Abstract
Stromal derived factor-1 (SDF-1 or CXCL12) expressed by osteoblasts and endothelial cells, and its receptors CXCR4 and CXCR7/RDC1 are key molecular determinants in prostate cancer (PCa) metastasis. What drives PCa cells into the extravascular marrow space(s) once they make contact with the blood vessel endothelium, however remains unclear. Here, we evaluated whether degradation of CXCL12 facilitates PCa cell entry into the marrow cavity by locally lowering CXCL12 levels intravascularly. To explore this possibility, co-cultured conditioned media from PCa cells and endothelial cells were evaluated for their ability to degrade biotinylated CXCL12 (bCXCL12). Co-culture of PCa cells/endothelial cells resulted in greater digestion of CXCL12 than was achieved by either cell type alone, and this activity regulated invasion in vitro. The ability to degrade CXCL12 was not however observed in PCa and osteoblasts co-cultures. Fractionation and inhibitor studies suggested that the activity was CD26/dipeptidyl peptidase IV (DPPIV) and possibly other cysteine/serine proteases. By inhibiting CD26/DPPIV, invasion and metastasis of PCa cell lines were enhanced in in vitro and in vivo metastasis assays. Together, these data suggest that the degradation of CXCL12 by CD26/DPPIV may be involved in the metastatic cascades of PCa, and suggests that inhibition of CD26/DPPIV may be a trigger of PCa metastasis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
One of the most severe complications of prostate cancer (PCa) are skeletal metastases. Identifying the molecular mechanisms that regulate metastases is of clinical importance to determine those individuals at greatest risk. Yet many of these events remain unclear. In some cases, the anatomy of the efferent venous and lymphatic drainages have been put forth as potential mechanisms, however, it is also clear that anatomy alone is insufficient to explain metastatic patterns [1]. It has been recently appreciated that the expression of tissue-specific vascular ‘addresses’ that regulate leukocyte trafficking to specific vascular beds may be critical for the regulation of tumor metastasis [2–4].
Likewise, the metastatic process is functionally similar to the migrational or ‘homing’ behavior of hematopoietic stem cells (HSC) to the bone marrow. Numerous molecules have been implicated in regulating HSC homing, participating as both chemoattractants and regulators of cell growth. Our previous work in this field has drawn heavily on establishing parallels between the HSC homing and the PCa metastasis to the marrow. As a result, we identified that PCa cells use the CXC chemokine stromal derived factor-1 (SDF-1 or CXCL12) and its receptors CXCR4 [5–8] and CXCR7/RDC1 [9] as key elements in metastasis and growth in bone. We have observed that CXCR4 expression relates to increasing tumor grade [6] and that CXCL12 signaling through CXCR4 triggers the adhesion of PCa to bone marrow endothelial cells [5], possibly by activating and increasing the expression of αvß3 integrins [10] and CD164 [11]. Moreover, a positive correlation exists between tissue levels of CXCL12 and sites where metastatic PCa lesions are observed suggesting a selective effect [7]. Critically, antibody to CXCR4 significantly reduces the number of bone metastasis of PCa in vivo [7]. More recently we have demonstrated that annexin II expressed by osteoblasts and endothelial cells plays a critical role not only in HSC niche selection [12], but PCa metastasis [13].
What drives PCa cells into the extravascular spaces once they make contact with the endothelium remains unclear. Binding and immobilization of chemokines to glycosaminoglycan (GAG) side-chains of proteoglycans is believed to establish chemotactic gradients for chemokines present at very low concentrations [14]. Recent reports have also suggested a unique function for CXCR4 expressed on bone marrow endothelial cells, which efficiently internalizes circulating CXCL12, resulting in translocation of CXCL12 into the bone marrow [15].
Chemokine activity is known to be regulated by receptor expression and shedding, plasma membrane trafficking and proteolysis [14]. For example it is known that granulocyte colony-stimulating factor (G-CSF) treatment induces stem cell mobilization in the bone marrow by stimulating the CXCL12 degradation by leukocyte elastase [16]. CXCL12 is also known to be inactivated through cleavage by CD26/dipeptidyl peptidase IV (DPPIV) [17, 18], metalloproteinases [14] and serine proteases [19]. In addition, CD26/DPPIV has been reported to regulate G-CSF induced stem cell mobilization [20, 21], and inhibition of CD26/DPPIV has been demonstrated to improve hematopoietic stem cell engraftment during bone marrow transplantation [22]. CD26/DPPIV is a 110 kDa cell surface glycoprotein that belongs to the serine protease family. CD26/DPPIV is expressed on a variety of tissues including T lymphocyte, endothelial cells, and epithelial cells [23]. CD26/DPPIV also appears to play an important role in tumor progression [23].
In this study we determined if degradation of CXCL12 by CD26/DPPIV regulates PCa metastasis. We demonstrate that PCa cells and human endothelial cells together up-regulate their expression of CD26/DPPIV and degraded CXCL12 in co-culture. We also found that the inhibition of CD26/DPPIV in vitro was involved in PCa invasion. Using a novel in vivo PCa metastasis model recently developed by our group [24], we observed that inhibition of CD26/DPPIV increased metastatic seeding to peripheral organs. Thus, we believe that the degradation of CXCL12 by CD26/DPPIV may be involved in the metastatic cascades of PCa.
