Abstract
Pain resulting from renal and ureteral stones is a common cause for patients presenting in the acute setting. Since the late 1990s, computed tomography (CT) has been the initial imaging method of choice to evaluate patients with suspected ureteral stones; however, concerns regarding both radiation dose and cost-effectiveness have prompted investigations into a different imaging algorithm. Studies utilizing ultrasound have provided evidence indicating that it may be a more appropriate first step, with selective use of CT in selected cases, in the diagnostic work-up. Techniques have evolved with low-dose CT, dual-energy CT, and magnetic resonance urography emerging as useful in imaging of renal colic patients. This manuscript reviews the current literature on state-of-the-art imaging for acute flank pain and proposes a new imaging algorithm in the evaluation of patients with acute flank pain and suspected ureteral stones.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Clinical background
Ureteral stones are a frequent cause for emergency room visits, which results in substantial health care costs. A staggering 1 million Americans visit the emergency department for flank pain resulting from obstructive nephrourolithiasis [1]. Approximately, half a million of these will undergo imaging with non-contrast computed tomography (CT) [2]. Estimated lifetime prevalence for kidney stone disease is approximately 7 % for women and 13 % for men [1] and appears to be continuously increasing with lifestyle changes and better diagnostic tools [2, 3].
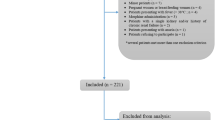
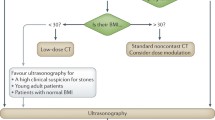
Patients presenting with severe acute onset flank pain usually undergo additional evaluation with imaging to determine the precise etiology. The optimal imaging work-up should be dependent on the clinical context and the specifics of each patient. Multiple factors play a role in the most appropriate imaging when evaluating suspected urolithiasis. A clinical scoring scheme has been developed in the emergency medicine literature, acronymed STONE [4]: sex, timing, origin (race), nausea/vomiting, and erythrocytes (urine red blood cells). This calculates a risk quotient for obstructive nephroureterolithiasis and the need for further imaging in these patients. While initial data from applying STONE criteria suggested that imaging could be deferred in lower-risk patients, recent data has questioned whether CT imaging can be avoided in the current practice setting [5]. This manuscript provides an analysis of available imaging techniques to evaluate the patients presenting with acute flank pain in the emergency department, and an imaging algorithm is proposed (Fig. 1).
Conventional imaging with non-contrast CT
CT remains the most commonly ordered modality to image suspected nephrolithiasis in the acute setting [6, 7]. This offers several advantages such as high sensitivity and diagnostic accuracy as well as the potential to evaluate for non-urinary tract causes of acute flank pain and hence, provide alternate diagnoses. Large-scale meta-analysis has suggested a sensitivity of 97 % and a specificity of 95 % for the detection of obstructive nephroureterolithiasis, even with low-dose computed tomography (CT) [8]. Up to 10 % of patients being evaluated with non-contrast CT for acute flank pain will have alternative etiologies for their symptoms [9, 10]. About half of these will have findings requiring acute detection and management [9, 10].
Alternative diagnosis
One significant advantage of performing CT in an acute setting is detecting alternative diagnosis. CT has been recommended as the standard of care in evaluation of patients with acute onset flank pain both by the American Urological Association and the Agency for Healthcare Research and Quality [6, 11]. This recommendation is based not only on the high sensitivity of CT but also its sensitivity for detection of surgical emergencies. Katz et al. demonstrated that alternative diagnoses for flank pain are encountered with non-contrast CT at a rate of about 10 % [12]. These included both genitourinary as well as non-genitourinary findings, such as adnexal masses, pyelonephritis, genitourinary obstruction at multiple locations, perinephric hemorrhage, renal cell carcinoma, colonic pathology, appendicitis, small bowel disease, cholecystitis, pancreatitis, amongst others [12]. However, due to the methodological concerns of this study, it has been claimed that the authors may have possibly overestimated the prevalence of alternative diagnosis. Moore et al. performed a similar study in patients with flank or back pain in the absence of pyuria and again demonstrated 10 % incidence of alternative diagnosis, although only about 3 % of these were truly emergent findings [9]. Recent studies have indeed demonstrated that in otherwise healthy, young patients (less than 50 years of age) without urinary tract infection or trauma, the risk of dangerous alternative diagnoses is likely quite low [13]. This is also the population most vulnerable to radiation given their young age and the possibility of repeated imaging in the future. Even with repeat visits, symptomatic relief and medical expulsive therapy was felt to be sufficient and not requiring inpatient treatment. Authors have also suggested that non-resolution of pain in the ER after supportive therapy can be used as a possible criterion to guide CT imaging [13].
