Abstract
Sleep problems are common in autism and ADHD. No study has compared sleep problems by age in 2 to 17 year olds with autism versus ADHD-Combined versus ADHD-Inattentive type. Mothers rated 1415 youth with autism and 1041 with ADHD on 10 Pediatric Behavior Scale sleep items. Nighttime sleep problems were most severe in autism, followed by ADHD-Combined, and then ADHD-Inattentive. Difficulty falling asleep, restless during sleep, and waking during the night were the most common problems. Adolescents slept more at night than other age groups, and youth who slept more at night were sleepier during the day. Sleep problems declined with age, but correlations were small. In adolescence, 63% with autism, 53% with ADHD-Combined, and 57% with ADHD-Inattentive had difficulty falling asleep. Given that the majority of children in all age groups had one or more sleep problem, developmentally appropriate interventions are needed to address sleep difficulties and limit their adverse effects.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
For children in a general population sample, 19% had parent-reported difficulty falling and/or staying asleep (Calhoun et al., 2014). Sleep problems are even more common in youth with autism and in youth with ADHD. In comparison to typical peers, parent-reported sleep problems are more frequent in autism (Hodge et al., 2014; Krakowiak et al., 2008; Mayes et al., 2009a, 2012a) and in ADHD (Mayes et al., 2009b, 2012a). Youth with autism also have more sleep problems than youth with other neurodevelopmental disorders (Krakowiak et al., 2008; Mayes et al., 2012a). Youth with ADHD-Combined (ADHD-C) have higher rates of parent-reported sleep problems than youth with ADHD-Inattentive/ADHD-I (Mayes et al., 2012a), and increased movement during sleep is characteristic of ADHD-C and not ADHD-I (Corkum et al., 1999). A study of children with ADHD showed that comorbid anxiety and depression increased sleep problems, whereas comorbid oppositional defiant disorder (ODD) did not (Mayes et al., 2009b).
The causes of sleep problems in youth with autism and youth with ADHD are multifaceted and include pathophysiological, genetic, medical, psychological, and pharmacological factors, as well as parenting practices (Stores, 2016). Sleep problems can negatively impact daytime functioning (Becker et al., 2015). Studies have shown an association between sleep problems and neurocognitive functioning, emotional regulation, and behavior (Sadeh, 2007). Child sleep problems also disrupt the sleep of parents and siblings and cause stress for families (Hoffman et al., 2008). When sleep problems are successfully treated, daytime functioning can improve in youth with autism (Rossignol & Frye, 2011) and with ADHD (Keshavarzi et al., 2014).
Studies investigating the relationship between age and parent-reported sleep problems in autism yield contradictory results. Cross-sectional age analyses revealed nonsignificant age group differences in sleep onset delay, reduced sleep duration, waking during the night, parasomnias, and daytime sleepiness in 108 youth 3–5 versus 6–9 versus 10–17 years (Hodge et al., 2014), 106 youth 4–10 versus 11–16 years (Hoffman et al., 2006), and 210 youth 2–5 versus 6–11 versus 12–16 years (Williams et al., 2004). Relatedly, age was not a significant predictor of a composite sleep problems score in 477 youth with autism 1 to 15 years of age (Mayes & Calhoun, 2009). Furthermore, 69 youth with autism, 5–16 years with versus without sleep problems, did not differ significantly in age (Wiggs & Stores, 2004). In contrast, research using a much larger autism sample of 1859 youth (thereby increasing the likelihood of finding significant differences) compared four age groups (3–4, 5–6, 7–10, and 11–18 years) and found a nonsignificant difference between groups in the composite sleep problems score but significant differences for some specific sleep item scores. Older youth had greater sleep onset delay, shorter sleep duration, and more daytime sleepiness, while younger youth had more night wakings and parasomnias (Goldman et al., 2012). In a longitudinal study of youth assessed at 7–9 and 11–13 years of age, the 28 youth with autism developed more difficulty initiating and maintaining sleep over time than controls and this problem persisted longer, with a remission rate of 8% for autism and 52% for controls (Silversten et al., 2012).
The relationship between age and sleep problems in youth with ADHD has received little attention. In a study of 195 youth with ADHD 5–13 years of age, parents were asked at baseline and at 6 and 12 months follow-up, “Has your child’s sleep been a problem for you over the past 4 weeks?” Sleep problems persisted over a 1-year period for only 20 (10%) of the youth (Lycetta et al., 2014). In marked contrast, a study of 27 youth 7–13 years of age receiving outpatient intervention for ADHD showed that at 18-month follow-up, 71% of the youth with ADHD (vs. 50% of the controls) who had a clinically elevated total sleep problem score at baseline continued to be elevated at follow-up (Hansen et al., 2013).
