Abstract
Bone marrow is a viscous tissue that resides in the confines of bones and houses the vitally important pluripotent stem cells. Due to its confinement by bones, the marrow has a unique mechanical environment which has been shown to be affected from external factors, such as physiological activity and disuse. The mechanical environment of bone marrow can be defined by determining hydrostatic pressure, fluid flow induced shear stress, and viscosity. The hydrostatic pressure values of bone marrow reported in the literature vary in the range of 10.7–120 mmHg for mammals, which is generally accepted to be around one fourth of the systemic blood pressure. Viscosity values of bone marrow have been reported to be between 37.5 and 400 cP for mammals, which is dependent on the marrow composition and temperature. Marrow’s mechanical and compositional properties have been implicated to be changing during common bone diseases, aging or disuse. In vitro experiments have demonstrated that the resident mesenchymal stem and progenitor cells in adult marrow are responsive to hydrostatic pressure, fluid shear or to local compositional factors such as medium viscosity. Therefore, the changes in the mechanical and compositional microenvironment of marrow may affect the fate of resident stem cells in vivo as well, which in turn may alter the homeostasis of bone. The aim of this review is to highlight the marrow tissue within the context of its mechanical environment during normal physiology and underline perturbations during disease.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
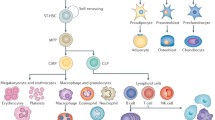
Bone marrow is the soft tissue residing in the cavities of the bones housing the essential pluripotent precursor cells for the living organism. It is the major source of hematopoietic stem cells (HSCs) which have the role of renewing the elements (monocytes, macrophages, neutrophils, eosinophils, erythroblasts, erythrocytes, megakaryocytes, platelets) in the blood.12 Adult bone marrow also contains the mesenchymal stem cells which contribute to the regeneration of tissues such as bone, cartilage, muscle, adipose, tendon, ligament and stroma by differentiating into osteoblasts, chondrocytes, myocytes, adipocytes, tenocytes and neuronal cells in vivo and in vitro.6,18,57,76–78,87 Mesenchymal stem cells have been proven to be responsive to mechanical signals such as hydrostatic pressure,2,27,86,87 fluid flow induced shear stress51 and the rheological properties (viscosity) of their environment.21,89,93
Bones are primarily responsible for countering physiological loads. The close proximity of marrow within medullary cavities of bones subject the marrow to physiological loads as well.53,79,80,97,116 The key variables of the mechanical environment of marrow due to the external factors can be listed as the intramedullary pressure and the fluid flow generated by pressure gradients. These variables change during regular physical activities.23,79,97,123 Intramedullary pressure elevations are reported in response to drugs and steroids.3,55,59,90,96 Composition and rheological properties of marrow are also reported to change during aging and drug use.39,59 Studies also suggest these properties of marrow to change during aging, osteoporosis or disuse.39,90,91 Since these anomalies have the common hallmark of bone loss, the possibility arises that the mechanical environment of marrow may be a key player in homeostasis of bone by way of the mechanically responsive resident stem cells.110
Structure and Function of Bone Marrow
In adults, marrow tissue located in the mid-diaphyseal portions of peripheral bones in the body mostly consists of adipose tissue which imparts a yellowish color (fatty marrow).104 In the axial skeleton however, the adipose tissue coexist with the hematopoietic tissue in a variable but roughly equal proportion. Bones provide a confined environment for marrow. Therefore, changes in the volume of active marrow (where hematopoiesis occurs) should be compensated by the expansion of a space-occupying component.30 This component is commonly accepted to be the adipose tissue. When the marrow hematopoietic activity increases, adipose tissue undergoes resorption to provide more space, or vice versa.
Hematopoietic tissue imparts a reddish color to marrow (red marrow) due to the high content of heme chromogen.104 Red marrow houses the red blood cells, platelets and white blood cells and resides in the flat bones such as skull, ribs, vertebrae, the proximal halves and the endosteal surfaces of the long bones. Red marrow tissue is rich in a variety of cellular components comprised mostly of hematopoietic cells. The hematopoietic cells give rise to monocytes, macrophages, neutrophils, eosinophils, erythroblasts, erythrocytes, megakaryocytes, platelets, and osteoclasts.12,15,78,109,117 Marrow’s other cellular component is a highly organized stroma that supports the proliferation of the hematopoietic cells.117 The organized stroma is composed of reticular cells which form a spongy framework on which hematopoietic cells are arranged. Upon maturation, hematopoietic cells migrate into the blood stream. Therefore, hematopoietic cells are temporary residents of marrow. Conversely, the stroma remains as a scaffold for the differentiation and maturation of the hematopoietic cells.104 Bone marrow also contains mesenchymal stem cells which have been shown to differentiate into osteoblasts, chondrocytes, myocytes, adipocytes and neuronal cells in vivo and in vitro.6,18,57,76–78,87
The organization of the marrow can be best understood by following its vascular layout. In a tubular bone, the nutrient artery enters the marrow cavity, runs longitudinally in the center, then branches out toward the endosteum of the surrounding bone, leading to specialized vascular structures known as sinuses or sinusoids (Fig. 1).7,109 Several of these sinuses may then combine to form collecting sinuses which lead to the central sinus or vein. This vein runs longitudinally next to the nutrient artery. Blood in marrow flows from the center toward the bone and then returns back to the center.104,109 This structural configuration yields high numbers of vessels and sinuses in the periphery (resulting in a slower flow rate of blood and higher surface area) where most of the exchange occurs. Therefore, hematopoiesis is maximal in the closer proximities to the bone surface leaving the central parts with relatively little hematopoietic activity (Fig. 1).103 Due to this fact, it is possible to observe a transition region between red marrow and fatty marrow radially (red marrow being closer to the endosteal surfaces, Fig. 1).104 Similarly, a longitudinal macroscopic distribution is observed as red marrow in the proximal half and fatty marrow in the distal half of the bones.104 Bone and marrow are connected by vasculature. Bone nutrient vessels enter the marrow cavity to make connections with marrow vessels. Small arteries of marrow also enter the bone, make a loop and return back to where they originated from.104,109 A more detailed description of the structural organization and function of marrow can be found elsewhere.104,109
(a) Layout of bone marrow in a cross-sectional view of a tubular bone. Bone (B) is surrounding the bone marrow (BM). Central artery (CA) and central vein (CV) are running parallel to each other and longitudinally along the long bone (perpendicular to the plane of the page). The central artery and central vein branch toward the periphery to form arterioles (A) and sinusoids (S) which then combine and join with the central vein. Hematopoietic space (H) is interspersed by the sinuses. Developing red blood cells and granulocytic cells appear in the hematopoietic space. Megakaryocytes develop subjacent to the endothelium of marrow sinuses. It is possible to observe the radial distribution of marrow as the yellow marrow in the central regions and the red marrow in the periphery (Adapted from Tavassoli and Yoffey104 and reprinted with permission of John Wiley & Sons, Inc.). (b) A toluidine-blue stained section taken transversely to the longer axis of a tubular bone. The micrograph displays the endosteal junction between bone and marrow (125×). The distribution of abundant number of red blood cells indicates that the bone marrow is hematopoietic (Courtesy of David C. Van Sickle, Purdue University)
The Mechanical Environment of Bone Marrow
Hydrostatic Pressure
One of the first studies on the bone medullary pressure reported extensive necrosis of the bone after intramedullary infusion of high pressure saline solution.49 Numerous subsequent studies tried to elucidate the possible relationship between the medullary pressure and the hemodynamics of the bone (Table 1). The systemic blood pressure in animals has been reported to be in the range of 110–140 mmHg, whereas the normal intramedullary pressure (IMP) was generally about 30 mmHg which is approximately one fourth of the systemic blood pressure (Table 1). This generalization is known as the one-forth rule.90,91
It was observed that intramedullary blood flow is directly related to the IMP and was suggested that the IMP is the resultant of the total blood flow entering the bone and the total blood flow leaving it.25,90 In addition, marrow pressure depends on the relative degree of resistance to flow between arteries and marrow blood vessels, and between marrow blood vessels and veins. Moreover, IMP and blood-pressure has variations with the phases of respiration such that IMP increases with inspiration and decreases with respiration.97 Tondevold et al.108 investigated the changes in IMP in relation to mean arterial pressure. Interestingly, they observed that the medullary pressure remained essentially constant and independent of the mean arterial pressure as long as the latter remained above 81 mmHg. Therefore, it was suggested that there has to be a regulatory system trying to keep the medullary pressure constant, which may be the arterioles of the bone marrow that are supplied by sympathetic nerve fibers with a vasoconstrictor function.24 Shim et al.92 observed the relationship between IMP and hemodynamics of bone by focusing on the blood supplies of bone. This approach was in contrast to previous studies, which focused on systemic blood circulation. Experiments carried out by Shim et al. indicated that IMP rises if the arterial blood supply to the bone increases or venous congestion occurs in the limb (Table 2). It was further demonstrated that increased marrow cavity pressure due to venous congestion decreases the blood supply to the bone.92 It was also suggested that the elevation of the IMP due to muscle contraction, which mimics physiological activity, may have significance in the maintenance of structural integrity of the bone. Although some researchers claimed to be able to define a relationship between the IMP and the blood circulation in bones, there is neither an agreement nor a consistency in the findings as it can be seen in Table 1. Nevertheless, a common finding in these studies is that the IMP has a pulsatile regime synchronous with the arterial blood pressure and respiration.