Role of dual-energy CT
Dual-energy CT (DECT) functions by scanning at two separate energy levels, typically 80 and 140 kV, and then utilizes the resulting differential photoelectric absorption to calculate an attenuation ratio [14]. This technique has been shown to accurately classify in vivo stone composition as verified with crystallography [15, 16]. Patients whose renal stone may not reasonably be expected to pass spontaneously may benefit from dual-energy CT in an acute setting to guide therapy as the preferred treatment may depend on the chemical composition of the stone. Both the decision to use shockwave lithotripsy versus percutaneous neprholithotomy for active stone removal, as well as the optimization of a recurrence prevention regimen, can benefit from understanding stone composition [17].
While the role of dual-energy contrast-enhanced CT in the non-acute setting to analyze the composition of urinary tract stones has been well studied [18], authors have also recently evaluated the use of dual-energy CT in the acute setting [19, 20]. They proposed calculation of virtual non-contrast images to evaluate for stone disease, while the contrast-enhanced portion of the study will adequately evaluate alternative intra-abdominal pathology. Chen et al. demonstrated that split bolus DECT could be used to calculate virtual non-contrast images for renal stones. Using this method, they reported overall sensitivity of stone detection to be 87.5 % in virtual unenhanced images, compared to non-contrast images. Omitting the unenhanced scan as a part of this protocol reduced the mean radiation dose from 15.6 to 6.7 mSv [19, 20]. While radiation dose has been a concern with dual-energy CT, recent studies have demonstrated that a reduced radiation dosage can be achieved by lowering the tube current by as much as 38 % without compromising diagnosis [18].
Radiation dose from computed tomography
In recent years, the debate over dose issues and the public awareness of radiation exposure has become more prevalent. Despite its increased sensitivity for diagnosing urolithiasis, CT delivers ionizing radiation to the patient. A recent report from the American College of Radiology National Radiology Data Registry examined over 49,000 renal colic protocol CT examinations [21]. This large review of the Dose Index Registry found the overall mean institutional dose-length product (DLP) was 746 mGycm (effective dose, 11.2 mSv), with a range of 307–1497 mGycm (effective dose, 4.6–22.5 mSv) for mean DLPs. Only 10 % of institutions reviewed kept the DLP to 400 mGycm (effective dose, 6 mSv) or less in at least 50 % of their patients.
As federal and state regulators continue to scrutinize the use of medical radiation, practices have adapted their protocols and upgraded their CT scanners to implement reduced-dose techniques. Protocols for renal colic and suspected urolithiasis have been targeted as an area for significant dose savings [22]. In general, CT scans with an effective dose of 3 mSv or less have been considered low dose [22]. Comparative evaluation of standard versus low-dose techniques for patients with renal colic has yielded encouraging results. A study utilizing low-dose CT in patients with body mass index (BMI) <30 demonstrated a sensitivity of 95 % and a specificity of 97 % for detecting ureteral calculi, and was 86 % sensitive for detecting calculi <3 mm [23]. The modified protocol in this study applied a tube current ≤30 mAs for these non-obese patients. Despite this and multiple other publications, which have similar results for low-dose scans, reduced-dose renal protocol CT is used infrequently in the USA, and institutional variation is substantial [22].
Risks of ionizing radiation for the doses typically administered are difficult to quantify. Extrapolation of the linear no-threshold model has been used to help evaluate the biologic impact of these exposures. Radiation-associated cancer risk for effective doses in the ranges described for renal stone protocols has been estimated to be approximately one additional cancer per 1000 CT examinations over a lifetime, when averaging patient age and sex [22, 24]. It has been estimated that the risk of fatal cancer is 0.05 % (1 in 2000) for 10 mSv of ionizing radiation [24]. The risks for each individual patient can vary significantly depending on factors such as habitus, age, and frequency of repeat scans.
