11 mM Glucose (pH 7.4). The Ca+2 free perfusion was then switched to recirculating mode with the buffer containing 25 mM calcium, 0.1% w/v collagenase, and 0.25% w/v bovine serum albumin, for 30 min. The collagenase-digested ventricles were chopped into small pieces and gently passed through pipettes with progressively smaller tip diameters and with an increasing concentration of CaCl2. The suspension was filtered through a nylon mesh (200 μm) and was allowed to settle for 10 min. The supernatant was discarded and the cell pellet was resuspended in medium M199 containing CaCl2 (1.8 mM). Cardiomyocytes (106 per dish) were plated in laminin-coated (20 μg/ml) polystyrene tissue culture dishes. Plated cells were incubated in serum-free culture medium M199 supplemented with antibiotics (streptomycin/penicillin, 100 mg/ml) at 37°C under a 5% CO2, 95% O2 air atmosphere. Two hours after plating, the culture medium was changed to remove unattached dead cells, and the viable cardiomyocytes were incubated overnight.
Treatment of cardiomyocytes
After initial incubation of 24 h, 95% of cardiomyocytes were viable and these cells were treated with one of the following: Control, cardiomyocytes cultured in M199 only; Vit C (5–100 μM) (Sigma); Dox (0.01–10 μM) (Adriamycin®, Pfizer); and combination of Vit C + Dox for 24 h.
Assessment of cardiomyocyte viability, ATP production, and cell leakage
Viability of the cultured cardiomyocytes was determined by trypan blue staining (Sigma), 0.4% (w/v). MTT (3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide, a tetrazole) (Sigma) assay was also performed to confirm viability of cells [20]. The yellow MTT is reduced to purple formazan in the mitochondria of living cells, therefore providing a measure of mitochondrial function and viability of cells. Cells were seeded in 96-well microplates with the same starting cell number per well (2 × 104 cells/well). After drug treatment, 5 mg/ml MTT was added to the media in each well and further incubated at 37°C for 2 h. All the remaining supernatant was removed carefully and 150 μl of dimethyl sulfoxide was added to each well and mixed thoroughly to dissolve the formed crystal formazan. After 10 min of incubation to ensure all crystal formazan were dissolved, the cytotoxicity of Dox was detected by measuring the absorbance of each well at 570 nm using ELISA plate reader. Mean absorbance of the treated group was quantified.
Adenosine triphosphate (ATP) was measured in cardiomyocytes using ViaLight BioAssay kit (Lonza). Cardiomyocytes (104 cells/well) were seeded into a 96 well white walled laminin-coated tissue culture plate, and allowed to settle overnight under normal culture conditions. After different treatments, the plates were incubated in a humidified atmosphere at 37°C, 5% (v/v) CO2 for 24 h. ATP monitoring reagent plus (100 μl) was added to each well and incubated for an additional 2 min. The plate was read on a Molecular Devices Lmax II microplate luminometer programmed to take a 1 s integrated reading of each well. Mean luminescence (RLU) of the all treated groups was quantified.
Cellular leakage was evaluated by measurement of the release of creatine kinase (CK) in the culture medium after treatment. A spectrophotometric assay was performed for CK with an ultraviolet-rate assay kit (Stanbio Laboratory, Boerne, TX). Mean absorbance of the treated groups was expressed as percentage of the control set as 100%.
Measurement of ROS
The level of oxidative stress was monitored by the measurement of ROS. Cardiomyocytes from different treatment groups in the culture dishes were washed with phosphate-buffered saline (PBS) and incubated with 10 μM solution of fluorescent probe, 5-(6)-chloromethyl-2070-dihydroflourescein diacetate probe (DCFDA) (Molecular Probes, Eugene, Oregon, USA) at 37°C for 30 min in a humidified chamber [21]. Fluorescent images from multiple fields per dish were recorded with the Olympus BX 51 fluorescent microscope with an excitation and emission wavelength of 488 and 525 nm, respectively. Fluorescence intensity was measured using digital image-processing software (Image Pro Plus).
