Abstract
Two isoforms of guanylate cyclase, GC1 and GC2 encoded by GUCY2D and GUCY2F, are responsible for the replenishment of cGMP in photoreceptors after exposure to light. Both are required for the normal kinetics of photoreceptor sensitivity and recovery, although disease mutations are restricted to GUCY2D. Recessive mutations in this gene cause the severe early-onset blinding disorder Leber congenital amaurosis whereas dominant mutations result in a later onset less severe cone–rod dystrophy. Cyclase activity is regulated by Ca2+ which binds to the GC-associated proteins, GCAP1 and GCAP2 encoded by GUCA1A and GUCA1B, respectively. No recessive mutations in either of these genes have been reported. Dominant missense mutations are largely confined to the Ca2+-binding EF hands of the proteins. In a similar fashion to the disease mechanism for the dominant GUCY2D mutations, these mutations generally alter the sensitivity of the cyclase to inhibition as Ca2+ levels rise following a light flash.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Retinal-specific guanylate cyclases (GCs) and their associated activator proteins (GCAPs) are responsible for the Ca2+-sensitive restoration of cGMP levels after the light activation of the phototransduction cascade. These proteins play a central role in phototransduction (Fig. 1) and it is perhaps not surprising that mutations in the corresponding genes result in blinding disorders.
Guanylate cyclases
Early studies showed that two forms of guanylate cyclase are present in rod and cone photoreceptors [1–3]. Both show inhibition by Ca2+ (reviewed in [4, 5]) via interaction with GCAPs. GCAPs bind constitutively to GCs; in the absence of Ca2+, they stimulate cyclase activity whereas in the presence of Ca2+, they are inhibitory. The human forms (retGC1 and retGC2) are encoded by the genes GUCY2D and GUCY2F but are referred to as ROS-GC1 and ROS-GC2 in bovine and GC-E and GC-F in mouse. In this review, the notation of GC1 and GC2 will be adopted. Both genes comprise 18 coding exons plus a 5′ and a 3′ non-coding exon that specify proteins with predicted functional domains that consist of an extracellular or intradiskal domain, a transmembrane segment, a kinase homology domain, a dimerization domain and a catalytic domain (Fig. 2a). Sequence motifs within the kinase homology domain are important for interactions with GCAPs [6, 7] although the critical region for this lies within the catalytic domain [8–11]. GC1 is detected in the retina, pineal gland, olfactory bulb, cochlear nerve and organ of Corti [12–14], whereas GC2 is found only in the retina. cGMP synthesis requires dimerization to create the catalytic site of the cyclase and this is achieved by an α-helical coiled-coil structure that maintains the interaction between subunits [15] (Fig. 2b). Heterodimers between GC1 and GC2 subunits can be formed in vitro, although experiments with retinal tissue indicate that homodimers predominate [16].
a Exons of GC1 gene and corresponding protein domain structure. b Schematic model of the regulation of wild-type GC1 by GCAP1 under light and dark conditions. Maximal activation occurs only at free Ca2+ concentrations below 100 nM, and above 1 μM < 10% activity persists. c Arg838 mutant GC1 alters the position of the equilibrium as a result of the increased stability of the coiled-coil structure holding the activated dimer together. In consequence 60% of maximal activation by GCAP1 persists at high Ca2+ concentrations
The relative roles of GC1 and GC2 in phototransduction have been clarified largely through the study of mouse mutants with null mutations in GC1 and GC2, respectively. Disruption of GC1 while leaving GC2 intact [17] had little effect on rod numbers or rod morphology but increased the rate of recovery of rods from a light flash. In contrast, cones appeared initially unaffected, but had disappeared by 5 weeks of age [17, 18]. Scotopic electroretinogram (ERG) a- and b-wave amplitudes were reduced in GC1 −/− mutant mice but were completely absent in GC1 −/− GC2 −/− double knockout mice, confirming that no other guanylate cyclase is present that is functional in retinal phototransduction. Delayed recovery of the a-wave in GC1 −/− and GC2 −/− mice indicates that both contribute to the recovery of photoreceptors after exposure to intense bleaching. Dark currents of GC1 −/− and GC2 −/− mice were not significantly different from wild type (WT); the basal activity of either GC1 or GC2 is sufficient therefore to maintain dark current in rods. The sensitivity of GC2 −/− rods was similar to WT whereas the sensitivity of GC1 −/− rods was about 3.5 fold higher than WT. These findings suggest an important physiological role of both GC1 and GC2, with neither alone being able to support normal phototransduction. It is therefore surprising that mutations in GC2 associated with retinal disorders have yet to be identified.
Recessive mutations in GC1
Recessive mutations in GC1 are a major cause of Leber congenital amaurosis (LCA). It is now recognised that LCA represents the most severe end of the spectrum of infantile onset rod–cone dystrophies. This has led to the use of the term early onset severe retinal dystrophy (EOSRD) to describe this group of disorders. LCA was first described by Theodore Leber in 1869 [19], and although it has a population frequency of only about 1 in 30,000, it is a major cause of blindness in children [20]. It presents at birth or soon after with severe visual loss, sensory nystagmus, reduced or absent papillary response and a flat ERG. Visual acuity ranges from 20/200 to light perception, with progression not being a feature of all EOSRD phenotypes (Fig. 3). The underlying genetic cause is heterogeneous and the associated phenotype varying with the gene involved. Recessive mutations in 14 different genes have now been described [21]. However, the first gene to be associated with LCA was GC1 [22]. Recessive mutations in GC1 are one of the most common causes of LCA, with a variable frequency ranging from 21% [23] to 12% [24] of all LCA cases depending on the population studied. Mutations are scattered across the gene, with reported mutations in most coding exons, in several introns, and in the 5′-UTR [22, 23, 25–32]. A post-mortem study [33] of the eye of a patient diagnosed with LCA associated with a missense mutation in one allele of GC1 and a putative deletion in the other demonstrated that rods and cones, although absent in the mid-periphery of the retina, were still present in the macular and far periphery of the retina. These photoreceptors lacked outer segments. Cones formed a monolayer of cells bodies but rods were clustered and had sprouted neurites in the periphery. The presence of significant numbers of residual photoreceptors is encouraging for the potential success of future gene therapy-related treatment studies.
Many of the LCA-1-causing GC1 mutations are nonsense mutations that if translated would encode truncated proteins which would lack domains critical to normal function, although the intervention of nonsense-mediated mRNA decay would most likely mean that no protein is produced, resulting in the total absence of cyclase activity. There are nevertheless several missense mutations; those within the catalytic domain show severely reduced or absent cyclase activity as a direct interference with the catalytic site [34–37] whereas those within the extracellular domain have only a moderate effect on cyclase activity [37] (Fig. 4). It is presumed in the latter cases that misfolding of the mutant protein results in degradation and thereby loss of activity [36, 37].
