Abstract
Conceptual frameworks bring together existing theories and models in order to identify, consolidate, and fill in gaps between theory, practice, and evidence. Given the vast number of possible outcomes that could be studied in genetic counseling, a framework for organizing outcomes and postulating relationships between communication services and genetic counseling outcomes was sought. Through an iterative approach involving literature review, thematic analysis, and consolidation, outcomes and processes were categorized to create and define components of a conceptual framework. The final product, “Framework for Outcomes of Clinical commUnication Services” (FOCUS) contains the following domains: communication strategy; communication process measures; patient care experience, patient changes, patient health; and family changes. A website was created to allow easier access and ongoing modifications to the framework. In addition, a step-by-step guide and two examples were created to show flexibility in how the framework can be used. FOCUS may help in conceptualizing, organizing and summarizing outcomes research related to risk communication and counseling in genetic service delivery as well as other healthcare settings.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Measuring the impact of genetic counseling (GC) on patient outcomes is critical for improving patient care and establishing the added value and quality of care provided by genetic counselors. Clinical communication encompasses many of the education, counseling, and care coordination processes that genetic counselors perform. Clinical communication is a critical component of patient-centered care and may influence patient health outcomes indirectly through cognitive, emotional, or behavioral patient changes that occur as a result of clinical services (Epstein and Street 2007; Street 2013; Street et al. 2009).
We and other researchers have recognized that a comprehensive conceptual framework would be helpful in promoting the use of theory in practice and research related to clinical communication processes and outcomes (McAllister et al. 2016). A framework can be defined as “a structure, overview, outline, system or plan consisting of various descriptive categories, e.g. concepts, constructs or variables…that are presumed to account for a phenomenon” (Nilsen et al. 2015). A framework could help guide hypothesis driven research, selection of outcome measures, and the development of a systematic approach to evaluate the impact of a communication strategy on patient outcomes. Furthermore, use of a conceptual framework helps ensure that potentially important factors have been considered as part of an outcomes assessment (Glanz and Bishop 2010). Finally, a framework can help in hypothesizing and testing proposed relationships between GC communication processes and outcomes (Glanz and Bishop 2010).
Prior efforts to develop a conceptual framework for evaluating genetic service delivery have been made using different approaches. Wang et al. reviewed the scientific literature and developed a basic framework by outlining goals of genetic counseling as well as some examples of process variables and outcome variables (Wang et al. 2004). In a separate effort, Veach et al. used information elicited from GC experts to develop the Reciprocal Engagement Model (REM) of genetic counseling practice which outlines tenets, goals, strategies, and behaviors relevant to the GC profession along with a few outcomes (Veach et al. 2007). Efforts to systematically or comprehensively identify important genetic services outcomes have been conducted by several groups. Two groups in the United Kingdom analyzed qualitative patient data and independently defined similar sets of outcomes that are important to patients (Marion McAllister et al. 2007, 2008; Pithara 2014). One of these groups subsequently developed and validated the Genetic Counseling Outcomes Scale to assess the overarching construct of patient empowerment, defined as “a set of beliefs that enables a person from a family affected by a genetic condition to feel they have some control over and hope for the future” (Mcallister et al. 2011). In the United States (U.S.), the Western States Regional Genetics Collaborative developed a menu of outcomes related to genetic service delivery in clinical and public health settings (Silvey et al. 2009). In another effort, a multidisciplinary group of health care professionals from the U.S. and United Kingdom identified and prioritized a set of “quality indicators” for clinical genetics (Zellerino et al. 2009). Based on a literature review of outcome measures, a group in the United Kingdom identified 19 key domains captured by genetic service outcomes measures and asked patients and providers to determine which are most appropriate to measure (Payne et al. 2007a; Payne et al. 2007b). Most recently, work by U.S. researchers in collaboration with a National Society of Genetic Counselors (NSGC) sub-committee has generated outcomes specific to genetic counseling sessions (Redlinger-Grosse et al. 2015; Zierhut et al. 2016).
Recognizing the need to cohesively synthesize prior efforts, our initial aim was to develop a framework that: 1) organizes, consolidates, and conceptualizes clinical outcomes; 2) postulates how these outcomes connect to GC skills and processes that can be combined to form an overall communication strategy; and 3) aligns framework components with possible measures that have previously or could be used in conducting genetic counseling outcomes research. The framework intentionally concentrates on clinical communication services in GC and does not encompass other medical aspects of genetic service delivery which were outside the scope of this project. In this paper we describe framework development and the creation of a website prototype to house information about the framework. We also illustrate how to tailor the framework for practical use in considering genetic counseling-specific outcomes using a step-by-step guide. Finally, we discuss future directions for using and refining the framework and how it may help in gathering an evidence base for defining quality in genetic counseling.