There was a significant variation in the intramedullary pressure measurements reported by various authors in the literature (Table 1). This could be due to the differences in the marrow tissue of different species.3 Another explanation to these variations was that the blood channels in the bone marrow were damaged by the insertion of the cannula and it was quite possible that there was a blood pool forming at the tip of the cannula. Therefore, sizes of the damaged channels, the amount of the damage in blood channels and in the extravascular tissue could be causing the variation.3 Similar concerns related to variations in pressure measurements due to lesions formed at the tip of the cannula were raised by various researchers.56,92 In order to eliminate the negative effects of hemorrhage or lesions forming, a tonometric pressure transducer was employed which was positioned on the intact endosteal membrane through a cortical hole of about 7.3 mm in diameter.121 Although the enhancing characteristics of the measurement technique were not discussed in detail, less variation was observed in the IMP measurements (Table 1). However, the difficulties in the surgical techniques used in this study caused puncture of the endosteal membrane and gross trauma in half of the animals. Due to the advances in sensing electronics and telemetry, it has been recently possible to conduct in vivo IMP pressure measurements on unanesthetized ambulatory mice by implantation of a radiotelemetry pressure transducer.97,98 The transducer was composed of a 0.4 mm diameter catheter, which was inserted through a 0.5 mm hole in the femoral cortex and sealed with tissue cement. The catheter was connected to a transmitter, which was secured in the peritoneal cavity, onto the abdominal wall. The new technique was successfully employed for long term, in vivo measurements of IMP in venous ligation and hindlimb suspension mice models (Tables 1 and 2). This new technique has proved to be more efficient in yielding in vivo pressure measurements with more accurate readings.
The response of the mechanical environment of the bone medullary cavity to various factors has revealed that the marrow environment is quite susceptible to external factors. In addition, this response has been shown to be quite robust in its recovery towards its normal state after its dynamics were disturbed. The studies in this regard aimed to elucidate the hemodynamic changes in bone marrow due to external effects such as occlusion of regional vessels, injection of epinephrine, norepinephrine, acetylcholine, pressor and depressor drugs, and skeletal muscle contraction (Table 2).
It is commonly anticipated that physiological loading (i.e. walking or running) perturbs the IMP.53,79,80,97,116 This supposition was tested by externally stimulating skeletal muscles of anesthetized animals to mimic the physiological loading conditions. The results (Table 2) showed that IMP rises due to muscle contraction. In a more recent in vivo study, the effect of hindlimb suspension and venous ligation on the medullary pressure was successfully measured by telemetry in ambulatory mice.97 In this study, surgical venous ligation increased the IMP by 25%. In addition, IMP decreased by 23% in normal mice and decreased by 33% in ligated mice upon hindlimb suspension (Table 2). In general, arterial occlusion yielded a decrease while venous occlusion yielded a rise in the medullary pressure, both of which verify the direct relationship between the blood flow into the bone and the IMP (Table 2). The effects of vasodilator, vasoconstrictor drugs and steroids on marrow pressure were investigated on anesthetized animals.3,55,59,90,96 Vasodilator drugs tend to lower both the marrow and the systemic blood pressure while vasoconstrictor drugs tend to increase both of them (Table 2). Miyanishi et al.59 attempted to relate steroid-induced osteonecrosis with intraosseous pressure rise in rabbits. They observed that steroid treatment significantly increased marrow pressure, decreased bone blood flow and also caused fat cell enlargement.
Rheology
It has recently been indicated that marrow viscosity is a critical parameter modulating the shear stresses experienced by the trabecular surfaces in the vertebral bodies due to vibratory loads.19 Since the potential rheological changes in the marrow due to bone diseases and aging is likely to affect the shear stresses experienced by the progenitor cells in marrow, it is essential to quantify and characterize these parameters. Bone marrow (bovine) has been shown to present Newtonian fluid characteristics (i.e. constant viscosity which is independent of shear rate) at near body temperatures.10 It should be noted that marrow has a slightly lower temperature (1.6–4.8 °C below) than normal body temperature in humans.73 Bryant et al.10 observed the dependence of bovine bone marrow’s rheological properties on temperature and anatomical location. The measured viscosity of the proximal marrow at 35 °C (≈400 cP, viscosity of water is 1 cP) was found to be about ten times that of the distal samples (≈40 cP) which can be associated with compositional variations of marrow along the bones (Table 3).20 Noting that the proximal ends of bones contain red marrow, whereas the distal ends contain yellow (fatty) marrow104; it is reasonable to infer that the increased fat content in marrow may reduce its viscosity. Interestingly, removal of cell debris, blood cells and other granular matter from the marrow by centrifugation decreased the dependence of its viscosity on temperature.10 Considering the durations of viscosity measurement intervals of as long as 6 h; the potential effect of coagulation of marrow samples was not discussed in this study.10 In a more recent study on the measurement of femoral bovine marrow viscosity with an implantable wireless method, a viscosity value of 123 cP was reported.31 The only study on the viscosity of human bone marrow (calcaneal marrow which was reported to be mainly yellow or fatty) reports values in the range of 37.5 cP (at 36 °C) and Newtonian fluid characteristics (i.e. viscosity is not dependent on the shear rate).17 However the authors report non-Newtonian behavior for the bone marrow specimens with red components (i.e. higher blood cell concentration).17 This finding is not surprising as it is known that human blood displays non-Newtonian characteristics.26 In addition, the density of red bone marrow (1.06 g/cm3)120 has been reported to be comparable to that of blood (1.05 g/cm3).26 It should be noted that there is limited information available in the literature on the density of fatty marrow (0.89 g/cm3)31 which is comparable to that of fat tissue (0.92 g/cm3).120 The viscosity values reported in the literature for bone marrow and blood are summarized in Table 3.
The variation of marrow composition along the bones and in the different parts of the body is still a question to be answered. This variation can be explained by the temperature dependence of marrow. Marrow composition is highly affected from variations in temperature. Huggins et al.33–35 evidenced that the fat content of bone marrow in the limb bones (femur, radius) are higher than the bones in the central parts of the body (ribs, vertebra). This was suggested to be associated with greater body temperatures in central bones. Similarly, Weiss et al. demonstrated that in summer times, the bony exoskeleton of the nine-banded armadillo (Dasypus novemcinctus) displayed a red or erythropoietic marrow; whereas in winter times, when the ambient temperature is low, the marrow was yellow or fatty.118
The rheological properties of bone marrow in different parts of the body and in osteoporotic, disused or aged bones are not known. In vivo monitoring of marrow in bone disease and disuse models can provide more realistic values due to the elimination of effects of extraction. The outcomes of future investigations in this area may prove to be valuable for researchers trying to simulate the natural environment of stem and progenitor cells in mechanically stimulated cell cultures in an effort to better understand bone loss.
