Abstract
Finite element (FE) modelling can be a very resourceful tool in the field of cardiovascular devices. To ensure result reliability, FE models must be validated experimentally against physical data. Their clinical application (e.g., patients’ suitability, morphological evaluation) also requires fast simulation process and access to results, while engineering applications need highly accurate results. This study shows how FE models with different mesh discretisations can suit clinical and engineering requirements for studying a novel device designed for percutaneous valve implantation. Following sensitivity analysis and experimental characterisation of the materials, the stent-graft was first studied in a simplified geometry (i.e., compliant cylinder) and validated against in vitro data, and then in a patient-specific implantation site (i.e., distensible right ventricular outflow tract). Different meshing strategies using solid, beam and shell elements were tested. Results showed excellent agreement between computational and experimental data in the simplified implantation site. Beam elements were found to be convenient for clinical applications, providing reliable results in less than one hour in a patient-specific anatomical model. Solid elements remain the FE choice for engineering applications, albeit more computationally expensive (>100 times). This work also showed how information on device mechanical behaviour differs when acquired in a simplified model as opposed to a patient-specific model.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Over the last decade, increasingly refined computational methods have become accepted tools to study biomedical devices as part of the pre-clinical stage of device design, not only by the device manufactures, but also by the regulatory bodies, such as the Food and Drug Administration.18 However, the application of these techniques is still often limited to the study of the device in isolation and not within the context of its application—i.e., the patient environment.15 For the majority of medical applications, information about each individual patient characteristics and an understanding of the interactions between the device and the patient’s anatomy and function are essential to ensure safe device design. If patient-specific considerations are taken into account,24 computational analyses can help enhance the optimisation of the mechanical performance of devices, accelerating the time of development and reducing testing costs.3
Patient-specific cardiovascular modelling, combining computational techniques with clinical data, can be a resourceful tool to improve operational planning and procedural outcomes31,35,36 This method has already been employed in understanding cardiac electro-mechanics33 and blood fluid dynamics in large part of the circulatory system11,12,20,34 Such models can also drive the development of novel devices,29 taking into account anatomical elements that are more representative than animal surrogates,6 and integrating standard in vitro tests with patient-specific loading conditions.30
While some cardiovascular applications (e.g., coronary stents) could benefit from a patient-specific approach, but do not strictly require it,23 for percutaneous heart valve implantation these models are crucial. Percutaneous techniques are relatively new,7,14 or even under development,13,21 hence modelling tools can contribute to improve these procedures (e.g., design modifications or identification of optimal route for device insertion) and increase patient safety in the early introduction of these devices into clinical practice. In particular, in percutaneous pulmonary valve implantation (PPVI), the range of potential implantation site anatomies, sizes and dynamics is vast and the interaction between the device and each individual’s implantation site (i.e., valved stent positioning and anchoring) is the determinant of procedural success and device performance.28
In general computational cardiovascular models need to be robustly validated.2 The primary goal of validation is to provide confidence that experimental and computational data are sufficiently related within definite boundary condition.25 Following validation, in order for a clinical application of computational methods to be viable, they need to flexibly take into account patient-specific properties, and provide a comprehensive set of results in a short time. On the other hand, from an engineering perspective, models can cost-effectively aid the design phase by integrating realistic loading scenarios for accurate simulation of “worst case” mechanical behaviour. However, they require higher degrees of complexity at the expense of time and computational cost.19
This study aims to validate and identify the optimal computational modelling strategies to respond to both clinical and engineering requirements for simulations involving percutaneous devices. As a case study, this approach has been implemented on a novel PPVI device.29
Materials and Methods
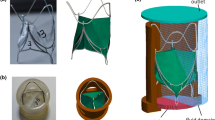
The novel PPVI device (Medtronic Inc, MN, USA) is a self-expandable stent-graft with a porcine pericardial valve sewn into its central portion.29 The stent-graft is composed of six Nitinol zigzag rings interwoven with a Polyester fabric to form an hourglass symmetrical shape (Fig. 1). The external rings (rings 1 and 6, Fig. 1a) are connected to the rest of the structure by means of the graft alone, thus withstanding deformations more independently from the rest of the rings, where zigzag crown-to-crown sutures are placed.8
Finite element (FE) analysis of the implantation and function of such a complex device in a patient-specific vessel was developed through steps of increasing complexity, in order to find the most efficient modelling strategy in response to either clinical and/or engineering needs. The first step was the study of the selected finite elements and material models by means of a sensitivity analysis on a single Nitinol wire (rod bending test) and characterisation of a simple implantation site with in vitro data (tube compliance test). Following from these considerations, the device FE model was built, deployed inside the simplified implantation site and the numerical results validated against a purposely designed experimental test (stent-graft tested in a compliant tube). Finally, the validated model of the device was studied in a patient-specific anatomy (stent-graft tested in a patient-specific implantation site).