Assessment of cardiomyocyte apoptosis
Apoptosis was determined by Hoescht 33258 (Sigma) staining of nuclei. For this, cardiomyocytes from different treatment groups in culture dishes were washed three times with PBS and incubated with Hoescht 33258 (1 mg/ml) for 10 min in a humidified chamber, protected from light, at 37°C. After staining, the culture plates were examined using fluorescent microscope (Olympus BX 51). Percentage of cells containing fragmented nuclei was counted.
Western blot analysis
Phosphorylated and total protein levels for ASK-1, p53, and p38, as well as caspase-3 cleavage, Bax, and Bcl-xl were measured by western blot [22] using specific antibody kits (Cell Signaling Technology). Proteins were extracted from control and treated cardiomyocytes in different groups in PBS containing protease (Roche Diagnostics, USA) and phosphatase inhibitor cocktails (Santa Cruz). The quantity of protein in the samples was measured by a dye-binding assay (Bio-Rad Laboratories). The protein samples (45 μg) were then subjected to 12% sodium dodecyl sulfate polyacrylamide gel electrophoresis and transferred to polyvinylidene difluoride (Roche Diagnostics, USA) membrane. Proteins bound to the membrane were detected with chemiluminescence blotting substrate kit (Roche Diagnostics, USA). Bands were visualized with Fluor S-MultiImager MAX System (Bio-Rad Laboratories, Canada) and quantified by image analysis software (Quantity One, Bio-Rad Laboratories, Canada). Mean densitometric units of the ratios (phospho/total/actin, cleaved/total/actin or Bax/bcl-xl/actin) of the treated groups were expressed as the percentage of the control set as 100%.
Statistical analysis
All experiments were done in duplicates for each treatment group and repeated five times (n = 5). For the study of viability test, ROS, and nuclear fragmentation, a total of 10 dishes (35 × 10 mm2) were prepared for each treatment group and ten different fields per dish were counted for the quantitative analysis. Data are expressed as the mean ± SEM. Groups were compared by one-way analysis-of-variance (ANOVA), and Bonferroni’s test was performed to identify differences between groups. P value of ≤0.05 was considered significant.
Results
Dose–response for Dox and Vit C
Concentration of the Dox as well as of Vit C used in this study were carefully selected. The dose of Dox (0.01–10 μM) and treatment protocol is based on our previous studies [6], as well as the pilot experiments done in the present study (Table 1). Furthermore, 10 μM of Dox has been reported to be clinically relevant, as at this dose, the drug is effective in its antitumor activity [23].
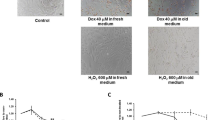
In order to determine the most optimal concentration of Vit C, in terms of viability of cells and ROS production, cardiomyocytes were exposed to Dox (10 μM) for 24 h in the presence of different concentrations of the vitamin (5, 10, 25, 50, and 100 μM) and these results are in Fig. 1. There was no significant protection at 5 and 10 μM of Vit C. The most optimal effect was seen at 25 μM and further increase to 50 and 100 μM of Vit C did not show any additional benefit. For this reason, 25 μM was chosen as the concentration of Vit C for further studies.
Cardiomyocytes treated with different concentrations of Vit C (5–100 μM) in the presence of doxorubicin (10 μM): Upper panel—viabillity of cells evaluated by Trypan Blue staining. Lower panel—reactive oxygen species (ROS) generation measured by DCFDA fluorescence. Data expressed as mean percentage ± SEM of five different experiments. *Significantly different (P < 0.05) from 5 to 10 μM
Cardiomyocyte viability and ATP levels
Trypan blue (0.4%) was used for the visualization of damaged cells. Intact cardiomyocytes in medium not stained with Trypan blue were counted along with the dead cells that picked up the stain. After 24 h of treatment, about 90% of cardiomyocytes were viable in the control and Vit C groups (Fig. 2a and b). Cell viability was reduced to 73% with Dox alone, while Dox in the presence of Vit C was able to significantly (P ≤ 0.05) prevent this decrease in the cell viability. The conversion of MTT substrate can also be directly related to the number of viable cells. A decrease in the ability of the cardiomyocytes to convert the MTT substrate was seen in a dose-dependent manner for different concentrations of Dox, and Vit C was able to counteract Dox effects, preserving mitochondrial function (Table 1). ATP levels were also measured to evaluate mitochondria function. For this, the highly sensitive ViaLight assay kit (Lonza) was used to provide accurate analysis with the advantage of the power of bioluminescent detection of ATP. ATP levels were significantly reduced in Dox group in a dose-dependent manner and this effect was mitigated in the presence of Vit C.