While the intramedullary pressure and the rheology of marrow are relatively well investigated, the shear stress in the marrow during ambulation is largely unknown. Shear stress within the marrow as well as between the marrow and the endosteal bone may play a role in terms of modulating the biological response of marrow resident cells and the endosteal lining. The deformation and flow of marrow due to mechanical loading and associated effects on the stromal cells is an area open to investigation and it needs to be studied further.51,100
External Influences to the Mechanical Environment of Bone Marrow
Effects of Physiological Activity and Loading
When the mechanical loading on bones is removed due to extended periods of inactivity, such as bed rest or during space-flights, bone mineral density decreases.50,84,122 On the other hand, elevated amounts of loading on bones due to exercise causes increased bone mass and bone turnover.16,45,61,62,65,112 Even though there is in vivo evidence that exercise induced mechanical loading enhances bone mass, the cellular and molecular mechanisms underlying this fact are still being studied. Bone homeostasis is a balanced system of formation by osteoblasts and resorption by osteoclasts. Osteoblasts are the bone forming cells that originate from mesenchymal stem cells residing in marrow. Whereas osteoclasts are the bone resorbing cells that originate from the hematopoietic stem cells in marrow.13 Bone marrow mechanical environment is known to be affected from loading of bones with variations in intramedullary pressure, intramedullary and interstitial fluid flow.53,74,80,97,116 Since marrow is housing the precursors of osteoblasts and osteoclasts, the changes in the mechanical environment of marrow due to physiological activity and loading may play a role in bone homeostasis.
The earlier studies on the effects of loading on the mechanical environment of bone marrow tried to elucidate the strengthening characteristics of marrow as a slightly compressed liquid in the trabecular regions. It has been suggested that intertrabecular fluid (marrow) pressurized by compressive deformation of the bone may provide load bearing capabilities.9,40,41 The related ex vivo and in vivo studies proved that marrow inside the trabecular regions of femoral head provides stiffness to subchondral trabecular bone.70,71 It was also suggested that bone marrow acts as an intermediate transferring the external loads by means of pressurization to trabecular bones, which are acting as trusses in subchondral regions. Therefore, the trabeculum bears only the modest pressure difference across it as a tensile load.95
Researchers have used both in vivo and in vitro models to study the effects of physiological loading and activity on bone marrow. Kumar et al.46 loaded the fixed femurs of rats in vivo applying loads ranging from 0 to 12.25 kg for 1 min. They observed pressure values to rise about two-fold (12–14 mmHg increase) upon loading. They also studied contraction of the quadriceps muscles with electrical stimulation, resulting in a pressure increase of 60 mmHg.46 Another study loaded the tibiae of the sheep in impact in vitro with loads of 2000 N for durations of 0.015 s and observed elevations up to 300 mmHg.7 Downey et al.23 studied the effects of in vitro compressive loading in the human femoral head. The extracted human hips from cadavers were subjected to load by means of a mechanical testing device. They observed the IMP rise by 55 (±66) mmHg per 980 N of load applied over 0.1 s. The load values and the application durations were estimated to be comparable to physiologic conditions. They also presented an interesting finding about an osteoporotic bone with a much higher pressure rise of about 220 mmHg as a result of a relatively less load of 590 N. However, due to the lack of blood flow in the bone resting IMP of the bones was zero and the resemblance of these loading conditions and models to natural physiological loading conditions are disputable. These studies, regardless they are in vivo or in vitro, apply artificial external loads with assumed similarity to physiological loads. Moreover, in vitro studies lack blood circulation in the bone and in the muscle tissue, both of which may have potent effects on the pressure of bone marrow during physiological loading. An ideal study investigating the effects of physiological loading on the mechanical environment of bone marrow should employ slightly invasive or noninvasive instrumentation which at the same time facilitates continuous measurements in unanesthetized ambulatory animal models. Furthermore it should be noted that the magnitudes of the loading induced IMP is dependent on factors such as loading rate, viscosity of marrow and porosity of the surrounding bone.19,80 Therefore these factors should be taken into consideration when evaluating the relative magnitudes of loading induced IMP.
An explanation for bone loss due to lack of exercise and physical activity is decreased medullary cavity pressurization.84 It has been reported that bone loss is not equal throughout the skeleton in long-term bed rest. Bone loss is the greatest in lower extremities, where the medullary pressure is significantly decreased due to lack of activity. On the other hand, bone formation is observed in the head, where the intracranial pressure is increased due to body orientation and shift of body fluids.50 This suggestion has recently been supported by a mouse hind limb suspension model with in vivo femoral IMP measurements for extended durations.97 The study aimed to infer the interstitial fluid flow changes due to pressure gradients between the endosteum and periosteum. A decrease of 23% in the IMP was observed upon hindlimb suspension. Although the correlation between the IMP and the bone formation or bone loss was not reported, it was shown that medullary pressure is sensitive to disuse with an in vivo, unanesthetized and ambulatory animal model. Correspondingly, a strengthening treatment technique for osteoporotic long bones has recently been put forward, which elicits cortical bone formation in the femoral neck region of mice by means of knee loading in situ.124,125 It has been verified by a following study that the intramedullary pressure is altered in synchrony with the knee loading.123 It should be noted that 2/3 of the blood supply of cortical bone is provided by the endosteal surface.80,102 It has also been shown that the variations and oscillations in IMP play an important role on the loading induced fluid flow developed in the interstices of the cortical bones as well as of the trabecular bones.97,101,124 Therefore it is likely that the variations in the IMP not only affect the resident pluripotent stem cells but also serve as one of the players which are driving the fluid flow within the intersticies of cortical bone by way of generating pressure gradients between the envelopes of bone. This flow is essential to provide nutrients and to remove the metabolic byproducts of osteocytes resident in mineralized cortex.
Effects of Osteoporosis and Aging
Osteoporosis is a disease of bone in which fracture susceptibility is compromised by decreased bone mineral density. It mostly involves the hip, the wrist and the lumbar vertebrae.81 It is estimated that over 20% of women and 7% of men over the age of 50 have osteoporosis. Osteoporosis is responsible for over 1.5 million fractures in the United States annually.72 It has been evidenced that there is a significant change in marrow composition and mechanics due to osteoporosis and aging.39,90,91,115 The only study in this regard stated that the IMP in the tibial diaphysis of children with paralytic osteoporosis approximates the arterial blood pressure. Whereas the tibial IMP of the healthy children with the same age was only about one quarter of the arterial blood pressure.90,91 In addition, the adipose tissue fraction in marrow increases significantly with osteoporosis,39,115 which may be yielding to obstruction of blood circulation.59 Increased adipose fraction, thus decreased viscosity may be causing the overall shear stress in the medullary cavity to decrease in osteoporosis. Potential elevations in pressure or decrease in shear stress in osteoporotic bones may contribute to osteoporosis by way of altering the milieu of the bone marrow progenitor, precursor and stem cells.
Osteoblasts and adipocyte cells both originate from the mesenchymal stem cells.76 It has been suggested that the commitment of stem cell fate is integral with mechanical cues experienced in developmental and adult contexts, embodied in cell shape, cytoskeletal tension and RhoA signaling.54 RhoA is a small GTPase protein known to regulate the actin cytoskeleton in the formation of stress fibers. It has been shown that human mesenchymal stem cells subjected to different mechanical environments differentiate into either osteoblasts or adipocytes depending on the RhoA activity (RhoA active: osteogenesis, RhoA negative: adipogenesis).54 Likewise, adipocyte tissue volume in bone marrow has been shown to increase with aging and in patients with osteoporosis.39,115 Therefore, it can be hypothesized that osteoporosis may be due to a greater portion of mesenchymal stem cells differentiating into adipocytes than osteoblasts due to the changes in the cell properties and/or the mechanical environment of the marrow.
Effects of the Mechanical Environment on Stem and Progenitor Cells
It should be noted that the responses of the marrow derived progenitor cells to physical factors such as hydrostatic pressure, fluid shear and the rheology of the environment have been extensively studied in vitro. The question about the natural physiological and altered mechanical conditions of these cells in the bone marrow remains to be answered. Therefore, the review focuses on the effects of mechanical loading to stem and progenitor cells in vitro to illustrate that stem cells are responsive to mechanical cues. However, it remains to be determined as to whether this mechanical responsiveness exists in vivo.