Recessive LCA-1 mutations. a Basal and stimulated in vitro activity of WT and mutant GCs with Pro858 and Leu954Pro catalytic domain mutations. b Basal and stimulated in vitro activity of WT and mutant GCs with Cys105Tyr and Leu325Pro extracellular domain mutations. Mutant GCs were expressed and analysed in vitro either singly or in combination. Redrawn from [37]
A dominant negative effect of the Pro858Ser and Leu954Pro mutations has been demonstrated in in vitro activity studies [37]. Both mutations severely impair basal and GCAP-stimulated catalytic activity of the enzyme, and when co-expressed with a WT allele, show a reduced activity of GC1. This is consistent with a dominant negative effect as indicated by cone ERG abnormalities in heterozygous carriers of the Leu954Pro mutation [20].
A novel mutation in GC1 underlies an early onset form of retinitis pigmentosa which presents as a severe rod–cone dystrophy with progressive high myopia and macular preservation [38]. The disorder was shown to arise from a homozygous 4 bp insertion in exon 19 of GC1, a mutation which would be expected to result in a 28 amino acid elongation of the protein. The cyclase generated by this recessive mutation may not therefore lack activity as expected for typical LCA-1 mutations. However, when present in the heterozygous state with a more typical GC1 null mutation, it nevertheless gave rise to a typical LCA-1 phenotype [38].
Animal models and treatments
The GC1 knock out mutation in the mouse results in a null allele with a partially deleted exon 5 [18]. It would appear to be a good genetic model for LCA since in both mutant mice and human patients, activity of GC1 is either absent or severely curtailed. Results show that the rate of cone cell loss in the GC1 −/− null mutant mice is comparable to that found in humans with LCA [18, 39]. Cones are still abundant at 2 months but show a gradual decrease. They have highly disorganized outer segments [17], reduced levels of cone opsins, and lack cone transducin (α and γ subunits), cone α′ phosphodiesterase and the G-protein-coupled receptor kinase 1 [17]. The light dependent translocation of cone arrestin was also absent but could be restored by gene therapy treatment of GC −/− mice with an AAV-GC1 construct [40], indicating a role for GC1 in the trafficking of these proteins within photoreceptors. The translocation of rod arrestin and rod α-transducin in rod photoreceptors were, however, not affected [41]. These observations indicate a severe cone dystrophy which does not extend to the rods, unlike LCA/EOSRD in humans. Rods appear morphologically normal, although they do display altered responses to light [18].
The retinal degeneration (rd) mutation in chickens, first identified in Rhode Island Reds [42], arises from a deletion/insertion mutation in the avian GC1 orthologue. In this mutation, exons 4–7 are replaced by an 81-bp fragment with 89% sequence identity to a portion of exon 9 in reverse orientation [43, 44]. The reading frame is not disrupted by this event but the mutant protein would be predicted to lack the membrane-spanning domain and flanking regions; it is unlikely that any cyclase activity would be retained. This chicken mutant thereby shares a common genetic basis therefore to LCA-1 in man. At hatching the retinae of affected chicks appear morphologically normal but no ERG can be measured under either light- or dark-adapted conditions [42]. Rods and cones of affected animals undergo degenerative changes after about 1 week post-hatching, with clear signs of reduced and disorganized outer segments and photoreceptor loss by 21 days, in keeping with human LCA/EOSRD. By 6 months, very few photoreceptor inner segments and nuclei remain. Pathological changes were frequently noted in the pigment epithelium overlying the degenerating retina. Recent trials with a lentivirus-based gene transfer vector carrying the GC1 gene injected into early-stage mutant embryos showed a partial restoration of ERG responses and a slowing in the rate of retinal degeneration [45].
Dominant mutations in cone and cone–rod dystrophies
The cone and cone–rod dystrophies are both clinically and genetically heterogeneous. They represent a group of progressive retinal disorders which are an important cause of blindness in childhood and early adulthood [46]. The first dominant mutation in GC1 was identified in an extended family (designated as CORD6) with a severe cone–rod dystrophy (CORD) [47] in which linkage analysis had previously mapped the disease gene to chromosome 17p12–p13 [48]. CORD in this family displayed an early onset, with marked loss of central vision in the first decade and peripheral field loss by the fourth decade. Affected subjects often had photophobia, nystagmus and myopia. Fundoscopy revealed a ‘bull’s eye’ maculopathy early in the disease, with later involvement of the peripheral retina (Fig. 5). ERGs showed no detectable cone responses early in disease, with progressive abnormality of rod responses appearing later [49–51]. The ERG was often ‘electronegative’, suggesting early involvement of inner retinal neurons.
Two heterozygous missense mutations in adjacent codons were identified in the CORD6 family that encode Glu837Asp and Arg838Ser substitutions [47, 52]. A second CORD family was subsequently identified [53] with changes in three adjacent codons that result in Glu837Asp, Arg838Cys, Thr839Met substitutions. The disease-causing change is, however, most likely the substitution at site 838 as subsequent CORD patients identified with mutations in GC1 possess only a codon 838 change (Table 1).
Mutations in GC1 are a major cause of dominant cone–rod and cone dystrophies, accounting for up to 35% of all such cases [51, 52, 54]. With one exception, all are confined to codon 838. The exception is a mutation in exon 8 that encodes a Pro575Leu substitution within the kinase-homology domain of the cyclase [55]. The clinical phenotype of this disorder is more accurately described as a dominant cone dystrophy as scotopic (rod) function was normal but photopic function was generally absent.
Mutations at site 838 of GC1 have been subjected to functional analysis of cyclase activity [56, 57]. When modelled in vitro, the Arg838 substitutions result in an increase in the apparent affinity of GC1 for GCAP-1 and a decrease in the Ca2+ sensitivity of the GCAP-1 mediated response, thereby allowing the catalytic activity of the mutant protein to be stimulated by GCAP-1 at higher Ca2+ concentrations than WT (Fig. 6). Stimulation by GCAP-2 is also dramatically reduced [56]. The effect of substitutions at site 838 on the Ca2+ sensitivity of the GCAP1 activation increases from WT < R838C < R838H < R838A < R838S [57]. This is consistent with the report that patients with Arg838Cys or Arg838His substitutions have milder clinical phenotypes that the original CORD6 patients with a Arg838Ser substitution [46, 49].
In vitro wild type and mutant GC1 activity at varying free Ca2+ concentrations. Activities are presented as percentages of maximum GC1 activation. WT: filled circles, solid line. Arg858Cys: open circles, dashed line. Arg858Ser: squares, dotted line. Arg858His: triangles, dotted and dashed line. Shaded boxes indicate Ca2+ concentrations in light and dark. Re-drawn from [57]
The cyclase activity of GC1 requires dimerization to form the catalytic site [15]. This dimerization requires an α-helical coiled-coil structure between the dimerization domains of the two subunits (Fig. 2b). The strength of this coiled-coil structure must be strictly regulated for normal interaction with GCAP1; this is altered by substitutions at site 838 which disrupt a small network of salt bridges and allows an abnormal extension of the coiled-coil structure (Fig. 2c) and thereby a reduction in Ca2+ sensitivity of the cyclase [15, 57]. An alternative explanation is that these substitutions cause a change in the relative affinities of the mutant cyclases for Ca2+- and Mg2+-bound forms of GCAPs [58]. In either case, mutant cyclase activity would be maintained at high physiological intracellular Ca2+ concentrations.