Materials and methods
Cell cultures
PC3 (CRL-1435) and LNCaP (CRL-1740) PCa cell lines were obtained from the American Type Culture Collection (Rockville, MD). PC3 was originally isolated from a vertebral metastasis and LNCaP was isolated from a lymph node of a patient with disseminated bony and lymph node involvement. C4-2B was derived from the parental LNCaP cell lines that were serially passaged in mice to obtain a more metastatic cell line [25]. The human bone marrow endothelial cells (HBME) were isolated from a normal Caucasian male and immortalized with SV40 large T-antigen [26]. PC3, LNCaP, C4-2B, and HBME were cultured in RPMI 1640 (Invitrogen, Carlsbad, CA), supplemented with 10% (v/v) fetal bovine serum (FBS; Invitrogen), 1% (v/v) penicillin-streptomycin (Invitrogen), and 1% (v/v) l-glutamine (Invitrogen). Primary human umbilical vein endothelial cells (HUVEC) and human dermal microvascular endothelial cells (HDMEC) were cultured as suggested by the vendor (Cambrex, Walkersville, MD). Human osteoblasts were established by explant culture from normal human trabecular bone obtained from patients undergoing orthopedic surgery in accordance with the University of Michigan’s Investigational Review Board, as previously described [27]. All cultures were maintained at 37°C, 5% CO2, and 100% humidity.
Generation of co-culture conditioned medium (CM)
Human endothelial cells or human osteoblast cells were seeded at a concentration of 2 × 105 cells per well in 500 μl of RPMI 1640 supplemented with 10% (v/v) FBS on 24-well tissue culture plate. After 24 h, PCa cells in 500 μl of RPMI 1640 supplemented with 10% (v/v) FBS were overlaid at 2 × 104 cells per well onto the endothelial cells or osteoblast cells. PCa cells alone (without endothelial or osteoblast cells) were maintained as additional controls. At 12, 24, or 48 h of co-culture, supernatant was collected, cleared from any free-floating cells by centrifugation for 5 min at 1,000g, and then stored at −80°C.
Enzyme-linked immunosorbent assay (ELISA)
CXCL12 and CD26/DPPIV levels of CM were determined by double-antibody sandwich method assembled with commercially available components (R&D systems, Minneapolis, MN), according to the directions of the manufacturer. Data were normalized to the total cell numbers.
CXCL12 degradation assay
CM (30 μl) were incubated with 200 ng/ml biotinylated CXCL12 (bCXCL12; R&D systems) for 2.5 h at 37°C. After incubation, the medium were run on 20% Tricine gels and the detection of the remaining bCXCL12 was accomplished by using strepavidin–horseradish peroxidase (HRP) and enhanced chemiluminescent (ECL). In some cases, CM were incubated with protease inhibitors (2.0 mM), at different concentrations (0.002–2.0 mM) of CD26/DPPIV inhibitor (diprotin A; Peptide Institute, Osaka, Japan) or 1 μg/ml of rhCD26/DPPIV (R&D systems) for 1 h at 4°C before bCXCL12 incubation. The densities of the bands were quantified with Image J software (version 1.40; National Institutes of Health (NIH), Bethesda, MD).
Immunohistochemistry
HBME and PC3 cells were either cultured alone or co-cultured on Lab-Tek II 4-chamber slides (Nalge Nunc International, Naperville, IL). HBME was cultured at 5 × 105 cells/chamber. After 24 h, PC3 cells were plated onto the HBME at 5 × 104 cells/chamber. At 48 h, the cells were fixed in 4% paraformaldehyde for 25 min at room temperature, washed and endogenous peroxidase activity quenched with 75 mM NH4Cl and 20 mM glycine in PBS at room temperature for 10 min. Thereafter, the cells were incubated with a 1:50 dilution of either the anti-CD26/DPPIV antibody (clone M-A261, BD Pharmingen, San Jose, CA) or an IgG1 matched isotype control antibody (clone G18-145, BD Pharmingen) for 1 h at room temperature. Antibody detection was performed by using a mouse HRP-AEC staining kit (R&D Systems). The staining intensities of the slides were quantified with Image J software, and data were normalized to the total cell numbers.
Invasion assays
Cell invasion assays were performed by using matrigel coated invasion chambers (BD Biosciences, San Jose, CA). PC3 cells were placed in the upper well (1 × 105 cells/well) in 100 μl of serum free RPMI 1640, and 600 μl of RPMI 1640 with or without CXCL12 (200 ng/ml) or 600 μl of CM was added to the bottom well. In some case, 2 mM of diprotin A were incubated with the CM for 30 min at 4°C. Invasion chambers were incubated at 37°C for 24 h. Thereafter, 40 μl (5 mg/ml) and 80 μl of 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT; Sigma-Aldrich, St Louis, MO) were added to the top and the bottom well, respectively, and then incubated for further 4 h. At the termination of the assay, the cells on the upper side of the membrane were removed with a cotton swab and the cells on the lower surface were released with 1 ml of isopropanol (Sigma-Aldrich) for 30 min. The 100 μl of extracts from each well were read on a multi-well scanning spectrophotometer (Molecular Devices, Sunnyvale, CA) at OD450.
In vivo PCa metastasis assay
Minimal PCa metastases that were observed in the severe combined immunodeficiency (SCID) mouse were assessed by using real-time polymerase chain reaction (QPCR), as previously described [24].
Male 5- to 7-week-old CB.17. SCID mice (Charles River, Wilmington, MA) were implanted with 2 × 105 cells of PC3 cells in sterile collagen scaffolds (3 × 3 × 3 mm3, Gelfoam; Pharmacia & Upjohn, New York, NY) in the mid dorsal region of each mouse. Thereafter, 5 μmol of diprotin A in 100 μl of 0.9% (w/v) saline (Fisher Diagnostics, Middle town, VA) was administered subcutaneously twice a day. A control group was administered equal volume of 0.9% (w/v) saline on the same schedule. The animals were then sacrificed, and tissue samples from the animals’ left organ/tissue (the original scaffold, brain, liver, spleen, periaortic lymph nodes, kidney, adrenal gland, prostate, calvaria, mandible, humeri, femur, tibia, pelvis, spine, and peripheral blood) were dissected and stored at −80°C until genomic DNA extraction.
All experimental procedures were approved by the University of Michigan Committee for the Use and Care of Animals (UCUCA).