It is commonly accepted that stem cells’ microenvironment, which includes biochemical and biomechanical factors, has an important role on their differentiation and phenotypic expression. Even though most studies in the literature place an emphasis on growth factors and cytokines, it has been evidenced that the differentiation of precursor, progenitor and stem cells are also significantly influenced by mechanical factors.27 The main mechanical signals that are accepted to be effective on marrow precursor cell proliferation and function are: hydrostatic pressure and fluid-flow induced shear.27,93 The viscosity of marrow is also important since it directly relates to the fluid shear stress magnitudes experienced by the cells. The influences of these factors are considered to be significant in regulating the stem cell phenotype and may have synergistic and/or supplemental effects in combination with the biochemical factors. The employment of such mechanical effects in specially designed “bioreactors” may enhance current standard biochemical signaling pathways for promoting engineered tissue growth.27,42,88
Marrow-derived mesenchymal stem and/or progenitor cells offer novel treatment techniques in tissue engineering research. They are already cultured ex vivo in mechanically active environments for various purposes, such as tissue engineering of bone and cartilage.6,15,47,69,77,93,94,99,114 The main goal of moving from conventional 2-D methods to 3-D mechanically active systems is to attain more physiological (or natural) culture environments for the cells. Although these studies prove improvements over conventional culturing techniques, they are far from in vivo conditions in efficiency.
Hydrostatic Pressure
There are two main reasons why hydrostatic pressure is considered as an important stimulating factor for bone marrow progenitor and stem cells. First of all, marrow derived mesenchymal progenitor cells can express chondrogenic phenotypes under appropriate hydrostatic pressure conditions. There are numerous in vitro studies subjecting marrow-derived mesenchymal stem cells to high hydrostatic pressures (750–75,000 mmHg) in an effort to induce chondrogenic phenotype.1,2,57,58,68,87 Even though the chondrogenic differentiation of the progenitor cells does not take place in marrow cavity, those studies are related in indicating the sensitivity of the progenitors to the magnitude and the mode (cyclic, intermittent or static) of loading. In general, higher pressure (∼75,000 mmHg) over lower (∼750 mmHg) and intermittent loading over static have proved to be more effective in chondrogenesis.57,58 Second, hydrostatic pressures in the medullary cavities of long bones due to physiological loading (50–200 mmHg rise)8,23,46,84,110 have osteogenic effects.86 It has been shown that constant hydrostatic pressure applied in-vitro at physiologic levels (30–60 mmHg) decreases osteoclast formation.85 Similarly, cyclic pressures of 75–300 mmHg in magnitude decreases formation of osteoclasts from their progenitors and decreases bone resorptive activity by osteoclasts in vitro.63 Furthermore, this loading scheme enhances osteoblast functions pertinent to new bone formation by stimulating both synthesis and deposition of collagen accompanied by increased accumulation of calcium-containing crystals.63,64 A general conclusion that can be drawn from those in vitro studies is that the osteogenic response of the cells are not always linearly proportional to the value of the mechanical signals, rather there is an optimal amplitude interval for each loading pattern and frequency. Limited number of in-vivo studies in this regard report similar results. Oscillatory hydrostatic pressure (60 mmHg, 20 Hz) applied in-vivo for 10 min per day for 4 weeks to avian ulnae elicited new bone formation on the periosteal surface79 possibly due to increased intracortical fluid flow as suggested by the authors. It was also suggested that since the applied loading regime has bone forming effects; it should be similar to the physiological loading conditions. Similarly, intramedullary hypertension due to venous occlusion (pressure increased to about 28.7 mmHg from 15.5 mmHg) has periosteal (138%), endocortical (369%) and cancellous (889%) bone forming effects at the caprine tibial metaphysis.119 One of the suggestions on how the marrow pressure affects bone formation is that the progenitors in the marrow may be directly reacting to marrow pressure or extracellular fluid flow (developed by pressure gradients) by differentiating into osteoblasts and forming new bone.51,110 On the other hand, it is suggested that nitric oxide is imperative in signaling of mechanically induced bone formation.28,75,113 Nitric oxide is a signaling molecule and it is synthesized by nitric oxide synthase which is produced by osteoprogenitor cells in bone marrow, by osteocytes in bone and bone lining cells.29 Therefore, it is probable that the production of this signaling molecule by the osteoprogenitor cells in the marrow is mediated by bone marrow pressure or pressure gradients.110
Fluid Shear
Mechanical loading and bending of bones cause strain gradients as well as local pressure gradients in the bone and in the medullary cavity that can drive the interstitial fluid flow53,74,80,116 and can result in shear stresses on the endosteal surface. Fluid flow induced fluid shear on bone marrow derived cells has been investigated extensively to assess its effects on cell differentiation, proliferation and function.6,15,51,63,94 Besides, it has been evidenced by a number of researchers that interstitial fluid flow may play an important role in bone remodeling, formation and adaptation.11,37,53,67,79,111 The mechanisms of flow-induced remodeling have been studied in vitro by subjecting osteoblasts,22,37,43,48 osteocytes37,44 and osteoclasts53,85 to fluid shear. The studies on osteoblasts and osteocytes showed that several osseoactive agents are stimulated by fluid flow such as nitric oxide,38,75 prostaglandins E2 and I2,43,52,66,67,82 cyclic adenosine monophosphate,82 intracellular free calcium,14,22,36,37,64,86 inositol triphosphate,36,82,83 and transforming growth factor β.27,43,57,58 On the other hand, osteoblast-mediated mineralization is preceded by osteoclast-mediated resorption with osteoclast resorption rates being about 20 times higher than osteoblast deposition rates.106 Therefore, osteoclast function may dominate the dynamic osteoclast-osteoblast balance that regulates bone turnover and degradation. Moreover, it is suggested that physiological load induced fluid flow in cortical bone is radially outward from endosteal surface to the periosteal surface,60,80 which makes it difficult for osteoblast or osteocyte secreted mediators to diffuse against the current and reach the osteoclasts or osteoclast progenitors in the marrow cavity.53 The osteoprogenitor cells are reported to be residing in bone marrow, one to three cell layers away from the endosteal surface.105 Accordingly, it has been suggested that osteoclasts and their precursors, which are located in the close vicinity of endosteal surface, may be fluid flow induced shear sensitive and that osteoclast remodeling activities may be under the control of autocrine factors.53 Bone marrow derived osteoclast-like cells are mechanosensitive to fluid flow induced shear and secrete autocrine factors, such as nitric oxide, prostaglandins E2 and I2, which can regulate local resorptive activity.53 Therefore, fluid flow induced shear developing on the endosteal surface in the medullary cavity may be the significant stimulant for osteoprogenitors in the marrow that recruits them to bone formation sites. Human marrow stromal cells subjected to oscillatory fluid flow of 1 Hz are shown to have increased proliferation rates,51 which means more osteoprogenitor cells to participate bone formation process. Similarly, the sensitivity of the cells in fluidic environment to flow frequency has been studied to find the potent optimal frequency values for cell phenotype determination.4 However, the flow mode that is naturally experienced by osteoprogenitors in marrow has not been revealed yet.
Rheology
Viscosity of the environment in which cells reside is important since it directly affects the shear stresses experienced by cells if the medium is flowing. The studies in this field investigate the viscosity of the environment in mechanically active cell cultures or perfusion bioreactors.21,89,93 In one such study, the effect of medium viscosity on marrow stromal osteoblastic cells seeded on 3D fiber meshes was studied by adding dextran (a complex, branched polysaccharide) to flowing medium in a perfusion bioreactor.93 Increasing medium viscosity with constant flow rates resulted in 2- to 3-fold increases in the shear stresses experienced by the cultured cells without changing chemotransport characteristics significantly. It was reported that increased medium viscosity not only enhances mineralized matrix deposition but also provided a better matrix distribution in the porosity of the 3D scaffolds. In a similar study, the effect of fluid flow induced shear and chemotransport on bone cells was studied in oscillatory flow.21 The medium viscosity was varied to obtain different shear stress values on the cultured cells under constant flow rates. It was shown that fluid flow induced chemotransport and shear stress acting on the cells play a synergistic role to elicit cell response to oscillatory fluid flow induced shear stress. In an effort to control the cell aggregate sizes in neural stem cell cultures, researchers tried to alter the kinematic viscosity of culture medium by adding dextran and carboxymethylcellulose.89 The results indicate that viscosity is an important parameter to consider for scale-up of stem cell bioreactors. The viscosity values of the media employed in these studies were in the range of 1–4 cP, whereas the reported viscosity values for bovine marrow was in the range of 44–400 cP.10 Therefore there is a need to revisit these studies and assess stem cell response at these higher viscosity media.