All simulations were performed with the commercial finite element code ABAQUS/Explicit 6.10 (Simulia, Providence, RI, USA) assuming quasi-static conditions, and run on an 8-node computing cluster. The quasi-static condition was verified with kinetic energy values lower than the internal energies (ratio <5%32). Simulation times were compared between different FE strategies.
Rod Bending Test
A thin rod resembling the geometry of one strut of the stent (cross-section diameter = 0.28 mm, length = 13.4 mm) was designed. Nitinol properties were provided by the manufacturer9 and super-elastic behaviour was implemented using the built-in user material model.1 Two classes of elements were considered to mesh the rod: 8-node linear hexahedral solid elements, with reduced integration and hourglass stabilisation, and 2-node Timoshenko beam elements, with 5 × 5 cross section integration points. The solid elements were chosen for accurate and detailed simulation of the complex problem of stent deployment. The beam elements, on the other hand, were chosen to reduce the computational costs as a result of a slenderness assumption on the wire struts. A grid sensitivity analysis was carried out comparing four solid (solid6, solid8, solid10, and solid12 with 6 × 6, 8 × 8, 10 × 10, and 12 × 12 elements along the rod section diameters, respectively) and four beam (beam6, beam12, beam45 and beam200 with 6, 12, 45, and 200 elements along the beam length) mesh densities. A bending test was performed with a low and a high load (F = 0.026 N and 0.2 N, respectively) to analyse the model’s response both in the linear and super-elastic region. For the low load, displacements and deformations were compared with the analytical solution of a rod bending under a tip load. For the high load, considerations were made on the basis of the results obtained with the finest solid mesh (solid12) that was assumed to be the closest to the continuous problem solution. One extremity of the rod was constrained by encastre, and the load was concentrated on the free tip.
Tube Compliance Test
A cylindrical tube (internal diameter = 23 mm, thickness = 1.5 mm, length = 80 mm) was designed to replicate the simplified environment adopted during stent preclinical testing. The tube was modelled as homogeneous, isotropic and linear-elastic material. Two types of meshes were tested to compare accuracy and computational costs: 16,024 eight-node linear hexahedral elements and 7,040 four-node quadrangular shell elements. These models were validated experimentally. The same cylinder was in fact rapid prototyped by PolyJet technique.5 A compliance test was carried out starting from a closed volume of water V 0 = 29.9 ml and varying the volume (ΔV = 10 ml) incrementally in steps of dV = 1 ml. Pressure (P) was simultaneously recorded inside the cylinder using a fiber-optic pressure catheter (Preclin 420, Samba Sensors, Västra Frölunda, Sweden). The pressure–volume relationship was analysed to deduce a compliance value C equal to 0.1 ml mmHg−1 for the imposed ΔV, as estimated from the slope of the PV-curve. The value of the experimental Young’s modulus was \( E = \frac{PR}{k} \cdot \frac{\Updelta Circ}{{Circ_{0} }} \) = 0.7 MPa, where R is the internal radius, k the wall thickness, \( \Updelta Circ \) the variation in circumference and \( Circ_{0} \) the initial circumference. These experimental values were fed into the FE model, imposing the same E and the measured density of the material (ρ = 1190 kg m−3), and assuming Poisson’s ratio of 0.25.22 The compliance test was repeated computationally, imposing a variation in the internal pressure ΔP [0–82.5 mmHg] equal to that measured experimentally. The corresponding ΔV was calculated and compared between the two meshes and with the in vitro data. Constrains were applied to the nodes of the cylinder extremity sections to allow only radial displacements.
