Abstract
Paraprofessional workforces are becoming more common and can serve the otherwise unmet needs of diverse children and families. Compared to other workforces, limited research to date has explored factors such as stress and burnout that influence the sustainability of this workforce. Mindfulness-based interventions have been studied as stress-reduction programs for other workforces, but it is currently unknown whether mindfulness is acceptable to paraprofessionals, particularly those of a diverse ethnicity living in low-income, urban environments. The current investigation is a pilot study examining whether six weeks of mindfulness-based skills training can reduce stress, burnout, and improve sleep quality among a diverse paraprofessional workforce. Twenty six paraprofessionals (ages 24–58, M = 37.04, SD = 9.65) completed measures pre-training, post-training, and at a four week follow-up. Results indicated that this paraprofessional workforce found mindfulness practices acceptable and experienced significant reductions in perceived stress and emotional exhaustion, as well as improved sleep quality (p < .05) Mindfulness-based interventions may be useful in supporting the wellbeing of paraprofessionals from diverse backgrounds working in low-income, urban environments.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
To better serve children and families in low-income, urban environments; service agencies have begun to recruit community members to a diverse paraprofessional workforce strategically positioned to deliver mental health services (e.g., Musser-Granski and Carrillo 1997; Walter and Petr 2006). Paraprofessionals are defined by Durlak (1981) as individuals who have not received post-baccalaureate clinical training. Using a paraprofessional workforce for minority health promotion has several advantages including (1) reaching difficult-to-access populations, (2) the paraprofessional’s understanding of the culture of the community they serve, (3) reducing the cost of services, and (4) contributing to community empowerment (Gilkey et al. 2011; U.S. Department of Health and Human Services 2007; Witmer et al. 1995).
The role of a paraprofessional shares commonalities with the role of the mental health professional in dissemination of psychoeducational information, implementation of interventions, and the provision of psychosocial support (Kakuma et al. 2011). On the other hand, paraprofessionals are similar to mentors in that they are near-peers to the population with whom they work (Eby et al. 2013; Reinschmidt et al. 2006). As such, paraprofessionals assist in the engagement process and their role has been highlighted as crucial in the areas of disease prevention and public health promotion (Ramos et al. 2006; Rhodes et al. 2007), health education and intervention (Kim et al. 2005; Mullany et al. 2012), and family-school partnerships (Callejas et al. 2006). Moreover, paraprofessionals enhance efforts to prevent mental and physical illness (Ramos et al. 2006) as well as promote public health (Rhodes et al. 2007), health education (Kim et al. 2005), and the receipt of mental health services (Montgomery et al. 2010).
As paraprofessionals assume more complex and demanding roles in human service sectors, more attention must be paid to the management and sustainability of this unique workforce (Calzada et al. 2005). To date, limited research has examined how stress may influence paraprofessionals. Similar to mental health providers, paraprofessionals are likely to experience high levels of work-related stress and burnout given the nature of their profession where they are the “helper” and their clients are “help recipients” (Awa et al. 2010). Paraprofessionals who live and work in low-income, urban communities may be at particularly high-risk for psychological stress and burnout given they often experience the same stressors as the populations they serve (Frazier et al. 2007). These stressors include significant environmental and structural stressors such as poor living conditions, higher costs for basic goods and services, and decreased access to health care, which can contribute to chronically stressful working environments (Roth and Robbins 2004). Further, compared to traditional workforces, paraprofessionals are more likely to experience an imbalance between job demands and job skills, a lack of job control, and discrepancies between resources, expectations, and job reality; all of which can increase the risk for work-related stress and burnout (Schaufeli and Buunk 2003).
Chronic levels of high occupational stress can lead to a number of psychological, social, and physical problems for the affected individual and organization (Belkic et al. 2004; Cohen et al. 2007). Studies suggest that workplace stress negatively impacts cognitive functioning, interpersonal communication, job satisfaction, and staff burnout; contributing to poor morale, absenteeism, and high staff turnover (Michie and Williams 2003; Noblet and LaMontagne 2006). In mental health settings, work-related stress can interfere with staff’s ability to effectively communicate; thus contributing to reductions in effective treatment delivery, poorer service outcomes, and reduced recipient satisfaction (Brady et al. 2012; Garman et al. 2002).
Mindfulness has emerged as an evidence-based stress reduction program (e.g., Grossman et al. 2004). Mindfulness can be defined simply as paying attention to the present moment (Kabat-Zinn 1994). As such, mindfulness involves deliberately bringing one’s attention to current experience in a non-judgmental way. Indeed, studies have found that mindfulness-based interventions have a positive effect on mood, wellbeing, and psychological functioning among high-stress workforces such as nurses (Cohen-Katz et al. 2005; Foureur et al. 2013), teachers (Gold et al. 2010; Schonert-Reichl et al. 2015), primary care physicians (Krasner et al. 2009), and mental health trainees (Shapiro et al. 2007). In one study, individuals who participated in mindfulness training demonstrated improvement in a number of self-reported outcomes, including perceived stress, sleep quality, and decreased job burnout when compared to controls (Byron et al. 2015).
