Abstract
Biologic scaffold materials composed of allogeneic or xenogeneic extracellular matrix (ECM) are commonly used for the repair and remodeling of injured tissue. The clinical outcomes associated with implantation of ECM-based materials range from unacceptable to excellent. The variable clinical results are largely due to differences in the preparation of the material, including characteristics of the source tissue, the method and efficacy of decellularization, and post-decellularization processing steps. The mechanisms by which ECM scaffolds promote constructive tissue remodeling include mechanical support, degradation and release of bioactive molecules, recruitment and differentiation of endogenous stem/progenitor cells, and modulation of the immune response toward an anti-inflammatory phenotype. The methods of ECM preparation and the impact of these methods on the quality of the final product are described herein. Examples of favorable cellular responses of immune and stem cells associated with constructive tissue remodeling of ECM bioscaffolds are described.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction: Bioscaffolds Derived from Extracellular Matrix
Biologic materials composed of mammalian extracellular matrix (ECM) have been effectively used for the repair and reconstruction of a variety of tissues, including skeletal muscle,69,162,228,254 esophagus,11,111,183,184 tendon,15,49,62,91,93 lower urinary tract,13,28,142,168,198 and heart,12,90,139,196,216,268 among others51,88,137,138 in both preclinical animal studies and human clinical studies. These studies have largely shown constructive, functional tissue remodeling with the partial restoration of site appropriate tissue.8 This deviation from the default tissue injury response of inflammation and scar tissue formation is consistently associated with modulation of the host innate and adaptive immune response6,16,34,35,70 and the recruitment and differentiation of endogenous stem cells.2,22,70 However, not all studies in which ECM-based materials have been used report this type of constructive healing response.235,259 Alternative and less favorable outcomes include serous fluid accumulation at the implant site, rapid degradation of the material with associated mechanical failure in load bearing sites, or a lack of biomaterial degradation and an associated foreign body response.106,125,217,235,246,259 These alternative outcomes have typically been associated with variations in manufacturing methods and/or source tissues. A partial list of commercially available ECM bioscaffolds is provided in Table 1 to show the variability of source materials and approved clinical indications. The present manuscript provides an overview of the effects of production methods upon the quality of and cellular response to ECM bioscaffolds.
Methods of Preparation
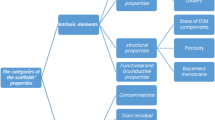
ECM bioscaffolds are typically prepared by the decellularization of mammalian tissue, either xenogeneic or allogeneic in origin, to produce a material consisting of the remaining native ECM, and the inherent signaling molecules therein. Though simple in principle, the manufacturing process of ECM biomaterials is actually quite complex and non-trivial. Considerations that must be taken into account include selection of the source tissue, method of decellularization, and inclusion of post-decellularization processing steps such as terminal sterilization or chemical crosslinking. The choices made at each step of manufacturing can markedly affect the physical and biochemical properties of the scaffold and the downstream cellular response and remodeling outcome. The characteristics of ECM bioscaffolds that can influence cell behavior are summarized in Fig. 1 and described in detail below.
Tissue Source
Species
ECM bioscaffolds are prepared by decellularization and processing of source tissues harvested from humans (allogeneic) or other (xenogeneic) species. The constituent molecules of the ECM are highly conserved across mammalian species which is one of the reasons that devices manufactured from xenogeneic ECM do not elicit an adverse inflammatory response when implanted in humans. Basement membrane proteins, such as laminin and collagen IV, are some of the most highly evolutionarily conserved proteins.116,117,141 High cross-species homology has been observed for other ECM components, including collagens,50,74 fibronectin,187 glycosaminoglycans (GAGs)118,187 and growth factors.147 Stated simply, bioactive ECM components are very similar across species; therefore similar cellular responses are elicited by allogeneic and xenogeneic bioscaffolds.131 Importantly, the host immune response and downstream constructive remodeling are also similar between ECM-based bioscaffolds derived from different species.34,35
Multiple studies have attempted to compare the cellular response to ECM scaffolds from xenogeneic and allogeneic sources.7,38,96,127,143,182,221,256 However, a systematic comparison between bioscaffolds from different species is essentially impossible due to numerous confounding variables.131,256 Commercially available biologic scaffolds can differ in the source tissue, tissue supplier, processing and sterilization methods, and packaging or storage conditions. The majority of the processing steps for commercial scaffolds are also proprietary which limits the ability to isolate specific factors that may affect the cellular response.
Allogeneic biological scaffolds are procured from cadaveric tissue and therefore allow limited control of variables that may affect the ECM properties, such as age or health status of the donor.127,131 As discussed in detail below, the age of the source tissue, decellularization protocol, and post-decellularization processing can affect the cellular response to ECM bioscaffolds. Either innate species-related or age-related changes in the ECM between species often necessitate different decellularization or processing protocols for the same tissue type harvested from different species.127
Commercially available human and porcine matrices have shown differences in the growth of fibroblasts in vitro,7 and the extent of cellular infiltration38 and rate of remodeling182in vivo. VeDepo et al. compared species-specific effects of the same decellularization protocol on aortic valve tissue from human and ovine sources.256 In this study, the same decellularization protocol was able to effectively remove cellular material from both species, despite almost triple the cell density in ovine leaflets compared to human. However, the same decellularization process induced different effects on the collagen crosslinking density, GAG content and mechanical properties of the ovine vs. human tissue.256 This study emphasizes the difficulty in isolating the species related differences in the cell response to ECM bioscaffolds.
Anatomic Site
The ECM consists of the structural and functional molecules secreted by the resident cells of an organ or tissue. Therefore the composition, structural and mechanical properties of the ECM vary widely for each tissue and organ.132,140,164,276 As a result of these organ-specific differences in structure and composition, the isolation of ECM from diverse anatomic sites typically requires a tissue specific decellularization protocol. As described above, dissimilarities in the processing of ECM from different tissue anatomic locations makes direct comparison of ECM properties between tissues a challenging task. The native ECM of a tissue is the optimal substrate for survival, differentiation and function of the resident cells. Intuitively it would seem that exogenously implanted ECM bioscaffolds from the same tissue anatomic location (homologous) should provide advantages and improved outcomes compared to non-homologous ECM. However, in reality the impact of the anatomic site of ECM source tissue (homologous vs. heterologous) is often non-intuitive and not predictable.
Depending on the context or specific outcome measured, homologous ECM has been reported to be superior,56,132,140,164,218,275,293 similar56,132,140,276 or even inferior77 to heterologous ECM. For example, Keane et al. compared the response of esophageal stem cells to hydrogels derived from homologous esophageal mucosa ECM and heterologous small intestinal submucosa (SIS-ECM) and urinary bladder (UBM-ECM).132 Each tissue type had a distinct protein profile as indicated by gel chromatography. In vitro homologous esophageal ECM promoted migration of esophageal stem cells and formation of significantly more esophageal organoids than both heterologous ECM types. However, there was no difference in the size or number of proliferating cells within an individual organoid between esophageal ECM and UBM-ECM. In vivo, esophageal ECM and UBM-ECM promoted essentially identical remodeling of the esophageal mucosa.132 This study suggested that homologous ECM does maintain some site-specific favorable properties of the native tissue, but these properties may contribute only minimally to the overall remodeling response.
The cell and host response to ECM derived from source tissue of different heterologous anatomic sites also varies. The biochemical composition of ECM hydrogels prepared from a wide range of heterologous tissue sources can promote different activation states of macrophages in vitro.72,166 The mechanical properties of ECM prepared from different anatomic locations varies widely and can be misleading with respect to expected performance in different clinical applications. ECM bioscaffolds derived from dermis are stronger than UBM-ECM and SIS-ECM bioscaffolds. However, despite differences in pre-implantation strength, UBM-ECM285 and SIS-ECM149 have both been reported to promote equivalent strength of the implantation site as dermis ECM following tissue integration. Further, the ECM scaffolds derived from dermis showed little tissue incorporation and a poor remodeling outcome compared to UBM-ECM285 and SIS-ECM.149
Age of Source Animal
The age of the source tissue donor affects the mechanical properties and composition of the resulting ECM bioscaffold.153,154,214,230,245,270,271,274 The ECM of fetal and neonatal tissues is enriched in GAGs such as hyaluronic acid152,214,244,264 and fibronectin153 compared to adult ECM. Laminin,97 elastin,97,264 and growth factor245 content is reduced with age. The collagen of young animals contains fewer crosslinks than that of adult ECM155; a factor that contributes to more rapid degradation of young ECM compared to the ECM of adults.245
The changes that occur within the native ECM during aging have a direct effect on the in vitro and in vivo cellular response and remodeling outcome of decellularized ECM bioscaffolds prepared from these tissues. The first systematic examination of the effect of source animal age was performed by Tottey et al.245 SIS-ECM bioscaffolds were produced from pigs that differed only in age (3, 12, 26, or > 56 weeks old). Differences in the physical and compositional properties of the scaffolds were associated with a distinct cellular response in vitro. The ECM from 52 weeks old animals was significantly less chemotactic for perivascular stem cells than the ECM harvested from younger 12 weeks old animals.245 ECM derived from old animals promoted an altered macrophage phenotype associated with reduced expression of both pro- and anti-inflammatory markers compared to ECM from younger animals in vitro.154 In a pro-inflammatory environment, macrophages treated with ECM from 52 weeks old animals had significantly increased pro-inflammatory iNOS expression, decreased MHC-II expression, and decreased nitric oxide production compared to macrophages treated with ECM from 12 weeks old animals.154
The host response and remodeling outcome to equivalent SIS-ECM scaffolds were evaluated in vivo following implantation in a rat model of abdominal wall repair.227 ECM harvested from 3 to 12 week old pigs promoted the formation of more site appropriate skeletal muscle than ECM from older pigs. This constructive remodeling response to young ECM was associated with a predominately anti-inflammatory (M2-like) macrophage phenotype. Implanted scaffolds derived from 52 weeks old animals elicited limited cellular infiltrate that did not completely penetrate the thickness of the scaffold, and the macrophages that did infiltrate the matrix comprised a balance of pro-inflammatory (M1-like) and anti-inflammatory (M2-like) phenotypes. At 6 months post implantation of the 52 weeks old ECM, the site was characterized by deposition of a dense collagenous connective tissue with no evidence of innervation or new skeletal muscle formation, a stark contrast to the response to ECM from younger animals.227
The impact of source animal age has also been demonstrated in the heart. ECM derived from the heart of fetal mice promoted increased adhesion and expansion of neonatal cardiomyocytes230,274 and heart-derived progenitor cells230in vitro compared to adult mouse heart ECM. ECM from the hearts of neonatal mice promoted angiogenesis and increased endothelial cell activity compared to adult heart ECM both in vitro and in vivo.264 In a mouse model of myocardial infarction, a single injection of neonatal heart ECM into the ventricle resulted in significantly improved dimensional and functional parameters at 6 weeks compared to adult heart ECM.264 Neonatal ECM also significantly reduced fibrosis, ventricular stiffening and the chronic inflammatory response. The injection of adult mouse heart ECM did not show any significant improvement compared to saline control in any of the parameters evaluated.264
Decellularization Efficiency
The ultimate goal of decellularization is the removal of all cellular components from the source tissue while preserving the complex structure and composition of the native ECM. In reality however, any process that disrupts and removes the cellular components of a tissue will alter the ECM ultrastructure and composition to some extent. Complete removal of all cellular remnants is not possible because of the intimate relationship between cell membranes and the surrounding matrix, the adhesive nature of the negatively charged nucleic acids, and the entrapment of cell debris within the structural matrix molecules. However, a balance between thorough removal of cells and maintenance of ECM integrity must be achieved to avoid a pro-inflammatory response when the ECM-based material is used as a biologic scaffold. The optimal decellularization method for each tissue depends on multiple variables including the tissue source, size, thickness, morphology, and cell and matrix density.273
Adequate Removal of Cellular Material
Failure to adequately remove cellular material promotes an intense inflammatory response in the recipient that is associated with poor downstream tissue remodeling.134,150,209 Keane et al. compared SIS-ECM produced by three different decellularization protocols and showed that more effective removal of DNA was associated with a more favorable host tissue response in a rodent model of body wall repair.134 However, DNA content is not the only determinant of the host response to ECM scaffolds: mitochondria and cell membrane remnants also induced a pro-inflammatory response in a dose dependent manner in vivo.150 There are likely many other yet to be identified quantifiable indicators of decellularization efficiency. The value in identifying such indicators is significant and additional work in the area is needed.
Although there are no standard criteria by which to determine adequate decellularization of a source tissue to produce an ECM biomaterial, Crapo et al. have suggested three quantitative criteria: (1) lack of visible nuclei in tissue sections stained with 4’,6-diamino-phenylindole (DAPI) and hematoxylin and eosin, (2) < 50 ng of double-strand DNA per mg of dry weight ECM, and (3) fragment length of remnant DNA < 200 base pairs.55 These criteria are relatively stringent and may be too conservative for certain tissue types or applications.53 In fact, many commercially available ECM scaffold materials fail to meet these criteria and are still associated with largely positive clinical outcomes.89,190
Preservation of ECM Structure and Composition
The specific decellularization protocol can have dramatic effects on the mechanical and biological properties of the resulting scaffold.146,148,157,199 A detailed description of the most commonly used decellularization agents and techniques and their effect on the ECM can be found in reviews specific to this topic.55,95,135 In general, decellularization protocols consist of a combination of physical and chemical treatments.
Physical methods such as sonication, freezing/thawing, and direct application of pressure or force are commonly used to disrupt cell membranes and facilitate the release of cellular remnants from the scaffold. Physical methods can directly disrupt the structure of the ECM, but otherwise cause minimal damage to the composition and bioactivity of the material and therefore are safely incorporated into tissue processing protocols.135
Chemical methods are generally more damaging to the ECM ultrastructure and molecular integrity than physical methods. However, use of these agents is often necessary to achieve adequate removal of cell debris. Each chemical agent has a unique mode of action in aiding cell removal and therefore has a different effect on the resulting ECM bioscaffold. Detrimental effects on the ECM can include removal of growth factors and GAGs, damage to collagen, and crosslinking of ECM proteins. Ionic detergents such as sodium dodecyl sulfate (SDS) and sodium deoxycholate (DOC) are effective decellularization agents but unavoidably alter critical ECM components such as basement membrane proteins and GAGs.75,199,231 Non-ionic detergents such as CHAPS and zwitterionic detergents such as Triton-X 100 are less disruptive than SDS and DOC but also have detrimental effects upon composition and molecular integrity.75,170,200,231 Exposure to solvents such as alcohols are typically included as a step in the decellularization of tissues with a high lipid content, including brain, pancreas and adipose.33,56,164
The use of supercritical carbon dioxide as a decellularization agent is increasingly common and could represent an attractive approach which has relatively less disruptive effects.40,100,112,213,219,265,287 The low viscosity and high transport rate characteristic of supercritical fluids enable short and simple decellularization protocols and the inert carbon dioxide causes minimal alteration of the ECM mechanical properties.40,112,135,213,265
Not only can the combination of decellularization reagents change for each protocol, the concentration, duration, sequence of treatment, and technique for application are additional variables to consider. The complexity and duration of the overall decellularization protocol is often related to the geometric conservation desired in the ECM product (i.e. small pieces or slices vs. intact whole organ).55 In general, thin laminate tissues such as urinary bladder, small intestine, pericardium and amnion can be sufficiently decellularized with mechanical disruption followed by relatively mild detergents or acids.81,85,135,253 Tissues that are more dense, such as dermis or myocardium, often require exposure to harsh enzymes (e.g. trypsin) and ionic detergents (e.g. DOC, SDS) for extended periods of time.126,199,220,275 When access to intact vasculature is possible, removal of cellular material can be achieved by perfusion of the decellularization agent through the whole organ.27,76,195
An often overlooked consequence of the use of such detergents is the necessity for thorough rinsing to remove residual detergent that can negatively impact the cellular response to the material.42,273 A study by White et al. used time of flight secondary ion mass spectroscopy (ToF–SIMS) to detect residual detergents following decellularization of a UBM-ECM scaffold. Detergent fragments of DOC, SDS, and Triton X-100 were detected in the scaffolds despite extensive washing. Residual SDS in particular was associated with abnormal phenotype, poor viability and low confluence of cells in a dose dependent manner in this study273 and in other studies.201,210,266
Post-Decellularization Processing
Physical Form
The physical form of the ECM can dictate the relevant clinical applications of the ECM-based product, and can also directly impact the cellular response.73 Immediately following the decellularization process, the ECM is typically in a hydrated state. Maintaining hydration of the ECM through the decellularization process better preserves the structural protein architecture (e.g., collagen) and promotes improved cellular infiltration and attachment compared to dehydrated/rehydrated scaffolds.86 However the hydrated ECM is susceptible to continuous elution of soluble bioactive molecules such as cytokines and growth factors.199 ECM-based bioscaffolds are therefore typically dehydrated by lyophilization to minimize the loss of soluble factors and improve stability (e.g., shelf life). Dehydration of the ECM also allows for further processing to change the physical form or configuration of the material.