Methods
Overview of Framework Development and “Outcomes” Categorization
Models, theories and frameworks are all tools for conceptualizing, evaluating, and understanding phenomena; and distinctions between these three terms are not critical for our purposes. Terminology for the components of a framework can vary, but we use the terms constructs (abstract ideas or concepts) and domains (groupings of similar or related constructs).
In developing the framework we drew upon our collective training and experience related to: 1) clinical genetic counseling practice and research; 2) existing behavioral or communication models and published literature from several targeted reviews; and 3) a list of nearly 200 outcomes generated as part of prior and ongoing efforts to elicit GC outcomes (Redlinger-Grosse et al. 2015). We began by grouping the list of “outcomes” into broad domains using a modified logic model approach beginning with the most distal patient outcomes and working backwards toward “outcomes” that would be more directly influenced by GC (Kenyon et al. 2015). An initial attempt to further categorize and consolidate these was taken by the first author and then audited by the other author. Discrepancies in categorization and in domain and construct labels were discussed until a consensus was reached between authors. Framework development was iterative and involved weekly discussions between the authors over a period of approximately 2 years, with additional revisions over the course of several months.
Early in our process we defined several framework domains. The first, which we ultimately called “patient health”, reflects changes in patients’ mental, physical, or social health that are hypothesized to be indirectly influenced by genetic counseling. We then worked backwards to propose how genetic counseling might mediate (i.e., influence or lead to) patient health. Using the “Direct and Indirect Pathways from Communication to Health Outcomes” model (Street 2013; Street and Epstein 2007; Street et al. 2009), Wang’s framework for evaluating genetic services (Wang et al. 2004), Donabedian’s Model of Quality Care (Donabedian 1988), and the National Quality Measures Clearninghouse (“National Quality Measures Clearninghouse 2017) to guide our efforts, we defined three additional domains, which we ultimately called:“process measures”; “patient care experience”; and “patient changes”. We also added a “family changes” domain to reflect findings that genetic services can impact outcomes for other family members (Marion McAllister et al. 2007; Payne et al. 2007a, 2007b). During this process we further categorized and re-categorized “outcomes” using thematic analysis and then defined constructs using emergent themes and prior work by other researchers (Mcallister et al. 2011; Epstein and Street 2007; Payne et al. 2007a, 2007b; Pithara 2014; Silvey et al. 2009; Street 2013; Wang et al. 2004). We also added constructs from several widely used theories or frameworks such as the Health Belief Model, Theory of Planned Behavior, Self-determination Theory, and Extended Parallel Process Model, (DiClemente et al. 2009; Glanz and Bishop 2010; Witte 1992). To preserve parsimony in an already complex framework, we combined constructs we deemed to have substantial overlap and selected or created labels we agreed were most descriptive of blended or newly created constructs.
Linking “Outcomes” to Communication Skills and Processes
When considering how genetic counseling might influence various outcomes, we extracted several lists of behaviors, techniques, processes, and communication functions from the REM (Veach et al. 2007), GC competencies (Accreditation Counsel for Genetic Counseling 2015), framework for evaluating genetic services (Wang et al. 2004), Direct and Indirect Pathways to Patient Outcomes model (Epstein and Street 2007; Street 2013; Street et al. 2009), Social Support Theory (House 1981), Motivational Interviewing (Lundahl et al. 2013; Miller and Rollnick 2013), Self-determination Theory (SDT) (DiClemente et al. 2009), the Ottowa Decision Making Framework (Légaré et al. 2006), GC research (Hallowell et al. 2005; Lerner et al. 2015; Meiser et al. 2008; Roter et al. 2006), and widely used GC texts (Hartmann et al. 2015; Uhlmann et al. 2009; Veach et al. 2010; Veach et al. 2003). Using a similar iterative approach used to organize outcomes, we categorized items on these lists using thematic analysis and then consolidated them into communication skills categories that are each comprised of several communication processes.
Our approach to link outcomes with communication skills and processes was largely influenced by the REM (Veach et al. 2007) and Direct and Indirect Pathways to Patient Outcomes model (Hoerger et al. 2013; Epstein and Street 2007; Street 2013; Street et al. 2009). Through co-opting, blending, and modifying visual representations of patient-centered communication illustrated by (Hoerger et al. 2013) and (Street 2013; Street et al. 2009), we depicted the following framework components: 1) influence of patient and provider goals; 2) skills and processes that comprise a communication strategy; 3) reciprocal communication that occurs between genetic service providers and patients, which is central to the REM; and 4) possible links by which hypothesized strategies may improve the patient care experience and lead to desired cognitive, emotional, or behavioral changes in patients or their family members.
