Abstract
Ablative fractional lasers were introduced for treating facial rhytides. Few studies have compared fractional CO2 and Er:YAG lasers on cutaneous photodamages by a split trial. The aim of the present study was to compare these modalities in a randomized controlled double-blind split-face design with multiple sessions and larger sample size compared to previous studies done before. Forty patients with facial wrinkles were enrolled. Patients were randomly assigned to receive three monthly treatments on each side of the face, one with a fractional CO2 and one with a fractional Er:YAG laser. The evaluations included investigating clinical outcome determined by two independent dermatologists not enrolled in the treatment along with measuring skin biomechanical property of cheeks using a sensitive biometrologic device with the assessment of cutaneous resonance running time (CRRT). Moreover, possible side effects and patients’ satisfaction have been recorded at baseline, 1 month after each treatment, and 3 months after the last treatment session. Clinical assessment showed both modalities significantly reduce facial wrinkles (p value < 0.05), with no appreciable difference between two lasers. Mean CRRT values also decreased significantly after the laser treatment compared to the baseline in both laser groups. There was no serious long-standing adverse effect after both laser treatments, but the discomfort was more pronounced by the participants after CO2 laser treatment. According to the present study, both fractional CO2 and fractional Er:YAG lasers show considerable clinical improvement of facial skin wrinkles with no serious adverse effects, but post-treatment discomfort seems to be lower with Er:YAG laser.
Similar content being viewed by others

Avoid common mistakes on your manuscript.
Introduction
Skin aging is a multifactorial phenomenon. The environmental factors, primarily UV radiation, along with cutaneous structural alterations due to intrinsic aging process gradually lead to development of signs and symptoms of aging on the skin [1, 2]. Facial rejuvenation can be achieved using a variety of techniques, from simple noninvasive procedures to more invasive surgical treatments. Laser technology is widely used for cosmetic surgery [3]. Furthermore, there is controversy regarding the optimal laser treatment of rhytides. Carbon dioxide (CO2) and erbium:yttrium–aluminum–garnet (Er:YAG) laser ablation are accepted and widely used for the treatment of facial rhytides. Carbon dioxide lasers emit light at 10,600 nm in the far-infrared spectrum, while Er:YAG lasers are flash lamp-pumped crystal lasers that emit light at a wavelength of 2940 nm, which closely approximates the absorption peak of water (3000 nm). It allows for superficial skin ablation and less underlying thermal damage compared with the CO2 laser. The findings of ablative fractional photothermolysis of rhytides that have been published so far are encouraging, but they are inconsistent in detail as far as study design and the respective efficacy of different laser modalities are concerned [4].
Many authors believe that fractional Er:YAG laser equals fractional CO2 laser in efficacy and has a favorable side effect profile due to improved control of the total depth of injury and decreased underlying thermal injury [5, 6]. Those who support the considerable efficacy of Er:YAG laser contend that the depth of ablation is what determines the degree of dermal remodeling, not the depth of underlying thermal injury [7–9]. However, there is little evidence on the comparative safety and efficacy of both modalities [4]. Therefore, this study attempts to compare both methods in terms of the effect of multiple treatment sessions on wrinkle depth, side effects, tolerability, and the patient satisfaction.
Materials and methods
Study design
We performed a randomized controlled double-blind trial in a split-face design. The present study was conducted on 40 volunteers presenting to our office for desired treatment of facial skin wrinkles between November 2014 and May 2015; subjects were between 34 and 62 years of age with mild to moderate facial rhytides at rest. This study was approved by the Ethical Committee of Shahid Beheshti University of Medical Sciences and was performed according to the principles of the Declaration of Helsinki. All of the subjects signed a written informed consent after explanation of the procedure. The protocol was approved by the Iranian Registry of Clinical Trials (IRCT ID 2014122820468N1). We have no conflict of interest to declare. This study was funded by Skin Research Center, Shahid Beheshti University of Medical Sciences, Tehran, Iran.
Patients with any active skin disease within the treatment area (e.g., cancer, autoimmune disease, or active infection), pregnancy, history of isotretinoin use in the year before laser treatment, coagulation disorders or anticoagulant treatment, history of keloid scarring, known allergy to topical lidocaine anesthetic, history of photosensitizing medications, or any cosmetic procedure in areas of treatment in the last 12 months were excluded from the study.