Genomic DNA extraction and QPCR
The genomic DNA from the designated tissues was extracted by using DNeasy Blood and Tissue Kit (Qiagen, Valencia, CA), according to the manufactural protocol.
PC3 engraftments were assessed by QPCR using for human Alu sequences (Foward—5′-CAT GGT GAA ACC CCG TCT CTA-3′, Reverse—5′-GCC TCA GCC TCC CGA GTA G-3′, and TaqMan probe—5′-FAM-ATT AGC CGG GCG TGG TGG CG-TAMRA-3′; Applied Biosystems, Foster City, CA).
QPCR analysis was performed using 15.0 μl of TaqMan® Universal PCR Master Mix (Applied Biosystems), 1.5 μl of TaqMan® Gene Expression Assay or 3.0 μl of human Alu (forward and reverse primers at 18 μM and Taqman probe at 5 μM), 2 μg of the isolated tissue genomic DNA, and RNAse/DNAse-free water in a total volume of 30 μl. The level of expression was detected as an increase in fluorescence using an ABI PRISM 7700 instrument (Applied Biosystems). All sample concentrations were standardized in each reaction to exclude false-positive results. Reactions without template and/or enzyme were used as negative controls.
Data were normalized to murine tissue β-actin (TaqMan® Gene Expression Assays, mm00607939-s1; Applied Biosystems) and numerical data were determined against a standard curve established using murine bone marrow containing log-fold dilutions of human PCa cells [24].
Statistical analyses
All in vitro experiments were performed at least three times with similar results and representative assay are shown. Numerical data are expressed as mean ± standard deviation. Statistical analysis was performed by ANOVA or Student’s t-test using the GraphPad Instat statistical program (GraphPad Software, San Diego, CA) with significance at P < 0.05. For the QPCR assays, a Kruskal–Wallis test and Dunn’s multiple comparisons tests were utilized with the level of significance set at P < 0.05.
Results
Alterations of CXCL12 levels in co-cultures
CXCL12 is a critical component in the bone and organ homing cascade of PCa [6]. In the present study we explored if the production of CXCL12 by PCa cells or endothelial cells was altered in co-culture as assessed by ELISA. As reported previously, the LNCaP cell line produced the most CXCL12 in culture, followed by the LNCaP subline C4-2B (Fig. 1). PC3 cells generated the least CXCL12 among the PCa cell lines during the culture period. Human aortic vascular endothelia cells (HUVEC) and HBME produced 431 ± 35 and 478 ± 19 pg/ml/104 cells in a 48 h period. Human dermal endothelial cells (HDMEC) produced the most CXCL12 of any of the cell lines tested generating 5100 ± 541 pg/ml/104 cells in the 48 h period. Co-culture of the PCa cells with any of the endothelial cell lines resulted in less CXCL12 detected by ELISA, than either cell type alone (Fig. 1).
Co-culture of endothelial and PCa cell lines reduce CXCL12 levels. CXCL12 levels were monitored by ELISA at 48 h after the establishment of cultures of human umbilical vein, dermal or bone marrow endothelial cells (HUVEC, HDMEC or HBME, respectively) alone or in co-culture with human PCa cell lines. The data are expressed as mean ± standard deviation. * Indicates significant difference from either cell type alone at P < 0.05. The data demonstrate that all of the cell lines generate CXCL12 levels, but that together the levels are less than either cell type alone
Co-culture of PCa cells with endothelial cells results in degradation of CXCL12
One mechanism to account for the reduction in CXCL12 detected in the co-culture CM was that CXCL12 was cleaved and unable to be detected by the ELISA [14]. To determine if the reduction in CXCL12 was due to destruction of the molecule, co-culture CM was collected as before, and incubated with bCXCL12. Thereafter, the samples were separated on Tricine gels, and bCXCL12 was detected using strepavidin–HRP in conjunction with chemoluminescence. As shown in Fig. 2a, b, CM of HBME produced a small reduction in the levels bCXCL12 detected by Western blot. In the majority of the cases, PCa cell CM failed to affect bCXCL12 levels, where as co-incubation of CM derived from HBME cultured in direct contact with or separated by a porous membrane with PC3 or C4-2B cells resulted in decreased CXCL12 levels (Fig. 2a, b). Variable effects were observed when the experiment was repeated when CM from the PCa cells was collected and used to stimulate HBME. Likewise, CM collected from HBME and used to stimulate PCa cells had little effect on CXCL12 digestion. To determine if the loss of CXCL12 in co-culture was cell-type specific, co-cultures of PCa cells with human osteoblasts were established. In contrast with the PCa cell/endothelial cell cultures, co-culture of PCa cells with human osteoblasts did not result in the reduction or loss of CXCL12 observed (Fig. 2c, d).
Co-culture CM of endothelial and PCa cells cleave CXCL12. In (a) CM was collected at 48 h from cultures of HBME alone or in co-culture with human PCa cell lines in direct contact or separated in Transwell® plates (TW). Biotinylated SDF-1 was added to the CM, and was incubated further for 2.5 h at 4 or 37°C After incubation, the media were run on 20% Tricine gels and the detection of the bCXC12 was accomplished using strepavidin–HRP and ECL. (b) Quantitative densitometry of (a). The data are expressed as mean ± standard deviation of independent studies. # Indicates significant difference from either cell type alone at P < 0.01. In (c) the investigations were repeated with primary human osteoblasts. (d) Quantitative densitometry of (c). The data are expressed as mean ± standard deviation. The data demonstrates that CM from PCa/HBME cells cleaves CXCL12, whereas CM from PCa/osteoblasts does not
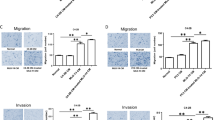
In vitro invasion assays were performed to evaluate if the changes in CXCL12 levels detected by ELISA and Western blot assays corresponds with changes in CXCL12 function. For these investigations CM from the HBME cell line was chosen for further study since these endothelial cells best represent endothelial cells that PCa must traverse in the marrow [28]. CXCL12 (200 ng/ml) stimulated more invasive activity than medium alone (Fig. 3). HBME CM alone stimulated some invasive activity but this activity was abolished when the CM was generated in the presence PC3 cells, and could not be rescued even when exogenous CXCL12 was added.