a, b Protective effects of Vit C on doxorubicin (10 μM) induced cell death. Cardiomyocytes were exposed to 25 μM of Vit C for 1 h prior to treatment with 10 μM of doxorubicin and cultured for a total of 24 h. a Representative images of adult rat cardiomyocytes. Dead cells are stained with trypan blue. b Percentage of viable cardiomyocytes: data are expressed as mean ± SEM of five different experiments. *Significantly different (P < 0.05) from control and # significantly different (P < 0.05) from the Dox group. Control cardiomyocytes cultured in M199; Dox with 10 μM of doxorubicin; Vit C with 25 μM of Vit C; and Dox (10 μM) + Vit C (25 μM)
ROS production and cardiomyocyte membrane leakage
Oxidative stress was monitored in terms of production of ROS (Fig. 3a, b). The production of intracellular ROS was increased by 98% in Dox-exposed cardiomyocytes. This Dox-induced increase in ROS production was significantly (P ≤ 0.05) mitigated in Dox + Vit C group. ROS levels were not different between control and Vit C-treated cells.
a, b ROS generation. a Representative DCFDA fluorescent microscopic images of adult rat cardiomyocytes. b Fluorescence intensity (percentage of control): data are expressed as mean ± SEM of five different experiments. *Significantly different (P < 0.05) from control and # significantly different (P < 0.05) from the Dox group. Symbols are the same as in Fig. 2
Cell injury was evaluated by the measurement of CK release from cardiomyocytes in the culture medium after treatment with Dox with and without Vit C (Fig. 4). Dox-treatment led to an increase in cellular damage shown by a significant increase (P ≤ 0.05) in CK release. Vit C alone did not show any significant effect but Dox-induced increase in CK release was significantly (P ≤ 0.05) decreased in the presence of Vit C.
Cell injury as indicated by CK release in the culture medium. Data are expressed as mean ± SEM of five different experiments. *Significantly different (P < 0.05) from control and # significantly different (P < 0.05) from the Dox group. Symbols are the same as in Fig. 2
Apoptosis
Dox-induced apoptosis and its modulation by Vit C were studied by staining the cardiomyocytes with Hoescht 33258 and these data are shown in Fig. 5. In the control group, the cells were rod-shaped, binucleated, and the nuclei had normal appearance. Exposure to Dox resulted in nuclear fragmentation (arrows) and the number of apoptotic cells significantly increased. Treatment with Vit C was able to significantly (P ≤ 0.05) decrease this change caused by Dox (Fig. 5a and b).
a, b Nuclear fragmentation as seen by Hoechst 33258 staining. Representative images (a) and quantitative analysis (b) of the nuclear fragmentation in adult rat cardiomyocytes. Data are expressed as mean ± SEM of five different experiments. *Significantly different (P < 0.05) from control and # significantly different (P < 0.05) from the Dox group. Symbols are the same as in Fig. 2
Pro- and anti-apoptotic proteins Bax and Bcl-xl were studied using western blot analysis. The ratio of Bax/Bcl-xl showed a significant increase in the Dox-challenged cardiomyocytes (Fig. 6a), whereas, Vit C was able to mitigate this change. Additionally, full length as well as cleaved caspase-3 proteins were examined (Fig. 6b). The activity of caspase-3 was expressed as the ratio of cleaved caspase-3 (17 kDa) over full length of caspase-3. When compared with the control, caspase-3 was activated (+30%) in Dox-treated cardiomyocytes. Vit C significantly decreased (P ≤ 0.05) this activation.
