Abstract
Tumor endothelial cells (TEC) differ from the normal counterpart, in both gene expression and functionality. TEC may acquire drug resistance, a characteristic that is maintained in vitro. There is evidence that TEC are more resistant to chemotherapeutic drugs, substrates of ATP-binding cassette (ABC) transporters. TEC express p-glycoprotein (encoded by ABCB1), while no difference in other ABC transporters was revealed compared to normal endothelia. A class of tyrosine kinase inhibitors (TKI), used as angiostatic compounds, interferes with the ATPase activity of p-glycoprotein, thus impairing its functionality. The exposure of ovarian adenocarcinoma TEC to the TKIs sunitinib or sorafenib was found to abrogate resistance (proliferation and motility) to doxorubicin and paclitaxel in vitro, increasing intracellular drug accumulation. A similar effect has been reported by the p-glycoprotein inhibitor verapamil. No beneficial effect was observed in combination with cytotoxic drugs that are not p-glycoprotein substrates. The current paper reviews the mechanisms of TEC chemoresistance and shows the role of p-glycoprotein in mediating such resistance. Inhibition of p-glycoprotein by anti-angiogenic TKI might contribute to the beneficial effect of these small molecules, when combined with chemotherapy, in counteracting acquired drug resistance.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Chemoresistance is the main limitation to cancer treatment. Almost all the work on this phenomenon has been restricted to tumor cells. Recent studies have shown the relevant role of the tumor microenvironment in acquired drug resistance [1–3]. Proficient delivery of chemotherapeutic drugs to a solid tumor, and thus eradication of cancer cells, relies on drug uptake across the tumor vessels. Tumor vasculature differs from the normal vascular bed; it comprises irregular, dilated, leaky and dead-end-containing vessels, which cause high tumor interstitial fluid pressure and are responsible for a low and heterogeneous blood flow in tumor tissue [4]. Thus, the vessel structure is the first barrier to an efficient delivery of drugs to the tumor parenchyma [5]. Recent studies demonstrate the acquisition of drug resistance by the tumor endothelium, which represents another hurdle to cancer therapy [6].
In this study, we will discuss a mechanism of chemoresistance in tumor endothelial cells and the potential role of therapeutic intervention that can be exploited to ameliorate drug response.
Tumor endothelial cells acquire drug resistance
Endothelial cells from tumor blood vessels (TEC) differ from endothelial cells in normal tissues. We and others have shown that TEC display altered phenotypic and functional features [7–11], which reflect alterations at transcriptional level [12–15].
Among key functional characteristics, TEC show reduced sensitivity to certain chemotherapeutic drugs compared to normal endothelia. For example, renal carcinoma endothelial cells are resistant to vincristine, likewise breast cancer [16, 17] and hepatocellular carcinoma endothelium to doxorubicin and 5-fluorouracil [18].
In agreement with those reports, we demonstrate that endothelial cells from human ovarian carcinoma (HOC–EC) are less sensitive than normal endothelium (HUVEC) to paclitaxel (Fig. 1a), doxorubicin (Fig. 1b) and vincristine (not shown), in terms of proliferative and migrative capabilities, two fundamental functions for the growth and remodeling of the tumor vasculature.
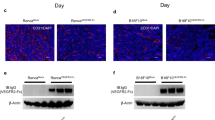
HOC–EC are resistant to chemotherapy by up-regulation of p-glycoprotein. a, b Responsiveness of tumor and normal endothelial cells to chemotherapeutics. HOC–EC and HUVEC were exposed to increasing doses of paclitaxel and doxorubicin for the duration of the assays (72 h for proliferation and 4 h for migration). Proliferation and motility are expressed as percentage of control (in the absence of chemotherapeutic drugs). Data are representative of at least three independent experiments. c Doxorubicin uptake in tumor and normal endothelial cells. Intracellular concentration of doxorubicin in HOC–EC and HUVEC was measured by fluorescence after 3-h exposure. d Expression of ABC transporters by tumor and normal endothelial cells. ABCB1 (MDR1), ABCC1 (MRP1), ABCC2 (MRP2) and ABCG2 (BCRP) expression was assayed by RT-qPCR. The box plots show the DCt values of HOC–EC (N = 11) and HUVEC (N = 5): the lower DCt corresponds to the higher expression. e Expression of p-glycoprotein by tumor and normal endothelial cells. Western blot detection of p-glycoprotein in HOC–EC and HUVEC lysates. Tubulin was used as internal control. P < 0.05 (*), P < 0.01 (**), P < 0.001 (***) P < 0.0001 (****)
ABCB1 is overexpressed in TEC and mediates chemoresistance
Investigating the mechanisms of increased resistance, we put to use our previous results that demonstrated ATP-binding cassette (ABC) transporters family members, responsible for the removal of drugs from cells, to be among the genes overexpressed by tumor versus normal endothelium [15]. ABC transporters are energy-dependent plasma membrane glycoproteins that pump substrates against a chemical gradient, a process that requires ATP hydrolysis as a driving force. Thus, we measured the uptake of Hoechst 33342, rodhamine-123 (not shown) and doxorubicin and found reduced intracellular accumulation in HOC–EC compared to HUVEC, reflecting increased transporter activity (Fig. 1c).
