Abstract
Objective
Electrochemical skin conductance (ESC) is a non-invasive test of sweat function developed as a potential marker of small fiber neuropathy. Here we systematically review the evolution of this device and the data obtained from studies of ESC across different diseases.
Methods
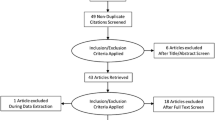
Electronic databases, including MEDLINE, and Google Scholar were searched through to February 2018. The search strategy included the following terms: “electrochemical skin conductance,” “EZSCAN,” and “Sudoscan.” The data values provided by each paper were extracted, where available, and input into tabular and figure data for direct comparison.
Results
Thirty-seven studies were included this systematic review. ESC did not change by age or gender, and there was significant variability in ESC values between diseases, some of which exceeded control values. Longitudinal studies of disease demonstrated changes in ESC that were not biologically plausible. Of the 37 studies assessed, 25 received support from the device manufacturer. The extracted data did not agree with other published normative values. Prior studies do not support claims that ESC is a measure of small fiber sensory function or autonomic function.
Conclusions
Although many papers report significant differences in ESC values between disease and control subjects, the compiled data assessed in this review raises questions about the technique. Many of the published results violate biologic plausibility. A single funding source with a vested interest in the study outcomes has supported most of the studies. Normative values are inconsistent across publications, and large combined data sets do not support a high sensitivity and specificity. Finally, there is insufficient evidence supporting the claim that Sudoscan tests sudomotor or sensory nerve fiber function.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The goal of a sensitive, specific, rapid, reproducible, non-invasive test for the evaluation of small fiber neuropathy is not quite the search for the Holy Grail, but has certainly dashed the hopes of many inventors against the rocks of reality. However, significant inroads into the study of small fiber structure have been made through the use of skin biopsies for evaluation of intra-epidermal and autonomic nerve fibers. Despite these advances, skin biopsies remain invasive, expensive, and slow because of the need for complex immunostaining.
More recently, confocal corneal microscopy has been developed as a surrogate marker of neuropathy in patients with disease. Despite the initial enthusiasm for this non-invasive approach to study unmyelinated nerve fibers, additional investigation has suggested that the receiver operator characteristic curves peak at about 0.80, despite significant differences between study populations and controls [1]. Therefore, there is only a modest correlation with disease in any particular patient, and this correlation is of limited utility in clinical practice [2, 3].
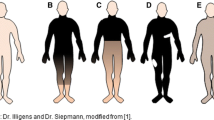
The most recent tools to investigate peripheral autonomic function is based on the use of electrochemical skin conductance (ESC) [4,5,6,7,8]. In theory, ESC electrically stimulates sudomotor nerve fibers that in turn activate sweat glands; this activation can be used as a method to study peripheral sudomotor nerve function. ESC uses an incremental low direct voltage current (a stepwise increase from 1.2 to 3.8 V) that is applied to the palms of the hands and soles of the feet for 15 s. The anode and cathode are placed on the feet or hands (left/right) for one stepwise test, and then switched and the test repeated. The electrical stimulation creates a flow of chloride ions, which then alters the flow of the electrical current through the stratum corneum. The ESC result is expressed in microsiemens (µS) [4, 5, 7, 9]. Many studies have reported that Sudoscan (Impeto Medical, Paris, France), a medical device that measures ESC, is effective at detecting disease-related abnormalities across a number of disease states [10,11,12,13,14,15,16,17,18].
A recent publication on this topic provides a systematic review of ESC [7]. The purpose of the present study, and how it differs from the previously published systematic review, is by: (1) reviewing the preliminary data supporting the use of this device, (2) providing a systematic interpretation of the published data and comparing the results to the published claims, and (3) defining the plausibility of the results as they relate to biological mechanisms.
Methods
Electronic databases, including MEDLINE, and Google Scholar were searched through to 1 February 2018. The search strategy included the following terms: “electrochemical skin conductance,” “EZSCAN,” and” “Sudoscan”. All identified articles were included for review. Review articles, meta-analyses, and non-original data were included in the review but not included in primary data extraction. All references from identified articles were screened for possible inclusion in the review if they did not appear in the primary search. All data were extracted from published work by two independent researchers (SR, MC). Extracted data (where available) included study period, methods, disease state, subject characteristics, comorbid illness, risk factors, medication use, neurological examinations, neurophysiologic testing, laboratory studies, and sources of funding. The data values provided by each paper for each disease state were extracted, where available, and input into tabular and figure data for direct comparison between studies. Raw data are presented as the mean and standard deviation, with control data also expressed by age. Disease data are represented in total and by disease state (studies that included more than one disease state have data reported separately for each disease). Specifically, no modification, normalization, or exclusion of outliers was performed in this review to aid in understanding the biological underpinning of the test result.
