Abstract
Introduction Numerous studies have shown that the constructs of the Theory of Reasoned Action (TRA), Theory of Planned Behavior (TPB) and Breastfeeding Self-Efficacy (BSE) Framework can effectively identify relationships between maternal psychosocial factors and breastfeeding initiation. However, the ability of these theories to predict breastfeeding duration has not been adequately analyzed. The aim of the review was to examine the utility of the constructs of TRA/TPB and BSE to predict breastfeeding duration. Methods We conducted a literature search using Pubmed (1980-May 2015), Medline (1966-May 2015), CINAHL (1980-May 2015), EMBASE (1980-May 2015) and PsycINFO (1980-May 2015). We selected studies that were observational studies without randomization or blinding, using TRA, TPB or BSE as the framework for analysis. Only studies reporting on breastfeeding duration were included. Results Thirty studies were selected, which include four using TRA, 10 using TPB, 15 using BSE and one using a combination of TPB and BSE. Maternal intention and breastfeeding self-efficacy were found to be important predictors of breastfeeding duration. Inconsistent findings were found in assessing the relationship between maternal attitudes, subjective norms, perceived behavior control and breastfeeding duration. Discussion The inadequacy of these constructs in explaining breastfeeding duration indicates a need to further explore the role of maternal self-determination in breastfeeding behavior.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Significance
There has not been a thorough analysis of the utility of the constructs of TRA/TPB and BSE in predicting breastfeeding duration. Conducting a thorough systematic review allowed us to explore the limitations of these constructs. Further research is necessary to study the relationship between maternal self-determination and breastfeeding duration.
Introduction
Many governmental and non-governmental bodies worldwide have put substantial effort into breastfeeding promotion. The majority of new mothers intend to breastfeed but few exclusively breastfeed for 6 months, the duration recommended by the World Health Organization (World Health Organization 2003). It is widely known that breast milk helps protect against infection and allergies, which commonly occur in infants (American Academy of Pediatrics 2012). However, new mothers may face psychosocial barriers to breastfeeding, such as unfavorable opinions about breastfeeding from significant others, and stigmatization associated with breastfeeding in public venues (Dignam 1995; Kong and Lee 2004; Scott et al. 2003). Breastfeeding researchers have used social psychology theories to explore the relationships between psychosocial determinants and breastfeeding behavior. The theories that have been used most frequently are the Theory of Reasoned Action (TRA)/ Theory of Planned Behavior (TPB) and the Breastfeeding Self-Efficacy (BSE) Framework.
The TRA proposes that intention reflects people’s perceived likelihood of performing a given behavior (Fishbein 1967; Fishbein and Ajzen 1975, 2010). Women who intend to breastfeed exclusively are approximately twice as likely to achieve their own exclusive breastfeeding goals when compared with women who do not intend to exclusively breastfeed (Chezem et al. 2003; Otsuka et al. 2008). Other studies have found that mothers who intend to breastfeed antenatally are more likely to feed their baby breast milk and less likely to give infant formula in the early postpartum period (Lawton et al. 2012; Manstead et al. 1983).
The antecedents of intentions are attitudes and subjective norms toward a behavior (Fishbein 1967; Fishbein and Ajzen 1975, 2010) Attitude is defined as spontaneous and unconscious beliefs about a particular behavior (Fishbein and Ajzen 2010), while subjective norms describe what behaviors people perceive their significant others think they should or should not carry out (Fishbein and Ajzen 2010). In breastfeeding and postpartum women, significant others may include a person’s peers and social network or significant family members such as the partner, parents or parents-in-law, or siblings (Bai et al. 2011, 2016; Campbell et al. 2014; Tarrant et al. 2004; Tsai 2014; Ismail et al. 2013). Manstead et al. (1983) found that mothers who breastfed their infants scored higher in behavioral beliefs and normative beliefs about breastfeeding than mothers who formula fed. In the same study, maternal attitudes and subjective norms toward breastfeeding were found to be associated with intention to breastfeed. In another study, among women who initiated breastfeeding, maternal attitudes and subjective norms toward breastfeeding were associated with intention to continue breastfeeding, and maternal attitudes were the sole factor that predicted their intention to continue breastfeeding (Bai et al. 2010). Moreover, the effect of subjective norms for predicting intention to continue breastfeeding was stronger in married than unmarried women (Bai et al. 2010), which may suggest that for married women breastfeeding support from the baby’s father and other family members was more available than in unmarried mothers.
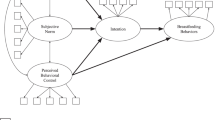
However, the TRA does not account for environmental constraints or personal control factors on pregnant women’s decisions about breastfeeding. This limitation of the TRA was improved by adding a new component, perceived behavioral control (PBC). PBC measures how mothers perceive their own level of control over breastfeeding (Dodgson et al. 2003; Fishbein and Ajzen 2010). The modified TRA is now called the TPB and it is able to predict intention to breastfeed. Swanson and Power (2005) demonstrated that mothers holding favorable attitudes towards formula feeding were less likely to plan to initiate breastfeeding. Duckett et al. (1998) used structural equation modeling to assess the relationship between TPB constructs and breastfeeding intention and found that maternal attitudes, subjective norms and PBC were significant predictors of breastfeeding intentions, even after controlling for maternal education and perceived insufficient milk. These findings were similar to the findings of other researchers who have studied the association between TPB constructs and breastfeeding intentions (Dodgson et al. 2003; McMillan et al. 2009; Wambach 1997).
Self-efficacy refers to one’s perceived ability and confidence to perform an activity (Bandura 1977). BSE theory proposes that past breastfeeding experiences, observational learning from competent role models, verbal appraisals from trusted individuals, and maternal emotional relaxation towards breastfeeding improves maternal confidence and self-efficacy in mothers intending to breastfeed (Dennis 1999). Several studies have found that at 6-week postpartum, mothers with higher baseline breastfeeding self-efficacy scores were more likely to be exclusively breastfeeding (Dennis and Faux 1999; Loke and Chan 2013). Greater breastfeeding self-efficacy is also associated with stronger breastfeeding intentions (Mitra et al. 2004; Otsuka et al. 2008) and intention to exclusively breastfeed in women who had initiated breastfeeding (de Jager et al. 2014). Semenic et al. (2008) found that in a group of Canadian mothers who breastfed exclusively, breastfeeding self-efficacy scores increased significantly from the immediate postpartum period to 4 months postpartum.