We thus investigated the expression of those transporters considered responsible for the efflux of chemotherapeutics and decreased therapeutic efficacy. The group includes ABCB1 (known as p-glycoprotein) one of the best-studied ABC transporters, ABCC1 (also known as MRP1), ABCC2 (or MRP2) and ABCG2 (also called BCRP). They extrude a wide variety of hydrophobic compounds including doxorubicin, vinblastine and paclitaxel. When highly expressed in the plasma membrane of tumor cells, they protect cancer cells from the cytotoxic drugs, resulting in chemotherapy failure [19].
Here we demonstrate that p-glycoprotein, but not ABCC1, ABCC2 or ABCG2, is expressed at higher levels in HOC–EC than in HUVEC (Fig. 1d). Protein analysis confirmed the high levels of p-glycoprotein by HOC–EC, while no expression was detected in HUVEC (Fig. 1e). This feature is a novel finding for ovarian adenocarcinoma and suggests that increased drug extrusion by the intratumor endothelium is mediated by p-glycoprotein. The relevance of the data obtained ex vivo is supported by immunohistochemistry on human tissue specimens. P-glycoprotein has been shown associated with neovasculature of brain malignancies, nephroblastoma and ependymomas, where it presented a luminal localization to efficiently mediate the polarized efflux of drugs to the blood [20–22]. Moreover, p-glycoprotein expression by intratumor endothelium, but not by cancer cells, correlated with the unfavorable outcome [20]. Overexpression of p-glycoprotein by TEC might depend on the in vivo continuous stimulation of endothelial cells by the tumor microenvironment and cancer cells. Indeed, tumor cell-conditioned medium, containing angiogenic growth factors, up-regulated p-glycoprotein on mouse TEC isolated from a human melanoma xenograft [23].
P-glycoprotein is physiologically present in endothelium of the brain, testis and placental vasculature, likely functioning as protection from circulating toxic agents [24]. In intratumor vessels, it might contribute to create a “blood-tumor barrier”, interfering with the delivery of chemotherapy to neoplastic cells. It is reasonable to speculate that this can contribute to the first line of resistance to treatments, the efficacy of which is then further impaired by drug resistance of cancer cells.
Inhibition of p-glycoprotein restores chemosensitivity
To verify whether p-glycoprotein functionally mediates the chemoresistance of HOC–EC, the drug sensitivity was investigated in presence of the p-glycoprotein blocker verapamil [25]. Verapamil enhanced the HOC–EC intracellular accumulation of doxorubicin (as described for p-glycoprotein proficient cancer cells), while it did not affect HUVEC (Fig. 2a). Accordingly, treatment of HOC–EC with verapamil increased doxorubicin (Fig. 3a, left panel) and vincristine (not shown) cytotoxicity, while no effect was observed in HUVEC (Fig. 3a right panel). At the same extent, verapamil improved the activity of paclitaxel on both proliferation and migration of HOC–EC (Fig. 3b). The use of verapamil in clinic is limited by its toxicity. Effort is being made to identify selective inhibitors for ABC transporters.