Data of computational and experimental analyses were compared using Pearson’s correlation and p < 0.05 was considered to denote statistical significance. Statistical analysis was performed using SPSS for Windows, version 19 (SPSS, Chicago, IL, USA).
Stent-Graft Tested in a Compliant Tube
The CAD model of the stent-graft was designed resembling the original design (Fig. 1). The valve was not modelled in FE analysis. The Nitinol stent wires were recreated with 0.28 mm diameter for ring 1, 2, 5 and 6 and 0.38 mm diameter for ring 3 and 4, according to manufacturer specifications.
Following from sensitivity analysis results on the rod bending test, the six stent rings were meshed using 370,176 hexahedral solid elements and 900 beam elements. In both cases, the fabric, designed as a surface connecting the wires, was meshed with quadrilateral shell elements as the thickness is significantly smaller than the other dimensions, using 38,994 and 5,094 elements, respectively. The fabric mesh shared edge-nodes with the corresponding stent ring elements in order to mimic the suture between stent and graft. The polyester constitutive behaviour was described through a reduced polynomial hyperelastic model.9
Four analyses were performed by testing the different available combinations of mesh elements, hereby abbreviated:
-
SoSo: stent and implantation site both meshed with solid elements;
-
SoSh: stent meshed with solid elements and implantation site with shell elements;
-
BeSo: stent meshed with beam elements and implantation site with solid elements; and
-
BeSh: stent meshed with beam elements and implantation site with shell elements.
Simulations were performed following four steps to replicate the implantation procedure and function of the stent-graft during a simulated cardiac cycle. Firstly, the device was positioned coaxially and in the central portion of the cylinder model. Secondly, the stent-graft was crimped down from its original configuration to 8.3 mm diameter (catheter dimensions) by a applying a radial displacement (=16.75 mm) to a cylindrical sheath made of 4-node quadrilateral surface elements with reduced integration. Thirdly, the sheath was retracted with rigid axial displacement (=80 mm), causing the gradual release of the stent-graft inside the compliant cylinder model and consequent interaction of the terminal rings with the cylinder wall. Lastly, a linear pressure variation (ΔP = 46 mmHg) was applied to the internal surface of the stented vessel to mimic the effects of the cardiac cycle following from data gathered in the analogous experimental model and lying within a physiological range.4,10,16 The extremities of the implantation site were constrained to prevent rigid displacements.
For validation purposes, results from each computational model were compared with an experimental test involving the release of the stent-graft without valve inside the same rapid prototyped cylinder. A simple mock circulatory system4 was assembled including a ventricular assist device (Excor 60 cc, Berlin Heart, Berlin, Germany) driven by a PC-controlled piston, and implementing pulmonary resistance (=3.9 WU) and compliance (=1.65 ml/mmHg) with needle-pinch valves and Windkessel chambers, respectively. These values are within a physiological range.4 Pressure was monitored inside the cylinder using a fiber-optic sensor (Preclin 420), measuring a pulse of 100 mmHg.
Following the application of the same pressure variation to the FE model, the deployment diameter of the distal ring inside the cylinder at systole and diastole was compared between the four computational models against the in vitro results. Maximum principal strains in the stent rings after crimping were also evaluated.
Stent-Graft Tested in a Patient-Specific Implantation Site
The model of patient-specific anatomy was derived from a 33-year-old male referred to our centre for treatment of pulmonary valve dysfunction. The dimensions of the patient’s pulmonary artery precluded a percutaneous approach to pulmonary valve replacement with the current PPVI device, but the patient was considered a suitable candidate for the novel device.4 The right ventricular outflow tract (RVOT) and main pulmonary artery morphology was reconstructed from CT images.28 This was imported into the FE code and meshed with 60,932 solid elements and 30,466 shell elements, according to the mesh results of the simplified implantation site.