Commonly used ECM-based medical devices such as those composed of SIS, UBM and dermis, are usually in a two-dimensional sheet configuration. Single-layer SIS-ECM and UBM-ECM sheets have a distinct “sided-ness” that can affect cellular behavior on the surface.32 However single-layer SIS-ECM and UBM-ECM often lack the mechanical strength required for load-bearing applications such as body wall repair.91,246,252 One method to increase the strength of the material is lamination of multiple sheets of ECM by vacuum pressing.81,84 The multilaminate material can be specifically designed to minimize anisotropy of a single sheet (i.e. by altering the orientation of each layer), and to either maintain or eliminate the sidedness of the exposed layers.9 Vacuum pressing can also be used to create 3-D shapes to fit an anatomical location such as the gastroesophageal junction or esophagus.9
Single or multilayered sheet forms of the ECM have limitations of their clinical utility due to their fixed geometry and inability to be implanted by minimally invasive procedures. A powder or particulate form of the ECM can be obtained by comminution of the lyophilized sheet form of the material. The particle size, homogeneity and ultrastructure of the material depend on the source of the ECM and the method used to produce the powder.92 The powder form retains the micro and ultrastructural characteristics of the parent ECM, but has greatly increased surface area available to interact with host cells.92 Further, the powder configuration allows for manufacture of a compact 3-D scaffold,71,225 delivery by topical application,137,202,294 or injection of a suspension.47,207,234,238,279 ECM powder suspensions have been successfully administered by injection, but the needle size required to accommodate the particle can be prohibitive for certain clinical applications, and a carrier such as glycerin is often required to increase the viscosity.9,279
The discovery that the ECM could be manufactured into a liquid or gel form has greatly expanded its potential use in vitro and in vivo. The gel form can be more readily passed through a needle or catheter than a suspension of particles and can conform to the 3-D space upon injection.82,232 The hydrogel form is produced first by solubilization of the ECM material into protein monomeric components (“pre-gel”) followed by spontaneous reformation of the intramolecular bonds into a hydrogel upon neutralization to physiologic conditions and exposure to body temperature (37 °C).30,82,208 The most prevalent method of solubilization into the pre-gel form is enzymatic digestion of the powdered ECM with pepsin in a dilute acid solution,82,258 although other techniques have also been used.248 Entropy-driven self-assembly into the hydrogel form occurs following neutralization of the pH and salts to physiologic conditions and raising the temperature to 37 °C. Importantly, these properties allow delivery of the neutralized pre-gel as a viscous solution to an anatomic location where it will subsequently gel in situ. The gelation kinetics and mechanical properties of ECM hydrogels depend on multiple factors including tissue source, pre-gel concentration and neutralization conditions.128,145,151,248,275 The formulation, characterization and cellular response to ECM hydrogels have been extensively reviewed elsewhere.208,239,261
Chemical Crosslinking
Chemical crosslinking agents are frequently included in the processing of biologic scaffolds as a method to increase the mechanical strength and decrease the rate of degradation.158,189,267 It should be noted that significant natural crosslinks exist within the structural molecules (such as collagen) of the native ECM. Chemically mediated crosslinking has also been investigated as a method to mask antigenic epitopes within the ECM after the decellularization process,54,180 although credible citations for the specific molecular basis and rationale of this approach cannot be found. In certain applications the use of chemical crosslinking may be justified and successfully implemented,25,46,123,158,212 but in general there are more negative consequences than positive consequences.
Glutaraldehyde is the most commonly described approach to crosslinking collagen-based materials, including ECM bioscaffolds. Glutaraldehyde increases the mechanical strength of scaffolds. However, glutaraldehyde is also associated various adverse effects including cellular toxicity and mineralization of the implanted material.4,159,215,233 Alternative crosslinking strategies have been investigated, primarily to mitigate cytotoxic effects. A wide range of crosslinking agents, including genipin,17,25,46,242,260,269 carbodiimide,16,43,185,252 hexamethylene diisocyanate (HMDI),185,252 glyoxal,31 and vitamin B2123 have been considered and have generally shown improved biocompatibility compared to glutaraldehyde. The mechanism of action of the various crosslinking agents differs and can therefore confer specific effects on the surface characteristics and microstructure of the material. For example, carbodiimide crosslinked UBM-ECM scaffolds are associated with a dense, compact fiber network with small pore size.32 Glutaraldehyde crosslinked ECM-based bioscaffolds produce thick bundles of collagen but maintain a similar pore size to that of non-crosslinked UBM-ECM.32
Regardless of the agent used, the very nature of crosslinking changes the cellular response to the ECM scaffold. The process of ECM scaffold degradation generates bioactive cryptic peptides and releases embedded growth factors, cytokines and ECM-associated extracellular vesicles, termed matrix-bound nanovesicles (MBV), that contain protein, microRNA and lipid cargo.115 These degradation products have been associated with chemoattraction of progenitor cells, recruitment and subsequent activation of macrophages toward a pro-remodeling phenotype, promotion of angiogenesis and antimicrobial activity. By definition, changing the degradation behavior of the ECM through crosslinking changes the release profile of these bioactive degradation products thereby eliciting a distinct, and often unfavorable, response. Finally, delaying or preventing ECM-based bioscaffold degradation results in a foreign body reaction.34,54,61,278
The detrimental effects caused by chemical crosslinking of ECM bioscaffolds have been extensively studied, particularly in the context of soft-tissue repair. Multiple studies have evaluated commercially available scaffolds in a rat model of partial thickness abdominal wall repair.16,34,252 The source tissue, bioscaffold configuration and processing methods that have been investigated vary widely. In all cases, chemical crosslinking of the ECM device has led to a poor remodeling outcome. Commercially available ECM products that are chemically crosslinked were invariably associated with the presence of multinucleate giant cells252 and chronic foreign body response with associated fibrous encapsulation.34,252 The same rat model has also been used to evaluate the effect of carbodiimide crosslinking upon scaffolds composed of SIS-ECM253 and ACell MatriStem®, a commercially available UBM-ECM product.278 Carbodiimide crosslinking was associated with minimal cellular infiltration into the scaffold,253 a predominately pro-inflammatory macrophage phenotype,278 and no evidence of degradation or remodeling of the scaffold.253
Small animal,101,129,130,169,177 large animal37,41,165 and human clinical studies44 have all shown potential disadvantages of chemically crosslinked ECM scaffolds for ventral hernia repair. Implantation of non-crosslinked ECM scaffolds have been associated with significantly lower adhesion surface area and adhesion tenacity compared to crosslinked ECM scaffolds in both rat129,177 and guinea pig37 models of ventral hernia repair. Hernia repair in Yucatan minipigs showed greater cellular infiltration, ECM deposition and neovascularization for non-crosslinked scaffolds at 1 month post-surgery,41,165 consistent with improved early remodeling. No significant differences were observed in the strength of the repair site at 1 month41,165 or at 12 months41 between crosslinked and non-crosslinked scaffolds, despite greater mechanical strength of crosslinked scaffolds at the time of implantation.
Pre-clinical studies have also found that Strattice™ (non-crosslinked porcine dermis ECM) is less susceptible to infection177 and is better able to clear bacteria101 in a deliberately contaminated surgical area compared to Permacol™ (crosslinked porcine dermis ECM). A retrospective review was conducted of patients who underwent abdominal wall hernia repair with Strattice™ and Permacol™.44 Non-crosslinked Strattice™ was associated with a significantly lower overall short-term complication rate, including significantly fewer occurrences of wound infection compared to Permacol™.44 A recently registered clinical trial will be the first randomized controlled study to evaluate the rate of recurrence and postoperative complications for Permacol™ vs. Strattice™ in abdominal wall reconstruction.39
Terminal Sterilization
The large majority of ECM-based biologic scaffolds are classified as a surgical mesh with the primary mechanism of action being “to provide reinforcement for soft tissue where weakness exists”, and therefore are regulated as a medical device by the Food and Drug Administration (FDA). According to the International Organization for Standardization (ISO) medical devices should be terminally sterilized to achieve a log10 reduction in virus sufficient to produce a safe product wherever possible, but aseptic processing can be used as an alternative (ISO 22442-1, ISO 13408-1).119,120 Though current FDA guidelines include case-by-case validation of sterilization of devices derived from animal tissue due to their complexity, terminal sterilization remains the standard for ECM bioscaffolds.250 Allografts composed of human ECM are considered “human cells, tissues, and cellular and tissue-based product” (HCT/P) by the FDA and are therefore not required to be sterile. The industry standard for HCT/P includes the use of aseptic technique during harvesting and processing to prevent contamination.249
Terminal sterilization is performed following the physical methods of tissue preparation, the decellularization process, and the occasional use of disinfection agents. Chemical disinfection agents (e.g., hydrogen peroxide or peracetic acid) can cause oxidation of ECM proteins and alter cross-linking patterns of collagen fibers,107 but the altered ECM can still support cell attachment.108,163 Terminal sterilization processes can alter the ultrastructure, biologic activity and mechanical properties of an ECM bioscaffold which in turn can affect the cellular response to the material. Heat-based sterilization methods cannot be used for ECM bioscaffolds because the majority of ECM proteins are subject to irreversible denaturation at temperatures between 60 and 65 °C.53 The most commonly used methods of terminal sterilization for ECM bioscaffolds are ionizing radiation and ethylene oxide.
The effect of exposure to ionizing radiation, including electron beam and gamma irradiation, on ECM bioscaffolds has been investigated. Low doses of gamma irradiation (< 15 kGy) have been reported to increase the strength and stiffness of the scaffold,99 but higher doses decrease the mechanical properties in a dose dependent manner.60,99 Gamma irradiation can induce structural247 and biochemical60,211 changes in the scaffold. Even very low doses of irradiation can affect collagen crosslinking241 and the scission of collagen chains increases with dose.18 Gamma irradiation can also negatively impact cell attachment163 and induce cell death due to peroxidation of residual lipids in the scaffold.174 Dearth et al. found that increasing the dose of gamma and electron beam irradiation to 40 kGy adversely affected the material properties and changed the degradation rate and cellular response to a porcine dermis ECM scaffold in vivo.60
The reported effects of ethylene oxide (EtO) sterilization on ECM scaffolds are variable and depend on the parameters of each study. Exposure to EtO can have minimal effects on the mechanical properties60,85,121 or can substantially increase the stiffness of the scaffold.203 EtO sterilization did not affect the attachment or activity of fibroblasts107 or endothelial cells60in vitro, but did inhibit cell attachment, proliferation, and viability of human umbilical cord Wharton’s Jelly matrix cells compared to a non-sterilized scaffold.163 EtO reduces the DNA, total protein and growth factor content compared to other sterilization methods60 and can render proteins inactive or undetectable by alkylation.64 EtO treatment has the potential to leave behind harmful residues within the ECM that can cause an adverse host immune response and poor remodeling outcome,122 but has also been shown to successfully promote a constructive remodeling response in a rodent model of abdominal wall repair.60
Sterilization by supercritical carbon dioxide is prevalent in food and pharmaceuticals,229 and is emerging as a promising technique for ECM bioscaffolds. Supercritical carbon dioxide sterilization has been shown to successfully inactivate a large panel of microorganisms.24 Exposure of ECM scaffolds to supercritical carbon dioxide has shown minimal damage to the mechanical properties, tissue architecture and ECM content.19,24,104,287 Bioscaffolds sterilized by this method support cell viability and proliferation in vitro.19,24,287 Supercritical carbon dioxide has also recently been shown to successfully sterilize a hydrogel form of ECM while maintaining the ability of the solubilized ECM to form a gel and exert known effects upon macrophages and perivascular stem cells.272 The host response to supercritical carbon dioxide sterilized ECM scaffolds has yet to be evaluated in vivo.
Favorable Cellular Response to ECM Bioscaffolds
As described in detail above, there are many factors that contribute to the overall quality of an ECM bioscaffold and each of these can affect the host response to the material. The seemingly endless variables involved in producing an ECM scaffold and the wide range of clinical applications make the definition of an “ideal” ECM bioscaffold impossible. However, when close attention is given to the variables known to affect the host response the chance for a favorable outcome can be maximized.
The term “constructive remodeling” has been used to describe the in vivo events that occur following implantation of a thoroughly decellularized, sterile ECM bioscaffold.8,11,35,69,162,254 Constructive remodeling is characterized by degradation and gradual replacement of the bioscaffold with site appropriate functional tissue. This type of in vivo response to an implanted biomaterial is in stark contrast to the default wound healing response that is associated with a pro-inflammatory environment and the deposition of dense scar tissue.
As stated in the introduction, the remodeling outcomes following ECM bioscaffold implantation have not always been constructive.106,125,217,235,246,259 A mild or intense inflammatory response and/or a serous fluid accumulation have occurred with associated scar tissue formation as occurs with the default wound healing response. Such results are commonly associated with ECM-based products that have significant cell remnants, residual chemicals from disinfection and decellularization processes, or the use of chemical crosslinking methods that alter structural and functional protein constituents and that inhibit or delay degradation of the scaffold.34,35,134,150,175
Though the specific mechanisms by which ECM bioscaffolds promote a positive constructive tissue remodeling are not fully understood, the following processes are consistently associated with such outcomes: (1) degradation of the ECM bioscaffold to release bioactive signaling molecules,3,58,253 (2) modulation of the host immune response toward a pro-remodeling and regulatory type 2 phenotype,6,16,34,35,70 and (3) recruitment and differentiation of endogenous stem/progenitor cells.2,22,71 The potential favorable response of immune cells and stem/progenitor cells to ECM bioscaffolds is described in detail below.