Co-culture CM of endothelial and PCa cells cleave CXCL12 rendering it inactive to support invasion by PCa. Matrigel coated invasion chambers were used to assess the ability of the presence (black bar) or absence (white bar) of CXCL12 (200 ng/ml) to support invasion of PCa cells in combination with co-culture CM. After removing the non-migrating cells, invasion was quantified by MTT assay and the data expressed as % invasion ± standard deviation with 100% set for invasion supported by RPMI alone. * P < 0.05 versus control. The data demonstrate that CXCL12 is digested by and rendered inactive to support invasion
Cysteine or serine proteases degrade CXCL12
To characterize the activity that degrades CXCL12 in co-culture CM, the previous investigations were again performed, this time in the presence of a series of protease inhibitors. bCXCL12 was then added to the CM and the reactions incubated further to determine if any of the protease inhibitors prevented the cleavage of CXCL12. AEBSF, a serine protease inhibitor known to inhibit trypsin, chymotrypsin, plasmin, kallikrein and thrombin prevented the digestion of CXCL12 by the co-culture CM (Fig. 4a, b). Likewise, calpectin (a membrane permeable inhibitor of calpain I and II and cathepsin L) and PMSF (interacts with serine residues to inhibit trypsin, chymotrypsin, thrombin and papain) prevented CXCL12 degradation (Fig. 4a, b). EST, a membrane-permeable thiolprotease inhibitor, did not prevent CXCL12 degradation, nor did pepstatin, EDTA and the elastase-like serine protease elastatinal (not shown) (Fig. 4a, b). Protein fractionation using molecular weight cut-off spin columns were used to determine the size of the activity. Here the CM was fractionated and normalized to protein content prior to the addition of bCXCL12. As shown in Fig. 4c, degradation of bCXCL12 resulted from CM fractions where the size of the protein is greater than 50 kD.
Cleavage of CXCL12 by co-culture CM of endothelial and PCa cells is dependent on serine/cysteine proteases. In (a) CM was collected at 48 h from cultures of HBME in co-culture with PC3 cells. Where indicated protease inhibitors were added the CM for 30 min at 4°C, prior to the addition of bCXCL12. After 2.5 h incubation at 37°C, the media were run on Tricine gels and the detection of the bCXCL12 was performed using strepavidin–HRP and ECL. (b) Quantitative densitometry of (a). The data are expressed as mean ± standard deviation. # Indicates significant difference from control at P < 0.01. In (c), the CM was fractionated by using molecular weight cut-off spin columns. After protein normalization, bCXCL12 was added, incubated, and detected by Western blot. In (d) matrigel coated invasion chambers were used in conjunction with protease inhibitors in the absence (white bar) or presence (black bar) of 200 ng/ml CXCL12. After removing the non-migrating cells, invasion was quantified by MTT assay and the data expressed as % invasion ± standard deviation with 100% set for invasion supported by RPMI alone. * P < 0.05 versus control. The data demonstrate that the co-culture CM activity responsible cleavage of CXCL12 is a serine or cysteine protease which is >50 kD
To verify the inhibitor studies, functional invasion assays were performed. Both calpectin and EST were able to maintain the activity of CXCL12 in the invasion assay, despite reducing the overall invasive activities (Fig. 4d). AEBSF, while it was able to inhibit CXCL12 degradation in the western blots, was not compatible with the invasion of the PCa cells (Fig. 4a, b, d). Pepstatin, elastatinal (Fig. 4c) and EDTA (not shown) were inactive. Based upon these results, the activity generated in PCa cell/HBME co-culture CM that degrades CXCL12 appears to be either a cysteine or a serine protease.
CD26/DPPIV degrades CXCL12 in the co-culture CM
Recently it was reported that CD26, a 110-kD cell surface glycoprotein, also known as DPPIV is capable of cleaving CXCL12 and cleaving amino-terminal dipeptides with either l-proline or l-alanine at the penultimate position. CD26 exists in both soluble and membrane-expressed forms. Soluble forms of CD26 have been identified in cell cultures and in human serum [29], although CD26 may be more active when expressed as an ectoenzyme at high concentrations on endothelial cells, hepatocytes, kidney brush border membranes, and leukocytes [29]. To determine if CD26/DPPIV plays a role in PCa extravasation through cleavage of CXCL12, our studies were repeated in the presence or absence of the CD26/DPPIV and an specific inhibitor of the enzyme, diprotin A [22]. CD26/DPPIV alone or in the presence of CM was able to completely digest CXCL12 (Fig. 5a, b). Addition of diprotin A was able to prevent CXCL12 degradation in a dose-dependent manner (Fig. 5a, b). Functional assays were used to confirm these results. As before, CXCL12 stimulated invasion, but this activity was abrogated when added to co-culture CM of HBME and PC3 cells (Fig. 5c). Addition of diprotin A to the CM with or without additional CXCL12 increased the invasive activity.