Although social and behavioral constructs are correlated with breastfeeding intentions and intentions are associated with breastfeeding duration and exclusivity, it is worthwhile to directly examine whether the TRA/TPB and/or BSE are effective in predicting the actual duration of breastfeeding. As a longer duration of breastfeeding provides greater health benefits to infants and mothers, there is a need to evaluate the association between the constructs of TRA/TPB and BSE and actual breastfeeding duration. Thus, the aim of the review is to examine whether the constructs of TRA/TPB and Self-Efficacy Framework are able to predict breastfeeding duration.
Methods
This systematic review was conducted in accordance with the Preferred Reporting Items for Systematic Reviews and Meta- Analyses (PRISMA) statement (Moher et al. 2009). The focus was on the effects of psychosocial factors on breastfeeding continuation. The models of interest were the TRA, TPB and BSE.
Eligibility Criteria
Studies met the inclusion criteria if they were were observational studies without randomization or blinding.
Studies were excluded if study participants were (1) adolescent mothers; (2) pregnant women with high-risk pregnancies; or (3) mothers of infants born preterm and/or hospitalized. We also excluded (1) studies involving translation or validation of instruments; (2) randomized clinical trials or quasi-experimental studies; (3) educational interventions; (4) qualitative studies; (5) psychometric testing studies and (6) review articles.
Exposure of Interest
Research studies were included if it was explicitly stated that the constructs of the TRA, TBP, BSE, or a combination, were used to assess the effect on breastfeeding duration. Studies were excluded if (1) the aim of the study was to describe knowledge, beliefs, or choice of feeding method or (2) the outcome variables were only intention to breastfeed or breastfeeding initiation.
Outcome of Interest
To be included, at least one of the measured outcomes was the duration of exclusive or any breastfeeding.
Search Strategy
Studies were located through electronic databases including PubMed (1980-May 2015), Medline (1966-May 2015), CINAHL (1980-May 2015), EMBASE (1980-May 2015) and PsycINFO (1980-May 2015). The following keywords were used to search for relevant research papers:
-
#1: breastfeeding OR breast-feed OR breast feed;
-
#2: continuation OR discontinuation OR cessation OR duration OR maintenance;
-
#3: Theory of Reasoned Action OR TRA;
-
#4: Theory of Planned Behavior OR TPB OR Theory of Planned Behaviour;
-
#5: breastfeeding self-efficacy OR BSE;
-
#6: (#1 AND #2 AND #3) OR (#1 AND #2 AND #4) OR (#1 AND #2 AND #5).
Data Extraction and Analysis
Two reviewers (CL and KL) separately extracted the data from the selected papers and evaluated the methodological quality of the reported studies. The following information was extracted: year of publication, study design, participant characteristics, country where the study was conducted, psychosocial theories used, sample size, outcome measures, statistical methods, and study findings. We assessed the reported association between breastfeeding intentions, attitudes, subjective norms, perceived behavioral control and/or breastfeeding self-efficacy and breastfeeding duration.
Quality Appraisal of Observational Studies
We used the Newcastle/Ottawa Quality Assessment Scale (NOS) to evaluate the quality of cohort studies and cross-sectional studies (Institute OHR 2014). Studies were appraised using three broad categories: (1) selection of group/cohort (4 criteria), (2) confounder (1 criterion), and (3) outcome (3 criteria). Each criterion received a maximum score of one point. Cohort studies were evaluated against all 8 criteria while cross-sectional studies were evaluated against 5 criteria. Cohort studies that received total scores of 7–8, 5–6, 4 and 0–3 and cross-sectional studies that received total scores of 5, 4, 3, or 0–2 were rated as very good, good, satisfactory or unsatisfactory, respectively.
Results
Search Results
Initially, 264 items were retrieved from the databases and other sources (Fig. 1). After removing 141 duplicate reports we reviewed 123 items. After screening the titles and abstracts, we excluded 84 items. The full texts of the remaining 39 papers were reviewed and we further excluded 9 reports. A total of 30 studies were included in the final review.
Overview of Included Studies
The characteristics of the included studies are described in Table 1. The earliest study was published in 1983 and the latest in 2015. Ten studies were conducted in the United States (US), six in the United Kingdom (UK), three each in Canada and Hong Kong, and one each in Turkey, Denmark and Japan. One Australian study recruited only rural participants (O’Brien and Fallon 2005) and one study used an online questionnaire to recruit participants from Australia, North American, and Europe (de Jager et al. 2014). One US study recruited participants of African origin (McCarter-Spaulding and Gore 2009) and a Canadian study recruited Aboriginal women (McQueen et al. 2015). Women living in economically deprived regions were recruited in three studies (Glassman et al. 2014; Lawton et al. 2012; McMillan et al. 2009).
The psychosocial models used to predict breastfeeding continuation in the selected studies include the TRA in four studies, the TPB in 10, BSE in 15 and a combination of TPB and BSE in one study (Table 1). The majority of study designs were prospective cohort studies (N = 27) and cross sectional studies (N = 3). The sample sizes ranged from 57 (Bailey et al. 2008) to 602 participants (Avery et al. 1998; Duckett et al. 1998). The mean ages of the study participants ranged from 24 years (McMillan et al. 2009) to 31.5 years (Otsuka et al. 2008).
Summary of Findings
Breastfeeding duration was assessed at various time points across the first year after birth, from the first week up to 1 year. However, the majority of studies (N = 26) reported breastfeeding outcomes within the first 6 months and only four studies followed participants beyond this time period (DiGirolamo et al. 2005; Dodgson et al. 2003; Duckett et al. 1998; Rempel 2004). In a majority of the reviewed studies, the authors examined duration of any breastfeeding (N = 22) with only six studies reporting on exclusive breastfeeding outcomes and two studies reporting on ‘full’ breastfeeding (Goksen 2002; O’Brien et al. 2008).