Guanylate cyclase activating proteins
The guanylate cyclase activating proteins belong to a family of neuronal Ca2+ sensors. In many mammalian species including human, chimpanzee, macaque and dog [59], three forms of GCAP have been identified (GCAP1 encoded by GUCA1A, GCAP2 encoded by GUCA1B and GCAP3 encoded by GUCA1C) but only GCAP1 and GCAP2 are present in the mouse genome, GCAP3 being represented as a pseudogene [60]. Immunocytochemical studies in mice have shown that GCAP1 is expressed in rods and cones whereas GCAP2 is predominately expressed in rods and may also be present in cells of the inner retina [61–63]. In lower vertebrates, additional copies may be present, with up to eight different GCAP genes in teleosts [60, 64]. In humans, GCAP1 and GCAP2 are expressed in rod and cone photoreceptors, whereas GCAP3 is expressed in cones only [60, 65].
Immunolabelling studies [66] have shown that GCAP1 is predominantly present in cone outer segments with only sparse and low level labelling in rod outer segments. In contrast, GCAP2 is more concentrated in rods than cones, although the synaptic regions of both types of photoreceptors were labelled. The different localizations of GCAPs suggest that the roles of GCAP1 and GCAP2 may be different.
The genes for GCAP1 (GUCA1A) and GCAP2 (GUCA1B) are arranged in a tail-to-tail array on human chromosome 6p21.1 [67] and mouse chromosome 17 [62] whereas GCAP3 (GUCA1C) is on human chromosome 3q13.1. The GCAP proteins contain four EF hands that each comprise a helix-loop-helix conformation, with EF1 modified for interface with GCs [68], leaving EF2-4 for Ca2+ binding (Fig. 7). These loops have canonical Ca2+ binding sites formed by acidic residues for Ca2+ coordination. EF1 and 2 are contained within the N-terminal domain of the protein whereas EF3 and 4 are within the C-terminal region [69]. Many members of the family of neuronal calcium sensors have a ‘calcium-myristoyl switch’ where a myristoyl group is buried inside the protein in the Ca2+-free state but becomes fully exposed on Ca2+-binding. However, GCAP2 has been shown to lack a Ca2+ -myristoyl switch [70, 71] and recent studies on the conformational structure of GCAP1 indicates that the myristoyl group remains fully buried in both the Ca2+-free and Ca2+-bound state [72].
a Fundus photographs showing bilateral macular atrophy, more marked in the left than right eye. b Typical electrophysiological findings seen in isolated cone dystrophy. The rod specific and maximal ERGs fall within the normal range. The 30 Hz flicker ERG is both delayed and reduced, typical of most cone dystrophies. The photopic single flash ERG is markedly subnormal with particular reduction in the b-wave. However, it is of note that cone single flash and flicker ERGs often have minimal implicit time shift (delay) in subjects harbouring GCAP1 Tyr99Cys mutations [96]. The pattern ERG (PERG) is profoundly subnormal in keeping with marked macular involvement. Figure kindly provided by Professor Graham E. Holder, Moorfields Eye Hospital
The relative roles of GCAP1 and GCAP2 have been largely determined by studies with mouse knockout mutations. In mice in which both genes have been disrupted, GC activity lacks Ca2+ dependence, confirming the role of GCAPs in the Ca2+ regulation [73]. In these mice, flash responses from dark-adapted rods are larger and slower than WT, and incremental flash sensitivity of rods fails to be maintained at a WT type level. Restoration of GCAP2 production via a transgene restores maximal light-induced GC activity but does not restore normal kinetics to responses evoked by saturating flashes [73]. In contrast, the provision of GCAP1 via a transgene shows that the degree of recovery of the rod a-wave is correlated with the level of expression of GCAP1. In single cell recordings, the majority of rods generated flash responses identical to WT [74].
A more direct study of the role of GCAP2 on phototransduction has been carried out in mice with a disrupted GCAP2 gene but retaining a fully functional GCAP1 gene [75]. In these mice, rod viability and outer segment morphology appeared normal, and there were no compensatory changes in the levels of GC1, GC2 or GCAP1. However, there was a two-fold drop in the maximal rate of cGMP synthesis at low Ca2+ concentrations, and an increase in the Ca2+ concentration at which the half-maximal rate of cGMP synthesis was achieved. Flash responses recovered more slowly than WT and rods were more sensitive to flashes but tended to saturate at lower intensities. GCAP2 is necessary therefore for normal recovery of rods and for light adaptation; for the rapid activation and deactivation of GC activity in response to light, both isoforms of GCAP are required.
Cone responses are also affected by GCAP-knockout mutations. Under cone isolation conditions, ERGs recorded from mice lacking both GCAP1 and GCAP2 had normal amplitudes of the saturated a-wave and b-wave [76]. However, the b-wave was widened, there was an increase in the sensitivity of both M- and UV-cones, and the recoveries of the cone-driven a-wave and b-wave were delayed. Restoration of GCAP1 via a transgene showed that recovery of the cone-driven a-wave was restored to normal, although the recovery of the cone-driven b-wave was slightly faster than that observed in WT mice. These studies reveal that the absence of GCAP1 and GCAP2 delays the recovery of light responses, and that GCAP1 restores the recovery of cone responses in the absence of GCAP2 [76], suggesting a more important role for GCAP1 in cone phototransduction, consistent with the proposal that GCAP1 is more highly expressed in cones than in rods [66].
Mutations in GCAPs
No mutations in GCAP3 have so far been found in retinal disease [77]. A dominant Gly157Arg missense mutation in GCAP2 was identified in three independent families with incomplete penetrance and a spectrum of disease phenotypes that included retinitis pigmentosa (RP), RP with macular involvement and macular degeneration [78]. The first reported mutation in GCAP1 was a missense mutation in codon 99 that results in the replacement of a highly conserved Tyr with Cys (Tyr99Cys) [79]. Other reported mutations are listed in Table 2. The clinical phenotype for Tyr99Cys patients was initially reported as an isolated progressive cone dystrophy [79] and this is a feature of many of the other GCAP1 mutations [46], although a recent clinical re-evaluation of the original family with the Tyr99Cys mutation [80] found a range of phenotypes that included reduced cone and rod responses (with cone loss greater than rod, in keeping with CORD), and isolated macular dysfunction (Fig. 7). This demonstrates the extent of intrafamilial heterogeneity in retinal dysfunction that may be present in persons with the same gene mutation. All affected subjects complained of mild photophobia and reduced central vision and colour vision. Onset is between the third and fifth decade, with subsequent gradual deterioration of visual acuity and colour vision.
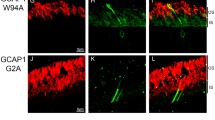
The Tyr99Cys substitution (Fig. 8) is located in the helical region of EF3 and does not interfere with the ability of mutant GCAP1 to activate GC1 at low Ca2+ concentrations but does prevent Ca2+-bound mutant GCAP1 from inhibiting GC1, thus making GC constitutively active at physiological Ca2+ concentrations. Tyr99 is part of a hydrogen bond network that includes Ser173 and Tyr55; the Tyr99Cys substitution would disrupt this network and thereby destabilize the specific inter-domain orientation of the Ca2+-bound GCAP [69]. Another mutation that is reported to cause a cone dystrophy results from an Asn104Lys substitution in EF3 [81].