Inhibition of CD26/DPPIV activity by diprotin A prevents cleavage of CXCL12 by co-culture CM of endothelial and PCa. In (a) CM was collected at 48 h from cultures of HBME in co-culture with PC3 cells. Where indicated or rhCD26/DPPIV were added the CM for 30 min at 4°C, prior to the addition of bCXCL12. After 2.5 h incubation at 37°C, the media were run on Tricine gels and the detection of the bCXCL12 was accomplished using strepavidin–HRP and ECL. (b) Quantitative densitometry of (a). The data are expressed as mean ± standard deviation. * Indicates significant difference at P < 0.05. In (c) matrigel coated invasion chambers were used in conjunction with diprotin A (2.5 mM) in the presence or absence of 200 ng/ml CXCL12. After removing the non-migrating cells, invasion was quantified by MTT assay and the data expressed as % invasion ± standard deviation with 100% set for invasion supported by RPMI alone. * P < 0.05 versus control. The data demonstrate that CD26/DPPIV activity was responsible the cleavage of CXCL12
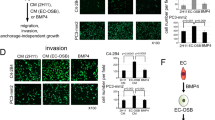
To verify that CD26/DPPIV levels increase when endothelial and PCa cells are cultured together, CM was evaluated by ELISA for the soluble protein, and immunohistochemistry was performed to detect the cell-associated protein. At 48 h of culture, CD26/DPPIV levels were below the level of detection of the ELISA for any cell type when cultured alone. In co-cultures the levels of CD26/DPPIV rose by 6 h and continued to rise as long as the investigation was performed (Fig. 6a). Cell associated CD26/DPPIV levels were also observed in the HBME cells and PC3 cells as detected by immunohistochemistry (Fig. 6b, c). These data suggest that CD26/DPPIV may be a regulator of the CXCL12/CXCR4 chemokine axis in PCa extravasation and possibly metastasis.
Co-culture of PCa and endothelial cells increases CD26/DPPIV expression. Cultures were established at a 1:1 ratio of HBME in co-culture with PC3, LNCaP and C4-2B cells. In (a) CM was collected over a 48 h period and assayed for secreted CD26/DPPIV protein by ELISA. The data is expressed as mean ± standard deviation for quadruplicate determinations. * Indicates significant difference from either cell type alone at P < 0.05. In (b) immunohistochemistry for CD26/DPPIV was performed on HBME in co-culture with PC3 cells at 0 and 48 h using monoclonal antibodies or immunoglobin controls. The data demonstrate that CD26/DPPIV is increasingly expressed in co-culture. (c) Quantitative digital image analyses of (b). The data are expressed as mean ± standard deviation. * Indicates significant difference at P < 0.05. The data suggest that co-cultures of PCa/HBME increases CD26/DPPIV expression
Inhibition of CD26/DPPIV alters metastasis in vivo
To directly determine if CD26/DPPIV is involved in PCa metastasis, an in vivo PCa metastasis assay that was recently developed by our group was utilized [24]. In this model, primary tumors are established subcutaneously (s.c.) in immune deficient mice, and over time, cells shed from the primary tumor are capable of generating metastatic lesions. Twenty-four hours after establishing the primary s.c. tumors, one group of animals were treated twice daily with the CD26/DPPIV inhibitor, diprotin A. A second group of animals were treated with vehicle only. Over the 3 week course of the study, no palpable or measurable differences were noted in the size of the s.c. tumor in the diprotin A treated group compared to controls using calipers (data not shown).
Next, the levels of PCa cells recovered from a number of tissues were evaluated by QPCR at 3 weeks.
Diprotin A treatments produced variable levels of tumor cells in each of the tissues (Fig. 7a, b). Most notably, diprotin A reduced the number of PC3 cells were found in the peripheral blood and primary tumor (sponge) (Fig. 7a). Increasing number of PCa cells were found in each of the tissues, especially in the osseous tissues (e.g. mandible, humerus, tibia, pelvis) in the diprotin A treatment group (Fig. 7b). Together, these findings suggest that the inhibition of CD26/DPPIV facilitates PCa extravasation into the marrow and metastasis through CXCL12/CXCR4 chemokine axis in vivo.
Modulation of tumor dissemination by daily administration of CD26/DPPIV inhibitor. Subcutaneous tumors were established in SCID mice using PC3 cells. Mice were injected subcutaneously with diprotin A (CD26/DPPIV inhibitor) at 5 μmol twice a day or with the vehicle (acidified saline), 7 days/week for 3 weeks (n = 3 per group). (a) The levels of PC3 cells recovered from a number of tissues and (b) from peripheral blood and sponge were evaluated by QPCR at 3 weeks. Data are presented as mean ± standard error of mean using a Krusal–Wallis test and Dunn’s multiple comparisons tests with the level of significance set at P < 0.05
Discussion
In this study, we explored whether the local degradation of CXCL12 at the blood vessel lumen facilitates PCa cell entry into the marrow cavity. Initially, we found that the CXCL12 levels in CM from co-culture of endothelial cell and PCa cells were lower than the levels generated by either endothelial cells or PCa cells alone. Yet, degradation of CXCL12 did not occur in co-culture of PCa cells with human osteoblasts—major sources of the protein in marrow [30, 31]. Western blot analysis confirmed that proteolytic degradation of CXCL12 occurred in the co-culture CM. Inhibitor and size fractionation studies demonstrated that the activity was primarily a serine or cysteine protease with an MW of greater than 50 kD. Although AEBSF was able to inhibit CXCL12 degradation in the western blots, it was not compatible with the invasion of the PCa cells (Fig. 4a, c). The reason for this is not clear, but is probably not due to cell toxicity, which was also the case for PMSF, and therefore prevented further evaluation of these compounds (data not shown). Based upon the available data, we explored if CD26/DPPIV was responsible for the degradation of CXCL12. Using a specific inhibitor of CD26/DPPIV, we determined that CXCL12 in the co-culture CM was most likely degraded by CD26/DPPIV. In vitro invasion assays further confirmed that CD26/DPPIV is involved in PCa invasion, and that the level of the protein increased in co-cultures. We also evaluated the metastatic effect of the CD26/DPPIV inhibitor by using in vivo PCa metastasis mouse model. Inhibition of CD26/DPPIV either had no effect, or increased the number of metastatic cells in the bones that were evaluated. This suggests that functionally a gradient could be established in marrow based upon selective degradation of CXCL12 by PCa/endothelial cells but not by PCa/osteoblastic cells to guide PCa cells to endosteal niches (Fig. 8).