All publications were scrutinized for veracity of pre-existing reference data by two independent researchers. Claims of prior (referenced) studies were reviewed to determine if: (1) such data existed in the original study, (2) the results supported the claim of the referring study, and (3) if sufficient detail was provided in the study methods and results to interpret the data. If the two researchers did not agree, a third investigator was used to arbitrate a final decision.
Data analytic techniques for each paper were reviewed to determine if the appropriate analyses were performed to support the claims made in the discussion.
Results
A total of 37 studies were included in this data review [4,5,6, 10,11,12,13,14,15,16,17, 19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44]. Several additional articles of interest did not meet inclusion criteria for original research but were included in "Discussion" section of the paper because of their relevance to the topic. Original research studies spanned a number of disease states (including type 1 diabetes [T1DM], type 2 diabetes [T2DM], pre-diabetes or metabolic syndrome, rheumatoid arthritis, ankylosing spondylitis, small fiber neuropathy, distal symmetric polyneuropathy, Fabry’s disease, amyloidosis, cystic fibrosis [CF], and chronic kidney disease). Many studies included either lean or obese control subjects for comparison.
Reproducibility
In healthy control subjects and disease states (CF and diabetes) the coefficient of variations between left and right sides calculated on 1365 subjects was 3% for the hands and 2% for the feet. There was no observed gender effect. Reproducibility was 7% in the hands and 5% in the feet in healthy subjects on same-day testing [8]. The coefficient of variation in patients with cardiovascular risk was 15% in the hands and 7% in the feet. The coefficient of variation in subjects with diabetes was 32% (hands/feet not specified) [8], but neither detailed subject information nor study results were available in any form; thus information from this study was not included in our final analysis.
Review of funding sources
Of the 37 reviewed studies, 25 were funded in part by Impeto Medical, had data analyzed by Impeto Medical, had control data provided by Impeto Medical, or were authored by an Impeto Medical employee. Of the remaining studies, several did not report funding sources.
Overall data review
The raw data for each individual study and for patients and controls are is reported in Fig. 1 for both the hands and the feet. The 95% cutoff values for the population were provided based on the control samples (Fig. 1a, solid gray lines) and are included in the study of disease states (Fig. 1b, solid gray lines) as comparison. As noted in Fig. 1b and d, the vast majority of the patient populations fall within the normative range for the population. The data is compared to another recently published normative database, these results are also included in Fig. 1 as separate 5–95% confidence intervals (Fig. 1, dashed black lines) [9].
Electrochemical skin conductance (ESC) values in the hands and feet for control and disease populations. Data are presented as the mean ± standard deviation (SD) for all published studies. a, c ESC values of control subjects in the hands (a) and feet (c) by age. b, d ESC values across disease states in the hands (b) and feet (d) by age for all published studies. Solid gray lines indicate 5–95% confidence intervals for the control population calculated from subjects included in this study. Dashed black lines indicate the 5–95% confidence intervals from a prior publication [9]
Impact of age and gender
As seen in Fig. 1a, c, there is no significant effect of age on ESC values in the hands or the feet in our data review. A modest age-related decline was noted in one prior analysis of several studies [9]. No significant difference in ESC values between genders was detected in our study, which is in agreement with the lack of gender difference detected in a prior analysis of several studies [9].
Impact of race
As noted in Fig. 2, individuals of African-American heritage have a significantly lower ESC results in both the hands and the feet compared to their European American counterparts [17, 32]. African–American controls have the same ESC results in both the hands and the feet as the European–Americans with diabetic kidney disease [17, 32]. The effect of race on ESC has been described in a recent review article of sudoscan data [9]. There are also significantly different values obtained in individuals of Asian heritage, with Chinese subjects the most heavily studied [6, 9, 11, 34].
Impact of disease state
As noted in Fig. 3, the ESC was not reduced in subjects with longstanding T1DM, but it was reduced in obese control subjects, subjects with pre-diabetes, and those with T2DM. ESC values of individuals with rheumatoid arthritis and ankylosing spondylitis were similar to subjects with T2DM (ESC ~ 60 μS) [13, 22, 30]. In contrast, ESC values were increased in individuals with CF [27].