Technical data
The Er:YAG 2940 nm laser used in this study has a fractional handpiece (LOTUSII; Laseroptek Co., Ltd., Sungnam, Gyenggido, Korea). We used short pulse (350 μs) mode with a spot size of 7 mm2, fluence of 3.12 J/cm2, pulse energy of 1–1.2 J, and repetition rate of 3–5 Hz. The fractional CO2 10,600 nm laser (MIXEL; Hironic Co., Ltd., Sungnam, Korea) was used in the study with the power of 20–18 mJ/cm2, distance of 1 mm, and overlap 1 step with scattering operation mode.
Treatment protocol
The treatment area was thoroughly cleansed before the procedure with a gentle skin cleanser.
Five percent lidocaine ointment was applied to the entire facial area at least 30 min before the treatment. After wiping off the lidocaine with gauze, acetone was used to completely wipe it off. The patients were advised to keep their eyes closed, and the eyes were covered with a moist gauze held in place by an assistant during the entire procedure. On the basis of a randomization table that was generated by an external statistician not otherwise involved in the study, each half of the face has undergone a different laser resurfacing treatment. Laser therapy was done from the hairline to the chin. Zinc oxide ointment was applied to the treatment areas immediately after the procedure. Patients were instructed to gently cleanse their face with normal saline and to re-apply zinc oxide ointment as needed. Also, they were advised to stay away from direct sun exposure.
Patients were assigned to receive three monthly treatments on each side of the face, one with fractional CO2 laser and the other with fractional Er:YAG laser. Photographs were taken with a Canon Digital Camera (Power Shot S110 with 12.1 megapixel high-sensitivity CMOS sensor; Canon, Inc., Japan) at baseline, before each treatment session, and 3 months after the final treatment. Two board-certified dermatologists were asked to score the clinical outcome regarding the improvement of wrinkles, skin texture, and clinical appearance in a blinded fashion. The wrinkle improvement was calculated with the use of visual analog scale (VAS). Degree of clinical improvement was defined as the percentage of improvement: no response (less than 10%), mild response (10–25%), moderate response (25–50%), good response (50–75%), and excellent response (more than 75%). Outcomes were evaluated by investigators at each session and 3 months after the third treatment.
Patients were asked to specify their level of satisfaction to the statements in the questionnaire by marking a position along a continuous black line between two endpoints measuring 10 cm, which served as a visual analog scale (VAS). Patients were asked to come for check-up 1 week after the first treatment session, and all undesired effects of the procedures such as pain, erythema, edema, hypopigmentation, hyperpigmentation, scars, and atrophy were recorded. The severity of side effect was also assessed with the use of visual analog scale (VAS). We also asked the patient to declare the laser system that they have experienced more discomfort with.
Skin biomechanical properties
We used Multi-Probe Adaptor System (MPA 9; Courage & Khazaka Electronic GmbH, Köln, Germany) to assess skin biomechanical properties. MPA-9 has several handpieces to assess various skin biophysical properties such as stratum corneum hydration, skin erythema, trans-epidermal water loss (TEWL), and cutaneous resonance running time (CRRT). We have only measured cutaneous resonance running time (CRRT) with Reviscometer® RVM 600 handpiece that allows for the evaluation of the biomechanical properties of skin by measuring the propagation time of a shear wave between two sensors placed on the skin surface; one is transmitting an acoustical shockwave and the other is the receiver. The time the wave needs to propagate from transmitter to recipient is the measured parameter that is defined as cutaneous resonance running time (CRRT). It determines the mechanical properties of the skin and the direction of collagen and elastic fibers. The CRRT is expressed in arbitrary units (AU). CRRT is mainly influenced by collagen fibers in the papillary layers of dermis and correlates negatively with skin stiffness. Directional changes of CRRTs in the specific diseases or after skin procedures have been reported in some studies, which could reflect the dermal biomechanical property at various conditions [10, 11].
Two sensors are applied to the skin surface in supine position. The mean CRRT over the four axes (0°, 180°, 90°, and 270°) was calculated for the cheeks. These measurements were conducted at room temperature 24–26 °C with a relative humidity of 50 ± 3%. These measurements were recorded for each patient at baseline, before each treatment session, and 3 months after the final treatment.