Considering Context
To complete the framework, we followed Epstein and Street’s recommendation to consider the important influence of individual-, family-, cultural-, institutional-, or policy-level factors that may influence patient outcomes (Epstein and Street 2007). Examples of these include; sociodemographics of both the patient and genetic service provider as well as disease-related factors, patient’s illness representation, health literacy and numeracy, family structure, social distance from family members, health insurance status and type, social support, cultural context, policies, laws, health care system factors, and provider self-awareness. Although contextual factors could mediate or moderate proposed relationships between many of the framework constructs, these are external to the main framework domains.
Creation of a Website, Concrete Examples, and Step-by-Step Guide
Due to the large amount of content in the framework and the foreseeable need to continue making ongoing modifications or updates, an on-line website was created under the domain https://www.focusoutcomes.com/. The website was designed to assist in disseminating the framework and to help people navigate framework content while minimizing the likelihood they will be overwhelmed with too much information at one time. Concrete examples were created to illustrate how components of the framework can be combined in different ways to illustrate different outcomes. Finally, a step-by-step guide was also created to help demonstrate one way in which the framework can be used to develop a plan for evaluating genetic counseling services or conducting a research study.
Results
General Framework
The title we selected, “Framework for outcomes of clinical communication services (FOCUS),” reflects the framework’s general purposes which are to: 1) organize and consolidate outcomes to help researchers and health care providers select and focus on outcome(s) they are interested in evaluating; 2) hypothesize how the outcomes may relate to each other and to various skills and processes that may be employed as part of a communication strategy in clinical settings; and 3) align framework components with possible measures. The general relationships between domains that comprise FOCUS and patient and provider goals are depicted in Fig. 1. FOCUS domains include: 1) communication strategy (i.e., the overall combination of skills and processes employed to achieve the goals); 2) communication process measures; 3) patient care experience; 4) patient changes; 5) patient health; and 6) family changes. The resulting framework provides clinicians and researchers with flexibility to combine communication skills in various ways in order to design a strategy hypothesized to achieve specific outcomes of interest.
Patient and provider goals within the context of genetic counseling have been described or studied previously by other researchers (Bernhardt et al. 2000; Hartmann et al. 2015; Peters and Petrill 2011; Veach et al. 2007; Wang et al. 2004). Our targeted literature review revealed that goals vary from patient to patient in different subspecialty settings (Peters and Petrill 2011) and many patients are unaware of what to expect from genetic counseling and therefore lack well-defined goals (Bernhardt et al. 2000). Genetic counseling goals from the REM fall into four main categories: 1) understanding and appreciation; 2) support and guidance; 3) facilitative decision-making; and 4) patient-centered education (Hartmann et al. 2015). These goals are similar to the three overarching goals of genetic counseling described by Wang et al., which include: 1) educate and inform, 2) provide support and help cope, and 3) facilitate informed decision-making (Wang et al. 2004).
A communication strategy is a plan or method for achieving patient and provider goals and positively influencing patient care experiences, changes, and/or health. A strategy can be created by combining various communication skills and processes that are categorized in Table 1. Communication process measures reflect the clinical communication services that take place. Processes can be measured using checklists, chart reviews, or third-party observation to document use of communication skills, adherence to professional guidelines, patients’ level of involvement, and other components of care. Constructs within the communication process domain and some example measures that may assess these constructs are listed in Table 2.
Patient care experiences consist of different types of feedback from patients and their families or caregivers about the delivery of patient care. Some of the examples listed in Table 3 include: meeting patient needs, perceptions of the patient/provider relationship, perceptions of communication, and perceptions of information received. These reflect the level of patient-centered care and may influence other downstream changes.
Patient changes are cognitive, emotional or behavioral factors that change during or after the visit with the healthcare provider as a direct or indirect result of the care they received. These are listed in Table 4 along with a few examples of possible measures that have or could possibly be used to measure these changes.
Patient health includes both objective and patient reported changes in mental, physical, or social health that result from the clinical care received. In the case of clinical communication services, changes in patient health are more likely to occur indirectly as the result of upstream influences services may have on patient care experiences or patient changes. Patient health outcomes are listed in Table 5 along with some measures to serve as examples.
Family changes consist of factors that change among the patient’s family as an indirect result of health services provided to a patient. These can include: family communication, family functioning, family member access to appropriate care, and caregiver burden detailed in Table 6. Several of these changes may be important contributors to improved health outcomes among family members.