A substantially larger number of disease study subjects had ‘abnormal’ values using the previously published normative database [9] compared to the normative values calculated in the present study.
Impact of disease-modifying therapy
In one study of obese subjects who underwent bariatric surgery, there was a significant improvement in ESC scores in individuals with T2DM (ESC in the feet improved from ~ 57 to ~ 70 over 24 weeks), but not in obese non-diabetic or obese pre-diabetic individuals who underwent bariatric surgery [16]. The only difference between these three groups that underwent bariatric surgery was the change in glycated hemoglobin (HbA1c), which was the highest in those with diabetes. The ESC values in the subjects with T2DM at 24 weeks exceeded the ESC values of the non-diabetic and pre-diabetic cohorts [16]. In another series of studies that included patients with rheumatoid arthritis and ankylosing spondylitis, the authors concluded that the subjects had achieved an improvement in ‘sudomotor’ neuropathy after 5 and 12 weeks of treatment with disease-modifying therapy based on increases in ESC scores [30].
Review of references and pre-existing data claims
All studies were reviewed and the references evaluated to determine the accuracy of pre-existing data claims. In all cases, the two reviewers agreed with the result; therefore, a third reviewer was not required for arbitration. The majority of the published studies (84%; 31 of the 37 reviewed studies) refer to prior publications that do not support their claims, specifically the claims that ESC is a measure of small nerve fiber function. One study described ESC as an effective method to detect abnormalities in individuals with hyperglycemia that was due to either diabetes or impaired glucose tolerance [45]. The authors of this study hypothesized that higher than expected ESC readings could be due to “sweat gland nerves going through a phase of hypersensitivity during the IGT phase before entering the hypo sensitivity phase in DM” [45]. This hypothesis was never tested. One study published during the same time frame investigated the use of ESC for the evaluation of sudomotor function [28]. The authors of this study concluded that sweat gland dysfunction could be measured and further hypothesized that because this dysfunction was controlled by the sympathetic nervous system, ESC could be a measure of the sympathetic nervous system [28]. This hypothesis was also never tested. The authors of another publication compared ESC to vibration perception threshold in individuals with diabetes and concluded that a modest correlation was sufficient to state “Assessment of sudomotor function using Sudoscan™ may be considered as part of the screening test for DPN, and may also help to identify patients with small-fibre neuropathy indicative of potentially greater levels of foot risk” [29]. No testing of small fiber function was performed during that study [29]. All follow-up publications reference these papers (and the follow-up papers that appear), as proof that ESC measures small fiber autonomic or sensory function. No publications testing these theories were ever identified in our extensive review of the literature.
Discussion
We systematically reviewed the literature on electrochemical skin conductance for evaluation of sudomotor function. A total of 37 papers with thousands of control and disease subjects were incorporated into the summary results, with additional papers providing background or review data included as well. Our findings suggest a lack of biologic plausibility, a high risk of bias in most studies from extensive involvement of the device manufacturer, normative data that are not reflected by the identified literature, and a lack of testing of hypotheses for claims made in articles that are subsequently referenced by other authors [46].
Biologic plausibility of data
We know based on extensive pathologic investigation of the structure and innervation of glandular tissue that there is an age-related decline in both sudomotor nerve density and sudomotor function [47]. Large population-based studies show a significant increase in neuropathy prevalence with age [48, 49]. Detailed neuropathologic examinations carried out in the framework of multicenter studies reveal evidence of an age-related decline in intra-epidermal nerve fiber density [50]. Furthermore, there is also a gender-related difference in intra-epidermal fiber density [50]. It is also well established that sudomotor function declines with age while men have a significantly greater sweat output than women [51]. However, there is minimal to no age or gender effect on sudoscan ESC results [9]. There is a demonstrable effect of age on quantified neurological examinations, neuropathologic findings and neurophysiologic testing [48, 50, 52]. Similarly, gender effects have been detected both neuropathologically and neurophysiologically, specifically in sweat production and sudomotor function [48, 50,51,52]. The lack of findings on an age or gender effect on ESC has not been adequately explained.