Despite the high-stress nature of the paraprofessional role, limited research to date has examined whether stress reduction programs such as mindfulness training may be useful in reducing job burnout. What is more, the bulk of research on mindfulness has been conducted among majority group populations (i.e., European-Americans and individuals from middle to high socioeconomic status). A recent meta-analysis indicated that of the 300 published studies on mindfulness-based interventions, only 10% included participants from non-dominant, traditionally underserved communities or populations (Fuchs et al. 2013).
Thus, the current study examines the potential effect and acceptability of a mindfulness-based skills program delivered to a culturally-diverse group of paraprofessionals in a high-stress role. To examine the effect of mindfulness on stress, we focused on: (1) psychological wellbeing as measured by perceived stress and job burnout; and (2) sleep, as a physical index of stress. Acceptability of mindfulness was assessed with open-ended questions following training. We hypothesized that the paraprofessionals would report a reduction in physical and psychological stress following six sessions of mindfulness-based skills training. We also predicted that paraprofessionals would report acceptability of the mindfulness practices.
Method
Participants
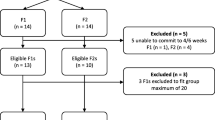
Twenty-six of 30 (87%) eligible staff at four agencies consented to complete measures assessing their demographics, stress, sleep, burnout, and the acceptability of mindfulness. Five individuals worked at Agency 1, four at Agency 2; eight at Agency 3, and nine at Agency 4. The majority (92%) were female. Participating staff ranged in age from 24 to 58 years old (M = 37.04, SD = 9.65), and had lived in Chicago for 2–55 years (M = 29.44, SD = 11.25). Participants resided in 25 different communities around Chicago, many within or adjacent to the communities in which they provided services. The majority were African-American (n = 17; 65%), and 35% (n = 9) were Hispanic/Latino. Participants reported educational levels ranging between High School/GED and Master’s Degree, with the modal response indicating “some college or other classes/training.” Sixty percent had worked in social services, youth services, or community organizations for 2 years or less. The majority of participants (46%) had worked in the overarching program for 2 years or more. Paraprofessional caseloads ranged from 15–25 children, (M = 19.46, SD = 2.45), with a modal caseload of 20 (n = 14).
Procedure
The current study took place within a paraprofessional-led early intervention and prevention program among low-income, urban African American and Latino communities. The program was offered in pre-Kindergarten through 3rd grade classrooms in 16 public schools for children demonstrating signs of emotional, behavioral, and/or academic risk. The paraprofessional staff, called School Family Liaisons (SFLs), were hired full-time by the four social service agencies and were supervised by master’s level clinicians. In addition to providing direct support to students, SFLs developed positive and supportive relationships with families—modeling and imparting information to parents about their children, the school, and strategies to support learning goals. SFLs also met critical family needs through case management services.
Paraprofessionals served families that were African American and Latino (61.3 and 33.0% respectively, in 2013–2014). Although income data was not collected from families participating in the school-based program, the percentage of students eligible for free lunch at participating schools ranged from 91.9–99.3% based on school reports. The four agencies in which SFLs worked were located in ethnically diverse neighborhoods with approximately 13–50% of the population living below the federal poverty line. The largest agency fell within one of the worst five neighborhoods in Chicago based on a hardship index calculated using census data from 2008–2012 on a number of socioeconomic indices (Chicago Department of Public Health 2014).
SFLs and their supervisors had identified stress reduction training as a need within the overarching school-based program. Due to this request, a six-session mindfulness-based skills training was provided to all SFLs as part of ongoing mandatory training at the four collaborating social service agencies. Researchers provided an overview of the study to eligible participants during an information session at each agency. Those who chose to participate were given the opportunity to ask questions and sign informed consent in one-on-one meetings. The six-session training was led by the first author, who had 6 years of personal mindfulness experience as well as previous studies adapting mindfulness practices for high-risk youth urban communities (Jacobs et al. 2016).
Training was conducted in two groups to balance travel time and staff availability. The first group met at Agency 1 and included Agencies 1 and 2 (n = 9). The second group met at Agency 3 and included staff from Agencies 3 and 4 (n = 17). The six training sessions were delivered over the span of 8 weeks and the follow-up assessment took place 4 weeks after the final session. Participants received a gift card valued at $10 for completing measures at each time point, with the possibility of obtaining $30 in total remuneration at the end of the study. All study procedures were approved by the Institutional Review Board of the participating university.
The mindfulness-based skills training consisted of six 90-minute sessions. Each session included four main components: didactic presentation, experiential exercises, group discussions, and weekly homework assignments for personal practice. The first author presented each week’s theme through didactic and interactive materials. Topics included awareness of thoughts and emotions, identifying warning signs of stress in the mind and body, increasing attention to the positive, noticing when you are getting stuck in an unhelpful pattern, strategies for changing to a more adaptive pattern, self-care, an introduction to mindful parenting, and gratitude practices.