Immune Cells
Implantation of any material, including ECM scaffolds, is associated with the immediate adsorption of proteins to the surface. Competitive protein exchange results in a dynamic mixture of adsorbed proteins (Vroman effect).105 At early time points the composition is dominated by high concentration proteins that are eventually displaced by proteins with a higher affinity for the implanted material. Protein adsorption is followed by activation of the innate immune response, including dendritic cells, neutrophils and macrophages.10,48 The adaptive immune system consisting of lymphocytes (B and T cells) may also be activated depending on the type of the biomaterial.79,173 Both macrophages and T helper cells can assume diverse phenotypes that are characterized by their gene and protein expression profiles, and associated functions. In simplified terms, a pro-inflammatory phenotype of macrophages and T helper cells is associated with expression of cytotoxic signaling molecules, and a pro-healing phenotype is associated with anti-inflammatory and regulatory signaling molecules.23,98,160,161,171,176 ECM-based biomaterials that are devoid of cellular material, retain the ultrastructure and bioactive components of the native ECM, and that can be readily degraded by infiltrating host cells have been repeatedly shown to stimulate a strong pro-healing phenotype of both the adaptive and innate immune systems.6,16,34,35,70
A seminal study by Allman et al. in 2001 showed that there is a robust host immune response to implanted ECM bioscaffolds with activation of T helper cells to a “Th2” phenotype. Implantation of porcine-derived ECM in a murine host elicited production of anti-inflammatory cytokines, including interleukin (IL)-4 and IL-10, and noncomplement fixing IgG1 antibody isotype. Both of these responses were consistent with recognition of the presence of the biomaterial, acceptance of the decellularized xenogeneic scaffold, and lack of an adverse immune response. The constructive remodeling response to the scaffold was reported as T cell independent in this model although macrophage participation and macrophage phenotype were not examined.5 Importantly, the strong Th2 response induced by ECM scaffolds was maintained following a secondary exposure to the scaffold5 and therefore was not associated with an adverse sensitization phenomenon. The same group subsequently showed that ECM bioscaffold implantation did not cause generalized immune suppression, did not impair the antibody-mediated immune response to viral or bacterial infection, and did not impair the cell-mediated immune response to contact or xenogeneic skin graft rejection.6
In 2009 Valentin et al. showed that ECM bioscaffolds induce a favorable host innate immune response, specifically the macrophage phenotype component of the innate response. This macrophage response was not only sufficient but was required for constructive remodeling of the scaffold.253 Further, the early macrophage phenotypic profile induced by degradation of an ECM bioscaffold in vivo was predictive of downstream remodeling responses.34 That is, increased infiltration of M2-like CD206+ macrophages and higher ratios of M2:M1 macrophages within the implantation site at 14 days were associated with more positive remodeling outcomes.34 Macrophages exposed to the degradation products of ECM bioscaffolds can directly activate macrophages towards an anti-inflammatory M2-like (iNOS−/Fizz1+) phenotype.72,226 The ECM-induced macrophage phenotype has been extensively characterized and is broadly associated with upregulation of anti-inflammatory genes and proteins,71,78,206 downregulation or suppression of pro-inflammatory genes and proteins,114,133 high antigen presenting capabilities205 and expression of damage associated molecular patterns (DAMPs).207 Increased expression of DAMPs is hypothesized to contribute to a constructive wound healing response by amplifying endogenous wound-associated signaling pathways.207
The macrophage phenotype induced by ECM bioscaffolds is complex and varies depending on the source and/or processing of the ECM.72,114,205 The phenotype in response to ECM scaffolds is distinct from that induced by IFNγ + LPS (classically activated), IL-4 (alternatively activated), cellular xenogeneic scaffolds and synthetic scaffolds.114,207 Importantly, the phenotype elicited by ECM-based bioscaffolds is different from that of tumor associated macrophages, another subset of M2 macrophages.277 The activation of M2-like macrophages by ECM bioscaffolds is dependent on the presence of Th2 cells.206,277 Although the exact mechanisms by which the ECM promotes a type 2-like immune response is only partially understood, it is known that degradation of the ECM and subsequent release of cryptic peptides, growth factors, MBV, and other bioactive molecules is required. Huleihel et al. showed that MBV alone can recapitulate the immunomodulatory properties of the parent ECM.113,115 Whole UBM-ECM as well as isolated UBM-MBV can also activate microglia, the resident macrophages of the central nervous system, to an anti-inflammatory type 2 phenotype.77,255
Recent studies have characterized the ECM-induced immune cells infiltrating within the bioscaffold and within the adjacent native tissue in detail with a multicolor flow cytometry panel and have shown robust populations of macrophages, dendritic cells, T cells and B cells.205,206,–207 The overall profile of infiltrating immune cells was significantly different between ECM bioscaffolds prepared from different source tissues (bone, cardiac, liver, spleen and lung), but the general pattern was very similar.205 ECM bioscaffolds elicited a higher proportion of T helper cells than cytotoxic T cells.205,206,263 Regulatory T cells (Tregs) were also recruited to the site of implantation and were associated with increased levels of anti-inflammatory IL-10 cytokine secretion compared to autograft or saline.78,103,205,206
Wang et al. used a humanized mouse model to characterize the temporal human immune response to xenogeneic and allogeneic decellularized myocardial ECM hydrogels. Although both decellularized scaffolds elicited a Th2 and M2-like macrophage phenotype, the quantity of cells and Th2 phenotype were more robust in response to the xenogeneic scaffold compared to the allogeneic scaffold. However, it is unknown if the amplified type 2 response was due to the xenogenecity of the bioscaffold or to differences in the source tissue, including older source age, greater collagen crosslinking and a more vigorous decellularization protocol associated with the allogeneic ECM.263
Stem and Progenitor Cells
ECM bioscaffolds, or more specifically the products of ECM bioscaffold degradation, have been shown to be chemotactic for stem and progenitor cells in vitro and in vivo.22,29,56,200 Implantation of ECM bioscaffolds promotes recruitment of marrow-derived progenitor cells,14,288 cardiomyocyte progenitor cells,136,268,291 skeletal muscle interstitial stem cells,194 and perivascular stem cells to the site of implantation.71,228
Perivascular stem cells (PVSC) are typically found surrounding microvessels and capillaries and can contribute to remodeling of acute skeletal muscle injury and contribute to the satellite cell pool if mobilized outside of their normal niche.65 Implantation of an SIS-ECM bioscaffold in a volumetric skeletal muscle defect promoted mobilization of perivascular stem cells away from their normal perivascular niche to the site of the defect in both a rodent model and in human patients.71,228 SIS-ECM implantation resulted in significantly more CD146+ PVSC both at the margin and the center of the remodeling ECM within the defect site and was associated with subsequent formation of functional vascularized and innervated striated functional muscle.71,228 Although the specific mechanism directing stem cell recruitment is not known, cryptic peptides from the α subunit of collagen III recapitulate progenitor cell chemotaxis in vitro and site-directed accumulation in vivo.3
The ability of ECM bioscaffolds to support stem cell differentiation or commitment towards a specific lineage is well established and has recently been reviewed in detail.1 ECM derived from adipose,33,156,191,283,284 bone,102,240 central nervous system,17,56,67,164 cartilage,45,46,191,243,251,257,280 heart,66,68,80,83,87,127,197,230 kidney,27,36,186,204 liver,20,21,124,144,181,289 lung,52,57,94,179,222,224,292 salivary gland,223 skeletal muscle,66,110,193,194,228,262 tendon,188,281,282,286,290 among other tissues63,109,167,172,178,192 have been studied in the context of stem cell differentiation. This concept is based upon the premise that the ECM of each tissue represents the secreted product of the cells that reside within that tissue, possesses tissue specific biologic signals, and is therefore the ideal substrate for supporting cell attachment, growth, and homeostatic differentiation.26,29,132 These same concepts are part of the tissue organization field theory (TOFT) that, in part, supposes that the microenvironment created by the ECM facilitates either a normal or neoplastic differentiation state.236,237 ECM prepared in several different forms (whole organ, tissue slices, hydrogel, coating) have been investigated for their differentiation effects upon cells ranging from pluripotent embryonic stem cells to tissue specific progenitor cells.1 ECM-induced stem cell differentiation in the context of the heart will briefly be described to highlight the potential of the ECM and bioscaffolds composed of ECM in directing cell fate.
In multiple contexts and culture systems, ECM derived from the myocardium has been shown to support cardiac cell differentiation or maturation. Gaetani et al. showed that 3D culture in a hydrogel from porcine ventricular ECM could support cardiogenic differentiation of human adult and fetal cardiac progenitor cells.87 The myocardial matrix hydrogel promoted increased gene expression of cardiac markers (GATA-4 and MLC2v) and vascular marker (VEGFR2) in fetal cardiac progenitor cells. Expression of early cardiac markers (Nkx2.5 and MEF2c) and vascular markers (VEGFR2 and CD31) were also increased in adult cardiac progenitor cells after 4 days in culture within myocardial ECM hydrogel compared to a collagen type I hydrogel. The ECM hydrogel supported increased proliferation of the progenitor cells, and cells cultured within the myocardial matrix were better able to maintain viability in an environment of oxidative stress induced by hydrogen peroxide. This study demonstrated that a cardiac-specific hydrogel could enhance the cardiogenic commitment, proliferation and survival of human cardiac progenitor cells in 3D culture.87
Though ECM bioscaffolds are most commonly used as a tool to help direct stem cell differentiation or commitment towards a specific lineage, one study instead looked at the ability of ECM to maintain an undifferentiated phenotype. De Waele et al. used decellularized mouse brain ECM sections as a 3D substrate for culture of rat neural stem cells.59 In the presence of mitogenic stimuli (epidermal growth factor and human basic fibroblast growth factor), the majority of seeded neural stem cells retained their stemness and did not differentiate towards astrocytes or neurons after 7 weeks in culture.59
Summary
Bioscaffolds composed of mammalian ECM have the potential to facilitate favorable remodeling processes in a wide range of clinical applications. The mechanisms by which ECM mediates constructive tissue remodeling include degradation and generation of bioactive molecules, recruitment and differentiation of endogenous stem and progenitor cells, and modulation of the immune response, among others. These positive outcomes are critically dependent upon the methods used to manufacture the ECM material. As described above, the source of the tissue, decellularization protocol and inclusion of additional processing steps affect the cellular response and remodeling outcome elicited by ECM bioscaffolds. Commercially available ECM products vary in their manufacturing methods and therefore can be associated with markedly different clinical outcomes.
Abbreviations
- ECM:
-
Extracellular matrix
- SIS:
-
Small intestinal submucosa
- UBM:
-
Urinary bladder matrix
- GAGs:
-
Glycosaminoglycans
- SDS:
-
Sodium dodecyl sulfate
- DOC:
-
Sodium deoxycholate
- ToF–SIMS:
-
Time of flight secondary ion mass spectroscopy
- HMDI:
-
Hexamethylene diisocyanate
- MBV:
-
Matrix bound nanovesicles
- FDA:
-
United States Food and Drug Administration
- ISO:
-
International Organization for Standardization
- HCT/P:
-
Human cell and tissue product
- EtO:
-
Ethylene oxide
- TOFT:
-
Tissue organization field theory
- DAMPs:
-
Damage associated molecular patterns
- PVSC:
-
Perivascular stem cells
References
Agmon, G., and K. L. Christman. Controlling stem cell behavior with decellularized extracellular matrix scaffolds. Curr. Opin. Solid State Mater. Sci. 20:193–201, 2016.
Agrawal, V., S. A. Johnson, J. Reing, L. Zhang, S. Tottey, G. Wang, K. K. Hirschi, S. Braunhut, L. J. Gudas, and S. F. Badylak. Epimorphic regeneration approach to tissue replacement in adult mammals. Proc. Natl. Acad. Sci. USA 107:3351–3355, 2010.
Agrawal, V., S. Tottey, S. A. Johnson, J. M. Freund, B. F. Siu, and S. F. Badylak. Recruitment of progenitor cells by an extracellular matrix cryptic peptide in a mouse model of digit amputation. Tissue Eng: Part A 17:2435–2443, 2011.
Aguiari, P., L. Iop, F. Favaretto, C. M. L. Fidalgo, F. Naso, G. Milan, V. Vindigni, M. Spina, F. Bassetto, A. Bagno, R. Vettor, and G. Gerosa. In vitro comparative assessment of decellularized bovine pericardial patches and commercial bioprosthetic heart valves. Biomed. Mater. 12:015021, 2017.
Allman, A. J., T. B. McPherson, S. F. Badylak, L. C. Merrill, B. Kallakury, C. Sheehan, R. H. Raeder, and D. W. Metzger. Xenogeneic extracellular matrix grafts elicit a Th2-restricted immune response. Transplantation 71:1631–1640, 2001.
Allman, A. J., T. B. McPherson, L. C. Merrill, S. F. Badylak, and D. W. Metzger. The Th2-restricted immune response to xenogeneic small intestinal submucosa does not influence systemic protective immunity to viral and bacterial pathogens. Tissue Eng. 8:53–62, 2002.
Armour, A. D., J. S. Fish, K. A. Woodhouse, and J. L. Semple. A comparison of human and porcine acellularized dermis: Interactions with human fibroblasts in vitro. Plast. Reconstr. Surg. 117:845–856, 2006.
Badylak, S. F. The extracellular matrix as a biologic scaffold material. Biomaterials 28:3587–3593, 2007.
Badylak, S. F., D. O. Freytes, and T. W. Gilbert. Extracellular matrix as a biological scaffold material: Structure and function. Acta Biomater. 5:1–13, 2009.
Badylak, S. F., and T. W. Gilbert. Immune response to biologic scaffold materials. Semin. Immunol. 20:109–116, 2008.
Badylak, S. F., T. Hoppo, A. Nieponice, T. W. Gilbert, J. M. Davison, and B. A. Jobe. Esophageal preservation in five male patients after endoscopic inner-layer circumferential resection in the setting of superficial cancer: A regenerative medicine approach with a biologic scaffold. Tissue Eng. Part A 17:1643–1650, 2011.
Badylak, S. F., P. V. Kochupura, I. S. Cohen, S. V. Doronin, A. E. Saltman, T. W. Gilbert, D. J. Kelly, R. A. Ignotz, and G. R. Gaudette. The use of extracellular matrix as an inductive scaffold for the partial replacement of functional myocardium. Cell Transplant. 15(Supp 1):S29–S40, 2006.
Badylak, S. F., B. Kropp, T. McPherson, H. Liang, and P. W. Snyder. Small intestional submucosa: A rapidly resorbed bioscaffold for augmentation cystoplasty in a dog model. Tissue Eng. 4:379–387, 1998.
Badylak, S. F., K. Park, N. Peppas, G. McCabe, and M. Yoder. Marrow-derived cells populate scaffolds composed of xenogeneic extracellular matrix. Exp. Hematol. 29:1310–1318, 2001.
Badylak, S. F., R. Tullius, K. Kokini, K. D. Shelbourne, T. Klootwyk, S. L. Voytik, M. R. Kraine, and C. Simmons. The use of xenogeneic small intestinal submucosa as a biomaterial for Achille’s tendon repair in a dog model. J. Biomed. Mater. Res. 29:977–985, 1995.
Badylak, S. F., J. E. Valentin, A. K. Ravindra, G. P. McCabe, and A. M. Stewart-Akers. Macrophage phenotype as a determinant of biologic scaffold remodeling. Tissue Eng. Part A 14:1835–1842, 2008.