A study of treatment of rheumatoid arthritis and ankylosing spondylitis found improved ESC values over 6 weeks during treatment [30]. However, prior studies of nerve regeneration raise questions about the likelihood of nerve recovery over as short a period as 6 weeks. Thus, despite the improvements in ESC noted by the authors over 6–12 weeks in these individuals with rheumatoid arthritis or ankylosing spondylitis [30], this time frame would appear to be too short for distal neural repair in humans based on studies of human pathophysiology. To date, no other neurophysiologic or neuropathologic testing has confirmed the improvements detected in ESC.
The majority of published studies report that ESC is a technological advance that measures sweat function through the quantitation of chronoamperometry [4,5,6, 10,11,12,13,14,15,16,17, 19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44]. The resulting data are correlated to other physiologic parameters, including nerve function, kidney function, metabolic function, disease state, and/or cardiovascular risk [4,5,6, 10,11,12,13,14,15,16,17, 19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44]. Despite the significance of the correlations (which are often in the modest range of correlation coefficients, namely, 0.4–0.7), the results are then suggested to serve as a valid marker of disease or even as a screening tool for disease.
An initial clinical study in CF reported increased ESC in those subjects with CF compared to control subjects [27]. Although the ‘delta’ ESC was much lower in the feet of CF subjects compared to controls, there was a greater overlap in the ‘delta’ ESC in the hands of CF subjects and control subjects. The difference in ESC values between subjects with CF and healthy control subjects does raise the question of whether ESC is actually a surrogate marker of sensory or autonomic nerve function [27].
Several additional violations of biological plausibility occur in published ESC studies involving patients with diabetes. First, studies in bariatric surgery suggest that individuals with T2DM can regain nerve fiber function that exceeds the control group 24 weeks post-surgery [16]. However, extensive studies of nerve fiber structure and function in individuals with T2DM do not support a theory of complete nerve fiber recovery post-gastric bypass [53], although it has been noted in pilot studies that symptoms of neuropathy can improve [54, 55]. Also, the possibility that nerve fiber function in individuals with chronic T2DM will exceed that of the control group within 24 weeks violates biologic plausibility [16]. Second, the ESC values in individuals with chronic T1DM also appear to exceed those of control subjects despite other noted abnormalities in testing [4, 10] and a substantial body of data supporting the association with diabetes duration and neuropathy progression [56, 57]. Third, the use of insulin by T2DM patients [25] has been reported to improve ESC values over a 1-year period of time compared to those not using insulin, despite the insulin-treated group having higher HbA1c values [25]. To date, there has been limited evidence of peripheral nerve re-innervation in individuals with T2DM treated with insulin, or any other agent, over long periods of time [58, 59]. Furthermore, those same individuals with diabetes that had an improvement in ESC had significantly more severe diabetic retinopathy and nephropathy, but simultaneously had normal ESC values at baseline and follow-up [25]. No adequate explanation for this discrepancy was provided by the authors of the study.
Counter-intuitively, studies of renal disease also concluded that ESC was associated with estimated glomerular filtration rate, and would decline as renal function worsened [5, 6, 17, 32]. It is difficult to comprehend how a single test of sweat function can simultaneously reveal renal disease and neuropathy, and it would raise the question of whether an abnormal result implied renal disease, neuropathy or both.
The role of the device manufacturer in study outcomes
The vast majority of all published studies are linked in some way to the manufacturer of the device. Many published studies include employees of the device manufacturer as co-authors of the paper, the manufacturer has analyzed the data, or the manufacturer provided the raw data for control subjects in the publication. Although there is no inherent problem with the involvement of a device manufacturer in studies, many of the publications do not appropriately report any conflicts of interest. Over 65% of the studies included in our review were funded by Impeto Medical, published by Impeto Medical employees, had data analyzed by Impeto Medical, and/or were of low quality [5, 10, 11, 13, 16, 17, 19,20,21,22,23,24,25, 27,28,29,30,31,32,33, 36, 37, 40, 41, 44]. The extensive list of publications supported by Impeto Medial was generally used as proof the test was measuring nerve fiber function. This risk of systematic bias introduced by a single funding source with a vested interest in the study outcomes is high.