a, b The effects of different treatments on the Bax/Bcl-xl ratio (a) and Caspase 3 cleavage (b). In both figures, upper part is the western blot analysis and the lower part shows densitometric analysis. Data are expressed as mean ± SEM of five different experiments. *Significantly different (P < 0.05) from control and # significantly different (P < 0.05) from the Dox group. Symbols are the same as in Fig. 2
In an effort to understand the underlying mechanisms involved in Dox-induced cardiotoxicity, phosphorylated and total ASK-1, p38, and p53 were examined in cardiomyocytes from different treatment groups, and the data are shown in Fig. 7a–c. The activity of these proteins was expressed as the ratio of the phosphorylated to total protein. The activation of ASK-1, a MAPK kinase kinase, an upstream regulator of p38 was evaluated along with the downstream, p38. Phosphorylation and activation of ASK-1 and p38 in the Dox-treated cardiomyocytes showed a significant increase by 71 and 40%, respectively of the control (Fig. 7a and b). Vit C prevented significantly (P ≤ 0.05) this increase. Total levels of expression of p53 were also significantly higher 70% in the Dox group when compared to control levels. This increase in p53 activation was significantly (P ≤ 0.05) less when Vit C was present (Fig. 7c).
a–c The effects of different treatments on the ASK-1 (a), p38 (b), and p53 (c) activities. In each figure, upper part is the western blot analysis and the lower part is densitometric analysis. Data are expressed as mean ± SEM of five different experiments. *Significantly different (P < 0.05) from control and # significantly different (P < 0.05) from the Dox group. Symbols are the same as in Fig. 2
Discussion
In spite of significant improvements in the understanding of the subcellular basis of Dox-induced cardiomyopathy [1, 24], we still do not have an ideal cardioprotective drug to prevent this side effect of Dox [25]. Among different mechanisms for Dox-induced cardiotoxicity, occurrence of oxidative stress has gained significant support [5–7, 26, 27]. As a result, several different antioxidants have been tried to mitigate Dox-induced oxidative stress and thus cardiotoxicity [25, 28]. This study investigated the role of Vit C, a water soluble antioxidant, on Dox-induced oxidative stress in cardiomyocytes as well as downstream processes leading to apoptosis. We found that Dox altered cardiomyocytes permeability, increasing cell injury, and membrane leakage as indicated by CK release in the culture medium. This effect may be due to membrane solubility of Dox and its reported direct effects on the sarcolemma [5, 29]. A significant reduction in Dox-induced CK release by Vit C suggests maintenance of cell membrane integrity.
It is important to note that Vit C did not appear to improve cell oxidative stress status as well as its effects in the baseline situation in the control cells, treated with Vit C alone. It is likely that the antioxidant effects of Vit C come into play only under the enhanced oxidative stress condition such as is imposed by Dox. In this regard, antioxidants are reported to be beneficial only when oxidative damage contribute significantly to the disease pathology [30–32].
Along with the membrane damage caused by Dox, this study also showed a sharp increase in oxidative stress, MAPK and p53 activation followed by apoptotic cell death. There is evidence supporting oxidative stress as a major player in Dox-induced cardiomyopathy [5, 26]. Increase in oxidative stress can also lead to an activation of ASK-1, which activates c-Jun N-terminal kinase and p38 [9]. In this regard, we observed an increase in the activation of ASK-1 as well as p38 in Dox-challenged cardiomyocytes. Although Dox-induced increase in p38 has been reported earlier [7, 33], to the best of our knowledge this is the first time that the upstream MAPKKK, ASK-1, is reported to be activated in Dox-induced cardiotoxicity. The antioxidant effects of Vit C were evident from a significant decrease in ROS production in the cardiomyocytes exposed to Dox in the presence of this vitamin. Furthermore, this decrease in oxidative stress was associated with a decrease in ASK-1 and p38 activation. Antioxidants have been reported to reduce the activity of MAPKs in myocardial ischemia-reperfusion [34], further supporting a functional role of MAPKs in the oxidative stress-induced myocardial damage. Trolox, a water soluble antioxidant, was also able to decrease p38 activation and apoptosis in isolated adult cardiomyocytes challenged by Dox [7]. In addition, Vit C treatment of H9c2 (cardiomyocyte-like) cells has been reported to preserve endogenous antioxidants (superoxide dismutase, catalase, glutathione) in the presence of Dox [35]. Besides, Vit C is an important cofactor in many biological reactions [36].