FOCUS-GC Step-by-Step Guide and Examples
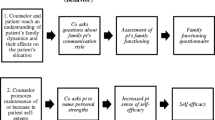
Two concrete examples of how FOCUS can be applied to genetic counseling were created. The first example, entitled “FOCUS on Genetic Counseling to Improve Family Risk Communication and Appropriate Uptake of Health Services”, is illustrated in Fig. 2 and described briefly below. This example could be useful for researching the effectiveness of genetic counseling interventions on conditions, such as hereditary cancer syndromes and familial hypercholesterolemia, where genetic testing/screening can empower family members to access genetic services and take appropriate actions that can ultimately reduce morbidity and mortality (George et al. 2015).
The second example uses the step-by-step guide to illustrate how FOCUS can be applied in designing research studies and is summarized in Fig. 3. To complete the first step, we selected our primary goal and used Tables 4 and 5 to identify indicators or outcomes related to the goal. The primary goal was “to promote quality health decisions”; and the primary indicators/outcomes, selected to reflect the extent to which this goal is achieved, include: 1) patient makes an informed decision; 2) the decision is based upon best available evidence; 3) the decision aligns with the patient’s values and goals; and 4) the decision can be put into action.
In the second step we created a strategy for the intervention by listing communication skills from Table 1 that together would likely help achieve the primary goal (either directly or indirectly). As part of this step we also began developing a rationale for choosing these specific skills based on logic, empirical research findings and other frameworks or theories in order to explain why and how combining these communication skills in a specific way would be expected to improve the select indicators and outcomes. The skills we combined to create our strategy included: 1) establish rapport and a mutual agenda; 2) gather information, educate, and check understanding; 3) respond to emotions and engage patient in decision making; 4) support patient autonomy and mobilize or provide resources; 5) decide and engage in action planning. These skills are each comprised of several processes, including several from the Ottowa Decision-making Framework and those that were identified as critical to shared decision making in a review article (Légaré et al. 2006; Makoul and Clayman 2006). We then mapped out direct and indirect pathways through which our strategy may influence the patient care experience as well as cognitive, emotional or behavioral changes among the patient.
To complete step 3 we identified measures to ensure that the strategy was implemented with fidelity (process measures). Measures were also selected for inclusion on patient surveys in order to evaluate the patient care experience and measure direct patient changes (Fig. 3). Additionally, indirect patient changes and patient health measures were considered for inclusion on a follow-up survey and medical record review 3–6 months later. Finally, to complete step 4 we considered some of the general contextual variables that might modify or confound decision making studies and are therefore important to measure so that they can be used as covariates in the analysis. Although we elected to create a somewhat general decision-making example, literature on a specific type of decision and/or specific setting in which it occurs may identify other important contextual variables.
Discussion
The unique contribution of FOCUS is that it consolidates prior models, published literature, and professional experience into a more comprehensive framework that defines terms and helps postulate general mechanisms by which clinical communication services (including genetic counseling, health coaching and care-coordination) may influence patients and families either directly or indirectly and result in improved care experiences and health outcomes. FOCUS is purposefully agnostic to any specific outcome or context in order to maintain flexibility and applicability to a variety of clinical settings in which GC or other communication intense health services are provided. The examples we created demonstrate how FOCUS can be tailored to examine different outcomes. Ultimately, this type of framework may help in designing studies to demonstrate and establish the gold standard of quality in genetic counseling and other healthcare communication services more generally.
The Institute of Medicine (IOM) has defined quality based on the extent to which health care services are patient-centered, equitable, effective, timely, safe and efficient (Committee on Quality of Health Care in America 2001). Development of quality measures begin with clinical research that links clinical care processes with the IOM quality indicators. The two examples we created using FOCUS can help conceptualize how GC may impact quality. Specifically, with regard to our first example, increasing family members’ uptake of testing may improve timeliness of identifying at-risk family members and contribute to effective care through the prevention or early detection of disease. In addition, efficiency can be improved through ordering single site testing for family members (as opposed to full gene sequencing); and this is only possible if a patient accurately communicates test results to family members. In relation to our second example, using a shared decision-making strategy is considered high quality care because it takes into consideration the patients’ needs, values, and goals and therefore the approach is patient-centered. Furthermore, a quality health decision is hypothesized to indirectly increase the effectiveness of care in some settings or contexts by improving patient adherence to evidence-based health recommendations.