TKI increase HOC–EC intracellular doxorubicin concentration. HOC–EC and HUVEC were incubated with 10 μM doxorubicin in the absence or presence of verapamil (a), sorafenib (b) or sunitinib (c). Cells were lysed and fluorescence quantified by a plate reader. Data are representative of three independent experiments
TKI enhance HOC–EC responsiveness to doxorubicin, paclitaxel but not cisplatin. a–c In vitro responsiveness of TEC to chemotherapeutics. HOC–EC or HUVEC were exposed to increasing doses of doxorubicin (a), paclitaxel (b) or cisplatin (c) for the duration of the assays (72 h for proliferation and 4 h for migration). Verapamil, sorafenib or sunitinib at the indicated concentrations were added 2 h earlier. Proliferation and motility are expressed as percentage of control (in the absence of chemotherapeutic drugs). Data are representative of at least three independent experiments. d In vivo tumor growth inhibition. A2780-1A9 ovarian cancer cells (10 × 106) were transplanted subcutaneously in nude mice that were randomized to treatments at tumor volume of 150 mm3 (eight mice per group). Vandetanib was administered p.o. at a dose of 50 mg/kg for 5 days. Doxorubicin (8 mg/kg), paclitaxel (20 mg/kg) or cisplatin (5 mg/kg) were administered i.v. as a single bolus (arrowhead). Response is shown as tumor volume over time. P < 0.05 (*), P < 0.01 (**), P < 0.001 (***)
Tyrosine kinase inhibitors as p-glycoprotein inhibitors
The tyrosine kinase inhibitors (TKI) are small molecules designed to arrest signaling pathways and block the phosphorylation of intracellular targets by competing with ATP at the active site of several tyrosine kinases. Sorafenib (Nexavar™), sunitinib (Sutent™), vandetanib (Caprelsa™) and cediranib (Zemfirza™) that primarily target VEGF receptors (mainly VEGFR2) at various affinities are TKI that have shown clinical efficacy as angiogenesis inhibitors [26].
Interestingly, these TKI have been reported to interfere with the ATPase activity of p-glycoprotein. By using cancer cells resistant to chemotherapy (p-glycoprotein overexpressing cells), sunitinib has been shown to enhance the cytotoxicity of doxorubicin and vincristine in gastric cancer cells [27], cediranib to enhance responsiveness of oral epidermoid carcinoma and breast carcinoma cells to doxorubicin and/or vincristine [28] and vandetanib to antagonize doxorubicin and docetaxel in breast [29] and ovarian cancer cells [30]. None of these TKI was able to modulate p-glycoprotein transcript and protein expression in cancer cells. Instead, they were capable of interfering with the ATPase activity and as a consequence of inhibiting the function of p-glycoprotein, allowing the accumulation of the transporter substrates (like rodhamine-123) [27–30].
No data are available on the effect of TKI on “naturally” chemoresistant endothelium. Here, we show that sorafenib and sunitinib increased intracellular accumulation of doxorubicin in p-glycoprotein proficient HOC–EC in a dose dependent manner, demonstrating a functional inhibition of the transporter (Fig. 2).
TKI reverse tumor endothelial cell multidrug resistance
The above observation allowed us to hypothesize that the anti-angiogenic activity of the TKI might be potentiated by the inhibition of p-glycoprotein activity that sensitizes TEC to cytotoxic agents. We tested whether sunitinib and sorafenib could ameliorate HOC–EC sensitivity to chemotherapy. To exclude a direct effect of TKI, the concentrations that “per se” do not affect endothelial cells proliferation and migration were used. The addition of sorafenib or sunitinib (not shown) to doxorubicin significantly impaired HOC–EC proliferation, while neither one affected HUVEC (Fig. 3a) as happened with verapamil. Similarly, sorafenib and sunitinib potentiated paclitaxel efficacy on both proliferation and migration of HOC–EC (Fig. 3b). The addition of TKI did not significantly alter the efficacy of cisplatin on HOC–EC (Fig. 3c) nor on HUVEC (not shown). Altogether our results indicate that anti-angiogenic TKI directly affect HOC–EC p-glycoprotein activity, resulting in improved cytotoxicity by chemotherapy, evident only when substrates of p-glycoprotein were used.
To translate the in vitro observation to an in vivo preclinical setting, the activity of chemotherapy in combination with a TKI was tested on A2780-1A9 ovarian cancer xenograft, which does not express p-glycoprotein on tumor cells. A2780-1A9 xenograft is equally responsive to a single bolus of doxorubicin, cisplatin or paclitaxel (T/C 42, 39, 50%, respectively) (Fig. 3d) and, as previously shown [31] to 5 days treatment with vandetanib (T/C 47%). Co-administration of vandetanib with doxorubicin or paclitaxel significantly inhibited tumor growth (T/C 9 and 7%, respectively) compared to the single treatments (Fig. 3d). Conversely, the addition of vandetanib to cisplatin did not significantly increase antitumor efficacy (T/C 31%), thus endorsing the in vitro results on the role of p-glycoprotein in tumor endothelium drug resistance. This result is corroborated by studies on a melanoma xenograft model, showing that murine TEC also express high levels of p-glycoprotein and are resistant to paclitaxel. Verapamil restored the effect of paclitaxel on TEC proliferation in vitro [23] and in vivo increased the antitumor effect of paclitaxel, but not of 5-fluorouracil [32].