Another important protein involved in Dox-induced cardiotoxicity is the tumor suppressor p53 [11]. Our results showed overexpression and activation of p53 in Dox-treated cardiomyocytes. One can speculate that the increase in apoptosis may be associated with the increase in p53. Vit C not only decreased Dox-induced p53 activation but there was also a decrease in apoptosis. In agreement with our findings, pitavastatin and quercetin were able to attenuate the Dox-induced cardiotoxicity by decreasing p53 activation and apoptosis [37, 38]. In addition, a reduction of p53 activity via genetic deletion [39] or chemical inhibition [40] was also found to be cardioprotective against Dox-induced apoptosis. Furthermore, a significant increase in the apoptotis may also have been supported by an increase in the expression of Bax/Bcl-xl ratio, caspase 3 cleavage, and DNA fragmentation. It has been reported that Dox can induce DNA damage, inhibit DNA and protein synthesis, inhibit transcription of specific gene programs, and induce cardiomyocyte apoptosis via a caspase-3-dependent mechanism [41]. This increase in pro-apoptotic proteins was mitigated by Vit C demonstrating that apoptosis can be partially prevented by this vitamin.
Considerable data indicate that cardiomyocyte death through apoptosis, necrosis, and other forms is a primary contributor to the progression of Dox-induced cardiomyopathy [42]. In our study, after Dox treatment, about 20% of the cells were dead as determined by trypan blue staining. Since the results showed more cardiomyocytes dying (20%) compared to 12% undergoing nuclear fragmentation and actual apoptotic cell death, it can be suggested that necrosis is also taking place. In addition, MTT assay and ATP levels, representing mitochondrial activity, showed a 22% reduction in Dox-treated cells when compared to control. The different types of cell death may result from the activation of various pathways that include oxidative stress, mitochondrial damage, DNA damage, and induction of pro-apoptotic proteins and cell membrane injury. Mitochondria have been suggested to play an important role in cell death due to autophagy, apoptotis, and necrosis [26, 42, 43]. From these data, it appears that Vit C was able to protect the cardiomyocytes from Dox-induced necrosis by rescuing the mitochondria thus preserving cell viability.
Vitamin C is considered to be one of the most potent and least toxic antioxidants for humans [44]. Although earlier studies on animals have shown that Vit C reduces cardiotoxicity [16–19], there is no adequate information about subcellular mechanisms of this beneficial effect. Vit C, which is readily soluble in water, can be seen to serve as an antioxidant in the water phase. However, Vit C is also known to regenerate Vit E from its reduced form [45]. Because of its solubility in lipids, Vit E serves as antioxidant in the lipid phase. Thus, our in vitro studies provide a strong basis for the design of further animal and clinical studies using Vit C.
This study suggests that physiological doses of Vit C could be beneficial as cardioprotective strategy to cancer patients. Some clinical studies did not find significant positive results with Vit C supplementation and a reduction of other cardiovascular diseases [46, 47]. The reason is likely to be related to the fact that these studies were performed in well-nourished populations and/or it could be simply due to the failure of these compounds to decrease oxidative damage in the subjects tested [48]. Therefore, it is imperative to have more studies like ours to determine the amount of the single agent that should be given to individuals. From our study, we can conclude that oxidative stress is a major player in Dox-induced cardiotoxicity, and effective antioxidant therapy can rescue the injury. Clinical trials often use oral administration in a single dose of the therapeutical strategy. Comparatively, in our study, Vit C was delivered in its active form directly to cells. Thus, titration of an appropriate oral dose to achieve target blood levels of Vit C appears to be of paramount importance. Due to its short half life [49], a frequent oral intake of physiological doses may be one alternative to achieve high plasma levels of Vit C. And cancer patients who generally present low concentrations of ascorbic acid in plasma [50] could benefit from Vit C supplementation. The Recommended Dietary Allowance (RDA) for Vit C is 90 and 75 mg/day for males and females, respectively. This recommendation continues to be based primarily on the prevention of deficiency diseases such as scurvy, rather than promotion of optimum health or the prevention of chronic diseases. In this regard, complete plasma saturation occurs at oral doses of ≥400 mg daily, achieving physiological blood concentrations of 60–100 μM [51]. In adults, there is significant evidence that Vit C is safe at a dose of 1 g/day [52]. We believe that doses within the RDA and 1 g/day taken in smaller amounts at frequent intervals could be tried as a cardioprotective adjunct therapy in the design of in vivo studies in order to benefit cancer patients.