Model of CD26/DPPIV action in PCa metastasis. As a neoplasm progresses towards malignancy primary tumor (1° tumor) begin to express CD26/DPPIV to facilitate intravasation into the blood stream. Upon entering the marrow where local levels of CXCL12 are higher than in the circulation, activation of a number of cell surface adhesive receptors occurs. In order for the cells to egress from the luminal side of the vessel, CXCL12 is both actively transported across the vascular endothelium [15] and/or degraded by enhanced expression of CD26/DPPIV following PCa/endothelial interactions. With endosteal osteoblasts expressing high levels of CXCL12, the PCa cells thereby follow the local gradient towards the endosteal surfaces. PCa cells are kept in the extravascular marrow space(s) of the endosteal environment since CD26/DPPIV levels remain low. The molecular events that regulate PCa/endothelial expression of CD26/DPPIV remain to be determined
CD26/DPPIV is a serine-type exopeptidase that is secreted by the prostate and increased in PCa [32–34]. Yet its role in PCa disease is poorly understood. In the present study, LNCaP cells were the least able to cleave bCXCL12 suggesting that co-culture of the bone homing PCa with bone marrow endothelium results in degradation of CXCL12 (C4-2B, PC3), whereas little degradation was observed with the non-bone homing cell line (LNCaP). Phenotyping studies have shown that the LNCaP derivative cell lines are very dissimilar—early all express CD26/DPPIV (+), but only approximately 10% of LNCaP cells are CD26/DPPIV (−) suggesting that the more metastatic sublines probably arose from CD26/DPPIV (−) LNCaP cells [35]. Moreover, plasminogen interaction with CD26/DPPIV initiates a signal transduction mechanism which regulates expression of matrix metalloproteinase-9 by PCa cells which is probably involved in invasion [36]. However, CD26/DPPIV is also known to regulate the stability of mitogenic peptides and bFGF intracellular signaling such that increased expression of CD26/DPPIV in PCa is associated with the induction of apoptosis, cell cycle arrest, inhibition of in vitro cell migration, and invasion [37]. In fact, siRNA silencing of CD26/DPPIV results in increased bFGF levels and restoration of mitogen-activated protein kinase (MAPK)-extracellular signal-regulated kinase (ERK) 1/2 activation suggesting that CD26/DPPIV inhibits the malignant phenotype of PCa cells by blocking bFGF signaling pathway [37]. Thus tight control of CD26/DPPIV would appear to be a critical for tumor and metastatic survival.
Proteolytic degradation of CXCL12 in the bone marrow is known to have a central role critical in regulating stem cell and progenitor mobilization into the peripheral circulation [16, 38, 39]. CXCL12 is known to be inactivated by cleavage of metalloproteinases, leukocyte elastase, serine proteases and CD26/DPPIV [14, 17–19, 40, 41]. When exposed to serum, CXCL12 is rapidly altered to be unable to bind CXCR4. Conceptually, the degradation of CXCL12 at endothelial surfaces once PCa are bound to them is an attractive model to facilitate egress out of the vasculature only if there is a constant source of CXCL12 originating at a site distant to where it is locally cleaved. In fact, this appears to be the case as osteoblasts are rich sources of the protein and together with PCa does not generate additional degradation. This model also would in part explain how PCa are retained within the marrow.
It is likely that the stability of CXCL12 plays a role in regulating PCa cell metastasis. We have demonstrated that CXCL12 stimulates an increase in the expression of CD164 and activated αvβ3 receptors in two lines of metastatic PCa, PC3 and LNCaP C4-2B, but does not affect αvβ3 receptor expression in non-metastatic LNCaP cells [10, 11]. This in turn enhances their adhesion and invasion to extracellular matrix by PCa cells in vitro. Therefore that PCa in conjunction with HUVEC, HDMEC and HMBE endothelial cells cleave CXCL12 suggests that this mechanism alone does not regulate the localization of PCa to the marrow. In keeping with this notion, are findings that PCa adhere preferentially to human bone marrow endothelial (HBME) cells versus other types of vascular endothelial cells [26]. However, tumor cell migration and invasion depends largely on an enzymatic cascade of proteolysis. Interestingly, diprotin A reduced the number of PC3 cells were found in the peripheral blood and primary tumor (sponge) (Fig. 7a), suggesting inhibition of CD26/DPPIV facilitates transport of PCa cells from the circulation into peripheral tissues. Given the ability of CD26/DPPIV to regulate the bioavailability of CXCL12, which is known to regulate the PCa cell metastasis, proliferation, and cell motility through extracellular matrices, these findings add a more complete comprehension of PCa progression.
