Abstract
Background
Mucopolysaccharidosis type IIIB (MPS IIIB) is a rare genetic disorder in which the deficiency of the lysosomal enzyme N-acetyl-α-glucosaminidase (NAGLU) results in the accumulation of heparan sulfate (HS), leading to progressive neurocognitive deterioration. In MPS IIIB a wide spectrum of disease severity is seen. Due to a large allelic heterogeneity, establishing genotype-phenotype correlations is difficult. However, reliable prediction of the natural course of the disease is needed, in particular for the assessment of the efficacy of potential therapies.
Methods
To identify markers that correlate with disease severity, all Dutch patients diagnosed with MPS IIIB were characterised as either rapid (RP; classical, severe phenotype) or slow progressors (SP; non-classical, less severe phenotype), based on clinical data. NAGLU activity and HS levels were measured in patients’ fibroblasts after culturing at different temperatures.
Results
A small, though significant difference in NAGLU activity was measured between RP and SP patients after culturing at 37 °C (p < 0.01). Culturing at 30 °C resulted in more pronounced and significantly higher NAGLU activity levels in SP patients (p < 0.001) with a NAGLU activity of 0.58 nmol.mg-1.hr-1 calculated to be the optimal cut-off value to distinguish between the groups (sensitivity and specificity 100 %). A lower capacity of patients’ fibroblasts to increase NAGLU activity at 30 °C could significantly predict for the loss of several disease specific functions.
Conclusion
NAGLU activity in fibroblasts cultured at 30 °C can be used to discriminate between RP and SP MPS IIIB patients and the capacity of cells to increase NAGLU activity at lower temperatures correlates with disease symptoms.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Mucopolysaccharidosis type III (MPS III or Sanfilippo disease) is a rare autosomal recessive lysosomal storage disorder in which the deficiency of one of four enzymes involved in the degradation of heparan sulfate (HS) leads to the accumulation of this specific glycosaminoglycan (GAG) (Muenzer 2011). The reported birth incidence for MPS III ranges from 1.52 to 1.89 per 100,000 newborns (Poorthuis et al 1999; Baehner et al 2005). Based on the deficient enzyme, four different MPS III subtypes are distinguished referred to as MPS IIIA (OMIM #252900), B (OMIM #252920), C (OMIM #252930) and D (OMIM #252940) (Muenzer 2011). Clinically these subtypes are indistinguishable.
The clinical course of the disease is generally divided into three stages. After a symptom-free interval, patients normally present between the age of 1 and 4 years with a delay in cognitive development, especially in the development of speech and language skills. The second phase of the disease starts at the age of 3 to 4 years and is marked by a progressive intellectual decline which is accompanied by behavioral and sleeping problems. Eventually, the third phase sets in, characterized by the regression of motor functions. Patients lose the ability to walk independently, become wheelchair bound and fully care dependent. Patients with this rapidly progressing classical phenotype (rapid progressors, RP) usually die at the end of the second or in the beginning of the third decade of life (Valstar et al 2008). However, in recent years it has been recognized that MPS III is characterized by a much broader spectrum of disease progression and severity. Survival well into adulthood has been reported and patients may show a stable developmental impairment for many years (Moog et al 2007; Valstar et al 2010a, b). In the Netherlands, most patients with MPS IIIB display this slowly progressing attenuated phenotype (slow progressors, SP) (Valstar et al 2010a).
MPS IIIB is caused by a deficiency of the enzyme N-acetyl-α-glucosaminidase (EC 3.2.1.50) which is responsible for the hydrolysis of the α, 1 → 4 linkage between N-acetylglucosamine and the adjacent glucuronic or iduronic acid residue (Esko et al 2009). The gene encoding for NAGLU is localized on chromosome 17q21.1 (Zhao et al 1996) and over 100 mutations in the NAGLU gene (HGNC: 7632) have been identified (van de Kamp et al 1976; Beesley et al 1998, 2004, 2005; Schmidtchen et al 1998; Zhao et al 1998; Bunge et al 1999; Weber et al 1999; Esposito et al 2000; Tessitore et al 2000; Emre et al 2002; Chinen et al 2005; Champion et al 2010; Valstar et al 2010a; Ouesleti et al 2011; Selmer et al 2012; Tang et al 2013). Due to this large allelic heterogeneity, establishing a genotype-phenotype correlation is difficult.