Study Limitations
Despite the potential usefulness of FOCUS, there were limitations with the approach used to construct the framework. First, the process of developing the framework was not entirely systematic. However, it would have been impractical to review all literature within all relevant disciplines and to provide detailed examples or evidence for each of the proposed relationships between framework components. Thus, additional work is needed to comprehensively review research findings and to indicate the strength of evidence supporting or refuting the proposed relationships between constructs. Second, this framework was informed largely by the GC literature. As a result, some components of the framework may be less relevant to health service delivery that occurs outside the context of GC. Further, the process of consolidating and determining labels and definitions for FOCUS domains and constructs was challenging due to notable similarities between several outcomes or communication skills and processes as well as insufficient evidence to suggest that one label or description is superior to another. Subsequently, nuances in constructs and labels may have been lost during the consolidation process. Finally, there are several important limitations related to the sample measures included in the FOCUS tables. Although researchers may find some of these measures useful, we did not use any type of systematic method in their selection and we created several of the measures to serve as examples. Consequently, we are unable to endorse any of the measures because we have not evaluated or generated evidence of their reliability or validity.
Practice Implications
FOCUS could be used to evaluate GC service delivery and help answer relevant clinical questions like: 1) How do genetic counselors contribute to improvements in patient care experiences and outcomes? and 2) What are best practices in genetic counseling? Professional consensus regarding terminology related to GC processes and outcomes together with widespread use of a consolidated framework (such as a modified version of FOCUS) may help move genetic counseling outcomes research ahead more quickly in order to build a strong evidence base for GC practice. Currently evidence supporting linkages between communication strategies and outcomes is somewhat limited in GC (Bettina Meiser et al. 2008; Paul et al. 2015). However, several propositions linking some of the FOCUS constructs do exist and provide rich areas of continued exploration. For example, patient-centered strategies based on Self-determination Theory, Motivational Interviewing techniques, and/or the Extended Parallel Process Model have increased autonomous motivation, improved perceived competence and self-efficacy, and/or changed cognitions, emotions or behaviors (DiClemente et al. 2009; Kinney et al. 2014; Lundahl et al. 2013; Miller and Rollnick 2013; Pengchit et al. 2011; Ruiter et al. 2014). These strategies consist of skills and techniques that are included in FOCUS such as asking the patient what she/he wants to achieve; refraining from judgment; encouraging questions; exploring and resolving ambivalence in decision making; altering risk perceptions; and/or promoting beliefs that certain actions or resources can help the patient effectively mitigate their risks.
Research Recommendations
In order for FOCUS to impact clinical practice, additional efforts are needed that go beyond the scope of the current study. Identifying appropriate outcome measures is still an important research area that will require additional efforts. A few articles have identified and reviewed measures that capture some GC outcomes (M McAllister and Dearing 2015; B Meiser et al. 2001; Payne et al. 2007a, 2007b) and we have included several other potential measures as examples. However, it will be critical to ensure these measures are well validated in a variety of GC contexts. Efforts will also be needed to further hypothesize and test specific direct and indirect relationships between constructs using methods such as structural equation modeling. As empirical evidence is gathered to support or refute hypothesized relationships, additional modifications to FOCUS may be necessary. We also anticipate that constructs will be added to the framework over time and that FOCUS will be used in conjunction with other models and theories.
Conclusion
FOCUS provides a comprehensive way of thinking about clinical communication services and has the potential to help researchers: 1) develop ideas about how to evaluate clinical communication services (including genetic counseling); 2) organize, categorize, and define a broad array of possible outcomes; 3) select outcomes and measures; 4) hypothesize how communication strategies may positively impact health care quality; 5) guide comparative effectiveness research to determine whether and how differences in GC may or may not be associated with differences in patient outcomes. Use and refinement of this type of macro-level framework is expected to improve our ability to conceptualize and summarize genetic counseling outcome studies (both past and future) and help to collate much needed evidence on what communication strategies could be endorsed as best practices in GC. It is our hope that patients, healthcare providers, and researchers in many different areas may benefit from applying this type of framework in research and practice.
References
Accreditation Counsel for Genetic Counseling. (2015). Practice-Based Competencies for Genetic Counselors. Retrieved from http://www.gceducation.org/Documents/ACGC%20Core%20Competencies%20Brochure_15_Web.pdf. Accessed 28 Sept 2017
Agency for Healthcare Research and Quality. National Quality Measures Clearninghouse. (2017). https://www.qualitymeasures.ahrq.gov/. Accessed 6 Feb 2017.
Bernhardt, B. A., Biesecker, B. B., & Mastromarino, C. L. (2000). Goals, benefits, and outcomes of genetic counseling: Client and genetic counselor assessment. American Journal of Medical Genetics, 94(3), 189–197.
Committee on Quality of Health Care in America. (2001). Crossing the quality chasm: A new health system for the 21st century. National Academies Press. http://www.ncbi.nlm.nih.gov/pubmed/25057539.