Abbreviations
- SDF-1 or CXCL12:
-
Stromal derived factor-1
- PCa:
-
Prostate cancer
- DPPIV:
-
Dipeptidyl peptidase IV
- HSC:
-
Hematopoietic stem cells
- GAG:
-
Glycosaminoglycan
- G-CSF:
-
Granulocyte colony-stimulating factor
- HBME:
-
Human bone marrow endothelial cells
- FBS:
-
Fetal bovine serum
- HUVEC:
-
Human umbilical vein endothelial cells
- HDMEC:
-
Human dermal microvascular endothelial cells
- CM:
-
Conditioned medium
- ELISA:
-
Enzyme-linked immunosorbent assay
- bCXCL12:
-
Biotinylated CXCL12
- HRP:
-
Horseradish peroxidase
- ECL:
-
Enhanced chemiluminescent
- NIH:
-
National Institutes of Health
- MTT:
-
3-(4,5-Dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide
- SCID:
-
Severe combined immunodeficiency
- QPCR:
-
Real-time polymerase chain reaction
- MAPK:
-
Mitogen-activated protein kinase
- ERK:
-
Extracellular signal-regulated kinase
References
Nicolson GL, Custead SE (1982) Tumor metastasis is not due to adaptation of cells to a new organ environment. Science 215(4529):176–178. doi:10.1126/science.7053568
Ruoslahti E, Rajotte D (2000) An address system in the vasculature of normal tissues and tumors. Annu Rev Immunol 18:813–827. doi:10.1146/annurev.immunol.18.1.813
Taichman DB, Cybulsky MI, Djaffar I et al (1991) Tumor cell surface alpha 4 beta 1 integrin mediates adhesion to vascular endothelium: demonstration of an interaction with the N-terminal domains of INCAM-110/VCAM-1. Cell Regul 2(5):347–355
Parsonage G, Filer AD, Haworth O et al (2005) A stromal address code defined by fibroblasts. Trends Immunol 26(3):150–156. doi:10.1016/j.it.2004.11.014
Taichman RS, Cooper C, Keller ET et al (2002) Use of the stromal cell-derived factor-1/CXCR4 pathway in prostate cancer metastasis to bone. Cancer Res 62(6):1832–1837
Sun YX, Wang J, Shelburne CE et al (2003) Expression of CXCR4 and CXCL12 (SDF-1) in human prostate cancers (PCa) in vivo. J Cell Biochem 89(3):462–473. doi:10.1002/jcb.10522
Sun YX, Schneider A, Jung Y et al (2005) Skeletal localization and neutralization of the SDF-1(CXCL12)/CXCR4 axis blocks prostate cancer metastasis and growth in osseous sites in vivo. J Bone Miner Res 20(2):318–329. doi:10.1359/JBMR.041109
Wang J, Sun Y, Song W et al (2005) Diverse signaling pathways through the SDF-1/CXCR4 chemokine axis in prostate cancer cell lines leads to altered patterns of cytokine secretion and angiogenesis. Cell Signal 17(12):1578–1592. doi:10.1016/j.cellsig.2005.03.022
Wang J, Shiozawa Y, Wang Y et al (2008) The role of CXCR7/RDC1 as a chemokine receptor for CXCL12/SDF-1 in prostate cancer. J Biol Chem 283(7):4283–4294. doi:10.1074/jbc.M707465200
Sun YX, Fang M, Wang J et al (2007) Expression and activation of alpha v beta 3 integrins by SDF-1/CXC12 increases the aggressiveness of prostate cancer cells. Prostate 67(1):61–73. doi:10.1002/pros.20500
Havens AM, Jung Y, Sun YX et al (2006) The role of sialomucin CD164 (MGC-24v or endolyn) in prostate cancer metastasis. BMC Cancer 6:195. doi:10.1186/1471-2407-6-195
Jung Y, Wang J, Song J et al (2007) Annexin II expressed by osteoblasts and endothelial cells regulates stem cell adhesion, homing, and engraftment following transplantation. Blood 110(1):82–90. doi:10.1182/blood-2006-05-021352
Shiozawa Y, Havens AM, Jung Y et al (2008) Annexin II/Annexin II receptor axis regulates adhesion, migration, homing, and growth of prostate cancer. J Cell Biochem (in press)
McQuibban GA, Butler GS, Gong JH et al (2001) Matrix metalloproteinase activity inactivates the CXC chemokine stromal cell-derived factor-1. J Biol Chem 276(47):43503–43508. doi:10.1074/jbc.M107736200
Dar A, Goichberg P, Shinder V et al (2005) Chemokine receptor CXCR4-dependent internalization and resecretion of functional chemokine SDF-1 by bone marrow endothelial and stromal cells. Nat Immunol 6(10):1038–1046. doi:10.1038/ni1251
Petit I, Szyper-Kravitz M, Nagler A et al (2002) G-CSF induces stem cell mobilization by decreasing bone marrow SDF-1 and up-regulating CXCR4. Nat Immunol 3(7):687–694. doi:10.1038/ni813
Lambeir AM, Proost P, Durinx C et al (2001) Kinetic investigation of chemokine truncation by CD26/dipeptidyl peptidase IV reveals a striking selectivity within the chemokine family. J Biol Chem 276(32):29839–29845. doi:10.1074/jbc.M103106200
De La Luz Sierra M, Yang F, Narazaki M et al (2004) Differential processing of stromal-derived factor-1alpha and stromal-derived factor-1beta explains functional diversity. Blood 103(7):2452–2459. doi:10.1182/blood-2003-08-2857
Delgado MB, Clark-Lewis I, Loetscher P et al (2001) Rapid inactivation of stromal cell-derived factor-1 by cathepsin G associated with lymphocytes. Eur J Immunol 31(3), 699–707. doi:10.1002/1521-4141(200103)31:3≤699::AID-IMMU699≥3.0.CO;2-6
Christopherson KW 2nd, Cooper S, Broxmeyer HE (2003) Cell surface peptidase CD26/DPPIV mediates G-CSF mobilization of mouse progenitor cells. Blood 101(12):4680–4686. doi:10.1182/blood-2002-12-3893
Christopherson KW, Cooper S, Hangoc G et al (2003) CD26 is essential for normal G-CSF-induced progenitor cell mobilization as determined by CD26−/− mice. Exp Hematol 31(11):1126–1134
Christopherson KWII, Hangoc G, Mantel CR et al (2004) Modulation of hematopoietic stem cell homing and engraftment by CD26. Science 305(5686):1000–1003. doi:10.1126/science.1097071