TRA/TPB and Breastfeeding Duration
Five studies reported an estimation of the association between intention and breastfeeding duration (Avery et al. 1998; Bai et al. 2010; Donnan et al. 2013; Manstead et al. 1983; McMillan et al. 2009). Bai et al. (2010) reported that at 3 months postpartum, participants intending to exclusively breastfeed for 6 months were 65% more likely to be exclusively breastfeeding when compared with participants not having such intentions (OR 1.65, 95% CI 1.08–2.52) (Table 2). Avery et al. (1998) reported that the likelihood of breastfeeding cessation before 4 weeks postpartum was reduced by 4% for every additional week of intended breastfeeding duration (OR 0.96, 95% CI 0.94–0.97). Manstead et al. (1983) found a significantly positive relationship between longer intended breastfeeding duration and continued breastfeeding at 6 weeks postpartum (OR 2.60, p < 0.001). Four studies reported significantly higher rates of continued breastfeeding among mothers who intended to breastfeed when compared with mothers who did not (Dodgson et al. 2003; Duckett et al. 1998; Johns Hopkins University 1988; Wambach 1997). Duckett et al. (1998) found that one additional week of breastfeeding intention was significantly associated with a 0.4 week increment in the duration of breastfeeding (coefficient = 0.43, p < 0.05). Dodgson et al. (2003) found that the magnitude of the association between intention and breastfeeding duration were moderate for a modified TPB model (coefficient = 0.37, p < 0.05), a TPB model looking at working mothers (coefficient = 0.42, p < 0.05), and a TPB model with PBC as a mediator (coefficient = 0.36, p < 0.05). Two studies reported similar positive findings but the point estimates lacked precision as there were wide confidence intervals (CI) or the CIs were not reported (DiGirolamo et al. 2005; Rempel 2004). DiGirolamo et al. (2005) found that mothers who intended to stop breastfeeding at 2 months postpartum had a significantly higher risk of stopping breastfeeding by 9 weeks postpartum when compared with mothers who intended to stop breastfeeding at 12 months postpartum (OR 47.9, 95% CI 15.7–145.6). Two other studies reported a null association between intention and breastfeeding duration (Goksen 2002; Lawton et al. 2012). Lawton et al. (2012) found that mothers who had strong breastfeeding intentions were significantly more likely to initiate breastfeeding but were not more likely to be breastfeeding at 6 months postpartum (OR 1.41, 95% CI 0.58–3.40). Goksen (2002) investigated breastfeeding continuation up to 2 months postpartum and found no effect of breastfeeding intentions and breastfeeding status at either 1 or 2 months postpartum (gamma = 0.24, p < 0.07). Overall, the majority of the reviewed studies supported a positive relationship between maternal breastfeeding intentions and breastfeeding duration.
Study results were inconsistent in determining a relationship between maternal attitudes and breastfeeding duration (Table 2). Avery et al. (1998) reported that maternal attitudes toward breastfeeding were associated with a reduced risk of weaning at 4 weeks postpartum (OR 0.98, 95% CI 0.97–0.99). Manstead et al. (1983) reported that the log odds of breastfeeding from birth to 6 weeks postpartum among mothers with better attitudes towards breastfeeding was 0.02 times that of mothers with less positive attitudes (beta coefficient = 0.0194, p < 0.01). Duckett et al. (1998), who used structural equation modeling, found that positive maternal attitudes of working mothers were significantly associated with longer breastfeeding duration (coefficient = 0.11, p < 0.05). In contrast, three studies demonstrated no positive association between maternal attitudes and breastfeeding duration (DiGirolamo et al. 2005; Johns Hopkins University 1988; Lawton et al. 2012). DiGirolamo et al. (2005), assessed maternal attitudes immediately after childbirth and breastfeeding continuation up to 10 weeks postpartum and found that participants’ breastfeeding status did not differ by attitude score (OR 0.97, 95% CI 0.82–1.16). Other researchers also found no relationship between breastfeeding continuation at 6 months postpartum and maternal breastfeeding attitudes (Johns Hopkins University 1988; Lawton et al. 2012). In Lawton et al. study (2012) they assessed instrumental attitudes and affective attitudes towards breastfeeding, in which the instrumental attitudes measured the tangible rewards of breastfeeding, whereas the affective attitudes measured maternal self-fulfilment in breastfeeding. Lawton et al. (2012) found no relationship between breastfeeding continuation at 6 months postpartum and maternal instrumental attitudes (OR 0.45, 95% CI 0.12–1.69), but they reported a positive relationship between maternal affective attitudes and breastfeeding continuation at 6 months postpartum (OR 4.54, 95% CI 1.70–12.10).
No studies found a positive association between breastfeeding duration and subjective norms (Table 2). In a cohort of underprivileged mothers, Lawton et al. (2012) found that rates of breastfeeding continuation at 6 months postpartum did not differ among mothers with high and low scores on measures of subjective norms in the third trimester of pregnancy (injunctive norms OR 0.92, 95% CI 0.52–1.62; descriptive norms OR 1.10, 95% CI 0.73–1.67). Similarly, two studies, one by Manstead et al. (1983) in a sample of English mothers (logistic regression, beta coefficient = − 0.006, p > 0.05), and one by Swanson and Power (2005) in a sample of Scottish mothers (OR 1.01, 95% CI 0.99–1.03), found no associations between breastfeeding continuation at 6 weeks postpartum and subjective norms measured prenatally (Manstead et al. 1983) or immediately postpartum (Swanson and Power 2005), respectively.