Although there is no disease modifying treatment available for MPS IIIB, several promising therapies are currently under investigation. A trial on intravenous enzyme replacement therapy (ERT) has recently been initiated (clinicaltrials.gov identifier: NCT02324049) and a study on intrathecal ERT is in a preclinical phase for MPS IIIB (http://www.bmrn.com/pipeline/index.php). The latter approach is already in a phase 2b study for MPS IIIA (clinicaltrials.gov identifiers: NCT01299727 and NCT02060526). Intracerebral gene therapy has been developed for MPS IIIB and is now in a phase 1/2 study (ISRCTN identifier: ISRCTN19853672). Furthermore, the efficacy of high dose oral genistein, which reduces the accumulation of HS in MPS III mice (Malinowska et al 2009, 2010) is being investigated in patients with all MPS III subtypes (EudraCT number: 2013-001479-18).
In order to properly target a disease modifying therapy, and to allow accurate evaluation of potential clinical benefits, it is essential to reliably predict the natural course of the disease for each individual patient at an early stage. We therefore aimed to identify markers that correlate with disease severity in MPS IIIB patients. We analyzed NAGLU activity and levels of stored HS in fibroblasts of MPS IIIB patients after culturing cells at different temperatures and correlated this to their clinical phenotype.
Material and methods
Patients
All Dutch patients diagnosed with MPS IIIB of whom cultured skin fibroblasts were available and essential clinical data could be retrieved from medical records, were included in this study. Data was collected on survival and the age at which the ability to speak (defined as: to verbally communicate intentionally with meaningful words) and to walk (defined as: to walk independently without any assistance) was lost. Based on the essential clinical data set, patients were divided into two groups by a clinician experienced in the diagnosis and treatment of lysosomal storage disorders, including MPS IIIB (FAW). The rapid progressor group (RP) consisted of patients with a classical, severe form of the disease and the slow progressor group (SP) of patients with a non-classical, less severe phenotype.
Informed consent for the use of patient data and fibroblasts was obtained from parents or legal representatives for all patients. This study was submitted to the Medical Ethical Review Board of the Academic Medical Center in Amsterdam who declared that ethical approval was not necessary because of the observational nature of the study.
Mutation analysis
Mutation analysis had been performed in most patients within the scope of the diagnostic workup. If not, mutation analysis of the NAGLU gene was performed in fibroblasts by standard Sanger sequencing methods. Mutation nomenclature is according the HGVS (http://www.hgvs.org/mutnomen/). Sequence reference for the NAGLU gene is NM 000263.3.
Cell culture
Fibroblast cell lines were tested for mycoplasma contamination and were subsequently cultured in Dulbecco’s Modified Eagle's Medium supplemented with 10 % inactivated Fetal Bovine Serum (FBS) and 100 U/mL penicillin, 100 μg/mL streptomycin, and 250 μg/mL amphotericin in a humidified atmosphere containing 5 % CO2. To remove bovine NAGLU in the FBS, NAGLU was inactivated by incubation of FBS at 65 °C for 35 minutes.
Fibroblasts were plated at 70 % confluence and cultured at a temperature of either 37 °C or 30 °C for 7 days. After a week the medium was removed and cell layers were washed twice with phosphate buffered saline (PBS). After harvesting, cell pellets were washed once with PBS and twice with 0.9 % NaCl and stored at −20 °C until further analysis.