Purpose
Our study focuses on ADHD and autism, two of the most common referrals to child psychiatric diagnostic clinics and two disorders known to be highly associated with sleep problems. The study is the first to analyze and compare types and frequencies of sleep problems by age in large samples of youth 2–17 years of age with autism, ADHD-Combined presentation (ADHD-C), and ADHD-Inattentive presentation (ADHD-I). ADHD-C and ADHD-I have not typically been separated in previous studies, which is important because sleep problems differ between the two subtypes. Study objectives were to (1) determine the frequency and severity of mother-reported sleep problems at successive ages, (2) examine the pattern of sleep problems relative to age (when specific sleep problems were likely to occur, peak, decline, or remain stable), and (3) compare sleep problems and age-related patterns between diagnostic groups (autism, ADHD-C, and ADHD-I). We hypothesize that age may be significantly related to some specific sleep problems, but that the associations will be small given that prior research has yielded inconsistent findings. Results of our study will inform clinicians and caregivers about developmental aspects of sleep problems in particularly vulnerable populations to aid in their management.
Methods
Samples
The study was approved by the Institutional Review Board, which waived informed consent because analyses were conducted retrospectively on existing clinical data. The sample included 2456 youth (1415 with autism, 739 with ADHD-C, and 302 with ADHD-I) evaluated in a Psychiatry diagnostic clinic over the past 25 years. Youth were referred to the clinic by primary care or intervention providers, schools, and parents because of possible ADHD or autism or significant behavior problems. The clinic serves rural, suburban, and urban areas. Clinical diagnoses of autism and ADHD were made by a licensed PhD psychologist based on a comprehensive psychological evaluation including diagnostic interviews with the parents and child, parent and teacher rating scale scores, review of educational and medical records, psychological testing (IQ, achievement, attention, and neuropsychological), and clinical observations during the psychological evaluation. Demographic and psychotropic medication data are presented in Table 1. Prescribed psychotropic medication percentages for the total sample were 24.0% ADHD medication (usually a stimulant), 7.8% antipsychotic (most often risperidone), 5.5% SSRI (most often sertraline), and 4.9% alpha agonist (clonidine or guanfacine). Less frequently prescribed psychotropic medications were an anticonvulsant, non-SSRI antidepressant, lithium, anxiolytic, and amantadine.
Youth in the autism sample had a DSM-IV or DSM-5 diagnosis of autism (i.e., autistic disorder, Asperger’s disorder, or autism spectrum disorder) using the DSM version that was current at the time the child was evaluated, and all youth had a score in the autism range on the Checklist for Autism Spectrum Disorder (CASD, Mayes, 2012). The CASD is 30-item diagnostic checklist normed and standardized on 2469 youth (1–18 years, IQs 9–146) with autism, other clinical disorders, and typical development (Mayes, 2012). In the national standardization study, the CASD differentiated youth with and without autism with 99.5% accuracy. Studies demonstrate that the CASD distinguishes youth with autism from youth with intellectual disability, learning disability, traumatic brain injury, language disorder, ADHD, ODD, and anxiety disorder (Mayes, 2012), apraxia of speech (Tierney et al., 2015), and reactive attachment disorder (Mayes et al., 2017). Concurrent validity is strong, and studies (Mayes et al., 2009c; Murray et al., 2011) demonstrate high diagnostic agreement between the CASD and the Childhood Autism Rating Scale (98%), the Gilliam Asperger’s Disorder Scale (94%), and the Autism Diagnostic Interview-R (93%).
All youth in the ADHD group had a DSM-IV or DSM-5 diagnosis of ADHD and fulfilled the following criteria: (1) symptoms of ADHD observed during psychological testing, (2) low scores on psychometric measures of attention, and (3) ratings of short attention span or distractible as often or very often a problem on the Pediatric Behavior Scale (PBS, Lindgren & Koeppl, 1987) by at least two raters (mother, father, teacher). Youth were classified with ADHD-C if the median item score across raters on the PBS hyperactive-impulsive subscale was often or very often a problem. Youth were classified with ADHD-I if the median hyperactive-impulsive score was less than often a problem.