Conclusion and future perspective
Increasing evidence suggests that TEC are the first line of tumor chemoresistance. Up-regulation of p-glycoprotein is a mechanism that influences drug response. Our data, together with published reports, suggest that the anti-angiogenic TKI, such as sunitinib, sorafenib and vandetanib, act as p-glycoprotein inhibitors.
We propose that the TKI exert the anti-angiogenic effect on tumor endothelium by two complementary mechanisms. As exemplified in Fig. 4, TKI (1) directly inhibit the angiogenic factors-driven signaling pathways needed for growth and maintenance of tumor vessels and (2) sensitize tumor endothelium to chemotherapeutics, by inhibiting p-glycoprotein. The antitumor outcome might be amplified by a direct inhibitory effect of TKI on p-glycoprotein expressing tumor cells.
Dual targeting of tumor vasculature by anti-angiogenic TKI. In a tumor environment, TKI exert a dual effect on TEC: (1) by inhibiting the signal transduction pathway of its targets, the TKI reduce the capacity of TEC to react to pro-angiogenic stimuli (direct anti-angiogenic effect), (2) by inhibiting the activity of the TEC p-glycoprotein, the TKI enhance the “toxic” effect of chemotherapeutics that are substrate of the pump (revert TEC drug resistance) with a net amplified effect on the responsiveness to the combined treatment
TEC have been shown to be resistant not only to p-glycoprotein substrate drugs, but also to other chemotherapy. Human hepatocellular-derived endothelial cells have been described resistant to 5-fluorouracil [18] and we found that HOC–EC are poorly responsive to cisplatin. All these drugs are not ABC transporter substrates, suggesting that other mechanisms are involved.
In conclusion, we highlight the contribution of tumor vasculature to drug resistance and show a distinctive mechanism helping to explain the beneficial effect of anti-angiogenic TKI combined with chemotherapy.
Materials and methods
Isolation, culture and characterization of endothelial cells from human tissues
HOC–EC were isolated (as described in [33, 34]) from neoplastic tissues of patients undergoing therapeutic surgery, with their full informed consent [10]. Primary cultures of human umbilical vein endothelial cells [HUVECs] were isolated from umbilical cord veins [35] and grown as described [36]. Cells were used between the third and fifth passage.
For experimental purposes, endothelial cells were analyzed in the presence of an “angiogenic milieu” reconstituted in vitro, mimicking the “in vivo” rich environment, namely human recombinant vascular endothelial growth factor (VEGF; 10 ng/ml), fibroblast growth factor-2 (FGF-2; 2 ng/ml) and epidermal growth factor (EGF; 10 ng/ml) [10, 15].
Quantitative real-time PCR (RT-qPCR)
One microgram of total RNA was reverse-transcribed using the High-Capacity cDNA Reverse Transcription Kit and Random Hexamer primers (Applied Biosystems) according to the manufacturer’s protocols. RT-qPCR reactions were done in duplicate on the 7900HT Fast Real-Time PCR System (Applied Biosystems). Specific TaqMan® Gene Expression Assays were purchased from Applied Biosystems and Integrated DNA Technologies (IDT). Target expression was normalized to the human 18s rRNA for each endothelial cell population (DCt = Ct target gene-Ct 18s).
Western blot analysis
Proteins were separated by 6% SDS–polyacrylamide gel electrophoresis, transferred to nitrocellulose membranes (Millipore) and incubated for 1 h at room temperature in blocking buffer containing 5% dry fat milk and 0.1% Tween 20 in PBS. The membranes were probed with anti MDR-1 (1:200, Santa Cruz Biotechnology) or anti α-tubulin (1:1000, Sigma-Aldrich) antibody overnight at 4 °C. Antibody binding was detected with anti-mouse IgG-HRP (1:10,000, Sigma-Aldrich) for 45 min at room temperature. The signals were detected with ECL prime (GE-Healthcare).