SFLs participated in a number of exercises such as progressive muscle relaxation, three-part breath, a body scan, mindful walking, lovingkindness, mindfulness of sound, and mindful listening. These exercises were short with the majority of practices lasting 5 min or less. Participants reflected upon their experience of mindfulness practices, shared their stressors in the workplace and at home, and discussed their sense of meaning in their professional and personal lives (e.g., their role as paraprofessionals, parents, and colleagues). Participants received handouts with information on mindfulness exercises, printed assignments, and online resources to facilitate participation inside and outside of training. These exercises and intervention components were developed based on those of Jacobs et al.’s (2016) study with adolescents, which taught short mindfulness exercises as a rumination reduction strategy.
Measures
Demographics
Information on SFL’s age, ethnicity, education status, and work experiences were obtained pre-training. This measure also asked about the value of the following factors in supporting job performance: sleep, feeling calm, the work environment, familial support, a supportive supervisor, and availability of job resources. SFLs were also asked to indicate whether they had prior exposure to the term or the practice of mindfulness.
Burnout
The Maslach Burnout Inventory (MBI; Maslach and Jackson 1981) was administered as a measure of burnout at pre-training, post-training, and at follow-up. The 22-item questionnaire assesses how individuals view their jobs and the people with whom they work on a seven-point Likert scale. The MBI consists of three subscales: emotional exhaustion, depersonalization, and reduced personal accomplishment. This measure’s properties are well established, particularly among human services professions (Cohen-Katz et al. 2005). Cronbach’s alpha for the subscales are reported as 0.90 for emotional exhaustion, 0.76 for depersonalization, and 0.76 for personal accomplishment (Iwanicki and Schwab 1981).
Stress
Stress was assessed at pre-training, post-training, and at follow-up using the 10-item Perceived Stress Scale (PSS; Cohen et al. 1983). The PSS examines the degree to which situations in one’s life are appraised as stressful in the past month. Items were rated on a five-point Likert scale. Higher scores indicate greater levels of perceived stress.
Sleep quality
The Pittsburg Sleep Quality Index (PSQI; Buysse et al. 1989) was used to assess quality of sleep among participants at pre-, post-, and follow-up time points. The PSQI is a 9-item questionnaire that evaluates indices of sleep characteristics (sleep quality, latency, duration, efficiency) on a four-point Likert scale. A total score above five is considered indicative of poor sleep quality (Buysse et al. 1989).
Acceptability
To examine participants’ attitudes toward mindfulness, we developed an acceptability questionnaire based on previous research with mental health staff who received similar mindfulness trainings (Marx et al. 2014). Questions administered post-training and at follow-up were open-ended and included the following: (1) How important has the training program been for you? (2) Would you recommend the training program to a work colleague? (3) Do you feel that the training has been beneficial in your work role? (4) Do you feel the training program has made a positive difference in your interactions with families? (5) Do you feel that the training program has made a positive difference in your interactions with work colleagues? Participant responses were subsequently coded by the first and third author as negative, neutral, and positive. Participants were also asked to answer the following questions on a Likert scale (0 = not at all; 5 = very much): (1) How relevant was what you learned to the stress you face in your life? (2) How likely are you to use mindfulness in your life (outside of this group)? and (4) How likely are you to use some of these skills with others (the families you work with)?
Homework completion
We assessed frequency of mindfulness practice outside of training at the start of each session during the six-week training. Participants were asked to rate (1) how many times they practiced being mindful during the past week (response options ranged from not at all to more than once a day) and (2) how much of the assigned mindfulness homework they attempted (response options ranged from not at all to more than once a day).
Data Analyses
Changes from pre-training to post-training and from pre-training to follow-up were compared using paired t-tests. The significance level for all tests was set at p < .05. All participants completed measures at pre-training, whereas two participants did not complete measures at post-training, and three participants did not complete measures at follow-up, due to no longer being employed at the respective agencies. These two cases were included in analyses using the strategy of last observation carried forward (except in the case of the qualitative acceptability responses). A completer analysis was also conducted for the sample that completed all time points (n = 24). For item-level missing data, the sample mean for the given item at that time-point was imputed if 70% or more of the individual’s measure was completed. Cohen’s d was calculated according to guidelines for within-subjects studies correcting for dependence among means (Cohen 1988; Morris and DeShon 2002).
Results
Pre-training
SFLs indicated that the following factors benefitted their job performance: a good night’s sleep, feeling calm, feeling unhurried in their workload, having a supportive relationship with a supervisor, having access to needed resources to complete job tasks, and having a supportive family. Sixty five percent of SFLs indicated that they had encountered the term ‘mindfulness’ prior to the training (n = 5 read about mindfulness, n = 14 had heard about mindfulness from friends or colleagues, n = 3 had attended a mindfulness training session previously).