In conclusion, Dox-induced cell death appears to be mediated by a direct membrane effect as well as intracytoplasmic changes and Vit C seems to offer protection against both changes. At the membrane level, this vitamin must detoxify peroxyl radicals in the aqueous phase before they can reach the lipid-rich membranes and initiate lipid peroxidation, protecting biomembranes against primary peroxidative damage [53, 54]. In the intracytoplasmic compartment, the cardioprotective effects of Vit C may also be associated with a decrease in oxidative stress as well as a decrease in the activation of ASK-1, p38, and p53, reducing apoptosis. Randomized clinical trials and epidemiological studies should be designed to evaluate whether patients receiving antioxidant therapy concomitantly with chemotherapy are less prone to Dox-induced cardiotoxicity.
References
Singal PK, Iliskovic N (1998) Doxorubicin-induced cardiomyopathy. N Engl J Med 339:900–905
Chatterjee K, Zhang J, Honbo N, Karliner JS (2010) Doxorubicin cardiomyopathy. Cardiology 115:155–162
Lefrak EA, Pitha J, Rosenheim S, Gottlieb JA (1973) A clinicopathologic analysis of adriamycin cardiotoxicity. Cancer 32:302–314
Yeh ET, Tong AT, Lenihan DJ, Yusuf SW, Swafford J, Champion C, Durand JB, Gibbs H, Zafarmand AA, Ewer MS (2004) Cardiovascular complications of cancer therapy: diagnosis, pathogenesis, and management. Circulation 109:3122–3131
Singal PK, Iliskovic N, Li T, Kumar D (1997) Adriamycin cardiomyopathy: pathophysiology and prevention. FASEB J 11:931–936
Kumar D, Kirshenbaum LA, Li T, Danelisen I, Singal PK (2001) Apoptosis in adriamycin cardiomyopathy and its modulation by probucol. Antioxid Redox Signal 3:135–145
Lou H, Kaur K, Sharma AK, Singal PK (2006) Adriamycin-induced oxidative stress, activation of MAP kinases and apoptosis in isolated cardiomyocytes. Pathophysiology 13:103–109
Matsuzawa A, Nishitoh H, Tobiume K, Takeda K, Ichijo H (2002) Physiological roles of ASK1-mediated signal transduction in oxidative stress- and endoplasmic reticulum stress-induced apoptosis: advanced findings from ASK1 knockout mice. Antioxid Redox Signal 4:415–425
Matsuzawa A, Ichijo H (2008) Redox control of cell fate by MAP kinase: physiological roles of ASK1-MAP kinase pathway in stress signaling. Biochim Biophys Acta 1780:1325–1336
Lou H, Danelisen I, Singal PK (2005) Involvement of mitogen-activated protein kinases in adriamycin-induced cardiomyopathy. Am J Physiol Heart Circ Physiol 288:H1925–H1930
Suzuki K, Inageda K, Nishitai G, Matsuoka M (2007) Phosphorylation of p53 at serine 15 in A549 pulmonary epithelial cells exposed to vanadate: involvement of ATM pathway. Toxicol Appl Pharmacol 220:83–91
Gutteridge JM, Halliwell B (2000) Free radicals and antioxidants in the year 2000. A historical look to the future. Ann NY Acad Sci 899:136–147
Lykkesfeldt J, Poulsen HE (2010) Is vitamin C supplementation beneficial? Lessons learned from randomised controlled trials. Br J Nutr 103:1251–1259
Mayland CR, Bennett MI, Allan K (2005) Vitamin C deficiency in cancer patients. Palliat Med 19:17–20
Fujita K, Shinpo K, Yamada K, Sato T, Niimi H, Shamoto M, Nagatsu T, Takeuchi T, Umezawa H (1982) Reduction of adriamycin toxicity by ascorbate in mice and guinea pigs. Cancer Res 42:309–316
Shimpo K, Nagatsu T, Yamada K, Sato T, Niimi H, Shamoto M, Takeuchi T, Umezawa H, Fujita K (1991) Ascorbic acid and adriamycin toxicity. Am J Clin Nutr 54:1298S–1301S
Wold LE, Aberle NS 2nd, Ren J (2005) Doxorubicin induces cardiomyocyte dysfunction via a p38 MAP kinase-dependent oxidative stress mechanism. Cancer Detect Prev 29:294–299