Conclusion
Bone marrow mechanical environment is susceptible to external effects such as physiological activity and disuse. Moreover, there is a potential relation between the bone diseases such as osteoporosis, and aging or disuse-related bone loss and the marrow composition and mechanics. The changes in the bone marrow mechanical environment is likely to be effective on the occupant precursor and progenitor cells, which are accepted to be responsive to mechanical factors such as hydrostatic pressure, fluid shear and the viscosity of their environment. Although the effects of these mechanical factors and viscosity on mesenchymal stem and progenitor cells are being widely investigated in vitro, the naturally occurring and altered cues in the cells’ natural environment (bone marrow) have not been well characterized yet.
Bone marrow mechanical environment can be completely defined by quantifying and characterizing the hydrostatic pressure, fluid flow induced shear and viscosity in natural and altered conditions. The results of these studies can be compiled to generate physiologically relevant in vitro mechanical environments for cell cultures, stem cell bioreactors and computational models to better understand the effects of mechanical signals on stem, progenitor and precursor cells; and potentially the nature of associated bone diseases.
References
Angele P., D. Schumann, M. Angele, B. Kinner, C. Englert, R. Hente, B. Fuchtmeier, M. Nerlich, C. Neumann, R. Kujat, 2004 Cyclic, mechanical compression enhances chondrogenesis of mesenchymal progenitor cells in tissue engineering scaffolds. Biorheology, 41(3–4):335–346
Angele P., J. U. Yoo, C. Smith, J. Mansour, K. J. Jepsen, M. Nerlich, B. Johnstone 2003 Cyclic hydrostatic pressure enhances the chondrogenic phenotype of human mesenchymal progenitor cells differentiated in vitro. Journal of Orthopaedic Research, 21(3):451–457. 10.1016/S0736-0266(02)00230-9
Azuma, H., Intraosseous Pressure as Measure of Hemodynamic Changes in Bone Marrow. Angiology, 1964. 15(9): p. 396-&. doi:10.1177/000331976401500903
Balcells, M., M. F. Suarez, M. Vazquez, E. R. Edelman 2005 Cells in fluidic environments are sensitive to flow frequency. Journal of Cellular Physiology, 204(1):329–335. 10.1002/jcp.20281
Bauer, M. S., T. L. Walker 1988 Intramedullary pressure in canine long bones. American Journal of Veterinary Research, 49(3):425–427
Braccini A., D. Wendt, C. Jaquiery, M. Jakob, M. Heberer, L. Kenins, A. Wodnar-Filipowicz, R. Quarto, I. Martin, 2005 Three-dimensional perfusion culture of human bone marrow cells and generation of osteoinductive grafts. Stem Cells, 23(8):1066–1072. 10.1634/stemcells.2005-0002
Branemark P. I., 1959 Vital microscopy of bone marrow in rabbit. Scand J Clin Lab Invest, 11(Suppl 38):1–82. 10.3109/00365515909060400
Bryant, J. D., The Effect of Impact on the Marrow Pressure of Long Bones Invitro. Journal of Biomechanics, 1983. 16(8): p. 659-&. doi:10.1016/0021-9290(83)90117-3
Bryant J. D., 1995 On Hydraulic Strengthening of Bones. Journal of Biomechanics, 28(3):353–354. 10.1016/0021-9290(95)90563-L
Bryant J. D., T. David, P. H. Gaskell, S. King, G. Lond, 1989 Rheology of bovine bone marrow. Proc Inst Mech Eng [H], 203(2):71–5. 10.1243/PIME_PROC_1989_203_013_01
Burr D. B., A. G. Robling, C. H. Turner, 2002 Effects of biomechanical stress on bones in animals. Bone, 30(5):781–786. 10.1016/S8756-3282(02)00707-X
Cabrita G. J. M., B. S. Ferreira, C. L. da Silva, R. Goncalves, G. Almeida-Porada, J. M. S. Cabral, 2003 Hematopoietic stem cells: from the bone to the bioreactor. Trends in Biotechnology, 21(5):233–240. 10.1016/S0167-7799(03)00076-3
Canalis E., 2005 The fate of circulating osteoblasts. New England Journal of Medicine, 352(19):2014–2016. 10.1056/NEJMe058080
Chen N. X., K. D. Ryder, F. M. Pavalko, C. H. Turner, D. B. Burr, J. Y. Qiu, R. L. Duncan, 2000 Ca2+ regulates fluid shear-induced cytoskeletal reorganization and gene expression in osteoblasts. American Journal of Physiology-Cell Physiology, 278(5):C989-C997
Chen X., H. Xu, C. Wan, M. McCaigue, G. Li, 2006 Bioreactor expansion of human adult bone marrow-derived mesenchymal stem cells. Stem Cells, 24(9):2052–2059. 10.1634/stemcells.2005-0591
Courteix D., E. Lespessailles, S. L. Peres, P. Obert, P. Germain, C. L. Benhamou, 1998 Effect of physical training on bone mineral density in prepubertal girls: A comparative study between impact-loading and non-impact-loading sports. Osteoporosis International, 8(2):152–158. 10.1007/BF02672512
Davis, L. B., and S. S. Praveen. Nonlinear versus linear behavior of calcaneal bone marrow at different shear rates. In: American Society of Biomechanics Annual Meeting, Blacksburg, VA, 2006. Available from: http://www.asbweb.org/conferences/2006/pdfs/304.pdf.
Dennis J. E., A. I. Caplan, 2003 Bone Marrow Mesenchymal Stem Cells. In S. Sell (Eds) Stem Cells Handbook. Humana Press Inc.: Totowa, NJ. p 107–118
Dickerson, D. A., E. A. Sander, and E. A. Nauman. Modeling the mechanical consequences of vibratory loading in the vertebral body: microscale effects. Biomech. Model. Mechanobiol., 2007.
Dietz A. A., 1946 Composition of Normal Bone Marrow in Rabbits. Journal of Biological Chemistry, 165(2):505–511
Donahue T. L. H., T. R. Haut, C. E. Yellowley, H. J. Donahue, C. R. Jacobs, 2003 Mechanosensitivity of bone cells to oscillating fluid flow induced shear stress may be modulated by chemotransport. Journal of Biomechanics, 36(9):1363–1371. 10.1016/S0021-9290(03)00118-0
Donahue S. W., C. R. Jacobs, H. J. Donahue, 2001 Flow-induced calcium oscillations in rat osteoblasts are age, loading frequency, and shear stress dependent. American Journal of Physiology-Cell Physiology, 281(5):C1635–C1641
Downey D. J., P. A. Simkin, R. Taggart, 1988 The Effect of Compressive Loading on Intraosseous Pressure in the Femoral-Head Invitro. Journal of Bone and Joint Surgery-American Volume, 70A(6):871–877
Drinker C. K., K. R. Drinker, 1916 A Method for Maintaining an Artificial Circulation through the Tibia of the Dog, With a Demonstration of the Vasomotor Control of the Marrow Vessels. American Journal of Physiology, 40:514–521
Drinker C. K., K. R. Drinker, C. C. Lund, 1922 The circulation in the mammalian bone-marrow - With especial reference to the factors concerned in the movement of red blood cells from the bone marrow into the circulating blood as disclosed by perfusion of the tibia of the dog and by injections of the bone-marrow in the rabbit and cat. American Journal of Physiology, 62(1):1–92
Eguchi Y., T. Karino, 2008 Measurement of rheologic property of blood by a falling-ball blood viscometer. Annals of Biomedical Engineering, 36(4):545–553. 10.1007/s10439-008-9454-7
Estes B. T., J. M. Gimble, F. Guilak, 2004 Mechanical signals as regulators of stem cell fate. Stem Cells in Development and Disease, 60:91–126. 10.1016/S0070-2153(04)60004-4
Fox S. W., T. J. Chambers, J. W. M. Chow, 1996 Nitric oxide is an early mediator of the increase in bone formation by mechanical stimulation. American Journal of Physiology-Endocrinology and Metabolism, 33(6):E955–E960
Fox S. W., J. W. M. Chow, 1998 Nitric oxide synthase expression in bone cells. Bone, 23(1):1–6. 10.1016/S8756-3282(98)00070-2
Gimble J. M., C. E. Robinson, X. Wu, K. A. Kelly, 1996 The function of adipocytes in the bone marrow stroma: An update. Bone, 19(5):421–428. 10.1016/S8756-3282(96)00258-X
Gurkan, U. A., and O. Akkus. An implantable magnetoelastic sensor system for wireless physiological sensing of viscosity. In: Proceeding of the ASME Summer Bioengineering Conference - 2007. New York: Amer. Soc. Mechanical Engineers, 2007, pp. 759–760
Harrelson, J. M., and B. A. Hills. Changes in bone marrow pressure in response to hyperbaric exposure. Aerospace Med. 41(9):1018–1021, 1970.