Patients with urinary tract stone disease are likely candidates for repeat imaging, hence raising concerns for increased risk of cancer induction. Radiation dose reduction with iterative reconstruction (IR) techniques has been evaluated by Andrabi et al. [11]. Three vendor techniques, namely, ASIR, iDOSE, and SAFIRE, were compared with conventional filtered back projection (FBP), and significantly higher subjective and objective measurements of image noise were found in FBP examinations compared with dose-modified iterative reconstruction examinations. Compared to FBP, radiation dose was lower for all the three IR techniques but within similar range to each other [11]. While aggressively dose-reduced studies performed with radiation doses in the range of 1 mSv detect stones larger than 3 mm, these scans underperform in the detection of stones smaller than this size [12].
The rationale for non-contrast CT in the acute setting is still actively debated. In addition to radiation concerns, a study performed by Westphalen et al. evaluating the National Hospital Ambulatory Medical Care Survey (NHAMCS) database reflected a tenfold increase in the incidence of CT utilization without an associated increase in incidence of nephroureterolithiasis, diagnosis of significant alternative diagnoses, or hospital admissions [25]. In the face of such information, the role of CT in actually changing patient management and the overutilization of CT in the emergent setting has been questioned. Hence, other modalities have been studied as an alternative to CT in the acute setting.
Ultrasound
Studies have evaluated the role for ultrasound for the initial assessment of acute flank pain. One recent article published in the New England Journal of Medicine [26] supports using ultrasound as an initial imaging modality for acute onset flank pain. The data comes from a multicenter comparative effectiveness trial performed by Bindman et al. evaluating point-of-care ultrasonography in the emergency department, ultrasonography performed by a radiologist, and abdominal CT. The randomized trial, composed of 2759 patients, compared each group’s cumulative radiation exposure, number of serious adverse events, return emergency department visits, hospitalizations, and diagnostic accuracy [26]. The number of serious adverse events amongst the three groups ranged 10.8–12.4 % and was not significantly different (p value = 0.50). Secondary outcomes of pain scores, hospital admissions, and emergency department readmissions also did not significantly differ among the groups. Some of the patients initially evaluated by ultrasound (40.7 % of patient’s in the point-of-care ultrasonography group and 27.0 % of the patient’s in the radiology ultrasound group) did eventually undergo additional imaging with a CT scan, and therefore, their cumulative radiation dose was not zero yet still significantly less than the CT group. This supports the idea that ultrasound should be performed as a screening study in the acute setting eliminating radiation exposure for the majority of patients, without changing patient outcomes and morbidity. However, there have been some concerns regarding the reference standard utilized by the study. The reference standard used was reported passage or surgical removal of a stone, which is an imperfect standard [27]. Additionally, the study was not designed or powered to compare sensitivity or specificity of ultrasonography versus CT [26]. Also, ultrasound may not depict the stone itself, which may lead to management issues, where in the stone size plays a major role [28].
The sensitivity for ultrasound detection of urolithiasis is operator-dependent and has been reported to range between 12 and 98 % [29–32]. The wide range may reflect varying levels of experience for sonographers and whether the studies are performed by radiologists or sonographers. Ultrasonography has limited ability to visualize stones less than 3 mm; however, it can reliably detect stones greater than 5 mm [29]. Fortunately, approximately 70 % of stones equal to or less than 5 mm are expected to pass spontaneously [33, 34]. The location of stones can affect sonographic detection. Stones in the mid ureter are more difficult to identify often due to the presence of overlying bowel gas. Larger body habitus may also limit detection of stones. A secondary finding of hydronephrosis, which can be effectively diagnosed with ultrasound, in a patient with classic signs and symptoms of renal colic, is argued to be definitive for urolithiasis [35]. Ultrasound also requires a longer time to perform compared to CT.
Ultrasonography as a first test for suspected urolithiasis generating renal colic has been widely supported in Europe. The 2015 European Association of Urology Urolithiasis Guideline Panel published guidelines recommending ultrasound be the primary diagnostic imaging tool partly due to factors of radiation and cost [36]. A proposed clinical algorithm for suspected renal colic, which begins with bedside ultrasound and stratifies patients on degree of hydronephrosis, allowed for discharge of up to 50 % of patients with no further imaging in the emergency department. After 2 months, these patients demonstrated no serious adverse effects [37]. In Europe, radiologists themselves perform ultrasounds whereas in North America, the sonographers perform ultrasounds under a radiologist’s supervision. Allowing for differences in practice patterns, the European experience should be translatable to a North American setting as well.