Proliferation assay
Proliferation was measured using the CellTiter 96® AQueous Non-Radioactive Cell Proliferation Assay (Promega). Briefly, 2 × 103 HOC–EC or HUVEC were plated into 96-well plates and placed at 37 °C in 5% CO2. After 24 h, drugs were added to the cells and incubated for 72 h. For the combination experiments, verapamil, sorafenib or sunitinib were added 2 h before chemotherapy (doxorubicin, paclitaxel and cisplatin). Doses are given in the figure legends. At the end of the experiment, MTS solution was added to each well and incubated for 3 h at 37 °C in 5% CO2. Plates were thoroughly shaken, and the absorbance at 490 nm was recorded with the microplate reader (Infinite® 200, Tecan).
Motility assay
Chemotaxis was assessed using Boyden chambers and gelatin-coated polycarbonate nucleopore filters (8-µm pore size) [36]. The supernatant of NIH-3T3 cells was used as the attractant. Cells were resuspended in Dulbecco’s modified Eagle’s medium/0.1% BSA and added to the upper compartment of the chamber (30,000 cells/well). Paclitaxel, sorafenib, sunitinib and verapamil at the indicated concentration were added to the cells and incubated throughout the assay (4 h). At the end of incubation, filters were stained with Diff-Quik (Siemens Healthcare) and the migrated cells counted in ten high-power fields.
Doxorubicin uptake assay
Cells were seeded in 96-well plates (7000 cells/well) and let to adhere overnight. Cells were incubated with 10 μM doxorubicin for 3 h at 37 °C, then washed with PBS (4 °C) and lysed in 10% Triton X-100. The concentrations of doxorubicin in each sample were determined by fluorescence spectrofluorometry (λ em = 590 nm) (Infinite®200, TECAN). Cells were pre-treated with verapamil, sorafenib or sunitinib at the indicated concentrations for 1 h and incubated with 10 μM doxorubicin for 3 h.
In vivo experiment
Six- to 8-week-old female NCr-nu/nu mice were obtained from Harlan Laboratories. They were maintained under specific pathogen-free conditions, housed in isolated vented cages and handled using aseptic procedures. Procedures involving animals and their care were conducted in conformity with institutional guidelines that comply with national (Legislative Decree 26, March 4, 2014) and international (EEC Council Directive 2010/63) laws and policies, in line with guidelines for the welfare and use of animals in cancer research [37]. A2780-1A9 human ovarian carcinoma cells (10 × 106) were implanted subcutaneously [31]. Tumor growth was measured with a caliper and tumor volume (mm3) calculated as [length (mm) × width2 (mm2)]/2. Mice were randomized (8 mice/group) at approximately 150 mm3 of tumor volume to receive treatments. Vandetanib (AstraZeneca) was administered p.o. at 50 mg/kg for 5 days. Paclitaxel (PTX; kindly provided by Indena S.p.A., Milan, Italy), doxorubicin (kindly provided by Nerviano Medical Science) or cisplatin (DDP; Sigma-Aldrich) were administered intravenously (i.v.) as a single bolus at a dose of 20, 8 and 5 mg/kg, respectively. Efficacy of the treatment was evaluated as the best tumor growth inhibition: %T/C = (median volume of treated tumors/median volume of control tumors) × 100.
Statistical analyses
Statistical analyses were carried out using Prism 7 (GraphPad Software). Differences among three or more groups were analyzed by the Kruskal–Wallis test followed by Dunn’s multiple comparison posttest). Two group comparisons were done by Student’s t test.
Change history
09 May 2017
An erratum to this article has been published.