The four device-implantation site models (i.e., SoSo, SoSh, BeSo and BeSh) were tested also in this scenario. Simulations were performed following the four steps described above, with the distal portion of the device positioned close to the bifurcation in relation to the patient-specific geometry and a physiological cyclic load of ΔP = 46 mmHg. The pulsatile load was applied three times to stabilise the strain variation 17 and therefore evaluate the wire mechanical behaviour in patient-specific conditions.26, 27
Differences between the four meshing models were evaluated in terms of displacements from the undeformed shape and strain distribution. Displacements were calculated at the crowns of all rings both in systole and diastole. The coefficient of variation (CV = standard deviation/mean × 100, [%]) of the displacements was calculated for each crown vertex. Maximum principal strains were evaluated at systole and diastole for all simulations. The mean and amplitude strains from the third loading cycle were used to evaluate the influence of implantation site morphology on device deformation. Results of SoSo tests were compared between the RVOT and simplified cylindrical models, both subjected to the same physiological ΔP.
Finally, two parameters were adopted to assess clinical feasibility of the PPVI procedure in the selected candidate. (i) A standardised ring diameter was calculated as the mean between the 3 diameters (D1, D2 and D3 as from Fig. 1b) obtained for each section of the stent-graft. This diameter indicates the degree of compression of the struts compared to the undeformed configuration which has to be >20% in either the proximal or the distal ring to guarantee safe anchoring.9 (ii) The ratio between maximum and minimum diameters was calculated for the central rings as an indication of eccentricity. Indeed, the central portion of the stent-graft which hosts the valve needs to be circular for optimal valve function.
Results
Rod Bending Tests
The results of the sensitivity test are reported in Table 1. For the solid discretisation, a good compromise between number of elements, convergence and calculation time was met with mesh solid8, which was therefore chosen for modelling the wires of the entire stent. When beam elements were used, in the case of elastic material properties, there were no substantial differences in the solutions using coarse or refined meshes. However, in the nonlinear analysis, the solution diverged when using a high number of elements. The low number of elements in beam6 was not sufficient to replicate reliably the curved zigzag geometry of the stent rings; therefore, beam12 was chosen to mesh the wires of the full stent.
Tube Compliance Test
The results of the compliance tests on the cylinder are shown in the pressure–volume curve in Fig. 2. There was excellent correlation between in vitro measured volumes and computational calculated volumes when both solid (R = 0.9997, p < 0.0001) and shell (R = 0.9994, p < 0.0001) elements were used to discretise the cylinder.
Stent-Graft Tested in a Compliant Tube
The distribution of maximum principal strains on the stent at the end of the crimping phase was equivalent, with highest values close to the crowns of each ring, but differences were documented in terms of peaks: solid and beam models showed a peak of 7.2% and 6.5% respectively on ring 1 and 6; 6.3% and 6.5% on ring 2 and 5; and 6.5 and 7.7% on ring 3 and 4.
The results following release and pressurisation in the cylinder are reported in Table 2. In the experimental setup, diameters were measured as 23.83 mm and 27.55 mm in diastole and systole, respectively.4 The maximum diameter difference of computational and in vitro tests varied between 1.4% during diastole (BeSh) and 2.2% during systole (SoSo). Maximum principal strains were concentrated in the external rings (i.e., ring 1 and 6) which were the most compressed rings after release and fully in contact with the cylindrical wall. Overall, the stents meshed with beam elements showed higher peaks of strain than the solid counterparts at deployment. Furthermore, in beam models, the displacements due to pressure variation provided higher strain amplitudes than in solid models (0.33% vs. 0.15%).
Stent-Graft Tested in a Patient-Specific Implantation Site
The sequential phases of device implantation within the patient-specific geometry are shown in Fig. 3. The presence of the protective sheath, that was retrieved to allow release of the device, guaranteed realistic deployment and positioning in the patient model with the distal part anchoring to the outflow tract followed by expansion of the central portion and, lastly, opening of the proximal rings.
The four simulations were completed in greatly different running times (Table 3), with SoSo lasting up to 140 h, while BeSh lasted slightly less than 1 h.
Values of CV (Table 4) showed a maximum average variation for the proximal ring during both systole (6.2%) and diastole (5.3%). The positioning discrepancy was lower than 5% for all the other rings.