Enzymatic activity of NAGLU in fibroblasts
NAGLU activity in fibroblasts was measured using the fluorogenic substrate 4-methylumbelliferyl-2-acetamido-2-deoxy-α-D-glucopyranoside (4MU-α-GlcNAc) (Moscerdam, Oegstgeest, The Netherlands) using a modified version of the method described by Marsh and Fensom (Marsh and Fensom 1985). The 4MU-α-GlcNAc substrate was dissolved to a concentration of 6 mg/mL in 0.1 M citrate 0.2 M phosphate buffer pH 4.3. Cell pellets were resuspended in milliQ (Synergy® Water Purification System, Millipore, Billerica, MA, USA) supplemented with one cOmplete™ protease inhibitor cocktail tablet per 10 mL milliQ (Roche, Mannheim, Germany). Cells were disrupted by sonification uing a Vibra Cell sonicator (Sonics & Materials Inc., Newtown, CT, USA). Subsequently, protein concentration was measured in whole cell lysates as described by Lowry et al (Lowry et al 1951). For the determination of NAGLU activity, cell lysates were diluted to a concentration of 1 mg/mL and 30 μL of cell lysate was added to 15 μL 4MU-α-GlcNAc solution and 15 μL of a 0.1 M citrate 0.2 M phosphate buffer with pH 3.85. After 4 hours incubation at 37 °C, the reaction was stopped with 1440 μL 0.2 M sodium carbonate 0.5 M glycine buffer, pH 10.5. Released 4-methylumbelliferone was measured fluorometrically with an excitation wavelength of 360 nm and emission wavelength of 450 nm using a Perkin Elmer LS45 fluorescence spectrometer (Perkin Elmer, Waltham, MA, USA). NAGLU activity in each sample was calculated using a calibration curve of 4-methylumbelliferone (Glycosynth Ltd., Warrington, Cheshire, UK). All enzyme activity assays were performed in duplicate and repeated at least once in independent fibroblast cultures.
HS analysis in fibroblasts
HS levels were determined as described previously (Kingma et al 2013). HS in 25 μg of fibroblast lysate was enzymatically digested into disaccharides. As a final deproteination step samples were loaded on an Amicon Ultra 10 kD centrifugal filter (EMD Millipore, Billerica, MA, USA) and centrifuged at 14,000 g for 30 minutes at a temperature of 25 °C.
Statistical analysis
All data analyses were performed using SPSS software for Windows (version 21.0, SPSS Inc., Chicago, IL, USA). Non-parametric statistical tests were used to analyze the relationship between MPS IIIB phenotype and NAGLU activity levels after cell culturing at 37 °C and 30 °C and the NAGLU activity ratio after culturing at 30 °C over the activity after culturing at 37 °C, respectively. Linear regression was performed to determine the correlation between the ratio of NAGLU activity after cell culturing at 30 °C over 37 °C and clinical signs of disease progression. Cut-off values of NAGLU activity that could discriminate between MPS III phenotypes, were identified using receiver operating characteristic (ROC) curve analysis. True positive rates (sensitivity) were plotted against false positive rates (1-specificity) for all classification points and p-values were calculated for the area under the curve. A p-value of < 0.05 was considered statistically significant.
Results
Patients
Twenty-eight patients from 17 different families were included in this study (Table 1). Six patients were classified as RP patients and 22 as SP patients. At the time of this study 15 out of 28 patients were still alive. In the RP patients death occurred at a younger age than in the SP patients (median age 14 years, range 13–20 years vs. median age 51 years, range 28–69 years, respectively. p < 0.001). RP patients lost their ability to communicate in a meaningful way at a median age of 6 years (range 5–10 years). In patients with the SP phenotype this was 24 years (range 8–69 years) (p < 0.001). The median age at loss of the ability to walk independently was 14 years (range 8–18 years) in RP patients and 50 years (range 18–68 years) in the SP patients (p < 0.001).
Mutations
For all patients mutations are presented in Table 1. All mutations in our cohort have been reported previously, except the missense mutation c.509G > A; p.(Gly170Asp) found in patient 15 (Zhao et al 1996; Beesley et al 1998; Schmidtchen et al 1998; Weber et al 1999; Valstar et al 2010a).