Assessment of the association between PBC and breastfeeding duration produced inconsistent findings. McMillan et al. (2009) found that among mothers with higher PBC scores, the odds of breastfeeding continuation was higher than among mothers with lower PBC scores (OR 1.16, p < 0.001). Dodgson et al. (2003), using structural equation modeling, examined the association between breastfeeding duration and PBC and found that the magnitude of the associations were small for both a modified TPB model (coefficient = 0.18, p < 0.05) and a TPB model with PBC as a mediator (coefficient = 0.17, p < 0.05). In contrast, three studies failed to demonstrate any positive association between these variables (Lawton et al. 2012; Rempel 2004; Swanson and Power 2005). Both Lawton et al. (2012) and Swanson and Power (2005) found that the risks of stopping breastfeeding at 6 months postpartum (OR 1.01, 95% CI 0.77–1.32) or at 6 weeks postpartum (OR 0.72, 95% CI 0.03–17.5), respectively, were similar, regardless of the PBC scores. Rempel (2004) also did not find any association between PBC and breastfeeding duration. In summary, there is limited evidence of an association between PBC and a longer duration of breastfeeding, but the overall magnitude of the effect is small.
The overall performance of TPB models in predicting breastfeeding duration was assessed by examining the percentage of variance that the models explain (Table 2). Wambach’s (1997) simplified TPB model only explained 4% of the variance. Extending the TPB models improved the explanatory power of the models significantly, with explained variance percentages ranging from 21 to 38% (Duckett et al. 1998; Dodgson et al. 2003) using structural equation modeling, and up to 53% using logistic regression (McMillan et al. 2009). Extended TPB models outperformed simple TPB models in prediction of breastfeeding duration because the authors took antecedents of the TPB constructs and other important predictors of breastfeeding duration into consideration when developing their models. For example, Duckett et al. (1998) and Dodgson et al. (2003) formulated separate extended TPB models for mothers with different employment status and/or different working hours.
Breastfeeding Self-Efficacy Scale (BSES) and Breastfeeding Duration
The BSE Framework and the BSES have been used frequently to predict breastfeeding continuation. Baghurst et al. (2007) reported that the odds of weaning at 6 months postpartum was reduced by 3% for every one-unit increase in the BSES score (OR 0.97, 95% CI 0.96–0.98) (Table 2). O’Brien et al. (2008) found similar reductions in breastfeeding cessation at 6 months postpartum (OR 0.95, 95% CI 0.93–0.97), and the discontinuation of exclusive breastfeeding at 6 weeks postpartum (OR 0.94, 95% CI 0.90–0.97). Similarly, other studies revealed that breastfeeding duration was significantly and positively associated with BSES scores (Loke and Chan 2013; Glassman et al. 2014; Ku and Chow 2010; McQueen et al. 2015; Otsuka et al. 2008). Although several studies reported statistically significant positive associations between breastfeeding duration and BSES scores, the authors did not report the confidence intervals (Bailey et al. 2008; Blyth et al. 2002; de Jager et al. 2014; McCarter-Spaulding and Gore 2009; Pollard and Guill 2009). For example, McCarter-Spaulding and Gore (2009) found that the likelihood of weaning at 6 months postpartum decreased by 4% for every one-unit increment in the BSES score (OR 0.96, p < 0.05). Conversely, two groups of researchers were unable to find a significant association between breastfeeding cessation at 6 months postpartum and BSES scores (Aquilina 2011; Semenic et al. 2008). Aquilina (2011) found that breastfeeding duration failed to correlate with the BSES score (Pearson correlation coefficient = 0.21, p > 0.05) and Semenic et al. (2008) found that the risk of weaning was not different in mothers with higher and lower BSES scores (beta coefficient = − 0.01, p = 0.25). To summarize, the majority of reviewed studies supported the association between BSES scores and a longer duration of breastfeeding.
As reflected by the percent of variance explained, regression models that included the BSES while controlling for other confounders, showed satisfactory performance in predicting breastfeeding duration (Table 2). In studies that used linear regression and Cox regression models, the percent of variance explained by the BSES was reported at 23% by O’Brien and Fallon (2005) and 28% by Blyth et al. (2002). Although Bailey et al. (2008) reported that the BSES could explain 64% of the variance, the study had a small sample size.
Kronborg and Vaeth (2004) found that intention (HR 0.40, 95% CI 0.24–0.67) and BSES (HR 1.90, 95% CI 1.33–2.73) were strong predictors for duration, but they did not report the percentage of variance explained by the model.
Quality Appraisal of Observational Studies
According to the NOS criteria, four cohort studies were of good quality, 20 cohort studies were satisfactory, and three cohort and three cross sectional studies had a quality rating of unsatisfactory (Table 3). Among the 27 cohort studies, 21 studies had no description of the characteristics of participants who were lost to follow-up, and thus were deficient on the indicator “Adequacy of follow-up of cohort.” In all of the observational studies, investigators used convenience sampling, potentially introducing selection bias in the recruitment of study participants, and therefore did not meet the criteria “Representativeness of cohort” and “Selection of non-exposed group/cohort”. Investigators of all reviewed studies depended on mothers’ self-reported breastfeeding outcomes that were not objectively measured. As a result, all studies scored 0 in the criterion “Assessment of outcome.”
Discussion
The current review demonstrated that breastfeeding intention and self-efficacy were positively associated with breastfeeding duration. Intention to feed a baby breast milk for a longer duration is more likely to translate into actual action when a mother is committed to breastfeed. Commitment comes from positive breastfeeding experiences and maternal commitment to overcome breastfeeding difficulties or obstacles (Tarrant et al. 2004).
Self-efficacy is linked to confidence, and the latter is boosted when mothers succeed in breastfeeding in the early postnatal period. This success comes from belief in the nutritional value of breast milk and perceived adequate supply of breast milk with frequent feeding, persistence in trying despite pain and other problems, and accommodating breastfeeding to daily routines (Avery et al. 2009; Blyth et al. 2002; Burns et al. 2010; Dykes and Williams 1999; Scott et al. 2006). When mothers feel competent in breastfeeding, they are willing and self-endorsed to continue breastfeeding.