Baiguera, S., C. Del Gaudio, E. Lucatelli, E. Kuevda, M. Boieri, B. Mazzanti, A. Bianco, and P. Macchiarini. Electrospun gelatin scaffolds incorporating rat decellularized brain extracellular matrix for neural tissue engineering. Biomaterials 35:1205–1214, 2014.
Bailey, A. J., and W. J. Tromans. Effects of ionizing radiation on the ultrastructure of collagen fibrils. Radiat. Res. 23:145–155, 1964.
Balestrini, J. L., A. Liu, A. L. Gard, J. Huie, K. M. S. Blatt, J. Schwan, L. Zhao, T. J. Broekelmann, R. P. Mecham, E. C. Wilcox, and L. E. Niklason. Sterilization of lung matrices by supercritical carbon dioxide. Tissue Eng. Part C Methods 22:260–269, 2016.
Bao, J., Q. Wu, Y. Wang, Y. Li, L. Li, F. Chen, X. Wu, M. Xie, and H. Bu. Enhanced hepatic differentiation of rat bone marrow-derived mesenchymal stem cells in spheroidal aggregate culture on a decellularized liver scaffold. Int. J. Mol. Med. 38:457–465, 2016.
Barakat, O., S. Abbasi, G. Rodriguez, J. Rios, R. P. Wood, C. Ozaki, L. S. Holley, and P. K. Gauthier. Use of decellularized porcine liver for engineering humanized liver organ. J. Surg. Res. 173:e11–e25, 2012.
Beattie, A. J., T. W. Gilbert, J. P. Guyot, A. J. Yates, and S. F. Badylak. Chemoattraction of progenitor cells by remodeling extracellular matrix scaffolds. Tissue Eng. Part A 15:1119–1125, 2009.
Berger, A. Th1 and Th2 responses: What are they ? BMJ 321:424, 2000.
Bernhardt, A., M. Wehrl, B. Paul, T. Hochmuth, M. Schumacher, K. Schütz, and M. Gelinsky. Improved sterilization of sensitive biomaterials with supercritical carbon dioxide at low temperature. PLoS ONE 10:1–19, 2015.
Bhrany, A. D., C. J. Lien, B. L. Beckstead, N. D. Futran, N. H. Muni, C. M. Giachelli, and B. D. Ratner. Crosslinking of an oesophagus acellular matrix tissue scaffold. J. Tissue Eng. Regen. Med. 2:365–372, 2008.
Bissell, M. J., and T. G. Ram. Regulation of functional cytodifferentiation and histogenesis in mammary epithelial cells: Role of the extracellular matrix. Environ. Health Perspect. 80:61–70, 1989.
Bonandrini, B., M. Figliuzzi, E. Papadimou, M. Morigi, N. Perico, F. Casiraghi, C. Dipl, F. Sangalli, S. Conti, A. Benigni, A. Remuzzi, and G. Remuzzi. Recellularization of well-preserved acellular kidney scaffold using embryonic stem cells. Tissue Eng. Part A 20:1486–1498, 2014.
Boruch, A. V., A. Nieponice, I. R. Qureshi, T. W. Gilbert, and S. F. Badylak. Constructive remodeling of biologic scaffolds is dependent on early exposure to physiologic bladder filling in a canine partial cystectomy model. J. Surg. Res. 161:217–225, 2010.
Brennan, E. P., X. Tang, A. M. Stewart-Akers, L. J. Gudas, and S. F. Badylak. Chemoattractant activity of degradation products of fetal and adult skin extracellular matrix for keratinocyte progenitor cells. J. Tissue Eng. Regen. Med. 2:491–498, 2008.
Brightman, A. O., B. P. Rajwa, J. E. Sturgis, M. E. Mccallister, J. P. Robinson, and S. L. Voytik-Harbin. Time-lapse confocal reflection microscopy of collagen fibrillogenesis and extracellular matrix assembly in vitro. Biopolymers 54:222–234, 2000.
Browe, D. C., O. R. Mahon, P. J. Díaz-Payno, N. Cassidy, I. Dudurych, A. Dunne, C. T. Buckley, and D. J. Kelly. Glyoxal cross-linking of solubilised extracellular matrix to produce highly porous, elastic and chondro-permissive scaffolds for orthopaedic tissue engineering. J. Biomed. Mater. Res. Part A 2019. https://doi.org/10.1002/jbm.a.36731.
Brown, B. N., C. A. Barnes, R. T. Kasick, R. Michel, T. W. Gilbert, D. Beer-Stolz, D. G. Castner, B. D. Ratner, and S. F. Badylak. Surface characterization of extracellular matrix scaffolds. Biomaterials 31:428–437, 2010.
Brown, B. N., J. M. Freund, L. Han, J. P. Rubin, J. E. Reing, E. M. Jeffries, M. T. Wolf, S. Tottey, C. A. Barnes, B. D. Ratner, and S. F. Badylak. Comparison of three methods for the derivation of a biologic scaffold composed of adipose tissue extracellular matrix. Tissue Eng. Part C Methods 17:411–421, 2010.
Brown, B. N., R. Londono, S. Tottey, L. Zhang, K. A. Kukla, M. T. Wolf, K. A. Daly, J. E. Reing, and S. F. Badylak. Macrophage phenotype as a predictor of constructive remodeling following the implantation of biologically derived surgical mesh materials. Acta Biomater. 8:978–987, 2012.
Brown, B. N., J. E. Valentin, A. M. Stewart-Akers, G. P. McCabe, and S. F. Badylak. Macrophage phenotype and remodeling outcomes in response to biologic scaffolds with and without a cellular component. Biomaterials 30:1482–1491, 2009.
Burgkart, R., A. Tron, P. Prodinger, M. Culmes, J. Tuebel, M. Van Griensven, B. Saldamli, and A. Schmitt. Decellularized kidney matrix for perfused bone engineering. Tissue Eng. Part C Methods 20:553–561, 2014.
Butler, C. E., N. K. Burns, K. T. Campbell, A. B. Mathur, M. V. Jaffari, and C. N. Rios. Comparison of cross-linked and non-cross-linked porcine acellular dermal matrices for ventral hernia repair. J. Am. Coll. Surg. 211:368–376, 2010.
Campbell, K. T., N. K. Burns, C. N. Rios, A. B. Mathur, and C. E. Butler. Human versus non-cross-linked porcine acellular dermal matrix used for ventral hernia repair: Comparison of in vivo fibrovascular remodeling and mechanical repair strength. Plast. Reconstr. Surg. 127:2321–2332, 2011.
Carver, D. A., A. W. Kirkpatrick, T. L. Eberle, and C. G. Ball. Performance of biological mesh materials in abdominal wall reconstruction: Study protocol for a randomised controlled trial. BMJ Open 9:e024091, 2019.
Casali, D. M., R. M. Handleton, T. Shazly, and M. A. Matthews. A novel supercritical CO2-based decellularization method for maintaining scaffold hydration and mechanical properties. J. Supercrit. Fluids 131:72–81, 2018.
Cavallo, J. A., S. C. Greco, J. Liu, M. M. Frisella, C. R. Deeken, and B. D. Matthews. Remodeling characteristics and biomechanical properties of a crosslinked versus a non-crosslinked porcine dermis scaffolds in a porcine model of ventral hernia repair. Hernia 19:207–218, 2015.
Cebotari, S., I. Tudorache, T. Jaekel, A. Hilfiker, S. Dorfman, W. Ternes, A. Haverich, and A. Lichtenberg. Detergent decellularization of heart valves for tissue engineering: Toxicological effects of residual detergents on human endothelial cells. Artif. Organs 34:206–210, 2010.
Chen, L., Z. He, B. Chen, M. Yang, Y. Zhao, W. Sun, Z. Xiao, J. Zhang, and J. Dai. Loading of VEGF to the heparin cross-linked demineralized bone matrix improves vascularization of the scaffold. J. Mater. Sci. Mater. Med. 21:309–317, 2010.
Cheng, A. M. Y. W., M. A. Abbas, and T. Tejirian. Outcome of abdominal wall hernia repair with biologic mesh: Permacol versus Strattice. Am. Surg. 80:999–1002, 2014.
Cheng, N. C., B. T. Estes, H. A. Awad, and F. Guilak. Chondrogenic differentiation of adipose-derived adult stem cells by a porous scaffold derived from native articular cartilage extracellular matrix. Tissue Eng. Part A 15:231–241, 2009.
Cheng, N.-C., B. T. Estes, T.-H. Young, and F. Guilak. Genipin-crosslinked cartilage-derived matrix as a scaffold for human adipose-derived stem cell chondrogenesis. Tissue Eng. Part A 19:484–496, 2012.
Choi, J. S., H. J. Yang, B. S. Kim, J. D. Kim, J. Y. Kim, B. Yoo, K. Park, H. Y. Lee, and Y. W. Cho. Human extracellular matrix (ECM) powders for injectable cell delivery and adipose tissue engineering. J. Control. Release 139:2–7, 2009.
Christo, S. N., K. R. Diener, A. Bachhuka, K. Vasilev, and J. D. Hayball. Innate Immunity and Biomaterials at the Nexus : Friends or Foes. Biomed Res. Int. 2015:342304, 2015.
Consigliere, P., I. Polyzois, T. Sarkhel, R. Gupta, O. Levy, and A. A. Narvani. Preliminary results of a consecutive series of large & massive rotator cuff tears treated with arthroscopic rotator cuff repairs augmented with extracellular matrix. Arch. Bone Jt. Surg. 5:14–21, 2017.
Constantinou, C. D., and S. A. Jimenez. Structure of cDNAs encoding the triple-helical domain of murine alpha 2 (VI) collagen chain and comparison to human and chick homologues. Use of polymerase chain reaction and partially degenerate oligonucleotide for generation of novel cDNA clones. Matrix 11:1–9, 1991.
Cook, J. L., D. B. Fox, K. Kuroki, M. Jayo, and P. G. De Deyne. In vitro and in vivo comparison of five biomaterials used for orthopedic soft tissue augmentation. Am. J. Vet. Res. 69:148–156, 2008.
Cortiella, J., J. Niles, A. Cantu, A. Brettler, A. Pham, G. Vargas, S. Winston, J. Wang, S. Walls, and J. E. Nichols. Influence of acellular natural lung matrix on murine embryonic stem cell differentiation and tissue formation. Tissue Eng. Part A 16:2565–2580, 2010.
Costa, A., J. D. Naranjo, R. Londono, and S. F. Badylak. Biologic scaffolds. Cold Spring Harb. Perspect. Biol. 7:a025676, 2017.
Courtman, D. W., B. F. Errett, and G. J. Wilson. The role of crosslinking in modification of the immune response elicited against xenogenic vascular acellular matrices. J. Biomed. Mater. Res. 55:576–586, 2001.
Crapo, P. M., T. W. Gilbert, and D. V. M. Badylak. An overview of tissue and whole organ decellularization processes. Biomaterials 32:3233–3243, 2011.
Crapo, P. M., C. J. Medberry, J. E. Reing, S. Tottey, Y. van der Merwe, K. E. Jones, and S. F. Badylak. Biologic scaffolds composed of central nervous system extracellular matrix. Biomaterials 33:3539–3547, 2012.
Daly, A. B., J. M. Wallis, Z. D. Borg, R. W. Bonvillain, B. Deng, B. A. Ballif, D. M. Jaworski, G. B. Allen, and D. J. Weiss. Initial binding and recellularization of decellularized mouse lung scaffolds with bone marrow-derived mesenchymal stromal cells. Tissue Eng. Part A 18:1–16, 2012.
Davis, G. E., K. J. Bayless, M. J. Davis, and G. A. Meininger. Regulation of tissue injury responses by the exposure of matricryptic sites within extracellular matrix molecules. Am. J. Pathol. 156:1489–1498, 2000.
De Waele, J., K. Reekmans, J. Daans, H. Goossens, Z. Berneman, and P. Ponsaerts. 3D culture of murine neural stem cells on decellularized mouse brain sections. Biomaterials 41:122–131, 2015.
Dearth, C. L., T. J. Keane, C. A. Carruthers, J. E. Reing, L. Huleihel, C. A. Ranallo, E. W. Kollar, and S. F. Badylak. The effect of terminal sterilization on the material properties and in vivo remodeling of a porcine dermal biologic scaffold. Acta Biomater. 33:78–87, 2016.
Deeken, C. R., L. Melman, E. D. Jenkins, S. C. Greco, M. M. Frisella, and B. D. Matthews. Histologic and biomechanical evaluation of crosslinked and non-crosslinked biologic meshes in a porcine model of ventral incisional hernia repair. J. Am. Coll. Surg. 212:880–888, 2011.
Dejardin, L. M., S. P. Arnoczky, B. J. Ewers, R. C. Haut, and R. B. Clarke. Tissue-engineered rotator cuff tendon using porcine small intestine submucosa: Histologic and mechanical evaluation in dogs. Am. J. Sports Med. 29:175–184, 2001.
del Barrio, J. L. A., M. Chiesa, N. Garagorri, N. Garcia-Urquia, J. Fernandez-Delgado, L. Bataille, A. Rodriguez, F. Arnalich-Montiel, T. Zarnowski, J. P. Á. de Toledo, J. L. Alio, and M. P. De Miguel. Acellular human corneal matrix sheets seeded with human adipose-derived mesenchymal stem cells integrate functionally in an experimental animal model. Exp. Eye Res. 132:91–100, 2015.
Dellarco, V. L., W. M. Generoso, G. A. Sega, J. R. Fowle, D. Jacobson-Kram, and H. E. Brockman. Review of the mutagenicity of ethylene oxide. Environ. Mol. Mutagen. 16:85–103, 1990.
Dellavalle, A., G. Maroli, Azzoni E. CovarelloD, A. Innocenzi, L. Perani, S. Antonini, R. Sambasivan, S. Brunelli, S. Tajbakhsh, and G. Cossu. Pericytes resident in postnatal skeletal muscle differentiate into muscle fibres and generate satellite cells. Nat. Commun. 2:411–499, 2011.
Dequach, J. A., V. Mezzano, A. Miglani, S. Lange, G. M. Keller, and K. L. Christman. Simple and high yielding method for preparing tissue specific extracellular matrix coatings for cell culture. PLoS ONE 5:1–11, 2010.
Dequach, J. A., S. H. Yuan, L. S. B. Goldstein, and K. L. Christman. Decellularized porcine brain matrix for cell culture and tissue engineering scaffolds. Tissue Eng. Part A 17:2583–2592, 2011.
Duan, Y., Z. Liu, J. O’Neill, L. Q. Wan, D. O. Freytes, and G. Vunjak-Novakovic. Hybrid gel composed of native heart matrix and collagen induces cardiac differentiation of human embryonic stem cells without supplemental growth factors. J. Cardiovasc. Transl. Res. 4:605–615, 2011.
Dziki, J., S. Badylak, M. Yabroudi, B. Sicari, F. Ambrosio, K. Stearns, N. Turner, A. Wyse, M. L. Boninger, E. H. P. Brown, and J. P. Rubin. An acellular biologic scaffold treatment for volumetric muscle loss: Results of a 13-patient cohort study. NPJ Regen. Med. 1:16008, 2016.
Dziki, J. L., L. Huleihel, M. E. Scarritt, and S. F. Badylak. Extracellular matrix bioscaffolds as immunomodulatory biomaterials. Tissue Eng. Part A 23:1152–1159, 2017.
Dziki, J. L., B. M. Sicari, M. T. Wolf, M. C. Cramer, and S. F. Badylak. Immunomodulation and mobilization of progenitor cells by extracellular matrix bioscaffolds for volumetric muscle loss treatment. Tissue Eng. Part A 22:1129–1139, 2016.