Youth with autism who also had symptoms of ADHD were only included in the autism sample. An additional clinical diagnosis of ADHD could not be made because the DSM-IV did not permit an ADHD diagnosis with autism. In the autism sample, 79.5% had elevated (often or very often a problem) maternal ratings on the ADHD-C scale and 9.1% had elevated ratings on the attention deficit subscale but not on impulsivity/hyperactivity (ADHD-I). There were not enough youth with ADHD-Hyperactive/Impulsive presentation to include in the study. Youth with comorbid conditions (e.g., anxiety, depression, and/or ODD) were not excluded from the study so that the autism and ADHD samples were representative of referred youth.
Instrument
Mothers rated their children on the 165-item PBS on a 4-point scale (0 = almost never or not at all, 1 = sometimes, 2 = often, and 3 = very often a problem). The PBS assesses multiple psychological, developmental, and somatic problems and has 10 sleep items: difficulty falling asleep, restless during sleep, wakes during the night, nightmares, talks/walks in sleep, wets bed, wakes early, sleeps less than normal, sleeps more than normal, and daytime sleepiness. The PBS total sleep problems’ score correlates highly with scores on the Children’s Sleep–Wake Scale and on the Pediatric Sleep Questionnaire, with correlations of 0.76 and 0.72 (Mayes et al., 2008). The PBS corresponds well with established measures of psychopathology (Bixler et al., 2009; Mayes et al., 2014) and has been used to differentiate diagnostic groups and assess sleep and psychological problems in several published studies (Calhoun et al., 2017; Conrad et al., 2010; Mayes et al., 2011; Mayes et al., 2008, 2009a, 2012a; Waxmonsky et al., 2017).
Data Analyses
Differences in the 10 sleep problem scores between diagnostic and age groups were investigated with ANCOVA and post-hoc t tests, and the linear relationships between age and sleep problem scores were determined using partial correlations. Because of significant differences between diagnostic groups on most demographic variables, including age (Table 1), these variables were covaried in ANCOVA when comparing differences in sleep scores between diagnostic groups. Within the autism, ADHD-C, and ADHD-I samples, nonsignificant differences (p > 0.05) between the four age groups (preschool 2–5, early childhood 6–8, late childhood 9–12, and adolescence 13–17 years) were found for intellectual disability (ID, χ2 = 2.4–10.5), sex (χ2 = 1.9–9.6), race (χ2 = 7.3–8.0), and parent occupation (χ2 = 2.1–5.2), but psychotropic medication use differed by age group (χ2 = 11.7–250.9). Therefore, psychotropic medication status was controlled using ANCOVA when comparing sleep scores between age groups and using partial correlations when correlating age and sleep scores. The binomial test was used to investigate the pattern of the correlations (positive or negative) between sleep problems and age. All reported p values are 2 tailed and have a Bonferroni correction for the number of comparisons made.
Results
Differences in Sleep Problems between Diagnostic Groups
Overall, youth with autism had significantly higher sleep problem scores than youth with ADHD-C, who had higher scores than youth with ADHD-I (Table 2).
Correlations Between Age and Sleep Problem Scores
For autism, the linear relationships between age and sleep problem scores were significant for 7 of the 10 sleep variables (Table 3), but the significant correlations explained less than 6% of the variance. Sleeping more than normal and daytime sleepiness were positively associated with increasing age, and the nighttime sleep disturbance scores (difficulty falling asleep, restless during sleep, wakes during the night, nightmares, talks/walks in sleep, wets bed, wakes early, and sleeping less than normal) decreased as age increased. Although not all individual nighttime sleep problems were significantly correlated with age, the pattern of the correlations (all negative) was statistically significant (binomial p = 0.008). The strongest correlation (− 0.23) was a decrease in bed wetting with increasing age.
For ADHD-C, the linear relationships between age and sleep problems were significant for 5 of the 10 sleep variables (Table 3), but the significant correlations explained < 5% of the variance. Like autism, correlations between nighttime sleep problems and age were all negative (binomial p = 0.008) and the association between age and sleeping more than normal and daytime sleepiness was positive. The strongest correlation (− 0.22) was again between increasing age and a decrease in bed wetting.
For ADHD-I (Table 3), the only significant correlation was between increasing age and increasing difficulty falling asleep (0.16, explained variance 2.6%). Correlations indicated a negative relationship with age for 5 of the 10 variables (binomial p = 1.0). Like autism and ADHD-C, sleeping more than normal and daytime sleepiness were positively associated with increasing age and bedwetting was negatively associated with age.