Differences in normative values
The significant difference between the confidence values established in this study and that in a prior publication [9] are difficult to address. In our publication all studies with data on healthy subjects were included in the analysis [4,5,6, 10,11,12,13,14,15,16,17, 19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44], while in the prior study only data from three large studies [9, 28, 31, 44] were included. However, even the mean values published from the prior studies [28, 31, 44] do not seem to provide the same result reported in the combined study [9]. Nonetheless, a number of differences in study inclusion and data analysis could explain these differences. The ESC values reported across a large number of control subjects have often reported normative value cutoffs based on the specific control population studied. No standardized threshold for abnormality has been universally accepted, and it appears that the most commonly used methods may create false positive results in a large population of patients [4,5,6, 10,11,12,13,14,15,16,17, 19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44]. The different ESC values noted between individuals of European or African descent does raise important questions about the need for adequate clinical data in devices prior to clinical use. In this case, control data from African-American individuals could be falsely reported as abnormal in many healthy subjects who undergo testing [17, 32]. False positive diagnostic tests create unnecessary anxiety about disease, result in additional diagnostic testing, and place patients at risk for unnecessary procedures, exposure to harmful medications, and increased healthcare expenditure [60].
Lack of adequate testing despite claims
Despite dozens of publications across a variety of journals and specialties, there is no evidence offered that ESC is a measure of sympathetic—or small nerve fiber—function. The results of our systematic review indicate that most publications report ESC to be a measure of small fiber or autonomic function using a standard set of references and standard language that is offered by the device manufacturer. These theories on ESC are offered as evidence in many follow-up publications, but are never verified by either the scientific community or the study authors. Despite the scarcity of published evidence, ongoing reports continue to state that ESC is a sensitive and specific test of autonomic and small nerve fiber function [7, 9, 14, 15, 24]. The gradual transition of ESC initially as a test of sweat function [28], then a test of sudomotor function [19, 29], and finally a test of autonomic and small fiber function [4, 5, 18, 21,22,23, 25, 26, 31, 61] through a string of manufacturer-supported studies that did not actually investigate nerve function does raise concerns about a manipulation of language to improve marketing prospects. The gradual shift in published language surrounding Sudoscan has enabled the device to be marketed, and billed, as a test of sympathetic cholinergic function, without any evidence supporting this claim. Specific marketing to consumers with this information does suggest that the manufacturer was aware of, and supportive of, the misdirection (http://www.sudoscan.com).
Limitations
There are a number of limitations to this systematic review. It is a retrospective review of previously published data. The results for some studies were not available in table or figure format for extraction, and the results from other papers were extracted from figures, which can result in a modest miscalculation of the mean and range of the data. In some of these studies data were not reported by race at the time of publication, thereby preventing us from determining if race was a factor. It has also been suggested that ‘functional variations’ could explain some of the data, such as the increase in glomerular filtration rate seen in individuals with newly diagnosed diabetes. We agree that functional perturbations in certain types of tests can occur, although sudomotor testing typically is reported as being decreased in individuals with diabetic neuropathy [62]. There may have been variations in the technical aspects of ESC testing that are not reported in the literature, and not reported by the manufacturer, that we cannot account for. The conclusions we have drawn and reported in our paper do not agree with vast majority of published studies about the use of ESC, although we do draw similar conclusions to those reported in some of the most recent publications [10, 36].
Despite these limitations, the inclusion of data from several thousand healthy controls and disease participants in the analysis of Sudoscan as a tool for diagnosis of sudomotor dysfunction provides a powerful assessment of the level of evidence that is currently available. At this time, despite clinical and research use of ESC, there are four key problems systematically identified in the literature: (1) many of the published results violate biologic plausibility because of a failure to detect age-, gender-, and disease-appropriate changes; (2) the exact method by which the Sudoscan device calculates ESC values is not reported, thereby creating some ambiguity in interpreting the results; (3) there is a high risk of systematic bias introduced by a single funding source with a vested interest in the study outcomes; (4) there is a failure of consistency in published normative values along with substantial racial variation in ESC results; and (5) there is no evidence supporting the claim that Sudoscan tests sudomotor or sensory nerve fiber structure or function. There is significant heterogeneity to testing results across populations, and an inability to differentiate between disease and control subjects. These findings raise serious questions not only about the clinical use of this device but also about the large number of studies, many supported by the device manufacturer, that report positive results.
There are a number of methodological studies that could, and should, be performed to understand exactly what is being measured using the Sudoscan device. Detailed comparison to standard sudomotor testing, longitudinal follow-up, and mechanistic studies of neural blockade would be of great value, although ideally would have occurred prior to the clinical use of the device. At this time, the existing gaps in knowledge do not allow us to recommend the clinical use of Sudoscan [46].