Dziki, J. L., D. S. Wang, C. Pineda, B. M. Sicari, T. Rausch, and S. F. Badylak. Solubilized extracellular matrix bioscaffolds derived from diverse source tissues differentially influence macrophage phenotype. J. Biomed. Mater. Res. Part A 105:138–147, 2017.
Efraim, Y., B. Schoen, S. Zahran, T. Davidov, G. Vasilyev, L. Baruch, E. Zussman, and M. Machluf. 3D structure and processing methods direct the biological attributes of ECM-based cardiac scaffolds. Sci. Rep. 9:1–13, 2019.
Exposito, J. Y., M. D’Alessio, M. Solursh, and F. Ramirez. Sea urchin collagen evolutionarily homologous to vertebrate pro-α2(I) collagen. J. Biol. Chem. 267:15559–15562, 1992.
Faulk, D. M., C. A. Carruthers, H. J. Warner, C. R. Kramer, J. E. Reing, L. Zhang, A. D’Amore, and S. F. Badylak. The effect of detergents on the basement membrane complex of a biologic scaffold material. Acta Biomater. 10:183–193, 2014.
Faulk, D. M., J. D. Wildemann, and S. F. Badylak. Decellularization and cell seeding of whole liver biologic scaffolds composed of extracellular matrix. J. Clin. Exp. Hepatol. 5:69–80, 2015.
Faust, A., A. Kandakatla, Y. Van Der Merwe, T. Ren, L. Huleihel, G. Hussey, J. D. Naranjo, S. Johnson, S. Badylak, and M. Steketee. Urinary bladder extracellular matrix hydrogels and matrix-bound vesicles differentially regulate central nervous system neuron viability and axon growth and branching. J. Biomater. Appl. 31:1277–1295, 2017.
Fishman, J. M., M. W. Lowdell, L. Urbani, T. Ansari, A. J. Burns, M. Turmaine, J. North, P. Sibbons, A. M. Seifalian, K. J. Wood, M. A. Birchall, and P. De Coppi. Immunomodulatory effect of a decellularized skeletal muscle scaffold in a discordant xenotransplantation model. Proc. Natl. Acad. Sci. USA 110:14360–14365, 2013.
Franz, S., S. Rammelt, D. Scharnweber, and J. C. Simon. Immune responses to implants—A review of the implications for the design of immunomodulatory biomaterials. Biomaterials 32:6692–6709, 2011.
French, K., A. Boopathy, J. DeQuach, L. Chingozha, H. Lu, K. L. Christman, and M. E. Davis. A naturally derived cardiac extracellular matrix enhances cardiac progenitor cell behavior in vitro. Acta Biomater. 8:4357–4364, 2012.
Freytes, D. O., S. F. Badylak, T. J. Webster, L. A. Geddes, and A. E. Rundell. Biaxial strength of multilaminated extracellular matrix scaffolds. Biomaterials 25:2353–2361, 2004.
Freytes, D. O., J. Martin, S. S. Velankar, A. S. Lee, and S. F. Badylak. Preparation and rheological characterization of a gel form of the porcine urinary bladder matrix. Biomaterials 29:1630–1637, 2008.
Freytes, D. O., J. D. O’Neill, Y. Duan-Arnold, E. Wrona, and G. Vunjak-Novakovic. Native cardiac extracellular matrix hydrogels for cultivation of human stem cell-derived cardiomyocytes. Methods Mol Biol 1181:69–81, 2014.
Freytes, D. O., A. E. Rundell, J. Vande Geest, D. A. Vorp, T. J. Webster, and S. F. Badylak. Analytically derived material properties of multilaminated extracellular matrix devices using the ball-burst test. Biomaterials 26:5518–5531, 2005.
Freytes, D. O., R. M. Stoner, and S. F. Badylak. Uniaxial and biaxial properties of terminally sterilized porcine urinary bladder matrix scaffolds. J. Biomed. Mater. Res. B. Appl. Biomater. 84B:408–414, 2008.
Freytes, D. O., R. S. Tullius, J. E. Valentin, A. M. Stewart-Akers, and S. F. Badylak. Hydrated versus lyophilized forms of porcine extracellular matrix derived from the urinary bladder. J. Biomed. Mater. Res. A 87:862–872, 2008.
Gaetani, R., C. Yin, N. Srikumar, R. Braden, P. A. Doevendans, J. P. G. Sluijter, and K. L. Christman. Cardiac-derived extracellular matrix enhances cardiogenic properties of human cardiac progenitor cells. Cell Transplant. 25:1653–1663, 2016.
Geiger, S. E., O. A. Deigni, J. T. Watson, and B. A. Kraemer. Management of open distal lower extremity wounds with exposed tendons using porcine urinary bladder matrix. Wounds: A Compend. Clin. Res. Pract. 28:306–316, 2016.
Gilbert, T. W., J. Freund, and S. F. Badylak. Quantification of DNA in biologic scaffold materials. J. Surg. Res. 152:135–139, 2009.
Gilbert, T. W., A. Nieponice, A. R. Spievack, J. Holcomb, S. Gilbert, and S. F. Badylak. Repair of the thoracic wall with an extracellular matrix scaffold in a canine model. J. Surg. Res. 147:61–67, 2008.
Gilbert, T. W., A. M. Stewart-Akers, A. Simmons-Byrd, and S. F. Badylak. Degradation and remodeling of small intestinal submucosa in canine Achilles tendon repair. J. Bone Jt. Surg. Am. 89:621–630, 2007.
Gilbert, T. W., D. B. Stolz, F. Biancaniello, A. Simmons-Byrd, and S. F. Badylak. Production and characterization of ECM powder: Implications for tissue engineering applications. Biomaterials 26:1431–1435, 2005.
Gilot, G. J., A. M. Alvarez-Pinzon, L. Barcksdale, D. Westerdahl, M. Krill, and E. Peck. Outcome of large to massive rotator cuff tears repaired with and without extracellular matrix augmentation: A prospective comparative study. Arthrosc. J. Arthrosc. Relat. Surg. 31:1459–1465, 2015.
Gilpin, S. E., X. Ren, T. Okamoto, J. P. Guyette, H. Mou, J. Rajagopal, D. J. Mathisen, J. P. Vacanti, and H. C. Ott. Enhanced lung epithelial specification of human induced pluripotent stem cells on decellularized lung matrix. Ann. Thorac. Surg. 98:1721–1729, 2014.
Gilpin, A., and Y. Yang. Decellularization strategies for regenerative medicine: From processing techniques to applications. Biomed Res. Int. 2017. https://doi.org/10.1155/2017/9831534.
Glasberg, S. B., and D. Light. AlloDerm and Strattice in breast reconstruction: A comparison and techniques for optimizing outcomes. Plast. Reconstr. Surg. 129:1223–1233, 2012.
Godin, L. M., B. J. Sandri, D. E. Wagner, C. M. Meyer, A. P. Price, I. Akinnola, D. J. Weiss, and A. P. M. Panoskaltsis-Mortari. Decreased laminin expression by human lung epithelial cells and fibroblasts cultured in acellular lung scaffolds from aged mice. PLoS ONE 11:1–17, 2016.
Gordon, S., and P. R. Taylor. Monocyte and macrophage heterogeneity. Nat. Rev. Immunol. 5:953–964, 2005.
Gouk, S.-S., T.-M. Lim, S.-H. Teoh, and W. Q. Sun. Alterations of human acellular tissue matrix by gamma irradiation: Histology, biomechanical property, stability, in vitro cell repopulation, and remodeling. J Biomed. Mater. Res. Part B Appl. Biomater. 84B:205–217, 2008.
Guler, S., B. Aslan, P. Hosseinian, and H. M. Aydin. Supercritical carbon dioxide-assisted decellularization of aorta and cornea. Tissue Eng. Part C Methods 23:540–547, 2017.
Harth, K. C., A. M. Broome, M. R. Jacobs, J. A. Blatnik, F. Zeinali, S. Bajaksouzian, and M. J. Rosen. Bacterial clearance of biologic grafts used in hernia repair: An experimental study. Surg. Endosc. 25:2224–2229, 2011.
Hashimoto, Y., S. Funamoto, T. Kimura, K. Nam, T. Fujisato, and A. Kishida. The effect of decellularized bone/bone marrow produced by high-hydrostatic pressurization on the osteogenic differentiation of mesenchymal stem cells. Biomaterials 32:7060–7067, 2011.
Haykal, S., Y. Zhou, P. Marcus, M. Salna, T. Machuca, S. O. P. Hofer, and T. K. Waddell. The effect of decellularization of tracheal allografts on leukocyte infiltration and of recellularization on regulatory T cell recruitment. Biomaterials 34:5821–5832, 2013.
Hennessy, R. S., S. Jana, B. J. Tefft, M. R. Helder, M. D. Young, R. R. Hennessy, N. J. Stoyles, and A. Lerman. Supercritical carbon dioxide–based sterilization of decellularized heart valves. JACC Basic Transl. Sci. 2:71–84, 2017.
Hirsh, S. L., D. R. McKenzie, N. J. Nosworthy, J. A. Denman, O. U. Sezerman, and M. M. M. Bilek. The Vroman effect: Competitive protein exchange with dynamic multilayer protein aggregates. Coll. Surf. B Biointerfaces 103:395–404, 2013.
HO, K. L., V. M. N. Witte, and E. T. Bird. 8-ply small intestinal submucosa tension-free sling: Spectrum of postoperative inflammation. J. Urol. 171:268–271, 2004.
Hodde, J., A. Janis, D. Ernst, D. Zopf, D. Sherman, and C. Johnson. Effects of sterilization on an extracellular matrix scaffold: Part I. Composition and matrix architecture. J. Mater. Sci. Mater. Med. 18:537–543, 2007.
Hodde, J., A. Janis, and M. Hiles. Effects of sterilization on an extracellular matrix scaffold: Part II. Bioactivity and matrix interaction. J. Mater. Sci. Mater. Med. 18:545–550, 2007.
Hoganson, D. M., A. M. Meppelink, C. J. Hinkel, S. M. Goldman, X.-H. Liu, R. M. Nunley, J. P. Gaut, and J. P. Vacanti. Differentiation of human bone marrow mesenchymal stem cells on decellularized extracellular matrix materials. J. Biomed. Mater. Res. A 102:2875–2883, 2014.
Hong, X., Y. Yuan, X. Sun, M. Zhou, G. Guo, Q. Zhang, J. Hescheler, and J. Xi. Skeletal extracellular matrix supports cardiac differentiation of embryonic stem cells: A potential scaffold for engineered cardiac tissue. Cell. Physiol. Biochem. 45:319–331, 2018.
Hoppo, T., S. F. Badylak, and B. A. Jobe. A novel esophageal-preserving approach to treat high-grade dysplasia and superficial adenocarcinoma in the presence of chronic gastroesophageal reflux disease. World J. Surg. 36:2390–2393, 2012.
Huang, Y. H., F. W. Tseng, W. H. Chang, I. C. Peng, D. J. Hsieh, S. W. Wu, and M. L. Yeh. Preparation of acellular scaffold for corneal tissue engineering by supercritical carbon dioxide extraction technology. Acta Biomater. 58:238–243, 2017.
Huleihel, L., J. G. Bartolacci, J. L. Dziki, T. Vorobyov, B. Arnold, M. E. Scarritt, C. Pineda Molina, S. T. LoPresti, B. N. Brown, J. D. Naranjo, and S. F. Badylak. Matrix-bound nanovesicles recapitulate extracellular matrix effects on macrophage phenotype. Tissue Eng. Part A 23:1283–1294, 2017.
Huleihel, L., J. L. Dziki, J. G. Bartolacci, T. Rausch, M. E. Scarritt, M. C. Cramer, T. Vorobyov, S. T. LoPresti, I. T. Swineheart, L. J. White, B. N. Brown, and S. F. Badylak. Macrophage phenotype in response to ECM bioscaffolds. Semin. Immunol. 29:2–13, 2017.
Huleihel, L., G. S. Hussey, J. D. Naranjo, L. Zhang, J. L. Dziki, N. J. Turner, D. B. Stolz, and S. F. Badylak. Matrix-bound nanovesicles within ECM bioscaffolds. Sci. Adv. 2:e1600502, 2016.
Hutter, H., B. E. Vogel, J. D. Plenefisch, C. R. Norris, R. B. Proenca, J. Spieth, C. Guo, S. Mastwal, X. Zhu, J. Scheel, and E. M. Hedgecock. Conservation and novelty in the evolution of cell adhesion and extracellular matrix genes. Science (80-) 287:989–1010, 2000.
Hynes, R. O. The evolution of metazoan extracellular matrix. J. Cell Biol. 196:671–679, 2012.
Iozzo, R. V. Perlecan: A gem of a proteoglycan. Matrix Biol. 14:203–208, 1994.
ISO 13408-1. Aseptic processing of health care products — Part 1: General requirements., 2008.
ISO 22442-1. Medical devices utilizing animal tissues and their derivatives — Part 1: Application of risk management., 2015.
Jackson, D. W., E. S. Grood, P. Wilcox, D. L. Butler, T. M. Simon, and J. P. Holden. The effects of processing techniques on the mechanical properties of bone-anterior cruciate ligament-bone allografts. An experimental study in goats. Am. J. Sports Med. 16:101–105, 1988.
Jackson, D. W., G. E. Windler, and T. M. Simon. Intraarticular reaction associated with the use of freeze-dried, ethylene oxide-sterilized bone-patella tendon-bone allografts in the reconstruction of the anterior cruciate ligament. Am. J. Sports Med. 18:1–11, 1990.
Jang, J., T. G. Kim, B. S. Kim, S. W. Kim, S. M. Kwon, and D. W. Cho. Tailoring mechanical properties of decellularized extracellular matrix bioink by vitamin B2-induced photo-crosslinking. Acta Biomater. 33:88–95, 2016.
Ji, R., N. Zhang, N. You, Q. Li, W. Liu, N. Jiang, J. Liu, H. Zhang, D. Wang, K. Tao, and K. Dou. The differentiation of MSCs into functional hepatocyte-like cells in a liver biomatrix scaffold and their transplantation into liver-fibrotic mice. Biomaterials 33:8995–9008, 2012.
John, T. T., N. Aggarwal, A. K. Singla, and R. A. Santucci. Intense inflammatory reaction with porcine small intestine submucosa pubovaginal sling or tape for stress urinary incontinence. Urology 72:1036–1039, 2008.
Johnson, T. D., R. L. Braden, and K. L. Christman. Injectable ECM scaffolds for cardiac repair. Methods Mol. Biol. 1181:109–120, 2014.
Johnson, T. D., J. A. Dequach, R. Gaetani, J. Ungerleider, D. Elhag, V. Nigam, A. Behfar, and K. L. Christman. Human versus porcine tissue sourcing for an injectable myocardial matrix hydrogel. Biomater. Sci. 29:13–17, 2014.
Johnson, T. D., S. Y. Lin, and K. L. Christman. Tailoring material properties of a nanofibrous extracellular matrix derived hydrogel. Nanotechnology 22:494015, 2011.
Kaufmann, R., A. P. Jairam, I. M. Mulder, Z. Wu, J. Verhelst, S. Vennix, L. J. X. Giesen, M. C. Clahsen-van Groningen, and J. Jeekel. Lange JF (2019) Non-cross-linked collagen mesh performs best in a physiologic, noncontaminated rat model. Surg. Innov. 26:302–311, 2019.