Differences in Sleep Problem Scores between Age Groups
Autism
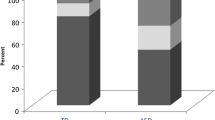
Six nighttime sleep problems were more frequent in the preschool than older age groups, and sleeping more than normal and daytime sleepiness were greatest in adolescents (Table 4 and Fig. 1). For the majority of youth with autism in all age groups, difficulty falling asleep and restless during sleep occurred sometimes or more. Bed wetting decreased with each successive age group, and sleeping more than normal and daytime sleepiness increased with each successive age group. Frequencies for the other sleep problems did not show a consistent linear pattern across age groups (Fig. 1). Sleep problems were more likely to be often or very often than sometimes a problem at almost all ages for difficulty falling asleep, restless during sleep, and sleeps less than normal.
ADHD-C
Overall, preschool children had the most severe nighttime sleep problems and were least likely to sleep more than normal or experience daytime sleepiness (Table 4 and Fig. 1). Sleeping more than normal and daytime sleepiness were greatest in adolescence. Bed wetting and waking early decreased in each successive age group, and daytime sleepiness increased. Sleep problems were more likely to occur often or very often than sometimes at almost all ages for difficulty falling asleep, restless during sleep, and sleeps less than normal.
ADHD-I
Most nighttime sleep problem scores were highest in preschool children with ADHD-I versus other age groups, but significant differences between age groups were few (Table 4). In contrast to findings for autism and ADHD-C, preschool children with ADHD-I were more likely to sleep more than the other age groups. As with the other diagnostic groups, daytime sleepiness was greatest in the 13–17 year age group (Fig. 1), but the difference was statistically nonsignificant. Only bed wetting decreased with each successive age group. Unlike autism and ADHD-C, nighttime sleep problems were not more likely to be severe than mild.
Correlations Between Sleep Duration and Daytime Sleepiness
Correlations between sleeping more than normal and daytime sleepiness (autism 0.28, ADHD-C 0.30, and ADHD-I 0.41) were highly significant (p < 0.0001) and were stronger than correlations between sleeping less than normal and daytime sleepiness (autism 0.12, ADHD-C 0.06, and ADHD-I 0.14).
Discussion
Our study samples were much larger (N = 2456) than in previous publications, and psychotropic medication (which can affect sleep) was controlled in the analyses, which has not been done in most prior research. Ten specific sleep problems were analyzed: difficulty falling asleep, restless during sleep, wakes during the night, nightmares, talks/walks in sleep, wets bed, wakes early, sleeps less than normal, sleeps more than normal, and daytime sleepiness. Hodge et al. (2014) emphasize the importance of analyzing types of sleep problems separately because different problems may or may not be related to age, which is obscured when a sleep problems composite score is used. Further, instead of simply dichotomizing sleep problems as present or absent, as done in most studies, our study differentiated mild from severe sleep problems.
Youth with autism had more nighttime sleep problems than youth with ADHD-C, who had more sleep problems than youth with ADHD-I. Nighttime sleep problems were more likely to be severe in autism and ADHD-C than in ADHD-I. For autism, ADHD-C, and ADHD-I, difficulty falling asleep, restless during sleep, and wakes during the night were the most common problems, occurring at least sometimes across age groups for 42–71% with autism, 37–58% with ADHD-C, and 24–64% with ADHD-I.
The linear association between age and sleep problems was strongest for autism, followed by ADHD-C, but all significant correlations (positive and negative) were small (< 0.24). As noted in the Introduction, no previous studies of children with autism or with ADHD have reported correlations between sleep problems and age, so our correlational findings cannot be compared with those of prior studies. Some small studies have found nonsignificant differences in sleep problems between age groups in youth with autism (Hodge et al., 2014; Hoffman et al., 2006; Williams et al., 2004), whereas a much larger study found significant age group differences for some specific sleep problems (Goldman et al., 2012).
Nighttime sleep problems in our study were negatively correlated with age in autism and ADHD-C, and most were negatively correlated with age in ADHD-I. Sleeping more than normal and daytime sleepiness were positively correlated with age (adolescents were the sleepiest) and were moderately correlated with each other (youth who were sleepier at night were also sleepier during the day). This suggests an underlying physiological basis for sleeping more than normal and daytime sleepiness and not that sleeping less than normal is the primary cause of daytime sleepiness. Daytime sleepiness was at least sometimes a problem for 39% of adolescents with autism, 30% with ADHD-C, and 38% with ADHD-I. Sleeping less than normal was least likely to occur in adolescents than all other age groups across diagnoses. These results are consistent with developmental changes in the circadian rhythm following puberty that can result in delayed sleep onset and increased need for sleep (Carskadon, 2011).