References
Scarr D Lovblom LE, Lovshin JA et al (2017) Lower corneal nerve fibre length identifies diabetic neuropathy in older adults with diabetes: results from the Canadian Study of Longevity in Type 1 Diabetes. Diabetologia 60(12):2529–2531
Kass-Iliyya L, Javed S, Gosal D et al (2015) Small fiber neuropathy in Parkinson’s disease: a clinical, pathological and corneal confocal microscopy study. Parkinsonism Relat Disord 21(12):1454–1460
Scarr D, Lovblom LE, Ostrovski I et al (2017) Agreement between automated and manual quantification of corneal nerve fiber length: implications for diabetic neuropathy research. J Diabetes Complications 31(6):1066–1073
Selvarajah D, Cash T, Davies J et al (2015) SUDOSCAN: a simple, rapid, and objective method with potential for screening for diabetic peripheral neuropathy. PLoS One 10(10):e0138224
Luk AO, Fu WC, Li X et al (2015) The clinical utility of SUDOSCAN in chronic kidney disease in Chinese patients with type 2 diabetes. PLoS One 10(8):e0134981
Mao F, Liu S, Qiao X et al (2016) Sudoscan is an effective screening method for asymptomatic diabetic neuropathy in Chinese type 2 diabetes mellitus patients. J Diabetes Investig. 2016
Novak P (2017) Electrochemical skin conductance: a systematic review. Clin Auton Res. doi: https://doi.org/10.1007/s10286-017-0467-x.
Khalfallah K, Ayoub H, Calvet JH, Neveu X, Brunswick P, Griveau S, Lair V, Casir M, Bedioui F (2010) Noninvasive galvanic skin sensor for early diagnosis of sudomotor dysfunction: application to diabetes. IEEE Sens J 12(3):8
Vinik AI, Smith AG, Singleton JR et al (2016) Normative values for electrochemical skin conductances and impact of ethnicity on quantitative assessment of sudomotor function. Diabetes Technol Ther 18(6):391–398
Ang L, Jaiswal M, Callaghan B et al (2017) Sudomotor dysfunction as a measure of small fiber neuropathy in type 1 diabetes. Auton Neurosci 205:87–92
Zhu L, Zhao X, Zeng P et al (2016) Study on autonomic dysfunction and metabolic syndrome in Chinese patients. J Diabetes Invest 7(6):901–907
Chahal S, Vohra K, Syngle A (2016) Association of sudomotor function with peripheral artery disease in type 2 diabetes. Neurol Sci 38:151–156
Syngle V, Syngle A, Garg N, Krishan P, Verma I (2016) Predictors of autonomic neuropathy in rheumatoid arthritis. Auton Neurosci 201:54–59
Castro J, Miranda B, Castro I, de Carvalho M, Conceicao I (2016) The diagnostic accuracy of Sudoscan in transthyretin familial amyloid polyneuropathy. Clin Neurophysiol 127(5):2222–2227
Sahuc P, Chiche L, Dussol B, Pouget J, Franques J (2016) Sudoscan as a noninvasive tool to assess sudomotor dysfunction in patients with Fabry disease: results from a case–control study. Ther Clin Risk Manag 12:135–138
Casellini CM, Parson HK, Hodges K et al (2016) Bariatric surgery restores cardiac and sudomotor autonomic C-fiber dysfunction towards normal in obese subjects with type 2 diabetes. PLoS One 11(5):e0154211
Freedman BI, Smith SC, Bagwell BM et al (2015) Electrochemical skin conductance in diabetic kidney disease. Am J Nephrol 41(6):438–447
Névoret ML, Vinik AI (2015) CIDP variants in diabetes: measuring treatment response with a small nerve fiber test. J Diabetes Complications 29(2):313–317
Yajnik CS, Kantikar VV, Pande AJ, Deslypere JP et al (2012) Quick and simple evaluation of sudomotor function for screening of diabetic neuropathy. ISRN Endocrinol 2012:103714
Casellini CM, Parson HK, Richardson MS, Nevoret ML, Vinik AI (2013) Sudoscan, a noninvasive tool for detecting diabetic small fiber neuropathy and autonomic dysfunction. Diabetes Technol Ther 15(11):948–953
Eranki VG, Santosh R, Rajitha K et al (2013) Sudomotor function assessment as a screening tool for microvascular complications in type 2 diabetes. Diabetes Res Clin Pract 101(3):e11–e13
Syngle A, Verma I, Garg N, Krishan P et al (2013) Autonomic dysfunction in psoriatic arthritis. Clin Rheumatol 32(7):1059–1064