Kaufmann, R., A. P. Jairam, I. M. Mulder, Z. Wu, J. Verhelst, S. Vennix, L. J. X. Giesen, M. C. Clahsen-van Groningen, J. Jeekel, and J. F. Lange. Characteristics of different mesh types for abdominal wall repair in an experimental model of peritonitis. Br. J. Surg. 104:1884–1893, 2017.
Keane, T. J., and S. F. Badylak. The host response to allogeneic and xenogeneic biological scaffold materials. J. Tissue Eng. Regen. Med. 9:504–511, 2015.
Keane, T. J., A. DeWard, R. Londono, L. T. Saldin, A. A. Castleton, L. Carey, A. Nieponice, E. Lagasse, and S. F. Badylak. Tissue-specific effects of esophageal extracellular matrix. Tissue Eng. Part A 21:2293–2300, 2015.
Keane, T. J., J. Dziki, E. Sobieski, A. Smoulder, A. Castleton, N. Turne, L. J. White, and S. F. Badylak. Restoring mucosal barrier function and modifying macrophage phenotype with an extracellular matrix hydrogel: Potential therapy for ulcerative colitis. J. Crohn’s Colitis 11:360–368, 2017.
Keane, T. J., R. Londono, N. J. Turner, and S. F. Badylak. Consequences of ineffective decellularization of biologic scaffolds on the host response. Biomaterials 33:1771–1781, 2012.
Keane, T. J., I. T. Swinehart, and S. F. Badylak. Methods of tissue decellularization used for preparation of biologic scaffolds and in vivo relevance. Methods 84:25–34, 2015.
Kelly, D. J., A. B. Rosen, A. J. T. Schuldt, P. V. Kochupura, S. V. Doronin, I. A. Potapova, E. U. Azeloglu, S. F. Badylak, P. R. Brink, I. S. Cohen, and G. R. Gaudette. Increased myocyte content and mechanical function within a tissue-engineered myocardial patch following implantation. Tissue Eng. Part A 15:2189–2201, 2009.
Kimmel, H., M. Rahn, and T. W. Gilbert. The clinical effectiveness in wound healing with extracellular matrix derived from porcine urinary bladder matrix: A case series on severe chronic wounds. J. Am. Col. Certif. Wound Spec. 2:55–59, 2010.
Knoll, L. D. Use of small intestinal submucosa graft for the surgical management of Peyronie’s disease. J. Urol. 178:2474–2478, 2007.
Kochupura, P. V., E. U. Azeloglu, D. J. Kelly, S. V. Doronin, S. F. Badylak, I. B. Krukenkamp, I. S. Cohen, and G. R. Gaudette. Tissue-engineered myocardial patch derived from extracellular matrix provides regional mechanical function. Circulation 112:144–149, 2005.
Koci, Z., K. Vyborny, J. Dubisova, I. Vackova, A. Jager, O. Lunov, K. Jirakova, and S. Kubinova. Extracellular matrix hydrogel derived from human umbilical cord as a scaffold for neural tissue repair and its comparison with extracellular matrix from porcine tissues. Tissue Eng. Part C Methods 23:333–345, 2017.
Kramer, J. Extracellular matrix. In: C. elegans II, edited by D. Riddle, T. Blumenthal, and B. Meyer. Boston: Springer, 1997.
Kropp, B. P., B. L. Eppley, C. D. Prevel, M. K. Rippy, R. C. Harruff, S. F. Badylak, M. C. Adams, R. C. Rink, and M. A. Keating. Experimental assessment of small intestinal submucosa as a bladder wall substitute. Urology 46:396–400, 1995.
Kulig, K. M., X. Luo, E. B. Finkelstein, X. H. Liu, S. M. Goldman, C. A. Sundback, J. P. Vacanti, and C. M. Neville. Biologic properties of surgical scaffold materials derived from dermal ECM. Biomaterials 34:5776–5784, 2013.
Lee, J. S., J. Shin, H. M. Park, Y. G. Kim, B. G. Kim, J. W. Oh, and S. W. Cho. Liver extracellular matrix providing dual functions of two-dimensional substrate coating and three-dimensional injectable hydrogel platform for liver tissue engineering. Biomacromolecules 15:206–218, 2014.
Liang, R., G. Yang, K. E. Kim, A. D’Amore, A. N. Pickering, C. Zhang, and S. L.-Y. Woo. Positive effects of an extracellular matrix hydrogel on rat anterior cruciate ligament fibroblast proliferation and collagen mRNA expression. J. Orthop. Transl. 3:114–122, 2015.
Liao, J., E. M. Joyce, and M. S. Sacks. Effects of decellularization on the mechanical and structural properties of the porcine aortic valve leaflet. Biomaterials 29:1065–1074, 2008.
Liu, C. J., S. D. Dib-Hajj, and S. G. Waxman. Fibroblast growth factor homologous factor 1B binds to the C terminus of the tetrodotoxin-resistant sodium channel rNav1.9a (NaN). J. Biol. Chem. 276:18925–18933, 2001.
Liu, X., N. Li, D. Gong, C. Xia, and Z. Xu. Comparison of detergent-based decellularization protocols for the removal of antigenic cellular components in porcine aortic valve. Xenotransplantation 25:1–13, 2018.
Liu, Z., R. Tang, Z. Zhou, Z. Song, H. Wang, and Y. Gu. Comparison of two porcine-derived materials for repairing abdominal wall defects in rats. PLoS ONE 6:e20520, 2011.
Londono, R., J. L. Dziki, E. Haljasmaa, N. J. Turner, C. A. Leifer, and S. F. Badylak. The effect of cell debris within biologic scaffolds upon the macrophage response. J. Biomed. Mater. Res. Part A 105:2109–2118, 2017.
Loneker, A. E., D. M. Faulk, G. S. Hussey, A. D’Amore, and S. F. Badylak. Solubilized liver extracellular matrix maintains primary rat hepatocyte phenotype in-vitro. J. Biomed. Mater. Res. A 104:957–965, 2016.
Longaker, M. T., E. S. Chu, N. S. Adzick, M. Stern, M. R. Harrison, and R. Stern. Studies in fetal wound healing. V. A prolonged presence of hyaluronic acid characterizes fetal wound fluid. Ann. Surg. 213:292–296, 1991.
Longaker, M. T., D. J. Whitby, M. W. J. Ferguson, M. R. Harrison, T. M. Crombleholme, J. C. Langer, K. C. Cochrum, E. D. Verrier, and R. Stern. Studies in fetal wound healing: III. Early deposition of fibronectin distinguishes fetal from adult wound healing. J. Pediatr. Surg. 24:799–805, 1989.
LoPresti, S. T., and B. N. Brown. Effect of source animal age upon macrophage response to extracellular matrix biomaterials. J. Immunol. Regen. Med. 1:57–66, 2018.
Lovvorn, III, H. N., D. T. Cheung, M. E. Nimni, N. Perelman, J. M. Estes, and N. S. Adzick. Relative distribution and crosslinking of collagen distinguish fetal from adult sheep wound repair. J. Pediatr. Surg. 34:218–223, 1999.
Lu, Q., M. Li, Y. Zou, and T. Cao. Delivery of basic fibroblast growth factors from heparinized decellularized adipose tissue stimulates potent de novo adipogenesis. J. Control. Release 174:43–50, 2014.
Lumpkins, S. B., N. Pierre, and P. S. McFetridge. A mechanical evaluation of three decellularization methods in the design of a xenogeneic scaffold for tissue engineering the temporomandibular joint disc. Acta Biomater. 4:808–816, 2008.
Ma, B., X. Wang, C. Wu, and J. Chang. Crosslinking strategies for preparation of extracellular matrix-derived cardiovascular scaffolds. Regen. Biomater. 1:81–89, 2014.
Manji, R. A., L. F. Zhu, N. K. Nijjar, D. C. Rayner, G. S. Korbutt, T. A. Churchill, R. V. Rajotte, A. Koshal, and D. B. Ross. Glutaraldehyde-fixed bioprosthetic heart valve conduits calcify and fail from xenograft rejection. Circulation 114:318–327, 2006.
Mantovani, A., S. K. Biswas, M. R. Galdiero, A. Sica, and M. Locati. Macrophage plasticity and polarization in tissue repair and remodelling. J. Pathol. 229:176–185, 2013.
Mantovani, A., A. Sica, S. Sozzani, P. Allavena, A. Vecchi, and M. Locati. The chemokine system in diverse forms of macrophage activation and polarization. Trends Immunol. 25:677–686, 2004.
Mase, V., J. Hsu, S. Wolf, J. Wenke, D. Baer, J. Owens, S. Badylak, and T. Walters. Clinical application of an acellular biologic scaffold for surgical repair of a large, traumatic quadriceps femoris muscle defect. Orthopedics 33:511, 2010.
Matuska, A. M., and P. S. McFetridge. The effect of terminal sterilization on structural and biophysical properties of a decellularized collagen-based scaffold; Implications for stem cell adhesion. J. Biomed. Mater. Res. Part B Appl. Biomater. 103:397–406, 2015.
Medberry, C. J., P. M. Crapo, B. F. Siu, C. A. Carruthers, M. T. Wolf, S. P. Nagarkar, V. Agrawal, K. E. Jones, J. Kelly, S. A. Johnson, S. S. Velankar, S. C. Watkins, M. Modo, and S. F. Badylak. Hydrogels derived from central nervous system extracellular matrix. Biomaterials 34:1033–1040, 2013.
Melman, L., E. D. Jenkins, N. A. Hamilton, L. C. Bender, M. D. Brodt, C. R. Deeken, S. C. Greco, M. M. Frisella, and B. D. Matthews. Early biocompatibility of crosslinked and non-crosslinked biologic meshes in a porcine model of ventral hernia repair. Hernia 15:157–164, 2011.
Meng, F. W., P. F. Slivka, C. L. Dearth, and S. F. Badylak. Solubilized extracellular matrix from brain and urinary bladder elicits distinct functional and phenotypic responses in macrophages. Biomaterials 46:131–140, 2015.
Mercuri, J. J., S. Patnaik, G. Dion, S. S. Gill, J. Liao, and D. T. Simionescu. Regenerative potential of decellularized porcine nucleus pulposus hydrogel scaffolds: Stem cell differentiation, matrix remodeling, and biocompatibility studies. Tissue Eng. Part A 19:952–966, 2013.
Merguerian, P. A., P. P. Reddy, D. J. Barrieras, G. J. Wilson, K. Woodhouse, D. J. Bagli, G. A. McLorie, and A. E. Khoury. Acellular bladder matrix allografts in the regeneration of functional bladders: Evaluation of large-segment (> 24 cm) substitution in a porcine model. BJU Int. 85:894–898, 2000.
Mestak, O., Z. Spurkova, K. Benkova, P. Vesely, V. Hromadkova, J. Miletin, R. Juzek, J. Mestak, M. Molitor, and A. Sukop. Comparison of cross-linked and non-cross-linked acellular porcine dermal scaffolds for long-term full-thickness hernia repair in a small animal model. Eplasty 14:172–183, 2014.
Meyer, S. R., B. Chiu, T. A. Churchill, L. Zhu, J. R. T. Lakey, and D. B. Ross. Comparison of aortic valve allograft decellularization techniques in the rat. J. Biomed. Mater. Res. 79A:254–262, 2006.
Mills, C. D., K. Kincaid, J. M. Alt, M. J. Heilman, and A. M. Hill. M-1/M-2 macrophages and the Th1/Th2 paradigm. J. Immunol. 164:6166–6173, 2000.
Miyazaki, K., and T. Maruyama. Partial regeneration and reconstruction of the rat uterus through recellularization of a decellularized uterine matrix. Biomaterials 35:8791–8800, 2014.
Mora-Solano, C., and J. H. Collier. Engaging adaptive immunity with biomaterials. J. Mater. Chem. B 2:2409–2421, 2014.
Moreau, M. F., Y. Gallois, M. F. Baslé, and D. Chappard. Gamma irradiation of human bone allografts alters medullary lipids and releases toxic compounds for osteoblast-like cells. Biomaterials 21:369–376, 2000.
Morris, A. H., J. Chang, and T. R. Kyriakides. Inadequate processing of decellularized dermal matrix reduces cell viability in vitro and increases apoptosis and acute inflammation in vivo. Biores. Open Access 5(1):177–187, 2016.
Mosmann, T. R., and S. Sad. The expanding universe of T-cell subsets: Th1, Th2 and more. Immunol. Today 17:138–146, 1996.
Mulder, I. M., E. B. Deerenberg, W. A. Bemelman, J. Jeekel, and J. F. Lange. Infection susceptibility of crosslinked and non-crosslinked biological meshes in an experimental contaminated environment. Am. J. Surg. 210:159–166, 2015.
Nakatsu, H., T. Ueno, A. Oga, M. Nakao, T. Nishimura, S. Kobayashi, and M. Oka. Influence of mesenchymal stem cells on stomach tissue engineering using small intestinal submucosa. J. Tissue Eng. Regen. Med. 9:296–304, 2015.
Nakayama, K. H., C. C. I. Lee, C. A. Batchelder, and A. F. Tarantal. Tissue specificity of decellularized rhesus monkey kidney and lung scaffolds. PLoS ONE 8:e64134, 2013.
Naso, F., A. Gandaglia, T. Bottio, V. Tarzia, M. B. Nottle, A. J. F. d’Apice, P. J. Cowan, E. Cozzi, C. Galli, I. Lagutina, G. Lazzari, L. Iop, M. Spina, and G. Gerosa. First quantification of alpha-Gal epitope in current glutaraldehyde-fixed heart valve bioprostheses. Xenotransplantation 20:252–261, 2013.
Navarro-Tableros, V., M. B. Herrera Sanchez, F. Figliolini, R. Romagnoli, C. Tetta, and G. Camussi. Recellularization of rat liver scaffolds by human liver stem cells. Tissue Eng. Part A 21:1929–1939, 2015.
Ngo, M. D., H. M. Aberman, M. L. Hawes, B. Choi, and A. A. Gertzman. Evaluation of human acellular dermis versus porcine acellular dermis in an in vivo model for incisional hernia repair. Cell Tissue Bank. 12:135–145, 2011.
Nieponice, A., F. F. Ciotola, F. Nachman, B. A. Jobe, T. Hoppo, R. Londono, S. Badylak, and A. E. Badaloni. Patch esophagoplasty: Esophageal reconstruction using biologic scaffolds. Ann. Thorac. Surg. 97:283–288, 2014.
Nieponice, A., K. McGrath, I. Qureshi, E. J. Beckman, J. D. Luketich, T. W. Gilbert, and S. F. Badylak. An extracellular matrix scaffold for esophageal stricture prevention after circumferential EMR. Gastrointest. Endosc. 69:289–296, 2009.
Novitsky, Y. W., S. B. Orenstein, and D. L. Kreutzer. Comparative analysis of histopathologic responses to implanted porcine biologic meshes. Hernia 18:713–721, 2014.
O’Neill, J. D., D. O. Freytes, A. Anandappa, J. A. Oliver, and G. Vunjak-Novakovic. The regulation of growth and metabolism of kidney stem cell with regional specificity using extracellular matrix derived from kidney. Biomaterials 34:1–7, 2013.