NAGLU activity in fibroblasts after culturing at 37 °C and 30 °C
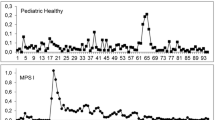
To investigate whether residual enzyme activity in cultured skin fibroblasts differentiates between RP and SP patients, NAGLU activity in fibroblasts was measured. In Fig. 1a, NAGLU activity levels in fibroblasts of all individual MPS IIIB patients are depicted after culturing at 37 °C and 30 °C. Very low levels of NAGLU activity were observed for all patients after culturing at 37 °C. Under these conditions fibroblasts from RP patients showed a median enzymatic activity of 0.17 nmol.mg−1.hr−1 (range 0.14-0.23 nmol.mg−1.hr−1) compared to a median enzymatic activity of 0.27 nmol.mg−1.hr−1 (range 0.16-3.84 nmol.mg−1.hr−1) in fibroblasts from SP patients. As is shown in Fig. 1b, a small, though significant difference in NAGLU activity between the RP and SP group was seen after culturing at 37 °C (p < 0.01). However, when looking at individual values of enzymatic activity there is still considerable overlap between the two groups. Figure 1c shows that culturing fibroblasts at 30 °C for 1 week resulted in a more pronounced difference in NAGLU activity between the two groups. After culturing fibroblasts at 30 °C significantly higher NAGLU activity levels were found in SP patients (median NAGLU activity 2.92 nmol.mg−1.hr−1 (range 0.66-13.70 nmol.mg−1.hr−1)) compared to RP patients (median NAGLU activity after culturing at 30 °C 0.30 nmol.mg−1.hr−1 (range 0.15-0.50 nmol.mg−1.hr−1)) (p < 0.001). ROC analysis showed an area under the curve of 1.0, indicating that NAGLU activity after culturing at 30 °C is a very accurate tool to discriminate between RP and SP patients (p < 0.001). A NAGLU activity of 0.58 nmol.mg−1.hr−1 was calculated to be the optimal cut-off value to distinguish RP patients from SP patients with a sensitivity and specificity of 100 % (Fig. 1d).
a. Mean NAGLU activity (nmol.mg−1.hr−1) of duplicate measurement in fibroblasts of the individual MPS IIIB patients after culturing cells at 37 °C and 30 °C for 1 week. Patient numbers correspond with the numbers in Table 1. Data of one representative experiment are shown. b and c. NAGLU activity (nmol.mg−1.hr−1) measured in fibroblasts of SP and RP MPS IIIB patients after culturing cells at 37 °C and 30 °C for 1 week, respectively. Medians are given. Data of one representative experiment are shown. d. Sensitivity and specificity for cut-off levels of NAGLU activity in fibroblasts after culturing at 30 °C to distinguish between RP and SP MPS IIIB patients. The dashed line indicates the calculated optimal cut-off level of 0.58 nmol.mg−1.hr−1
HS levels in fibroblasts
HS levels in RP and SP MPS IIIB patients’ fibroblasts were analyzed to assess whether storage levels are influenced by the differences in NAGLU activity levels observed between the two groups. No significant difference was found in HS level between the groups when fibroblasts were cultured at 37 °C (Fig. 2). However, in fibroblasts cultured at 30 °C HS levels were significantly lower in fibroblasts from patients with an SP phenotype compared to fibroblasts from patients with an RP phenotype (p < 0.05). Culturing fibroblasts of RP patients at either 37 °C or 30 °C, did not result in any significant differences in HS levels, while significantly lower HS levels after culturing at 30 °C were found in patients within the SP group, compared to levels after culturing at 37 °C (p < 0.01). This indicates that the increased NAGLU activity, measured in vitro after culturing cells at 30 °C, indeed corresponds to higher levels of functional NAGLU in fibroblasts of SP patients.
Disease symptoms and NAGLU activity ratio after culturing at 30 °C over 37 °C
The capacity of patients’ fibroblasts to increase residual enzyme activity was further assessed by calculating the ratio of NAGLU activity after culturing at 30 °C over the activity after culturing at 37 °C. The ratio of NAGLU activity after culturing at 30 °C over 37 °C was 9.36 (range 1.93-31.49) in SP patients, which was significantly higher compared to patients in the RP group, who had a median ratio of NAGLU activity of 1.78 (range 0.96-2.39) (p < 0.001) (Fig. 3a). Because MPS IIIB comprises a continuous spectrum of disease severity, we assessed whether this ratio correlated more specifically with the age at which patients lost specific functions. A lower capacity of patients’ fibroblasts to increase NAGLU activity at 30 °C could significantly predict for the loss of the ability to communicate verbally in a meaningful manner and the loss of the ability to walk independently at a younger age (Fig. 3b and c). Also, the age of demise correlated with the NAGLU activity ratio after culturing at 30 °C over the activity after culturing at 37 °C (Fig. 3d).
a. Ratio of NAGLU activity after culturing at 30 °C over the activity after culturing at 37 °C measured in fibroblasts of SP and RP MPS IIIB patients. Medians are given. Data of one representative experiment are shown. b-d. Ratio of NAGLU activity after culturing at 30 °C over the activity after culturing at 37 °C in fibroblasts, correlated to the age of speech loss (23 out of 28 patients), to the age of loss of mobility (19 out of 28 patients), and correlated to the age of demise (13 out of 28 patients who had died at time of this study). Data of one representative experiment are shown
Discussion
Over recent years, a number of studies on potential disease modifying treatment options for MPS IIIB have been initiated. For evaluating clinical efficacy as well as for assessing which patients may benefit the most from a specific treatment, it will be essential to predict the natural course of the disease for each individual patient at an early stage. Here, we investigate an approach to discriminate between MPS IIIB patients with a rapidly progressing (RP, classical or severe) phenotype and patients with a slowly progressing (SP, attenuated) phenotype, using cultured skin fibroblasts.