Studies included in the present review were unable to demonstrate a positive relationship between breastfeeding duration and maternal attitudes, subjective norms or PBC. On the other hand, other studies have found that maternal commitment to breastfeeding comes from maternal contentment and perceived breastfeeding competence (Kingston et al. 2007; Tarrant et al. 2004). Mothers who felt competent and satisfied with breastfeeding reported that practical support from significant others, maternal breastfeeding self-efficacy and freedom from emotional distress were important to breastfeeding success (Avery et al. 2009; Dennis 1999; Dignam 1995). The fact that some mothers breastfeed with confidence, competence and enjoyment is likely related to psychological needs for autonomy, competence and relatedness (Ryan 1995). The concept of autonomy posits that free will to choose and a genuine interest in a health behavior are vital for people to commit to and participate in that behavior (Ryan and Deci 2000). Competence indicates that people are confident and competent to meet the challenges they may face when engaging in a certain health behavior (Williams et al. 1998). Relatedness implies that people need rapport and respect from their significant others when they take part in a health behavior (Williams et al. 2006). People are autonomously motivated to continue to engage in a behavior when their psychological needs for autonomy, competence and relatedness are fulfilled. In other words, they are self-determined to participate in an activity and to enjoy and persevere in that activity (Ryan 1995).
We suggest that fulfillment of these needs could be indispensable to the interplay between maternal attitudes, subjective norms and PBC in boosting maternal commitment to breastfeeding continuation. New mothers who do not have prior knowledge of or experience in breastfeeding, may choose to breastfeed because of persuasion by a healthcare professional (Manhire et al. 2007) or to avoid feelings of guilt and/or shame if they choose not to breastfeed (Hauck and Irurita 2003; Hoddinott and Pill 1999; Labbok 2008; McNatt and Freston 1992; Mozingo et al. 2000). As a result, their psychological needs towards breastfeeding are unfulfilled and they are not self-determined (Ryan 1995). Maternal fulfillment of psychological needs can be boosted by internalization (Ryan 1995). Mothers may internalize externally referenced values of breastfeeding (e.g., the doctor said breast milk was good for the baby and so they choose to breastfeed) and assimilate these values into their own self-endorsed values (e.g., they personally believe in the benefits of breastfeeding). When mothers regard breastfeeding as their internal authentic belief, they may formulate a more autonomous and self-determined motivation toward breastfeeding. Promoting autonomous self-determined breastfeeding is better than coercive persuasion because mothers are more likely to enjoy satisfaction and psychological well-being and continue breastfeeding (Bottorff 1990; Dennis 1999; Kong and Lee 2004). Internalization could be facilitated by observational learning of breastfeeding (Dennis 1999), and peer sharing of breastfeeding experiences (Finigan 2003; Hoddinott and Pill 1999; Kong and Lee 2004), but may be diminished by, for instance, the sexualizing of women’s breasts (Ahn et al. 2010; Bridges 2007; Dignam 1995; Kong and Lee 2004). Further studies are warranted to investigate the role played by autonomous motivation on the duration and exclusivity of breastfeeding.
The review has some limitations. The first is that the selected studies were written in English only and therefore generalizability to other populations may be limited. However, although all studies were published in English, six studies focused on non-English speaking population groups; three were conducted with Chinese speaking mothers in Hong Kong (Dodgson et al. 2003; Ku and Chow 2010; Loke and Chan 2013), one in Japan (Otsuka et al. 2008) and one in Denmark (Kronborg and Vaeth 2004). The second limitation was that only observational studies were included and they can only infer association, not causation. The observed relationships could be bidirectional, for example, mothers who intend to breastfeed could prompt their significant others to be more supportive and positive toward breastfeeding. Yet observational studies allow us to observe the effects of psychosocial factors and changes in outcomes in natural occurrence without intentional manipulation by study investigators. Despite observational studies being susceptible to confounding and reverse-causation bias, the majority of studies in this review (26/30) used robust data analysis methods, such as multiple regression and structural equation modeling to control confounders and minimize bias in reporting point estimates of association between the constructs and breastfeeding duration. Finally, we reviewed studies that were conducted from 1983 to 2015. Over this 30-year time period, maternal views on breastfeeding have changed as a result of research findings on the benefits of breastfeeding and health policies that promote breastfeeding in hospitals, workplaces and other public arenas (UNICEF UK Baby Friendly Initiative n.d.). Restrictions on the marketing of breast milk substitutes have also been implemented and strengthened worldwide (World Health Organization 1981). These initiatives have facilitated a more supportive breastfeeding climate, reduced breastfeeding barriers and changed social norms toward breastfeeding. We did not assess whether the effect of constructs such as maternal breastfeeding attitudes, subjective norms or PBC on breastfeeding duration changed over this time period.
Implications
Mothers strive for needs for autonomy, competence and relatedness (Ryan 1995) in making a commitment to continue breastfeeding. Since maternal needs for autonomy, competence and relatedness are modifiable, interventions targeted toward satisfying these needs could be introduced in breastfeeding education and promotion programs. Maternal needs for autonomy and competence towards breastfeeding could be enhanced if health professionals, including nurses, could provide breastfeeding mothers with autonomy support and emotional support (Dignam 1995; McNatt and Freston 1992). Autonomy support means that when helping new mothers, nurses could avoid persuasion and could assist their clients in making choices and reasonable strategies to breastfeed their infants that are compatible with their daily routines (Johnson 2007). Conventional prenatal breastfeeding education organized by healthcare professionals may not be sufficient to facilitate autonomy support to pregnant women. An autonomy supportive climate in prenatal lactation workshops could be facilitated through interactive discussions and feedback (Johnson 2007). Interactive communications between midwives or lactation consultants and pregnant women may focus on realistic and pragmatic planning and management of breastfeeding, in terms of breastfeeding duration, goals, expectations, concerns and lifestyle adaptation. Feedback sessions, which include clients’ own reflections about their breastfeeding management to meet their daily routine, positive feedback given by nurses, and problem-solving skills, could be essential to boost maternal needs for autonomy and competence towards breastfeeding. Similarly, in the postnatal period, it is necessary to support a mother’s needs for autonomy, competence and relatedness. A recent cluster randomized controlled trial demonstrated that individualized postpartum professional telephone support enhanced the duration of exclusive or any breastfeeding (Fu et al. 2014). This observation lends support to the view that by staying connected with healthcare professionals during the postpartum period, fulfillment of maternal needs for autonomy and competence toward breastfeeding could be achieved, thus boosting maternal confidence and self-efficacy. Emotional support to nursing mothers postpartum may play a role in helping mothers to become self-determined and competent in breastfeeding continuation. Nurses could support distressed mothers by showing their empathy that mothering and nurturing duties are not easy, and by praising the new moms for their efforts, as well as acknowledging breastfeeding difficulties and maternal failures or disappointments (Bottorff 1990; Dennis 1999; Kong and Lee 2004). Anxious mothers may therefore preserve their self-esteem and confidence to seek help and actively discuss their problems. Alleviating emotional stress in breastfeeding facilitates the let-down reflex of breastfeeding (Dennis 1999) and mothers may be more relaxed and willing to continue breastfeeding. Further research is needed to investigate whether introducing autonomy supportive components in breastfeeding education and promotion is effective in fulfilling maternal needs for autonomy, competence and relatedness toward breastfeeding, as well as enhancing breastfeeding duration and exclusivity.