Okumura, M., R. J. Matthews, B. Robb, G. W. Litman, P. Bork, and M. L. Thomas. Comparison of CD45 extracellular domain sequences from divergent vertebrate species suggests the conservation of three fibronectin type III domains. J. Immunol. 157:1569–1575, 1996.
Omae, H., C. Zhao, L. S. Yu, K. N. An, and P. C. Amadio. Multilayer tendon slices seeded with bone marrow stromal cells: A novel composite for tendon engineering. J. Orthop. Res. 27:937–942, 2009.
Oswal, D., S. Korossis, S. Mirsadraee, H. Wilcox, and K. Watterson. Biomechanical characterization of decellularized and cross-linked bovine pericardium. J. Heart Valve Dis. 16:165–174, 2007.
Pashos, N. C., M. E. Scarritt, Z. R. Eagle, J. M. Gimble, A. E. Chaffin, and B. A. Bunnell. Characterization of an acellular scaffold for a tissue engineering approach to the nipple-areolar complex reconstruction. Cells Tissues Organs 203:183–193, 2017.
Pati, F., J. Jang, D.-H. Ha, S. Won Kim, J.-W. Rhie, J.-H. Shim, D.-H. Kim, and D.-W. Cho. Printing three-dimensional tissue analogues with decellularized extracellular matrix bioink. Nat. Commun. 5:3935, 2014.
Patil, P. B., P. B. Chogue, V. K. Kumar, S. Almstrom, H. Backdahl, D. Banerjee, G. Hernlenius, M. Olausson, and S. Sumitran-Holgersson. Recellularization of acellular human small intestine using bone marrow stem cells. Stem Cells Transl. Med. 2:307–315, 2013.
Perniconi, B., D. Coletti, P. Aulino, A. Costa, P. Aprile, L. Santacroce, E. Chiaravalloti, L. Coquelin, N. Chevallier, L. Teodori, S. Adamo, M. Marrelli, and M. Tatullo. Muscle acellular scaffold as a biomaterial: Effects on C2C12 cell differentiation and interaction with the murine host environment. Front. Physiol. 5:1–13, 2014.
Perniconi, B., A. Costa, P. Aulino, L. Teodori, S. Adamo, and D. Coletti. The pro-myogenic environment provided by whole organ scale acellular scaffolds from skeletal muscle. Biomaterials 32:7870–7882, 2011.
Price, A. P., K. A. England, A. M. Matson, B. R. Blazar, and A. Panoskaltsis-Mortari. Development of a decellularized lung bioreactor system for bioengineering the lung: The matrix reloaded. Tissue Eng. Part A 16:2581–2591, 2010.
Quarti, A., S. Nardone, M. Colaneri, G. Santoro, and M. Pozzi. Preliminary experience in the use of an extracellular matrix to repair congenital heart diseases. Interact. Cardiovasc. Thorac. Surg. 13:569–572, 2011.
Rajabi-Zeleti, S., S. Jalili-Firoozinezhad, M. Azarnia, F. Khayyatan, S. Vahdat, S. Nikeghbalian, A. Khademhosseini, H. Baharvand, and N. Aghdami. The behavior of cardiac progenitor cells on macroporous pericardium-derived scaffolds. Biomaterials 35:970–982, 2014.
Reddy, P. P., D. J. Barrieras, G. Wilson, D. J. Bagli, G. A. McLorie, A. E. Khoury, and P. A. Merguerian. Regeneration of functional bladder substitutes using large segment acellular matrix allografts in a porcine model. J. Urol. 164:936–941, 2000.
Reing, J. E., B. N. Brown, K. A. Daly, J. M. Freund, T. W. Gilbert, S. X. Hsiong, A. Huber, K. E. Kullas, S. Tottey, M. T. Wolf, and S. F. Badylak. The effects of processing methods upon mechanical and biologic properties of porcine dermal extracellular matrix scaffolds. Biomaterials 31:8626–8633, 2010.
Reing, J. E., L. Zhang, J. Myers-Irvin, K. E. Cordero, D. O. Freytes, E. Heber-Katz, K. Bedelbaeva, D. McIntosh, A. Dewilde, S. J. Braunhut, and S. F. Badylak. Degradation products of extracellular matrix affect cell migration and proliferation. Tissue Eng. Part A 15:605–614, 2009.
Rieder, E., M. T. Kasimir, G. Silberhumer, G. Seebacher, E. Wolner, P. Simon, and G. Weigel. Decellularization protocols of porcine heart valves differ importantly in efficiency of cell removal and susceptibility of the matrix to recellularization with human vascular cells. J. Thorac. Cardiovasc. Surg. 127:399–405, 2004.
Rommer, E. A., M. Peric, and A. Wong. Urinary bladder matrix for the treatment of recalcitrant nonhealing radiation wounds. Adv. Skin Wound Care 26:450–455, 2013.
Rosario, D. J., G. C. Reilly, E. A. Salah, M. Glover, A. J. Bullock, and S. MacNeil. Decellularization and sterilization of porcine urinary bladder matrix for tissue engineering in the lower urinary tract. Regen. Med. 3:145–156, 2008.
Ross, E. A., M. J. Williams, T. Hamazaki, N. Terada, W. L. Clapp, C. Adin, G. W. Ellison, M. Jorgensen, and C. D. Batich. Embryonic stem cells proliferate and differentiate when seeded into kidney scaffolds. J. Am. Soc. Nephrol. 20:2338–2347, 2009.
Sadtler, K., B. W. Allen, K. Estrellas, F. Housseau, D. M. Pardoll, and J. H. Elisseeff. The scaffold immune microenvironment: Biomaterial-mediated immune polarization in traumatic and nontraumatic applications. Tissue Eng. Part A 23:1044–1053, 2017.
Sadtler, K., K. Estrellas, B. W. Allen, M. T. Wolf, H. Fan, A. J. Tam, C. H. Patel, B. S. Luber, H. Wang, K. R. Wagner, J. D. Powell, F. Housseau, D. M. Pardoll, and J. H. Elisseeff. Developing a pro-regenerative biomaterial scaffold microenvironment requires T helper 2 cells. Science 352:366–370, 2016.
Sadtler, K., M. T. Wolf, S. Ganguly, C. A. Moad, L. Chung, S. Majumdar, F. Housseau, D. M. Pardoll, and J. H. Elisseeff. Divergent immune responses to synthetic and biological scaffolds. Biomaterials 192:405–415, 2019.
Saldin, L. T., M. C. Cramer, S. S. Velankar, L. J. White, and S. F. Badylak. Extracellular matrix hydrogels from decellularized tissues: Structure and function. Acta Biomater. 49:1–15, 2017.
Sandor, M., H. Xu, J. Connor, J. Lombardi, J. R. Harper, R. P. Silverman, and D. J. McQuillan. Host response to implanted porcine-derived biologic materials in a primate model of abdominal wall repair. Tissue Eng. Part A 14:2021–2031, 2008.
Santoso, E. G., K. Yoshida, Y. Hirota, M. Aizawa, O. Yoshino, A. Kishida, Y. Osuga, S. Saito, T. Ushida, and K. S. Furukawa. Application of detergents or high hydrostatic pressure as decellularization processes in uterine tissues and their subsequent effects on in vivo uterine regeneration in murine models. PLoS ONE 9:e103201, 2014.
Sarathchandra, P., R. T. Smolenski, A. H. Y. Yuen, A. H. Chester, S. Goldstein, A. E. Heacox, M. H. Yacoub, and P. M. Taylor. Impact of γ-irradiation on extracellular matrix of porcine pulmonary valves. J. Surg. Res. 176:376–385, 2012.
Sasikumar, S., S. Chameettachal, B. Cromer, F. Pati, and P. Kingshott. Decellularized extracellular matrix hydrogels– cell behavior as function of matrix stiffness. Curr. Opin. Biomed. Eng. 10:123–133, 2019.
Sawada, K., D. Terada, T. Yamaoka, S. Kitamura, and T. Fujisato. Cell removal with supercritical carbon dioxide for acellular artificial tissue. J. Chem. Technol. Biotechnol. 83:943–949, 2008.
Sawai, T., N. Usui, K. Sando, Y. Fukui, S. Kamata, A. Okada, N. Taniguchi, N. Itano, and K. Kimata. Hyaluronic acid of wound fluid in adult and fetal rabbits. J. Pediatr. Surg. 32:41–43, 1997.
Schoen, F. J., and R. J. Levy. Calcification of tissue heart valve substitutes: Progress toward understanding and prevention. Ann. Thorac. Surg. 79:1072–1080, 2005.
Scholl, F. G., M. M. Boucek, K.-C. Chan, L. Valdes-Cruz, and R. Perryman. Preliminary experience with cardiac reconstruction using decellularized porcine extracellular matrix scaffold: Human applications in congenital heart disease. World J. Pediatr. Congenit. Hear. Surg. 1:132–136, 2010.
Sclamberg, S. G., J. E. Tibone, J. M. Itamura, and S. Kasraeian. Six-month magnetic resonance imaging follow-up of large and massive rotator cuff repairs reinforced with porcine small intestinal submucosa. J. Shoulder Elb. Surg. 13:538–541, 2004.
Sellaro, T. L., A. K. Ravindra, D. B. Stolz, and S. F. Badylak. Maintenance of hepatic sinusoidal endothelial cell phenotype in vitro using organ-specific extracellular matrix scaffolds. Tissue Eng. 13:2301–2310, 2007.
Seo, Y., Y. Jung, and S. H. Kim. Decellularized heart ECM hydrogel using supercritical carbon dioxide for improved angiogenesis. Acta Biomater. 67:270–281, 2018.
Shah, M., P. Kc, K. M. Copeland, J. Liao, and G. Zhang. A thin layer of decellularized porcine myocardium for cell delivery. Sci. Rep. 8:1–11, 2018.
Shah, B. C., M. M. Tiwari, M. R. Goede, M. J. Eichler, R. R. Hollins, C. L. McBride, J. S. Thompson, and D. Oleynikov. Not all biologics are equal!. Hernia 15:165–171, 2011.
Shamis, Y., E. Hasson, A. Soroker, E. Bassat, Y. Shimoni, T. Ziv, R. V. Sionov, and E. Mitrani. Organ-specific scaffolds for in vitro expansion, differentiation, and organization of primary lung cells. Tissue Eng. Part C Methods 17:861–870, 2011.
Shin, K., K. H. Koo, J. Jeong, S. J. Park, D. J. Choi, Y.-G. Ko, and H. Kwon. Three-dimensional culture of salivary gland stem cell in orthotropic decellularized extracellular matrix hydrogels. Tissue Eng. Part A 2019. https://doi.org/10.1089/ten.tea.2018.0308.
Shojaie, S., L. Ermini, C. Ackerley, J. Wang, S. Chin, B. Yeganeh, M. Bilodeau, M. Sambi, I. Rogers, J. Rossant, C. E. Bear, and M. Post. Acellular lung scaffolds direct differentiation of endoderm to functional airway epithelial cells: Requirement of matrix-bound HS proteoglycans. Stem Cell Rep. 4:419–430, 2015.
Sicari, B. M., V. Agrawal, B. F. Siu, C. J. Medberry, C. L. Dearth, N. J. Turner, and S. F. Badylak. A murine model of volumetric muscle loss and a regenerative medicine approach for tissue replacement. Tissue Eng. Part A 18:1941–1948, 2012.
Sicari, B. M., J. L. Dziki, B. F. Siu, C. J. Medberry, C. L. Dearth, and S. F. Badylak. The promotion of a constructive macrophage phenotype by solubilized extracellular matrix. Biomaterials 35:8605–8612, 2014.
Sicari, B. M., S. A. Johnson, B. F. Siu, P. M. Crapo, K. A. Daly, H. Jiang, C. J. Medberry, S. Tottey, N. J. Turner, and S. F. Badylak. The effect of source animal age upon the in vivo remodeling characteristics of an extracellular matrix scaffold. Biomaterials 33:5524–5533, 2012.
Sicari, B. M., J. P. Rubin, C. L. Dearth, M. T. Wolf, F. Ambrosio, M. Boninger, N. J. Turner, D. J. Weber, T. W. Simpson, A. Wyse, E. H. P. Brown, J. L. Dziki, L. E. Fisher, S. Brown, and S. F. Badylak. An acellular biologic scaffold promotes skeletal muscle formation in mice and humans with volumetric muscle loss. Sci. Transl. Med. 6:234ra58, 2014.
Sikin, A. M., and S. S. H. Rizvi. Recent patents on food, nutrition, and agriculture. Preface. Recent. Pat. Food Nutr. Agric 5:1, 2013.
Silva, A. C., S. C. Rodrigues, J. Caldeira, A. M. Nunes, V. Sampaio-Pinto, T. P. Resende, M. J. Oliveira, M. A. Barbosa, S. Thorsteinsdóttir, D. S. Nascimento, and P. Pinto-do-Ó. Three-dimensional scaffolds of fetal decellularized hearts exhibit enhanced potential to support cardiac cells in comparison to the adult. Biomaterials 104:52–64, 2016.
Simsa, R., A. M. Padma, P. Heher, M. Hellström, A. Teuschl, L. Jenndahl, N. Bergh, and P. Fogelstrand. Systematic in vitro comparison of decellularization protocols for blood vessels. PLoS ONE 13:1–19, 2018.
Singelyn, J. M., and J. A. DeQuach. Naturally derived myocardial matrix as an injectable scaffold for cardiac tissue engineering. Biomaterials 30:5409–5416, 2009.
Sinha, P., D. Zurakowski, T. K. S. Kumar, D. He, C. Rossi, and R. A. Jonas. Effects of glutaraldehyde concentration, pretreatment time, and type of tissue (porcine versus bovine) on postimplantation calcification. J. Thorac. Cardiovasc. Surg. 143:224–227, 2012.
Slaughter, M. S., K. G. Soucy, R. G. Matheny, B. C. Lewis, M. F. Hennick, Y. Choi, G. Monreal, M. A. Sobieski, G. A. Giridharan, and S. C. Koenig. Development of an extracellular matrix delivery system for effective intramyocardial injection in ischemic tissue. ASAIO J. 60:730–736, 2014.
Soler, J. A., S. Gidwani, and M. J. Curtis. Early complications from the use of porcine dermal collagen implants (Permacol ™) as bridging constructs in the repair of massive rotator cuff tears: A report of 4 cases. Acta Orthop. Belg. 73:432–436, 2007.
Sonnenschein, C., and A. M. Soto. The society of cells—Cancer and control of cell proliferation. New York: Springer Verlag, pp. 99–133, 1999.
Soto, A. M., and C. Sonnenschein. The tissue organization field theory of cancer: A testable replacement for the somatic mutation theory. Bioessays 33:332–340, 2011.
Soucy, K. G., E. F. Smith, G. Monreal, G. Rokosh, B. B. Keller, F. Yuan, R. G. Matheny, A. M. Fallon, B. C. Lewis, L. C. Sherwood, M. A. Sobieski, G. A. Giridharan, S. C. Koenig, and M. S. Slaughter. Feasibility study of particulate extracellular matrix (P-ECM) and left ventricular assist device (HVAD) therapy in chronic ischemic heart failure bovine model. ASAIO J. 61:161–169, 2015.
Spang, M. T., and K. L. Christman. Extracellular matrix hydrogel therapies: In vivo applications and development. Acta Biomater. 68:1–14, 2018.
Sun, Y., G. Chen, and Y. Lv. Effects of hypoxia on the biological behavior of MSCs seeded in demineralized bone scaffolds with different stiffness. Acta Mech. Sin. Xuebao 35:309–320, 2019.