GCAP1 model based on the crystal structure of GCAP3. a Mutated residues Tyr99, Ile143, Leu151, Glu155 which alter Ca2+ sensitivity are coloured in green. Residue Pro50 where mutation appears to reduce stability is shown in yellow. b Close up of residues around residue Tyr99 showing the hydrogen bonding interaction with Ser173 from the kinked C-terminal helix (coloured orange). c Close up of the Ca2+-binding loops of EF 3 and 4 showing the highlighting the Ca2+-coordinating function of Glu155 and the hydrophobic pocket that accommodates residues Ile143 and Leu151. Note color is only available in the online version of the figure. Reproduced from [69] with permission
The Glu155Gly substitution in the loop region of EF4 replaces the negatively charged Glu residue that is directly responsible for coordinating Ca2+ with an uncharged residue, Gly. Two other sites in EF4 where mutations have been reported are Leu151 [82, 83] and Ile143 [84]. The former is a simple point mutation generating a Leu151Phe substitution, but the latter is a complex change involving a single bp deletion in codon 143 followed by a 4 bp insertion which results in the substitution of Ile by Asn and the insertion of Thr (Ile143AsnThr) [84]. This mutation was identified in two patients (father and son) with dominant cone degeneration. A histopathological evaluation of the father’s eyes at autopsy (age 75 years) showed no foveal cones but a few, scattered cones remaining in the peripheral retina. The side-chains of Ile143 and Leu151 lie in the hydrophobic pocket that stabilizes the conformational structure of EF4 and the replacement by Asn/Thr and Phe, respectively, may interfere with the hydrophobic core and Ca2+-binding loop of EF4 [69].
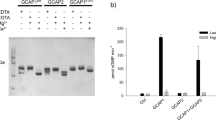
Functional in vitro analyses of GCAP1 mutations have been carried out with the Tyr99Cys [85–87], Gly155Gly [88], Ile143AsnThr [84], Glu89Lys, Asp100Glu and Gly159Val [89] substitutions; in all cases, the substitutions alter the level of cyclase inactivation at higher Ca2+ concentrations (Fig. 9). Tyr99Cys, Asp100Glu and Asn104Lys lie within EF3 while Ile143AsnThr, Leu151Phe, Glu155Gly and Gly159Val are located in EF4, respectively; in all cases therefore, the number of unaltered Ca2+-binding sites is reduced to two. This is consistent with the findings from in vitro studies that the main functional consequence of these missense mutations is a loss of Ca2+ sensitivity, and thereby reduced GC1 inhibition by mutant GCAP1s at higher intracellular Ca2+ concentrations. In addition, biochemical analysis showed that the Ile143AsnThr mutant protein adopted a conformation that was more susceptible to proteolysis. The Pro50Leu mutation [90] also gives an altered conformation and an increased susceptibility to proteolysis has been suggested as the disease mechanism in this case.
Ca2+ sensitivity of activation of GC1 by wild-type and mutant GCAP1. Activities are presented as percentages of maximum GC1 activation. Shaded boxes indicate Ca2+ concentrations in light and dark. WT diamonds, Glu155Gly triangles, Tyr99Cys squares. Data from [88]
Animal models
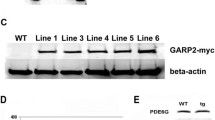
The double knock-out of GCAP1 and GCAP2 in mice has little or no effect on retinal morphology [73]. Extrapolating to humans, this would imply that the loss of functional GCAPs would not cause any overt retinal degeneration and it is perhaps significant that no inherited retinal disorders with null mutations in either GCAP1 or GCAP2 have been reported to date. This contrasts with GC1 where recessive mutations are responsible for LCA. With one exception (Pro50Leu), the dominantly inherited disorders described above reduce the sensitivity of cGMP synthesis to Ca2+ via GCAP-activated GCs. The Tyr99Cys disorder has been modelled in the mouse [86] by the expression of a mutant transgene driven by a promoter active in both rods and cones [91]. The enhanced activity of the cyclase in the dark increased cGMP-gated channel activity and elevated the rod outer segment Ca2+ concentration. In different lines of transgenic mice, the magnitude of this effect rose in parallel with increases in the expression of mutant GCAP1. Surprisingly, there was little change in the rod photoresponse, indicating that dynamic Ca2+-dependent regulation of cGMP synthesis was preserved. However, the photoreceptors in these mice degenerated, and the rate of the cell loss increased with the level of the transgene expression, unlike in transgenic mice that over-expressed normal GCAP1. The direct role of the elevated cGMP and Ca2+ levels arising from the activity of mutant Tyr99Cys and Glu155Gly cyclases in this degeneration is demonstrated, however, by the observation that an increased rate of cGMP removal in the dark achieved via the activation of phosphodiesterase (PDE6) by a constitutively active Gly90Asp rod opsin mutation slows degeneration without affecting the Ca2+-sensitivity of either mutant cyclase [92].
A gene targeting approach introducing a Glu155Gly mutation into the mouse GCAP1 gene has generated a more accurate model of the disease in man [93]. In these mice, a progressive loss of cone-mediated ERG is evident in both mutant heterozygotes and homozygotes with b-wave amplitudes down to 17% of WT in 12-month old mice. Mutant mice also lack a flicker response to 10- and 15-Hz light stimuli. Rod-mediated b-wave amplitudes were reduced in mutant mice, although in 12 month-old homozygous mice, the rod dominated ERG was still 44% of WT suggesting that the mutation primarily affects cone function. Histological analysis showed significant loss of photoreceptor cells at 5 months of age, with up to 47% loss in homozygotes. Overall therefore, the mutant mice have a phenotype that is consistent with a far greater alteration in cone than rod cell function, in keeping with human disease.
Conclusions
-
Both GC1 and GC2 are required for normal phototransduction. Cone photoreceptors die in the GC1 knock-out mouse whereas there is no loss of rods. This suggests a more critical role for GC1 in the protection of cones than rods.
-
No disease-associated mutations have been reported for GC2.
-
Recessive mutations in GC1 are a major cause of LCA in humans. The mechanism of mutant gene action would appear to arise from the loss of functional cyclase.
-
Dominant mutations in GC1 are a major cause of inherited CORD. Mutations are clustered in codon 838 with replacement of Arg with either Cys, Ser or His. The mutant cyclase remains functional but with a reduced sensitivity to Ca2+-dependent inhibition.
-
GCAP1 and GCAP2 are both required for normal phototransduction. The pattern of expression differs, with GCAP1 predominantly present in cones and GCAP2 more concentrated in rods.
-
In mouse models, the double deletion of GCAP1 and GCAP2 does not result in photoreceptor loss. Consistent with this, no recessive disease-associated mutations for either gene have been reported in humans.
-
A single dominant missense mutation in GCAP2 is associated with incomplete penetrance and a spectrum of disease phenotypes that includes RP with and without macular involvement, and macular degeneration.