Yajnik CS, Kantikar V, Pande A et al (2013) Screening of cardiovascular autonomic neuropathy in patients with diabetes using non-invasive quick and simple assessment of sudomotor function. Diabetes Metab 39(2):126–131
Saad M, Psimaras D, Tafani C et al (2016) Quick, non-invasive and quantitative assessment of small fiber neuropathy in patients receiving chemotherapy. J Neurooncol 127(2):373–380
Calvet JH, Dupin J, Winiecki H, Schwarz PE (2013) Assessment of small fiber neuropathy through a quick, simple and non invasive method in a German diabetes outpatient clinic. Exp Clin Endocrinol Diabetes 121(2):80–83
Sheshah E, Madanat A, Al-Greesheh F et al (2015) Electrochemical skin conductance to detect sudomotor dysfunction, peripheral neuropathy and the risk of foot ulceration among Saudi patients with diabetes mellitus. J Diabetes Metab Disord 15:29
Hubert D, Brunswick P, Calvet JH, Dusser D, Fajac I et al (2011) Abnormal electrochemical skin conductance in cystic fibrosis. J Cyst Fibros 10(1):15–20
Mayaudon H, Miloche PO, Bauduceau B (2010) A new simple method for assessing sudomotor function: relevance in type 2 diabetes. Diabetes Metab 36(6 Pt 1):450–454
Gin H, Baudoin R, Raffaitin CH, Rigalleau V, Gonzalez C (2011) Non-invasive and quantitative assessment of sudomotor function for peripheral diabetic neuropathy evaluation. Diabetes Metab 37(6):527–532
Syngle A, Verma I, Krishan P, Garg N, Syngle V (2015) Disease-modifying anti-rheumatic drugs improve autonomic neuropathy in arthritis: DIANA study. Clin Rheumatol 34(7):1233–1241
Raisanen A, Eklund J, Calvet JH, Tuomilehto J (2014) Sudomotor function as a tool for cardiorespiratory fitness level evaluation: comparison with maximal exercise capacity. Int J Environ Res Public Health 11(6):5839–5848
Freedman BI, Bowden DW, Smith SC, Xu J, Divers J (2014) Relationships between electrochemical skin conductance and kidney disease in type 2 diabetes. J Diabetes Complications 28(1):56–60
Smith AG, Lessard M, Reyna S, Doudova M, Singleton JR (2014) The diagnostic utility of Sudoscan for distal symmetric peripheral neuropathy. J Diabetes Complications 28(4):511–516
Zeng Q, Dong SY, Wang ML et al (2016) Cardiac autonomic neuropathy risk estimated by sudomotor function and arterial stiffness in Chinese subjects. J Hum Hypertens 30(11):720–725
Lefaucheur JP, Wahab A, Plante-Bordeneuve V et al (2015) Diagnosis of small fiber neuropathy: a comparative study of five neurophysiological tests. Neurophysiol Clin 45(6):445–455
Callaghan BC, Xia R, Reynolds E et al (2018) Better diagnostic accuracy of neuropathy in obesity: a new challenge for neurologists. Clin Neurophysiol 129(3):654–662
Novak P (2016) Electrochemical skin conductance correlates with skin nerve fiber density. Front Aging Neurosci 8:199
Mao F, Liu S, Qiao X et al (2017) SUDOSCAN, an effective tool for screening chronic kidney disease in patients with type 2 diabetes. Exp Ther Med 14(2):1343–1350
Mao F, Zhu X, Lu B, Li Y (2018) Detection of relationships between SUDOSCAN with estimated glomerular filtration rate (eGFR) in Chinese patients with type 2 diabetes. Diabetes Res Clin Pract 138:113–118
Chae CS, Park GY, Choi YM et al (2017) Rapid, objective and non-invasive diagnosis of sudomotor dysfunction in patients with lower extremity dysesthesia: a cross-sectional study. Ann Rehabil Med 41(6):1028–1038
Ozaki R, Cheung KK, Wu E et al (2011) A new tool to detect kidney disease in Chinese type 2 diabetes patients: comparison of EZSCAN with standard screening methods. Diabetes Technol Ther 13(9):937–943
Jin J, Wang W, Gu T et al (2017) The application of SUDOSCAN for Screening Diabetic Peripheral Neuropathy in Chinese Population Screening DPN by SUDOSCAN. Exp Clin Endocrinol Diabetes. https://doi.org/10.1055/s-0043-116673