Statistical analysis
All data were analyzed using the Statistical Package for Social Sciences (SPSS) program (version 20.0 for Windows). Comparison of outcome variables between any two timepoints was done by Wilcoxon signed-rank test and Mann–Whitney U test. Trend of measures for the grade of wrinkles as an ordinal variable was investigated using Friedman’ test statistic. The significance level was set at p <0.05. Descriptive statistics were also calculated (mean, standard deviation, median, minimum, maximum, numbers, percentage rate).
Results
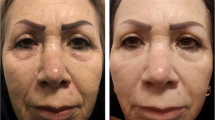
The mean age of the participants was 45.50 (+7.94) years. Standardized images of the full face taken at baseline and at each follow-up visits were evaluated. Among 40 female volunteers, 34 subjects completed the study, while 2 participants were lost at the third visit and 4 others did not come for the last follow-up visit. Mean wrinkle improvement for fractional Er:YAG laser 1 month after the first treatment, 1 month after the second treatment, and 3 months after the final treatment was 18.08 ± 4.55%, 28.91 ± 8.04%, and 40.45 ± 9.15%, respectively, with significant improvement in comparison with the baseline condition (p value < 0.001). Mean wrinkle improvement for fractional CO2 laser 1 month after the first treatment, 1 month after the second treatment, and 3 months after the final treatment was 19.03 ± 4.89, 29.97 ± 8.05, and 39.62 ± 8.6, respectively, with significant improvement in comparison with the baseline condition (p value < 0.001) (Table 1; Figs. 1 and 2). There was no significant difference in efficacy between two lasers 1 month after the first treatment, 1 month after the second treatment, and 3 months after the final treatment (p value > 0.05) (Fig. 3).
Three months after the final treatment, 12.5% of the sides treated with fractional CO2 laser and 15% of those treated with fractional Er:YAG laser showed “good response.” Moreover, 70% of the sides treated with fractional CO2 laser and 67.5% of those treated with fractional Er:YAG laser showed “moderate response” (Table 2). The patients showed considerable satisfaction with both laser methods with no statistically significant difference (p > 0.05) (Table 1).
Skin biomechanical properties
The mean CRRT at the baseline, before each treatment session, and 3 months after the final treatment are shown in Table 1. It showed a significant decrease of mean CRRT at each visit in comparison with the baseline measurements in both laser systems. Mean CRRT showed a significant decrease in both fractional CO2-treated site (p = 0.043) and fractional Er:YAG-treated site (p = 0.011) 3 months after the final treatment (Fig. 4). However, there was no significant difference in CRRT measurements between two lasers (Table 1).
Side effects
No serious or persistent complications, such as prolonged erythema, pain, dyspigmentation, and scarring, developed in the participants. Short-lasting adverse effects included erythema (up to 7 days) and edema (up to 7 days) on both sides with more intensity in the CO2-treated side. The most common adverse reaction was erythema in both lasers. The difference between two lasers was not statistically significant in the rate of adverse effect (Table 3). The frequency of mentioned post-procedure discomfort was 69.4% in fractional CO2-treated side versus 22.2% in fractional Er:YAG-treated side.
Discussion
Non-ablative fractional laser offers the potential benefits of full-surface skin resurfacing while minimizing adverse effects [12], but these laser systems could not show improvement as good as conventional ablative lasers. Therefore, it finally leads to the invention of ablative fractional devices. Fractional CO2 laser and fractional Er:YAG laser are two main ablative fractional laser devices used for skin rejuvenation. These procedures both seem to be effective, but sometimes they are painful and have significant downtime or adverse effects [13, 14]. However, limited data are available on comparing these modalities in regard to their efficacy and tolerability or side effects.
In this study, we performed a randomized controlled double-blinded trial in a split-face design comparing the efficacy and safety of fractional CO2 and fractional Er:YAG lasers on facial wrinkles on 40 volunteers in 3 treatment sessions. Previous data on the efficacy and safety of fractional CO2 and fractional Er:YAG lasers were mostly with a small number of patients and fewer treatment sessions. These limited studies also showed some controversies about the efficacy and safety of these methods [6, 14–16]. Karsai et al. conducted a split-face comparative trial of ablative fractional CO2 laser and ablative fractional Er:YAG laser in the treatment of periorbital rhytides. They showed both modalities have a roughly equivalent effect, while discomfort was slightly more pronounced after Er:YAG treatment in the first few days of treatment, but later on, there were more complaints following CO2 laser [6]. Alexiades-Armenakas et al. commented that fractional CO2 laser might show superior results but fractional Er:YAG laser is better tolerated with less downtime in acne scar patients [14]. Waibel et al. consider fractional CO2 laser treatment superior to fractional Er:YAG, but this conclusion was based on a limited number of patients and declared preliminary by the authors themselves [15]. Khatri et al. showed CO2 laser had relatively better wrinkle improvement, but subjects treated with Er:YAG laser recover more quickly [16].