-
Dominant mutations in GCAP1 result in either cone or CORDs and this may reflect the higher levels of GCAP1 in cones.
-
Mutant GCAP1 proteins are functional but generally have a reduced capacity to bind Ca2+ as a result of substitutions in the EF hands responsible for Ca2+ binding. As a consequence, cyclase activity is less sensitive to inhibition at higher Ca2+ concentrations.
-
A novel knock-in mouse model of a dominant human GCAP1 mutation shows significant cone loss with a more limited effect on rod survival and function.
References
Goraczniak R, Duda T, Sharma RK (1997) Structural and functional characterization of a second subfamily member of the calcium-modulated bovine rod outer segment membrane guanylate cyclase, ROS-GC2. Biochem Biophys Res Commun 234:666–670
Goraczniak RM, Duda T, Sitaramayya A, Sharma RK (1994) Structural and functional characterization of the rod outer segment membrane guanylate cyclase. Biochem J 302:455–461
Yang RB, Foster DC, Garbers DL, Fulle HJ (1995) Two membrane forms of guanylyl cyclase found in the eye. Proc Natl Acad Sci USA 92:602–606
Pugh EN Jr, Duda T, Sitaramayya A, Sharma RK (1997) Photoreceptor guanylate cyclases: a review. Biosci Rep 17:429–473
Dizhoor AM, Hurley JB (1999) Regulation of photoreceptor membrane guanylyl cyclases by guanylyl cyclase activator proteins. Methods 19:521–531
Lange C, Duda T, Beyermann M, Sharma RK, Koch KW (1999) Regions in vertebrate photoreceptor guanylyl cyclase ROS-GC1 involved in Ca(2+)-dependent regulation by guanylyl cyclase-activating protein GCAP-1. FEBS Lett 460:27–31
Krylov DM, Hurley JB (2001) Identification of proximate regions in a complex of retinal guanylyl cyclase 1 and guanylyl cyclase-activating protein-1 by a novel mass spectrometry-based method. J Biol Chem 276:30648–30654
Sokal I, Haeseleer F, Arendt A, Adman ET, Hargrave PA, Palczewski K (1999) Identification of a guanylyl cyclase-activating protein-binding site within the catalytic domain of retinal guanylyl cyclase 1. Biochemistry 38:1387–1393
Duda T, Goraczniak R, Surgucheva I, Rudnicka-Nawrot M, Gorczyca WA, Palczewski K, Sitaramayya A, Baehr W, Sharma RK (1996) Calcium modulation of bovine photoreceptor guanylate cyclase. Biochemistry 35:8478–8482
Laura RP, Hurley JB (1998) The kinase homology domain of retinal guanylyl cyclases 1 and 2 specifies the affinity and cooperativity of interaction with guanylyl cyclase activating protein-2. Biochemistry 37:11264–11271
Tucker CL, Laura RP, Hurley JB (1997) Domain-specific stabilization of photoreceptor membrane guanylyl cyclase by adenine nucleotides and guanylyl cyclase activating proteins (GCAPs). Biochemistry 36:11995–12000
Duda T, Koch KW (2002) Retinal diseases linked with photoreceptor guanylate cyclase. Mol Cell Biochem 230:129–138
Seebacher T, Beitz E, Kumagami H, Wild K, Ruppersberg JP, Schultz JE (1999) Expression of membrane-bound and cytosolic guanylyl cyclases in the rat inner ear. Hear Res 127:95–102
Venkataraman V, Nagele R, Duda T, Sharma RK (2000) Rod outer segment membrane guanylate cyclase type 1-linked stimulatory and inhibitory calcium signaling systems in the pineal gland: biochemical, molecular, and immunohistochemical evidence. Biochemistry 39:6042–6052
Ramamurthy V, Tucker C, Wilkie SE, Daggett V, Hunt DM, Hurley JB (2001) Interactions within the coiled-coil domain of RetGC-1 guanylyl cyclase are optimized for regulation rather than for high affinity. J Biol Chem 276:26218–26229
Yang RB, Garbers DL (1997) Two eye guanylyl cyclases are expressed in the same photoreceptor cells and form homomers in preference to heteromers. J Biol Chem 272:13738–13742
Baehr W, Karan S, Maeda T, Luo DG, Li S, Bronson JD, Watt CB, Yau KW, Frederick JM, Palczewski K (2007) The function of guanylate cyclase 1 and guanylate cyclase 2 in rod and cone photoreceptors. J Biol Chem 282:8837–8847
Yang RB, Robinson SW, Xiong WH, Yau KW, Birch DG, Garbers DL (1999) Disruption of a retinal guanylyl cyclase gene leads to cone-specific dystrophy and paradoxical rod behavior. J Neurosci 19:5889–5897
Leber T (1869) Ueber Retinitis pigmentosa und angeborene Amaurose. Albrecht von Graefes Arch Ophthal 15:1–25
Koenekoop RK (2004) An overview of Leber congenital amaurosis: a model to understand human retinal development. Surv Ophthalmol 49:379–398
Kaplan J (2008) Leber congenital amaurosis: from darkness to spotlight. Ophthalmic Genet 29:92–98
Perrault I, Rozet JM, Calvas P, Gerber S, Camuzat A, Dollfus H, Chatelin S, Souied E, Ghazi I, Leowski C, Bonnemaison M, Le Paslier D, Frezal J, Dufier JL, Pittler S, Munnich A, Kaplan J (1996) Retinal-specific guanylate cyclase gene mutations in Leber’s congenital amaurosis. Nat Genet 14:461–464
Hanein S, Perrault I, Gerber S, Tanguy G, Barbet F, Ducroq D, Calvas P, Dollfus H, Hamel C, Lopponen T, Munier F, Santos L, Shalev S, Zafeiriou D, Dufier JL, Munnich A, Rozet JM, Kaplan J (2004) Leber congenital amaurosis: comprehensive survey of the genetic heterogeneity, refinement of the clinical definition, and genotype-phenotype correlations as a strategy for molecular diagnosis. Hum Mutat 23:306–317
den Hollander AI, Roepman R, Koenekoop RK, Cremers FP (2008) Leber congenital amaurosis: genes, proteins and disease mechanisms. Prog Retin Eye Res 27:391–419
Dharmaraj SR, Silva ER, Pina AL, Li YY, Yang JM, Carter CR, Loyer MK, El-Hilali HK, Traboulsi EK, Sundin OK, Zhu DK, Koenekoop RK, Maumenee IH (2000) Mutational analysis and clinical correlation in Leber congenital amaurosis. Ophthalmic Genet 21:135–150
Lotery AJ, Namperumalsamy P, Jacobson SG, Weleber RG, Fishman GA, Musarella MA, Hoyt CS, Heon E, Levin A, Jan J, Lam B, Carr RE, Franklin A, Radha S, Andorf JL, Sheffield VC, Stone EM (2000) Mutation analysis of 3 genes in patients with Leber congenital amaurosis. Arch Ophthalmol 118:538–543