Baseline scores indicated poor sleep quality (M = 6.16, SD = 3.15), with 62% of the sample falling at or above the threshold for poor sleep. Average perceived stress for the current sample (M = 14.46, SD = 5.53) was only slightly elevated compared to age-based norms (M = 13.0, SD = 6.2; Cohen and Williamson 1988). Emotional exhaustion (M = 17.00, SD = 8.93) and depersonalization were in the low range (M = 2.21, SD = 3.02) compared to other health care professionals (Maslach et al. 1996), whereas level of personal accomplishment was average (M = 38.64, SD = 5.96).
Post-training and Follow-up
Attendance across the six training sessions ranged between 75–100%. Figure 1 summarizes change over time. Sleep quality improved from pre-training to post-training, but was not significant (t = 1.27, df = 25, p = .22). Sleep quality continued to improve between post-training and follow-up (t = 3.76, df = 24, p < .01; Cohen’s d = .45). The difference between baseline and follow-up was also significant (t = 3.51, df = 25, p < .01; Cohen’s d = 0.62) with the number of participants meeting criteria for poor sleep reduced to 42% (compared to 62% at baseline). Change in perceived stress was statistically significant from pre-training to post-training (t = 2.48, df = 25, p = .02; Cohen’s d = 0.33) and from pre-training to follow-up (t = 3.15, df = 25, p < .01; Cohen’s d = 0.47). The difference between post-training and follow-up on perceived stress was not significant. The only component of burnout to improve significantly between pre-training and follow-up was on the emotional exhaustion component (t = −3.35, df = 25, p < .01; Cohen’s d = .55), with the majority of change occurring between post-training and follow-up (t = 3.92, df = 25, p < .01; Cohen’s d = .47). Analyses conducted on the completer sample were the same for all outcomes.
Significant improvement in sleep, stress, and emotional exhaustion in a pilot study of mindfulness-based skills training. Note. Panel a Sleep disturbance as measured by the Pittsburgh Sleep Quality Index; Panel b Perceived stress as measured by the Perceived Stress Scale; and Panel c Emotional exhaustion as measured by the Maslach Burnout Inventory
Table 1 details means, standard deviations, and the range of responses at pre-treatment, post-treatment, and follow-up.
Homework Completion
Modal responses indicated that SFLs practiced being mindful in some form two to three times a week and that they practiced the specific assigned exercise approximately once in-between sessions.
Acceptability
Table 2 displays the percentage of SFLs responding positively, neutrally, or negatively to open-ended acceptability questions at follow-up and indicated that the majority of SFL’s responses were positive. Figure 2 displays Likert scale responses provided by SFL’s regarding their perceptions of the relevance of mindfulness (Panel a), the likelihood that they would use mindfulness in their own lives (Panel b), and the likelihood of implementing mindfulness with others (Panel c). Responses indicate that SFLs found mindfulness practices relevant and useful to their personal and work lives.
A majority of participant responses to questions assessing acceptability of mindfulness were coded as positive. Example themes extracted from these responses included participants’ perceptions that mindfulness training and skills were relevant for general personal improvement (e.g., “taught me how to calm myself using positive techniques”; “reminded me of simple ways to improve my day”), self-awareness and focus (e.g., “helped me reflect on my thinking”, “helped me stay focused on completing one task before moving on to the next”), interactions with families and schools (“provided more insight on how I can get families to relax more and stay focused”, “helped me implement exercises and games in sessions to help students be more mindful”), and relationships/interactions with co-workers (e.g., “helped me better deal with stress surrounding colleagues”; “helped me think why others are upset…It might be other issues and not me”). For some participants, exposure to mindfulness concepts and practices may have dispelled myths about mindfulness (“I thought it was some kind of chanting practice… so I wasn’t that excited at first”; “It showed me that I was already using some mindfulness before and I didn’t know I was using it”). A small percentage of comments indicated that not all participants found the training particularly useful (e.g., “… was difficult because I have a hard time relaxing in a large setting”).
Discussion
The current study suggests that 6 weeks of mindfulness-based skills training can result in reductions in perceived stress among a diverse paraprofessional workforce working in environments of urban poverty. Follow-up data indicate that stress continued to improve over four additional weeks. Follow-up data also indicate significant improvement in sleep quality and emotional exhaustion. Open-ended responses from participants suggested that the overwhelming majority of this sample found mindfulness skills acceptable and useful to their personal lives and work roles.
These findings are consistent with studies examining mindfulness in the reduction of perceived stress (Shapiro et al. 2007) and burnout (Cohen-Katz et al. 2005) among health care professionals and add to a growing body of literature suggesting that these practices can be useful with diverse populations (Le and Gobert 2015; Roth and Robbins 2004). It is noteworthy that the largest effect size was found for improvement in sleep quality. Meta-analytic results have varied in their estimates of the influence of mindfulness on physical health outcomes, such as sleep. For example one meta-analysis of mindfulness-based stress reduction (MBSR) found an overall medium effect size for mental and physical health outcomes (Grossman et al. 2004), whereas a more recent meta-analysis of meditation programs found limited evidence of influence on sleep (Goyal et al. 2014). This finding is also noteworthy given a documented sleep disparity in that poor sleep quality has been associated with poverty and race (Patel et al. 2010). Our finding of significant change may be due to the fact that the current sample had a greater potential to change in the domain of sleep compared to the samples included in meta-analyses to date.