Maximum mean strain of 3.79% and 4.48% were measured on models SoSh and BeSh, respectively. In all simulations, the strain amplitude did not significantly differ between 0.24% (SoSh) and 0.27% (BeSh).
Diameters of each ring are reported in Fig. 4 during systole and diastole. Overall, the measures of the proximal and distal rings guaranteed safe anchoring throughout the simulated cardiac cycle, the average of ring 6 being smaller than 80% compared to the undeformed shape (=33.8 mm). Maximum values of eccentricity at the central section were 1.05 in systole in BeSh model and 1.11 in diastole in BeSh and BeSo models, showing quasi-circular cross section of the rings holding the valve.
Comparison of SoSo models in both cylindrical and patient-specific implantation sites is shown in Fig. 5. Maximum principal stresses distributed on the inner wall of the implantation site are shown at end diastole (Fig. 6). Higher stresses were observed for those simulations with the RVOTs modelled with shell elements and the stent modelled with beam elements.
Discussion
Different finite element strategies were investigated to find the most efficient technique to test cardiovascular devices using a patient-specific approach. This study focused on a novel stent-graft for percutaneous pulmonary valve implantation, which was virtually implanted in a realistic anatomical model.
Prior to modelling the stent in a patient-specific morphology, investigation of different FE characteristics and experimental validation of material properties provided a robust basis on which more clinically relevant simulations could be confidently performed.
The comparative analyses of patient-specific models led to the following findings. Running times were greatly different between solid and beam models, the first being more than 100 times computationally more expensive than the second. Shell elements, chosen for implantation site (i.e., RVOT) modelling, further reduced the running time by 25% in beam models, while, within solid models, differences were negligible (≤3%). Despite such a considerable difference in simulation time, the displacements of the stent rings differed on average only less than 5% between solid and beam meshes. In terms of strain distribution, the difference between meshing strategies was more evident with strain mean varying between 3.6 and 4.4%. Peak strains were higher in the beam models compared to their solid counterparts throughout the simulated pressure cycle. This result was consistent with the considerations gathered from the rod bending test, a simpler scenario which was compared with its analytical solution. Despite this difference, the alternate strain varied only between 0.24 (SoSo) and 0.27 (BeSh).
While solid elements would traditionally be the method of choice for modelling a device like the stent here described, it has been shown that using beam elements can also confidently simulate its deployment, positioning and displacement. Consequently, considering the substantial difference in simulation time between solid and beam mesh, the result of a “beam simulation” can quickly and reliably support the clinician in assessing the feasibility of this kind of intervention. The rapid nature of these simulations can eventually lead to efficiently test the same device in a wide patient population and/or promptly testing a range of devices for the same patient, ultimately resulting in tailoring the treatment for each patient.36 Moreover, it has been shown that information on device anchoring and the roundness of its central portion can be readily quantified from virtual stent modelling, in the form of diameter measurements, eccentricity values, and comparative analyses of stresses distributed on the implantation site. These clinical considerations have been expanded in a separate study from our group.4
From the engineering perspective, including more realistic boundary conditions in the analyses can help the designer to address issues related to long term mechanical behaviour of devices subjected to multi-axial loading conditions due to the interaction with cardiac structures and great vessels in a series of worse case scenarios. Our results also highlighted and reinforced the impact of the implantation site morphology (idealised vs. patient-specific) in evaluating mechanical behaviour overtime, hence device durability. Excessive simplification of the implantation site morphology can result in over-estimation of the stent long-term performance; therefore, selection of appropriate implantation site geometries becomes an important parameter for defining testing protocols to characterise device fatigue-life. Results suggest that solid elements would remain the modelling method of choice for engineering applications by providing accurate strain mapping and refined local information on the stent struts.
This study presents novelties in simulating the device itself. The stent-graft was modelled as self-expandable, including the fabric as a structural element connecting the rings. In addition, virtual implantation mimicked the actual procedure by positioning the device according to clinical indications, retrieving a membrane sheath and finally anchoring the stent-graft from its distal sections, as observed in clinical practice.29 Realistic virtual deployment affects the final configuration of both the device and the implantation site.