We observed a significant difference in residual activity of NAGLU between fibroblasts from RP and SP patients when fibroblasts were cultured at 37 °C. However, NAGLU activity did not completely discriminate between the two groups. Culturing fibroblasts at 30 °C, however, allowed for complete separation between RP and SP patients. Accordingly, HS levels after culturing at 30 °C were significantly lower in fibroblasts from the SP group than in fibroblasts from the RP group. This indicates that the increased NAGLU activity measured in protein lysates after culture at 30 °C comprises a form of the enzyme that is biochemically active in living cells and exerts its catalytic function in the lysosome. Nevertheless, it should be taken into consideration that other factors, such as alteration of GAG synthesis, are responsible for lower HS levels. However, it is unlikely that this only affects the SP group.
MPS IIIB is characterized by a large genetic heterogeneity which is probably the most important cause of the phenotypic variability. Although some genotype-phenotype correlations have been established in MPS IIIB, previously unrecognized mutations are frequently reported. In our limited series of patients, the RP patients all have two nonsense or frameshift mutations, whereas all the SP patients have at least one missense mutation. Irrespectively of genotype, NAGLU activity in fibroblasts after culturing at 30 °C appears to reliably predict for an RP or SP phenotype.
MPS IIIB comprises a continuous spectrum of disease severity, and a division in only an RP and an SP group does no justice to the clinical variability observed in patients. Valstar et al showed that the loss to communicate in a meaningful manner and the ability to walk independently are key symptoms in the assessment of disease progression (Valstar et al 2010a). We therefore correlated the loss of these functions to the ratio of NAGLU activity at 30 °C over 37 °C. The capacity of fibroblasts to enhance residual enzyme activity at 30 °C correlated with the course of the disease. However, since not all patients had already reached these stages of disease, patient numbers are small and more patients would be needed to validate these correlations.
The increased levels of residual NAGLU measured in SP patients after culturing cells at 30 °C, might be due to more efficient protein folding at this lower temperature, thereby stimulating the activity of mutant enzymes (Gootjes et al 2004; Diekman et al 2015). The positive effect of culturing human fibroblasts at 30 °C on protein quantity and enzymatic activity has already been demonstrated for a distinct metabolic disorder by another group in our lab (Houten et al 2002). Cells of patients with a mild mevalonate kinase deficiency showed higher enzymatic activity after culturing at 30 °C which correlated with higher protein levels on Western blot. Culture temperature had no effect on cells of patients with a severe mevalonate kinase deficiency. We hypothesize that the higher levels of NAGLU activity found in SP patients might be caused by the presence of molecular chaperones or differences in the regulation of the endoplasmic-reticulum-associated protein degradation machinery which only become apparent at 30 °C culture conditions, at least in the in vitro setting.
In most SP fibroblasts, culturing at 30 °C resulted in levels of NAGLU activity that exceeded 10 % of control enzyme activity (reference values for NAGLU activity in fibroblasts used in our diagnostic laboratory are 9–17 nmol.mg−1.hr−1). Ten percent of control NAGLU activity is often associated with the amelioration of symptoms. Our findings indicate that residual NAGLU activity can potentially be enhanced and that MPS IIIB patients with a SP phenotype might benefit from therapies that interfere with protein folding, such as chemical and pharmacological chaperones (Meijer et al 2013). However, more research is needed to elucidate the underlying processes and the effects of therapies that interfere with these mechanisms.