However, our study did not show considerable difference between these resurfacing methods in the improvement of skin wrinkles in an experimental setting with randomized, blind allocation of treatment sites in a split-face design and an additive objective assessment of skin biomechanical property. Both laser systems showed significant improvement of skin wrinkles, and the efficacy of both methods was approximately equal. Both laser systems caused no serious long-standing side effects and seem to be well tolerated by the participants, but the discomfort was somewhat more pronounced after fractional CO2 laser.
Measurement of cutaneous resonance running time (CRRT) is a non-invasive approach to assess skin biophysical property. CRRT, which is mainly influenced by collagen fibers in the papillary layers of the dermis, correlates negatively with skin stiffness. It seems that CRRTs vary with age, body sites, and gender [17]. Some systemic diseases like diabetes or keratoconus could also affect CRRT values [10, 18]. It seems that these variations of CRRT values could give us some clues to assess skin biomechanical property more objectively. Therefore, we used CRRT assessment as an additive measure beside the clinical evaluation of laser efficacy. In our study, mean CRRT values decreased significantly after treatment in both laser groups. These changes in CRRT values could imply some alterations of skin stiffness and elasticity, but defining an exact relationship between these parameters is quite difficult. However, the alterations of CRRT after laser treatment could give use some additive objective clues for better assessment of laser efficacy in this study. Therefore, our study seems to be distinctive in the literature as a prospective, randomized study used skin biomechanical evaluation along with clinical assessment to compare the efficacy of fractional CO2 and fractional Er:YAG lasers in the treatment of facial skin wrinkles. It would be better if we could perform a skin biopsy 6 months after the procedures to assess the histopathological pattern of possible neocollagenesis. Unfortunately, none of the participants agreed to undergo skin biopsy procedure in this study.
There are some studies that indicate the considerable efficacy of fractional Er:YAG laser in skin resurfacing [19, 20], but we find no study that compares the efficacy and tolerability of this laser with the fractional CO2 laser in skin rejuvenation. However, there is one study in the literature that compares these laser methods in the treatment of atrophic acne scar. They indicate similar to our results that both laser systems are effective on improvement of atrophic acne scar with no significant difference, but the participants faced less discomfort and downtime with fractional Er:YAG laser [21]. In conclusion, we find in our study that both fractional CO2 and fractional Er:YAG lasers seem to be effective and safe in the treatment of facial skin wrinkles, but patients will experience less discomfort with fractional Er:YAG laser. Therefore, we suggest that fractional Er:YAG laser might be a more convenient option for skin rejuvenation with acceptable efficacy. However, future studies with larger sample size and histopathology evaluation of neocollagenesis after laser treatment would be more beneficial to elucidate any possible difference in the efficacy of fractional CO2 and fractional Er:YAG lasers in skin resurfacing.