Huggins C., B. H. Blocksom, 1936 Changes in outlying bone marrow accompanying a local increase of temperature within physiological limits. Journal of Experimental Medicine, 64(2):253–U4. 10.1084/jem.64.2.253
Huggins C., B. H. Blocksom, W. J. Noonan, 1936 Temperature conditions in the bone marrow of rabbit, pigeon and albino rat. American Journal of Physiology, 115(2):395–401
Huggins C., W. J. Noonan, 1936 An increase in reticulo-endothelial cells in outlying bone marrow consequent upon a local increase in temperature. Journal of Experimental Medicine, 64(2):275-U7. 10.1084/jem.64.2.275
Hung C. T., S. R. Pollack, T. M. Reilly, C. T. Brighton, 1995 Real-Time Calcium Response of Cultured Bone-Cells to Fluid-Flow. Clinical Orthopaedics and Related Research, 313:256–269
Jacobs C. R., C. E. Yellowley, B. R. Davis, Z. Zhou, J. M. Cimbala, H. J. Donahue, 1998 Differential effect of steady versus oscillating flow on bone cells. Journal of Biomechanics, 31(11):969–976. 10.1016/S0021-9290(98)00114-6
Johnson D. L., T. N. McAllister, J. A. Frangos, 1996 Fluid flow stimulates rapid and continuous release of nitric oxide in osteoblasts. American Journal of Physiology-Endocrinology and Metabolism, 34(1):E205–E208
Justesen J., K. Stenderup, E. N. Ebbesen, L. Mosekilde, T. Steiniche, M. Kassem, 2001 Adipocyte tissue volume in bone marrow is increased with aging and in patients with osteoporosis. Biogerontology, 2(3):165–171. 10.1023/A:1011513223894
Kafka V., 1983 On Hydraulic Strengthening of Bones. Biorheology, 20(6):789–793
Kafka V., 1993 On Hydraulic Strengthening of Bones. Journal of Biomechanics, 26(6):761–762. 10.1016/0021-9290(93)90038-G
Khademhosseini A., R. Langer, J. Borenstein, J. P. Vacanti, 2006 Microscale technologies for tissue engineering and biology. Proc Natl Acad Sci U S A, 103(8):2480–7. 10.1073/pnas.0507681102
KleinNulend J., C. M. Semeins, E. H. Burger, 1996 Prostaglandin mediated modulation of transforming growth factor-beta metabolism in primary mouse osteoblastic cells in vitro. Journal of Cellular Physiology, 168(1):1–7. doi:10.1002/(SICI)1097-4652(199607)168:1<1::AID-JCP1>3.0.CO;2-T
Kleinnulend J., A. Vanderplas, C. M. Semeins, N. E. Ajubi, J. A. Frangos, P. J. Nijweide, E. H. Burger, 1995 Sensitivity of Osteocytes to Biomechanical Stress in-Vitro. Faseb Journal, 9(5):441–445
Krolner B., B. Toft, S. P. Nielsen, E. Tondevold, 1983 Physical Exercise as Prophylaxis against Involutional Vertebral Bone Loss - a Controlled Trial. Clinical Science, 64(5):541–546
Kumar S., P. R. Davis, B. Pickles, 1979 Bone-Marrow Pressure and Bone Strength. Acta Orthopaedica Scandinavica, 50(5):507–512
Kuo C. K., W. J. Li, R. L. Mauck, R. S. Tuan, 2006 Cartilage tissue engineering: its potential and uses. Current Opinion in Rheumatology, 18(1):64–73. 10.1097/01.bor.0000198005.88568.df
Kurokouchi K., C. R. Jacobs, H. J. Donahue, 2001 Oscillating fluid flow inhibits TNF-alpha-induced NF-kappa B activation via an I kappa B kinase pathway in osteoblast-like UMR106 cells. Journal of Biological Chemistry, 276(16):13499–13504. 10.1074/jbc.M003795200
Larsen R. M., 1938 Intramedullary pressure with particular reference to massive diaphyseal bone necrosis experimental observations. Annals of Surgery, 108:127–140. 10.1097/00000658-193807000-00009
Leblanc A. D., V. S. Schneider, H. J. Evans, D. A. Engelbretson, J. M. Krebs, 1990 Bone-Mineral Loss and Recovery after 17 Weeks of Bed Rest. Journal of Bone and Mineral Research, 5(8):843–850
Li Y. J., N. N. Batra, L. D. You, S. C. Meier, I. A. Coe, C. E. Yellowley, C. R. Jacobs, 2004 Oscillatory fluid flow affects human marrow stromal cell proliferation and differentiation. Journal of Orthopaedic Research, 22(6):1283–1289. 10.1016/j.orthres.2004.04.002
Li J. L., D. W. Liu, H. Z. Ke, R. L. Duncan, C. H. Turner, 2005 The P2X(7) nucleotide receptor mediates skeletal mechanotransduction. Journal of Biological Chemistry, 280(52):42952–42959. 10.1074/jbc.M506415200
McAllister T. N., T. Du, J. A. Frangos, 2000 Fluid shear stress stimulates prostaglandin and nitric oxide release in bone marrow-derived preosteoclast-like cells. Biochemical and Biophysical Research Communications, 270(2):643–648. 10.1006/bbrc.2000.2467
McBeath R., D. M. Pirone, C. M. Nelson, K. Bhadriraju, C. S. Chen, 2004 Cell shape, cytoskeletal tension, and RhoA regulate stem cell lineage commitment. Developmental Cell, 6(4):483–495. 10.1016/S1534-5807(04)00075-9
Michelsen, K., Pressure Relationships in Bone Marrow Vascular Bed. Acta Physiologica Scandinavica, 1967 71(1): p. 16-&
Michelsen K., 1968 Hemodynamics of the bone marrow circulation. Acta Physiol Scand, 73(3):264–80
Miyanishi K., M. C. D. Trindade, D. P. Lindsey, G. S. Beaupre, D. R. Carter, S. B. Goodman, D. J. Schurman, R. L. Smith, 2006 Effects of hydrostatic pressure and transforming growth factor-beta 3 on adult human mesenchymal stem cell chondrogenesis in vitro. Tissue Engineering, 12(6):1419–1428. 10.1089/ten.2006.12.1419
Miyanishi K., M. C. D. Trindade, D. P. Lindsey, G. S. Beaupre, D. R. Carter, S. B. Goodman, D. J. Schurman, R. L. Smith, 2006 Dose- and time-dependent effects of cyclic hydrostatic pressure on transforming growth factor-beta 3-induced chondrogenesis by adult human mesenchymal stem cells in vitro. Tissue Engineering, 12(8):2253–2262. 10.1089/ten.2006.12.2253
Miyanishi K., T. Yamamoto, T. Irisa, A. Yamashita, S. Jingushi, Y. Noguchi, Y. Iwamoto, 2002 Bone marrow fat cell enlargement and a rise in Intraosseous pressure in steroid-treated rabbits with osteonecrosis. Bone, 30(1):185–190. 10.1016/S8756-3282(01)00663-9
Montgomery R. J., B. D. Sutker, J. T. Bronk, S. R. Smith, P. J. Kelly, 1988 Interstitial Fluid-Flow in Cortical Bone. Microvascular Research, 35(3):295–307. 10.1016/0026-2862(88)90084-2
Mori T., N. Okimoto, A. Sakai, Y. Okazaki, N. Nakura, T. Notomi, T. Nakamura, 2003 Climbing exercise increases bone mass and trabecular bone turnover through transient regulation of marrow osteogenic and osteoclastogenic potentials in mice. Journal of Bone and Mineral Research, 18(11):2002–2009. 10.1359/jbmr.2003.18.11.2002