To be able to measure low levels of NAGLU activity and to detect minor changes in enzyme activity at different conditions in all patient cell lines, we optimized the assay normally used in our diagnostic department. Using this optimized assay, in patient 25 remarkably high levels of NAGLU activity and low HS levels were found at all culture conditions, despite previous genetic and biochemical confirmation of the diagnosis MPS IIIB. The use of high concentrations of 4MU-α-G1cNAc substrate (1.5 mg/mL final concentration) in combination with an optimized pH and incubation time, might have favored the particular kinetic properties of the mutant enzyme in this patient. Furthermore, NAGLU with this particular mutation might have an increased affinity to the 4MU-substrate, as compared to natural substrates present in vivo. This is currently being further investigated.
In conclusion, we show that NAGLU activity in fibroblasts cultured at 30 °C can be used to discriminate between RP and SP MPS IIIB patients and that the capacity of cells to increase NAGLU activity at lower temperatures correlates with disease severity and progression. Prediction of the phenotype of an individual patient may become of high relevance in the near future for assessment of the efficacy of disease modifying treatments for MPS IIIB.
References
Baehner F, Schmiedeskamp C, Krummenauer F et al (2005) Cumulative incidence rates of the mucopolysaccharidoses in Germany. J Inherit Metab Dis 28:1011–1017
Beesley CE, Young EP, Vellodi A, Winchester BG (1998) Identification of 12 novel mutations in the α-N-acetylglucosaminidase gene in 14 patients with Sanfilippo syndrome type B (mucopolysaccharidosis type IIIB). J Med Genet 35:910–914
Beesley C, Moraitou M, Winchester B et al (2004) Sanfilippo B syndrome: Molecular defects in Greek patients. Clin Genet 65:143–149
Beesley CE, Jackson M, Young EP et al (2005) Molecular defects in Sanfilippo syndrome type B (mucopolysaccharidosis IIIB). J Inherit Metab Dis 28:759–767
Bunge S, Knigge A, Steglich C et al (1999) Mucopolysaccharidosis type IIIB (Sanfilippo B): identification of 18 novel α-N-acetylglucosaminidase gene mutations. J Med Genet 36:28–31
Champion KJ, Basehore MJ, Wood T et al (2010) Identification and characterization of a novel homozygous deletion in the α-N-acetylglucosaminidase gene in a patient with Sanfilippo type B syndrome (mucopolysaccharidosis IIIB). Mol Genet Metab 100:51–56
Chinen Y, Tohma T, Izumikawa Y et al (2005) Sanfilippo type B syndrome: five patients with an R565P homozygous mutation in the α-N-acetylglucosaminidase gene from the Okinawa islands in Japan. J Hum Genet 50:357–359
Diekman EF, Ferdinandusse S, van der Pol L et al (2015) Fatty acid oxidation flux predicts the clinical severity of VLCAD deficiency. Genet Med. doi:10.1038/gim.2015.22
Emre S, Terzioglu M, Tokatli A et al (2002) Sanfilippo syndrome in Turkey: identification of novel mutations in subtypes A and B. Hum Mutat 19:184–185
Esko JD, Kimata K, Lindahl U (2009) Chapter 16 Proteoglycans and Sulfated Glycosaminoglycans. In: Varki A, Cummings RD, Esko JD (eds) Essentials of glycobiology, 2nd edn. Cold Spring Harbor Laboratory Press, Cold Spring Harbor (NY)
Esposito S, Balzano N, Daniele A et al (2000) Heparan N-sulfatase gene: two novel mutations and transient expression of 15 defects. Biochim Biophys Acta 1501:1–11
Gootjes J, Schmohl F, Mooijer PA et al (2004) Identification of the molecular defect in patients with peroxisomal mosaicism using a novel method involving culturing of cells at 40°C: implications for other inborn errors of metabolism. Hum Mutat 24:130–139
Houten SM, Frenkel J, Rijkers GT et al (2002) Temperature dependence of mutant mevalonate kinase activity as a pathogenic factor in hyper-IgD and periodic fever syndrome. Hum Mol Genet 11:3115–3124
Kingma SDK, Langereis EJ, de Klerk CM et al (2013) An algorithm to predict phenotypic severity in mucopolysaccharidosis type I in the first month of life. Orphanet J Rare Dis 8:99
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ (1951) Protein measurement with the Folin phenol reagent. J Biol Chem 193:265–275