Booij JC, Florijn RJ, ten Brink JB, Loves W, Meire F, van Schooneveld MJ, de Jong PT, Bergen AA (2005) Identification of mutations in the AIPL1, CRB1, GUCY2D, RPE65, and RPGRIP1 genes in patients with juvenile retinitis pigmentosa. J Med Genet 42:e67
Zernant J, Kulm M, Dharmaraj S, den Hollander AI, Perrault I, Preising MN, Lorenz B, Kaplan J, Cremers FP, Maumenee I, Koenekoop RK, Allikmets R (2005) Genotyping microarray (disease chip) for Leber congenital amaurosis: detection of modifier alleles. Invest Ophthalmol Vis Sci 46:3052–3059
Simonelli F, Ziviello C, Testa F, Rossi S, Fazzi E, Bianchi PE, Fossarello M, Signorini S, Bertone C, Galantuomo S, Brancati F, Valente EM, Ciccodicola A, Rinaldi E, Auricchio A, Banfi S (2007) Clinical and molecular genetics of Leber’s congenital amaurosis: a multicenter study of Italian patients. Invest Ophthalmol Vis Sci 48:4284–4290
Avila-Fernandez A, Vallespin E, Cantalapiedra D, Riveiro-Alvarez R, Gimenez A, Trujillo-Tiebas MJ, Ayuso C (2007) Novel human pathological mutations. Gene symbol: GUCY2D. Disease: early onset retinitis pigmentosa. Hum Genet 121:650–651
Vallespin E, Cantalapiedra D, Riveiro-Alvarez R, Wilke R, Aguirre-Lamban J, Avila-Fernandez A, Lopez-Martinez MA, Gimenez A, Trujillo-Tiebas MJ, Ramos C, Ayuso C (2007) Mutation screening of 299 Spanish families with retinal dystrophies by Leber congenital amaurosis genotyping microarray. Invest Ophthalmol Vis Sci 48:5653–5661
Perrault I, Rozet JM, Gerber S, Ghazi I, Ducroq D, Souied E, Leowski C, Bonnemaison M, Dufier JL, Munnich A, Kaplan J (2000) Spectrum of retGC1 mutations in Leber’s congenital amaurosis. Eur J Hum Genet 8:578–582
Milam AH, Barakat MR, Gupta N, Rose L, Aleman TS, Pianta MJ, Cideciyan AV, Sheffield VC, Stone EM, Jacobson SG (2003) Clinicopathologic effects of mutant GUCY2D in Leber congenital amaurosis. Ophthalmology 110:549–558
Duda T, Krishnan A, Venkataraman V, Lange C, Koch KW, Sharma RK (1999) Mutations in the rod outer segment membrane guanylate cyclase in a cone-rod dystrophy cause defects in calcium signaling. Biochemistry 38:13912–13919
Duda T, Venkataraman V, Goraczniak R, Lange C, Koch KW, Sharma RK (1999) Functional consequences of a rod outer segment membrane guanylate cyclase (ROS-GC1) gene mutation linked with Leber’s congenital amaurosis. Biochemistry 38:509–515
Rozet JM, Perrault I, Gerber S, Hanein S, Barbet F, Ducroq D, Souied E, Munnich A, Kaplan J (2001) Complete abolition of the retinal-specific guanylyl cyclase (retGC-1) catalytic ability consistently leads to Leber congenital amaurosis (LCA). Invest Ophthalmol Vis Sci 42:1190–1192
Tucker CL, Ramamurthy V, Pina AL, Loyer M, Dharmaraj S, Li Y, Maumenee IH, Hurley JB, Koenekoop RK (2004) Functional analyses of mutant recessive GUCY2D alleles identified in Leber congenital amaurosis patients: protein domain comparisons and dominant negative effects. Mol Vis 10:297–303
Perrault I, Hanein S, Gerber S, Lebail B, Vlajnik P, Barbet F, Ducroq D, Dollfus H, Dufier JL, Munnich A, Kaplan J, Rozet JM (2005) A novel mutation in the GUCY2D gene responsible for an early onset severe RP different from the usual GUCY2D-LCA phenotype. Hum Mutat 25:775
Coleman JE, Zhang Y, Brown GA, Semple-Rowland SL (2004) Cone cell survival and downregulation of GCAP1 protein in the retinas of GC1 knockout mice. Invest Ophthalmol Vis Sci 45:3397–3403
Haire SE, Pang J, Boye SL, Sokal I, Craft CM, Palczewski K, Hauswirth WW, Semple-Rowland SL (2006) Light-driven cone arrestin translocation in cones of postnatal guanylate cyclase-1 knockout mouse retina treated with AAV-GC1. Invest Ophthalmol Vis Sci 47:3745–3753
Coleman JE, Semple-Rowland SL (2005) GC1 deletion prevents light-dependent arrestin translocation in mouse cone photoreceptor cells. Invest Ophthalmol Vis Sci 46:12–16
Ulshafer RJ, Allen C, Dawson WW, Wolf ED (1984) Hereditary retinal degeneration in the Rhode Island Red chicken. I. Histology and ERG. Exp Eye Res 39:125–135
Semple-Rowland SL, Lee NR, Van Hooser JP, Palczewski K, Baehr W (1998) A null mutation in the photoreceptor guanylate cyclase gene causes the retinal degeneration chicken phenotype. Proc Natl Acad Sci USA 95:1271–1276
Semple-Rowland SL, Cheng KM (1999) rd and rc Chickens carry the same GC1 null allele (GUCY1*). Exp Eye Res 69:579–581
Williams ML, Coleman JE, Haire SE, Aleman TS, Cideciyan AV, Sokal I, Palczewski K, Jacobson SG, Semple-Rowland SL (2006) Lentiviral expression of retinal guanylate cyclase-1 (RetGC1) restores vision in an avian model of childhood blindness. PLoS Med 3:e201
Michaelides M, Hardcastle AJ, Hunt DM, Moore AT (2006) Progressive cone and cone-rod dystrophies: phenotypes and underlying molecular genetic basis. Surv Ophthalmol 51:232–258
Kelsell RE, Gregory-Evans K, Payne AM, Perrault I, Kaplan J, Yang RB, Garbers DL, Bird AC, Moore AT, Hunt DM (1998) Mutations in the retinal guanylate cyclase (RETGC-1) gene in dominant cone-rod dystrophy. Hum Mol Genet 7:1179–1184
Kelsell RE, Gregory-Evans K, Gregory-Evans CY, Holder GE, Jay MR, Weber BH, Moore AT, Bird AC, Hunt DM (1998) Localization of a gene (CORD7) for a dominant cone-rod dystrophy to chromosome 6q. Am J Hum Genet 63:274–279
Downes SM, Payne AM, Kelsell RE, Fitzke FW, Holder GE, Hunt DM, Moore AT, Bird AC (2001) Autosomal dominant cone-rod dystrophy with mutations in the guanylate cyclase 2D gene encoding retinal guanylate cyclase-1. Arch Ophthalmol 119:1667–1673