The major limitation of this study is the inclusion of only a single patient. However, the aim was to fully explore meshing strategies rather than simulating a cohort of patients, whose number would not have influenced methodological observations. Also, this patient appeared to be a suitable case study to emphasise the clinical application of virtual stent modelling, as not only it provided a realistic anatomy, but it was also a case specifically referred for treatment with the same device discussed in this paper.
Another limitation is the lack of representation of specific material properties for the patient’s implantation site. Therefore, this study performed comparative analyses of the results against a material (i.e., TangoPlus) which was characterized experimentally. Despite this compound was shown to behave within a physiological distensibility range,5 future studies will aim to include mechanical characteristics of specific vascular structures.
From a modelling perspective, inclusion of the valve leaflets in the central portion of the stent for a more realistic simulation of the hemodynamics would imply a fluid–structure interaction approach, which was not implemented in this study. However, the valve does not play a major structural role in the stent-graft analysis we have discussed and therefore it was neglected in this study.
Conclusion
Importantly, this study demonstrated that beam elements are a convenient choice toward a practical and reliable clinical application of FE modelling of percutaneous devices for valve implantation, as they were validated, patient-specific and computationally inexpensive. Potentially, this may lead to optimal and tailored device selection in real-time, or within a clinically acceptable time frame. On the other hand, not surprisingly, solid elements appeared to be a preferable option for engineering and manufacturing applications of this technique, despite requiring longer computational times, as they can provide detailed mechanical characterisation, while incorporating anatomical information.
References
Auricchio, F., and R. L. Taylor. Shape-memory alloys: modelling and numerical simulations of the finite-strain superelastic behaviour. Comput. Method. Appl. Mech. 143(1–2):175–194, 1997.
Babuska, I., and J. T. Oden. Verification and validation in computational engineering and science: basic concepts. Comput. Method. Appl. Methods 193:4057–4066, 2004.
Biglino, G., S. Schievano, V. Muthurangu, and A. M. Taylor. Cardiovascular modelling. In: Clinical Cardiac MRI-II, edited by J. Bogaart, S. Dymarowski, V. Muthurangu, and A. M. Taylor. Berlin: Springer-Verlag, 2012, pp. 669–694.
Biglino, G., C. Capelli, A. Binazzi, R. Reggiani, D. Cosentino, F. Migliavacca, P. Bonhoeffer, A. M. Taylor, and S. Schievano. Virtual and real bench testing: case study of a new percutaneous valve device. Eurointervention 8:120–128, 2012.
Biglino, G., P. Verschueren, R. Zegels, A. M. Taylor, and S. Schievano. Quantification of TangoPlus FullCure® 930 compliance for printing patient-specific vascular models. ASAIO J. 57:74, 2011.
Bonhoeffer, P. Are animal experiments the crux for decision making in whether new heart valves can be brought to clinical practice? EuroIntervention. 5:643–645, 2010.
Bonhoeffer, P., Y. Boudjemline, Z. Saliba, J. Merckx, Y. Aggoun, D. Bonnet, P. Acar, J. Le Bidois, D. Sidi, and J. Kachaner. Percutaneous replacement of pulmonary valve in a right-ventricle to pulmonary-artery prosthetic conduit with valve dysfunction. Lancet 356:1403–1405, 2000.
Bonhoeffer, P., R. Huynh, M. House, N. Douk, M. Kopcak, A. Hill, and N. Rafiee. Transcatheter pulmonic valve replacement in sheep using a grafted self-expanding stent with tissue valve. Circulation 118:S812, 2008.
Capelli, C., A. M. Taylor, F. Migliavacca, P. Bonhoeffer, and S. Schievano. Patient-specific reconstructed anatomies and computer simulations are fundamental for selecting medical device treatment: application to a new percutaneous pulmonary valve. Philos. Transact. A Math. Phys. Eng. Sci. 368:3027–3038, 2010.