Santos RV, Batista ML Jr, Caperuto EC, Costa Rosa LF (2007) Chronic supplementation of creatine and vitamins C and E increases survival and improves biochemical parameters after Doxorubicin treatment in rats. Clin Exp Pharmacol Physiol 34:1294–1299
Lai KB, Sanderson JE, Yu CM (2009) High dose norepinephrine-induced apoptosis in cultured rat cardiac fibroblast. Int J Cardiol 136:33–39
Chua CC, Liu X, Gao J, Hamdy RC, Chua BH (2006) Multiple actions of pifithrin-alpha on doxorubicin-induced apoptosis in rat myoblastic H9c2 cells. Am J Physiol Heart Circ Physiol 290:H2606–H2613
Sharma AK, Dhingra S, Khaper N, Singal PK (2007) Activation of apoptotic processes during transition from hypertrophy to heart failure in guinea pigs. Am J Physiol Heart Circ Physiol 293:H1384–H1390
Laemmli UK (1970) Cleavage of structural proteins during the assembly of the head of bacteriophage T4. Nature 227:680–685
McHowat J, Swift LM, Arutunyan A, Sarvazyan N (2001) Clinical concentrations of doxorubicin inhibit activity of myocardial membrane-associated, calcium-independent phospholipase A(2). Cancer Res 61:4024–4029
Minotti G, Menna P, Salvatorelli E, Cairo G, Gianni L (2004) Anthracyclines: molecular advances and pharmacologic developments in antitumor activity and cardiotoxicity. Pharmacol Rev 56:185–229
Ludke AR, Al-Shudiefat AA, Dhingra S, Jassal DS, Singal PK (2009) A concise description of cardioprotective strategies in doxorubicin-induced cardiotoxicity. Can J Physiol Pharmacol 87:756–763
Zhou S, Starkov A, Froberg MK, Leino RL, Wallace KB (2001) Cumulative and irreversible cardiac mitochondrial dysfunction induced by doxorubicin. Cancer Res 61:771–777
Mizutani H, Tada-Oikawa S, Hiraku Y, Kojima M, Kawanishi S (2005) Mechanism of apoptosis induced by doxorubicin through the generation of hydrogen peroxide. Life Sci 76:1439–1453
Quiles JL, Huertas JR, Battino M, Mataix J, Ramirez-Tortosa MC (2002) Antioxidant nutrients and adriamycin toxicity. Toxicology 180:79–95
Singal PK, Panagia V (1984) Direct effects of adriamycin on the rat heart sarcolemma. Res Commun Chem Pathol Pharmacol 43:67–77
Halliwell B (2001) Role of free radicals in the neurodegenerative diseases: therapeutic implications for antioxidant treatment. Drugs Aging 18:685–716
Galli RL, Shukitt-Hale B, Youdim KA, Joseph JA (2002) Fruit polyphenolics and brain aging: nutritional interventions targeting age-related neuronal and behavioral deficits. Ann NY Acad Sci 959:128–132
Steinberg D, Witztum JL (2002) Is the oxidative modification hypothesis relevant to human atherosclerosis? Do the antioxidant trials conducted to date refute the hypothesis? Circulation 105:2107–2111
Kang YJ, Zhou ZX, Wang GW, Buridi A, Klein JB (2000) Suppression by metallothionein of doxorubicin-induced cardiomyocyte apoptosis through inhibition of p38 mitogen-activated protein kinases. J Biol Chem 275:13690–13698
Qin F, Shite J, Liang CS (2003) Antioxidants attenuate myocyte apoptosis and improve cardiac function in CHF: association with changes in MAPK pathways. Am J Physiol Heart Circ Physiol 285:H822–H832
Kim DS, Kim HR, Woo ER, Kwon DY, Kim MS, Chae SW, Chae HJ (2006) Protective effect of calceolarioside on adriamycin-induced cardiomyocyte toxicity. Eur J Pharmacol 541:24–32
Arrigoni O, De Tullio MC (2002) Ascorbic acid: much more than just an antioxidant. Biochim Biophys Acta 1569:1–9
Pei TX, Xu CQ, Li B, Zhang ZR, Gao XX, Yu J, Li HZ, Yang BF (2007) Protective effect of quercetin against adriamycin-induced cardiotoxicity and its mechanism in mice. Yao Xue Xue Bao 42:1029–1033