Gregory-Evans K, Kelsell RE, Gregory-Evans CY, Downes SM, Fitzke FW, Holder GE, Simunovic M, Mollon JD, Taylor R, Hunt DM, Bird AC, Moore AT (2000) Autosomal dominant cone-rod retinal dystrophy (CORD6) from heterozygous mutation of GUCY2D, which encodes retinal guanylate cyclase. Ophthalmology 107:55–61
Kitiratschky VB, Wilke R, Renner AB, Kellner U, Vadala M, Birch DG, Wissinger B, Zrenner E, Kohl S (2008) Mutation analysis identifies GUCY2D as the major gene responsible for autosomal dominant progressive cone degeneration. Invest Ophthalmol Vis Sci 49:5015–5023
Payne AM, Morris AG, Downes SM, Johnson S, Bird AC, Moore AT, Bhattacharya SS, Hunt DM (2001) Clustering and frequency of mutations in the retinal guanylate cyclase (GUCY2D) gene in patients with dominant cone-rod dystrophies. J Med Genet 38:611–614
Perrault I, Rozet JM, Gerber S, Kelsell RE, Souied E, Cabot A, Hunt DM, Munnich A, Kaplan J (1998) A retGC-1 mutation in autosomal dominant cone-rod dystrophy. Am J Hum Genet 63:651–654
Ito S, Nakamura M, Ohnishi Y, Miyake Y (2004) Autosomal dominant cone-rod dystrophy with R838H and R838C mutations in the GUCY2D gene in Japanese patients. Jpn J Ophthalmol 48:228–235
Small KW, Silva-Garcia R, Udar N, Nguyen EV, Heckenlively JR (2008) New mutation, P575L, in the GUCY2D gene in a family with autosomal dominant progressive cone degeneration. Arch Ophthalmol 126:397–403
Tucker CL, Woodcock SC, Kelsell RE, Ramamurthy V, Hunt DM, Hurley JB (1999) Biochemical analysis of a dimerization domain mutation in RetGC-1 associated with dominant cone-rod dystrophy. Proc Natl Acad Sci USA 96:9039–9044
Wilkie SE, Newbold RJ, Deery E, Walker CE, Stinton I, Ramamurthy V, Hurley JB, Bhattacharya SS, Warren MJ, Hunt DM (2000) Functional characterization of missense mutations at codon 838 in retinal guanylate cyclase correlates with disease severity in patients with autosomal dominant cone-rod dystrophy. Hum Mol Genet 9:3065–3073
Peshenko IV, Moiseyev GP, Olshevskaya EV, Dizhoor AM (2004) Factors that determine Ca2+ sensitivity of photoreceptor guanylyl cyclase. Kinetic analysis of the interaction between the Ca2+-bound and the Ca2+-free guanylyl cyclase activating proteins (GCAPs) and recombinant photoreceptor guanylyl cyclase 1 (RetGC-1). Biochemistry 43:13796–13804
Baehr W, Palczewski K (2007) Guanylate cyclase-activating proteins and retina disease. In: Carafoli E, Brini M (eds) Calcium signalling and disease. Springer, Netherlands, pp 71–91
Imanishi Y, Li N, Sokal I, Sowa ME, Lichtarge O, Wensel TG, Saperstein DA, Baehr W, Palczewski K (2002) Characterization of retinal guanylate cyclase-activating protein 3 (GCAP3) from zebrafish to man. Eur J Neurosci 15:63–78
Cuenca N, Lopez S, Howes K, Kolb H (1998) The localization of guanylyl cyclase-activating proteins in the mammalian retina. Invest Ophthalmol Vis Sci 39:1243–1250
Howes K, Bronson JD, Dang YL, Li N, Zhang K, Ruiz C, Helekar B, Lee M, Subbaraya I, Kolb H, Chen J, Baehr W (1998) Gene array and expression of mouse retina guanylate cyclase activating proteins 1 and 2. Invest Ophthalmol Vis Sci 39:867–875
Otto-Bruc A, Fariss RN, Haeseleer F, Huang J, Buczylko J, Surgucheva I, Baehr W, Milam AH, Palczewski K (1997) Localization of guanylate cyclase-activating protein 2 in mammalian retinas. Proc Natl Acad Sci USA 94:4727–4732
Imanishi Y, Yang L, Sokal I, Filipek S, Palczewski K, Baehr W (2004) Diversity of guanylate cyclase-activating proteins (GCAPs) in teleost fish: characterization of three novel GCAPs (GCAP4, GCAP5, GCAP7) from zebrafish (Danio rerio) and prediction of eight GCAPs (GCAP1–8) in pufferfish (Fugu rubripes). J Mol Evol 59:204–217
Palczewski K, Sokal I, Baehr W (2004) Guanylate cyclase-activating proteins: structure, function, and diversity. Biochem Biophys Res Commun 322:1123–1130
Kachi S, Nishizawa Y, Olshevskaya E, Yamazaki A, Miyake Y, Wakabayashi T, Dizhoor A, Usukura J (1999) Detailed localization of photoreceptor guanylate cyclase activating protein-1 and -2 in mammalian retinas using light and electron microscopy. Exp Eye Res 68:465–473
Surguchov A, Bronson JD, Banerjee P, Knowles JA, Ruiz C, Subbaraya I, Palczewski K, Baehr W (1997) The human GCAP1 and GCAP2 genes are arranged in a tail-to-tail array on the short arm of chromosome 6 (p21.1). Genomics 39:312–322
Ermilov AN, Olshevskaya EV, Dizhoor AM (2001) Instead of binding calcium, one of the EF-hand structures in guanylyl cyclase activating protein-2 is required for targeting photoreceptor guanylyl cyclase. J Biol Chem 276:48143–48148
Stephen R, Palczewski K, Sousa MC (2006) The crystal structure of GCAP3 suggests molecular mechanism of GCAP-linked cone dystrophies. J Mol Biol 359:266–275
Hughes RE, Brzovic PS, Dizhoor AM, Klevit RE, Hurley JB (1998) Ca2+-dependent conformational changes in bovine GCAP-2. Protein Sci 7:2675–2680
Olshevskaya EV, Hughes RE, Hurley JB, Dizhoor AM (1997) Calcium binding, but not a calcium-myristoyl switch, controls the ability of guanylyl cyclase-activating protein GCAP-2 to regulate photoreceptor guanylyl cyclase. J Biol Chem 272:14327–14333
Stephen R, Bereta G, Golczak M, Palczewski K, Sousa MC (2007) Stabilizing function for myristoyl group revealed by the crystal structure of a neuronal calcium sensor, guanylate cyclase-activating protein 1. Structure 15:1392–1402
Mendez A, Burns ME, Sokal I, Dizhoor AM, Baehr W, Palczewski K, Baylor DA, Chen J (2001) Role of guanylate cyclase-activating proteins (GCAPs) in setting the flash sensitivity of rod photoreceptors. Proc Natl Acad Sci USA 98:9948–9953
Howes KA, Pennesi ME, Sokal I, Church-Kopish J, Schmidt B, Margolis D, Frederick JM, Rieke F, Palczewski K, Wu SM, Detwiler PB, Baehr W (2002) GCAP1 rescues rod photoreceptor response in GCAP1/GCAP2 knockout mice. EMBO J 21:1545–1554