Castelain, V., P. Hervé, Y. Lecarpentier, P. Duroux, G. Simonneau, and D. Chemla. Pulmonary artery pulse pressure and wave reflection in chronic pulmonary thromboembolism and primary pulmonary hypertension. J. Am. Coll. Cardiol. 37(4):1085–1092, 2001.
Cebral, J. R., M. A. Castro, J. E. Burgess, R. S. Pergolizzi, M. J. Sheridan, and C. M. Putman. Characterization of cerebral aneurysms for assessing risk of rupture by using patient-specific computational hemodynamics models. Am. J. Neuroradiol. 26(10):2550–2559, 2005.
Cebral, J. R., P. J. Yim, R. Löhner, O. Soto, and P. L. Choyke. Blood flow modeling in carotid arteries with computational fluid dynamics and MR imaging. Acad. Radiol. 9(11):1286–1299, 2002.
Condado, J. A., and M. Vélez-Gimón. Catheter-based approach to mitral regurgitation. J. Interv. Cardiol. 16(6):523–534, 2003.
Cribier, A., H. Eltchaninoff, A. Bash, N. Borenstein, C. Tron, F. Bauer, G. Derumeaux, F. Anselme, F. Laborde, and M. B. Leon. Percutaneous transcatheter implantation of an aortic valve prosthesis for calcific aortic stenosis—first human case description. Circulation 106:3006–3008, 2002.
EN ISO 5840-03. Cardiovascular implants. Cardiac valve prostheses. Part 3: Heart valve substitutes implanted by minimally invasive techniques, 2010.
Gan, C. T. J., J. W. Lankhaar, N. Westerhof, J. T. Marcus, A. Becker, J. W. R. Twisk, A. Boonstra, P. E. Postmus, and A. Vonk-Noordergaaf. Noninvasively assessed pulmonary artery stiffness predicts mortality in pulmonary arterial hypertension. Chest. 132:1906–1912, 2007.
Grujicic, M., B. Pandurangan, A. Arakere, and J. S. Snipes. Fatigue-life computational analysis for the self-expanding endovascular nitinol stents. J. Mater. Eng. Perform. 21(1):1–13, 2012.
Guidance for industry and FDA staff. Non-clinical engineering tests and recommended labeling for intravascular stents and associated delivery systems. Document issued on April 18, 2010.
Hall, G. J., and E. P. Kasper. Comparison of element technologies for modeling stent expansion. J. Biomech. Eng-T. ASME. 128:751–756, 2006.
Koo, B. K., A. Erglis, J. H. Doh, D. V. Daniels, S. Jegere, H. S. Kim, A. Dunning, T. Defrance, A. Lansky, J. Leipsic, and J. K. Min. Diagnosis of ischemia-causing coronary stenoses by noninvasive fractional flow reserve computed from coronary computed tomographic angiograms results from the prospective multicenter discover-flow (diagnosis of ischemia-causing stenoses obtained via noninvasive fractional flow reserve) study. J. Am. Coll. Cardiol. 58(19):1989–1997, 2011.
Lauten, A., M. Ferrari, K. Hekmat, R. Pfeifer, G. Dannberg, A. Ragoschke-Schumm, and H. R. Figulla. Heterotopic transcatheter tricuspid valve implantation: first-in-man application of a novel approach to tricuspid regurgitation. Eur. Heart. J. 32(10):1207–1213, 2011.
Migwi, C. M., M. I. Darby, G. H. Wostenholm, B. Yates, R. Duffy, and M. Moss. A method of determining the shear modulus and Poisson’s ratio of polymer materials. J. Mater. Sci. 29:3430–3432, 1994.
Morlacchi, S., C. Chiastra, D. Gastaldi, G. Pennati, G. Dubini, and F. Migliavacca. Sequential structural and fluid dynamic numerical simulations of a stented bifurcated coronary artery. J. Biomech. Eng. 133(12):121010, 2011.
Morlacchi, S., B. Keller, P. Arcangeli, M. Balzan, F. Migliavacca, G. Dubini, J. Gunn, N. Arnold, A. Narracott, D. Evans, and P. Lawford. Hemodynamics and in-stent restenosis: micro-CT images, histology, and computer simulations. Ann. Biomed. Eng. 39(10):2615–2626, 2011.