Pro B, Dang NH (2004) CD26/dipeptidyl peptidase IV and its role in cancer. Histol Histopathol 19(4):1345–1351
Havens A, Pedersen E, Shiozawa Y et al (2008) An in vivo mouse model for human prostate cancer metastasis. Neoplasia 10(4):371–380
Wu TT, Sikes RA, Cui Q et al (1998) Establishing human prostate cancer cell xenografts in bone: induction of osteoblastic reaction by prostate-specific antigen-producing tumors in athymic and SCID/bg mice using LNCaP and lineage-derived metastatic sublines. Int J Cancer 77(6):887–894. doi :10.1002/(SICI)1097-0215(19980911)77:6≤887::AID-IJC15≥3.0.CO;2-Z
Lehr JE, Pienta KJ (1998) Preferential adhesion of prostate cancer cells to a human bone marrow endothelial cell line. J Natl Cancer Inst 90(2):118–123. doi:10.1093/jnci/90.2.118
Taichman RS, Emerson SG (1994) Human osteoblasts support hematopoiesis through the production of granulocyte colony-stimulating factor. J Exp Med 179(5):1677–1682. doi:10.1084/jem.179.5.1677
Cooper CR, Chay CH, Gendernalik JD et al (2003) Stromal factors involved in prostate carcinoma metastasis to bone. Cancer 97(3, Suppl):739–747. doi:10.1002/cncr.11181
Oravecz T, Pall M, Roderiquez G et al (1997) Regulation of the receptor specificity and function of the chemokine RANTES (regulated on activation, normal T cell expressed and secreted) by dipeptidyl peptidase IV (CD26)-mediated cleavage. J Exp Med 186(11):1865–1872. doi:10.1084/jem.186.11.1865
Ponomaryov T, Peled A, Petit I et al (2000) Induction of the chemokine stromal-derived factor-1 following DNA damage improves human stem cell function. J Clin Invest 106(11):1331–1339. doi:10.1172/JCI10329
Taichman RS (2005) Blood and bone: two tissues whose fates are intertwined to create the hematopoietic stem-cell niche. Blood 105(7):2631–2639. doi:10.1182/blood-2004-06-2480
Wilson MJ, Ruhland AR, Quast BJ et al (2000) Dipeptidylpeptidase IV activities are elevated in prostate cancers and adjacent benign hyperplastic glands. J Androl 21(2):220–226
Bogenrieder T, Finstad CL, Freeman RH, et al (1997) Expression and localization of aminopeptidase A, aminopeptidase N, and dipeptidyl peptidase IV in benign and malignant human prostate tissue. Prostate 33(4):225-232. doi :10.1002/(SICI)1097-0045(19971201)33:4≤225::AID-PROS1≥3.0.CO;2-G
Wilson MJ, Haller R, Li SY et al (2005) Elevation of dipeptidylpeptidase iv activities in the prostate peripheral zone and prostatic secretions of men with prostate cancer: possible prostate cancer disease marker. J Urol 174(3):1124–1128. doi:10.1097/01.ju.0000168621.84017.5c
Liu AY, Brubaker KD, Goo YA et al (2004) Lineage relationship between LNCaP and LNCaP-derived prostate cancer cell lines. Prostate 60(2):98–108. doi:10.1002/pros.20031
Gonzalez-Gronow M, Grenett HE, Weber MR et al (2001) Interaction of plasminogen with dipeptidyl peptidase IV initiates a signal transduction mechanism which regulates expression of matrix metalloproteinase-9 by prostate cancer cells. Biochem J 355(Pt 2):397–407. doi:10.1042/0264-6021:3550397
Wesley UV, McGroarty M, Homoyouni A (2005) Dipeptidyl peptidase inhibits malignant phenotype of prostate cancer cells by blocking basic fibroblast growth factor signaling pathway. Cancer Res 65(4):1325–1334. doi:10.1158/0008-5472.CAN-04-1852
Levesque JP, Hendy J, Takamatsu Y et al (2003) Disruption of the CXCR4/CXCL12 chemotactic interaction during hematopoietic stem cell mobilization induced by GCSF or cyclophosphamide. J Clin Invest 111(2):187–196
Pelus LM, Bian H, King AG et al (2004) Neutrophil-derived MMP-9 mediates synergistic mobilization of hematopoietic stem and progenitor cells by the combination of G-CSF and the chemokines GRObeta/CXCL2 and GRObetaT/CXCL2delta4. Blood 103(1):110–119. doi:10.1182/blood-2003-04-1115
Villalba S, Salvucci O, Aoki Y et al (2003) Serum inactivation contributes to the failure of stromal-derived factor-1 to block HIV-I infection in vivo. J Leukoc Biol 74(5):880–888. doi:10.1189/jlb.0403149
Valenzuela-Fernandez A, Planchenault T, Baleux F et al (2002) Leukocyte elastase negatively regulates stromal cell-derived factor-1 (SDF-1)/CXCR4 binding and functions by amino-terminal processing of SDF-1 and CXCR4. J Biol Chem 277(18):15677–15689. doi:10.1074/jbc.M111388200
Acknowledgments
This work was directly supported by the Charles Eliot Ware Memorial Fellowship (AM. Havens), Pediatric Oncology Research Fellowship (Y. Shiozawa), CA93900 (K.J. Pienta and R.S. Taichman), the Department of Defense PC060857 and PC073952 (R.S. Taichman), P50 CA69568 (K.J. Pienta), U19 CA113317 (K.J. Pienta), and 2006 and 2007 awards from the Prostate Cancer Foundation (R.S. Taichman and K.J. Pienta). K.J. Pienta receives support as an American Cancer Society Clinical Research Professor. These investigations were also supported in part by the Tissue Procurement Core of the University of Michigan Comprehensive Cancer Center, Grant #CA46952.
Author information
Authors and Affiliations
Corresponding author
Additional information
Yan-Xi Sun and Elisabeth A. Pedersen contributed equally to this work.
Rights and permissions
About this article
Cite this article
Sun, YX., Pedersen, E.A., Shiozawa, Y. et al. CD26/dipeptidyl peptidase IV regulates prostate cancer metastasis by degrading SDF-1/CXCL12. Clin Exp Metastasis 25, 765–776 (2008). https://doi.org/10.1007/s10585-008-9188-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10585-008-9188-9