It is nevertheless impressive that these gains were made with a staff experiencing considerable stress and living and working in communities of extreme poverty. Specifically, these improvements were observed in the context of reductions in funding at all four agencies from state budget cuts, and the impending end of funding for the overarching project. Thus, many SFLs were experiencing the stress of preparing to enter the job market due to necessity and their positive experiences with mindfulness training suggests that it allowed them to better cope with their stress in spite of these employment and funding challenges. The current results should be replicated, but indicate that mindfulness training may be useful in reducing sleep disparities even in the face of chronic and acute stress.
It is striking that the current sample did not report high levels of burnout prior to training. However, despite indicating a lower level of emotional exhaustion than other health care professionals, SFLs still experienced a significant reduction in work-related emotional overextension and exhaustion over the follow-up. The burnout measure used for the current study was selected to parallel other studies of wellbeing among those in health workforces, but it is possible the current measure is less relevant to the current sample. It is also possible that unmeasured traits of this specific workforce contribute to resilience to burnout. For example, commitment to their local community may protect against depersonalization. Indeed, SFLs reported average levels of personal accomplishment, which included feelings of competence and successful achievement in one’s work. SFLs did not endorse any depersonalization, which captures an unfeeling and impersonal response towards recipients. This is perhaps not surprising given that SFLs were often recruited for their position due to their personal and professional connections with the schools, communities, or agencies as well as their defined role as facilitator of connections between parents, children, teachers, and schools.
It is also worth noting that the current sample indicated some previous exposure to the concept of mindfulness prior to training. It is possible that awareness of the term may have made the current sample more open to learning about these practices. In fact, the majority of the first session was spent discussing the concept of mindfulness and what it might include. Many SFLs associated mindfulness with general concepts of self-care or “going to a spa.” On the other hand, over the course of training, SFLs also became aware that certain skills they already employed could be included under the umbrella term of mindfulness. For example, one SFL noted that the training “showed me that I was already using some mindfulness before and I didn’t know I was using it.”
As noted, this training was delivered in response to ongoing concerns from SFLs about managing their own stress as well as working with families that face ongoing chronic stress. Attending to the expressed need for support in these areas was critical for agency leadership and university partners for two reasons. First, given the high risk for stress, burnout, and turnover in a paraprofessional workforce (Frazier et al. 2007; Schaufeli and Buunk 2003), providing SFLs with strategies to manage their own stress was understood as important. Second, ongoing training opportunities and development for paraprofessionals around skills that directly relate to or inform their roles and responsibilities have been identified as essential in order for this workforce to deliver high quality services (Calzada et al. 2005; Catalani et al. 2009). Since chronic stress was identified as a significant challenge facing the families SFLs served, and because parental and family stress contributes to decreased capacity for positive and engaged parenting (Conger and Donnellan 2007), equipping the SFLs with stress-reduction strategies that they could potentially pass on to families represented a critical area for training and support. While there is always a cost associated with training and professional development—time spent in training is time that cannot be spent on other important weekly tasks—the roughly 9 h total across 6 weeks was understood by agencies as a feasible and acceptable investment in their paraprofessional staff. Future research can include specific analyses of cost-benefit ratios and the sustainability of such training within various systems of care.
Limitations
The current study has several limitations. The first is the lack of a control group, which does not allow us to test whether the observed changes are specific to the mindfulness training. Thus, we cannot rule out unobserved variables that may have led to improvements in wellbeing over the course of the study. However, given the extra stress of the decrease in funding at the agencies in particular, the opposite may have been expected. Another limitation is that the level of homework completion for the current study could be considered minimal when compared to traditional MBSR. It is interesting that significant change was observed despite relatively low levels of practice. Future research can examine methods for supporting more regular practice in these communities as well as the effect of dose of practice on response. We might expect similar minimal homework dosage with parents or families in these communities, as SFLs can be regarded as a gauge for the implementation of practices in a real-world, urban sample. As such, it is possible that lower engagement in homework practices may still yield positive effects in these communities. In addition, the coding of acceptability questionnaires was conducted by part of the research team who were not blind to study hypotheses. Future studies should include blind review of qualitative data to ensure bias-free assessment. However, it is worth noting that 80% of responses included clear words such as “yes” or “no.” Thus, only 20% of the current study responses were exposed to potential bias. Last, the current study did not include a mindfulness measure. This was due to the desire to keep the battery short and the limitations of self-report mindfulness measures (Bergomi et al. 2013); however, without a measure of mindfulness, we cannot say the changes observed were due to mindfulness per se. For example it is possible that group processing of stress led to the positive effects of the current intervention. Future studies can include a larger assessment battery to examine these possibilities.