Wang D, Shen B, Wu C, Xue Y, Liu Y (2017) The relationship between cardiovascular autonomic dysfunction and ocular abnormality in Chinese T2DM. J Diabetes Res 2017:7125760
Hupin D, Pichot V, Celle S et al (2015) Sudomotor function and obesity-related risk factors in an elderly healthy population: the PROOF–Synapse Study. Int J Cardiol 186:247–249
Ramachandran A, Moses A, Shetty S et al (2010) A new non-invasive technology to screen for dysglycaemia including diabetes. Diabetes Res Clin Pract 88(3):302–306
ESHRE Capri Workshop (ECW) Group (2018) Protect us from poor-quality medical research. Hum Reprod 33(5):770–776
Abdel-Rahman TA, Collins KJ, Cowen T, Rustin M (1992) Immunohistochemical, morphological and functional changes in the peripheral sudomotor neuro-effector system in elderly people. J Auton Nerv Syst 37(3):187–197
Hanewinckel R, Drenthen J, van Oijen M et al (2016) Prevalence of polyneuropathy in the general middle-aged and elderly population. Neurology 87(18):1892–1898
Hanewinckel R, van Oijen M, Ikram MA, van Doorn PA (2016) The epidemiology and risk factors of chronic polyneuropathy. Eur J Epidemiol 31(1):5–20
Lauria G, Bakkers M, Schmitz C et al (2010) Intraepidermal nerve fiber density at the distal leg: a worldwide normative reference study. J Peripher Nerv Syst 15(3):202–207
Low PA, Denq JC, Opfer-Gehrking TL et al (1997) Effect of age and gender on sudomotor and cardiovagal function and blood pressure response to tilt in normal subjects. Muscle Nerve 20(12):1561–1568
Albers JW, Brown MB, Sima AA, Greene DA (1996) Nerve conduction measures in mild diabetic neuropathy in the Early Diabetes Intervention Trial: the effects of age, sex, type of diabetes, disease duration, and anthropometric factors. Neurology 46(1):85–91
Miras AD, Chuah LL, Khalil N et al (2015) Type 2 diabetes mellitus and microvascular complications 1 year after Roux-en-Y gastric bypass: a case–control study. Diabetologia 58(7):1443–1447
Muller-Stich BP, Fischer L, Kenngott HG et al (2013) Gastric bypass leads to improvement of diabetic neuropathy independent of glucose normalization—results of a prospective cohort study (DiaSurg 1 study). Ann Surg 258(5):760–765 (discussion 765-6)
Muller-Stich BP, Billeter AT, Fleming T et al (2015) Nitrosative stress but not glycemic parameters correlate with improved neuropathy in nonseverely obese diabetic patients after Roux-Y gastric bypass. Surg Obes Relat Dis 11(4):847–854
Pop-Busui R, Boulton AJ, Feldman EL et al (2017) Diabetic neuropathy: a position statement by the American Diabetes Association. Diabetes Care 40(1):136–154
Martin CL, Albers JW, Pop-Busui R (2014) Neuropathy and related findings in the diabetes control and complications trial/epidemiology of diabetes interventions and complications study. Diabetes Care 37(1):31–38
Penza P, Lombardi R, Camozzi F, Ciano C, Lauria G (2009) Painful neuropathy in subclinical hypothyroidism: clinical and neuropathological recovery after hormone replacement therapy. Neurol Sci 30(2):149–151
Singleton JR, Marcus RL, Lessard MK, Jackson JE, Smith AG (2015) Supervised exercise improves cutaneous reinnervation capacity in metabolic syndrome patients. Ann Neurol 77(1):146–153
Grimes DA, Schulz KF (2002) Uses and abuses of screening tests. Lancet 359(9309):881–884
Papanas N, Ziegler D (2014) New vistas in the diagnosis of diabetic polyneuropathy. Endocrine 47(3):690–698
Low VA, Sandroni P, Fealey RD, Low PA (2006) Detection of small-fiber neuropathy by sudomotor testing. Muscle Nerve 34(1):57–61
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Rights and permissions
About this article
Cite this article
Rajan, S., Campagnolo, M., Callaghan, B. et al. Sudomotor function testing by electrochemical skin conductance: does it really measure sudomotor function?. Clin Auton Res 29, 31–39 (2019). https://doi.org/10.1007/s10286-018-0540-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10286-018-0540-0