For all diagnostic groups, the strongest relationship between age and sleep problems was a decrease in bed wetting with increasing age. Even so, bedwetting occurred at least sometimes for 29% of 9 to12 year olds and 13% of adolescents with autism. Corresponding percentages were 19% and 5% for ADHD-C and 15% and 5% for ADHD-I. Other studies have also reported a decrease in bed wetting with age in autism (Williams et al., 2004), ADHD (Baeyens et al., 2007), and general population samples (Yeung et al., 2006).
For autism, some significant differences in mean sleep problem scores between age groups were found for all sleep variables except nightmares. Nighttime sleep problems were generally greatest in preschool children, whereas sleeping more than normal and daytime sleepiness were greatest in adolescence. For youth with ADHD-C, significant differences in mean sleep problem scores between age groups were found for 7 of the 10 sleep variables, but restless and talks/walks during sleep and sleeps more than normal were not significantly related to age. The pattern was similar to that for autism in that preschoolers tended to have the greatest nighttime sleep problems, and sleeping more than normal and daytime sleepiness were greatest in adolescence. For youth with ADHD-I, only 3 of the 10 sleep variables differed significantly between age groups, and the pattern was different than for autism and ADHD-C. Preschoolers slept more than normal and talked/walked in their sleep more than some older age groups, and adolescents had the most difficulty falling asleep. Furthermore, sleep problems were milder in ADHD-I than in ADHD-C and autism. Relatedly, other studies show that youth with ADHD-I (vs. ADHD-C) have better sleep efficiency and less fragmented sleep according to polysomnograph data (Ramos Platon et al., 1990), move less during sleep (Corkum et al., 1999), and have more daytime sleepiness assessed by multiple sleep latency tests (Lecendreux et al., 2000). Given the significant differences in sleep problems between ADHD-C and ADHD-I, it is important that future studies analyze ADHD-C and ADHD-I separately and not combine the two subtypes, as is typically done. Multiple studies demonstrate that youth with ADHD-C and ADHD-I differ on other critical dimensions as well. For example, in comparison to ADHD-I, youth with ADHD-C have more irritability and oppositional and aggressive behavior (Connor et al., 2010; Mayes et al., 2011, 2012b, 2015; Milich et al., 2001; MTA 1999).
Our study has several limitations. Sleep problems were based on maternal report and not self-report or objective sleep data; scores were cross sectional and not longitudinal; and our ADHD and autism samples were from a single clinical site. There were too few youth with ADHD-Hyperactive/Impulsive presentation to include in the study. Therefore, study findings need to be replicated with other samples and should include longitudinal data and additional measures of sleep problems, as well as autism and ADHD and sleep hygiene (e.g., electronics use during bedtime). Although medication status was controlled in our statistical analyses, the influence of specific medications needs to be investigated in future studies. Some psychotropic medications can disturb sleep (e.g., stimulants) and others can improve sleep (e.g., alpha agonists and antipsychotics). Psychotropic use also differs between diagnostic groups. For example, youth with ADHD-C and youth with autism are more likely to be treated with medication than youth with ADHD-I (Mayes et al., 2019).
Conclusions
Collectively, results show that nighttime sleep problems tend to decline with age. Even so, difficulty falling asleep occurred at least sometimes for 63% of adolescents with autism, 53% with ADHD-C, and 57% with ADHD-I. Waking during the night was at least sometimes a problem in adolescence for 42% with autism, 44% with ADHD-C, and 24% with ADHD-I. These findings support systematic screening and assessment of potential co-occurring sleep difficulties in youth with autism and ADHD so that intervention can be provided if needed. Evidence-based treatments to reduce sleep problems (specifically, difficulty falling asleep, waking during the night, and reduced sleep duration) in youth with autism and ADHD include (1) behavioral interventions and sleep hygiene techniques (Keshavarzi et al., 2014; Weiss et al., 2006), (2) melatonin (Garstang & Wallis, 2006; Rossignol & Frye, 2011; Weiss et al., 2006), (3) prescription medication, such as clonidine and guanfacine (Coleman et al., 2019), (4) cognitive behavioral therapy for insomnia (Paine & Gradisar, 2011), and (5) bedwetting alarms and prescribed medication for nocturnal enuresis (Crimmins et al., 2003). Given that the majority of children with autism or ADHD in all age groups in our study had one or more sleep problem, developmentally appropriate interventions are needed to address sleep difficulties and limit their adverse effects.