Oberkampf, W. L., T. G. Trucano, and C. Hirsch. Verification validation and predictive capability in computational engineering and physics. Appl. Mech. Rev. 57:345–384, 2004.
Pelton, A. R., V. Schroeder, M. R. Mitchell, X. Y. Gong, M. Barney, and S. W. Robertson. Fatigue and durability of nitinol stents. J Mech. Behav. Biomed. Mater. 1(2):153–164, 2008.
Rebelo, N., X. Y. Gong, A. Hall, A. R. Pelton, and W. Duerig. Finite element analysis on the cyclic properties of superelastic nitinol. Proceedings of the International Conference on Shape Memory and Superelastic Technologies, pp. 157–163, 2006.
Schievano, S., F. Migliavacca, L. Coats, S. Khambadkone, M. Carminati, N. Wilson, J. E. Deanfield, P. Bonhoeffer, and A. M. Taylor. Percutaneous pulmonary valve implantation based on rapid prototyping of right ventricular outflow tract and pulmonary trunk from MR data. Radiology 242:490–497, 2007.
Schievano, S., A. M. Taylor, C. Capelli, L. Coats, F. Walker, P. Lurz, J. Nordmeyer, S. Wright, S. Khambadkone, V. Tsang, M. Carminati, and P. Bonhoeffer. First-in-man implantation of a novel percutaneous valve: A new approach to medical device development. Eurointervention. 5:745–750, 2010.
Schievano, S., A. M. Taylor, C. Capelli, P. Lurz, J. Nordmeyer, F. Migliavacca, and P. Bonhoeffer. Patient specific finite element analysis results in more accurate prediction of stent fractures: application to percutaneous pulmonary valve implantation. J. Biomech. 43(4):687–693, 2010.
Schoenhagen, P., A. Hill, T. Kelley, Z. Popovic, and S. S. Halliburton. In vivo imaging and computational analysis of the aortic root. Application in clinical research and design of transcatheter aortic valve systems. J. Cardiovasc. Transl. Res. 4(4):459–469, 2011.
Simulia Abaqus analysis user’s manual, v. 6.10-EF Dassault Systèmes, Vélizy-Villacoublay, France, vol. V:31.4 (2010).
Smith, N., A. de Vecchi, M. McCormick, D. Nordsletten, O. Camara, A. F. Frangi, H. Delingette, M. Sermesant, J. Relan, N. Ayache, N. W. Krueger, W. H. W. Schulze, R. Hose, I. Valverde, P. Beerbaum, C. Staicu, M. Siebes, J. Spaan, P. Hunter, J. Weese, H. Lehmann, D. Chapelle, and R. Rezavi. EuHeart: personalized and integrated cardiac care using patient-specific cardiovascular modelling. Interface Focus. 1:349–364, 2011.
Steinman, D., and C. A. Taylor. Flow imaging and computing: large artery hemodynamics. Ann. Biomed. Eng. 33(12):1704–1709, 2005.
Taylor, C. A., and C. A. Figueroa. Patient-specific modelling of cardiovascular mechanics. Annu. Rev. Biomed. Eng. 11:109–134, 2009.
Viceconti, M., G. Clapworthy, and S. Van Sint Jan. The virtual physiological human—a European initiative for in silico human modelling. J. Physiol. Sci. 58(7):441–446, 2008.
Acknowledgments
We gratefully acknowledge the support of the following funding bodies: Rosetrees Trust, Fondation Leducq, British Heart Foundation, Royal Academy of Engineering/EPSRC and the UK National Institute of Health Research. We also thank the scientists from Medtronic Cardiovascular for their technical support.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Joel D. Stitzel oversaw the review of this article.
Claudio Capelli and Giovanni Biglino contributed equally to this publication.
Rights and permissions
About this article
Cite this article
Capelli, C., Biglino, G., Petrini, L. et al. Finite Element Strategies to Satisfy Clinical and Engineering Requirements in the Field of Percutaneous Valves. Ann Biomed Eng 40, 2663–2673 (2012). https://doi.org/10.1007/s10439-012-0617-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-012-0617-1