Mori T., N. Okimoto, H. Tsurukami, A. Sakai, Y. Okazaki, S. Uchida, T. Notomi, T. Nakamura, 2001 Effects of tower climbing exercise on bone mass and turnover in growing mice. Journal of Bone and Mineral Research, 16(Suppl 1):S362
Nagatomi J., B. P. Arulanandam, D. W. Metzger, A. Meunier, R. Bizios, 2002 Effects of cyclic pressure on bone marrow cell cultures. Journal of Biomechanical Engineering-Transactions of the Asme, 124(3):308–314. 10.1115/1.1468867
Nagatomi J., B. R. Arulanandam, D. W. Metzger, A. Meunier, R. Bizios, 2003 Cyclic pressure affects osteoblast functions pertinent to osteogenesis. Annals of Biomedical Engineering, 31(8):917–923. 10.1114/1.1590663
Nakura N., T. Mori, N. Okimoto, A. Sakai, T. Nakamura, 2005 The climbing exercise prevents trabecular bone loss with highly expressed mRNA of estrogen receptor alpha in bone cells after ovariectomy in mice. Journal of Bone and Mineral Research, 20(9):S73–S73
Nauman E. A., R. L. Satcher, T. M. Keaveny, B. P. Halloran, D. D. Bikle, 2000 Osteoblasts in culture respond to in vitro pulsatile fluid flow with short term increases in PGE2 and long term increases in cell proliferation. Journal of Bone and Mineral Research, 15(Suppl 1):S500
Nauman E. A., R. L. Satcher, T. M. Keaveny, B. P. Halloran, D. D. Bikle, 2001 Osteoblasts respond to pulsatile fluid flow with shortterm increases in PGE(2) but no change in mineralization. Journal of Applied Physiology, 90(5):1849–1854
Nerlich M., D. Schumann, R. Kujat, P. Angele, 2004 Mechanobiological conditioning on mesenchymal stem cells during chondrogenesis. Shock, 21:136–136
Nesic D., R. Whiteside, M. Brittberg, D. Wendt, I. Martin, P. Mainil-Varlet, 2006 Cartilage tissue engineering for degenerative joint disease. Advanced Drug Delivery Reviews, 58(2):300–322. 10.1016/j.addr.2006.01.012
Ochoa J. A., A. P. Sanders, D. A. Heck, B. M. Hillberry, 1991 Stiffening of the Femoral-Head Due to Intertrabecular Fluid and Intraosseous Pressure. Journal of Biomechanical Engineering-Transactions of the Asme, 113(3):259–262. 10.1115/1.2894882
Ochoa J. A., A. P. Sanders, T. W. Kiesler, D. A. Heck, J. P. Toombs, K. D. Brandt, B. M. Hillberry, 1997 In vivo observations of hydraulic stiffening in the canine femoral head. Journal of Biomechanical Engineering-Transactions of the Asme, 119(1):103–108. 10.1115/1.2796051
Osteoporosis - Fast Facts. 2006, National Osteoporosis Foundation, http://www.nof.org/osteoporosis/diseasefacts.htm.
Petrakis N. L., 1952 Temperature of Human Bone Marrow. Journal of Applied Physiology, 4(7):549–553
Piekarski K., M. Munro, 1977 Transport Mechanism Operating between Blood-Supply and Osteocytes in Long Bones. Nature, 269(5623):80–82. 10.1038/269080a0
Pitsillides A. A., S. C. F. Rawlinson, R. F. L. Suswillo, G. Zaman, P. I. Nijweide, L. E. Lanyon, 1995 Mechanical Strain-Induced Nitric-Oxide Production by Osteoblasts and Osteocytes. Journal of Bone and Mineral Research, 10(Suppl 1):S217
Pittenger M. F., A. M. Mackay, S. C. Beck, R. K. Jaiswal, R. Douglas, J. D. Mosca, M. A. Moorman, D. W. Simonetti, S. Craig, D. R. Marshak, 1999 Multilineage potential of adult human mesenchymal stem cells. Science, 284(5411):143–147. 10.1126/science.284.5411.143
Polak, J. M., and A. E. Bishop. Stem cells and tissue engineering: past, present, and future. Ann. NY Acad. Sci. 1068:352–366, 2006
Priller J., From Marrow to Brain. in Adult Stem Cells, K. Turksen Editor. 2004, Humana Press Inc.: Totowa, NJ. p. 215–233
Qin Y. X., T. Kaplan, A. Saldanha, C. Rubin, 2003 Fluid pressure gradients, arising from oscillations in intramedullary pressure, is correlated with the formation of bone and inhibition of intracortical porosity. Journal of Biomechanics, 36(10):1427–1437. 10.1016/S0021-9290(03)00127-1
Qin Y. X., W. Lin, C. Rubin, 2002 The pathway of bone fluid flow as defined by in vivo intramedullary pressure and streaming potential measurements. Annals of Biomedical Engineering, 30(5):693–702. 10.1114/1.1483863
Raisz L. G., 2005 Pathogenesis of osteoporosis: concepts, conflicts, and prospects. Journal of Clinical Investigation, 115(12):3318–3325. 10.1172/JCI27071
Reich K. M., J. A. Frangos, 1991 Effect of Flow on Prostaglandin-E2 and Inositol Trisphosphate Levels in Osteoblasts. American Journal of Physiology, 261(3):C428–C432
Reich K. M., T. N. Mcallister, S. Gudi, J. A. Frangos, 1997 Activation of G proteins mediates flow-induced prostaglandin E(2) production in osteoblasts. Endocrinology, 138(3):1014–1018. 10.1210/en.138.3.1014
Robling A. G., A. B. Castillo, C. H. Turner, 2006 Biomechanical and molecular regulation of bone remodeling. Annual Review of Biomedical Engineering, 8:455–498. 10.1146/annurev.bioeng.8.061505.095721
Rubin J., D. Biskobing, X. A. Fan, C. Rubin, K. McLeod, W. R. Taylor, 1997 Pressure regulates osteoclast formation and MCSF expression in marrow culture. Journal of Cellular Physiology, 170(1):81–87. 10.1002/(SICI)1097-4652(199701)170:1<81::AID-JCP9>3.0.CO;2-H
Rubin J., C. Rubin, C. R. Jacobs, 2006 Molecular pathways mediating mechanical signaling in bone. Gene, 367:1–16. 10.1016/j.gene.2005.10.028
Schumann D., R. Kujat, M. Nerlich, P. Angele, 2006 Mechanobiological conditioning of stem cells for cartilage tissue engineering. Bio-Medical Materials and Engineering, 16(4):S37–S52
Semino, C.E., 2003 Can We Build Artificial Stem Cell Compartments? J Biomed Biotechnol, 2003(3), 164–169. doi:10.1155/S1110724303208019
Sen A., M. S. Kallos, L. A. Behie, 2002 Expansion of mammalian neural stem cells in bioreactors: effect of power input and medium viscosity. Developmental Brain Research, 134(1–2):103–113. 10.1016/S0165-3806(01)00328-5
Shaw, N.E., Observations on Intramedullary Blood-Flow and Marrow-Pressure in Bone. Clinical Science, 1963. 24(3): p. 311-&
Shaw, N.E., Studies on Intramedullary Pressure + Blood Flow in Bone. American Heart Journal, 1964. 68(1): p. 134-&. doi:10.1016/0002-8703(64)90250-9
Shim, S. S., W. Y. Yu, and H. E. Hawk. Relationship between blood-flow and marrow cavity pressure of bone. Surgery Gynecology and Obstetrics with International Abstracts of Surgery 135(3):353, 1972.