Makino CL, Peshenko IV, Wen XH, Olshevskaya EV, Barrett R, Dizhoor AM (2008) A role for GCAP2 in regulating the photoresponse. Guanylyl cyclase activation and rod electrophysiology in GUCA1B knock-out mice. J Biol Chem 283:29135–29143
Pennesi ME, Howes KA, Baehr W, Wu SM (2003) Guanylate cyclase-activating protein (GCAP) 1 rescues cone recovery kinetics in GCAP1/GCAP2 knockout mice. Proc Natl Acad Sci USA 100:6783–6788
Payne AM, Downes SM, Bessant DA, Plant C, Moore T, Bird AC, Bhattacharya SS (1999) Genetic analysis of the guanylate cyclase activator 1B (GUCA1B) gene in patients with autosomal dominant retinal dystrophies. J Med Genet 36:691–693
Sato M, Nakazawa M, Usui T, Tanimoto N, Abe H, Ohguro H (2005) Mutations in the gene coding for guanylate cyclase-activating protein 2 (GUCA1B gene) in patients with autosomal dominant retinal dystrophies. Graefes Arch Clin Exp Ophthalmol 243:235–242
Payne AM, Downes SM, Bessant DA, Taylor R, Holder GE, Warren MJ, Bird AC, Bhattacharya SS (1998) A mutation in guanylate cyclase activator 1A (GUCA1A) in an autosomal dominant cone dystrophy pedigree mapping to a new locus on chromosome 6p21.1. Hum Mol Genet 7:273–277
Michaelides M, Wilkie SE, Jenkins S, Holder GE, Hunt DM, Moore AT, Webster AR (2005) Mutation in the gene GUCA1A, encoding guanylate cyclase-activating protein 1, causes cone, cone-rod, and macular dystrophy. Ophthalmology 112:1442–1447
Jiang L, Wheaton D, Bereta G, Zhang K, Palczewski K, Birch DG, Baehr W (2008) A novel GCAP1(N104 K) mutation in EF-hand 3 (EF3) linked to autosomal dominant cone dystrophy. Vis Res 48:2425–2432
Jiang L, Katz BJ, Yang Z, Zhao Y, Faulkner N, Hu J, Baird J, Baehr W, Creel DJ, Zhang K (2004) Autosomal dominant cone dystrophy caused by a novel mutation in the GCAP1 gene (GUCA1A). Mol Vis 11:143–151
Sokal I, Dupps WJ, Grassi MA, Brown J Jr, Affatigato LM, Roychowdhury N, Yang L, Filipek S, Palczewski K, Stone EM, Baehr W (2005) A novel GCAP1 missense mutation (L151F) in a large family with autosomal dominant cone-rod dystrophy (adCORD). Invest Ophthalmol Vis Sci 46:1124–1132
Nishiguchi KM, Sokal I, Yang L, Roychowdhury N, Palczewski K, Berson EL, Dryja TP, Baehr W (2004) A novel mutation (I143NT) in guanylate cyclase-activating protein 1 (GCAP1) associated with autosomal dominant cone degeneration. Invest Ophthalmol Vis Sci 45:3863–3870
Dizhoor AM, Boikov SG, Olshevskaya EV (1998) Constitutive activation of photoreceptor guanylate cyclase by Y99C mutant of GCAP-1. Possible role in causing human autosomal dominant cone degeneration. J Biol Chem 273:17311–17314
Olshevskaya EV, Calvert PD, Woodruff ML, Peshenko IV, Savchenko AB, Makino CL, Ho YS, Fain GL, Dizhoor AM (2004) The Y99C mutation in guanylyl cyclase-activating protein 1 increases intracellular Ca2+ and causes photoreceptor degeneration in transgenic mice. J Neurosci 24:6078–6085
Sokal I, Li N, Surgucheva I, Warren MJ, Payne AM, Bhattacharya SS, Baehr W, Palczewski K (1998) GCAP1 (Y99C) mutant is constitutively active in autosomal dominant cone dystrophy. Mol Cell 2:129–133
Wilkie SE, Li Y, Deery EC, Newbold RJ, Garibaldi D, Bateman JB, Zhang H, Lin W, Zack DJ, Bhattacharya SS, Warren MJ, Hunt DM, Zhang K (2001) Identification and functional consequences of a new mutation (E155G) in the gene for GCAP1 that causes autosomal dominant cone dystrophy. Am J Hum Genet 69:471–480
Kitiratschky VB, Behnen P, Kellner U, Heckenlively JR, Zrenner E, Jagle H, Kohl S, Wissinger B, Koch KW (2009) Mutations in the GUCA1A gene involved in hereditary cone dystrophies impair calcium-mediated regulation of guanylate cyclase. Hum Mutat 30:E782–E796
Newbold RJ, Deery EC, Walker CE, Wilkie SE, Srinivasan N, Hunt DM, Bhattacharya SS, Warren MJ (2001) The destabilization of human GCAP1 by a proline to leucine mutation might cause cone-rod dystrophy. Hum Mol Genet 10:47–54
Woodford BJ, Chen J, Simon MI (1994) Expression of rhodopsin promoter transgene product in both rods and cones. Exp Eye Res 58:631–635
Woodruff ML, Olshevskaya EV, Savchenko AB, Peshenko IV, Barrett R, Bush RA, Sieving PA, Fain GL, Dizhoor AM (2007) Constitutive excitation by Gly90Asp rhodopsin rescues rods from degeneration caused by elevated production of cGMP in the dark. J Neurosci 27:8805–8815
Buch PK, Cottrill P, Wilkie SE, Pearson RA, Duran Y, West EL, Bhattacharya SS, Dizhoor AM, Ali RR, Hunt DM (2008) A novel ‘knock-in’ mouse model for cone dystrophy: a point mutation in guca1a causes a loss of cone-mediated retinal function and photoreceptor degeneration. ARVO 2008 Presentation no. 4036
Van Ghelue M, Eriksen HL, Ponjavic V, Fagerheim T, Andreasson S, Forsman-Semb K, Sandgren O, Holmgren G, Tranebjaerg L (2000) Autosomal dominant cone-rod dystrophy due to a missense mutation (R838C) in the guanylate cyclase 2D gene (GUCY2D) with preserved rod function in one branch of the family. Ophthalmic Genet 21:197–209
Weigell-Weber M, Fokstuen S, Torok B, Niemeyer G, Schinzel A, Hergersberg M (2000) Codons 837 and 838 in the retinal guanylate cyclase gene on chromosome 17p: hot spots for mutations in autosomal dominant cone-rod dystrophy? Arch Ophthalmol 118:300
Downes SM, Holder GE, Fitzke FW, Payne AM, Warren MJ, Bhattacharya SS, Bird AC (2001) Autosomal dominant cone and cone-rod dystrophy with mutations in the guanylate cyclase activator 1A gene-encoding guanylate cyclase activating protein-1. Arch Ophthalmol 119:96–105
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hunt, D.M., Buch, P. & Michaelides, M. Guanylate cyclases and associated activator proteins in retinal disease. Mol Cell Biochem 334, 157–168 (2010). https://doi.org/10.1007/s11010-009-0331-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-009-0331-y