DiClemente, R. J., Crosby, R. A., & Kegler, M. (2009). In R. J. DiClemente, R. A. Crosby, & M. Kegler (Eds.), Emerging theories in health promotion pracitce and research (2nd ed.). San Francisco: Jossey-Bass.
Donabedian, A. (1988). The quality of care - how can it be assessed? JAMA, 260(12), 1743–1748. https://doi.org/10.1001/jama.1988.03410120089033.
Epstein, R.M., Street, R.L., Jr. (2007) Patient-Centered Communication in Cancer Care: Promoting Healing and Reducing Suffering. National Cancer Institute, NIH Publication No. 07-6225. Bethesda. Retrieved from https://healthcaredelivery.cancer.gov/pcc/pcc_monograph.pdf.
George, R., Kovak, K., & Cox, S. L. (2015). Aligning policy to promote cascade genetic screening for prevention and early diagnosis of heritable diseases. Journal of Genetic Counseling, 24(3), 388–399. doi:https://doi.org/10.1007/s10897-014-9805-5.
Glanz, K., & Bishop, D. B. (2010). The role of behavioral science theory in development and implementation of public health interventions. Annual Review of Public Health, 31, 399–418. https://doi.org/10.1146/annurev.publhealth.012809.103604.
Hallowell, N., Lawton, J., & Gregory, S. (2005). Reflections on research: The Realitities of doing research in the social sciences. New York: Open University Press.
Hartmann, J. E., Veach, P. M., MacFarlane, I. M., & LeRoy, B. S. (2015). Genetic counselor perceptions of genetic counseling session goals: A validation study of the reciprocal-engagement model. Journal of Genetic Counseling, 24(2), 225–237. https://doi.org/10.1007/s10897-013-9647-6.
Hoerger, M., Epstein, R. M., Winters, P. C., Fiscella, K., Duberstein, P. R., Gramling, R., et al. (2013). Values and options in cancer care (VOICE): Study design and rationale for a patient-centered communication and decision-making intervention for physicians, patients with advanced cancer, and their caregivers. BMC Cancer, 13, 188. https://doi.org/10.1186/1471-2407-13-188.
House, J. S. (1981). Work stress and social support. Boston: Addison-Wesley Pub Co..
Kenyon, C. C., Palakshappa, D., & Feudtner, C. (2015). Logic models--tools to bridge the theory-research-practice divide. JAMA Pediatrics, 169(9), 801–802. https://doi.org/10.1001/jamapediatrics.2015.1365.
Kinney, A. Y., Boonyasiriwat, W., Walters, S. T., Pappas, L. M., Stroup, A. M., Schwartz, M. D., et al. (2014). Telehealth personalized cancer risk communication to motivate colonoscopy in relatives of patients with colorectal cancer: The family CARE randomized controlled trial. Journal of Clinical Oncology: Official Journal of the American Society of Clinical Oncology, 32(7), 654–662. https://doi.org/10.1200/JCO.2013.51.6765.
Légaré, F., O’Connor, A. C., Graham, I., Saucier, D., Côté, L., Cauchon, M., & Paré, L. (2006). Supporting patients facing difficult health care decisions: Use of the Ottawa decision support framework. Canadian Family Physician Medecin de Famille Canadien, 52, 476–477 http://www.ncbi.nlm.nih.gov/pubmed/17327891.
Lerner, J. S., Li, Y., Valdesolo, P., & Kassam, K. S. (2015). Emotion and decision making. Annual Review of Psychology, 66(1), 799–823. https://doi.org/10.1146/annurev-psych-010213-115043.
Lundahl, B., Moleni, T., Burke, B. L., Butters, R., Tollefson, D., Butler, C., & Rollnick, S. (2013). Motivational interviewing in medical care settings: A systematic review and meta-analysis of randomized controlled trials. Patient Education and Counseling, 93(2), 157–168. https://doi.org/10.1016/j.pec.2013.07.012.
Makoul, G., & Clayman, M. L. (2006). An integrative model of shared decision making in medical encounters. Patient Education and Counseling, 60(3), 301–312. https://doi.org/10.1016/j.pec.2005.06.010.
McAllister, M., & Dearing, A. (2015). Patient reported outcomes and patient empowerment in clinical genetics services. Clinical Genetics, 88(2), 114–121. https://doi.org/10.1111/cge.12520.
McAllister, M., Payne, K., Nicholls, S., MacLeod, R., Donnai, D., & Davies, L. M. (2007). Improving service evaluation in clinical genetics: Identifying effects of genetic diseases on individuals and families. Journal of Genetic Counseling, 16(1), 71–83. https://doi.org/10.1007/s10897-006-9046-3.