Yoshida M, Shiojima I, Ikeda H, Komuro I (2009) Chronic doxorubicin cardiotoxicity is mediated by oxidative DNA damage-ATM-p53-apoptosis pathway and attenuated by pitavastatin through the inhibition of Rac1 activity. J Mol Cell Cardiol 47:698–705
Shizukuda Y, Matoba S, Mian OY, Nguyen T, Hwang PM (2005) Targeted disruption of p53 attenuates doxorubicin-induced cardiac toxicity in mice. Mol Cell Biochem 273:25–32
Liu X, Chua CC, Gao J, Chen Z, Landy CL, Hamdy R, Chua BH (2004) Pifithrin-alpha protects against doxorubicin-induced apoptosis and acute cardiotoxicity in mice. Am J Physiol Heart Circ Physiol 286:H933–H939
Zhang YW, Shi J, Li YJ, Wei L (2009) Cardiomyocyte death in doxorubicin-induced cardiotoxicity. Arch Immunol Ther Exp (Warsz) 57:435–445
Lebrecht D, Walker UA (2007) Role of mtDNA lesions in anthracycline cardiotoxicity. Cardiovasc Toxicol 7:108–113
Wallace KB (2007) Adriamycin-induced interference with cardiac mitochondrial calcium homeostasis. Cardiovasc Toxicol 7:101–107
Sauberlich HE (1994) Pharmacology of vitamin C. Annu Rev Nutr 14:371–391
Amorati R, Ferroni F, Lucarini M, Pedulli GF, Valgimigli L (2002) A quantitative approach to the recycling of alpha-tocopherol by coantioxidants. J Org Chem 67:9295–9303
Losonczy KG, Harris TB, Havlik RJ (1996) Vitamin E and vitamin C supplement use and risk of all-cause and coronary heart disease mortality in older persons: the established populations for epidemiologic studies of the elderly. Am J Clin Nutr 64:190–196
Kushi LH, Folsom AR, Prineas RJ, Mink PJ, Wu Y, Bostick RM (1996) Dietary antioxidant vitamins and death from coronary heart disease in postmenopausal women. N Engl J Med 334:1156–1162
Halliwell B (2009) The wanderings of a free radical. Free Radic Biol Med 46:531–542
Verrax J, Calderon PB (2009) Pharmacologic concentrations of ascorbate are achieved by parenteral administration and exhibit antitumoral effects. Free Radic Biol Med 47:32–40
Goncalves TL, Erthal F, Corte CL, Muller LG, Piovezan CM, Nogueira CW, Rocha JB (2005) Involvement of oxidative stress in the pre-malignant and malignant states of cervical cancer in women. Clin Biochem 38:1071–1075
Padayatty SJ, Sun H, Wang Y, Riordan HD, Hewitt SM, Katz A, Wesley RA, Levine M (2004) Vitamin C pharmacokinetics: implications for oral and intravenous use. Ann Intern Med 140:533–537
Meadows GG, Pierson HF, Abdallah RM (1991) Ascorbate in the treatment of experimental transplanted melanoma. Am J Clin Nutr 54:1284S–1291S
Frei B, England L, Ames BN (1989) Ascorbate is an outstanding antioxidant in human blood plasma. Proc Natl Acad Sci USA 86:6377–6381
Niki E (1991) Action of ascorbic acid as a scavenger of active and stable oxygen radicals. Am J Clin Nutr 54:1119S–1124S
Acknowledgment
The support from the Canadian Circulatory and Respiratory Institute (Dr. Singal) is greatly acknowledged. Mrs. Ana Ludke is supported by a studentship from Manitoba Health Research Council. Dr. Pawan Singal is holder of the Naranjan Dhalla Chair in Cardiovascular Research supported by the St. Boniface Hospital and Research Foundation.
Conflict of Interest
The authors have declared no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ludke, A., Sharma, A.K., Bagchi, A.K. et al. Subcellular basis of vitamin C protection against doxorubicin-induced changes in rat cardiomyocytes. Mol Cell Biochem 360, 215–224 (2012). https://doi.org/10.1007/s11010-011-1059-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-011-1059-z