References
McMillin DW, Negri JM, Mitsiades CS (2013) The role of tumour–stromal interactions in modifying drug response: challenges and opportunities. Nat Rev Drug Discov 12:217–228. doi:10.1038/nrd3870
van Beijnum JR, Nowak-Sliwinska P, Huijbers EJM et al (2015) The great escape; the hallmarks of resistance to antiangiogenic therapy. Pharmacol Rev 67:441–461. doi:10.1124/pr.114.010215
Huijbers EJM, van Beijnum JR, Thijssen VL et al (2016) Role of the tumor stroma in resistance to anti-angiogenic therapy. Drug Resist Updat Rev Comment Antimicrob Anticancer Chemother 25:26–37. doi:10.1016/j.drup.2016.02.002
Nagy JA, Chang S-H, Shih S-C et al (2010) Heterogeneity of the tumor vasculature. Semin Thromb Hemost 36:321–331. doi:10.1055/s-0030-1253454
Heldin C-H, Rubin K, Pietras K, Ostman A (2004) High interstitial fluid pressure—an obstacle in cancer therapy. Nat Rev Cancer 4:806–813. doi:10.1038/nrc1456
Hida K, Akiyama K, Ohga N et al (2013) Tumour endothelial cells acquire drug resistance in a tumour microenvironment. J Biochem (Tokyo) 153:243–249. doi:10.1093/jb/mvs152
Alessandri G, Chirivi RG, Fiorentini S et al (1999) Phenotypic and functional characteristics of tumour-derived microvascular endothelial cells. Clin Exp Metastas 17:655–662
Bussolati B, Deregibus MC, Camussi G (2010) Characterization of molecular and functional alterations of tumor endothelial cells to design anti-angiogenic strategies. Curr Vasc Pharmacol 8:220–232
Silini A, Ghilardi C, Figini S et al (2012) Regulator of G-protein signaling 5 (RGS5) protein: a novel marker of cancer vasculature elicited and sustained by the tumor’s proangiogenic microenvironment. Cell Mol Life Sci CMLS 69:1167–1178. doi:10.1007/s00018-011-0862-8
Ghilardi C, Silini A, Figini S et al (2015) Trypsinogen 4 boosts tumor endothelial cells migration through proteolysis of tissue factor pathway inhibitor-2. Oncotarget 6:28389–28400. doi:10.18632/oncotarget.4949
Hida K, Maishi N, Torii C, Hida Y (2016) Tumor angiogenesis—characteristics of tumor endothelial cells. Int J Clin Oncol 21:206–212. doi:10.1007/s10147-016-0957-1
St Croix B, Rago C, Velculescu V et al (2000) Genes expressed in human tumor endothelium. Science 289:1197–1202
Lu C, Bonome T, Li Y et al (2007) Gene alterations identified by expression profiling in tumor-associated endothelial cells from invasive ovarian carcinoma. Cancer Res 67:1757–1768. doi:10.1158/0008-5472.CAN-06-3700
Seaman S, Stevens J, Yang MY et al (2007) Genes that distinguish physiological and pathological angiogenesis. Cancer Cell 11:539–554. doi:10.1016/j.ccr.2007.04.017
Ghilardi C, Chiorino G, Dossi R et al (2008) Identification of novel vascular markers through gene expression profiling of tumor-derived endothelium. BMC Genom 9:201. doi:10.1186/1471-2164-9-201
Bussolati B, Deambrosis I, Russo S et al (2003) Altered angiogenesis and survival in human tumor-derived endothelial cells. FASEB J Off Publ Fed Am Soc Exp Biol 17:1159–1161. doi:10.1096/fj.02-0557fje
Grange C, Bussolati B, Bruno S et al (2006) Isolation and characterization of human breast tumor-derived endothelial cells. Oncol Rep 15:381–386
Xiong Y-Q, Sun H-C, Zhang W et al (2009) Human hepatocellular carcinoma tumor-derived endothelial cells manifest increased angiogenesis capability and drug resistance compared with normal endothelial cells. Clin Cancer Res Off J Am Assoc Cancer Res 15:4838–4846. doi:10.1158/1078-0432.CCR-08-2780
Holohan C, Van Schaeybroeck S, Longley DB, Johnston PG (2013) Cancer drug resistance: an evolving paradigm. Nat Rev Cancer 13:714–726. doi:10.1038/nrc3599
Camassei FD, Arancia G, Cianfriglia M et al (2002) Nephroblastoma: multidrug-resistance p-glycoprotein expression in tumor cells and intratumoral capillary endothelial cells. Am J Clin Pathol 117:484–490. doi:10.1309/L44X-L5DN-1VHV-X30N
Fattori S, Becherini F, Cianfriglia M et al (2007) Human brain tumors: multidrug-resistance p-glycoprotein expression in tumor cells and intratumoral capillary endothelial cells. Virchows Arch Int J Pathol 451:81–87. doi:10.1007/s00428-007-0401-z