There is indeed a subset of patients with small renal stones that do not develop hydronephrosis. This subset may remain undiagnosed with the ultrasound only approach, and hence, ultrasound is an imperfect imaging modality in this situation [28]. However, a review of urology literature indicates that even patients with severe hydronephrosis may not suffer permanent damage to the kidneys until 2–4 weeks after initial insult and therefore, may not require further emergent imaging or inpatient management [37, 38]. This data suggest that ultrasonography is a better imaging alternative than CT in the acute setting for appropriately selected patients suspected to have urolithiasis.
Magnetic resonance imaging
While ultrasound and CT are expected to remain the mainstays for renal colic imaging, magnetic resonance imaging (MRI) may serve a role in select patients. Primarily, MRI is usually reserved for patients with non-diagnostic ultrasounds in the setting of acute flank pain, and ionizing radiation exposure needs to be significantly limited, such as for pregnant and pediatric patients (Figs. 2 and 3). However, MRI should be considered as the second-line test after the initial ultrasound (US) fails to establish a diagnosis and symptoms continue despite conservative management [39]. Physiologic hydronephrosis is seen in a majority of pregnant patients, and the ureter will display smooth tapering between the iliopsoas and uterus, typically on the right (Fig. 3) [40]. Moreover, hydronephrosis from acute obstruction may not be evident for several hours, and a non-dilated distal ureter may be difficult to visualize on ultrasound. MR imaging may be able to differentiate physiologic hydronephrosis of pregnancy from pathologic obstruction [39]. When combined with a KUB, magnetic resonance urography (MRU) using T2 fat-saturated fast spin-echo sequences has been shown to be an accurate alternative to unenhanced CT for detecting ureteral stones [41]. Additionally, MRI can detect periureteral edema often associated with urinary obstruction, not easily demonstrated on ultrasound [42].
33-year-old pregnant woman presenting with left flank pain. a Coronal T2-weighted images demonstrate bilateral hydronephrosis. No obstructing stone or lesions were identified, consistent with physiologic hydronephrosis of pregnancy. b Axial T1-weighted image demonstrates edematous pancreatic head and body with ductal dilation (arrow) suggestive of pancreatitis
MRI has a high sensitivity (94–100 %) [43] in the setting of urinary obstruction. Additionally, MRI can diagnose a wide variety of acute diseases in the abdomen with the benefit of no ionizing radiation. However, issues of access, cost, and patient tolerance continue to limit the widespread use of MRI in the acute setting.
Conclusion
Based on the current literature, the authors recommend renal ultrasound to be the preferred initial imaging study in a patient with flank pain and suspected ureteral stone, particularly in the absence of pyuria, signs of an alternative diagnosis, and trauma (Fig. 1). Ultrasound is a quick, cost-effective, and readily available modality, which is advantageous in being free of ionizing radiation. If ultrasound demonstrates hydronephrosis, then obstruction from stone disease is the most plausible diagnosis, and treatment can be initiated. Sometimes, ultrasound will demonstrate the site of obstruction and/or lack of urine flow jets in the bladder. If there is no hydronephrosis on ultrasound, consider supportive therapy and short-term non-emergent follow-up can be obtained. If US is negative or inconclusive and pain persists after conservative management, the possibility of an alternative diagnoses should be entertained, and a contrast-enhanced CT can be done. MRI should be considered after a non-contributory ultrasound in limited circumstances such as in pregnant or pediatric patients.