References
Baeyens, D., Roeyers, H., Van Erdeghem, S., Hoebeke, P., & Walle, J. V. (2007). The prevalence of attention deficit-hyperactivity disorder in children with nonmonosymptomatic nocturnal enuresis: A 4-year followup study. Journal of Urology, 178, 2616–2620.
Becker, S. P., Langberg, J. M., & Byars, K. C. (2015). Advancing a biopsychosocial and contextual model of sleep in adolescence: A review and introduction to the special issue. Journal of Youth and Adolescence, 44, 239–270.
Bixler, E. O., Vgontzas, A. N., Lin, H-M., Calhoun, S., Vela-Bueno, A., Fedok, F., … Graff, G. (2009). Sleep disordered breathing in children in a general population sample: Prevalence and risk factors. Sleep, 32, 731–736.
Calhoun, S. L., Fernandez-Mendoza, J., Vgontzas, A. N., Liao, D., & Bixler, E. O. (2014). Prevalence of insomnia symptoms in a general population sample of young children and preadolescents: Gender effects. Sleep Medicine, 15, 91–95.
Calhoun, S. L., Fernandez-Mendoza, J., Vgontzas, A. N., Mayes, S. D., Liao, D., & Bixler, E. O. (2017). Behavioral profiles associated with objective sleep duration in young children with insomnia symptoms. Journal of Abnormal Child Psychology, 45, 337–344.
Carskadon, M. A. (2011). Sleep in adolescents: The perfect storm. Pediatric Clinics of North America, 58, 637–647.
Coleman, D. M., Adams, J. B., Anderson, A. L., & Frye, R. E. (2019). Rating of the effectiveness of 26 psychiatric and seizure medications for autism spectrum disorder: Results of a national survey. Journal of Child and Adolescent Psychopharmacology, 29, 1–17.
Connor, D. F., Steeber, J., & McBurnett, K. (2010). A review of attention-deficit/hyperactivity disorder complicated by symptoms of oppositional defiant disorder or conduct disorder. Journal of Developmental and Behavioral Pediatrics, 31, 427–440.
Conrad, A. L., Richman, L., Lindgren, S., & Nopoulos, P. (2010). Biological and environmental predictors of behavioral sequelae in children born preterm. Pediatrics, 125, e83–e89.
Corkum, P., Moldofsky, H., Hogg-Johnson, S., Humphries, T., & Tannock, R. (1999). Sleep problems in children with Attention-Deficit/Hyperactivity Disorder: Impact of subtype, comorbidity, and stimulant medication. Journal of the American Academy of Child and Adolescent Psychiatry, 38, 1285–1293.
Crimmins, C. R., Rathbun, S. R., & Husmann, D. A. (2003). Management of urinary incontinence and nocturnal enuresis in attention deficit hyperactivity disorder. Journal of Urology, 170, 1347–1350.
Garstang, J., & Wallis, M. (2006). Randomized controlled trial of melatonin for children with autistic spectrum disorders and sleep problems. Child: Care Health and Development, 32, 585–589.
Goldman, S. E., Richdale, A. L., Clemons, T., & Malow, B. A. (2012). Parental sleep concerns in autism spectrum disorders: Variations from childhood to adolescence. Journal of Autism and Developmental Disorders, 42, 531–538.
Hansen, B. H., Skirbekk, B., Oerbeck, B., Wentzel-Larsen, T., & Kristensen, H. (2013). Persistence of sleep problems in children with anxiety and attention deficit hyperactivity disorders. Child Psychiatry and Human Development, 44, 290–304.
Hodge, D., Carollo, T. M., Lewin, M., Hoffman, C. D., & Sweeney, D. P. (2014). Sleep patterns in children with and without autism spectrum disorders: Developmental comparisons. Research in Developmental Disabilities, 35, 1631–1638.
Hoffman, C. D., Sweeney, D. P., Gilliam, J. E., & Lopez-Wagnaer, M. C. (2006). Sleep problems in children with autism and in typically developing children. Focus on Autism and Other Developmental Disorders, 21, 146–152.
Hoffman, C. D., Sweeney, D. P., Lopez-Wagnaer, M. C., Hodge, D., Nam, C. Y., & Botts, B. H. (2008). Sleep problems and mothers’ stress. Focus on Autism and Other Developmental Disorders, 23, 155–165.