Sikavitsas V. I., G. N. Bancroft, H. L. Holtorf, J. A. Jansen, A. G. Mikos, 2003 Mineralized matrix deposition by marrow stromal osteoblasts in 3D perfusion culture increases with increasing fluid shear forces. Proceedings of the National Academy of Sciences of the United States of America, 100(25):14683–14688. 10.1073/pnas.2434367100
Sikavitsas V. I., G. N. Bancroft, J. J. Lemoine, M. A. K. Liebschner, M. Dauner, A. G. Mikos, 2005 Flow perfusion enhances the calcified matrix deposition of marrow stromal cells in biodegradable nonwoven fiber mesh scaffolds. Annals of Biomedical Engineering, 33(1):63–70. 10.1007/s10439-005-8963-x
Simkin P. A., 2004 Hydraulically loaded the trabeculae may serve as springs within normal femoral head. Arthritis and Rheumatism, 50(10):3068–3075. 10.1002/art.20563
Stein A. H., H. C. Morgan, R. F. Porras, 1958 The Effect of Pressor and Depressor Drugs on Intramedullary Bone-Marrow Pressure. Journal of Bone and Joint Surgery-American Volume, 40(5):1103–1110
Stevens H. Y., D. R. Meays, J. A. Frangos, 2006 Pressure gradients and transport in the murine femur upon hindlimb suspension. Bone, 39(3):565–572. 10.1016/j.bone.2006.03.007
Stevens H. Y., D. R. Meays, J. Yeh, L. M. Bjursten, J. A. Frangos, 2006 COX-2 is necessary for venous ligation-mediated bone adaptation in mice. Bone, 38(1):93–104. 10.1016/j.bone.2005.07.006
Stoltz J. F., D. Bensoussan, V. Decot, P. Netter, A. Ciree, P. Gillet, 2006 Cell and tissue engineering and clinical applications: An overview. Bio-Medical Materials and Engineering, 16(4):S3–S18
Tate M. L. K., 2003 "Whither flows the fluid in bone?" An osteocyte's perspective. Journal of Biomechanics, 36(10):1409–1424. 10.1016/S0021-9290(03)00123-4
Tate M. L. K., U. Knothe, 2000 An ex vivo model to study transport processes and fluid flow in loaded bone. Journal of Biomechanics, 33(2):247–254. 10.1016/S0021-9290(99)00143-8
Tate M. L. K., P. Niederer, U. Knothe, 1998 In vivo tracer transport through the lacunocanalicular system of rat bone in an environment devoid of mechanical loading. Bone, 22(2):107–117. 10.1016/S8756-3282(97)00234-2
Tavassoli M., 1976 Ultrastructural development of bone marrow adipose cell. Acta Anat (Basel), 94(1):65–77
Tavassoli, M., and J. M. Yoffey. Bone Marrow, Structure and Function. New York: A.R. Liss, pp. xii, 300, 1983.
Tenenbaum H. C., Cellular Origins and Theories of Differentiation of Bone-Forming Cells, in In Bone: The Osteoblast and Osteocyte, B.K. Hall, Editor. 1992, CRC Press: Boca Raton, FL. p. 41–69
Tettelbaum S. L., M. M. Tondravi F. P. Ross, Osteoclast Biology, in Osteoporosis, S.E. Papapoulos, Editor. 1996, Academic Press: San Diego, CA. p. 61–71
Thomas, I. H., P. J. Gregg, and D.N. Walder. Intra-osseous phlebography and intra-medullary pressure in the rabbit femur. J. Bone Joint Surg. Br. 64(2):239–242, 1982
Tondevold E., J. Eriksen, E. Jansen, 1979 Observations on Long-Bone Medullary Pressure in Relation to Mean Arterial Blood-Pressure in the Anesthetized Dog. Acta Orthopaedica Scandinavica, 50(5):527–531
Travlos G. S., 2006 Normal structure, function, and histology of the bone marrow. Toxicologic Pathology, 34(5):548–565. 10.1080/01926230600939856
Turner C. H., V. Anne, R. M. V. Pidaparti, 1997 A uniform strain criterion for trabecular bone adaptation: Do continuum-level strain gradients drive adaptation? Journal of Biomechanics, 30(6):555–563. 10.1016/S0021-9290(97)84505-8
Turner C. H., M. R. Forwood, M. W. Otter, 1994 Mechanotransduction in Bone - Do Bone-Cells Act as Sensors of Fluid-Flow. Faseb Journal, 8(11):875–878
Turner C. H., A. G. Robling, 2005 Mechanisms by which exercise improves bone strength. Journal of Bone and Mineral Metabolism, 23:16–22
Turner C. H., Y. Takano, I. Owan, G. A. C. Murrell, 1996 Nitric oxide inhibitor L-NAME suppresses mechanically induced bone formation in rats. American Journal of Physiology-Endocrinology and Metabolism, 33(4):E634–E639
Van den Dolder J., G. N. Bancroft, V. I. Sikavitsas, P. H. M. Spauwen, J. A. Jansen, A. G. Mikos, 2003 Flow perfusion culture of marrow stromal osteoblasts in titanium fiber mesh. Journal of Biomedical Materials Research Part A, 64A(2):235–241. 10.1002/jbm.a.10365
Verma S., J. H. Rajaratnam, J. Denton, J. A. Hoyland, R. J. Byers, 2002 Adipocytic proportion of bone marrow is inversely related to bone formation in osteoporosis. J Clin Pathol, 55(9):693–8. 10.1136/jcp.55.9.693
Weinbaum S., S. C. Cowin, Y. Zeng, 1994 A Model for the Excitation of Osteocytes by Mechanical Loading-Induced Bone Fluid Shear Stresses. Journal of Biomechanics, 27(3):339–360. 10.1016/0021-9290(94)90010-8
Weiss L., 1976 Hematopoietic Microenvironment of Bone-Marrow - Ultrastructural-Study of Stroma in Rats. Anatomical Record, 186(2):161–184. 10.1002/ar.1091860204
Weiss, L. P., G. B. Wislocki, 1956 Seasonal Variations in Hematopoiesis in the Dermal Bones of the 9-Banded Armadillo. Anatomical Record, 126(2): p. 143-&. doi:10.1002/ar.1091260203
Welch R. D., C. E. Johnston, M. J. Waldron, B. Poteet, 1993 Bone Changes Associated with Intraosseous Hypertension in the Caprine Tibia. Journal of Bone and Joint Surgery-American Volume, 75A(1):53–60
White D. R., H. Q. Woodard, S. M. Hammond, 1987 Average Soft-Tissue and Bone Models for Use in Radiation-Dosimetry. British Journal of Radiology, 60(717):907–913
Wilkes C. H., M. B. Visscher, 1975 Some Physiological Aspects of Bone-Marrow Pressure. Journal of Bone and Joint Surgery-American Volume, A 57(1):49–57
Zerwekh J. E., L. A. Ruml, F. Gottschalk, C. Y. C. Pak, 1998 The effects of twelve weeks of bed rest on bone histology, biochemical markers of bone turnover, and calcium homeostasis in eleven normal subjects. Journal of Bone and Mineral Research, 13(10):1594–1601. 10.1359/jbmr.1998.13.10.1594
Zhang P., M. Su, Y. L. Liu, A. Hsu, H. Yokota, 2007 Knee loading dynamically alters intramedullary pressure in mouse femora. Bone, 40(2):538–543. 10.1016/j.bone.2006.09.018
Zhang, P., M. Su, S. M. Tanaka, and H. Yokota. Knee loading stimulates cortical bone formation in murine femurs. BMC Musculoskelet. Disord. 7, 2006.
Zhang P., S. M. Tanaka, H. Jiang, M. Su, H. Yokota, 2005 Loading frequency-dependent enhancement of bone formation in mouse tibia with knee-loading modality. Journal of Bone and Mineral Research, 20(9):S134–S135
Acknowledgments
We would like to acknowledge Dr. David C. Van Sickle for inspiring discussions and providing the histological figure of bone marrow; Sharon Evander and Carol Bain for their help in preparing the histological figure for publication.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gurkan, U.A., Akkus, O. The Mechanical Environment of Bone Marrow: A Review. Ann Biomed Eng 36, 1978–1991 (2008). https://doi.org/10.1007/s10439-008-9577-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-008-9577-x