Conclusion
TRA/TPB and the BSE are useful in predicting initiation of breastfeeding. However, this does not necessarily equate with good prediction of the duration of breastfeeding. Maternal motivation to continue breastfeeding is affected by the needs for self-determination, relatedness and competence. New studies are necessary to delineate the relationship between autonomous breastfeeding motivation and breastfeeding duration and exclusivity. By targeting these psychological needs, tailor-made breastfeeding support or interventions can be formulated to help women with different backgrounds and character traits, so as to delay early breastfeeding cessation.
References
Ahn, Y., Sohn, M., & Yoo, E. (2010). Breast functions perceived by Korean mothers: infant nutrition and female sexuality. Western Journal of Nursing Research, 32(3), 363–378. https://doi.org/10.1177/0193945909349252.
American Academy of Pediatrics. (2012). Breastfeeding and the use of human milk. Pediatrics.
Aquilina, S. (2011). The relationship between self-efficacy and breastfeeding duration. (Doctoral degree), Carlow University.
Avery, A., Zimmermann, K., Underwood, P. W., & Magnus, J. H. (2009). Confident commitment is a key factor for sustained breastfeeding. Birth: Issues in Perinatal Care, 36(2), 141–148. https://doi.org/10.1111/j.1523-536X.2009.00312.x.
Avery, M., Duckett, L., Dodgson, J., Savik, K., & Henly, S. J. (1998). Factors associated with very early weaning among primiparas intending to breastfeed. Maternal and Child Health Journal, 2(3), 167–179.
Baghurst, P., Pincombe, J., Brian, P., Henderson, A., Reddin, E., & Antoniou, G. (2007). Breast feeding self-efficacy and other determinants of the duration of breast feeding in a cohort of first-time mothers in Adelaide, Australia. Midwifery, 23, 382–391.
Bai, D. L., Fong, D. Y., Lok, K. Y., & Tarrant, M. (2016). Relationship between the Infant feeding preferences of Chinese mothers’ immediate social network and early breastfeeding cessation. Journal of Human Lactation, 32(2), 301–308. https://doi.org/10.1177/0890334416630537.
Bai, Y., Middlestadt, S. E., Peng, C. Y., & Fly, A. D. (2010). Predictors of continuation of exclusive breastfeeding for the first six months of life. Journal of Human Lactation, 26(1), 26–34. https://doi.org/10.1177/0890334409350168.
Bai, Y., Wunderlich, S. M., & Fly, A. D. (2011). Predicting intentions to continue exclusive breastfeeding for 6 months: A comparison among racial/ethnic groups. Maternal and Child Health Journal, 15(8), 1257–1264. https://doi.org/10.1007/s10995-010-0703-7.
Bailey, J., Clark, M., & Shepherd, R. (2008). Duration of breastfeeding in young women: Psychological influences. British Journal of Midwifery, 16(3), 172–178.
Bandura, A. (1977). Self-efficacy: Toward a unifying theory of behavioral change. Psychological Review, 84(2), 191–215.
Blyth, R., Creedy, D. K., Dennis, C. L., Moyle, W., Pratt, J., & De Vries, S. M. (2002). Effect of maternal confidence on breastfeeding duration: An application of breastfeeding self-efficacy theory. Birth, 29(4), 278–284.
Bottorff, J. L. (1990). Persistence in breastfeeding: A phenomenological investigation. Journal of Advanced Nursing, 15(2), 201–209.
Bridges, N. (2007). Ethical responsibilities of the Australian media in the representations of infant feeding. Breastfeeding Review, 15(1), 17–21.
Burns, E., Schmied, V., Sheehan, A., & Fenwick, J. (2010). A meta-ethnographic synthesis of women’s experience of breastfeeding. Maternal and Child Nutrition, 6(3), 201–219. https://doi.org/10.1111/j.1740-8709.2009.00209.x.
Campbell, L. A., Wan, J., Speck, P. M., & Hartig, M. T. (2014). Women, Infant and Children (WIC) peer counselor contact with first time breastfeeding mothers. Public Health Nursing, 31(1), 3–9. https://doi.org/10.1111/phn.12055.
Chezem, J., Friesen, C., & Boettcher, J. (2003). Breastfeeding knowledge, breastfeeding confidence, and infant feeding plans: Effects on actual feeding practices. JOGNN, 32(1), 40–47.
de Jager, E., Broadbent, J., Fuller-Tyszkiewicz, M., & Skouteris, H. (2014). The role of psychosocial factors in exclusive breastfeeding to six months postpartum. Midwifery, 30(6), 657–666. https://doi.org/10.1016/j.midw.2013.07.008.
Dennis, C. L. (1999). Theoretical underpinnings of breastfeeding confidence: A self-efficacy framework. Journal of Human Lactation, 15(3), 195–201.
Dennis, C. L., & Faux, S. (1999). Development and psychometric testing of the Breastfeeding Self-Efficacy Scale. Research in Nursing and Health, 22(5), 399–409.
DiGirolamo, A., Thompson, N., Martorell, R., Fein, S., & Grummer-Strawn, L. (2005). Intention or experience? Predictors of continued breastfeeding. Health Education and Behavior, 32(2), 208–226. https://doi.org/10.1177/1090198104271971.