Keshavarzi, Z., Bajoghli, H., Mohanadi, M. R., Salmanian, M., Kirov, R., Gerber, M., … Brand, S. (2014). In a randomized case-control trial with 10-years olds suffering from ADHD sleep and psychological functioning improved during a 12-week sleep-training program. World Journal of Biological Psychiatry, 15, 609–619.
Krakowiak, P., Goodlin-Jones, B., Hertz-Picciotto, I., Croen, L. A., & Hansen, R. L. (2008). Sleep problems in children with autism spectrum disorders, developmental delays, and typical development: A population-based study. Journal of Sleep Research, 17, 197–206.
Lecendreux, M., Konofal, E., Bouvard, M., Falissard, B., & Mouren-Simeoni, M.-C. (2000). Sleep and alertness in children with ADHD. Journal of Child Psychiatry, 41, 803–812.
Lindgren, S. D., & Koeppl, G. K. (1987). Assessing child behavior problems in a medical setting: Development of the pediatric behavior scale. In R. J. Prinz (Ed.), Advances in behavioral assessment of children and families (pp. 57–90). JAI.
Lycetta, K., Mensahb, F. L., Hiscockc, H., & Sciberras, E. (2014). A prospective study of sleep problems in children with ADHD. Sleep Medicine, 15, 1354–1361.
Mayes, S. D. (2012). Checklist for autism spectrum disorder. Stoelting.
Mayes, S. D., & Calhoun, S. L. (2009). Variables related to sleep problems in children with autism. Research in Autism Spectrum Disorders, 3, 931–941.
Mayes, S. D., Calhoun, S. L., Aggarwal, R., Baker, C., Mathapati, S., Anderson, R., & Petersen, C. (2012a). Explosive, oppositional, and aggressive behavior in children with autism compared to other clinical disorders and typical development. Research in Autism Spectrum Disorders, 6, 1–10.
Mayes, S. D., Calhoun, S. L., Bixler, E. O., & Vgontzas, A. N. (2008). Nonsignificance of sleep relative to IQ and neuropsychological test scores in predicting academic achievement. Journal of Developmental and Behavioral Pediatrics, 29, 206–212.
Mayes, S. D., Calhoun, S. L., Bixler, E. O., & Vgontzas, A. N. (2009a). Sleep problems in children with autism, ADHD, anxiety, depression, acquired brain injury, and typical development. Sleep Medicine Clinics, 4, 19–25.
Mayes, S. D., Calhoun, S. L., Bixler, E. O., Vgontzas, A. N., Mahr, F., Hillwig-Garcia, J., … Parvin, M. (2009b). ADHD subtypes and comorbid anxiety, depression, and oppositional-defiant disorder: Differences in sleep problems. Journal of Pediatric Psychology, 34, 328-337.
Mayes, S. D., Calhoun, S. L., Mayes, R. D., & Molitoris, S. (2012b). Autism and ADHD: Overlapping and discriminating symptoms. Research in Autism Spectrum Disorders, 6, 277–285.
Mayes, S. D., Calhoun, S. L., Murray, M. J., Ahuja, M., & Smith, L. A. (2011). Anxiety, depression, and irritability in children with autism relative to children with other neuropsychiatric disorders and typical development. Research in Autism Spectrum Disorders, 5, 474–485.
Mayes, S. D., Calhoun, S. L., Murray, M. J., Morrow, J. D., Yurich, K. K. L., Mahr, F., … Petersen, C. (2009c). Comparison of scores on the Checklist for Autism Spectrum Disorder, Childhood Autism Rating Scale (CARS), and Gilliam Asperger’s Disorder Scale (GADS) for children with low functioning autism, high functioning autism or Asperger’s disorder, ADHD, and typical development. Journal of Autism and Developmental Disorders, 39, 1682–1693.
Mayes, S. D., Calhoun, S. L., Waschbusch, D., & Baweja, R. (2017). Autism and reactive attachment/disinhibited social engagement disorders: Co-occurrence and differentiation. Clinical Child Psychology and Psychiatry, 22, 620–631.
Mayes, S. D., Gordon, M., Calhoun, S. L., & Bixler, E. O. (2014). Long-term temporal stability of measured inattention and impulsivity in typical and referred children. Journal of Attention Disorders, 18, 23–30.
Mayes, S. D., Waxmonsky, J., Calhoun, S. L., Kokotovich, C., Mathiowetz, C., & Baweja, R. (2015). Disruptive mood dysregulation disorder (DMDD) symptoms in children with autism, ADHD, and neurotypical development and impact of co-occurring ODD, depression, and anxiety. Research in Autism Spectrum Disorders, 18, 64–72.