Sun, W. Q., and P. Leung. Calorimetric study of extracellular tissue matrix degradation and instability after gamma irradiation. Acta Biomater. 4:817–826, 2008.
Sung, H. W., Y. Chang, C. T. Chiu, C. N. Chen, and H. C. Liang. Crosslinking characteristics and mechanical properties of a bovine pericardium fixed with a naturally occurring crosslinking agent. J. Biomed. Mater. Res. 47:116–126, 1999.
Sutherland, A. J., E. C. Beck, S. C. Dennis, G. L. Converse, R. A. Hopkins, C. J. Berkland, and M. S. Detamore. Decellularized cartilage may be a chondroinductive material for osteochondral tissue engineering. PLoS ONE 10:1–13, 2015.
Toole, B. P., T. N. Wight, and M. I. Tammi. Hyaluronan-cell interactions in cancer and vascular disease. J. Biol. Chem. 277:4593–4596, 2002.
Tottey, S., S. A. Johnson, P. M. Crapo, J. E. Reing, L. Zhang, H. Jiang, C. J. Medberry, B. Reines, and S. F. Badylak. The effect of source animal age upon extracellular matrix scaffold properties. Biomaterials 32:128–136, 2011.
Turner, N. J., J. S. Badylak, D. J. Weber, and S. F. Badylak. Biologic scaffold remodeling in a dog model of complex musculoskeletal injury. J. Surg. Res. 176:490–502, 2012.
Uriarte, J. J., P. N. Nonaka, N. Campillo, R. K. Palma, E. Melo, L. V. F. de Oliveira, D. Navajas, and R. Farré. Mechanical properties of acellular mouse lungs after sterilization by gamma irradiation. J. Mech. Behav. Biomed. Mater. 40:168–177, 2014.
Uriel, S., D. Ph, E. Labay, M. Francis-sedlak, M. L. Moya, R. R. Weichselbaum, N. Ervin, Z. Cankova, E. M. Brey, and D. Ph. Extraction and assembly of tissue-derived gels for cell culture and tissue engineering. Tissue Eng. Part C. Methods 15:309–321, 2009.
U.S. Food and Drug Administration. Guidance for industry: Current good tissue practice (CGTP) and additional requirements for manufacturers of human cells, tissues, and cellular and tissue-based products (HCT/Ps)., 2011.
U.S. Food and Drug Administration. Medical devices containing materials derived from animal sources (Except for in vitro diagnostic devices): Guidance for industry and Food and Drug Administration staff., 2019.
Utomo, L., M. Pleumeekers, L. Nimeskern, S. Nürnberger, K. S. Stok, F. Hildner, and G. J. V. M. Van Osch. Preparation and characterization of a decellularized cartilage scaffold for ear cartilage reconstruction. Biomed. Mater. 10:015010, 2015.
Valentin, J. E., J. S. Badylak, G. P. McCabe, and S. F. Badylak. Extracellular matrix bioscaffolds for orthopaedic applications: A comparative histologic study. J. Bone Jt. Surg. 88A:2673–2686, 2006.
Valentin, J. E., A. M. Stewart-Akers, T. W. Gilbert, and S. F. Badylak. Macrophage participation in the degradation and remodeling of extracellular matrix scaffolds. Tissue Eng. Part A 15:1687–1694, 2009.
Valentin, J. E., N. J. Turner, T. W. Gilbert, and S. F. Badylak. Functional skeletal muscle formation with a biologic scaffold. Biomaterials 31:7475–7484, 2010.
Van Der Merwe, Y., A. E. Faust, E. T. Sakalli, C. C. Westrick, G. Hussey, I. P. Con, V. L. N. Fu, S. F. Badylak, and M. B. Steketee. Matrix-bound nanovesicles prevent ischemia-induced retinal ganglion cell axon degeneration and death and preserve visual function. Sci. Rep. 9:3482, 2019.
VeDepo, M. C., E. E. Buse, R. W. Quinn, T. D. Williams, M. S. Detamore, R. A. Hopkins, and G. L. Converse. Species-specific effects of aortic valve decellularization. Acta Biomater. 50:249–258, 2017.
Visser, J., P. A. Levett, N. C. R. Te Moller, J. Besems, K. W. M. Boere, M. H. P. Van Rijen, J. C. De Grauw, W. J. A. Dhert, P. R. Van Weeren, and J. Malda. Crosslinkable hydrogels derived from cartilage, meniscus, and tendon tissue. Tissue Eng. Part A 21:1195–1206, 2015.
Voytik-Harbin, S. L., A. O. Brightman, B. Z. Waisner, J. P. Robinson, and C. H. Lamar. Small intestinal submucosa: A tissue-derived extracellular matrix that promotes tissue-specific growth and differentiation of cells in vitro. Tissue Eng. 4:157–174, 1998.
Walton, J. R., N. K. Bowman, Y. Khatib, J. Linklater, and G. A. C. Murrell. Restore orthobiologic implant: Not recommended for augmentation of rotator cuff repairs. J. Bone Jt. Surg. Ser. A 89:786–791, 2007.
Wang, Y., J. Bao, X. Wu, Q. Wu, Y. Li, Y. Zhou, L. Li, and H. Bu. Genipin crosslinking reduced the immunogenicity of xenogeneic decellularized porcine whole-liver matrices through regulation of immune cell proliferation and polarization. Sci. Rep. 6:1–16, 2016.
Wang, R. M., and K. L. Christman. Decellularized myocardial matrix hydrogels: In basic research and preclinical studies. Adv. Drug Deliv. Rev. 96:77–82, 2016.
Wang, L., J. A. Johnson, D. W. Chang, and Q. Zhang. Decellularized musculofascial extracellular matrix for tissue engineering. Biomaterials 34:2641–2654, 2013.
Wang, R. M., T. D. Johnson, J. He, Z. Rong, M. Wong, V. Nigam, A. Behfar, Y. Xu, and K. L. Christman. Humanized mouse model for assessing the human immune response to xenogeneic and allogeneic decellularized biomaterials. Biomaterials 129:98–110, 2017.
Wang, Z., D. W. Long, Y. Huang, W. C. W. Chen, K. Kim, and Y. Wang. Decellularized neonatal cardiac extracellular matrix prevents widespread ventricular remodeling in adult mammals after myocardial infarction. Acta Biomater. 87:140–151, 2019.
Wang, J. K., B. Luo, V. Guneta, L. Li, S. E. M. Foo, Y. Dai, T. T. Y. Tan, N. S. Tan, C. Choong, and M. T. C. Wong. Supercritical carbon dioxide extracted extracellular matrix material from adipose tissue. Mater. Sci. Eng. C 75:349–358, 2017.
Wang, Q., C. Zhang, L. Zhang, W. Guo, G. Feng, S. Zhou, Y. Zhang, T. Tian, Z. Li, and F. Huang. The preparation and comparison of decellularized nerve scaffold of tissue engineering. J. Biomed. Mater. Res. A 102:4301–4308, 2014.
Wassenaar, J. W., R. L. Braden, K. G. Osborn, and K. L. Christman. Modulating in vivo degradation rate of injectable extracellular matrix hydrogels. J. Mater. Chem. B 4:2794–2802, 2016.
Wassenaar, J. W., R. Gaetani, J. J. Garcia, R. L. Braden, C. G. Luo, D. Huang, A. N. DeMaria, J. H. Omens, and K. L. Christman. Evidence for mechanisms underlying the functional benefits of a myocardial matrix hydrogel for post-MI treatment. J. Am. Coll. Cardiol. 67:1074–1086, 2016.
Wei, H. J., H. C. Liang, M. H. Lee, Y. C. Huang, Y. Chang, and H. W. Sung. Construction of varying porous structures in acellular bovine pericardia as a tissue-engineering extracellular matrix. Biomaterials 26:1905–1913, 2005.
West, D. C., D. M. Shaw, P. Lorenz, N. S. Adzick, and M. T. Longaker. Fibrotic healing of adult and late gestation fetal wounds correlates with increased hyaluronidase activity and removal of hyaluronan. Int. J. Biochem. Cell Biol. 29:201–210, 1997.
Whitby, D. J., and M. W. J. Ferguson. The extracellular matrix of lip wounds in fetal, neonatal and adult mice. Development 112:651–668, 1991.
White, L. J., T. J. Keane, A. Smoulder, L. Zhang, A. A. Castleton, J. E. Reing, N. J. Turner, C. L. Dearth, and S. F. Badylak. The impact of sterilization upon extracellular matrix hydrogel structure and function. J. Immunol. Regen. Med. 2:11–20, 2018.
White, L. J., A. J. Taylor, D. M. Faulk, T. J. Keane, L. T. Saldin, J. E. Reing, I. T. Swinehart, N. J. Turner, B. D. Ratner, and S. F. Badylak. The impact of detergents on the tissue decellularization process: A ToF-SIMS study. Acta Biomater. 50:207–219, 2017.
Williams, C., K. P. Quinn, I. Georgakoudi, and L. D. Black. Young developmental age cardiac extracellular matrix promotes the expansion of neonatal cardiomyocytes in vitro. Acta Biomater. 10:194–204, 2014.
Wolf, M. T., K. A. Daly, E. P. Brennan-Pierce, S. A. Johnson, C. Carruthers, A. D. Amore, S. P. Nagarkar, S. S. Velankar, and S. F. Badylak. A hydrogel derived from decellularized dermal extracellular matrix. Biomaterials 33:7028–7038, 2012.
Wolf, M. T., K. A. Daly, J. E. Reing, and S. F. Badylak. Biologic scaffold composed of skeletal muscle extracellular matrix. Biomaterials 33:2916–2925, 2012.
Wolf, M. T., S. Ganguly, T. L. Wang, C. W. Anderson, K. Sadtler, R. Narain, C. Cherry, A. J. Parrillo, B. V. Park, G. Wang, F. Pan, S. Sukumar, D. M. Pardoll, and J. H. Elisseeff. A biologic scaffold–associated type 2 immune microenvironment inhibits tumor formation and synergizes with checkpoint immunotherapy. Sci. Transl. Med. 11:eaat7973, 2019.
Wolf, M. T., Y. Vodovotz, S. Tottey, B. N. Brown, and S. F. Badylak. Predicting in vivo responses to biomaterials via combined in vitro and in silico analysis. Tissue Eng. Part C Methods 21:148–159, 2015.
Wood, J. D., A. Simmons-Byrd, A. R. Spievack, and S. F. Badylak. Use of a particulate extracellular matrix bioscaffold for treatment of acquired urinary incontinence in dogs. J. Am. Vet. Med. Assoc. 226:1095–1097, 2005.
Yang, Q., J. Peng, Q. Guo, J. Huang, L. Zhang, J. Yao, F. Yang, S. Wang, W. Xu, A. Wang, and S. Lu. A cartilage ECM-derived 3-D porous acellular matrix scaffold for in vivo cartilage tissue engineering with PKH26-labeled chondrogenic bone marrow-derived mesenchymal stem cells. Biomaterials 29:2378–2387, 2008.
Yang, G., B. B. Rothrauff, H. Lin, R. Gottardi, P. G. Alexander, and R. S. Tuan. Enhancement of tenogenic differentiation of human adipose stem cells by tendon-derived extracellular matrix. Biomaterials 34:9295–9306, 2013.
Yin, Z., X. Chen, T. Zhu, J. J. Hu, H. X. Song, W. L. Shen, L. Y. Jiang, B. C. Heng, J. F. Ji, and H. W. Ouyang. The effect of decellularized matrices on human tendon stem/progenitor cell differentiation and tendon repair. Acta Biomater. 9:9317–9329, 2013.
Young, D. A., V. Bajaj, and K. L. Christman. Decellularized adipose matrix hydrogels stimulate in vivo neovascularization and adipose formation. J. Biomed. Mater. Res. Part A 102:1641–1651, 2014.
Young, D. A., Y. S. Choi, A. J. Engler, and K. L. Christman. Stimulation of adipogenesis of adult adipose-derived stem cells using substrates that mimic the stiffness of adipose tissue. Biomaterials 34:8581–8588, 2013.
Young, D. A., K. C. McGilvray, N. Ehrhart, and T. W. Gilbert. Comparison of in vivo remodeling of urinary bladder matrix and acellular dermal matrix in an ovine model. Regen. Med. 13:759–773, 2018.
Youngstrom, D. W., I. Rajpar, D. L. Kaplan, and J. G. Barrett. A bioreactor system for in vitro tendon differentiation and tendon tissue engineering. J. Orthop. Res. 33:911–918, 2015.
Zambon, A., M. Vetralla, L. Urbani, M. F. Pantano, G. Ferrentino, M. Pozzobon, N. Pugno, P. De Coppi, N. Elvassore, and S. Spilimbergo. Dry acellular oesophageal matrix prepared by supercritical carbon dioxide. J. Supercrit. Fluids 115:33–41, 2016.
Zantop, T., T. W. Gilbert, M. Yoder, and S. F. Badylak. Extracellular matrix scaffolds are repopulated by bone marrow-derived cells in a mouse model of achilles tendon reconstruction. J. Orthop. Res. 24:1299–1309, 2006.
Zhang, X., and J. Dong. Direct comparison of different coating matrix on the hepatic differentiation from adipose-derived stem cells. Biochem. Biophys. Res. Commun. 456:938–944, 2015.
Zhang, J., B. Li, and J. H.-C. Wang. The role of engineered tendon matrix in the stemness of tendon stem cells in vitro and the promotion of tendon-like tissue formation in vivo. Biomaterials 32:6972–6981, 2011.
Zhao, Z. Q., J. D. Puskas, D. Xu, N. P. Wang, M. Mosunjac, R. A. Guyton, J. Vinten-Johansen, and R. Matheny. Improvement in cardiac function with small intestine extracellular matrix is associated with recruitment of C-kit cells, myofibroblasts, and macrophages after myocardial infarction. J. Am. Coll. Cardiol. 55:1250–1261, 2010.
Zhou, Q., X. Ye, R. Sun, Y. Matsumoto, M. Moriyama, Y. Asano, Y. Ajioka, and Y. Sauo. Differentiation of mouse induced pluripotent stem cells into alveolar epithelial cells in vitro for use in vivo. Stem Cells Transl. Med. 3:675–685, 2014.
Zhu, T., Q. Tang, Y. Shen, H. Tang, L. Chen, and J. Zhu. An acellular cerebellar biological scaffold: Preparation, characterization, biocompatibility and effects on neural stem cells. Brain Res. Bull. 113:48–57, 2015.
Zuo, H., D. Peng, B. Zheng, X. Liu, Y. Wang, L. Wang, X. Zhou, and J. Liu. Regeneration of mature dermis by transplanted particulate acellular dermal matrix in a rat model of skin defect wound. J. Mater. Sci. Mater. Med. 23:2933–2944, 2012.
Conflict of interest
SF Badylak is the Chief Scientific Officer of ECM Therapeutics, Inc. MC Cramer has nothing to disclose.
Funding
MC Cramer was supported by the National Heart, Lung and Blood Institute of the National Institutes of Health (5T32HL076124-12).
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Jennifer West oversaw the review of this article.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Cramer, M.C., Badylak, S.F. Extracellular Matrix-Based Biomaterials and Their Influence Upon Cell Behavior. Ann Biomed Eng 48, 2132–2153 (2020). https://doi.org/10.1007/s10439-019-02408-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-019-02408-9