Ginguené C, Champier J, Maallem S et al (2010) P-glycoprotein (ABCB1) and breast cancer resistance protein (ABCG2) localize in the microvessels forming the blood-tumor barrier in ependymomas. Brain Pathol Zur Switz 20:926–935. doi:10.1111/j.1750-3639.2010.00389.x
Akiyama K, Ohga N, Hida Y et al (2012) Tumor endothelial cells acquire drug resistance by MDR1 up-regulation via VEGF signaling in tumor microenvironment. Am J Pathol 180:1283–1293. doi:10.1016/j.ajpath.2011.11.029
Ambudkar SV, Dey S, Hrycyna CA et al (1999) Biochemical, cellular, and pharmacological aspects of the multidrug transporter. Annu Rev Pharmacol Toxicol 39:361–398. doi:10.1146/annurev.pharmtox.39.1.361
Amin ML (2013) P-glycoprotein inhibition for optimal drug delivery. Drug Target Insights 7:27–34. doi:10.4137/DTI.S12519
Gotink KJ, Verheul HMW (2010) Anti-angiogenic tyrosine kinase inhibitors: what is their mechanism of action? Angiogenesis 13:1–14. doi:10.1007/s10456-009-9160-6
Zhang Y, Wang Q (2013) Sunitinib reverse multidrug resistance in gastric cancer cells by modulating Stat3 and inhibiting P-gp function. Cell Biochem Biophys 67:575–581. doi:10.1007/s12013-013-9544-5
Tao L-Y, Liang Y-J, Wang F et al (2009) Cediranib (recentin, AZD2171) reverses ABCB1- and ABCC1-mediated multidrug resistance by inhibition of their transport function. Cancer Chemother Pharmacol 64:961–969. doi:10.1007/s00280-009-0949-1
Mi Y, Lou L (2007) ZD6474 reverses multidrug resistance by directly inhibiting the function of p-glycoprotein. Br J Cancer 97:934–940. doi:10.1038/sj.bjc.6603985
Jovelet C, Bénard J, Forestier F et al (2012) Inhibition of p-glycoprotein functionality by vandetanib may reverse cancer cell resistance to doxorubicin. Eur J Pharm Sci Off J Eur Fed Pharm Sci 46:484–491. doi:10.1016/j.ejps.2012.03.012
Cesca M, Frapolli R, Berndt A et al (2009) The effects of vandetanib on paclitaxel tumor distribution and antitumor activity in a xenograft model of human ovarian carcinoma. Neoplasia N Y N 11:1155–1164
Akiyama K, Maishi N, Ohga N et al (2015) Inhibition of multidrug transporter in tumor endothelial cells enhances antiangiogenic effects of low-dose metronomic paclitaxel. Am J Pathol 185:572–580. doi:10.1016/j.ajpath.2014.10.017
Alessandri G, Chirivi RG, Castellani P et al (1998) Isolation and characterization of human tumor-derived capillary endothelial cells: role of oncofetal fibronectin. Lab Investig J Tech Methods Pathol 78:127–128
van Beijnum JR, Rousch M, Castermans K et al (2008) Isolation of endothelial cells from fresh tissues. Nat Protoc 3:1085–1091
Jaffe EA, Nachman RL, Becker CG, Minick CR (1973) Culture of human endothelial cells derived from umbilical veins. Identification by morphologic and immunologic criteria. J Clin Invest 52:2745–2756. doi:10.1172/JCI107470
Bonezzi K, Belotti D, North BJ et al (2012) Inhibition of SIRT2 potentiates the anti-motility activity of taxanes: implications for antineoplastic combination therapies. Neoplasia N Y N 14:846–854
Workman P, Aboagye EO, Balkwill F et al (2010) Guidelines for the welfare and use of animals in cancer research. Br J Cancer 102:1555–1577. doi:10.1038/sj.bjc.6605642
Acknowledgements
We are grateful to Sara Figini for technical support and to Viviana Rossi for assistance in manuscript preparation.
Funding
This study was supported by a Grant from the Italian Association for Cancer Research (AIRC No. 12182 and IG No. 18853 to RG).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical approval
All applicable international, national and/or institutional guidelines for the care and use of animals were followed. All procedures performed in studies involving animals were in accordance with ethical standards of the institution or practice at which the studies were conducted.
Additional information
An erratum to this article is available at https://doi.org/10.1007/s10456-017-9558-5.
Rights and permissions
About this article
Cite this article
Bani, M., Decio, A., Giavazzi, R. et al. Contribution of tumor endothelial cells to drug resistance: anti-angiogenic tyrosine kinase inhibitors act as p-glycoprotein antagonists. Angiogenesis 20, 233–241 (2017). https://doi.org/10.1007/s10456-017-9549-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10456-017-9549-6