Malinowska M, Wilkinson FL, Bennett W et al (2009) Genistein reduces lysosomal storage in peripheral tissues of mucopolysaccharide IIIB mice. Mol Genet Metab 98:235–242
Malinowska M, Wilkinson FL, Langford-Smith KJ et al (2010) Genistein improves neuropathology and corrects behaviour in a mouse model of neurodegenerative metabolic disease. PLoS One 5, e14192
Marsh J, Fensom AH (1985) 4-Methylumbelliferyl α-N-acetylglucosaminidase activity for diagnosis of Sanfilippo B disease. Clin Genet 27:258–262
Meijer OL, van Vlies N, Wijburg FA (2013) Treatment of mucopolysaccharidosis type III (Sanfilippo syndrome). Expert Opin Orphan Drugs 1:717–730
Moog U, van Mierlo I, van Schrojenstein Lantman-de Valk HM et al (2007) Is Sanfilippo type B in your mind when you see adults with mental retardation and behavioral problems? Am J Med Genet C: Semin Med Genet 145C:293–301
Muenzer J (2011) Overview of the mucopolysaccharidoses. Rheumatology 50(Suppl 5):v4–v12
Ouesleti S, Brunel V, Ben TH et al (2011) Molecular characterization of MPS IIIA, MPS IIIB and MPS IIIC in Tunisian patients. Clin Chim Acta 412:2326–2331
Poorthuis BJ, Wevers RA, Kleijer WJ et al (1999) The frequency of lysosomal storage diseases in The Netherlands. Hum Genet 105:151–156
Schmidtchen A, Greenberg D, Zhao H et al (1998) NAGLU mutations underlying Sanfilippo syndrome type B. Am J Hum Genet 62:64–69
Selmer KK, Gilfillan GD, Strømme P et al (2012) A mild form of Mucopolysaccharidosis IIIB diagnosed with targeted next-generation sequencing of linked genomic regions. Eur J Hum Genet 20:58–63
Tang J, Pan J, Guo Y et al (2013) Mucopolysaccharidosis type IIIB mutations in Chinese patients: identification of two novel NAGLU mutations and analysis of two cases involving prenatal diagnosis. Clin Chim Acta 419:33–38
Tessitore A, Villani GR, Di Domenico C et al (2000) Molecular defects in the α-N-acetylglucosaminidase gene in Italian Sanfilippo type B patients. Hum Genet 107:568–576
Valstar MJ, Ruijter GJ, Van Diggelen OP et al (2008) Sanfilippo syndrome: a mini-review. J Inherit Metab Dis 31:240–252
Valstar MJ, Bruggenwirth HT, Olmer R et al (2010a) Mucopolysaccharidosis type IIIB may predominantly present with an attenuated clinical phenotype. J Inherit Metab Dis 33:759–767
Valstar MJ, Neijs S, Bruggenwirth HT et al (2010b) Mucopolysaccharidosis type IIIA: clinical spectrum and genotype-phenotype correlations. Ann Neurol 68:876–887
Van de Kamp JJ, van Pelt JF, Liem KO et al (1976) Clinical variability in Sanfilippo B disease: a report on six patients in two related sibships. Clin Genet 10:279–284
Weber B, Guo XH, Kleijer WJ et al (1999) Sanfilippo type B syndrome (mucopolysaccharidosis III B): allelic heterogeneity corresponds to the wide spectrum of clinical phenotypes. Eur J Hum Genet 7:34–44
Zhao HG, Li HH, Bach G et al (1996) The molecular basis of Sanfilippo syndrome type B. Proc Natl Acad Sci U S A 93:6101–6105
Zhao HG, Aronovich EL, Whitley CB (1998) Genotype-phenotype correspondence in Sanfilippo syndrome type B. Am J Hum Genet 62:53–63
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Informed consent
Informed consent for the use of patient data and fibroblasts was obtained from parents or legal representatives for all patients. This study was submitted to the Medical Ethical Review Board of the Academic Medical Center in Amsterdam who declared that ethical approval was not necessary because of the observational nature of the study. All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000 (5).
Animal rights
This article does not contain any studies with animal subjects performed by any of the authors.
Additional information
Communicated by: Robert Steiner
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Meijer, O.L.M., Welling, L., Valstar, M.J. et al. Residual N-acetyl-α-glucosaminidase activity in fibroblasts correlates with disease severity in patients with mucopolysaccharidosis type IIIB. J Inherit Metab Dis 39, 437–445 (2016). https://doi.org/10.1007/s10545-016-9916-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10545-016-9916-2