References
Yaar M, Gilchrest BA (2007) Photoageing: mechanism, prevention and therapy. Br J Dermatol 157:874–87
El-Domyati M, Attia S, Saleh F, Brown D, Birk DE, Gasparro F, Ahmad H, Uitto J (2002) Intrinsic aging vs. photoaging: a comparative histopathological, immunohistochemical, and ultrastructural study of skin. Exp Dermatol 11:398–405
Kim BJ, Choi JH, Lee Y (2015) Development of facial rejuvenation procedures: thirty years of clinical experience with face lifts. Arch Plast Surg 42:521–31
Riggs K, Keller M, Humphreys TR (2007) Ablative laser resurfacing: high-energy pulsed carbon dioxide and erbium:yttrium-aluminum-garnet. Clin Dermatol 25:462–73
Hunzeker CM, Weiss ET, Geronemus RG (2009) Fractionated CO2 laser resurfacing: our experience with more than 2000 treatments. Aesthet Surg J 29:317–22
Karsai S, Czarnecka A, Jünger M, Raulin C (2010) Ablative fractional lasers (CO(2) and Er:YAG): a randomized controlled double-blind split-face trial of the treatment of peri-orbital rhytides. Lasers Surg Med 42:160–7
Jung KE, Jung KH, Park YM, Lee JY, Kim TY, Kim HO, Kim HS (2013) A split-face comparison of ablative fractional lasers (CO(2) and Er:YAG) in Asian patients; postprocedure erythema, pain and patient’s satisfaction. J Cosmet Laser Ther 15:70–3
Trelles MA, Mordon S, Velez M, Urdiales F, Levy JL (2009) Results of fractional ablative facial skin resurfacing with the erbium:yttrium-aluminium-garnet laser 1 week and 2 months after one single treatment in 30 patients. Lasers Med Sci 24:186–94
Fleming D (1999) Controversies in skin resurfacing: the role of erbium. J Cutan Laser Ther 1:15–21
Robati RM, Einollahi B, Einollahi H, Younespour S, Fadaifard S (2016) Skin biophysical characteristics in patients with keratoconus: a controlled study. Scientifica (Cairo) 2016:6789081
Robati RM, Abdollahimajd F, Robati AM (2015) Evaluation of subcision for the correction of the prominent nasolabial folds. Dermatol Res Pract 2015:976153
Dierickx CC, Khatri KA, Tannous ZS, Childs JJ, Cohen RH, Erofeev A, Tabatadze D, Yaroslavsky IV, Altshuler GB (2008) Micro-fractional ablative skin resurfacing with two novel erbium laser systems. Lasers Surg Med 40:113–23
Hantash BM, Bedi VP, Kapadia B, Rahman Z, Jiang K, Tanner H, Chan KF, Zachary CB (2007) In vivo histological evaluation of a novel ablative fractional resurfacing device. Lasers Surg Med 39:96–107
Alexiades-Armenakas MR, Dover JS, Arndt KA (2008) The spectrum of laser skin resurfacing: nonablative, fractional, and ablative laser resurfacing. J Am Acad Dermatol 58:719–37
Waibel J, Beer K, Narurkar V, Alster T (2009) Preliminary observations on fractional ablative resurfacing devices: clinical impressions. J Drugs Dermatol 8:481–5
Khatri KA, Ross V, Grevelink JM, Magro CM, Anderson RR (1999) Comparison of erbium:YAG and carbon dioxide lasers in resurfacing of facial rhytides. Arch Dermatol 135:391–7
Xin S, Man W, Fluhr JW, Song S, Elias PM, Man MQ (2010) Cutaneous resonance running time varies with age, body site and gender in a normal Chinese population. Skin Res Technol 16:413–21
Seirafi H, Farsinejad K, Firooz A, Davoudi SM, Robati RM, Hoseini MS, Ehsani AH, Sadr B (2009) Biophysical characteristics of skin in diabetes: a controlled study. J Eur Acad Dermatol Venereol 23:146–9
Lee HM, Haw S, Kim JE, Won CH, Lee MW, Choi JH, Chang SE, Kim YJ, Goo BL (2012) A fractional 2940 nm short-pulsed, erbium-doped yttrium aluminium garnet laser is effective and minimally invasive for the treatment of photodamaged skin in Asians. J Cosmet Laser Ther 14:253–9
El-Domyati M, Abd-El-Raheem T, Medhat W, Abdel-Wahab H, Al Anwer M (2014) Multiple fractional erbium: yttrium-aluminum-garnet laser sessions for upper facial rejuvenation: clinical and histological implications and expectations. J Cosmet Dermatol 13:30–7
Manuskiatti W, Iamphonrat T, Wanitphakdeedecha R, Eimpunth S (2013) Comparison of fractional erbium-doped yttrium aluminum garnet and carbon dioxide lasers in resurfacing of atrophic acne scars in Asians. Dermatol Surg 39(1 Pt 1):111–20
Acknowledgements
This paper has been extracted from the dermatology residency thesis written by Dr. Elmira Asadi in School of Medicine, Shahid Beheshti University of Medical Sciences (registration no. 528).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Clinical trial registration number: IRCT ID: 2014122820468N1
Rights and permissions
About this article
Cite this article
Robati, R.M., Asadi, E. Efficacy and safety of fractional CO2 laser versus fractional Er:YAG laser in the treatment of facial skin wrinkles. Lasers Med Sci 32, 283–289 (2017). https://doi.org/10.1007/s10103-016-2111-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-016-2111-8