Mayes, S.D., Waxmonsky, J.G., Baweja, R., Mattison, R.E., Memon, H., Hameed, U., & Waschbusch, D. (2019). Symptom and demographic predictors of psychotropic Medication use in ADHD and autism. International Journal of Clinical Psychiatry and Mental Health, 7, 10–20.
Milich, R., Balentine, A. C., & Lynam, D. R. (2001). ADHD combined type and ADHD predominantly inattentive are distinct and unrelated disorders. Clinical Psychology: Science and Practice, 8, 463–488.
MTA Cooperative Group. (1999). A 14-month randomized clinical trial of treatment strategies for attention-deficit/hyperactivity disorder. Archives of General Psychiatry, 56, 1073–1086.
Murray, M. J., Mayes, S. D., & Smith, L. A. (2011). Brief report: Excellent agreement between two brief autism scales (Checklist for Autism Spectrum Disorder and Social Responsiveness Scale) completed independently by parents and the Autism Diagnostic Interview-Revised. Journal of Autism and Developmental Disorders, 41, 1586–1590.
Paine, S., & Gradisar, M. (2011). A randomized controlled trial of cognitive-behaviour therapy for behavioural insomnia of childhood in school-aged children. Behavior Research and Therapy, 49, 379–388.
Ramos Platon, M. J., Vela Bueno, A., Espinar Sierra, J., & Kales, S. (1990). Hypnopolygraphic alternations in attention deficit disorder (ADD) children. International Journal of Neuroscience, 53, 87–101.
Rossignol, D. A., & Frye, R. E. (2011). Melatonin in autism spectrum disorder: A systematic review and meta-analysis. Developmental Medicine and Child Neurology, 53, 783–792.
Sadeh, A. (2007). Consequences of sleep loss or sleep disruption in children. Sleep Medicine Clinics, 2, 513–520.
Silversten, B., Posserud, M.-B., Gillberg, C., Lundervold, A. J., & Hysing, M. (2012). Sleep problems in children with autism spectrum problems: A longitudinal population-based study. Autism, 16, 139–150.
Stores, G. (2016). Multifactorial influences, including comorbidities, contributing to sleep disturbance in children with a neurodevelopmental disorder. CNS Neuroscience and Therapeutics, 22, 875–879.
Tierney, C., Mayes, S. D., Lohs, S. R., Black, A., Gisin, E., & Veglia, M. (2015). How valid is the checklist for autism spectrum disorder when a child has apraxia of speech? Journal of Developmental and Behavioral Pediatrics, 36, 569–574.
Waxmonsky, J., Mayes, S. D., Calhoun, S. L., Fernandez-Mendoza, J., Waschbusch, D., & Bixler, E. O. (2017). The association between disruptive mood dysregulation disorder symptoms and sleep problems in children with and without ADHD. Sleep Medicine, 37, 180–186.
Weiss, M. D., Wasdell, M. B., Bomben, M. M., Rea, K. J., & Freeman, R. D. (2006). Sleep hygiene and melatonin treatment for children and adolescents with ADHD and initial insomnia. Journal of the American Academy of Child and Adolescent Psychiatry, 45, 512–519.
Wiggs, L., & Stores, G. (2004). Sleep patterns and sleep disorders in children with autistic spectrum disorders: Insights using parent report and actigraphy. Developmental Medicine and Child Neurology, 46, 372–380.
Williams, P. G., Sears, L. L., & Allard, A. (2004). Sleep problems in children with autism. Journal of Sleep Research, 13, 265–268.
Yeung, C. K., Sreedhar, B., Sihoe, J. D. Y., Sit, F. K. Y., & Lau, J. (2006). Differences in characteristics of nocturnal enuresis between children and adolescents: A critical appraisal from a large epidemiological study. British Journal of Urology International, 97, 1069–1073.
Funding
None.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design, material preparation, data collection, and data analysis and interpretations. The first draft of the manuscript was written by Susan D. Mayes, and all authors commented on and revised all subsequent drafts of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest to declare.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
The study was approved by the Institutional Review Board, which waived informed consent because analyses were conducted retrospectively on existing clinical data.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mayes, S.D., Puzino, K., DiGiovanni, C. et al. Cross-Sectional Age Analysis of Sleep Problems in 2 to 17 Year Olds with ADHD Combined, ADHD Inattentive, or Autism. J Clin Psychol Med Settings 29, 239–248 (2022). https://doi.org/10.1007/s10880-021-09799-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10880-021-09799-9