Our findings indicate that mindfulness training and practices may be viewed as acceptable to a paraprofessional workforce living and working within primarily low-income and racially diverse neighborhoods. Acceptability, the perception of an innovation as agreeable and appealing, has been identified as one important individual-level factor affecting the extent to which a setting will implement a particular practice or innovation (Proctor et al. 2010). Individual attitudes and beliefs have been linked to successful dissemination and implementation (Rogers 2003). The current preliminary evidence of acceptability among this population supports future research that can examine whether paraprofessionals can teach stress-reduction techniques to children and families living in urban poverty. In addition, paraprofessionals may be able to support recent implementation and dissemination efforts to deliver mindfulness in schools. For example, recent pilot work suggests that mindfulness training among lower-income and ethnic minority elementary school children may improve classroom behavior as rated by teachers (Black and Fernando 2014). Given the goals of the current overarching school-based program, we hope to design future studies to examine whether mindfulness skills improve SFLs’ abilities to interact with parents, teachers, and children and measure whether and how SFLs pass on these skills to promote wellness among youth.
References
Awa, W. L., Plaumann, M., & Walter, U. (2010). Burnout prevention: A review of intervention programs. Patient Education and Counseling, 78, 184–190.
Belkic, K. L., Landsbergis, P. A., Schnall, P. L., & Baker, D. (2004). Is job strain a major source of cardiovascular disease risk? Scandinavian Journal of Work, Environment & Health, 30, 85–128.
Bergomi, C., Tschacher, W., & Kupper, Z. (2013). The assessment of mindfulness with self-report measures: Existing scales and open issues. Mindfulness, 4, 191–202.
Black, D. S., & Fernando, R. (2014). Mindfulness training and classroom behavior among lower-income and ethnic minority elementary school children. Journal of Child and Family Studies, 23, 1242–1246.
Brady, S., O’Connor, N., Burgermeister, D., & Hanson, P. (2012). The impact of mindfulness meditation in promoting a culture of safety on an acute psychiatric unit. Perspectives in Psychiatric Care, 48, 129–137.
Buysse, D. J., Reynolds, C. F., Monk, T. H., Berman, S. R., & Kupfer, D. J. (1989). The Pittsburgh sleep quality index: A new instrument for psychiatric practice and research. Psychiatry Research, 28, 193–213.
Byron, G., Ziedonis, D. M., McGrath, C., Frazier, J. A., & Fulwiler, C. (2015). Implementation of mindfulness training for mental health staff: Organizational context and stakeholder perspectives. Mindfulness, 6, 861–872.
Callejas, L., Nesman, R., Mowery, D., & Garnache, P. (2006). Research with Latino populations. In M. Hernandez et al. (Eds.). Examining the research base supporting culturally competent children’s mental health services (pp. 83–116). Tampa, FL: Research & Training Center for Children’s Mental Health.
Calzada, E. J., Caldwell, M. B., Brotman, L. M., Brown, E. J., Wallace, S. A., McQuaid, J. H., & O’Neal, C. R. (2005). Training community members to serve as paraprofessionals in an evidence-based, prevention program for parents of preschoolers. Journal of Child and Family Studies, 14, 387–402.
Catalani, C. E. C., Findley, S. E., Matos, S., & Rodriguez, R. (2009). Community health worker insights on their training and certification. Progress in Community Health Partnerships:Research, Education, and Action, 3, 201–202.
Chicago Department of Public Health (2014). Selected socioeconomic indicators in Chicago, 2008 – 2012. Retrieved July 11, 2016 from https://data.cityofchicago.org/Health-Human-Services/Census-Data-Selected-socioeconomic-indicators-in-C/kn9c-c2s2
Cohen, S., & Williamson, G. (1988). Perceived Stress in a Probability Sample of the United States. In Spacapan, S. and Oskamp, S. (Eds.) The Social Psychology of Health. Newbury Park, CA: Sage.
Cohen, S., Kamarck, T., & Mermelstein, R. (1983). A global measure of perceived stress. Journal of Health and Social Behavior, 24, 386–396.
Cohen, S., Janicki-Deverts, D., & Miller, G. E. (2007). Psychological stress and disease. JAMA : the Journal of the American Medical Association, 298, 1685–1687.
Cohen-Katz, J., Wiley, S. D., Capuano, T., Schaufeli, D. M., & Shapiro, S. (2005). The effects of mindfulness‐based stress reduction on nurse stress and burnout, part II: A quantitative and qualitative study. Holistic Nursing Practice, 19, 26–35.
Conger, R.D., & Donnellan, M.B. (2007). An interactionist perspective on the socioeconomic context of human development. Annual Review of Psychology, 58, 175–199.
Durlak, J. A. (1981). Evaluating comparative studies of paraprofessional and professional helpers: A reply to Nietzel and Fisher. Psychological Bulletin, 89, 566–569.