McAllister, M., Payne, K., Macleod, R., Nicholls, S., Donnai, D., & Davies, L. (2008). Patient empowerment in clinical genetics services. Journal of Health Psychology, 13(7), 895–905. https://doi.org/10.1177/1359105308095063.
Mcallister, M., Wood, A., Dunn, G., Shiloh, S., & Todd, C. (2011). The genetic counseling outcome scale: A new patient-reported outcome measure for clinical genetics services. Clinical Genetics, 79, 413–424. https://doi.org/10.1111/j.1399-0004.2011.01636.x.
McAllister, M., Moldovan, R., Paneque, M., & Skirton, H. (2016). The need to develop an evidence base for genetic counselling in Europe. European Journal of Human Genetics: EJHG, 24(4), 504–505. https://doi.org/10.1038/ejhg.2015.134.
Meiser, B., Butow, P. N., Barratt, A. L., Schnieden, V., Gattas, M., Kirk, J., & Psychological Impact Collaborative Group. (2001). Long-term outcomes of genetic counseling in women at increased risk of developing hereditary breast cancer. Patient Education and Counseling, 44(3), 215–225.
Meiser, B., Irle, J., Lobb, E., & Barlow-Stewart, K. (2008). Assessment of the content and process of genetic counseling: A critical review of empirical studies. Journal of Genetic Counseling, 17(5), 434–451. https://doi.org/10.1007/s10897-008-9173-0.
Miller, W. R., & Rollnick, S. (2013). Motivational interviewing: Helping people change (3rd ed.). New York: The Guilford Press.
Nilsen, P., Eccles, M., Grimshaw, J., Walker, A., Johnston, M., Pitts, N., et al. (2015). Making sense of implementation theories, models and frameworks. Implementation Science, 10(1), 53. https://doi.org/10.1186/s13012-015-0242-0.
Paul, J., Metcalfe, S., Stirling, L., Wilson, B., & Hodgson, J. (2015). Analyzing communication in genetic consultations--a systematic review. Patient Education and Counseling, 98(1), 15–33. https://doi.org/10.1016/j.pec.2014.09.017.
Payne, K., Nicholls, S., McAllister, M., Macleod, R., Donnai, D., & Davies, L. M. (2007a). Outcome measurement in clinical genetics services: A systematic review of validated measures. Value in Health : The Journal of the International Society for Pharmacoeconomics and Outcomes Research, 11(3), 497–508. https://doi.org/10.1111/j.1524-4733.2007.00259.x.
Payne, K., Nicholls, S. G., McAllister, M., MacLeod, R., Ellis, I., Donnai, D., & Davies, L. M. (2007b). Outcome measures for clinical genetics services: A comparison of genetics healthcare professionals and patients’ views. Health Policy (Amsterdam, Netherlands), 84(1), 112–122. https://doi.org/10.1016/j.healthpol.2007.03.005.
Pengchit, W., Walters, S. T., Simmons, R. G., Kohlmann, W., Burt, R. W., Schwartz, M. D., & Kinney, A. Y. (2011). Motivation-based intervention to promote colonoscopy screening: An integration of a fear management model and motivational interviewing. Journal of Health Psychology, 16(8), 1187–1197. https://doi.org/10.1177/1359105311402408.
Peters, K. F., & Petrill, S. A. (2011). A comparison of the background, needs, and expectations of patients seeking genetic counseling services. American Journal of Medical Genetics. Part A, 155A(4), 697–705. https://doi.org/10.1002/ajmg.a.33979.
Pithara, C. (2014). Identifying outcomes of clinical genetic services: Qualitative evidence and methodological considerations. Journal of Genetic Counseling, 23(2), 229–238. https://doi.org/10.1007/s10897-013-9654-7.
Redlinger-Grosse, K., Veach, P. M., Cohen, S., LeRoy, B. S., MacFarlane, I. M., & Zierhut, H. (2015). Defining our clinical practice: The identification of genetic counseling outcomes utilizing the reciprocal engagement model. Journal of Genetic Counseling. https://doi.org/10.1007/s10897-015-9864-2.
Roter, D., Ellington, L., Erby, L. H., Larson, S., & Dudley, W. (2006). The genetic counseling video project (GCVP): Models of practice. American Journal of Medical Genetics. Part C, Seminars in Medical Genetics, 142C(4), 209–220. https://doi.org/10.1002/ajmg.c.30094.
Ruiter, R. A. C., Kessels, L. T. E., Peters, G.-J. Y., & Kok, G. (2014). Sixty years of fear appeal research: Current state of the evidence. International Journal of Psychology : Journal International de Psychologie, 49(2), 63–70. https://doi.org/10.1002/ijop.12042.