Dignam, D. M. (1995). Understanding intimacy as experienced by breastfeeding women. Health Care for Women International, 16(5), 477–485. https://doi.org/10.1080/07399339509516200.
Dodgson, J. E., Henly, S. J., Duckett, L., & Tarrant, M. (2003). Theory of planned behavior-based models for breastfeeding duration among Hong Kong mothers. Nursing Research, 52(3), 148–158.
Donnan, P. T., Dalzell, J., Symon, A., Rauchhaus, P., Monteith-Hodge, E., Kellett, G., … Whitford, H. M. (2013). Prediction of initiation and cessation of breastfeeding from late pregnancy to 16 weeks: The feeding your baby (FYB) cohort study. British Medical Journal Open. https://doi.org/10.1136/bmjopen-2013-003274.
Duckett, L., Henly, S., Avery, M., Potter, S., Hills-Bonczyk, S., Hulden, R., & Savik, K. (1998). A theory of planned behavior-based structural model for breast-feeding. Nursing Research, 47(6), 325–336.
Dykes, F., & Williams, C. (1999). Falling by the wayside: A phenomenological exploration of perceived breast-milk inadequacy in lactating women. Midwifery, 15(4), 232–246. https://doi.org/10.1054/midw.1999.0185.
Finigan, V. (2003). Providing breastfeeding support to ethnically diverse groups of mothers. Professional nurse, 18(9), 524–528.
Fishbein, M. & Ajzen, I. (1975). Belief, attitude, intention, and behavior: an introduction to theory and research. Boston: Addison-Wesley Pub. Co.
Fishbein, M. (1967). Readings in attitude theory and measurement. New York: Wiley.
Fishbein, M., & Ajzen, I. (2010). Predicting and changing behavior: The reasoned action approach. New York: Psychology Press.
Fu, I., Fong, D., Heys, M., Lee, I., Sham, A., & Tarrant, M. (2014). Professional breastfeeding support for first-time mothers: A multicentre cluster randomised controlled trial. BJOG, 121(13), 1673–1683.
Glassman, M. E., McKearney, K., Saslaw, M., & Sirota, D. R. (2014). Impact of breastfeeding self-efficacy and sociocultural factors on early breastfeeding in an urban, predominantly Dominican community. Breastfeeding Medicine, 9(6), 301–307. https://doi.org/10.1089/bfm.2014.0015.
Goksen, F. (2002). Normative vs. attitudinal considerations in breastfeeding behavior: Multifaceted social influences in a developing country context. Social Science and Medicine, 54(12), 1743–1753.
Hauck, Y. L., & Irurita, V. F. (2003). Incompatible expectations: The dilemma of breastfeeding mothers. Health Care for Women International, 24(1), 62–78. https://doi.org/10.1080/07399330390170024.
Hoddinott, P., & Pill, R. (1999). Nobody actually tells you: A study of infant feeding. British Journal of Midwifery, 7(9), 558–565. https://doi.org/10.12968/bjom.1999.7.9.8264.
Institute OHR (2014). The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses http://www.ohri.ca/programs/clincal_epidemiology/oxford.asp. Accessed date 20 Jul 2015.
Ismail, T. A., Muda, W. M., & Bakar, M. I. (2013). Intention of pregnant women to exclusively breastfeed their infants: The role of beliefs in the theory of planned behaviour. Journal of Child Health Care. https://doi.org/10.1177/1367493512473857.
Johns Hopkins University. School of Hygiene Public Health, & Faden, R. R. (1988). Determinants of Infant Feeding: Breast VS Bottle.
Johnson, V. D. (2007). Promoting behavior change: making healthy choices in wellness and healing choices in illness—use of self-determination theory in nursing practice. The Nursing Clinics in North America, 42(2), 229–241. https://doi.org/10.1016/j.cnur.2007.02.003. vi.
Kingston, D., Dennis, C. L., & Sword, W. (2007). Exploring breast-feeding self-efficacy. Journal of Perinatal and Neonatal Nursing, 21(3), 207–215. https://doi.org/10.1097/01.JPN.0000285810.13527.a7.
Kong, S. K., & Lee, D. T. (2004). Factors influencing decision to breastfeed. Journal of Advanced Nursing, 46(4), 369–379. https://doi.org/10.1111/j.1365-2648.2004.03003.x.
Kronborg, H., & Vaeth, M. (2004). The influence of psychosocial factors on the duration of breastfeeding. Scandinavian Journal of Public Health, 32(3), 210–216. https://doi.org/10.1080/14034940310019218.
Ku, C.-M., & Chow, S. K. Y. (2010). Factors influencing the practice of exclusive breastfeeding among Hong Kong Chinese women: A questionnaire survey. Journal Of Clinical Nursing, 19(17–18), 2434–2445. https://doi.org/10.1111/j.1365-2702.2010.03302.x.
Labbok, M. (2008). Exploration of guilt among mothers who do not breastfeed: The physician’s role. Journal of Human Lactation, 24(1), 80–84. https://doi.org/10.1177/0890334407312002.
Lawton, R., Ashley, L., Dawson, S., Waiblinger, D., & Conner, M. (2012). Employing an extended Theory of Planned Behaviour to predict breastfeeding intention, initiation, and maintenance in White British and South-Asian mothers living in Bradford. British Journal of Health Psychology, 17(4), 854–871. https://doi.org/10.1111/j.2044-8287.2012.02083.x.
Loke, A. Y., & Chan, L. S. (2013). Maternal breastfeeding self-efficacy and the breastfeeding behaviors of newborns in the practice of exclusive breastfeeding. JOGNN, 42(6), 672–684.
Manhire, K. M., Hagan, A. E., & Floyd, S. A. (2007). A descriptive account of New Zealand mothers’ responses to open-ended questions on their breast feeding experiences. Midwifery, 23(4), 372–381. https://doi.org/10.1016/j.midw.2006.01.002.
Manstead, A. S., Proffitt, C., & Smart, J. L. (1983). Predicting and understanding mothers’ infant-feeding intentions and behavior: Testing the theory of reasoned action. Journal of Personality and Social Psychology, 44(4), 657–671.