Eby, L. T. D., Allen, T. D., Hoffman, B. J., Baranik, L. E., Sauer, J. B., Baldwin, S., & Evans, S. C. (2013). An interdisciplinary meta-analysis of the potential antecedents, correlates, and consequences of protégé perceptions of mentoring. Psychological Bulletin, 139, 441–476.
Foureur, M., Besley, K., Burton, G., Yu, N., & Crisp, J. (2013). Enhancing the resilience of nurses and midwives: Pilot of a mindfulness based program for increased health, sense of coherence and decreased depression, anxiety and stress. Contemporary Nurse, 45, 114–125.
Frazier, S. L., Abdul-Adil, J., Atkins, M. S., Gathright, T., & Jackson, M. (2007). Can’t have one without the other: Mental health providers and community parents reducing barriers to services for families in urban poverty. Journal of Community Psychology, 35, 435–446.
Fuchs, C., Lee, J. K., Roemer, L., & Orsillo, S. M. (2013). Using mindfulness-and acceptance-based treatments with clients from nondominant cultural and/or marginalized backgrounds: Clinical considerations, meta-analysis findings, and introduction to the special series: Clinical considerations in using acceptance-and mindfulness-based treatments with diverse populations. Cognitive and Behavioral Practice, 20, 1–12.
Garman, A. N., Corrigan, P. W., & Morris, S. (2002). Staff burnout and patient satisfaction: Evidence of relationships at the care unit level. Journal of Occupational Health Psychology, 7, 235–241.
Gilkey, M., Garcia, C. C., & Rush, C. (2011). Professionalization and the experience-based expert: Strengthening partnerships between health educators and community health workers. Health Promotion Practice, 12, 178–182.
Gold, E., Smith, A., Hopper, I., Herne, D., Tansey, G., & Hulland, C. (2010). Mindfulness-based stress reduction (MBSR) for primary school teachers. Journal of Child and Family Studies, 19, 184–189.
Goyal, M., Singh, S., Sibinga, E. M., Gould, N. F., Rowland-Seymour, A., & Haythornthwaite, J. A. (2014). Meditation programs for psychological stress and well-being: A systematic review and meta-analysis. JAMA Internal Medicine, 174, 357–368.
Grossman, P., Niemann, L., Schmidt, S., & Walach, H. (2004). Mindfulness-based stress reduction and health benefits. A meta-analysis. Journal of Psychosomatic Research, 57, 35–43.
Iwanicki, E. F., & Schwab, R. L. (1981). A cross-validation study of the Maslach Burnout Inventory. Educational and Psychological Measurement, 41, 1167–1174.
Jacobs, R. H., Watkins, E. R., Peters, A. T., Feldhaus, C. G., Barba, A., Carbray, J., & Langenecker, S. A. (2016). Targeting ruminative thinking in adolescents at risk for depressive relapse: Rumination-focused Cognitive Behavioral Therapy in a pilot randomized controlled trial with resting state fMRI. PLoS ONE, 11, e0163952.
Kabat-Zinn, J. (1994). Wherever you go, there you are: Mindfulness meditation in everyday life. New York, NY: Hyperion.
Kakuma, R., Minas, H., van Ginneken, N., Dal Poz, M. R., Desiraju, K., Morris, J. E., & Scheffler, R. M. (2011). Human resources for mental health care: Current situation and strategies for action. The Lancet, 378, 1654–1663.
Kim, S., Flaskerud, J. H., Koniak-Griffin, D., & Dixon, E. L. (2005). Using community-partnered participatory research to address health disparities in a Latino community. Journal of Professional Nursing, 21, 199–209.
Krasner, M. S., Epstein, R. M., Beckman, H., Suchman, A. L., Chapman, B., Mooney, C. J., & Quill, T. E. (2009). Association of an educational program in mindful communication with burnout, empathy, and attitudes among primary care physicians. JAMA: the Journal of the American Medical Association, 302, 1284–1293.
Le, T. N., & Gobert, J. M. (2015). Translating and implementing a mindfulness-based youth suicide prevention intervention in a Native American Community. Journal of Child and Family Studies, 24, 12–23.
Marx, R., Strauss, C., Williamson, C., & Karunavira, T. (2014). The eye of the storm: A feasibility study of an adapted mindfulness-based cognitive therapy (MBCT) group intervention to manage NHS staff stress. The Cognitive Behaviour Therapist, 7, 1–17.
Maslach, C., & Jackson, S. E. (1981). The measurement of experienced burnout. Journal of Occupational Behavior, 2, 99–113.
Maslach, C., Jackson, S. E., & Leiter, M. P. (1996). Maslach burnout inventory manual. Palo Alto, CA: Consulting Psychologists Press.
Michie, S., & Williams, S. (2003). Reducing work related psychological ill health and sickness absence: A systematic literature review. Occupational and Environmental Medicine, 60, 3–9.