Silvey, K., Stock, J., Hasegawa, L. E., & Au, S. M. (2009). Outcomes of genetics services: Creating an inclusive definition and outcomes menu for public health and clinical genetics services. American Journal of Medical Genetics. Part C, Seminars in Medical Genetics, 151C(3), 207–213. https://doi.org/10.1002/ajmg.c.30218.
Street, R. L. (2013). How clinician-patient communication contributes to health improvement: Modeling pathways from talk to outcome. Patient Education and Counseling, 92(3), 286–291. https://doi.org/10.1016/j.pec.2013.05.004.
Street, R. L., & Epstein, R. M. (2007). Patient-Centered Communication in Cancer Care: Promoting Healing & Reducing Suffering. Bethesda: NIH publication.
Street, R. L., Makoul, G., Arora, N. K., & Epstein, R. M. (2009). How does communication heal? Pathways linking clinician-patient communication to health outcomes. Patient Education and Counseling, 74(3), 295–301. https://doi.org/10.1016/j.pec.2008.11.015.
Uhlmann, W. R., Schuette, J. L., & Yashar, B. M. (2009). In W. R. Uhlmann, J. L. Schuette, & B. M. Yashar (Eds.), A guide to genetic counseling (2nd ed.). Hoboken: Wiley-Blackwell.
Veach, P. M., LeRoy, B. S., & Bartels, D. M. (2003). Facilitating the genetic counseling process: A practice manual. New York: Springer-Verlag.
Veach, P. M., Bartels, D. M., & LeRoy, B. S. (2007). Coming full circle: A reciprocal-engagement model of genetic counseling practice. Journal of Genetic Counseling, 16, 713–728. https://doi.org/10.1007/s10897-007-9113-4.
Veach, P. M., LeRoy, B., & Bartels, D. M. (2010). Genetic counseling practice : Advanced concepts and skills. Hoboken: Wiley-Blackwell.
Wang, C., Gonzalez, R., & Merajver, S. D. S. D. (2004). Assessment of genetic testing and related counseling services: Current research and future directions. Social Science & Medicine, 58, 1427–1442. https://doi.org/10.1016/S0277-9536(03)00337-X.
Witte, K. (1992). Putting the fear back into fear appeals: The extended parallel process model. Communication Monographs, 59(4), 329–349. https://doi.org/10.1080/03637759209376276.
Zellerino, B. C., Milligan, S. A., Gray, J. R., Williams, M. S., & Brooks, R. (2009). Identification and prioritization of quality indicators in clinical genetics: An international survey. American Journal of Medical Genetics. Part C, Seminars in Medical Genetics, 151C(3), 179–190. https://doi.org/10.1002/ajmg.c.30220.
Zierhut, H. A., Shannon, K. M., Cragun, D. L., & Cohen, S. A. (2016). Elucidating genetic counseling outcomes from the perspective of genetic counselors. Journal of Genetic Counseling, 25(5), 993–1001. https://doi.org/10.1007/s10897-015-9930-9.
Acknowledgements
Partial support for Deborah Cragun’s time was provided during her postdoctoral training fellowship funded by a NCI R25 training grant awarded to Moffitt Cancer Center (5R25CA147832-05). However, this work reflects the authors’ opinions and has neither been reviewed nor endorsed by the NCI or entities acknowledged below. The authors would like to acknowledge the National Society of Genetic Counselors outcomes work group because serving on this group revealed the need for and helped in conceptualizing this framework. Deborah Cragun would also like to acknowledge that framework development was inspired and/or influenced by: 1) training she received from her mentors (Dr. Rita DeBate and Dr. Tuya Pal); 2) discussions with Dr. Courtney Scherr and Dr. Anita Kinney; and 3) participation in the Mentored Training in Dissemination and Implementation Research in Cancer (MT-DIRC) program. MT-DIRC is supported through a NCI grant (R25CA171994-02) and by the Veterans Administration.
Dr. Christina Palmer served as Action Editor on the manuscript review process and publication decision.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Heather Zierhut, PhD, MS and Deborah Cragun, PhD, MS declare that they have no conflict of interest.
Human Subjects & Informed Consent
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000. Informed consent was obtained from all patients for being included in the study.
Animal Studies
No animal studies were carried out by the authors for this article.
Rights and permissions
About this article
Cite this article
Cragun, D., Zierhut, H. Development of FOCUS-GC: Framework for Outcomes of Clinical Communication Services in Genetic Counseling. J Genet Counsel 27, 33–58 (2018). https://doi.org/10.1007/s10897-017-0145-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10897-017-0145-0