McCarter-Spaulding, D., & Gore, R. (2009). Breastfeeding self-efficacy in women of African descent. JOGNN, 38(2), 230–243. https://doi.org/10.1111/j.1552-6909.2009.01011.x.
McMillan, B., Conner, M., Green, J., Dyson, L., Renfrew, M., & Woolridge, M. (2009). Using an extended theory of planned behaviour to inform interventions aimed at increasing breastfeeding uptake in primiparas experiencing material deprivation. British Journal of Health Psychology, 14(Pt 2), 379–403. https://doi.org/10.1348/135910708x336112.
McNatt, M. H., & Freston, M. S. (1992). Social support and lactation outcomes in postpartum women. Journal of Human Lactation, 8(2), 73–77.
McQueen, K., Sieswerda, L. E., Montelpare, W., & Dennis, C. L. (2015). Prevalence and factors affecting breastfeeding among Aboriginal women in Northwestern Ontario. JOGNN, 44(1), 51–68. https://doi.org/10.1111/1552-6909.12526.
Mitra, A. K., Khoury, A. J., Hinton, A. W., & Carothers, C. (2004). Predictors of breastfeeding intention among low-income women. Maternal and Child Health Journal, 8(2), 65–70.
Moher, D., Liberati, A., Tetzlaff, J., Altman, D. G., & Group, P. (2009). Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Annals of Internal Medicine, 151(4), 264–269, W264.
Mozingo, J. N., Davis, M. W., Droppleman, P. G., & Merideth, A. (2000). “It wasn’t working. " Women’s experiences with short-term breastfeeding. American Journal of Maternal Child Nursing, 25(3), 120–126.
O’Brien, M., Buikstra, E., & Hegney, D. (2008). The influence of psychological factors on breastfeeding duration. Journal of Advanced Nursing, 63(4), 397–408. https://doi.org/10.1111/j.1365-2648.2008.04722.x.
O’Brien, M., & Fallon, A. (2005). The effect of breastfeeding self-efficacy on breastfeeding duration. Birth Issues, 14(4), 135–142.
Otsuka, K., Dennis, C. L., Tatsuoka, H., & Jimba, M. (2008). The relationship between breastfeeding self-efficacy and perceived insufficient milk among Japanese mothers. JOGNN, 37(5), 546–555. https://doi.org/10.1111/j.1552-6909.2008.00277.x.
Pollard, D. L., & Guill, M. (2009). The relationship between baseline self-efficacy and breastfeeding duration. Southern Online Journal of Nursing Research, 9(4), 1–6.
Rempel, L. A. (2004). Factors influencing the breastfeeding decisions of long-term breastfeeders. Journal of Human Lactation, 20(3), 306–318. https://doi.org/10.1177/0890334404266969.
Ryan, R. (1995). Psychological needs and the facilitation of integrative processes. Journal of Personality, 63(3), 397–427. https://doi.org/10.1111/1467-6494.ep9510042298.
Ryan, R., & Deci, E. L. (2000). Self-determination theory and the facilitation of intrinsic motivation, social development, and well-being. American Psychologist, 55(1), 68–78. https://doi.org/10.1037//0003-066x.55.1.68. doi.
Scott, J. A., Binns, C. W., Oddy, W. H., & Graham, K. I. (2006). Predictors of breastfeeding duration: Evidence from a cohort study. Pediatrics, 117(4), e646-655. https://doi.org/10.1542/peds.2005-1991.
Scott, J. A., & Mostyn, T. & Greater Glasgow Breastfeeding Initiative Management Team. (2003). Women’s experiences of breastfeeding in a bottle-feeding culture. Journal of Human Lactation, 19(3), 270–277.
Semenic, S., Loiselle, C., & Gottlieb, L. (2008). Predictors of the duration of exclusive breastfeeding among first-time mothers. Research in Nursing and Health, 31(5), 428–441. https://doi.org/10.1002/nur.20275.
Swanson, V., & Power, K. G. (2005). Initiation and continuation of breastfeeding: Theory of planned behaviour. Journal of Advanced Nursing, 50(3), 272–282. https://doi.org/10.1111/j.1365-2648.2005.03390.x.
Tarrant, M., Dodgson, J. E., & Choi, V. W. (2004). Becoming a role model: The breastfeeding trajectory of Hong Kong women breastfeeding longer than 6 months. International Journal of Nursing Studies, 41(5), 535–546. https://doi.org/10.1016/j.ijnurstu.2003.12.007.
Tsai, S. Y. (2014). Influence of partner support on an employed mother’s intention to breastfeed after returning to work. Breastfeeding Medicine, 9(4), 222–230. https://doi.org/10.1089/bfm.2013.0127.
UNICEF UK Baby Friendly Initiative. (n.d.) The Baby Friendly Initiative. Accessed 21 Jan 2015. Available at http://www.babyfriendly.org.uk.
Wambach, K. A. (1997). Breastfeeding intention and outcome: A test of the theory of planned behavior. Research in Nursing and Health, 20(1), 51–59.
Williams, G. C., Freedman, Z. R., & Deci, E. L. (1998). Supporting autonomy to motivate patients with diabetes for glucose control. Diabetes Care, 21(10), 1644–1651.
Williams, G. C., Lynch, M. F., McGregor, H. A., Ryan, R. M., Sharp, D., & Deci, E. L. (2006). Validation of the “important other” climate questionnaire: Assessing autonomy support for health-related change. Families, Systems, and Health, 24(2), 179–194. https://doi.org/10.1037/1091-7527.24.2.179.
World Health Organization. (1981). International Code of Marketing of Breast-Milk Substitutes.
World Health Organization. (2003). Global Strategy for Infant and Young Children Feeding.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lau, C.Y.K., Lok, K.Y.W. & Tarrant, M. Breastfeeding Duration and the Theory of Planned Behavior and Breastfeeding Self-Efficacy Framework: A Systematic Review of Observational Studies. Matern Child Health J 22, 327–342 (2018). https://doi.org/10.1007/s10995-018-2453-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-018-2453-x