Montgomery, E. C., Kunik, M. E., Wilson, N., Stanley, M. A., & Weiss, B. (2010). Can paraprofessionals deliver cognitive-behavioral therapy to treat anxiety and depressive symptoms? Bulletin of the Menninger Clinic, 74, 45–62.
Morris, S. B., & DeShon, R. P. (2002). Combining effect size estimates in meta-analysis with repeated measures and independent-groups designs. Psychological Methods, 7, 105–125.
Mullany, B., Barlow, A., Neault, N., Billy, T., Jones, T., Tortice, I., & Walkup, J. (2012). The family spirit trial for American Indian teen mothers and their children: CBPR rationale, design, methods, and baseline characteristics. Prevention Science, 13, 504–518.
Musser-Granski, J., & Carrillo, D. F. (1997). The use of bilingual, bicultural paraprofessionals in mental health services: Issues for hiring, training, and supervision. Community Mental Health Journal, 33, 51–60.
Noblet, A., & LaMontagne, A. D. (2006). The role of workplace health promotion in addressing job stress. Health Promotion International, 21, 346–353.
Patel, N. P., Grandner, M. A., Xie, D., Branas, C. C., & Gooneratne, N. (2010). “Sleep disparity” in the population: Poor sleep quality is strongly associated with poverty and ethnicity. BMC Public Health, 10, 475.
Proctor, E., Silmere, H., Raghaven, R., Hovmand, P., Aarons, G., Bunger, A., Griffey, R., & Hensley, M. (2010). Outcomes for implementation research: Conceptual distinctions, measurement challenges, and research agenda. Administrative Policy in Mental Health, 38, 65–76.
Ramos, R. L., Hernandez, A., Ferreira-Pinto, J. B., Ortiz, M., & Somerville, G. G. (2006). Promovision: Designing a capacity-building program to strengthen and expand the role of promotores in HIV prevention. Health Promotion Practice, 7, 444–449.
Reinschmidt, K. M., Hunter, J. B., Fernandez, M. L., Lacy-Martínez, C. R., Guernsey de Zapien, J., & Meister, J. (2006). Understanding the success of promotoras in increasing chronic diseases screening. Journal of Health Care for the Poor and Underserved, 17, 256–264.
Rhodes, S. D., Foley, K. L., Zometa, C. S., & Bloom, F. R. (2007). Lay health advisor interventions among Hispanics/Latinos: A qualitative systematic review. American Journal of Preventive Medicine, 33, 418–427.
Rogers, E. M. (2003). Diffusion of innovations. New York, NY: Free Press.
Roth, B., & Robbins, D. (2004). Mindfulness-based stress reduction and health-related quality of life: Findings from a bilingual inner-city patient population. Psychosomatic Medicine, 66, 113–123.
Schaufeli, W. B., & Buunk, B. P. (2003). Burnout: An overview of 25 years of research and theorizing. In M. J. Schabracq, J. A. M. Winnubst, & C. L. Cooper (Eds.), The Handbook of work and health psychology. 2nd Edn. (pp. 383–425). West Sussex, England: Wiley.
Schonert-Reichl, K. A., Oberle, E., & Lawlor, M. S. (2015). Enhancing cognitive and social–emotional development through a simple-to-administer mindfulness-based school program for elementary school children: A randomized controlled trial. Developmental Psychology, 51, 52–66.
Shapiro, S. L., Brown, K. W., & Biegel, G. M. (2007). Teaching self-care to caregivers: Effects of mindfulness-based stress reduction on the mental health of therapists in training. Training and Education in Professional Psychology, 1, 105.
U.S. Department of Health and Human Services. (2007). Community health worker national workforce study. San Antonio: Regional Center for Health Workforce Studies of the University of Texas Health Science Center. Retrieved from http://bhpr.hrsa.gov/healthworkforce/reports/chwstudy2007.pdf.
Walter, U. M., & Petr, C. G. (2006). Lessons from the research on paraprofessionals for attendant care in children’s mental health. Community Mental Health Journal, 42, 459–475.
Witmer, A., Seifer, S. D., Finocchio, L., Leslie, J., & O’Neil, E. H. (1995). Community health workers: Integral members of the health care work force. American Journal of Public Health, 85, 1055–1058.
Funding
The study was funded by an anonymous donor.
Author Contributions
R.H.J., S.G., D.R., T.M., M.A.: designed and executed the study and wrote the paper. R.H.J., D.L., J.K.: analyzed the data. D.L., A.W. collaborated in the writing and editing of the final manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Ethical approval
All procedures performed were in accordance with ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments.
Rights and permissions
About this article
Cite this article
Jacobs, R.H., Guo, S., Kaundinya, P. et al. A Pilot Study of Mindfulness Skills to Reduce Stress among a Diverse Paraprofessional Workforce. J Child Fam Stud 26, 2579–2588 (2017). https://doi.org/10.1007/s10826-017-0771-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10826-017-0771-z