References
Pearle MS, Calhoun EA, Curhan GC, Urologic Diseases of America Project (2005) Urologic diseases in America project: urolithiasis. J Urol 173(3):848–857
Fwu CW, Eggers PW, Kimmel PL, Kusek JW, Kirkali Z (2013) Emergency department visits, use of imaging, and drugs for urolithiasis have increased in the United States. Kidney Int 83(3):479–486
Foster G, Stocks C, Brorofsky MS (2012) Emergency Department visits and hospital admissions for kidney stone disease, 2009: statistical brief #139. In: Healthcase Cose and Utilization Project (HCUP) Statistical Breids (Internet). Rockville (MD): Agency for Health Care Policy and Research (US); 2006 Feb-. 2009 [cited 2016 February 29th]; Available from: http://www.ncbi.nih.gov/books/NBK100827/
Moore CL, Bomann S, Daniels B et al (2014) Derivation and validation of a clinical prediction rule for uncomplicated ureteral stone—the STONE score: retrospective and prospective observational cohort studies. BMJ 348:g2191
Wang RC, Rodriguez RM, Moghadassi M et al (2016) External validation of the STONE score, a clinical prediction rule for ureteral stone: an observational multi-institutional study. Ann Emerg Med 67(4):423–432.e2
Coursey CA, Casalino DD, Remer EM et al (2012) ACR Appropriateness Criteria® acute onset flank pain—suspicion of stone disease. Ultrasound Q 28(3):227–233
Teichman JM (2004) Clinical practice. Acute renal colic from ureteral calculus. N Engl J Med 350(7):684–693
Niemann T, Kollmann T, Bongartz G (2008) Diagnostic performance of low-dose CT for the detection of urolithiasis: a meta-analysis. AJR Am J Roentgenol 191(2):396–401
Moore CL, Daniels B, Singh D, Luty S, Molinaro A (2013) Prevalence and clinical importance of alternative causes of symptoms using a renal colic computed tomography protocol in patients with flank or back pain and absence of pyuria. Acad Emerg Med Off J Soc Acad Emerg Med 20(5):470–478
Ather MH, Faizullah K, Achakzai I, Siwani R, Irani F (2009) Alternate and incidental diagnoses on noncontrast-enhanced spiral computed tomography for acute flank pain. Urol J 6(1):14–18
Fulgham PF, Assimos DG, Pearle MS, Preminger GM (2013) Clinical effectiveness protocols for imaging in the management of ureteral calculous disease: AUA technology assessment. J Urol 189(4):1203–1213
Katz DS, Scheer M, Lumerman JH, Mellinger BC, Stillman CA, Lane MJ (2000) Alternative or additional diagnoses on unenhanced helical computed tomography for suspected renal colic: experience with 1000 consecutive examinations. Urology 56(1):53–57
Schoenfeld EM, Poronsky KE, Elia TR, Budhram GR, Garb JL, Mader TJ (2015) Young patients with suspected uncomplicated renal colic are unlikely to have dangerous alternative diagnoses or need emergent intervention. West J Emerg Med 16(2):269–275
Coursey CA, Nelson RC, Boll DT et al (2010) Dual-energy multidetector CT: how does it work, what can it tell us, and when can we use it in abdominopelvic imaging? Radiographics 30(4):1037–1055
Hidas G, Eliahou R, Duvdevani M et al (2010) Determination of renal stone composition with dual-energy CT: in vivo analysis and comparison with x-ray diffraction. Radiology 257(2):394–401
Manglaviti G, Tresoldi S, Guerrer CS et al (2011) In vivo evaluation of the chemical composition of urinary stones using dual-energy CT. AJR Am J Roentgenol 197(1):W76–W83
Tiselius HG, Ackermann D, Alken P et al (2001) Guidelines on urolithiasis. Eur Urol 40(4):362–371
Wilhelm K, Schoenthaler M, Hein S et al (2015) Focused dual-energy CT maintains diagnostic and compositional accuracy for urolithiasis using ultralow-dose noncontrast CT. Urology 86(6):1097–1102
Chen CY, Hsu JS, Jaw TS et al (2015) Split-bolus portal venous phase dual-energy CT urography: protocol design, image quality, and dose reduction. AJR Am J Roentgenol 205(5):W492–W501
Chen CY, Tsai TH, Jaw TS et al (2016) Diagnostic performance of split-bolus portal venous phase dual-energy CT urography in patients with hematuria. AJR Am J Roentgenol 206(5):1013–1022
Lukasiewicz A, Bhargavan-Chatfield M, Coombs L et al (2014) Radiation dose index of renal colic protocol CT studies in the United States: a report from the American College of Radiology National Radiology Data Registry. Radiology 271(2):445–451
Hara AK, Wellnitz CV, Paden RG, Pavlicek W, Sahani DV (2013) Reducing body CT radiation dose: beyond just changing the numbers. AJR Am J Roentgenol 201(1):33–40
Poletti PA, Platon A, Rutschmann OT, Schmidlin FR, Iselin CE, Becker CD (2007) Low-dose versus standard-dose CT protocol in patients with clinically suspected renal colic. AJR Am J Roentgenol 188(4):927–933
Brenner DJ, Elliston CD (2004) Estimated radiation risks potentially associated with full-body CT screening. Radiology 232(3):735–738
Westphalen AC, Hsia RY, Maselli JH, Wang R, Gonzales R (2011) Radiological imaging of patients with suspected urinary tract stones: national trends, diagnoses, and predictors. Acad Emerg Med Off J Soc Acad Emerg Med 18(7):699–707
Smith-Bindman R, Aubin C, Bailitz J et al (2014) Ultrasonography versus computed tomography for suspected nephrolithiasis. N Engl J Med 371(12):1100–1110
Luyckx F (2015) Who wants to go further has to know the past: A comment upon: Ultrasonography versus computed tomography for suspected nephrolithiasis-R. Smith-Bindman et al. N Engl J Med. 2014 Sep 18;371(12):1100-1110. World J Urol 33(10):1371–1372
Song Y, Hernandez N, Gee MS, Noble VE, Eisner BH (2015) Can ureteral stones cause pain without causing hydronephrosis? World J Urol
Fowler KA, Locken JA, Duchesne JH, Williamson MR (2002) US for detecting renal calculi with nonenhanced CT as a reference standard. Radiology 222(1):109–113
Patlas M, Farkas A, Fisher D, Zaghal I, Hadas-Halpern I (2001) Ultrasound vs CT for the detection of ureteric stones in patients with renal colic. Br J Radiol 74(886):901–904
Ripolles T, Errando J, Agramunt M, Martinez MJ (2004) Ureteral colic: US versus CT. Abdom Imaging 29(2):263–266
Sheafor DH, Hertzberg BS, Freed KS et al (2000) Nonenhanced helical CT and US in the emergency evaluation of patients with renal colic: prospective comparison. Radiology 217(3):792–797
Coll DM, Varanelli MJ, Smith RC (2002) Relationship of spontaneous passage of ureteral calculi to stone size and location as revealed by unenhanced helical CT. AJR Am J Roentgenol 178(1):101–103
Johri N, Cooper B, Robertson W, Choong S, Rickards D, Unwin R (2010) An update and practical guide to renal stone management. Nephron Clin Pract 116(3):c159–c171
Moore CL, Scoutt L (2012) Sonography first for acute flank pain? J Ultrasound Med Off J Am Inst Ultrasound Med 31(11):1703–1711
European Association of Urology. Guidelines on urolithiasis. http://uroweb.org/guideline/urolithiasis/. Accessed 8 Sept 2016
Dalziel PJ, Noble VE (2013) Bedside ultrasound and the assessment of renal colic: a review. Emerg Med J EMJ 30(1):3–8
Manthey DE, Teichman J (2001) Nephrolithiasis. Emerg Med Clin North Am 19(3):633–654, viii
Masselli G, Weston M, Spencer J (2015) The role of imaging in the diagnosis and management of renal stone disease in pregnancy. Clin Radiol 70(12):1462–1471
Wallace GW, Davis MA, Semelka RC, Fielding JR (2012) Imaging the pregnant patient with abdominal pain. Abdom Imaging 37(5):849–860
Regan F, Kuszyk B, Bohlman ME, Jackman S (2005) Acute ureteric calculus obstruction: unenhanced spiral CT versus HASTE MR urography and abdominal radiograph. Br J Radiol 78(930):506–511
Lubarsky M, Kalb B, Sharma P, Keim SM, Martin DR (2013) MR imaging for acute nontraumatic abdominopelvic pain: rationale and practical considerations. Radiographics 33(2):313–337
Bannas P, Pickhardt PJ (2015) MR evaluation of the nontraumatic acute abdomen with CT correlation. Radiol Clin N Am 53(6):1327–1339
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Jha, P., Bentley, B., Behr, S. et al. Imaging of flank pain: readdressing state-of-the-art. Emerg Radiol 24, 81–86 (2017). https://doi.org/10.1007/s10140-016-1443-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10140-016-1443-9